Minimally Invasive Plate Osteosynthesis Using a Screw Compression Method for Treatment of Humeral Shaft Fractures
|
|
|
- Marcus York
- 5 years ago
- Views:
Transcription
1 Original Article Clinics in Orthopedic Surgery 2017;9: Minimally Invasive Plate Osteosynthesis Using a Screw Compression Method for Treatment of Humeral Shaft Fractures Sang-Hun Ko, MD, Jae-Ryong Cha, MD, Chae Chil Lee, MD, Yong Tae Joo, MD, Kyeong Su Eom, MD Department of Orthopedic Surgery, Ulsan University Hospital, University of Ulsan College of Medicine, Ulsan, Korea Background: This study aims to compare the surgical outcomes of open reduction and internal fixation (ORIF) and minimally invasive plate osteosynthesis (MIPO) using a screw compression method in simple humeral shaft fractures. Methods: This retrospective study was performed with 50 patients who had surgical interventions for the treatment of simple humeral shaft fractures and had follow-ups of at least 12 months in Ulsan University Hospital between August 2008 and June Group 1 included 23 patients treated with ORIF and group 2 included 27 patients treated with the MIPO technique using a locking screw plate. The time to clinical/radiographic union, the joint range of motion (ROM), and function were evaluated. Results: The average time to clinical/radiographic bone union was shorter in group 2 (12.0 ± 3.7 weeks/14.8 ± 2.0 weeks in group 1 and 9.4 ± 1.3 weeks/12.0 ± 3.3 weeks in group 2; p = 0.022/p = 0.034). Shoulder and elbow joint function evaluated by joint ROM and visual analogue scale (VAS), Korean Shoulder Elbow Society (KSS), American Shoulder and Elbow Surgeons (ASES), and the University of California at Los Angeles (UCLA) scores was excellent in both groups. On the average shoulder ROM at 12 months after the operation, group 1 had forward elevation of 160, external rotation of 30 in adduction and lumbar vertebra 10 level in internal rotation and group 2 had forward elevation of 170, external rotation of 35 in adduction and lumbar vertebra 9 level in internal rotation. The mean VAS, KSS, ASES, and UCLA scores were 2.8, 87.0 ± 0.9, 89.4 ± 0.9, and 31.0 ± 1.4, respectively, in group 1 and 1.7, 89.1 ± 2.7, 91.0 ± 1.6, and 32.4 ± 3.2, respectively, in group 2. There were statistically significant intergroup differences in VAS score (p = 0.011). There were significantly less postoperative infections in group 2 (three cases, 10.7% in group 1 and 0 case in group 2; p = 0.041) although all of them were superficial infections and well-treated by an average 4-week course of antibiotics (range, 2 to 6 weeks). Conclusions: MIPO using a screw compression method in simple humeral shaft fractures demonstrated superior efficacy to ORIF in terms of the time to clinical/radiographic union, pain score, and postoperative infection rate. Keywords: Humeral fractures, Fracture fixation, Screw compression method, Union period, Complication Received July 12, 2017; Accepted September 25, 2017 Correspondence to: Sang-Hun Ko, MD Department of Orthopedic Surgery, Ulsan University Hospital, University of Ulsan College of Medicine, 877 Bangeojinsunhwando-ro, Dong-gu, Ulsan 44033, Korea Tel: , Fax: , shkoshko@naver.com Co-Correspondence to: Jae-Ryong Cha, MD Department of Orthopedic Surgery, Ulsan University Hospital, University of Ulsan College of Medicine, 877 Bangeojinsunhwando-ro, Dong-gu, Ulsan 44033, Korea Tel: , Fax: , fissura@naver.com Copyright 2017 by The Korean Orthopaedic Association This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Clinics in Orthopedic Surgery pissn X eissn
2 507 Increasing traffic accidents and sports activities result in the increased incidence of humeral fractures, about 30% 50% of which are humeral shaft fractures. 1) It is known that union can be achieved by conservative management in humeral shaft fractures but operative intervention may be helpful to accelerate bone union and rehabilitation. 2-4) Although there are established surgical indications for humeral shaft fractures, 5) in recent years, operative treatment is often performed for early rehabilitation and return to daily life activities. 6) In the case of tibial fractures, the minimally invasive plate osteosynthesis (MIPO) technique is commonly used for internal fixation to increase the chance of bone union by preserving the biological environment. 7) Although there are growing attempts to implement the MIPO technique in humeral shaft fractures, the treatment outcome of MIPO in simple humeral fractures has not been satisfactory because it is difficult to obtain additional compressive strength at the fracture site. 8,9) Therefore, open reduction and internal fixation (ORIF) is the preferred surgical method for simple humeral fractures, despite the problems innate in the open reduction technique. Extensive skin incisions raise the risk of postoperative infection and cosmetic problems and periosteal exposure requires a longer bone union time. To avoid such problems inherent to ORIF, we have attempted to perform the MIPO technique using a screw compression method, which we believed would provide additional compressive strength at the fracture site. In this study, we compared the surgical outcomes of ORIF and MIPO using a screw compression method in simple humeral shaft fractures. METHODS Subjects This retrospective study was performed with 50 patients who had surgical interventions for the treatment of simple humeral shaft fractures and had follow-ups for at least 12 months in Ulsan University Hospital between August 2008 and June The demographics of study population are presented in Table 1. Patients with open fractures and any nerve injury before surgery were excluded in this study. The subjects were divided into two groups. Group 1 included 23 patients who had ORIF and group 2 included 27 patients who were treated with the MIPO technique using a locking screw plate. This study was approved by the Institutional Review Board of Ulsan University Hospital (IRB No ) and informed consent was obtained from all subjects. The mean age of the subjects was 50 years (range, 35 to 70 years) and there were 34 male patients and 16 female patients. There were 11 cases of transverse fracture, five cases of oblique fracture, and seven cases of spiral fracture in group 1 and 16 cases of transverse fracture, five cases of oblique fracture, and six cases of spiral fracture in group 2. The sufficient sample size suggested by a power analysis was 52 patients (26 patients in each group) to achieve a statistical power of 99% with a two-sided α level of 0.05 presuming an effect size of 0.8. Surgical Method For all subjects, 4.5-mm narrow limited contact locking compression plates (LC-LCP; Synthes, Zuchwil, Switzerland) and locking screws were used and conventional Table 1. Characteristics of Study Population Characteristic Group 1 (n = 23) Group 2 (n = 27) p-value Age (yr) 56.0 ± 10.8 (35 67) 55.9 ± 10.0 (37 70) Sex (male:female) 16:7 18: Follow-up time (mo) 18.5 ± ± Surgical delay (day) 4.4 ± ± Fracture type - Transverse Oblique 5 5 Spiral 7 6 Values are presented as mean ± standard deviation (range) or mean ± standard deviation. Group 1: patients who had open reduction and internal fixation, Group 2: patients who were treated with the minimally invasive plate osteosynthesis technique using a locking screw plate.
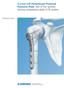
3 508 screws were additionally used for effective reduction. The patients were positioned in supine position under general anesthesia and the upper arm was abducted to 90 and the forearm was supinated to visualize the anterior site of the upper arm. In group 1, a conventional anterolateral approach was used. In supine position, a 10-cm skin incision was made on the fracture site and the deltoid muscle and the biceps brachii muscle were exposed. The biceps brachii was medially retracted and the brachialis muscle was vertically incised to expose the fracture site. Once the periosteum was detached and a hematoma was evacuated, a locking plate and screws were applied using a reduction clamp. In group 2, about 4-cm skin incision (range, 2 to 6 cm) was made on the proximal area of the fracture site for proximal window. With the anterolateral approach, an incision was made on the proximal humerus and the periosteum of the proximal humerus shaft was exposed between the deltoid muscle and the long head of the biceps brachii. About 3-cm skin incision (range, 2 to 4 cm) was anteriorly made on the distal humerus from 5 6 cm superior to the elbow joint for distal window. The biceps brachii muscle was medially retracted and the musculocutaneous nerve was carefully dissected and laterally retracted. When the brachialis was exposed, a vertical incision was made in the middle portion, and the distal humerus was exposed. Paying special attention not to damage the nearby soft tissues and the periosteum around the fracture site, a locking plate was placed on the anterior surface of the humeral shaft and a locking screw was inserted through the proximal incision. Then, indirect reduction was performed using an image intensifier and another locking screw was inserted through the distal incision. To avoid periosteal tears and radial nerve injuries during the insertion of the locking plate and screws, external rotation of the forearm during the intervention is recommended. When a proper bone alignment was achieved, compressive strength was obtained using conventional screws. For that purpose, the locking screws were slightly loosened (about 1/3) to maintain the bone alignment, and the conventional screws were inserted into the nearest holes from the fracture site to obtain compression. The holes were drilled further away from the fracture site and conventional screws were applied to obtain compression. Once the compressive strength was obtained on the fracture site, 2 3 locking screws were additionally applied inferior and superior to the fracture site. The locking screws initially inserted to maintain the bone alignment were removed at the end. Only after satisfactory reduction was achieved, two compression screws were replaced with locking screws. This operative procedure is demonstrated in Fig. 1 and a successful case using this technique is demonstrated in Figs The understanding of the anatomy of the radial nerve is important because percutaneous insertion of a plate can cause radial nerve palsy. The radial nerve runs medially from the humeral shaft in the proximal third of the humerus, posteriorly from the humeral shaft in the middle third of the humerus and laterally from the humeral shaft in the distal third of the humerus. Thus, the plate was anteriorly inserted to minimize lateral dissection and radial nerve injuries. If a plate is laterally inserted during MIPO, special attention should be paid during the advancement of the plate towards the distal humerus. The plate should be placed posterior to the long head of the biceps brachii and the holes should be carefully drilled through the other side of the cortex of the humerus to prevent radial nerve damage. The length of the plate was determined allowing for insertion of 3 4 screws in the plate holes from the fracture Fig. 1. Minimally invasive plate osteosynthesis using a screw compression method. (A) A proper bone alignment is achieved using two locking screws. (B) Compressive force is obtained at the fracture site using two compression screws. (C) Additional locking screws are inserted. (D) Compression screws are replaced with locking screws. A B C D
4 509 A A B B Fig. 3. Simple radiographs showing satisfactory results in the immediate postoperative period. (A) Anteroposterior view. (B) Lateral view. Fig. 2. Preoperative radiographs of a 33-year-old male showing a trans v erse fracture in the middle portion of the humeral shaft. (A) Anteroposterior view. (B) Lateral view. site. The distance to the nearest screws on both sides from the fracture site (working distance) was determined to evenly distribute the stress on the plate. Rehabilitation A right-angled long arm splint that protects the elbow joint was applied immediately after the operation, and the development of radial nerve injury was closely observed on a regular basis. Shoulder, elbow, finger, and wrist range of motion (ROM) exercises were carefully started on the postoperative day 2 or 3. After 2 weeks, the long arm splint was removed and active exercises were commenced. Resistant exercises were initiated after 3 months. Postoperative Management Radiographic examination was performed immediately after the operation and then every 2 weeks for the first 4 months, every month for the next 2 months, and every 3 months afterwards to evaluate radiographic union and deformity. Radiographic union was considered achieved when bone bridges of the three cortices became visible on anteroposterior and lateral X-ray views. Clinical union was defined as the absence of pain or tenderness at the fracture site. The subjects were followed up every 6 months for functional assessment after union. Postoperative evaluation was done in an outpatient clinic setting solely by a A B Fig. 4. Simple radiographs showing radiologic union 5 months post operatively. (A) Anteroposterior view. (B) Lateral view. single operator. Clinical Evaluation Postoperative functional ability was evaluated using Korean Shoulder Elbow Society (KSS) score (100 points) which is comprised of activities of daily living function (30 points), pain (20 points), self-reported assessment (10
5 510 points), shoulder ROM (20 points), muscle strength (10 points), and endurance (10 points). American Shoulder and Elbow Surgeons (ASES) score and the University of California at Los Angeles (UCLA) score (35 points) were also used to evaluate shoulder function. Pain was assessed using a visual analogue scale (VAS). For the evaluation of the shoulder ROM, forward elevation, external rotation, and internal rotation were measured with the shoulder abducted, and flexion and extension angles of the elbow joint were assessed. Statistical Analysis Statistical analysis was performed using SPSS ver (SPSS Inc., Chicago, IL, USA) with a significance level set at p < To evaluate characteristics of study population and compare postoperative outcomes between two groups, statistical analyses were performed using a Mann-Whitney U-test. Due to the limitation of the retrospective study design, there were a slightly insufficient number of subjects, which was compensated by using nonparametric statistics. RESULTS There were no significant differences in the mean age, sex, follow-up time, delayed surgical days, and fracture patterns between the two patient groups (Table 1). Complete bone union was obtained during the follow-up period in all subjects. The average time to clinical/radiographic bone union was shorter in group 2 (12.0 ± 3.7 weeks/14.8 ± 2.0 weeks in group 1 vs. 9.4 ± 1.3 weeks/12.0 ± 3.3 weeks in group 2), showing statistically significant difference (p = and p = 0.034). Shoulder and elbow joint function evaluated by joint ROM and VAS, KSS, ASES, and UCLA scores was excellent in both groups. The average shoulder ROM of group 1 at 12 months after the operation was forward elevation of 160, external rotation of 30 in adduction and thoracic vertebra 10 level in internal rotation. The average shoulder ROM of the group 2 at 12 months after the operation was forward elevation of 170, external rotation in adduction of 35 and thoracic vertebra 9 level in internal rotation. The mean VAS, KSS, ASES, and UCLA scores of group 1 were 2.8, 87.0 ± 0.9, 89.4 ± 0.9, and 31.0 ± 1.4, respectively. Those of group 2 were 1.7, 89.1 ± 2.7, 91.0 ± 1.6, and 32.4 ± 3.2, respectively. There were statistically significant differences in VAS scores (p = 0.011) (Table 2). Radial nerve palsy occurred in two patients in group 1 (7.2%) and in one patient in group 2 (4.2%), all of which subsided within 3 months. There were significantly less postoperative infections in group 2 (three cases, 10.7% in group 1 vs. 0 case in group 2; p = 0.041) although all were superficial infections and well-treated by an average 4-week course of Table 2. Comparison of 12-Month Postoperative Outcomes between Two Groups Characteristic Group 1 Group 2 p-value Union time (clinical, wk) 12.0 ± ± Union time (radiologic, wk) 14.8 ± ± Functional outcome VAS score KSS score 87.0 ± ± UCLA score 31.0 ± ± ASES score 89.4 ± ± Complication Malunion Nonunion Radial nerve palsy Infection Values are presented as mean ± standard deviation. Group 1: patients who had open reduction and internal fixation, Group 2: patients who were treated with the minimally invasive plate osteosynthesis technique using a locking screw plate, VAS: visual analogue scale, KSS: Korean Shoulder Elbow Society, UCLA: University of California at Los Angeles, ASES: American Shoulder and Elbow Surgeons.
6 511 antibiotics (range, 2 to 6 weeks). DISCUSSION The study results demonstrated satisfactory surgical outcomes of MIPO using a screw compression method in the treatment of humeral simple fractures. The use of MIPO technique is gradually increasing not only for the treatment of humeral shaft fractures but also for other fractures since it facilitates bone healing process by preserving the biological environment of fracture sites and the technique is easy to perform. 10) Conservative management used to be the gold standard for the treatment of humeral shaft fractures. Lately, however, the use of operative treatment is increasing for rapid return to daily life. In the past, internal fixation or intramedullary nailing fixation with conventional screws and plates was primarily performed for the treatment of humeral shaft fracture, but, in recent years, the use of MIPO technique is increasing ) The MIPO technique is generally used for shaft fractures and metaphyseal fractures accompanying osteoporosis, which can be treated with indirect reduction as anatomical reduction is not required and for multi-fragmentary fractures, which can be treated with bridging plate fixation. However, the MIPO technique can also be used for simple shaft fractures and metaphyseal fractures ) Bae et al. 6) reported that there were no statistically significant differences in the time to union among the plate fixation, intramedullary fixation and external fixation performed for the treatment of humeral shaft fractures. Among humeral shaft fractures, simple fractures which can be treated with conventional ORIF with excellent surgical outcomes can also be an indication for MIPO considering the convenience of the MIPO technique. The convenience of the technique includes wide acceptable range of fragmentary displacement and unproblematic use of the devices. In cases of simple humeral shaft fractures, conventional ORIF without excessive stripping of soft tissues, performed by experienced surgeons, resulted in excellent postoperative ROM and minimal postoperative infections. In general, postoperative infection rates are lower in MIPO than in conventional ORIF because MIPO preserves blood supply to the bone and nearby soft tissues ) Furthermore, postoperative infections after MIPO are less aggressive and easier to manage than those after conventional ORIF because infection after MIPO tends to be limited in the plate and soft tissues and the periosteum is well preserved. 7) Despite the advantages of MIPO, ORIF remains the most popular treatment option for the management of simple humeral shaft fractures by achieving anatomical reduction; MIPO has not yet been fully proven to be an equally effective method for the treatment of humeral shaft fractures. We have achieved satisfactory results by using the MIPO technique to overcome the disadvantages of ORIF; by applying additional compressive force to the fracture site using compression screws, we have successfully minimized the fracture gap size. In addition to the technical convenience mentioned above, the advantages of MIPO encompass creating a better biological environment around the fracture site, omission of plate bending and cosmetic benefits. 25,26) Moreover, possible complications such as iatrogenic fractures and limited ROM after intramedullary fixation were significantly reduced. 27) In our study, significantly shorter clinical/radiographic bone union time was found in the MIPO group, probably due to the intact periosteum and periosteal vessels. In addition, the VAS score 1 year postoperatively was also significantly lower in the MIPO group due to the relatively small skin incision and less soft tissue stripping. Elbow and shoulder function and ROM assessed using KSS, UCLA, and ASES scoring systems showed excellent results in both groups. Risks of secondary radial nerve injury, as one of the most serious complications that may occur in both ORIF and MIPO groups, associated with surgical treatment of humeral shaft fractures should be acknowledged. In ORIF, the radial nerve can be exposed and protected. In MIPO, however, the understanding of the anatomic course of the nerves is required as nerves cannot be visualized, increasing the risk of intraoperative nerve injury. The radial nerve can be damaged by a retractor or a plate and screws because it is located medial to the proximal one third of the humerus, posterior to the middle one third of the humerus, and lateral to the distal one third of the humerus. 19,28) Thus, special attention should be paid when a retractor is used during the operation and a plate is inserted into the distal humerus. Apivatthakakul et al. 28) reported that radial nerve damages and plate bending can be prevented if the forearm is kept in full supination during the insertion of a plate in a cadaver study. We also used this method in this study, which resulted in temporary radial nerve palsy in one case. Drilling at the middle of the humerus to make holes for screws as well as screw insertion should be carefully done to avoid too deep insertion of the screws. Radial nerve damage could be minimized with this method, so there was only one case of postoperative radial nerve palsy in group 2 in contrast to two cases in group 1. Although there is a risk of radial nerve damage in
7 512 the MIPO technique, it can be prevented by careful manipulation to maximize advantages of the technique. This study results showed that the use of MIPO technique in the treatment of humeral shaft fractures provided an excellent bone union rate and functional outcome. Limitations of this study include the small sample size and the retrospective study design. Therefore, prospective studies involving a greater number of subjects are needed for objective comparison with our findings in the future. The surgical outcome of MIPO using a screw compression method in simple humeral shaft fractures demonstrated results superior to those of ORIF in terms of the time to clinical/radiographic union, pain score, and postoperative infection rate. CONFLICT OF INTEREST No potential conflict of interest relevant to this article was reported. REFERENCES 1. Volgas DA, Stannard JP, Alonso JE. Nonunions of the humerus. Clin Orthop Relat Res. 2004;(419): Fears RL, Gleis GE, Seligson D. Diagnosis and treatment of complications: fractures of the diaphyseal humerus. In: Browner BD, Jupiter JB, Levine AM, Trafton PG, eds. Skeletal trauma: fractures, dislocations, ligamentous injuries. Toronto: WB Saunders; Gregory PR. Fractures of the humeral shaft. In: Rockwood CA, Green DP, Heckman JD, Bucholz RW, eds. Rockwood and Green's fractures in adults. Philadelphia, PA: Lippincott Williams & Wilkins; Schemitsch EH, Bhandari M. Fractures of the diaphyseal humerus. In: Browner BD, Jupiter JB, Levine AM, Trafton PG, eds. Skeletal trauma: basic science, management, and reconstruction. Toronto: WB Saunders; McKee MD. Fractures of the shaft of the humerus. In: Bucholz RW, Heckman JD, Court-Brown C, Koval KJ, Tornetta P, Wirth MA, eds. Rockwood and Green's fractures in adults. Philadelphia, PA: Lippincott Williams & Wilkins; Bae SW, Kim WJ, Song BY, Choi NH, Lee JH. Postoperative functional assessments in adult humerus shaft fractures: comparison among plates and screws, intramedullary nail and external fixator. J Korean Soc Fract. 2001;14(2): Byun YS. Minimally invasive plate osteosynthesis, MIPO. J Korean Fract Soc. 2007;20(1): Sohn HS, Shin SJ. Minimally invasive plate osteosynthesis for proximal humeral fractures: clinical and radiologic outcomes according to fracture type. J Shoulder Elbow Surg. 2014;23(9): Shin SJ, Sohn HS, Do NH. Minimally invasive plate osteosynthesis of humeral shaft fractures: a technique to aid fracture reduction and minimize complications. J Orthop Trauma. 2012;26(10): Xue Z, Jiang C, Hu C, Qin H, Ding H, An Z. Effects of different surgical techniques on mid-distal humeral shaft vascularity: open reduction and internal fixation versus minimally invasive plate osteosynthesis. BMC Musculoskelet Disord. 2016;17: Kim JW, Oh CW, Byun YS, Kim JJ, Park KC. A prospective randomized study of operative treatment for noncomminuted humeral shaft fractures: conventional open plating versus minimal invasive plate osteosynthesis. J Orthop Trauma. 2015;29(4): Moon JG, Kwon HN, Biraris S, Shon WY. Minimally invasive plate osteosynthesis using a helical plate for metadiaphyseal complex fractures of the proximal humerus. Orthopedics. 2014;37(3):e Esmailiejah AA, Abbasian MR, Safdari F, Ashoori K. Treatment of humeral shaft fractures: minimally invasive plate osteosynthesis versus open reduction and internal fixation. Trauma Mon. 2015;20(3):e Shetty MS, Kumar MA, Sujay K, Kini AR, Kanthi KG. Minimally invasive plate osteosynthesis for humerus diaphyseal fractures. Indian J Orthop. 2011;45(6): Gautier E, Sommer C. Guidelines for the clinical application of the LCP. Injury. 2003;34 Suppl 2:B Mast J, Jakob R, Ganz R. Planning and reduction technique in fracture surgery. Berlin, Germany: Springer-Verlag; Perren SM. Evolution of the internal fixation of long bone fractures: the scientific basis of biological internal fixation: choosing a new balance between stability and biology. J Bone Joint Surg Br. 2002;84(8): Ruedi TP, Murphy WM. AO principles of fracture management. Stuttgart, Germany: Thieme; Tong GO, Bavonratanavech S. Minimally invasive plate osteosynthesis (MIPO): concepts and cases presented by AO East Aisa. Stuttgart, Germany: Thieme;
8 Wagner M. General principles for the clinical use of the LCP. Injury. 2003;34 Suppl 2:B Collinge C, Sanders R, DiPasquale T. Treatment of complex tibial periarticular fractures using percutaneous techniques. Clin Orthop Relat Res. 2000;(375): Krettek C, Schandelmaier P, Miclau T, Tscherne H. Minimally invasive percutaneous plate osteosynthesis (MIPPO) using the DCS in proximal and distal femoral fractures. Injury. 1997;28 Suppl 1:A Schutz M, Muller M, Krettek C, et al. Minimally invasive fracture stabilization of distal femoral fractures with the LISS: a prospective multicenter study. Results of a clinical study with special emphasis on difficult cases. Injury. 2001;32 Suppl 3:SC Stannard JP, Wilson TC, Volgas DA, Alonso JE. Fracture stabilization of proximal tibial fractures with the proximal tibial LISS: early experience in Birmingham, Alabama (USA). Injury. 2003;34 Suppl 1:A Jung SW. Indirect reduction maneuver and minimally invasive approach for displaced proximal humerus fractures in elderly patients. Clin Orthop Surg. 2013;5(1): Park J, Jeong SY. Complications and outcomes of minimally invasive percutaneous plating for proximal humeral fractures. Clin Orthop Surg. 2014;6(2): Kobayashi M, Watanabe Y, Matsushita T. Early full range of shoulder and elbow motion is possible after minimally invasive plate osteosynthesis for humeral shaft fractures. J Orthop Trauma. 2010;24(4): Apivatthakakul T, Arpornchayanon O, Bavornratanavech S. Minimally invasive plate osteosynthesis (MIPO) of the humeral shaft fracture. Is it possible? A cadaveric study and preliminary report. Injury. 2005;36(4):530-8.
Distal femoral fracture with subsequent ipsilateral proximal femoral fracture
 Distal femoral fracture with subsequent ipsilateral proximal femoral fracture by M Agarwal, MS FRCS, AA Syed, FRCSI, PV Giannoudis (!), BSc,MB,MD,EEC(Orth) Dept. of Orthopaedics and Trauma, St.James University
Distal femoral fracture with subsequent ipsilateral proximal femoral fracture by M Agarwal, MS FRCS, AA Syed, FRCSI, PV Giannoudis (!), BSc,MB,MD,EEC(Orth) Dept. of Orthopaedics and Trauma, St.James University
CiSE. PHILOS Plate Osteosynthesis in Metaphyseal Fractures of the Distal Humerus through an Anterolateral Approach. Introduction ORIGINAL ARTICLE
 ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 18, No. 3, September, 2015 http://dx.doi.org/10.5397/cise.2015.18.3.128 CiSE Clinics in Shoulder and Elbow PHILOS Plate Osteosynthesis in Metaphyseal
ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 18, No. 3, September, 2015 http://dx.doi.org/10.5397/cise.2015.18.3.128 CiSE Clinics in Shoulder and Elbow PHILOS Plate Osteosynthesis in Metaphyseal
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
Orthopedics in Motion Tristan Hartzell, MD January 27, 2016
 Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
Orthopedics in Motion 2016 Tristan Hartzell, MD January 27, 2016 Humerus fractures Proximal Shaft Distal Objectives 1) Understand the anatomy 2) Epidemiology and mechanisms of injury 3) Types of fractures
The study of distal ¼ diaphyseal extra articular fractures of humerus treated with antegrade intramedullary interlocking nailing
 2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
2018; 4(4): 46-50 ISSN: 2395-1958 IJOS 2018; 4(4): 46-50 2018 IJOS www.orthopaper.com Received: 01-08-2018 Accepted: 03-09-2018 Dr. Ankur Parikh Orthopaedics, Jehangir Hospital, Sassoon road, Pune, Dr.
Technique Guide. 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Proximal Humerus Plate 2 AO Principles
Technique Guide 3.5 mm LCP Periarticular Proximal Humerus Plate. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Proximal Humerus Plate 2 AO Principles
Minimally invasive plate osteosynthesis (MIPO) of the humeral shaft fracture Is it possible? A cadaveric study and preliminary report
 Injury, Int. J. Care Injured (2005) 36, 530 538 www.elsevier.com/locate/injury Minimally invasive plate osteosynthesis (MIPO) of the humeral shaft fracture Is it possible? A cadaveric study and preliminary
Injury, Int. J. Care Injured (2005) 36, 530 538 www.elsevier.com/locate/injury Minimally invasive plate osteosynthesis (MIPO) of the humeral shaft fracture Is it possible? A cadaveric study and preliminary
A clinical study of minimal invasive anterior bridge plating for humerus shaft fractures
 2018; 4(2): 01-05 ISSN: 2395-1958 IJOS 2018; 4(2): 01-05 2018 IJOS www.orthopaper.com Received: 01-02-2018 Accepted: 02-03-2018 Mohammed Ibrahim Dr. Vijay H Rathod A clinical study of minimal invasive
2018; 4(2): 01-05 ISSN: 2395-1958 IJOS 2018; 4(2): 01-05 2018 IJOS www.orthopaper.com Received: 01-02-2018 Accepted: 02-03-2018 Mohammed Ibrahim Dr. Vijay H Rathod A clinical study of minimal invasive
Comparison between Intramedullary Nailing and Percutaneous K-Wire Fixation for Fractures in the Distal Third of the Metacarpal Bone
 Comparison between Nailing and K-Wire Fixation for Fractures in the Distal Third of the Metacarpal Bone Original Article Sung Jun Moon 1, Jae-Won Yang 2, Si Young Roh 1, Dong Chul Lee 1, Jin Soo Kim 1
Comparison between Nailing and K-Wire Fixation for Fractures in the Distal Third of the Metacarpal Bone Original Article Sung Jun Moon 1, Jae-Won Yang 2, Si Young Roh 1, Dong Chul Lee 1, Jin Soo Kim 1
Minimally Invasive Plating of Fractures:
 Minimally Invasive Plating of Fractures: Advantages, Techniques and Trade-offs Matthew Garner, MD Created January 2016 OUTLINE Principles of fracture management The importance of vascular supply Equipment
Minimally Invasive Plating of Fractures: Advantages, Techniques and Trade-offs Matthew Garner, MD Created January 2016 OUTLINE Principles of fracture management The importance of vascular supply Equipment
Clinico-radiological outcome of closed reduction and percutaneous fixation of proximal humerus fractures
 2018; 4(1): 614-618 ISSN: 2395-1958 IJOS 2018; 4(1): 614-618 2018 IJOS www.orthopaper.com Received: 10-11-2017 Accepted: 11-12-2017 Dr. Dharmendra Kumar Assistant Professor, KGMU, Lucknow, Dr. Neerav Anand
2018; 4(1): 614-618 ISSN: 2395-1958 IJOS 2018; 4(1): 614-618 2018 IJOS www.orthopaper.com Received: 10-11-2017 Accepted: 11-12-2017 Dr. Dharmendra Kumar Assistant Professor, KGMU, Lucknow, Dr. Neerav Anand
Diaphyseal Humerus Fractures. OTA Course Dallas, TX 1/20/17 Ellen Fitzpatrick MD
 Diaphyseal Humerus Fractures OTA Course Dallas, TX 1/20/17 Ellen Fitzpatrick MD OBJECTIVES TREATMENT OPTIONS SURGICAL INDICATIONS CONTROVERSIES IN MANAGEMENT Humerus Fractures Treatment Goals: Functional
Diaphyseal Humerus Fractures OTA Course Dallas, TX 1/20/17 Ellen Fitzpatrick MD OBJECTIVES TREATMENT OPTIONS SURGICAL INDICATIONS CONTROVERSIES IN MANAGEMENT Humerus Fractures Treatment Goals: Functional
The Journal of the Korean Society of Fractures Vol.16, No.1, January, 2003
 The Journal of the Korean Society of Fractures Vol16, No1, January, 2003 : 351 ( )463-712 TEL: (031) 780-5270/5271 FAX : (031) 708-3578 E-mail: bskima@netsgocom 16,, ( > 20mm ) 5, ) 20 % 1 ), 6,, 3 8 8
The Journal of the Korean Society of Fractures Vol16, No1, January, 2003 : 351 ( )463-712 TEL: (031) 780-5270/5271 FAX : (031) 708-3578 E-mail: bskima@netsgocom 16,, ( > 20mm ) 5, ) 20 % 1 ), 6,, 3 8 8
HUMERAL SHAFT FRACTURES: ORIF, IMN, NONOP What to do?
 HUMERAL SHAFT FRACTURES: ORIF, IMN, NONOP What to do? TRAUMA 101 2018 FRACTURE CARE FOR THE COMMUNITY ORTHOPEDIST William W. Cross III, MD Assistant Professor Division of Orthopaedic Trauma Chair, Division
HUMERAL SHAFT FRACTURES: ORIF, IMN, NONOP What to do? TRAUMA 101 2018 FRACTURE CARE FOR THE COMMUNITY ORTHOPEDIST William W. Cross III, MD Assistant Professor Division of Orthopaedic Trauma Chair, Division
Distal Femur Fractures: Tips and Tricks for Plating and Nailing? Conflict of Interest 9/24/2015
 Distal Femur Fractures: Tips and Tricks for Plating and Nailing? Cory Collinge, MD Professor of Orthopedic Surgery Vanderbilt University Medical Center Nashville, TN Conflict of Interest Consultant: Smith
Distal Femur Fractures: Tips and Tricks for Plating and Nailing? Cory Collinge, MD Professor of Orthopedic Surgery Vanderbilt University Medical Center Nashville, TN Conflict of Interest Consultant: Smith
MINIMALLY INVASIVE PLATE OSTEOSYNTHESIS FOR DISTAL RADIUS FRACTURES: SURGICAL TECHNIQUE M. TOBE 1, K. MIZUTANI 1, Y. TSUBUKU 1, Y.
 Riv Chir Mano - Vol. 43 (3) 2006 MINIMALLY INVASIVE PLATE OSTEOSYNTHESIS FOR DISTAL RADIUS FRACTURES: SURGICAL TECHNIQUE M. TOBE 1, K. MIZUTANI 1, Y. TSUBUKU 1, Y. YANAGIHARA 2 1 Department of 2nd Orthopaedic
Riv Chir Mano - Vol. 43 (3) 2006 MINIMALLY INVASIVE PLATE OSTEOSYNTHESIS FOR DISTAL RADIUS FRACTURES: SURGICAL TECHNIQUE M. TOBE 1, K. MIZUTANI 1, Y. TSUBUKU 1, Y. YANAGIHARA 2 1 Department of 2nd Orthopaedic
Posteromedial approach to the distal humerus for fracture fixation
 Acta Orthop. Belg., 2006, 72, 395-399 ORIGINAL STUDY Posteromedial approach to the distal humerus for fracture fixation Cédric LAPORTE, Maurice THIONGO, Dominique JEGOU From the General Hospital of Meaux,
Acta Orthop. Belg., 2006, 72, 395-399 ORIGINAL STUDY Posteromedial approach to the distal humerus for fracture fixation Cédric LAPORTE, Maurice THIONGO, Dominique JEGOU From the General Hospital of Meaux,
Minimally Invasive Helical Plating for Shaft of Humerus Fractures: Technique and Outcome
 184 The Open Orthopaedics Journal, 2012, 6, 184-188 Open Access Minimally Invasive Helical Plating for Shaft of Humerus Fractures: Technique and Outcome James Chung Hui Tan *,1,2, Fareed Husain Yusuf Kagda
184 The Open Orthopaedics Journal, 2012, 6, 184-188 Open Access Minimally Invasive Helical Plating for Shaft of Humerus Fractures: Technique and Outcome James Chung Hui Tan *,1,2, Fareed Husain Yusuf Kagda
Humerus shaft - Reduction & Fixation - Compression plate - AO Surgery Reference. Compression plating
 Humerus shaft 12-A3 ORIF 1. Principles Compression plating Authors Compression plate Compression plating provides fixation with absolute stability for two-part fracture patterns, where the bone fragments
Humerus shaft 12-A3 ORIF 1. Principles Compression plating Authors Compression plate Compression plating provides fixation with absolute stability for two-part fracture patterns, where the bone fragments
AO / Synthes Proximal Posterior Medial Tibia Plate. Tibial Plateau Fx. Osteosynthesis
 Tibial Plateau Fx. Osteosynthesis Articular Fractures Osteosynthesis Characteristics of the LCP system LCP 3.5 system LCP 4.5 system Many different traditional plates (small, large) Lag screws Rafting
Tibial Plateau Fx. Osteosynthesis Articular Fractures Osteosynthesis Characteristics of the LCP system LCP 3.5 system LCP 4.5 system Many different traditional plates (small, large) Lag screws Rafting
Primary internal fixation of fractures of both bones forearm by intramedullary nailing
 Original article 21 Primary internal fixation of fractures of both bones forearm by intramedullary nailing Nepal Medical College and Teaching Hospital, Kathmandu, Nepal Correspondenc to: Dr R P Singh,
Original article 21 Primary internal fixation of fractures of both bones forearm by intramedullary nailing Nepal Medical College and Teaching Hospital, Kathmandu, Nepal Correspondenc to: Dr R P Singh,
VA-LCP Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle.
 Technique Guide VA-LCP Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Table of Contents Introduction VA-LCP Anterior
Technique Guide VA-LCP Anterior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Table of Contents Introduction VA-LCP Anterior
A Patient s Guide to Adult Forearm Fractures
 A Patient s Guide to Adult Forearm Fractures Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 1 DISCLAIMER: The information in this
A Patient s Guide to Adult Forearm Fractures Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 1 DISCLAIMER: The information in this
Plate Fixation Options
 Distal tibia extra-articular fractures can be difficult to treat Tenuous soft tissue Complex fracture patterns Plate Fixation Options Medial plating: Minimally invasive approach Technical ease Anterolateral
Distal tibia extra-articular fractures can be difficult to treat Tenuous soft tissue Complex fracture patterns Plate Fixation Options Medial plating: Minimally invasive approach Technical ease Anterolateral
LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle.
 Technique Guide LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Table of Contents Introduction LCP Superior Clavicle
Technique Guide LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Table of Contents Introduction LCP Superior Clavicle
Index. B Backslap technique depth assessment, 82, 83 diaphysis distal trocar, 82 83
 Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Index A Acromial impingement, 75, 76 Aequalis intramedullary locking avascular necrosis, 95 central humeral head, 78, 80 clinical and functional outcomes, 95, 96 design, 77, 79 perioperative complications,
Medial approach to treat humeral mid-shaft fractures: a retrospective study
 Lu et al. Journal of Orthopaedic Surgery and Research (2016) 11:32 DOI 10.1186/s13018-016-0366-1 RESEARCH ARTICLE Open Access Medial approach to treat humeral mid-shaft fractures: a retrospective study
Lu et al. Journal of Orthopaedic Surgery and Research (2016) 11:32 DOI 10.1186/s13018-016-0366-1 RESEARCH ARTICLE Open Access Medial approach to treat humeral mid-shaft fractures: a retrospective study
Study of Evaluation of Lateral Surgical Approach for Diaphyseal Fractures of Distal 2/3rd of Radius at a Tertiary Care Teaching Centre
 Original article : Study of Evaluation of Lateral Surgical Approach for Diaphyseal Fractures of Distal 2/3rd of Radius at a Tertiary Care Teaching Centre Chandra Prakash Singh Associate Professor, Department
Original article : Study of Evaluation of Lateral Surgical Approach for Diaphyseal Fractures of Distal 2/3rd of Radius at a Tertiary Care Teaching Centre Chandra Prakash Singh Associate Professor, Department
A Patient s Guide to Adult Humerus Shaft Fractures
 A Patient s Guide to Adult Humerus Shaft Fractures Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 1 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult Humerus Shaft Fractures Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 1 DISCLAIMER: The information in this booklet is compiled
Technical Note Clinics in Orthopedic Surgery 2013;5:
 Technical Note Clinics in Orthopedic Surgery 2013;5:327-333 http://dx.doi.org/10.4055/cios.2013.5.4.327 Biologic Fixation through Bridge Plating for Comminuted Shaft Fracture of the Clavicle: Technical
Technical Note Clinics in Orthopedic Surgery 2013;5:327-333 http://dx.doi.org/10.4055/cios.2013.5.4.327 Biologic Fixation through Bridge Plating for Comminuted Shaft Fracture of the Clavicle: Technical
Results of lateral pin fixation for the displaced supracondylar fracture of humerus in children
 Journal of College of Medical Sciences-Nepal, 2012, Vol-8, No-1,13-17 Original Article Results of lateral pin fixation for the displaced supracondylar fracture of humerus in children H.K. Gupta 1, K.D.
Journal of College of Medical Sciences-Nepal, 2012, Vol-8, No-1,13-17 Original Article Results of lateral pin fixation for the displaced supracondylar fracture of humerus in children H.K. Gupta 1, K.D.
COMPARATIVE STUDY OF MANAGEMENT OF DIAPHYSEAL FEMUR FRACTURE WITH INTRAMEDULLARY INTERLOCKING NAIL AND K. NAIL
 International Journal of Innovation and Applied Studies ISSN 2028-9324 Vol. 15 No. 3 Apr. 2016, pp. 560-564 2016 Innovative Space of Scientific Research Journals http://www.ijias.issr-journals.org/ COMPARATIVE
International Journal of Innovation and Applied Studies ISSN 2028-9324 Vol. 15 No. 3 Apr. 2016, pp. 560-564 2016 Innovative Space of Scientific Research Journals http://www.ijias.issr-journals.org/ COMPARATIVE
Open reduction; plate fixation 1 Principles
 Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
P.R.C.T II FIXATION PLATE FOR ARTICULAR FRACTURE OF THE PROXIMAL HUMERUS SURGICAL TECHNIQUE
 P.R.C.T II FIXATION PLATE FOR ARTICULAR FRACTURE OF THE PROXIMAL HUMERUS SURGICAL TECHNIQUE INDICATIONS - Surgical technique...page 0 - Mini invasive approach...page 04 - Diaphyseal plates...page 05 -
P.R.C.T II FIXATION PLATE FOR ARTICULAR FRACTURE OF THE PROXIMAL HUMERUS SURGICAL TECHNIQUE INDICATIONS - Surgical technique...page 0 - Mini invasive approach...page 04 - Diaphyseal plates...page 05 -
Techique. Results. Discussion. Materials & Methods. Vol. 2 - Year 1 - December 2005
 to each other. The most distal interlocking hole is 3 mm proximal to distal end of nail, is in anteroposterior direction & proximal distal interlocking hole is in medial to lateral direction i.e. at right
to each other. The most distal interlocking hole is 3 mm proximal to distal end of nail, is in anteroposterior direction & proximal distal interlocking hole is in medial to lateral direction i.e. at right
ROTATIONAL PILON FRACTURES
 CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
CHAPTER 31 ROTATIONAL PILON FRACTURES George S. Gumann, DPM The opinions and commentary of the author should not be construed as refl ecting offi cial U.S. Army Medical Department policy. Pilon injuries
LCP Distal Humerus Plates
 The anatomic fixation system for the distal humerus with angular stability Surgical technique LCP Locking Compression Plate Contents Indications and contraindications 2 Implants 3 Instruments 5 Preparation
The anatomic fixation system for the distal humerus with angular stability Surgical technique LCP Locking Compression Plate Contents Indications and contraindications 2 Implants 3 Instruments 5 Preparation
A study of functional outcome of distal tibial extraarticular fracture fixed with locking compression plate using MIPPO technique
 2017; 1(3): 13-18 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2017; 1(3): 13-18 Received: 03-08-2017 Accepted: 04-09-2017 Dr. Somashekar Dr. Girish S Dr.
2017; 1(3): 13-18 ISSN (P): 2521-3466 ISSN (E): 2521-3474 Clinical Orthopaedics www.orthoresearchjournal.com 2017; 1(3): 13-18 Received: 03-08-2017 Accepted: 04-09-2017 Dr. Somashekar Dr. Girish S Dr.
3.5 mm LCP Clavicle Hook Plates
 Part of the Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Clavicle Hook Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Clavicle Hook Plates 2 AO Principles 4 Indications
Part of the Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Clavicle Hook Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Clavicle Hook Plates 2 AO Principles 4 Indications
BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES
 BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES Mohammad Abul kalam, Pradeep Kumar, Mohammad Afzal Hussain and Iqbal Ahmad Abstract A prospective study of forty comminuted femoral shaft fractures,
BRIDGE PLATING OF COMMINUTED SHAFT OF FEMUR FRACTURES Mohammad Abul kalam, Pradeep Kumar, Mohammad Afzal Hussain and Iqbal Ahmad Abstract A prospective study of forty comminuted femoral shaft fractures,
Anatomical Considerations Regarding the Posterior Interosseous Nerve During Posterolateral Approaches to the Proximal Part of the Radius *
 Anatomical Considerations Regarding the Posterior Interosseous Nerve During Posterolateral Approaches to the Proximal Part of the Radius * BY THOMAS DILIBERTI, M.D., MICHAEL J. BOTTE, M.D., AND REID A.
Anatomical Considerations Regarding the Posterior Interosseous Nerve During Posterolateral Approaches to the Proximal Part of the Radius * BY THOMAS DILIBERTI, M.D., MICHAEL J. BOTTE, M.D., AND REID A.
Locked Plating: Biomechanics and Biology
 Techniques in Orthopaedics 22(4):E1 E6 2007 Lippincott Williams & Wilkins, Inc. Locked Plating: Biomechanics and Biology Kyle F. Dickson, M.D., M.B.A., John W. Munz, M.D. Summary: Since the early ideas
Techniques in Orthopaedics 22(4):E1 E6 2007 Lippincott Williams & Wilkins, Inc. Locked Plating: Biomechanics and Biology Kyle F. Dickson, M.D., M.B.A., John W. Munz, M.D. Summary: Since the early ideas
Locked Plating: Clinical Indications
 Techniques in Orthopaedics 22(3):181 185 2007 Lippincott Williams & Wilkins, Inc. Locked Plating: Clinical Indications Kyle F. Dickson, M.D., M.B.A., John Munz, M.D. Summary: As shown in the previous article,
Techniques in Orthopaedics 22(3):181 185 2007 Lippincott Williams & Wilkins, Inc. Locked Plating: Clinical Indications Kyle F. Dickson, M.D., M.B.A., John Munz, M.D. Summary: As shown in the previous article,
Long Volar Plates for Diaphyseal-Metaphyseal Radius Fractures LCP. Dia-Meta Volar Distal Radius Plates. Surgical Technique
 Long Volar Plates for Diaphyseal-Metaphyseal Radius Fractures LCP Dia-Meta Volar Distal Radius Plates Surgical Technique Table of Contents Introduction LCP Dia-Meta Volar Distal Radius Plates 2 AO Principles
Long Volar Plates for Diaphyseal-Metaphyseal Radius Fractures LCP Dia-Meta Volar Distal Radius Plates Surgical Technique Table of Contents Introduction LCP Dia-Meta Volar Distal Radius Plates 2 AO Principles
Technique Guide. LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System.
 Technique Guide LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Table of Contents Introduction Features and Benefits 2 AO ASIF Principles 4 Indications 5 Surgical
Technique Guide LCP Proximal Femoral Hook Plate 4.5/5.0. Part of the LCP Periarticular Plating System. Table of Contents Introduction Features and Benefits 2 AO ASIF Principles 4 Indications 5 Surgical
Minimally invasive plate osteosynthesis for distal tibial fractures
 Journal of Orthopaedic Surgery 2014;22(3):299-303 Minimally invasive plate osteosynthesis for distal tibial fractures Pramod Devkota, 1 Javed A Khan, 2 Suman K Shrestha, 2 Balakrishnan M Acharya, 2 Nabeesman
Journal of Orthopaedic Surgery 2014;22(3):299-303 Minimally invasive plate osteosynthesis for distal tibial fractures Pramod Devkota, 1 Javed A Khan, 2 Suman K Shrestha, 2 Balakrishnan M Acharya, 2 Nabeesman
The Effect of Distal Location of the Volar Short Arm Splint on the Metacarpophalangeal Joint Motion
 Original Article Clinics in Orthopedic Surgery 2016;8:181-186 http://dx.doi.org/10.4055/cios.2016.8.2.181 The Effect of Distal Location of the Volar Short Arm Splint on the Metacarpophalangeal Joint Motion
Original Article Clinics in Orthopedic Surgery 2016;8:181-186 http://dx.doi.org/10.4055/cios.2016.8.2.181 The Effect of Distal Location of the Volar Short Arm Splint on the Metacarpophalangeal Joint Motion
COMPARATIVE STUDY OF FUNCTIONAL OUTCOME OF OPERATIVE AND NON-OPERATIVE TREATMENT IN MIDSHAFT CLAVICLE FRACTURES
 COMPARATIVE STUDY OF FUNCTIONAL OUTCOME OF OPERATIVE AND NON-OPERATIVE TREATMENT IN MIDSHAFT CLAVICLE FRACTURES R. Sahaya Jose 1 1Assistant Professor, Department of Orthopaedics, Sree Mookambika Institute
COMPARATIVE STUDY OF FUNCTIONAL OUTCOME OF OPERATIVE AND NON-OPERATIVE TREATMENT IN MIDSHAFT CLAVICLE FRACTURES R. Sahaya Jose 1 1Assistant Professor, Department of Orthopaedics, Sree Mookambika Institute
Fractures and dislocations around elbow in adult
 Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
3.5 mm Clavicle Hook Plates
 A Single Solution for Lateral Clavicle Fractures and Acromioclavicular Joint Dislocations 3.5 mm Clavicle Hook Plates Surgical Technique Discontinued December 2017 DSUS/TRM/1016/1126(1) Table of Contents
A Single Solution for Lateral Clavicle Fractures and Acromioclavicular Joint Dislocations 3.5 mm Clavicle Hook Plates Surgical Technique Discontinued December 2017 DSUS/TRM/1016/1126(1) Table of Contents
陳書佑 / 吳基銓副部長
 陳書佑 / 吳基銓副部長 2012-12-25 1 30 y/o male, TA no radial nerve injury 2 s/p splint arrange functional brace 3 1 month 4 2 months 5 3 months 6 4 months 7 One year 8 Conservative Treatment of Humeral Shaft Fractures
陳書佑 / 吳基銓副部長 2012-12-25 1 30 y/o male, TA no radial nerve injury 2 s/p splint arrange functional brace 3 1 month 4 2 months 5 3 months 6 4 months 7 One year 8 Conservative Treatment of Humeral Shaft Fractures
Minimally Invasive Plate Osteosynthesis (MIPO) for Proximal and Distal Fractures of The Tibia: A Biological Approach
 http://dx.doi.org/10.5704/moj.1603.006 Minimally Invasive Plate Osteosynthesis (MIPO) for Proximal and Distal Fractures of The Tibia: A Biological Approach Gupta P, MS Orth, Tiwari A, MS Orth, Thora A,
http://dx.doi.org/10.5704/moj.1603.006 Minimally Invasive Plate Osteosynthesis (MIPO) for Proximal and Distal Fractures of The Tibia: A Biological Approach Gupta P, MS Orth, Tiwari A, MS Orth, Thora A,
LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system.
 LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system. Technique Guide This publication is not intended for distribution in the USA. Instruments
LCP Medial Proximal Tibial Plate 3.5. Part of the Synthes small fragment Locking Compression Plate (LCP) system. Technique Guide This publication is not intended for distribution in the USA. Instruments
3.5 mm LCP Extra-articular Distal Humerus Plate
 Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Extra-articular Distal Humerus Plate Surgical Technique Table of Contents Introduction 3.5 mm LCP Extra-articular Distal Humerus
Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Extra-articular Distal Humerus Plate Surgical Technique Table of Contents Introduction 3.5 mm LCP Extra-articular Distal Humerus
Technique Guide. LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction LCP Distal Fibula Plates 2 AO Principles 4 Indications 5 Surgical Technique
Technique Guide LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction LCP Distal Fibula Plates 2 AO Principles 4 Indications 5 Surgical Technique
OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3
 OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3 HOW TO CITE THIS ARTICLE: Karan Mehta, Prashanth G. Shiblee Siddiqui,
OUTCOME OF MANAGEMENT OF CLOSED PROXIMAL TIBIA FRACTURES IN TERTIARY HOSPITAL OF SURAT Karan Mehta 1, Prashanth G 2, Shiblee Siddiqui 3 HOW TO CITE THIS ARTICLE: Karan Mehta, Prashanth G. Shiblee Siddiqui,
Anterior Plating of Displaced Middle Third Fractures of Clavicle An Effective Alternate Method
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver.8 March. (2018), PP 24-28 www.iosrjournals.org Anterior Plating of Displaced Middle Third
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver.8 March. (2018), PP 24-28 www.iosrjournals.org Anterior Plating of Displaced Middle Third
Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini
 Open Access Case report Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini Address: Department of Orthopaedic
Open Access Case report Posterolateral elbow dislocation with entrapment of the medial epicondyle in children: a case report Juan Rodríguez Martín* and Juan Pretell Mazzini Address: Department of Orthopaedic
COMPARATIVE STUDY OF FUNCTIONAL OUTCOME OF EXTERNAL AND INTERNAL FIXATION IN TREATMENT OF COMMINUTED DISTAL RADIUS FRACTURES
 COMPARATIVE STUDY OF FUNCTIONAL OUTCOME OF EXTERNAL AND INTERNAL FIXATION IN TREATMENT OF COMMINUTED DISTAL RADIUS FRACTURES R. Sahaya Jose 1 1Assistant Professor, Department of Orthopaedics, Sree Mookambika
COMPARATIVE STUDY OF FUNCTIONAL OUTCOME OF EXTERNAL AND INTERNAL FIXATION IN TREATMENT OF COMMINUTED DISTAL RADIUS FRACTURES R. Sahaya Jose 1 1Assistant Professor, Department of Orthopaedics, Sree Mookambika
Minimally Invasive Surgery by Angular Stability Systems in Proximal Tibia Fractures Biomechanical Characteristics and Preliminary Results
 Minimally Invasive Surgery by Angular Stability Systems in Proximal Tibia Fractures Biomechanical Characteristics and Preliminary Results P.D. Sirbu 1, E. Carata 2, T. Petreus 1, F. Munteanu 1, C. Popescu
Minimally Invasive Surgery by Angular Stability Systems in Proximal Tibia Fractures Biomechanical Characteristics and Preliminary Results P.D. Sirbu 1, E. Carata 2, T. Petreus 1, F. Munteanu 1, C. Popescu
Mini-open Treatment Using Plate of Clavicle Mid-shaft Fractures. Yong-Geun Park*, Hyunseong Kang*, Shinil Kim, Jong-Hwan Bae, Sungwook Choi
 ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 20, No. 1, March, 2017 https://doi.org/10.5397/cise.2017.20.1.37 CiSE Clinics in Shoulder and Elbow Mini-open Treatment Using Plate of Clavicle Mid-shaft
ORIGINAL ARTICLE Clinics in Shoulder and Elbow Vol. 20, No. 1, March, 2017 https://doi.org/10.5397/cise.2017.20.1.37 CiSE Clinics in Shoulder and Elbow Mini-open Treatment Using Plate of Clavicle Mid-shaft
3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM
 3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM Part of the DePuy Synthes Variable Angle Periarticular Plating System SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION 3.5 mm VA-LCP Proximal Tibial Plate 2 AO
3.5 MM VA-LCP PROXIMAL TIBIA PLATE SYSTEM Part of the DePuy Synthes Variable Angle Periarticular Plating System SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION 3.5 mm VA-LCP Proximal Tibial Plate 2 AO
3.5 mm LCP Olecranon Plates
 Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Olecranon Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Olecranon Plates 2 AO Principles 3 Indications
Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Olecranon Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Olecranon Plates 2 AO Principles 3 Indications
Chapter 4: Forearm 4.3 Forearm shaft fractures, transverse (12-D/4)
 AO Manual of ESIN in children s fractures Chapter 4: Forearm 4.3 Forearm shaft fractures, transverse (12-D/4) Title AO Manual of ESIN in children Subtitle Elastic stable intramedullary nailing (ESIN) Author
AO Manual of ESIN in children s fractures Chapter 4: Forearm 4.3 Forearm shaft fractures, transverse (12-D/4) Title AO Manual of ESIN in children Subtitle Elastic stable intramedullary nailing (ESIN) Author
LESS INVASIVE STABILIZATION SYSTEM (LISS) IN THE TREATMENT OF DISTAL FEMUR FRACTURES
 Trakia Journal of Sciences, No 4, pp 56-61, 2015 Copyright 2015 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2015.04.009 ISSN 1313-3551 (online) Original
Trakia Journal of Sciences, No 4, pp 56-61, 2015 Copyright 2015 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2015.04.009 ISSN 1313-3551 (online) Original
Forearm Fracture Solutions. Product Overview
 Forearm Fracture Solutions Product Overview Acumed Forearm Fracture Solutions Acumed Forearm Fracture Solutions includes plating and rodding systems with a range of diaphyseal radius and ulna fracture
Forearm Fracture Solutions Product Overview Acumed Forearm Fracture Solutions Acumed Forearm Fracture Solutions includes plating and rodding systems with a range of diaphyseal radius and ulna fracture
Outcome of Surgical Treatment of AO Type C Pelvic Ring Injury
 ORIGINAL ARTICLE Hip Pelvis 26(4): 269-274, 2014 http://dx.doi.org/10.5371/hp.2014.26.4.269 Print ISSN 2287-3260 Online ISSN 2287-3279 Outcome of Surgical Treatment of AO Type C Pelvic Ring Injury Do Hyeon
ORIGINAL ARTICLE Hip Pelvis 26(4): 269-274, 2014 http://dx.doi.org/10.5371/hp.2014.26.4.269 Print ISSN 2287-3260 Online ISSN 2287-3279 Outcome of Surgical Treatment of AO Type C Pelvic Ring Injury Do Hyeon
LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle.
 LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for distribution
LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for distribution
FUNCTIONAL OUTCOME OF PROXIMAL TIBIA EXTR-ARTICULAR FRACTURES TREATED WITH LOCKING COMPRESSION PLATING
 FUNCTIONAL OUTCOME OF PROXIMAL TIBIA EXTR-ARTICULAR FRACTURES TREATED WITH LOCKING COMPRESSION PLATING Original Article Orthopaedics Pradip B. Patil 1, Dhanish V. Mehendiratta 2, S.A. Lad 3, Rishi K. Doshi
FUNCTIONAL OUTCOME OF PROXIMAL TIBIA EXTR-ARTICULAR FRACTURES TREATED WITH LOCKING COMPRESSION PLATING Original Article Orthopaedics Pradip B. Patil 1, Dhanish V. Mehendiratta 2, S.A. Lad 3, Rishi K. Doshi
3.5 mm LCP Superior Anterior Clavicle Plates
 Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Superior Anterior Clavicle Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Superior Anterior Clavicle Plates
Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Superior Anterior Clavicle Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Superior Anterior Clavicle Plates
Treatment of fracture of shaft of humerus in adults by intramedullary interlocking nail fixation
 Original Article Chaudhary et.al. of shaft of humerus in adults by intramedullary interlocking nail fixation P Chaudhary, NK Karn, BP Shrestha, GP Khanal, RPS Kalawar Department of Othopaedics B.P. Koirala
Original Article Chaudhary et.al. of shaft of humerus in adults by intramedullary interlocking nail fixation P Chaudhary, NK Karn, BP Shrestha, GP Khanal, RPS Kalawar Department of Othopaedics B.P. Koirala
Biomedical Research 2017; 28 (14): ISSN X
 Biomedical Research 2017; 28 (14): 6251-6255 ISSN 0970-938X www.biomedres.info Comparison study of the clinical effect and biomechanics between locking compression plate and interlocking intramedullary
Biomedical Research 2017; 28 (14): 6251-6255 ISSN 0970-938X www.biomedres.info Comparison study of the clinical effect and biomechanics between locking compression plate and interlocking intramedullary
Advantage and limitations of a minimally-invasive approach and early weight bearing in the treatment of tibial shaft fractures with locking plates
 Orthopaedics & Traumatology: Surgery & Research (2012) 98, 564 569 Available online at www.sciencedirect.com ORIGINAL ARTICLE Advantage and limitations of a minimally-invasive approach and early weight
Orthopaedics & Traumatology: Surgery & Research (2012) 98, 564 569 Available online at www.sciencedirect.com ORIGINAL ARTICLE Advantage and limitations of a minimally-invasive approach and early weight
2.4 mm LCP Radial Head Plates. Part of the Synthes LCP Distal Radius Plate System.
 2.4 mm LCP Radial Head Plates. Part of the Synthes LCP Distal Radius Plate System. Technique Guide Instruments and Implants approved by the AO Foundation Table of Contents Introduction 2.4 mm LCP Radial
2.4 mm LCP Radial Head Plates. Part of the Synthes LCP Distal Radius Plate System. Technique Guide Instruments and Implants approved by the AO Foundation Table of Contents Introduction 2.4 mm LCP Radial
Complex fractures of the humeral shaft. Janos Solyom Sahlgrenska University Hospital Gothenburg, Sweden
 Complex fractures of the humeral shaft Janos Solyom Sahlgrenska University Hospital Gothenburg, Sweden Kopenhagen 2018 Complex fracture Changes in the AO/OTA classification system Complex Multifragmentary
Complex fractures of the humeral shaft Janos Solyom Sahlgrenska University Hospital Gothenburg, Sweden Kopenhagen 2018 Complex fracture Changes in the AO/OTA classification system Complex Multifragmentary
Humerus Block. Discontinued December 2016 DSEM/TRM/0115/0296(1) Surgical Technique. This publication is not intended for distribution in the USA.
 Humerus Block Surgical Technique Discontinued December 2016 DSEM/TRM/0115/0296(1) This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Contents
Humerus Block Surgical Technique Discontinued December 2016 DSEM/TRM/0115/0296(1) This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Contents
NEW INSTRUMENTS FOR INTERNAL FIXATION OF FRACTURES USING MINIMALLY INVASIVE TECHNIQUES
 NEW INSTRUMENTS FOR INTERNAL FIXATION OF FRACTURES USING MINIMALLY INVASIVE TECHNIQUES Dr.eng. Comşa Stanca, sing. Gheorghiu Doina, eng. Ciobota Dan National Institute of Research & Development for fine
NEW INSTRUMENTS FOR INTERNAL FIXATION OF FRACTURES USING MINIMALLY INVASIVE TECHNIQUES Dr.eng. Comşa Stanca, sing. Gheorghiu Doina, eng. Ciobota Dan National Institute of Research & Development for fine
THE HUMERUS 20 THE HUMERUS* CROSS SECTION CROSS SECTION SUPERIOR VIEW
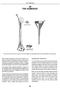 20 THE HUMERUS* CROSS SECTION CROSS SECTION SUPERIOR VIEW The marrow canal of the humerus is funnel-shaped. Its successful pinning is influenced by many factors. With a few exceptions, the entire humerus
20 THE HUMERUS* CROSS SECTION CROSS SECTION SUPERIOR VIEW The marrow canal of the humerus is funnel-shaped. Its successful pinning is influenced by many factors. With a few exceptions, the entire humerus
Technique Guide. PHILOS and PHILOS Long. The anatomic fixation system for the proximal humerus.
 Technique Guide PHILOS and PHILOS Long. The anatomic fixation system for the proximal humerus. Table of Contents Introduction PHILOS and PHILOS Long 2 AO Principles 4 Indications 5 Surgical Technique
Technique Guide PHILOS and PHILOS Long. The anatomic fixation system for the proximal humerus. Table of Contents Introduction PHILOS and PHILOS Long 2 AO Principles 4 Indications 5 Surgical Technique
Risk of Axillary Nerve Injury in Standard Anterolateral Approach of Shoulder: Cadaveric Study
 doi: http://dx.doi.org/10.5704/moj.1811.001 Risk of Axillary Nerve Injury in Standard Anterolateral Approach of Shoulder: Cadaveric Study Kongcharoensombat W, MD, Wattananon P, MD Department of Orthopaedics,
doi: http://dx.doi.org/10.5704/moj.1811.001 Risk of Axillary Nerve Injury in Standard Anterolateral Approach of Shoulder: Cadaveric Study Kongcharoensombat W, MD, Wattananon P, MD Department of Orthopaedics,
Minimally Invasive Plating Osteosynthesis for Mid-distal Third Humeral Shaft Fractures
 Minimally Invasive Plating Osteosynthesis for Mid-distal Third Humeral Shaft Fractures Kejian Lian, MD; Lei Wang, MD; Dasheng Lin, MD; Zhiwen Chen, MD abstract Full article available online at Healio.com/Orthopedics.
Minimally Invasive Plating Osteosynthesis for Mid-distal Third Humeral Shaft Fractures Kejian Lian, MD; Lei Wang, MD; Dasheng Lin, MD; Zhiwen Chen, MD abstract Full article available online at Healio.com/Orthopedics.
Surgical management of fracture both bone forearm in adult using limited contact dynamic compression plate
 2017; 3(2): 852-856 ISSN: 2395-1958 IJOS 2017; 3(2): 852-856 2017 IJOS www.orthopaper.com Received: 01-02-2017 Accepted: 02-03-2017 Muralidhar BM Associate Professor, Department Ravi KB Assistant Professor,
2017; 3(2): 852-856 ISSN: 2395-1958 IJOS 2017; 3(2): 852-856 2017 IJOS www.orthopaper.com Received: 01-02-2017 Accepted: 02-03-2017 Muralidhar BM Associate Professor, Department Ravi KB Assistant Professor,
LCP Proximal Radius Plates 2.4. Plates for radial head rim and for radial head neck address individual fracture patterns of the proximal radius.
 Technique Guide LCP Proximal Radius Plates 2.4. Plates for radial head rim and for radial head neck address individual fracture patterns of the proximal radius. Table of Contents Introduction LCP Proximal
Technique Guide LCP Proximal Radius Plates 2.4. Plates for radial head rim and for radial head neck address individual fracture patterns of the proximal radius. Table of Contents Introduction LCP Proximal
Orthopedics - Dr. Ahmad - Lecture 2 - Injuries of the Upper Limb
 The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
Technique Guide. 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm LCP Distal Fibula Plates 2 AO Principles
Technique Guide 2.7 mm/3.5 mm LCP Distal Fibula Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm LCP Distal Fibula Plates 2 AO Principles
LCP Medial Proximal Tibial Plate 4.5/5.0. Part of the Synthes LCP periarticular plating system.
 LCP Medial Proximal Tibial Plate 4.5/5.0. Part of the Synthes LCP periarticular plating system. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
LCP Medial Proximal Tibial Plate 4.5/5.0. Part of the Synthes LCP periarticular plating system. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Implant failure within 3 days after plating of fracture shaft humerus
 Basic Research Journal of Medicine and Clinical Sciences ISSN 2315-6864 Vol. 2(3) pp. 32-36 March 2013 Available online http//www.basicresearchjournals.org Copyright 2013 Basic Research Journal Case Report
Basic Research Journal of Medicine and Clinical Sciences ISSN 2315-6864 Vol. 2(3) pp. 32-36 March 2013 Available online http//www.basicresearchjournals.org Copyright 2013 Basic Research Journal Case Report
AcUMEDr. LoCKING CLAVICLE PLATE SYSTEM
 AcUMEDr LoCKING CLAVICLE PLATE SYSTEM LoCKING CLAVICLE PLATE SYSTEM Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients.
AcUMEDr LoCKING CLAVICLE PLATE SYSTEM LoCKING CLAVICLE PLATE SYSTEM Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients.
CURRENT TREATMENT OPTIONS
 CURRENT TREATMENT OPTIONS Fix single column or both: Always fix both. A study by Svend-Hansen corroborated the poor results associated with isolated medial malleolar fixation in bimalleolar ankle fractures.
CURRENT TREATMENT OPTIONS Fix single column or both: Always fix both. A study by Svend-Hansen corroborated the poor results associated with isolated medial malleolar fixation in bimalleolar ankle fractures.
Olecranon fracture. Lonnie Froberg, MD, Ph.D Rigshospitalet, Copenhagen University Hospital
 Olecranon fracture Lonnie Froberg, MD, Ph.D Rigshospitalet, Copenhagen University Hospital 20% of forearm fracture 12 per 100.000 persons per year Low-energy fall Increased risk >50 years 90% AO 21.B1.1
Olecranon fracture Lonnie Froberg, MD, Ph.D Rigshospitalet, Copenhagen University Hospital 20% of forearm fracture 12 per 100.000 persons per year Low-energy fall Increased risk >50 years 90% AO 21.B1.1
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article To Study the Functional Outcome of Locking Compression Plate in Metaphyseal Fractures Saraf
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article To Study the Functional Outcome of Locking Compression Plate in Metaphyseal Fractures Saraf
Technique Guide. 3.5 mm LCP Olecranon Plates. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide 3.5 mm LCP Olecranon Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Olecranon Plates 2 AO Principles 3 Indications 3 Clinical
Technique Guide 3.5 mm LCP Olecranon Plates. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction 3.5 mm LCP Olecranon Plates 2 AO Principles 3 Indications 3 Clinical
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture.
 Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture. stud. med. David Andreas Lunde Hatfield stud. med. Mohammed Sherif
Results of tibia nailing with Angular Stable Locking Screws (ASLS); A retrospective study of 107 patients with distal tibia fracture. stud. med. David Andreas Lunde Hatfield stud. med. Mohammed Sherif
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES. Clavicle fractures Proximal head of humerus fractures
 REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
3.5 mm LCP Distal Tibia T-Plates
 Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Distal Tibia T-Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Distal Tibia T-Plates 2 AO Principles 4 Indications
Part of the DePuy Synthes Locking Compression Plate (LCP ) System 3.5 mm LCP Distal Tibia T-Plates Surgical Technique Table of Contents Introduction 3.5 mm LCP Distal Tibia T-Plates 2 AO Principles 4 Indications
A locking plate system that expands a surgeon s options in trauma surgery. Zimmer NCB Plating System
 A locking plate system that expands a surgeon s options in trauma surgery Zimmer NCB Plating System The Power of Choice The power of having true intraoperative options is at your fingertips. Using standard
A locking plate system that expands a surgeon s options in trauma surgery Zimmer NCB Plating System The Power of Choice The power of having true intraoperative options is at your fingertips. Using standard
