19 Arthrodesis of the First Metatarsocuneiform Joint
|
|
|
- Melissa McCoy
- 6 years ago
- Views:
Transcription
1 19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in Lapidus in 1934 advocated fusion of the first and second metatarsals with the first cuneiform. 2 Overall uses of the procedure since its initiation have been dedicated to hallux valgus with a relatively high intermetatarsal angle. Clark, Veith, Sangeorzan, and Hansen have utilized the Lapidus procedure for correction in postadolescent hallux valgus. 3,4 Bacardi and Saffo have advocated the utilization of the procedure for severe metatarsus primus varus. 5,6 The procedure has gained popularity in the past 10 years, perhaps because The Association for the Study of Internal Fixation (ASIF) techniques, with more precise placement of the distal first metatarsal and high fusion rates, have been used. Objectives of the procedure include reduction of the high intermetatarsal angle and stabilization of obliquity/hypermobility at the first metatarsocuneiform joint. Previous complications of the procedure included less than optimal position of the first metatarsal head, secondary to elevation, or nonunion, which may produce moderate to severe forefoot instability. 1,2,5-7 Patient selection varies with age; however, most procedures have been targeted to the adolescent-to- 50-year-old population. In most instances, the patient complains of shoe-fitting difficulties as well as appearance problems, pain, ambulatory difficulties, and impingement syndromes to the lateral forefoot, including formation of metatarsalgia, hammer toes, and Morton's neuroma. Specific indications for the procedure include juvenile hallux valgus with obliquity or hypermobility at the first metatarsocuneiform joint, paralytic hallux valgus (either spastic or flaccid in nature), osteoarthritis, traumatic degenerative joint disease secondary to an old Lisfranc injury, severe adult hallux valgus with intermetatarsal angles exceeding 18 (Fig. 19-1), and as an ancillary procedure for the correction of flatfoot of an idiopathic nature or secondary to a posterior tibial tendon rupture, generalized ligamentous laxity, or medial column instability. The procedure is usually combined with a distal first metatarsal procedure, including exostectomy, sesamoid release, distal or midshaft first metatarsal osteotomy, joint implant and proximal phalangeal techniques, including the modified Keller bunionectomy or Regnauld procedure. Arthrodesis is used less frequently than proximal metatarsal osteotomies or distal osteotomies, which may be secondary to the complications encountered in performing the technique. Excess bone removal or elevation of the distal fragment will cause severe forefoot dysfunction, a result that is less than optimal. Patient selection is of paramount importance in the procedure. The long-term effects of fusion of the first metatarsocuneiform joint in the adolescent population are not specifically known at this time. The incidence of nonunion approaches 10 percent and is also a factor in increasing the complication rate with this procedure. 5 Specific preoperative criteria can be highlighted in three areas: (1) hallux valgus; (2) osteoarthritis of degenerative joint disease of the metatarsocuneiform articulation; and (3) as an adjunct procedure to increase 279
2 280 HALLUX VALGUS AND FOREFOOT SURGERY taken to assess the articular surface because in severe cases of hallux valgus, the functional articular surface is percent of the total joint area. Repositioning in instances such as these may cause increased evidence of osteoarthritis and future disability. Fusion of the first metatarsocuneiform joint is indicated in cases of degenerative joint disease or osteoarthritis (Fig. 19-2), which is often secondary to Lisfranc's fracture/dislocation or overt injury to this area. Distal medial column stabilization procedures are indicated by the use of this technique when there has Fig Severe hallux valgus. medial column stability secondary to paralytic dysfunction or tendon rupture. Hallux valgus-specific criteria include an intermetatarsal angle exceeding 18 and hypermobility or obliquity of the first metatarsocuneiform joint. The distal first metatarsophalangeal joint should have a hallux abductus angle exceeding 25, with moderate to severe hallux valgus present. There is no contraindication in performing this procedure on an arthritic joint; however, ancillary procedures such as a Keller bunionectomy or Silastic prosthesis may be utilized in cases in which arthritis is present. Care must also be Fig Osteoarthritis secondary to an old Lisfranc injury.
3 ARTHRODESIS OF THE FIRST METATARSOCUNEIFORM JOINT 281 been a disturbance to the medial column, secondary to a tendon injury such as a partial or complete rupture of the posterior tibial tendon or an overt or subtle Lisfranc's derangement. Paralytic deformities that affect muscle tendon units surrounding this joint system are also indications for this procedure. Stabilization in the presence of spastic or flaccid paralysis of the external or intrinsic muscle groups is indicated for direct control of the unstable area. Whether one fuses the joint for osteoarthritis or for correction of severe hallux valgus, two factors are of primary importance. The first is fusion. Throughout literature reviews, nonunion of the joint has been as high as 10 percent. Although most authors state that they have very little problem with nonunions in this area, the long-term effect can be disastrous. The second is exact placement of the metatarsal so that proper metatarsal declination is achieved. It is a common tendency to elevate the first metatarsal, thus imparting undue stress on the lateral metatarsals. The overall principles of the procedure have changed, especially with the introduction of small ASIF screws and plates. Crossed Kirschner wires (K-wires) were formerly the procedure of choice, with long-term non-weight-bearing for fusion. In the mid-1970s, screws became the procedure of choice, as advocated by Clark, Hansen, Veith, and others in the latter part of the 1970s and early 1980s. 3,4 During the past 7 years, we have used a small plate combined with screw fixation to achieve more exact reduction (Fig. 19-3). The use of a soft template allows the proper declination to be imparted to the fusion site, and from this template, the plate can be prebent to achieve this process. The plate can also be utilized with or without a bone graft. Other technical considerations include protection of the medial nerve, which courses along the incision sites in many cases. Care also must be taken not to remove excess bone to avoid shortening with subsequent lateral forefoot dysfunction. When more than 2 mm of bone removal is anticipated, the utilization of a small bone graft from the medial cuneiform is extremely helpful. THE PROCEDURE The first metatarsophalangeal joint is generally exposed, and distal procedures are performed initially. If an osteotomy is performed or an implant is to be inserted, the cuts are made without fixation until the fusion site is stabilized proximally. Before the proximal incision is made, the outline of the joint is marked with a skin-marking pencil. This allows the incision to be placed correctly and provides maximum exposure to the bean-shaped joint. The incision is made approximately 1 to 1.5 in. long dorsomedially, with great care being taken to protect the medial nerve. Care must also be exercised to preserve the attachment of the tibialis anterior, as well as the Fig Plate fixation of first metatarsocuneiform fusion.
4 282 HALLUX VALGUS AND FOREFOOT SURGERY distal attachments of the posterior tibial tendon. A sharp incision should be made to the joint and a very sharp periosteal elevator utilized to elevate both the ligaments and the capsule from the articulation for later repositioning over the fusion site. The area and amount of bone removed depend on the desired result. Generally, however, as little bone as possible is removed. Enough bone should be removed plantarly to allow some plantar flexion of the first metatarsal. A laminar spreader may be helpful in visualizing the plantar surface of this somewhat irregular bean-shaped joint. If failed reconstructive bunion surgery or severe intermetatarsal angle correction is necessary, 3-5 mm of bone graft may be necessary to avoid shortening. The bone can be obtained from the posterior iliac crest or as a small wedge from the first cuneiform. The graft should be wedged safe with the base directed dorsally. The metatarsal should be plantar-flexed in approximately of plantar flexion. When there is significant diastasis between the first and second metatarsals, the medial aspect of the second metatarsal metaphysis should be incorporated into the fusion. Once the bone cuts have been made and the graft inserted (if necessary), a simple technique allows preliminary manipulation of the fusion site before final fixation is applied. We utilize this in not only first metatarsocuneiform, but also great toe joint fusions. The techniques involve driving a 0.45 or 0.62 K-wire through the fusion site and graft, if inserted. The distal metatarsal is then plantar-flexed and abducted the desired amount until correct positioning is achieved. Once this position is achieved, we use a small plate and one or two screws for fixation. We previously utilized a 2.7 or 3.5 semi-tubular plate to achieve rigid stability, but now use the titanium limited contact dynamic compression plate for this joint (Fig. 19-4). The plates are thinner, lighter in weight, and rigid, and can be prebent more easily. In most instances, two holes are utilized for the cuneiform and two holes for the first metatarsal. As previously mentioned, the plate should be prebent to approximately of plantar flexion, as well as the desired amount of abduction, to achieve correction. Sangeorzan, Veith, and Hansen advocate the use of cortical screws for stabilization of the fusion site. 3,4 One screw is used to stabilize the first metatarsocuneiform joint and the second to stabilize the first metatarsal against the medial as- Fig Titanium limited contact dynamic compression plate fixation with bone graft. pect of the second metatarsal. We have also used this technique, but found that limited metaphyseal curvature on the bone may make insertion of these screws somewhat difficult. Other types of fixation that can be utilized are crossed K-wires and staples. It is important to realize the dimensional analysis of this procedure. In cases of hallux valgus, the average intermetatarsal angle exceeds normal by When the osteotomy is completed, the intermetatarsal angle should be reduced to less than this; this angle should be carefully measured at the operative site to avoid overcorrection. It is also extremely important to achieve degrees of plantar declination of the distal first metatarsal. As mentioned before, this is best achieved by the use of a combination of plate and screw fixation techniques to achieve good alignment. Great care also must be taken to measure the length of the first metatarsal pre- and postoperatively, to assess
5 ARTHRODESIS OF THE FIRST METATARSOCUNEIFORM JOINT 283 the amount of shortening that is likely to occur. Excess shortening of the first metatarsal can create an adverse biomechanical situation on the lateral forefoot, resulting in disability and pain. The key points of the procedure include protecting the medial nerve from transection or irritation, obtaining adequate position of the distal first metatarsal in plantar flexion and abduction if necessary, good compression across the osteotomy site (our preference is plates and screws), utilization of a bone graft when necessary to prevent shortening, and careful tissue handling to avoid necrosis and infection. Potential intraoperative difficulties include damage to the neurovascular bundle, elevation of the first metatarsal, excess bone removal, and excessive soft tissue damage. Additional complications can occur distally where severe hallux valgus may render the first metatarsophalangeal joint (MPJ) cartilage less than optimum. Therefore, the patient should understand that ancillary procedures may have to be performed, including fusion or limited-resection Keller bunionectomy, or first metatarsal osteotomy to achieve first MPJ mobilization. Care must be taken not to overcorrect the hallux so that a varus occurs. 7 The procedure is extremely technically demanding and should be attempted only by a surgeon familiar with the area, and who has had some previous training in this technique. The criteria for excellent results, similar to those established by Bonney and McNab, 8 include a normal intermetatarsal angle of approximately 8, a normal hallux abductus angle of approximately 15, elimination of pain at the joint site or first metatarsophalangeal joint, elimination of first-ray hypermobility, functional and cosmetic patient satisfaction, ability to wear normal shoe gear, and absence of stiffness of the first metatarsophalangeal joint. Specific complications of this procedure include medial neuralgia, which has been mentioned in many studies because of the close proximity of the nerve medially. Great care must be taken to protect the nerve to avoid this complication. Nonunion has been mentioned in as many as 10 percent of cases by Clark, 3 and in 6 of 54 feet by Saffo et al. 6 Mauldin et al. reported 50 percent formation of plantar osteophytes at the fusion site (Fig. 19-5). Transfer lesions have been found in as many as 14 percent of the patients 6 secondary to elevation or shortening of the first metatarsal. In 54 procedures, Saffo et al. found the average shortening of the first metatarsal to be approximately 6 mm. 6 Other studies indicate elevation of the first metatarsal may occur in as often as 20 percent of the procedures. Other complications include hallux varus, noted in 15.7 percent of Mauldin's study (Fig. 19-6). 7 Additional findings/complications include formation of plantar osteophytes between the first metatarsocuneiform plantar fusion site. Other complications include fractured screws or plates. We have seen a 5 percent screw fracture rate in Fig Potential nonunion of the first metatarsocuneiform joint.
6 284 HALLUX VALGUS AND FOREFOOT SURGERY phase of gait. If shortening or elevation occur, however, medial column rigidity is decreased, with subsequent increase in lateral forefoot pressure and the possibility of metatarsalgia or the formation of hammer toes or claw toes. Elevation of the first metatarsal may cause an iatrogenic primus elevatus leading to hallux limitus or rigidus. Postoperative Care Most authors prefer non-weight-bearing or limited weight-bearing for 6-8 weeks. It has been our experience to note that a total non-weight-bearing regimen should be enforced for the first 6 weeks after surgery, followed by an additional 2 weeks if necessary. After that time, the patient may start gradual touchdown during the next 2-3 weeks. After 3 months, intensive physical therapy may be initiated with walking, exercises, and gradual fitting into a normal shoe. It is not uncommon for mild to moderate edema to be present from 12 to 18 months with this procedure. REFERENCES Fig Hallux varus. oblique screws across the first metatarsocuneiform joint. A small percentage of plates will fracture. All plates and screws should be removed 6 to 12 months after surgery. Specific Biomechanical Considerations Fusion of the first metatarsocuneiform joint is believed to help prevent medial column collapse and hypermobility at the first metatarsal cuneiform joint. The proper performance of this technique will lead to increased stability during the midstance and toe-off 1. Albrecht GH: The pathology and treatment of hallux valgus. Russ Vrach 10:14, Lapidus PW: The operative correction of the metatarsus primus varus in hallux valgus. Surg Gynecol Obstet 58:183, Sangeorzan BJ, Hansen ST Jr: Modified Lapidus procedure for hallux valgus. Foot Ankle 9:262, Clark HR, Veith RG, Hansen ST Jr: Adolescent bunions treated by the modified Lapidus procedure. Bull Hosp Joint Dis Ortho Inst 47:109, Bacardi BE, Boysen TJ: Considerations for the Lapidus operation.j Foot Surg 25:133, Saffo G, Wooster MF, Stevens M, et al: First metatarsocuneiform joint arthrodesis: a five-year retrospective analysis. J Foot Surg 28:459, Mauldin DM, Sanders M, Whitmer WW: Correction of hallux valgus with metatarsocuneiform stabilization. Foot Ankle 11:59, Bonney G, McNab I: Hallux valgus and hallux rigidus: a critical survey of operative results. J Bone Joint Surg 34:366, 1952
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow.
 Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Matthew Beuchel MD 2 C. Luke Rust MD 3 Jessica Hooper MD 3
 A Prospective, Randomized,Controlled Trial Comparing Early- Weightbearing vs. Non-Weightbearing Following Modified Lapidus Arthrodesis Intermediate Results - Donald R. Bohay, MD, FACS Professor, Michigan
A Prospective, Randomized,Controlled Trial Comparing Early- Weightbearing vs. Non-Weightbearing Following Modified Lapidus Arthrodesis Intermediate Results - Donald R. Bohay, MD, FACS Professor, Michigan
PEDUS-L. Locking Plantar Lapidus Plate
 PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
6/5/2018. Forefoot Disorders. Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) Hallux Rigidus
 Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot
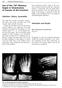 168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
1 st MP Arthrodesis. - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA
 1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity
 REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
Section 6: Preoperative Planning
 Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Lesser MPJ Hemi Implant
 Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
DRACO FOOT & ANKLE SYSTEM PRODUCT INFORMATION
 DRACO FOOT & ANKLE SYSTEM PRODUCT INFORMATION 2 DRACO FOOT & ANKLE SYSTEM www.hnmtotal.com DRACO Foot & Ankle System CONTENTS MetaFuse L Plate 3 MetaFuse BLP Plate 4 MetaFuse Midfoot/Lisfranc Plate 5 MetaFuse
DRACO FOOT & ANKLE SYSTEM PRODUCT INFORMATION 2 DRACO FOOT & ANKLE SYSTEM www.hnmtotal.com DRACO Foot & Ankle System CONTENTS MetaFuse L Plate 3 MetaFuse BLP Plate 4 MetaFuse Midfoot/Lisfranc Plate 5 MetaFuse
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium
 MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy
 CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY
 60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot.
 Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus
 Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
Angle-stable Foot plate system Pedus-O and Pedus-U
 www.marquardt-medizintechnik.de Angle-stable Foot plate system Pedus-O and Pedus-U Angle-stable Pedus-O and Pedus-U foot plate system > Angle-stable Pedus-O foot plate system 1. Product characteristics
www.marquardt-medizintechnik.de Angle-stable Foot plate system Pedus-O and Pedus-U Angle-stable Pedus-O and Pedus-U foot plate system > Angle-stable Pedus-O foot plate system 1. Product characteristics
Index. Note: Page numbers of article titles are in bold face type.
 Index Note: Page numbers of article titles are in bold face type. A Achilles tendon, Zadek osteotomy effects on, 430 Adult acquired flatfoot disorder, 387 403 calcaneal Z osteotomy for, 397 399 historical
Index Note: Page numbers of article titles are in bold face type. A Achilles tendon, Zadek osteotomy effects on, 430 Adult acquired flatfoot disorder, 387 403 calcaneal Z osteotomy for, 397 399 historical
Merete BLP. Surgical Technique. - Bunion Locking Plate - Low Profile Locking Bone Plate System
 Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
Low Profile Medial Locking plate augmentation Lapidus Arthrodesis with an early weight bearing protocol: Clinical and Radiographic Analysis
 Low Profile Medial Locking plate augmentation Lapidus Arthrodesis with an early weight bearing protocol: Clinical and Radiographic Analysis James Cottom, DPM Anand Vora, MD Low Profile Medial Locking plate
Low Profile Medial Locking plate augmentation Lapidus Arthrodesis with an early weight bearing protocol: Clinical and Radiographic Analysis James Cottom, DPM Anand Vora, MD Low Profile Medial Locking plate
LAPIDUS What is Old is New
 LAPIDUS What is Old is New Alan Jay Block, DPM, MS, FASPS, FACFAS Fellowship trained in Advanced Ankle Techniques Adjunct Professor Dept Of Orthopeadics The Ohio State University Board Member The Ohio
LAPIDUS What is Old is New Alan Jay Block, DPM, MS, FASPS, FACFAS Fellowship trained in Advanced Ankle Techniques Adjunct Professor Dept Of Orthopeadics The Ohio State University Board Member The Ohio
REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY
 C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
JUVENILE AND ADOLESCENT HALLUX VALGUS. George E. Quill, Jr., M.D.
 JUVENILE AND ADOLESCENT HALLUX VALGUS George E. Quill, Jr., M.D. The development of a hallux valgus deformity in children and adolescents is actually an uncommon entity. Most of these occurrences can be
JUVENILE AND ADOLESCENT HALLUX VALGUS George E. Quill, Jr., M.D. The development of a hallux valgus deformity in children and adolescents is actually an uncommon entity. Most of these occurrences can be
20 Cuneiform Osteotomy
 20 Cuneiform Osteotomy FRANCIS LYNCH While the use of the cuneiform osteotomy for surgical repair of hallux abducto valgus has never gained significant notoriety, there has been a recent heightened interest
20 Cuneiform Osteotomy FRANCIS LYNCH While the use of the cuneiform osteotomy for surgical repair of hallux abducto valgus has never gained significant notoriety, there has been a recent heightened interest
Index. Clin Podiatr Med Surg 22 (2005) Note: Page numbers of article titles are in boldface type.
 Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
CHARLOTTE Lisfranc. Recontruction System SURGICAL TECHNIQUE
 CHARLOTTE Lisfranc Recontruction System SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 4 4 4 4 4 Chapter 3 5 5 5 6 6 6 7 7 8 Chapter 4 8 8 9 10 Appendix 10 Introduction Indications and Contraindications
CHARLOTTE Lisfranc Recontruction System SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 4 4 4 4 4 Chapter 3 5 5 5 6 6 6 7 7 8 Chapter 4 8 8 9 10 Appendix 10 Introduction Indications and Contraindications
HemiEDGE. Patent No. 8,845,750. Surgical Technique
 HemiEDGE Patent No. 8,845,750 Surgical Technique Contents Product Based on the clinical success of our First MPJ Hemi Implant, the HemiEDGE, incorporates an overlapping edge extending around the medial,
HemiEDGE Patent No. 8,845,750 Surgical Technique Contents Product Based on the clinical success of our First MPJ Hemi Implant, the HemiEDGE, incorporates an overlapping edge extending around the medial,
CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS
 CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS ABC s of Comprehensive Musculoskeletal Care December 1 st, 2007 Stephen Pinney MD Chief, UCSF Foot and Ankle Service Chronic problems typically occur gradually
CHRONIC FOOT PROBLEMS FOOT and ANKLE BASICS ABC s of Comprehensive Musculoskeletal Care December 1 st, 2007 Stephen Pinney MD Chief, UCSF Foot and Ankle Service Chronic problems typically occur gradually
MULTIPLE APPLICATIONS OF THE MINIRAIL
 C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
Increased pressures at
 Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
MICA. Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE
 MICA Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 5 Indications and Warnings Chapter 3 6 Patient Positioning and Set Up Chapter 4 7
MICA Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 5 Indications and Warnings Chapter 3 6 Patient Positioning and Set Up Chapter 4 7
Technique Guide. 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot.
 Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Integra. ADVANSYS Plating System SURGICAL TECHNIQUE
 Integra ADVANSYS Plating System SURGICAL TECHNIQUE Table of Contents Dorsal Lisfranc Plate Indications...2 Contraindications...2 Description...2 Surgical Technique...3 Surgical Site Preparation...3 Step
Integra ADVANSYS Plating System SURGICAL TECHNIQUE Table of Contents Dorsal Lisfranc Plate Indications...2 Contraindications...2 Description...2 Surgical Technique...3 Surgical Site Preparation...3 Step
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities
 Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION. At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral)
 PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
SURGICAL TECHNIQUE CHI. Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY
 CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
DARCO. Bow 2 Plate SURGIC AL TECHNIQUE
 DARCO Bow 2 Plate SURGIC AL TECHNIQUE Contents 2 Preface 3 Chapter 1 4 Chapter 2 5 6 7 8 9 Appendix 10 10 11 Intended Use Indications/Contraindications Design Rationale Preoperative Planning Surgical Technique
DARCO Bow 2 Plate SURGIC AL TECHNIQUE Contents 2 Preface 3 Chapter 1 4 Chapter 2 5 6 7 8 9 Appendix 10 10 11 Intended Use Indications/Contraindications Design Rationale Preoperative Planning Surgical Technique
CLAD Error Key. Error Levels: Definite, Possible. Error Procedure Scope. Validation Scope. Location Scope. Violation/Information Text
 CLAD Key s: Definite, Possible Procedure 1 2 3 4 5 6 7 8 9 10 Two or more category 1 procedures Digit Definite 1.6 plus one or more of the following: 2.1.3, 2.1.7, 2.2.2, 2.2.6, and 2.3.4 Side Definite
CLAD Key s: Definite, Possible Procedure 1 2 3 4 5 6 7 8 9 10 Two or more category 1 procedures Digit Definite 1.6 plus one or more of the following: 2.1.3, 2.1.7, 2.2.2, 2.2.6, and 2.3.4 Side Definite
NORTHERN OHIO FOUNDATION
 NORTHERN OHIO FOOT & ANKLE FOUNDATION! The!Northern!Ohio!Foot!and!Ankle!Journal!!!!!!!!!!!!!!!Official!Publication!of!the!NOFA!Foundation!! First MPJ Proximal Phalanx Hemi Implant Arthroplasty Literature
NORTHERN OHIO FOOT & ANKLE FOUNDATION! The!Northern!Ohio!Foot!and!Ankle!Journal!!!!!!!!!!!!!!!Official!Publication!of!the!NOFA!Foundation!! First MPJ Proximal Phalanx Hemi Implant Arthroplasty Literature
FOOT & ANKLE ORTHOPAEDIC PROCEDURES
 FOOT & ANKLE ORTHOPAEDIC FOOT & ANKLE PROCEDURES FOREFOOT PROCEDURES PIP (Proximal Interphalangeal) Joint Fusion for Hammertoe and DIP (Distal Interphalangeal) Joint Fusion for Mallet Toe Metatarsal Shortening
FOOT & ANKLE ORTHOPAEDIC FOOT & ANKLE PROCEDURES FOREFOOT PROCEDURES PIP (Proximal Interphalangeal) Joint Fusion for Hammertoe and DIP (Distal Interphalangeal) Joint Fusion for Mallet Toe Metatarsal Shortening
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair
 Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Foot & Ankle Disorders
 Foot & Ankle Disorders Hillingdon PGMC 6-7-2013 Htwe Zaw FRCS (Tr&Orth) Consultant Foot & Ankle and Trauma Surgeon Hillingdon Hospitals NHS Foundation Trust Overview Anatomy: hindfoot-midfoot coupling
Foot & Ankle Disorders Hillingdon PGMC 6-7-2013 Htwe Zaw FRCS (Tr&Orth) Consultant Foot & Ankle and Trauma Surgeon Hillingdon Hospitals NHS Foundation Trust Overview Anatomy: hindfoot-midfoot coupling
Joint Preserving Surgery in Severe Forefoot Disorders
 Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
Forefoot/Midfoot Plating System. Surgical Technique
 Forefoot/Midfoot Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Forefoot/Midfoot Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT
 C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
The Flower Medial Column Fusion Plate
 The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy
 Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
ToeMobile. Surgical Technique. Great Toe Endoprosthesis
 Great Toe Endoprosthesis Surgical Technique Merete Medical, Inc. 99 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 Fax: 914-967-1542 E-Mail: service@merete-medical.com www.merete-medical.com - Description
Great Toe Endoprosthesis Surgical Technique Merete Medical, Inc. 99 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 Fax: 914-967-1542 E-Mail: service@merete-medical.com www.merete-medical.com - Description
The Ludloff Osteotomy
 Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
AUTHOR(S): COUGHLIN, MICHAEL J., M.D., BOISE, IDAHO. An Instructional Course Lecture, The American Academy of Orthopaedic Surgeons
 JBJA Journal of Bone and Joint Surgery - American 1996-1998 June 1996, Volume 78-A, Number 6 932 Instructional Course Lectures, The American Academy of Orthopaedic Surgeons - Hallux Valgus* Instructional
JBJA Journal of Bone and Joint Surgery - American 1996-1998 June 1996, Volume 78-A, Number 6 932 Instructional Course Lectures, The American Academy of Orthopaedic Surgeons - Hallux Valgus* Instructional
REVISIONAT HAttUX VATGUS SURGERY
 REVISIONAT HAttUX VATGUS SURGERY Bradley Castellano, D.P.M. Recurrence of deformity is one of the more common complications in hallux valgus surgery (1-3). The deformity may have been undercorrected with
REVISIONAT HAttUX VATGUS SURGERY Bradley Castellano, D.P.M. Recurrence of deformity is one of the more common complications in hallux valgus surgery (1-3). The deformity may have been undercorrected with
Congenital Hallux Varus with Polydactyly and Syndactyly- Correction in an Adult - A Case Report
 Case Report Journal of Orthopaedic Case Reports 2014 April-June;4(2): Page 64-68 Abstract Congenital Hallux Varus with Polydactyly and Syndactyly- Correction in an Adult - A Case Report 1,2 3 1 2 Sampat
Case Report Journal of Orthopaedic Case Reports 2014 April-June;4(2): Page 64-68 Abstract Congenital Hallux Varus with Polydactyly and Syndactyly- Correction in an Adult - A Case Report 1,2 3 1 2 Sampat
CARTIVA. Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING.
 CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
The American Academy of Foot & Ankle Osteosynthesis. presents
 The American Academy of Foot & Ankle Osteosynthesis presents Comprehensive Course of Internal Fixation for Reconstructive Surgery and Trauma of the Foot & Ankle September 4-6, 2014 Goodlett Farms Innovation
The American Academy of Foot & Ankle Osteosynthesis presents Comprehensive Course of Internal Fixation for Reconstructive Surgery and Trauma of the Foot & Ankle September 4-6, 2014 Goodlett Farms Innovation
6.5 mm midfoot fusion bolt
 6.5 mm midfoot fusion bolt For intramedullary fixation of the medial column of the foot SurgIcal technique Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
6.5 mm midfoot fusion bolt For intramedullary fixation of the medial column of the foot SurgIcal technique Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
2017 SAFSA CONGRESS PROGRAMME
 2017 SAFSA CONGRESS PROGRAMME THURSDAY, MAY 25 07h45 07h55: WELCOME & INTRODUCTIONS Forefoot I: Hallux Valgus and Lesser Toes (08h00-10h00 Lectures) 08h00 08h30: Surgical Management of Hallux Valgus Rippstein,
2017 SAFSA CONGRESS PROGRAMME THURSDAY, MAY 25 07h45 07h55: WELCOME & INTRODUCTIONS Forefoot I: Hallux Valgus and Lesser Toes (08h00-10h00 Lectures) 08h00 08h30: Surgical Management of Hallux Valgus Rippstein,
Midfoot - Reduction & Fixation - ORIF - screw fixation - AO Surgery Reference. ORIF - screw fixation
 Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
EFFECT OF EARLY WEIGHTBEARING AFTER MODIFIED LAPIDUS ARTHRODESIS: A Retrospective Study
 C H A P T E R 4 EFFECT OF EARLY WEIGHTBEARING AFTER MODIFIED LAPIDUS ARTHRODESIS: A Retrospective Study Irene O. Nwokolo, DPM Tony C. Nguyen, DPM Dan P. McDermott, DPM INTRODUCTION The modified Lapidus
C H A P T E R 4 EFFECT OF EARLY WEIGHTBEARING AFTER MODIFIED LAPIDUS ARTHRODESIS: A Retrospective Study Irene O. Nwokolo, DPM Tony C. Nguyen, DPM Dan P. McDermott, DPM INTRODUCTION The modified Lapidus
InCoreTM Lapidus System
 InCoreTM Lapidus System Precision Guided Correction Surgical Technique InCore TM Lapidus System Precision Guided Correction Tri-Planar Correction Targeting Guide is intended to aid and stabilize angular/rotational
InCoreTM Lapidus System Precision Guided Correction Surgical Technique InCore TM Lapidus System Precision Guided Correction Tri-Planar Correction Targeting Guide is intended to aid and stabilize angular/rotational
HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT
 C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
CHARLOTTE. 3.0 and 4.3 Multi-Use Compression Screws SURGIC A L T ECHNIQUE
 CHARLOTTE 3.0 and 4.3 Multi-Use Compression Screws SURGIC A L T ECHNIQUE CHARLOTTE 3.0 and 4.3 Multi-Use Compression Screws SURGICAL TECHNIQUE Surgical Technique as described by: Robert Anderson, MD Bruce
CHARLOTTE 3.0 and 4.3 Multi-Use Compression Screws SURGIC A L T ECHNIQUE CHARLOTTE 3.0 and 4.3 Multi-Use Compression Screws SURGICAL TECHNIQUE Surgical Technique as described by: Robert Anderson, MD Bruce
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity
 Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
QUICK REFERENCE GUIDE. MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING
 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING ORDERING INFORMATION Sterilization box, empty M190 Can accommodate: M101 Standard MiniRail
14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING ORDERING INFORMATION Sterilization box, empty M190 Can accommodate: M101 Standard MiniRail
Endolog Implant for Correction of Hallux Valgus
 Endolog Implant for Correction of Hallux Valgus Surgical Technique Distributed by: Simple and precise Mini-invasive For mild, moderate and severe HV Surgical Indications Endolog implant is proposed for
Endolog Implant for Correction of Hallux Valgus Surgical Technique Distributed by: Simple and precise Mini-invasive For mild, moderate and severe HV Surgical Indications Endolog implant is proposed for
Integra. surgical technique. Advansys Midfoot Plating System. eng. D.L.P. Dorsal Lisfranc Plate. M.L.P. Medial Lisfranc Plate
 eng Integra Advansys Midfoot Plating System surgical technique D.L.P. Dorsal Lisfranc Plate M.L.P. Medial Lisfranc Plate Table of Contents Advansys Medial Lisfranc Plate (DLP)... 4 Indications... 4 Contraindications...
eng Integra Advansys Midfoot Plating System surgical technique D.L.P. Dorsal Lisfranc Plate M.L.P. Medial Lisfranc Plate Table of Contents Advansys Medial Lisfranc Plate (DLP)... 4 Indications... 4 Contraindications...
First MPJ Hemi Implant
 First MPJ Hemi Implant Surgical Technique Contents Product The BioPro First MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the hallux metatarsophalangeal joint
First MPJ Hemi Implant Surgical Technique Contents Product The BioPro First MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the hallux metatarsophalangeal joint
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING.
 LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
A Patient s Guide to Adult-Acquired Flatfoot Deformity
 A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
3 section of the Foot
 TERMINOLOGY 101 How many Bones 3 section of the Foot Bilateral Relating to both Plantar Relating to the bottom or sole Lateral Relating to the outside or farther from the median Medial Relating to the
TERMINOLOGY 101 How many Bones 3 section of the Foot Bilateral Relating to both Plantar Relating to the bottom or sole Lateral Relating to the outside or farther from the median Medial Relating to the
ORTHOLOC 3Di. Foot Reconstruction System SURGIC AL TECHNIQUE
 ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
Chevron Osteotomy With Lateral Soft Tissue Release
 5(4):250 256, 2006 T E C H N I Q U E Chevron Osteotomy With Lateral Soft Tissue Release Hans-Jörg Trnka, MD, PhD and Stefan Gerhard Hofstaetter, MD Foot and Ankle Center Vienna Vienna, Austria Ó 2006 Lippincott
5(4):250 256, 2006 T E C H N I Q U E Chevron Osteotomy With Lateral Soft Tissue Release Hans-Jörg Trnka, MD, PhD and Stefan Gerhard Hofstaetter, MD Foot and Ankle Center Vienna Vienna, Austria Ó 2006 Lippincott
Moderate to severe hallux valgus deformity: correction with proximal crescentic osteotomy and distal soft-tissue release
 Arch Orthop Trauma Surg (2000) 120 : 397 402 Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal
Arch Orthop Trauma Surg (2000) 120 : 397 402 Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal
Pedographic, clinical, and functional Outcome after Scarf Osteotomy Timo J. Lorei, MD Christian Kinast,
 Zentrum FuSS & Sprunggelenk Dr. Kinast Prof. Dr. Hamel Pedographic, clinical, and functional Outcome after Scarf Osteotomy Timo J. Lorei, MD Christian Kinast, MD Hans Klärner, MD and Dieter Rosenbaum,
Zentrum FuSS & Sprunggelenk Dr. Kinast Prof. Dr. Hamel Pedographic, clinical, and functional Outcome after Scarf Osteotomy Timo J. Lorei, MD Christian Kinast, MD Hans Klärner, MD and Dieter Rosenbaum,
Foot Reconstruction System SURGICAL TECHNIQUE
 ORTHOLOC 3Di Foot Reconstruction System SURGICAL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: Robert B. Anderson, MD OrthoCarolina Charlotte,
ORTHOLOC 3Di Foot Reconstruction System SURGICAL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: Robert B. Anderson, MD OrthoCarolina Charlotte,
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abscess, in puncture wounds, 531 Absorbable fixation, for Lisfranc joint injuries, 556 Advanced glycosylation end products, complications due
Note: Page numbers of article titles are in boldface type. A Abscess, in puncture wounds, 531 Absorbable fixation, for Lisfranc joint injuries, 556 Advanced glycosylation end products, complications due
MetaFix Ludloff Plate
 Merete MetaFix Ludloff Plate Low Profile Locking Bone Plate System Surgical Technique and Ordering Information - Content - Content 1. Description.................................................. 3 2.
Merete MetaFix Ludloff Plate Low Profile Locking Bone Plate System Surgical Technique and Ordering Information - Content - Content 1. Description.................................................. 3 2.
Introduction Basics MIS Screw 2 System Characteristics 2 Indication 2
 Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint
 Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
1. Orthoapedic Associates of Michigan, PC, Grand Rapids, MI 2. Michigan State University College of Human Medicine, Grand Rapids, MI
 Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
*Rippstein, Trnka, Saragas, Hoffman
 THURS 25th MAY 07:00 07:10 Welcome and Introductions Paulo Ferrao Lecture 1: 07:10 09:45 Forefoot I: Hallux Valgus and Lesser Toes Mark Easley 40 mins 07:10 07:50 Surgical Management of Hallux Valgus 30
THURS 25th MAY 07:00 07:10 Welcome and Introductions Paulo Ferrao Lecture 1: 07:10 09:45 Forefoot I: Hallux Valgus and Lesser Toes Mark Easley 40 mins 07:10 07:50 Surgical Management of Hallux Valgus 30
Proper Logging of Surgical Procedures (Effective July 1, 2018)
 Proper Logging of Surgical Procedures (Effective July 1, 2018) GENERAL GUIDELINES: 1) For the procedure codes listed below, the program director must review each entry to determine proper usage. The following
Proper Logging of Surgical Procedures (Effective July 1, 2018) GENERAL GUIDELINES: 1) For the procedure codes listed below, the program director must review each entry to determine proper usage. The following
The Journal of Foot & Ankle Surgery
 The Journal of Foot & Ankle Surgery 50 (2011) 377 382 Contents lists available at ScienceDirect The Journal of Foot & Ankle Surgery journal homepage: www.jfas.org Lapidus Arthrodesis with a Single Lag
The Journal of Foot & Ankle Surgery 50 (2011) 377 382 Contents lists available at ScienceDirect The Journal of Foot & Ankle Surgery journal homepage: www.jfas.org Lapidus Arthrodesis with a Single Lag
Rippstein, Trnka, Saragas, Narramore
 THURS 25th MAY 07:45 07:55 Welcome and Introductions Paulo Ferrao Lecture 1: 08:00 10:20 Forefoot I: Hallux Valgus and Lesser Toes Mark Easley 30 mins 08:00 08:30 Surgical Management of Hallux Valgus Saragas,
THURS 25th MAY 07:45 07:55 Welcome and Introductions Paulo Ferrao Lecture 1: 08:00 10:20 Forefoot I: Hallux Valgus and Lesser Toes Mark Easley 30 mins 08:00 08:30 Surgical Management of Hallux Valgus Saragas,
Forefoot/Midfoot Plating System
 Surgical Technique Forefoot/Midfoot Plating System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Surgical Technique Forefoot/Midfoot Plating System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito
 Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
with regard to our presentation.
 Rotated Insertion Metatarsal Osteotomy with Distal Soft Tissue Procedure for Severe Hallux Valgus Deformity Novel Procedure of the 1 st metatarsal osteotomy Norihiro Samoto MD, Ph.D. Director of Department
Rotated Insertion Metatarsal Osteotomy with Distal Soft Tissue Procedure for Severe Hallux Valgus Deformity Novel Procedure of the 1 st metatarsal osteotomy Norihiro Samoto MD, Ph.D. Director of Department
A perspective on MPJ implant arthroplasty.
 A perspective on MPJ implant arthroplasty. The BioPro MPJ Hemi Implant System: +65 years of successful clinical use. Pre-op Post-op 20+ year implant survivorship 14 96% Survivorship 1 97% Patient Satisfaction
A perspective on MPJ implant arthroplasty. The BioPro MPJ Hemi Implant System: +65 years of successful clinical use. Pre-op Post-op 20+ year implant survivorship 14 96% Survivorship 1 97% Patient Satisfaction
Axi+LineTM Proximal Bunion CorrectionSystem. Surgical Technique
 Axi+LineTM Proximal Bunion CorrectionSystem Surgical Technique A i Line Proximal Bunion Correction System TM Desired angle correction is built into the plate, providing a self-reducing, 5-hole construct
Axi+LineTM Proximal Bunion CorrectionSystem Surgical Technique A i Line Proximal Bunion Correction System TM Desired angle correction is built into the plate, providing a self-reducing, 5-hole construct
The American Academy of Foot & Ankle Osteosynthesis. presents
 The American Academy of Foot & Ankle Osteosynthesis presents Comprehensive Course of Internal Fixation for Reconstructive Surgery and Trauma of the Foot & Ankle Hyatt DFW Airport Dallas, Texas SCIENTIFIC
The American Academy of Foot & Ankle Osteosynthesis presents Comprehensive Course of Internal Fixation for Reconstructive Surgery and Trauma of the Foot & Ankle Hyatt DFW Airport Dallas, Texas SCIENTIFIC
pedcat Clinical Case Studies
 pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS
 C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
Locking Ankle Plating System. Surgical Technique
 Locking Ankle Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Locking Ankle Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Columbia/NYOH FOOT and ANKLE ROTATION-SPECIFIC OBJECTIVES
 Updated 2/8/10 Columbia/NYOH FOOT and ANKLE ROTATION-SPECIFIC OBJECTIVES INTERPERSONAL AND COMMUNICATION SKILLS Resident will at all times demonstrate behavior that is beyond reproach. Residents must be
Updated 2/8/10 Columbia/NYOH FOOT and ANKLE ROTATION-SPECIFIC OBJECTIVES INTERPERSONAL AND COMMUNICATION SKILLS Resident will at all times demonstrate behavior that is beyond reproach. Residents must be
Other Congenital and Developmental Diseases of the Foot. Department of Orthopedic Surgery St. Vincent s s Hospital, The Catholic University
 Other Congenital and Developmental Diseases of the Foot Department of Orthopedic Surgery St. Vincent s s Hospital, The Catholic University Contents Metatarsus Adductus Skewfoot Hallux Valgus Hallux Valgus
Other Congenital and Developmental Diseases of the Foot Department of Orthopedic Surgery St. Vincent s s Hospital, The Catholic University Contents Metatarsus Adductus Skewfoot Hallux Valgus Hallux Valgus
American Board of Foot and Ankle Surgery
 American Board of Foot and Ankle Surgery Logging Guidelines Revisions ABFAS Task Force Mindy Benton, DPM Randall Dei, DPM Charles Lombardi, DPM John Thomas Marcoux, DPM Roya Mirmiran, DPM Michael Vaardahl,
American Board of Foot and Ankle Surgery Logging Guidelines Revisions ABFAS Task Force Mindy Benton, DPM Randall Dei, DPM Charles Lombardi, DPM John Thomas Marcoux, DPM Roya Mirmiran, DPM Michael Vaardahl,
Lisfranc Fracture-Dislocation/ Arthrodesis
 Lisfranc Fracture-Dislocation/ Arthrodesis 16 Lawrence A. Di Domenico and Frank A. Luckino Introduction L.A. Di Domenico (*) Ankle and Foot Care Centers, Youngstown, OH, USA Kent State University, College
Lisfranc Fracture-Dislocation/ Arthrodesis 16 Lawrence A. Di Domenico and Frank A. Luckino Introduction L.A. Di Domenico (*) Ankle and Foot Care Centers, Youngstown, OH, USA Kent State University, College
Digital Surgery Complications
 Annual Surgical Conference 2018 Digital Surgery Complications Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Presentation Outline Differentials
Annual Surgical Conference 2018 Digital Surgery Complications Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Presentation Outline Differentials
