on the elbow. Individuals, but most typically overhead athletes may injure this ligament,
|
|
|
- Ethelbert Goodwin
- 6 years ago
- Views:
Transcription
1 Ulnar Collateral Ligament Repair Niomi Eipp Robert Osborne Brittany Young Abstract The ulnar collateral ligament, specifically the anterior bundle, resists valgus force on the elbow. Individuals, but most typically overhead athletes may injure this ligament, causing decreased stability and joint laxity. Palpation, stress tests, and imaging are used to diagnose a UCL tear. Determining the need for surgery depends on current and desired level of functioning, and should be discussed with the surgeon initially. The most common surgical method for this type of injury is the well known Tommy John Surgery. This method published by Dr. Frank Jobe in 1986 was the first to successfully return overhead throwing athletes to their previous level of competition or higher. Since the widespread popularization of the Jobe technique, there have been many modifications suggested to improve surgical outcomes and patient function postoperatively. Some of these methods include the ZipLoop, docki ng, and ulnar nerve transposition techniques. As with any surgical procedure, limitations still exist which ought to eventually be attenuated with additional exploration of surgical methods. A successful rehabilitation is dependent upon close supervision by the physical therapist to facilitate slow and gradual progression of the recently repaired tissues. Most athletes return to sport about a year post-surgery and often see similar if not better physical function at that time.
2 Introduction The ulnar collateral ligament (UCL) provides elbow stability by resisting valgus stress placed on the medial aspect of the humeroulnar joint 1. Injury often occurs in the athletic population, since the unique force required to cause microtears is much greater than in normal functional activity. Baseball and javelin throwers comprise the most common population in which UCL injury occurs, but injury may also occur in many other sports such as soccer and tennis. 2 The UCL is made up of three portions anterior, posterior, and transverse. These combine to make a triangular complex with its role of medial elbow stability. The anterior bundle acts as the primary stabilizer against valgus forces 3. Repeated tensile trauma to the anterior bundle can lead to partial or complete tear of the ligament, which may cause elbow instability. Acute disruption of UCL is typically what causes patients to seek medical attention and potential surgery. Posterior dislocation may also occur due to acute loss of stability during a powerful overhead throw 2. Injury to the UCL can occur three ways: chronic microtears without complete disruption, an acute tear of the UCL without prior injury, or chronic microtears, which weaken the tissue enough for an acute disruption to occur. The last of the three is the most common, but it is not impossible to see the others, as well. 4 The typical force that may lead to UCL injury has three components: rapid shoulder medial rotation, near forearm full supination, and elbow flexion from approximately 90 to 125. This phase from arm-cocking to arm acceleration places the maximum load on UCL throughout a complete pitch 1. It has been reported that the UCL 1
3 can resist a maximum valgus torque of 33 Newton meters while pitching can produce an external torque of up to 64 Newton meters in professional pitchers 1,5. Since the external torque produced is greater than the maximum internal tensile force of the UCL, small tears in the ligament can result. The ulna and humerus have increased movement due to disruption of the UCL 2. The excess movement can cause the development of painful calcifications along the ulna and humerus 6. Diagnosis Diagnosis for UCL tear is often inaccurate, and may require multiple examinations and thorough history-taking. Primary symptoms include joint laxity and pain caused by improper articulation. Initially after an acute rupture, pai n and swelling occur, but tends to subside within four to five days of rest 6. If the patient also reports hearing a pop at the onset of injury, it is likely the UCL was ruptured. The patient may also report a decrease in throwing velocity, distance, or accuracy; compensatory change in biomechanics or throwing; or inability to throw due to pain. These symptoms are also likely to occur in an athlete who has repeated chronic injury to the UCL without a complete disruption. Palpation of the UCL may aid in diagnosis. Although it is not always associated with UCL injury, the patient may also experience neuropathy of the ulnar nerve, and distinguishing between the two is important for accurate diagnosis. Valgus stress test or moving valgus stress test can be performed on the affected elbow of the patient to test medial instability. A positive test result is reproduction of the pain or joint laxity increased >1 mm 5. Contralateral comparison can help determine significant joint laxity. Diminished sensitivity of the special tests also limits the ability to accurately diagnose an indi vidual. One study reported that the anterior bundle had to be 2
4 completely disrupted in order to test positive for 1-2mm of laxity 5. Since manual testing can be unreliable, proper diagnosis should include a stress radiograph, where the examiner applies a valgus stress to the elbow while being radiographed 7. Additional images may be taken using MRI, computer tomography arthrogram, and ultrasound 4. Injection of a dye prior to an MRI or adding contrast to the image increases the sensitivity 7. Determining whether or not the patient requires surgery is dependent on current and desired level of function. Ulnar collateral ligament repair aims to restore valgus stability lost due to injury by replacing the deteriorated ligament. Athletes comprise the majority population to receive ulnar collateral ligament repair surgery. Overhead athletes of any age may desire the surgery if their performance has declined significantly due to pain or instability. 83% of patients return to previous, or higher, level of performance within 11.5 months, but there is no guarantee the surgery is successful for every individual 1. However, athletes may also choose not to have the surgery if they decide not to return to play, or if the ligamentous injury does not affect the level or performance. All of these factors must be discussed between the patient, the surgeon, and any other figures, such as parents or coaches. For the non-athlete, surgery is only required if the patient feels that the ligamentous injury disrupts daily function enough to withstand surgery and rehabilitation. Surgical Methods The Jobe Technique In 1986, Dr. Frank Jobe published an article outlining a surgical technique for UCL reconstruction. Jobe s technique became known as the Tommy John Surgery, and 3
5 was the first to successfully return overhead throwing athletes to previous level of competition or higher. In this surgery, the torn or ruptured UCL is reconstructed using a tendon graft from the patient s own body, called an autograft 9. The palmaris longus tendon is the most common used, but the gracilis or plantaris tendons, or even a section of the achilles tendon, may also be used 4. To begin the surgical procedure, the medial aspect of the elbow is opened and the fascia divided longitudi nally. A second longitudinal cut is made in the flexor and pronator muscles from their attachment on the medial epicondyle of the humerus. The muscle fibers are then elevated from the medial epicondyle, leaving only a small portion of the tendon on the epicondyle for reattachment. Once these steps are completed, the anterior portion of the UCL is exposed adequately for the procedure to progress9. Bone tunnels are created by drilling three holes in the medial epicondyle, and two holes centered at the sublime tubercle of the ulna. A bone bridge of 1 cm or greater is created between the drilled holes, with bone tunnels placed in order to approximate the insertion sites of the anterior band. Two divergent tunnels on the medial epicondyle are created for insertion of the graft. The posterior cortex of the humerus is also penetrated to allow for suturing of the graft 10. Once the bone tunnels are drilled, the graft is then looped through the holes in a figure-of-eight pattern, pulled taut and sutured to itself with the elbow placed at 45 of flexion. If there are any remaining fibers from the native UCL, it is recommended that they be sutured over the graft for added strength 6. Complications and failures exist with the original Jobe technique. As a result, some alternative options are available in attempt to eliminate or at least minimize post- 4
6 operative complications. Some issues most commonly discovered include fractures in the ulnar and/or medial epicondylar bone tunnels, difficulty in proper tensioning of the tendon graft, and ulnar nerve disruption 10. Alternative methods such as the Docking and ZipLoop techniques, as well as ulnar nerve transposition methods, attempt to address some of these failures. Zip-Loop Technique The ZipLoop is a suspensory device that allows tensioning of the graft after cortical fixation of the grafts within the bone tunnels. This mechanism provides the first opportunity for re-tensioning the graft after ulnar and humeral fixation has been secured. In addition, the single-tunnel configuration of the ZipLoop also allows for more isometric insertion of the graft in the ulnar tunnel. Therefore, the risk of ulnar bone bridge fracture becomes greatly minimized if not eliminated. 10 To perform the surgery using the ZipLoop device, the single ulnar tunnel is drilled at the center of the attachment of the anterior bundle on the sublime tubercle. The ZipLoop device is then attached to the tendon graft; the middle portion of the graft is placed in the loop of the ZipLoop and the loop is shortened to match the total length of the ulnar tunnel. The ZipLoop is then passed through the ulnar tunnel for cortical fixation 10. Ulnar Nerve Transposition Since ulnar nerve symptoms were one of the most common complications with the orignial Jobe technique, there was interest in developing methods to more adequately address the nerve. The anterior subcutaneous ulnar nerve transposition (UNT) involves rerouting the nerve to run anteriorly across the cubital fossa, rather than 5
7 through the cubital tunnel at the posterior elbow 12.The Anterior FCU Retraction suggests muscle splitting of the flexor/pronator mass through the posterior third of the common flexor bundle, which ultimately transects the anterior-most fibers of the flexor carpi ulnaris. This method does not require transposition of the ulnar nerve unless the patient was experiencing pre-operative impingement symptoms 11. Ultimately, these methods decrease the amount of handling of the nerve and subsequently decrease the chances of post-operative neuropraxic symptoms. 12 Docking Technique The docking technique was designed as a slight alteration on the original Jobe technique in order to minimize chances of bone tunnel fracture when valgus stresses are placed on the reconstructed UCL. The bone tunnels are drilled in a way so that the tendon can pulled through in a triangular configuration. The ends are tied over the humeral bone bridge to secure and tension the graft 11,12. According to a study conducted by Ciccotti et al., both the docking and the original Jobe techniques closely approximate valgus stability provided by the native UCL at higher flexion angles, ranging from 90 to 110 degrees. However, neither technique was able to restore full valgus stability at lower elbow flexion angles, especially around 30. Thus, post-operative patients should exercise great caution when completing activities that induce valgus stresses at minimal elbow flexion, such as sidearm throwing 11. Rehabilitation The primary goals of the first phase of UCL graft recovery are to limit inflammation and pai n while also initiating tissue healing, range of motion recovery and 6
8 preventing muscle atrophy. Immediately post-surgery, the patient is placed in a posterior splint to immobilize the elbow at 90 degrees of elbow flexion and in a compressive elbow sleeve. 1 Although the splint is intended to limit movement, the patient should also be instructed to avoid active hyperextension of the wrist and external rotation of the shoulder greater than 90 degrees. However, if the modified Jobe musclesplitting procedure was performed, the patient may be allowed to perform range of motion exercises and well as isometric exercises in these first few days post-surgery. 5 Furthermore, if the ulnar nerve was transposed, the patient should undergo nerve testing to ensure it has maintained its integrity and is fully functioning. Along with testing its function, special care should be taken to avoid over-stretching the transposed nerve. After the first 2-3 days of recovery, the patient s compression dressing can be removed while the hard splint is removed around day 7. It is important to be mindful that this patient may be on analgesics for pain relief and their ability to give accurate feedback on sensation and pai n will be impaired. During the first 72 hours following surgery exercise interventions are performed to improve joint and scar nutrition as well as prevent loss of range of motion. It is important to stress the importance of immobilization in this acute healing phase as many everyday motions can cause injury to the recently repaired ligament. Passive and active-assisted range of motion should be performed at the humeroulnar joint as well as the radial-ulnar joint in all planes. 5 The intensity of this phase may vary based on the surgeon's instructions and the method of surgery performed. As previously stated, the musclesplitting approach allows for a more expedited return to activity. Low intensity strength exercises can be performed isometrically to ward off atrophy of the associated tissues. 5 7
9 Ball squeezes are often introduced immediately while bicep isometric holds are performed later in the first week. The modalities in this phase include cryotherapy, electrical stimulation and ultrasound 5. These are intended to primarily reduce pain and inflammation in the surgical area. Beginning in the second week of recovery, the patient is placed in a functional brace that is adjusted to allow 30 to 100 of elbow flexion. From this poi nt on, the brace s range of motion is increased weekly by 5 of extension and 10 of flexion until full return to pre-surgery range of motion around week 6 when the brace can be removed. Proprioceptive stretching should be incorporated to prevent loss of kinesthetic awareness in the end range of elbow. Low intensity passive range-of-motion exercises can also be performed at the elbow and wrist to prevent elbow flexion contractions. Strength exercises at this time include elbow, wrist and shoulder isometrics as well as wrist range of motion and gripping training. As the patient progresses in this postoperative phase, light tubing resistance and light dumbbell exercises can be performed to strengthen the shoulder and actively take the joi nts of the arm through an increasing range of motion. The incision site should receive scar mobilization at this time as well through massage to improve collagen re-alignment and minimize scar tissue formation. In weeks 5 and 6, the second phase of rehabilitation focuses primarily on increasing range of motion and improving strength. The patient should have full range of motion at all joints by this time except external rotation of the shoulder. Light resistance exercises such as wrist curls and lateral raises should be continued throughout this phase and resistance can increase slightly 6. Once the full range of motion requirement is met, the functional brace is removed and only re-applied when the patient feels they are at risk 8
10 for falls. Isotonic exercises with precaution given to avoiding elbow valgus stress are performed at all joi nts to return patient to pre-surgical strength. If the patient is healing sufficiently, 6 to 8 weeks post-op brings about an increase in functional full range of motion training. A comprehensive exercise program is often initiated around week 6 to re-strengthen the sport-essential muscles that have may have undergone atrophy due to the relative inactivity since the surgical procedure. Around this time the patient will begin to transition to the advanced strengthening phase that concentrates on returning the athlete to their pre-surgical functional status. Plyometrics such as medicine ball throws are extremely effective at stressi ng the targeted tissues while also posing no significant risk of re-injuring the ulnar collateral ligament 4. Throughout this period of increased intensity, it is important for the physical therapist to intuitively know when to challenge the patient s body but also not overstress his UCL to the point of inhibited recovery. If the initial phases of rehabilitation progress according to plan, athletes may begin to throw a ball in a gentle toss manner around month four or five. The most important concept of this phase is to progressively increase the intensity of training to allow the tissues to heal following each trai ning session. If pain increases or range of motion is affected, the physical therapist should re-evaluate the current interventions to diagnose the cause of the negative effects. Throwing volume should begin around 25 throws per session, 3 days a week on non-consecutive days and progressively increase in distance and total volume 1. Special attention should be placed on proper warm-up and cool down surroundi ng the throwing trai ning. A month later, pitchers can combine the wind-up into their throwing motion and can return to throwing off a mound around month 7. As 9
11 velocity approaches pre-surgical speeds, many therapists and coaches will decrease total volume to around 75 pitches not including the warm-up and cool down phase to limit total workload 6. Within the next two months, full recovery is expected and all precautions can be removed. The prognosis following UCL surgery is extremely positive. Dr. James Andrews, the most prominent Tommy John surgeon in Major League Baseball, finds that 83% of his patients return to activity at or above their previous playing level 1. Andrews also claims the majority of his patients return to play in less than a year, with the average time of eleven and a half months. Position players are often able to return to play around 6 months, while pitchers usually are given the Go around a year post-surgery. 10
12 References 1. Azar FM, Andrews JR, Wilk KE, Groh D. Operative treatment of ulnar collateral ligament injuries of the elbow in athletes. Am J Sports Med. 2000; 28: Nakanishi K, Masatomi T, Ochi T, et al. MR arthrography of elbow: evaluation of ulnar collateral ligament of elbow. Skeletal Radiol. 1996; 25(7) doi: /s Tommy John Surgery. WebMD Medical Reference. /fitness -exercise/tommy-john-surgery-uclreconstruction. Published February 11, Accessed November 2, Ulnar Collateral Ligament Injury (Tommy John Surgery). Gamradt Orthopedics Accessed January 8, Langer P, Fadale P, Hulstyn M. Evolution of the treatment options of ulnar collateral ligament injuries of the elbow. Br J Sports Med. 2006;40(6): Jobe FW, Stark H, Lombardo SJ. Reconstruction of the ulnar collateral ligament in athletes. J Bone Joint Surg Am, 1986; 68(8): McMahon PJ, Kaplan LD, Popkin CA. Chapter 3. Sports Medicine. In: Skinner HB, McMahon PJ. eds. Current Diagnosis & Treatment in Orthopedics, 5e. New York, NY: McGraw-Hill; bookid=675§ionid= Accessed November 02, Johns Hopkins Sports Medicine Patient Guide to UCL Injuries of the Elbow (Ulnar Collateral Ligament). Johns Hopkins Medicine. Accessed November 2, Cain EL, Andrews JR, Dugas JR, et al. Outcome of Ulnar Collateral Ligament Reconstruction of the Elbow in 1281 Athletes: Results in 743 Athletes with Minimum 2-Year Follow-Up. Am J Sports Med. 2010; 38(12): Morgan RJ, Starman JS, Habet NA, et al. A Biomechanical Evaluation of Ulnar Collateral Ligament Reconstruction Using a Novel Technique 11
13 for Ulnar-Sided Fixation. Am J Sports Med. 2010; 38(7): Ciccotti MG, Siegler S, Kuri JA, Thinnes JH, Murphy DJ. Comparison of the Biomechanical Profile of the Intact Ulnar Collateral Ligament With the Modified Jobe and the Docking Reconstructed Elbow: An In Vitro Study. Am J Sports Med. 2009; 37: Langer P, Fadale P, Hulstyn M. Evolution of the treatment options of ulnar collateral ligament injuries of the elbow. Br J Sports Med. 2006; 40(6):
Rehabilitation Guidelines for UCL Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for UCL Repair The elbow is a complex system of three joints formed from three bones; the humerus (the upper arm bone), the ulna (the larger bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for UCL Repair The elbow is a complex system of three joints formed from three bones; the humerus (the upper arm bone), the ulna (the larger bone
Introduction. Anatomy
 Introduction The doctors call it a UCLR ulnar collateral ligament reconstruction. Baseball players and fans call it Tommy John surgery -- named after the pitcher (Los Angeles Dodgers) who was the first
Introduction The doctors call it a UCLR ulnar collateral ligament reconstruction. Baseball players and fans call it Tommy John surgery -- named after the pitcher (Los Angeles Dodgers) who was the first
A Patient s Guide to Ulnar Collateral Ligament Injuries
 A Patient s Guide to Ulnar Collateral Ligament Injuries 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information
A Patient s Guide to Ulnar Collateral Ligament Injuries 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information
Ulnar Collateral Ligament Reconstruction
 Ulnar Collateral Ligament Reconstruction 1. Defined a. The ulnar collateral ligament is critical for valgus stability of the elbow. It serves as the primary elbow stabilizer and as such, serves a very
Ulnar Collateral Ligament Reconstruction 1. Defined a. The ulnar collateral ligament is critical for valgus stability of the elbow. It serves as the primary elbow stabilizer and as such, serves a very
First awareness of problems with the ulnar collateral ligament. Ulnar Collateral Ligament Reconstruction
 Ulnar Collateral Ligament Reconstruction Richard Lehman, md Ulnar collateral ligament reconstruction, which is commonly known as Tommy John surgery, was first performed on Tommy John who was a pitcher
Ulnar Collateral Ligament Reconstruction Richard Lehman, md Ulnar collateral ligament reconstruction, which is commonly known as Tommy John surgery, was first performed on Tommy John who was a pitcher
1. Scope vs No Scope. UCL Reconstruction Variations 11/19/2018. Evolutionary Pressure. Complexity of the Surgery Extensive Dissection
 UCL Reconstruction Variations Christopher S. Ahmad, MD Professor Orthopedic Surgery Chief Sports Medicine Head Team Physician New York Yankees New York City Football Club Evolutionary Pressure Complexity
UCL Reconstruction Variations Christopher S. Ahmad, MD Professor Orthopedic Surgery Chief Sports Medicine Head Team Physician New York Yankees New York City Football Club Evolutionary Pressure Complexity
Disclosures. Throwing is NOT Normal MCL RECONSTRUCTION: INDICATIONS, TECHNIQUE, RESULTS. Joshua S. Dines, MD. Sports Medicine and Shoulder Service
 MCL RECONSTRUCTION: INDICATIONS, TECHNIQUE, RESULTS Joshua S. Dines, MD Sports Medicine and Shoulder Service Disclosures Consultant: Arthrex, Conmed Linvatec, Ossur IP/Royalties: Conmed Linvatec Editorial
MCL RECONSTRUCTION: INDICATIONS, TECHNIQUE, RESULTS Joshua S. Dines, MD Sports Medicine and Shoulder Service Disclosures Consultant: Arthrex, Conmed Linvatec, Ossur IP/Royalties: Conmed Linvatec Editorial
Medial Collateral Instability of the Elbow. CSES Residents Course Calgary AB February 1-3, 2017 WD Regan MD
 Medial Collateral Instability of the Elbow CSES Residents Course Calgary AB February 1-3, 2017 WD Regan MD Disclosures I have no disclosures to report Anatomy Medial Collateral Ligament Anterior Oblique
Medial Collateral Instability of the Elbow CSES Residents Course Calgary AB February 1-3, 2017 WD Regan MD Disclosures I have no disclosures to report Anatomy Medial Collateral Ligament Anterior Oblique
Patient Education Ulnar Collateral Ligament Reconstruction
 Explanation of Procedure and/or Diagnosis Overview is commonly referred to as Tommy John Surgery. Tommy John was a baseball pitcher who played for the Los Angeles Dodgers. He was the first person to have
Explanation of Procedure and/or Diagnosis Overview is commonly referred to as Tommy John Surgery. Tommy John was a baseball pitcher who played for the Los Angeles Dodgers. He was the first person to have
A Patient s Guide to. Ulnar Collateral Ligament Reconstruction (Tommy John Surgery)
 A Patient s Guide to Ulnar Collateral Ligament Reconstruction (Tommy John Surgery) 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.com DISCLAIMER:
A Patient s Guide to Ulnar Collateral Ligament Reconstruction (Tommy John Surgery) 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.com DISCLAIMER:
POST-OPERATIVE REHABILITATION PROTOCOL FOLLOWING ULNAR COLLATERAL LIGAMENT RECONSTRUCTION USING AUTOGENOUS GRACILIS GRAFT
 Therapist POST-OPERATIVE REHABILITATION PROTOCOL FOLLOWING ULNAR COLLATERAL LIGAMENT RECONSTRUCTION USING AUTOGENOUS GRACILIS GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (0-3 weeks) Protect healing tissue
Therapist POST-OPERATIVE REHABILITATION PROTOCOL FOLLOWING ULNAR COLLATERAL LIGAMENT RECONSTRUCTION USING AUTOGENOUS GRACILIS GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (0-3 weeks) Protect healing tissue
Medial Elbow Instability & Ulnar Collateral Ligament Reconstruction in a Collegiate Baseball Player.
 Medial Elbow Instability & Ulnar Collateral Ligament Reconstruction in a Collegiate Baseball Player www.fisiokinesiterapia.biz PLAN for the day: Brief introduction Review of elbow anatomy Ulnar Collateral
Medial Elbow Instability & Ulnar Collateral Ligament Reconstruction in a Collegiate Baseball Player www.fisiokinesiterapia.biz PLAN for the day: Brief introduction Review of elbow anatomy Ulnar Collateral
Elbow Injuries in the Adult Athlete. Tamara A. Scerpella, MD Professor, Orthopedic Surgery University of Wisconsin
 Elbow Injuries in the Adult Athlete Tamara A. Scerpella, MD Professor, Orthopedic Surgery University of Wisconsin Acute Elbow Dislocation Fracture Distal humerus Olecranon Radial head Distal Biceps Rupture
Elbow Injuries in the Adult Athlete Tamara A. Scerpella, MD Professor, Orthopedic Surgery University of Wisconsin Acute Elbow Dislocation Fracture Distal humerus Olecranon Radial head Distal Biceps Rupture
Throwing is NOT Normal TREATMENT OF ELBOW INJURIES. Joshua S. Dines, MD IN OVERHEAD ATHLETES: HOW HAS IT EVOLVED?
 TREATMENT OF ELBOW INJURIES IN OVERHEAD ATHLETES: HOW HAS IT EVOLVED? Joshua S. Dines, MD Sports Medicine and Shoulder Service Hospital for Special Surgery Throwing is NOT Normal Excessive Joint Forces
TREATMENT OF ELBOW INJURIES IN OVERHEAD ATHLETES: HOW HAS IT EVOLVED? Joshua S. Dines, MD Sports Medicine and Shoulder Service Hospital for Special Surgery Throwing is NOT Normal Excessive Joint Forces
Sports Medicine Unit 16 Elbow
 Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
ADVENTURES AND LESSONS LEARNED ON THE UCL
 ADVENTURES AND LESSONS LEARNED ON THE UCL Michael G. Ciccotti, M.D. Department of Orthopaedics The Rothman Institute Thomas Jefferson University Philadelphia, PA Eastern Athletic Trainers Association Philadelphia,
ADVENTURES AND LESSONS LEARNED ON THE UCL Michael G. Ciccotti, M.D. Department of Orthopaedics The Rothman Institute Thomas Jefferson University Philadelphia, PA Eastern Athletic Trainers Association Philadelphia,
I (and/or my co-authors) have something to disclose.
 Elbow Anatomy And Biomechanics Nikhil N Verma, MD Director, Division of Sports Medicine Professor, Department of Orthopedics Rush University Medical Center Team Physician, Chicago White Sox and Bulls I
Elbow Anatomy And Biomechanics Nikhil N Verma, MD Director, Division of Sports Medicine Professor, Department of Orthopedics Rush University Medical Center Team Physician, Chicago White Sox and Bulls I
Type II SLAP lesions are created when the biceps anchor has pulled away from the glenoid attachment.
 Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
MEDIAL ELBOW INSTABILITY
 MEDIAL ELBOW INSTABILITY Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA Royalties: none Stock: none Stock option: Cayenne
MEDIAL ELBOW INSTABILITY Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA Royalties: none Stock: none Stock option: Cayenne
Slide 1. Slide 2. Slide 3. The Thrower s Elbow: When to Operate. Medial Elbow Pain in the Athlete. Goal of This Talk
 Slide 1 The Thrower s Elbow: When to Operate Luke S. Oh, MD Massachusetts General Hospital Team Physician, Boston Red Sox Team Physician, New England Revolution Consultant, Harvard University Athletics
Slide 1 The Thrower s Elbow: When to Operate Luke S. Oh, MD Massachusetts General Hospital Team Physician, Boston Red Sox Team Physician, New England Revolution Consultant, Harvard University Athletics
The Elbow. The Elbow. The Elbow 12/11/2017. Oak Ridge High School Conroe, Texas. Compose of three bones. Ligaments of the Elbow
 Oak Ridge High School Conroe, Texas Compose of three bones The humerus The radius The ulna Ligaments of the Elbow Ulnar collateral ligament Radial collateral ligament Annular ligament 1 The elbow is considered
Oak Ridge High School Conroe, Texas Compose of three bones The humerus The radius The ulna Ligaments of the Elbow Ulnar collateral ligament Radial collateral ligament Annular ligament 1 The elbow is considered
Upper Extremity Injuries in Youth Baseball: Causes and Prevention
 Upper Extremity Injuries in Youth Baseball: Causes and Prevention Biomechanics Throwing a baseball is an unnatural movement Excessively high forces are generated at the elbow and shoulder Throwing requires
Upper Extremity Injuries in Youth Baseball: Causes and Prevention Biomechanics Throwing a baseball is an unnatural movement Excessively high forces are generated at the elbow and shoulder Throwing requires
No financial disclosures
 Thomas J. Noonan, MD Steadman Hawkins Clinic Denver University of Colorado No financial disclosures Thomas Noonan, Gregory Ford, James Genuario, Jason Kinkartz, Thomas Githens, Scott Murayama Steadman
Thomas J. Noonan, MD Steadman Hawkins Clinic Denver University of Colorado No financial disclosures Thomas Noonan, Gregory Ford, James Genuario, Jason Kinkartz, Thomas Githens, Scott Murayama Steadman
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency
 Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency Justin E. Chronister, MD 1, Randal P. Morris, BS 2, Clark R. Andersen, MS 2, J. Michael Bennett, MD 3, Thomas
Biomechanics of Two Reconstruction Techniques for Elbow Ulnar Collateral Ligament Insufficiency Justin E. Chronister, MD 1, Randal P. Morris, BS 2, Clark R. Andersen, MS 2, J. Michael Bennett, MD 3, Thomas
Other Elbow Concerns in Overhead Athletes
 Other Elbow Concerns in Overhead Athletes John A. Steubs, M.D. Team Physician, Minnesota Twins TRIA Orthopaedic Center Disclosures None relevant to this presentation. Other Elbow Problems Valgus extension
Other Elbow Concerns in Overhead Athletes John A. Steubs, M.D. Team Physician, Minnesota Twins TRIA Orthopaedic Center Disclosures None relevant to this presentation. Other Elbow Problems Valgus extension
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Elbow injuries in athletes
 Elbow injuries in athletes Babette Pluim IOC Advanced Team Physician s Course, Oslo Case # 1 13 yr old junior elite tennis player Medial and lateral elbow pain 24-month history with episodes of elbow pain,
Elbow injuries in athletes Babette Pluim IOC Advanced Team Physician s Course, Oslo Case # 1 13 yr old junior elite tennis player Medial and lateral elbow pain 24-month history with episodes of elbow pain,
Elbow Injuries in the Throwing Athlete
 Elbow Injuries in the Throwing Athlete Overhand throwing places extremely high stresses on the elbow. In baseball pitchers and other throwing athletes, these high stresses are repeated many times and can
Elbow Injuries in the Throwing Athlete Overhand throwing places extremely high stresses on the elbow. In baseball pitchers and other throwing athletes, these high stresses are repeated many times and can
Arthroscopic Anterior Stabilization Rehab
 Arthroscopic Anterior Stabilization Rehab Phase I (0-3weeks) Sling immobilization-md directed Codmans/Pendulum exercises Wrist/Elbow ROM Gripping exercises FF-AAROM (supine)-limit to 90 o ER to 0 o Sub
Arthroscopic Anterior Stabilization Rehab Phase I (0-3weeks) Sling immobilization-md directed Codmans/Pendulum exercises Wrist/Elbow ROM Gripping exercises FF-AAROM (supine)-limit to 90 o ER to 0 o Sub
MUCL REPAIR. Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA
 MUCL REPAIR Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA MUCL INJURY EPIDEMIC Frequency increasing despite major efforts
MUCL REPAIR Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA MUCL INJURY EPIDEMIC Frequency increasing despite major efforts
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline
 Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Risk Factors Leading to UCL Reconstruction and Revision Surgery: A Case Report of a Division I Collegiate Pitcher
 Skyline - The Big Sky Undergraduate Journal Volume 2 Issue 1 Article 2 2014 Risk Factors Leading to UCL Reconstruction and Revision Surgery: A Case Report of a Division I Collegiate Pitcher Taylor M. Bennett
Skyline - The Big Sky Undergraduate Journal Volume 2 Issue 1 Article 2 2014 Risk Factors Leading to UCL Reconstruction and Revision Surgery: A Case Report of a Division I Collegiate Pitcher Taylor M. Bennett
Jin-Young Park, MD, Kyung-Soo Oh, MD, Seung-Chul Bahng, MD, Seok-Won Chung, MD, Jin-Ho Choi, MD
 Original Article Clinics in Orthopedic Surgery 2014;6:190-195 http://dx.doi.org/10.4055/cios.2014.6.2.190 Does Well Maintained Graft Provide Consistent Return to Play after Medial Ulnar Collateral Ligament
Original Article Clinics in Orthopedic Surgery 2014;6:190-195 http://dx.doi.org/10.4055/cios.2014.6.2.190 Does Well Maintained Graft Provide Consistent Return to Play after Medial Ulnar Collateral Ligament
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Sterile gauze used at incision site. Check brace for rubbing or irritation. Compression garment at elbow to be used with physician s authorization
 ULNAR COLLATERAL LIGAMENT RECONSTRUCTION GUIDELINE Functional Outcome Measure KJOC (Appendix 1) should be completed at initial evaluation and at all identified times through guideline, Phase 1 Immediate
ULNAR COLLATERAL LIGAMENT RECONSTRUCTION GUIDELINE Functional Outcome Measure KJOC (Appendix 1) should be completed at initial evaluation and at all identified times through guideline, Phase 1 Immediate
A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) William T. Grant, MD
 A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh,
A Patient s Guide to Medial Epicondylitis (Golfer s Elbow) Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh,
Adam J. Seidl, MD Assistant Professor University of Colorado School of Medicine Shoulder & Elbow Surgery Division of Sports Medicine and Shoulder
 Adam J. Seidl, MD Assistant Professor University of Colorado School of Medicine Shoulder & Elbow Surgery Division of Sports Medicine and Shoulder Surgery Division of Hand, Wrist, and Elbow Surgery Anatomy
Adam J. Seidl, MD Assistant Professor University of Colorado School of Medicine Shoulder & Elbow Surgery Division of Sports Medicine and Shoulder Surgery Division of Hand, Wrist, and Elbow Surgery Anatomy
Recurrent and Chronic Elbow Instability
 Recurrent and Chronic Elbow Instability Elbow instability is a looseness in the elbow joint that may cause the joint to catch, pop, or slide out of place during certain arm movements. It most often occurs
Recurrent and Chronic Elbow Instability Elbow instability is a looseness in the elbow joint that may cause the joint to catch, pop, or slide out of place during certain arm movements. It most often occurs
The Cryo/Cuff provides two functions: 1. Compression - to keep swelling down. 2. Ice Therapy - to keep swelling down and to help minimize pain. Patien
 The Cryo/Cuff provides two functions: 1. Compression - to keep swelling down. 2. Ice Therapy - to keep swelling down and to help minimize pain. Patients, for the most part, experience less pain and/or
The Cryo/Cuff provides two functions: 1. Compression - to keep swelling down. 2. Ice Therapy - to keep swelling down and to help minimize pain. Patients, for the most part, experience less pain and/or
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
Revision Tommy John. Disclosure. Revision UCL Recon 11/11/2016. Christopher S. Ahmad, MD
 Revision Tommy John Christopher S. Ahmad, MD Professor of Orthopaedic Surgery Chief of Sports Medicine Head Team Physician New York Yankees Disclosure 1. Basic Science Support a. Arthrex b. Smith-Nephew
Revision Tommy John Christopher S. Ahmad, MD Professor of Orthopaedic Surgery Chief of Sports Medicine Head Team Physician New York Yankees Disclosure 1. Basic Science Support a. Arthrex b. Smith-Nephew
Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521 ELBOW S/P LOOSE BODY REMOVAL PROTOCOL This rehabilitation protocol
Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521 ELBOW S/P LOOSE BODY REMOVAL PROTOCOL This rehabilitation protocol
Rehabilitation Guidelines for Large Rotator Cuff Repair
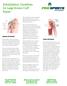 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
A Patient s Guide to Biceps Rupture. William T. Grant, MD
 A Patient s Guide to Biceps Rupture Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves
A Patient s Guide to Biceps Rupture Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer
 Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521 DISTAL BICEPS TENDON REPAIR PROTOCOL This rehabilitation protocol
Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521 DISTAL BICEPS TENDON REPAIR PROTOCOL This rehabilitation protocol
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
Grundkurs SGSM-SSMS Sion Sports Elbow. Dr Stéphane Kämpfen
 Grundkurs SGSM-SSMS Sion 2015 Sports Elbow Dr Stéphane Kämpfen Type of pathologies! Acute:! Fractures - dislocation! Sprain! Chronic:! Overload syndrome Fractures - Radial head: Mason classification Mason
Grundkurs SGSM-SSMS Sion 2015 Sports Elbow Dr Stéphane Kämpfen Type of pathologies! Acute:! Fractures - dislocation! Sprain! Chronic:! Overload syndrome Fractures - Radial head: Mason classification Mason
Functional Anatomy of the Elbow
 Functional Anatomy of the Elbow Orthopedic Institute Daryl C. Osbahr, M.D. Chief of Sports Medicine, Orlando Health Chief Medical Officer, Orlando City Soccer Club Orthopedic Consultant, Washington Nationals
Functional Anatomy of the Elbow Orthopedic Institute Daryl C. Osbahr, M.D. Chief of Sports Medicine, Orlando Health Chief Medical Officer, Orlando City Soccer Club Orthopedic Consultant, Washington Nationals
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX Tel#
 Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
---Start of Pediatric and Adolescent Upper Extremity Fractures---
 Presented by: Mary Lloyd Ireland Professor Dept. of Orthopaedic Surgery and Sports Medicine University of Kentucky Lexington KY www.marylloydireland.com ---Start of Pediatric and Adolescent Upper Extremity
Presented by: Mary Lloyd Ireland Professor Dept. of Orthopaedic Surgery and Sports Medicine University of Kentucky Lexington KY www.marylloydireland.com ---Start of Pediatric and Adolescent Upper Extremity
The Upper Limb. Elbow Rotation 4/25/18. Dr Peter Friis
 The Upper Limb Dr Peter Friis Elbow Rotation Depending upon the sport, the elbow moves through an arc of approximately 75⁰ to 100⁰ in about 20 to 35 msec. The resultant angular velocity is between 1185
The Upper Limb Dr Peter Friis Elbow Rotation Depending upon the sport, the elbow moves through an arc of approximately 75⁰ to 100⁰ in about 20 to 35 msec. The resultant angular velocity is between 1185
Cubital Tunnel Syndrome
 Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about must be made in conjunction with your Physician or a licensed healthcare provider.
Disclaimer This movie is an educational resource only and should not be used to manage Orthopaedic Health. All decisions about must be made in conjunction with your Physician or a licensed healthcare provider.
Biceps Tenodesis Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
A Patient s Guide to Elbow Dislocation
 A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
WRIST SPRAIN. Description
 WRIST SPRAIN Description Other sports, such as skiing, bowling, pole vaulting Wrist sprain is a violent overstretching and tearing of one Poor physical conditioning (strength and flexibility) or more ligaments
WRIST SPRAIN Description Other sports, such as skiing, bowling, pole vaulting Wrist sprain is a violent overstretching and tearing of one Poor physical conditioning (strength and flexibility) or more ligaments
Disclosures. UCL Reconstruction: Technical Variations 11/18/2016. UCLR: Technical Variations
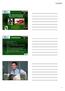 UCL Reconstruction: Technical Variations Anthony A. Romeo, MD Professor, Department of Orthopedics Rush University Medical Center Section Head, Shoulder and Elbow Chicago, Illinois Disclosures 1. Royalties:
UCL Reconstruction: Technical Variations Anthony A. Romeo, MD Professor, Department of Orthopedics Rush University Medical Center Section Head, Shoulder and Elbow Chicago, Illinois Disclosures 1. Royalties:
POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair)
 Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Biceps Tenodesis Protocol
 Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Aquatic Exercise. Rehabilitation after the SLAP lesion repair. I. Anatomy & Function SLAP 의가장흔한손상기전. Anatomy of the Shoulder (I)
 Aquatic Exercise Rehabilitation after the SLAP lesion repair Sports Medicine Clinic Sky 임승길 ATC 2 SLAP 의가장흔한손상기전 SLAP Superior Labrum Anterior to Posterior 1. Compression force Attempting to catch a heavy
Aquatic Exercise Rehabilitation after the SLAP lesion repair Sports Medicine Clinic Sky 임승길 ATC 2 SLAP 의가장흔한손상기전 SLAP Superior Labrum Anterior to Posterior 1. Compression force Attempting to catch a heavy
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME
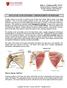 ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
MEDIAL EPICONDYLE FRACTURES
 MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
MEDIAL EPICONDYLE FRACTURES Demographic 20% of elbow fractures 60% of which are associated with elbow dislocation. 75% in boys between 6-12 years 20% of elbow dislocation with ME fracture, the ME is incarcerated
EPICONDYLITIS, LATERAL (Tennis Elbow)
 EPICONDYLITIS, LATERAL (Tennis Elbow) Description Expected Outcome Lateral epicondylitis (tennis elbow) is the most common painful condition of the elbow. Inflammation and pain occur on the outer side
EPICONDYLITIS, LATERAL (Tennis Elbow) Description Expected Outcome Lateral epicondylitis (tennis elbow) is the most common painful condition of the elbow. Inflammation and pain occur on the outer side
Overuse Injuries & special skeletal injuries Dr M.Taghavi Director of sport medicine center of olympic academy
 Overuse Injuries & special skeletal injuries Dr M.Taghavi Director of sport medicine center of olympic academy Prevalence of Overuse Injuries 30 to 50% of all sport injuries are from overuse In some sports
Overuse Injuries & special skeletal injuries Dr M.Taghavi Director of sport medicine center of olympic academy Prevalence of Overuse Injuries 30 to 50% of all sport injuries are from overuse In some sports
Early Elbow Motion Protocol Ligament Repair of the elbow
 499 Blossom Hill Rd, San Jose, Ca 95123 Tel: 408-268-8536 Fax: 408-268-8727 www.handsoncaretherapy.com Early Elbow Motion Protocol Ligament Repair of the elbow EARLY MOTION PROTOCOL 1-3 DAYS POST OP LIGAMENT
499 Blossom Hill Rd, San Jose, Ca 95123 Tel: 408-268-8536 Fax: 408-268-8727 www.handsoncaretherapy.com Early Elbow Motion Protocol Ligament Repair of the elbow EARLY MOTION PROTOCOL 1-3 DAYS POST OP LIGAMENT
Inspection. Physical Examination of the Elbow. Anterior Elbow 2/14/2017. Inspection. Carrying angle. Lateral dimple. Physical Exam of the Elbow
 of the Elbow Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Rush University President-Elect, American Shoulder Elbow Surgeons Team Physician, Chicago
of the Elbow Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Rush University President-Elect, American Shoulder Elbow Surgeons Team Physician, Chicago
After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection)
 After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection) Rehabilitation Protocol Phase 1: Weeks 0-4 Restrictions ROM 140 degrees of forward flexion 40 degrees of external
After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection) Rehabilitation Protocol Phase 1: Weeks 0-4 Restrictions ROM 140 degrees of forward flexion 40 degrees of external
Clinical Orthopaedic Rehabilitation Volume 1 and 2
 Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
Elbow Anatomy, Growth and Physical Exam. Donna M. Pacicca, MD Section of Sports Medicine Division of Orthopaedic Surgery Children s Mercy Hospital
 Elbow Anatomy, Growth and Physical Exam Donna M. Pacicca, MD Section of Sports Medicine Division of Orthopaedic Surgery Children s Mercy Hospital Contributing Factors to Elbow Injury The elbow is affected
Elbow Anatomy, Growth and Physical Exam Donna M. Pacicca, MD Section of Sports Medicine Division of Orthopaedic Surgery Children s Mercy Hospital Contributing Factors to Elbow Injury The elbow is affected
Anterior Labrum Repair Protocol
 Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Arm Pain in Throwing Athletes. Eric N. Hoeper, MD Primary Care Sports Medicine NorthShore University HealthSystem
 Arm Pain in Throwing Athletes Eric N. Hoeper, MD Primary Care Sports Medicine NorthShore University HealthSystem I have no potential conflicts of interest to declare. What s the Big Deal? Between 26% and
Arm Pain in Throwing Athletes Eric N. Hoeper, MD Primary Care Sports Medicine NorthShore University HealthSystem I have no potential conflicts of interest to declare. What s the Big Deal? Between 26% and
Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD
 General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
Upper Limb Biomechanics SCHOOL OF HUMAN MOVEMENT STUDIES
 Upper Limb Biomechanics Phases of throwing motion 1. Wind up Starts: initiate first movement Ends: lead leg is lifted & throwing hand removed from glove COG raised 2. Early Cocking Start: lead leg is lifted
Upper Limb Biomechanics Phases of throwing motion 1. Wind up Starts: initiate first movement Ends: lead leg is lifted & throwing hand removed from glove COG raised 2. Early Cocking Start: lead leg is lifted
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
The Biomechanics of the Human Upper Extremity-The Elbow Joint C. Mirzanli Istanbul Gelisim University
 The Biomechanics of the Human Upper Extremity-The Elbow Joint C. Mirzanli Istanbul Gelisim University Structure of The Elbow Joint A simple hinge joint, actually categorized as a trochoginglymus joint
The Biomechanics of the Human Upper Extremity-The Elbow Joint C. Mirzanli Istanbul Gelisim University Structure of The Elbow Joint A simple hinge joint, actually categorized as a trochoginglymus joint
Disclaimer. Evaluation & Treatment of Shoulder and Elbow Pain in the Adult Patient. Objectives. Anatomy
 Evaluation & Treatment of Shoulder and Elbow Pain in the Adult Patient William T. Crowe, RN-C, FNP, MSN, MBA Disclaimer! I, William T Crowe, have relevant financial relationships to be discussed, directly
Evaluation & Treatment of Shoulder and Elbow Pain in the Adult Patient William T. Crowe, RN-C, FNP, MSN, MBA Disclaimer! I, William T Crowe, have relevant financial relationships to be discussed, directly
SHOULDER INSTABILITY - DISLOCATION AND SUBLUXATION
 SHOULDER INSTABILITY - DISLOCATION AND SUBLUXATION THE INJURY The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade (scapula). The shallow
SHOULDER INSTABILITY - DISLOCATION AND SUBLUXATION THE INJURY The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade (scapula). The shallow
Elbow Injuries in Young Athletes!
 Elbow Injuries in Young Athletes! Andrew Martin DO, MBA, CAQSM! Director Sports Medicine Campbell University! Head Team Physician, Associate Professor Sports Medicine Disclosures None based on the content
Elbow Injuries in Young Athletes! Andrew Martin DO, MBA, CAQSM! Director Sports Medicine Campbell University! Head Team Physician, Associate Professor Sports Medicine Disclosures None based on the content
Biceps Tendon Tear at the Elbow
 DISEASES & CONDITIONS Biceps Tendon Tear at the Elbow The biceps muscle is located in the front of your upper arm. It is attached to the bones of the shoulder and elbow by tendons strong cords of fibrous
DISEASES & CONDITIONS Biceps Tendon Tear at the Elbow The biceps muscle is located in the front of your upper arm. It is attached to the bones of the shoulder and elbow by tendons strong cords of fibrous
Elbow Muscle Power Deficits
 1 Elbow Muscle Power Deficits ICD-9-CM code: 726.32 Lateral epicondylitis ICF codes: Activities and Participation code: d4300 Lifting, d4452 Reaching, d4401 Grasping Body Structure code: s73012 Muscles
1 Elbow Muscle Power Deficits ICD-9-CM code: 726.32 Lateral epicondylitis ICF codes: Activities and Participation code: d4300 Lifting, d4452 Reaching, d4401 Grasping Body Structure code: s73012 Muscles
Shoulder Arthroscopy with Rotator Cuff Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Pectorlais Major Tendon Repair
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Pectorlais Major Tendon Repair The pectoralis major muscle
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Pectorlais Major Tendon Repair The pectoralis major muscle
Shoulder Arthroscopy with Posterior Labral Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
ANTERIOR OPEN CAPSULAR SHIFT REHABILITATION PROTOCOL (Accelerated - Overhead Athlete)
 ANTERIOR OPEN CAPSULAR SHIFT REHABILITATION PROTOCOL (Accelerated - Overhead Athlete) This rehabilitation program's goal is to return the patient/athlete to their activity/sport as quickly and safely as
ANTERIOR OPEN CAPSULAR SHIFT REHABILITATION PROTOCOL (Accelerated - Overhead Athlete) This rehabilitation program's goal is to return the patient/athlete to their activity/sport as quickly and safely as
Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm)
 Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm) Therapist Phone I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity
Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm) Therapist Phone I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 Pectoralis Major Tendon Repair The pectoralis major is a thick, fan-shaped
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 Pectoralis Major Tendon Repair The pectoralis major is a thick, fan-shaped
A Patient s Guide to Labral Tears
 A Patient s Guide to Labral Tears Sports-related injuries require specialized care to promote optimum healing. Whether you are a weekend jogger or tennis player, a professional soccer player or marathon
A Patient s Guide to Labral Tears Sports-related injuries require specialized care to promote optimum healing. Whether you are a weekend jogger or tennis player, a professional soccer player or marathon
(PROTOCOL #18) REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
 The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Rehabilitation following Arthroscopic Rotator Cuff Repair: Medium Tears Phase I: Immediate Postsurgical Phase (Days 10-14) Precautions: No lifting of objects; No excessive arm motions; No excessive external
Rehabilitation following Arthroscopic Rotator Cuff Repair: Medium Tears Phase I: Immediate Postsurgical Phase (Days 10-14) Precautions: No lifting of objects; No excessive arm motions; No excessive external
Throwing Injuries and Prevention: The Physical Therapy Perspective
 Throwing Injuries and Prevention: The Physical Therapy Perspective Andrew M Jordan, PT, DPT, OCS Staff Physical Therapist, Cayuga Medical Center Physical Therapy and Sports Medicine ajordan@cayugamed.org
Throwing Injuries and Prevention: The Physical Therapy Perspective Andrew M Jordan, PT, DPT, OCS Staff Physical Therapist, Cayuga Medical Center Physical Therapy and Sports Medicine ajordan@cayugamed.org
Therapeutic Exercise Program for Epicondylitis (Tennis Elbow / Golfer s Elbow)
 Prepared for: Prepared by: Therapeutic (Tennis Elbow / Golfer s Elbow) To ensure that this exercise program is safe and effective for you, it should be performed under your doctor's supervision. Talk to
Prepared for: Prepared by: Therapeutic (Tennis Elbow / Golfer s Elbow) To ensure that this exercise program is safe and effective for you, it should be performed under your doctor's supervision. Talk to
ULNAR COLLATERAL LIGAMENT (UCL) RECONSTRUCTION REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
THERMAL - ASSISTED CAPSULORRAPHY With or without SLAP Repair
 THERMAL - ASSISTED CAPSULORRAPHY With or without SLAP Repair **It is important for the clinician to determine the capsular response to the heat probe. Patients that have excessive ROM early in the rehab
THERMAL - ASSISTED CAPSULORRAPHY With or without SLAP Repair **It is important for the clinician to determine the capsular response to the heat probe. Patients that have excessive ROM early in the rehab
P.O. Box Sierra Park Road Mammoth Lakes, CA Orthopedic Surgery & Sports Medicine
 P.O. Box 660 85 Sierra Park Road Mammoth Lakes, CA 93546 SHOULDER: Instability Dislocation Labral Tears The shoulder is the most mobile joint in the body, but to have this amount of motion, it is also
P.O. Box 660 85 Sierra Park Road Mammoth Lakes, CA 93546 SHOULDER: Instability Dislocation Labral Tears The shoulder is the most mobile joint in the body, but to have this amount of motion, it is also
