Platelet Rich Plasma: Current Indications and Use In Orthopaedic Care
|
|
|
- Lester Reed
- 5 years ago
- Views:
Transcription
1 Platelet Rich Plasma: Current Indications and Use In Orthopaedic Care Author: Richard Judd Robins, MD, Assistant Professor of Surgery Uniformed Services University of the Health Sciences Dept. of Orthopaedics; Sports Medicine Service U.S. Air Force Academy Abstract Platelet Rich Plasma (PRP) is a ubiquitous term for a type of therapy that applies autologous platelets collected from whole blood and then concentrated via centrifuge that are re-applied to injured musculoskeletal tissue. The intent of most PRP therapies is to locally create or support a healing response, that instigates earlier healing, or to initiate a response in chronic degenerative and painful tissue. Complicating research efforts are the high number of different types and methods of PRP therapies, and the multiple anatomic and tissue sites of treatment that may potentially benefit from PRP. One of the greatest challenges in the development of PRP therapy have been translating promising laboratory and animal study results to clinical studies outcomes. While enthusiasm for PRP therapy has often exceeded the evidence to support therapeutic benefits, recent studies and experience does support the use of specific types of PRP therapy in specific degenerative and injury patterns. Keywords: Platelet Rich Plasma; Tendinosis; Osteoarthritis; Injection Therapy Page 1
2 1. Introduction Recovery from musculoskeletal injuries at times can be a slow and incomplete process leading to prolonged time away from work, sport, and loss of functional capacity. The repair process after injury starts with the inflammatory process, and is regulated by complex interactions of multiple growth factors to help restore damaged tissue. Over the last decade, efforts to improve or expedite healing injuries in the musculoskeletal system have focused on applying these growth factors. PRP has gained traction in research and treatment efforts as PRP provides a relatively simple, low cost, and fairly easy mode to acquire these growth factors in what is assumed to be physiologically balanced concentrations that can then be applied to damaged tissue.(kon, Filardo, Di Martino, & Marcacci, 2011) PRP is obtained from a patient s own whole blood (typically 15-60cc) that is centrifuged once or twice to separate out platelets with (double spin) or without (single spin) white blood cells, with concentrations anywhere from twice to nine times normal concentrations. It is most often mixed with an exogenous activator of platelets (ex: thrombin, calcium chloride, calcium citrate) which causes release of alpha granules from the platelets containing multiple cytokines and growth factors. The activated platelet concentrate is then injected into a damaged musculoskeletal tissue site (tendon, muscle, joint/cartilage, etc.) to either activate or enhance a healing response. In more acute settings, endogenous activation relies on the platelet concentrate being activated when coming in contact with damaged collagen or other musculoskeletal tissue. Protocols call for either 1 to 4 injections spread out at least 4 to 7 days based upon evidence that release of cytokines and growth factors primarily occur in the first hours after injection, while platelet viability and cytokine release continues up to seven days after activation.(marx, 2004) Categories of PRP application fall into the 4 areas: chronic tendinosis, acute ligament injury, muscle injury, and intraoperative tissue repair augmentation.(hsu et al., 2013) Enthusiasm for clinical use and application of PRP has often outpaced solid evidence to support its use.(sampson, Gerhardt, & Mandelbaum, 2008) The typical pattern in PRP research has shown very promising results in laboratory and animal studies, but translation of PRP therapy to clinical trials has been at times disappointing.(robins, 2014) However, recent advances in specific areas of treatment with specific types of PRP therapy have demonstrated good evidence to support use in clinical settings.(fitzpatrick, Bulsara, & Zheng, 2017; Gosens, Peerbooms, van Laar, & den Oudsten, 2011; Hsu et al., 2013; Meheux, McCulloch, Lintner, Varner, & Harris, 2016) 2. Basic Science of PRP PRP falls under a class of therapeutic approaches termed biologics, which refers to using natural products to augment the physiological process of healing. At times, PRP may be classified under the umbrella of prolotherapy or regenerative medicine, but PRP does not precisely meet the definition or the intent of these therapeutic philosophies. From a regulatory standpoint, the FDA defines biologics or biologic therapy as requiring minimal manipulation of an autologous source of cellular treatment, and whose efficacy does not relate to the metabolic activity of the cells being applied for therapy. Biologic treatment currently falls into 3 classes of therapy: growth factors (PRP), cells (ex: stem cells), and tissue patches for surgical augmentation.(williams, Moran, Bradley, N, & Dines, 2015) Page 2
3 PRP therapy is based on the premise that it benefits musculoskeletal tissue healing due to the high concentration of cytokines and growth factors that normally are involved in the initial and follow-on stages of the inflammatory process at recruiting and stimulating cell proliferation as well as producing extra-cellular matrix proteins.(anitua et al., 2006; Williams et al., 2015) A list of these growth factors and cytokines are listed in Table 1. While the theoretical advantage of using PRP administers these growth factors in physiological concentrations relative to each other, the reality is that these concentrations vary depending of the method of PRP preparations, amount of whole blood used, type of platelet activation, and the final total volume of PRP injected.(fitzpatrick, Bulsara, McCrory, Richardson, & Zheng, 2017) In addition, the concentration of platelets and associated cytokines varies between patients, and even within the same patient at different points in time.(creaney & Hamilton, 2008; Mazzocca et al., 2012) In other words, a patient receiving a series of treatment of 3 PRP injections one week apart, even when standardizing for type of PRP preparation, activation, and volume administered, will receive different concentrations of platelets in each of the PRP injections due to the variability of available platelets and leukocytes in the whole blood obtained from the patient at the time of collection. 2.1 Challenges in PRP Research Many factors make interpreting and applying PRP research results challenging to clinical application. Two of these biggest factors include the plethora of different PRP preparations available for use, and the challenge of translating the success found in laboratory and animal research to clinical outcomes PRP Preparation Variability PRP encompasses many variations of preparation methods, but can be best divided into plasma-based and buffy-coat based preparations. Plasma-based preparations are a result of a single-spin centrifuge process, which separates out and concentrates red blood cells, the buffy coat made up of white-blood cells, and plasma, which contains platelets concentrated on average between 2-5 times that of whole blood (Figure 1). If the preparation undergoes a second centrifuge spin (double spin), this serves to concentrate the platelets even further, resulting in a platelet-rich and a platelet-poor plasma, but also include leukocytes in the platelet rich portion of the plasma. This results in different effects from the prepared PRP, with plasma based, single-spin PRP preparations demonstrating anabolic and cartilage extra-cellular-matrix stabilization effects, while white blood cell-containing double-spin PRP preparations create a stronger inflammatory and catabolic response.(braun, Kim, Chu, & Dragoo, 2014) As a result, the indications of treatment may dictate that different preparations may provide a better response based upon the tissue environment and pathology being treated. Page 3
4 Page 4
5 Figure 1. Sample of Single-Spin PRP Preparation Immediately After Centrifugation Challenges with Comparison Analysis When evaluating results of PRP, it is imperative to determine the type of preparation of PRP used. Mishra et al and DeLong and associates proposed classification systems be adopted when evaluating and comparing PRP that takes into account the concentration of platelets, the type of activation that occurs, and the absence or presence of white blood cells.(delong, Russell, & Mazzocca, 2012; A. Mishra, Harmon, Woodall, & Vieira, 2012) Using DeLong s PAW classification system, over 32 different types of PRP classifications are identified. DeLong s classification could be delineated even further by sub-classifying the different substrates used for exogenous activation (thrombin, calcium-chloride, calcium citrate, etc.) and endogenous preparations which could lead to approximately 160 different classifications of PRP. While multiple systematic reviews and metanalyses have been accomplished on PRP treatments, caution is recommended when interpreting the findings of all of these comparison studies, as all have used a collation of different PRP preparation studies to draw conclusions. Hall and colleagues noted that with the qualitative and quantitative differences, reported evidence for clinical effectiveness of PRP cannot be generalized across preparation systems. (Hall, Band, Meislin, Jazrawi, & Cardone, 2009) Page 5
6 3. Current Clinical Applications In addition to the multitude of PRP preparations, the different sites and types of injured tissue make comparison of PRP difficult. However, recent advances in specific pathologies has shown promising results, in particular for the treatment of mild to moderate degenerative joint disease of the knee, lateral epicondylitis, and patellar tendinitis. Other areas of treatment have included muscle belly injury, and surgical augmentation, in particular with rotator cuff tendon repair and anterior cruciate ligament reconstruction. 3.1 Knee Osteoarthritis Use of PRP in preclinical data provided evidence that single spin, leukocyte poor preparations of PRP reduced inflammatory cytokines (in particular IL- 1b), and helped to stabilize the extracellular matrix of damaged hyaline cartilage.(durant et al., 2017; Filardo et al., 2015) In particular, PRP preparations with higher concentrations of white blood cells seemed to have a catabolic effect and increased the inflammatory response for intra-articular synovial cells verses plasma based PRP preparations that demonstrated an in-vitro anabolic, anti-inflammatory effect.(braun et al., 2014; Filardo et al., 2012; Osterman et al., 2015; Riboh, Saltzman, Yanke, Fortier, & Cole, 2016) Multiple lower level studies using plasma based PRP with low concentrations of white blood cells have been completed comparing this type of PRP to other forms of intra-articular injection therapy, which demonstrated positive effects at reducing pain and improving outcomes scores in degenerative joint disease of the knee.(cerza et al., 2012; Filardo et al., 2013; Filardo et al., 2011) Smith performed a double blinded randomized control trial comparing autologous conditioned plasma (ACP single spin, leukocyte poor, 2-5x platelet concentrated PRP) vs. saline injections in small but acceptably powered populations of patients with mild to moderate degenerative joint disease, and demonstrated statistically significant improvements in visual analog pain scores for 12 months after therapy, with 78% improvement in WOMAC scores compared to 7% in the placebo control group.(smith, 2016) Cole et al. performed a double blinded randomized control trial comparing hyaluronic acid vs the same PRP preparation used in the Smith study, which demonstrated improvement in pain symptoms in both groups, but significantly better outcomes scores at 24 weeks in the PRP study group.(cole, Karas, Hussey, Pilz, & Fortier, 2017) A recent metanalysis, while suffering from the limitations of comparative studies as noted above, evaluated PRP injections for knee degenerative disease and concluded PRP injections resulted in clinically significant improvements out to 12 months after therapy, with pain scores and clinical outcomes that were better than hyaluronic acid injections at 3-12 months.(meheux et al., 2016) Indirect evidence demonstrated leukocyte poor PRP injections resulted in better clinical outcomes compared to hyaluronic acid than leukocyte rich PRP injections vs hyaluronic acid, but no direct comparison between the PRP preparations have been completed at this time. Another meta-analysis of only level-i studies demonstrated more pain relief and functional improvement in treating symptomatic knee osteoarthritis at 1 year post-injection when compared to hyaluronic acid injections.(dai, Zhou, Zhang, & Zhang, 2017) In summary, there is growing evidence to support the use of PRP injections for treatment of degenerative joint disease of the knee, with some basic science and clinical evidence favoring use of PRP preparations low in white blood cells.(hunt, 2017) Page 6
7 3.2 Lateral Epicondylitis PRP therapy was initially thought to be a potentially beneficial treatment for chronic tendinopathy and tendinosis. To date, lateral epicondylitis has demonstrated the best response to PRP treatment of all chronic tendinopathy conditions. Unlike treatment of intra-articular and cartilage pathology, leukocyte-rich PRP therapies have demonstrated better pain scores and functional outcomes than leukocyte-poor PRP as well as have performed better than local anesthetics, corticosteroids, or dry needling.(fitzpatrick, Bulsara, & Zheng, 2017) Gosens and colleagues conducted a randomized control trial comparing corticosteroid injections to leukocyte-rich PRP, and noted 73% of patients improved in pain (VAS) and functional (DASH) outcomes scores versus approximately 50% in the corticosteroid group over the 1 st year.(peerbooms, Sluimer, Bruijn, & Gosens, 2010) They also noted that the corticosteroid group initially had a quick response compared to the PRP group during the 1 st 6 to 12 weeks, but the effects dropped off rapidly and returned to baseline, while the PRP group continued to demonstrate clinically significant improvements over the 2 years following treatment.(gosens et al., 2011) These studies had similar findings when compared to Mishra and Pavelko s study which compared leukocyte-rich PRP to local anesthetic, and was able to find significant improvement in both VAS and functional outcomes out to 25.6 months.(a. Mishra & Pavelko, 2006) A recent double blinded randomized control trail conducted at multiple centers compared leukocyte-rich PRP added to dry needling of patients who have failed prior conservative therapy. The study resulted in 84% of the PRP group having successful treatment vs. 68% in the needling-only group.(a. K. Mishra et al., 2014) A systematic review in 2013 noted that of 9 studies, only 2 randomized control trials showed no differences compared to corticosteroid injections, but that these studies were limited to 3 month follow up.(ahmad et al., 2013) In contrast to this, a systematic review conducted in 2014 stated that no benefit was found from performing PRP for lateral epicondylitis.(de Vos, Windt, & Weir, 2014) However, these findings have been disputed as using incorrect grading of the included studies, and drawing incorrect assumptions and conclusions based upon the studies included due to limited (<24 week) follow up.(gosens & Mishra, 2014) A recent randomized control trial compared leukocyte-poor PRP to corticosteroid injections, and found similar positive results in pain and DASH outcomes scores, favoring PRP treatment at 1 year.(lebiedzinski et al., 2015) In conclusion, several small and large randomized trials have demonstrated better long-term outcomes with leukocyte-rich PRP injections over corticosteroid injections, with a more recent study demonstrating similar results with leukocyte-poor PRP over corticosteroids. 3.3 Ulnar Collateral Ligament (UCL) Injuries to the UCL are common in overhead athletes, in particular to pitchers in baseball. While full UCL sprains require surgery and generally have good outcomes at returning athletes back to sports, recovery can take upwards of 12 months. In recent years, efforts have been made to evaluate if nonoperative interventions can be used to treat partial UCL tears over surgery. Podesta et al. evaluated grade I and II UCL sprains in 34 athletes treated with leukocyterich PRP with ultrasound guidance.(podesta, Crow, Volkmer, Bert, & Yocum, 2013) They noted by 6 months, 88% of athletes had returned to play at the same level without complaints, improvement on Page 7
8 outcomes scores, and decrease in medial elbow joint space opening from 7mm to 2.5mm. Dines and colleagues noted an earlier return to sport in 4 of 6 professional athletes with use of leukocyte-poor PRP for partial UCL injuries in baseball players, with return to competition between 5-24 weeks (average 12 weeks).(dines et al., 2016) 72% of athletes had a good or excellent outcome. Though limited data is available, PRP therapy may be considered in partial UCL injuries as an option prior to surgical reconstruction. 3.3 Patellar Tendinosis Initial clinical results demonstrated promise for using PRP in patellar tendinosis. A pilot study of 20 patients with refractory jumper s knee were treated with 3 injections using 5mL of a double-spin, leukocyte-rich PRP (6x concentration of platelets) preparation activated with calcium chloride with 15 days in-between each injection.(kon et al., 2009) At 6 months, statistically significant clinical improvements were noted in all factors including physical functional, with 80% of participants returned back to sport 4 months after therapy was administered. A follow-on comparative study evaluated patients refractory to established physical therapy treated with the same type of PRP as noted above with physical therapy only. The study demonstrated improved outcomes at 6 months in outcomes and pain scores in the study group, which represents a difficult patient cohort to successfully treat.(filardo et al., 2010) A recent randomized control trial compared eccentric strengthening, dry needling, and one leukocyte-rich PRP to eccentric exercises and dry needling only.(dragoo, Wasterlain, Braun, & Nead, 2014) Results demonstrated PRP helped to improve initial recovery, but the results between the two groups equalized by 26 weeks. Gosens and colleagues noted clinically meaningful improvement after treatment with PRP in patients with patellar tendinopathy, but saw greater improvement in the patient cohort who had not had prior corticosteroid, ethoxysclerol, or surgery.(gosens, Den Oudsten, Fievez, van 't Spijker, & Fievez, 2012) Using 3 injections of leukocyte poor PRP (ACP) in a prospective study, 75% of patients had the ability to return to sports, with 57% of patients demonstrating complete resolution of tendon structure at 3 months from treatment. At 2 years, all patients were satisfied with the procedure with significant improvements in outcomes and pain scores.(charousset, Zaoui, Bellaiche, & Bouyer, 2014) A recent systematic review of 6 randomized control trials and 19 total studies demonstrated that patellar tendinopathy treated with PRP demonstrated benefits in the higher level randomized control trials, and the treatment benefits were supported by findings in lower-level studies.(filardo, Di Matteo, Kon, Merli, & Marcacci, 2016) At this point in time, there is support for use of PRP in the treatment of patellar tendinosis with positive benefit, but questions on type of preparation and number of injections remain unclarified. 3.4 Achilles Tendinosis Use of PRP in the treatment of Achilles tendinosis has been disappointing. de Vos and associates performed a randomized control trial comparing treatment for Achilles tendinosis with a double-blind injection of leukocyte-rich PRP vs saline.(de Vos et al., 2010) Both groups improved and there was no statistically significant difference between the control and PRP groups. This group performed a follow-up study with ultrasound and clinical outcomes at 1 year out from treatment, and again found no difference between the PRP and control groups.(de Jonge et al., 2011) 24 studies were included Page 8
9 in a systematic review which demonstrated mixed outcomes, and with higher level studies demonstrating no measurable difference between the PRP and control groups.(filardo et al., 2016) This collection of studies also suffers from inappropriate comparison as different preparations and numbers of injections were used. 4. Muscle injury Treatment of muscle injury has been proposed to potentially benefit from PRP therapy. While regeneration of muscle tissue is possible after fetal development, many intra-muscular injuries heal with the development of a dense fibrotic scar, which forms at 7-14 days after injury. Therefore, an important aspect that has yet to be ascertained is the timing and appropriate dosing of growth factors to help modulate this process. There is also appropriate concern that the application of PRP may in fact promote the formation of fibrosis and scar due to the high concentrations of growth factors contained in PRP.(Kon et al., 2011) Another factor limiting use of PRP in muscle injury is that the World Anti-Doping Agency (WADA) has listed PRP intramuscular injections as a prohibited intervention for athletes, due to the possible systemic anabolic effects of PRP, making this therapy for muscle injury limited to sports not regulated by WADA.(Kon et al., 2011; Wasterlain, Braun, Harris, Kim, & Dragoo, 2013) 4.1 Hamstring Injury Hamstring injuries are one of the most common injuries encountered in sports medicine. Despite the high number of injuries, treatment is restricted to physical therapy and conservative measures. Time away from sports can typically be 6 weeks, and risk of recurrent injury persists during the first season following recovery. Initial laboratory data supported the possible use of PRP in shortening the length of time for return to sports and normal function.(hammond, Hinton, Curl, Muriel, & Lovering, 2009) Mejia and Bradley treated 12 NFL players with hamstring injuries using single spin PRP (ACP) with the 1 st injection hours after injury, and a 2 nd injection 5-7 days later, with a 3 rd injection administered only if necessary. In their small case series, they noted a 1 day earlier return to play (RTP) for grade I injuries, 5 day earlier RTP for grade II injuries, and a 1 game difference in return to play. (Mejias & Bradley, 2011) The most notable finding was a reduction in recurrent injury to 0, where they typically experience 2-4 recurrent hamstring injuries per season over their 20 year experience. These findings have not been validated in other studies. Rettig and colleagues studied the use of 1 injection of leukocyte-rich PRP administered hours of injury in NFL players with hamstring injury, but noted no difference in time to return to play between those treated with PRP and those without treatment.(rettig, Meyer, & Bhadra, 2013) In the Dutch-HIT study, there was no difference in return to play or difference in 1 year re-injury rate in their double-blind randomized control trial using 2 injections of the same type of single-spin leukocytepoor PRP (ACP) used in Mejia and Bradley s study.(reurink et al., 2015) The difference between these two studies is that the latter study initiated the 1 st injection within 5 days after injury, while Mejia and Bradley administered the first injection hours after injury. Hamid et al. in a randomized control trial conducted in Malaysia used a single 3mL leukocyte-rich PRP injection given between 1-7 days after injury and compared to a physical rehabilitation group.(hamid, Yusof, & Mohamed Ali, 2014) The PRP group demonstrated a significantly faster return to sport than the control group with lower pain Page 9
10 scores, and concluded PRP therapy to be helpful in early return to sports. However, another 3-arm study conducted in Qatar evaluating soccer football athletes found no difference in RTP when comparing the same leukocyte-rich PRP preparation used in the Hamid et al. study combined with physical rehabilitation when compared to the physical rehabilitation-only group.(hamilton et al., 2015) Davenport et al. placed a single injection of PRP vs whole blood and found no significant differences in outcomes between the groups.(davenport et al., 2015) Zanon and colleagues from Italy performed a leukocyte-rich series of 2 or 3 PRP injections starting hours after injury in professional soccer football players, and found PRP did not shorten return to sport, had a 12% recurrent injury rate, but did lead to a smaller scar at the injury site on followup imaging studies.(zanon et al., 2016) A recent meta-analysis showed no effect of PRP therapy on acute hamstring injury, and identified improved study design for future research efforts.(pas et al., 2015) The concern with PRP for hamstring muscle injury therapy is confounded by not only preparation variation and number of injections, but also timing for initiation of treatment before stronger recommendations can be made regarding the use of PRP for treatment of acute hamstring injury. 5. Surgical Augmentation Use of PRP therapy for surgical augmentation has initially demonstrated promise in pre-clinical studies, but to date, there has been no conclusive data to suggest efficacy or benefit in terms of clinical outcomes.(robins, 2014) Two main areas of focus have been in anterior cruciate ligament reconstruction (ACL) surgery and rotator cuff repair Anterior Cruciate Ligament Reconstruction Multiple studies have evaluated the effects of PRP on ACL graft maturation which would presume better healing and lower re-tear rates. A recent systematic review concluded that PRP may provide a 20-30% beneficial effect on graft maturation, but that there is no evidence of improved graft-bone interface healing, nor is there any difference in clinical outcomes.(vavken, Sadoghi, & Murray, 2011) In both a level I randomized control trial, and in the large Multicenter Orthopaedic Outcomes Network (MOON) ACL study cohort, addition of PRP to ACL allografts was shown to have no significant difference in any outcomes or parameters following surgery.(magnusson, Romano, Hallberg, Wadenvik, & Breimer, 1998; Nin, Gasque, Azcarate, Beola, & Gonzalez, 2009) In relation to treatment of patellar tendinopathy, two studies have evaluated adding 2 different types of PRP gel preparations to the harvest site of the central portion of the patellar tendon created during ACL reconstruction.(de Almeida et al., 2012; Seijas et al., 2013) Both studies showed significant reduction in early postoperative pain, and de Almeida et al. demonstrated significantly-improved healing compared to the control group at 6 months on MRI. However, one of the limitations to de Almedia et al. s application of PRP is that 50mL of PRP was applied to the harvest site, which requires 450mL of blood volume be at least temporarily withdrawn for preparation of this large volume of PRP. In Sejia and colleagues study, only 4cc of PRP (PRGF) was applied to the donor sites, which reduced pain during the first 2 months compared to the control group. While use of PRP may reduce pain in the postoperative period, further research is needed to determine if the Page 10
11 cost-effectiveness of this application of PRP is a reasonable option. 5.2 Rotator Cuff Repair PRP applied to augment rotator cuff repair has followed the pattern of early promising results in pre-clinical and laboratory data, but without demonstrating benefit with application in clinical series.(robins, 2014) In a randomized control trial, application of PRP fibrin matrix (PRFM) to the rotator cuff repair site was found to correlate with worse healing rates, indicating the possibility the PRP gel interfered rather than benefited tendon-tobone healing.(rodeo et al., 2012) Out of 18 randomized control trials on PRP augmentation in rotator cuff repair, 10 demonstrated no differences between intervention and control groups, 2 demonstrated improved pain control during the 1 st two months after surgery, and 5 showed lower re-tear rates on imaging but not necessarily any difference in clinical outcomes.(filardo et al., 2016) The high degree of heterogeneity in application and types of injections utilized in rotator cuff repair make interpreting which type of PRP and when to inject difficult to determine. In addition the cost-effectiveness of adding PRP to rotator cuff repair would have to show at least a reduced re-tear rate of 9.1% to be worth adding to surgical treatment.(samuelson, Odum, & Fleischli, 2016) Metanalysis demonstrated PRP had no effect on large rotator cuff repairs, did help in small and medium tears at reducing re-tear rate, but was too costly to make adding PRP to this cohort of injury justifiable.(vavken et al., 2015) 6. Conclusion PRP, as a biologic therapy, presents the possibility of benefit to multiple musculoskeletal injury sites. Use of leukocyte-poor PRP in the treatment of knee osteoarthritis has demonstrated significant benefits in multiple trials and case series. Use of PRP in the treatment of lateral epicondylitis, in particular with leukocyterich preparations, had some evidence to support its use for therapeutic benefit. A small amount of evidence supports the possibility of PRP helping in treating partial UCL tears in the elbow. There is also limited evidence to consider the use of PRP in the management of patellar tendinosis. Most evidence supports not using PRP in the treatment of Achilles tendon partial tears or tendinopathy. Use of PRP in muscle injury and specifically in hamstring injury has mixed results in the data, and it appears that besides type and number of injections, the timing of PRP injections is important in promoting muscle regeneration versus inadvertently stimulating increased fibrosis across the injury site. Finally, PRP in augmenting ACL and rotator cuff tendon repair have mixed results and cannot be recommended for routine use at this point in time. Page 11
12 References 1. Ahmad, Z., Brooks, R., Kang, S. N., Weaver, H., Nunney, I., Tytherleigh- Strong, G., & Rushton, N. (2013). The effect of platelet-rich plasma on clinical outcomes in lateral epicondylitis. Arthroscopy, 29(11), doi: /j.arthro Anitua, E., Sanchez, M., Nurden, A. T., Nurden, P., Orive, G., & Andia, I. (2006). New insights into and novel applications for platelet-rich fibrin therapies. Trends Biotechnol, 24(5), doi: /j.tibtech Braun, H. J., Kim, H. J., Chu, C. R., & Dragoo, J. L. (2014). The effect of platelet-rich plasma formulations and blood products on human synoviocytes: implications for intraarticular injury and therapy. Am J Sports Med, 42(5), doi: / Cerza, F., Carni, S., Carcangiu, A., Di Vavo, I., Schiavilla, V., Pecora, A.,... Ciuffreda, M. (2012). Comparison between hyaluronic acid and plateletrich plasma, intra-articular infiltration in the treatment of gonarthrosis. Am J Sports Med, 40(12), doi: / Charousset, C., Zaoui, A., Bellaiche, L., & Bouyer, B. (2014). Are multiple platelet-rich plasma injections useful for treatment of chronic patellar tendinopathy in athletes? a prospective study. Am J Sports Med, 42(4), doi: / Cole, B. J., Karas, V., Hussey, K., Pilz, K., & Fortier, L. A. (2017). Hyaluronic Acid Versus Platelet-Rich Plasma: A Prospective, Double-Blind Randomized Controlled Trial Comparing Clinical Outcomes and Effects on Intra-articular Biology for the Treatment of Knee Osteoarthritis. Am J Sports Med, 45(2), doi: / Creaney, L., & Hamilton, B. (2008). Growth factor delivery methods in the management of sports injuries: the state of play. Br J Sports Med, 42(5), doi: /bjsm Dai, W. L., Zhou, A. G., Zhang, H., & Zhang, J. (2017). Efficacy of Platelet- Rich Plasma in the Treatment of Knee Osteoarthritis: A Meta-analysis of Randomized Controlled Trials. Arthroscopy, 33(3), e651. doi: /j.arthro Davenport, K. L., Campos, J. S., Nguyen, J., Saboeiro, G., Adler, R. S., & Moley, P. J. (2015). Ultrasound- Guided Intratendinous Injections With Platelet-Rich Plasma or Autologous Whole Blood for Treatment of Proximal Hamstring Tendinopathy: A Double-Blind Randomized Controlled Trial. J Ultrasound Med, 34(8), doi: /ultra de Almeida, A. M., Demange, M. K., Sobrado, M. F., Rodrigues, M. B., Pedrinelli, A., & Hernandez, A. J. (2012). Patellar tendon healing with platelet-rich plasma: a prospective randomized controlled trial. Am J Sports Med, 40(6), doi: / de Jonge, S., de Vos, R. J., Weir, A., van Schie, H. T., Bierma-Zeinstra, S. M., Verhaar, J. A.,... Tol, J. L. (2011). Page 12
13 One-year follow-up of platelet-rich plasma treatment in chronic Achilles tendinopathy: a double-blind randomized placebo-controlled trial. Am J Sports Med, 39(8), doi: / de Vos, R. J., Weir, A., van Schie, H. T., Bierma-Zeinstra, S. M., Verhaar, J. A., Weinans, H., & Tol, J. L. (2010). Platelet-rich plasma injection for chronic Achilles tendinopathy: a randomized controlled trial. JAMA, 303(2), doi: /jama de Vos, R. J., Windt, J., & Weir, A. (2014). Strong evidence against platelet-rich plasma injections for chronic lateral epicondylar tendinopathy: a systematic review. Br J Sports Med, 48(12), doi: /bjsports DeLong, J. M., Russell, R. P., & Mazzocca, A. D. (2012). Platelet-rich plasma: the PAW classification system. Arthroscopy, 28(7), doi: /j.arthro Dines, J. S., Williams, P. N., ElAttrache, N., Conte, S., Tomczyk, T., Osbahr, D. C.,... Ahmad, C. S. (2016). Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High-Level Throwers. Am J Orthop (Belle Mead NJ), 45(5), Dragoo, J. L., Wasterlain, A. S., Braun, H. J., & Nead, K. T. (2014). Plateletrich plasma as a treatment for patellar tendinopathy: a double-blind, randomized controlled trial. Am J Sports Med, 42(3), doi: / Durant, T. J., Dwyer, C. R., McCarthy, M. B., Cote, M. P., Bradley, J. P., & Mazzocca, A. D. (2017). Protective Nature of Platelet-Rich Plasma Against Chondrocyte Death When Combined With Corticosteroids or Local Anesthetics. Am J Sports Med, 45(1), doi: / Filardo, G., Di Matteo, B., Kon, E., Dhillon, M. S., Patel, S., & Marwaha, N. (2013). Platelet-rich plasma for knee osteoarthritis. Am J Sports Med, 41(9), NP doi: / Filardo, G., Di Matteo, B., Kon, E., Merli, G., & Marcacci, M. (2016). Platelet-rich plasma in tendon-related disorders: results and indications. Knee Surg Sports Traumatol Arthrosc. doi: /s Filardo, G., Kon, E., Buda, R., Timoncini, A., Di Martino, A., Cenacchi, A.,... Marcacci, M. (2011). Platelet-rich plasma intraarticular knee injections for the treatment of degenerative cartilage lesions and osteoarthritis. Knee Surg Sports Traumatol Arthrosc, 19(4), doi: /s Filardo, G., Kon, E., Della Villa, S., Vincentelli, F., Fornasari, P. M., & Marcacci, M. (2010). Use of plateletrich plasma for the treatment of refractory jumper's knee. Int Orthop, 34(6), doi: /s Filardo, G., Kon, E., Pereira Ruiz, M. T., Vaccaro, F., Guitaldi, R., Di Martino, A.,... Marcacci, M. (2012). Plateletrich plasma intra-articular injections for cartilage degeneration and osteoarthritis: single- versus doublespinning approach. Knee Surg Sports Page 13
14 Traumatol Arthrosc, 20(10), doi: /s x 23. Filardo, G., Kon, E., Roffi, A., Di Matteo, B., Merli, M. L., & Marcacci, M. (2015). Platelet-rich plasma: why intra-articular? A systematic review of preclinical studies and clinical evidence on PRP for joint degeneration. Knee Surg Sports Traumatol Arthrosc, 23(9), doi: /s Fitzpatrick, J., Bulsara, M., & Zheng, M. H. (2017). The Effectiveness of Platelet-Rich Plasma in the Treatment of Tendinopathy. Am J Sports Med, 45(1), doi: / Fitzpatrick, J., Bulsara, M. K., McCrory, P. R., Richardson, M. D., & Zheng, M. H. (2017). Analysis of Platelet-Rich Plasma Extraction: Variations in Platelet and Blood Components Between 4 Common Commercial Kits. Orthop J Sports Med, 5(1), doi: / Gosens, T., Den Oudsten, B. L., Fievez, E., van 't Spijker, P., & Fievez, A. (2012). Pain and activity levels before and after platelet-rich plasma injection treatment of patellar tendinopathy: a prospective cohort study and the influence of previous treatments. Int Orthop, 36(9), doi: /s Gosens, T., & Mishra, A. K. (2014). Editorial in response to the systematic review by de Vos et al: 'Strong evidence against platelet-rich plasma injections for chronic lateral epicondylar tendinopathy: a systematic review'. Br J Sports Med, 48(12), doi: /bjsports Gosens, T., Peerbooms, J. C., van Laar, W., & den Oudsten, B. L. (2011). Ongoing positive effect of platelet-rich plasma versus corticosteroid injection in lateral epicondylitis: a double-blind randomized controlled trial with 2- year follow-up. Am J Sports Med, 39(6), doi: / Hall, M. P., Band, P. A., Meislin, R. J., Jazrawi, L. M., & Cardone, D. A. (2009). Platelet-rich plasma: current concepts and application in sports medicine. J Am Acad Orthop Surg, 17(10), Hamid, M. S., Yusof, A., & Mohamed Ali, M. R. (2014). Platelet-rich plasma (PRP) for acute muscle injury: a systematic review. PLoS One, 9(2), e doi: /journal.pone Hamilton, B., Tol, J. L., Almusa, E., Boukarroum, S., Eirale, C., Farooq, A.,... Chalabi, H. (2015). Plateletrich plasma does not enhance return to play in hamstring injuries: a randomised controlled trial. Br J Sports Med, 49(14), doi: /bjsports Hammond, J. W., Hinton, R. Y., Curl, L. A., Muriel, J. M., & Lovering, R. M. (2009). Use of autologous platelet-rich plasma to treat muscle strain injuries. Am J Sports Med, 37(6), doi: / Hsu, W. K., Mishra, A., Rodeo, S. R., Fu, F., Terry, M. A., Randelli, P.,... Kelly, F. B. (2013). Platelet-rich plasma in orthopaedic applications: evidence-based recommendations for treatment. J Am Acad Orthop Surg, 21(12), doi: /jaaos Page 14
15 34. Hunt, T. J. (2017). Editorial Commentary: The Time Has Come to Try Intra-articular Platelet-Rich Plasma Injections for Your Patients With Symptomatic Knee Osteoarthritis. Arthroscopy, 33(3), doi: /j.arthro Kon, E., Filardo, G., Delcogliano, M., Presti, M. L., Russo, A., Bondi, A.,... Marcacci, M. (2009). Platelet-rich plasma: new clinical application: a pilot study for treatment of jumper's knee. Injury, 40(6), doi: /j.injury Kon, E., Filardo, G., Di Martino, A., & Marcacci, M. (2011). Platelet-rich plasma (PRP) to treat sports injuries: evidence to support its use. Knee Surg Sports Traumatol Arthrosc, 19(4), doi: /s y 37. Lebiedzinski, R., Synder, M., Buchcic, P., Polguj, M., Grzegorzewski, A., & Sibinski, M. (2015). A randomized study of autologous conditioned plasma and steroid injections in the treatment of lateral epicondylitis. Int Orthop, 39(11), doi: /s Magnusson, S., Romano, E. L., Hallberg, E., Wadenvik, H., & Breimer, M. E. (1998). Soluble saccharides block the inhibition of agonist-induced human platelet aggregation observed after in vitro incubation of human platelet-rich plasma with porcine aortic endothelial cells. Transpl Int, 11(5), Marx, R. E. (2004). Platelet-rich plasma: evidence to support its use. J Oral Maxillofac Surg, 62(4), Mazzocca, A. D., McCarthy, M. B., Chowaniec, D. M., Cote, M. P., Romeo, A. A., Bradley, J. P.,... Beitzel, K. (2012). Platelet-rich plasma differs according to preparation method and human variability. J Bone Joint Surg Am, 94(4), doi: /jbjs.k Meheux, C. J., McCulloch, P. C., Lintner, D. M., Varner, K. E., & Harris, J. D. (2016). Efficacy of Intraarticular Platelet-Rich Plasma Injections in Knee Osteoarthritis: A Systematic Review. Arthroscopy, 32(3), doi: /j.arthro Mejias, H. A., & Bradley, J. P. (2011). The Effects of Platelet-Rich Plasma on Muscle: Basic Science and Clinical Application. Operative Techniques in Sports Medicine, 19(3), Mishra, A., Harmon, K., Woodall, J., & Vieira, A. (2012). Sports medicine applications of platelet rich plasma. Curr Pharm Biotechnol, 13(7), Mishra, A., & Pavelko, T. (2006). Treatment of chronic elbow tendinosis with buffered platelet-rich plasma. Am J Sports Med, 34(11), doi: / Mishra, A. K., Skrepnik, N. V., Edwards, S. G., Jones, G. L., Sampson, S., Vermillion, D. A.,... Rettig, A. C. (2014). Efficacy of platelet-rich plasma for chronic tennis elbow: a double-blind, prospective, multicenter, randomized controlled trial of 230 patients. Am J Sports Med, 42(2), doi: / Page 15
16 46. Nin, J. R., Gasque, G. M., Azcarate, A. V., Beola, J. D., & Gonzalez, M. H. (2009). Has platelet-rich plasma any role in anterior cruciate ligament allograft healing? Arthroscopy, 25(11), doi: /j.arthro Osterman, C., McCarthy, M. B., Cote, M. P., Beitzel, K., Bradley, J., Polkowski, G., & Mazzocca, A. D. (2015). Platelet-Rich Plasma Increases Anti-inflammatory Markers in a Human Coculture Model for Osteoarthritis. Am J Sports Med, 43(6), doi: / Pas, H. I., Reurink, G., Tol, J. L., Weir, A., Winters, M., & Moen, M. H. (2015). Efficacy of rehabilitation (lengthening) exercises, platelet-rich plasma injections, and other conservative interventions in acute hamstring injuries: an updated systematic review and meta-analysis. Br J Sports Med, 49(18), doi: /bjsports Peerbooms, J. C., Sluimer, J., Bruijn, D. J., & Gosens, T. (2010). Positive effect of an autologous platelet concentrate in lateral epicondylitis in a double-blind randomized controlled trial: platelet-rich plasma versus corticosteroid injection with a 1-year follow-up. Am J Sports Med, 38(2), doi: / Podesta, L., Crow, S. A., Volkmer, D., Bert, T., & Yocum, L. A. (2013). Treatment of partial ulnar collateral ligament tears in the elbow with platelet-rich plasma. Am J Sports Med, 41(7), doi: / Rettig, A. C., Meyer, S., & Bhadra, A. K. (2013). Platelet-Rich Plasma in Addition to Rehabilitation for Acute Hamstring Injuries in NFL Players: Clinical Effects and Time to Return to Play. Orthop J Sports Med, 1(1), doi: / Reurink, G., Goudswaard, G. J., Moen, M. H., Weir, A., Verhaar, J. A., Bierma-Zeinstra, S. M.,... Dutch, H. I. T. s. I. (2015). Rationale, secondary outcome scores and 1-year follow-up of a randomised trial of platelet-rich plasma injections in acute hamstring muscle injury: the Dutch Hamstring Injection Therapy study. Br J Sports Med, 49(18), doi: /bjsports Riboh, J. C., Saltzman, B. M., Yanke, A. B., Fortier, L., & Cole, B. J. (2016). Effect of Leukocyte Concentration on the Efficacy of Platelet-Rich Plasma in the Treatment of Knee Osteoarthritis. Am J Sports Med, 44(3), doi: / Robins, R. J. (2014). PRP in ACL reconstruction--another indication for surgical augmentation? J Surg Res, 186(1), doi: /j.jss Rodeo, S. A., Delos, D., Williams, R. J., Adler, R. S., Pearle, A., & Warren, R. F. (2012). The effect of platelet-rich fibrin matrix on rotator cuff tendon healing: a prospective, randomized clinical study. Am J Sports Med, 40(6), doi: / Sampson, S., Gerhardt, M., & Mandelbaum, B. (2008). Platelet rich plasma injection grafts for musculoskeletal injuries: a review. Curr Rev Musculoskelet Med, 1(3-4), Page 16
17 doi: /s Samuelson, E. M., Odum, S. M., & Fleischli, J. E. (2016). The Cost- Effectiveness of Using Platelet-Rich Plasma During Rotator Cuff Repair: A Markov Model Analysis. Arthroscopy, 32(7), doi: /j.arthro Seijas, R., Ares, O., Catala, J., Alvarez- Diaz, P., Cusco, X., & Cugat, R. (2013). Magnetic resonance imaging evaluation of patellar tendon graft remodelling after anterior cruciate ligament reconstruction with or without platelet-rich plasma. J Orthop Surg (Hong Kong), 21(1), doi: / Smith, P. A. (2016). Intra-articular Autologous Conditioned Plasma Injections Provide Safe and Efficacious Treatment for Knee Osteoarthritis: An FDA-Sanctioned, Randomized, Double-blind, Placebocontrolled Clinical Trial. Am J Sports Med, 44(4), doi: / Vavken, P., Sadoghi, P., & Murray, M. M. (2011). The effect of platelet concentrates on graft maturation and graft-bone interface healing in anterior cruciate ligament reconstruction in human patients: a systematic review of controlled trials. Arthroscopy, 27(11), doi: /j.arthro Vavken, P., Sadoghi, P., Palmer, M., Rosso, C., Mueller, A. M., Szoelloesy, G., & Valderrabano, V. (2015). Platelet-Rich Plasma Reduces Retear Rates After Arthroscopic Repair of Small- and Medium-Sized Rotator Cuff Tears but Is Not Cost-Effective. Am J Sports Med, 43(12), doi: / Wasterlain, A. S., Braun, H. J., Harris, A. H., Kim, H. J., & Dragoo, J. L. (2013). The systemic effects of platelet-rich plasma injection. Am J Sports Med, 41(1), doi: / Williams, P. N., Moran, G., Bradley, J. P., N, S. E., & Dines, J. S. (2015). Platelet-rich plasma and other cellular strategies in orthopedic surgery. Curr Rev Musculoskelet Med, 8(1), doi: /s Zanon, G., Combi, F., Combi, A., Perticarini, L., Sammarchi, L., & Benazzo, F. (2016). Platelet-rich plasma in the treatment of acute hamstring injuries in professional football players. Joints, 4(1), doi: /jts/ Funding Source Financial support for this review has been provided from research funds of the 10 th Surgical Operations Squadron, 10 th Medical Group, United States Air Force Academy, Colorado. Disclaimer *The viewpoints presented in this article do not represent the official position of the United States government, the Department of Defense, the United States Air Force, or the United States Air Force Academy. Page 17
Conflicts of Interest. I have no conflicts of interest regarding this presentation
 Conflicts of Interest I have no conflicts of interest regarding this presentation Ramon Ylanan MD CAQSM Team Physician University of Arkansas Advanced Orthopeadic Specialists Goals Background Healing Response
Conflicts of Interest I have no conflicts of interest regarding this presentation Ramon Ylanan MD CAQSM Team Physician University of Arkansas Advanced Orthopeadic Specialists Goals Background Healing Response
Platelet Rich Plasma (PRP) injections. by Dr George Pitsis
 Platelet Rich Plasma (PRP) injections by Dr George Pitsis Platelet Rich Plasma (PRP) injections have in the more recent years attracted significant attention as a clinical tools to assist with treatment
Platelet Rich Plasma (PRP) injections by Dr George Pitsis Platelet Rich Plasma (PRP) injections have in the more recent years attracted significant attention as a clinical tools to assist with treatment
10/8/14. Revision Date(s): Policy Number: MCP-207. Review Date: 12/16/15, 9/15/16
 Subject: Platelet-rich Plasma (PRP) Policy Number: MCP-207 Review Date: 12/16/15, 9/15/16 Revision Date(s): Original Effective Date: 10/8/14 DISCLAIMER This Molina Clinical Policy (MCP) is intended to
Subject: Platelet-rich Plasma (PRP) Policy Number: MCP-207 Review Date: 12/16/15, 9/15/16 Revision Date(s): Original Effective Date: 10/8/14 DISCLAIMER This Molina Clinical Policy (MCP) is intended to
Platelet Rich Plasma (PRP) Dania Segreti, SPT Vanguard In-service - July 31, 2013
 Platelet Rich Plasma (PRP) Dania Segreti, SPT Vanguard In-service - July 31, 2013 What is PRP? In medicine since 1970s First uses in bone healing began in late 1990s Gained popularity for tissue healing
Platelet Rich Plasma (PRP) Dania Segreti, SPT Vanguard In-service - July 31, 2013 What is PRP? In medicine since 1970s First uses in bone healing began in late 1990s Gained popularity for tissue healing
Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers
 Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers Am J Orthop. 2016 May;45(4):296-300 Authors: Dines JS Williams PN Elattrache
Platelet-Rich Plasma Can Be Used to Successfully Treat Elbow Ulnar Collateral Ligament Insufficiency in High- Level Throwers Am J Orthop. 2016 May;45(4):296-300 Authors: Dines JS Williams PN Elattrache
DESCRIPTION OF PROCEDURE/SERVICE/PHARMACEUTICAL
 Subject: Platelet-rich Plasma (PRP) Policy Number: MCP-207 Review Date: 12/16/15, 9/15/16, 9/19/17 Revision Date(s): Original Effective Date: 10/8/14 DISCLAIMER This Molina Clinical Policy (MCP) is intended
Subject: Platelet-rich Plasma (PRP) Policy Number: MCP-207 Review Date: 12/16/15, 9/15/16, 9/19/17 Revision Date(s): Original Effective Date: 10/8/14 DISCLAIMER This Molina Clinical Policy (MCP) is intended
Platelet-Rich Plasma Compared With Other Common Injection Therapies in the Treatment of Chronic Lateral Epicondylitis
 Journal of Sport Rehabilitation, 2016, 25, 77-82 http://dx.doi.org/10.1123/jsr.2014-0198 2016 Human Kinetics, Inc. CRITICALLY APPRAISED TOPIC Platelet-Rich Plasma Compared With Other Common Injection Therapies
Journal of Sport Rehabilitation, 2016, 25, 77-82 http://dx.doi.org/10.1123/jsr.2014-0198 2016 Human Kinetics, Inc. CRITICALLY APPRAISED TOPIC Platelet-Rich Plasma Compared With Other Common Injection Therapies
ORTHOBIOLOGIC TREATMENTS IN BASEBALL. Casey G. Batten MD PBATS - January 19th, 2018
 ORTHOBIOLOGIC TREATMENTS IN BASEBALL Casey G. Batten MD PBATS - January 19th, 2018 The Problem Musculoskeletal injuries are common in sport Pressure to minimize down time, swift return Many injuries involve
ORTHOBIOLOGIC TREATMENTS IN BASEBALL Casey G. Batten MD PBATS - January 19th, 2018 The Problem Musculoskeletal injuries are common in sport Pressure to minimize down time, swift return Many injuries involve
Clinical Review Criteria
 Clinical Review Criteria Autologous Platelet Derived Wound Healing Factors for Treatment of: Non Healing Cutaneous Wounds (Procuren) Non-Healing Fractures and the Associated GEM 21STM Device Platelet Rich
Clinical Review Criteria Autologous Platelet Derived Wound Healing Factors for Treatment of: Non Healing Cutaneous Wounds (Procuren) Non-Healing Fractures and the Associated GEM 21STM Device Platelet Rich
BIOLOGICS STEM CELL AND PLATELET- RICH PLASMA FOR JOINT MANAGEMENT 1/10/ AAOS ANNUAL MEETING 2018 AAOS ANNUAL MEETING
 STEM CELL AND PLATELET- RICH PLASMA FOR JOINT MANAGEMENT BIOLOGICS o Injectable therapies that may suppress inflammation and promote regenerative pathways o Natural products that are harvested and are
STEM CELL AND PLATELET- RICH PLASMA FOR JOINT MANAGEMENT BIOLOGICS o Injectable therapies that may suppress inflammation and promote regenerative pathways o Natural products that are harvested and are
Platelet-Rich Plasma Treatment With Physical Therapy in Chronic Partial Supraspinatus Tears
 Iran Red Crescent Med J. 2015 September; 17(9): e23732. Published online 2015 September 28. DOI: 10.5812/ircmj.23732 Research Article Platelet-Rich Plasma Treatment With Physical Therapy in Chronic Partial
Iran Red Crescent Med J. 2015 September; 17(9): e23732. Published online 2015 September 28. DOI: 10.5812/ircmj.23732 Research Article Platelet-Rich Plasma Treatment With Physical Therapy in Chronic Partial
Platelet-Rich Plasma in the Lower Extremity
 Platelet-Rich Plasma in the Lower Extremity Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
Platelet-Rich Plasma in the Lower Extremity Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
ORTHOPEDICS BONE Recalcitrant nonunions In total hip replacement total knee surgery increased callus volume
 ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
Platelet Rich Plasma CLINICAL BRIEF
 Platelet Rich Plasma CLINICAL BRIEF Introduction As physicians continue to seek biologic solutions to improve healing of soft tissue pathologies, worldwide interest in the use of platelet rich plasma (PRP)
Platelet Rich Plasma CLINICAL BRIEF Introduction As physicians continue to seek biologic solutions to improve healing of soft tissue pathologies, worldwide interest in the use of platelet rich plasma (PRP)
Therapy with PRP. Flachau S.I.T.E.M.S.H Dr. Jürgen BARTHOFER. Trauma Hospital Linz - Austria Team Doctor ÖSV (Ski Jumping and Nordic Combined)
 Dr. Jürgen BARTHOFER Trauma Hospital Linz - Austria Team Doctor ÖSV (Ski Jumping and Nordic Combined) Flachau S.I.T.E.M.S.H 2014 Where are we? Methods : PRP (Platelet-rich Plasma) Buffy-Coat / Plasma-based
Dr. Jürgen BARTHOFER Trauma Hospital Linz - Austria Team Doctor ÖSV (Ski Jumping and Nordic Combined) Flachau S.I.T.E.M.S.H 2014 Where are we? Methods : PRP (Platelet-rich Plasma) Buffy-Coat / Plasma-based
Platelet rich plasma for the treatment of osteoarthrosis knee
 International Journal of Research in Orthopaedics Maheshwari P et al. Int J Res Orthop. 2017 Mar;3(2):242-246 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20170781
International Journal of Research in Orthopaedics Maheshwari P et al. Int J Res Orthop. 2017 Mar;3(2):242-246 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20170781
A Patient s Guide to Platelet-Rich Plasma Treatment of Musculoskeletal Compliments of: The Central Orthopedic Group
 A Patient s Guide to Platelet-Rich Plasma Treatment of Musculoskeletal Problems The Central Orthopedic Group 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com
A Patient s Guide to Platelet-Rich Plasma Treatment of Musculoskeletal Problems The Central Orthopedic Group 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com
Platelet-rich plasma application in the management of chronic tendinopathies
 Acta Orthop. Belg., 2013, 79, 10-15 REVIEW ARTICLE Platelet-rich plasma application in the management of chronic tendinopathies Jean-François Kaux, Jean-Michel Crielaard From the University and University
Acta Orthop. Belg., 2013, 79, 10-15 REVIEW ARTICLE Platelet-rich plasma application in the management of chronic tendinopathies Jean-François Kaux, Jean-Michel Crielaard From the University and University
Considered Judgement Form
 Considered Judgement Form This form is a checklist of issues that may be considered by the Purchasing Guidance Advisory Group when making purchasing recommendations. Meeting date: 14 October 2014 Topic:
Considered Judgement Form This form is a checklist of issues that may be considered by the Purchasing Guidance Advisory Group when making purchasing recommendations. Meeting date: 14 October 2014 Topic:
Platelet-rich plasma (PRP) for muscle injuries. Mohamad Shariff A Hamid MBBS (Adel), Master Sports Med (UM), PhD (UM)
 Platelet-rich plasma (PRP) for muscle injuries Mohamad Shariff A Hamid MBBS (Adel), Master Sports Med (UM), PhD (UM) Overview Muscle injury Management PRP PRP for muscle injuries - evidence? Introduction
Platelet-rich plasma (PRP) for muscle injuries Mohamad Shariff A Hamid MBBS (Adel), Master Sports Med (UM), PhD (UM) Overview Muscle injury Management PRP PRP for muscle injuries - evidence? Introduction
Biologics in ACL: What s the Data?
 Biologics in ACL: What s the Data? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior Scientist Sports Medicine and Shoulder
Biologics in ACL: What s the Data? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior Scientist Sports Medicine and Shoulder
A Patient s Guide to Platelet-Rich Plasma Treatment of Musculoskeletal Problems
 A Patient s Guide to Platelet-Rich Plasma Treatment of Musculoskeletal Problems Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with
A Patient s Guide to Platelet-Rich Plasma Treatment of Musculoskeletal Problems Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with
Utilization of Platelet-Rich Plasma for Musculoskeletal Injuries
 Original Research Utilization of Platelet-Rich Plasma for Musculoskeletal Injuries An Analysis of Current Treatment Trends in the United States Joanne Y. Zhang,* MD, MBA, Peter D. Fabricant, MD, MPH, Chad
Original Research Utilization of Platelet-Rich Plasma for Musculoskeletal Injuries An Analysis of Current Treatment Trends in the United States Joanne Y. Zhang,* MD, MBA, Peter D. Fabricant, MD, MPH, Chad
Prof. FABIO CERZA A.Carcangiu, S.Carnì, A. Pecora, I. Di Vavo, V. Schiavilla
 Department of Orthopaedics and Traumatology P.Colombo Hospital Velletri(ROME) Prof. FABIO CERZA A.Carcangiu, S.Carnì, A. Pecora, I. Di Vavo, V. Schiavilla 4 million Italians suffer from arthrosis Most
Department of Orthopaedics and Traumatology P.Colombo Hospital Velletri(ROME) Prof. FABIO CERZA A.Carcangiu, S.Carnì, A. Pecora, I. Di Vavo, V. Schiavilla 4 million Italians suffer from arthrosis Most
Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions
 APPENDIX G Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions The purpose of this document is to provide information for physiotherapists of common medical and surgical interventions
APPENDIX G Treatment of Lateral Elbow Tendinopathy: Medical and Surgical Interventions The purpose of this document is to provide information for physiotherapists of common medical and surgical interventions
Intraarticular platelet-rich plasma injection in the treatment of knee osteoarthritis: review and recommendations.
 Am J Phys Med Rehabil. 2014 Nov;93(11 Suppl 3):S108-21. doi: 10.1097/PHM.0000000000000115. Intraarticular platelet-rich plasma injection in the treatment of knee osteoarthritis: review and recommendations.
Am J Phys Med Rehabil. 2014 Nov;93(11 Suppl 3):S108-21. doi: 10.1097/PHM.0000000000000115. Intraarticular platelet-rich plasma injection in the treatment of knee osteoarthritis: review and recommendations.
An Owner's Guide to Natural Healing. Autologous Conditioned Plasma (ACP)
 An Owner's Guide to Natural Healing Autologous Conditioned Plasma (ACP) Healing after an injury involves a well-orchestrated and complex series of events where proteins in the blood have primary roles,
An Owner's Guide to Natural Healing Autologous Conditioned Plasma (ACP) Healing after an injury involves a well-orchestrated and complex series of events where proteins in the blood have primary roles,
John J Christoforetti, MD Pittsburgh, Pennsylvania
 ARTHROSCOPIC ASSISTED PROXIMAL HAMSTRINGS REPAIR WITH HUMAN ACELLULAR DERMAL ALLOGRAFT PATCH AUGMENTATION FOR REVISION OF FAILED PROXIMAL HAMSTRINGS REPAIR: SHORT TERM CLINICAL AND MRI RESULT John J Christoforetti,
ARTHROSCOPIC ASSISTED PROXIMAL HAMSTRINGS REPAIR WITH HUMAN ACELLULAR DERMAL ALLOGRAFT PATCH AUGMENTATION FOR REVISION OF FAILED PROXIMAL HAMSTRINGS REPAIR: SHORT TERM CLINICAL AND MRI RESULT John J Christoforetti,
Biologics for Sports Injuries
 Biologics for Sports Injuries Jason L. Dragoo, MD Associate Professor Department of Orthopaedic Surgery Introduction Survey of common conditions Cover only injuries with evidence NOT RTC RTC Pectoralis
Biologics for Sports Injuries Jason L. Dragoo, MD Associate Professor Department of Orthopaedic Surgery Introduction Survey of common conditions Cover only injuries with evidence NOT RTC RTC Pectoralis
US guided injection of highly concentrated PRP in chronic refractary tendinopathies: preliminary results
 US guided injection of highly concentrated PRP in chronic refractary tendinopathies: preliminary results Poster No.: C-0795 Congress: ECR 2012 Type: Scientific Paper Authors: A. De Marchi, S. Pozza, E.
US guided injection of highly concentrated PRP in chronic refractary tendinopathies: preliminary results Poster No.: C-0795 Congress: ECR 2012 Type: Scientific Paper Authors: A. De Marchi, S. Pozza, E.
Inflammation is Not the Enemy
 6/22/2017 Inflammation is Not the Enemy Sean Mulvaney, MD 1 6/22/2017 2 6/22/2017 Lascaux 7.4 Billion 3 This image cannot currently be displayed. 6/22/2017 Goals 4 ANTI INFLAMMATORY THERAPIES NSAIDS 5
6/22/2017 Inflammation is Not the Enemy Sean Mulvaney, MD 1 6/22/2017 2 6/22/2017 Lascaux 7.4 Billion 3 This image cannot currently be displayed. 6/22/2017 Goals 4 ANTI INFLAMMATORY THERAPIES NSAIDS 5
Platelet-rich plasma (PRP) in chronic epicondylitis: study protocol for a randomized controlled trial
 Martin et al. Trials 2013, 14:410 TRIALS STUDY PROTOCOL Open Access Platelet-rich plasma (PRP) in chronic epicondylitis: study protocol for a randomized controlled trial Jose I Martin 1, Josu Merino 2,
Martin et al. Trials 2013, 14:410 TRIALS STUDY PROTOCOL Open Access Platelet-rich plasma (PRP) in chronic epicondylitis: study protocol for a randomized controlled trial Jose I Martin 1, Josu Merino 2,
ISSN (O): ; ISSN (P): Effectiveness of Platelet-Rich Plasma in the Treatment of Moderate Knee Osteoarthritis.
 DOI: 10.21276/aimdr.2017.3.4.OR9 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Effectiveness of Platelet-Rich Plasma in the Treatment of Moderate Knee Osteoarthritis. S.L.Munde 1, Vivek Jha 2,
DOI: 10.21276/aimdr.2017.3.4.OR9 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Effectiveness of Platelet-Rich Plasma in the Treatment of Moderate Knee Osteoarthritis. S.L.Munde 1, Vivek Jha 2,
Tendon & Ligament Application of PRP
 Tendon & Ligament Application of PRP Sang Chul Lee, M.D, PhD. Department of Physical Medicine & Rehabilitation, Myongji hospital, Kwandong University College of Medicine Tendon and Ligament Low metabolic
Tendon & Ligament Application of PRP Sang Chul Lee, M.D, PhD. Department of Physical Medicine & Rehabilitation, Myongji hospital, Kwandong University College of Medicine Tendon and Ligament Low metabolic
Orthopedic Applications of Platelet- Rich Plasma
 Orthopedic Applications of Platelet- Rich Plasma Policy Number: 2.01.98 Last Review: 5/2018 Origination: 5/2016 Next Review: 5/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Orthopedic Applications of Platelet- Rich Plasma Policy Number: 2.01.98 Last Review: 5/2018 Origination: 5/2016 Next Review: 5/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Ricardo E. Colberg, MD, RMSK. PM&R Sports Medicine Physician Andrews Sports Medicine and Orthopedic Center American Sports Medicine Institute
 Ricardo E. Colberg, MD, RMSK PM&R Sports Medicine Physician Andrews Sports Medicine and Orthopedic Center American Sports Medicine Institute Pathophysiology of chronic orthopedic injuries Definition of
Ricardo E. Colberg, MD, RMSK PM&R Sports Medicine Physician Andrews Sports Medicine and Orthopedic Center American Sports Medicine Institute Pathophysiology of chronic orthopedic injuries Definition of
Priorities Forum Statement
 Priorities Forum Statement Number 75 Subject Autologous Blood and Platelet-Rich Plasma Injection in Tendinopathy Date of decision February 2017 Date refreshed February 2017 Date of review February 2020
Priorities Forum Statement Number 75 Subject Autologous Blood and Platelet-Rich Plasma Injection in Tendinopathy Date of decision February 2017 Date refreshed February 2017 Date of review February 2020
Arthrex ACP Double Syringe. ACP - Autologous Conditioned Plasma
 Arthrex ACP Double Syringe ACP - Autologous Conditioned Plasma Autologous Conditioned Plasma Introduction Autologous blood products have created a growing interest for use in a number of therapies. The
Arthrex ACP Double Syringe ACP - Autologous Conditioned Plasma Autologous Conditioned Plasma Introduction Autologous blood products have created a growing interest for use in a number of therapies. The
KNEE INJURIES IN SPORTS MEDICINE
 KNEE INJURIES IN SPORTS MEDICINE Irving Raphael, MD June 13, 2014 RSM Medical Associates Head Team Physician Syracuse University Outline Meniscal Injuries anatomy Exam Treatment ACL Injuries Etiology Physical
KNEE INJURIES IN SPORTS MEDICINE Irving Raphael, MD June 13, 2014 RSM Medical Associates Head Team Physician Syracuse University Outline Meniscal Injuries anatomy Exam Treatment ACL Injuries Etiology Physical
Sonographically occult intrasubstance tendon tears revealed by platelet rich plasma injection: evidence of a frequently overlooked pathology?
 Sonographically occult intrasubstance tendon tears revealed by platelet rich plasma injection: evidence of a frequently overlooked pathology? Poster No.: C-1603 Congress: ECR 2013 Type: Scientific Exhibit
Sonographically occult intrasubstance tendon tears revealed by platelet rich plasma injection: evidence of a frequently overlooked pathology? Poster No.: C-1603 Congress: ECR 2013 Type: Scientific Exhibit
Evidence Based Report Autologous Blood Injections for Musculoskeletal Disorders
 Evidence Based Report Autologous Blood Injections for Musculoskeletal Disorders Reviewer Mark Ayson Date Report Completed September 2014 Important Note: The purpose of this brief report is to summarise
Evidence Based Report Autologous Blood Injections for Musculoskeletal Disorders Reviewer Mark Ayson Date Report Completed September 2014 Important Note: The purpose of this brief report is to summarise
Platelet Rich Plasma in Musculoskeletal Pathology: A Necessary Rescue or a Lost Cause?
 Pain Physician 2017; 20:E345-E356 ISSN 2150-1149 Narrative Review Platelet Rich Plasma in Musculoskeletal Pathology: A Necessary Rescue or a Lost Cause? Annu Navani, MD 1, Gang Li, MD, PhD 2, and Joshua
Pain Physician 2017; 20:E345-E356 ISSN 2150-1149 Narrative Review Platelet Rich Plasma in Musculoskeletal Pathology: A Necessary Rescue or a Lost Cause? Annu Navani, MD 1, Gang Li, MD, PhD 2, and Joshua
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow.
 Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Preliminary Report Choosing Wisely Identifying Musculoskeletal Interventions with Limited Levels of Efficacy in the Shoulder & Elbow. Prepared for The Canadian Orthopaedic Association Contents Executive
Role of Autologus platelet rich plasma injection in treatment of tennis elbow
 Document heading doi: 10.21276/apjhs.2017.4.3.6 Research Article Role of Autologus platelet rich plasma injection in treatment of tennis elbow B.S. Rao 1 *, Avinash Kumar 2 1 Assistant professor, Department
Document heading doi: 10.21276/apjhs.2017.4.3.6 Research Article Role of Autologus platelet rich plasma injection in treatment of tennis elbow B.S. Rao 1 *, Avinash Kumar 2 1 Assistant professor, Department
JMSCR Vol 06 Issue 12 Page December 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.94 Estimate the effectiveness of
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.94 Estimate the effectiveness of
PRPP Injection Dora Street, Hurstville MBBS FACSP. Dr Paul Annett Sport & Exercise Medicine Physician
 PRPP Injection Dr. Paul Annett MBBS FACSP Sport and Exercise Medicine Physician www.orthosports.com.au 29 31 Dora Street, Hurstville PRP injection - Outline Basic science PRPP preparations Literature Patient
PRPP Injection Dr. Paul Annett MBBS FACSP Sport and Exercise Medicine Physician www.orthosports.com.au 29 31 Dora Street, Hurstville PRP injection - Outline Basic science PRPP preparations Literature Patient
Platelet-rich plasma versus other intra-articular injections for treatment of knee
 Intervention protocol Platelet-rich plasma versus other intra-articular injections for treatment of knee osteoarthritis Abstract This is the protocol for a non-cochrane review and there is no abstract.
Intervention protocol Platelet-rich plasma versus other intra-articular injections for treatment of knee osteoarthritis Abstract This is the protocol for a non-cochrane review and there is no abstract.
In the Treatment of Patients With Knee Joint Osteoarthritis, Are Platelet Rich Plasma Injections More Effective Than Hyaluronic Acid Injections?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2015 In the Treatment of Patients With Knee
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2015 In the Treatment of Patients With Knee
The healthcare environment is
 Review Article Platelet-rich Plasma in Orthopaedic Applications: Evidence-based Recommendations for Treatment Downloaded from http://journals.lww.com/jaaos by k38zdthxkv6xg2uya2wsbisxlamxpb/xenqi6wdshkkgg3a+mcn2rqarcprdp+lutjpipmob6bnm1owem6xa6l/kfgyxmyzaq6rkxqdhadam14buwtbhhljupt3iwmhetb6kybrxtrg=
Review Article Platelet-rich Plasma in Orthopaedic Applications: Evidence-based Recommendations for Treatment Downloaded from http://journals.lww.com/jaaos by k38zdthxkv6xg2uya2wsbisxlamxpb/xenqi6wdshkkgg3a+mcn2rqarcprdp+lutjpipmob6bnm1owem6xa6l/kfgyxmyzaq6rkxqdhadam14buwtbhhljupt3iwmhetb6kybrxtrg=
Clinical Policy Title: Platelet rich plasma
 Clinical Policy Title: Platelet rich plasma Clinical Policy Number: 05.02.10 Effective Date: February 1, 2017 Initial Review Date: November 16, 2016 Most Recent Review Date: November 16, 2017 Next Review
Clinical Policy Title: Platelet rich plasma Clinical Policy Number: 05.02.10 Effective Date: February 1, 2017 Initial Review Date: November 16, 2016 Most Recent Review Date: November 16, 2017 Next Review
Joint Preservation And Biologic Program
 SPORTS INSTITUTE Joint Preservation And Biologic Program The latest and most innovative treatment options available today for a multitude of orthopaedic injuries and pathologies Ellis and Badenhausen Sports
SPORTS INSTITUTE Joint Preservation And Biologic Program The latest and most innovative treatment options available today for a multitude of orthopaedic injuries and pathologies Ellis and Badenhausen Sports
Anterior Cruciate Ligament Injuries
 Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
STUDY OF PLATELET RICH PLASMA INJECTIONS IN PATIENTS OF TENDINOPATHY IN SOUTH GUJARAT POPULATION
 ORIGINAL ARTICLE STUDY OF PLATELET RICH PLASMA INJECTIONS IN PATIENTS OF TENDINOPATHY IN SOUTH GUJARAT POPULATION Manish Patel 1, Chintan Sheth 2, Jignesh Patel 1, PrabhavTijoriwala 1 Author s Affiliations:
ORIGINAL ARTICLE STUDY OF PLATELET RICH PLASMA INJECTIONS IN PATIENTS OF TENDINOPATHY IN SOUTH GUJARAT POPULATION Manish Patel 1, Chintan Sheth 2, Jignesh Patel 1, PrabhavTijoriwala 1 Author s Affiliations:
Platelet Rich Plasma: Hoax or Hope
 Platelet Rich Plasma: Hoax or Hope Peter Pryzbylkowski, MD Professional Background Double Boarded in both Anesthesiology and Pain Medicine Residency and Fellowship at the University of Pennsylvania Assistant
Platelet Rich Plasma: Hoax or Hope Peter Pryzbylkowski, MD Professional Background Double Boarded in both Anesthesiology and Pain Medicine Residency and Fellowship at the University of Pennsylvania Assistant
ˉ\_( ツ )_/ˉ. In office Use of PRP, Stem Cells etc.. 7/26/2017. I have no disclosures.
 In office Use of PRP, Stem Cells etc.. Kevin E. Elder, MD, FAAFP Adult and Pediatric Sports Medicine Affiliate Associate Professor, University of South Florida Affiliate Assistant Professor, Florida State
In office Use of PRP, Stem Cells etc.. Kevin E. Elder, MD, FAAFP Adult and Pediatric Sports Medicine Affiliate Associate Professor, University of South Florida Affiliate Assistant Professor, Florida State
Scientific Exhibit 73 Platelet-Rich Plasma in Orthopaedic Surgery: Where do we stand in 2017?
 Scientific Exhibit 73 Platelet-Rich Plasma in Orthopaedic Surgery: Where do we stand in 2017? Nikolas Baksh M.D. 1, Charles P. Hannon M.D. 2, Rachel M. Frank M.D. 2, Jacqueline Munch M.D. 1, John G. Kennedy
Scientific Exhibit 73 Platelet-Rich Plasma in Orthopaedic Surgery: Where do we stand in 2017? Nikolas Baksh M.D. 1, Charles P. Hannon M.D. 2, Rachel M. Frank M.D. 2, Jacqueline Munch M.D. 1, John G. Kennedy
Role of Platelet-Rich Plasma in Articular Cartilage Injury and Disease
 Special Focus Section 3 Role of Platelet-Rich Plasma in Articular Cartilage Injury and Disease Randy Mascarenhas, MD, FRCSC 1 Bryan M. Saltzman, MD 1 Lisa A. Fortier, PhD, DVM 2 BrianJ.Cole,MD,MBA 1 1
Special Focus Section 3 Role of Platelet-Rich Plasma in Articular Cartilage Injury and Disease Randy Mascarenhas, MD, FRCSC 1 Bryan M. Saltzman, MD 1 Lisa A. Fortier, PhD, DVM 2 BrianJ.Cole,MD,MBA 1 1
Foot, Ankle, Knee & Hip Surgery Update. What s s New. Platelet Rich Plasma (PRP) Platelet Rich Plasma Total Ankle Replacement.
 Foot, Ankle, Knee & Hip Surgery Update Geoffrey S. Landis D.O. April 29, 2010 Southwestern Conference on Medicine What s s New Platelet Rich Plasma Total Platelet Rich Plasma (PRP) Why- Need or Desire
Foot, Ankle, Knee & Hip Surgery Update Geoffrey S. Landis D.O. April 29, 2010 Southwestern Conference on Medicine What s s New Platelet Rich Plasma Total Platelet Rich Plasma (PRP) Why- Need or Desire
AN INTRODUCTION TO REGENERATIVE MEDICINE
 AN INTRODUCTION TO REGENERATIVE MEDICINE You ve undoubtedly come across some discussion of stem cells, likely with regard to stem cell research. But stem cells have a wide variety of uses in the medical
AN INTRODUCTION TO REGENERATIVE MEDICINE You ve undoubtedly come across some discussion of stem cells, likely with regard to stem cell research. But stem cells have a wide variety of uses in the medical
Regenerative Therapies - Stem Cell & Platelet Rich Plasma (PRP)
 Regenerative Therapies - Stem Cell & Platelet Rich Plasma (PRP) An Introduction to Regenerative Medicine Platelet Rich Plasma (PRP) and Stem Cell injections are part of an emerging field called regenerative
Regenerative Therapies - Stem Cell & Platelet Rich Plasma (PRP) An Introduction to Regenerative Medicine Platelet Rich Plasma (PRP) and Stem Cell injections are part of an emerging field called regenerative
tissue, Interventional non-vascular /ecr2014/C-1241
 Effectiveness of Ultrasound-guided Platelet Rich Plasma (PRP) injections after needle tenotomy in the treatment of chronic tendinopathies : A prospective study. Poster No.: C-1241 Congress: ECR 2014 Type:
Effectiveness of Ultrasound-guided Platelet Rich Plasma (PRP) injections after needle tenotomy in the treatment of chronic tendinopathies : A prospective study. Poster No.: C-1241 Congress: ECR 2014 Type:
MUCL REPAIR. Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA
 MUCL REPAIR Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA MUCL INJURY EPIDEMIC Frequency increasing despite major efforts
MUCL REPAIR Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA MUCL INJURY EPIDEMIC Frequency increasing despite major efforts
UNIVERSITA DEGLI STUDI DI NAPOLI FEDERICO II DIPARTIMENTO DI INGEGNERIA DEI MATERIALI E DELLA PRODUZIONE
 CLINICAL CASES IN SPORTS MEDICINE (TENNIS ELBOW), IN ORTHOPEDIC SURGERY (ACHILLES TENDON), MAXILLO-FACIAL SURGERY (ELEVATION OF THE MAXILLARY SINUS), IN PLASTIC SURGERY (TREATMENT OF WRINKLES) SOFT TISSUE
CLINICAL CASES IN SPORTS MEDICINE (TENNIS ELBOW), IN ORTHOPEDIC SURGERY (ACHILLES TENDON), MAXILLO-FACIAL SURGERY (ELEVATION OF THE MAXILLARY SINUS), IN PLASTIC SURGERY (TREATMENT OF WRINKLES) SOFT TISSUE
Correspondence to Dr Leon Creaney, BUPA Health and Wellbeing, 3 White Lyon Court, London EC2Y 8EA, UK;
 www.medscape.com Authors and Disclosures Leon Creaney, 1 Andrew Wallace, 3 Mark Curtis, 4 and David Connell 2 1 BUPA Health and Wellbeing, Barbican, London, UK 2 Royal National Orthopaedic Hospital, Stanmore,
www.medscape.com Authors and Disclosures Leon Creaney, 1 Andrew Wallace, 3 Mark Curtis, 4 and David Connell 2 1 BUPA Health and Wellbeing, Barbican, London, UK 2 Royal National Orthopaedic Hospital, Stanmore,
No financial disclosures
 Thomas J. Noonan, MD Steadman Hawkins Clinic Denver University of Colorado No financial disclosures Thomas Noonan, Gregory Ford, James Genuario, Jason Kinkartz, Thomas Githens, Scott Murayama Steadman
Thomas J. Noonan, MD Steadman Hawkins Clinic Denver University of Colorado No financial disclosures Thomas Noonan, Gregory Ford, James Genuario, Jason Kinkartz, Thomas Githens, Scott Murayama Steadman
Chronic musculoskeletal pain accounts for the most commonly reported medical
 The Emerging Use of Platelet-Rich Plasma in Musculoskeletal Medicine Jamil Bashir, MD Alberto J. Panero, DO Andrew L. Sherman, MD From the Department of Physical Medicine and Rehabilitation at the University
The Emerging Use of Platelet-Rich Plasma in Musculoskeletal Medicine Jamil Bashir, MD Alberto J. Panero, DO Andrew L. Sherman, MD From the Department of Physical Medicine and Rehabilitation at the University
Platelet-Rich Plasma Therapy for Knee Joint Problems: Review of the Literature, Current Practice and Legal Perspectives in Korea
 Review Article Knee Surg Relat Res 2012;24(2):70-78 http://dx.doi.org/10.5792/ksrr.2012.24.2.70 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Platelet-Rich Plasma Therapy for Knee Joint
Review Article Knee Surg Relat Res 2012;24(2):70-78 http://dx.doi.org/10.5792/ksrr.2012.24.2.70 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Platelet-Rich Plasma Therapy for Knee Joint
Minimally Invasive ACL Surgery
 Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Non-Operative Options for Articular Cartilage Issues in the Athlete s Knee
 Non-Operative Options for Articular Cartilage Issues in the Athlete s Knee Sourav Poddar, MD Associate Professor Director, Primary Care Sports Medicine University of Colorado School of Medicine OBJECTIVES
Non-Operative Options for Articular Cartilage Issues in the Athlete s Knee Sourav Poddar, MD Associate Professor Director, Primary Care Sports Medicine University of Colorado School of Medicine OBJECTIVES
Orthopedic Applications of Platelet-Rich Plasma
 Section: Medicine Effective Date: October 15, Subject: Orthopedic Applications of Platelet-Rich Plasma Page: 1 of 11 Last Review Status/Date: September Orthopedic Applications of Platelet-Rich Plasma Summary
Section: Medicine Effective Date: October 15, Subject: Orthopedic Applications of Platelet-Rich Plasma Page: 1 of 11 Last Review Status/Date: September Orthopedic Applications of Platelet-Rich Plasma Summary
Cartilage Care in the Mature Female Athlete
 Cartilage Care in the Mature Female Athlete K. Linnea Welton, MD Hip Preservation Fellow Department of Orthopedic Surgery University of Colorado Women in Sports Medicine Conference February 24, 2018 Disclosures
Cartilage Care in the Mature Female Athlete K. Linnea Welton, MD Hip Preservation Fellow Department of Orthopedic Surgery University of Colorado Women in Sports Medicine Conference February 24, 2018 Disclosures
TOPAZ TM What you should know
 TOPAZ TM What you should know Not for distribution in the United States. Need to know 2 Tendon: is a tough band of fibrous connective tissue that connects muscle to bone and is capable of withstanding
TOPAZ TM What you should know Not for distribution in the United States. Need to know 2 Tendon: is a tough band of fibrous connective tissue that connects muscle to bone and is capable of withstanding
CARTILAGE REPAIR INTRODUCTION. M. BERRUTO and G.M. PERETTI 1,2. Received January 6, Accepted January 8, 2013
 CARTILAGE REPAIR INTRODUCTION M. BERRUTO and G.M. PERETTI 1,2 Gaetano Pini Orthopedic Institute, Milan; 1 Department of Biomedical Sciences for Health, University of Milan, 2 IRCCS Galeazzi Orthopedic
CARTILAGE REPAIR INTRODUCTION M. BERRUTO and G.M. PERETTI 1,2 Gaetano Pini Orthopedic Institute, Milan; 1 Department of Biomedical Sciences for Health, University of Milan, 2 IRCCS Galeazzi Orthopedic
Ke-Vin Chang, MD Chen-Yu Hung, MD Fanny Aliwarga, MD Tyng-Guey Wang, MD Der-Sheng Han, MD, PhD Wen-Shiang Chen, MD, PhD
 Accepted Manuscript Comparative Effectiveness of Platelet-Rich Plasma Injections for Treating Knee Joint Cartilage Degenerative Pathology: A Systematic Review and Meta-analysis Ke-Vin Chang, MD Chen-Yu
Accepted Manuscript Comparative Effectiveness of Platelet-Rich Plasma Injections for Treating Knee Joint Cartilage Degenerative Pathology: A Systematic Review and Meta-analysis Ke-Vin Chang, MD Chen-Yu
PRP: Evidence and Use in Sports Medicine
 PRP: Evidence and Use in Sports Medicine Joanne Borg-Stein, MD Spaulding Rehabilitation Hospital Newton Wellesley Hospital Assistant Professor of PM&R, Harvard Medical School Director, Sports Medicine
PRP: Evidence and Use in Sports Medicine Joanne Borg-Stein, MD Spaulding Rehabilitation Hospital Newton Wellesley Hospital Assistant Professor of PM&R, Harvard Medical School Director, Sports Medicine
SUFFERING FROM INJURIES THAT JUST WON T HEAL? DO YOU SUFFER FROM ANY OF THE FOLLOWING CONDITIONS?
 SUFFERING FROM INJURIES THAT JUST WON T HEAL? If you are one of the many people suffering from pain caused by injured tendons, muscles, ligaments, and joints that heal at a remarkably slow pace or not
SUFFERING FROM INJURIES THAT JUST WON T HEAL? If you are one of the many people suffering from pain caused by injured tendons, muscles, ligaments, and joints that heal at a remarkably slow pace or not
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries This article is also available in Spanish: Lesiones del ligamento cruzado anterior (topic.cfm?topic=a00697) and Portuguese: Lesões do ligamento cruzado anterior
Anterior Cruciate Ligament (ACL) Injuries This article is also available in Spanish: Lesiones del ligamento cruzado anterior (topic.cfm?topic=a00697) and Portuguese: Lesões do ligamento cruzado anterior
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Orthopedic Applications of Platelet-Rich Plasma Page 1 of 23 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Orthopedic Applications of Platelet-Rich Plasma Professional
Orthopedic Applications of Platelet-Rich Plasma Page 1 of 23 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Orthopedic Applications of Platelet-Rich Plasma Professional
Platelet Rich Plasma Regenerative Medicine Sports Medicine Orthopedic And Recovery Of Musculoskeletal Injuries Lecture Notes In Bioengineering
 Platelet Rich Plasma Regenerative Medicine Sports Medicine Orthopedic And Recovery Of Musculoskeletal We have made it easy for you to find a PDF Ebooks without any digging. And by having access to our
Platelet Rich Plasma Regenerative Medicine Sports Medicine Orthopedic And Recovery Of Musculoskeletal We have made it easy for you to find a PDF Ebooks without any digging. And by having access to our
Tendon Fenestration. Disclosures. Outline: questions. Introduction: Peritendon Steroid Injections. Jon A. Jacobson, MD. Patellar Tendon: tendinosis
 Tendon Fenestration Jon A. Jacobson, MD Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures Consultant: Bioclinica Advisory Board: GE, Philips Book
Tendon Fenestration Jon A. Jacobson, MD Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures Consultant: Bioclinica Advisory Board: GE, Philips Book
Platelet-rich plasma vs hyaluronic acid to treat knee degenerative pathology: study design and preliminary results of a randomized controlled trial
 Filardo et al. BMC Musculoskeletal Disorders 2012, 13:229 RESEARCH ARTICLE Open Access Platelet-rich plasma vs hyaluronic acid to treat knee degenerative pathology: study design and preliminary results
Filardo et al. BMC Musculoskeletal Disorders 2012, 13:229 RESEARCH ARTICLE Open Access Platelet-rich plasma vs hyaluronic acid to treat knee degenerative pathology: study design and preliminary results
Analysis of Results of Platelet-rich Plasma with Arthroscopic Acromioplasty and Arthroscopic Acromioplasty: A Comparative Study
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2016/381 Analysis of Results of Platelet-rich Plasma with Arthroscopic Acromioplasty and Arthroscopic Acromioplasty: A Comparative
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2016/381 Analysis of Results of Platelet-rich Plasma with Arthroscopic Acromioplasty and Arthroscopic Acromioplasty: A Comparative
Ming Hao Zheng, PhD, DM, FRC Path Centre For Orthopaedic Research, The University of Western Australia; Paul Anderson MD Orthocell Pty Ltd
 Autologous Tenocyte Implantation for Refractory Tendonopathy Ming Hao Zheng, PhD, DM, FRC Path Centre For Orthopaedic Research, The University of Western Australia; Paul Anderson MD Orthocell Pty Ltd Tendon
Autologous Tenocyte Implantation for Refractory Tendonopathy Ming Hao Zheng, PhD, DM, FRC Path Centre For Orthopaedic Research, The University of Western Australia; Paul Anderson MD Orthocell Pty Ltd Tendon
Clinical Study Leukocyte-Reduced Platelet-Rich Plasma Treatment of Basal Thumb Arthritis: A Pilot Study
 Hindawi Publishing Corporation BioMed Research International Volume 216, Article ID 926299, 6 pages http://dx.doi.org/1.1155/216/926299 Clinical Study Leukocyte-Reduced Platelet-Rich Plasma Treatment of
Hindawi Publishing Corporation BioMed Research International Volume 216, Article ID 926299, 6 pages http://dx.doi.org/1.1155/216/926299 Clinical Study Leukocyte-Reduced Platelet-Rich Plasma Treatment of
Platelet-Rich Plasma for Primary Treatment of Partial Ulnar Collateral Ligament Tears
 Original Research Platelet-Rich Plasma for Primary Treatment of Partial Ulnar Collateral Ligament Tears MRI Correlation With Results J. Banks Deal,* MD, Ed Smith,* MD, Wendell Heard,* MD, Michael J. O
Original Research Platelet-Rich Plasma for Primary Treatment of Partial Ulnar Collateral Ligament Tears MRI Correlation With Results J. Banks Deal,* MD, Ed Smith,* MD, Wendell Heard,* MD, Michael J. O
Introduction. Christian Duif 1 Tobias Vogel. Christoph von Schulze Pellengahr 1 Matthias Lahner
 DOI 10.1007/s00402-015-2227-5 ARTHROSCOPY AND SPORTS MEDICINE Does intraoperative application of leukocyte-poor platelet-rich plasma during arthroscopy for knee degeneration affect postoperative pain,
DOI 10.1007/s00402-015-2227-5 ARTHROSCOPY AND SPORTS MEDICINE Does intraoperative application of leukocyte-poor platelet-rich plasma during arthroscopy for knee degeneration affect postoperative pain,
Platelet-rich plasma intra-articular injections for cartilage degeneration and osteoarthritis: single- versus double-spinning approach
 Knee Surg Sports Traumatol Arthrosc (2012) 20:2082 2091 DOI 10.1007/s00167-011-1837-x KNEE Platelet-rich plasma intra-articular injections for cartilage degeneration and osteoarthritis: single- versus
Knee Surg Sports Traumatol Arthrosc (2012) 20:2082 2091 DOI 10.1007/s00167-011-1837-x KNEE Platelet-rich plasma intra-articular injections for cartilage degeneration and osteoarthritis: single- versus
Non-operative Management of UCL Injuries
 Non-operative Management of UCL Injuries Mark S. Schickendantz, MD Professor of Surgery Director of Sports Medicine Cleveland Clinic Head Team Physician Cleveland Indians Disclosures Arthrex DJO Smith
Non-operative Management of UCL Injuries Mark S. Schickendantz, MD Professor of Surgery Director of Sports Medicine Cleveland Clinic Head Team Physician Cleveland Indians Disclosures Arthrex DJO Smith
The In Vivo Impact of Leukocyte Injections on Normal Rat Achilles Tendons: Potential Detriment to Tendon Morphology, Cellularity, and Vascularity
 The In Vivo Impact of Leukocyte Injections on Normal Rat Achilles Tendons: Potential Detriment to Tendon Morphology, Cellularity, and Vascularity Publish date: October 1, 2018 Authors: David E. Komatsu,
The In Vivo Impact of Leukocyte Injections on Normal Rat Achilles Tendons: Potential Detriment to Tendon Morphology, Cellularity, and Vascularity Publish date: October 1, 2018 Authors: David E. Komatsu,
Regenerative Medicine and the Future of Interventional Orthopaedics: Repair, Regenerate, Restore. Mark W. McFarland, D.O. Orthopaedic & Spine Center
 Regenerative Medicine and the Future of Interventional Orthopaedics: Repair, Regenerate, Restore Mark W. McFarland, D.O. Orthopaedic & Spine Center Overview Existing pain management treatments have been
Regenerative Medicine and the Future of Interventional Orthopaedics: Repair, Regenerate, Restore Mark W. McFarland, D.O. Orthopaedic & Spine Center Overview Existing pain management treatments have been
Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells,
 What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
Application of Platelet Rich Plasma (PRP) for Hip Related Pathologies: A Systematic Review of the Indications, PRP Processing Methods and Outcomes
 1 2 3 4 Application of Platelet Rich Plasma (PRP) for Hip Related Pathologies: A Systematic Review of the Indications, PRP Processing Methods and Outcomes 5 6 7 8 9 10 11 12 13 Jorge Chahla, MD, PhD 4
1 2 3 4 Application of Platelet Rich Plasma (PRP) for Hip Related Pathologies: A Systematic Review of the Indications, PRP Processing Methods and Outcomes 5 6 7 8 9 10 11 12 13 Jorge Chahla, MD, PhD 4
Platelet-Rich Plasma Significantly Improves Clinical Outcomes in Patients With Chronic Tennis Elbow
 AJSM PreView, published on July 3, 2013 as doi:10.1177/0363546513494359 Platelet-Rich Plasma Significantly Improves Clinical Outcomes in Patients With Chronic Tennis Elbow A Double-Blind, Prospective,
AJSM PreView, published on July 3, 2013 as doi:10.1177/0363546513494359 Platelet-Rich Plasma Significantly Improves Clinical Outcomes in Patients With Chronic Tennis Elbow A Double-Blind, Prospective,
The Aging Athletes Knee
 The Aging Athletes Knee Douglas P Tewes Orthopedic Sports Medicine Lincoln Orthopedic Center 1 Common Sports Knee Injuries Cartilage defects/chondromalacia Meniscal tears ACL tear Articular Cartilage injury/chondromalacia
The Aging Athletes Knee Douglas P Tewes Orthopedic Sports Medicine Lincoln Orthopedic Center 1 Common Sports Knee Injuries Cartilage defects/chondromalacia Meniscal tears ACL tear Articular Cartilage injury/chondromalacia
Worker's Compensation Shoulder Practices
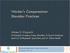 Worker's Compensation Shoulder Practices Aimee S. Klapach Orthopedic Surgeon; Knee, Shoulder, & Sports Medicine Sports & Orthopaedic Specialists, part of Allina Health Minnesota Department of Labor and
Worker's Compensation Shoulder Practices Aimee S. Klapach Orthopedic Surgeon; Knee, Shoulder, & Sports Medicine Sports & Orthopaedic Specialists, part of Allina Health Minnesota Department of Labor and
PLATELET-RICH PLASMA FOR TREATING CHRONIC TENDINOPATHY
 PLATELET-RICH PLASMA FOR TREATING CHRONIC TENDINOPATHY Written by Jean-François Kaux, Belgium Tendinopathy is a major problem in medicine and sports traumatology 1. It is due, inter alia, to mechanical
PLATELET-RICH PLASMA FOR TREATING CHRONIC TENDINOPATHY Written by Jean-François Kaux, Belgium Tendinopathy is a major problem in medicine and sports traumatology 1. It is due, inter alia, to mechanical
ACL Reconstruction: What is the Role of Sex and Sport in Graft Choice?
 ACL Reconstruction: What is the Role of Sex and Sport in Graft Choice? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior
ACL Reconstruction: What is the Role of Sex and Sport in Graft Choice? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior
The Society for Patient Centered Orthopedics. Choosing Wisely List. James Rickert, MD 1
 The Society for Patient Centered Orthopedics Choosing Wisely List James Rickert, MD 1 Extremities and Trauma Vertebroplasty Rotator Cuff Repair: For atraumatic (degenerative) tears in patients greater
The Society for Patient Centered Orthopedics Choosing Wisely List James Rickert, MD 1 Extremities and Trauma Vertebroplasty Rotator Cuff Repair: For atraumatic (degenerative) tears in patients greater
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
