Intramedullary Nailing for Femur Fracture Management
|
|
|
- Colin Warren
- 5 years ago
- Views:
Transcription
1 , ext thechildren.com/trauma Intramedullary Nailing for Femur Fracture Management A Guide for Parents The femur is the longest bone in the body. It begins at the hip joint and ends at the knee. A femur fracture is typically sustained from high-energy impact such as motor vehicle collisions, falls from playground equipment, falls from furniture or resulting from a twisting mechanism. Children who have sustained a femur fracture are hospitalized on the Surgical/Trauma Unit in order to receive appropriate medical, nursing and rehabilitation care. FEMUR (thigh bone) Head Neck Lesser trochanter Greater trochanter Shaft Medial epicondyle Lateral epicondyle Illustration Copyright 2016 Nucleus Medical Media, All rights reserved.
2 FEMUR FRACTURE MANAGEMENT The pediatric Orthopedic Surgeon will assess your child in order to determine the optimal treatment method. Treatment goals include: achieving proper bone realignment, rapid healing, and the return to normal daily activities. The treatment method chosen is primarily based on the child s age but also taken into consideration are: fracture type, location and other injuries sustained if applicable. Prior to the surgery, your child may be placed in skin traction. This will ensure the bone is in an optimal healing position until it is surgically repaired. Occasionally, traction may be used for a longer period of time. The surgeon will determine if this management is needed based on the specific fracture type and/or location. ELASTIC/FLEXIBLE INTRAMEDULLARY NAILING This surgery is performed by the Orthopedic Surgeon in the Operating Room under general anesthesia. The surgeon will usually make two small incisions near the knee joint in order to insert two flexible titanium rods (intramedullary nails) through the femur. Occasionally, additional small incisions may be necessary to realign the bone or insert the rod. The rods will maintain the bone s optimal healing position. Flexible intramedullary nail In most cases, neither a cast nor brace will be required post-surgery. Your child will therefore be able to move his hip, knee and ankle on the affected side. The joints will remain flexible and muscle strength will be maintained. You can expect that your child s hip will appear swollen and you will notice small incisions on the sides. Your child will not be permitted to walk on the affected leg for approximately six weeks after the injury in order for the bone to heal. Usually the rods are removed within 6-12 months post-surgery. Removal of the flexible intramedullary nail is a quick procedure which is done in Day Surgery. Incision With kind permission from Springer Science+Business Media: Surgical Technique: Basic Principles, Flexible Intramedullary Nailing in Children, 2010, Pierre Lascombes and Jean-Damien Métaizeau, Copyright 2010.
3 TYPICAL FEMUR FRACTURE MANAGEMENT Age Range Intervention 0-5 years old Spica cast* 5-10 year old females 5-12 year old males 10 years and older females 12 years and older males Flexible IM nailing Flexible IM nailing Rigid IM nailing Rigid IM nailing * See Spica Cast brochure RIGID INTRAMEDULLARY NAILING This surgery is also performed by the Orthopedic Surgeon in the Operating Room under general anesthesia. The surgeon will make an incision near the hip joint in order to insert a rigid rod (intramedullary nail) through the femur. The rod is fixed by screws at both ends and will keep the bone stable in order to ensure proper healing. In most cases, neither a cast nor brace will be required post-surgery. Your child will be able to move his hip, knee and ankle on the operated side. The joints will remain flexible and muscle strength will be maintained. The hip will be swollen and you will notice small incisions on the side. Incision Rigid intramedullary nail Screw Depending on the fracture pattern, your child will be permitted to walk on the affected leg. In some instances weight bearing on the affected leg is not permitted for up to six weeks. Once the fracture has healed, the rod will remain within the femur and is typically not removed. Illustration Copyright 2016 Nucleus Medical Media, All rights reserved.
4 YOUR CHILD S HOSPITALIZATION Your child will typically remain in the hospital for 3-5 days post-surgery. In order to ensure his safety at home, he will need to be medically stable, comfortable and mobile. The MCH Trauma Interprofessional Team will follow him in order to ensure his well-being and progress. In order to facilitate the recovery process, it is essential that your child moves as much as tolerated in order to prevent complications resulting from immobility. Your child will be given exercises for the affected leg and will be shown how to transfer from a wheelchair. He will also be shown how to stand and ambulate using a walker or crutches depending on his abilities. Teaching for going up and down the stairs will be provided. He can do this on his buttocks or using crutches. Practice physiotherapy exercises outside of the scheduled sessions. Nurses and/or Patient Care Attendants can assist you as needed Practice transfer techniques in order to become comfortable with the maneuvers as you are the primary care giver for your child at home Teach the transfer techniques to anyone closely involved in your child s care CARE AT HOME Throughout your child s hospitalization, the Trauma Coordinator and the Physiotherapist will help prepare you for your child s discharge home. Your child will be discharged when deemed medically appropriate and when his safety and comfort at home is assured. The following information will be requested in order to facilitate a safe return home: Do you have stairs at home? If so, are they inside or outside, or both? Where is your child s bedroom situated? Where is the bathroom situated? Who will care for your child at home during recovery? What mode of transport does your child use to get to school? Does your child have access to an elevator at school? Some children are discharged using crutches, others require a walker and some use a wheelchair for a period of time depending on their abilities, tolerance and comfort. Equipment can be rented or purchased. You will be provided with vendor information. During automobile travel, support the injured leg using pillows Reach out to family and friends for help when your child returns home from the hospital
5 Circulation Verify the blood flow circulation to the injured leg by comparing the following to the uninjured leg: Color your child s foot and toes should remain its normal skin color Warmth your child s foot and toes should feel warm to the touch Sensation your child should be able to feel you touching his foot and toes Movement your child should be able to move his foot and toes Verify the circulation every four hours for the first 24 hours, then twice daily for the remainder of the time. Pain Children typically experience pain and discomfort following the surgery. You will be provided with a prescription for pain medication. Give the medication as prescribed and instructed by the doctor and/or nurse. It is strongly recommended that you give the medication on a regular basis for the first hours. This will help ease your child s pain and/or discomfort. Swelling Elevate your child s leg as much as possible in order to help decrease swelling and pain. Follow the exercise recommendations provided by the Physiotherapist in order to prevent swelling and joint stiffness. Bathing Your child will not be permitted to take a shower or a bath until the incision has healed. The Orthopedic Surgeon will inform you when this will be possible. Bathroom Your child may use a regular toilet seat if he is able and comfortable doing so. A urinal and/or bedpan can also be used and is available for purchase in local pharmacies. Place a stool in front of the toilet seat in order for your child to rest the injured leg School Your child may return to school when comfortable and once the school has been determined safe and accessible. Guidance will be provided by the Trauma Coordinator and the Physiotherapist. Most schools have an elevator accessible to students as needed. Contact your child s school administrator for more information on elevator accessibility. For those children who cannot attend school due to the injury, homebound teaching can be arranged with the school. The Trauma Coordinator will provide you with the necessary documentation. Some families find a progressive return to school helpful. Start with half-days as tolerated. Contact your child s school in order to discuss this gradual return option In order to avoid crowds, request that your child be allowed to leave class 5 minutes before or after all other students Arrange for a classmate to help carry books and supplies
6 You will receive the following documentation before you are discharged: Prescription for analgesics Prescription for equipment Follow-up appointment with the Orthopedic Surgeon Follow-up appointment with the Physiotherapist (if needed) Home exercise program Medical note for school and gym I Should Call my Doctor if: Persistent numbness or tingling despite change of position Reddening or blue toes Swelling which increases or does not resolve Decreased mobility in toes Pain not relieved with medication Persistent fever for more than one day Foul odor or any drainage from the dressing RETURN TO SPORTS AND ACTIVITIES If your child is not permitted to walk on the injured leg it is expected that within 6-8 weeks he will be able to resume weight bearing (as indicated by the Orthopedic Surgeon). The Physiotherapist will follow-up with you regularly in order to progress exercises to promote the return of strength and flexibility in the affected leg. Once your child is able to run and jump, he will be permitted to progressively return to physical activities and/or sports. This typically takes about 3-4 months post injury. Higher level sports may be delayed for a longer period. Always follow the recommendations provided by the Orthopedic Surgeon and Physiotherapist! Complications and residual problems following a femur fracture in children are rare. If you or your child notices any new difficulty functioning since the injury or persistent discomfort in the affected leg, contact the Orthopedic Surgeon. IMPORTANT CONTACT INFORMATION: Alternative Care Module Nurse Monday to Friday 8h00-18h , extension Pediatric Orthopedic Clinic Monday to Friday 8h00-16h Trauma Monday to Friday 8h00-16h , extension Physiotherapy Department Monday to Friday 8h30-16h Surgical/Trauma Unit Available at all times , extension 22433
ACL RECONSTRUCTION. Date of Surgery. Please bring this booklet the day of your surgery. QHC#65
 ACL RECONSTRUCTION Date of Surgery Please bring this booklet the day of your surgery. QHC#65 The ACL (Anterior Cruciate Ligament) is the major stabilizing ligament of the knee. The ACL is located in the
ACL RECONSTRUCTION Date of Surgery Please bring this booklet the day of your surgery. QHC#65 The ACL (Anterior Cruciate Ligament) is the major stabilizing ligament of the knee. The ACL is located in the
Ankle Fracture Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Before, During and After Hip and Knee Replacement
 Working Together for Healthy Joints Before, During and After Hip and Knee Replacement Last revised October 2012 Introduction Paperwork Washrooms Things that beep Today s Main Message: Your hospital stay
Working Together for Healthy Joints Before, During and After Hip and Knee Replacement Last revised October 2012 Introduction Paperwork Washrooms Things that beep Today s Main Message: Your hospital stay
Physiotherapy following peri acetabular osteotomy (PAO) surgery
 Physiotherapy following peri acetabular osteotomy (PAO) surgery This leaflet explains more about returning to your everyday activities after your peri acetabular osteotomy (PAO). It explains the exercises
Physiotherapy following peri acetabular osteotomy (PAO) surgery This leaflet explains more about returning to your everyday activities after your peri acetabular osteotomy (PAO). It explains the exercises
Before, During and After Hip and Knee Replacement
 Working Together for Healthy Joints Before, During and After Hip and Knee Replacement December 2017 Introduction Paperwork Washrooms Things that beep Today s Main Message: Your hospital stay is short so
Working Together for Healthy Joints Before, During and After Hip and Knee Replacement December 2017 Introduction Paperwork Washrooms Things that beep Today s Main Message: Your hospital stay is short so
Before, During and After Hip and Knee Replacement
 Working Together for Healthy Joints Before, During and After Hip and Knee Replacement June 2018 Introduction Paperwork Washrooms Things that beep Today s Main Message: Your hospital stay will be anywhere
Working Together for Healthy Joints Before, During and After Hip and Knee Replacement June 2018 Introduction Paperwork Washrooms Things that beep Today s Main Message: Your hospital stay will be anywhere
KNEE ARTHROSCOPY SURGERY
 KNEE ARTHROSCOPY SURGERY SUMMARY OF PROCEDURE Arthroscopy involves looking at the inside of the knee joint with a small telescope and camera (arthroscope). The image is projected onto a television monitor
KNEE ARTHROSCOPY SURGERY SUMMARY OF PROCEDURE Arthroscopy involves looking at the inside of the knee joint with a small telescope and camera (arthroscope). The image is projected onto a television monitor
Knee Replacement Recovery Guide
 Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
Ankle arthroscopy. If you have any further questions, please speak to a doctor or nurse caring for you
 Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Patient Information for Consent
 Patient Information for Consent OS12 Femoral Shaft Fracture Surgery (Femoral Nailing) Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your
Patient Information for Consent OS12 Femoral Shaft Fracture Surgery (Femoral Nailing) Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your
A Guide to Common Ankle Injuries
 A Guide to Common Ankle Injuries Learn About: Common ankle injuries Feet and Ankle Diagnosis and Treatment Ankle exercises Beginning your recovery Frequently asked questions Do s and Don t s Arthroscopy
A Guide to Common Ankle Injuries Learn About: Common ankle injuries Feet and Ankle Diagnosis and Treatment Ankle exercises Beginning your recovery Frequently asked questions Do s and Don t s Arthroscopy
Femoral shaft fracture surgery (femoral nailing)
 Femoral shaft fracture surgery (femoral nailing) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Femoral shaft fracture surgery (femoral nailing) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Soft tissue Injury of the Knee (self-management) Knee 3
 Soft tissue Injury of the Knee (self-management) Knee 3 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows
Soft tissue Injury of the Knee (self-management) Knee 3 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows
Tibia intramedullary nail operation physiotherapy advice
 Tibia intramedullary nail operation physiotherapy advice This leaflet gives you advice about recovering after your operation. It also explains exercises you should do each day, things to look out for and
Tibia intramedullary nail operation physiotherapy advice This leaflet gives you advice about recovering after your operation. It also explains exercises you should do each day, things to look out for and
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Inner side of knee. Outer side of knee. PCL - Posterior cruciate ligament. Femur Articular cartilage. ACL - Anterior cruciate ligament
 ACL surgery Outer side of knee Inner side of knee PCL - Posterior cruciate ligament Femur Articular cartilage LCL - Lateral collateral ligament Lateral meniscus Tibia ACL - Anterior cruciate ligament MCL
ACL surgery Outer side of knee Inner side of knee PCL - Posterior cruciate ligament Femur Articular cartilage LCL - Lateral collateral ligament Lateral meniscus Tibia ACL - Anterior cruciate ligament MCL
Dr. Roy Davidovitch Next Day Discharge Total Hip Replacement Recovery Guide
 Dr. Roy Davidovitch Next Day Discharge Total Hip Replacement Recovery Guide PREOPERATIVE INSTRUCTIONS Your Preadmission Testing Visit About 2 weeks prior to your surgical date, you will be required to
Dr. Roy Davidovitch Next Day Discharge Total Hip Replacement Recovery Guide PREOPERATIVE INSTRUCTIONS Your Preadmission Testing Visit About 2 weeks prior to your surgical date, you will be required to
General Cast and Splint Care
 General Cast and Splint Care Casts and splints provide limb support after a fracture or surgery. They may also be used to stretch the muscles in a limb. The cast or splint keeps the arm or leg in the proper
General Cast and Splint Care Casts and splints provide limb support after a fracture or surgery. They may also be used to stretch the muscles in a limb. The cast or splint keeps the arm or leg in the proper
Physiotherapy after your hip arthroscopy
 Physiotherapy after your hip arthroscopy This leaflet gives you advice about recovering from your hip arthroscopy. It explains exercises you should do each day, things to look out for and some general
Physiotherapy after your hip arthroscopy This leaflet gives you advice about recovering from your hip arthroscopy. It explains exercises you should do each day, things to look out for and some general
Total hip replacement
 Total hip replacement 2 Hip pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that 1 in 5 people
Total hip replacement 2 Hip pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that 1 in 5 people
MENISCUS TEAR. Description
 MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET
 TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your knee replacement. However if you still have any concerns or queries
TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your knee replacement. However if you still have any concerns or queries
James R. Romanowski, M.D.
 James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
Knee MPFL Reconstruction FAQ
 Knee MPFL Reconstruction FAQ Ryan W. Hess, MD Office: 763-302-2223 Fax: 763-302-2402 Twitter: RyanHessMD Q: WHAT IS ACCOMPLISHED DURING THE PROCEDURE? MPFL stands for Medial Patellofemoral Ligament. This
Knee MPFL Reconstruction FAQ Ryan W. Hess, MD Office: 763-302-2223 Fax: 763-302-2402 Twitter: RyanHessMD Q: WHAT IS ACCOMPLISHED DURING THE PROCEDURE? MPFL stands for Medial Patellofemoral Ligament. This
Total Hip Replacement. Information and exercises for patients
 Total Hip Replacement Information and exercises for patients The following guide is designed to help you understand more about your operation and the therapy you will receive Author: Orthopaedic Therapy
Total Hip Replacement Information and exercises for patients The following guide is designed to help you understand more about your operation and the therapy you will receive Author: Orthopaedic Therapy
Rehabilitation Protocol Bunion Surgery. What to expect after bunion surgery
 Rehabilitation Protocol Bunion Surgery What to expect after bunion surgery The most common types of bunion surgery are scarf osteotomy and chevron osteotomy. Both are normally carried out as day case procedures
Rehabilitation Protocol Bunion Surgery What to expect after bunion surgery The most common types of bunion surgery are scarf osteotomy and chevron osteotomy. Both are normally carried out as day case procedures
Guidelines for patients having. Achilles Tendon Repair. Achilles Tendon Repair
 Guidelines for patients having ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Achilles Tendon Repair Please stick addressograph
Guidelines for patients having ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Achilles Tendon Repair Please stick addressograph
Non weight bearing advice (post operative)
 Non weight bearing advice (post operative) Physiotherapy Department Patient information leaflet Who is this booklet for? This booklet is for post-operative patients who have been told that they will have
Non weight bearing advice (post operative) Physiotherapy Department Patient information leaflet Who is this booklet for? This booklet is for post-operative patients who have been told that they will have
Foot and Ankle Surgery
 Information about Foot and Ankle Surgery Statement of Use The information in this leaflet is intended solely for the person to whom it was given by the health care team and is provided as a general information
Information about Foot and Ankle Surgery Statement of Use The information in this leaflet is intended solely for the person to whom it was given by the health care team and is provided as a general information
You and Your Knee Joint Replacement. Joint School Surgical Rehabilitation Team
 You and Your Knee Joint Replacement Joint School Surgical Rehabilitation Team Housekeeping Length of Session Questions during the session Fire Toilet Facilities Moving around to relieve discomfort Enhanced
You and Your Knee Joint Replacement Joint School Surgical Rehabilitation Team Housekeeping Length of Session Questions during the session Fire Toilet Facilities Moving around to relieve discomfort Enhanced
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Weil osteotomy for the treatment of metatarsalgia. Information for patients Department of Podiatric Surgery
 Weil osteotomy for the treatment of metatarsalgia Information for patients Department of Podiatric Surgery What is metatarsalgia? Metatarsalgia is a type of pain that occurs in the ball of the foot, also
Weil osteotomy for the treatment of metatarsalgia Information for patients Department of Podiatric Surgery What is metatarsalgia? Metatarsalgia is a type of pain that occurs in the ball of the foot, also
The aim of this booklet is to provide you with information about your operation and the treatment you will receive.
 Patient Information Physiotherapy after Hip Resurfacing Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you will
Patient Information Physiotherapy after Hip Resurfacing Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you will
Anterior Cruciate Ligament (ACL) Repair
 Anterior Cruciate Ligament (ACL) Repair Information for patients preparing for recovery at home Read this brochure to learn about: How to take care of yourself at home How to cope with pain Problems to
Anterior Cruciate Ligament (ACL) Repair Information for patients preparing for recovery at home Read this brochure to learn about: How to take care of yourself at home How to cope with pain Problems to
METATARSAL FRACTURE (Including Jones and Dancer s Fractures)
 METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
Rehabilitation programme after cannulated hip screw surgery
 Rehabilitation programme after cannulated hip screw surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation
Rehabilitation programme after cannulated hip screw surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation
Therapy following a neck of femur fracture
 INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
A Patient s Guide to Stress Fractures of the Hip
 A Patient s Guide to Stress Fractures of the Hip Introduction Stress fractures of the hip once most commonly affected military personnel who marched and ran day after day. Today, stress fractures of the
A Patient s Guide to Stress Fractures of the Hip Introduction Stress fractures of the hip once most commonly affected military personnel who marched and ran day after day. Today, stress fractures of the
Hip Fracture. Information and exercises for patients
 Hip Fracture Information and exercises for patients The following guide is designed to help you understand more about your operation and the therapy you will receive Author: Orthopaedic Therapy Team Date:
Hip Fracture Information and exercises for patients The following guide is designed to help you understand more about your operation and the therapy you will receive Author: Orthopaedic Therapy Team Date:
Total Knee Replacement
 Total Knee Replacement STEPHEN M. DESIO, M.D. Hospital Stay Most patients are in the hospital for two to three days. A Case Manager is part of our team whom you will meet after surgery. We will work together
Total Knee Replacement STEPHEN M. DESIO, M.D. Hospital Stay Most patients are in the hospital for two to three days. A Case Manager is part of our team whom you will meet after surgery. We will work together
Advice: After the Removal of a Lower Leg Cast
 Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
Lesser Toe Correction
 Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Explanation: Lesser Toe Correction Lesser toe deformities are classified
Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Explanation: Lesser Toe Correction Lesser toe deformities are classified
Anterior Cruciate Ligament (ACL) Tears
 WASHINGTON UNIVERSITY ORTHOPEDICS Anterior Cruciate Ligament (ACL) Tears Knowing what to expect for ACL surgery is key for a healthy surgery and recovery. Our sports medicine specialists are committed
WASHINGTON UNIVERSITY ORTHOPEDICS Anterior Cruciate Ligament (ACL) Tears Knowing what to expect for ACL surgery is key for a healthy surgery and recovery. Our sports medicine specialists are committed
Your Guide To Anterior Cruciate Ligament Reconstruction
 Your Guide To Anterior Cruciate Ligament Reconstruction Your Guide To Anterior Cruciate Ligament Reconstruction C O N T E N T S Foreword 2 Introduction 3 Anterior Cruciate Ligament 4 Preparation before
Your Guide To Anterior Cruciate Ligament Reconstruction Your Guide To Anterior Cruciate Ligament Reconstruction C O N T E N T S Foreword 2 Introduction 3 Anterior Cruciate Ligament 4 Preparation before
Hip Fractures. Anatomy. Causes. Symptoms
 Hip Fractures A hip fracture is a break in the upper quarter of the femur (thigh) bone. The extent of the break depends on the forces that are involved. The type of surgery used to treat a hip fracture
Hip Fractures A hip fracture is a break in the upper quarter of the femur (thigh) bone. The extent of the break depends on the forces that are involved. The type of surgery used to treat a hip fracture
Knee arthroscopy surgery
 Patient information Knee arthroscopy surgery i Important information for all orthopaedic patients undergoing knee arthroscopy surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY
Patient information Knee arthroscopy surgery i Important information for all orthopaedic patients undergoing knee arthroscopy surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY
Anterior Cruciate Ligament (ACL) Repair
 Form: D-5483 Anterior Cruciate Ligament (ACL) Repair Information for patients preparing for recovery at home Read this brochure to learn about: How to take care of yourself at home What activities are
Form: D-5483 Anterior Cruciate Ligament (ACL) Repair Information for patients preparing for recovery at home Read this brochure to learn about: How to take care of yourself at home What activities are
HIP REPLACEMENT SURGERY
 HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
KUCHING SPECIALIST HOSPITAL - Arthritis and Sports Injury Centre -
 KUCHING SPECIALIST HOSPITAL - Arthritis and Sports Injury Centre - ARTHROSCOPY FOR TORN MENISCI You have had problems with your knee and your orthopaedic surgeon suspects that you may have a torn meniscus,
KUCHING SPECIALIST HOSPITAL - Arthritis and Sports Injury Centre - ARTHROSCOPY FOR TORN MENISCI You have had problems with your knee and your orthopaedic surgeon suspects that you may have a torn meniscus,
Posterior Lumbar Spinal Fusion
 Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Rehabilitation programme after hemiarthroplasty surgery
 Rehabilitation programme after hemiarthroplasty surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Rehabilitation programme after hemiarthroplasty surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Knee Arthroscopy Meniscus Surgery FAQ
 Knee Arthroscopy Meniscus Surgery FAQ Ryan W. Hess, MD Office: 763-302-2223 Fax: 763-302-2402 Twitter: RyanHessMD Q: WHAT IS ACCOMPLISHED DURING THE PROCEDURE? Knee arthroscopy is when a small camera is
Knee Arthroscopy Meniscus Surgery FAQ Ryan W. Hess, MD Office: 763-302-2223 Fax: 763-302-2402 Twitter: RyanHessMD Q: WHAT IS ACCOMPLISHED DURING THE PROCEDURE? Knee arthroscopy is when a small camera is
Ankle Fracture Weber B Ankle 3
 Ankle Fracture Weber B Ankle 3 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Ankle Fracture Weber B Ankle 3 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
FAQ s: Hip Arthroscopy with Dr. Boyle
 AUT Millennium, 17 Antares Place Telephone: 09 281 6733 Mairangi Bay, Auckland 0632 Fax: 09 479 3805 www.matthewboyle.co.nz office@matthewboyle.co.nz FAQ s: Hip Arthroscopy with Dr. Boyle What is hip arthroscopy?
AUT Millennium, 17 Antares Place Telephone: 09 281 6733 Mairangi Bay, Auckland 0632 Fax: 09 479 3805 www.matthewboyle.co.nz office@matthewboyle.co.nz FAQ s: Hip Arthroscopy with Dr. Boyle What is hip arthroscopy?
Anterior Cruciate Ligament Reconstruction
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery
 Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery We want to make this experience as pleasant as possible for you and your family. If you have any questions before or after
Dr. Anant Kumar, M.D. Post-Operative Instructions after Cervical Spine Surgery We want to make this experience as pleasant as possible for you and your family. If you have any questions before or after
Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan
 Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan Orthopaedic Department Tunbridge Wells Hospital Tonbridge Road Pembury TN2 4QJ Telephone: 07734370108 Email:
Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan Orthopaedic Department Tunbridge Wells Hospital Tonbridge Road Pembury TN2 4QJ Telephone: 07734370108 Email:
The aim of this booklet is to provide you with information about your operation and the treatment you will receive.
 Patient Information Physiotherapy after Total Hip Replacement Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you
Patient Information Physiotherapy after Total Hip Replacement Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you
OSCELL MICROFRACTURE OR DRILLING OPERATION (FEMORAL CONDYLE SITES) PATIENT ADVICE.
 OSCELL MICROFRACTURE OR DRILLING OPERATION ( SITES) PATIENT ADVICE. Anatomy of the Right Knee example of a femoral condyle articular defect site Knee Straight Knee Bent KEY: Patella Kneecap Trochlea Groove
OSCELL MICROFRACTURE OR DRILLING OPERATION ( SITES) PATIENT ADVICE. Anatomy of the Right Knee example of a femoral condyle articular defect site Knee Straight Knee Bent KEY: Patella Kneecap Trochlea Groove
ACL Reconstruction surgery
 Golden Jubilee National Hospital NHS National Waiting Times Centre ACL Reconstruction surgery Patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk 2
Golden Jubilee National Hospital NHS National Waiting Times Centre ACL Reconstruction surgery Patient information guide Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk 2
Plantar plate injuries
 Plantar plate injuries Introduction A plantar plate tear is caused by a specific injury to the toe and the joint, or overuse of the joint over time. Often this can be associated with a bunion deformity
Plantar plate injuries Introduction A plantar plate tear is caused by a specific injury to the toe and the joint, or overuse of the joint over time. Often this can be associated with a bunion deformity
Pilon Fractures - OrthoInfo - AAOS. Copyright 2010 American Academy of Orthopaedic Surgeons. Pilon Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Pilon Fractures Pilon fractures affect the bottom of the shinbone (tibia) at the ankle joint. In most cases, both bones in the lower leg, the tibia
Copyright 2010 American Academy of Orthopaedic Surgeons Pilon Fractures Pilon fractures affect the bottom of the shinbone (tibia) at the ankle joint. In most cases, both bones in the lower leg, the tibia
Patient & Family Guide
 Patient & Family Guide 2018 Discharge from Orthopaedics Congratulations! You will soon be discharged home. This booklet explains the information that you were given during your hospital stay. We hope that
Patient & Family Guide 2018 Discharge from Orthopaedics Congratulations! You will soon be discharged home. This booklet explains the information that you were given during your hospital stay. We hope that
Rehabilitation programme after internal fixation surgery
 Rehabilitation programme after internal fixation surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Rehabilitation programme after internal fixation surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Knee Arthroscopy: Postoperative Instructions
 Knee Arthroscopy: Postoperative Instructions John P. Woll, MD Knee arthroscopy is a commonly performed procedure that is much less invasive than previous open techniques, but it is still an operation,
Knee Arthroscopy: Postoperative Instructions John P. Woll, MD Knee arthroscopy is a commonly performed procedure that is much less invasive than previous open techniques, but it is still an operation,
TIBIAL PLATEAU FRACTURE
 TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
Tibial shaft fracture surgery (tibial nailing)
 Tibial shaft fracture surgery (tibial nailing) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we
Tibial shaft fracture surgery (tibial nailing) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we
At Home After Surgery
 Now that your surgery is done, your focus should be on healing. If you follow the recommendations listed in this section, you will help ensure that your new hip will last for the rest of your life. patients.d-h.org/ortho/hips
Now that your surgery is done, your focus should be on healing. If you follow the recommendations listed in this section, you will help ensure that your new hip will last for the rest of your life. patients.d-h.org/ortho/hips
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
A Patient s Guide to Rotational Deformities in Children
 A Patient s Guide to Rotational Deformities in Children 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Rotational Deformities in Children 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
introduction jointunderstanding benefits of knee-replacement surgery
 introduction When knee pain becomes so severe that drugs do not provide relief or when knee problems make daily activities painful, difficult, or even impossible, surgeons can sometimes replace the damaged
introduction When knee pain becomes so severe that drugs do not provide relief or when knee problems make daily activities painful, difficult, or even impossible, surgeons can sometimes replace the damaged
James R. Romanowski, M.D.
 James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
Hip Replacement Recovery Guide
 Hip Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Safe Activities & Movements... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering...
Hip Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Safe Activities & Movements... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering...
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Total Knee Replacement
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Total Knee Replacement This is a general information packet for patients undergoing Total Knee Replacement. Osteoarthritis (OA) is
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Total Knee Replacement This is a general information packet for patients undergoing Total Knee Replacement. Osteoarthritis (OA) is
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg)
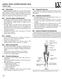 MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
AFTER TOTAL HIP REPLACEMENT
 AFTER TOTAL HIP REPLACEMENT Living in Comfort with Your New Hip Getting Back in Step By having a total hip replacement, you re taking the first step toward returning to an active lifestyle. The next step
AFTER TOTAL HIP REPLACEMENT Living in Comfort with Your New Hip Getting Back in Step By having a total hip replacement, you re taking the first step toward returning to an active lifestyle. The next step
Dr. McCormack Patient Instructions
 Robert G. McCormack, MD, FRCS(c), INC. Diploma in Sport Medicine Professor Orthopaedic Surgery University of British Columbia ANTERIOR CRUCIATE LIGAMENT SURGERY Dr. McCormack Patient Instructions PREPARATION
Robert G. McCormack, MD, FRCS(c), INC. Diploma in Sport Medicine Professor Orthopaedic Surgery University of British Columbia ANTERIOR CRUCIATE LIGAMENT SURGERY Dr. McCormack Patient Instructions PREPARATION
HemiCap Knee Resurfacing and Joint preservation Post-operative Instructions
 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 ORTHOPAEDIC WARD: 01-293 8687 /01-293 6602 PHYSIOTHERAPY DEPARTMENT: 01-2936692 HemiCap Knee Resurfacing and Joint preservation Post-operative Instructions Please
BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 ORTHOPAEDIC WARD: 01-293 8687 /01-293 6602 PHYSIOTHERAPY DEPARTMENT: 01-2936692 HemiCap Knee Resurfacing and Joint preservation Post-operative Instructions Please
Total Hip Replacement. Find out why Total Hip Replacement may be right for you.
 Total Hip Replacement Find out why Total Hip Replacement may be right for you. UNDERSTANDING TOTAL HIP REPLACEMENT This brochure offers a brief overview of hip anatomy, arthritis and total hip arthroplasty.
Total Hip Replacement Find out why Total Hip Replacement may be right for you. UNDERSTANDING TOTAL HIP REPLACEMENT This brochure offers a brief overview of hip anatomy, arthritis and total hip arthroplasty.
General physiotherapy instructions after ACL reconstruction surgery
 General physiotherapy instructions after ACL reconstruction surgery For a successful outcome of surgery, rehabilitation exercises are of utmost importance. These have to be started from the day following
General physiotherapy instructions after ACL reconstruction surgery For a successful outcome of surgery, rehabilitation exercises are of utmost importance. These have to be started from the day following
POSTERIOR TIBIAL TENDON RUPTURE
 POSTERIOR TIBIAL TENDON RUPTURE Description Expected Outcome Posterior tibial tendon rupture is a complete tear of the posterior tibial tendon. This structure is the tendon attachment of leg muscles (posterior
POSTERIOR TIBIAL TENDON RUPTURE Description Expected Outcome Posterior tibial tendon rupture is a complete tear of the posterior tibial tendon. This structure is the tendon attachment of leg muscles (posterior
Patellar Instability. OrthoInfo Patella Instability Page 1 of 5
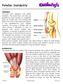 Patellar Instability OVERVIEW You have been diagnosed with patella instability. This means that your knee cap (patella) has been partially or completely going out of place and is not tracking well against
Patellar Instability OVERVIEW You have been diagnosed with patella instability. This means that your knee cap (patella) has been partially or completely going out of place and is not tracking well against
The S.T.A.R. Scandinavian Total Ankle Replacement. Patient Information
 The S.T.A.R. Scandinavian Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please
The S.T.A.R. Scandinavian Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please
ANTERIOR CRUCIATE LIGAMENT INFORMATION PACKET
 ANTERIOR CRUCIATE LIGAMENT INFORMATION PACKET Anterior Cruciate Ligament (ACL) Posterior Cruciate Ligament (PCL) Michael Angeline, MD Orthopedic and Sports Medicine Mercy Health System - 1 - Instructions
ANTERIOR CRUCIATE LIGAMENT INFORMATION PACKET Anterior Cruciate Ligament (ACL) Posterior Cruciate Ligament (PCL) Michael Angeline, MD Orthopedic and Sports Medicine Mercy Health System - 1 - Instructions
Knee arthroscopy. Physiotherapy Department. Patient information leaflet
 Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
OSCELL MICROFRACTURE OR DRILLING OPERATION (PATELLOFEMORAL SITES) PATIENT ADVICE.
 OSCELL MICROFRACTURE OR DRILLING OPERATION ( SITES) PATIENT ADVICE. Anatomy of the Right Knee example of a trochlea articular defect site Knee Straight Knee Bent KEY: Patella Kneecap Trochlea Groove on
OSCELL MICROFRACTURE OR DRILLING OPERATION ( SITES) PATIENT ADVICE. Anatomy of the Right Knee example of a trochlea articular defect site Knee Straight Knee Bent KEY: Patella Kneecap Trochlea Groove on
A Patient information guide to. Ankle Arthroscopy. Foot and Ankle Unit. Mr Amit Amin Mr Ali Abbasian ANKLE ARTHROSCOPY JAN
 A Patient information guide to Ankle Arthroscopy Foot and Ankle Unit Mr Amit Amin Mr Ali Abbasian 1 What does surgery involve? An ankle arthroscopy is a keyhole operation to gain access to the inside of
A Patient information guide to Ankle Arthroscopy Foot and Ankle Unit Mr Amit Amin Mr Ali Abbasian 1 What does surgery involve? An ankle arthroscopy is a keyhole operation to gain access to the inside of
ANTERIOR KNEE PAIN. Explanation. Causes. Symptoms
 ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
Tibial Nailing for Tibial Shaft Fracture
 Tibial Nailing for Tibial Shaft Fracture Patient Information Trauma and Orthopaedics Department Author ID: KC Leaflet Number: Musc 015 Name of Leaflet: Tibial Nailing for Nail Shaft Fracture Version: 4
Tibial Nailing for Tibial Shaft Fracture Patient Information Trauma and Orthopaedics Department Author ID: KC Leaflet Number: Musc 015 Name of Leaflet: Tibial Nailing for Nail Shaft Fracture Version: 4
Knee Arthroplasty Total knee Arthroplasty Hemi Knee Arthroplasty
 P A T IENT INFORMAT ION Knee Arthroplasty Total knee Arthroplasty Hemi Knee Arthroplasty Please pack this booklet with your belongings that you will bring to hospital. You will need to refer to this booklet
P A T IENT INFORMAT ION Knee Arthroplasty Total knee Arthroplasty Hemi Knee Arthroplasty Please pack this booklet with your belongings that you will bring to hospital. You will need to refer to this booklet
Information for patients preparing for recovery at home. You have had an anesthetic or narcotic medicine.
 Hip Arthroscopy Information for patients preparing for recovery at home Read this brochure to learn about: How to take care of yourself at home How to cope with pain Problems to watch for When to get medical
Hip Arthroscopy Information for patients preparing for recovery at home Read this brochure to learn about: How to take care of yourself at home How to cope with pain Problems to watch for When to get medical
Anterior Cruciate Ligament (ACL) Reconstruction
 Further information Information on who to contact, i.e. web sites / telephone numbers of other departments / organisations which may be of help. How to contact us Watford General Hospital West Hertfordshire
Further information Information on who to contact, i.e. web sites / telephone numbers of other departments / organisations which may be of help. How to contact us Watford General Hospital West Hertfordshire
Lumbar Decompression GUIDELINES FOR PATIENTS HAVING A. Lumbar Decompression
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
Hip Surgery and Mobility
 Orthopedic Nursing, Part 1 Hip Surgery and Mobility Nursing Best Practice Guidelines Clinical Indications for Hip Surgery Selected fractures of the hip Unremitting pain and irreversible damaged joint from
Orthopedic Nursing, Part 1 Hip Surgery and Mobility Nursing Best Practice Guidelines Clinical Indications for Hip Surgery Selected fractures of the hip Unremitting pain and irreversible damaged joint from
PATELLA INSTABILITY AND REALIGNMENT
 Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando PATELLA INSTABILITY
Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando PATELLA INSTABILITY
Patella Instability in Children and Adolescents
 Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
Patella Instability in Children and Adolescents Description Patella Instability is an injury to the kneecap (patella) affecting the joint it forms with the thigh bone (femur) Patella Instability can occur
