Andrew B. Stein, MD Boston University Medical Center May 2 & 3, 2016
|
|
|
- Donald Greer
- 5 years ago
- Views:
Transcription
1 Andrew B. Stein, MD Boston University Medical Center Work Related Workshop WorkInjuries Related Injuries Workshop
2 Tendon injuries may be obvious or subtle History (mechanism of injury) and PE should allow diagnosis X-ray usually indicated Ultrasound/MRI may be helpful
3 History Galen ( A.D.): in Ars Parva, stated that tendons composed of both ligaments & nerves, and that placing sutures in tendons would lead to pain, twitching, & eventual convulsions Avicenna (9th cent.): Arab surgeon, credited w/1st tendon repair Meekren (1682): 1st European to describe repair Albrecht von Haller (1752): Conclusively demonstrated insensibility of tendons, after which tenorrhaphy became accepted practice
4 Introduction Bunnell (1918, 1956): Because of inadequate suture materials & techniques frequent failure of primary repair strongly advised wound debridement & closure, followed by delayed tendon grafting Verdan & Kleinert (1950 s 1960 s): concluded that primary flexor tendon repair superior to delayed reconstruction Evolution of suture & rehabilitation techniques, importance of tendon sheath & pulleys re-emphasized
5 Tendon Nutrition: Vascularity From forearm into palm, blood supply received from segmental vessels arising from paratenon, entering the tendon & traveling longitudinally btwn fascicles In mid-prox. phalanx, tendons supplied by branches off digital arteries through the vincular system
6 Tendon Nutrition: Synovial Fluid Synovial fluid, formed principally by tendon sheaths, acts as medium for diffusion of nutrients to tendons Variety of studies (using tracers, etc.) have shown that synovial diffusion more important (Manske, et al, J Hand Surg 3:32, 1978)
7 Tendon Healing Previously thought that healing occurs by fibroblastic response of surrounding tissues whose own integrity has been violated Currently believed that tendons possess an intrinsic capacity to heal themselves without depending on extra-tendinous cells or adhesions
8 Tendon Healing Collagen synthesis seen w/in 1st wk after tendon repair; fibers initially laid down in random, disorganized fashion By 8 wks., fibers reorganized into more linear pattern, w/ crosslinking Tensile strength of flexor tendon repair site decreases between days 4-10, thereafter slowly increasing to near normal by 6 wks. (re-rupture seen late as 7 wks) Wait 8 weeks to start resistance/strengthening
9 Flexor Tendon Healing: Mobilization Gelberman et al: in vitro & in vivo studies showing repaired tendons subject early mobilization had consistently greater tensile strength, excursion (i.e. fewer adhesions), and ultimate function than those immobilized Adhesion formation associated primarily with immobilization Active mobilization may provide best environment Good OT critical to outcomes!
10 Emergency Room Care Irrigation and debridement of the wound Wound closure Update tetanus immunization Administer oral antibiotics Early referral for purpose of repair Within 2 weeks ideal (4 weeks generally upper limit for primary repair) 1 week for FDP avulsion injuries
11 Inspection for Wounds/Scars Note size and location of any acute wounds Can often predict likelihood of tendon damage just based upon location of wound & resting posture finger Painful digital flexion is suggestive of partial tendon injury
12 Testing for flexor digitorum profundus musculotendinous function
13 Testing flexor digitorum superficialis musculotendonious function
14 Zones of Flexor Tendon Injury Zone I Zone II Zone III Zone IV Zone V The classification of flexor tendon injuries using zones of the hand
15 Repair Fundamentals Zone II flexor tendon repair Restore anatomy Minimize tendon handling to avoid adhesions Create a smooth repair that allows gliding of the repair site Perform a repair that is strong enough to allow an early active motion rehabilitation method
16 Flexor Tendon Repair Should be done in the operating room Incorporate the existing laceration into surgical approach Focus on atraumatic tissue handling Choose a tendon repair method based on intra-operative findings and the anticipated rehabilitation method Start rehabilitation as soon as practical following repair
17 Surgical Approach Preserve A2 and A4 pulley Use cruciate pulley windows (A3) Raise flap of C1, A3 and C2 for exposure Preserve rim for possible later repair of sheath A2 A4
18 General Considerations: Suture Techniques Suture material: braided non-resorbable: nonreactive, pliable, strong Multiple suture techniques have been developed, Many different studies looking at in vivo and in vitro strengths of various techniques, with little agreement One technique has not been unequivocally accepted as the best
19 Primary & Delayed Primary Repair While primary repair is theoretically preferable, delayed primary may be performed without adversely effecting the end result (Green & Niebauer, JBJS, 1974) In some cases, delayed primary repair may be possible 6 weeks or more after injury In others, it may be impossible only 2 weeks after injury Therefore, have alternative plan (e.g., tendon grafting) in mind if repair found intra-operatively to be impossible
20 General Considerations: PostOperative Mobilization Based on data showing improved outcomes with early motion, immediate postoperative passive mobilization advocated. Variety of protocols Duran & Houser demonstrated that 3-5 mm extension motion sufficient to prevent adhesion formation
21 Partial Tendon Lacerations Unlikely need to repair lacerations under 50% Address triggering and tendon sheath 50%-75% lacerations probably repair Consider epitendinous only repair Repair if greater than 75% Include core suture
22 FDP Insertion Avulsion Common, esp. in athletes First described by von Zander (1891) Typically occurs in young males when playing football / rugby While attempting to to grasp a jersey, FDP eccentrically contracts as opponent pulls away, extending finger
23 FDP Avulsion Frequently a delay in treatment unless active DIP joint flexion tested specifically Vast majority involve ring finger, possibly because of weaker profundus tendon insertion in ring finger (Manske & Lesker, Hand, 1978)
24 FDP Avulsion: Classification (Leddy & Packer, J Hand Surg 2:66, 1977) Type I (least common): Tendon retracts all the way into palm beneath A1 pulley, vincula rupture, synovial fluid nutrient diffusion interrupted No active DIP flexion, excellent PIP flexion Tender mass in palm Reinsertion within 7-10 days before tendon contracts
25 Complications Re-rupture: 3-15%, usually within 2-3 wks of repair, occasionally as late as 7 weeks Adhesions / loss of ROM: occurs to some degree in nearly all pts.; >64% of pts had total loss of greater than 25 deg.
26 Tenolysis Surgical release of flexor tendons from their restricting adhesions Indicated when passive flexion significantly exceeds active flexion at a joint, suggesting restriction of flexor tendon excursion by adhesions Prerequisites: healed Fxs; full passive ROM (no joint contractures); tissue equilibrium; compliant/motivated patient
27 Tenolysis Timing: Controversial, based on conflicting animal and clinical data Not before 3 mos, possibly not until 6 mos. Some advocate performing the procedure under local anesthesia, allowing the pt to actively flex the digit intra-operatively to assess tendon excursion Technically demanding
28 Tenolysis Early (within 12 hours) aggressive therapy must be initiated Significant complication rate, especially tendon rupture in the post-operative period Pt should be prepared for ultimate tendon grafting if primary repair impossible
29 Flexor Tendon Reconstruction (Failed Repair) Two stage Silicone rod insertion and pulley reconstruction, followed by second stage graft Procedures are done approximately 3-6 months apart
30 Extensor Injuries
31 Extensors at the Wrist Wrist encompasses six discrete dorsal compartments that contain the extensor tendons
32 Zone 1: terminal tendon Zone 2: triangular ligament Zone 3: central slip Zone 4: over proximal phalanx Zone 5: over metacarpal phalangeal joint Zone 6: over metacarpals Other (7, 8, 9): proximal Zones of extensor tendon injury Work Related Workshop WorkInjuries Related Injuries Workshop
33 Extensor Tendon Injuries Occur following dorsal hand or digit laceration Also commonly occur by avulsion of the tendon from its site of insertion by blunt trauma
34 Closed Injuries More likely to be overlooked or misdiagnosed Distinguish from ligament injuries/fractures X-rays Consider ultrasound/mri
35 Anatomy of the Extensor Apparatus
36 Principle A more predictable result, in terms of full active digital flexion and extension (ie no extensor lag at either the DIP or the PIP joints) may be expected if the tendon heals without formation of a repair site gap
37 Even a small gap formation at the extensor tendon repair site leads to digital extensor lag Early diagnosis and treatment of injury of the extensor mechanism is as important as the treatment of flexor tendon injuries If external splints cannot keep the digit immobilized effectively, consider trans-articular fixation with Kwires and/or tendon repair
38 Loss of Terminal DIP Extension Mallet Finger Swan neck deformity
39 Closed Injuries Zone 1: Tendinous Mallet Loss of terminal extension of the DIP Usually as a result of forced flexion of the DIP Splint DIP in extension for 6-8 weeks Then 6-8 weeks night-time splinting Either a dorsal or a volar splint is acceptable Consider pinning if patient can t tolerate splint?earlier RTW
40 Zone 1: Tendinous Mallet Treatment Continuous splinting for 6 weeks Monitor the patient for skin problems Work Related Workshop WorkInjuries Related Injuries Workshop
41 Closed Injuries Zone 1: Bony Mallet Mallet injury that is associated with a fracture of the distal phalanx Diagnosis confirmed by the appearance on lateral radiograph Generally do well with splinting (4 wks.) May require surgical repair if there is palmar translation of the distal phalanx
42 Loss of Active PIP Extension Boutonniere Deformity
43 Zone 3 Central slip injury/avulsion Boutonniere deformity (flexion of the PIP and hyperextension of the DIP) develops if lateral bands subluxate palmar to axis of rotation of PIP joint The majority of patients can be treated with closed reduction and extension splinting of the PIP joint Work Related Workshop WorkInjuries Related Injuries Workshop
44 Zone 3 Central slip injury/avulsion Treated by splinting the PIP joint in extension for 6 weeks Active DIP flexion exercised with the middle phalanx blocked is done during the period of immobilization Work Related Workshop WorkInjuries Related Injuries Workshop
45 Stiffness Following Tendon Repair Incomplete flexion of the MCP, PIP and DIP joints may develop following a dorsal injury from loss of tendon excursion or from joint contracture Restoration of full digital flexion and extension may require greater than one surgical procedure
46 Extensor Tendon Adhesions Peritendinous adhesions limit tendon excursion Early intensive post-op occupational therapy is important to maintain the range of motion obtained at surgery Digital stiffness following extensor tendon repair or healing can often be treated successfully with outpatient hand therapy Extensor tenolysis may be useful to regain digital flexion as well as digital extension
47 Approach to the Stiff Finger Treatment is Elective (Choose patients carefully) Compliant patient Pain controllable- narcotics, NSAIDs Employer s understanding Have focused GOALS: Restore power grip? Restore active extension? Restore hand s ability to get into tight spaces?
48 Summary Early diagnosis of traumatic tendon injuries helpful Compliant patient/appropriate OT as important as surgery for achieving good outcome Full recovery often prolonged even in ideal situation There are no shortcuts Employer should be aware
49 Thank You! Boston Medical Center
50 F/U to 1st Case Multiple MCP Fxs & Tendon Loss Plates & Hunter Rods
51 Groin Flap for Coverage Result
FINGER INJURIES. Chapter 24, pgs ,
 FINGER INJURIES Chapter 24, pgs 727 730, 741 743 1. Demonstrate mastery of anatomical references to the hand and fingers. 2. Compare and contrast Mallet Finger, Swan Neck Deformity and Boutonnière Deformity.
FINGER INJURIES Chapter 24, pgs 727 730, 741 743 1. Demonstrate mastery of anatomical references to the hand and fingers. 2. Compare and contrast Mallet Finger, Swan Neck Deformity and Boutonnière Deformity.
5/8/2017. Finger Injuries in Football. Tendon Injuries of the Hand and Wrist in Football Steve Kronlage, MD Andrews Institute Gulf Breeze, Florida
 Finger Injuries in Football Tendon Injuries of the Hand and Wrist in Football Steve Kronlage, MD Andrews Institute Gulf Breeze, Florida A jammed finger is an injury (at very least a torn ligament) A swollen
Finger Injuries in Football Tendon Injuries of the Hand and Wrist in Football Steve Kronlage, MD Andrews Institute Gulf Breeze, Florida A jammed finger is an injury (at very least a torn ligament) A swollen
Swan-Neck Deformity. Introduction. Anatomy
 Swan-Neck Deformity Introduction Normal finger position and movement occur from the balanced actions of many important structures. Ligaments support the finger joints. Muscles hold and move the fingers.
Swan-Neck Deformity Introduction Normal finger position and movement occur from the balanced actions of many important structures. Ligaments support the finger joints. Muscles hold and move the fingers.
Clinical Orthopaedic Rehabilitation Volume 1 and 2
 Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
Clinical Orthopaedic Rehabilitation Volume 1 and 2 COURSE DESCRIPTION This program is a practical, clinical guide that provides guidance on the evaluation, differential diagnosis, treatment, and rehabilitation
11/13/2017. Complications of Flexor Tendon Repair. Brandon E. Earp, M.D. How do we best get there?
 Complications of Flexor Tendon Repair Brandon E. Earp, M.D. Chief of Orthopaedic Surgery Brigham and Women s Faulkner Hospital Vice-Chair of Clinical Operations Brigham and Women s Hospital Frontiers in
Complications of Flexor Tendon Repair Brandon E. Earp, M.D. Chief of Orthopaedic Surgery Brigham and Women s Faulkner Hospital Vice-Chair of Clinical Operations Brigham and Women s Hospital Frontiers in
The Rheumatoid Hand Deformities & Management. Dr. Anirudh Sharma Resident Department of Orthopedics
 + The Rheumatoid Hand Deformities & Management Dr. Anirudh Sharma Resident Department of Orthopedics + Why is Rheumatoid Arthritis important? + RA is a very debilitating disease median life expectancy
+ The Rheumatoid Hand Deformities & Management Dr. Anirudh Sharma Resident Department of Orthopedics + Why is Rheumatoid Arthritis important? + RA is a very debilitating disease median life expectancy
Interesting Case Series. Zone I Flexor Tendon Injuries
 Interesting Case Series Zone I Flexor Tendon Injuries Evgenios Evgeniou, MBBS, MRCS, a and Harriet Walker, MBBS, MRCS b a North Bristol NHS Trust, Bristol, United Kingdom, b Plymouth Hospitals NHS Trust,
Interesting Case Series Zone I Flexor Tendon Injuries Evgenios Evgeniou, MBBS, MRCS, a and Harriet Walker, MBBS, MRCS b a North Bristol NHS Trust, Bristol, United Kingdom, b Plymouth Hospitals NHS Trust,
Hand injuries. The metacarpal bones may fracture through the base, shaft or the neck.
 Hand injuries Metacarpal injuries The metacarpal bones may fracture through the base, shaft or the neck. Shaft fractures; these are caused by direct trauma which may cause transverse # of one or more metacarpal
Hand injuries Metacarpal injuries The metacarpal bones may fracture through the base, shaft or the neck. Shaft fractures; these are caused by direct trauma which may cause transverse # of one or more metacarpal
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 The Stiff Hand: Boutonniere & Sylvia Dávila, PT, CHT San Antonio, Texas Extensor Mechanism Central slip inserts into base of the middle phalanx Lateral bands lie dorsal to the PIP joint center of rotation
The Stiff Hand: Boutonniere & Sylvia Dávila, PT, CHT San Antonio, Texas Extensor Mechanism Central slip inserts into base of the middle phalanx Lateral bands lie dorsal to the PIP joint center of rotation
MR: Finger and Thumb Injuries
 MR: Finger and Thumb Injuries Laura W. Bancroft, M.D. Professor of Radiology University of Central Florida Florida State University Outline Normal anatomy of the fingers and thumb MR imaging protocols
MR: Finger and Thumb Injuries Laura W. Bancroft, M.D. Professor of Radiology University of Central Florida Florida State University Outline Normal anatomy of the fingers and thumb MR imaging protocols
Reversing PIP Joint Contractures:
 Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System John M. Agee M.D. Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System
Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System John M. Agee M.D. Reversing PIP Joint Contractures: Applicability of the Digit Widget External Fixation System
Revisiting the Curtis Procedure for Boutonniere Deformity Correction
 180 Letter to Editor Revisiting the Curtis Procedure for Boutonniere Deformity Correction Lee Seng Khoo*, Vasco Senna-Fernandes Ivo Pitanguy Institute, Rua Dona Mariana 65, Botafogo, Rio De Janeiro, Brazil
180 Letter to Editor Revisiting the Curtis Procedure for Boutonniere Deformity Correction Lee Seng Khoo*, Vasco Senna-Fernandes Ivo Pitanguy Institute, Rua Dona Mariana 65, Botafogo, Rio De Janeiro, Brazil
Fractures of the Hand in Children Which are simple? And Which have pitfalls??
 Fractures of the Hand in Children Which are simple? And Which have pitfalls?? Kaye E Wilkins DVM, MD Professor of Orthopedics and Pediatrics Departments of Orthopedics and Pediatrics University of Texas
Fractures of the Hand in Children Which are simple? And Which have pitfalls?? Kaye E Wilkins DVM, MD Professor of Orthopedics and Pediatrics Departments of Orthopedics and Pediatrics University of Texas
A Patient s Guide to Adult Finger Fractures
 A Patient s Guide to Adult Finger Fractures 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 1 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Adult Finger Fractures 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 1 DISCLAIMER: The information in this booklet is compiled from a variety
Hand Fractures: When is closed treatment OK? Epidemiology in USA: Metacarpal fractures: Page 1
 Hand Fractures: When is closed treatment OK? Robert J Strauch MD Professor of Orthopaedic Surgery Columbia University New York City Epidemiology in USA: 2009 Distal radius fx s: 16/10,000 Phalangeal fx
Hand Fractures: When is closed treatment OK? Robert J Strauch MD Professor of Orthopaedic Surgery Columbia University New York City Epidemiology in USA: 2009 Distal radius fx s: 16/10,000 Phalangeal fx
Physical therapy of the wrist and hand
 Physical therapy of the wrist and hand Functional anatomy wrist and hand The wrist includes distal radius, scaphoid, lunate, triquetrum, pisiform, trapezium, trapezoid, capitate, and hamate. The hand includes
Physical therapy of the wrist and hand Functional anatomy wrist and hand The wrist includes distal radius, scaphoid, lunate, triquetrum, pisiform, trapezium, trapezoid, capitate, and hamate. The hand includes
PIP Joint Injuries of the Finger A Patient's Guide to PIP Joint Injuries of the Finger
 PIP Joint Injuries of the Finger A Patient's Guide to PIP Joint Injuries of the Finger Introduction We use our hands constantly, placing them in harm's way continuously. Injuries to the finger joints are
PIP Joint Injuries of the Finger A Patient's Guide to PIP Joint Injuries of the Finger Introduction We use our hands constantly, placing them in harm's way continuously. Injuries to the finger joints are
FACTORS INFLUENCING THE MANAGEMENT OF THE FLEXOR TENDON INJURIES IN THE HAND
 Basrah Journal of Surgery FACTORS INFLUENCING THE MANAGEMENT OF THE FLEXOR TENDON INJURIES IN THE HAND Avadis F.I.C.M.S. Lecturer in Orthopaedic, Department of Surgery, College of Medicine, and specialist
Basrah Journal of Surgery FACTORS INFLUENCING THE MANAGEMENT OF THE FLEXOR TENDON INJURIES IN THE HAND Avadis F.I.C.M.S. Lecturer in Orthopaedic, Department of Surgery, College of Medicine, and specialist
AROM of DIP flex/ext, 10 reps hourly.
 BRIGHAM AND WOMEN S HOSPITAL A Teaching Affiliate of Harvard Medical School 75 Francis St. Boston, Massachusetts 02115 Department of Rehabilitation Services Physical Therapy The intent of this protocol
BRIGHAM AND WOMEN S HOSPITAL A Teaching Affiliate of Harvard Medical School 75 Francis St. Boston, Massachusetts 02115 Department of Rehabilitation Services Physical Therapy The intent of this protocol
Hand Anatomy A Patient's Guide to Hand Anatomy
 Hand Anatomy A Patient's Guide to Hand Anatomy Introduction Few structures of the human anatomy are as unique as the hand. The hand needs to be mobile in order to position the fingers and thumb. Adequate
Hand Anatomy A Patient's Guide to Hand Anatomy Introduction Few structures of the human anatomy are as unique as the hand. The hand needs to be mobile in order to position the fingers and thumb. Adequate
Extensor Tendon Repair Zones II, III, IV
 Zones II, III, IV D. WATTS, MD Indications Lacerations to the central slip, lateral bends and/or triangular ligament Rupture of the central slip in association with a PIP joint volar dislocation Avulsion
Zones II, III, IV D. WATTS, MD Indications Lacerations to the central slip, lateral bends and/or triangular ligament Rupture of the central slip in association with a PIP joint volar dislocation Avulsion
Mallet Baseball Finger
 Mallet Baseball Finger Introduction When you think about how much we use our hands, it's not hard to understand why injuries to the fingers are common. Most of these injuries heal without significant problems.
Mallet Baseball Finger Introduction When you think about how much we use our hands, it's not hard to understand why injuries to the fingers are common. Most of these injuries heal without significant problems.
Wrist and Hand Complaints
 Wrist and Hand Complaints Charles S. Day, M.D., M.B.A. Chief, Hand & Upper Extremity Surgery St. Elizabeth s Medical Center Tufts University School of Medicine Primary Care Internal Medicine 2018 Outline
Wrist and Hand Complaints Charles S. Day, M.D., M.B.A. Chief, Hand & Upper Extremity Surgery St. Elizabeth s Medical Center Tufts University School of Medicine Primary Care Internal Medicine 2018 Outline
Fractures and dislocations of the fingers
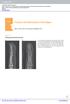 Chapter 1 Fractures and dislocations of the fingers Felix S. Chew, M.D., and Catherine Maldjian, M.D. Case 1 1 Phalangeal tuft avulsion fracture 31-year-old woman injured in a ground-level fall. Lateral
Chapter 1 Fractures and dislocations of the fingers Felix S. Chew, M.D., and Catherine Maldjian, M.D. Case 1 1 Phalangeal tuft avulsion fracture 31-year-old woman injured in a ground-level fall. Lateral
Interesting Case Series. Swan-Neck Deformity in Cerebral Palsy
 Interesting Case Series Swan-Neck Deformity in Cerebral Palsy Leyu Chiu, BA, a Nicholas S. Adams, MD, a,b and Paul A. Luce, MD, a,b,c a Michigan State University College of Human Medicine, Grand Rapids,
Interesting Case Series Swan-Neck Deformity in Cerebral Palsy Leyu Chiu, BA, a Nicholas S. Adams, MD, a,b and Paul A. Luce, MD, a,b,c a Michigan State University College of Human Medicine, Grand Rapids,
What you don t want to miss
 March 25, 2009 Vishal Michael Shah, M.D. What you don t want to miss Spectrum of Injuries Contusions Sprains Dislocations Fractures Lacerations Tendon Avulsions Ligament Tears Overuse Injuries FINGER
March 25, 2009 Vishal Michael Shah, M.D. What you don t want to miss Spectrum of Injuries Contusions Sprains Dislocations Fractures Lacerations Tendon Avulsions Ligament Tears Overuse Injuries FINGER
8 Recovering From HAND FRACTURE SURGERY
 8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
Classification of Established Volkmann s Ischemic Contracture and the Program for Its Treatment
 10 Classification of Established Volkmann s Ischemic Contracture and the Program for Its Treatment In spite of the advances made in preventive treatment of muscular ischemia at the forearm and hand, there
10 Classification of Established Volkmann s Ischemic Contracture and the Program for Its Treatment In spite of the advances made in preventive treatment of muscular ischemia at the forearm and hand, there
Kristin Kelley, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville Trauma/Fractures
 WRIST/HAND PATHOLOGY Kristin Kelley, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Trauma/Fractures Hook of Hamate Fractures Triangular Fibrocartilage Complex (TFCC)
WRIST/HAND PATHOLOGY Kristin Kelley, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Trauma/Fractures Hook of Hamate Fractures Triangular Fibrocartilage Complex (TFCC)
Trauma/Fractures WRIST/HAND PATHOLOGY. TFCC Injury. Hook of Hamate Fracture. Property of VOMPTI, LLC
 WRIST/HAND PATHOLOGY Kristin Kelley, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Trauma/Fractures Hook of Hamate Fractures Triangular Fibrocartilage Complex (TFCC)
WRIST/HAND PATHOLOGY Kristin Kelley, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 Trauma/Fractures Hook of Hamate Fractures Triangular Fibrocartilage Complex (TFCC)
Flexor Tendon Case Conundrums
 Flexor Tendon Case Conundrums Philly Meeting 2018 Rowena McBeath, MD, PhD Jeffrey A. Greenberg, MD Nancy M. Cannon, OTR, CHT Faculty Rowena McBeath, MD, PhD Yale molecular biochemistry & biophysics John
Flexor Tendon Case Conundrums Philly Meeting 2018 Rowena McBeath, MD, PhD Jeffrey A. Greenberg, MD Nancy M. Cannon, OTR, CHT Faculty Rowena McBeath, MD, PhD Yale molecular biochemistry & biophysics John
RHEUMATOID HAND. History Pain Loss of function Neck pain. Diminished ADL assessment:
 RHEUMATOID HAND History Pain Loss of function Neck pain Diminished ADL assessment: Using toothbrush, hairbrush, knife, fork Dressing bra, Pulling up trousers / stockings Operating remote control Hobbies
RHEUMATOID HAND History Pain Loss of function Neck pain Diminished ADL assessment: Using toothbrush, hairbrush, knife, fork Dressing bra, Pulling up trousers / stockings Operating remote control Hobbies
(iii) Twenty questions on tendon injuries in the hand
 Current Orthopaedics (2008) 22, 17 24 Available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/cuor MINI-SYMPOSIUM: HAND TRAUMA (iii) Twenty questions on tendon injuries in the hand
Current Orthopaedics (2008) 22, 17 24 Available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/cuor MINI-SYMPOSIUM: HAND TRAUMA (iii) Twenty questions on tendon injuries in the hand
Finger Mobility Deficits Fracture of metacarpal Fracture of phalanx of phalanges
 1 Finger Mobility Deficits ICD-9-CM codes: 715.4 Osteoarthrosis of the hand 815.0 Fracture of metacarpal 816.0 Fracture of phalanx of phalanges ICF codes: Activities and Participation code: d4301 Carrying
1 Finger Mobility Deficits ICD-9-CM codes: 715.4 Osteoarthrosis of the hand 815.0 Fracture of metacarpal 816.0 Fracture of phalanx of phalanges ICF codes: Activities and Participation code: d4301 Carrying
BASIC PRINCIPLES OF HAND TRAUMA: ARE CHILDREN DIFFERENT? SUSAN THOMPSON, MD, FRCSC
 BASIC PRINCIPLES OF HAND TRAUMA: ARE CHILDREN DIFFERENT? SUSAN THOMPSON, MD, FRCSC EPIDEMIOLOGY HAND FRACTURES MAKE UP 2.3% OF ER VISITS INCIDENCE VARIES WITH AGE LOW IN TODDLERS INCREASES WITH AGE (20
BASIC PRINCIPLES OF HAND TRAUMA: ARE CHILDREN DIFFERENT? SUSAN THOMPSON, MD, FRCSC EPIDEMIOLOGY HAND FRACTURES MAKE UP 2.3% OF ER VISITS INCIDENCE VARIES WITH AGE LOW IN TODDLERS INCREASES WITH AGE (20
THE EPIDEMIOLOGY OF HAND EMERGENCIES
 THE EPIDEMIOLOGY OF HAND EMERGENCIES Dr. Adel Abdel Aziz Senior Emergency Physician Honorary Senior Clinical Lecturer, University of Southampton Training Program Director Emergency Medicine/ Health Education
THE EPIDEMIOLOGY OF HAND EMERGENCIES Dr. Adel Abdel Aziz Senior Emergency Physician Honorary Senior Clinical Lecturer, University of Southampton Training Program Director Emergency Medicine/ Health Education
Current Practice in Tendon Management
 Current Practice in Tendon Management Handout www.indianahandtoshoulder.com Click on Therapy Flexor Tendons Denver Nancy M. Cannon, OTR, CHT Director Hand to Shoulder Therapy Center Indianapolis, Indiana
Current Practice in Tendon Management Handout www.indianahandtoshoulder.com Click on Therapy Flexor Tendons Denver Nancy M. Cannon, OTR, CHT Director Hand to Shoulder Therapy Center Indianapolis, Indiana
1. A 40-year-old male has dislocated his right 2 nd MCP. You have pulled as hard as you can but cannot reduce the dislocation. The problem is likely:
 CHAPTER 50 HAND 2 OCTOBER 2013 1. A 40-year-old male has dislocated his right 2 nd MCP. You have pulled as hard as you can but cannot reduce the dislocation. The problem is likely: A. He is a gamer and
CHAPTER 50 HAND 2 OCTOBER 2013 1. A 40-year-old male has dislocated his right 2 nd MCP. You have pulled as hard as you can but cannot reduce the dislocation. The problem is likely: A. He is a gamer and
Common. Common Hand Problems in Elite Athletes
 Common Hand Problems in Elite Athletes Fred Corley M.D. Dept. of Orthopaedic Surgery UTHSCSA I have no disclosures concerning this talk. The University of Texas Health Science Center @ San Antonio - Orthopaedics
Common Hand Problems in Elite Athletes Fred Corley M.D. Dept. of Orthopaedic Surgery UTHSCSA I have no disclosures concerning this talk. The University of Texas Health Science Center @ San Antonio - Orthopaedics
The Forearm, Wrist, Hand and Fingers. Contusion Injuries to the Forearm. Forearm Fractures 12/11/2017. Oak Ridge High School Conroe, Texas
 The Forearm, Wrist, Hand and Fingers Oak Ridge High School Conroe, Texas Contusion Injuries to the Forearm The forearm is constantly exposed to bruising and contusions in contact sports. The ulna receives
The Forearm, Wrist, Hand and Fingers Oak Ridge High School Conroe, Texas Contusion Injuries to the Forearm The forearm is constantly exposed to bruising and contusions in contact sports. The ulna receives
Trigger Digits, Mallet Finger & Metacarpal Injuries. Joseph P. McCormick, M.D. Affinity Orthopaedics & Sports Medicine 2013
 Trigger Digits, Mallet Finger & Metacarpal Injuries Joseph P. McCormick, M.D. Affinity Orthopaedics & Sports Medicine 2013 Overview Trigger Digits: diagnosis and treatment Bonus: approach in children Mallet
Trigger Digits, Mallet Finger & Metacarpal Injuries Joseph P. McCormick, M.D. Affinity Orthopaedics & Sports Medicine 2013 Overview Trigger Digits: diagnosis and treatment Bonus: approach in children Mallet
Trigger Finger Release
 Trigger Finger Release Trigger finger, also known as stenosing tenosynovitis, occurs when one of the tendons responsible for bending a finger or the thumb develops a thickening, known as a nodule, and
Trigger Finger Release Trigger finger, also known as stenosing tenosynovitis, occurs when one of the tendons responsible for bending a finger or the thumb develops a thickening, known as a nodule, and
PIPR Proximal Interphalangeal Replacement. Operative Technique
 PIPR Proximal Interphalangeal Replacement Operative Technique Contents PIPR Proximal Interphalangeal Replacement Developed in association with Mr I Trail and The Wrightington Hospital. Contents Section
PIPR Proximal Interphalangeal Replacement Operative Technique Contents PIPR Proximal Interphalangeal Replacement Developed in association with Mr I Trail and The Wrightington Hospital. Contents Section
Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure
 Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure TRUONG LE DAO, MD, IFAAD 1 Burkhalter W.E, Cristhensen R.C, Brown P.W, Extensor Indicis Proprius opponensplasty
Intrinsic muscles palsies of the hand Management of Thumb Opposition with BURKHALTER s Procedure TRUONG LE DAO, MD, IFAAD 1 Burkhalter W.E, Cristhensen R.C, Brown P.W, Extensor Indicis Proprius opponensplasty
Objectives. Anatomy Review FDP and FDS Interrelationship. Keys to Successful Treatment
 Flexor Tendon Rehabilitation Joanne Mimm, MPT, CHT University of California, Irvine Irvine, CA February 9-11, 2018 Objectives Understand tendon healing/repair Tensile strength Controlled Stress Rehabilitation
Flexor Tendon Rehabilitation Joanne Mimm, MPT, CHT University of California, Irvine Irvine, CA February 9-11, 2018 Objectives Understand tendon healing/repair Tensile strength Controlled Stress Rehabilitation
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Exam of the Injured Hand and Wrist. Christina M. Ward, MD Regions Hospital TRIA Woodbury
 Exam of the Injured Hand and Wrist Christina M. Ward, MD Regions Hospital TRIA Woodbury Disclosures We have no disclosures that are pertinent to this presentation Terminology Ring Long Index Small Thumb
Exam of the Injured Hand and Wrist Christina M. Ward, MD Regions Hospital TRIA Woodbury Disclosures We have no disclosures that are pertinent to this presentation Terminology Ring Long Index Small Thumb
Institute of Reconstructive Surgery, Sofia, Bulgaria
 TRANSPOSITION OF THE LATERAL SLIPS OF THE APONEUROSIS IN TREATMENT OF LONG-STANDING " BOUTONNIERE DEFORMITY " OF THE FINGERS By IVAN MATEV Institute of Reconstructive Surgery, Sofia, Bulgaria RUPTURE of
TRANSPOSITION OF THE LATERAL SLIPS OF THE APONEUROSIS IN TREATMENT OF LONG-STANDING " BOUTONNIERE DEFORMITY " OF THE FINGERS By IVAN MATEV Institute of Reconstructive Surgery, Sofia, Bulgaria RUPTURE of
A Patient s Guide to Adult Thumb Metacarpal Fractures
 A Patient s Guide to Adult Thumb Metacarpal Fractures 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com 1 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult Thumb Metacarpal Fractures 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com 1 DISCLAIMER: The information in this booklet is compiled
The Birmingham Hook Plate Treatment Of Irreduceable Displaced Mallet Avulsion Fractures: A Technical Note
 ISPUB.COM The Internet Journal of Hand Surgery Volume 1 Number 1 The Birmingham Hook Plate Treatment Of Irreduceable Displaced Mallet Avulsion Fractures: A Technical S Tan, D Power Citation S Tan, D Power..
ISPUB.COM The Internet Journal of Hand Surgery Volume 1 Number 1 The Birmingham Hook Plate Treatment Of Irreduceable Displaced Mallet Avulsion Fractures: A Technical S Tan, D Power Citation S Tan, D Power..
Clinical examination of the wrist, thumb and hand
 Clinical examination of the wrist, thumb and hand 20 CHAPTER CONTENTS Referred pain 319 History 319 Inspection 320 Functional examination 320 The distal radioulnar joint.............. 320 The wrist.......................
Clinical examination of the wrist, thumb and hand 20 CHAPTER CONTENTS Referred pain 319 History 319 Inspection 320 Functional examination 320 The distal radioulnar joint.............. 320 The wrist.......................
Silicone PIP, MCP & MCP-X (PreFlex)
 Silicone PIP, MCP & MCP-X (PreFlex) Finger Joint Arthroplasty Operative Technique Silicone PIP Silicone MCP Silicone PreFlex (MCP-X) Stryker Disclaimer This publication sets forth detailed recommended
Silicone PIP, MCP & MCP-X (PreFlex) Finger Joint Arthroplasty Operative Technique Silicone PIP Silicone MCP Silicone PreFlex (MCP-X) Stryker Disclaimer This publication sets forth detailed recommended
Muscle/Tendon Functions: Thumb. Extensor Tendon Healing. Digital Extension. Digital Extension. Supporting Ligaments: ORL. Supporting Ligaments
 Extensor Tendon Anatomy, Common Injury and Treatment Christina Schmidt, OTR/L, CHT University of California, Irvine Irvine, CA February 9-11, 2018 2 How Extensor Tendons Differ from Flexor Tendons Dorsum
Extensor Tendon Anatomy, Common Injury and Treatment Christina Schmidt, OTR/L, CHT University of California, Irvine Irvine, CA February 9-11, 2018 2 How Extensor Tendons Differ from Flexor Tendons Dorsum
Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL
 Andrew McNamara, MD The Orthopaedic and Fracture Clinic 1431 Premier Drive Mankato, MN 56001 507-386-6600 Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL Patient Name: Date: Diagnosis:
Andrew McNamara, MD The Orthopaedic and Fracture Clinic 1431 Premier Drive Mankato, MN 56001 507-386-6600 Metacarpophalangeal Joint Implant Arthroplasty REHABILITATION PROTOCOL Patient Name: Date: Diagnosis:
A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report
 CASE REPORT 41 OPEN ACCESS A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report Aysha Rajeev, John Harrison ABSTRACT Introduction: The phalangeal
CASE REPORT 41 OPEN ACCESS A novel method of treating isolated unicondylar fracture of the head of the proximal phalanx: A case report Aysha Rajeev, John Harrison ABSTRACT Introduction: The phalangeal
Introduction to Ultrasound Examination of the Hand and upper
 Introduction to Ultrasound Examination of the Hand and upper Emil Dionysian, M.D. Ultrasound of upper ext. Upside Convenient Opens another exam dimension Can be like a stethoscope Helps 3-D D visualization
Introduction to Ultrasound Examination of the Hand and upper Emil Dionysian, M.D. Ultrasound of upper ext. Upside Convenient Opens another exam dimension Can be like a stethoscope Helps 3-D D visualization
Pediatric Phalanx Fractures
 Pediatric Phalanx Fractures Julie Balch Samora, MD/PhD/MPH March 1, 2019.... Disclosures Board/committee member: AOA, AAOS, ASSH, RJOS, POSNA Globus (spouse) Goals To identify the most common phalanx fractures
Pediatric Phalanx Fractures Julie Balch Samora, MD/PhD/MPH March 1, 2019.... Disclosures Board/committee member: AOA, AAOS, ASSH, RJOS, POSNA Globus (spouse) Goals To identify the most common phalanx fractures
A Patient s Guide to Adult Thumb Metacarpal Fractures
 A Patient s Guide to Adult Thumb Metacarpal Fractures Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 1 DISCLAIMER: The information
A Patient s Guide to Adult Thumb Metacarpal Fractures Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 1 DISCLAIMER: The information
SPORTS RELATED HAND INJURIES
 HKJOT 2010;20(1):13 18 ORIGINAL ARTICLE SPORTS RELATED HAND INJURIES IN HONG KONG Hercy C.K. Li 1 and Cecilia W.P. Li-Tsang 2 Objective: This study attempted to review the incidence of sports related hand
HKJOT 2010;20(1):13 18 ORIGINAL ARTICLE SPORTS RELATED HAND INJURIES IN HONG KONG Hercy C.K. Li 1 and Cecilia W.P. Li-Tsang 2 Objective: This study attempted to review the incidence of sports related hand
Kinesiology of The Wrist and Hand. Cuneyt Mirzanli Istanbul Gelisim University
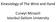 Kinesiology of The Wrist and Hand Cuneyt Mirzanli Istanbul Gelisim University Bones The wrist and hand contain 29 bones including the radius and ulna. There are eight carpal bones in two rows of four to
Kinesiology of The Wrist and Hand Cuneyt Mirzanli Istanbul Gelisim University Bones The wrist and hand contain 29 bones including the radius and ulna. There are eight carpal bones in two rows of four to
Rehabilitation Protocol: Primary Flexor Tendon Repair LHMC Protocol for Zone 1 & 2
 Rehabilitation Protocol: Primary Flexor Tendon Repair LHMC Protocol for Zone 1 & 2 Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
Rehabilitation Protocol: Primary Flexor Tendon Repair LHMC Protocol for Zone 1 & 2 Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington
HAND SURGERY- GUIDELINES for POST-OP TREATMENT and REFERRAL to HAND THERAPY
 HAND SURGERY- GUIDELINES for POST-OP TREATMENT and REFERRAL to HAND THERAPY Please use the specific hand therapy referral form. Always give at least one telephone number for the patient so that there is
HAND SURGERY- GUIDELINES for POST-OP TREATMENT and REFERRAL to HAND THERAPY Please use the specific hand therapy referral form. Always give at least one telephone number for the patient so that there is
Trapezium is by the thumb, Trapezoid is inside
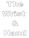 Trapezium is by the thumb, Trapezoid is inside Intercarpal Jt Radiocarpal Jt Distal Middle Proximal DIP PIP Interphalangeal Jts Metacarpalphalangeal (MCP) Jt Metacarpal Carpometacarpal (CMC) Jt Trapezium
Trapezium is by the thumb, Trapezoid is inside Intercarpal Jt Radiocarpal Jt Distal Middle Proximal DIP PIP Interphalangeal Jts Metacarpalphalangeal (MCP) Jt Metacarpal Carpometacarpal (CMC) Jt Trapezium
Mallet Finger Injuries
 A Patient s Guide to Mallet Finger Injuries 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.com DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Mallet Finger Injuries 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.com DISCLAIMER: The information in this booklet is compiled
Wrist & Hand Injury in Sports
 Wrist & Hand Injury in Sports Jennifer Allen,PT,DPT,OCS,SCS,CHT Return to Play Criteria, Clinical Pearls, & Rehab Considerations PBATS Baseball Medicine Conference 2018 Disclosures Wrist & Hand Injury
Wrist & Hand Injury in Sports Jennifer Allen,PT,DPT,OCS,SCS,CHT Return to Play Criteria, Clinical Pearls, & Rehab Considerations PBATS Baseball Medicine Conference 2018 Disclosures Wrist & Hand Injury
Volar Plate Avulsion Fractures
 Journal of the Accident and Medical Practitioners Association (JAMPA) 2006; Vol. 3 (No. 1) Accident and Medical Practitioners Association, New Zealand Volar Plate Avulsion Fractures Sarah Cooper, MBChB
Journal of the Accident and Medical Practitioners Association (JAMPA) 2006; Vol. 3 (No. 1) Accident and Medical Practitioners Association, New Zealand Volar Plate Avulsion Fractures Sarah Cooper, MBChB
Fracture and Dislocation of Metacarpal Bones, Metacarpophalangeal Joints, Phalanges, and Interphalangeal Joints ( 1-Jan-1985 )
 In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
Client centered approach to distal radius fracture management. Jared Rasmussen OTR
 Client centered approach to distal radius fracture management Jared Rasmussen OTR Disclosures Sadly, no financial disclosures Objectives Review of anatomy, common fractures of the distal radius, fixation
Client centered approach to distal radius fracture management Jared Rasmussen OTR Disclosures Sadly, no financial disclosures Objectives Review of anatomy, common fractures of the distal radius, fixation
Ascension. Silicone MCP surgical technique. surgical technique Ascension Silicone MCP
 Ascension Silicone MCP surgical technique WW 2 Introduction This manual describes the sequence of techniques and instruments used to implant the Ascension Silicone MCP (FIGURE 1A). Successful use of this
Ascension Silicone MCP surgical technique WW 2 Introduction This manual describes the sequence of techniques and instruments used to implant the Ascension Silicone MCP (FIGURE 1A). Successful use of this
Ulnar Collateral Ligament Injuries of the Thumb Game Keeper s Thumb A Patient's Guide to Ulnar Collateral Ligament Injuries of the Thumb
 Ulnar Collateral Ligament Injuries of the Thumb Game Keeper s Thumb A Patient's Guide to Ulnar Collateral Ligament Injuries of the Thumb 1 Introduction Injury to the ulnar collateral ligament of the thumb
Ulnar Collateral Ligament Injuries of the Thumb Game Keeper s Thumb A Patient's Guide to Ulnar Collateral Ligament Injuries of the Thumb 1 Introduction Injury to the ulnar collateral ligament of the thumb
Hand Trauma Update: Outline. Hand Surgeon s Area of Expertise. Orthopaedic Update 2015
 Hand Trauma Update: 2015 Orthopaedic Update 2015 March 21, 2015 Peter Tang, MD, MPH Director Hand, Upper Extremity & Microvascular Surgery Fellowship Associate Professor Drexel University College of Medicine
Hand Trauma Update: 2015 Orthopaedic Update 2015 March 21, 2015 Peter Tang, MD, MPH Director Hand, Upper Extremity & Microvascular Surgery Fellowship Associate Professor Drexel University College of Medicine
Dr Klika Proximal & Middle Phalanx Fracture with CRPP
 Dr Klika Proximal & Middle Phalanx Fracture with CRPP Phase 1- Early Protective Phase (0-2 or 3 weeks) Goals for phase 1 Protect healing fracture and surgical fixation Reduce pain & swelling Promote motion
Dr Klika Proximal & Middle Phalanx Fracture with CRPP Phase 1- Early Protective Phase (0-2 or 3 weeks) Goals for phase 1 Protect healing fracture and surgical fixation Reduce pain & swelling Promote motion
SPECIAL ARTICLE. Missed tendon injuries INTRODUCTION
 Archives of Emergency Medicine, 1991, 8, 87-91 SPECIAL ARTICLE Missed tendon injuries H. R. GULY Consultant in A & E, Derriford Hospital, Plymouth INTRODUCTION The timing of the repair of divided tendons
Archives of Emergency Medicine, 1991, 8, 87-91 SPECIAL ARTICLE Missed tendon injuries H. R. GULY Consultant in A & E, Derriford Hospital, Plymouth INTRODUCTION The timing of the repair of divided tendons
SWAN'S NECK DEFORMITY OF THE FINGERS
 SWAN'S NECK DEFORMITY OF THE FINGERS By STEWART H. HARRISON, F.R.C.S., L.D.S.R.C.S.(Edin.) The Mount Vernon Centre of Plastic Surgery, Northwood, Middlesex, and the Windsor Group of Hospitals HYPEREXTENSION
SWAN'S NECK DEFORMITY OF THE FINGERS By STEWART H. HARRISON, F.R.C.S., L.D.S.R.C.S.(Edin.) The Mount Vernon Centre of Plastic Surgery, Northwood, Middlesex, and the Windsor Group of Hospitals HYPEREXTENSION
INTERNAL FIXATION OF THE METACARPALS AND PHALANGES P. BURGE
 Riv Chir Mano - Vol. 43 (3) 2006 INTERNL FIXTION OF THE METCRPLS ND PHLNGES P. URGE Nuffield Orthopaedic Centre, Oxford, UK SUMMRY Techniques and instrumentation for open reduction and internal fixation
Riv Chir Mano - Vol. 43 (3) 2006 INTERNL FIXTION OF THE METCRPLS ND PHLNGES P. URGE Nuffield Orthopaedic Centre, Oxford, UK SUMMRY Techniques and instrumentation for open reduction and internal fixation
Emile N. Brown, MD, and Scott D. Lifchez, MD
 Flexor Pollicis Longus Tendon Rupture After Volar Plating of a Distal Radius Fracture: Pronator Quadratus Plate Coverage May Not Adequately Protect Tendons Emile N. Brown, MD, and Scott D. Lifchez, MD
Flexor Pollicis Longus Tendon Rupture After Volar Plating of a Distal Radius Fracture: Pronator Quadratus Plate Coverage May Not Adequately Protect Tendons Emile N. Brown, MD, and Scott D. Lifchez, MD
Anatomy of the Hand and Nomenclature. R K Kankate Specialist Registrar St.George s Hospital
 Anatomy of the Hand and Nomenclature R K Kankate Specialist Registrar St.George s Hospital Bony skeleton muscles and ligaments nervous, arterial and venous system Ossification of bones: carpus Most carpal
Anatomy of the Hand and Nomenclature R K Kankate Specialist Registrar St.George s Hospital Bony skeleton muscles and ligaments nervous, arterial and venous system Ossification of bones: carpus Most carpal
Hand Therapy Protocols
 Hand Therapy Protocols Post Repair Therapy Protocols Page 1 of 10 Following are representative protocols for each of the three basic approaches to flexor tendon post repair management: immobilization,
Hand Therapy Protocols Post Repair Therapy Protocols Page 1 of 10 Following are representative protocols for each of the three basic approaches to flexor tendon post repair management: immobilization,
Closed Proximal Phalangeal Fracture Management in Hand: An Outcome Analysis
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/577 Closed Proximal Phalangeal Fracture Management in Hand: An Outcome Analysis R Senthilkumar 1, E Kovarthini 2, Heber
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/577 Closed Proximal Phalangeal Fracture Management in Hand: An Outcome Analysis R Senthilkumar 1, E Kovarthini 2, Heber
Interesting Case Series. Ring Avulsion Injuries
 Interesting Case Series Ring Avulsion Injuries Matt Jones BMBS, BSc, MRCS, and Sameer Gujral MBChB, BSc, MRCS Department of Plastic Surgery, Royal Devon & Exeter Hospital, Exeter, Devon, England Correspondence:
Interesting Case Series Ring Avulsion Injuries Matt Jones BMBS, BSc, MRCS, and Sameer Gujral MBChB, BSc, MRCS Department of Plastic Surgery, Royal Devon & Exeter Hospital, Exeter, Devon, England Correspondence:
FINGERTIP INJURIES ARE THEY REALLY THAT SIMPLE? SANJAY K SHARMA, MD, FACS INSTITUTE OF RECONSTRUCTIVE PLASTIC SURGERY
 FINGERTIP INJURIES ARE THEY REALLY THAT SIMPLE? SANJAY K SHARMA, MD, FACS INSTITUTE OF RECONSTRUCTIVE PLASTIC SURGERY Austin Trauma and Critical Care Conference 2018 May 31-June 1, 2018 Outline 1. Scope
FINGERTIP INJURIES ARE THEY REALLY THAT SIMPLE? SANJAY K SHARMA, MD, FACS INSTITUTE OF RECONSTRUCTIVE PLASTIC SURGERY Austin Trauma and Critical Care Conference 2018 May 31-June 1, 2018 Outline 1. Scope
HAND INJURY REHAB CONCEPTS AND RETURN TO PLAY
 HAND INJURY REHAB CONCEPTS AND RETURN TO PLAY DAVID COLVIN, PT, DPT, OCS, MS, ATC Presentation Overview Discuss common hand and finger injuries/rehabilitation in baseball UCL of the Thumb Tear Rehab comparisons
HAND INJURY REHAB CONCEPTS AND RETURN TO PLAY DAVID COLVIN, PT, DPT, OCS, MS, ATC Presentation Overview Discuss common hand and finger injuries/rehabilitation in baseball UCL of the Thumb Tear Rehab comparisons
TENDINOSIS: TRIGGER FINGER DE QUERVAIN S TENOSYNOVITIS. Renita Sirisena Mark Puhaindran
 TENDINOSIS: TRIGGER FINGER DE QUERVAIN S TENOSYNOVITIS Renita Sirisena Mark Puhaindran Tendinosis vs Tendinitis Tendinosis: Degeneration of the tendon s collagen Related to chronic use Tendinitis Tendon
TENDINOSIS: TRIGGER FINGER DE QUERVAIN S TENOSYNOVITIS Renita Sirisena Mark Puhaindran Tendinosis vs Tendinitis Tendinosis: Degeneration of the tendon s collagen Related to chronic use Tendinitis Tendon
Fig Fig Fig. 6-3
 CHAPTER 6 UPPER EXTREMITY The surgical treatment of hand problems is a specialized area of interest in plastic surgery. The hand is a unique organ which transmits sensations from the external environment
CHAPTER 6 UPPER EXTREMITY The surgical treatment of hand problems is a specialized area of interest in plastic surgery. The hand is a unique organ which transmits sensations from the external environment
Wrist & Hand Assessment and General View
 Wrist & Hand Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The hand can be divided
Wrist & Hand Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The hand can be divided
Wrist and Hand Injuries in the Athlete
 University of Kentucky UKnowledge Rehabilitation Sciences Faculty Publications Rehabilitation Sciences 2001 Wrist and Hand Injuries in the Athlete Timothy L. Uhl University of Kentucky, tluhl2@uky.edu
University of Kentucky UKnowledge Rehabilitation Sciences Faculty Publications Rehabilitation Sciences 2001 Wrist and Hand Injuries in the Athlete Timothy L. Uhl University of Kentucky, tluhl2@uky.edu
A Patient's Guide to Ganglions of the Wrist
 Introduction A ganglion is a small, harmless cyst, or sac of fluid, that sometimes develops in the wrist. Doctors don't know exactly what causes ganglions, but a ganglion that isn't painful and doesn't
Introduction A ganglion is a small, harmless cyst, or sac of fluid, that sometimes develops in the wrist. Doctors don't know exactly what causes ganglions, but a ganglion that isn't painful and doesn't
Ligaments of Elbow hinge: sagittal plane so need lateral and medial ligaments
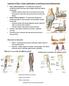 Ligaments of Elbow hinge: sagittal plane so need lateral and medial ligaments Ulnar Collateral ligament on medial side; arising from medial epicondyle and stops excess valgus movement (lateral movement)
Ligaments of Elbow hinge: sagittal plane so need lateral and medial ligaments Ulnar Collateral ligament on medial side; arising from medial epicondyle and stops excess valgus movement (lateral movement)
Early motion or immobilisation of Hand Fractures? Nikki Burr Consultant Hand Therapist Royal Free Hospital London Mount Vernon Hospital
 Early motion or immobilisation of Hand Fractures? Nikki Burr Consultant Hand Therapist Royal Free Hospital London Mount Vernon Hospital Hand Fractures (distal to carpus) Soft tissue injury with an underlying
Early motion or immobilisation of Hand Fractures? Nikki Burr Consultant Hand Therapist Royal Free Hospital London Mount Vernon Hospital Hand Fractures (distal to carpus) Soft tissue injury with an underlying
A Patient s Guide to Biceps Tendon Tears at the Elbow
 A Patient s Guide to Biceps Tendon Tears at the Elbow Introduction The muscles which flex the elbow are the bicep complex. Like all musculoskeletal units, the end connection is a tendon composed of strong,
A Patient s Guide to Biceps Tendon Tears at the Elbow Introduction The muscles which flex the elbow are the bicep complex. Like all musculoskeletal units, the end connection is a tendon composed of strong,
MULTIMEDIA ARTICLES. Mary C. Burns & Brian Derby & Michael W. Neumeister
 HAND (2013) 8:17 22 DOI 10.1007/s11552-012-9488-z MULTIMEDIA ARTICLES Wyndell merritt immediate controlled active motion (ICAM) protocol following extensor tendon repairs in zone IV VII: review of literature,
HAND (2013) 8:17 22 DOI 10.1007/s11552-012-9488-z MULTIMEDIA ARTICLES Wyndell merritt immediate controlled active motion (ICAM) protocol following extensor tendon repairs in zone IV VII: review of literature,
Andrew L Terrono, MD Chief Hand Surgery Service NEBH Clinical Professor Orthopaedics Tufts University. May 2 & 3, 2016
 Andrew L Terrono, MD Chief Hand Surgery Service NEBH Clinical Professor Orthopaedics Tufts University Work Related Workshop WorkInjuries Related Injuries Workshop Exertional??? Webster- precipitated by
Andrew L Terrono, MD Chief Hand Surgery Service NEBH Clinical Professor Orthopaedics Tufts University Work Related Workshop WorkInjuries Related Injuries Workshop Exertional??? Webster- precipitated by
Complications of Distal Radius Fractures. How to Treat a Distal Radius Fx 11/13/2017. Michael S. Bednar, M.D. Loyola University Chicago
 Complications of Distal Radius Fractures Michael S. Bednar, M.D. Loyola University Chicago How to Treat a Distal Radius Fx Need to restore motion, begin with uninvolved parts Need to reduce an unreduced
Complications of Distal Radius Fractures Michael S. Bednar, M.D. Loyola University Chicago How to Treat a Distal Radius Fx Need to restore motion, begin with uninvolved parts Need to reduce an unreduced
Finger fractures and dislocations may
 Common Finger Fractures and Dislocations JAMES R. BORCHERS, MD, MPH, and THOMAS M. BEST, MD, PhD, The Ohio State University, Columbus, Ohio Finger fractures and dislocations are common injuries that are
Common Finger Fractures and Dislocations JAMES R. BORCHERS, MD, MPH, and THOMAS M. BEST, MD, PhD, The Ohio State University, Columbus, Ohio Finger fractures and dislocations are common injuries that are
A Patient s Guide to Elbow Dislocation
 A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
THE 9 FINGER flexor pulleys maintain the course. Quantification of Partial or Complete A4 Pulley Release With FDP Repair in Cadaveric Tendons
 SCIENTIFIC ARTICLE Quantification of Partial or Complete A4 Pulley Release With FDP Repair in Cadaveric Tendons Orrin I. Franko, MD, Nathan M. Lee, BS, John J. Finneran, BA, Matthew C. Shillito, MD, Matthew
SCIENTIFIC ARTICLE Quantification of Partial or Complete A4 Pulley Release With FDP Repair in Cadaveric Tendons Orrin I. Franko, MD, Nathan M. Lee, BS, John J. Finneran, BA, Matthew C. Shillito, MD, Matthew
Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley.
 TRIGGER DIGITS Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley. Abstract Primary stenosing tenosynovitis is usually idiopathic
TRIGGER DIGITS Definition: This problem generally is caused by a size mismatch between the flexor tendon and the first annular (A-1) pulley. Abstract Primary stenosing tenosynovitis is usually idiopathic
Common Tendon Disorders of the Upper Extremity. Mark Tait MD
 Common Tendon Disorders of the Upper Extremity Mark Tait MD Tendonitis History Pain and swelling (any tendon, any location) Overuse Physical examination findings Localized swelling Pain with resistance
Common Tendon Disorders of the Upper Extremity Mark Tait MD Tendonitis History Pain and swelling (any tendon, any location) Overuse Physical examination findings Localized swelling Pain with resistance
Musculoskeletal Imaging of the Digits. Arash David Tehranzadeh, MD UCSD MSK Radiology May 11 th, 2006
 Musculoskeletal Imaging of the Digits Arash David Tehranzadeh, MD UCSD MSK Radiology May 11 th, 2006 Musculoskeletal Imaging of the Digit Anatomy & Internal Derangement The Extensor System The Flexor System
Musculoskeletal Imaging of the Digits Arash David Tehranzadeh, MD UCSD MSK Radiology May 11 th, 2006 Musculoskeletal Imaging of the Digit Anatomy & Internal Derangement The Extensor System The Flexor System
