Reverse Total Shoulder
|
|
|
- Jane Loraine Hancock
- 6 years ago
- Views:
Transcription
1 Rehabilitation Protocol: Reverse Total Shoulder Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington Lahey Outpatient Center, Lexington Lahey Medical Center, Peabody Department of Rehabilitation Services Lahey Hospital & Medical Center, Burlington Lahey Hospital & Medical Center, Wall Street, Burlington Lahey Danvers Lahey Outpatient Center, Lexington
2 Overview The reverse total shoulder arthroplasty (rtsa) uses the deltoid as a replacement for the rotator cuff during elevation and abduction of the humerus. RTSA is indicated when there is a combination of a degenerative glenohumeral joint and an irreparable massive rotator cuff tear or rotator cuff arthropathy in a patient who is unable to actively elevate the arm above 90º. These conditions are most often seen in an elderly population. RTSA is also considered in patients with proximal humeral nonunion fractures, acute fractures, revision arthroplasties and pseudoparalysis. An intact deltoid is critical to the successful outcome of rtsa. The goal of rtsa is to restore deltoid tension and treat the underlying degeneration of the joint. With a nonfunctioning rotator cuff, the humeral head translates superiorly during contraction of the deltoid. The rtsa reverses the normal relationship between the scapular and humeral components, increasing the deltoid moment arm and deltoid tension to compensate for rotator cuff deficiency. With a rtsa the rotator cuff (RC) is either absent or minimally functional, therefore the rehabilitation approach for a patient following rtsa is distinctly different than the rehabilitation following a traditional total shoulder arthroplasty (TSA). Precautions for the rtsa are not only distinctly different than those for TSA but are also dependent upon the surgical approach. There are two surgical approaches to rtsa. One medializes the center of rotation, this is the approach primarily used at Lahey, the other lateralizes it. The choice of approach is dependent upon surgeon preference as well as several factors including proximal humeral bone loss, scapular anatomy, and surgical diagnosis (e.g., rotator cuff arthropathy vs failed arthroplasty). It is important to clarify the surgical approach with the surgeon prior to initiating post-operative rehabilitation. There is a higher risk of shoulder dislocation following rtsa than conventional TSA. If rtsa prostheses dislocate, they do so with combined internal rotation, adduction and extension. Patients can expect 80 to 140 of active elevation following rtsa, depending upon the underlying preoperative pathology of the shoulder. Complications of rtsa include instability, infection and neurovascular injury.
3 Phase I Immediate Post Surgical Phase Day 1 to Week 6 Goals Patient and family independent with joint protection Passive range of motion (PROM) Assisting with putting on and taking off sling/clothing Assisting with home exercise program (HEP) Cryotherapy Precautions - Sling is worn for 3-4 weeks. (May be extended to 6 weeks if rtsa is a revision surgery) - While lying supine, the elbow should be supported by towel roll to avoid shoulder extension. Patient should be instructed to always be able to visualize their elbow while lying supine. - NO Active Range of Motion (AROM) - NO lifting of objects with operative arm - Important to clarify surgical approach - With the Lateral Surgical approach ER to neutral only - Keep incision clean and dry (NO soaking/wetting for 2 weeks) - NO Whirlpool, Jacuzzi, ocean or lake wading for 4 weeks Days 1 to 4 - Begin PROM in supine - Scaption to 90º - External Rotation (ER) in the scapula plane to 20º-30º With the Lateral Surgical approach ER to neutral only - No internal Rotation (IR) ROM - Pendulum exercise with-in hours - Active assistive ROM of the cervical spine, elbow, wrist and hand - Pain free scapula isometric retraction - Insure that patient is independent in bed mobility, transfers and ambulation - Instruct patient and family in proper positioning, protection and written Home Exercise Program (HEP) - Frequent cryotherapy application 4-5 times a day for about 20 minutes
4 Protective Phase Days Continue all exercises as above - Begin submaximal pain-free deltoid isometrics in the scapula plane (Avoid shoulder extension) - Continue frequent Cryotherapy 4-5 times day for about twenty minutes - NO strengthening or resistance until 6 weeks Weeks 3-6 Progress exercise listed above Progress PROM: - Flexion and elevation in the scapular plane to 120º - ER in scapula plane to tolerance, respecting soft tissue constraints - With the Lateral Surgical approach initiate ER to tolerance at 4 6 weeks post op Gentle resisted exercise of the elbow, wrist and hand Continue cryotherapy Precautions At 4 weeks when sling is discontinued - Encourage normal arm swing and use of arm for light ADL s (feeding, writing) Criteria to progress to Phase II - Patient tolerates PROM and AROM and demonstrates isometric contraction of all components of the deltoid and periscapular muscles
5 Phase II Active ROM/Early strengthening phase Week 6-8 Goals - Continue progression of PROM (full PROM is not expected) - Gradually restore AROM - Control pain and inflammation - Allow for continued soft tissue healing - Re-establish dynamic shoulder and scapula stability Precautions - Continue to avoid shoulder hyperextension, horizontal adduction beyond neutral, or IR behind the back - In the presence of poor shoulder mechanics avoid repetitive shoulder AROM - Restrict lifting of objects to no heavier than a coffee cup - NO supporting of body weight by involved upper extremity Continue with PROM - At 6 weeks post op start PROM/AAROM IR to tolerance (not to exceed 50º in the scapula plane) - Begin shoulder A/AAROM as appropriate - Forward flexion and elevation in scapula plane supine with progression to sitting/standing (beach chair) - ER and IR in the scapula plane in supine with progression to sitting/standing - Begin gentle glenohumeral IR and ER submaximal pain free isometrics - Initiate gentle scapulothoracic rhythmic stabilization. - Begin gentle periscapular and deltoid sub-max pain free isotonic exercise (8 weeks) - Gentle glenohumeral and scapthoracic joint mobilization (grade I-II) as indicated Week 9-12 Continue with above exercises and functional activity progression - Begin light weight forward elevation (1-3 lbs) - Progress IR/ER isotonic strengthening (1-3 lbs) in side lying and /or light resistive bands. Criteria to progress Patient demonstrates the ability to isotonically activate all components of the deltoid and periscapular musculature is gaining strength.
6 Phase III Moderate strengthening Week 12+ Goals - Enhance functional use of the operative extremity and advance functional activities Precautions - NO Lifting of objects heavier than 6 lbs with the operative side - NO sudden lifting or pushing activities Continue with previous program as indicated - Progress to gentle resisted standing flexion/elevation Phase IV Continued HEP Typically 4+ months Goals - Patient is on a HEP performed 3-4 week focusing on strength and function Criteria for discharge from skilled therapy: Patient is able to maintain pain free AROM (typically 80º -120º of elevation with functional ER of about 30º). Patient is able to perform light household and work activities.
7 Post op Phase/Goals Range of Motion Precautions Phase 1 Immediate Postsurgical Day 1-4 Joint Protection (day 1-6 weeks) - Patient and family independent with joint protection PROM - Assisting with putting on and taking off sling - Assisting with Home Exercise Program (HEP) - Promote healing of soft tissue/maintain integrity of joint replacement - Enhance PROM of the shoulder - Restore AROM of elbow/wrist hand - Independence in activities of daily living (ADL s) with modification - Independent with transfers and ambulation as preadmission state Begin PROM in supine - Scaption plane to 90º - External Rotation (ER) in the scapula plane to 20º-30º - No internal Rotation (IR) ROM With the Lateral Surgical approach ER to neutral only - Pendulum exercise with-in hours - Active assistive ROM of the cervical spine, elbow, wrist and hand - Pain free scapula isometric retraction - Insure that patient is independent in bed mobility, transfers and ambulation - Instruct patient and family in proper positioning, protection and written Home Exercise Program(HEP) - Frequent cryotherapy application 4-5 times a day for about 20 minutes Important to clarify surgical approach Sling is worn for 3-4 weeks. (May be extended to 6 weeks if rtsa is a revision surgery) While lying supine, the elbow should be supported by towel roll to avoid shoulder extension. Patient should be instructed to always be able to visualize their elbow while lying supine. NO Active Range of Motion (AROM) NO lifting of objects with operated arm Keep incision clean and dry (NO soaking/wetting for 2 weeks) NO Whirlpool, Jacuzzi ocean or lake wading for 4 weeks
8 Post op Phase/Goals Range of Motion Precautions Day 5-21 Protective Phase - Continue all exercises as above - Begin sub maximal deltoid isometrics in the scapula plane (Avoid shoulder extension) - Continue frequent Cryotherapy 4-5 times day for about twenty minutes NO strengthening or resistance until 6 weeks 3-6 Weeks Progress exercise listed above Progress PROM: - Flexion in the scaption plane to 120º - ER in scapula plane to tolerance, respecting soft tissue constraints. With the Lateral Surgical approach initiate ER to tolerance at 4 6 weeks post op Gentle resisted exercise of the elbow, wrist and hand At 4 weeks when sling is discontinued - Encourage normal arm swing and use of arm of light ADL s (feeding, writing) Criteria to progress Continue cryotherapy Patient tolerates PROM and isometrics and AROM Patient demonstrates isometric contraction of all components of the deltoid and periscapular muscles
9 Post op Phase/Goals Range of Motion Precautions Phase II Week 6-8 Active ROM/strengthening phase Goals: - Continue progression of PROM (full PROM is not expected) - Gradually restore AROM - Control pain and inflammation - Allow for continued soft tissue healing - Re-establish dynamic shoulder and scapula stability Continue with PROM - At 6 weeks post op start PROM to tolerance (not to exceed 50º in the scapula plane) - Begin shoulder A/AAROM as appropriate - Forward flexion and elevation in scapula plane supine with progression to sitting/standing ER and IR in the scapula plane in the supine with progression to sitting/standing Continue to avoid shoulder hyperextension, horizontal adduction beyond neutral, or IR behind the back In the presence of poor shoulder mechanics avoid repetitive shoulder AROM Restrict lifting of objects to no heavier than a coffee cup NO supporting of body weight be involved upper extremity - Begin gentle glenohumeral IR and ER submax pain free isometrics Week Initiate gentle scapulothoracic rhythmic stabilization. Begin gentle periscapular and deltoid submax pain free isotonic exercise (8 weeks) - Gentle glenohumeral and scapthoracic joint mobilization (grade I-II) as indicated Continue with above exercises and functional activity progression - Begin light weight forward elevation (1-3 lbs) - Progress IR/ER isotonic strengthening (1-3 lbs) in side lying and /or light resistive bands.
10 Criteria to progress Patient tolerates PROM and isometrics and AROM - Patient demonstrated the ability to isometrically activate all components of the deltoid and periscapular muscles Post op Phase/Goals Range of Motion Precautions Phase II Week 6-8 Active ROM/strengthening phase Goals: - Continue progression of PROM (full PROM is not expected) - Gradually restore AROM - Control pain and inflammation - Allow for continued soft tissue healing - Re-establish dynamic shoulder and scapula stability Continue with PROM - At 6 weeks post op start PROM to tolerance (not to exceed 50º in the scapula plane) - Begin shoulder A/AAROM as appropriate - Forward flexion and elevation in scapula plane supine with progression to sitting/standing ER and IR in the scapula plane in the supine with progression to sitting/standing Continue to avoid shoulder hyperextension, horizontal adduction beyond neutral, or IR behind the back In the presence of poor shoulder mechanics avoid repetitive shoulder AROM Restrict lifting of objects to no heavier than a coffee cup NO supporting of body weight be involved upper extremity - Begin gentle glenohumeral IR and ER submax pain free isometrics - Initiate gentle scapulothoracic rhythmic stabilization. Begin gentle periscapular and deltoid submax pain free isotonic exercise (8 weeks) - Gentle glenohumeral and scapthoracic joint mobilization (grade I-II) as indicated
11 Post op Phase/Goals Range of Motion Precautions Week 9-12 Continue with above exercises and functional activity progression Criteria to progress Phase III Moderate strengthening Week 12+ Phase IV Continued HEP Typically 4+ months - Begin light weight forward elevation (1-3 lbs) - Progress IR/ER isotonic strengthening (1-3 lbs) in side lying and /or light resistive bands. Patient demonstrates the ability to isotonically activate all components of the deltoid and periscapular musculature is gaining strength Goals: Continue with previous program as - Enhance functional use of the indicated operative extremity and advance functional activities Goals: - Patient is on a HEP performed 3-4 week focusing on strength and function - Progress to gentle resisted standing flexion/elevation NO Lifting of objects heavier than 6 lbs with the operative side NO sudden lifting or pushing activities Criteria for discharge Patient is able to maintain pain free AROM, typically 80º-120º of elevation with functional ER of about 30º. Patient able to complete light household and work activities.
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Reverse Total Shoulder Protocol
 Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
(PROTOCOL #18) REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
 The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD
 General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL Shoulder
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL Shoulder
WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C
 WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C Post-Operative Rehabilitation Guidelines for Total Shoulder Arthroplasty (TSA) The intent of this protocol is to provide the physical therapist with a guideline/treatment
WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C Post-Operative Rehabilitation Guidelines for Total Shoulder Arthroplasty (TSA) The intent of this protocol is to provide the physical therapist with a guideline/treatment
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Total Shoulder Rehab Protocol Dr. Payne
 Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
PROM is not stretching!
 Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY
 Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol:
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol: General Information:
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol: General Information:
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) REHABILITATION AFTER REVERSE SHOULDER ARTHROPLASTY
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Orthopedic Surgery and Sports Medicine FL License:
 Reverse Shoulder Arthroplasty Protocol: The intent of this protocol is to provide the therapist with a guideline for the post-operative rehabilitation course of a patient that has undergone a Reverse Shoulder
Reverse Shoulder Arthroplasty Protocol: The intent of this protocol is to provide the therapist with a guideline for the post-operative rehabilitation course of a patient that has undergone a Reverse Shoulder
Christopher K. Jones, MD Colorado Springs Orthopaedic Group
 Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Total Shoulder Arthroplasty / Hemiarthroplasty Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Rehab protocol. Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits. Goals:
 Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty
 Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol
 Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY
 TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY Philosophy The following is an outline of the standard post-operative rehabilitation program following total shoulder arthroplasty.
TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY Philosophy The following is an outline of the standard post-operative rehabilitation program following total shoulder arthroplasty.
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Progression to the next phase based on clinical criteria and time frames as appropriate
 Indications Reverse total shoulder replacement is indicated for use in grossly rotator cuff deficient joints with severe arthropathy, or for use when a previous joint replacement has failed with a grossly
Indications Reverse total shoulder replacement is indicated for use in grossly rotator cuff deficient joints with severe arthropathy, or for use when a previous joint replacement has failed with a grossly
Rehabilitation Protocol: Massive Rotator Cuff Tear Repair
 Rehabilitation Protocol: Massive Rotator Cuff Tear Repair Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey
Rehabilitation Protocol: Massive Rotator Cuff Tear Repair Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines
 Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Jennifer L. Cook, MD Stephen A. Hanff, MD. Rotator Cuff Type I Repair (Small Large Tear)
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Important rehabilitation management concepts to consider for a postoperative physical therapy RSA program are:
 : General Information: Reverse or Inverse Shoulder Arthroplasty (RSA) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff damage,
: General Information: Reverse or Inverse Shoulder Arthroplasty (RSA) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff damage,
Biceps Tenotomy Protocol
 Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery. Phase 1: Immediate postoperative period (weeks 0-6) Goals
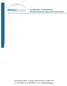 The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery Phase 1: Immediate postoperative period (weeks 0-6) Maintain/protect integrity of repair Gradually increase PROM Diminish
The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery Phase 1: Immediate postoperative period (weeks 0-6) Maintain/protect integrity of repair Gradually increase PROM Diminish
SHOULDER ARTHROSCOPY WITH ANTERIOR STABILIZATION / CAPSULORRHAPHY REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm)
 Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm) Therapist Phone I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity
Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm) Therapist Phone I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity
Arthroscopic Rotator Cuff Repair Protocol:
 Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Biceps Tenodesis Protocol
 Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Latissimus dorsi tendon transfer protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the physical therapist with a guideline/treatment protocol for the postoperative rehabilitation management
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the physical therapist with a guideline/treatment protocol for the postoperative rehabilitation management
REVERSE SHOULDER ARTHROPLASTY
 William J. Robertson, MD TMI Sports Medicine 3533 Matlock Rd Arlington, TX 76015 Office: (817) 419-0303 Fax: (817) 468-5963 www.billrobertsonmd.com www.hipkneepreservation.com REVERSE SHOULDER ARTHROPLASTY
William J. Robertson, MD TMI Sports Medicine 3533 Matlock Rd Arlington, TX 76015 Office: (817) 419-0303 Fax: (817) 468-5963 www.billrobertsonmd.com www.hipkneepreservation.com REVERSE SHOULDER ARTHROPLASTY
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer
 Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Shoulder Arthroscopy with Rotator Cuff Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Anterior Stabilization of the Shoulder: Distal Tibial Allograft
 Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Rehabilitation following Arthroscopic Rotator Cuff Repair: Medium Tears Phase I: Immediate Postsurgical Phase (Days 10-14) Precautions: No lifting of objects; No excessive arm motions; No excessive external
Rehabilitation following Arthroscopic Rotator Cuff Repair: Medium Tears Phase I: Immediate Postsurgical Phase (Days 10-14) Precautions: No lifting of objects; No excessive arm motions; No excessive external
TALLGRASS ORTHOPEDIC & SPORTS MEDICINE. Phase I Immediate Post-Surgical Phase (Weeks 0-2) Date: Maintain/protect integrity of the repair
 TALLGRASS ORTHOPEDIC & SPORTS MEDICINE Name: Date of Surgery: Patient Flow Sheet Arthroscopic Rotator Cuff Repair Small to Medium Tears Benedict Figuerres, MD Phase I Immediate Post-Surgical Phase (Weeks
TALLGRASS ORTHOPEDIC & SPORTS MEDICINE Name: Date of Surgery: Patient Flow Sheet Arthroscopic Rotator Cuff Repair Small to Medium Tears Benedict Figuerres, MD Phase I Immediate Post-Surgical Phase (Weeks
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 1 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 1 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
Shoulder Arthroscopy with Posterior Labral Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Total Shoulder Arthroplasty
 1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
Progression to the next phase based on Clinic Criteria and or Time Frames as Appropriate
 Bicep Tenodesis D. WATTS, M.D. Progression to the next phase based on Clinic Criteria and or Time Frames as Appropriate PHASE I PASSIVE RANG OF MOTION PHASE (STARTS APPROXIMATELY POST OP WEEKS 1-2) Minimize
Bicep Tenodesis D. WATTS, M.D. Progression to the next phase based on Clinic Criteria and or Time Frames as Appropriate PHASE I PASSIVE RANG OF MOTION PHASE (STARTS APPROXIMATELY POST OP WEEKS 1-2) Minimize
Biceps Tenotomy Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Biceps Tenodesis Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
ROTATOR CUFF REPAIR REHAB PROTOCOL
 Jayesh K. Patel, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX 75701 (903) 510-8840 ROTATOR CUFF REPAIR REHAB PROTOCOL This rehabilitation protocol has been developed for
Jayesh K. Patel, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX 75701 (903) 510-8840 ROTATOR CUFF REPAIR REHAB PROTOCOL This rehabilitation protocol has been developed for
Rotator Cuff Repair Protocol
 Protocol This rehabilitation protocol has been developed for the patient following a rotator cuff surgical procedure. This protocol will vary in length and aggressiveness depending on factors such as:
Protocol This rehabilitation protocol has been developed for the patient following a rotator cuff surgical procedure. This protocol will vary in length and aggressiveness depending on factors such as:
No Financial Disclosures
 Rehabilitation Following Total and Reverse Shoulder Arthroplasty, PT, DPT, SCS, CSCS No Financial Disclosures Total Shoulder Arthroplasty Arthritic shoulder increasing in prevalence More active as we age
Rehabilitation Following Total and Reverse Shoulder Arthroplasty, PT, DPT, SCS, CSCS No Financial Disclosures Total Shoulder Arthroplasty Arthritic shoulder increasing in prevalence More active as we age
REHABILITATION FOLLOWING OPEN AND MINI-OPEN ROTATOR CUFF REPAIR
 REHABILITATION FOLLOWING OPEN AND MINI-OPEN ROTATOR CUFF REPAIR Post-Operative Physical Therapy Protocol Philip A. Davidson M.D. Phase I Immediate Post-Surgical Phase (Week 1-2) Maintain integrity of the
REHABILITATION FOLLOWING OPEN AND MINI-OPEN ROTATOR CUFF REPAIR Post-Operative Physical Therapy Protocol Philip A. Davidson M.D. Phase I Immediate Post-Surgical Phase (Week 1-2) Maintain integrity of the
Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft
 Day of Surgery Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft A. Relax. Diet as tolerated. B. Icing is important for the first 5-7 days post-op. While the post-op
Day of Surgery Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft A. Relax. Diet as tolerated. B. Icing is important for the first 5-7 days post-op. While the post-op
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
AC reconstruction Protocol: Dr. Rolf
 AC reconstruction Protocol: Dr. Rolf The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient that has undergone a AC reconstruction
AC reconstruction Protocol: Dr. Rolf The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient that has undergone a AC reconstruction
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL BENJAMIN J. DAVIS, MD Type Two Rotator Cuff Repair
 I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity of the Repair Gradually Increase Passive Range of Motion Diminish Pain and Inflammation Prevent Muscular Inhibition Passive
I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity of the Repair Gradually Increase Passive Range of Motion Diminish Pain and Inflammation Prevent Muscular Inhibition Passive
Mini Open Rotator Cuff Repair Small Tears < 1 cm
 Mini Open Rotator Cuff Repair Small Tears < 1 cm **It is the treating therapist s responsibility along with the referring physician s guidance to determine the actual progression of the patient within
Mini Open Rotator Cuff Repair Small Tears < 1 cm **It is the treating therapist s responsibility along with the referring physician s guidance to determine the actual progression of the patient within
Latarjet Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol. Phase 1 Maximum Protection (0-4 weeks)
 Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol Goals for phase 1 Minimize Pain and inflammation Protect integrity of repair Initiate shoulder PROM Reduce muscular inhibition Maintain AROM of elbow,
Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol Goals for phase 1 Minimize Pain and inflammation Protect integrity of repair Initiate shoulder PROM Reduce muscular inhibition Maintain AROM of elbow,
Mini Open Rotator Cuff Repair Large (3 5 cm)
 Mini Open Rotator Cuff Repair Large (3 5 cm) Size: small = < 1 cm, medium = 1 3 cm, large 3 5 cm, massive = > 5 cm **It is the treating therapist s responsibility along with the referring physician s guidance
Mini Open Rotator Cuff Repair Large (3 5 cm) Size: small = < 1 cm, medium = 1 3 cm, large 3 5 cm, massive = > 5 cm **It is the treating therapist s responsibility along with the referring physician s guidance
Type II SLAP lesions are created when the biceps anchor has pulled away from the glenoid attachment.
 Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Shoulder Impingement Rehabilitation Recommendations
 Shoulder Impingement Rehabilitation Recommendations The following protocol can be utilized for conservative care of shoulder impingement as well as post- operative subacromial decompression (SAD) surgery.
Shoulder Impingement Rehabilitation Recommendations The following protocol can be utilized for conservative care of shoulder impingement as well as post- operative subacromial decompression (SAD) surgery.
BANKART REPAIR PROTOCOL
 BANKART REPAIR PROTOCOL Clarkstown Division This rehabilitation protocol has been developed for the patient following Bankart surgical procedure for anterior shoulder instability. The protocol is divided
BANKART REPAIR PROTOCOL Clarkstown Division This rehabilitation protocol has been developed for the patient following Bankart surgical procedure for anterior shoulder instability. The protocol is divided
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s R E V E R S E T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s R E V E R S E T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s R E V E R S E T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation
SLAP LESION REPAIR PROTOCOL
 SLAP LESION REPAIR PROTOCOL Clarkstown Division This rehabilitation protocol has been developed for the patient following a SLAP (Superior Labrum Anterior Posterior) repair. It is extremely important to
SLAP LESION REPAIR PROTOCOL Clarkstown Division This rehabilitation protocol has been developed for the patient following a SLAP (Superior Labrum Anterior Posterior) repair. It is extremely important to
Arthroscopic Anterior Stabilization Rehab
 Arthroscopic Anterior Stabilization Rehab Phase I (0-3weeks) Sling immobilization-md directed Codmans/Pendulum exercises Wrist/Elbow ROM Gripping exercises FF-AAROM (supine)-limit to 90 o ER to 0 o Sub
Arthroscopic Anterior Stabilization Rehab Phase I (0-3weeks) Sling immobilization-md directed Codmans/Pendulum exercises Wrist/Elbow ROM Gripping exercises FF-AAROM (supine)-limit to 90 o ER to 0 o Sub
Rotator Cuff Repair +/- Acromioplasty/Mumford. Phase I: 0 to 2 weeks after surgery
 Rotator Cuff Repair +/- Acromioplasty/Mumford 2. Ensure wound healing Phase I: 0 to 2 weeks after surgery 1. Sling: Use your sling all of the time. 2. Use of the affected arm: You may use your hand on
Rotator Cuff Repair +/- Acromioplasty/Mumford 2. Ensure wound healing Phase I: 0 to 2 weeks after surgery 1. Sling: Use your sling all of the time. 2. Use of the affected arm: You may use your hand on
Arthroscopic Bankart Repair Rehabilitation Protocol Dr. Mark Adickes
 Arthroscopic Bankart Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following an arthroscopic Bankart (anteroinferior labral
Arthroscopic Bankart Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following an arthroscopic Bankart (anteroinferior labral
Limited Goals Program (Examples Include: Cuff Tear Arthropathy, Massive Irrepairable Rotator Cuff Tear, Selected Revision Surgeries)
 Limited Goals Program (Examples Include: Cuff Tear Arthropathy, Massive Irrepairable Rotator Cuff Tear, Selected Revision Surgeries) All information contained in this protocol is to be used as general
Limited Goals Program (Examples Include: Cuff Tear Arthropathy, Massive Irrepairable Rotator Cuff Tear, Selected Revision Surgeries) All information contained in this protocol is to be used as general
 Appendix A: The American Society Of Shoulder And Elbow Therapists Arthroscopic Rotator Cuff Repair Rehabilitation Guide Phase 1 (POD 1 to ~ POW 6) GOALS: Maintain integrity of repair Minimize pain and
Appendix A: The American Society Of Shoulder And Elbow Therapists Arthroscopic Rotator Cuff Repair Rehabilitation Guide Phase 1 (POD 1 to ~ POW 6) GOALS: Maintain integrity of repair Minimize pain and
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation of patients
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation of patients
PHASE I (Begin PT 3-5 days post-op) DOS:
 REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIRS The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIRS The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
SLAP LESION REPAIR PROTOCOL Dr. Steven Flores
 SLAP LESION REPAIR PROTOCOL Dr. Steven Flores This rehabilitation protocol has been developed for the patient following a SLAP (Superior Labrum Anterior Posterior) repair. It is extremely important to
SLAP LESION REPAIR PROTOCOL Dr. Steven Flores This rehabilitation protocol has been developed for the patient following a SLAP (Superior Labrum Anterior Posterior) repair. It is extremely important to
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
REHABILITATION PROTOCOL ARTHROSCOPIC ROTATOR CUFF REPAIR (1 and 2 tendon repairs <4cm²)
 Phil Davidson M.D. Eric Heiden M.D. Karen Heiden M.D. 2200 Park Ave, Bld. D, Ste. 100 Park City, Utah 84060 435.615.8822 435.615.8823 fax REHABILITATION PROTOCOL ARTHROSCOPIC ROTATOR CUFF REPAIR (1 and
Phil Davidson M.D. Eric Heiden M.D. Karen Heiden M.D. 2200 Park Ave, Bld. D, Ste. 100 Park City, Utah 84060 435.615.8822 435.615.8823 fax REHABILITATION PROTOCOL ARTHROSCOPIC ROTATOR CUFF REPAIR (1 and
Reverse Total Shoulder Rehabilitation Protocol
 Reverse Total Shoulder Rehabilitation Protocol The Reverse Ball and Socket Arthroplasty is a new implant design for severely damaged shoulders. It is generally used for rotator cuff tear arthropathy, and
Reverse Total Shoulder Rehabilitation Protocol The Reverse Ball and Socket Arthroplasty is a new implant design for severely damaged shoulders. It is generally used for rotator cuff tear arthropathy, and
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s M A S S I V E R O T A T O R C U F F R E P A I R P R O T O C O L
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s M A S S I V E R O T A T O R C U F F R E P A I R P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation of patients
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s M A S S I V E R O T A T O R C U F F R E P A I R P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation of patients
REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR
 REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
Rehabilitation Guidelines for Large Rotator Cuff Repair
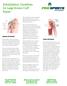 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Phase I: 0 to 3 weeks after surgery
 Dx: Right Left RTC (Massive) Repair Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: 2. Ensure wound healing Phase I:
Dx: Right Left RTC (Massive) Repair Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: 2. Ensure wound healing Phase I:
Rotator Cuff Repair Therapy Protocol
 Bart Eastwood D.O. 825 Davis st Blacksburg, VA 24060 540-951-6000 All information contained in this protocol is to be used as general guidelines only. Specific variations may be appropriate for each patient
Bart Eastwood D.O. 825 Davis st Blacksburg, VA 24060 540-951-6000 All information contained in this protocol is to be used as general guidelines only. Specific variations may be appropriate for each patient
SMALL-MEDIUM ROTATOR CUFF REPAIR GUIDELINE
 SMALL-MEDIUM ROTATOR CUFF REPAIR GUIDELINE The rotator cuff is responsible for stabilization and active movement of the glenohumeral joint. An acute or overuse injury may cause the rotator cuff to be injured
SMALL-MEDIUM ROTATOR CUFF REPAIR GUIDELINE The rotator cuff is responsible for stabilization and active movement of the glenohumeral joint. An acute or overuse injury may cause the rotator cuff to be injured
SLAP Lesion Type II Repair Rehabilitation Program
 SLAP Lesion Type II Repair Rehabilitation Program The GLSM SLAP Type II Repair Rehabilitation Program is an evidence-based and soft tissue healing dependent program allowing patients to progress to vocational
SLAP Lesion Type II Repair Rehabilitation Program The GLSM SLAP Type II Repair Rehabilitation Program is an evidence-based and soft tissue healing dependent program allowing patients to progress to vocational
Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521 ROTATOR CUFF REPAIR PROTOCOL This rehabilitation protocol has
Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521 ROTATOR CUFF REPAIR PROTOCOL This rehabilitation protocol has
REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMIAL DECOMPRESSION) Dr. Carson
 REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMIAL DECOMPRESSION) Dr. Carson The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMIAL DECOMPRESSION) Dr. Carson The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline
 Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are
MASSIVE ROTATOR CUFF REPAIR. REHABITATION PROTOCOL >3 cm
 MASSIVE ROTATOR CUFF REPAIR REHABITATION PROTOCOL >3 cm Phase I: (Protective Phase) Weeks 0 to 8 Goals: Minimize pain and inflammatory response Achieve ROM goals Establish stable scapula 1. Elbow, wrist
MASSIVE ROTATOR CUFF REPAIR REHABITATION PROTOCOL >3 cm Phase I: (Protective Phase) Weeks 0 to 8 Goals: Minimize pain and inflammatory response Achieve ROM goals Establish stable scapula 1. Elbow, wrist
OrthoCarolina. Arthroscopic SLAP Lesion (Type II) Repair Protocol
 OrthoCarolina Arthroscopic SLAP Lesion (Type II) Repair Protocol Surgical Overview: SLAP, which stands for superior labrum anterior to posterior, lesions are labral detachments that originate posterior
OrthoCarolina Arthroscopic SLAP Lesion (Type II) Repair Protocol Surgical Overview: SLAP, which stands for superior labrum anterior to posterior, lesions are labral detachments that originate posterior
Large/Massive Rotator Cuff Repair
 Large/Massive Rotator Cuff Repair 1. Defined a. Suturing of tears within the rotator cuff (most commonly supraspinatus muscle). Massive RCR usually involve more than the supraspinatus. b. May be done arthroscopically
Large/Massive Rotator Cuff Repair 1. Defined a. Suturing of tears within the rotator cuff (most commonly supraspinatus muscle). Massive RCR usually involve more than the supraspinatus. b. May be done arthroscopically
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT
 REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
