Zimmer FuZion Instruments. Surgical Technique (Beta Version)
|
|
|
- Juliana Elliott
- 6 years ago
- Views:
Transcription
1 Zimmer FuZion Surgical Technique (Beta Version)
2 INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation, and adequate soft tissue balancing and stability. The are designed to help accomplish these goals by providing the surgeon with dynamic ligament feedback, as well as empirical data. The are based on two platforms: the Spacer Block and Tensor, and were specifically designed to provide crossover utility, harmonizing measured resection and gap balancing philosophies. This surgical technique describes the use of the in common surgical workflows, used in conjunction with the Persona Primary. Surgical Sequence 1. Resect the proximal tibia and the distal femur in preferred order 2. Select the preferred instrument platform 3. Use the to establish the joint tension, while evaluating limb alignment in extension and flexion 4. Using the dynamic and empirical data provided by the, select the optimal implant size and position. INTRO.1
3 Surgical Technique TOC Surgical Technique Table Of Contents Surgical Workflow Steps 1 Surgical Technique: The Basics 5 Tensor with Sizer 6 Spacer Block with Measured Resection 14 Spacer Block with Sizer 22 Tensor with Gap Referencing Drill Guide 30 Transition from a CR to PS 37 Balancing Matrix 38 Persona Knee Surgical Technique Library 40 TOC.1
4 SECTION 1 Surgical Workflow Steps Surgical Workflow Steps Tensor with Sizer 3.5mm Hex Head Screwdriver Assembly Medial Decrease Femoral Rotation Lateral Increase Femoral Rotation Fig. 1 Every click of the tensor pinion is 1mm. Fig. 3 Fig. 7 Femoral sizes are staggered on both sides of the Sizer. Depress the button to adjust the rotation of the sizer body if the femur is internally or over externally rotated. Resect distal femur and proximal tibia. Measure extension space height & angle. Establish flexion space, size, set external rotation (drill holes for Persona Posterior Referencing 4-in-1 Cut Guide). Fig. 9 Place Persona Posterior Referencing 4-in-1 Cut Guide on the bone. Fig. 10 Double check position of the cut guide with the 4-in-1 Adapter. Fig. 11 Optional: Use the shift block to adjust the Persona Posterior Referencing 4-in-1 Cut Guide, 1mm anterior or posterior, or 2 internally or externally. 3.2mm Drill Hole Fig. 12 Fig. 13 Check for notching and complete femoral resections. Verify flexion space and complete procedure. 1
5 Surgical Workflow Steps SECTION 1 Spacer Block with Measured Resection Angle is read using the angle scale and arm of proximal attachment Fig. 14 Arm of proximal attachment Fig. 16 Fig. 19 Resect distal femur and proximal tibia. Measure extension space height & angle. Measure posterior condylar axis angle under tension relative to the tibia. Fig. 22 Fig. 23 Fig. 24 Use Persona Posterior Referencing Sizer to size and set rotation. Place Persona Posterior Referencing 4-in-1 Cut Guide on the bone. Double check position of the cut guide with the 4-in-1 Adapter Fig. 25 Fig. 26 Fig. 27 Optional: Use the shift block to adjust the Persona Posterior Referencing 4-in-1 Cut Guide, 1mm anterior or posterior, or 2 internally or externally. Check for notching and complete femoral resections. Verify flexion space and complete procedure. 2
6 SECTION 1 Surgical Workflow Steps Spacer Block with Sizer Angle is read using the angle scale and arm of proximal attachment Medial Decrease Femoral Rotation Lateral Increase Femoral Rotation Femoral sizes are staggered on both sides of the Sizer. Fig. 28 Fig. 30 Arm of proximal attachment Fig. 36 Depress the button to adjust the rotation of the sizer body if the femur is internally or over externally rotated. Resect distal femur and proximal tibia. Measure extension space height & angle. Establish flexion space, size, set external rotation (drill holes for Persona Posterior Referencing 4-in-1 Cut Guide). Fig. 38 Place Persona Posterior Referencing 4-in-1 Cut Guide on the bone. Fig. 39 Double check position of the cut guide with the 4-in-1 Adapter. Fig. 40 Optional: Use the shift block to adjust the Persona Posterior Referencing 4-in-1 Cut Guide, 1mm anterior or posterior, or 2 internally or externally. 3.2mm Drill Hole Fig. 41 Fig. 42 Check for notching and complete femoral resections. Verify flexion space and complete procedure. 3
7 Surgical Workflow Steps SECTION 1 Tensor with Gap Referencing Drill Guide 3.5mm Hex Head Screwdriver Assembly Stay between 3-7 of rotation. Every click of the tensor pinion is 1mm. Distance should be within 2mm of extension measurement. Fig. 43 Fig. 45 Fig. 48 Resect distal femur and proximal tibia. Measure extension space height & angle. Establish flexion space and set external rotation (drill holes for Persona Posterior Referencing 4-in-1 Cut Guide ) Fig. 51 Fig. 51 Fig. 52 Size the femur with the Persona Posterior Referencing Sizer. DO NOT DRILL THE HOLES! Place Persona Posterior Referencing 4-in-1 Cut Guide on the bone. Double check position of the cut guide with the 4-in-1 Adapter. 3.2mm Drill Hole Fig. 53 Fig. 54 Fig. 55 Optional: Use the shift block to adjust the Persona Posterior Referencing 4-in-1 Cut Guide, 1mm anterior or posterior, or 2 internally or externally Check for notching and complete femoral resections. Verify flexion space and complete procedure. 4
8 SECTION 2 Surgical Technique: The Basics Surgical Technique: The Basics The clinical results of Total Knee Arthroplasty (TKA) are dependent on the surgical technique for both posterior cruciate retaining and substituting designs. The goal of TKA is to reestablish the mechanical axis and restore stability. This is achieved by appropriate bone resection and soft tissue balance. The femoral component should be aligned with the mechanical axis. The tibia should be resected perpendicular to the mechanical axis in the coronal plane. The tibial slope is dictated by the implant design or by the natural slope of the tibia, depending on surgical philosophy. There are three basic bone cuts in TKA: first, the proximal tibia, which influences the flexion and extension gaps; second the distal femur, which influences the extension gap; and third, the posterior femur, which influences the flexion gap. The more bone resected from the proximal tibia, the thicker the tibial component. Resected distal femoral bone will be replaced by the femoral component. Over resection may create an extension gap that is larger than the flexion gap, resulting in instability in extension. Under-resection may create a flexion contracture. Resection of the posterior femoral condyle influences the flexion. Over resection relative to the distal femoral resection may result in a larger flexion gap resulting in flexion instability. A fourth cut, that receives less attention, is the anterior femur, which influences the flexion gap and the patella-femoral joint. The amount of bone resected from the anterior femur is dependent on sizing and the AP position of the resection guide. Under-resection of the anterior femur may be caused by an oversized femoral component or by anterior placement of the correct component with excessive resection of the posterior condyles. This can lead to overstuffing of the patellofemoral joint with possible loss of flexion and increased tension of the anterior soft tissues. Conversely, over-resection of the anterior femur may result in notching of the distal femur. The traditional principles for ligament release state that the tight contracted concave side is released to create a rectangular gap. For a fixed varus deformity, the medial release can include the deep and superficial medial collateral ligament, the semitentinosus tendon and the pes anserenius tendons. Correction of a fixed valgus deformity, the lateral release can include the arcuate complex, iliotibial band, popliteus, and lateral collateral ligament. Following bone resection and soft tissue release the flexion and extension gaps are assessed and should be equal and symmetrical. Note: When assessing femoral rotation and/or tightness it is important to consider: Removing retractors or releasing pressure caused by retractors on the surrounding soft tissues. Removing the foot from the leg holder to avoid biasing the forces on the joint caused by the tibia's position relative to the femur. Ensuring that the flat surfaces of the cut bone are resting completely on the flat surfaces of the spacer block or tensor during assessment and there is no gapping. Ensuring the leg is at 90 when evaluating the flexion space. Everting the patella and/or a small incision window can laterally bias the flexion assessment. While assessing the gap, it is very important to align the spacer block's or tensor's center pivot of the femoral paddle with the center of the knee and the AP Axis of the tibial (medial 1/3 of the tibial tubercle and the anterior insertion of the posterior cruciate). Magnet Usage: Warning: Some instruments in the and the Persona Personalized Knee System contain magnets. All magnetic instruments should be kept a safe distance from a patient's active implantable medical device(s) (i.e. pacemaker). These types of device may be adversely affected by magnets. containing magnets should be kept on an appropriate table or stand when not in use at the surgical site. References Scuderi GR. The Basic Principles in Surgical Techniques in Total Knee Arthroplasty. Knee Arthroplasty Handbook, Springer NY. 2002;
9 Tensor with Zimmer FuZion Sizer Tensor with Zimmer Measured FuZion Resection: Sizer Posterior Referencing 4SECTION 3
10
11 Tensor with Sizer SECTION 3 Tensor with Sizer 1. Perform Distal Femoral and Proximal Tibial Resection (Fig. 1) Verify that the cut surface of the tibia is perpendicular to the long axis of the tibia and the valgus angle of the distal femoral cut restores neutral leg alignment. If desired, a drop rod can be used through the alignment hole and/or slot in the tensor. Note: Osteophytes can impact ligament tension. Ensure all osteophytes are removed prior to assessing soft tissues. Fig. 1 6
12 SECTION 3 Tensor with Sizer 2. Extension Gap Assessment and Initial Ligament Balancing Note: are left and right specific. Remove all the osteophytes and complete the initial ligament balancing. Place the leg in extension. Assemble the Tensor with the +9mm Paddle (Fig. 2). Insert the Tensor into the extension gap. Note: Use the +0mm Femoral Paddle to evaluate the joint space prior to resection. Attach the +9mm Zimmer FuZion Femoral Paddle to the +0mm Femoral Paddle (attachment is magnetic) to evaluate the joint space after the femoral condyles have been resected (Fig. 2 ). Scale indicates varus/valgus and femoral rotation Fig. 2 Scale indicates articular surface thickness Tensor Assembly View +9mm Zimmer FuZion Femoral Paddle Attachment +0mm Femoral Paddle Alignment Rod Features Using 3.5mm Hex Head Screwdriver, apply the appropriate amount of force to the tensor to distract the joint (Fig 3). 3.5mm Hex Head Screwdriver Assembly Every click of the tensor pinion is 1mm. Fig mm, Left Tensor, Femoral Assembly, Left Tensor, Tibial Assembly, Left mm Hex Head Screwdriver mm
13 Tensor with Sizer SECTION 3 The angle scale on the medial side of the instrument should read 0 indicating a rectangular gap. If needed, balance the extension gap using ligament release (Fig. 4). After the gap is balanced and rectangular, measure the gap distance using the gap scale on the anterior face of the Tensor (Fig. 4). Note the extension gap measurement. It will be used to create the appropriate flexion space. While assessing the gap, it is very important to align the tensor's center pivot of the femoral paddle with the center of the knee and the AP Axis of the tibia (medial 1/3 of the tibial tubercle and the anterior insertion of the posterior cruciate) (Fig. 4 & Fig 5). Arm of proximal attachment Angle is read using the angle scale and arm of proximal attachment Fig. 4 Read the gap size from the engrave line on the pin 3. Flexion Gap and Setting Femoral Rotation Remove the Tensor from the extension gap. Remove the +9mm Femoral Paddle. Bring the leg into 90 of flexion. Insert the Tensor with the +0mm Femoral Paddle between the cut tibial surface and the uncut posterior condyles, as shown (Fig. 5). Using the 3.5mm Hex Head Screwdriver, apply the appropriate amount of force to distract the joint. Note: The medial collateral ligament will engage first. The femur will then rotate internally, tightening the lateral collateral until equal tension of both is achieved. Fig. 5 +0mm, Left Tensor, Femoral Assembly, Left Tensor, Tibial Assembly, Left mm Hex Head Screwdriver mm
14 SECTION 3 Tensor with Sizer Assemble the Sizer (Fig. 6). Attach the Sizer to the proximal face of the Femoral Assembly. The wide flat distal face of the Sizer will magnetically attach to the Tensor (Fig. 6). Note: The Sizer is free to slide in any direction on the proximal surface of the femoral arm. 1. Note: The Sizer can be attached to the Tensor after the tensor has been inserted in the joint. 2. Slide the Sizer up to the distal femur so that the bone side of the Sizer is sitting flush against the cut distal surface. Note: The Sizer can be used to adjust the amount of femoral rotation if the natural femur is internally or over externally rotated (Fig. 7). The Sizer offers 2 increments of adjustment. Consider adjusting rotation if the scale is outside 3-7 of external rotation. Use Whiteside's line and/or the epicondylar axis as an additional visual reference to confirm component rotation. If the collateral soft-tissue does not provide adequate stability, the surgeon should use his/her professional medical judgment to assess whether a more constraining implant/system or revision implant/system is necessary. Fig. 6 Sizer magnetically attaches and freely slides into position. Decrease Femoral Rotation Medial Lateral Increase Femoral Rotation Femoral sizes are staggered on both sides of the Zimmer FuZion Sizer. Depress the button to adjust the rotation of the sizer body if the femur is internally or over externally rotated. Fig. 7 9 Posterior Referencing Sizer Stylus Posterior Referencing Sizer Drill Guide mm, Left Tensor, Femoral Assembly, Left Tensor, Tibial Assembly, Left
15 Tensor with Sizer SECTION 3 Position the tip of the Sizer stylus onto the anterior cortex and size the femur (Fig. 8). Caution: If a posterior rough cut is made do not use the angle and gap scales on the Tensor. Note: The Sizer can only be used with the Persona Posterior Referencing 4-in-1 Cut Guides Use the 3.2mm Drill in the drill holes of the Sizer to position the Persona Posterior Referencing 4-in-1 Cut Guides. If needed, use the +2mm/-2mm holes to adjust the flexion space as appropriate (Fig. 8). Fig. 8 Posterior Referencing Posterior Referencing Sizer Stylus Sizer Drill Guide mm, Left Tensor, Femoral Assembly, Left Tensor, Tibial Assembly, Left mm Drill
16 SECTION 3 Tensor with Sizer 4. Verify Rotation of Persona 4-in-1 Cut Guide and Ensure No Notching Insert the Persona Posterior Referencing 4-in-1 Cut Guide (Fig.9). Fig. 9 Prior to resection of the posterior condyles, attach the 4-in-1 Cut Guide Adapter to the Zimmer FuZion Tensor and insert into the posterior holes of the Persona Posterior Referencing 4-in-1 Cut Guide (Fig. 10). Using the 3.5mm Hex Head Screwdriver apply the appropriate amount of force to distract the joint Check to ensure the posterior surface of the Persona Posterior Referencing 4-in-1 Cut Guide is parallel to the tibia and the angle read out is 0 and flexion gap is appropriate based on what was measured in extension. Fig Tensor, Femoral Assembly, Left Tensor, Tibial Assembly, Left Persona Posterior Referencing 4-in-1 Cut Guide - Size in-1 Cut Guide Adapter, Left mm Drill mm Hex Head Screwdriver
17 Tensor with Sizer SECTION 3 If needed, use the Persona Shift Block to adjust the Persona Posterior Referencing 4-in-1 Cut Guide rotation (2 ) or AP position (1mm) prior to making any cuts with the Persona Posterior Referencing 4-in-1 Cut Guide. Place the pegs of the Persona Shift Block in the holes created by the Zimmer FuZion Sizer for the Persona Posterior Referencing 4-in-1 Cut Guide. Establish the new block position by drilling through the holes on the face of the Persona Shift Block that specifies the adjustment that is intended. Use a 3.2mm Drill to drill the holes. Remove the shift block (Fig. 11). Place the Persona Posterior Referencing 4-in-1 Cut Guide on the bone. Use the 4-in-1 Cut Guide Adapter to verify the Persona Posterior Referencing 4-in-1 Cut Guide's new position is correct. Caution: Be sure to put the Persona Posterior Referencing 4-in-1 Cut Guide in the new holes created by the Persona Shift Block. Fig. 11 Persona Shift Block Check for notching by placing a resection guide in the anterior cut slot or by using a 3.2mm Drill in the drill hole in the anterior cut slot of the Persona Posterior Referencing 4-in-1 Cut Guide before making cuts. Change size as appropriate to avoid notching (Fig. 12). 3.2mm Drill Hole Fig. 12 Persona Posterior Referencing 4-in-1 Cut Guide - Size mm Drill Persona Shift Block Resection Guide
18 SECTION 3 Tensor with Sizer 5. Check Flexion Gap Note: The +9mm Femoral Paddle can be attached to the +0mm Femoral Paddle and used with the Tensor to check the flexion gap after resection (Fig. 13). Fig Complete Procedure Use Persona Primary to complete the procedure. 13 Tensor, Femoral Assembly, Left Tensor, Tibial Assembly, Left mm, Left mm
19 Spacer Block with Measured Resection 4SECTION Spacer Block with Measured Resection
20
21 Spacer Block with Measured Resection SECTION 4 Spacer Block with Measured Resection 1. Perform Distal Femoral and Proximal Tibial Resection (Fig. 14) Verify that the cut surface of the tibia is perpendicular to the long axis of the tibia and that the valgus angle of the distal femoral cut restores neutral leg alignment. If desired, a drop rod can be used through the alignment hold and/or slot in the spacer block. Note: Osteophytes can impact ligament tension. Ensure all osteophytes are removed prior to assessing soft tissues. Fig
22 SECTION 4 Spacer Block with Measured Resection 2. Extension Gap Assessment and Initial Ligament Balancing Note: are left and right specific. Remove all the osteophytes and complete the initial ligament balancing. Place the leg in extension. Assemble the Spacer Block (Fig. 15). Insert the Spacer Block into the extension gap (Fig. 16). While assessing the gap, it is very important to align the spacer block's center pivot of the femoral paddle with the center of the knee and the AP Axis of the tibial (medial 1/3 of the tibial tubercle and the anterior insertion of the posterior cruciate) (Fig. 16). Note: Use the +0mm Femoral Paddle to evaluate the joint space prior to resection. Add the +9mm Femoral Paddle to the +0mm Femoral Paddle (attachment is magnetic) to evaluate the joint space after femoral condyles have been resected (Fig. 15). Slot B Tab A Alignment rod features Slide external dovetail (Tab A) into internal dovetail (Slot B) Shims can be added to bottom of Zimmer FuZion Spacer Block to increase the construct thickness and achieve the proper joint tension (Fig. 15). Shims are available for 11, 12, 13, 14, 16, 18, and 20mm construct thicknesses (default thickness of spacer block is 10mm) (Fig. 15). The angle scale is on the medial side of the instrument should read 0 indicating a rectangular gap. If needed, balance the extension gap using ligament release (Fig. 16). Note the Spacer Block construct thickness. It will be used to create the appropriate flexion space. Fig. 15 Angle is read using the angle scale and arm of proximal attachment Arm of proximal attachment Fig Spacer Block, Left mm, Left Spacer Block Shim, 11mm, Left mm
23 Spacer Block with Measured Resection SECTION 4 The Spacer Block can be used as a conventional solid spacer block. The femoral paddle rotation can be locked at 0, in both +0mm and +9mm configurations, by pushing the femoral paddle towards the t-handle (Fig. 17). Paddle release button in locked position Fig. 17 Side view: +0mm Paddle in the locked position (top) Side view: +9mm Paddle in the locked position (bottom) To release, simply push the button created by the femoral paddle when in the lock position until it is flush with the face of the spacer (Fig. 18). Paddle release button in unlocked position Fig. 18 Side view: +0mm Paddle in the unlocked position (top) Side view: +9mm Paddle in the unlocked position (bottom) Spacer Block, Left mm, Left mm
24 SECTION 4 Spacer Block with Measured Resection 3. Size Femur and Set External Rotation Remove the Spacer Block from the extension gap. Dissassemble the +9mm Femoral Paddle from +0mm Femoral Paddle. Bring the leg into 90 of flexion. Insert the Spacer Block between the cut tibial surface and the uncut posterior condyles, as shown (Fig. 19). Shims can be added to the bottom of the Spacer Block to increase the construct thickness and achieve the proper joint tension. Shims are available for 11, 12, 13, 14, 16, 18, and 20mm construct thicknesses (default thickness of spacer is 10mm). Ensure that the posterior condyles are contacting the flat surfaces of the medial and lateral sides of the femoral paddle, that the tibial paddle is sitting flush against the tibial surface and that joint is tensed. Read the angle in the angle display. If the angle is in the positive portion of the angle display, set your Persona Posterior Referencing Sizer to that angle (external rotation). If the scale is in the negative portion of the angle display (portion of the angle scale without numbers) the medial compartment is opening wider than the lateral and the appropriate steps should be made to insure a rectangular flexion space when the posterior resection is made (Fig. 19). If the collateral soft-tissue does not provide adequate stability, the surgeon should use his/her professional medical judgment to assess whether a more constraining implant/system or revision implant/system is necessary. Assemble the Posterior Referencing Sizer Boom with the Posterior Referencing Sizer (Fig. 20). Establish the initial external rotation setting by holding the body (silver portion) of the sizer in one hand, positioning the opposite index finger behind the L or R with the thumb over the L or R, squeeze, adjust to desired setting and release (Fig. 21). External rotation can be set at 0, 3, 5, 7, or 9 left or right. Fig. 19 Fig. 20 Insert and Rotate Squeeze to Unlock Fig Persona Posterior Referencing Sizer Persona Posterior Referencing Sizer Boom Spacer Block, Left mm, Left mm
25 Spacer Block with Measured Resection SECTION 4 Refer to Persona The Personalized Knee System Posterior Referencing Surgical Technique ( ) for instructions and feature highlights of the Posterior Referencing Sizer and 4-in-1 Cut Guides. The Persona Posterior Referencing Sizer is used to size and set rotation without the spacer block in this step (Fig. 22). Fig. 22 Insert the Persona Posterior Referencing 4-in-1 Cut Guide (Fig. 23). Fig. 23 Persona Posterior Referencing 4-in-1 Cut Guide - Size Persona Posterior Referencing Sizer Persona Posterior Referencing Sizer Boom
26 SECTION 4 Spacer Block with Measured Resection 4. Verify Rotation of the Persona 4-in-1 Cut Guide and Ensure No Notching. Prior to resection of the posterior condyles, attach the 4-in-1 Cut Guide Adapter to the Zimmer FuZion Spacer Block and insert into the posterior holes of the Persona Posterior Referencing 4-in-1 Cut Guide (Fig. 24). Shims can be added to bottom of spacer block to increase the construct thickness and achieve the proper joint tension. Shims are available for 11, 12, 13, 14, 16, 18, and 20mm construct thickness (default thickness of spacer block is 10mm). Check to ensure the posterior surface of the Persona Posterior Referencing 4-in-1 Cut Guide is parallel to the tibia, the angle read out is 0, and the flexion gap is appropriate based on what was measured in extension. If needed, use the Persona Shift Block to adjust the Persona Posterior Referencing 4-in-1 Cut Guide rotation (2 ) or AP position (1mm) prior to making any cuts with the Persona Posterior Referencing 4-in-1 Cut Guide. Place the pegs of the Persona Shift Block in the holes created by the Zimmer FuZion Sizer for the Persona Posterior Referencing 4-in-1 Cut Guide. Establish the new block position by drilling through the holes on the face of the Persona Shift Block that specifies the adjustment that is intended. Use a 3.2mm Drill to drill the holes (Fig. 25). Use the 4-in-1 Cut Guide Adapter to verify the Persona Posterior Referencing 4-in-1 Cut Guide's new position is correct. Caution: Be sure to put the Persona Posterior Referencing 4-in-1 Cut Guide in the new holes created by the Persona Shift Block. Fig in-1 Cut Guide Adapter Fig. 25 Persona Shift Block 19 Persona Posterior Referencing 4-in-1 Cut Guide - Size Spacer Block, Left Spacer Block Shim, 11mm, Left Persona Shift Block in-1 Cut Guide Adapter, Left mm Drill
27 Spacer Block with Measured Resection SECTION 4 Check for notching by placing a resection guide in the anterior cut slot or by using a 3.2mm Drill in the drill hole in the anterior cut slot of the Persona Posterior Referencing 4-in-1 Cut Guide before making cuts. Change size as appropriate to avoid notching (Fig. 26). Fig. 26 Persona Posterior Referencing 4-in-1 Cut Guide - Size Spacer Block, Left Spacer Block Shim, 11mm, Left in-1 Cut Guide Adapter, Left Resection Guide mm Drill
28 SECTION 4 Spacer Block with Measured Resection 5. Check the Flexion Space The +9mm Femoral Paddle can be attached to the +0mm Femoral Paddle and used with the Spacer Block to check the flexion gap after resection (Fig. 27). Fig Complete Procedure Use Persona Primary to complete the procedure. 21 Spacer Block, Left mm, Left mm
29 Spacer Block with Sizer SECTION 5 Spacer Block with Sizer
30
31 Spacer Block with Sizer SECTION 5 Spacer Block with Sizer 1. Perform Distal Femoral and Proximal Tibial Resection (Fig. 28) Verify that the cut surface of the tibia is perpendicular to the long axis of the tibia and that the valgus angle of the distal femoral cut restores neutral leg alignment. If desired, a drop rod can be usd through the alignment hole and/or slot in the spacer block. Note: Osteophytes can impact ligament tension. Ensure all osteophytes are removed prior to assessing soft tissues. Fig
32 SECTION 5 Spacer Block with Sizer 2. Extension Gap Assessment and Initial Ligament Balancing Note: are left and right specific. Remove all the osteophytes and complete the initial ligament balancing. Place the leg in extension. Assemble the Spacer Block (Fig. 29). Insert the Spacer Block into the extension gap (Fig. 30). While assessing the gap, it is very important to align the spacer block's center pivot of the femoral paddle with the center of the knee and the AP Axis of the tibial (medial 1/3 of the tibial tubercle and the anterior insertion of the posterior cruciate) (Fig. 30). Note: Use the +0mm Femoral Paddle to evaluate the joint space prior to resection. Add the +9mm Femoral Paddle to the +0mm Femoral Paddle (attachment is magnetic) to evaluate the joint space after femoral condyles have been resected (Fig. 29). Slot B Tab A Alignment rod features Slide external dovetail (Tab A) into internal dovetail (Slot B) Shims can be added to bottom of Zimmer FuZion Spacer Block to increase the construct thickness and achieve the proper joint tension (Fig. 29). Shims are available for 11, 12, 13, 14, 16, 18, and 20mm construct thicknesses (default thickness of spacer block is 10mm) (Fig. 29). The angle scale is on the medial side of the instrument should read 0 indicating a rectangular gap. If needed, balance the extension gap using ligament release (Fig. 30). Note the Spacer Block construct thickness. It will be used to create the appropriate flexion space. Fig. 29 Angle is read using the angle scale and arm of proximal attachment Arm of proximal attachment Fig Spacer Block, Left mm, Left Spacer Block Shim, 11mm, Left mm
33 SECTION Spacer Block with Sizer 5 The Spacer Block can be used as a conventional solid spacer block. The femoral paddle rotation can be locked at 0, in both +0mm and +9mm configurations, by pushing the femoral paddle towards the t-handle (Fig. 31 ). Paddle release button in locked position Fig. 31 Side view: +0mm Paddle in the locked position (top) Side view: +9mm Paddle in the locked position (bottom) To release, simply push the button created by the femoral paddle when it is in the lock position until it is flush with the face of the spacer (Fig. 32). Paddle release button in unlocked position Fig. 32 Side view: +0mm Paddle in the unlocked position (top) Side view: +9mm Paddle in the unlocked position (bottom) Spacer Block, Left mm, Left mm
34 SECTION 5 Spacer Block with Sizer 3. Flexion Gap and Setting Femoral Rotation Remove the Spacer Block from the extension gap. Dissassemble the +9mm Femoral Paddle from +0mm Femoral Paddle. Bring the leg into 90 of flexion. Insert the Spacer Block between the cut tibial surface and the uncut posterior condyles, as shown (Fig. 33). Shims can be added to the bottom of the Spacer Block to increase the construct thickness and achieve the proper joint tension. Shims are available for 11, 12, 13, 14, 16, 18, and 20mm construct thicknesses (default thickness of spacer block is 10mm). Fig. 33 Assemble Sizer. Attach the Sizer to the proximal face of the Spacer Block. The wide flat distal face of the Sizer will magnetically attach to the Spacer Block (Fig. 34) Fig. 34 Sizer magnetically attaches and freely slides into position. 25 Posterior Referencing Sizer Stylus Posterior Referencing Sizer Drill Guide Spacer Block, Left mm, Left Spacer Block Shim, 11mm, Left
35 SECTION Spacer Block with Sizer 5 Note: The Sizer is free to slide in any direction on the proximal surface of the spacer block. Slide the Sizer up to the distal femur so that the bone side of the Sizer is sitting flush against the cut distal surface. Position the tip of the Sizer stylus onto the anterior cortex and size the femur (Fig. 35). Fig. 35 Note: The Sizer can be used to adjust the amount of femoral rotation if the natural femur is internally or over externally rotated (Fig. 36). The Sizer offers 2 increments of adjustment. Consider adjusting rotation if the scale is outside 3-7 of external rotation. Use Whiteside's line and/or the epicondylar axis as an additional visual reference to confirm component rotation. If the collateral soft-tissue does not provide adequate stability, the surgeon should use his/her professional medical judgment to assess whether a more constraining implant/system or revision implant/system is necessary. Decrease Femoral Rotation Medial Lateral Increase Femoral Rotation Femoral sizes are staggered on both sides of the Zimmer FuZion Sizer. Depress the button to adjust the rotation of the sizer body if the femur is internally or over externally rotated. Fig. 36 Posterior Referencing Sizer Stylus Posterior Referencing Sizer Drill Guide Spacer Block, Left mm, Left
36 SECTION 5 Spacer Block with Sizer Caution: If a posterior rough cut is made do not use the angle and gap scales on the Spacer Block. Note: The Sizer can only be used with the Persona Posterior Referencing 4-in-1 Cut Guides Use the 3.2mm Drill in the drill holes of the Sizer to position the Posterior Referencing 4-in-1 Cut Guides. If needed, use the +2mm/-2mm holes to adjust the flexion space as appropriate (Fig. 37). Fig. 37 Remove Spacer Block and Sizer. Insert Persona Posterior Referencing 4-in1 Cut Guide (Fig. 38). Fig Posterior Referencing Sizer Stylus Posterior Referencing Sizer Drill Guide Spacer Block, Left mm, Left Persona Posterior Referencing 4-in-1 Cut Guide - Size mm Drill
37 SECTION Spacer Block with Sizer 5 4. Verify Rotation of Persona 4-in-1 Cut Guide and Ensure No Notching Prior to resection of the posterior condyles, attach the 4-in-1 Cut Guide Adapter to the Zimmer FuZion Spacer Block and insert into the posterior holes of the Persona Posterior Referencing 4-in-1 Cut Guide (Fig. 39). Shims can be added to bottom of spacer block to increase the construct thickness and achieve the proper joint tension. Shims are available for 11, 12, 13, 14, 16, 18, and 20mm construct thicknesses (default thickness of spacer block is 10mm). Check to ensure the posterior surface of the Persona Posterior Referencing 4-in-1 Cut Guide is parallel to the tibia and the angle read out is 0 and flexion gap (articular surface thickness) is appropriate based on what was measured in extension. If needed, use the Persona Shift Block to adjust the Persona Posterior Referencing 4-in-1 Cut Guide rotation (2 ) or AP position (1mm) prior to making any cuts with the Persona Posterior Referencing 4-in-1 Cut Guide (Fig. 40). Place the pegs of the Persona Shift Block in the holes created by the Sizer for the Persona Posterior Referencing 4-in-1 Cut Guide. Establish the new block position by drilling through the holes on the face of the Persona Shift Block that specifies the adjustment that is intended. Use a 3.2mm Drill to drill the holes. Use the 4-in-1 Cut Guide Adapter to verify the Persona Posterior Referencing 4-in-1 Cut Guide's new position is correct. Caution: Be sure to put the Persona Posterior Referencing 4-in-1 Cut Guide in the new holes created by the Persona Shift Block. Fig in-1 Cut Guide Adapter Fig. 40 Persona Shift Block Persona Posterior Referencing 4-in-1 Cut Guide - Size Spacer Block, Left Spacer Block Shim, 11mm, Left Persona Shift Block in-1 Cut Guide Adapter, Left mm Drill
38 SECTION 5 Spacer Block with Sizer Check for notching by placing a resection guide in the anterior cut slot or by using a 3.2mm Drill in the drill hole in the anterior cut slot of the Persona Posterior Referencing 4-in-1 Cut Guide before making cuts. Change size as appropriate to avoid notching (Fig. 41). 3.2mm Drill Hole Fig. 41 Check the Flexion Space The +9mm Femoral Paddle can be attached to the +0mm Femoral Paddle and used with the Spacer Block to check the flexion gap after resection (Fig. 42). 5. Complete Procedure Use Persona Primary to complete the procedure. Fig Spacer Block, Left mm, Left mm Resection Guide mm Drill Persona Posterior Referencing 4-in-1 Cut Guide - Size in-1 Cut Guide Adapter, Left
39 Tensor with Gap Referencing Drill Guide 6SECTION Tensor with Gap Referencing Drill Guide
40
41 Tensor with Gap Referencing Drill Guide SECTION 6 Tensor with Gap Referencing Drill Guide 1. Perform Distal Femoral and Proximal Tibial Resection (Fig. 43) Verify that the cut surface of the tibia is perpendicular to the long axis of the tibia and the valgus angle of the distal femoral cut restores neutral leg alignment. If desired, a drop rod can be used through the alignment hole and/or slot in the tensor. Note: Osteophytes can impact ligament tension. Ensure all osteophytes are removed prior to assessing soft tissues. Fig
42 SECTION 6 Tensor with Gap Referencing Drill Guide 2. Extension Gap Assessment and Initial Ligament Balancing Note: are left and right specific. Remove all the osteophytes and complete the initial ligament balancing. Place the leg in extension. Assemble the Tensor with the +9mm Paddle (Fig. 44). Insert the Tensor into the extension gap. Note: Use the +0mm Femoral Paddle to evaluate the joint space prior to resection. Attach the +9mm Femoral Paddle to the +0mm Femoral Paddle (attachment is magnetic) to evaluate the joint space after the femoral condyles have been resected (Fig. 44). Scale indicates varus/valgus and femoral rotation Fig. 44 Scale indicates articular surface thickness Tensor Assembly View +9mm Zimmer FuZion Femoral Paddle Attachment +0mm Femoral Paddle Alignment Rod Features Using 3.5mm Hex Head Screwdriver, apply the appropriate amount of force to the tensor to distract the joint (Fig 45). 3.5mm Hex Head Screwdriver Assembly Every click of the tensor pinion is 1mm. Fig mm, Left Tensor, Femoral Assembly, Left Tensor, Tibial Assembly, Left mm Hex Head Screwdriver mm
43 Tensor with Gap Referencing Drill Guide SECTION 6 While assessing the gap, it is very important to align the tensor's center pivot of the femoral paddle with the center of the knee and the AP Axis of the tibia (medial 1/3 of the tibial tubercle and the anterior insertion of the posterior cruciate) (Fig. 46 & Fig. 48). The angle scale on the medial side of the instrument should read 0 indicating a rectangular gap. If needed, balance the extension gap using ligament release (Fig. 46). After the gap is balanced and rectangular, measure the gap distance using the gap scale on the anterior face of the Tensor (Fig. 46). Note the extension gap measurement. It will be used to create the appropriate flexion space. Arm of proximal attachment Angle is read using the angle scale and arm of proximal attachment Fig. 46 Read the gap size from the engrave line on the pin 3. Flexion Gap and Setting Femoral Rotation Remove the Tensor from the extension gap. Remove the +9mm Femoral Paddle. Assemble the Gap Referencing Drill Guide to the Zimmer FuZion Tensor (Fig. 47). Fig. 47 Tensor, Femoral Assembly, Left Tensor, Tibial Assembly, Left Gap Referencing Drill Guide mm, Left mm Hex Head Screwdriver mm
44 SECTION 6 Tensor with Gap Referencing Drill Guide Bring the leg into 90 of flexion. Insert the Tensor between the cut tibial surface and the uncut posterior condyles, as shown (Fig. 48). Using the 3.5mm Hex Head Screwdriver, apply the appropriate amount of force to distract the joint (Fig. 48). Note: The medial collateral ligament will engage first. The femur will then rotate internally, tightening the lateral collateral until equal tension of both is achieved. Caution: If a posterior rough cut is made do not use the angle and gap scales on the Tensor. Ensure that the scale reads between 3-7 of rotation using Whiteside's line and/or the epicondylar axis as an additional visual reference to confirm component rotation (Fig. 48). If the collateral soft-tissue does not provide adequate stability, the surgeon should use his/her professional medical judgment to assess whether a more constraining implant/system or revision implant/system is necessary. Double check the posterior cut creates a flexion gap within 2mm of the extension gap (Fig. 48). Stay between 3-7 of rotation. Distance should be within 2mm of extension measurement. Fig. 48 Caution: Double check, when measuring in flexion, that the distance on the tensor scale is within 2mm of what was measured in extension. Remember to use the +0mm Zimmer FuZion Femoral Paddle to evaluate the joint space prior to resection and +9mm Femoral Paddle to evaluate the joint space after resection (Fig. 48). Select the holes on the drill guide that match the gap measured in extension. Drill the holes using the 3.2mm Drill. These will position the Persona Posterior Referencing 4-in-1 Cut Guide (Fig. 49). Note: Ensure the Gap Referencing Drill Guide is parallel to the face of the distal femur. Fig. 49 Note: The gap referencing drill guide can only be used with the Persona Posterior Referencing 4-in-1 Cut Guides. Note: The Gap Referencing Drill Guide is designed to ensure a rectangular flexion space without consideration of the posteriorcondylar position. 33 Tensor, Femoral Assembly, Left Tensor, Tibial Assembly, Left Gap Referencing Drill Guide mm, Left mm Hex Head Screwdriver mm mm Drill Persona Posterior Referencing 4-in-1 Cut Guide - Size
45 Tensor with Gap Referencing Drill Guide SECTION 6 4. Size Femur Assemble the Posterior Referencing Sizer Boom with the Posterior Referencing Sizer (Fig. 50). Note: The Persona Posterior Referencing Sizer is only intended to provide an estimated component size at this point in the surgical technique. Do not use the sizer to drill holes for the 4-in-1 Cut Guide. Insert and Rotate Fig. 50 Refer to Persona The Personalized Knee System Posterior Referencing Surgical Technique ( ) for instructions and feature highlights of the Posterior Referencing Sizer and 4-in-1 Cut Guides. Use the Persona Posterior Referencing Sizer to size the femur (Fig. 51). Insert the Persona Posterior Referencing 4-in-1 Cut Guide (Fig. 51). Fig. 51 Persona Posterior Referencing Sizer Persona Posterior Referencing Sizer Boom Persona Posterior Referencing 4-in-1 Cut Guide - Size
46 SECTION 6 Tensor with Gap Referencing Drill Guide 5. Verify Rotation of Persona 4-in-1 Cut Guide and Ensure No Notching Prior to resection of the posterior condyles, attach the 4-in-1 Cut Guide Adapter to the Zimmer FuZion Tensor and insert into the posterior holes of the Persona Posterior Referencing 4-in-1 Cut Guide (Fig. 52). Using the 3.5mm Hex Head Screwdriver apply the appropriate amount of force to distract the joint Check to ensure the posterior surface of the Persona Posterior Referencing 4-in-1 Cut Guide is parallel to the tibia and the angle read out is 0 and flexion gap is appropriate based on what was measured in extension. Fig. 52 If needed, use the Persona Shift Block to adjust the Persona Posterior Referencing 4-in-1 Cut Guide rotation (2 ) or AP position (1mm) prior to making any cuts with the Persona Posterior Referencing 4-in-1 Cut Guide. Place the pegs of the Persona Shift Block in the holes created by the Zimmer FuZion Sizer for the Persona Posterior Referencing 4-in-1 Cut Guide. Establish the new block position by drilling through the holes on the face of the Persona Shift Block that specifies the adjustment that is intended. Use a 3.2mm Drill to drill the holes. Remove the shift block, Place the Persona Posterior Referencing 4-in-1 Cut Guide back on the bone (Fig. 53.). Use the 4-in-1 Cut Guide Adapter to verify the Persona Posterior Referencing 4-in-1 Cut Guide's new position is correct. Caution: Be sure to put the Persona Posterior Referencing 4-in-1 Cut Guide in the new holes created by the Persona Shift Block. Fig. 53 Persona Shift Block mm Drill Persona Shift Block Persona Posterior Referencing 4-in-1 Cut Guide - Size Resection Guide Tensor, Femoral Assembly, Left Tensor, Tibial Assembly, Left in-1 Cut Guide Adapter, Left mm Hex Head Screwdriver
47 Tensor with Gap Referencing Drill Guide SECTION 6 Check for notching by placing a resection guide in the anterior cut slot or by using a 3.2mm Drill in the drill hole in the anterior cut slot of the Persona Posterior Referencing 4-in-1 Cut Guide before making cuts. Change size as appropriate to avoid notching (Fig. 54). 3.2mm Drill Hole Caution: By matching the extension gap the posterior condylar resection may be significantly greater or less than the standard 9mm posterior resection. Fig Check the Flexion Space The +9mm Femoral Paddle can be attached to the +0mm Femoral Paddle and used with the Tensor to check the flexion gap after resection (Fig. 55). 7. Complete Procedure Use Persona Primary to complete the procedure. Fig mm Hex Head Screwdriver mm, Left Tensor, Femoral Assembly, Left Tensor, Tibial Assembly, Left mm mm Drill Resection Guide Persona Posterior Referencing 4-in-1 Cut Guide - Size
48 SECTION 7 Transitioning from CR to PS Transitioning from CR to PS The transition from Cruciate Retaining (CR) component to a Posterior Stabilized (PS) component is a fundamental shift in philosophy. Both systems utilize component geometry and positioning to optimize kinematics and survivorship. Both systems have unique approaches to implantation and both systems are successfully used. Zimmer s Persona Personalized Knee System CR component carries its attributes from Zimmer s Natural-Knee System. The geometry of the femoral component utilizes a big wheel/ little wheel design that provides rollback replicating the natural kinematics of the knee. In addition, the tibial polyethelene is more conforming medially and less conforming laterally. The slope of the poly is recommended to be 7 to align to the slope of the natural anatomy. The geometry and cuts are intended to put the components in a position to work with the natural anatomy given the preservation of the cruciate ligament, to provide a natural feel and motion. A transition from CR to a posterior cruciate substituting constraint within this system is typically an Ultra-Congruent (UC) polyethelene tibial insert design that drives motion with a deep concave dish in the medial compartment. The tibial insert also has pronounced anterior and posterior lips to provide anterior/posterior constraint and prevent posterior roll off. The transition to the UC is seamless. The CR femoral component is used with the UC. Removal of the PCL is the only requirement when using the UC component. The UC tibial polyethelene is attached to the tibial baseplate implant in the same manner as the CR tibial polyethelene. Zimmer s Persona Personalized Knee System PS component carries its attributes from Zimmer s NexGen Knee System. The geometry of the femoral component is symmetric, with a posterior condyle that s 1mm thicker than the distal condyle. The post that is used as a substitute for the posterior cruciate engages the cam of the femoral component in mid-flexion and forces femoral rollback. The recommended tibial slope for this component 3. The geometry and cuts are intended to drive motion. In the situations when starting with a CR approach and determining in-situ that a higher level of constraint is needed, certain considerations should be used to ensure that a stable knee with full extension is enabled. The 1mm thicker posterior condyle of the PS femoral component and the box that houses the PS post tibial polyethelene will require some additional preparation when making the transition. Considerations transitioning from CR to a PS design: 1. Utilize a UC tibial insert 2. Recut the tibial slope (from 7 to 3 ) 3. Remove the posterior cruciate ligament 37
49 Balancing Matrix SECTION 8 Balancing Matrix Check Extension Gap After the proximal tibia and distal femur have been resected, the extension gap can be evaluated using the Spacer Block or the Tensor. Position the knee in full extension. The distal thickness of the Persona femoral component is 9mm and the minimum Persona tibial articular surface/baseplate construct is 10mm. If the Spacer Block with the +9mm Paddle (19mm) does not fit into the resected joint space in extension, it will be necessary to remove additional bone from the femur. Use the Spacer Block or the Tensor to check the extension gap. Insert the Spacer Block or Tensor between the resected surfaces of the femur and tibia. If necessary, add Shims to the Spacer Block or adjust the Zimmer FuZion Tensor until the desired soft tissue tension is obtained. Use the alignment rod to check overall alignment. Varus and valgus stress can be used to evaluate ligament stability. Ligament releases can be performed, at this point, to create an extension gap that is rectangular. When the extension gap is balanced, proceed to size femur, establish external rotation and finish the femoral cuts. Tight Extension Tight OK Loose Reduce articular surface thickness Recut tibia Release PCL, Change to a UC For Anterior Referencing: Down size femoral component For Posterior Referencing: Down size femoral component and shift anterior Down size femoral component increase articular surface thickness For Anterior Referencing: Down size femoral component; increase tibial articular surface thickness For Posterior Referencing: Down size femoral component and shift anterior; increase tibial articular surface thickness Check Flexion Gap After the femoral finishing cuts have been completed and with the knee in 90 flexion, use the Spacer Block or the Tensor to check ligament balance and joint alignment in flexion. Check ligament balance. If necessary, insert progressively thicker Zimmer FuZion Spacer Block Shims underneath Spacer Block or adjust the Tensor until the desired soft tissue tension is obtained. Correcting Gaps (Fig. 56): 1. If a knee is too tight in both flexion and extension, reducing the height of the tibial articular surface may be sufficient to balance the construct. If the thinnest tibial articular surface is too tight, resect more tibia. 2. If the knee is tight in flexion but acceptable in extension, two options exist. One option is to release the PCL. If the PCL is absent, change constraint to UC. The second option is to downsize the femoral component. 3. If the joint is loose in extension and tight in flexion one option is to use a smaller sized femoral component possibly with a thicker polyethylene component. 4. If the joint is acceptable in flexion but tight in extension, two options exist. One is to release the posterior capsule from the femur. Another alternative is to resect more distal femoral bone. This moves the femoral component proximally on the femur at the expense of elevating the joint line. Flexion Loose OK Fig Release the posterior capsule from the femur Resect more distal femur (will elevate the joint line) OK Down size femoral component, increase articular surface thickness For Anterior Referencing: Down size femoral component; increase tibial articular surface thickness For Posterior Referencing: Down size femoral component and shift anterior; increase tibial articular surface thickness For Anterior Referencing: Up size femoral component For Posterior Referencing: Up size femoral component and shift posterior Reduce articular surface thickness Posterior release, increase articular surface thickness For Anterior Referencing: Up size femoral component For Posterior Referencing: Up size femoral component and shift posterior Posterior release, increase articular surface thickness Increase articular surface thickness 38
50 SECTION 8 Balancing Matrix 5. If both components are acceptable, no further modification is necessary. 6. If the joint is acceptable in flexion and loose in extension, consider downsizing the femoral component with a thicker tibial articular surface. 7. If the joint is loose in flexion and tight in extension, a larger femoral component may suffice combined with a posterior release. 8. If the joint is loose in flexion and acceptable in extension, increasing the femoral size may equalize the gaps. Alternatively, moving the femoral component proximally and applying a thicker tibial articular surface will equalize the gaps. Another option is to fill the flexion gap with the appropriate poly and perform a posterior release to increase the extension gap. 9. If a joint is symmetrically loose in both flexion and extension, a thicker tibial articular surface will usually solve both problems. Tight Extension Tight OK Loose Reduce articular surface thickness Recut tibia Release PCL, Change to a UC For Anterior Referencing: Down size femoral component Down size femoral component increase articular surface thickness For Anterior Referencing: Down size femoral component; increase tibial articular surface thickness TECHNIQUE TIP 8.A Also consider the position of the patella and/or the joint line when deciding which correction to make. For Posterior Referencing: Down size femoral component and shift anterior For Posterior Referencing: Down size femoral component and shift anterior; increase tibial articular surface thickness Note: after applying one of these solutions, perform another trial reduction. This will identify any new problem or a variation of the initial problem that may exist. Flexion OK Release the posterior capsule from the femur Resect more distal femur (will elevate the joint line) OK Down size femoral component, increase articular surface thickness For Anterior Referencing: Down size femoral component; increase tibial articular surface thickness For Posterior Referencing: Down size femoral component and shift anterior; increase tibial articular surface thickness For Anterior Referencing: Up size femoral component For Anterior Referencing: Up size femoral component Increase articular surface thickness Loose For Posterior Referencing: Up size femoral component and shift posterior Reduce articular surface thickness Posterior release, increase articular surface thickness For Posterior Referencing: Up size femoral component and shift posterior Posterior release, increase articular surface thickness Fig
51 Persona Knee Surgical Technique Library SECTION 9 Persona Knee Surgical Technique Library Surgical Technique Name Literature Number Persona The Personalized Knee System Surgical Technique Persona The Personalized Knee System Posterior Referencing Surgical Technique Persona The Personalized Knee System Trabecular Metal Tibia Surgical Technique Persona The Personalized Knee System Trabecular Metal Femur Surgical Technique
52 Disclaimer This documentation is intended exclusively for physicians and is not intended for laypersons. Information on the products and procedures contained in this document is of a general nature and does not represent and does not constitute medical advice or recommendations. Because this information does not purport to constitute any diagnostic or therapeutic statement with regard to any individual medical case, each patient must be examined and advised individually, and this document does not replace the need for such examination and/or advice in whole or in part. Please refer to the package inserts for important product information, including, but not limited to, contraindications, warnings, precautions, and adverse effects. Contact your Zimmer representative or visit us at MC /06/ Zimmer, Inc.
Constrained Posterior Stabilized (CPS) Surgical Technique
 Constrained Posterior Stabilized (CPS) Surgical Technique Constrained Posterior Stabilized (CPS) Surgical Technique INTRO Introduction The Constrained Posterior Stabilized (CPS) articular surfaces can
Constrained Posterior Stabilized (CPS) Surgical Technique Constrained Posterior Stabilized (CPS) Surgical Technique INTRO Introduction The Constrained Posterior Stabilized (CPS) articular surfaces can
TOTAL KNEE ARTHROPLASTY SYSTEM
 SURGICAL TECHNIQUE TOTAL KNEE ARTHROPLASTY SYSTEM 90-SRK-700000 B.0 0 Contents 1. Implant Sizing 2. Surgical Technique a. Incision and Exposure b. Distal Femoral Resection c. Tibial Resection d. Femoral
SURGICAL TECHNIQUE TOTAL KNEE ARTHROPLASTY SYSTEM 90-SRK-700000 B.0 0 Contents 1. Implant Sizing 2. Surgical Technique a. Incision and Exposure b. Distal Femoral Resection c. Tibial Resection d. Femoral
Revolution. Unicompartmental Knee System
 Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Constrained Posterior Stabilized (CPS)
 Constrained Posterior Stabilized (CPS) Persona The Personalized Knee Surgical Technique Table of Contents Introduction... 2 Constraint Options Initial Knee Assessment... 3 Femoral Box Cut CPS Tibial Bearing
Constrained Posterior Stabilized (CPS) Persona The Personalized Knee Surgical Technique Table of Contents Introduction... 2 Constraint Options Initial Knee Assessment... 3 Femoral Box Cut CPS Tibial Bearing
Distal Cut First Femoral Preparation
 Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Persona. The Personalized Knee. Trabecular Metal Tibia. Surgical Technique
 Persona The Personalized Knee Trabecular Metal Tibia Surgical Technique Table of Contents Resect the Tibia... 4 Size and Finish the Tibia... 4 Trial Fit... 6 Component Implantation... 7 Inserter/Implant
Persona The Personalized Knee Trabecular Metal Tibia Surgical Technique Table of Contents Resect the Tibia... 4 Size and Finish the Tibia... 4 Trial Fit... 6 Component Implantation... 7 Inserter/Implant
Extramedullary Tibial Preparation
 Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Contact your Zimmer representative or visit us at
 Please refer to the package inserts for complete product information, including contraindications, warnings, precautions, and adverse effects. Contact your Zimmer representative or visit us at www.zimmer.com
Please refer to the package inserts for complete product information, including contraindications, warnings, precautions, and adverse effects. Contact your Zimmer representative or visit us at www.zimmer.com
Surgical Technique. VISIONAIRE FastPak Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE FastPak Instruments for the LEGION Total Knee System VISIONAIRE FastPak for LEGION Instrument Technique* Nota Bene The technique description herein is made available to the
Surgical Technique VISIONAIRE FastPak Instruments for the LEGION Total Knee System VISIONAIRE FastPak for LEGION Instrument Technique* Nota Bene The technique description herein is made available to the
NATURAL MOTION TECHNOLOGY SURGICAL TECHNIQUE. EMPOWR 3D Knee. EMPOWR PS Knee
 NATURAL MOTION TECHNOLOGY EMPOWR 3D Knee EMPOWR PS Knee SURGICAL TECHNIQUE Contents System Features.... 3 Indications and Contraindications.... 4 Surgical Snap Shot.... Preoperative Planning.... Surgical
NATURAL MOTION TECHNOLOGY EMPOWR 3D Knee EMPOWR PS Knee SURGICAL TECHNIQUE Contents System Features.... 3 Indications and Contraindications.... 4 Surgical Snap Shot.... Preoperative Planning.... Surgical
Intramedullary Tibial Preparation
 Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Triathlon Knee System
 Triathlon Knee System Express Instruments Surgical Protocol Posterior Stabilized & Cruciate Retaining TriathlonKneeSystem Express Instruments Surgical Protocol Acknowledgments..........................................................2
Triathlon Knee System Express Instruments Surgical Protocol Posterior Stabilized & Cruciate Retaining TriathlonKneeSystem Express Instruments Surgical Protocol Acknowledgments..........................................................2
NexGen Cruciate Retaining (CR) and Revision Instrumentation. Surgical Technique
 NexGen Cruciate Retaining (CR) and Revision Instrumentation Surgical Technique Table of Contents Introduction... 4 Revision Arthroplasty... 4 Multi-Reference 4-in-1 Instrumentation System MICRO-MILL Instrumentation
NexGen Cruciate Retaining (CR) and Revision Instrumentation Surgical Technique Table of Contents Introduction... 4 Revision Arthroplasty... 4 Multi-Reference 4-in-1 Instrumentation System MICRO-MILL Instrumentation
Trabecular Metal Femoral Component. Surgical Technique
 Trabecular Metal Femoral Component Surgical Technique INTRO Trabecular Metal Femoral Component Surgical Technique Introduction The Persona Trabecular Metal Femoral Component is designed to unite stable
Trabecular Metal Femoral Component Surgical Technique INTRO Trabecular Metal Femoral Component Surgical Technique Introduction The Persona Trabecular Metal Femoral Component is designed to unite stable
JOINT RULER. Surgical Technique For Knee Joint JRReplacement
 JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
JR JOINT RULER Surgical Technique For Knee Joint JRReplacement INTRODUCTION The Joint Ruler * is designed to help reduce the incidence of flexion, extension, and patellofemoral joint problems by allowing
Zimmer NexGen MIS Tibial Component. Cemented Surgical Technique IMAGE TO COME
 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
Zimmer NexGen Trabecular Metal Tibial Tray
 Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Give Bone A Solid Hold Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique
Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Give Bone A Solid Hold Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique
Masterclass. Tips and tricks for a successful outcome. E. Verhaven, M. Thaeter. September 15th, 2012, Brussels
 Masterclass Tips and tricks for a successful outcome September 15th, 2012, Brussels E. Verhaven, M. Thaeter Belgium St. Nikolaus-Hospital Orthopaedics & Traumatology Ultimate Goal of TKR Normal alignment
Masterclass Tips and tricks for a successful outcome September 15th, 2012, Brussels E. Verhaven, M. Thaeter Belgium St. Nikolaus-Hospital Orthopaedics & Traumatology Ultimate Goal of TKR Normal alignment
Surgical Technique. VISIONAIRE Disposable Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Persona The Personalized Knee. Surgical Technique
 Persona The Personalized Knee Surgical Technique Table of Contents Introduction... 2 Constraint Options Preoperative Planning Surgical Approach Patient Preparation Magnet Usage Symbols Screw/Pin Information
Persona The Personalized Knee Surgical Technique Table of Contents Introduction... 2 Constraint Options Preoperative Planning Surgical Approach Patient Preparation Magnet Usage Symbols Screw/Pin Information
Patient Specific Instruments. Surgical Technique
 Patient Specific Instruments Surgical Technique Patient Specific Instruments Surgical Technique INTRO Introduction General Considerations Zimmer Patient Specific Instruments (PSI) are not designed for
Patient Specific Instruments Surgical Technique Patient Specific Instruments Surgical Technique INTRO Introduction General Considerations Zimmer Patient Specific Instruments (PSI) are not designed for
The information contained in this document is intended for healthcare professionals only.
 The information contained in this document is intended for healthcare professionals only. Triathlon Knee System Posterior Stabilized & Cruciate Retaining Table of Contents Acknowledgments.......................................................1
The information contained in this document is intended for healthcare professionals only. Triathlon Knee System Posterior Stabilized & Cruciate Retaining Table of Contents Acknowledgments.......................................................1
POSTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION. Multi-Reference 4-in-1 Femoral Instrumentation Posterior Reference Surgical Technique
 POSTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Posterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees
POSTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Posterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees
TKA Gap Planning. Supporting healthcare professionals
 TKA Gap Planning The NAVIO TKA Gap Planning stage helps you adjust the plan based on gap information between the femur and tibia implants. Supporting healthcare professionals Interactive Views Four interactive
TKA Gap Planning The NAVIO TKA Gap Planning stage helps you adjust the plan based on gap information between the femur and tibia implants. Supporting healthcare professionals Interactive Views Four interactive
ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION. Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique
 ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees INTRODUCTION
ANTERIOR REFERENCE NEXGEN COMPLETE KNEE SOLUTION Multi-Reference 4-in-1 Femoral Instrumentation Anterior Reference Surgical Technique For NexGen Cruciate Retaining & Legacy Posterior Stabilized Knees INTRODUCTION
LAMINA SPREADER SURGICAL TECHNIQUE
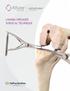 LAMINA SPREADER SURGICAL TECHNIQUE Balanced and appropriate external rotation of the femoral component is important for tibio-femoral stability in flexion and patello-femoral tracking/function. Depending
LAMINA SPREADER SURGICAL TECHNIQUE Balanced and appropriate external rotation of the femoral component is important for tibio-femoral stability in flexion and patello-femoral tracking/function. Depending
NexGen Complete Knee Solution. Cruciate Retaining (CR) and Revision Instrumentation Surgical Technique for Cruciate Retaining Augmentable (CRA) Knees
 NexGen Complete Knee Solution Cruciate Retaining (CR) and Revision Instrumentation Surgical Technique for Cruciate Retaining Augmentable (CRA) Knees INTRODUCTION This surgical technique document combines
NexGen Complete Knee Solution Cruciate Retaining (CR) and Revision Instrumentation Surgical Technique for Cruciate Retaining Augmentable (CRA) Knees INTRODUCTION This surgical technique document combines
MIS Cemented Tibial Component
 MIS Cemented Tibial Component NexGen Complete Knee Solution Surgical Technique Table of Contents Surgical Exposure... 2 Finish the Tibia... 2 Position Based on Anatomic Landmarks... 3 Lateral Posterior
MIS Cemented Tibial Component NexGen Complete Knee Solution Surgical Technique Table of Contents Surgical Exposure... 2 Finish the Tibia... 2 Position Based on Anatomic Landmarks... 3 Lateral Posterior
Zimmer Unicompartmental High Flex Knee. Spacer Block Surgical Technique
 Zimmer Unicompartmental High Flex Knee Spacer Block Surgical Technique INTRO Zimmer Unicompartmental High Flex Knee Spacer Block Surgical Technique Introduction Unicompartmental knee arthroplasty (UKA)
Zimmer Unicompartmental High Flex Knee Spacer Block Surgical Technique INTRO Zimmer Unicompartmental High Flex Knee Spacer Block Surgical Technique Introduction Unicompartmental knee arthroplasty (UKA)
PIN GUIDE SYSTEM SURGICAL TECHNIQUE. with the SIGMA High Performance Instruments System. This publication is not intended for distribution in the USA.
 PIN GUIDE SYSTEM with the SIGMA High Performance Instruments System This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Pin Guide Surgical Technique The following steps are
PIN GUIDE SYSTEM with the SIGMA High Performance Instruments System This publication is not intended for distribution in the USA. SURGICAL TECHNIQUE Pin Guide Surgical Technique The following steps are
Triathlon Knee System. Universal Baseplate Surgical Protocol
 Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments..........................................................2 Introduction...............................................................2
Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments..........................................................2 Introduction...............................................................2
INTUITION INSTRUMENTS SURGICAL TECHNIQUE
 INTUITION INSTRUMENTS SURGICAL TECHNIQUE Introduction This surgical technique provides guidelines for the implantation of the ATTUNE Knee System Family of Knee Implants with the INTUITION Instrumentation.
INTUITION INSTRUMENTS SURGICAL TECHNIQUE Introduction This surgical technique provides guidelines for the implantation of the ATTUNE Knee System Family of Knee Implants with the INTUITION Instrumentation.
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments
 TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Resection Guide System SURGICAL TECHNIQUE RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA
Zimmer Patient Specific Instruments. Surgical Techniques for NexGen Complete Knee Solution
 Zimmer Patient Specific Instruments Surgical Techniques for NexGen Complete Knee Solution INTRO Zimmer Patient Specific Instruments Surgical Techniques for NexGen Complete Knee Solution Table of Contents
Zimmer Patient Specific Instruments Surgical Techniques for NexGen Complete Knee Solution INTRO Zimmer Patient Specific Instruments Surgical Techniques for NexGen Complete Knee Solution Table of Contents
INTUITION INSTRUMENTS SURGICAL TECHNIQUE
 INTUITION INSTRUMENTS SURGICAL TECHNIQUE Introduction This surgical technique provides guidelines for the implantation of the ATTUNE Knee System Family of Knee Implants with the INTUITION Instrumentation.
INTUITION INSTRUMENTS SURGICAL TECHNIQUE Introduction This surgical technique provides guidelines for the implantation of the ATTUNE Knee System Family of Knee Implants with the INTUITION Instrumentation.
Triathlon Knee System Universal Baseplate Surgical Protocol
 Triathlon Knee System Universal Baseplate Surgical Protocol Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments... 2 Introduction... 2 Assembly Instructions...
Triathlon Knee System Universal Baseplate Surgical Protocol Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments... 2 Introduction... 2 Assembly Instructions...
Total Knee Original System Primary Surgical Technique
 Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Surgical Procedure Total Knee Original System Primary Surgical Technique Where as a total hip replacement is primarily a bony operation, a total knee replacement is primarily a soft tissue operation. Excellent
Zimmer Patient Specific Instruments. Surgical Technique for Gender Solutions Natural-Knee Flex System
 Zimmer Patient Specific Instruments Surgical Technique for Gender Solutions Natural-Knee Flex System TOC Zimmer Patient Specific Instruments Surgical Technique for Gender Solutions Natural-Knee Flex Table
Zimmer Patient Specific Instruments Surgical Technique for Gender Solutions Natural-Knee Flex System TOC Zimmer Patient Specific Instruments Surgical Technique for Gender Solutions Natural-Knee Flex Table
TRK REVISION KNEE Surgical Technique
 1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
ANATOMIC SURGICAL TECHNIQUE. 5 in 1. Conventional instrumentation 07/11/2013
 ANATOMIC SURGICAL TECHNIQUE 5 in 1 Conventional instrumentation PRO.GB.933/1.0 Octobre 2013 2 Tibial step 3 Intramedullary technique - Based on the preoperative plan, drill the medullary canal with the
ANATOMIC SURGICAL TECHNIQUE 5 in 1 Conventional instrumentation PRO.GB.933/1.0 Octobre 2013 2 Tibial step 3 Intramedullary technique - Based on the preoperative plan, drill the medullary canal with the
Zimmer NexGen. LPS-Flex Fixed Bearing Knee. Surgical Technique. Designed to accomodate resumption of high-flexion daily activities
 Zimmer NexGen LPS-Flex Fixed Bearing Knee Surgical Technique Designed to accomodate resumption of high-flexion daily activities Zimmer NexGen LPS-Flex Fixed Bearing Knee Surgical Technique 1 Zimmer NexGen
Zimmer NexGen LPS-Flex Fixed Bearing Knee Surgical Technique Designed to accomodate resumption of high-flexion daily activities Zimmer NexGen LPS-Flex Fixed Bearing Knee Surgical Technique 1 Zimmer NexGen
Zimmer Unicompartmental High Flex Knee. Intramedullary, Spacer Block Option and Extramedullary Minimally Invasive Surgical Techniques
 Zimmer Unicompartmental High Flex Knee Intramedullary, Spacer Block Option and Extramedullary Minimally Invasive Surgical Techniques ZIMMER UNICOMPARTMENTAL HIGH FLEX KNEE INTRAMEDULLARY, SPACER BLOCK
Zimmer Unicompartmental High Flex Knee Intramedullary, Spacer Block Option and Extramedullary Minimally Invasive Surgical Techniques ZIMMER UNICOMPARTMENTAL HIGH FLEX KNEE INTRAMEDULLARY, SPACER BLOCK
CONTRIBUTING SURGEON. Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD
 CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
NEXGEN COMPLETE KNEE SOLUTION
 NEXGEN COMPLETE KNEE SOLUTION Surgical Technique for the Legacy Knee LPS-Flex Mobile Bearing Knee This device is not available for commercial distribution in the U.S. Implants and Surgical Technique developed
NEXGEN COMPLETE KNEE SOLUTION Surgical Technique for the Legacy Knee LPS-Flex Mobile Bearing Knee This device is not available for commercial distribution in the U.S. Implants and Surgical Technique developed
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments
 TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Pin Guide System SURGICAL TECHNIQUE PIN GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA High Performance
TRUMATCH PERSONALIZED SOLUTIONS with the SIGMA High Performance Instruments Pin Guide System SURGICAL TECHNIQUE PIN GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the SIGMA High Performance
NexGen Trabecular Metal Tibial Tray. Surgical Technique
 NexGen Trabecular Metal Tibial Tray Surgical Technique Table of Contents Surgical Technique...2 Resect the Tibia...2 Finish the Tibia...2 Position Based Anatomic Landmarks...3 Position Based on Trial
NexGen Trabecular Metal Tibial Tray Surgical Technique Table of Contents Surgical Technique...2 Resect the Tibia...2 Finish the Tibia...2 Position Based Anatomic Landmarks...3 Position Based on Trial
OrthoMap Express Knee Product Guide. OrthoMap Express Knee Navigation Software 2.0
 OrthoMap Express Knee Product Guide OrthoMap Express Knee Navigation Software 2.0 Product Guide 1 Introduction Introduction The Stryker OrthoMap Express Knee Navigation System is providing surgeons with
OrthoMap Express Knee Product Guide OrthoMap Express Knee Navigation Software 2.0 Product Guide 1 Introduction Introduction The Stryker OrthoMap Express Knee Navigation System is providing surgeons with
unicompartmental knee SURGICAL TECHNIQUE limacorporate.com
 unicompartmental knee SURGICAL TECHNIQUE limacorporate.com Index INTRAMEDULLARY (IM) SURGICAL PROCEDURE Introduction Page >> 04 Rationale Page >> 05 Preoperative Planning Page >> 07 Patient Preparation
unicompartmental knee SURGICAL TECHNIQUE limacorporate.com Index INTRAMEDULLARY (IM) SURGICAL PROCEDURE Introduction Page >> 04 Rationale Page >> 05 Preoperative Planning Page >> 07 Patient Preparation
14 mm x +30 mm Stem Extension
 14 mm x +30 mm Stem Extension Persona The Personalized Knee Surgical Technique Table of Contents Introduction...2 Preoperative Planning Surgical Approach Patient Preparation Magnet Usage Symbols Screw/Pin
14 mm x +30 mm Stem Extension Persona The Personalized Knee Surgical Technique Table of Contents Introduction...2 Preoperative Planning Surgical Approach Patient Preparation Magnet Usage Symbols Screw/Pin
Triathlon Knee System. Anterior Referencing Surgical Protocol
 Triathlon Knee System Anterior Referencing Surgical Protocol Triathlon Knee System Anterior Referencing Surgical Protocol Table of Contents Acknowledgments..........................................................2
Triathlon Knee System Anterior Referencing Surgical Protocol Triathlon Knee System Anterior Referencing Surgical Protocol Table of Contents Acknowledgments..........................................................2
FLK167 02/08. Biomet UK Ltd Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom. Tel Fax:
 FLK167 02/08 Biomet UK Ltd Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom Tel. 01656 655221 Fax: 01656 645454 Premier Instrumentation CR or PS Surgical Technique Vanguard Premier
FLK167 02/08 Biomet UK Ltd Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom Tel. 01656 655221 Fax: 01656 645454 Premier Instrumentation CR or PS Surgical Technique Vanguard Premier
KneeAlign System Surgical Technique Guide
 KneeAlign System Surgical Technique Guide Table of Contents Step 1 System Assembly... 1 Step 2 System Assembly... 2 Step 3 System Assembly... 2 Step 4 System Assembly... 2 Step 5 Sensor Pairing... 2 Step
KneeAlign System Surgical Technique Guide Table of Contents Step 1 System Assembly... 1 Step 2 System Assembly... 2 Step 3 System Assembly... 2 Step 4 System Assembly... 2 Step 5 Sensor Pairing... 2 Step
Premier Total Knee Instrumentation
 Premier Total Knee Instrumentation Vanguard Complete Knee System Surgical Technique Table of Contents Indications and Contraindications... 3 Introduction... 4 Patient Selection Preoperative Planning Approaches...
Premier Total Knee Instrumentation Vanguard Complete Knee System Surgical Technique Table of Contents Indications and Contraindications... 3 Introduction... 4 Patient Selection Preoperative Planning Approaches...
Aesculap Orthopaedics Columbus MIOS
 Aesculap Orthopaedics Columbus MIOS Minimally Invasive Orthopaedic Solutions Manual TKA Surgical Technique MIOS 4-in-1 Cutting Block MIOS Distal Femoral Cutting Block MIOS Tibial Left and Right Cutting
Aesculap Orthopaedics Columbus MIOS Minimally Invasive Orthopaedic Solutions Manual TKA Surgical Technique MIOS 4-in-1 Cutting Block MIOS Distal Femoral Cutting Block MIOS Tibial Left and Right Cutting
Mako Partial Knee Medial bicompartmental
 Mako Partial Knee Medial bicompartmental Surgical reference guide Mako Robotic-Arm Assisted Surgery Table of contents Implant compatibility.... 3 Pre-operative planning.... 4 Intra-operative planning....
Mako Partial Knee Medial bicompartmental Surgical reference guide Mako Robotic-Arm Assisted Surgery Table of contents Implant compatibility.... 3 Pre-operative planning.... 4 Intra-operative planning....
Unicondylar Surgical Technique
 Unicondylar Surgical Technique Contents Indications, Contra-indications and X-ray Templating 2 Approach and Exposure 3 Proximal Tibial Resection 4 Tibial Jig Alignment 6 Tibial Sizing 9 Balancing 10 Distal
Unicondylar Surgical Technique Contents Indications, Contra-indications and X-ray Templating 2 Approach and Exposure 3 Proximal Tibial Resection 4 Tibial Jig Alignment 6 Tibial Sizing 9 Balancing 10 Distal
Zimmer NexGen RH Knee Primary/Revision. Surgical Technique
 Zimmer NexGen Primary/Revision Surgical Technique Zimmer NexGen Primary/Revision Surgical Technique INTRO Introduction The NexGen Rotating Hinge Knee () is designed for revision, difficult primary, and
Zimmer NexGen Primary/Revision Surgical Technique Zimmer NexGen Primary/Revision Surgical Technique INTRO Introduction The NexGen Rotating Hinge Knee () is designed for revision, difficult primary, and
Profix. Total Knee System. As described by
 Profix Total Knee System P R I M A R Y P R O C E D U R E As described by Leo A. Whiteside, M.D. Associate Research Professor Washington University School of Medicine Director, Biomechanical Research Laboratory
Profix Total Knee System P R I M A R Y P R O C E D U R E As described by Leo A. Whiteside, M.D. Associate Research Professor Washington University School of Medicine Director, Biomechanical Research Laboratory
NexGen CR-Flex Fixed Bearing Knee. Surgical Technique
 NexGen CR-Flex Fixed Bearing Knee Surgical Technique Table of Contents Introduction...2 Preoperative Conditioning... 3 Preoperative Planning... 3 Surgical Technique...4 Incision and Exposure... 4 Femoral
NexGen CR-Flex Fixed Bearing Knee Surgical Technique Table of Contents Introduction...2 Preoperative Conditioning... 3 Preoperative Planning... 3 Surgical Technique...4 Incision and Exposure... 4 Femoral
Mako. Total Knee with Triathlon. Surgical protocol
 Mako Total Knee with Triathlon Surgical protocol Mako Total Knee with Triathlon Surgical protocol Contents Introduction.... 4 Femoral.... 9 Femoral trial assessment... 14 Final tibial and trialing...
Mako Total Knee with Triathlon Surgical protocol Mako Total Knee with Triathlon Surgical protocol Contents Introduction.... 4 Femoral.... 9 Femoral trial assessment... 14 Final tibial and trialing...
U2 PSA. Revision Knee. Surgical Protocol
 U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
RESECTION GUIDE SYSTEM. TRUMATCH Personalized Solutions Surgical Technique with ATTUNE Knee INTUITION Instruments
 RESECTION GUIDE SYSTEM TRUMATCH Personalized Solutions Surgical Technique with ATTUNE Knee INTUITION Instruments RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the ATTUNE Knee
RESECTION GUIDE SYSTEM TRUMATCH Personalized Solutions Surgical Technique with ATTUNE Knee INTUITION Instruments RESECTION GUIDE SURGICAL TECHNIQUE The following steps are an addendum to the ATTUNE Knee
OPERATIVE TECHNIQUE SKS Total Knee Replacement
 OPERATIVE TECHNIQUE SKS Total Knee Replacement Femoral preparation A40577 1 2 5 1: Alignment rod A30049 + A30124 2: Centromedullary rod A40224 4: T-handle A40232 6: Femoral measuring device A40411 + A40414
OPERATIVE TECHNIQUE SKS Total Knee Replacement Femoral preparation A40577 1 2 5 1: Alignment rod A30049 + A30124 2: Centromedullary rod A40224 4: T-handle A40232 6: Femoral measuring device A40411 + A40414
Pin Guide System. Surgical Technique
 Pin Guide System Surgical Technique Pin Guide Surgical Technique The following steps are an addendum to the SIGMA High Performance (HP) Instruments, Fixed Reference Surgical Technique (Cat. No. 0612-87-510
Pin Guide System Surgical Technique Pin Guide Surgical Technique The following steps are an addendum to the SIGMA High Performance (HP) Instruments, Fixed Reference Surgical Technique (Cat. No. 0612-87-510
DePuy Orthopaedics, Inc. 700 Orthopaedic Drive Warsaw, IN USA Tel: +1 (800)
 DePuy Orthopaedics, Inc. 700 Orthopaedic Drive Warsaw, IN 46581-0988 USA Tel: +1 (800) 366 8143 0086 Printed in USA. DePuy Synthes Companies 2013 All rights reserved. 0612-09-512 Rev 1 5M 0513 Surgical
DePuy Orthopaedics, Inc. 700 Orthopaedic Drive Warsaw, IN 46581-0988 USA Tel: +1 (800) 366 8143 0086 Printed in USA. DePuy Synthes Companies 2013 All rights reserved. 0612-09-512 Rev 1 5M 0513 Surgical
SIGMA High Performance Partial Knee. Unicondylar. Surgical Technique
 SIGMA High Performance Partial Knee Unicondylar Surgical Technique Table of Contents Surgical Technique X-ray Templating 3 Approach and Exposure 4 Proximal Tibial Resection 5 Tibial Jig Alignment 7 Tibial
SIGMA High Performance Partial Knee Unicondylar Surgical Technique Table of Contents Surgical Technique X-ray Templating 3 Approach and Exposure 4 Proximal Tibial Resection 5 Tibial Jig Alignment 7 Tibial
Anterior Cut First Surgical Technique
 Anterior Cut First Surgical Technique GENESIS II Anterior Cut First Surgical Technique Table of Contents Introduction....................................... 2 Preop Planning....................................
Anterior Cut First Surgical Technique GENESIS II Anterior Cut First Surgical Technique Table of Contents Introduction....................................... 2 Preop Planning....................................
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer
 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
Resurfacing Distal Femur. Orthopaedic Salvage System
 Resurfacing Distal Femur Orthopaedic Salvage System Primary Arthroplasty OSS 3cm Resurfacing Distal Femur Distal Femoral Resection Drill and ream the distal femur in the following sequence: (Figure 1)
Resurfacing Distal Femur Orthopaedic Salvage System Primary Arthroplasty OSS 3cm Resurfacing Distal Femur Distal Femoral Resection Drill and ream the distal femur in the following sequence: (Figure 1)
Minimally Invasive Surgical Techniques for the Medial Compartment. Intramedullary, Spacer Block and Extramedullary techniques
 Minimally Invasive Surgical Techniques for the Medial Compartment Intramedullary, Spacer Block and Extramedullary techniques Unicompartmental High Flex Knee Intramedullary, Spacer Block and Extramedullary
Minimally Invasive Surgical Techniques for the Medial Compartment Intramedullary, Spacer Block and Extramedullary techniques Unicompartmental High Flex Knee Intramedullary, Spacer Block and Extramedullary
ZIMMER NEXGEN CRUCIATE RETAINING (CR) AND LEGACY KNEE POSTERIOR STABILIZED (LPS) TRABECULAR METAL MONOBLOCK TIBIAS. Surgical Technique Addendum
 ZIMMER NEXGEN CRUCIATE RETAINING (CR) AND LEGACY KNEE POSTERIOR STABILIZED (LPS) TRABECULAR METAL MONOBLOCK TIBIAS Surgical Technique Addendum SURGICAL TECHNIQUE FOR NEXGEN CRUCIATE RETAINING (CR) AND
ZIMMER NEXGEN CRUCIATE RETAINING (CR) AND LEGACY KNEE POSTERIOR STABILIZED (LPS) TRABECULAR METAL MONOBLOCK TIBIAS Surgical Technique Addendum SURGICAL TECHNIQUE FOR NEXGEN CRUCIATE RETAINING (CR) AND
Single Axis Revision Knee System
 Orthopaedics Scorpio TS Single Axis Revision Knee System Scorpio TS Trial Cutting Guide Surgical Protocol Orthopaedics Scorpio TS Single Axis Revision Knee System Scorpio TS Trial Cutting Guide Surgical
Orthopaedics Scorpio TS Single Axis Revision Knee System Scorpio TS Trial Cutting Guide Surgical Protocol Orthopaedics Scorpio TS Single Axis Revision Knee System Scorpio TS Trial Cutting Guide Surgical
ClassiQ. Scorpio. Anterior Referencing Surgical Protocol. Anterior Referencing. For use with Scorpio ClassiQ Instrument System
 Scorpio ClassiQ Anterior Referencing Surgical Protocol For use with Scorpio ClassiQ Instrument System For use with Scorpio ClassiQ Single Radius Total Knee System AR Anterior Referencing This document
Scorpio ClassiQ Anterior Referencing Surgical Protocol For use with Scorpio ClassiQ Instrument System For use with Scorpio ClassiQ Single Radius Total Knee System AR Anterior Referencing This document
Zimmer MIS Intramedullary Instrumentation
 Zimmer MIS Intramedullary Instrumentation Surgical Technique For NexGen Cruciate Retaining & NexGen Legacy Posterior Stabilized Knees Zimmer MIS Intramedullary Instrumentation Surgical Technique Surgical
Zimmer MIS Intramedullary Instrumentation Surgical Technique For NexGen Cruciate Retaining & NexGen Legacy Posterior Stabilized Knees Zimmer MIS Intramedullary Instrumentation Surgical Technique Surgical
NexGen CR-Flex Mobile Bearing Knee. Surgical Technique
 NexGen CR-Flex Mobile Bearing Knee Surgical Technique Table of Contents Introduction...2 Cruciate Retaining...2 Cruciate Sacrificing...3 MIS Multi-Reference 4-in-1 Instruments...3 Patient Selection...4
NexGen CR-Flex Mobile Bearing Knee Surgical Technique Table of Contents Introduction...2 Cruciate Retaining...2 Cruciate Sacrificing...3 MIS Multi-Reference 4-in-1 Instruments...3 Patient Selection...4
Triathlon with Single-Use Instrumentation Optimize Your TKA Experience. Posterior Referencing Surgical Protocol
 Triathlon with Single-Use Instrumentation Optimize Your TKA Experience Posterior Referencing Surgical Protocol Introduction............................................................2 Assembly Instructions...................................................6
Triathlon with Single-Use Instrumentation Optimize Your TKA Experience Posterior Referencing Surgical Protocol Introduction............................................................2 Assembly Instructions...................................................6
Vanguard ID Total Knee. Surgical Technique
 Vanguard ID Total Knee Surgical Technique Table of Contents Overview... 2 Preoperative Planning... 4 Incision... 4 Patella Preparation... 5 Patella Resection Femoral Preparation... 8 Distal Femoral Resection
Vanguard ID Total Knee Surgical Technique Table of Contents Overview... 2 Preoperative Planning... 4 Incision... 4 Patella Preparation... 5 Patella Resection Femoral Preparation... 8 Distal Femoral Resection
NexGen Intramedullary Instrumentation. Surgical Technique
 NexGen Intramedullary Instrumentation Surgical Technique Table of Contents Introduction... 2 Preoperative Planning... 2 Surgical Technique... 3 Step One: Size the Femur/Establish External Rotation...
NexGen Intramedullary Instrumentation Surgical Technique Table of Contents Introduction... 2 Preoperative Planning... 2 Surgical Technique... 3 Step One: Size the Femur/Establish External Rotation...
Microplasty Elite Total Knee Instrumentation
 Microplasty Elite Total Knee Instrumentation Vanguard Complete Knee System Surgical Technique Table of Contents Indications and Contraindications... 3 Introduction... 4 Patient Selection Preoperative
Microplasty Elite Total Knee Instrumentation Vanguard Complete Knee System Surgical Technique Table of Contents Indications and Contraindications... 3 Introduction... 4 Patient Selection Preoperative
TOTAL KNEE ARTHROPLASTY (TKA)
 TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
TOTAL KNEE ARTHROPLASTY (TKA) 1 Anatomy, Biomechanics, and Design 2 Femur Medial and lateral condyles Convex, asymmetric Medial larger than lateral 3 Tibia Tibial plateau Medial tibial condyle: concave
KneeAlign 2 System. Surgical Technique Manual Tibia and Distal Femur Navigation. About OrthAlign, Inc.
 About OrthAlign, Inc. KneeAlign 2 System Surgical Technique Manual and Distal Femur Navigation OrthAlign is committed to providing surgeons with user-friendly, cost-effective, surgical navigation products
About OrthAlign, Inc. KneeAlign 2 System Surgical Technique Manual and Distal Femur Navigation OrthAlign is committed to providing surgeons with user-friendly, cost-effective, surgical navigation products
Triathlon Tritanium. Surgical Protocol. with Triathlon Cementless Beaded PA Femoral Component
 Triathlon Tritanium Surgical Protocol with Triathlon Cementless Beaded PA Femoral Component Triathlon Tritanium Surgical Protocol with Triathlon Cementless Beaded PA Femoral Component Description...............................
Triathlon Tritanium Surgical Protocol with Triathlon Cementless Beaded PA Femoral Component Triathlon Tritanium Surgical Protocol with Triathlon Cementless Beaded PA Femoral Component Description...............................
Abramsohn Retractor 1
 Abramsohn Retractor 1 Calibrated Femoral Tibial Spreaders Small Medium Large Designed to remain in position, with the femur and tibia separated, without the need of an assistant, and to minimize crushing
Abramsohn Retractor 1 Calibrated Femoral Tibial Spreaders Small Medium Large Designed to remain in position, with the femur and tibia separated, without the need of an assistant, and to minimize crushing
Zimmer NexGen Rotating Hinge Knee Primary/ Revision
 Zimmer NexGen Rotating Hinge Knee Primary/ Revision Surgical Technique Designed for use in revision and difficult primary surgeries 1 INTRODUCTION The NexGen Rotating Hinge Knee Components are designed
Zimmer NexGen Rotating Hinge Knee Primary/ Revision Surgical Technique Designed for use in revision and difficult primary surgeries 1 INTRODUCTION The NexGen Rotating Hinge Knee Components are designed
G K SPHERE. Surgical Technique STABILITY FOR LIFE. Hip Knee Spine Navigation
 G K SPHERE M E D I A L L Y S T A B I L I Z E D K N E E STABILITY FOR LIFE Surgical Technique Hip Knee Spine Navigation GMK SPHERE Surgical Technique Hip Knee Spine Navigation INTRODUCTION This brochure
G K SPHERE M E D I A L L Y S T A B I L I Z E D K N E E STABILITY FOR LIFE Surgical Technique Hip Knee Spine Navigation GMK SPHERE Surgical Technique Hip Knee Spine Navigation INTRODUCTION This brochure
FOREWORD PRESERVATION UNICOMPARTMENTAL KNEE SYSTEM
 Surgical Technique FOREWORD PRESERVATION UNICOMPARTMENTAL KNEE SYSTEM Our surgeon design team first implanted the Preservation Unicompartmental Knee System in 2001. The system was developed with over
Surgical Technique FOREWORD PRESERVATION UNICOMPARTMENTAL KNEE SYSTEM Our surgeon design team first implanted the Preservation Unicompartmental Knee System in 2001. The system was developed with over
The ACL-PCL Substituting Knee. BioFoam Tibial Bases. Surgical Technique For Cementless Tibial Fixation
 The CL-PCL Substituting Knee BioFoam Surgical Technique For Cementless Tibial Fixation Surgical techniques and instrument recommendations were provided by: Michael nderson, MD Milwaukee, WI G. Lynn Rasmussen,
The CL-PCL Substituting Knee BioFoam Surgical Technique For Cementless Tibial Fixation Surgical techniques and instrument recommendations were provided by: Michael nderson, MD Milwaukee, WI G. Lynn Rasmussen,
NEXGEN COMPLETE KNEE SOLUTION. Revision Instrumentation Surgical Technique For Legacy Knee Constrained Condylar Knee
 NEXGEN COMPLETE KNEE SOLUTION Revision Instrumentation Surgical Technique For Legacy Knee Constrained Condylar Knee INTRODUCTION Revision total knee arthroplasty can be a very challenging task for any
NEXGEN COMPLETE KNEE SOLUTION Revision Instrumentation Surgical Technique For Legacy Knee Constrained Condylar Knee INTRODUCTION Revision total knee arthroplasty can be a very challenging task for any
Zimmer NexGen LPS-Flex Mobile and LPS-Mobile Bearing Knees. Surgical Technique United States Version IMAGE TO COME
 Zimmer NexGen LPS-Flex Mobile and LPS-Mobile Bearing Knees Surgical Technique United States Version IMAGE TO COME Zimmer NexGen LPS-Flex Mobile and LPS-Mobile Bearing Knees Surgical Technique 1 Zimmer
Zimmer NexGen LPS-Flex Mobile and LPS-Mobile Bearing Knees Surgical Technique United States Version IMAGE TO COME Zimmer NexGen LPS-Flex Mobile and LPS-Mobile Bearing Knees Surgical Technique 1 Zimmer
NexGen LPS Fixed Bearing Knee. Surgical Technique
 NexGen LPS Fixed Bearing Knee Surgical Technique Table of Contents Introduction...2 Preoperative Planning...2 Surgical Technique...3 Step One: Align the Tibia...3 MICRO-MILL Hand Piece Assembly and Usage
NexGen LPS Fixed Bearing Knee Surgical Technique Table of Contents Introduction...2 Preoperative Planning...2 Surgical Technique...3 Step One: Align the Tibia...3 MICRO-MILL Hand Piece Assembly and Usage
STABILITY FOR LIFE. Surgical Technique
 STABILITY FOR LIFE Surgical Technique Joint Spine Sports Med GMK Sphere Surgical Technique 2 INDEX 1. INTRODUCTION 4 1.1 Indications 4 1.2 Contraindications 4 1.3 Preoperative planning 5 1.4 Surgical approach
STABILITY FOR LIFE Surgical Technique Joint Spine Sports Med GMK Sphere Surgical Technique 2 INDEX 1. INTRODUCTION 4 1.1 Indications 4 1.2 Contraindications 4 1.3 Preoperative planning 5 1.4 Surgical approach
Jan Victor, MD Orthopaedic Department AZ Sint-Lucas Brugge, Belgium
 Surgical Technique Contributing surgeons: Johan Bellemans, MD, PhD Head of Orthopaedic Department University Hospital Pellenberg Pellenberg, Belgium Jonathan Garino, MD University of Pennsylvania Philadelphia,
Surgical Technique Contributing surgeons: Johan Bellemans, MD, PhD Head of Orthopaedic Department University Hospital Pellenberg Pellenberg, Belgium Jonathan Garino, MD University of Pennsylvania Philadelphia,
Stephen R Smith Northeast Nebraska Orthopaedics PC. Ligament Preserving Techniques in Total Knee Arthroplasty
 Stephen R Smith Northeast Nebraska Orthopaedics PC Ligament Preserving Techniques in Total Knee Arthroplasty 10-15% have Fair to poor Results? Why? The complication rate is 2.567% If It happens To You
Stephen R Smith Northeast Nebraska Orthopaedics PC Ligament Preserving Techniques in Total Knee Arthroplasty 10-15% have Fair to poor Results? Why? The complication rate is 2.567% If It happens To You
ANATOMIC. Navigated Surgical Technique 4 in 1 TO.G.GB.016/1.0
 ANATOMIC Navigated Surgical Technique 4 in 1 TO.G.GB.016/1.0 SCREEN LAYOUT Take screenshot Surgical step Dynamic navigation zone Information area and buttons 2 SCREEN LAYOUT Indicates action when yellow
ANATOMIC Navigated Surgical Technique 4 in 1 TO.G.GB.016/1.0 SCREEN LAYOUT Take screenshot Surgical step Dynamic navigation zone Information area and buttons 2 SCREEN LAYOUT Indicates action when yellow
PPS P I N P O S I T I O N I N G S Y S T E M GMK EFFICIENCY VERSION. Hip Knee Spine Navigation
 PPS P I N P O S I T I O N I N G S Y S T E M D ESIGNED FOR YOU BY YOU GMK EFFICIENCY VERSION Surgical Surgical Technique Hip Knee Spine Navigation MyKnee Surgical Technique Hip Knee Spine Navigation I N
PPS P I N P O S I T I O N I N G S Y S T E M D ESIGNED FOR YOU BY YOU GMK EFFICIENCY VERSION Surgical Surgical Technique Hip Knee Spine Navigation MyKnee Surgical Technique Hip Knee Spine Navigation I N
NEXGEN COMPLETE KNEE SOLUTION S A. Tibial Stem Extension & Augmentation Surgical. ATechnique
 NEXGEN COMPLETE KNEE SOLUTION ATechnique Tibial Stem Extension & Augmentation Surgical INTRODUCTION The NexGen Complete Knee Solution Intramedullary Tibial Instruments have been designed to provide an
NEXGEN COMPLETE KNEE SOLUTION ATechnique Tibial Stem Extension & Augmentation Surgical INTRODUCTION The NexGen Complete Knee Solution Intramedullary Tibial Instruments have been designed to provide an
Zimmer PSI Knee System For Use with Persona The Personalized Knee System Surgical Technique
 Zimmer PSI Knee System For Use with Persona The Personalized Knee System Surgical Technique TOC Zimmer PSI Knee Surgical Technique Zimmer PSI Knee Surgical Technique Table of Contents Intra-Operative Guide
Zimmer PSI Knee System For Use with Persona The Personalized Knee System Surgical Technique TOC Zimmer PSI Knee Surgical Technique Zimmer PSI Knee Surgical Technique Table of Contents Intra-Operative Guide
Zimmer NexGen Tibial Stem Extension & Augmentation. Surgical Technique IMAGE TO COME. Stem Extensions and Augments
 Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique IMAGE TO COME Stem Extensions and Augments Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique 1 Zimmer NexGen Tibial
Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique IMAGE TO COME Stem Extensions and Augments Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique 1 Zimmer NexGen Tibial
