Trends in Surgical Practices for Lateral Epicondylitis Among Newly Trained Orthopaedic Surgeons
|
|
|
- Mary Reed
- 6 years ago
- Views:
Transcription
1 Trends in Surgical Practices for Lateral Epicondylitis Among Newly Trained Orthopaedic Surgeons Original Research Dean Wang,* MD, Ryan M. Degen, MD, MSc, FRCSC, Christopher L. Camp, MD, Michael H. McGraw, MD, David W. Altchek, MD, and Joshua S. Dines, MD Investigation performed at the Hospital for Special Surgery, New York, New York, USA Background: Much controversy exists regarding the optimal surgical intervention for lateral epicondylitis because of a multitude of options available and the lack of comparative studies. Knowledge of the current practice trends would help guide the design of comparative studies needed to determine which surgical technique results in the best outcome. Purpose: To review the latest practice trends for the surgical treatment of lateral epicondylitis among newly trained surgeons in the United States utilizing the American Board of Orthopaedic Surgery (ABOS) database. Study Design: Cross-sectional study; Level of evidence, 3. Methods: The ABOS database was utilized to identify surgical cases for lateral epicondylitis submitted by Part II board certification examination candidates from 2004 through Inclusion criteria were predetermined using a combination of International Classification of Diseases, Ninth Revision (ICD-9) and Current Procedural Terminology (CPT) codes. Cases were organized by open and arthroscopic treatment groups and by fellowship training and were analyzed to determine differences in surgical techniques, complication rates, and concomitant procedures. Results: In total, 1150 surgeons submitted 2106 surgical cases for the treatment of lateral epicondylitis. The number of surgical cases for lateral epicondylitis performed per 10,000 submitted cases significantly decreased from 26.7 in 2004 to 21.1 in 2013 (P ¼.002). Among all cases, 92.2% were open and 7.8% were arthroscopic, with no change in the incidence of arthroscopic surgeries over the study period. Shoulder and elbow (18.1%) and sports medicine (11.4%) surgeons were more likely to perform surgery arthroscopically compared with hand surgeons (6.1%) (P <.001). There was no difference in overall self-reported complication rates between open (4.4%) and arthroscopic (5.5%) procedures (P ¼.666). Percutaneous tenotomy, debridement only, and debridement with tendon repair comprised 6.4%, 46.3%, and 47.3% of open treatment, respectively. Sports medicine, hand, and shoulder and elbow surgeons were more likely to repair the tendon after debridement compared with other surgeons, who were more likely to perform debridement alone (P <.001). Hand surgeons were most likely to perform concomitant procedures, of which the majority were neuroplasties. Conclusion: Although comparative studies are ultimately necessary for determining the optimal surgical technique, researchers should be mindful of the differences in practices according to training and the extent to which concomitant procedures are being performed, as both these factors may confound any future results. Keywords: lateral epicondylitis; tennis elbow; ECRB; enthesopathy; arthroscopic surgery *Address correspondence to Dean Wang, MD, Sports Medicine and Shoulder Service, Hospital for Special Surgery, 535 East 70th Street, New York, NY 10021, USA ( deanwangmd@gmail.com). Sports Medicine and Shoulder Service, Hospital for Special Surgery, New York, New York, USA. The authors declared that they have no conflicts of interest in the authorship and publication of this contribution. Ethical approval for this study was obtained from the American Board of Orthopaedic Surgery. The Orthopaedic Journal of Sports Medicine, 5(10), DOI: / ª The Author(s) 2017 Lateral epicondylitis, often referred to as tennis elbow, is a common condition thought to be related to overuse injuries to the extensor carpi radialis brevis (ECRB). The natural history of lateral epicondylitis typically involves the resolution of symptoms in 6 to 24 months, with most patients experiencing an improvement in symptoms within 1 year. 3,11 Despite this phenomenon, it is estimated that 4% to 11% of patients fail nonoperative treatment and still undergo surgery. 8 This may be related to the wide spectrum of tendinopathies in which mild forms (ie, loosening of the array of collagen fibers) may benefit from nonoperative measures, while more severe forms (ie, macroscopic tearing This open-access article is published and distributed under the Creative Commons Attribution - NonCommercial - No Derivatives License ( licenses/by-nc-nd/3.0/), which permits the noncommercial use, distribution, and reproduction of the article in any medium, provided the original author and source are credited. You may not alter, transform, or build upon this article without the permission of the Author(s). For reprints and permission queries, please visit SAGE s website at 1
2 2 Wang et al The Orthopaedic Journal of Sports Medicine of the tendon-to-bone enthesis) may be more likely to fail nonoperative treatment. 2 Much controversy exists regarding the optimal surgical intervention because of the many options available and the lack of comparative studies. Nirschl and Pettrone 17 first described success with surgical excision of the diseased ECRB with good long-term results. 6 Over the past decade, alternative surgical techniques have been posited to further improve upon clinical outcomes. Studies on arthroscopic and percutaneous techniques have reported a quicker recovery and return-to-work time, 5,10,18,21,22 which are notable given that lateral epicondylitis is highly prevalent among manual laborers. Additionally, many have proposed that a main advantage of arthroscopic treatment is the ability to address other intra-articular abnormalities. Improved grip and pinch strength has been described with anatomic suture anchor repair of the tendon back to the lateral epicondyle. 13,23 The extent to which these newer techniques have been adopted by surgeons, particularly newly practicing surgeons, is unknown. Given the multitude of options and the lack of consensus on the optimal surgical technique for lateral epicondylitis, knowledge of the current practice trends (and their contributing factors) would help guide the design of comparative studies needed to determine which procedure results in the best outcome. Therefore, the purpose of this study was to review the latest practice trends for the surgical treatment of lateral epicondylitis among newly trained surgeons in the United States utilizing the American Board of Orthopaedic Surgery (ABOS) database. We hypothesized that arthroscopic treatment would be increasingly performed by newly trained surgeons, given the recent evidence suggesting that it leads to good outcomes and an earlier return to work for patients. Additionally, in this population of newly practicing surgeons, we sought to determine any differences in practice according to fellowship training as well as any difference in complication rates between open and arthroscopic techniques. METHODS Data Collection A research proposal was submitted and approved by the ABOS to query the database for lateral epicondylitis procedures submitted for review by ABOS Part II examination candidates from 2004 to This database includes all case information from candidates case collection period, which consists of all operative cases performed over a 6- month period in preparation for Part II of their orthopaedic board certification. This case collection period typically occurs during an orthopaedic surgeon s first 2 years in clinical practice. Data from the ABOS database were devoid of patient- or surgeon-identifying information. The provided data included the year of the procedure, International Classification of Diseases, Ninth Revision (ICD-9) codes, Current Procedural Terminology (CPT) codes, total number of cases submitted by the candidate, total number of cases submitted by all candidates, fellowship training (if applicable), region of practice, patient age, patient sex, and any associated surgeon-related complications. From 2004 to 2013, 6854 board-eligible orthopaedic surgeons submitted a total of 858,146 cases for the ABOS Part II examination, resulting in a mean number of cases per surgeon. For this study, cases coded as ICD (lateral epicondylitis) and at least one of the open or arthroscopic CPT codes listed in the Appendix were collected. Before 2008, CPT codes for open epicondylitis procedures consisted of 24350, 24351, 24352, 24354, and Since 2008, these were replaced by more specific CPT codes: (percutaneous), (debridement only), and (debridement with tendon repair). Among the queried cases, those with secondary CPT codes were examined to determine the rates of concomitant procedures. Statistical Analysis Bivariate comparisons of means and proportions were performed using the Student t test and chi-square test, respectively. Comparisons of means and proportions among fellowship training were performed using 1-way analysis of variance and the chi-square test, respectively, with post hoc Bonferroni correction for multiple comparisons. To determine the significance of trends over time, a line of best fit was generated for the graphed data to illustrate the change over the years. The slope of this best-fit line was compared with a line with a slope of zero (no change over time) using chi-square linear-by-linear association analysis. Statistical significance was set at P <.05. RESULTS After querying the database for surgical procedure codes for lateral epicondylitis, we determined that 2106 cases submitted by 1150 surgeons met the inclusion criteria. Overall, the mean patient age was 45.7 ± 8.5 years, and 921 patients (43.7%) were male. The majority of cases were performed by surgeons with hand (44.3%), sports (27.4%), and no additional (15.7%) fellowship training. On average, surgeons with hand fellowship training performed more surgical cases (2.4) per 6-month collection period compared with those having sports medicine (1.5), adult reconstruction (1.4), and no additional (1.5) fellowship training (P <.001) (Table 1). The annual incidence, defined as the number of surgical cases for lateral epicondylitis performed per 10,000 submitted cases, significantly decreased from 26.7 in 2004 to 21.1 in 2013 (P ¼.002) (Figure 1A). Since 2008 (after the implementation of more specific CPT codes), percutaneous tenotomy, debridement only, and debridement with tendon repair comprised 6.4%,46.3%,and 47.3% of nonarthroscopic cases, respectively. Surgeons with sports medicine, hand, and shoulder and elbow fellowship training were more likely to perform debridement with tendon repair compared with other surgeons, who were more likely to perform debridement alone (P <.001) (Figure 2). More than half of open cases (55.8%) performedbysports medicine surgeons consisted of tendon repair, whereas this only consisted of a third (33.9%) of open cases performed by
3 The Orthopaedic Journal of Sports Medicine Surgical Trends in Lateral Epicondylitis 3 TABLE 1 Cases Submitted per 6-Month Collection Period by Fellowship Training Fellowship Training Mean No. of Cases Adult reconstruction 1.4 a Foot and ankle 1.5 Hand 2.4 Oncology 1.5 Pediatrics 1.6 Shoulder and elbow 1.9 Spine 1.6 Sports medicine 1.5 a Trauma 1.7 None 1.5 a a P <.001 versus hand and upper extremity cases. Figure 2. Percentage of percutaneous tenotomy, debridement only, and debridement with tendon repair cases by fellowship training. Cases presented are from 2008 to 2013 after the implementation of the latest Current Procedural Terminology (CPT) codes. *P <.001comparedwithhand, shoulder and elbow, and sports medicine. P <.001compared with sports medicine and P ¼.023 compared with shoulder and elbow. TABLE 2 Comparison of Open Versus Arthroscopic Surgical Treatment of Lateral Epicondylitis a Open Arthroscopic P Figure 1. Annual incidence of (A) total and (B) open/percutaneous versus arthroscopic treatment of lateral epicondylitis. The black line represents the linear trend for the presented data. non upper extremity surgeons. The rate of complications did not differ between the 3 treatment types (P ¼.412). There were 1942 (92.2%) open/percutaneous cases and 164 (7.8%) arthroscopic cases for the treatment of lateral epicondylitis (Table 2). The mean age and sex distribution did not differ between the 2 groups. Overall, 18.1% of cases performed by shoulder and elbow surgeons and 11.4% of cases performed by sports medicine surgeons were arthroscopic. In contrast, only 6.1% of cases performed by hand surgeons and 4.9% of cases performed by surgeons without fellowship training were arthroscopic. There were no significant differences in the annual incidence of open/percutaneous and arthroscopic cases over time (P ¼.320) (Figure 1B). A total of 95 self-reported complications were documented among all cases, resulting in an overall complication Overall 1942 (92.2) 164 (7.8) Mean age, y Sex.536 Male 845 (43.5) 76 (46.3) Female 1097 (56.5) 88 (53.7) Surgeon fellowship training <.001 Adult reconstruction 65 (89.0) 8 (11.0) Foot and ankle 27 (100.0) 0 (0.0) Hand 915 (93.9) 59 (6.1) Oncology 3 (100.0) 0 (0.0) Pediatric 10 (90.9) 1 (9.1) Shoulder and elbow 86 (81.9) 19 (18.1) <.001 b Spine 18 (100.0) 0 (0.0) Sports medicine 534 (88.6) 69 (11.4) <.001 b Trauma 37 (94.9) 2 (5.1) No fellowship 329 (95.1) 17 (4.9) a Data are presented as n (%) unless otherwise indicated. b Compared with hand. rate of 4.5% (Table 3). There was no significant difference in the rate of complications between open (4.4%) and arthroscopic (5.5%) procedures (P ¼.666). Similarly, there was no significant difference in the rate of complications when comparing surgeon fellowship training (P ¼.519). Concomitant procedures were seldom performed for both open and arthroscopic treatments of lateral epicondylitis (Table 4). Among open cases, cubital tunnel release (3.3%), neuroplasty (excluding ulnar) of the arm (3.2%), and
4 4 Wang et al The Orthopaedic Journal of Sports Medicine TABLE 3 Self-Reported Complication Rates Associated With Surgical Treatment of Lateral Epicondylitis Complication Open, % Arthroscopic, % Infection 0.93 Surgical, unspecified Nerve palsy or injury Wound healing delay or dehiscence 0.51 Medical, unspecified Skin ulcer or blister 0.41 Hemorrhage 0.21 Anesthetic complication Stiffness or arthrofibrosis 0.15 Hematoma or seroma 0.10 Surgical procedure intervention 0.10 Deep venous thrombosis 0.05 Dermatological complaint 0.05 Failure of tendon or ligament repair 0.05 Fall 0.05 Pain, uncontrolled Tendon or ligament injury 0.05 Total TABLE 4 Concomitant Procedures With Surgical Treatment of Lateral Epicondylitis a Concomitant Procedure Open, n(%) Arthroscopic, n(%) Performed by Fellowship Training, % Hand Sports Medicine Neuroplasty (excluding 62 (3.2) 1 (0.6) ulnar), arm Radial tunnel 36 (1.9) 1 (0.6) release b Cubital tunnel release 64 (3.3) 6 (3.7) Carpal tunnel release 63 (3.2) 3 (1.8) LCL repair or 13 (0.7) 1 (0.6) reconstruction Arthrotomy, elbow, 13 (0.7) 1 (0.6) with synovectomy Arthroscopic NA 22 (13.4) synovectomy Arthroscopic removal of loose bodies NA 7 (4.3) 42.9 c 85.7 c a LCL, lateral collateral ligament; NA, not applicable. b Cases of neuroplasty (excluding ulnar), arm coded with International Classification of Diseases, Ninth Revision (ICD-9) code (radial nerve syndrome). c Sum of percentages is >100 because of 1 surgeon with both hand and sports medicine fellowship training. carpal tunnel release were the most common concomitant procedures, and the majority of these were performed by surgeons with hand fellowship training. Specifically, 86.5% of concomitant radial tunnel releases were performed by surgeons with hand fellowship training. Arthroscopic synovectomy (13.4%) and removal of loose bodies (4.3%) were the most common concomitant procedures among arthroscopic cases. DISCUSSION The results of this study demonstrate a declining incidence of surgical procedures for lateral epicondylitis in recent years, with no change in the incidence of arthroscopic procedures being performed by newly trained surgeons. No significant difference in the overall complication rate was found between open and arthroscopic techniques. Substantial differences in practices were found among newly trained surgeons depending on fellowship training. Surgeons with hand fellowship training performed a higher number of surgical cases per collection period than those trained in other subspecialties and were most likely to perform concomitant procedures, of which the majority were to address compression neuropathies at the elbow and wrist. Most surgical cases were performed in an open fashion, although shoulder and elbow as well as sports medicine surgeons were most likely to perform arthroscopic surgery. Finally, sports medicine, hand, and shoulder and elbow surgeons were more likely to repair the tendon after debridement compared with other surgeons, who were more likely to perform debridement alone. The optimal management of lateral epicondylitis remains ambiguous, in part, because of the uncertainty regarding its pathological basis. Nevertheless, the natural history of lateral epicondylitis seems to indicate that it is a self-limiting condition, with 80% to 90% of patients reporting the resolution of symptoms within 1 year. 3,11 It stands to reason that symptoms persisting for longer than 1 year can still resolve without any particular treatment. In our study, the annual incidence of surgery declined over the observed decade, with an overall mean of 1.8 cases per surgeon per 6-month collection period, indicating that newly practicing surgeons are being more cautious in their approach. Additionally, this decline may be partially attributed to the popularization of platelet-rich plasma injections for the treatment of lateral epicondylitis 7,19 as well as the addition of eccentric exercises to improve physical therapy protocols. 25 Many patients, however, may be unwilling to pursue conservative modalities after a prolonged period of pain and dysfunction, and without a standardized treatment protocol for lateral epicondylitis, surgeons are not remiss in offering operative treatment with proven longterm success and a minimal risk to those who may have more severe grades of tendinopathy. 2,4,6,9 It is estimated that between 4% and 11% of patients eventually undergo surgery, 8 and our results demonstrate that newly practicing hand surgeons performed a higher rate of these surgeries than other fellowship-trained surgeons. Although it may be easy to attribute this observation to differences in the treatment culture between the hand community and others, additional factors, such as a higher clinic volume and patient demographics, may also contribute. Nevertheless, a more detailed comparison of the management strategies between newly trained hand and sports medicine
5 The Orthopaedic Journal of Sports Medicine Surgical Trends in Lateral Epicondylitis 5 surgeons, who performed the majority of surgical cases in this study, is warranted, as our results suggest vastly different philosophies between the 2 groups. The implementation of more specific CPT codes in 2008 allowed us to differentiate between 3 surgical techniques: percutaneous tenotomy, debridement only, and debridement with tendon repair. Interestingly, sports medicine, hand, and shoulder and elbow surgeons were more likely to repair the tendon compared with other surgeons, who were more likely to perform debridement alone. Although the early studies by Nirschl et al 6,14,17 described the excision of diseased tissue alone without reattachment to the lateral epicondyle, several recent studies have reported superior grip and pinch strength after suture anchor repair of the ECRB tendon to the lateral epicondyle after open debridement. 13,20,23 Surgeons specialized in hand, shoulder and elbow, and sports medicine may be more familiar with these recently published results, and thus, they may be more inclined to include suture anchor repair as part of their open treatment. Although several studies have advocated for percutaneous release, 5,10 the incidence of percutaneous treatment remained low throughout the observation period in our study. Our study suggests that percutaneous and arthroscopic techniques are not being increasingly adopted by newly trained surgeons, even as minimally invasive procedures are becoming more popular to patients in medicine overall. Arthroscopic treatment consisted of a small percentage of the total surgical cases for lateral epicondylitis, and there was high variation in the use of arthroscopic surgery among surgeons with different fellowship training. It is not surprising that shoulder and elbow as well as sports medicine surgeons were more likely to perform arthroscopic treatment, given the emphasis on arthroscopic surgery during their fellowship training. In contrast, hand surgeons typically receive less training in arthroscopic surgery during their fellowship and may be more resistant to performing arthroscopic treatment. In the past decade, there have been several studies comparing open versus arthroscopic techniques for lateral epicondylitis, with arthroscopic release demonstrating at least equivalent outcomes to open release and a more rapid return to work. 5,18,21,22 However, contrary to our hypothesis, the incidence of arthroscopic treatment did not change over the study period. Although arthroscopic treatment potentially offers the advantages of a faster return to work and less postoperative physical therapy, the disadvantages of increased operative time and technical challenges may continue to discourage surgeons from adopting this approach. A proposed advantage of arthroscopic treatment is the ability to address concomitant intra-articular abnormalities. Previous studies have reported addressing concomitant abnormalities in 18% to 58% of patients undergoing arthroscopic treatment for lateral epicondylitis, of which the vast majority of these conditions were synovitis. 1,9,12,22 This is consistent with the results of our study, in which arthroscopic synovectomy was coded in 13% of all arthroscopic cases. However, it is unclear what criteria are used to establish this diagnosis and, more importantly, to what degree the synovectomy portion of the procedure truly affects the outcome. Loose intra-articular bodies can be addressed arthroscopically, and doing so can have a significant impact on relieving mechanical symptoms. Szabo et al 22 reported a 5% incidence of loose bodies in their series, and Lattermann et al 12 reported a 3% incidence of loose bodies. Similarly, among newly trained surgeons, we found that removal of loose bodies was coded in 4% of arthroscopic cases. This indicates that concomitant abnormalities may be uncommon in the setting of lateral epicondylitis and that the proposed benefit of arthroscopic surgery for assessing and simultaneously addressing these conditions may be overstated. Interestingly, the most common concomitant procedure was neuroplasty, and a significant majority of these were performed by hand surgeons. Prior studies have shown that in patients with lateral epicondylitis, 5% have coexisting radial tunnel syndrome, while 50% of patients with radial tunnel syndrome may have concomitant lateral epicondylitis. 24 In contrast, the coexistence of cubital tunnel syndrome and carpal tunnel syndrome with lateral epicondylitis is less defined. Szabo et al 22 reported 7 posterior interosseous nerve releases and 3 carpal tunnel releases in their series of 109 patients. Dunn et al 6 reported 24 ulnar nerve releases and 1 carpal tunnel release in their series of 139 procedures. There is a subset of patients with compromised tendon durability, multiple tendinosis symptoms (rotator cuff, medial and lateral tennis elbow), and compression neuropathies (carpal tunnel syndrome, cubital tunnel syndrome) whose clinical presentations Nirschl et al 15,16 termed as mesenchymal syndrome. According to the results of the present study, hand surgeons seemed to be more cognizant of these compression neuropathies and were more inclined to treat them. Whether the ultimate outcomes are affected by these concomitant neuroplasties is unknown. There are several limitations to this study. As with any retrospective review of a national database, the results may be subject to errors in coding and data logging and are limited by the nonspecific description of certain codes. For instance, among the CPT codes for neuroplasties at the elbow, only one is specific to a single nerve (64718, neuroplasty and/or transposition of the ulnar nerve). Additionally, arthroscopic procedure codes specific to the treatment of lateral epicondylitis do not exist. This likely resulted in the underestimation of arthroscopic cases. Because the database is used for administrative and board certification purposes, detailed clinical patient information was not available, making it difficult to ascertain the homogeneity of the populations or the indications for concomitant procedures. The complications provided were often nonspecific and rare, preventing a more meaningful interpretation or conclusions. Furthermore, the follow-up for patients may have ranged from as short as 9 to 15 months because of the structure of the case collection period for the Part II examination. This may have substantially underreported the number of complications. In conclusion, the incidence of surgical procedures for lateral epicondylitis has declined in recent years, with no change in the incidence of arthroscopic procedures being performed among newly trained orthopaedic surgeons.
6 6 Wang et al The Orthopaedic Journal of Sports Medicine Although comparative studies are ultimately necessary for determining the optimal surgical technique, researchers should be mindful of the differences in practices according to training and the extent to which concomitant procedures are being performed, as both these factors may confound any future results. REFERENCES 1. Baker CL Jr, Baker CL 3rd. Long-term follow-up of arthroscopic treatment of lateral epicondylitis. Am J Sports Med. 2008;36(2): Bhabra G, Wang A, Ebert JR, Edwards P, Zheng M, Zheng MH. Lateral elbow tendinopathy: development of a pathophysiology-based treatment algorithm. Orthop J Sports Med. 2016;4(11): Binder AI, Hazleman BL. Lateral humeral epicondylitis: a study of natural history and the effect of conservative therapy. Br J Rheumatol. 1983;22(2): Calfee RP, Patel A, DaSilva MF, Akelman E. Management of lateral epicondylitis: current concepts. J Am Acad Orthop Surg. 2008;16(1): Dunkow PD, Jatti M, Muddu BN. A comparison of open and percutaneous techniques in the surgical treatment of tennis elbow. J Bone Joint Surg Br. 2004;86(5): Dunn JH, Kim JJ, Davis L, Nirschl RP. Ten- to 14-year follow-up of the Nirschl surgical technique for lateral epicondylitis. Am J Sports Med. 2008;36(2): Gosens T, Peerbooms JC, van Laar W, den Oudsten BL. Ongoing positive effect of platelet-rich plasma versus corticosteroid injection in lateral epicondylitis: a double-blind randomized controlled trial with 2-year follow-up. Am J Sports Med. 2011;39(6): Gregory BP, Wysocki RW, Cohen MS. Controversies in surgical management of recalcitrant enthesopathy of the extensor carpi radialis brevis. J Hand Surg Am. 2016;41(8): Grewal R, MacDermid JC, Shah P, King GJ. Functional outcome of arthroscopic extensor carpi radialis brevis tendon release in chronic lateral epicondylitis. J Hand Surg Am. 2009;34(5): Grundberg AB, Dobson JF. Percutaneous release of the common extensor origin for tennis elbow. Clin Orthop Relat Res. 2000;(376): Haahr JP, Andersen JH. Prognostic factors in lateral epicondylitis: a randomized trial with one-year follow-up in 266 new cases treated with minimal occupational intervention or the usual approach in general practice. Rheumatology (Oxford). 2003;42(10): Lattermann C, Romeo AA, Anbari A, et al. Arthroscopic debridement of the extensor carpi radialis brevis for recalcitrant lateral epicondylitis. J Shoulder Elbow Surg. 2010;19(5): Monto RR. Tennis elbow repair with or without suture anchors: a randomized clinical trial. Tech Shoulder Elbow Surg. 2014;15(3): Nirschl RP. Lateral extensor release for tennis elbow. J Bone Joint Surg Am. 1994;76(6): Nirschl RP. Mesenchymal syndrome. Va Med Mon (1918). 1969; 96(11): Nirschl RP, Ashman ES. Tennis elbow tendinosis (epicondylitis). Instr Course Lect. 2004;53: Nirschl RP, Pettrone FA. Tennis elbow: the surgical treatment of lateral epicondylitis. J Bone Joint Surg Am. 1979;61(6A): Peart RE, Strickler SS, Schweitzer KM Jr. Lateral epicondylitis: a comparative study of open and arthroscopic lateral release. Am J Orthop (Belle Mead NJ). 2004;33(11): Peerbooms JC, Sluimer J, Bruijn DJ, Gosens T. Positive effect of an autologous platelet concentrate in lateral epicondylitis in a doubleblind randomized controlled trial: platelet-rich plasma versus corticosteroid injection with a 1-year follow-up. Am J Sports Med. 2010; 38(2): Pruzansky ME, Gantsoudes GD, Watters N. Late surgical results of reattachment to bone in repair of chronic lateral epicondylitis. Am J Orthop (Belle Mead NJ). 2009;38(6): Solheim E, Hegna J, Oyen J. Arthroscopic versus open tennis elbow release: 3- to 6-year results of a case-control series of 305 elbows. Arthroscopy. 2013;29(5): Szabo SJ, Savoie FH 3rd, Field LD, Ramsey JR, Hosemann CD. Tendinosis of the extensor carpi radialis brevis: an evaluation of three methods of operative treatment. J Shoulder Elbow Surg. 2006;15(6): Thornton SJ, Rogers JR, Prickett WD, Dunn WR, Allen AA, Hannafin JA. Treatment of recalcitrant lateral epicondylitis with suture anchor repair. Am J Sports Med. 2005;33(10): Tsai P, Steinberg DR. Median and radial nerve compression about the elbow. Instr Course Lect. 2008;57: Tyler TF, Thomas GC, Nicholas SJ, McHugh MP. Addition of isolated wrist extensor eccentric exercise to standard treatment for chronic lateral epicondylosis: a prospective randomized trial. J Shoulder Elbow Surg. 2010;19(6): APPENDIX ICD-9 and CPT Codes Used a Diagnosis/Procedure ICD-9/CPT Code Diagnosis Lateral epicondylitis Radial nerve syndrome Open Treatment - Before 2008 Fasciotomy, lateral or medial (eg, tennis elbow or epicondylitis) Fasciotomy, lateral or medial (eg, tennis elbow or epicondylitis); with extensor origin detachment Fasciotomy, lateral or medial (eg, tennis elbow or epicondylitis); with annular ligament resection Fasciotomy, lateral or medial (eg, tennis elbow or epicondylitis); with stripping Fasciotomy, lateral or medial (eg, tennis elbow or epicondylitis); with partial ostectomy Open Treatment and After Tenotomy, elbow, lateral or medial (eg, epicondylitis, tennis elbow, golfer s elbow); percuteanous Tenotomy, elbow, lateral or medial (eg, epicondylitis, tennis elbow, golfer s elbow); debridement, soft tissue and/or bone, open Tenotomy, elbow, lateral or medial (eg, epicondylitis, tennis elbow, golfer s elbow); debridement, soft tissue and/or bone, open with tendon repair or reattachment (continued)
7 The Orthopaedic Journal of Sports Medicine Surgical Trends in Lateral Epicondylitis 7 ICD-9 and CPT Codes Used a (continued) Diagnosis/Procedure ICD-9/CPT Code Arthroscopic Treatment Arthroscopy, elbow, surgical; with removal of loose body or foreign body Arthroscopy, elbow, surgical; synovectomy, partial Arthroscopy, elbow, surgical; synovectomy, complete Arthroscopy, elbow, surgical; debridement, limited Arthroscopy, elbow, surgical; debridement, extensive Unlisted procedure, arthroscopy Concomitant Procedures Neuroplasty (excluding ulnar), arm 64708, Radial tunnel release 64708, 64722, and Cubital tunnel release Carpal tunnel release 64721, Lateral collateral ligament repair or reconstruction 24343, Arthrotomy, elbow, with synovectomy Arthroscopic synovectomy 29835, Arthroscopic removal of loose body a ICD-9, International Classification of Diseases, Ninth Revision; CPT, Current Procedural Terminology.
Demographic Trends and Complication Rates in Arthroscopic Elbow Surgery
 Demographic Trends and Complication Rates in Arthroscopic Elbow Surgery Natalie L. Leong 1 *, Jeremiah R. Cohen 1, Elizabeth Lord 1, Jeffrey C. Wang 2, David R. McAllister 1, and Frank A. Petrigliano 1
Demographic Trends and Complication Rates in Arthroscopic Elbow Surgery Natalie L. Leong 1 *, Jeremiah R. Cohen 1, Elizabeth Lord 1, Jeffrey C. Wang 2, David R. McAllister 1, and Frank A. Petrigliano 1
Platelet-Rich Plasma Compared With Other Common Injection Therapies in the Treatment of Chronic Lateral Epicondylitis
 Journal of Sport Rehabilitation, 2016, 25, 77-82 http://dx.doi.org/10.1123/jsr.2014-0198 2016 Human Kinetics, Inc. CRITICALLY APPRAISED TOPIC Platelet-Rich Plasma Compared With Other Common Injection Therapies
Journal of Sport Rehabilitation, 2016, 25, 77-82 http://dx.doi.org/10.1123/jsr.2014-0198 2016 Human Kinetics, Inc. CRITICALLY APPRAISED TOPIC Platelet-Rich Plasma Compared With Other Common Injection Therapies
N. Bigorre a,, G. Raimbeau b, P.-A. Fouque b, Y. Saint Cast b, F. Rabarin b, B. Cesari b ORIGINAL ARTICLE
 Orthopaedics & Traumatology: Surgery & Research (2011) 97, 159 163 ORIGINAL ARTICLE Lateral epicondylitis treatment by extensor carpi radialis fasciotomy and radial nerve decompression: Is outcome influenced
Orthopaedics & Traumatology: Surgery & Research (2011) 97, 159 163 ORIGINAL ARTICLE Lateral epicondylitis treatment by extensor carpi radialis fasciotomy and radial nerve decompression: Is outcome influenced
Mini-open Muscle Resection Procedure under Local Anesthesia for Lateral and Medial Epicondylitis
 Original Article Clinics in Orthopedic Surgery 2009;1:123-127 doi:10.4055/cios.2009.1.3.123 Mini-open Muscle Resection Procedure under Local Anesthesia for Lateral and Medial Epicondylitis Byung-Ki Cho,
Original Article Clinics in Orthopedic Surgery 2009;1:123-127 doi:10.4055/cios.2009.1.3.123 Mini-open Muscle Resection Procedure under Local Anesthesia for Lateral and Medial Epicondylitis Byung-Ki Cho,
OCCUPATIONAL INJURIES OF THE ELBOW
 PLEASE STAND BY WEBINAR WILL BEGIN AT 12:00 PM PST FOR AUDIO: CALL 866-740-1260 / ACCESS CODE: 764-4915# JAMES VAN DEN BOGAERDE, MD OCCUPATIONAL INJURIES OF THE ELBOW Conflict of Interest Disclosure I,
PLEASE STAND BY WEBINAR WILL BEGIN AT 12:00 PM PST FOR AUDIO: CALL 866-740-1260 / ACCESS CODE: 764-4915# JAMES VAN DEN BOGAERDE, MD OCCUPATIONAL INJURIES OF THE ELBOW Conflict of Interest Disclosure I,
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow.
 Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Seroma formation as a rare complication of lateral epicondylitis release: A case report
 Open Access Journal of Sports Medicine and Therapy Case Report ISSN 2573-1726 Seroma formation as a rare complication of lateral epicondylitis release: A case report Parth B Patel 1, Allison L Boden 2
Open Access Journal of Sports Medicine and Therapy Case Report ISSN 2573-1726 Seroma formation as a rare complication of lateral epicondylitis release: A case report Parth B Patel 1, Allison L Boden 2
ORIGINAL ARTICLE. Department of Orthopedic Surgery, Mashad University of Medical Sciences, Mashad, Iran
 Arch Iranian Med 2003; 6 (3): 196 199 ORIGINAL ARTICLE INJECTION OF METHYLPREDNISOLONE AND LIDOCAINE IN THE TREATMENT OF MEDIAL EPICONDYLITIS: A RANDOMIZED CLINICAL TRIAL Mahmood Bahari MD, Mohammad Gharehdaghi
Arch Iranian Med 2003; 6 (3): 196 199 ORIGINAL ARTICLE INJECTION OF METHYLPREDNISOLONE AND LIDOCAINE IN THE TREATMENT OF MEDIAL EPICONDYLITIS: A RANDOMIZED CLINICAL TRIAL Mahmood Bahari MD, Mohammad Gharehdaghi
Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions
 APPENDIX G Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions The purpose of this document is to provide information for physiotherapists of common medical and surgical interventions
APPENDIX G Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions The purpose of this document is to provide information for physiotherapists of common medical and surgical interventions
Clinical Orthopaedic Rehabilitation Volume 1 and 2
 Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
Grundkurs SGSM-SSMS Sion Sports Elbow. Dr Stéphane Kämpfen
 Grundkurs SGSM-SSMS Sion 2015 Sports Elbow Dr Stéphane Kämpfen Type of pathologies! Acute:! Fractures - dislocation! Sprain! Chronic:! Overload syndrome Fractures - Radial head: Mason classification Mason
Grundkurs SGSM-SSMS Sion 2015 Sports Elbow Dr Stéphane Kämpfen Type of pathologies! Acute:! Fractures - dislocation! Sprain! Chronic:! Overload syndrome Fractures - Radial head: Mason classification Mason
19 SYMPOSIUM. Felix H. Savoie III, MD Michael J. O Brien, MD
 19 SYMPOSIUM Arthroscopic Tennis Elbow Release Felix H. Savoie III, MD Michael J. O Brien, MD Abstract Lateral epicondylitis, originally referred to as tennis elbow, affects between 1% and 3% of the population
19 SYMPOSIUM Arthroscopic Tennis Elbow Release Felix H. Savoie III, MD Michael J. O Brien, MD Abstract Lateral epicondylitis, originally referred to as tennis elbow, affects between 1% and 3% of the population
Management of Chronic Elbow Pain
 Mr. Nashat Siddiqui Consultant Upper Limb Orthopaedic Surgeon Management of Chronic Elbow Pain Patients presenting with elbow pain can pose a diagnostic challenge, especially if there is no obvious recent
Mr. Nashat Siddiqui Consultant Upper Limb Orthopaedic Surgeon Management of Chronic Elbow Pain Patients presenting with elbow pain can pose a diagnostic challenge, especially if there is no obvious recent
Golf Injuries in the Upper Extremity
 Golf Injuries in the Upper Extremity David S. Zelouf, MD Philadelphia Hand to Shoulder Center March Meeting 2019 I have nothing to disclose Except that I m an avid, competitive golfer and I ve had golfer
Golf Injuries in the Upper Extremity David S. Zelouf, MD Philadelphia Hand to Shoulder Center March Meeting 2019 I have nothing to disclose Except that I m an avid, competitive golfer and I ve had golfer
October (Am Journal of Orthopedics, 2014)
 (Am Journal of Orthopedics, 2014) Darryl Barnes, Jim Beckley, and Jay Smith Ultrasonic Percutaneous Tenotomy for Chronic Elbow Tendonosis: A Prospective Study (Journal of Shoulder and Elbow Surgery, 2014).
(Am Journal of Orthopedics, 2014) Darryl Barnes, Jim Beckley, and Jay Smith Ultrasonic Percutaneous Tenotomy for Chronic Elbow Tendonosis: A Prospective Study (Journal of Shoulder and Elbow Surgery, 2014).
Original Research. The Orthopaedic Journal of Sports Medicine, 4(4), DOI: / ª The Author(s) 2016
 Original Research Evidence for an Environmental and Inherited Predisposition Contributing to the Risk for Global Tendinopathies or Compression Neuropathies in Patients With Rotator Cuff Tears Robert Z.
Original Research Evidence for an Environmental and Inherited Predisposition Contributing to the Risk for Global Tendinopathies or Compression Neuropathies in Patients With Rotator Cuff Tears Robert Z.
Management of the Persistently Painful Shoulder and Elbow
 Management of the Persistently Painful Shoulder and Elbow Mr Nashat Siddiqui Consultant Upper Limb Surgeon www.londonupperlimb.com Cannizaro House 2 nd March 2016 How to approach a painful shoulder/elbow
Management of the Persistently Painful Shoulder and Elbow Mr Nashat Siddiqui Consultant Upper Limb Surgeon www.londonupperlimb.com Cannizaro House 2 nd March 2016 How to approach a painful shoulder/elbow
Incidence and Complications of Open Hip Preservation Surgery: An American Board of Orthopaedic Surgery Database Review
 Incidence and Complications of Open Hip Preservation Surgery: An American Board of Orthopaedic Surgery Database Review Jon P Hedgecock MD, 1 P Christopher Cook MD FRCS(C), 1 John Harrast PhD,2 Judith F
Incidence and Complications of Open Hip Preservation Surgery: An American Board of Orthopaedic Surgery Database Review Jon P Hedgecock MD, 1 P Christopher Cook MD FRCS(C), 1 John Harrast PhD,2 Judith F
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 B F Morrey, MD Professor of Orthopedic Surgery, UTHSCSA Financial Disclosure Dr. Bernard Morrey has disclosed that he is the Medical director of Tenex Health. OUTLINE Muscles/tendons Ligaments Articulation
B F Morrey, MD Professor of Orthopedic Surgery, UTHSCSA Financial Disclosure Dr. Bernard Morrey has disclosed that he is the Medical director of Tenex Health. OUTLINE Muscles/tendons Ligaments Articulation
Lateral elbow tendinopathy
 Lateral elbow tendinopathy Lateral elbow tendinopathy is a common condition with an incidence of 1 2%. The pathology arises from the origin of extensor carpi radialis brevis where changes, consistent with
Lateral elbow tendinopathy Lateral elbow tendinopathy is a common condition with an incidence of 1 2%. The pathology arises from the origin of extensor carpi radialis brevis where changes, consistent with
Dr Hamish Osborne. Sport & Exercise Medicine Physician Dunedin
 Dr Hamish Osborne Sport & Exercise Medicine Physician Dunedin New Approaches to Handling Tendinopathies By Hamish Osborne Definition Tendinopathy Absence of tightly packed collagen bundles Large amount
Dr Hamish Osborne Sport & Exercise Medicine Physician Dunedin New Approaches to Handling Tendinopathies By Hamish Osborne Definition Tendinopathy Absence of tightly packed collagen bundles Large amount
Index. orthopedic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acetabular fractures thromboembolic disease after, 341 Achilles tendon rupture ACL. See Anterior cruciate ligament (ACL) Adolescent idiopathic
Index Note: Page numbers of article titles are in boldface type. A Acetabular fractures thromboembolic disease after, 341 Achilles tendon rupture ACL. See Anterior cruciate ligament (ACL) Adolescent idiopathic
Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers
 Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers Am J Orthop. 2016 May;45(4):296-300 Authors: Dines JS Williams PN Elattrache
Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers Am J Orthop. 2016 May;45(4):296-300 Authors: Dines JS Williams PN Elattrache
Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure)
 Acta Orthop. Belg., 2004, 70, 306-310 ORIGINAL STUDIES Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure) Bart VINGERHOEDS, Ilse DEGREEF, Luc DE SMET From the University
Acta Orthop. Belg., 2004, 70, 306-310 ORIGINAL STUDIES Debridement arthroplasty for osteoarthritis of the elbow (Outerbridge-Kashiwagi procedure) Bart VINGERHOEDS, Ilse DEGREEF, Luc DE SMET From the University
Overuse Injuries of the Upper Extremity. Overuse Injuries 7/23/2018. Peadiatric Overuse Sports Injuries. Al Hess, MD
 Overuse Injuries of the Upper Extremity Al Hess, MD 7/21/2018 1 Overuse Injuries Everything? Not Trauma, infection, tumor, rheumatoid arthritis, osteoarthritis Onset of pain associated with repetitive
Overuse Injuries of the Upper Extremity Al Hess, MD 7/21/2018 1 Overuse Injuries Everything? Not Trauma, infection, tumor, rheumatoid arthritis, osteoarthritis Onset of pain associated with repetitive
Modified anconeus muscle transfer as treatment of failed surgical release of lateral epicondylitis of the elbow
 310 Acta Orthop. Belg., 2017, t. luyckx, 83, 310-314 a. decramer, l. luyckx, j. noyez ORIGINAL STUDY Modified anconeus muscle transfer as treatment of failed surgical release of lateral epicondylitis of
310 Acta Orthop. Belg., 2017, t. luyckx, 83, 310-314 a. decramer, l. luyckx, j. noyez ORIGINAL STUDY Modified anconeus muscle transfer as treatment of failed surgical release of lateral epicondylitis of
ELBOW ARTHROSCOPY WHERE ARE WE NOW?
 ELBOW ARTHROSCOPY WHERE ARE WE NOW? Christian Veillette M.D., M.Sc., FRCSC Assistant Professor, University of Toronto Shoulder & Elbow Reconstructive Surgery Toronto Western Hospital @ University Health
ELBOW ARTHROSCOPY WHERE ARE WE NOW? Christian Veillette M.D., M.Sc., FRCSC Assistant Professor, University of Toronto Shoulder & Elbow Reconstructive Surgery Toronto Western Hospital @ University Health
Welcome to White Rock Orthopaedic Surgery Centre
 White Rock Orthopaedic Surgery Excellence in Orthopaedic Surgery since 2008 Over 700 surgical cases (spring of 2013) Fully Accredited Class-1 Facility Expedient initial assessment Secure, online registration
White Rock Orthopaedic Surgery Excellence in Orthopaedic Surgery since 2008 Over 700 surgical cases (spring of 2013) Fully Accredited Class-1 Facility Expedient initial assessment Secure, online registration
Common Tendon Disorders of the Upper Extremity. Mark Tait MD
 Common Tendon Disorders of the Upper Extremity Mark Tait MD Tendonitis History Pain and swelling (any tendon, any location) Overuse Physical examination findings Localized swelling Pain with resistance
Common Tendon Disorders of the Upper Extremity Mark Tait MD Tendonitis History Pain and swelling (any tendon, any location) Overuse Physical examination findings Localized swelling Pain with resistance
TOPAZ TM What you should know
 TOPAZ TM What you should know Not for distribution in the United States. Need to know 2 Tendon: is a tough band of fibrous connective tissue that connects muscle to bone and is capable of withstanding
TOPAZ TM What you should know Not for distribution in the United States. Need to know 2 Tendon: is a tough band of fibrous connective tissue that connects muscle to bone and is capable of withstanding
Latest technology in the treatment of chronic recalcitrant tendinopathy
 Latest technology in the treatment of chronic recalcitrant tendinopathy Dr K Arjun Rao Consultant Sport & Exercise Medicine Physician FACSEP FFSEM(UK) Specialist Sportscare W.A. WA Institute of Sport School
Latest technology in the treatment of chronic recalcitrant tendinopathy Dr K Arjun Rao Consultant Sport & Exercise Medicine Physician FACSEP FFSEM(UK) Specialist Sportscare W.A. WA Institute of Sport School
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Rotator Cuff Tears. Dr. Anthony Levenda September, 2017
 Rotator Cuff Tears Dr. Anthony Levenda September, 2017 Rotator cuff tears come in a variety of shapes and sizes. No two are exactly the same, and as such, they are not all treated the same. It is important
Rotator Cuff Tears Dr. Anthony Levenda September, 2017 Rotator cuff tears come in a variety of shapes and sizes. No two are exactly the same, and as such, they are not all treated the same. It is important
Evaluating concomitant lateral epicondylitis and cervical radiculopathy
 Evaluating concomitant lateral epicondylitis and cervical radiculopathy March 06, 2010 This article describes a study of the prevalence of lateral epicondylitis or tennis elbow among patients with neck
Evaluating concomitant lateral epicondylitis and cervical radiculopathy March 06, 2010 This article describes a study of the prevalence of lateral epicondylitis or tennis elbow among patients with neck
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatric Surgery. Procedure List. As Of.
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2016 Alberta Health Care Insurance Plan Page i Generated 2016/03/22 TABLE OF CONTENTS As of 2016/04/01 07 PHYSICAL MEDICINE, REHABILITATION,
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2016 Alberta Health Care Insurance Plan Page i Generated 2016/03/22 TABLE OF CONTENTS As of 2016/04/01 07 PHYSICAL MEDICINE, REHABILITATION,
ABOS/CORD Surgical Skills Assessment Program
 American Board of Orthopaedic Surgery Establishing Education & Performance Standards for Orthopaedic Surgeons ABOS/CORD Surgical Skills Assessment Program ABOS Essential Knowledge, Skills, and Behaviors
American Board of Orthopaedic Surgery Establishing Education & Performance Standards for Orthopaedic Surgeons ABOS/CORD Surgical Skills Assessment Program ABOS Essential Knowledge, Skills, and Behaviors
A retrospective comparison of the management of recalcitrant lateral elbow tendinosis: platelet-rich plasma injections versus surgery
 HAND (2015) 10:285 291 DOI 10.1007/s11552-014-9717-8 A retrospective comparison of the management of recalcitrant lateral elbow tendinosis: platelet-rich plasma injections versus surgery Ronald D. Ford
HAND (2015) 10:285 291 DOI 10.1007/s11552-014-9717-8 A retrospective comparison of the management of recalcitrant lateral elbow tendinosis: platelet-rich plasma injections versus surgery Ronald D. Ford
Trauma & Orthopaedic Undergraduate Syllabus
 Trauma & Orthopaedic Undergraduate Syllabus Introduction The purpose of this document is to provide a recommended syllabus for medical students in Trauma & Orthopaedics (T&0). It should help students on
Trauma & Orthopaedic Undergraduate Syllabus Introduction The purpose of this document is to provide a recommended syllabus for medical students in Trauma & Orthopaedics (T&0). It should help students on
Displaced Supracondylar Humerus Fractures in Children Are They All Identical?
 Doi: http://dx.doi.org/10.5704/moj.1707.017 Displaced Supracondylar Humerus Fractures in Children Are They All Identical? Gera SK, MS Orth, Tan MCH, MBBS, Lim YG, MRCS Ed, Lim KBL, FRCSEd Orth Department
Doi: http://dx.doi.org/10.5704/moj.1707.017 Displaced Supracondylar Humerus Fractures in Children Are They All Identical? Gera SK, MS Orth, Tan MCH, MBBS, Lim YG, MRCS Ed, Lim KBL, FRCSEd Orth Department
Patient-Related Risk Factors for Infection Following Ulnar Nerve Release at the Cubital Tunnel
 Original Research Patient-Related Risk Factors for Infection Following Ulnar Nerve Release at the Cubital Tunnel An Analysis of 15,188 Cases Christopher L. Camp,* MD, Collin C. Tebo, MA, Ryan M. Degen,
Original Research Patient-Related Risk Factors for Infection Following Ulnar Nerve Release at the Cubital Tunnel An Analysis of 15,188 Cases Christopher L. Camp,* MD, Collin C. Tebo, MA, Ryan M. Degen,
Inspection. Physical Examination of the Elbow. Anterior Elbow 2/14/2017. Inspection. Carrying angle. Lateral dimple. Physical Exam of the Elbow
 of the Elbow Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Rush University President-Elect, American Shoulder Elbow Surgeons Team Physician, Chicago
of the Elbow Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Rush University President-Elect, American Shoulder Elbow Surgeons Team Physician, Chicago
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatry. Procedure List. As Of. 01 April Government of Alberta
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
10/1/2009. October 15, 2009 Christina Kuo MD. Anatomy and pathophysiology of Epicondylitis Diagnosis
 October 15, 2009 Christina Kuo MD Anatomy and pathophysiology of Epicondylitis Diagnosis Treatment options Lawn tennis elbow Morris 1882 - described as an injury occurring from the backhand stroke Age
October 15, 2009 Christina Kuo MD Anatomy and pathophysiology of Epicondylitis Diagnosis Treatment options Lawn tennis elbow Morris 1882 - described as an injury occurring from the backhand stroke Age
Adult Reconstruction Hip Education Tracks
 Adult Reconstruction Hip Education Tracks Adult Reconstruction Hip Track for the Specialist - HIP1 ICL 281 A Case-based Approach to High Risk Total Hip - When Do I Do Something Differently? ICL 241 The
Adult Reconstruction Hip Education Tracks Adult Reconstruction Hip Track for the Specialist - HIP1 ICL 281 A Case-based Approach to High Risk Total Hip - When Do I Do Something Differently? ICL 241 The
Management of arthritis of the shoulder. Omar Haddo Consultant Orthopaedic Surgeon
 Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
Management of arthritis of the shoulder Omar Haddo Consultant Orthopaedic Surgeon Diagnosis Pain - with activity initially. As disease progresses night pain is common and sleep difficult Stiffness trouble
GENERAL ORTHOPAEDIC PROGRAM SCHEDULE 18. January 25 26, 2019 Rosemont, IL. Albert J. Aboulafia, MD & Isador H. Lieberman, MD, MBA, FRCSC
 AAOS Board Maintenance of Certification Preparation and Review GENERAL ORTHOPAEDIC PROGRAM SCHEDULE 18 CME Credits January 25 26, 2019 Rosemont, IL Albert J. Aboulafia, MD & Isador H. Lieberman, MD, MBA,
AAOS Board Maintenance of Certification Preparation and Review GENERAL ORTHOPAEDIC PROGRAM SCHEDULE 18 CME Credits January 25 26, 2019 Rosemont, IL Albert J. Aboulafia, MD & Isador H. Lieberman, MD, MBA,
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome)
 A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
JuggerKnot Soft Anchor 1.5 mm with Percutaneous Instrumentation for Low Profile/Trans-Cuff PASTA Repair
 JuggerKnot Soft Anchor 1.5 mm with Percutaneous Instrumentation for Low Profile/Trans-Cuff PASTA Repair Surgical Technique by Shabi Kahn, MD One Surgeon. One Patient. Over 1 million times per year, Biomet
JuggerKnot Soft Anchor 1.5 mm with Percutaneous Instrumentation for Low Profile/Trans-Cuff PASTA Repair Surgical Technique by Shabi Kahn, MD One Surgeon. One Patient. Over 1 million times per year, Biomet
8 Recovering From HAND FRACTURE SURGERY
 8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions
 Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions Orthopaedic Opinion Online is a website designed to provide information to patients who have
Welcome to the: Orthopaedic Opinion Online Website The website for the answer to all your Orthopaedic Questions Orthopaedic Opinion Online is a website designed to provide information to patients who have
Sports related injuries of the elbow. Dr. B. The, MD, PhD Upper Limb Unit Amphia Hospital Breda
 Sports related injuries of the elbow Dr. B. The, MD, PhD Upper Limb Unit Amphia Hospital Breda bthe@amphia.nl A short intro Work at hand Thrower s elbow First report 1941 (Bennet, JAMA) a possible complication
Sports related injuries of the elbow Dr. B. The, MD, PhD Upper Limb Unit Amphia Hospital Breda bthe@amphia.nl A short intro Work at hand Thrower s elbow First report 1941 (Bennet, JAMA) a possible complication
Elbow Muscle Power Deficits
 1 Elbow Muscle Power Deficits ICD-9-CM code: 726.32 Lateral epicondylitis ICF codes: Activities and Participation code: d4300 Lifting, d4452 Reaching, d4401 Grasping Body Structure code: s73012 Muscles
1 Elbow Muscle Power Deficits ICD-9-CM code: 726.32 Lateral epicondylitis ICF codes: Activities and Participation code: d4300 Lifting, d4452 Reaching, d4401 Grasping Body Structure code: s73012 Muscles
A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) William T. Grant, MD
 A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh,
A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Injection of Autologous Blood versus Corticosteroid Injection in the Treatment of Tennis Elbow:
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Injection of Autologous Blood versus Corticosteroid Injection in the Treatment of Tennis Elbow:
Rotator Cuff Tears: Surgical Treatment Options
 Rotator Cuff Tears: Surgical Treatment Options The following article provides in depth information about surgical treatment for rotator cuff injuries, and is a continuation of the article "Rotator Cuff
Rotator Cuff Tears: Surgical Treatment Options The following article provides in depth information about surgical treatment for rotator cuff injuries, and is a continuation of the article "Rotator Cuff
ORTHOPEDICS BONE Recalcitrant nonunions In total hip replacement total knee surgery increased callus volume
 ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
Columbia/NYOH Department of Orthopaedics Shoulder, Elbow, and Sports Medicine Service Competency Requirements
 Updated 2/8/10 Columbia/NYOH Department of Orthopaedics Shoulder, Elbow, and Sports Medicine Service Competency Requirements Patient Care Faculty will evaluate the resident s ability to obtain History,
Updated 2/8/10 Columbia/NYOH Department of Orthopaedics Shoulder, Elbow, and Sports Medicine Service Competency Requirements Patient Care Faculty will evaluate the resident s ability to obtain History,
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribution.
 COMMON ELBOW INJURIES In The Athlete B F Morrey, MD Professor of Orthopedics UTHSCSA Professor of Orthopedics Mayo Cllnic COMMON SPORTS INJURIES of the ELBOW Disclosure Potential conflicts Zimmer royalities,
COMMON ELBOW INJURIES In The Athlete B F Morrey, MD Professor of Orthopedics UTHSCSA Professor of Orthopedics Mayo Cllnic COMMON SPORTS INJURIES of the ELBOW Disclosure Potential conflicts Zimmer royalities,
Musculofascial lengthening for the treatment of patients with medial epicondylitis and coexistent ulnar neuropathy
 Musculofascial lengthening for the treatment of patients with medial epicondylitis and coexistent ulnar neuropathy H. S. Gong, M. S. Chung, E. S. Kang, J. H. Oh, Y. H. Lee, G. H. Baek From Seoul National
Musculofascial lengthening for the treatment of patients with medial epicondylitis and coexistent ulnar neuropathy H. S. Gong, M. S. Chung, E. S. Kang, J. H. Oh, Y. H. Lee, G. H. Baek From Seoul National
Functional Anatomy of the Elbow
 Functional Anatomy of the Elbow Orthopedic Institute Daryl C. Osbahr, M.D. Chief of Sports Medicine, Orlando Health Chief Medical Officer, Orlando City Soccer Club Orthopedic Consultant, Washington Nationals
Functional Anatomy of the Elbow Orthopedic Institute Daryl C. Osbahr, M.D. Chief of Sports Medicine, Orlando Health Chief Medical Officer, Orlando City Soccer Club Orthopedic Consultant, Washington Nationals
Arthroscopy in sports medicine
 Arthroscopy in sports medicine DR PABITRA KUMAR SAHOO, ASSISTANT PROFESSOR (PMR) Sports medicine is a special branch of rehab specialty which deals with training in anatomy, biomechanics, pathophysiology
Arthroscopy in sports medicine DR PABITRA KUMAR SAHOO, ASSISTANT PROFESSOR (PMR) Sports medicine is a special branch of rehab specialty which deals with training in anatomy, biomechanics, pathophysiology
Intraarticular platelet-rich plasma injection in the treatment of knee osteoarthritis: review and recommendations.
 Am J Phys Med Rehabil. 2014 Nov;93(11 Suppl 3):S108-21. doi: 10.1097/PHM.0000000000000115. Intraarticular platelet-rich plasma injection in the treatment of knee osteoarthritis: review and recommendations.
Am J Phys Med Rehabil. 2014 Nov;93(11 Suppl 3):S108-21. doi: 10.1097/PHM.0000000000000115. Intraarticular platelet-rich plasma injection in the treatment of knee osteoarthritis: review and recommendations.
Columbia/NYOH Department of Orthopaedics Hand Service Competency Requirements
 Revised 2/8/10 Columbia/NYOH Department of Orthopaedics Hand Service Competency Requirements Patient Care Faculty will evaluate the resident s ability to obtain an H&P and appropriate radiographs and formulate
Revised 2/8/10 Columbia/NYOH Department of Orthopaedics Hand Service Competency Requirements Patient Care Faculty will evaluate the resident s ability to obtain an H&P and appropriate radiographs and formulate
What Treatment Works, What Does Not, When Is ENOUGH Enough?
 What Treatment Works, What Does Not, When Is ENOUGH Enough? Hand And Elbow Injuries Dori Cage, M.D. Goals of Talk Provide cases to stimulate discussion Present an approach when considering further surgery
What Treatment Works, What Does Not, When Is ENOUGH Enough? Hand And Elbow Injuries Dori Cage, M.D. Goals of Talk Provide cases to stimulate discussion Present an approach when considering further surgery
There is an abundance of literature addressing the
 Arthroscopic Technique for Medial Epicondylitis: Technique and Safety Analysis Alan Zonno, M.D., Jennifer Manuel, M.D., Gregory Merrell, M.D., Paul Ramos, P.A., Edward Akelman, M.D., and Manuel F. DaSilva,
Arthroscopic Technique for Medial Epicondylitis: Technique and Safety Analysis Alan Zonno, M.D., Jennifer Manuel, M.D., Gregory Merrell, M.D., Paul Ramos, P.A., Edward Akelman, M.D., and Manuel F. DaSilva,
Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012
 Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012 Multiaxial ball and socket Little Inherent Instability Glenohumeral
Shoulder Injuries: Treatments that Work, Do Not Work, and When ENOUGH is Enough? Mark Ganjianpour, M.D. Beverly Hills, CA April 20, 2012 Multiaxial ball and socket Little Inherent Instability Glenohumeral
The Reasons We Experience Pain
 Pain signals can originate in the skin, bone, muscles or nerves. We have all experienced aches and pains from daily activities, work activities, sports activities or accidents and trauma. Our bodies have
Pain signals can originate in the skin, bone, muscles or nerves. We have all experienced aches and pains from daily activities, work activities, sports activities or accidents and trauma. Our bodies have
Recurrent and Chronic Elbow Instability
 Recurrent and Chronic Elbow Instability Elbow instability is a looseness in the elbow joint that may cause the joint to catch, pop, or slide out of place during certain arm movements. It most often occurs
Recurrent and Chronic Elbow Instability Elbow instability is a looseness in the elbow joint that may cause the joint to catch, pop, or slide out of place during certain arm movements. It most often occurs
New Complication Associated With All-Inside Meniscal Repair Device: Ultrasound-Aided Diagnosis and Operative Localization of Foreign Body Reaction
 Department of Orthopedics and Rehabilitation Publications 9-2-2016 New Complication Associated With All-Inside Meniscal Repair Device: Ultrasound-Aided Diagnosis and Operative Localization of Foreign Body
Department of Orthopedics and Rehabilitation Publications 9-2-2016 New Complication Associated With All-Inside Meniscal Repair Device: Ultrasound-Aided Diagnosis and Operative Localization of Foreign Body
Certificate for Advanced Practice in Hand Therapy
 Certificate for Advanced Practice in Hand Therapy Curriculum Effective: March 2016 EBP 6100 Evidence-based Practice I (15 hours/1 credit) ONLINE SELF-PACED, SELF-STUDY This course is designed to improve
Certificate for Advanced Practice in Hand Therapy Curriculum Effective: March 2016 EBP 6100 Evidence-based Practice I (15 hours/1 credit) ONLINE SELF-PACED, SELF-STUDY This course is designed to improve
Slide 1. Slide 2. Slide 3. The Thrower s Elbow: When to Operate. Medial Elbow Pain in the Athlete. Goal of This Talk
 Slide 1 The Thrower s Elbow: When to Operate Luke S. Oh, MD Massachusetts General Hospital Team Physician, Boston Red Sox Team Physician, New England Revolution Consultant, Harvard University Athletics
Slide 1 The Thrower s Elbow: When to Operate Luke S. Oh, MD Massachusetts General Hospital Team Physician, Boston Red Sox Team Physician, New England Revolution Consultant, Harvard University Athletics
Clinical Review Criteria
 Clinical Review Criteria Autologous Platelet Derived Wound Healing Factors for Treatment of: Non Healing Cutaneous Wounds (Procuren) Non-Healing Fractures and the Associated GEM 21STM Device Platelet Rich
Clinical Review Criteria Autologous Platelet Derived Wound Healing Factors for Treatment of: Non Healing Cutaneous Wounds (Procuren) Non-Healing Fractures and the Associated GEM 21STM Device Platelet Rich
1. Scope vs No Scope. UCL Reconstruction Variations 11/19/2018. Evolutionary Pressure. Complexity of the Surgery Extensive Dissection
 UCL Reconstruction Variations Christopher S. Ahmad, MD Professor Orthopedic Surgery Chief Sports Medicine Head Team Physician New York Yankees New York City Football Club Evolutionary Pressure Complexity
UCL Reconstruction Variations Christopher S. Ahmad, MD Professor Orthopedic Surgery Chief Sports Medicine Head Team Physician New York Yankees New York City Football Club Evolutionary Pressure Complexity
10/8/14. Revision Date(s): Policy Number: MCP-207. Review Date: 12/16/15, 9/15/16
 Subject: Platelet-rich Plasma (PRP) Policy Number: MCP-207 Review Date: 12/16/15, 9/15/16 Revision Date(s): Original Effective Date: 10/8/14 DISCLAIMER This Molina Clinical Policy (MCP) is intended to
Subject: Platelet-rich Plasma (PRP) Policy Number: MCP-207 Review Date: 12/16/15, 9/15/16 Revision Date(s): Original Effective Date: 10/8/14 DISCLAIMER This Molina Clinical Policy (MCP) is intended to
mechanical stresses on the tendon with repetitive loading
 Tendinopathy.. How does it happen? mechanical stresses on the tendon with repetitive loading Impingement of the tendon between adjacent structures (bones, ligaments) and impaired blood supply Presentation
Tendinopathy.. How does it happen? mechanical stresses on the tendon with repetitive loading Impingement of the tendon between adjacent structures (bones, ligaments) and impaired blood supply Presentation
JuggerKnot and JuggerKnotless Soft Anchor. All-Inclusive Brochure
 JuggerKnot and JuggerKnotless Soft Anchor All-Inclusive Brochure 3 JuggerKnot and JuggerKnotless Soft Anchor All-Inclusive Brochure JuggerKnot Soft Anchor The Leader in All-Suture Anchors 1 Zimmer Biomet
JuggerKnot and JuggerKnotless Soft Anchor All-Inclusive Brochure 3 JuggerKnot and JuggerKnotless Soft Anchor All-Inclusive Brochure JuggerKnot Soft Anchor The Leader in All-Suture Anchors 1 Zimmer Biomet
ORTHOPAEDIC INJECTION AND ASPIRATION TECHNIQUES
 ORTHOPAEDIC INJECTION AND ASPIRATION TECHNIQUES OAAPN October 20, 2016 David H. Sohn, JD MD Chief, Shoulder and Sports Medicine University of Toledo Medical Center When to aspirate? To rule out infection
ORTHOPAEDIC INJECTION AND ASPIRATION TECHNIQUES OAAPN October 20, 2016 David H. Sohn, JD MD Chief, Shoulder and Sports Medicine University of Toledo Medical Center When to aspirate? To rule out infection
Department of Orthopaedics and Rehabilitation
 Rotation: Department of Orthopaedics and Rehabilitation Resident Year-In-Training: Attending Physicians Rotation-Specific Objectives for Resident Education 1. Robert Orfaly, M.D., FRCS(C) Orthopaedic Surgeon,
Rotation: Department of Orthopaedics and Rehabilitation Resident Year-In-Training: Attending Physicians Rotation-Specific Objectives for Resident Education 1. Robert Orfaly, M.D., FRCS(C) Orthopaedic Surgeon,
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 COMMON ELBOW INJURIES In The Athlete B F Morrey, MD Professor of Orthopedics UTHSCSA Disclosure Potential conflicts Zimmer royalties, consultant Stryker royalties Tenex Medical director; Interim CEO Professor
COMMON ELBOW INJURIES In The Athlete B F Morrey, MD Professor of Orthopedics UTHSCSA Disclosure Potential conflicts Zimmer royalties, consultant Stryker royalties Tenex Medical director; Interim CEO Professor
Upper limb injuries II. Traumatology RHS 231 Dr. Einas Al-Eisa
 Upper limb injuries II Traumatology RHS 231 Dr. Einas Al-Eisa Capsulitis = inflammatory lesion of the glenohumeral joint capsule leading to: thickening and loss of joint volume painful stiffness of the
Upper limb injuries II Traumatology RHS 231 Dr. Einas Al-Eisa Capsulitis = inflammatory lesion of the glenohumeral joint capsule leading to: thickening and loss of joint volume painful stiffness of the
Internet Journal of Medical Update
 Internet Journal of Medical Update 2010 January;5(1):20-24 Internet Journal of Medical Update Journal home page: http://www.akspublication.com/ijmu Original Work Clinical assessment of functional outcome
Internet Journal of Medical Update 2010 January;5(1):20-24 Internet Journal of Medical Update Journal home page: http://www.akspublication.com/ijmu Original Work Clinical assessment of functional outcome
ELBOW INJURIES IN THE TENNIS PLAYER
 ELBOW INJURIES IN THE TENNIS PLAYER A CONCISE REVIEW Written by Brian Grawe, David Dines and Josh Dines, USA INTRODUCTION The worldwide popularity of tennis has grown in recent years and it is estimated
ELBOW INJURIES IN THE TENNIS PLAYER A CONCISE REVIEW Written by Brian Grawe, David Dines and Josh Dines, USA INTRODUCTION The worldwide popularity of tennis has grown in recent years and it is estimated
Sonographically occult intrasubstance tendon tears revealed by platelet rich plasma injection: evidence of a frequently overlooked pathology?
 Sonographically occult intrasubstance tendon tears revealed by platelet rich plasma injection: evidence of a frequently overlooked pathology? Poster No.: C-1603 Congress: ECR 2013 Type: Scientific Exhibit
Sonographically occult intrasubstance tendon tears revealed by platelet rich plasma injection: evidence of a frequently overlooked pathology? Poster No.: C-1603 Congress: ECR 2013 Type: Scientific Exhibit
Cubital Tunnel Syndrome
 Cubital Tunnel 2 3333 N CALVERT ST, SUITE 370, BALTIMORE, MD 21218 T410 467 5400 F410 366 9826 delloninstitutes.com your complaints are Numbness or tingling in the little/ring side of the front and back
Cubital Tunnel 2 3333 N CALVERT ST, SUITE 370, BALTIMORE, MD 21218 T410 467 5400 F410 366 9826 delloninstitutes.com your complaints are Numbness or tingling in the little/ring side of the front and back
Department of Orthopaedics
 OUTCOMES DIVISION OF MEDICINE Department of Orthopaedics About Cleveland Clinic Florida Cleveland Clinic Florida s medical staff are dedicated physicians who have joined the clinic as salaried doctors
OUTCOMES DIVISION OF MEDICINE Department of Orthopaedics About Cleveland Clinic Florida Cleveland Clinic Florida s medical staff are dedicated physicians who have joined the clinic as salaried doctors
MEDIAL EPICONDYLE FRACTURES
 MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
Overuse Injuries & special skeletal injuries Dr M.Taghavi Director of sport medicine center of olympic academy
 Overuse Injuries & special skeletal injuries Dr M.Taghavi Director of sport medicine center of olympic academy Prevalence of Overuse Injuries 30 to 50% of all sport injuries are from overuse In some sports
Overuse Injuries & special skeletal injuries Dr M.Taghavi Director of sport medicine center of olympic academy Prevalence of Overuse Injuries 30 to 50% of all sport injuries are from overuse In some sports
Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini
 Open Access Case report Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini Address: Department of Orthopaedic
Open Access Case report Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini Address: Department of Orthopaedic
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Spine Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Spine Neurosurgery Spine neurosurgeons treat
Introduction to Neurosurgical Subspecialties: Spine Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Spine Neurosurgery Spine neurosurgeons treat
Sports Medicine Unit 16 Elbow
 Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Introduction. Anatomy
 Introduction The doctors call it a UCLR ulnar collateral ligament reconstruction. Baseball players and fans call it Tommy John surgery -- named after the pitcher (Los Angeles Dodgers) who was the first
Introduction The doctors call it a UCLR ulnar collateral ligament reconstruction. Baseball players and fans call it Tommy John surgery -- named after the pitcher (Los Angeles Dodgers) who was the first
Arthroscopic Rotator Cuff Repair
 Arthroscopic Rotator Cuff Repair CHRISTOPHER S. AHMAD, MD; WILLIAM N. LEVINE, MD; LOUIS U. BIGLIANI, MD Arthroscopic rotator cuff repair offers less pain, quicker recovery, and less stiffness compared
Arthroscopic Rotator Cuff Repair CHRISTOPHER S. AHMAD, MD; WILLIAM N. LEVINE, MD; LOUIS U. BIGLIANI, MD Arthroscopic rotator cuff repair offers less pain, quicker recovery, and less stiffness compared
Autologous Bone Marrow Plasma Injection after Arthroscopic Debridement for Elbow Tendinosis
 Original Article 559 Autologous Bone Marrow Plasma Injection after Arthroscopic Debridement for Elbow Tendinosis Young Lae Moon, 1 MD, Sueng-Hwan Jo, 1 MD, Chang Hun Song, 2,4 MD, PhD, Geon Park, 3 MD,
Original Article 559 Autologous Bone Marrow Plasma Injection after Arthroscopic Debridement for Elbow Tendinosis Young Lae Moon, 1 MD, Sueng-Hwan Jo, 1 MD, Chang Hun Song, 2,4 MD, PhD, Geon Park, 3 MD,
MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM. What Are Musculoskeletal Disorders
 MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM What Are Musculoskeletal Disorders Every year more than 1.8 million workers in the United States suffer painful back and repetitive strain injuries,
MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM What Are Musculoskeletal Disorders Every year more than 1.8 million workers in the United States suffer painful back and repetitive strain injuries,
EXERCISE PRESCRIPTION PART 1
 EXERCISE PRESCRIPTION PART 1 Michael McMurray, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 What is MET? An active rehabilitation system based in the biopsychosocial
EXERCISE PRESCRIPTION PART 1 Michael McMurray, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 What is MET? An active rehabilitation system based in the biopsychosocial
Worker's Compensation Shoulder Practices
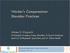 Worker's Compensation Shoulder Practices Aimee S. Klapach Orthopedic Surgeon; Knee, Shoulder, & Sports Medicine Sports & Orthopaedic Specialists, part of Allina Health Minnesota Department of Labor and
Worker's Compensation Shoulder Practices Aimee S. Klapach Orthopedic Surgeon; Knee, Shoulder, & Sports Medicine Sports & Orthopaedic Specialists, part of Allina Health Minnesota Department of Labor and
Common Elbow Problems
 Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Cubital Tunnel Syndrome
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about must be made in conjunction with your Physician or a licensed healthcare provider.
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about must be made in conjunction with your Physician or a licensed healthcare provider.
IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides
 IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 14 Madison, WI 53719 Phone: (608) 663-6355
IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 14 Madison, WI 53719 Phone: (608) 663-6355
Therapy of the Hand and Upper Extremity
 Therapy of the Hand and Upper Extremity Scott F.M. Duncan Christopher W. Flowers Therapy of the Hand and Upper Extremity Rehabilitation Protocols Scott F.M. Duncan Department of Orthopedic Surgery Boston
Therapy of the Hand and Upper Extremity Scott F.M. Duncan Christopher W. Flowers Therapy of the Hand and Upper Extremity Rehabilitation Protocols Scott F.M. Duncan Department of Orthopedic Surgery Boston
