Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion
|
|
|
- Beatrice Hawkins
- 5 years ago
- Views:
Transcription
1 Increased Fusion Rates With Cervical Plating for Two- Level Anterior Cervical Discectomy and Fusion SPINE Volume 25, Number 1, pp , Lippincott Williams & Wilkins, Inc. Jeffrey C. Wang, MD, Paul W. McDonough, MD, Kevin K. Endow, BS, and Rick B. Delamarter, MD Study Design. A retrospective review of all patients surgically treated with a two-level anterior cervical discectomy and fusion with and without anterior plate fixation by a single surgeon. Objectives. To compare the clinical and radiographic success of two-level discectomy and the effect of anterior cervical plate fixation. Summary of Background Data. Prior studies of multisegment fusions have shown decreased fusion rates correlating with the number of increased levels. The use of anterior plates for single-level cervical fusions is controversial. However, their use in multilevel fusions may be warranted because of the increased pseudarthrosis rates. Methods. Over a 6-year period, 60 patients were treated surgically with a two-level anterior cervical discectomy and fusion by the senior author. Thirty-two patients had cervical plates, and 28 underwent fusions without plates. These patients were followed for an average of 2.7 years. Clinical and radiographic follow-up evaluations were performed. Results. Of the 60 patients, 7 had a pseudarthrosis. The pseudarthrosis rates were 0% for patients with plating and 25% for those with no plating. This difference was statistically significant (P 0.003). No correlation of pseudarthrosis with gender, age, level of surgery, history of tobacco use, or the presence of prior anterior surgery was found. There was significantly less graft collapse (P ) in the patients without plates in whom pseudarthrosis developed (1.4 mm) than in those who had fusions with plates (0.3 mm). The amount of kyphotic deformity of the fused segment was 0.4 in patients with plating compared with 4.9 in those without plating who developed a pseudarthrosis (P ). Conclusions. The addition of plate fixation for twolevel anterior cervical discectomy and fusion is a safe procedure with no significant increase in complication rates. The pseudarthrosis rates are significantly higher in patients treated without plate fixation. No nonunions occurred in the patients treated with plate fixation. There was significantly less disc space collapse and kyphotic deformity with the plated fusions than with the nonplated fusions, in which a pseudarthrosis developed. The complication rates for plated fusions are extremely low and do not differ from those for nonplated fusions. [Key words: anterior plates, cervical, discectomy, fusion, pseudarthrosis, spine] Spine 2000;25:41 45 From the Department of Orthopaedic Surgery, University of California, Los Angeles, School of Medicine, Los Angeles, California. Acknowledgment date: August 6, First revision date: October 8, Second revision date: December 22, Acceptance date: February 9, Device status category: 11. Anterior cervical discectomy and fusion (ACDF), as originally described by Robinson, 12 is a highly successful procedure when there is neural compression by disc material or osteophytes. With modified burring of the vertebral endplates, Bohlman et al 1 3,8 demonstrated even higher fusion rates and successful outcomes. However, with multilevel procedures, the fusion rates decrease and are much lower than with single-level surgeries. 9 The lower fusion rates have been attributed to the increased number of grafts and interfaces that must consolidate with multilevel surgery, and to the increased stresses on the multiple graft sites and the resultant micromotion. Attempts to increase the fusion rates with two-level anterior cervical discectomies include the use of complete or subtotal vertebrectomies so that only two osseous surfaces (one single graft) need to heal to obtain a solid fusion. 7,9 Other methods involve the use of anterior cervical plates across the entire fusion construct to provide increased stability and minimize micromotion at the bone graft interface. 4 6,7,13 The use of anterior cervical plating in spinal surgery has increased recently. Several biomechanical studies have demonstrated the added stability provided by these plates, which theoretically may result in increased fusion rates. 5,6,10,14 The use of cervical plating for single-level ACDF is controversial. Whereas some studies demonstrate increased single-level fusion rates and decreased reoperation rates with the use of cervical plate fixation, others show decreased fusion rates for single-level fusions with the use of plates because they may hold the disc space in distraction and prevent graft settling, which may be important in graft consolidation. 4 6,15 The purpose of this study was to compare the results, complications, and fusion rates for primary, two-level ACDF between patients with and those without anterior cervical plate fixation. Material and Methods All patients at the authors institution having a two-level ACDF performed by the senior author were reviewed retrospectively. These patients all had disc herniation at two levels refractory to conservative management, which included the use of antiinflammatory medications, physical therapy, and a period of rest and immobilization. Patients with continued symptoms were offered surgical treatment consisting of an ACDF as originally described by Robinson. 12 All disc material was removed, along with endplate osteophytes, back to the posterior longitudinal ligament and the uncovertebral joints. Autogenous iliac crest bone graft 41
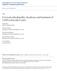
2 42 Spine Volume 25 Number Table 1. Odom s Criteria Excellent Good Fair Poor All preoperative symptoms relieved; abnormal findings improved Minimal persistence of preoperative symptoms; abnormal findings unchanged or improved Definite relief of some preoperative symptoms; other symptoms unchanged or slightly improved Symptoms and signs unchanged or exacerbated was placed into the disc space after the endplates were removed with a high-speed burr. Some of the patients were plated with an anterior vertebral body plate spanning the interspace fusion. Plate fixation was purely the choice of the operating surgeon and accomplished in a chronologic manner. The early patients were treated without plates, whereas the patients with more recent surgeries all had plate fixation. There were no significant differences between the groups. After surgery, all patients were treated with the same protocol consisting of immobilization with a hard cervical collar for 6 to 8 weeks. Radiographs were taken at 2 and 6 weeks after surgery, and then at monthly intervals until the fusion was judged to be solid or the presence of a pseudarthrosis was identified. Follow-up radiography and clinical examinations were performed by the surgeon, and the medical records were reviewed extensively. Fusion was judged by the absence of motion between the spinous processes on flexion extension lateral radiographs, the absence of a radiolucent gap between the graft and the endplate, and the presence of continuous bridging bony trabeculae at the graft endplate junction. A pseudarthrosis was judged radiographically by the absence of bridging osseous trabecular bone from the vertebral bodies to the graft, motion on dynamic radiographs, and the presence of a lucent line at the graft vertebral body junction. A pseudarthrosis was judged to be present after either a minimum follow-up assessment of 1 year had been carried out with the appropriate radiographic signs or the patient had undergone revision surgery. This was determined by the senior author. Clinical symptoms and neurologic findings were documented on follow-up assessment, and further cervical surgery also was documented. Hardware and graft complications were reviewed as well. All medical records, office charts, and radiographs were reviewed, and the information was entered into a spreadsheet database. Outcomes were subjectively graded on the basis of patient symptoms at final follow-up assessment, use of pain medications, work status, and a subjective rating of the pain level. These were graded by Odom s criteria as listed in Table Results A total of 60 consecutive patients (26 men and 34 women) who underwent adjacent two-level ACDF performed by the senior author between 1990 and 1996 were entered into the study. Thirty-two of these patients had fusions performed with the use of cervical plates, and 28 underwent fusions without the use of a plate. The average age of the patients was 47.6 years (range, years), and did not differ significantly between patients treated with or without cervical plates. Follow-up time averaged 2.7 years (range, 1 6 years). Plates were used in more patients who had surgery more recently than in patients who had undergone surgery farther in the past. A pseudarthrosis developed in 7 of the 60 patients. No pseudarthrosis occurred in patients with a cervical plate. All seven pseudarthroses occurred in patients without plate fixation. The overall rate of pseudarthrosis in the group with an anterior cervical plate was 0%, whereas the rate of pseudarthrosis in the group without an anterior cervical plate was 25%. This difference was statistically significant (P 0.003). No statistical correlation of pseudarthrosis with gender, age, level of surgery, or history of tobacco use was found. When radiographic data between the two groups of patients was compared, differences were discovered. These differences are summarized in Table 2. The average amount of graft collapse for patients with plating was 0.3 mm (range, 0 4 mm) as compared with 0.6 mm (range, 0 6 mm) for all patients without a plate. This difference was not significant according to a nonparametric rank-sum test (P 0.256). However, when the amount of collapse in patients with a plate (0.3 mm) and in those without a plate who developed a pseudarthrosis (1.4 mm) was compared, a statistically significant difference (P ) was observed. In comparisons between patients with a plate (0.3 mm) and those without a plate who successfully fused (0.3 mm), no difference was found. In comparing patients without a plate, the difference between those who fused (0.3 mm) and those who did not (1.4 mm) also is statistically significant (P ). The success of Figure 1. Lateral postoperative radiograph of a two-level anterior cervical discectomy and fusion using plate fixation with excellent preservation of anatomic alignment.
3 Plate Fixation for Two-Level ACDF Wang et al 43 Figure 2. A, Immediate postoperative radiograph of a two-level anterior cervical discectomy and fusion without plate fixation, showing initial preservation of anatomic alignment. B, The same patient after the development of a pseudarthrosis at the lower fusion level. Note the collapse of the graft and the resultant kyphotic deformity at the level of the nonunion. C, Radiograph taken after posterior fusion, demonstrating healing of the pseudarthrosis. Note the residual collapse and kyphosis even after successful fusion. the arthrodesis appears to decrease the amount of collapse significantly (Figure 1). The average amount of kyphotic deformity of the fused segment was 0.4 (range, 0 2 ) for patients with cervical plates, and 1.6 (range, 0 18 ) for patients with no plates. This difference was not significant (P 0.459). However, in comparing the amount of deformity between patients with a plate (0.4 ) and those without who developed a pseudarthrosis (4.9 ), a statistically significant difference was found (P ). In comparisons between patients with a plate (0.4 ) and those without who successfully fused (0.5 ), essentially no difference was observed. When patients without a plate were compared, the difference between those who fused (0.5 ) and those who did not (4.9 ) also was statistically significant (P ). The success of arthrodesis appears to decrease the amount of kyphotic deformity significantly. Table 2. The Amount of Graft Collapse and Kyphotic Deformity Sorted According to the Use of a Cervical Plate and the Presence of a Fusion Collapse (mm) Kyphosis ( ) Plate fused No plate fused No plate pseudarthrosis The difference between the patient with no plate and a pseudarthrosis and all the other groups is statistically significant for both collapse and kyphosis. Each pseudarthrosis occurred at the lower cervical fusion level, which was at C5 C6 or C6 C7. These two levels were the most common levels to be involved in the surgeries. All patients with a pseudarthrosis were moderately symptomatic and required further surgery to obtain osseous union. Overall, 25% of the patients without cervical plates had subsequent spinal surgery. These procedures were performed specifically to address the nonunion. The patients with plate fixation did not have any subsequent spinal procedures after the index operation. There were no complications related to the use of cervical plating. A pseudarthrosis developed in 2 of the 6 smokers (33.3%), whereas a nonunion occurred in 5 of the 52 nonsmokers (9.6%). A pseudarthrosis developed in both of the smokers without cervical plates, but in none of the smokers with cervical plates. Before surgery, all the patients had radiculopathy, with or without some component of axial neck pain. Of the 60 patients, 43 had subjective decreased sensation in the distribution of the compressed nerve root. A decreased reflex corresponding to the compressed nerve occurred in 23 patients, whereas 19 had at least a grade of weakness that corresponded to the compression. No new deficits occurred as part of the surgeries. Postoperatively at final follow-up assessment, three patients had remaining weakness of at least one grade, whereas four had subjective residual decreased sensation. Radic-
4 44 Spine Volume 25 Number Table 3. Results of Surgery Sorted According to Odom s Criteria Excellent Good Fair Poor Plate fused 38% (12) 50% (16) 12% (4) 0% (0) No plate fused 29% (6) 57% (12) 10% (2) 4% (1) No plate pseudarthrosis 14% (1) 14% (1) 58% (4) 14% (1) Note the percentage of good/excellent results is similar between the patients who fused, regardless of the use of a cervical plate. Inferior results are shown for the patients with a nonunion. ulopathy developed in one patient at a level adjacent to the new onset adjacent segment disease, but did not require surgical intervention. The results of the surgeries graded by Odom s criteria are listed in Table 3. The results in the patients with plates are markedly similar to those in the patients who fused without plates. The patients in whom a pseudarthrosis developed, all without cervical plates, demonstrate results inferior to those in patients who fused. Discussion Anterior cervical discectomy and fusion is a highly successful procedure with high fusion rates and excellent clinical results from the use of standard techniques without internal fixation. 1 3,8,12 The application of internal fixation, in the form of rigid plating in other areas of the skeleton, have resulted in improved fusion rates because of added stability. Interestingly, the literature is confusing as to the benefits of anterior cervical plating for single-level fusion. Previous studies have demonstrated increased fusion rates for single-level fusions with the use of cervical plating. 5 However, some studies have demonstrated decreased fusion rates with plating for single-level fusions. 4 The plate is believed to hold the disc graft complex rigidly, which does not allow for small amounts of collapse and subsequent graft compression. This compression is thought to be necessary to promote fusion. Therefore, the plate may hold the complex in a slight amount of distraction, thus leading to decreased fusion rates. The pseudarthrosis rates for single-level cervical fusions are low. Multilevel discectomies have decreased fusion rates because of the increased number of graft bone surfaces that must heal and the increased instability and micromotion that results from multilevel disc excision. 9 The pseudarthrosis rates for multilevel discectomies can range up to 54% for threelevel procedures. 9 In the current study, patients without cervical plate fixation experienced a higher pseudarthrosis rate. The pseudarthrosis rate for cervical plating was 0%, whereas the rate for patients without plating was 25%. This difference was statistically significant. The use of a cervical plate does appear to significantly affect the pseudarthrosis rate for primary adjacent twolevel ACDF. Although plate fixation appears to be controversial in single-level fusions, the use of cervical plates appears to be justified in two-level surgeries by significantly improved results. In this study, significantly less graft collapse and resultant kyphosis of the fusion segment occurred in the patients treated with cervical plating than in patients without plates in whom a pseudarthrosis developed. There were no significant differences between the patients with a plate and those without a plate who fused successfully. Therefore, if successful osseous union occurs, the plate is not necessary to preserve the normal anatomic lordotic curvature of the cervical spine and prevent disc space graft collapse. The benefits of the plate, in regard to collapse and kyphosis, appear to lie in the increased union rate that protects against deformity. Because no nonunions occurred in the patients with plates, it is not definitively known if the plate would preserve alignment in the presence of a pseudarthrosis. The actual significance of preserving the normal contour of the cervical spine is not known. A kyphotic posture of the cervical spine may lead to the development of adjacent segment degeneration. However, a longer follow-up period is needed to confirm a relationship. Although there are always potential hardware complications associated with the use of spinal instrumentation, the complication rate for cervical plating is extremely low. In this study, there were no complications associated specifically with the use of cervical plates. The overall complication rates for patients with plates and those without were exactly the same. The fusion rates for two-level ACDF are significantly higher with the use of an anterior cervical plate. Cervical plating should be considered for patients undergoing a two-level adjacent ACDF to decrease the pseudarthrosis rate. The lower cervical level appears to be the most common site for a nonunion. The complication rates are not increased with the use of a cervical plate. References 1. Bohlman HH. Cervical spondylosis and myelopathy: Instructional Course Lectures. Rosemont, IL: Am Acad Orthop Surgeons 1995;44: Bohlman HH. Cervical spondylosis with moderate to severe myelopathy: A report of seventeen cases treated by Robinson anterior cervical discectomy and fusion. Spine 1977;2: Bohlman HH, Emery SE, Goodfellow DB, Jones PK. Robinson anterior cervical discectomy and arthrodesis for cervical radiculopathy. J Bone Joint Surg [Am] 1993;75: Capen D, Rah A, Nagelberg S, Nelson R, Larsen J, Adkins R. Clinical Significance of Instrumented Versus Noninstrumented Anterior Cervical Discectomy and Fusion. Presented at the annual meeting of the North American Spine Society, New York, NY, October 25, Connolly PJ, Esses SI, Kostuik JP. Anterior cervical fusion: Outcome analysis of patients fused with and without anterior cervical plates. J Spinal Disord 1996; 9: Coric D, Branch CL Jr, Jenkins JD. Revision of anterior cervical pseudarthrosis with anterior allograft fusion and plating. J Neurosurg 1997;86: Ellison TS, Hartman MB, Brigham CD, et al. Fusion Rates for Two-Level ACDF Plating Versus Subtotal Corpectomy and Fusion. Presented at the annual meeting of the North American Spine Society, New York, NY, October 25, 1997.
5 Plate Fixation for Two-Level ACDF Wang et al Emery SE, Bolesta MJ, Banks MA, Jones PK. Robinson anterior cervical fusion: Comparison of standard and modified techniques. Spine 1994;19: Emery SE, Fisher JRS, Bohlman HH. Higher Incidence of Pseudarthrosis and Poor Outcomes for Three-Level Anterior Cervical Discectomy and Fusion. Presented at the annual meeting of the Cervical Spine Research Society, Palm Beach, FL, December 6, Griffith SL, Zogbi SW, Guyer RD, Shelokov AP, Contiliano JH, Geiger JM. Biomechanical comparison of anterior instrumentation for the cervical spine. J Spinal Disord 1995;8: Odom GL, Finney W, Woodhall B. Cervical disc lesions. JAMA 1958;166: Robinson RA, Walker AE, Ferlic DC, Wiecking DK. The results of anterior interbody fusion of the cervical spine. J Bone Joint Surg [Am] 1962;44: Shapiro S. Banked fibula and the locking anterior cervical plate in anterior cervical fusions following cervical discectomy. J Neurosurg 1996;84: Vaccaro AR, Balderston RA. Anterior plate instrumentation for disorders of the subaxial cervical spine. Clin Orthop 1997;335: Zoega B, Lind B, Rosen H. Outcome After Anterior Cervical Fusion With or Without Plate Fixation. Presented at the annual meeting of the North American Spine Society, New York, NY, October 25, Address reprint requests to Jeffrey C. Wang, MD UCLA Department of Orthopaedic Surgery UCLA School of Medicine Box Los Angeles, CA jwang@ortho.medsch.ucla.edu Point of View Sanford E. Emery, MD University Hospitals of Cleveland Cleveland, Ohio This article provides more data to help determine the appropriate role of internal fixation for anterior cervical arthrodesis procedures. It is a solid clinical study that has strengths and weaknesses. My criticisms would be the lack of an outcome vehicle for evaluating the true clinical results of the procedure, which could be obtained through one of several validated questionnaire methods. It appears that the study was a retrospective chart review, with the primary surgeon, rather than a third party, evaluating the patient s clinical progress. The primary surgeon also evaluated the radiographs and determined union versus nonunion. It might have been preferable to have one of the other authors make this determination to ensure that the results were as objective as possible. The greatest strength of this study is that it comprised a homogenous set of patients undergoing two-level anterior cervical discectomy and fusion procedures. Most of the literature on this subject is a mixed bag of singleand multilevel arthrodesis operations, which makes it difficult to sort out the data. Though the groups are not randomized or concurrent, the authors looked at the demographic data, and the patient populations were comparable. The fact that one surgeon did all of the procedures also provides a consistency of surgical technique, which strengthens the study. I believe that this report provides good evidence of the ability of anterior plating on two-level anterior cervical discectomy and fusion procedures to yield an increased union rate. The results of this study also show that bone grafts alone do not collapse or settle significantly, as long as a solid arthrodesis is achieved. This is an important point to remember in the near future; if bone morphogenetic proteins can overcome the pseudarthrosis problem, then internal fixation may not always be needed. The authors have shown that pseudarthroses will result in some bone resorption and loss of height plus loss of lordosis. The clinical importance of the magnitude of these values is less clear. In this study, all pseudarthrosis patients were symptomatic enough to desire another operation. This finding is different from that of an earlier study on a large group of patients with cervical radiculopathy, where two thirds of the patients with pseudarthrosis had symptoms, but only 25% of those had enough problems to warrant operative repair. 1 The current study is straightforward and retrospective and can help guide us in the optimal care of our patients with cervical spine disorders. We need to await future prospective studies with concurrent groups of patients to help determine issues of return to work and cost effectiveness of current operative procedures. Reference 1. Bohlman HH, Emery SE, Goodfellow DB, Jones PK. Robinson anterior cervical discectomy and arthrodesis for cervical radiculopathy: Long-term follow-up of 122 patients. J Bone Joint Surg [Am} 1993;75:
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft. Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD
 Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Dynamic anterior cervical plating for multi-level spondylosis: Does it help?
 Original research Dynamic anterior cervical plating for multi-level spondylosis: Does it help? 41 41 46 Dynamic anterior cervical plating for multi-level spondylosis: Does it help? Authors Ashraf A Ragab,
Original research Dynamic anterior cervical plating for multi-level spondylosis: Does it help? 41 41 46 Dynamic anterior cervical plating for multi-level spondylosis: Does it help? Authors Ashraf A Ragab,
Prospective assessment of cervical fusion status : plain radiographs versus CT-scan
 Acta Orthop. Belg., 2006, 72, 342-346 ORIGINAL STUDY Prospective assessment of cervical fusion status : plain radiographs versus CT-scan Avraam PLOUMIS, Amir MEHBOD, Timothy GARVEY, Thomas GILBERT, Ensor
Acta Orthop. Belg., 2006, 72, 342-346 ORIGINAL STUDY Prospective assessment of cervical fusion status : plain radiographs versus CT-scan Avraam PLOUMIS, Amir MEHBOD, Timothy GARVEY, Thomas GILBERT, Ensor
Outcomes and revision rates following multilevel anterior cervical discectomy and fusion
 Original Study Outcomes and revision rates following multilevel anterior cervical discectomy and fusion Joseph L. Laratta 1, Hemant P. Reddy 2, Kelly R. Bratcher 1, Katlyn E. McGraw 1, Leah Y. Carreon
Original Study Outcomes and revision rates following multilevel anterior cervical discectomy and fusion Joseph L. Laratta 1, Hemant P. Reddy 2, Kelly R. Bratcher 1, Katlyn E. McGraw 1, Leah Y. Carreon
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Anterior cervical dynamic ABC plating with single level corpectomy and fusion in forty-two patients
 (2003) 41, 153 ± 158 ã 2003 International Society All rights reserved 1362 ± 4393/03 $25.00 www.nature.com/sc Original Article Anterior cervical dynamic ABC plating with single level corpectomy and fusion
(2003) 41, 153 ± 158 ã 2003 International Society All rights reserved 1362 ± 4393/03 $25.00 www.nature.com/sc Original Article Anterior cervical dynamic ABC plating with single level corpectomy and fusion
Cervical Curvature Became More Lordotic in Flexion Post-Operatively Regardless of Type of Surgical Approach in Cervical Spondylotic Myelopathy
 Cervical Curvature Became More Lordotic in Flexion Post-Operatively Regardless of Type of Surgical Approach in Cervical Spondylotic Myelopathy Wen-Kai Chou 1, Andy Chien 1, Ya-Wen Kuo 1, Chia-Chin Lin
Cervical Curvature Became More Lordotic in Flexion Post-Operatively Regardless of Type of Surgical Approach in Cervical Spondylotic Myelopathy Wen-Kai Chou 1, Andy Chien 1, Ya-Wen Kuo 1, Chia-Chin Lin
Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic resonance imaging study evidence
 See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
Cervical Pseudarthrosis: Diagnosis and Revision Strategies
 Cervical Pseudarthrosis: Diagnosis and Revision Strategies William C. Welch, M.D., F.A.C.S., F.I.C.S. Professor of Neurological Surgery Chief, Neurological Surgery, Pennsylvania Hospital University of
Cervical Pseudarthrosis: Diagnosis and Revision Strategies William C. Welch, M.D., F.A.C.S., F.I.C.S. Professor of Neurological Surgery Chief, Neurological Surgery, Pennsylvania Hospital University of
Anterior cervical discectomy and fusion (ACDF) is a
 ORIGINAL ARTICLE The Use of Osteotech Surface-activated Cortical Lordotic Allograft in Anterior Cervical Discectomy and Fusion Sanjitpal S. Gill, MD,* Justin L. Sala, BS,w and Randy F. Davis, MDz Abstract:
ORIGINAL ARTICLE The Use of Osteotech Surface-activated Cortical Lordotic Allograft in Anterior Cervical Discectomy and Fusion Sanjitpal S. Gill, MD,* Justin L. Sala, BS,w and Randy F. Davis, MDz Abstract:
Pseuarthrosis Post Cervical Surgery
 Pseuarthrosis Post Cervical Surgery Don Moore, MD Center for Spine Health Cleveland Clinic May 12, 2018 Pseudarthrosis Post Cervical Surgery Patient factors Surgeon factors Efficacy of index procedure
Pseuarthrosis Post Cervical Surgery Don Moore, MD Center for Spine Health Cleveland Clinic May 12, 2018 Pseudarthrosis Post Cervical Surgery Patient factors Surgeon factors Efficacy of index procedure
Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki 3), Masatsune Yamagata 1), Yoshikazu Ikeda 1), Fumitake Nakajima 1)
 Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
Discecctomy and anterior fusion with cages: advantages and disavantages. A. Zagra
 Spinal Surgery Division 1 I. R. S. S. C. Galeazzi Orthpedic Institute Milan Chief : Prof. A. Zagra Discecctomy and anterior fusion with cages: advantages and disavantages A. Zagra CONSERVATIVE TREATMENT
Spinal Surgery Division 1 I. R. S. S. C. Galeazzi Orthpedic Institute Milan Chief : Prof. A. Zagra Discecctomy and anterior fusion with cages: advantages and disavantages A. Zagra CONSERVATIVE TREATMENT
Three-Level Anterior Cervical Discectomy and Fusion with Plate Fixation: Radiographic Results of 127 Patients
 ISPUB.COM The Internet Journal of Neurosurgery Volume 6 Number 1 Three-Level Anterior Cervical Discectomy and Fusion with Plate Fixation: Radiographic Results of 127 D Bullard, J Souza Citation D Bullard,
ISPUB.COM The Internet Journal of Neurosurgery Volume 6 Number 1 Three-Level Anterior Cervical Discectomy and Fusion with Plate Fixation: Radiographic Results of 127 D Bullard, J Souza Citation D Bullard,
Cervical radiculopathy: Incidence and treatment of 1,420 consecutive cases
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 Cervical radiculopathy: Incidence and treatment of 1,420 consecutive cases Han Jo Kim Weill Cornell Medical
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 Cervical radiculopathy: Incidence and treatment of 1,420 consecutive cases Han Jo Kim Weill Cornell Medical
ELY ASHKENAZI Israel Spine Center at Assuta Hospital Tel Aviv, Israel
 nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
Fixation of multiple level anterior cervical disc using cages versus cages and plating
 Elsayed and Sakr The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2019) 55:12 https://doi.org/10.1186/s41983-019-0062-2 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery RESEARCH
Elsayed and Sakr The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2019) 55:12 https://doi.org/10.1186/s41983-019-0062-2 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery RESEARCH
Introduction. CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Autumn 2011 Vol 10 No 1 / Page 25
 CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Autumn 211 Vol 1 No 1 / Page 25 C L I N I C A L A RT I C L E Cervical PEEK cage standalone fusion the issue of subsidence RN Dunn, MBChB(UCT), FCS(SA)Orth, MMed(Orth)
CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Autumn 211 Vol 1 No 1 / Page 25 C L I N I C A L A RT I C L E Cervical PEEK cage standalone fusion the issue of subsidence RN Dunn, MBChB(UCT), FCS(SA)Orth, MMed(Orth)
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
Christopher I. Shaffrey, MD
 CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Comparison of Anterior and Posterior Approaches in Cervical Spinal Cord Injuries
 Journal of Spinal Disorders & Techniques Vol. 16, No. 3, pp. 229 235 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Comparison of Anterior and Posterior Approaches in Cervical Spinal Cord Injuries
Journal of Spinal Disorders & Techniques Vol. 16, No. 3, pp. 229 235 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Comparison of Anterior and Posterior Approaches in Cervical Spinal Cord Injuries
5/27/2016. Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation. Disclosures. LLIF Approach
 Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Comparing anterior cervical fusion using titanium cage with hydroxyapatite and with autograft
 Asian Biomedicine Vol. 4 No. 1 February 2010; 147-152 Brief communication (Original) Comparing anterior cervical fusion using titanium cage with hydroxyapatite and with autograft Prakit Tienboon a, Surapon
Asian Biomedicine Vol. 4 No. 1 February 2010; 147-152 Brief communication (Original) Comparing anterior cervical fusion using titanium cage with hydroxyapatite and with autograft Prakit Tienboon a, Surapon
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
Anterior Plating for Cervical Traumatic Fractures: An Analysis of Graft Height and Segmental Lordosis Preservation
 ISPUB.COM The Internet Journal of Spine Surgery Volume 1 Number 2 Anterior Plating for Cervical Traumatic Fractures: An Analysis of Graft Height and Segmental Lordosis L Khoo, J Benae, T Gravori Citation
ISPUB.COM The Internet Journal of Spine Surgery Volume 1 Number 2 Anterior Plating for Cervical Traumatic Fractures: An Analysis of Graft Height and Segmental Lordosis L Khoo, J Benae, T Gravori Citation
Anterior Cervical Spine Fusion Rates Using a Frozen Laminated Composite Allograft and Plating
 ISPUB.COM The Internet Journal of Spine Surgery Volume 2 Number 1 Anterior Cervical Spine Fusion Rates Using a Frozen Laminated Composite Allograft and Plating B Fox, A Gopez, W Sukovich, M Kerner Citation
ISPUB.COM The Internet Journal of Spine Surgery Volume 2 Number 1 Anterior Cervical Spine Fusion Rates Using a Frozen Laminated Composite Allograft and Plating B Fox, A Gopez, W Sukovich, M Kerner Citation
Subaxial (C3 7) cervical instability in children may
 clinical article J Neurosurg Spine 24:892 896, 2016 Management of subaxial cervical instability in very young or small-for-age children using a static single-screw anterior cervical plate: indications,
clinical article J Neurosurg Spine 24:892 896, 2016 Management of subaxial cervical instability in very young or small-for-age children using a static single-screw anterior cervical plate: indications,
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device
 Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Zongyu Zhang 1, Yawei Li 2 and Weimin Jiang 1*
 Zhang et al. BMC Musculoskeletal Disorders (2018) 19:119 https://doi.org/10.1186/s12891-018-2033-7 RESEARCH ARTICLE Open Access A comparison of zero-profile anchored spacer (ROI-C) and plate fixation in
Zhang et al. BMC Musculoskeletal Disorders (2018) 19:119 https://doi.org/10.1186/s12891-018-2033-7 RESEARCH ARTICLE Open Access A comparison of zero-profile anchored spacer (ROI-C) and plate fixation in
Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis
 CLINICAL ARTICLE Kor J Spine 5(3):111-115, 2008 Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis Ki Suk Choi, M.D., Il Tae Jang, M.D., Jae Hyeon Lim,
CLINICAL ARTICLE Kor J Spine 5(3):111-115, 2008 Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis Ki Suk Choi, M.D., Il Tae Jang, M.D., Jae Hyeon Lim,
Cost-effectiveness of single-level anterior cervical discectomy and fusion for cervical spondylosis Angevine P D, Zivin J G, McCormick P C
 Cost-effectiveness of single-level anterior cervical discectomy and fusion for cervical spondylosis Angevine P D, Zivin J G, McCormick P C Record Status This is a critical abstract of an economic evaluation
Cost-effectiveness of single-level anterior cervical discectomy and fusion for cervical spondylosis Angevine P D, Zivin J G, McCormick P C Record Status This is a critical abstract of an economic evaluation
Anterior cervical interbody fusion with radiolucent carbon fiber cages : clinical and radiological results
 Acta Orthop. Belg., 2005, 71, 604-609 ORIGINAL STUDY Anterior cervical interbody fusion with radiolucent carbon fiber cages : clinical and radiological results Ibo VAN DER HAVEN, Piet J. M. VAN LOON, Ronald
Acta Orthop. Belg., 2005, 71, 604-609 ORIGINAL STUDY Anterior cervical interbody fusion with radiolucent carbon fiber cages : clinical and radiological results Ibo VAN DER HAVEN, Piet J. M. VAN LOON, Ronald
Artificial Disc Replacement, Cervical
 Artificial Disc Replacement, Cervical Policy Number: Original Effective Date: MM.06.001 02/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO 11/01/2011 Section: Surgery Place(s) of Service:
Artificial Disc Replacement, Cervical Policy Number: Original Effective Date: MM.06.001 02/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO 11/01/2011 Section: Surgery Place(s) of Service:
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
Innovative Techniques in Minimally Invasive Cervical Spine Surgery. Bruce McCormack, MD San Francisco California
 Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Radiographic and clinical outcomes following single-level anterior cervical discectomy and allograft fusion without plate placement or cervical collar
 J Neurosurg Spine 8:420 428, 2008 Radiographic and clinical outcomes following single-level anterior cervical discectomy and allograft fusion without plate placement or cervical collar JAY JAGANNATHAN,
J Neurosurg Spine 8:420 428, 2008 Radiographic and clinical outcomes following single-level anterior cervical discectomy and allograft fusion without plate placement or cervical collar JAY JAGANNATHAN,
Artificial Disc Replacement, Cervical
 Artificial Disc Replacement, Cervical Policy Number: Original Effective Date: MM.06.001 02/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 01/01/2014 Section: Surgery Place(s) of Service:
Artificial Disc Replacement, Cervical Policy Number: Original Effective Date: MM.06.001 02/01/2010 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 01/01/2014 Section: Surgery Place(s) of Service:
Distractable Vertebral Cages for Reconstruction After Cervical Corpectomy
 Distractable Vertebral Cages for Reconstruction After Cervical Corpectomy SPINE Volume 30, Number 15, pp 1736 1741 2005, Lippincott Williams & Wilkins, Inc. Christian Woiciechowsky, MD, PhD Study Design.
Distractable Vertebral Cages for Reconstruction After Cervical Corpectomy SPINE Volume 30, Number 15, pp 1736 1741 2005, Lippincott Williams & Wilkins, Inc. Christian Woiciechowsky, MD, PhD Study Design.
Spinal Fusion. North American Spine Society Public Education Series
 Spinal Fusion North American Spine Society Public Education Series What Is Spinal Fusion? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Spinal Fusion North American Spine Society Public Education Series What Is Spinal Fusion? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
Outcome of Anterior Cervical Discectomy and Fusion with Autograft and Plating in management of Cervical Spondylotic Myelopathy
 ISPUB.COM The Internet Journal of Spine Surgery Volume 5 Number 1 Outcome of Anterior Cervical Discectomy and Fusion with Autograft and Plating in management of Cervical Spondylotic Myelopathy V Kumar,
ISPUB.COM The Internet Journal of Spine Surgery Volume 5 Number 1 Outcome of Anterior Cervical Discectomy and Fusion with Autograft and Plating in management of Cervical Spondylotic Myelopathy V Kumar,
Anterior cervical diskectomy icd 10 procedure code
 Home Anterior cervical diskectomy icd 10 procedure code Access to discounts at hundreds of restaurants, travel destinations, retail stores, and service providers. AAPC members also have opportunities to
Home Anterior cervical diskectomy icd 10 procedure code Access to discounts at hundreds of restaurants, travel destinations, retail stores, and service providers. AAPC members also have opportunities to
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
PARADIGM SPINE. Anterior Cervical Fusion Cage. Cervical Interbody Fusion
 PARADIGM SPINE Anterior Cervical Fusion Cage Cervical Interbody Fusion DESIGN RATIONALE The OptiStrain TM C* interbody fusion cage follows well established biomechanical principles: The slot design of
PARADIGM SPINE Anterior Cervical Fusion Cage Cervical Interbody Fusion DESIGN RATIONALE The OptiStrain TM C* interbody fusion cage follows well established biomechanical principles: The slot design of
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy
 Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Fusion Device. Surgical Technique. Cervical Interbody Fusion with Trabecular Metal Technology
 TM-S Fusion Device Surgical Technique Cervical Interbody Fusion with Trabecular Metal Technology 2 TM-S Fusion Device Surgical Technique Disclaimer This surgical technique is not intended for use in the
TM-S Fusion Device Surgical Technique Cervical Interbody Fusion with Trabecular Metal Technology 2 TM-S Fusion Device Surgical Technique Disclaimer This surgical technique is not intended for use in the
Preoperative Narcotic Use as a Predictor of Clinical Outcome
 SPINE Volume 33, Number 19, pp 2074 2078 2008, Lippincott Williams & Wilkins Narcotic Use as a Predictor of Clinical Outcome Results Following Anterior Cervical Arthrodesis J. Todd R. Lawrence, MD, PhD,*
SPINE Volume 33, Number 19, pp 2074 2078 2008, Lippincott Williams & Wilkins Narcotic Use as a Predictor of Clinical Outcome Results Following Anterior Cervical Arthrodesis J. Todd R. Lawrence, MD, PhD,*
Cervical Spine Surgery: Approach related outcome
 Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Rick C. Sasso MD Professor Chief of Spine Surgery Clinical Orthopaedic Surgery Indiana University School of Medicine
 Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Comparative study on the effect of anterior and posterior decompression in the treatment of multi-segmental cervical spondylotic myelopathy
 92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
Matthew Colman, MD Assistant Professor, Spine Surgery and Musculoskeletal Oncology Rush University Medical Center ACDF
 is the most reliable option for twolevel anterior cervical surgery Matthew Colman, MD Assistant Professor, Spine Surgery and Musculoskeletal Oncology Rush University Medical Center Disclosures Medicrea:
is the most reliable option for twolevel anterior cervical surgery Matthew Colman, MD Assistant Professor, Spine Surgery and Musculoskeletal Oncology Rush University Medical Center Disclosures Medicrea:
Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report
 Int J Clin Exp Med 2016;9(4):7349-7353 www.ijcem.com /ISSN:1940-5901/IJCEM0018962 Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report Yi Yang 1, Mengying
Int J Clin Exp Med 2016;9(4):7349-7353 www.ijcem.com /ISSN:1940-5901/IJCEM0018962 Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report Yi Yang 1, Mengying
Unanswered Questions. Laminoplasty is best
 Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Common fracture & dislocation of the cervical spine. Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University
 Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Abstract Study Design This is a retrospective review of a prospectively maintained database of. Dennis E. Bullard 1,2,3 Jillian S.
 Original Research 13 Early Morbidity of Multilevel Anterior Cervical Discectomy and Fusion with Plating for Spondylosis: Does the Number of Levels Influence Early Complications? A Single Surgeon s Experience
Original Research 13 Early Morbidity of Multilevel Anterior Cervical Discectomy and Fusion with Plating for Spondylosis: Does the Number of Levels Influence Early Complications? A Single Surgeon s Experience
EFSPINE CERVICAL COMBINED SET DISC PROTHESIS ORGANIZER BOX
 EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
Cervical corpectomy for sub-axial retro-vertebral body lesions
 Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Anterior Discectomy With Fusion And Stabilization For The Management Of Mono-Segmental Cervical Spondylotic Radiculopathy And Myelopathy
 ISPUB.COM The Internet Journal of Spine Surgery Volume 3 Number 2 Anterior Discectomy With Fusion And Stabilization For The Management Of Mono-Segmental Cervical Spondylotic Radiculopathy And Myelopathy
ISPUB.COM The Internet Journal of Spine Surgery Volume 3 Number 2 Anterior Discectomy With Fusion And Stabilization For The Management Of Mono-Segmental Cervical Spondylotic Radiculopathy And Myelopathy
) ACDF. (Japanese Orthopaedic Association,JOA) ACCF (175.4±12.1ml VS 201.3±80.4ml) ACDF JOA VAS (P=0.000),ACCF :A : X(2015)
 2015 25 5 Chinese Journal of Spine and Spinal Cord,2015,Vol.25,No.5 433 1, 2, 2, 3, 3 (1 ;2 466000 ;3 466000 ) : (anterior cervical discectomy and fusion,acdf) (anterior cervical corpectomy and fusion,accf)
2015 25 5 Chinese Journal of Spine and Spinal Cord,2015,Vol.25,No.5 433 1, 2, 2, 3, 3 (1 ;2 466000 ;3 466000 ) : (anterior cervical discectomy and fusion,acdf) (anterior cervical corpectomy and fusion,accf)
Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review comparing multilevel versus single-level surgery
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review ( ) 19 19 30 Cervical artificial disc replacement versus fusion in the cervical spine: a
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review ( ) 19 19 30 Cervical artificial disc replacement versus fusion in the cervical spine: a
ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc disease: Is there a difference at 12 months?
 Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Case Report Two-year follow-up results of artificial disc replacement C7-T1
 Int J Clin Exp Med 2016;9(2):4748-4753 www.ijcem.com /ISSN:1940-5901/IJCEM0018942 Case Report Two-year follow-up results of artificial disc replacement C7-T1 Yi Yang 1, Litai Ma 1, Shan Wu 1, Ying Hong
Int J Clin Exp Med 2016;9(2):4748-4753 www.ijcem.com /ISSN:1940-5901/IJCEM0018942 Case Report Two-year follow-up results of artificial disc replacement C7-T1 Yi Yang 1, Litai Ma 1, Shan Wu 1, Ying Hong
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Cervical Motion Preservation
 Spinal Disorders D. Pelinkovic, M. D. M&M Orthopaedics 1259 Rickert Drive Naperville, IL 1900 Ogden Ave Aurora, IL Cervical Motion Preservation Neck Pain Symptoms Trapezius myalgia ( Phosphates Bengston
Spinal Disorders D. Pelinkovic, M. D. M&M Orthopaedics 1259 Rickert Drive Naperville, IL 1900 Ogden Ave Aurora, IL Cervical Motion Preservation Neck Pain Symptoms Trapezius myalgia ( Phosphates Bengston
Medical Policy. Cervical Spinal Fusion Effective Date December 15, Description. Related Policies. Policy. Subsection. 7.
 BSC7.05 Section 7.0 Surgery Subsection Cervical Spinal Fusion Effective Date December 15, 2014 Original Policy Date December 15, 2014 Next Review Date December 2015 Description Cervical spinal fusion (arthrodesis)
BSC7.05 Section 7.0 Surgery Subsection Cervical Spinal Fusion Effective Date December 15, 2014 Original Policy Date December 15, 2014 Next Review Date December 2015 Description Cervical spinal fusion (arthrodesis)
Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion
 Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion Andrei Stefan Iencean ROMANIA DOI:
Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion Andrei Stefan Iencean ROMANIA DOI:
CROSS -FUSE P E E K V B R / I B F SYST E M
 S U R G I C A L T E C H N I Q U E CROSS -FUSE P E E K V B R / I B F SYST E M S U R G I C A L S Y S T E M O V E R V I E W 2 CROSS-FUSE P E E K V B R / I B F S Y S T E M S U R G I C A L T E C H N I Q U E
S U R G I C A L T E C H N I Q U E CROSS -FUSE P E E K V B R / I B F SYST E M S U R G I C A L S Y S T E M O V E R V I E W 2 CROSS-FUSE P E E K V B R / I B F S Y S T E M S U R G I C A L T E C H N I Q U E
Subaxial Cervical Spine Trauma Dr Hesarikia BUMS
 Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
Surgical Management of Cervical Spondyloarthropathy in Hemodialysis Patients
 The Open Orthopaedics Journal, 2010, 4, 39-43 39 Open Access Surgical Management of Cervical Spondyloarthropathy in Hemodialysis Patients Panayiotis Spinos 1, Charalambos Matzaroglou *,2, Meni Partheni
The Open Orthopaedics Journal, 2010, 4, 39-43 39 Open Access Surgical Management of Cervical Spondyloarthropathy in Hemodialysis Patients Panayiotis Spinos 1, Charalambos Matzaroglou *,2, Meni Partheni
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF)
 Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF) Calusa Ambulatory Spine Conference 2016 Jason Inzana, PhD 1 ; Anup Gandhi,
Biomechanics of Interspinous Process Fixation and Lateral Modular Plate Fixation to Support Lateral Lumbar Interbody Fusion (LLIF) Calusa Ambulatory Spine Conference 2016 Jason Inzana, PhD 1 ; Anup Gandhi,
Anterior Cervical Discectomy with Stand Alone PEEK Cage for Management of 3 and 4 Level Degenerative Cervical Disc Disease *
 WScJ 3: 201-209, 2016 Anterior Cervical Discectomy with Stand Alone PEEK Cage for Management of 3 and 4 Level Degenerative Cervical Disc Disease * Khaled MF Saoud, Hazem A Mashaly, Hatem Sabry Department
WScJ 3: 201-209, 2016 Anterior Cervical Discectomy with Stand Alone PEEK Cage for Management of 3 and 4 Level Degenerative Cervical Disc Disease * Khaled MF Saoud, Hazem A Mashaly, Hatem Sabry Department
Treatment of Two Level Artificial Disc Replacement for Cervical Spondylotic Myelopathy
 Journal of Minimally Invasive Spine JMISST Surgery and Technique 3(1):34-38, 2018 Case Report eissn 2508-2043 https://doi.org/10.21182/jmisst.2017.00269 www.jmisst.org for Cervical Spondylotic Myelopathy
Journal of Minimally Invasive Spine JMISST Surgery and Technique 3(1):34-38, 2018 Case Report eissn 2508-2043 https://doi.org/10.21182/jmisst.2017.00269 www.jmisst.org for Cervical Spondylotic Myelopathy
Use of the operating microscope anterior cervical discectomy without fusion. KEY WORDS 9 cervical discectomy 9 fusion 9 intervertebral disc
 Use of the operating microscope anterior cervical discectomy without fusion in HAL L. HANKINSON, M.D., AND CHARLES B. WILSON, M.D. Department of Neurological Surgery, University of California School of
Use of the operating microscope anterior cervical discectomy without fusion in HAL L. HANKINSON, M.D., AND CHARLES B. WILSON, M.D. Department of Neurological Surgery, University of California School of
Risk factors for non-fusion segment disease after anterior cervical spondylosis surgery: a retrospective study with long-term followup of 171 patients
 Wang et al. Journal of Orthopaedic Surgery and Research (2018) 13:27 DOI 10.1186/s13018-018-0717-1 REGULAR ARTICLE Open Access Risk factors for non-fusion segment disease after anterior cervical spondylosis
Wang et al. Journal of Orthopaedic Surgery and Research (2018) 13:27 DOI 10.1186/s13018-018-0717-1 REGULAR ARTICLE Open Access Risk factors for non-fusion segment disease after anterior cervical spondylosis
Clinical Article Disc height loss after anterior cervical microdiscectomy with titanium intervertebral cage fusion
 Acta Neurochir (2003) 145: 565 570 DOI 10.1007/s00701-003-0050-1 Clinical Article Disc height loss after anterior cervical microdiscectomy with titanium intervertebral cage fusion K. Türeyen S uleyman
Acta Neurochir (2003) 145: 565 570 DOI 10.1007/s00701-003-0050-1 Clinical Article Disc height loss after anterior cervical microdiscectomy with titanium intervertebral cage fusion K. Türeyen S uleyman
Neurologic Recovery after Anterior Cervical Discectomy and Fusion
 Global Spine Journal Original Article 41 Neurologic Recovery after Anterior Cervical Discectomy and Fusion Charles L. Lehmann 1 Jacob M. Buchowski 1 Geoffrey E. Stoker 1 K. Daniel Riew 1 1 Department of
Global Spine Journal Original Article 41 Neurologic Recovery after Anterior Cervical Discectomy and Fusion Charles L. Lehmann 1 Jacob M. Buchowski 1 Geoffrey E. Stoker 1 K. Daniel Riew 1 1 Department of
Cervical canal stenosis and adjacent segment degeneration after anterior cervical arthrodesis
 Eur Spine J (215) 24:159 1596 DOI 1.17/s586-15-3975-1 ORIGINAL ARTICLE Cervical canal stenosis and adjacent segment degeneration after anterior cervical arthrodesis Jing Tao Zhang 1 Jun Ming Cao 1 Fan
Eur Spine J (215) 24:159 1596 DOI 1.17/s586-15-3975-1 ORIGINAL ARTICLE Cervical canal stenosis and adjacent segment degeneration after anterior cervical arthrodesis Jing Tao Zhang 1 Jun Ming Cao 1 Fan
Clinical Outcomes After Four-Level Anterior Cervical Discectomy and Fusion.
 Thomas Jefferson University Jefferson Digital Commons Rothman Institute Rothman Institute 12-1-2018 Clinical Outcomes After Four-Level Anterior Cervical Discectomy and Fusion. Tyler M Kreitz Thomas Jefferson
Thomas Jefferson University Jefferson Digital Commons Rothman Institute Rothman Institute 12-1-2018 Clinical Outcomes After Four-Level Anterior Cervical Discectomy and Fusion. Tyler M Kreitz Thomas Jefferson
Royal Oak Cervical Plate System
 Royal Oak Cervical Plate System Manufactured by Nexxt Spine, Inc. Royal Oak Cervical Plate System INTRODUCTION FEATURES AND BENEFITS Table of Contents SURGICAL TECHNIQUE Step 1. Patient Positioning Step
Royal Oak Cervical Plate System Manufactured by Nexxt Spine, Inc. Royal Oak Cervical Plate System INTRODUCTION FEATURES AND BENEFITS Table of Contents SURGICAL TECHNIQUE Step 1. Patient Positioning Step
Efficacy of PEEK Cages and Plate Augmentation in Three-Level Anterior Cervical Fusion of Elderly Patients
 Original Article Clinics in Orthopedic Surgery 2011;3:9-15 doi:10.4055/cios.2011.3.1.9 Efficacy of PEEK Cages and Plate Augmentation in Three-Level Anterior Cervical Fusion of Elderly Patients Kyung Jin
Original Article Clinics in Orthopedic Surgery 2011;3:9-15 doi:10.4055/cios.2011.3.1.9 Efficacy of PEEK Cages and Plate Augmentation in Three-Level Anterior Cervical Fusion of Elderly Patients Kyung Jin
Robinson anterior cervical discectomy and arthrodesis for cervical radiculopathy. Long-term follow-up of one hundred and twenty-two patients
 This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Robinson anterior cervical discectomy and arthrodesis for cervical radiculopathy.
This is an enhanced PDF from The Journal of Bone and Joint Surgery The PDF of the article you requested follows this cover page. Robinson anterior cervical discectomy and arthrodesis for cervical radiculopathy.
Clinical and radiographic outcome of dynamic cervical implant (DCI) arthroplasty for degenerative cervical disc disease: a minimal five-year follow-up
 Wang et al. BMC Musculoskeletal Disorders (2018) 19:101 https://doi.org/10.1186/s12891-018-2017-7 RESEARCH ARTICLE Open Access Clinical and radiographic outcome of dynamic cervical implant (DCI) arthroplasty
Wang et al. BMC Musculoskeletal Disorders (2018) 19:101 https://doi.org/10.1186/s12891-018-2017-7 RESEARCH ARTICLE Open Access Clinical and radiographic outcome of dynamic cervical implant (DCI) arthroplasty
C-THRU Anterior Spinal System
 C-THRU Anterior Spinal System Surgical Technique Manufactured From Contents Introduction... Page 1 Design Features... Page 2 Instruments... Page 3 Surgical Technique... Page 4 Product Information... Page
C-THRU Anterior Spinal System Surgical Technique Manufactured From Contents Introduction... Page 1 Design Features... Page 2 Instruments... Page 3 Surgical Technique... Page 4 Product Information... Page
5/19/2017. Disclosures. Introduction. How Much Kyphosis is Allowable for Cervical Total Disc Replacement? And Other Considerations
 How Much Kyphosis is Allowable for Cervical Total Disc Replacement? And Other Considerations Richard D. Guyer, M.D. Disclosures Guyer (a) Alphatec; (b) Spinal Kinetics, Spinal Ventures, Mimedix; (c) DePuy
How Much Kyphosis is Allowable for Cervical Total Disc Replacement? And Other Considerations Richard D. Guyer, M.D. Disclosures Guyer (a) Alphatec; (b) Spinal Kinetics, Spinal Ventures, Mimedix; (c) DePuy
Comparative Study of Clinical Outcomes of Anterior Cervical Discectomy and Fusion Using Autobone Graft or Cage with Bone Substitute
 Asian Spine Journal Vol. 5, No. 3, pp 169~175, 2011 http://dx.doi.org/10.4184/asj.2011.5.3.169 Comparative Study of Clinical Outcomes of Anterior Cervical Discectomy and Fusion Using Autobone Graft or
Asian Spine Journal Vol. 5, No. 3, pp 169~175, 2011 http://dx.doi.org/10.4184/asj.2011.5.3.169 Comparative Study of Clinical Outcomes of Anterior Cervical Discectomy and Fusion Using Autobone Graft or
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
Complex Spine Symposium January 12th, Balgrist University Hospital
 DEGENERATIVE CERVICAL MYELOPATHY CLINICAL DECISION MAKING Prof. Dr. Mazda Farshad Chair of Orthopedic Surgery Chief of Spine Surgery Medical Director CERVICAL MYELOPATHY - CAUSES degenerative cervical
DEGENERATIVE CERVICAL MYELOPATHY CLINICAL DECISION MAKING Prof. Dr. Mazda Farshad Chair of Orthopedic Surgery Chief of Spine Surgery Medical Director CERVICAL MYELOPATHY - CAUSES degenerative cervical
Original Policy Date
 MP 7.01.110 Axial Lumbosacral Interbody Fusion Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search12/2013 Return to Medical
MP 7.01.110 Axial Lumbosacral Interbody Fusion Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search12/2013 Return to Medical
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs. Cervical Disc Replacement
 SpineFAQs Cervical Disc Replacement Artificial disc replacement (ADR) is relatively new. In June 2004, the first ADR for the lumbar spine (low back) was approved by the FDA for use in the US. Replacing
SpineFAQs Cervical Disc Replacement Artificial disc replacement (ADR) is relatively new. In June 2004, the first ADR for the lumbar spine (low back) was approved by the FDA for use in the US. Replacing
Jing Tao Zhang 1, Lin Feng Wang 1, Yue Ju Liu 2, Jun Ming Cao 1, Jie Li 1, Shuai Wang 1 and Yong Shen 1*
 Zhang et al. BMC Musculoskeletal Disorders (2015) 16:267 DOI 10.1186/s12891-015-0728-6 RESEARCH ARTICLE Open Access Relationship between developmental canal stenosis and surgical results of anterior decompression
Zhang et al. BMC Musculoskeletal Disorders (2015) 16:267 DOI 10.1186/s12891-015-0728-6 RESEARCH ARTICLE Open Access Relationship between developmental canal stenosis and surgical results of anterior decompression
Medical Policy Original Effective Date: Revised Date: Page 1 of 11
 Page 1 of 11 Content Disclaimer Description Coverage Determination Clinical Indications Lumbar Spine Surgery Lumbar Spine Surgery Description Indication Coding Lumbar Spinal Fusion (single level)surgery
Page 1 of 11 Content Disclaimer Description Coverage Determination Clinical Indications Lumbar Spine Surgery Lumbar Spine Surgery Description Indication Coding Lumbar Spinal Fusion (single level)surgery
Cervical spondylotic myelopathy (CSM) is a progressive
 literature review J Neurosurg Spine 24:77 99, 2016 A systematic review of clinical and surgical predictors of complications following surgery for degenerative cervical myelopathy Lindsay Tetreault, BSc,
literature review J Neurosurg Spine 24:77 99, 2016 A systematic review of clinical and surgical predictors of complications following surgery for degenerative cervical myelopathy Lindsay Tetreault, BSc,
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY
 CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
Skip corpectomy in the treatment of multilevel cervical spondylotic myelopathy and ossified posterior longitudinal ligament
 J Neurosurg Spine 12:33 38, 2010 Skip corpectomy in the treatment of multilevel cervical spondylotic myelopathy and ossified posterior longitudinal ligament Technical note Se d a t Da l bay r a k, M.D.,
J Neurosurg Spine 12:33 38, 2010 Skip corpectomy in the treatment of multilevel cervical spondylotic myelopathy and ossified posterior longitudinal ligament Technical note Se d a t Da l bay r a k, M.D.,
OPERATIVE TECHNIQUE. CONSTRUX Mini PTC. Mini PTC Spacer System
 OPERATIVE TECHNIQUE CONSTRUX Mini PTC Mini PTC Spacer System TABLE OF CONTENTS Introduction 1 Operative Technique 2 Part Numbers 6 Indications For Use 7 INTRODUCTION 1 INTRODUCTION The CONSTRUX Mini PTC
OPERATIVE TECHNIQUE CONSTRUX Mini PTC Mini PTC Spacer System TABLE OF CONTENTS Introduction 1 Operative Technique 2 Part Numbers 6 Indications For Use 7 INTRODUCTION 1 INTRODUCTION The CONSTRUX Mini PTC
