Rehabilitation Guidelines for Meniscal Repair
|
|
|
- Barry Lucas
- 6 years ago
- Views:
Transcription
1 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen, proteoglycans and water and lines the end of the bones that meet to form a joint. The primary function of the articular cartilage is to provide a smooth gliding surface for joint motion. Rubbing articular cartilage on articular cartilage is approximately 5 times more smooth, or with less friction, than rubbing ice on ice. 1 The cartilage in the knee includes a medial (inside) and a lateral (outside). Together they are referred to as menisci. The menisci are wedge shaped, being thinner toward the center of the knee and thicker toward the outside of the knee joint (Figures 1 3). This shape is very important to its function. The primary function of the menisci is to improve load transmission. A relatively round femur sitting on a relatively flat tibia forms the knee joint. Without the menisci the area of contact force between these two bones would be relatively small, increasing the contact stress by % (Figure 4). The menisci also provide some shock absorption, lubrication and joint stability. There are two categories of meniscal tears: acute traumatic tears and degenerative tears. Degenerative tears most commonly occur in middle-aged people. They typically Lateral Figure 1 Meniscus cartilage (shown here from above the knee, without the femur) Image property of Primal Pictures, Ltd., primalpictures.com. Use of this image without authorization from Primal Pictures, Ltd. is prohibited. occur through repetitive stresses to the menisci over time, which severely weakens the tissue. This process of tissue degeneration makes it very unlikely that a surgical repair will heal or that the surrounding will be strong enough to hold the sutures used to repair it. One report showed that less than 10% of meniscal tears occurring in patients greater than forty years of age were repairable. Symptoms of a degenerative tear include swelling, pain along the joint line, catching and locking. Most often degenerative tears are surgically removed. Occasionally a patient may be able to regain function through rehabilitation without surgery. Acute traumatic tears occur most frequently in the athletic population as a result of a twisting injury to Figure 2 (inside) view of the knee Image property of Primal Pictures, Ltd., primalpictures.com. Use of this image without authorization from Primal Pictures, Ltd. is prohibited. Figure 3 Normal MRI (saggital view) of the knee, lateral (outside) view The world class health care team for the UW Badgers and proud sponsor of UW Athletics UWSPORTSMEDICINE.ORG
2 without with Figure 5 MRI (saggital view) of a lateral tear (yellow arrows) Figure 4 Schematic representation of the meniscal effect on contact pressure in the knee. Contact area is increased by 50% with addition of menisci. This reduces contact pressures. the knee when the foot is planted. Symptoms of an acute tear include swelling, pain along the joint line, catching, locking and a specific injury. Often times these tears can be diagnosed by taking a thorough history and completing a physical examination. An MRI may be used to assist in making the diagnosis. If an athlete suffers a meniscal tear, the three options for treatment Meniscus Figure 6 Perimeniscular capillary plexus (thick arrow) providing blood supply to the outer third of the. include: non-operative rehabilitation, surgery to trim out the area of torn, or surgery to repair (stitch together) the torn. The treatment chosen will depend on the location of the tear, the athlete s sport, ligamentous stability of the knee and any associated injury. 2 The location of tear is important because the outer portion of the has a good blood supply whereas the inner portion has a very poor blood supply. Figure 6 shows the blood vessels (perimeniscular capillary plexus) entering the outer portion of the. 3 This blood supply is necessary for a tear or a repair to heal. Without an adequate blood supply, the area of torn will have to be removed. After mensical surgery, rehabilitation with a physical therapist or athletic trainer is needed to restore range of motion, strength, movement control and guide the athlete s return to sport. When the is repaired there may be a period of restricted knee flexion, especially during weight bearing, to protect the repair sutures and the. The rehabilitation guidelines are presented in a criterion based progression. Specific time frames, restrictions and precautions are given to protect healing tissues and the surgical repair/reconstruction. General time frames are also given for reference to the average individual, but individual patients will progress at different rates depending on their age, associated injuries, pre-injury health status, rehabilitation compliance and injury severity. The size and location of the meniscal tear may also affect the rate of post-operative progression. 2 UWSPORTSMEDICINE.ORG
3 PHASE I (Surgery to 4 weeks after surgery) Note: The physician may extend this phase to 6 weeks for large repairs. Range of Motion Exercises Progression Criteria Rehabilitation appointments begin 3-5 days post-operatively and then approximately 1 time per week Protection of the post-surgical knee Restore normal knee extension Eliminate effusion (swelling) Restore leg control The patient may gradually wean from two crutches to one crutch to no crutches as long as the knee is in the locked knee brace, and there is no increase in pain or swelling for 4 weeks. Knee brace locked for all weight bearing activities for 4 weeks Do not flex the knee past 90 Knee extension on a bolster Prone hangs Supine wall slides Heel slides (caution with posterior medial repair secondary to the semimembranosus insertion) Knee flexion off the edge of the table Quadriceps sets Straight leg raises 4 way leg lifts in standing with brace on for balance and hip strength Abdominal isometrics Upper body circuit training or upper body ergometer 4 weeks after surgery Pain-free gait without crutches No effusion (swelling) 3 UWSPORTSMEDICINE.ORG
4 PHASE II (begin after meeting Phase I criteria, usually 4 weeks after surgery) Progression Criteria Rehabilitation appointments are once every 1-2 weeks Single leg stand control Normalize gait Good control and no pain with functional movements, including step up/down, squat, partial lunge (between 0 and 60 of knee flexion) No forced flexion with passive range of motion with knee flexion or weight bearing activities that push the knee past 60 of knee flexion Avoid post-activity swelling No impact activities Non-impact balance and proprioceptive drills Stationary bike Gait drills Hip and core strengthening Stretching for patient-specific muscle imbalances Quadriceps strengthening, making sure that closed chain exercises occur between 0 and 60 of knee flexion Non-impact endurance training: stationary bike, Nordic track, swimming, deep water running or cross trainer Normal gait on all surfaces Ability to carry out functional movements without unloading affected (injured) leg or pain, while demonstrating good control Single leg balance greater than 15 seconds 4 UWSPORTSMEDICINE.ORG
5 PHASE III (begin after meeting Phase II criteria, usually 3 months after surgery) Return To Sport/Work Criteria Rehabilitation appointments are once every 1 to 2 weeks Good control and no pain with sport and work specific movements, including impact Post-activity soreness should resolve within 24 hours Avoid post-activity swelling Avoid posterior knee pain with end range knee flexion Impact control exercises beginning 2 feet to 2 feet, progressing from 1 foot to the other and then 1 foot to the same foot Movement control exercises beginning with low velocity, single plane activities and progressing to higher velocity, multi-plane activities Strength and control drills related to sport specific movements Sport/work specific balance and proprioceptive drills Hip and core strengthening Stretching for patient specific muscle imbalances Replicate sport or work specific energy demands Dynamic neuromuscular control with multi-plane activities without pain or swelling These rehabilitation guidelines were developed collaboratively by Marc Sherry, PT, DPT, LAT, CSCS and the UW Health Sports Medicine physician group. Updated 11/2017 REFERENCES 1. Ulrich GS and Aronczyk SP. The basic science of repair. Tech in Ortho, 8(2): 56-62, Fowler PJ and Pompan D. Rehabilitation after mensical repair. Tech in Ortho, 8(2): , Arnoczky SP and Warren RF. Microvasculature of the human. Am J Sport Med, At UW Health, patients may have advanced diagnostic and /or treatment options, or may receive educational materials that vary from this information. Please be aware that this information is not intended to replace the care or advice given by your physician or health care provider. It is neither intended nor implied to be a substitute for professional advice. Call your health provider immediately if you think you may have a medical emergency. Always seek the advice of your physician or other qualified health provider prior to starting any new treatment or with any question you may have regarding a medical condition. Copyright 2017 UW Health Sports Medicine 5 UWSPORTSMEDICINE.ORG SM
Rehabilitation Guidelines for Knee Arthroscopy
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Rehabilitation Guidelines Following Microfracture Procedures to the Knee
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Patellar-quadriceps Tendon Repair Protocol
 Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 1/2018
Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 1/2018
Patellar-quadriceps Tendon Repair Protocol
 Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 3/2017
Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 3/2017
Rehabilitation Guidelines for Achilles Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
MENISCUS TEAR. Description
 MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
DISCOID MENISCUS. Description
 DISCOID MENISCUS Description For participation in jumping (basketball, volleyball) or The meniscus is a cartilage structure in the knee that sits on contact sports, protect the knee joint with supportive
DISCOID MENISCUS Description For participation in jumping (basketball, volleyball) or The meniscus is a cartilage structure in the knee that sits on contact sports, protect the knee joint with supportive
Anterior Cruciate Ligament (ACL)
 Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Rehabilitation Guidelines for Shoulder Arthroscopy
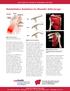 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Shoulder Arthroscopy Front View Acromion Supraspinatus Back View Supraspinatus Long head of bicep Type I Infraspinatus Short head of bicep
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Shoulder Arthroscopy Front View Acromion Supraspinatus Back View Supraspinatus Long head of bicep Type I Infraspinatus Short head of bicep
Meniscus Repair Rehabilitation Protocol
 Brian E. Camilleri, DO 2610 Enterprise Dr Anderson, IN 46013 Phone: (765) 683-4400 Fax: (765) 642-7903 www.ciocenter.com Meniscus Repair Rehabilitation Protocol The intent of this protocol is to provide
Brian E. Camilleri, DO 2610 Enterprise Dr Anderson, IN 46013 Phone: (765) 683-4400 Fax: (765) 642-7903 www.ciocenter.com Meniscus Repair Rehabilitation Protocol The intent of this protocol is to provide
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
DISCOID MENISCUS. Description
 Montefiore Pediatric Orthopedic and Scoliosis Center Children s Hospital at Montefiore Norman Otsuka MD Eric Fornari MD Jacob Schulz MD Jaime Gomez MD Christine Moloney PA 3400 Bainbridge Avenue, 6 th
Montefiore Pediatric Orthopedic and Scoliosis Center Children s Hospital at Montefiore Norman Otsuka MD Eric Fornari MD Jacob Schulz MD Jaime Gomez MD Christine Moloney PA 3400 Bainbridge Avenue, 6 th
A Patient s Guide. ACL Injury: Ø Frequently asked questions on injury, Ø Preoperative and postoperative. surgery and recovery.
 ACL Injury: A Patient s Guide Ø Frequently asked questions on injury, surgery and recovery Ø Preoperative and postoperative guidelines Mia S. Hagen, M.D. Assistant Professor Department of Orthopaedics
ACL Injury: A Patient s Guide Ø Frequently asked questions on injury, surgery and recovery Ø Preoperative and postoperative guidelines Mia S. Hagen, M.D. Assistant Professor Department of Orthopaedics
Meniscus Tears. Three bones meet to form your knee joint: your thighbone (femur), shinbone (tibia), and kneecap (patella).
 Meniscus Tears Information on meniscus tears is also available in Spanish: Desgarros de los meniscus (topic.cfm?topic=a00470) and Portuguese: Rupturas do menisco (topic.cfm?topic=a00754). Meniscus tears
Meniscus Tears Information on meniscus tears is also available in Spanish: Desgarros de los meniscus (topic.cfm?topic=a00470) and Portuguese: Rupturas do menisco (topic.cfm?topic=a00754). Meniscus tears
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep
ACL REHABILITATION PROTOCOL
 Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL. WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches.
 REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon
 Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
What is an ACL Tear?...2. Treatment Options...3. Surgical Techniques...4. Preoperative Care...5. Preoperative Requirements...6
 Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Table of Contents What is an ACL Tear?....2 Treatment Options...3 Surgical Techniques...4 Preoperative Care...5 Preoperative Requirements...6 Postoperative Care...................... 7 Crutch use...8 Initial
Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair
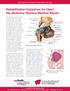 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair The hip joint is composed of the femur (the thigh bone) and the acetabulum (the socket which is from
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair The hip joint is composed of the femur (the thigh bone) and the acetabulum (the socket which is from
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound
REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION
 REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION I. IMMEDIATE POST OPERATIVE PHASE POD 1 POD 2 to 3 Brace: EZ Wrap brace locked at zero degrees extension or Protonics Rehab System (PRS) as directed by physician
REHABILITATION FOLLOWING ACL PTG RECONSTRUCTION I. IMMEDIATE POST OPERATIVE PHASE POD 1 POD 2 to 3 Brace: EZ Wrap brace locked at zero degrees extension or Protonics Rehab System (PRS) as directed by physician
9180 KATY FREEWAY, STE. 200 (713)
 AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
Meniscus Problems - Torn Meniscus Repair
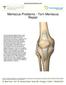 Meniscus Problems - Torn Meniscus Repair The two crescent-shaped menisci in each knee absorb shock, disperse weight, and reduce friction when the knee moves. Activities such as walking or jumping transfer
Meniscus Problems - Torn Meniscus Repair The two crescent-shaped menisci in each knee absorb shock, disperse weight, and reduce friction when the knee moves. Activities such as walking or jumping transfer
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
REHABILITATION GUIDELINES AFTER ACL RECONSTRUCTION. Shail Vyas, MD Orange County Orthopaedic Group (714)
 REHABILITATION GUIDELINES AFTER ACL RECONSTRUCTION Shail Vyas, MD Orange County Orthopaedic Group (714) 974-0100 The intent of this protocol is to provide the therapist with guidelines of the post-operative
REHABILITATION GUIDELINES AFTER ACL RECONSTRUCTION Shail Vyas, MD Orange County Orthopaedic Group (714) 974-0100 The intent of this protocol is to provide the therapist with guidelines of the post-operative
Rehabilitation Guidelines Following Proximal Hamstring Primary Repair
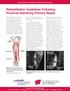 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Proximal Hamstring Primary Repair The hamstring muscle group consists of three muscles: the biceps femoris, semitendinosus and semimembranosus.
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Proximal Hamstring Primary Repair The hamstring muscle group consists of three muscles: the biceps femoris, semitendinosus and semimembranosus.
Sheena Black, MD. Orthopaedic Surgery, Sports Medicine PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE
 PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures:
PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION PATELLAR TENDON/ BTB TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures:
Rehabilitation Guidelines for Large Rotator Cuff Repair
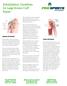 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
Patella Instability in Children and Adolescents
 Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
(Also known as a, Lateral Cartilage Tear,, Bucket Handle Tear of the Lateral Meniscus, Torn Cartilage)
 Lateral Meniscus Tear (Also known as a, Lateral Cartilage Tear,, Bucket Handle Tear of the Lateral Meniscus, Torn Cartilage) What is a lateral meniscus tear? The knee joint comprises of the union of two
Lateral Meniscus Tear (Also known as a, Lateral Cartilage Tear,, Bucket Handle Tear of the Lateral Meniscus, Torn Cartilage) What is a lateral meniscus tear? The knee joint comprises of the union of two
Sheena Black, MD. Orthopaedic Surgery, Sports Medicine PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE
 PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral
PHYSICAL THERAPY PRESCRIPTION ACL RECONSTRUCTION HAMSTRING TENDON TECHNIQUE Name: Date: Post-Operative Diagnosis: Right Left ACL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral
GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
ACL PATELLAR TENDON AUTOGRAFT RECONSTRUCTION PROTOCOL
 Dr. Matthew J. Boyle, BSc, MBChB, FRACS AUT Millennium, 17 Antares Place, Mairangi Bay & Ascot Hospital, 90 Green Lane E, Remuera P: (09) 281-6733 F: (09) 479-3805 office@matthewboyle.co.nz www.matthewboyle.co.nz
Dr. Matthew J. Boyle, BSc, MBChB, FRACS AUT Millennium, 17 Antares Place, Mairangi Bay & Ascot Hospital, 90 Green Lane E, Remuera P: (09) 281-6733 F: (09) 479-3805 office@matthewboyle.co.nz www.matthewboyle.co.nz
9180 KATY FREEWAY, STE. 200 (713)
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY
 A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
Femoral Condyle Rehabilitation Guidelines
 Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS)
 Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Post Operative ACL Reconstruction Protocol Brian J. White, MD
 Post Operative ACL Reconstruction Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve as
Post Operative ACL Reconstruction Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve as
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: - POD 1: Debulk dressing, TED Hose in place - POD 2: Change
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: - POD 1: Debulk dressing, TED Hose in place - POD 2: Change
Post-Operative Meniscus Repair Protocol Brian J.White, MD
 Post-Operative Meniscus Repair Protocol Brian J.White, MD www.western-ortho.com (This protocol should be used with combined a ACL Reconstruction and meniscus repair) The intent of this protocol is to provide
Post-Operative Meniscus Repair Protocol Brian J.White, MD www.western-ortho.com (This protocol should be used with combined a ACL Reconstruction and meniscus repair) The intent of this protocol is to provide
Hip Arthroscopy Protocol
 The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Grant H Garcia, MD Sports and Shoulder Surgeon
 What to Expect from your Anterior Cruciate Ligament Reconstruction Surgery A Guide for Patients Grant H Garcia, MD Sports and Shoulder Surgeon Important Contact Information Grant Garcia, MD Wallingford:
What to Expect from your Anterior Cruciate Ligament Reconstruction Surgery A Guide for Patients Grant H Garcia, MD Sports and Shoulder Surgeon Important Contact Information Grant Garcia, MD Wallingford:
KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC
 PHYSICAL THERAPY SECTION WILLIAM BEAUMONT ARMY MEDICAL CENTER 5005 N. PIEDRAS ST EL PASO, TEXAS 79920 KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC Revised August 2008 Post-op Days 1 14 Dressing POD
PHYSICAL THERAPY SECTION WILLIAM BEAUMONT ARMY MEDICAL CENTER 5005 N. PIEDRAS ST EL PASO, TEXAS 79920 KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC Revised August 2008 Post-op Days 1 14 Dressing POD
Anterior Cruciate Ligament (ACL) Rehabilitation
 Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation program and the
Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation program and the
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: MENISCAL REPAIR: 1. General Guidelines: Time lines in this rehabilitation protocol are approximate. If the
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: MENISCAL REPAIR: 1. General Guidelines: Time lines in this rehabilitation protocol are approximate. If the
Understanding Your ACL Injury
 Scott Bissell, MD Connecticut Orthopedic Associates www.ctorthoassociates.com Understanding Your ACL Injury The ACL (Anterior Cruciate Ligament) is a commonly injured ligament in the knee. Please see the
Scott Bissell, MD Connecticut Orthopedic Associates www.ctorthoassociates.com Understanding Your ACL Injury The ACL (Anterior Cruciate Ligament) is a commonly injured ligament in the knee. Please see the
KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE
 PHYSICAL THERAPY SECTION WILLIAM BEAUMONT ARMY MEDICAL CENTER 5005 N. PIEDRAS ST EL PASO, TEXAS 79920 KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE Revised August 2008 Post-op Days 1 14 Dressing POD
PHYSICAL THERAPY SECTION WILLIAM BEAUMONT ARMY MEDICAL CENTER 5005 N. PIEDRAS ST EL PASO, TEXAS 79920 KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE Revised August 2008 Post-op Days 1 14 Dressing POD
Anterior Cruciate Ligament Injuries
 Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Sheena Black, MD PHYSICAL THERAPY PRESCRIPTION MCL RECONSTRUCTION. Orthopaedic Surgery, Sports Medicine.
 PHYSICAL THERAPY PRESCRIPTION Name: Date: Post-Operative Diagnosis: Right Left MCL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral Menisectomy Medial Menisectomy Lateral Meniscal
PHYSICAL THERAPY PRESCRIPTION Name: Date: Post-Operative Diagnosis: Right Left MCL Reconstruction Graft: BTB Hamstring Allograft Additional Procedures: Lateral Menisectomy Medial Menisectomy Lateral Meniscal
MENISCAL REPAIR LOURDES MEDICAL ASSOCIATES PROFESSIONAL ORTHOPAEDICS SPORTS MEDICINE & ARTHROSCOPY
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
Rehabilitation Guidelines for UCL Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for UCL Repair The elbow is a complex system of three joints formed from three bones; the humerus (the upper arm bone), the ulna (the larger bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for UCL Repair The elbow is a complex system of three joints formed from three bones; the humerus (the upper arm bone), the ulna (the larger bone
Meniscal Injuries Introduction Welcome to BodyZone Physiotherapy's patient resource about Meniscal Injuries.
 Meniscal Injuries Introduction Welcome to BodyZone Physiotherapy's patient resource about Meniscal Injuries. The meniscus is a commonly injured structure in the knee. The injury can occur in any age group.
Meniscal Injuries Introduction Welcome to BodyZone Physiotherapy's patient resource about Meniscal Injuries. The meniscus is a commonly injured structure in the knee. The injury can occur in any age group.
Dr Schock High Tibial Osteotomy
 Dr Schock High Tibial Osteotomy Goals for phase 1 Control pain Control edema Initiate ROM and quad strengthening Maintain WB restrictions Appropriate brace wear Criteria for progression to Phase 2 Edema
Dr Schock High Tibial Osteotomy Goals for phase 1 Control pain Control edema Initiate ROM and quad strengthening Maintain WB restrictions Appropriate brace wear Criteria for progression to Phase 2 Edema
ACL Patella Tendon Autograft Reconstruction Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 ACL Patella Tendon Autograft Reconstruction Protocol The intent of this protocol is to provide the clinician
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 ACL Patella Tendon Autograft Reconstruction Protocol The intent of this protocol is to provide the clinician
Anterior Cruciate Ligament (ACL) Reconstruction Hamstring Graft/PTG-Accelerated Rehabilitation Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Cruciate Ligament (ACL) Reconstruction Hamstring Graft/PTG-Accelerated Rehabilitation
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Cruciate Ligament (ACL) Reconstruction Hamstring Graft/PTG-Accelerated Rehabilitation
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol
 Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Clarkstown Division This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Clarkstown Division This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT. Brace E-Z Wrap locked at zero degree extension, sleep in Brace
 Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
Medial Patellofemoral Ligament Repair/Reconstruction
 Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Alta View Sports Medicine Dr. James R. Meadows, MD Orthopedic Surgery & Sports Medicine 74 Kimballs Ln Ste 230, Draper, UT 84020 9844 S. 1300 E. Ste 100, Sandy, UT 84094 (801) 571-9433 www.meadowsmd.com
Athletic Preparation ACL Reconstruction - Accelerated Rehabilitation. Autologous Bone-Tendon-Bone, Patella Tendon Graft
 Orthopaedic Sports Specialists, P.C. Michael E. Joyce, M.D. 84 Glastonbury Blvd., Suite 101, Glastonbury, Connecticut 06033 Voice: 860-652-8883, Fax: 860-652-8887 Athletic Preparation ACL Reconstruction
Orthopaedic Sports Specialists, P.C. Michael E. Joyce, M.D. 84 Glastonbury Blvd., Suite 101, Glastonbury, Connecticut 06033 Voice: 860-652-8883, Fax: 860-652-8887 Athletic Preparation ACL Reconstruction
MENISCAL REPAIR ACCELERATED REHABILITATION GUIDELINES
 MENISCAL REPAIR ACCELERATED REHABILITATION GUIDELINES MIHAI VIOREANU MD, MCH, FRCSI (TR&ORTH) www.mrmv.ie MR. VIOREANU, WHERE POSSIBLE, WILL TRY TO PRESERVE AND REPAIR THE MENISCUS. Recent research has
MENISCAL REPAIR ACCELERATED REHABILITATION GUIDELINES MIHAI VIOREANU MD, MCH, FRCSI (TR&ORTH) www.mrmv.ie MR. VIOREANU, WHERE POSSIBLE, WILL TRY TO PRESERVE AND REPAIR THE MENISCUS. Recent research has
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) Fax: (763)
 Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
James R. Romanowski, M.D.
 James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
REHABILITATION GUIDELINES FOR ACL REPAIR
 Timothy Crall, MD US Ski Team Physician Bartlett White, PA-C Teaching Associate REHABILITATION GUIDELINES FOR ACL REPAIR PHASE I (0-2 WEEKS) Physical therapy 2-3x/week, beginning 2-5 days post-op Rehabilitation
Timothy Crall, MD US Ski Team Physician Bartlett White, PA-C Teaching Associate REHABILITATION GUIDELINES FOR ACL REPAIR PHASE I (0-2 WEEKS) Physical therapy 2-3x/week, beginning 2-5 days post-op Rehabilitation
Anterior Cruciate Ligament (ACL) Reconstruction Protocol. Hamstring Autograft, Allograft, or Revision
 Anterior Cruciate Ligament (ACL) Reconstruction Protocol Hamstring Autograft, Allograft, or Revision As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp,
Anterior Cruciate Ligament (ACL) Reconstruction Protocol Hamstring Autograft, Allograft, or Revision As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp,
GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
Hip Arthroscopy with CAM resection/labral Repair Protocol
 Hip Arthroscopy with CAM resection/labral Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are
Hip Arthroscopy with CAM resection/labral Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are
ACL Reconstruction Rehabilitation Protocol
 ACL Reconstruction Rehabilitation Protocol 1. Pre-OP Visit: a. Patient Education b. Exercises c. Gait Outline rehabilitation timeline. Discuss: Swelling/effusion control (PRICE). Quadriceps inhibition
ACL Reconstruction Rehabilitation Protocol 1. Pre-OP Visit: a. Patient Education b. Exercises c. Gait Outline rehabilitation timeline. Discuss: Swelling/effusion control (PRICE). Quadriceps inhibition
REHABILITATION GUIDELINES FOR ACL RECONSTRUCTION WITH MICROFRACTURE OR CARTIFORM/BIOCARTILAGE (TROCHLEA OR PATELLA)
 Timothy Crall, MD US Ski Team Physician Bartlett White, PA-C Teaching Associate REHABILITATION GUIDELINES FOR ACL RECONSTRUCTION PHASE I (0-3 WEEKS) Appointments Begin physical therapy 2-5 days post op
Timothy Crall, MD US Ski Team Physician Bartlett White, PA-C Teaching Associate REHABILITATION GUIDELINES FOR ACL RECONSTRUCTION PHASE I (0-3 WEEKS) Appointments Begin physical therapy 2-5 days post op
Rehabilitation Guidelines for ACL Reconstruction in the Older Adolescent Athlete (Hamstrings with No Hardware Across Growth Plates)
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for ACL Reconstruction in the Older Adolescent Athlete (Hamstrings with No Hardware Across Growth Plates) Anterior cruciate ligament (ACL) injuries
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for ACL Reconstruction in the Older Adolescent Athlete (Hamstrings with No Hardware Across Growth Plates) Anterior cruciate ligament (ACL) injuries
Common Knee Injuries
 Common Knee Injuries In 2010, there were roughly 10.4 million patient visits to doctors' offices because of common knee injuries such as fractures, dislocations, sprains, and ligament tears. Knee injury
Common Knee Injuries In 2010, there were roughly 10.4 million patient visits to doctors' offices because of common knee injuries such as fractures, dislocations, sprains, and ligament tears. Knee injury
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
GALLAND/KIRBY PCL RECONSTRUCTION POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY PCL RECONSTRUCTION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue TED Hose
GALLAND/KIRBY PCL RECONSTRUCTION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue TED Hose
Mosaicplasty and OATS Rehabilitation Protocol
 Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
Mosaicplasty and OATS Rehabilitation Protocol PHASE 1: 0 2 weeks after surgery You will go home with crutches, cryocuff cold therapy unit and a CPM machine. GOALS: 1. Protect the cartilage transfer avoid
Diagnosis: s/p ( LEFT / RIGHT ) Injury to MCL of the Knee -- Surgery Date:
 UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
Meniscal Repair Protocol-Dr. McClung
 Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL ACUTE PROXIMAL HAMSTRING TENDON REPAIR BENJAMIN J. DAVIS, MD
 Weeks 0-6 Goal: 1) Protection of the surgical repair Precautions: 1) Non-weight bearing with crutches for 6 weeks with foot flat or with knee Knee flexed to 90 degrees with sitting 2) No active hamstring
Weeks 0-6 Goal: 1) Protection of the surgical repair Precautions: 1) Non-weight bearing with crutches for 6 weeks with foot flat or with knee Knee flexed to 90 degrees with sitting 2) No active hamstring
ACL Reconstruction Physiotherapy advice for patients
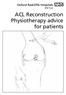 ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction of your anterior cruciate
ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction of your anterior cruciate
ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION
 ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION This DELAYED protocol is used if any of the following are present: meniscal repair, concomitant ligament repair or patellofemoral
ACL RECONSTRUCTION REHABILITATION PROTOCOL DELAYED DAVID R. MACK, M.D. INTRODUCTION This DELAYED protocol is used if any of the following are present: meniscal repair, concomitant ligament repair or patellofemoral
Medical Diagnosis for Michael s Knee
 Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
l. Initiate early proprioceptive activity and progress by means of distraction techniques: i. eyes open to eyes closed ii. stable to unstable m.
 Meniscus Repair 1. Defined a. Sutures or bioabsorbable fixation devices (arrows, darts, screws, etc.) bring together and fixate the edges of a tear in the meniscus in order to maintain the shock absorption
Meniscus Repair 1. Defined a. Sutures or bioabsorbable fixation devices (arrows, darts, screws, etc.) bring together and fixate the edges of a tear in the meniscus in order to maintain the shock absorption
