Arthroscopic cartilage regeneration facilitating procedure for osteoarthritic knee
|
|
|
- Moses Kelly
- 5 years ago
- Views:
Transcription
1 Arthroscopic cartilage regeneration facilitating procedure for osteoarthritic knee Lyu et al. Lyu et al. BMC Musculoskeletal Disorders 2012, 13:226
2 Lyu et al. BMC Musculoskeletal Disorders 2012, 13:226 TECHNICAL ADVANCE Open Access Arthroscopic cartilage regeneration facilitating procedure for osteoarthritic knee Shaw-Ruey Lyu 1,3*, Chia-Chen Hsu 1 and Chih-Wen Lin 2,3 Abstract Background: The effectiveness of arthroscopic treatment for osteoarthritic knee is a controversy. This study presents the technique of a novel concept of arthroscopic procedure and investigates its clinical outcome. Method: An arthroscopic procedure targeted on elimination of focal abrasion phenomenon and regaining soft tissue balance around patello-femoral joint was applied to treat osteoarthritis knees. Five hundred and seventy-one knees of 367 patients with osteoarthritis received this procedure. There were 70 (19%) male and 297 (81%) female and the mean age was 60 years (SD 10). The Knee Society score (KSS) and the knee injury and osteoarthritis outcome score (KOOS) were used for subjective outcome study. The roentgenographic changes of femoral-tibial angle and joint space width were evaluated for objective outcomes. The mean follow-up period was 38 months (SD 3). Results: There were 505 knees in 326 patients available with more than 3 years follow-up and the mean follow-up period was 38 months (SD 3). The subjective satisfactory rate for the whole series was 85.5%. For 134 knees with comprehensive follow-up evaluation, the KSS and all subscales of the KOOS improved statistically. The femoral-tibial angle improved from 1.57 degrees (SD 3.92) to 1.93 degrees (SD 4.12) (mean difference: 0.35, SD 0.17). The joint space width increased from 2.02 millimeters (SD 1.24) to 2.17 millimeters (SD 1.17) (mean difference: 0.13, SD 0.05). The degeneration process of the medial compartment was found being reversed in 82.1% of these knees by radiographic evaluation. Conclusions: Based on these observations arthroscopic cartilage regeneration facilitating procedure is an effective treatment for osteoarthritis of the knee joint and can be expected to satisfy the majority of patients and reverse the degenerative process of their knees. Keywords: Osteoarthritis, Knee, Medial plica, Arthroscopy, Cartilage, Regeneration Background Osteoarthritis (OA) of the knee affects a large population worldwide and is associated with an extremely high economic burden largely attributable to the effects of disability, comorbid disease, and the expense of treatment [1]. To date the established therapies have been directed towards symptom control. Since the initiating events that result in the cartilage degradation are poorly understood, there has been very limited success in demonstrating disease modification in clinical trials of potential therapies [2]. Arthroscopy for the management of OA knees, as a relative minor procedure, is popular in spite of the * Correspondence: srlyu@seed.net.tw 1 Joint Center, Buddhist Dalin Tzu Chi General Hospital, 2, Min-Shen Road, Chiayi 62247, Taiwan 3 Tzu Chi University, Hualien, Taiwan Full list of author information is available at the end of the article controversy concerning its effectiveness. Joint lavage [3,4], debridement [5-7], abrasion arthroplasty [7-11], and microfracture [12-14] are among the most commonly employed arthroscopic procedures for OA knees. The precise mechanism and consensus by which these procedures improve the course of degenerative conditions of the knee have not been established. A recent retrospective review of the current literature on the arthroscopic treatment of OA knee [15] has demonstrated limited evidence-based research to support the use of arthroscopy as a treatment method for OA knee. In 2008, a concept of arthroscopic medial release (AMR) for the treatment of osteoarthritis of the medial compartment of the knee joint was reported [16]. The clinical outcome of this series lured us to believe that, by eradication of the abrasion phenomenon between the tight, fibrotic and hypertrophied medial structure and 2012 Lyu et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
3 Lyu et al. BMC Musculoskeletal Disorders 2012, 13:226 Page 2 of 10 the adjacent medial femoral condyle, the pain of most patients could be reduced and the degenerative process in the medial compartment of these patients might be decelerated or arrested. In this report, we propose a concept of arthroscopic cartilage regeneration facilitating procedure (ACRFP) that combines arthroscopic medial release (AMR), percutaneous lateral release (PLR) and conventional debridement as a rationale for the deliberate arthroscopic management of OA knee. We hypothesized that the elimination of the detrimental factors including synovitis, chondral flaps, and abnormal focal stress caused by medial abrasion and lateral compression phenomena will provide a preferable environment for the regeneration of damaged cartilage. The details of this procedure and its clinical results are reported in this study. Methods The patients In a one-year duration, 571 knees of 367 patients with different grades of OA received this procedure. There were 78 (19%) male and 330 (81%) female. The age ranged from 29 to 82. The mean age of these patients at the time of surgery was 60 (SD 10). There were 406 knees (80.4%) of 269 patients received AMR and 99 knees (19.6%) of 57 patients received AMR+PLR. The anteroposterior standing and Merchant s axial radiographs were evaluated for the severity of degeneration for each compartment. The radiographic grading of each compartment according to Kellgren and Lawrence [17] was given by the senior author who was thesinglesurgeonperformedalloftheprocedures.the inclusion criteria were patients with OA knee of any grade involving medial compartment or combined with patellofemoral compartment and have been treated conservatively including non-steroidal anti-inflammatory drugs, nutrition supplements (glucosamine sulfate and/or hyaluronic acid injection) and physiotherapy for more than six months. The exclusion criteria were apparent lateral compartment OA (radiographic grading of III or IV or arthroscopic grading of III or IV by modified Outerbridge classification [18]), instability due to previous ligament injury, major meniscus tear, or OA due to trauma. This study was approved by the Research Ethics Committee of Buddhist Dalin Tzu-Chi General Hospital, which has been certificated by the Department of Health, Taiwan (IRB Approval Number: B ). Informed consents were obtained from all patients participating in the study. Radiographic Protocol The standing extended anteroposterior radiographs of the knee were obtained at 55 KV with a focus of 1.25 mm 2 and a focus-to-film distance of 100 cm, using cm computed radiographic film (Kodak Digital Science, CR 400). Radiographs of the extended knee were obtained with the patella in central position [19]. To assess the patellofemoral joint space, Merchant s view was obtained at 45 degrees of knee flexion with X-ray beam projected caudad at 30 degrees. For magnification correction in each examination, a 4.0-mm steel ball was affixed to the skin over the head of the fibula (standing extended AP view) and center of patella (Merchant s view) to permit correlation of the joint space width measurements [20]. Surgical procedure All procedures were performed under spinal or general anesthesia. Bloodless surgical field was obtained by pneumatic tourniquet. A 4 milimeters 30 degrees arthroscope with 6.5 milimeters sheath was used. An electronic shaver and hand instruments were used as necessitated. Arthroscopic examination Through inferolateral portal, routine arthroscopic examination was performed. Special attention was given to the presentation of medial plica related medial abrasion phenomenon or focal synovitis over the inferomedial region of the patella (Figure 1A). The tightness and balance of patellofemoral joint was then evaluated (Figure 1B, C). If the medial or lateral facet could not be easily passed by the scope, it was recognized as over-tightness. Patients having apparent lateral compartment OA (grade III or IV by modified Outerbridge classification), major meniscus tear which needs partial meniscectomy or instability due to ligament injury were excluded from this study. Medial release For the knees with medial abrasion phenomenon (Figure 1A), medial release [16] (Additional file 1: Video 1) was performed to eradicate the inflammatory tissue occupying the space over the inferomedial region of the patella including ligamentum mucosum, fibrotic or inflamed synovium, capsule and distal part of the medial plica. The tight and obliterated medial facet of patellofemoral joint (Figure 1B) was then released by resection of the fibrotic synovium, capsule and proximal part of the medial plica (Figure 1D). Sometimes, medial retinaculum including fibrotic fascia of pes anserinus should be released. The adequacy of the medial release was checked by passing the tip of the scope under the patella and verified if the previously tightly closed medial patellofemoral joint space could be easily opened and the medial retinaculum visualized when the knee was put in full extension position (Figure 1E). Percutaneous lateral release For the knees with lateral compression syndrome (Figure 1C), lateral release was performed by inserting the No.11scalpelintotheinferolateralportalandcutthelateral retinaculum percutaneously. The extent and adequacy of the release could be evaluated by direct vision through arthroscope (Figure 1F).
4 Lyu et al. BMC Musculoskeletal Disorders 2012, 13:226 Page 3 of 10 active range of motion and quadriceps strengthening, were emphasized. No supplementary treatment including oral glucosamine sulfate, steoid injection or intraarticular injection of hyaluronic acid was given during the whole post-operative follow-up period. Follow-up and evaluation of clinical outcome The patients were evaluated monthly for three months. Thereafter, they came back yearly for outcome assessment. The comparisons of both pre- and post-operative Knee Society score (KSS) and knee injury and osteoarthritis outcome score (KOOS) were used for outcome evaluation. Subjective satisfaction was assessed by direct question using a categorical scale prepared for this study: excellent, free of symptoms, no limitation in activities; good, greatly improved, occasional pain, normal activities; fair, same as pre-operative condition, no improvement; and poor, has received or considered further operative treatment. The outcome was regarded as satisfactory if subjective satisfaction was rated as excellent or good. The inquiry into subjective satisfaction and the evaluation of KSS and KOOS were conducted by nursing specialists. All investigations focused on individual knees in bilateral cases. Figure 1 Different stages of ACRFP. A, typical presentation of medial abrasion phenomenon, the space between patella (P) and medial femoral condyle (MFC) was occupied by fibrotic media plica (MP) and inflammatory synovium (S); B, before medial release, the space between patella (P) and medial femoral condyle (MFC) was tight; C, before lateral release, the space between patella (P) and lateral femoral condyle (LFC) was tight; D, after eradication of medial abrasion syndrome, medial gutter (MG) could be clearly visualized; E, after medial release, the medial facet of the patellofemoral joint was opened and the medial retinaculum (MR) could be visualized; F, after lateral release, the space between patella (P) and lateral femoral condyle (LFC) was opened. Synovectomy and chondroplasty Any focal synovitis or loose chondral flaps on the cartilaginous surface was removed as conventional arthroscopic debridement for osteoarthritis of the knee. At the end of the procedure, thorough irrigation was performed to remove any debris in the knee joint. No bony procedure such as drilling or microfracture was performed. Post-operative management Suction drain was used for 24~48 hours. The involved limb was protected by elastic bandage for one week. Full range of motion, full weight bearing and free ambulation were allowed as tolerated. The patient was discharged 2 days after the operation. Home exercise programs, including Evaluation of x-ray outcome The radiographic outcome was interpreted by comparing the pre-operative standing extended anteroposterior and Merchant s views with the ones taken at the last visit by digitized assessment (Image-Pro, Media Cybernetics, Inc., Bethesda, MD, USA). The interpreting parameters include: femoral-tibial angle (FTA), minimum joint space width (MJSW) [21], lateral tilt angle of patella [22], and the surface contour of the joint lines. Simplified outcomes of better, the same or worse was given to each knee after evaluation of the pre- and post-operative radiographs. The anatomic axis (femoral-tibial angle) was defined as the angle formed by the intersection of 2 lines originating from points bisecting the femur and tibia and converging at the center of the tibial spine tips [23]. The same radiologist performed these measurements and interpretations. Statistical analysis All values were presented with means and standard deviations. Comparisons were made using one-way analysis of variance (ANOVA) to detect differences in the distribution of patient age in each grade of osteoarthritis. Statistical analysis for comparing preoperative and postoperative KSS, KOOS, femoral-tibial angle, and joint space width was performed using the paired t test. P < 0.05 was considered to be statistically significant. All statistical analysis was carried out using JMP, the Statistical Discovery Software (Version , SAS Institute Inc., Cary, NC, USA).
5 Lyu et al. BMC Musculoskeletal Disorders 2012, 13:226 Page 4 of 10 Results There were 505 knees in 326 patients available with more than 3 years follow-up and the mean follow-up period was 38 months (SD 3). Ten of 59 knees (16.9%) with grade I osteoarthritic knees in six patients; twentyfive of 235 knees (10.6%) with grade II osteoarthritis in fifteen patients, twenty-six of 233 knees (11.2%) with grade III osteoarthritis in seventeen patients, and five of 44 knees (11.4%) with grade IV osteoarthritis in three patients were lost to follow-up. The total follow-up rate was 88.5%. One hundred and thirty-four knees returned and completed thorough outcome study including x-ray examination, KSS and KOOS evaluation. Another 371 knees completed the subjective outcome evaluation by telephone questionnaires. All of the knees were found to have the structure of pathologic medial plica. The mean age of these patients at the time of surgery was 60 (SD 10). ThemeanageanddistributionofdifferentgradeofOA stratified by the procedure they received were shown in Table 1. There were 406 knees (80.4%) of 269 patients received AMR and 99 knees (19.6%) of 57 patients received AMR+PLR. The mean age of the patients were positively correlated with the severity of OA by ANOVA in both surgical groups. In the group received AMR+PLR, the F/ M ratios were more prominent compared to that of the AMR group. Post-operative Complications Hematoma Hematoma with ecchymosis around the involved knee occurred in 16 knees (3.9%) in ten patients in AMR group and 8 knees (8.1%) in five patients in AMR+PLR group. All subsided uneventfully within one month. Persistent effusion Nine knees (2.2%) in seven patients in the AMR group and 4 knees (4%) in three patients in the AMR+PLR group experienced persistent effusion for more than one month after this procedure. After initial treatment including resting, compression bandaging and anti-inflammatory medication, the effusion subsided spontaneously within 2 weeks in 8 knees. The other 5 knees in three patients required aspiration of the knee to relieve the discomfort. Wound irritation Irritable pain, catching or giving way sensation when moving the involved knees were commonly complained during the first post-operative month. This discomfort was tolerable in most patients after reassurance and would usually subside spontaneously. In 13 knees (2.6%) of 13 patients there was persistent discomfort due to wound irritation for more than three months. After conservative treatment including local heat, massage, and stretching exercise by bending knee passively, all alleviated within one year. Outcome Of the 505 knees available for final review the subjective assessment was satisfactory in 432 (85.5%). Statistically it was less satisfactory in grade IV knees (59%) compared to other grades. In the AMR+PLR group, it was less satisfactory in grade III and IV knees compared to earlier grades (Table 2). For the 134 knees received in-depth outcome studies, the Knee Society pain scores statistically improved from 49.9 (SD 13.5) to 81.0 (SD 12.6) (p<0.001) in the AMR group and 53.0 (SD 11.0) to 76.7 (SD 16.1) (p<0.001) in the AMR+PLR group. The Knee Society function scores statistically improved from 53.5 (SD 15.3) to 71.1 (SD 14.4) (p<0.001) in the AMR group and 57.1 (SD 10.7) to 69.5 (SD 18.2) (p<0.001) in the AMR+PLR group (Table 3). All subscales of KOOS also improved statistically (Table 4). The FTA improved from 1.57 (SD 3.9) to 1.93 (SD 4.1) (p=0.03) and the JSW increased from 3.02 (SD 1.24) to 3.17 (SD 1.17) (p=0.01). The tilt angle of the patella decreased from 11.8 (SD 5.1) to 6.9 (SD 4.4) (p<0.0001) in the AMR+PLR group (N=29). The radiographic outcome revealed reversal of the degeneration process over the medial compartment in 82.1% of these knees (N=134) and 93.1% of the patellofemoral joint in the AMR+PLR group (N=29) (Table 5). Table 1 Age and sex distribution of different grade of medial compartment OA stratified by type of surgery AMR AMR + PLR Total Stage Age /No. F/M (Ratio) Age /No. F/M (Ratio) Age /No. F/M (Ratio) I 52 (9)/37 30/7 (4.3) 55 (10)/12 11/1 (11)* 53 (9)/49 41/8 (5.1) II 58 (11)/ /40 (3.1) 59 (11)/47 43/4 (10.8)* 58 (11)/ /44 (3.8) III 64 (8)/ /23 (6.4) 63 (5)/37 32/5 (6.4) 64 (7)/ /28 (4.6) IV 62 (7)/36 30/6 (5.0) 66 (1)/3 3/0 (NA)* 62 (7)/39 33/6 (5.5) Total 60 (9)/ /76 (4.3) 64 (11)/99 89/10 (8.9)* 60 (10)/ /86 (4.9) p<0.0001, R 2 =0.15 p=0.019, R 2 =0.07 p<0.0001, R 2 =0.13 * Statistically significant compared to that of the AMR group by comparisons for each pair using paired t test (p<0.05).
6 Lyu et al. BMC Musculoskeletal Disorders 2012, 13:226 Page 5 of 10 Table 2 Subjective outcomes of different grade of medial compartment OA stratified by type of surgery Grade AMR (N=406) AMR + PLR (N=99) Total E G F P Sat. (%) E G F P Sat. (%) (%) I 29 (78.4) 3 (8.1) 3 (8.1) 2 (5.4) (50) 5 (41.7) 0 (0) 1 (8.3) II 104 (63.8) 38 (23.3) 16 (9.8) 5 (3.1) (72.4) 11 (23.4) 1 (2.1) 1 (2.1) III 84 (49.4) 66 (38.8) 11 (6.5) 9 (5.3) (54.1) 9 (24.3) 4 (10.8) 4 (10.8) 78.4* 86.5 IV 15 (41.7) 8 (22.2) 4 (11.1) 9 (25) 63.9* 0 (0) 0 (0) 1 (33.3) 2 (66.7) 0* 59.0* Total 232 (57.1) 115 (28.3) 34 (8.4) 25 (6.2) (60.6) 25 (25.2) 6 (6.1) 8 (8.1) E excellent, G good, F fair, P poor, Sat.: satisfied = E + G. * Statistically significant by comparisons for each pair using paired t test (p<0.05). Evidence of Cartilage Regeneration In addition to the indirect evidence provided by radiographic images shown in Figures 2, 3, and 4, we had a chance to visualize the regeneration of a chondral defect when performing a second-look arthroscopy for a patient who suffered from hemoarthrosis due to an accident 3 years after the initial ACRFP for grade II osteoarthritis over the medial compartment of her right knee. The subjective outcome of her initial ACRFP was excellent (the Knee Society pain scores improved from 55 to 95, the Knee Society function scores improved from 35 to 80 and all subscales of KOOS also improved significantly: P- 36 to 94; S- 39 to 71; ADL- 53 to 97; S/R- 10 to 75; QOL- 6 to 88) and the degenerative medial compartment did not show any progression after the initial management according to her radiographic images (Figure 5, Additional file 2: Video 2). Discussion In this report we present the clinical and radiographic outcomes of our procedure of arthroscopic cartilage regeneration facilitating procedure (ACRFP) for OA knees involving mainly medial and patellofemoral compartments. Overall, the subjective satisfactory rate was 85.5%. Even in grade IV OA, 59% of satisfactory rate could be anticipated after at least 3 years follow-up. Besides the improvement of clinical symptoms and life quality according to the KSS and KOOS surveys, revitalizing of the degenerated cartilage and reversal of the degeneration process were perceived in 81.2% of the knees by radiographic evaluation. Therapeutic arthroscopic techniques including lavage, debridement, abrasional chondroplasty and microfracture are widely used for OA knee despite their unpredictable outcomes. A double-blinded, randomized, placebocontrolled trial to compare the effectiveness of arthroscopic lavage and arthroscopic debridement versus a sham procedure has been performed and the data suggest that the benefits of arthroscopy for the treatment of osteoarthritis of the knee are to provide subjective pain relief via a placebo effect [24]. The American Academy of Orthopaedic Surgeons (AAOS) clinical practice guideline on the treatment of OA knee also recommends against performing arthroscopy with debridement or lavage in patients with a primary diagnosis of symptomatic OA of the knee [25]. Dandy s abrasion chondroplasty [26] was popularized in the late 1980s. In 1993, Bert et al. found it appears to offer little benefit over partial meniscectomy and debridement in the degenerative knee [8]. It was also thought that this technique provide unpredictable results. Concerns include the durability of the fibrocartilage repair tissue and thermal damage to subchondral bone and adjacent normal articular cartilage during this procedure [27]. Microfracture, a modification of chondroplasty, might provide increase in joint space by growth of fibrocartilage Table 3 Pre-operative and post-operative knee society score for different grade of medical compartment OA AMR (N=105) AMR + PLR (N=29) Grade Pain Function Pain Function Pre-op. Post-op. Pre-op. Post-op. Pre-op. Post-op. Pre-op. Post-op. I 37.7 (18.8) 92.3 (13.3) 48.3 (20.2) 78.3 (20.2) II 53.0 (12.6) 84.1 (9.9) 54.0 (14.6) 73.2 (14.3) 53.6 (9.8) 80.7 (16.4) 56.6 (11.1) 71.6 (19.7) III 47.8 (13.6) 76.4 (12.4) 53.7 (16.1) 68.7 (13.1) 52.8 (14.2) 69.8 (14.1) 57.8 (10.9) 65.0 (15.8) IV 43.3 (12.8) 76.4 (20.6) 51.1 (16.9) 65.6 (18.1) 44.0 (N=1) 64.0 (N=1) 60.0 (N=1) 70.0 (N=1) Total 49.9 (13.5) 81.0 (12.6) 53.5 (15.3) 71.1 (14.4) 53.0 (11.0) 76.7 (16.1) 57.1 (10.7) 69.5 (18.2) P value <0.001 <0.001 <0.001 <0.001
7 Lyu et al. BMC Musculoskeletal Disorders 2012, 13:226 Page 6 of 10 Table 4 Pre-operative and post-operative KOOS of different grade of medial compartment OA P S ADL S/R QOL Grade (N) Pre-op. Post-op. Pre-op. Post-op. Pre-op. Post-op. Pre-op. Post-op. Pre-op. Post-op. I (3) 68.3 (1.2) 69.3 (9.8) 73.0 (13.9) 61.7 (4.0) 58.3 (5.8) 74.7 (11.0) 58.7 (7.5) 53.3 (11.6) 55.3 (11.9) 73.0 (3.5) II (75) 66.9 (18.9) 81.2 (14.9) 62.0 (20.0) 71.0 (15.9) 80.0 (16.5) 86.8 (13.3) 53.2 (31.5) 65.4 (25.1) 56.5 (22.7) 64.7 (18.8) III (46) 52.8 (21.0) 75.2 (15.8) 50.0 (18.8) 64.7 (16.3) 65.7 (20.0) 80.1 (16.5) 32.2 (26.7) 49.8 (26.6) 42.4 (20.1) 57.1 (21.6) IV (10) 49.0 (24.5) 74.6 (15.8) 49.6 (23.3) 65.4 (21.6) 69.7 (19.7) 77.9 (22.7) 33.5 (27.4) 55.5 (32.9) 35.7 (26.0) 55.1 (24.1) Total (134) 60.8 (21.0) 78.4 (15.4) 57.2 (20.6) 68.2 (16.5) 73.9 (19.1) 83.5 (15.5) 44.6 (30.9) 59.0 (26.8) 50.1 (23.0) 61.6 (20.3) P value <0.001 <0.001 <0.001 <0.001 <0.001 and achieve functional improvement for patients with fullthickness chondral defects in the osteoarthritic knees [28]. But an evidence-based systematic analysis declared that this technique could only provide short-term functional improvement. Shortcomings of this technique include limited hyaline repair tissue, variable repair cartilage volume and possible functional deterioration [12]. Autologous chondrocyte implantation (ACI) has become an accepted option for the treatment of chondral defects in carefully selected patients. Current recommendations limit this procedure to younger patients, as insufficient data are available to conclusively evaluate outcomes in patients older than 45 years, especially in OA patients [29]. The unconfirmed pathogenesis of OA knee and a lack of a clear consensus on the indications and surgical techniques as well as the variable outcomes make these commonly used arthroscopic techniques remain a source of controversy. Abrasion or impingement phenomenon between the medial plica and the opposite medial femoral condyle has been described in recent studies in patients with medial compartment OA knee [30-33]. The consequent study [34] found that the repeated injuries elicited by this abrasion phenomenon might trigger IL-1ß production, thus enhance the expression of MMP-3. Their demonstration of the expression of IL1-ß mrna, MMP-3 mrna and MMP-3 in medial plica of early stage OA knee suggests that this structure and its interplay with the facing medial femoral condyle might play an important role in the pathogenesis of medial compartment OA knee. These findings coincide with the fact that eradication of this structure by arthroscopic release could be effective in symptom relief or even might modify the disease process of medial compartment OA knees [16,35]. Based on these constitutional studies, we proposed a concept that by a purposeful eradication of all prejudicial factors in the degenerative knee, the jeopardized cartilage would have the chance to regenerate by its innate healing response. In comparison with the uncertain beneficial mechanism and the diversity of outcomes of current popular arthroscopic techniques for osteoarthritis of the knee, our concept of ACRFP had more precise rationale of treatment. The main theme of ACRFP was to remove any abnormal abrasion or impingement phenomenon and reestablish soft tissue balance around the patellofemoral joint. For knees demonstrating medial abrasion phenomenon, medial release [16] was performed to relief the tension and abrasion between the tight, fibrotic and hypertrophied medial plica and the adjacent medial femoral condyle. On the other hand, in knees demonstrating lateral compression syndrome over patellofemoral joint, percutaneous lateral capsular release that has the benefits of tension release and denervation [36-40] was added. The immediate effect of ACRFP was obtained by releasing the tension around patella caused by chronically inflamed soft tissue and by eradication of the hypertrophied and inflamed synovium that may cause pain in these degenerative knees over the medial compartment and patellofemoral joint. Furthermore, by eliminating these stress/inflammatory responses that are the key events on the onset and progression of osteoarthritis, this procedure would also Table 5 Radiographic outcome of different grade of medial compartment OA stratified by type of surgery Medial compartment (AMR and AMR+PLR, N=134) PF compartment (AMR+PLR, N=29) Grade Better Same Worse Rev. NC* Better Same Worse Rev. NC I 0 3 (100) 0 3 (100) II 26 (33.9) 38 (51.8) 11 (14.3) 64 (85.3) 19 (100) (100) III 24 (51.4) 11 (24.3) 11 (24.3) 35 (76.1) 7 (77.8) 0 2 (22.2) 7 (77.8) IV 5 (62.5) 3 (22.2) 2 (25.0) 8 (80.0) 1 (100) (100) Total 55 (41.0) 55 (41.0) 24 (18.1) 110 (82.1) 27 (93.1) 0 2 (6.9) 27 (93.1) * Reverse natural course = Better + Same.
8 Lyu et al. BMC Musculoskeletal Disorders 2012, 13:226 Page 7 of 10 Figure 2 An example of reversal of natural degenerative course by ACRFP. A 70 years old male patient having grade IV OA over his right knee: A, pre-operative standing AP view showing grade IV OA over medial compartment of right knee; B, three years after ACRFP, the joint space reopened, the FTA improved from 7 degrees varus to 3 degrees varus. bring forth to long-term favorable effects as a consequence of the global improvement of the environment of the knee joint for cartilaginous regeneration. Although articular hyaline cartilage was classically considered having no or low potential for regeneration [41-46], some still thought that it does have the capacity to grow and remodel extensively during pre- and postnatal development and after trauma [47,48]. Both direct and indirect evidence of articular cartilage regeneration have been reported after correction of varus deformity for osteoarthritis of the knee by some authors. According to their investigations about the beneficial effects of valgus osteotomy for medial gonarthrosis, the main repair feature was proliferation of fibrocartilage, which covered bone and areas of fibrillated cartilage and filled vertical clefts in hyaline cartilage. The hyaline cartilage was found to show an increased cellularity with numerous nests of proliferating chondrocytes [49]. There was also arthroscopic visible improvement of the articular surface after this procedure [50]. Moreover, it was observed by direct vision that mature regeneration was more frequently found in the knees with radiographic increased width of the medial joint space after high tibial valgus osteotomy, and this even happened in the knees with eburnation of the subchondral bone [51]. Recent studies also point out that, unlike the first impression of a more or less static tissue, articular cartilage shows a slow turnover. Anabolic and catabolic pathways were thought to be very much intermingled in articular cartilage metabolism [52]. Under normal conditions, chondrocytes maintain the dynamic equilibrium between synthesis and degradation of extracellular matrix components. In osteoarthritic states, however, there is a disruption of matrix equilibrium leading to progressive loss of cartilage tissue [53]. Thus, the aim of osteoarthritis therapy might neither to stimulate anabolism nor to knock down catabolism, but to titrate the balance of anabolic-catabolic activities. In this study, the clinical outcomes and the radiographic findings have given light to us that, by removal of all existed catabolic factors, the anabolism of Figure 3 Another example of reversal of natural course by ACRFP. A, AP standing view of a 58 years old female patient having bilateral grade IV OA with subluxation of medial femoral condyle; B, three years after ACRFP, obvious improvement of the radiographic manifestation could be observed.
9 Lyu et al. BMC Musculoskeletal Disorders 2012, 13:226 Page 8 of 10 Figure 4 An example of self-comparison showing the benefit of ACRFP. A, pre-operative AP standing view of a 61 years old male with grade III OA over medial compartment of right knee and grade II OA over medial compartment of left knee. ACRFP was performed for his right knee; B, 46 months later, he came back due to marked disability over his left knee, the condition of his right knee was excellent. The degenerative process over the right knee is ceased compared to the progressively degenerated left knee; and, C, unicompartmental arthroplasty should be performed for his left knee. the damaged cartilage might become dominant and regeneration unveiled. Although it was claimed that compared with the extended weight-bearing anterior-posterior (AP) radiograph, posteroanterior (PA) imaging of the knee in degrees flexion (the schuss position) increases the reproducibility of radiographic JSW measurements in OA knees [21], standing AP radiographic views of the knee have still been widely used to determine the rate of disease progression in OA knee by measuring joint space Figure 5 Evidence of cartilage regeneration by second-look arthroscopy. Cartilage regeneration demonstrated in the medial compartment of the left knee of a 56 years old lady having stage II OA: A, cartilage erosion was found over the medial femoral condyle opposite the removed pathologic medial plica; B, the defect was found regenerated during the second-look arthroscopy 3 years later when the same knee suffered from hemoarthrosis after a falling down accident; C and D, The grade II degenerative medial compartment did not show any progression.
10 Lyu et al. BMC Musculoskeletal Disorders 2012, 13:226 Page 9 of 10 narrowing and bony alignment [21,54-59]. Contrary to our observation, they all obtained the common finding of progressive narrowing of the joint space as the natural course of OA knee. Never the less, in order to get more convincing evidence, we need more precise methodology such as magnetic resonance images study for the evaluation of cartilage regeneration. Properly conducted randomized control clinical trials are also warranted. Conclusions According to the experience of performing this procedure, the data support our contention that arthroscopic cartilage regeneration facilitating procedure (ACRFP) is a good modality for the treatment of osteoarthritis of the knee joint if only medial and/or patellofemoral joint were involved. It could modify the natural course of this common disease. This novel concept of treatment might give hope to the majority of patients who are in the ambiguous stages of OA knee before arthroplasty could be beneficial for them. Additional files Additional file 1: Video 1. Arthroscopic medial release for medial abrasion phenomenon. An example of stage III medial compartment osteoarthritic knee with medial abrasion phenomenon treated by arthroscopic medial release is shown in this video clip. This is a 78 years old female suffering from left knee pain for more than 10 years. The arthroscopic examination revealed tightness of the medial facet of the patellofemoral joint and obliteration of the inferomedial region of the patella by hypertrophied medial plica and synovitis tissue. The abrasion phenomenon between fibrotic medial plica and medial femoal condyle could be reproduced by manipulation. After arthroscopic medial release, the medial gutter and the damaged medial femoral condyle could be clearly visualized and the medial abrasion phenomenon was also eliminated. Additional file 2: Video 2. Evidence of cartilage regeneration after ACRFP by a second-look arthroscopy. This 56 years old lady received ACRFP and have had experienced a satisfactory outcome until three years later when she suffered from a falling down accident with the same knee injured. We therefore had the chance to perform a secondlook arthroscopy and visualized the evidence of cartilage regeneration over her previous chondral defect on the medial femoral condyle. Competing interests The authors declare that they have no competing interests. Authors contributions SRL, CCH, and CWL were involved in the design of the study and performed the statistical analysis. SRL and CCH performed the operations and collected data. CWL evaluated the radiographic outcomes. SRL, CCH, and CWL were responsible for drafting the paper and revising it. And all authors commented on the draft. All authors have read and approved the final manuscript. Acknowledgements Funding from Clinical Research Grant Program of Buddhist Dalin Tzu-Chi General Hospital. Author details 1 Joint Center, Buddhist Dalin Tzu Chi General Hospital, 2, Min-Shen Road, Chiayi 62247, Taiwan. 2 Department of Medical Imaging, Buddhist Dalin Tzu Chi General Hospital, Chiayi, Taiwan. 3 Tzu Chi University, Hualien, Taiwan. Received: 6 April 2012 Accepted: 17 November 2012 Published: 21 November 2012 References 1. Bitton R: The economic burden of osteoarthritis. Am J Manag Care 2009, 15:S230 S Brandt KD, Mazzuca SA: Lessons learned from nine clinical trials of diseasemodifying osteoarthritis drugs. Arthritis Rheum 2005, 52: Chang RW, Falconer J, Stulberg SD, Arnold WJ, Manheim LM, Dyer AR: A randomized, controlled trial of arthroscopic surgery versus closed-needle joint lavage for patients with osteoarthritis of the knee. Arthritis Rheum 1993, 36: Al-Omran AS, Sadat-Ali M: Arthroscopic joint lavage in osteoarthritis of the knee. Is it effective? Saudi Med J 2009, 30: Jackson RW, Dieterichs C: The results of arthroscopic lavage and debridement of osteoarthritic knees based on the severity of degeneration: a 4- to 6-year symptomatic follow-up. Arthroscopy 2003, 19: Kuzmanova SI: Treatment of knee osteoarthritis by arthroscopic synovectomy and debridement of cartilage lesions late results. Folia Med (Plovdiv) 2003, 45: Laupattarakasem W, Laopaiboon M, Laupattarakasem P, Sumananont C: Arthroscopic debridement for knee osteoarthritis. Cochrane Database Syst Rev 2008, 1:CD Bert JM: Role of abrasion arthroplasty and debridement in the management of osteoarthritis of the knee. Rheum Dis Clin North Am 1993, 19: Singh S, Lee CC, Tay BK: Results of arthroscopic abrasion arthroplasty in osteoarthritis of the knee joint. Singapore Med J 1991, 32: Johnson LL: Arthroscopic abrasion arthroplasty historical and pathologic perspective: present status. Arthroscopy 1986, 2: Friedman MJ, Berasi CC, Fox JM, Del Pizzo W, Snyder SJ, Ferkel RD: Preliminary results with abrasion arthroplasty in the osteoarthritic knee. Clin Orthop Relat Res 1984, 182: Mithoefer K, McAdams T, Williams RJ, Kreuz PC, Mandelbaum BR: Clinical efficacy of the microfracture technique for articular cartilage repair in the knee: an evidence-based systematic analysis. Am J Sports Med 2009, 37: Asik M, Ciftci F, Sen C, Erdil M, Atalar A: The microfracture technique for the treatment of full-thickness articular cartilage lesions of the knee: midterm results. Arthroscopy 2008, 24: Miller BS, Steadman JR, Briggs KK, Rodrigo JJ, Rodkey WG: Patient satisfaction and outcome after microfracture of the degenerative knee. J Knee Surg 2004, 17: Siparsky P, Ryzewicz M, Peterson B, Bartz R: Arthroscopic treatment of osteoarthritis of the knee: are there any evidence-based indications? Clin Orthop Relat Res 2007, 455: Lyu SR: Arthroscopic medial release for medial compartment osteoarthritis of the knee: the result of a single surgeon series with a minimum follow-up of four years. J Bone Joint Surg Br 2008, 90: Kellgren JH LJ: Atlas of standard radiographs: the epidemiology of chronic rheumatism. Vol. 2. Oxford: Blackwell; Marx RG, Connor J, Lyman S, Amendola A, Andrish JT, Kaeding C, et al: Multirater agreement of arthroscopic grading of knee articular cartilage. Am J Sports Med 2005, 33: Brouwer GM, van Tol AW, Bergink AP, Belo JN, Bernsen RM, Reijman M, et al: Association between valgus and varus alignment and the development and progression of radiographic osteoarthritis of the knee. Arthritis Rheum 2007, 56: Mazzuca SA, Brandt KD, Buckwalter KA, Lequesne M: Pitfalls in the accurate measurement of joint space narrowing in semiflexed, anteroposterior radiographic imaging of the knee. Arthritis Rheum 2004, 50: Vignon E, Piperno M, Le Graverand MP, Mazzuca SA, Brandt KD, Mathieu P, et al: Measurement of radiographic joint space width in the tibiofemoral compartment of the osteoarthritic knee: comparison of standing anteroposterior and Lyon schuss views. Arthritis Rheum 2003, 48: Grelsamer RP, Bazos AN, Proctor CS: Radiographic analysis of patellar tilt. J Bone Joint Surg Br 1993, 75: Kraus VB, Vail TP, Worrell T, McDaniel G: A comparative assessment of alignment angle of the knee by radiographic and physical examination methods. Arthritis Rheum 2005, 52:
11 Lyu et al. BMC Musculoskeletal Disorders 2012, 13:226 Page 10 of Moseley JB, O'Malley K, Petersen NJ, Menke TJ, Brody BA, Kuykendall DH, et al: A controlled trial of arthroscopic surgery for osteoarthritis of the knee. N Engl J Med 2002, 347: Richmond J, Hunter D, Irrgang J, Jones MH, Snyder-Mackler L, Van Durme D, et al: American Academy of Orthopaedic Surgeons clinical practice guideline on the treatment of osteoarthritis (OA) of the knee. J Bone Joint Surg Am 2010, 92: Dandy DJ: Abrasion chondroplasty. Arthroscopy 1986, 2: Hunt SA, Jazrawi LM, Sherman OH: Arthroscopic management of osteoarthritis of the knee. J Am Acad Orthop Surg 2002, 10: Bae DK, Yoon KH, Song SJ: Cartilage healing after microfracture in osteoarthritic knees. Arthroscopy 2006, 22: Rosenberger RE, Gomoll AH, Bryant T, Minas T: Repair of large chondral defects of the knee with autologous chondrocyte implantation in patients 45 years or older. Am J Sports Med 2008, 36: Lyu SR, Hsu CC: Medial plicae and degeneration of the medial femoral condyle. Arthroscopy 2006, 22: Lyu SR, Tzeng JE, Kuo CY, Jian AR, Liu DS: Mechanical strength of mediopatellar plica--the influence of its fiber content. Clin Biomech (Bristol, Avon) 2006, 21: Lyu SR: Relationship of medial plica and medial femoral condyle during flexion. Clin Biomech (Bristol, Avon) 2007, 22: Lyu SR, Chiang JK, Tseng CE: Medial plica in patients with knee osteoarthritis: a histomorphological study. Knee Surg Sports Traumatol Arthrosc 2010, 18: Wang HS, Kuo PY, Yang CC, Lyu SR: Matrix metalloprotease-3 expression in the medial plica and pannus-like tissue in knees from patients with medial compartment osteoarthritis. Histopathology 2011, 58: Ikeuchi M, Takahashi T, Tani T: Localized synovial hypertrophy in the anteromedial compartment of the osteoarthritic knee. Arthroscopy 2005, 21: Paulos LE, O'Connor DL, Karistinos A: Partial lateral patellar facetectomy for treatment of arthritis due to lateral patellar compression syndrome. Arthroscopy 2008, 24: Calpur OU, Ozcan M, Gurbuz H, Turan FN: Full arthroscopic lateral retinacular release with hook knife and quadriceps pressure-pull test: long-term follow-up. Knee Surg Sports Traumatol Arthrosc 2005, 13: Larson RL, Cabaud HE, Slocum DB, James SL, Keenan T, Hutchinson T: The patellar compression syndrome: surgical treatment by lateral retinacular release. Clin Orthop Relat Res 1978, 134: Fu FH, Maday MG: Arthroscopic lateral release and the lateral patellar compression syndrome. Orthop Clin North Am 1992, 23: Bigos SJ, McBride GG: The isolated lateral retinacular release in the treatment of patellofemoral disorders. Clin Orthop Relat Res 1984, 186: Becerra J, Andrades JA, Guerado E, Zamora-Navas P, Lopez-Puertas JM, Reddi AH: Articular cartilage: structure and regeneration. Tissue Eng Part B Rev 2010, 16: Hwang NS, Elisseeff J: Application of stem cells for articular cartilage regeneration. J Knee Surg 2009, 22: Elder BD, Athanasiou KA: Hydrostatic pressure in articular cartilage tissue engineering: from chondrocytes to tissue regeneration. Tissue Eng Part B Rev 2009, 15: Pereira RC, Scaranari M, Castagnola P, Grandizio M, Azevedo HS, Reis RL, et al: Novel injectable gel (system) as a vehicle for human articular chondrocytes in cartilage tissue regeneration. J Tissue Eng Regen Med 2009, 3: Zhang L, Hu J, Athanasiou KA: The role of tissue engineering in articular cartilage repair and regeneration. Crit Rev Biomed Eng 2009, 37: Solchaga LA, Goldberg VM, Caplan AI: Cartilage regeneration using principles of tissue engineering. Clin Orthop Relat Res 2001, (391 Suppl): S161 S Gibson A: Hyaline cartilage: degeneration and regeneration. Can Med Assoc J 1955, 73: Onyekwelu I, Goldring MB, Hidaka C: Chondrogenesis, joint formation, and articular cartilage regeneration. J Cell Biochem 2009, 107: Odenbring S, Egund N, Lindstrand A, Lohmander LS, Willen H: Cartilage regeneration after proximal tibial osteotomy for medial gonarthrosis. An arthroscopic, roentgenographic, and histologic study. Clin Orthop Relat Res 1992, 277: Kanamiya T, Naito M, Hara M, Yoshimura I: The influences of biomechanical factors on cartilage regeneration after high tibial osteotomy for knees with medial compartment osteoarthritis: clinical and arthroscopic observations. Arthroscopy 2002, 18: Koshino T, Wada S, Ara Y, Saito T: Regeneration of degenerated articular cartilage after high tibial valgus osteotomy for medial compartmental osteoarthritis of the knee. Knee 2003, 10: Aigner T, Soeder S, Haag J: IL-1beta and BMPs--interactive players of cartilage matrix degradation and regeneration. Eur Cell Mater 2006, 12: discussion Sandell LJ, Aigner T: Articular cartilage and changes in arthritis. An introduction: cell biology of osteoarthritis. Arthritis Res 2001, 3: Thorstensson CA, Andersson ML, Jonsson H, Saxne T, Petersson IF: Natural course of knee osteoarthritis in middle-aged subjects with knee pain: 12-year follow-up using clinical and radiographic criteria. Ann Rheum Dis 2009, 68: Wolfe F, Lane NE: The longterm outcome of osteoarthritis: rates and predictors of joint space narrowing in symptomatic patients with knee osteoarthritis. J Rheumatol 2002, 29: Spector TD, Hart DJ, Doyle DV: Incidence and progression of osteoarthritis in women with unilateral knee disease in the general population: the effect of obesity. Ann Rheum Dis 1994, 53: Hernborg JS, Nilsson BE: The natural course of untreated osteoarthritis of the knee. Clin Orthop Relat Res 1977, Felson DT, Zhang Y, Hannan MT, Naimark A, Weissman BN, Aliabadi P, et al: The incidence and natural history of knee osteoarthritis in the elderly. The Framingham Osteoarthritis Study. Arthritis Rheum 1995, 38: Cooper C, Snow S, McAlindon TE, Kellingray S, Stuart B, Coggon D, et al: Risk factors for the incidence and progression of radiographic knee osteoarthritis. Arthritis Rheum 2000, 43: doi: / Cite this article as: Lyu et al.: Arthroscopic cartilage regeneration facilitating procedure for osteoarthritic knee. BMC Musculoskeletal Disorders :226. Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
H.P. Teng, Y.J. Chou, L.C. Lin, and C.Y. Wong Under general or spinal anesthesia, the knee was flexed gently. In the cases of limited ROM, gentle and
 THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
THE BENEFIT OF ARTHROSCOPY FOR SYMPTOMATIC TOTAL KNEE ARTHROPLASTY Hsiu-Peng Teng, Yi-Jiun Chou, Li-Chun Lin, and Chi-Yin Wong Department of Orthopedic Surgery, Kaohsiung Veterans General Hospital, Kaohsiung,
Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy: a case report
 Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Shaw-Ruey Lyu, M.D., Ph.D., and Chia-Chen Hsu, M.D.
 Medial Plicae and Degeneration of the Medial Femoral Condyle Shaw-Ruey Lyu, M.D., Ph.D., and Chia-Chen Hsu, M.D. Purpose: The purpose of this study was to evaluate and analyze the chronological changes
Medial Plicae and Degeneration of the Medial Femoral Condyle Shaw-Ruey Lyu, M.D., Ph.D., and Chia-Chen Hsu, M.D. Purpose: The purpose of this study was to evaluate and analyze the chronological changes
Life. Uncompromised. The KineSpring Knee Implant System Surgeon Handout
 Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Evaluation and Treatment of Knee Arthritis Classification of Knee Arthritis Osteoarthritis Osteoarthritis Osteoarthritis of Knee
 1 2 Evaluation and Treatment of Knee Arthritis John Zebrack, MD Reno Orthopaedic Clinic Classification of Knee Arthritis Non-inflammatory Osteoarthritis Primary Secondary Post-traumatic, dysplasia, neuropathic,
1 2 Evaluation and Treatment of Knee Arthritis John Zebrack, MD Reno Orthopaedic Clinic Classification of Knee Arthritis Non-inflammatory Osteoarthritis Primary Secondary Post-traumatic, dysplasia, neuropathic,
Surgical Considerations:
 Knee Osteoarthritis / Defects of the Articular Cartilage Articular cartilage defects are variable in their presentation, in terms of location as well as severity. Several surgical procedures have been
Knee Osteoarthritis / Defects of the Articular Cartilage Articular cartilage defects are variable in their presentation, in terms of location as well as severity. Several surgical procedures have been
Osteoarthritis. Dr Anthony Feher. With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides
 Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
New Directions in Osteoarthritis Research
 New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
For Commercial products, please refer to the following policy: Preauthorization via Web-Based Tool for Procedures
 Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping
 Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Comparison of high-flex and conventional implants for bilateral total knee arthroplasty
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Comparison of high-flex and conventional implants for bilateral total knee arthroplasty C Martin-Hernandez, M Guillen-Soriano, A
Periarticular knee osteotomy
 Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco
 Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
Knee Pain And Injuries In Adults W. Dilworth Cannon, M.D. Professor of Clinical Orthopaedic Surgery University of California San Francisco Pain Control Overview Narcotics rarely necessary after 1 st 1-2
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
OsteoArthritis and Cartilage (2005) 13, 1029e1036 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.07.004 Brief report Second-look
Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of the Tibia
 Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Ideal Candidate for Cartilage Restoration. Large or Complex Lesions
 Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes
 Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Clinical Evaluation and Imaging of the Patellofemoral Joint Common clinical syndromes A. Panagopoulos Lecturer in Orthopaedics Medical School, Patras University Objectives Anatomy of patellofemoral joint
Save the meniscus Mais pourquoi?
 Save the meniscus Mais pourquoi? #$%&' ()"*+!," Philippe Neyret E Servien S Lustig P Verdonk One or more of the authors of the next presentation have identified no potential conflicts of interest 2 Consequences
Save the meniscus Mais pourquoi? #$%&' ()"*+!," Philippe Neyret E Servien S Lustig P Verdonk One or more of the authors of the next presentation have identified no potential conflicts of interest 2 Consequences
Degenerative joint disease of the shoulder, while
 Arthroscopic Debridement of the Shoulder for Osteoarthritis David M. Weinstein, M.D., John S. Bucchieri, M.D., Roger G. Pollock, M.D., Evan L. Flatow, M.D., and Louis U. Bigliani, M.D. Summary: Twenty-five
Arthroscopic Debridement of the Shoulder for Osteoarthritis David M. Weinstein, M.D., John S. Bucchieri, M.D., Roger G. Pollock, M.D., Evan L. Flatow, M.D., and Louis U. Bigliani, M.D. Summary: Twenty-five
A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients
 Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
Original Research Article A study of functional outcome after Primary Total Knee Arthroplasty in elderly patients Ragesh Chandran 1*, Sanath K Shetty 2, Ashwin Shetty 3, Bijith Balan 1, Lawrence J Mathias
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
Why does it matter? Patellar Instability 7/23/2018. What is the current operation de jour? Common. Poorly taught. Poorly treated
 Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
Patellar Instability It s Really Not That Difficult! David Shneider MD East Lansing, MI www.patellamdcom Detroit Sports Medicine Foundation July 2018 Why does it matter? Common Poorly taught Poorly treated
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up
 Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up Ching-Jen Wang, M.D. Department of Orthopedic Surgery Kaohsiung Chang Gung Memorial Hospital Chang Gung University College
Functional Outcome of Uni-Knee Arthroplasty in Asians with six-year Follow-up Ching-Jen Wang, M.D. Department of Orthopedic Surgery Kaohsiung Chang Gung Memorial Hospital Chang Gung University College
Patellofemoral Instability
 Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage Patellofemoral Instability. All decisions about the management of Patellofemoral Instability must be made in conjunction
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Horizon Scanning Centre November Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects
 Horizon Scanning Centre November 2014 Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects SUMMARY NIHR HSC ID: 8515 This briefing is based on information
Horizon Scanning Centre November 2014 Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects SUMMARY NIHR HSC ID: 8515 This briefing is based on information
Osteoarthritis. RA Hughes
 Osteoarthritis RA Hughes Osteoarthritis (OA) OA is the most common form of arthritis and the most common joint disease Most of the people who have OA are older than age 45, and women are more commonly
Osteoarthritis RA Hughes Osteoarthritis (OA) OA is the most common form of arthritis and the most common joint disease Most of the people who have OA are older than age 45, and women are more commonly
Humber. Arthroscopy Knee
 Humber Arthroscopy Knee Intervention Diagnostic & Therapeutic Arthroscopy Knee OPCS Codes W85 Therapeutic endoscopic operations on cavity of knee joint W851 Endoscopic removal of loose body from knee joint
Humber Arthroscopy Knee Intervention Diagnostic & Therapeutic Arthroscopy Knee OPCS Codes W85 Therapeutic endoscopic operations on cavity of knee joint W851 Endoscopic removal of loose body from knee joint
Arthrographic study of the rheumatoid knee.
 Annals of the Rheumatic Diseases, 1981, 40, 344-349 Arthrographic study of the rheumatoid knee. Part 2. Articular cartilage and menisci KYOSUKE FUJIKAWA, YOSHINORI TANAKA, TSUNEYO MATSUBAYASHI, AND FUJIO
Annals of the Rheumatic Diseases, 1981, 40, 344-349 Arthrographic study of the rheumatoid knee. Part 2. Articular cartilage and menisci KYOSUKE FUJIKAWA, YOSHINORI TANAKA, TSUNEYO MATSUBAYASHI, AND FUJIO
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY
 SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR FOCAL ARTICULAR CARTILAGE LESIONS
 CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
Medial plica irritation: diagnosis and treatment
 Curr Rev Musculoskelet Med (2008) 1:53 60 DOI 10.1007/s12178-007-9006-z Medial plica irritation: diagnosis and treatment Chad J. Griffith Æ Robert F. LaPrade Published online: 27 November 2007 Ó Humana
Curr Rev Musculoskelet Med (2008) 1:53 60 DOI 10.1007/s12178-007-9006-z Medial plica irritation: diagnosis and treatment Chad J. Griffith Æ Robert F. LaPrade Published online: 27 November 2007 Ó Humana
Bone&JointAppraisal Vol
 Bone&JointAppraisal Vol 01 No 03 December 2016 COBLATION Chondroplasty Versus Mechanical Debridement: Randomized Controlled Trial with 10-Year Outcomes -Year Four-Year Ten-Year Group A COBLATION technology
Bone&JointAppraisal Vol 01 No 03 December 2016 COBLATION Chondroplasty Versus Mechanical Debridement: Randomized Controlled Trial with 10-Year Outcomes -Year Four-Year Ten-Year Group A COBLATION technology
1 Department of Orthopaedic Surgery, Akershus University Hospital,
 483546CARXXX10.1177/1947603513483546CartilageÅrøen et al research-article2013 Article Agreement in Arthroscopic and Arthrotomy Assessment of Full-Thickness Articular Cartilage Lesions of the Knee in a
483546CARXXX10.1177/1947603513483546CartilageÅrøen et al research-article2013 Article Agreement in Arthroscopic and Arthrotomy Assessment of Full-Thickness Articular Cartilage Lesions of the Knee in a
Priorities Forum Statement GUIDANCE
 Priorities Forum Statement Number 21 Subject Knee Arthroscopy including arthroscopic knee washouts Date of decision November 2016 Date refreshed March 2017 Date of review November 2018 Osteoarthritis of
Priorities Forum Statement Number 21 Subject Knee Arthroscopy including arthroscopic knee washouts Date of decision November 2016 Date refreshed March 2017 Date of review November 2018 Osteoarthritis of
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure)
 Acta Orthop. Belg., 2004, 70, 306-310 ORIGINAL STUDIES Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure) Bart VINGERHOEDS, Ilse DEGREEF, Luc DE SMET From the University
Acta Orthop. Belg., 2004, 70, 306-310 ORIGINAL STUDIES Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure) Bart VINGERHOEDS, Ilse DEGREEF, Luc DE SMET From the University
Conservative surgical treatments for osteoarthritis: A Finite Element Study
 Conservative surgical treatments for osteoarthritis: A Finite Element Study Diagarajen Carpanen, BEng (Hons), Franziska Reisse, BEng(Hons), Howard Hillstrom, PhD, Kevin Cheah, FRCS, Rob Walker, PhD, Rajshree
Conservative surgical treatments for osteoarthritis: A Finite Element Study Diagarajen Carpanen, BEng (Hons), Franziska Reisse, BEng(Hons), Howard Hillstrom, PhD, Kevin Cheah, FRCS, Rob Walker, PhD, Rajshree
PART III Case Studies
 PART III Case Studies Patellofemoral Disorders: Diagnosis and Treatment. Edited by Roland M. Biedert 2004 John Wiley & Sons, Ltd ISBN: 0-470-85011-6 CASE STUDY 1 Unspecific patellofemoral pain What do
PART III Case Studies Patellofemoral Disorders: Diagnosis and Treatment. Edited by Roland M. Biedert 2004 John Wiley & Sons, Ltd ISBN: 0-470-85011-6 CASE STUDY 1 Unspecific patellofemoral pain What do
Significant Weight Loss May Delay or Eliminate the Need for Total Knee Replacement
 www.ijpm.in www.ijpm.ir Significant Weight Loss May Delay or Eliminate the Need for Total Knee Replacement Jeffrey H. DeClaire 1,2,3,4, Tatjana T. Savich 5, B. S. Adrienne LeGasse Montgomery 6, Olayinka
www.ijpm.in www.ijpm.ir Significant Weight Loss May Delay or Eliminate the Need for Total Knee Replacement Jeffrey H. DeClaire 1,2,3,4, Tatjana T. Savich 5, B. S. Adrienne LeGasse Montgomery 6, Olayinka
Proximal fibular osteotomy: a new surgery for pain relief and improvement of joint function in patients with knee osteoarthritis
 Clinical Report Proximal fibular osteotomy: a new surgery for pain relief and improvement of joint function in patients with knee osteoarthritis Journal of International Medical Research 2017, Vol. 45(1)
Clinical Report Proximal fibular osteotomy: a new surgery for pain relief and improvement of joint function in patients with knee osteoarthritis Journal of International Medical Research 2017, Vol. 45(1)
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury
 Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
DISEASES AND DISORDERS
 DISEASES AND DISORDERS 9. 53 10. Rheumatoid arthritis 59 11. Spondyloarthropathies 69 12. Connective tissue diseases 77 13. Osteoporosis and metabolic bone disease 95 14. Crystal arthropathies 103 15.
DISEASES AND DISORDERS 9. 53 10. Rheumatoid arthritis 59 11. Spondyloarthropathies 69 12. Connective tissue diseases 77 13. Osteoporosis and metabolic bone disease 95 14. Crystal arthropathies 103 15.
Cartilage Repair Options
 Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3
 AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
Unicompartmental Knee Replacement
 Unicompartmental Knee Replacement Results and Techniques Alexander P. Sah, MD California Orthopaedic Association Meeting Laguna Niguel, CA May 20th, 2011 Overview Why partial knee replacement? - versus
Unicompartmental Knee Replacement Results and Techniques Alexander P. Sah, MD California Orthopaedic Association Meeting Laguna Niguel, CA May 20th, 2011 Overview Why partial knee replacement? - versus
Meniscal Tears/Deficiency in Athletes
 Meniscal Tears/Deficiency in Athletes A. Amendola MD Professor of Orthopaedic Surgery Director of Sports Medicine Duke University 1 2 Meniscal tears Introduction Meniscal tears are one of the most frequent
Meniscal Tears/Deficiency in Athletes A. Amendola MD Professor of Orthopaedic Surgery Director of Sports Medicine Duke University 1 2 Meniscal tears Introduction Meniscal tears are one of the most frequent
A Patient s Guide to Partial Knee Resurfacing
 A Patient s Guide to Partial Knee Resurfacing Surgical Outcomes System (SOS ) www.orthoillustrated.com OrthoIllustrated is a leading Internet-based resource for patient education. Please visit this website
A Patient s Guide to Partial Knee Resurfacing Surgical Outcomes System (SOS ) www.orthoillustrated.com OrthoIllustrated is a leading Internet-based resource for patient education. Please visit this website
Failed Cartilage Repair
 Chapter 27 Failed Cartilage Repair Robert C. Grumet, Sarvottam Bajaj, and Brian J. Cole The management of traumatic and degenerative cartilage lesions is a known challenge given the limited vascularity
Chapter 27 Failed Cartilage Repair Robert C. Grumet, Sarvottam Bajaj, and Brian J. Cole The management of traumatic and degenerative cartilage lesions is a known challenge given the limited vascularity
Mædica - a Journal of Clinical Medicine
 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Total Knee Arthroplasty Following High Tibial Osteotomy a Radiological Evaluation Horia ORBAN, MD, PhD; Emil MARES, MD; Mihaela DRAGUSANU, MD; Gabriel
Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Total Knee Arthroplasty Following High Tibial Osteotomy a Radiological Evaluation Horia ORBAN, MD, PhD; Emil MARES, MD; Mihaela DRAGUSANU, MD; Gabriel
BRIEF REPORT. KENNETH D. BRANDT, ROSE S. FIFE, ETHAN M. BRAUNSTEIN, and BARRY KATZ. From the Department of Medicine, the Department of
 1381 BRIEF REPORT RADIOGRAPHIC GRADING OF THE SEVERITY OF KNEE OSTEOARTHRITIS: RELATION OF THE KELLGREN AND LAWRENCE GRADE TO A GRADE BASED ON JOINT SPACE NARROWING, AND CORRELATION WITH ARTHROSCOPIC EVIDENCE
1381 BRIEF REPORT RADIOGRAPHIC GRADING OF THE SEVERITY OF KNEE OSTEOARTHRITIS: RELATION OF THE KELLGREN AND LAWRENCE GRADE TO A GRADE BASED ON JOINT SPACE NARROWING, AND CORRELATION WITH ARTHROSCOPIC EVIDENCE
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries. Cartilage Surgery. The Knee.
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Cartilage Surgery The Knee CARTILAGE INJURY Treatment of cartilage injury remains one of the most significant challenges
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Cartilage Surgery The Knee CARTILAGE INJURY Treatment of cartilage injury remains one of the most significant challenges
SCALENE ASIA PACIFIC SDN BHD ROTATIONAL FIELD QUANTUM NUCLEAR MAGNETIC RESONANCE (RFQMR) IN TREATMENT OF OSTEOARTHRITIS OF THE KNEE JOINT
 SCALENE ASIA PACIFIC SDN BHD ROTATIONAL FIELD QUANTUM NUCLEAR MAGNETIC RESONANCE (RFQMR) IN TREATMENT OF OSTEOARTHRITIS OF THE KNEE JOINT ROTATIONAL FIELD QUANTUM NUCLEAR MAGNETIC RESONANCE (RFQMR) IN
SCALENE ASIA PACIFIC SDN BHD ROTATIONAL FIELD QUANTUM NUCLEAR MAGNETIC RESONANCE (RFQMR) IN TREATMENT OF OSTEOARTHRITIS OF THE KNEE JOINT ROTATIONAL FIELD QUANTUM NUCLEAR MAGNETIC RESONANCE (RFQMR) IN
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 2023/14
 WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 2023/14 BEFORE: A. T. Patterson: Vice-Chair HEARING: November 3, 2014 at Toronto Oral DATE OF DECISION: April 17, 2015 NEUTRAL CITATION: 2015
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 2023/14 BEFORE: A. T. Patterson: Vice-Chair HEARING: November 3, 2014 at Toronto Oral DATE OF DECISION: April 17, 2015 NEUTRAL CITATION: 2015
Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella Treated with a Different Method in Each Knee
 Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
Case Reports in Orthopedics Volume 2015, Article ID 890315, 5 pages http://dx.doi.org/10.1155/2015/890315 Case Report Total Knee Arthroplasty in a Patient with Bilateral Congenital Dislocation of the Patella
Unicompartmental Knee Resurfacing
 Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
General Concepts. Growth Around the Knee. Topics. Evaluation
 General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
General Concepts Knee Injuries in Skeletally Immature Athletes Zachary Stinson, M.D. Increased rate and ability of healing Higher strength of ligaments compared to growth plates Continued growth Children
Rehabilitation of an ACL injury in a 29 year old male with closed kinetic chain exercises: A case study
 Abstract Objective: This paper will examine a rehabilitation program for a healthy 29 year old male who sustained an incomplete tear of the left ACL. Results: Following a 9 week treatment plan focusing
Abstract Objective: This paper will examine a rehabilitation program for a healthy 29 year old male who sustained an incomplete tear of the left ACL. Results: Following a 9 week treatment plan focusing
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the
 The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
OSTEOCHONDRAL ALLOGRAFTS AND AUTOGRAFTS IN THE TREATMENT OF FOCAL ARTICULAR CARTILAGE LESIONS
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Patellofemoral Joint. Question? ANATOMY
 Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Doug Elenz is a paid Consultant/Advisor for the Biomet Manufacturing Corporation. Doug Elenz, MD Team Orthopaedic Surgeon The University of Texas Men s Athletic Department Question? Patellofemoral Joint
Treatment Options for Articular Cartilage Defects of the Knee
 Innovations Treatment Options for Articular Cartilage Defects of the Knee Alvin J. Detterline Steven Goldberg ernard R. ach, Jr. rian J. Cole The treatment of symptomatic articular cartilage defects of
Innovations Treatment Options for Articular Cartilage Defects of the Knee Alvin J. Detterline Steven Goldberg ernard R. ach, Jr. rian J. Cole The treatment of symptomatic articular cartilage defects of
Some illustrations are from the internet and intended for educational purpose only
 Some illustrations are from the internet and intended for educational purpose only นพ. ส หธ ช งามอ โฆษ ภาคว ชา ออร โธป ด กส คณะแพทย ศาสตร จ ฬาลงกรณ มหาว ทยาล ย Knee anatomy Femur Pathophysiology Symptoms
Some illustrations are from the internet and intended for educational purpose only นพ. ส หธ ช งามอ โฆษ ภาคว ชา ออร โธป ด กส คณะแพทย ศาสตร จ ฬาลงกรณ มหาว ทยาล ย Knee anatomy Femur Pathophysiology Symptoms
Management of Chronic Elbow Pain
 Mr. Nashat Siddiqui Consultant Upper Limb Orthopaedic Surgeon Management of Chronic Elbow Pain Patients presenting with elbow pain can pose a diagnostic challenge, especially if there is no obvious recent
Mr. Nashat Siddiqui Consultant Upper Limb Orthopaedic Surgeon Management of Chronic Elbow Pain Patients presenting with elbow pain can pose a diagnostic challenge, especially if there is no obvious recent
Outcome of Treatment of Osteoarthritis with Arthroscopic Debridement and Autologous Conditioned Plasma
 Doi: http://dx.doi.org/10.5704/moj.1703.008 Outcome of Treatment of Osteoarthritis with Arthroscopic Debridement and Autologous Conditioned Plasma King CKK, FRCS, Yung A, FRCS Department of Orthopaedics,
Doi: http://dx.doi.org/10.5704/moj.1703.008 Outcome of Treatment of Osteoarthritis with Arthroscopic Debridement and Autologous Conditioned Plasma King CKK, FRCS, Yung A, FRCS Department of Orthopaedics,
PARTIAL KNEE REPLACEMENT
 PARTIAL KNEE REPLACEMENT A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
PARTIAL KNEE REPLACEMENT A partial knee replacement removes damaged cartilage from the knee and replaces it with prosthetic implants. Unlike a total knee replacement, which removes all of the cartilage,
Femoral neck fracture during physical therapy following surface replacement arthroplasty: a preventable complication?
 CASE REPORT Open Access Femoral neck fracture during physical therapy following surface replacement arthroplasty: a preventable complication? A case report Timothy R Judkins, Michael R Dayton * Abstract
CASE REPORT Open Access Femoral neck fracture during physical therapy following surface replacement arthroplasty: a preventable complication? A case report Timothy R Judkins, Michael R Dayton * Abstract
Dimensions of the intercondylar notch and the distal femur throughout life
 Dimensions of the intercondylar notch and the distal femur throughout life Poster No.: P-0089 Congress: ESSR 2013 Type: Scientific Exhibit Authors: L. Hirtler, S. Röhrich, F. Kainberger; Vienna/AT Keywords:
Dimensions of the intercondylar notch and the distal femur throughout life Poster No.: P-0089 Congress: ESSR 2013 Type: Scientific Exhibit Authors: L. Hirtler, S. Röhrich, F. Kainberger; Vienna/AT Keywords:
Research Article Relationship between Pain and Medial Meniscal Extrusion in Knee Osteoarthritis
 Advances in Orthopedics Volume 2015, Article ID 210972, 4 pages http://dx.doi.org/10.1155/2015/210972 Research Article Relationship between Pain and Medial Meniscal Extrusion in Knee Osteoarthritis Hiroaki
Advances in Orthopedics Volume 2015, Article ID 210972, 4 pages http://dx.doi.org/10.1155/2015/210972 Research Article Relationship between Pain and Medial Meniscal Extrusion in Knee Osteoarthritis Hiroaki
21/01/10. Disclosures. Results of High Tibial Osteotomy Osteotomy: Review of the Literature. Introduction. OW osteotomy and bone graft
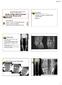 3rd Annual Advanced Course on Knee Surgery January 17-22, 2010, Val D Isere, Results of High Tibial Osteotomy Osteotomy: Review of the Literature Disclosures Conflict of interest related to this presentation:
3rd Annual Advanced Course on Knee Surgery January 17-22, 2010, Val D Isere, Results of High Tibial Osteotomy Osteotomy: Review of the Literature Disclosures Conflict of interest related to this presentation:
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE
 THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
THE DIAGNOSIS AND MANAGEMENT OF SPONTANEOUS AND POST-ARTHROSCOPY OSTEONECROSIS OF THE KNEE Abstract Spontaneous osteonecrosis of the knee (SPONK) and osteonecrosis in the postoperative knee (ONPK) are
Results of arthroscopic surgery, with or without high Tibial osteotomy, in osteoarthritis of knee
 2018; 2(3): 100-105 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2018; 2(3): 100-105 Received: 17-05-2018 Accepted: 18-06-2018 Dr. Tarkik Amin Assistant Professor,
2018; 2(3): 100-105 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2018; 2(3): 100-105 Received: 17-05-2018 Accepted: 18-06-2018 Dr. Tarkik Amin Assistant Professor,
Soft Tissue Releases in Valgus Knees
 Soft Tissue Releases in Valgus Knees Ke Xie, MD Steven Lyons, MD Florida Orthopaedic Institute June 17, 2016 Background Valgus deformities make up 10-15% of all primary TKA s performed Restoration of the
Soft Tissue Releases in Valgus Knees Ke Xie, MD Steven Lyons, MD Florida Orthopaedic Institute June 17, 2016 Background Valgus deformities make up 10-15% of all primary TKA s performed Restoration of the
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries
 What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What s your diagnosis?
 Case Study 58 A 61-year-old truck driver man presented with a valgus injury to the left knee joint when involved in a truck accident. What s your diagnosis? Diagnosis : Avulsion of Deep MCL The medial
Case Study 58 A 61-year-old truck driver man presented with a valgus injury to the left knee joint when involved in a truck accident. What s your diagnosis? Diagnosis : Avulsion of Deep MCL The medial
KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE
 KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
KNEE MICROFRACTURE CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Cartilage Repair Center Brigham and Women s Hospital Harvard Medical School
 Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at if you have any questions.
 OSU Sports Medicine Knee Microfracture Rehabilitation Guidelines These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at 614-293-2385 if you have any questions. Rehabilitation
OSU Sports Medicine Knee Microfracture Rehabilitation Guidelines These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at 614-293-2385 if you have any questions. Rehabilitation
evicore MSK joint surgery procedures requiring prior authorization
 evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
Latest Treatments for Hip Arthritis. Michael J. Repine MD Boulder Medical Center Orthopedics You re Not Alone
 Latest Treatments for Hip Arthritis Michael J. Repine MD Boulder Medical Center Orthopedics 303-502-9404 You re Not Alone More than 43 million people have some form of arthritis. It is estimated that the
Latest Treatments for Hip Arthritis Michael J. Repine MD Boulder Medical Center Orthopedics 303-502-9404 You re Not Alone More than 43 million people have some form of arthritis. It is estimated that the
The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy
 The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy Craig M. Capeci, MD Mohaned Al-Humadi, MD Malachy P. McHugh, PhD Alexis Chiang-Colvin,
The Relationship Between Hip Physical Examination Findings and Intra-articular Pathology Seen at the Time of Hip Arthroscopy Craig M. Capeci, MD Mohaned Al-Humadi, MD Malachy P. McHugh, PhD Alexis Chiang-Colvin,
7/20/14. Patella Instability. Alignment. PF contact areas. Tissue Restraints. Pain. Acute Blunt force trauma Disorders of the Patellafemoral Joint
 Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
Patella Instability Acute Blunt force trauma Disorders of the Patellafemoral Joint Evan G. Meeks, M.D. Orthopaedic Surgery Sports Medicine The University of Texas - Houston Pivoting action Large effusion
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Impingement Syndromes of the Ankle. Noaman W Siddiqi MD 5/4/2006
 Impingement Syndromes of the Ankle Noaman W Siddiqi MD 5/4/2006 Ankle Impingement Overview Clinical DX Increasingly recognized cause of chronic ankle pain Etiology can be soft tissue or osseous Professional
Impingement Syndromes of the Ankle Noaman W Siddiqi MD 5/4/2006 Ankle Impingement Overview Clinical DX Increasingly recognized cause of chronic ankle pain Etiology can be soft tissue or osseous Professional
BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS IN TOTAL KNEE REPLACEMENTS
 Journal of Mechanics in Medicine and Biology Vol. 5, No. 3 (2005) 469 475 c World Scientific Publishing Company BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS
Journal of Mechanics in Medicine and Biology Vol. 5, No. 3 (2005) 469 475 c World Scientific Publishing Company BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS
What is Medial Plica Syndrome?
 What is Medial Plica Syndrome? It is a congenital disorder in which the thin wall of fibrous tissue extends from the synovial capsule of the knee. Pain usually occurs when the synovial capsule becomes
What is Medial Plica Syndrome? It is a congenital disorder in which the thin wall of fibrous tissue extends from the synovial capsule of the knee. Pain usually occurs when the synovial capsule becomes
Rehabilitation Guidelines Following Microfracture Procedures to the Knee
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
DISCLOSURES. T. McAlindon: Samumed, grant/research support; Astellas, Flexion, Pfizer, Regeneron, Samumed,and Seikugaku, consulting
 Radiographic Outcomes from a Randomized, Double- Blind, Placebo-Controlled, Phase 2 Study of a Novel, Intra-Articular, Wnt Pathway Inhibitor (SM04690) for the Treatment of Osteoarthritis of the Knee: Week
Radiographic Outcomes from a Randomized, Double- Blind, Placebo-Controlled, Phase 2 Study of a Novel, Intra-Articular, Wnt Pathway Inhibitor (SM04690) for the Treatment of Osteoarthritis of the Knee: Week
Back out of Locking Pin with Hinge Fracture after High Tibial Osteotomy
 Case Report Knee Surg Relat Res 2018;30(2):171-175 https://doi.org/10.5792/ksrr.17.034 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Back out of Locking Pin with Hinge Fracture after
Case Report Knee Surg Relat Res 2018;30(2):171-175 https://doi.org/10.5792/ksrr.17.034 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Back out of Locking Pin with Hinge Fracture after
Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System
 Showa Univ J Med Sci 29 3, 289 296, September 2017 Original Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System Hiroshi TAKAGI 1 2, Soshi ASAI 1, Atsushi
Showa Univ J Med Sci 29 3, 289 296, September 2017 Original Kinematics Analysis of Different Types of Prosthesis in Total Knee Arthroplasty with a Navigation System Hiroshi TAKAGI 1 2, Soshi ASAI 1, Atsushi
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
Arthritis & Rheumatism
 ~ Arthritis & Rheumatism Official Journal of the American College of Rheumatology RELATIONSHIP BETWEEN ARTHROSCOPIC EVIDENCE OF CARTILAGE DAMAGE AND RADIOGRAPHIC EVIDENCE OF JOINT SPACE NARROWING IN EARLY
~ Arthritis & Rheumatism Official Journal of the American College of Rheumatology RELATIONSHIP BETWEEN ARTHROSCOPIC EVIDENCE OF CARTILAGE DAMAGE AND RADIOGRAPHIC EVIDENCE OF JOINT SPACE NARROWING IN EARLY
