Meniscal Allografts and Other Meniscal Implants. Populations Interventions Comparators Outcomes Individuals: Who are undergoing partial meniscectomy
|
|
|
- Polly Rose
- 5 years ago
- Views:
Transcription
1 Protocol Meniscal Allografts and Other Meniscal Implants (70115) Medical Benefit Effective Date: 01/01/14 Next Review Date: 09/18 Preauthorization No Review Dates: 02/07, 02/08, 03/09, 01/10, 01/11, 01/12, 09/12, 09/13, 09/14, 09/15, 09/16, 09/17 Preauthorization is not required. The following protocol contains medical necessity criteria that apply for this service. The criteria are also applicable to services provided in the local Medicare Advantage operating area for those members, unless separate Medicare Advantage criteria are indicated. If the criteria are not met, reimbursement will be denied and the patient cannot be billed. Please note that payment for covered services is subject to eligibility and the limitations noted in the patient s contract at the time the services are rendered. Populations Interventions Comparators Outcomes meniscectomy meniscectomy, and repair of malalignment, focal chondral defects, and/or ligamentous insufficiency meniscectomy meniscectomy Meniscal allograft Meniscal allograft Collagen meniscal implants Polyurethane meniscal implants without meniscal allograft without meniscal allograft without meniscal implant without meniscal implant Description Meniscal allografts and other meniscal implants (e.g., collagen or polyurethane) are intended to improve symptoms and reduce joint degeneration in patients who have had a total or partial meniscus resection. Summary of Evidence For individuals who are undergoing partial meniscectomy who receive meniscal allograft, the evidence includes systematic reviews of mostly case series. Relevant outcomes are symptoms, functional outcomes, and quality of life. The systematic reviews concluded that most studies have shown statistically significant improvements in pain and function following the procedure. The benefits have also been shown to have long-term effect (> 10 years). Reviews have also reported acceptable complication and failure rates. There Page 1 of 7
2 remains no evidence that meniscal allograft can delay or prevent the development of knee osteoarthritis. A limitation of the evidence is its reliance primarily on case series. The evidence is sufficient to determine that the technology results in a meaningful improvement in the net health outcome. For individuals who are undergoing partial meniscectomy and concomitant repair of malalignment, focal chondral defects, and/or ligamentous insufficiency who receive meniscal allograft, the evidence includes one systematic review of case series as well as case series published after the systematic review. Relevant outcomes are symptoms, functional outcomes, and quality of life. The systematic review concluded that pain and function improved following the procedure. One of the series published after the review showed that patients with more severe cartilage damage experienced favorable outcomes similar to patients with less cartilage damage. Another series published subsequently reported an overall 9.7-year survival of the implant. A limitation of the evidence is its reliance primarily on case series. The evidence is sufficient to determine that the technology results in a meaningful improvement in the net health outcome. For individuals who are undergoing partial meniscectomy who receive collagen meniscal implants, the evidence includes two systematic reviews primarily of case series. Relevant outcomes are symptoms, functional outcomes, and quality of life. The reviews reported overall positive results with the collagen meniscus implant, but the quality of the included studies (randomized controlled trials, observational studies) is low. Radiologic evaluations have shown reduced size of the implant in a large portion of patients. The evidence is insufficient to determine the effects of the technology on health outcomes. For individuals who are undergoing partial meniscectomy who receive polyurethane meniscal implants, the evidence includes a multicenter case series from the Actifit Study Group, an independently conducted pragmatic trial, and a small case series. Relevant outcomes are symptoms, functional outcomes, and quality of life. Overall improvements in pain and function have been seen following the implantation. The longest follow-up among these studies is five years. The studies had small sample sizes and were of low quality. Currently, no polyurethane meniscal implants have been approved by the Food and Drug Administration for use in the United States. The evidence is insufficient to determine the effects of the technology on health outcomes. Policy Meniscal allograft may be considered medically necessary in patients who have had a prior meniscectomy and have symptoms related to the affected side, when all of the following criteria are met: Adult patients should be too young to be considered an appropriate candidate for total knee arthroplasty or other reconstructive knee surgery (e.g., younger than 55 years) Disabling knee pain with activity that is refractory to conservative treatment Absence or near absence (more than 50%) of the meniscus, established by imaging or prior surgery Documented minimal to absent diffuse degenerative changes in the surrounding articular cartilage (e.g., Outerbridge Grade II or less, less than 50% joint space narrowing) Normal knee biomechanics, or alignment and stability achieved concurrently with meniscal. Meniscal allograft may be considered medically necessary when performed in combination, either concurrently or sequentially, with treatment of focal articular cartilage lesions using any of the following procedures: autologous chondrocyte implantation, or osteochondral allografting, or osteochondral autografting. Page 2 of 7
3 Use of other meniscal implants incorporating materials such as collagen and polyurethane are considered investigational. Policy Guidelines Patients should exhibit symptoms of persistent disabling knee pain that have adequately responded to physical therapy and analgesic medications. Uncorrected misalignment and instability of the joint are contraindications. Therefore additional procedures, such as repair of ligaments or tendons or creation of an osteotomy for realignment of the joint, may be performed at the same time. Severe obesity (e.g., body mass index greater than 35 kg/m 2 ) may affect outcomes due to the increased stress on weight bearing surfaces of the joint. Meniscal allograft is typically recommended for young active patients who are too young for total knee arthroplasty. Background Meniscal Cartilage Meniscal cartilage is an integral structural component of the human knee, functioning to absorb shocks and providing load sharing, joint stability, congruity, proprioception, and lubrication and nutrition of the cartilage surfaces. Total and partial meniscectomy frequently result in degenerative osteoarthritis (OA). The integrity of the menisci is particularly important in knees in which the anterior cruciate ligament (ACL) has been damaged. In these situations, the menisci act as secondary stabilizers of anteroposterior and varus-valgus translation. Treatment Meniscal allograft (MAT) has been investigated in patients with a previous meniscectomy, or in patients who require a total or near total meniscectomy for irreparable tears. There are three general groups of patients who have been treated with MAT: young patients with a history of meniscectomy who have symptoms of pain and discomfort associated with early OA that is localized to the meniscus-deficient compartment patients undergoing ACL reconstruction in whom a concomitant meniscal transplant is intended to provide increased stability young athletes with few symptoms in whom the allograft is intended to deter the development of OA. Due to the risks associated with this surgical procedure, prophylactic treatment for this purpose is not frequently recommended. Issues under study include techniques for processing and storing the grafts, proper sizing of the grafts, and appropriate surgical techniques. The four primary ways of processing and storing allografts are: fresh viable, fresh frozen, cryopreserved, and lyophilized. Fresh viable implants, harvested under sterile conditions, are less frequently used because the grafts must be used within a couple of days to maintain viability. Alternatively, the harvested meniscus can be fresh frozen for storage until needed. Cryopreservation freezes the graft in glycerol, which aids in preserving the cell membrane integrity and donor fibrochondrocyte viability. Cryolife (Marietta, GA) is a commercial supplier of such grafts. Donor tissues may also be dehydrated (freeze-dried or lyophilized), permitting storage at room temperature. Lyophilized grafts are prone to reduced tensile strength, shrinkage, poor rehydration, post- joint effusion, and synovitis; they are no longer used in the clinical setting. Several secondary sterilization techniques may be used, with gamma irradiation the most common. The dose of radiation considered effective has been shown to change the mechanical structure of the allograft; therefore, nonirradiated grafts from screened donors are most frequently used. In a survey conducted by the Page 3 of 7
4 International Meniscus Reconstruction Experts Forum, when surgeons were asked about allograft preference, 68% preferred fresh frozen nonirradiated allografts, with 14% responding fresh viable allografts. 1 There are several techniques for MAT; most are arthroscopically assisted or all-arthroscopic. Broadly, the techniques are either all-suture fixation or bone fixation. Within the bone fixation category, the surgeon may use either bone plugs or a bone bridge. Types of bone bridges include keyhole, trough, dove-tail, and bridge-in-slot. The technique used depends on laterality and the need for concomitant procedures. Patients with malalignment, focal chondral defects, and/or ligamentous insufficiency may need concomitant procedures (osteotomy, cartilage restoration, and/or ligament reconstruction, respectively). 2 Tissue engineering that grows new replacement host tissue is also being investigated. For example, the Collagen Meniscus Implant (Ivy Sports Medicine, formerly the ReGen Collagen Scaffold by ReGen Biologics), is a resorbable collagen matrix composed primarily of type I collagen from bovine Achilles tendons. The implant is provided in a semilunar shape and trimmed to size for suturing to the remaining meniscal rim. The implant provides an absorbable collagen scaffold that is replaced by the patient s own soft tissue; it is not intended to replace normal body structure. Because it requires a meniscal rim for attachment, it is intended to fill meniscus defects after a partial meniscectomy. Other scaffold materials and cell-seeding techniques are being investigated. For example, Actifit (Orteq) is a biodegradable polyurethane scaffold that currently has market approval in Europe. Nonabsorbable and nonporous synthetic implants for total meniscus replacement are in development. One total meniscus replacement that is in early phase clinical testing is NUsurface (Active Implants); it is composed of a polyethylene reinforced polycarbonate urethane. Regulatory Status Collagen Meniscus Implants In 2008, the ReGen Collagen Scaffold (CS) was cleared for marketing by the U.S. Food and Drug Administration (FDA) through the 510(k) process. FDA determined that this device was substantially equivalent to existing absorbable surgical mesh devices. The ReGen Collagen Scaffold (also known as MenaFlex TM CMI) was the only collagen meniscus implant (CMI) with FDA clearance at that time. Amid controversy about this 510(k) clearance decision, FDA reviewed the decision. In October 2010, FDA rescinded the approval, stating that MenaFlex TM is intended for different purposes and is technologically dissimilar from the predicate devices identified in the approval process. The manufacturer appealed the rescission, and won its appeal in The product, now called CMI, is manufactured by Ivy Sports Medicine. CMI is the only FDA-approved collagen meniscus product currently on the market. FDA product code: OLC. Polyurethane Meniscal Implant There are no FDA-approved polyurethane meniscal implants currently on the market in the United States. Actifit is approved for marketing in Europe. Related Protocols Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions Services that are the subject of a clinical trial do not meet our Technology Assessment Protocol criteria and are Page 4 of 7
5 considered investigational. For explanation of experimental and investigational, please refer to the Technology Assessment Protocol. It is expected that only appropriate and medically necessary services will be rendered. We reserve the right to conduct prepayment and postpayment reviews to assess the medical appropriateness of the above-referenced procedures. Some of this protocol may not pertain to the patients you provide care to, as it may relate to products that are not available in your geographic area. References We are not responsible for the continuing viability of web site addresses that may be listed in any references below. 1. Getgood A, LaPrade RF, Verdonk P, et al. International Meniscus Reconstruction Experts Forum (IMREF) 2015 consensus statement on the practice of meniscal allograft. Am J Sports Med. Aug PMID Frank RM, Cole BJ. Meniscus. Curr Rev Musculoskelet Med. Dec 2015; 8(4): PMID Cvetanovich GL, Yanke AB, McCormick F, et al. Trends in meniscal allograft in the United States, 2007 to Arthroscopy. Jun 2015; 31(6): PMID Elattar M, Dhollander A, Verdonk R, et al. Twenty-six years of meniscal allograft : is it still experimental? A meta-analysis of 44 trials. Knee Surg Sports Traumatol Arthrosc. Feb 2011; 19(2): PMID Hergan D, Thut D, Sherman O, et al. Meniscal allograft. Arthroscopy. Jan 2011; 27(1): PMID Rosso F, Bisicchia S, Bonasia DE, et al. Meniscal allograft : a systematic review. Am J Sports Med. Apr 2015; 43(4): PMID Verdonk PC, Demurie A, Almqvist KF, et al. Transplantation of viable meniscal allograft. Survivorship analysis and clinical outcome of one hundred cases. J Bone Joint Surg Am. Apr 2005; 87(4): PMID Hommen JP, Applegate GR, Del Pizzo W. Meniscus allograft : ten-year results of cryopreserved allografts. Arthroscopy. Apr 2007; 23(4): PMID van der Wal RJ, Thomassen BJ, van Arkel ER. Long-term clinical outcome of open meniscal allograft. Am J Sports Med. Nov 2009; 37(11): PMID Vundelinckx B, Bellemans J, Vanlauwe J. Arthroscopically assisted meniscal allograft in the knee: a medium-term subjective, clinical, and radiographical outcome evaluation. Am J Sports Med. Nov 2010; 38(11): PMID Harris JD, Cavo M, Brophy R, et al. Biological knee reconstruction: a systematic review of combined meniscal allograft and cartilage repair or restoration. Arthroscopy. Mar 2011; 27(3): PMID Stone KR, Adelson WS, Pelsis JR, et al. Long-term survival of concurrent meniscus allograft and repair of the articular cartilage: a prospective two- to 12-year follow-up report. J Bone Joint Surg Br. Jul 2010; 92(7): PMID Farr J, Rawal A, Marberry KM. Concomitant meniscal allograft and autologous chondrocyte implantation: minimum 2-year follow-up. Am J Sports Med. Sep 2007; 35(9): PMID Rue JP, Yanke AB, Busam ML, et al. Prospective evaluation of concurrent meniscus and articular cartilage repair: minimum 2-year follow-up. Am J Sports Med. Sep 2008; 36(9): PMID Page 5 of 7
6 15. Kempshall PJ, Parkinson B, Thomas M, et al. Outcome of meniscal allograft related to articular cartilage status: advanced chondral damage should not be a contraindication. Knee Surg Sports Traumatol Arthrosc. Jan 2015; 23(1): PMID Ogura T, Bryant T, Minas T. Biological knee reconstruction with concomitant autologous chondrocyte implantation and meniscal allograft : mid- to long-term outcomes. Orthop J Sports Med. Oct 2016; 4(10): PMID Zaffagnini S, Grassi A, Marcheggiani Muccioli GM, et al. Survivorship and clinical outcomes of 147 consecutive isolated or combined arthroscopic bone plug free meniscal allograft. Knee Surg Sports Traumatol Arthrosc. May 2016; 24(5): PMID Harston A, Nyland J, Brand E, et al. Collagen meniscus implantation: a systematic review including rehabilitation and return to sports activity. Knee Surg Sports Traumatol Arthrosc. Jan 2012; 20(1): PMID Warth RJ, Rodkey WG. Resorbable collagen scaffolds for the treatment of meniscus defects: a systematic review. Arthroscopy. May 2015; 31(5): PMID Zaffagnini S, Grassi A, Marcheggiani Muccioli GM, et al. MRI evaluation of a collagen meniscus implant: a systematic review. Knee Surg Sports Traumatol Arthrosc. Nov 2015; 23(11): PMID Rodkey WG, DeHaven KE, Montgomery WH, 3rd, et al. Comparison of the collagen meniscus implant with partial meniscectomy. A prospective randomized trial. J Bone Joint Surg Am. Jul 2008; 90(7): PMID Linke RD, Ulmer M, Imhoff AB. [Replacement of the meniscus with a collagen implant (CMI)] [German]. Oper Orthop Traumatol. Dec 2006; 18(5-6): PMID Zaffagnini S, Marcheggiani Muccioli GM, Lopomo N, et al. Prospective long-term outcomes of the medial collagen meniscus implant versus partial medial meniscectomy: a minimum 10-year follow-up study. Am J Sports Med. May 2011; 39(5): PMID Bulgheroni E, Grassi A, Bulgheroni P, et al. Long-term outcomes of medial CMI implant versus partial medial meniscectomy in patients with concomitant ACL reconstruction. Knee Surg Sports Traumatol Arthrosc. Nov 2015; 23(11): PMID Verdonk R, Verdonk P, Huysse W, et al. Tissue ingrowth after implantation of a novel, biodegradable polyurethane scaffold for treatment of partial meniscal lesions. Am J Sports Med. Apr 2011; 39(4): PMID Verdonk P, Beaufils P, Bellemans J, et al. Successful treatment of painful irreparable partial meniscal defects with a polyurethane scaffold: two-year safety and clinical outcomes. Am J Sports Med. Apr 2012; 40(4): PMID Dhollander A, Verdonk P, Verdonk R. Treatment of painful, irreparable partial meniscal defects with a polyurethane scaffold: midterm clinical outcomes and survival analysis. Am J Sports Med. Oct 2016; 44(10): PMID Bouyarmane H, Beaufils P, Pujol N, et al. Polyurethane scaffold in lateral meniscus segmental defects: Clinical outcomes at 24 months follow-up. Orthop Traumatol Surg Res. Feb 2014; 100(1): PMID Gelber PE, Isart A, Erquicia JI, et al. Partial meniscus substitution with a polyurethane scaffold does not improve outcome after an open-wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc. Jan 2015; 23(1): PMID Schuttler KF, Haberhauer F, Gesslein M, et al. Midterm follow-up after implantation of a polyurethane meniscal scaffold for segmental medial meniscus loss: maintenance of good clinical and MRI outcome. Knee Surg Sports Traumatol Arthrosc. May 2016; 24(5): PMID Efe T, Getgood A, Schofer MD, et al. The safety and short-term efficacy of a novel polyurethane meniscal scaffold for the treatment of segmental medial meniscus deficiency. Knee Surg Sports Traumatol Arthrosc. Sep 2012; 20(9): PMID Page 6 of 7
7 32. National Institute for Health and Clinical Excellence (NICE). Partial replacement of the meniscus of the knee using a biodegradable scaffold: guidance [IPG430 ]. 2012; Accessed April 6, American Academy of Orthopaedic Surgeons. Your Orthopaedic Connection: Meniscal transplant surgery. 2009; Accessed April 6, Centers for Medicare and Medicaid Services (CMS). Decision Memo for COLLAGEN MENISCUS IMPLANT (CAG-00414N). 2010; gen+meniscus+implant&keywordlookup=title&keywordsearchtype=and&id=235&bc=gaaaacaacaaaaa %3d%3d&. Accessed April 5, Page 7 of 7
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: meniscal_allografts_and_other_meniscal_implants 9/1993 6/2018 6/2019 6/2018 Description of Procedure or Service
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: meniscal_allografts_and_other_meniscal_implants 9/1993 6/2018 6/2019 6/2018 Description of Procedure or Service
Meniscal Allografts and Collagen Meniscus Implants. Original Policy Date
 MP 7.01.11 Meniscal Allografts and Collagen Meniscus Implants Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
MP 7.01.11 Meniscal Allografts and Collagen Meniscus Implants Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
MENISCUS IMPLANT AND ALLOGRAFT
 MENISCUS IMPLANT AND ALLOGRAFT UnitedHealthcare Commercial Medical Policy Policy Number: SUR063 Effective Date: January 1, 2019 Table of Contents Page COVERAGE RATIONALE... 1 APPLICABLE CODES... 1 DESCRIPTION
MENISCUS IMPLANT AND ALLOGRAFT UnitedHealthcare Commercial Medical Policy Policy Number: SUR063 Effective Date: January 1, 2019 Table of Contents Page COVERAGE RATIONALE... 1 APPLICABLE CODES... 1 DESCRIPTION
Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status
 # 154134 Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status Jun-Gu Park, Seong-Il Bin, Jong-Min Kim, Bum Sik Lee Department of Orthopaedic Surgery, Asan Medical
# 154134 Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status Jun-Gu Park, Seong-Il Bin, Jong-Min Kim, Bum Sik Lee Department of Orthopaedic Surgery, Asan Medical
Clinical Application of Scaffolds for Partial Meniscus Replacement
 1 Clinical Application of Scaffolds for Partial Meniscus Replacement 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 Cathal&J.&Moran,&MD,&FRCS(Orth)& 1,&Daniel&P&Withers&MB,&FRCS&(Orth)&
1 Clinical Application of Scaffolds for Partial Meniscus Replacement 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 Cathal&J.&Moran,&MD,&FRCS(Orth)& 1,&Daniel&P&Withers&MB,&FRCS&(Orth)&
Osteochondral allografting for all other joints is not covered as the evidence is insufficient to determine the
 Medical Coverage Policy Osteochondral Autologous Chrondrocyte Implantation for Focal Articular Cartilage Lesions EFFECTIVE DATE: 05 20 2008 POLICY LAST UPDATED: 10 16 2018 OVERVIEW A variety of procedures
Medical Coverage Policy Osteochondral Autologous Chrondrocyte Implantation for Focal Articular Cartilage Lesions EFFECTIVE DATE: 05 20 2008 POLICY LAST UPDATED: 10 16 2018 OVERVIEW A variety of procedures
NEW DEVELOPMENTS IN MENISCAL SURGERY
 NEW DEVELOPMENTS IN MENISCAL SURGERY Written by Peter Verdonk, Belgium and Francesco Perdisa, Italy Meniscectomy is one of the most common procedures in orthopaedic surgery, capable of returning the knee
NEW DEVELOPMENTS IN MENISCAL SURGERY Written by Peter Verdonk, Belgium and Francesco Perdisa, Italy Meniscectomy is one of the most common procedures in orthopaedic surgery, capable of returning the knee
Collagen meniscus implant for repair of medial meniscus injury of the knee. California Technology Assessment Forum
 TITLE: Collagen meniscus implant for repair of medial meniscus injury of the knee AUTHOR: Jeffrey A. Tice, MD Assistant Professor of Medicine Division of General Internal Medicine Department of Medicine
TITLE: Collagen meniscus implant for repair of medial meniscus injury of the knee AUTHOR: Jeffrey A. Tice, MD Assistant Professor of Medicine Division of General Internal Medicine Department of Medicine
Assessment of the Knee Articular Cartilage through MRI-T2 Mapping at Five Year Follow-Up of Meniscal Allograft Transplantation
 Assessment of the Knee Articular Cartilage through MRI-T2 Mapping at Five Year Follow-Up of Meniscal Allograft Transplantation Luis T. Llano-Rodriguez, MD, Mexico City, MEXICO Francisco Cruz-Lopez, Mexico
Assessment of the Knee Articular Cartilage through MRI-T2 Mapping at Five Year Follow-Up of Meniscal Allograft Transplantation Luis T. Llano-Rodriguez, MD, Mexico City, MEXICO Francisco Cruz-Lopez, Mexico
OSTEOCHONDRAL ALLOGRAFTS AND AUTOGRAFTS IN THE TREATMENT OF FOCAL ARTICULAR CARTILAGE LESIONS
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
5 Points on Meniscal Allograft Transplantation
 5 Points on Meniscal Allograft Transplantation Publish date: September 4, 2018 Authors: Matthew E. Gitelis, BS Rachel M. Frank, MD Maximillian A. Meyer, BS Gregory Cvetanovich, MD Brian J. Cole, MD, MBA
5 Points on Meniscal Allograft Transplantation Publish date: September 4, 2018 Authors: Matthew E. Gitelis, BS Rachel M. Frank, MD Maximillian A. Meyer, BS Gregory Cvetanovich, MD Brian J. Cole, MD, MBA
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
Long-term survival of concurrent meniscus allograft transplantation and repair of the articular cartilage
 Long-term survival of concurrent meniscus allograft transplantation and repair of the articular cartilage A PROSPECTIVE TWO- TO 12-YEAR FOLLOW-UP REPORT K. R. Stone, W. S. Adelson, J. R. Pelsis, A. W.
Long-term survival of concurrent meniscus allograft transplantation and repair of the articular cartilage A PROSPECTIVE TWO- TO 12-YEAR FOLLOW-UP REPORT K. R. Stone, W. S. Adelson, J. R. Pelsis, A. W.
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of partial replacement of the meniscus of the knee using a biodegradable scaffold
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of partial replacement of the meniscus of the knee using a biodegradable scaffold
Outcome after meniscectomy? Val D Isere 2014 update
 Outcome after meniscectomy? Val D Isere 2014 update Meniscus Allograft Transplantation and New Options by Peter Verdonk, MD, PhD Department of Orthopaedic Surgery, Monica Hospitals, Antwerp, Belgium Peter
Outcome after meniscectomy? Val D Isere 2014 update Meniscus Allograft Transplantation and New Options by Peter Verdonk, MD, PhD Department of Orthopaedic Surgery, Monica Hospitals, Antwerp, Belgium Peter
The American Journal of Sports Medicine
 The American Journal of Sports Medicine http://ajs.sagepub.com/ Long-term Survivorship and Function of Meniscus Transplantation Frank R. Noyes and Sue D. Barber-Westin Am J Sports Med 2016 44: 2330 originally
The American Journal of Sports Medicine http://ajs.sagepub.com/ Long-term Survivorship and Function of Meniscus Transplantation Frank R. Noyes and Sue D. Barber-Westin Am J Sports Med 2016 44: 2330 originally
Meniscal Tears/Deficiency in Athletes
 Meniscal Tears/Deficiency in Athletes A. Amendola MD Professor of Orthopaedic Surgery Director of Sports Medicine Duke University 1 2 Meniscal tears Introduction Meniscal tears are one of the most frequent
Meniscal Tears/Deficiency in Athletes A. Amendola MD Professor of Orthopaedic Surgery Director of Sports Medicine Duke University 1 2 Meniscal tears Introduction Meniscal tears are one of the most frequent
Meniscal Transplants and Scaffolds: A Systematic Review of the Literature
 Review Article Knee Surg Relat Res 2017;29(1):3-10 https://doi.org/10.5792/ksrr.16.059 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Meniscal Transplants and Scaffolds: A Systematic Review
Review Article Knee Surg Relat Res 2017;29(1):3-10 https://doi.org/10.5792/ksrr.16.059 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Meniscal Transplants and Scaffolds: A Systematic Review
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
Corporate Medical Policy
 Corporate Medical Policy Autologous Chondrocyte Implantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: autologous_chondrocyte_implantation 4/1996 6/2017 6/2018 6/2017 Description
Corporate Medical Policy Autologous Chondrocyte Implantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: autologous_chondrocyte_implantation 4/1996 6/2017 6/2018 6/2017 Description
2012 Meniscus Transplantation Study Group Tuesday, February 7, :00 3:30 PM
 2012 Meniscus Transplantation Study Group Tuesday, February 7, 2012 1:00 3:30 PM W Hotel, Industry Room 181 Third Street, San Francisco, CA 94103 At the 2012 AAOS Annual Meeting Meeting Agenda: INTRODUCTION:
2012 Meniscus Transplantation Study Group Tuesday, February 7, 2012 1:00 3:30 PM W Hotel, Industry Room 181 Third Street, San Francisco, CA 94103 At the 2012 AAOS Annual Meeting Meeting Agenda: INTRODUCTION:
MEDICAL POLICY SUBJECT: OSTEOCHONDRAL GRAFTING
 MEDICAL POLICY PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
MEDICAL POLICY PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
CARTILAGE REPAIR INTRODUCTION. M. BERRUTO and G.M. PERETTI 1,2. Received January 6, Accepted January 8, 2013
 CARTILAGE REPAIR INTRODUCTION M. BERRUTO and G.M. PERETTI 1,2 Gaetano Pini Orthopedic Institute, Milan; 1 Department of Biomedical Sciences for Health, University of Milan, 2 IRCCS Galeazzi Orthopedic
CARTILAGE REPAIR INTRODUCTION M. BERRUTO and G.M. PERETTI 1,2 Gaetano Pini Orthopedic Institute, Milan; 1 Department of Biomedical Sciences for Health, University of Milan, 2 IRCCS Galeazzi Orthopedic
Knee Cartilage Transplants
 Knee Cartilage Transplants Date of Origin: 3/2005 Last Review Date: 8/23/2017 Effective Date: 8/23/2017 Dates Reviewed: Developed By: Medical Necessity Criteria Committee I. Description Allograft transplants
Knee Cartilage Transplants Date of Origin: 3/2005 Last Review Date: 8/23/2017 Effective Date: 8/23/2017 Dates Reviewed: Developed By: Medical Necessity Criteria Committee I. Description Allograft transplants
Disclosures. Reverse Engineer To Solve a Problem. Consider the big 6. Natural history vs. Surgical intervention. Which is better?
 Disclosures A la carte rebuilding of the knee: Stability, alignment and surface Jason M. Scopp, M.D. Director Joint Preservation Center Peninsula Orthopaedic Associates, P.A. Arthrex consultant Vericel
Disclosures A la carte rebuilding of the knee: Stability, alignment and surface Jason M. Scopp, M.D. Director Joint Preservation Center Peninsula Orthopaedic Associates, P.A. Arthrex consultant Vericel
Systematic Review. Meniscal Allograft Transplantation. David Hergan, M.D., David Thut, M.D., Orrin Sherman, M.D., and Michael S. Day, M.Phil.
 Systematic Review Meniscal Allograft Transplantation David Hergan, M.D., David Thut, M.D., Orrin Sherman, M.D., and Michael S. Day, M.Phil. Purpose: Meniscal allograft transplantation (MAT) has become
Systematic Review Meniscal Allograft Transplantation David Hergan, M.D., David Thut, M.D., Orrin Sherman, M.D., and Michael S. Day, M.Phil. Purpose: Meniscal allograft transplantation (MAT) has become
Clinical Policy: Articular Cartilage Defect Repairs Reference Number: CP.MP.26
 Clinical Policy: Reference Number: CP.MP.26 Effective Date: 10/08 Last Review Date: 05/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.26 Effective Date: 10/08 Last Review Date: 05/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
AUTOLOGOUS CHONDROCYTE TRANSPLANTS & COLLAGEN MENISCUS IMPLANTS IN THE KNEE
 AUTOLOGOUS CHONDROCYTE TRANSPLANTS & COLLAGEN MENISCUS IMPLANTS IN THE KNEE Protocol: SUR048 Effective Date: September 1, 2016 Table of Contents Page COMMERCIAL, MEDICARE & MEDICAID COVERAGE RATIONALE...
AUTOLOGOUS CHONDROCYTE TRANSPLANTS & COLLAGEN MENISCUS IMPLANTS IN THE KNEE Protocol: SUR048 Effective Date: September 1, 2016 Table of Contents Page COMMERCIAL, MEDICARE & MEDICAID COVERAGE RATIONALE...
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries. Cartilage Surgery. The Knee.
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Cartilage Surgery The Knee CARTILAGE INJURY Treatment of cartilage injury remains one of the most significant challenges
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Cartilage Surgery The Knee CARTILAGE INJURY Treatment of cartilage injury remains one of the most significant challenges
Elizaveta Kon, Giuseppe Filardo, Stefano Zaffagnini, Alessandro Di Martino, Berardo Di Matteo, Giulio Maria Marcheggiani Muccioli, et al.
 Biodegradable polyurethane meniscal scaffold for isolated partial lesions or as combined procedure for knees with multiple comorbidities: clinical results at 2 years Elizaveta Kon, Giuseppe Filardo, Stefano
Biodegradable polyurethane meniscal scaffold for isolated partial lesions or as combined procedure for knees with multiple comorbidities: clinical results at 2 years Elizaveta Kon, Giuseppe Filardo, Stefano
Meniscus Transplantation
 Chapter 18 Meniscus Transplantation Introduction Any significant loss of meniscal function through injury or menisectomy alters the biomechanical and biological environment of the normal knee, eventually
Chapter 18 Meniscus Transplantation Introduction Any significant loss of meniscal function through injury or menisectomy alters the biomechanical and biological environment of the normal knee, eventually
Does Every Knee Need a Meniscus?
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/does-every-knee-need-a-meniscus/3799/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/does-every-knee-need-a-meniscus/3799/
New Directions in Osteoarthritis Research
 New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells,
 What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
Rehab Considerations: Meniscus
 Rehab Considerations: Meniscus Steve Cox, PT, DPT Department of Orthopaedics School of Medicine University of Texas Health Science Center at San Antonio 1 -Anatomy/ Function/ Injuries -Treatment Options
Rehab Considerations: Meniscus Steve Cox, PT, DPT Department of Orthopaedics School of Medicine University of Texas Health Science Center at San Antonio 1 -Anatomy/ Function/ Injuries -Treatment Options
American Journal of Sports Medicine
 American Journal of Sports Medicine http://ajs.sagepub.com Prospective Evaluation of Concurrent Meniscus Transplantation and Articular Cartilage Repair: Minimum 2-Year Follow-Up LCDR John-Paul H. Rue,
American Journal of Sports Medicine http://ajs.sagepub.com Prospective Evaluation of Concurrent Meniscus Transplantation and Articular Cartilage Repair: Minimum 2-Year Follow-Up LCDR John-Paul H. Rue,
The Treatment of the Early Degenerative Knee and Use of Biologics
 The Treatment of the Early Degenerative Knee and Use of Biologics Presented to: Insert relevant presenter information Calibri 16pt Brian Chilelli, MD Presented on: Month day, Year Department Presented
The Treatment of the Early Degenerative Knee and Use of Biologics Presented to: Insert relevant presenter information Calibri 16pt Brian Chilelli, MD Presented on: Month day, Year Department Presented
Meniscal Allografts & Cartilage Surgery in ACL revision surgery
 Meniscal Allografts & Cartilage Surgery in ACL revision surgery Peter Verdonk, MD, PhD Department of Orthopaedic Surgery, Ghent University Hospital, Belgium 1 Introduction Outcome after ACL reconstruction
Meniscal Allografts & Cartilage Surgery in ACL revision surgery Peter Verdonk, MD, PhD Department of Orthopaedic Surgery, Ghent University Hospital, Belgium 1 Introduction Outcome after ACL reconstruction
Ideal Candidate for Cartilage Restoration. Large or Complex Lesions
 Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques
 Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques R O B E R T N A S C I M E N TO, M D, M S C H I E F OF S P O RT S M E D I C I N E & SH O U L D E R S U R G E RY N E W TO N- W E L L E S L
Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques R O B E R T N A S C I M E N TO, M D, M S C H I E F OF S P O RT S M E D I C I N E & SH O U L D E R S U R G E RY N E W TO N- W E L L E S L
CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS
 CARTILAGE REPAIR TECHNIQUES CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS Written by Steffano Zaffagnini, Francesco Perdisa and Giuseppe Filardo, Italy Knee articular cartilage defects greater
CARTILAGE REPAIR TECHNIQUES CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS Written by Steffano Zaffagnini, Francesco Perdisa and Giuseppe Filardo, Italy Knee articular cartilage defects greater
Meniscal Allograft Transplantation in the Adolescent Population
 Meniscal Allograft Transplantation in the Adolescent Population Jonathan C. Riboh, M.D., Annemarie K. Tilton, B.S., Gregory L. Cvetanovich, M.D., Kirk A. Campbell, M.D., and Brian J. Cole, M.D., M.B.A.
Meniscal Allograft Transplantation in the Adolescent Population Jonathan C. Riboh, M.D., Annemarie K. Tilton, B.S., Gregory L. Cvetanovich, M.D., Kirk A. Campbell, M.D., and Brian J. Cole, M.D., M.B.A.
Clinical Policy Title: Autologous chondrocyte implantation
 Clinical Policy Title: Autologous chondrocyte implantation Clinical Policy Number: 14.03.07 Effective Date: March 1, 2017 Initial Review Date: February 15, 2017 Most Recent Review Date: February 6, 2018
Clinical Policy Title: Autologous chondrocyte implantation Clinical Policy Number: 14.03.07 Effective Date: March 1, 2017 Initial Review Date: February 15, 2017 Most Recent Review Date: February 6, 2018
Meniscectomy to Repair: Roots, Ramps, Buckets, and Biologics. Charles A. Bush-Joseph, MD Rush University Medical Center Chicago, IL
 Meniscectomy to Repair: Roots, Ramps, Buckets, and Biologics Charles A. Bush-Joseph, MD Rush University Medical Center Chicago, IL Disclosures: None Orthopaedic Trends: Increase in physician education
Meniscectomy to Repair: Roots, Ramps, Buckets, and Biologics Charles A. Bush-Joseph, MD Rush University Medical Center Chicago, IL Disclosures: None Orthopaedic Trends: Increase in physician education
Humber. Arthroscopy Knee
 Humber Arthroscopy Knee Intervention Diagnostic & Therapeutic Arthroscopy Knee OPCS Codes W85 Therapeutic endoscopic operations on cavity of knee joint W851 Endoscopic removal of loose body from knee joint
Humber Arthroscopy Knee Intervention Diagnostic & Therapeutic Arthroscopy Knee OPCS Codes W85 Therapeutic endoscopic operations on cavity of knee joint W851 Endoscopic removal of loose body from knee joint
Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions
 Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions Policy Number: Original Effective Date: MM.06.002 8/1/2009 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration
Autologous Chondrocyte Implantation for Focal Articular Cartilage Lesions Policy Number: Original Effective Date: MM.06.002 8/1/2009 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration
Meniscus Reconstruction: Trough Surgical Technique
 Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR FOCAL ARTICULAR CARTILAGE LESIONS
 CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Lateral extra-articular tenodesis (LET) does not Increase lateral compartment contact pressures even in the face of subtotal meniscectomy
 Click to edit Master title style Lateral extra-articular tenodesis (LET) does not Increase lateral compartment contact pressures even in the face of subtotal meniscectomy Tomoyuki Shimakawa 1, Timothy
Click to edit Master title style Lateral extra-articular tenodesis (LET) does not Increase lateral compartment contact pressures even in the face of subtotal meniscectomy Tomoyuki Shimakawa 1, Timothy
Osteochondral Grafting
 Last Review Date: January 19, 2017 Number: MG.MM.SU.68 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: January 19, 2017 Number: MG.MM.SU.68 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping
 Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS
 ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 76TH ANNUAL MEETING FEBRUARY 25-28, 2009 LAS
ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 76TH ANNUAL MEETING FEBRUARY 25-28, 2009 LAS
MEDICAL POLICY SUBJECT: COMPUTER ASSISTED NAVIGATION FOR KNEE AND HIP ARTHROPLASTY
 MEDICAL POLICY PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
MEDICAL POLICY PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
5:05 6:05 pm Live Surgery: office based Arthroscopy (Trice Medical) (1 hr) Surgeon: Sean McMillan, DO Moderator: Chris Uggen, MD
 AAOS Articular Cartilage Restoration: Current, Emerging, and Advanced Techniques Course # 3252 February 7-9, 2019 OLC Education and Conference Center, Rosemont, IL Course Directors: Kevin D. Plancher,
AAOS Articular Cartilage Restoration: Current, Emerging, and Advanced Techniques Course # 3252 February 7-9, 2019 OLC Education and Conference Center, Rosemont, IL Course Directors: Kevin D. Plancher,
Failed Cartilage Repair
 Chapter 27 Failed Cartilage Repair Robert C. Grumet, Sarvottam Bajaj, and Brian J. Cole The management of traumatic and degenerative cartilage lesions is a known challenge given the limited vascularity
Chapter 27 Failed Cartilage Repair Robert C. Grumet, Sarvottam Bajaj, and Brian J. Cole The management of traumatic and degenerative cartilage lesions is a known challenge given the limited vascularity
Life. Uncompromised. The KineSpring Knee Implant System Surgeon Handout
 Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Biologics in ACL: What s the Data?
 Biologics in ACL: What s the Data? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior Scientist Sports Medicine and Shoulder
Biologics in ACL: What s the Data? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior Scientist Sports Medicine and Shoulder
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
why bicompartmental? A REVOLUTIONARY ALTERNATIVE TO TOTAL KNEE REPLACEMENTS
 why bicompartmental? A REVOLUTIONARY ALTERNATIVE TO TOTAL KNEE REPLACEMENTS TKR is not always the answer Today, many patients with medial or lateral disease and patellofemoral involvement receive a Total
why bicompartmental? A REVOLUTIONARY ALTERNATIVE TO TOTAL KNEE REPLACEMENTS TKR is not always the answer Today, many patients with medial or lateral disease and patellofemoral involvement receive a Total
Osteochondral Transplant Delivery System
 Osteochondral Transplant Delivery System Team Leader: Alex Teague BPAG: David Fiflis Communicator/BWIG: Alex Babinski BSAC: Zach Wodushek Client: Dr. Brian Walczak, DO Advisor: Dr. Tracy Puccinelli, PhD
Osteochondral Transplant Delivery System Team Leader: Alex Teague BPAG: David Fiflis Communicator/BWIG: Alex Babinski BSAC: Zach Wodushek Client: Dr. Brian Walczak, DO Advisor: Dr. Tracy Puccinelli, PhD
Joint Preservation Clinical Case
 Joint Preservation Clinical Case Jason M. Scopp, M.D. Director of Joint Preservation Peninsula Orthopaedic Associates, 1/19/19 Rational Rationale There are no absolutes. There is no dogma. Organize thoughts,
Joint Preservation Clinical Case Jason M. Scopp, M.D. Director of Joint Preservation Peninsula Orthopaedic Associates, 1/19/19 Rational Rationale There are no absolutes. There is no dogma. Organize thoughts,
MEDICAL POLICY SUBJECT: COMPUTER ASSISTED NAVIGATION FOR KNEE AND HIP ARTHROPLASTY
 MEDICAL POLICY SUBJECT: COMPUTER ASSISTED PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including an
MEDICAL POLICY SUBJECT: COMPUTER ASSISTED PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including an
LARS (Ligament Augmentation & Reconstruction System) Literature
 LARS-Related Studies and Papers ACL: 1. Level of Evidence: IV Li, H. et al (2011). Enhancement of the osseointegration of a polyethylene Terephthalate artificial ligament graft in a bone tunnel using 58S
LARS-Related Studies and Papers ACL: 1. Level of Evidence: IV Li, H. et al (2011). Enhancement of the osseointegration of a polyethylene Terephthalate artificial ligament graft in a bone tunnel using 58S
Member of the Editorial board of EFORT open reviews and Austin Sport Medicine Journal.
 Tommaso Bonanzinga, MD Istituto Clinico Humanitas, Milano, Italy Orthopaedic surgeon, former staff member I Orthopaedic Clinic leaded by Prof. Marcacci (Rizzoli Orthopaedic Institute). Assistant Professor,
Tommaso Bonanzinga, MD Istituto Clinico Humanitas, Milano, Italy Orthopaedic surgeon, former staff member I Orthopaedic Clinic leaded by Prof. Marcacci (Rizzoli Orthopaedic Institute). Assistant Professor,
Outcomes of Osteochondral Allograft Transplantation With and Without Concomitant Meniscus Allograft Transplantation
 Outcomes of Osteochondral Allograft Transplantation With and Without Concomitant Meniscus Allograft Transplantation A Comparative Matched Group Analysis Rachel M. Frank,* y MD, Simon Lee, z MD, MPH, Eric
Outcomes of Osteochondral Allograft Transplantation With and Without Concomitant Meniscus Allograft Transplantation A Comparative Matched Group Analysis Rachel M. Frank,* y MD, Simon Lee, z MD, MPH, Eric
Original Article Comparison of the bone plug and bone bridge technique for lateral meniscus allograft transplantation
 Int J Clin Exp Med 2016;9(11):21866-21871 www.ijcem.com /ISSN:1940-5901/IJCEM0037402 Original Article Comparison of the bone plug and bone bridge technique for lateral meniscus allograft transplantation
Int J Clin Exp Med 2016;9(11):21866-21871 www.ijcem.com /ISSN:1940-5901/IJCEM0037402 Original Article Comparison of the bone plug and bone bridge technique for lateral meniscus allograft transplantation
Knee Preservation and Articular Cartilage Restoration
 Knee Preservation and Articular Cartilage Restoration With Special Thanks to Aaron Krych, MD and Riley Willims, MD Zak Knutson, MD Articular Cartilage Layer of tissue covering the bone which are part of
Knee Preservation and Articular Cartilage Restoration With Special Thanks to Aaron Krych, MD and Riley Willims, MD Zak Knutson, MD Articular Cartilage Layer of tissue covering the bone which are part of
evicore MSK joint surgery procedures requiring prior authorization
 evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
evicore MSK joint surgery procedures requiring prior authorization Moda Health Commercial Group and Individual Members* Updated 1/30/2018 *Check EBT to verify member enrollment in evicore program Radiology
Introduction Knee Anatomy and Function Making the Diagnosis
 Introduction Knee injuries are a very common problem among active individuals. It is important for us to understand how your knee was injured. Most knee injuries are associated with non-contact mechanisms.
Introduction Knee injuries are a very common problem among active individuals. It is important for us to understand how your knee was injured. Most knee injuries are associated with non-contact mechanisms.
Cartilage Repair Center Brigham and Women s Hospital Harvard Medical School
 Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Articular Cartilage Surgical Restoration Options
 Articular Cartilage Surgical Restoration Options Randy Schwartzberg, M.D. Assistant Professor - UCF College of Medicine Rationale Our bodies do not make articular/hyaline cartilage. gics injections to
Articular Cartilage Surgical Restoration Options Randy Schwartzberg, M.D. Assistant Professor - UCF College of Medicine Rationale Our bodies do not make articular/hyaline cartilage. gics injections to
Meniscal allograft transplantation: a meta-analysis
 SICOT J 2017, 3, 33 Ó The Authors, published by EDP Sciences, 2017 DOI: 10.1051/sicotj/2017016 Available online at: www.sicot-j.org REVIEW ARTICLE OPEN ACCESS Meniscal allograft transplantation: a meta-analysis
SICOT J 2017, 3, 33 Ó The Authors, published by EDP Sciences, 2017 DOI: 10.1051/sicotj/2017016 Available online at: www.sicot-j.org REVIEW ARTICLE OPEN ACCESS Meniscal allograft transplantation: a meta-analysis
Epidemiology. Meniscal Injury & Repair. Meniscus Anatomy. Meniscus Anatomy
 Epidemiology 60-70/100,000 per year Meniscal Injury & Repair Arthroscopic Mensiscectomy One of the most common orthopaedic procedures 20% of all surgeries at some centers Male:Female ratio - 2-4:1 Younger
Epidemiology 60-70/100,000 per year Meniscal Injury & Repair Arthroscopic Mensiscectomy One of the most common orthopaedic procedures 20% of all surgeries at some centers Male:Female ratio - 2-4:1 Younger
High Tibial Osteotomy
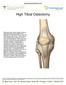 High Tibial Osteotomy With each step, forces equal to three to eight times your body weight travel between the thigh bone (femur) and shin bone (tibia) in your knee. These forces are dampened by a meniscus
High Tibial Osteotomy With each step, forces equal to three to eight times your body weight travel between the thigh bone (femur) and shin bone (tibia) in your knee. These forces are dampened by a meniscus
PRELIMINARY PROGRAM. AOSSM & ISAKOS Surgical Skills Course
 SURGICAL SKILLS AOSSM & ISAKOS Surgical Skills Course Osteotomies Around the Knee: From Ligament Insufficiency to Cartilage/Meniscus Pathologies and Arthritis April 12 13, 2019 OLC Education and Conference
SURGICAL SKILLS AOSSM & ISAKOS Surgical Skills Course Osteotomies Around the Knee: From Ligament Insufficiency to Cartilage/Meniscus Pathologies and Arthritis April 12 13, 2019 OLC Education and Conference
Protocol. Electrical Stimulation of the Spine as an Adjunct to Spinal Fusion Procedures
 Electrical Stimulation of the Spine as an Adjunct to Spinal Fusion (70185) Medical Benefit Effective Date: 07/01/12 Next Review Date: 01/19 Preauthorization Yes Review Dates: 09/07, 09/08, 09/09, 05/10,
Electrical Stimulation of the Spine as an Adjunct to Spinal Fusion (70185) Medical Benefit Effective Date: 07/01/12 Next Review Date: 01/19 Preauthorization Yes Review Dates: 09/07, 09/08, 09/09, 05/10,
Osteo-chondral Transplantation (OATS) The Unhappy ACL. Dr Ivan Popoff Knee, Elbow & Shoulder Surgery
 Osteo-chondral Transplantation (OATS) The Unhappy ACL The Unhappy ACL ACL reconstruction highly successful surgery for restoring stability and return to pre-injury levels of sporting activity? Return to
Osteo-chondral Transplantation (OATS) The Unhappy ACL The Unhappy ACL ACL reconstruction highly successful surgery for restoring stability and return to pre-injury levels of sporting activity? Return to
Cartilage repair update: Indications are being refined and the future is bright
 Cartilage repair update: Indications are being refined and the future is bright ORTHOPEDICS TODAY 2008; 28:46 September 2008 Cartilage is a highly structured tissue with low cellularity and virtually no
Cartilage repair update: Indications are being refined and the future is bright ORTHOPEDICS TODAY 2008; 28:46 September 2008 Cartilage is a highly structured tissue with low cellularity and virtually no
PCL and extra-articular applications. Stability Versatility Recovery
 PCL and extra-articular applications Stability Versatility Recovery The next generation in soft tissue internal fixation The most advanced non-biological soft tissue treatment option, LARS provides a high
PCL and extra-articular applications Stability Versatility Recovery The next generation in soft tissue internal fixation The most advanced non-biological soft tissue treatment option, LARS provides a high
Priorities Forum Statement GUIDANCE
 Priorities Forum Statement Number 21 Subject Knee Arthroscopy including arthroscopic knee washouts Date of decision November 2016 Date refreshed March 2017 Date of review November 2018 Osteoarthritis of
Priorities Forum Statement Number 21 Subject Knee Arthroscopy including arthroscopic knee washouts Date of decision November 2016 Date refreshed March 2017 Date of review November 2018 Osteoarthritis of
Why do they fail?? TOM MINAS MD MS. The Management of Failed Cartilage Repair Procedures PALM BEACH FL
 The Management of Failed Cartilage Repair Procedures Why do they fail?? TOM MINAS MD MS DIRECTOR, CARTILAGE REPAIR CENTER, PALEY ORTHOPEDIC INSTITUTE, PALM BEACH FL PROFESSOR EMERITUS, HARVARD MEDICAL
The Management of Failed Cartilage Repair Procedures Why do they fail?? TOM MINAS MD MS DIRECTOR, CARTILAGE REPAIR CENTER, PALEY ORTHOPEDIC INSTITUTE, PALM BEACH FL PROFESSOR EMERITUS, HARVARD MEDICAL
Osteoarthritis. Dr Anthony Feher. With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides
 Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury
 Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
The Impact of Age on Knee Injury Treatment
 The Impact of Age on Knee Injury Treatment Focus on the Meniscus Dr. Alvin J. Detterline, MD Sports Medicine and Orthopaedic Surgery Towson Orthopaedic Associates University of Maryland St. Joseph Medical
The Impact of Age on Knee Injury Treatment Focus on the Meniscus Dr. Alvin J. Detterline, MD Sports Medicine and Orthopaedic Surgery Towson Orthopaedic Associates University of Maryland St. Joseph Medical
Arthroscopic techniques and instruments for meniscal allograft transplantation using the bone bridge in trough method
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 17: 1351-1359, 2019 Arthroscopic techniques and instruments for meniscal allograft transplantation using the bone bridge in trough method YADONG ZHANG, SHUXUN HOU,
EXPERIMENTAL AND THERAPEUTIC MEDICINE 17: 1351-1359, 2019 Arthroscopic techniques and instruments for meniscal allograft transplantation using the bone bridge in trough method YADONG ZHANG, SHUXUN HOU,
Impact of surgical timing on the clinical outcomes of anatomic double-bundle anterior cruciate ligament reconstruction
 ISAKOS 2019 12 th -16 th May Cancun, Mexico Impact of surgical timing on the clinical outcomes of anatomic double-bundle anterior cruciate ligament reconstruction Baba R. 1, Kondo E. 2, Iwasaki K. 1, Joutoku
ISAKOS 2019 12 th -16 th May Cancun, Mexico Impact of surgical timing on the clinical outcomes of anatomic double-bundle anterior cruciate ligament reconstruction Baba R. 1, Kondo E. 2, Iwasaki K. 1, Joutoku
Japan Journal of Medicine 2018; 1(3): doi: /jjm
 Jpn J Med 2018,1:3 175 Japan Journal of Medicine 2018; 1(3): 175 182. doi: 10.31488/jjm.1000114 Mini Review Meniscal allograft transplantation, still unaccepted treatment option in Japan? review Yuji Uchio*
Jpn J Med 2018,1:3 175 Japan Journal of Medicine 2018; 1(3): 175 182. doi: 10.31488/jjm.1000114 Mini Review Meniscal allograft transplantation, still unaccepted treatment option in Japan? review Yuji Uchio*
Populations Interventions Comparators Outcomes Individuals: With heart transplant
 Protocol Laboratory Tests for Heart Transplant Rejection (20168) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/18 Preauthorization No Review Dates: 05/13, 05/14, 05/15, 05/16, 05/17 This
Protocol Laboratory Tests for Heart Transplant Rejection (20168) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/18 Preauthorization No Review Dates: 05/13, 05/14, 05/15, 05/16, 05/17 This
Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions
 Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions Policy Number: 7.01.78 Last Review: 2/2018 Origination: 8/2002 Next Review: 2/2019 Policy Blue Cross and Blue Shield of Kansas
Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions Policy Number: 7.01.78 Last Review: 2/2018 Origination: 8/2002 Next Review: 2/2019 Policy Blue Cross and Blue Shield of Kansas
Corporate Medical Policy
 Corporate Medical Policy Continuous Passive Motion in the Home Setting File Name: Origination: Last CAP Review: Next CAP Review: Last Review: continuous_passive_motion_in_the_home_setting 9/1993 6/2018
Corporate Medical Policy Continuous Passive Motion in the Home Setting File Name: Origination: Last CAP Review: Next CAP Review: Last Review: continuous_passive_motion_in_the_home_setting 9/1993 6/2018
Options in the Young ACL Deficient Knee
 BOSTON SHOULDER AND SPORTS SYMPOSIUM 2013 Thomas M. DeBerardino, MD Disclosure Information Disclosure Information: The following relationships exist: Research Support from: 1. Musculoskeletal Transplant
BOSTON SHOULDER AND SPORTS SYMPOSIUM 2013 Thomas M. DeBerardino, MD Disclosure Information Disclosure Information: The following relationships exist: Research Support from: 1. Musculoskeletal Transplant
The goals of treatment for patients with symptomatic
 REVIEW ARTICLE Managing the Patient With Failed Cartilage Restoration Jaskarndip Chahal, MD, FRCSC,* Geoffrey V. Thiel, MD, MBA,w Kristen Hussey, BSc,w and Brian J. Cole, MD, MBAw Abstract: In comparison
REVIEW ARTICLE Managing the Patient With Failed Cartilage Restoration Jaskarndip Chahal, MD, FRCSC,* Geoffrey V. Thiel, MD, MBA,w Kristen Hussey, BSc,w and Brian J. Cole, MD, MBAw Abstract: In comparison
Osteochondral Allograft Transplantation and Autograft Transfer System (OATS/mosaicplasty) in the Treatment of Articular
 Osteochondral Allograft Transplantation and Autograft Transfer System (OATS/mosaicplasty) in the Treatment of Articular Cartilage Lesions Corporate Medical Policy File name: Osteochondral Allograft Transplantation
Osteochondral Allograft Transplantation and Autograft Transfer System (OATS/mosaicplasty) in the Treatment of Articular Cartilage Lesions Corporate Medical Policy File name: Osteochondral Allograft Transplantation
09/24/2015. AGH Nuts and Bolts of Orthopedics Conference 2015 Chad J. Micucci, M.D. Disclosures NONE
 AGH Nuts and Bolts of Orthopedics Conference 2015 Chad J. Micucci, M.D. Disclosures NONE 1 ACL Reconstruction Approximately 400,000 ACL reconstructions are completed in the U.S. Over 20% of ACL reconstructions
AGH Nuts and Bolts of Orthopedics Conference 2015 Chad J. Micucci, M.D. Disclosures NONE 1 ACL Reconstruction Approximately 400,000 ACL reconstructions are completed in the U.S. Over 20% of ACL reconstructions
ORTHOPEDICS BONE Recalcitrant nonunions In total hip replacement total knee surgery increased callus volume
 ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
Populations Interventions Comparators Outcomes Individuals: With intestinal failure and evidence of impending end-stage liver failure
 Protocol Small Bowel/Liver and Multivisceral Transplant (70305) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/18 Preauthorization Yes Review Dates: 05/09, 05/10, 05/11, 05/12, 05/13, 07/13,
Protocol Small Bowel/Liver and Multivisceral Transplant (70305) Medical Benefit Effective Date: 07/01/14 Next Review Date: 05/18 Preauthorization Yes Review Dates: 05/09, 05/10, 05/11, 05/12, 05/13, 07/13,
Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of the Tibia
 Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Meniscal Scaffolds in the Clinics: Present and Future Trends
 Guest Editorial Asian Journal of Arthroscopy 2016 Aug-Nov ;1(2): 47-52 Meniscal Scaffolds in the Clinics: Present and Future Trends Ricardo Bastos¹ ² ³, Renato Andrade² ³ ⁴, Hélder Pereira⁵ ⁶ ⁷ ⁸, J. Miguel
Guest Editorial Asian Journal of Arthroscopy 2016 Aug-Nov ;1(2): 47-52 Meniscal Scaffolds in the Clinics: Present and Future Trends Ricardo Bastos¹ ² ³, Renato Andrade² ³ ⁴, Hélder Pereira⁵ ⁶ ⁷ ⁸, J. Miguel
