Parents Guide. Clubfoot. and its treatment using the Ponseti Method
|
|
|
- Kathleen Merritt
- 5 years ago
- Views:
Transcription
1 A Parents Guide to Clubfoot and its treatment using the Ponseti Method
2 Table of Contents Dedication and Introduction...2 About Dr. Ignacio Ponseti and his Method...3 Understanding Clubfoot...4 Clubfoot Treatment Overview...6 Clubfoot Treatment Timeline...8 Your Health Care Team...9 Your First Appointment...10 Straightening the Foot: Casting...11 When to Seek Medical Attention...13 Preventing Relapse: Bracing and Surveillance...16 Exercise and Physiotherapy...21 Parent Stories...22 Frequently Asked Questions...24 Famous People With Clubfeet...25 Resources...26 Glossary of Terms...27 Contributors...28 Your Baby s Milestones...29
3 Dedication by the Parent Authors: To all the parents of children with clubfoot; To all the previous, current and future kids with clubfoot; To their personal journeys and the success of their treatment; Walk tall! Introduction This booklet is intended for parents of children born with clubfoot to be treated using the Ponseti Method of correction. Whether your child is already born, or on the way and an ultrasound suggests a high likelihood of clubfoot or feet, this booklet will help you learn: About clubfeet, About the Ponseti Method of correction of clubfeet, About the important role of the parents in the correction process, What to expect from and how to prepare for treatment, and What to plan, prepare, and know that will help you and your child throughout the years of your child s treatment. There are many different treatments for clubfeet. With the Ponseti Method, fewer surgeries are performed and your child s feet will look and function better than ever before. In almost all cases, the Ponseti Method gives supple, strong, painless feet well into middle age. The idea for this booklet came from mothers Jillian Chateauneuf and Heather Cohen who each have children, Claire and Hayden respectively, born with clubfeet. Hayden and Claire are growing up normally after their clubfeet were treated without surgery by the Ponseti Method. Jillian and Heather felt a strong need for more parent-friendly material about the Ponseti treatment for clubfeet, which prompted them to spearhead an effort to ensure that parents in the future would benefit from their journey. This booklet was written by parents and for parents, with technical advice from the Clubfoot Team at the Royal Columbian Hospital and the Medical & Scientific Review Committee of the Canadian Orthopaedic Foundation. The Canadian Orthopaedic Foundation encourages you to learn all you can about clubfeet. This booklet will answer many of your questions, but it is equally important to discuss your expectations and concerns with your doctor and other health professionals involved in your child s care. An experienced and highly trained team of health care professionals is focused on correcting your child s foot or feet, and making the journey as smooth as possible for you and your child. Be an active participant in your child s care. 2
4 About Dr. Ponseti and his Method Dr. Ignacio Ponseti Dr. Ignacio Ponseti, Professor of Orthopaedics at the University of Iowa, pioneered his method in the 1940 s after extensive research into the long-term after-effects of surgery for clubfeet. He found that those who had surgery for clubfeet often experienced stiffness, pain, and limited function in their feet as adults. In many cases, further surgery was required. By studying the anatomy and function of the human foot, he discovered why earlier methods had been unsuccessful and started manipulating newborn clubfeet differently. In his career, he treated over 3,000 children with clubfeet and received testimonials and follow-ups from patients well into middle age with functional, pain-free feet. Photo courtesy of University of Iowa, Department of Orthopaedics and Rehabilitation Parents of infants born with clubfeet may be reassured that their baby, if otherwise normal, when treated by expert hands will have normal looking feet with normal function for all practical purposes. The well-treated clubfoot is no handicap and is fully compatible with a normal, active life. Dr. Ignacio Ponseti Initially Iowa City was the only place the Ponseti Method was available. In 1996 Dr. Ponseti published a book on his non-operative method, which helped doctors to better understand the techniques. This helped doctors around the world to learn, and then use, the method. Prior to his death in October 2009, Dr. Ponseti favourably reviewed this booklet. Dr. Shafique Pirani, an orthopaedic surgeon specially trained in the bone and joint problems of children and who was consulted extensively in the development of this booklet, runs the Clubfoot Clinic at the Royal Columbian Hospital. 3 I read Dr. Ponseti s book on his non-operative method for correcting clubfeet in disbelief, but when I tried his manipulative technique I was amazed at the corrections achieved. Dr. Ponseti developed his method after much careful observation and critical thinking based on an accurate knowledge of foot anatomy and biology of growing bones. I adopted the technique in 1998 and am delighted with the results. In almost every case, the deformity corrects with about five casts. Feet corrected without surgery are more supple and stronger than feet corrected with surgery. Dr. Shafique Pirani
5 Understanding Clubfoot What is clubfoot? Congenital clubfoot, or talipes equinovarus, is a complex deformity that is readily apparent at birth and affects the muscles, ligaments, bones and joints of the developing foot and ankle. The ankle is rotated downward and the toes point inward towards the opposite leg. All foot bones are usually present, but are out of normal alignment. All of the foot and leg muscles are also present, but some are smaller and weaker than normal. Tendons and ligaments are contracted, especially behind the ankle and along the instep. Why my baby? Many parents ask this question. It helps to understand that clubfoot is among the most common of birth defects. Worldwide, more than one baby in a thousand is born with this foot deformity. That may not sound like a lot, but it is: every year more than 100,000 babies worldwide are born with a clubfoot or clubfeet. Fifty percent of cases affect one foot, and fifty percent affect both feet. Boys are more commonly affected than girls. Sometimes clubfoot runs in families. It also helps to understand that clubfoot responds well to treatment. When treated by medical experts, children born with clubfeet and no other significant medical problems will have feet that are capable of a normal, active life. What causes clubfoot? There are many theories, however the actual cause is not known. There is no need for parents to feel at fault. Does this mean my baby has other problems? Your doctor will check your baby thoroughly directly after birth. Most often, clubfoot is an isolated condition from an unknown cause (idiopathic clubfoot). Rarely, there are other conditions that are also noted such as spina bifida (syndromic clubfoot). Occasionally the foot may have been held in a curved position in a crowded uterus (positional clubfoot); for example, if there are twins. Positional clubfoot is much quicker to correct than idiopathic or syndromic clubfoot. Your doctor will tell you what type of clubfoot your baby has. When should treatment begin? Babies suspected of having clubfoot at the newborn exam are usually referred right away to the orthopaedic team or clubfoot clinic. Infants are seen within a few weeks and treatment begins. How severe is my baby s clubfoot? All clubfeet are not of the same severity, although all have the same general appearance. Some doctors measure or score the amount of deformity present (see chart page 29). Scoring can assist the doctor to determine the severity of the clubfoot and to measure the progress of correction. 4
6 Understanding Clubfoot How is clubfoot treated with the Ponseti Method? Clubfoot treatment using the Ponseti Method can be considered in three phases (see Treatment Timeline page 8): 1. Correction. The Ponseti method uses very specific and gentle manipulations to align the foot in a more normal position, and casting to allow the soft bones to set. Usually, about five weekly casts and a minor procedure to the Achilles tendon (tenotomy) are all that is needed to achieve full correction. Difficult clubfeet sometimes need more casts. 2. Prevention of Relapse. After correction, a brace is then necessary to prevent relapse. The brace is worn full time for two to three months, and then during nighttime and naps until the child reaches at least four years of age. 3. Surveillance. Your child will have regular visits until fully grown to monitor how the legs and feet are growing. Keep in mind that all children are different and length of treatment may vary. What is relapse and how is it treated? Clubfeet have a stubborn tendency to relapse, or come back, after casting correction. Relapses are treated the same way, through manipulation and casts, although casts are applied less frequently and typically correct within fewer castings. Rarely a clubfoot may be resistant. In such a case, your orthopaedic surgeon may recommend surgery, such as a tendon transfer, which would be explained by your surgeon at that time. This booklet addresses non-surgical correction. What happens if clubfoot is not treated? Left untreated, the deformity persists and results in severe physical and emotional handicap. Will this process be painful for my baby? There may be some discomfort for your baby as he or she adjusts to the treatment, but the process is likely to be more painful for you as a caring parent than it is for your baby. This booklet explains the process and your important role in it to make correction easiest on both of you. How will my child do as a grown-up? Children with clubfeet corrected by the Ponseti Method grow up to have feet that are almost normal in shape and function. For children with one clubfoot, the corrected foot and calf may be slightly smaller. Children with corrected clubfeet grow normally and are able to participate in most sports or leisure activities. Studies in adults show that patients treated using the Ponseti Method continue to have as strong and as healthy feet as adults born with normal feet. 5
7 Clubfoot Treatment Overview The early stages of treatment are part of an intensive process that involves commitment by both the family and the health care team to achieve and maintain optimal results. This section provides an overview of the correction process, with more detail and specifics about care and your role, beginning on page 10. Straightening the Foot Ideally, treatment begins during the first few weeks of life to take advantage of the favorable elasticity, or suppleness, of the tissues at that age. At each weekly visit, your baby s foot will be gently manipulated to stretch the short, tight ligaments and tendons of the ankle and foot. The foot is then held in progressively corrected positions by a cast that extends from toes to groin. The cast holds the correction obtained by the manipulation. The time in the cast relaxes the tissues for the next weekly manipulation. Gradually, the displaced bones and joints are brought into correct alignment. Weekly casts showing change in foot shape as correction progresses: Casting corrects all the parts of the clubfoot except equinus, the downward pointing of the ankle. Equinus is corrected with the release of the Achilles tendon (called an Achilles tenotomy), and application of the last cast. 6
8 Clubfoot Treatment Overview Achilles Tenotomy In a clubfoot, the Achilles tendon is particularly thick and stiff making it resistant to stretching. To achieve good ankle motion, a minor procedure called an Achilles tenotomy is usually necessary to release the Achilles tendon and complete the correction. The tenotomy is a safe, short procedure for your baby, and is usually performed in the outpatient clinic under a local anaesthetic. The tenotomy creates a gap in the tendon, which then heals, resulting in a longer tendon with greater flexibility. The skin incision is very small and no stitches are needed. The ankle and foot are then casted for about three weeks in the fully corrected position. Bracing Clubfeet have a stubborn tendency to relapse, or come back, after casting correction. To prevent relapse, your doctor will prescribe a brace to hold the foot or feet in the corrected position after removal of the last cast. The brace is worn 23 hours per day for two to three months, allowing an hour for brace-free bathing and cuddling, and then during nighttime and naps until the child is approximately four years old. Sometimes the duration of brace wear will vary (up to six years of age) depending on the severity of the clubfoot and its tendency to relapse. This will be determined by your doctor as your child grows. The brace, called a foot abduction brace because it abducts or rotates the foot or feet outward, looks like two shoes connected by a bar. This simple design is effective in holding the feet in the corrected position. Normal shoes are fine for the child to wear when not wearing the brace. The foot abduction brace is the only brace that prevents relapse and is over 90% effective, if used as prescribed. Wearing the brace will not significantly delay your child s development with regard to sitting, crawling, or walking. However, NOT wearing the brace will significantly compromise the correction of the clubfoot or feet. 7 Follow Up and Supplemental Treatment As your child grows, you may notice and be concerned about a slight difference in leg length and foot size. Have your child s foot or feet checked regularly by your health care team to watch for relapse, and to detect and manage slight differences. Follow up is rarely needed after the bones stop growing at around age fourteen for girls and age sixteen for boys. Your doctor will advise you about the follow up schedule. Sometimes surgery is recommended if leg-length differences become bothersome or painful. Some doctors supplement treatment with physiotherapy. Appropriate exercises may be useful additions in preventing relapse, particularly if muscle imbalance within the foot is a problem. If you need help with an exercise program, a physiotherapist with paediatric experience can help gear exercises towards the age and interests of the child. Once correction is complete, foot orthotics, supporting devices or insoles to control joint motion, may be useful to help balance the forces that go through a corrected clubfoot and to make up for slight differences in foot size or leg length that may appear as the child grows. Orthotics and braces need to fit correctly, like shoes, and will need changing at regular intervals depending on how fast the feet are growing. The cost of orthotics and braces are covered by most extended health care benefit plans.
9 Clubfoot Treatment Timeline Straightening the Foot: About 2 months Full-Time Bracing: About 3 months Prevention of Relapse: Part-Time Bracing: About 4 years Surveillance: Until fully grown Casts applied at weekly intervals are all that is needed to correct clubfeet. Difficult clubfeet may need more casts. Usually a tenotomy is performed before the last cast is applied. The last cast stays on for 3 weeks. The brace is fitted the day the last cast is taken off. It is worn 23 hours a day for 2 to 3 months. After 2 to 3 months, bracing time is reduced to nighttime and naps only, usually until about 4 years of age. Clinic visits are every 3 to 6 months until approximately 4 to 5 years of age, to watch for relapse and change braces as your child outgrows them. Clinic visits every 6 to 12 months to check how the feet and legs are growing. Visits continue until the child is fully grown, about age 14 for girls and age 16 for boys REMEMBER: Each child s progress is unique. These are guidelines only. Treatment length may vary. 8
10 Your Health Care Team There are many health care professionals that play a role in your child s bone and joint health. The members of the team may vary, depending on your child s situation and needs. You have an important role to play, too. Be involved in the process ask questions, voice concerns, and ask for information about your baby s diagnosis, treatment alternatives and the course of care. Here are some of the health care professionals that you will likely meet during your child s treatment: Orthopaedic Surgeon An orthopaedic surgeon is trained to diagnose and treat a wide variety of musculoskeletal conditions and injuries. Paediatric orthopaedists are specially trained on the unique problems and needs of children. Orthopaedic Surgery Fellow or Resident Fellows are fully trained orthopaedic surgeons who are continuing training so that they can specialize in a specific area of orthopaedic care; for example paediatric orthopaedics. A resident is a licensed physician receiving training in a specialty, such as orthopaedics. Physiotherapist Physiotherapists are health care professionals trained to assess, treat and prevent disease, injury or conditions that affect the structure and/or movement of the human body through treatment, exercise and education. Orthopaedic Technologist or Cast Technician Orthopaedic technologists assist orthopaedic surgeons with the treatment of orthopaedic injuries and diseases by applying, adjusting, and removing a variety of casts, splints, bandages, and ambulatory aids. They may provide you with information and instructions regarding treatment. Clinic Nurse A clinic nurse is a registered nurse with a high degree of knowledge, skill and competence in a specialized area of nursing. Certified Orthotist Certified orthotists are health care professionals who assess, design, fabricate, and fit braces known as orthoses. The orthotist will help you to troubleshoot if your baby s feet are coming out of the brace or if your baby is experiencing any discomfort with the brace. The orthotist can make adjustments to the brace and educate you on how to apply it properly. 9 Medical Students Medical students are doctors-in-training and participate under supervision in most hospital clinics.
11 Your First Appointment Babies with clubfoot will be referred to an orthopaedic surgeon or clinic by their family doctor, delivering doctor, obstetrician, or the hospital paediatrician. At some hospitals, you will be contacted by the orthopaedic clinic to arrange your first visit. At your first visit, you will meet the orthopaedic surgeon and other professionals who will be part of your child s health care team. Your baby will be examined. Your orthopaedic surgeon will then discuss the findings with you and recommend a treatment plan. Often, the first casting treatment begins at this visit, so be sure to bathe your baby before the appointment. Your baby s cast will fit easily into car seats and strollers, so there is no special equipment to purchase. Your first appointment can be a stressful time for parents. Your baby is very young, so you are likely to be anxious, tired or emotional. This is all natural. To minimize stress and make the most of your appointment: Allow plenty of time to get to your appointment. Bring diapers and any other needs for your baby in case a change is needed. Bring a full bottle for feeding (if your baby is not breast-fed). Dress your baby in a loose-fitting sleeper or pants that snap all the way open to fit easily over a cast. Write down your questions so you don t forget them. Bring a pen and something to write instructions on this booklet or a notepad. Be patient the office or clinic may be busy. You may find it helpful to pay for additional parking time, if pre-payment is required at the clinic or hospital, so you don t feel rushed. Try not to have plans for later that day. Most importantly, take the time to discuss your concerns and expectations with your health care team. They are there to help you! Questions for the first appointment: 10
12 Straightening the Foot: Casting Casting You and your baby will visit your health care team initially to have the first cast applied, and then weekly to have the old cast removed and a new one applied. The success of Ponseti correction lies in the gentleness of manipulation and casting. It should not be uncomfortable for the baby, stressful for the parents, or rushed for the tending health care professionals. For these weekly visits, it can help to keep your baby a little hungry with bottles ready. Feeding babies are relaxed babies, and many surgeons are quite happy to have mothers feed by bottle or breast while the casts are being put on. Applying casts often requires two team members, one to manipulate and hold the limb in position and one to apply the cast. Although infants may fuss during the casting process, rest assured that the cast applications are not painful. Types of Casts There are many types of casting materials available: plaster of Paris, rigid fibreglass, semi-rigid fibreglass. Your doctor will determine what material will work best for your child. Cast Application Once the baby is made comfortable, the leg and foot are gently manipulated into position. A sock or soft padding to line the cast will be applied before or after manipulation. Some clinics apply the full cast at once. In others, the cast is applied in two stages: first the portion below the knee is applied and molded, and then the cast is extended to the upper thigh, with the knee in a relaxed flexed position. This long leg cast is essential for maintaining the foot in position. Casts usually dry in a few minutes. Once casting is complete, you are asked to wait 5 to 10 minutes to make sure your child is comfortable and their toes are pink, indicating good circulation. Your health care team will make sure that there are no problems prior to your baby going home. Tenotomy Before the last cast is applied, a small cut just above the heel releases a tight Achilles tendon. Your surgeon will decide if this is needed. This procedure, called a tenotomy, completes the correction of the clubfoot. 11 Most surgeons prefer to perform the tenotomy in the clinic treatment room using a local anaesthetic. No stitches are needed as the skin incision is only a few millimeters long. A bandage or small dressing is all that is needed to cover the incision, then the last cast is applied. Once the cast is dry, you may take your baby home after a team member has checked that all is well. A cast after a tenotomy stays on for about three weeks.
13 Straightening the Foot: Casting Some infants may be upset by the procedure, but will settle easily once the cast has set. Your doctor may suggest mild infant pain medicine for the first day. After the first day there usually is no discomfort. If your baby continues to cry, develops a fever, or you have concerns about the cast, contact your doctor immediately (see When to Seek Medical Attention ). Cast Care You will be guided in cast and skin care at each appointment. It is most important to remember that the cast is not waterproof and to keep it clean and dry at all times for your baby s comfort and to prevent skin irritations. The following reminders are general cast care instructions; your health care professional may have others be sure to take careful note of them: Keep cast clean and dry. Moisture under a cast can cause minor to severe skin conditions such as a rash or skin breakdown. Be extra careful with diapers. Changing them frequently helps prevent awkward leaks! The most difficult area is around the thigh-diaper region. Use disposable diapers with extra leak guards, or plastic covers that are snug around the leg for cloth diapering, to keep casts clean and dry. Never insert anything under the cast as skin may be damaged. Items such as knitting needles and rulers that are inserted into the cast can cause sores or scratches, which can lead to infection. Monitor your baby so that you become accustomed to watching for changes that may indicate a problem with the cast: these include skin colour and condition, an odour coming from the cast, or if your baby is fussier than normal. If you suspect that the inner lining of the cast is wet, it may need to be removed and replaced immediately. If this happens, immediately pat the cast as dry as you can without inserting anything underneath it. Leave your baby unclothed from the waist down except for the diaper, and call your doctor. When Everything Is Well A comfortable baby, adjusting well to the cast: Will move his or her legs without discomfort Will have normally-coloured, rash-free skin around and near the cast Will have normally-coloured toes that are not swollen May fuss a bit, but will be consolable See next page for When to Seek Medical Attention. 12
14 Straightening the Foot: Casting When to Seek Medical Attention Seek medical attention if: Your baby s toes are swollen or not normal in colour (are blue, black, white or red) The cast is wet with urine or other fluid Your baby s skin shows a red rash on the legs, or abnormal colour or condition You notice an odour coming from the cast Your baby is crying inconsolably During regular office hours: Contact the Cast Clinic where the cast was applied, or your doctor s office Expect a response within an hour or two If no response is forthcoming, take your baby to the emergency room Outside of regular office hours: Take your baby to the emergency room Emergency Contact Numbers: Cast Clinic Phone Number: Doctor s Office Phone Number: 13
15 Straightening the Foot: Casting At Home with the First Cast At first, your baby may be restless, but will settle after the first night. If you feel your baby is in pain, you may give him or her an infant pain reliever if approved by your doctor. If your baby does not settle, or the medicine does not calm your child, call your doctor. Dressing Baby Your baby s cast will fit under most baby pants and sleepers, so long as they are not tight fitting. Those with snap buttons that open right up, rather than having to be pulled off over the legs, are most easy to deal with. Stretchy pants with loose fitting legs and an elastic waistband also work well. Sleepers with toes will sometimes fit over the cast, or you can cut off part of the sleeper leg(s) and put a sock or soft bootie on your child to keep the foot or feet warm. Bathing Baby While your baby is wearing a cast, he or she will need to be sponge-bathed, as the cast is not waterproof and cannot become wet. You can place your baby in the tub or sink and have a bowl of warm water close by. Dip your cloth/sponge in the warm water, wring out excess water, and wash your baby. You may also find a sponge bath at the edge of the tub works well. Wearing shorts yourself, sit on the edge of the tub with your feet inside and your baby in your lap with a towel over the cast(s). This allows you to run the water at a trickle, while you wash your baby s hair, face and upper body. You can then clean the lower body with a washcloth later on. Parents have found that bathing this way is much faster and less stressful to one s back than bending over your baby or the sink, particularly as babies get heavier! Cast Removal At your next appointment, and at every subsequent casting appointment, the old cast will be removed. Usually casts are removed in the clinic. If semi-rigid fibreglass is used, no equipment is needed. The cast will simply be unwrapped similar to a roll of duct tape. 14
16 Straightening the Foot: Casting If plaster of Paris is used, it usually needs to be soaked prior to unraveling the material. Some clinics may have you soak your baby s cast at home, and will provide you with specific instructions. Others soak the cast at the clinic. Usually a bath or sink will be filled with warm water and the cast completely submersed under water. Then a wet towel is wrapped around the cast and leg to soak for minutes. The technician will likely have left a small bump of material on the cast. When this bump can be easily separated from the cast, the plaster is soft enough to unwrap. Rigid fibreglass casts are usually used for older children to treat a relapsed clubfoot. They are strong and must be cut on both sides with a cast saw for removal. Though the cast saw is loud and seems frightening, it is actually a very clever and safe machine. The cast saw uses round blades that do not spin or cut like a conventional saw; instead, the blades vibrate at high speed and therefore do not harm skin. A vacuum system minimizes any cast dust on or near your child. Ear protectors may be available if your child wishes to wear them. When the saw is in use, your child will feel a vibration, which most say feels like a tickle. Once the sides are split a spreader device is used to open the cast. Scissors are used to cut the cotton sock and padding completely, and the cast is then removed. At each weekly visit, the old cast will be removed, and a new one applied until this stage of correction is complete. You and your baby will get used to the cast and the appointments, becoming more comfortable with the procedures each time. Remember to check the tips in Your First Appointment to keep your weekly appointments as stress-free as you can. A special note for older children: An older child who has been immobilized in a cast for several weeks (to treat relapse) may experience some stiffness in the joints after the cast is removed. It s a good idea to prepare your child by mentioning this to him or her, and provide reassurance that it is normal. Additional instructions: 15
17 Preventing Relapse: Bracing and Surveillance After the last cast is removed, your baby graduates to wearing a brace. This is a new step for you and your baby, so use the checklist under Your First Appointment, and: Dress your baby in a sleeper or pants that open all the way on both sides so you don t have to remove the brace to change a diaper. Review the section The First Night In the Brace on page 19 for what you might expect or wish to prepare as your baby adjusts to the brace. About bracing Even after full correction, clubfeet have a stubborn tendency to recur or relapse. The tendency is much less after about age four. The best way to prevent recurrence is to use a special foot abduction brace consistently for 23 hours a day for two to three months, and then during nighttime and naps until four years of age. The duration of brace wear will vary depending on the severity of clubfoot and will be determined by your physician. You will follow up with your orthotist regularly as your child grows out of his or her boots or as they need adjustment. The foot abduction brace is the only successful method of preventing a relapse and is effective in 90 percent of patients when used consistently as described above. Use of the brace will not significantly delay your child s development with regard to sitting, crawling, or walking. What is a foot abduction brace? A foot abduction brace (FAB) is a brace specifically designed to abduct the foot and dorsiflex the ankle (toes pointing upward) to maintain treated clubfeet in a fully corrected position. It consists of two boots connected by a bar that holds the feet in the same corrected position as the last cast. There are different types available. Commonly used braces include the Markell, the Ponseti AFO, (also known as the Mitchell Brace), the ALFA-Flex, and the Horton Click (a bar to which a variety of shoes can be attached). Each type has unique characteristics. Your doctor will prescribe the brace best suited for your child. When is the brace applied for the first time? The best time to apply the brace is the day the last cast comes off, because the foot is used to being in the fully corrected position. Applying the brace immediately after the cast comes off lessens the risk of relapse. How is the brace set up? The FAB will be set up by your orthotist. As your child grows, larger shoes and longer bars will be supplied by the orthotist. It helps to be knowledgeable about some of the adjustments. Bar length: Your child s shoulders should fit in the distance between the inside heels of the boots. 16
18 Preventing Relapse: Bracing and Surveillance Foot abduction: Each brace has a slightly different recommended angle (ALFA-Flex: 70 degrees for the clubfoot and 40 degrees for the unaffected foot, Ponseti AFO: 60 degrees for the clubfoot and 40 degrees for the unaffected foot, Markell: 70 degrees for the clubfoot and 45 degrees for the unaffected foot). Your orthotist or surgeon will guide you on what is best for your child. Dorsiflexion: Usually 10 degrees of dorsiflexion is sufficient. The Ponseti AFO has this built in. The ALFA-Flex has an adjustable ball joint, and the Markell bar can either be bent or substituted for a Horton Click bar, which has foot plates with built in dorsiflexion of 10 degrees. How do I put the brace on my child? Tips in this section will help you learn how to use the brace. Your hospital, clinic, surgeon, and orthotist may have other tips be sure to make note of them. It is best to put the boots on when your child is relaxed and calm. You will find out through trial and error what works best for you and your child, but always ensure that the child s heels are all the way down to the bottom of the heel cup in the boots. Initially, you may find it easier to put the shoes on your child separate from the bar, and then reattach the shoes to the bar. You may want to mark the shoes and bar with right and left to ensure the marks on the bar correspond to the correct footplate. The pictures show the Markell shoe as an example. Other shoes work in a similar fashion. 17 Open the shoe up as much as possible by loosening the strap(s) and/or removing the laces. Insert the foot into the shoe with the knee bent to 90 degrees and the ankle flexed so that the toes point upwards. Make sure the heel is completely down and back in the shoe. There should be a hole in the heel of the shoe to allow you to check foot position. With the knees still bent and the toes pointing up, use your thumb to apply pressure to the tongue and strap while tightening the buckle, and if applicable, the laces. Follow the same procedure, one foot at a time, starting with the clubfoot, or weaker of the two. Try to pull the shoe off. If the heel rises, it is not tight enough. Re-tighten the shoe using the above technique until the foot is secure in the shoe. It must be snug, probably tighter than you think it should be, yet without cutting off circulation. You will be surprised at what your child can tolerate. Make sure your baby s toes are not curled under, and that wrinkles are smoothed out of the socks. To smooth wrinkles, pull the socks from the top and toe when the boot is on.
19 Preventing Relapse: Bracing and Surveillance To check circulation, cut the toe area out of a pair of socks. Press on the child s toe nail the nail will whiten then remove pressure to confirm that colour returns quickly to the toe. Once the shoes are snug on both feet and laced or strapped up, the bar is attached, making sure the shoes are set at the right degree of abduction (outward turn), and well-fastened. About the Ponseti AFO: The patented system features a soft rubber lining and soft leather straps for the comfort of the child. The location of the heel can easily be seen through two holes in the back of the AFO and the footwear attaches to the Ponseti Bar by means of a Quick Clip system which allows for easy changing and application of the shoes and brace. The bar can be clipped onto the shoes after they are applied. This is also useful when placing the child in a high chair or shopping cart. These unique features were designed with the child s comfort in mind and may increase compliance to the prescribed bracing schedule. A Pressure Saddle ( pringle ) can be ordered to improve the pressure distribution over the middle strap. The Ponseti AFO can be ordered with a Plantar Flexion Stop, which is useful for atypical clubfoot with neutral or negative dorsiflexion. The Ponseti AFO is also available in the Toe Stilt style which adds a wedge to the toe of the AFO to help the patient maintain good dorsiflexion by stretching the Achilles tendon and increasing flexibility. If your child is escaping from the Ponseti AFO, try tightening the middle strap by one buckle hole, then check to see that the baby s heel is down. The Ponseti AFO Brace and additional products can be ordered by visiting or calling PONSETI ( ) About Markell boots and bars: The boots are straight-last boots. The tongue can be adjusted to ensure the strap is keeping the foot well seated in the shoe. When the child s heel is well-positioned in the shoe, the foot is not able to slip up and blisters will not form. If your child is escaping from the boots: Tighten the strap by one buckle hole and check that baby s heel is down. Tighten the laces and check that baby s heel is down. Remove the tongue of the shoe, or make the tongue-keeper slit longer by cutting it higher up to the top of the tongue, but do not cut the stitching. Lace the shoe from top to bottom so the bow is by the toes. About the ALFA-Flex brace: This brace has soft leather sandals lined with memory foam and practical Velcro or buckle fasteners in colourful designs: Ball joints are moveable in two directions within therapeutic range. A secure click-system fastens braces and shoes together. Brace-length is adjustable allowing a single brace to be used for the duration of treatment. 18 About the Horton Click and 10 degree Kicker: This is an adjustable length bar that attaches to Markell boots by a quick release mechanism that incorporates 10 degrees of dorsiflexion.
20 Preventing Relapse: Bracing and Surveillance Encouragement and Inspiration The Canadian Orthopaedic Foundation offers Ortho Connect, a peer support program through which parents can talk to other parents who have been there, for a real-world view of what to expect. Visit or call for more information. The First Night in the Brace It s hard. Babies cry, and parents worry (Are the feet being damaged by the brace?) Some helpful tips: Providing the brace is fitted well, crying only indicates frustration at not being able to move their legs independently because of the brace. Once babies get used to wearing the brace, they become much more comfortable. Babies get used to the brace, usually after the first night or two, and a normal routine is established. If your baby is crying and you are worried that the brace may be damaging the feet, remove the brace. Rarely, the brace irritates the skin, particularly if it is improperly applied. Babies will then cry inconsolably. Check for signs of skin irritation, such as unusual redness, swelling, bruises, blisters, and sores. If you see these, do not reapply the brace and seek your doctor s advice. Brace adjustments may be needed. If the skin looks okay, reapply the brace right away. This will prevent your baby from learning that crying will result in parents removing the brace. Red Marks on Baby s Foot or Feet Correctly worn, the brace must be quite tight on your child, especially across the middle of the foot. You may notice red marks in this area, which is common. During the hour out of full-time wear you will notice these marks fade. Do not put lotion on these marks as the skin can break down (become macerated). Blistering on the heels can be a sign that the shoe was not worn tightly enough. The heel must stay down in the shoe. If you notice blistering, or signs of an infection, your doctor and/or orthotist should be notified so that this can be corrected as soon as possible. These issues need to be addressed right away to ensure your child s comfort. Baby s Comfort and Movement at Night Your baby may occasionally whine or cry when he or she wishes to turn over. Amazingly, they do figure out how to do it, so you won t lose sleep forever! Blankets may slip off during the night; if this is a concern, you might try a sleeping bag or sleep sack. These work well in the winter months, allowing babies to turn with their covers, or you can try dressing them in a warm, thick sleeper. These also muffle the sound of them hitting the brace against the sides of the crib as they turn over. The First Few Days Your child may fuss in the brace the first few days. This is not because the brace is painful, but because it is new and different. If your baby keeps crying, remove and reapply the brace. This will allow you to check for beginnings of blisters, indicating slipping in the shoes, and is good practice for putting the brace on. If your child seems uncomfortable at night, check the length of the bar by measuring it across your child s shoulders. A bar that is too short can be a cause of discomfort. 19
21 Preventing Relapse: Bracing and Surveillance Play with your child in the brace to help him or her get used to it. The child cannot move his or her legs independently, so teach your child that kicking and swinging the legs together is possible. Gently push and pull on the bar to flex and extend your child s knees. Kicking the bar straight will help to stretch the tight tendons of a clubfoot. Make it routine. Children will do better if you make this treatment a regular part of daily life. The bar of the brace can be padded with a bicycle handle pad to protect you, your child, and your furniture. Check your child s heels for bright red spots, which usually indicate that the shoe was not worn tightly enough. If you are having difficulty with this, your orthotist may add a pad above the heel. If red heel marks persist or are severe, contact your doctor. Occasionally check the bolts which attach the shoe to the bar and ensure that they are tight. Make sure your baby s socks fit well; poorly fitting socks can bunch up and cause friction or blisters. When your child graduates to nap and nighttime only wear, make putting on the brace a part of the ritual. Your child is less likely to fuss if the brace is a consistent part of their normal nap and bedtime routine. Dressing Your Baby in the Brace Your baby will need to be dressed in pants and sleepers that open all the way on both sides, so you don t have to remove the brace to change a diaper. Because the brace holds the feet at shoulder-width apart, stretchy pull-down pants will only come down as far as the knee and can be uncomfortable for the baby (and messy for you both!). As you become comfortable and confident at putting on the brace, you might wish to remove it briefly for diaper changes. However, this can be aggravating for your baby who thinks he or she is free, so it is best to avoid this in the beginning. To keep little toes warm, you can put socks over the boots. You might also try buying slightly larger-toed sleepers and just cut a slit from the last snap so you can hook it over the boot toe. Other Types of Orthoses Other types of orthoses are sometimes recommended for children with clubfoot after correction using the Ponseti Method. These are listed below. Though not part of the Ponseti treatment, they are used in certain circumstances. Ankle Foot Orthoses (AFOs) are custom-molded plastic boots secured with Velcro straps, meant to hold the foot in a neutral position. Since these cannot hold the foot in abduction, they are not used in place of a foot abduction brace for a Ponseti-corrected clubfoot. However, they may be used to maintain a surgically corrected foot. Some health care professionals will modify the AFOs to provide external rotation. Foot Orthotics are custom-made shoe inserts which may be used to support a child s foot to optimize alignment, accommodate a leg-length difference, or support collapsing arches. 20
22 Exercise and Physiotherapy Every child s life is about play! Make exercises fun so that it is a time of pure magic for both of you! Many clinics have physiotherapists to advise about exercise. Physiotherapists are health care professionals trained to assess and treat conditions that affect the structure and movement of the body through manual, hands-on exercise and education. During the correction phase, normal baby stimulation and play is all that is necessary. Although babies should sleep on their backs, the Canadian Paediatric Society recommends it is also important that they experience tummy time when they are settled and awake to learn how to hold up their head and put weight through their arms. Babies in casts can still be placed on their tummy or on their sides with support. Your doctor or a physiotherapist can show you various ways of positioning and holding your baby while in casts. Infants in casts can do most things considered normal for their age, except of course, take baths. After casting is finished and your baby is in braces, a physiotherapist may suggest some basic exercises to do during the one hour of off time from the brace, such as: Heel cord stretches, to maintain the elasticity of the Achilles tendon, and Moving the foot in every direction to maintain a full range of motion. Should my child do exercises to make their foot and ankle stronger? Most children treated in the Ponseti Method will build strength and flexibility through normal movement and activity. If the child has residual tightness or weakness in some muscle groups, the physiotherapist may recommend exercises specific to the concern. For younger children, this may include play activities that incorporate climbing, squatting, or walking on different angles or grades to naturally stimulate balanced use of the muscle groups. What do the exercises do? They improve the strength of your child s weaker leg and foot muscles, and stretch out the muscles that are too tight. Exercises also help your child keep up with age-appropriate motor skill development, improve balance, coordination and walking pattern. When and how often should exercises be done? Your physiotherapist will help you answer this question specifically for your child. Generally speaking, it is best to set aside a short period of time each day so that your child s exercises become a regular and expected part of the family s daily routine. It can be combined with the nightly ritual of putting on your child s brace, if that works for you. The important thing is to be consistent. 21
23 Parent Story: Jillian and Claire Claire at 1 year old Claire at 5 years old Cast at 6 years old On the rainy evening when I went into labour with my second child, it all happened so quickly that I thought she would be born in the Burnaby Hospital parking lot. Fortunately we made it to the delivery room in time. My doctor, however, did not. (That s another story.) Although I didn t see our daughter, Claire, when she was first born, my husband did, and he knew right away that something didn t look right about her left foot. When the doctor finally arrived, she told us Claire had a clubfoot and that it could be fixed with a cast. Oh, a cast, I thought. Well, that s fine; like a broken leg the cast will be on for six weeks and then we will be done. Little did I know where our journey would take us. That was years ago. Today, Claire runs, swims, skates and loves gymnastics. She is normal. But it took more than just a cast to get her this far. On our first visit to the Royal Columbian Hospital Cast Clinic, Claire was only six days old and I was nervous, exhausted and full of questions. She received a new cast every week and her foot started correcting. Meanwhile, we had to answer strangers questions about the cast and tell our family all we knew about why this had happened. You will face the same kinds of things. I was scared when Claire had her tenotomy. At that time it was done during day surgery under a local anesthetic and I was more worried about the anesthetic than the procedure. I know you will be nervous when it s your baby s turn, but you are fortunate that research has changed this procedure so that it s now most often done during your visit to the clinic. After the casts, you move on to boots and bars. When that happens, you will face even more questions from strangers and family. But by now you will be used to them, you'll have more answers and will feel more confident. The first night with the boots and bars Claire cried every time she tried to turn over and the toe of the boot got caught in the crib railings. I m not sure how she figured it out but by the second night she slept with only a few interruptions, and was fine after that. Babies are amazing at adapting, and if I could go back and do it again, I would worry less about her ability to handle it all. Finally, at five years old, she was out of the brace and I thought we were done, except for occasional visits to the clinic. Unfortunately I was wrong. When Claire was six-and-a-half her foot started turning in again, and I could tell things weren t looking right. Her next visit to the clinic confirmed it, and she went back into a cast. Now she was a big girl with a full leg cast, and I was worried about how she would cope with that. Once again she adapted, and within a week was running in the cast; she even figured out how to do somersaults in it! Kids are so adaptable. I, however, was wracked with guilt the relapse must have happened because I didn t force her to exercise every day, or I didn t do the stretches regularly. Eventually I realized that parents are not perfect and that parents of clubfoot babies have a little extra on their plates. For awhile Claire was back in her boots and bars. Although she was old enough to complain, she understood that it was important and wore them without complaint most of the time. Her biggest concern seems to be a desire to wear pretty girl shoes; she wants to wear flip flops but forgets that she that has two different sized feet and needs her orthotics. Although having a child with a clubfoot has its challenges, we are grateful that we live in a modern country where this condition can be corrected. My doctor says we are always shocked when things go wrong, but that we should really be shocked when babies are perfect. In the end, we have a wonderful, intelligent and healthy daughter. And she is normal! 22 Claire today
24 Parent Story: Heather and Hayden 23 My involvement with this booklet comes from a deep passion to help other parents understand the processes, the trials and the triumphs of having a child with clubfoot. My son was born in June 2005 with bilateral clubfoot. Since there had been no diagnosis of clubfoot prior to his birth, it came as a big surprise! Before we discovered the Ponseti Method of treatment, we were frustrated with how much we didn t know about the whole process. I really needed a booklet such as this! Royal Columbian Hospital does a huge service for the community and the parents of children with clubfoot by offering this method of treatment via Dr. Pirani, and we are fortunate to have this fabulous team of people available. With the combined efforts of your child s orthopaedic surgeon and the rest of the health care team, you will come away from this experience knowing you have had the best treatment possible for your child. Nothing is more rewarding than the first time you see your child stand up on those two perfect little feet. During Hayden s early days, we dealt with issues around clothing, equipment and skin problems. Certain clothing did not fit well and some baby equipment was hard to negotiate with either the casts or the brace. Hayden developed some skin rashes under his first casts. On the day of Hayden s tenotomy, I was anxious and nervous. I wondered how much he would cry and if he would experience much pain. I chose to remain in the room to assist in comforting him. The procedure was so fast! Hayden cried, but mostly because he was being held down (at this point he was about six months old older than most babies are when they have this procedure done) and he was annoyed. He settled down right away once it was over and fell asleep. Heather and Hayden with Dr. Pirani Once Hayden was finished with his casting phase, things got much easier with his transition into the boots and bar. I won t lie to you; the first night was rough. He woke up about every 20 minutes and cried, but by the next morning, he was totally fine and he never cried again about the brace. Yes, it was hard to always have him in it for the first little while. I had lots of bruises from accidental whacks. I had to make sure his pants and pajamas snapped all the way open, otherwise the brace would have to be removed for diaper changes and I didn t want to do that every time he needed changing. But before we knew it, his full-time brace wear (23 hours per day) was reduced to 12 to 14 hours a day in the brace. He continued wearing the brace until four years of age and now goes for regular follow up visits with Dr. Pirani. His development has not been affected at all. He has done pretty much everything on time. He had already figured out how to roll over in casts and clued in straight away with the brace. He crawled as well as stood up in the brace. In fact, one bonus I observed was that as soon as I put the brace on him at night, he begins to rub his eyes and yawn! If there is some advice I d like to pass on, it s this: Always trust your instincts as a parent. If you think there is something wrong, there probably is. You know your baby best. Therefore, if you feel there is a problem with a cast, call your doctor right away and remove it if that is advised. An extra week of correction is better than causing your baby distress. Also, parents are the ones responsible for the bracing. If we don t put it on, our child s feet will not stay corrected. All the best in your baby s journey! Hayden in his brace
25 Frequently Asked Questions What causes clubfoot? Is it my fault? No, it is not your fault. It may be hereditary, it may just happen; there is no proven cause. Feeling guilty is normal and those feelings can persist throughout this journey. Be careful not to let anyone else make you feel guilty. It is hard enough to raise a child even when everything is fine. Remember also that surgery is okay, it helps in all areas of life, and if this is the recommended treatment for your child, that is fine too. Will my child be normal, look normal, and participate in normal activities? Yes, your child will look normal. He or she may have one foot smaller than the other, or smaller feet or calf muscles than his or her peers, but these are things that people do not notice. Your baby may start walking a few months later than others, but he or she will be able to participate in all normal activities: swimming, running, jumping, and so much more. Foot at birth 3 years 5 years 7 years Photos are of Claire, whose mother helped create this booklet. What happens when they are older? When are we finished treatment? Clubfoot children lead normal lives once their feet are corrected. To stop clubfoot from coming back, braces should be worn at night until approximately the fourth birthday (sometimes longer if the doctor indicates). If there is no relapse within the first year or two of not bracing, then you are probably fine. However, follow-up visits may be necessary if one leg is longer than the other, as sometimes doctors recommend surgery to correct leg-length differences. Follow-up is rarely needed after the bones stop growing usually at age 14 for girls and age 16 for boys. Will my child have to wear different types of shoes? If your child only has one clubfoot his or her feet will likely be different sizes. An orthotic can be made to fit the shoe on the clubfoot; this will help hold the foot in a good position and fill the small foot area. If your orthotist recommends two different sized shoes, you can save money by buying three sizes of identical runners and then use these to make two mix-matched pairs for your child. Children with bilateral clubfoot can generally wear regular shoes once they re ready for them, although initially, barefoot at home is best for early walkers and perhaps a soft leather slipper-type shoe in colder months. What will my child s perspective on clubfoot be? If you treat the clubfoot as a normal part of life, your child will too. Some children need glasses, some need hearing aids, and your child will need a brace for a while.as they get older show them the babies starting out at the clinic so they see they are not alone. If they want to tell their friends about their clubfoot, that is fine. Children are much more accepting, and have fewer worries than adults. Older children requiring a cast may enjoy choosing their own colour, if available, or decorating their cast or brace. 24
26 Famous People With Clubfeet Sandra Schmirler, Olympic Curler Sandra was born June 11, 1963, with a clubfoot and had to wear a cast for two months. She began curling at the age of 12 and became known as Schmirler the Curler, an appropriate nickname as she escalated to greatness, highlighted by skipping her team to a gold medal in the 1998 Olympics in Nagano, Japan. (Sandra passed away in 2000 at the young age of 36, after a six-month battle with cancer.) Greg Barton, Sprint Kayaker and four-time Olympic Medalist Greg was born Dec. 2, 1959, with a clubfoot and walked with more difficulty after a surgery that fused some bones. He won two gold medals in the 1988 Seoul Olympics. A member of four consecutive Olympic teams, Greg won the bronze in K-1 (1,000 meters) in 1984 and It was at the 1988 Games, however, that he stole the show, winning the gold in K-1 (1,000 meters) and then coming back 90 minutes later to team with Norm Bellingham to win the gold in K-2 (1,000 meters). LeRoy Butler, Green Bay Packers Safety, played in four Pro Bowls Born July 19, 1968, LeRoy was diagnosed with bilateral clubfoot, when he was unable to crawl at six months of age. Within six months, he had corrective surgery and wore a body cast. When Butler first began to walk, he used corrective shoes, and by the time he reached kindergarten, he used canes with wrist attachments so he could keep his balance. If I wasn t in a wheelchair, I had a cast or I used a brace, LeRoy remembered. It wasn't until after his 8th birthday that he improved significantly and went on to play professional football. Jeff Gove, Pro Golfer Jeff overcame physical ailments that might have made others step lightly around golf. He was born on May 28, 1971, with a clubfoot, and required several surgeries and special orthotics. Today he wears a size 9 shoe on one foot, a size 7 on the other, and a slight limp can be detected in his march down the fairways. It hasn t affected his golf game! Mia Hamm, Women s Soccer Player Born March 17, 1972, with a partial clubfoot, Mia wore casts on her feet when she was a baby to help correct them. When the casts came off, her feet were ready to take on the world. Mia is considered the best all-around and most recognized woman soccer player in the world. She was a member of the gold medal-winning U.S. Women s National Team at the 1996 Olympic Games, and was named U.S. soccer's Female Athlete of the Year for three consecutive years from 1994 to 1996, becoming the first player to be honoured three times. 25 Kristi Yamaguchi, Olympic Figure Skating Gold Medalist Born July 12, 1971, Kristi is considered a veteran professional. Her professional career is marked by numerous major championship titles and critically acclaimed performances earning her accolades from major sportswriters as the best female skater in the world. Born with clubfeet, Kristi now leads a very active life.
27 Resources The Canadian Orthopaedic Foundation is Canada s only health charity dedicated solely to helping people maintain and restore their bone and joint, or orthopaedic, health. Below is an abbreviated list of resources that address clubfoot. Visit our website at for others. Peer Support Ortho Connect Would you like to talk to a parent of a child with clubfoot? Ortho Connect is a free, telephone-based peer support program that provides you with the opportunity to talk to a trained parent volunteer who has a child with clubfoot. To learn more about this program or to become a volunteer visit or call Below are selected resources that may be of interest, encouragement or comfort to parents. These are just some of the links and resources the Canadian Orthopaedic Foundation lists on its website at The Foundation has no control over the resources listed, other than its own. Information and Educational Websites The Canadian Orthopaedic Foundation provides information and education to help people become active participants in their orthopaedic treatment, including Ortho Connect, a peer-support program for new patients, or their parents or caregivers. Through its website the US-based Ponseti International Association promotes the Ponseti Method for the treatment of clubfoot, and provides information for patients. The Clubfoot Club website, maintained by a Canadian mom, provides insight, resources, and stories from the parents perspective. The Clubfoot Club has a stories section with shared experiences from infancy through adulthood. This website includes downloadable resources including the third edition of Ponseti Clubfoot Management. The Yahoo Health Groups listed below are on-line communities that are free to join. All that is required is a Yahoo ID, which is easy to set up yourself in just a minute or two. is an on-line community of parents of children in Canada with bilateral and unilateral clubfoot. is an on-line community of parents of children with clubfoot to discuss non-surgical methods of treating clubfoot, and specifically the Ponseti method. Clubfoot Supplies (Ponseti AFO/Mitchell brace) (Markell boots) (ALFA-Flex brace) (Horton Click with 10 degree Kicker) 26 Books Congenital Clubfoot: Fundamentals of Treatment, Ignacio V. Ponseti Homage to Iowa: The Inside Story of Ignacio V. Ponseti, Helena Percas-Ponseti
28 Glossary of Terms 27 Abduction In medicine, the movement of a limb away from the midline of the body. Abduction of both legs spreads the legs. The opposite of abduction is adduction. Adduction of the legs brings them together. Achilles Tendon A tough sinew that attaches the calf muscle to the back of the heel bone. The Achilles tendon is one of the longest tendons in the body. It is also called the tendo Achilles or the tendo calcaneus, the calcaneus being the heel bone. Bilateral Having, or relating to, two sides. Bilateral clubfoot means both feet are affected. Congenital Present at birth. A condition that is congenital is one that is present at the time of birth. Deformity A change from the normal size or shape of an anatomic structure due to mechanical forces that distort an otherwise normal structure. Dorsiflexion The turning of the foot or the toes upward, as when the foot is flexed. Equinus Deformity of the foot in which the heel is pulled up and the forefoot is pulled down. Equinovarus Similar to equinus, with additional inward turning of the forefoot. Gastrosoleus Muscles The calf or gastrosoleus is a pair of muscles the gastrocnemius and soleus at the back of the lower human leg. The gastrosoleus complex is connected to the foot through the Achilles tendon. Idiopathic Of unknown cause. Any disease that is of uncertain or unknown origin may be termed idiopathic. In Utero While you are still pregnant, or the baby is still in the womb. Ligament A tough band of connective tissue that connects various structures such as two bones; it comes from the Latin ligare, meaning to bind or tie. Maceration The word macerate comes from the Latin macero, meaning to soften by soaking (in a liquid). If your child s skin becomes wet underneath the casts, maceration can occur and the skin will break down. It is painful and can leave scarring. Orthopaedics The branch of surgery broadly concerned with the skeletal system (bones). The term is rooted in the word ortho, meaning straight, and the Greek word paes, meaning child, and refers to the practice, literally, of straightening the child. Orthosis (Orthoses, plural) An external orthopaedic appliance that prevents or assists the movement of the spine or limbs. Positional Relating to the position of a baby, or babies, in utero. Straight-last boots The boots are made on a straight-last, a shoemaker s model for shaping footwear. A straight-last shoe is symmetrical, relative to a line drawn on the bottom of the shoe from the middle of the heel to the middle of the toe. Syndromic Part of a syndrome, a group of symptoms leading to a diagnosis. Talipes Clubfoot. The Latin word talipes was compounded from talus (ankle) and pes (foot) since, with the common or classic type of clubfoot (talipes equinovarus), the foot is turned in sharply and the person seems to be walking on his or her ankle. Talipes equinovalgus refers to the malformation of the foot evident at birth in which the heel is elevated like a horse s hoof (equino-) and the heel is turned outward (valgus). Tendon The tissue by which a muscle attaches to bone. A tendon is somewhat flexible, but also fibrous and tough. Tenotomy A short procedure that releases the heel cord, or Achilles tendon. A small cut is made into the tendon (near the heel of the foot) with a tiny scalpel. This procedure is done to lengthen the tendon and enable it to function properly when the foot is flexing. Unilateral Having, or relating to, one side. In the case of clubfoot, this can be either the left foot or the right foot. Varus Angled inward, bent or twisted inward.
29 Contributors The Canadian Orthopaedic Foundation gratefully acknowledges the many people who generously contributed their time and knowledge to help create this booklet. A special thank you goes to: The Royal Columbian Hospital (RCH) in New Westminster, British Columbia, is one of 12 hospitals under the umbrella of the Fraser Health Authority. Location: 330 East Columbia Street, New Westminster, B.C. V3L 3W7. Phone: or or Facsimile: Ron and Audrey Plaster Grandparents of Clubfoot Patient, Claire Chateauneuf made a special contribution to this booklet through Audrey s establishing of a memorial fund with proceeds to the Royal Columbian Clubfoot Clinic following Ron s passing in Jillian Chateauneuf Parent of a Child with Clubfoot spearheaded this project, and as a photographer, contributed the photos. I have learned so much in the journey to correct my daughter s clubfoot and hope that every parent will benefit from the information provided in this booklet. Heather Cohen Parent of a Child with Clubfoot Heather also spearheaded the development of the content for this booklet. As a mother of three, my qualifications include mother s intuition, fierce protection of my children and a because I m the Mom attitude. I am happy to report my son s feet look perfect thanks to Dr. Pirani and the Ponseti Method! Dr. Shafique Pirani Orthopaedic Surgeon is a paediatric orthopaedic surgeon and professor at UBC, Faculty of Medicine, Department of Orthopaedics. He started the Clubfoot Clinic at Royal Columbian Hospital in 1991, and is a leader of development of Ponseti clubfoot programs worldwide. 28 Lisa Bennett BHK, CO(c) Certified Orthotist Brenda Horton Registered Physiotherapist Salena Mohammed Health Services Manager (Paediatrics and Neonatal) RCH Anna Stonehouse Medical Office Assistant Milton Tingle CSOTR-A Orthopaedic Technologist, RCH
30 Your Baby s Milestones Baby s Name: Significant Dates Due date: Birth date: Date of first clinic visit: First cast: Tenotomy: Bracing started: Night-time bracing only: Bracing discontinued: Other: Many doctors assess progress during treatment by measuring a number of scores that indicate the amount of deformity that remains in the foot. Use the table below if you wish to record the Pirani Total Clubfoot Score during treatment. PIRANI TOTAL CLUBFOOT SCORE (6 = severe deformity, 0 = normal) Week 1 Week 2 Week 3 Week 4 Week 5 Week 6 Week 7 Date Left foot Right foot 29
31 Progress Notes:
32 Talk to someone who s been there. Call the Canadian Orthopaedic Foundation at Or visit us on-line at This patient resource is supported in part with unrestricted educational grants from: This booklet provides general, practical information only and should not replace consultation with, or care or instructions provided by qualified health care professionals. The Canadian Orthopaedic Foundation does not endorse any product, treatment or therapy. The content of this booklet has been reviewed for accuracy, reliability and helpfulness to the intended audience by the Medical & Scientific Review Committee of the Canadian Orthopaedic Foundation. While the Canadian Orthopaedic Foundation makes effort to ensure the information in this booklet is accurate and reliable, it cannot guarantee that it is error-free or complete. Before making medical decisions or if you have questions about your child s medical situation, speak to your surgeon. 2 nd Edition
Patient and Family Education. Clubfoot Correction. Using casting followed by shoes on a bar (the Ponseti method) What is the cause of clubfoot?
 Patient and Family Education Clubfoot Correction Using casting followed by shoes on a bar (the Ponseti method) The results of treating a child with clubfoot using the Ponseti method are very good. This
Patient and Family Education Clubfoot Correction Using casting followed by shoes on a bar (the Ponseti method) The results of treating a child with clubfoot using the Ponseti method are very good. This
Congenital Talipes Equinovarus
 Congenital Talipes Equinovarus (CLUBFOOT) A GUIDE FOR PARENTS Clubfoot Clubfoot affects 1 in every 1000 births. Although we still don t know exactly what causes clubfoot, in most cases it can be quickly
Congenital Talipes Equinovarus (CLUBFOOT) A GUIDE FOR PARENTS Clubfoot Clubfoot affects 1 in every 1000 births. Although we still don t know exactly what causes clubfoot, in most cases it can be quickly
Club Feet, Flat Feet, Bow Legs, and Knock-Knees
 Club Feet, Flat Feet, Bow Legs, and Knock-Knees CHAPTER 11 113 WHAT IS A DEFORMITY AND WHAT IS? Sometimes parents worry because they think a part of their child s body is abnormal or deformed. But in small
Club Feet, Flat Feet, Bow Legs, and Knock-Knees CHAPTER 11 113 WHAT IS A DEFORMITY AND WHAT IS? Sometimes parents worry because they think a part of their child s body is abnormal or deformed. But in small
The Ponseti technique
 Patient Information The Ponseti technique Author: Trauma and orthopaedics Produced and designed by the communications team Issue date October 2017 - Review date October 2020 Version 3 Ref no. PILCOM1522
Patient Information The Ponseti technique Author: Trauma and orthopaedics Produced and designed by the communications team Issue date October 2017 - Review date October 2020 Version 3 Ref no. PILCOM1522
CAST CARE. Helping Broken Bones Heal
 CAST CARE Helping Broken Bones Heal When You Need a Cast Are you injured and in need of a cast? Don t worry, you ll get through it. Wearing a cast will help your injured body part heal. Healing takes time,
CAST CARE Helping Broken Bones Heal When You Need a Cast Are you injured and in need of a cast? Don t worry, you ll get through it. Wearing a cast will help your injured body part heal. Healing takes time,
Session 3 or 6: Being Active: A Way of Life.
 Session 3 or 6: Being Active: A Way of Life. You can find the time to be active. Set aside one block of time every day to be active. When can you set aside 20 to 30 minutes to do an activity you like?
Session 3 or 6: Being Active: A Way of Life. You can find the time to be active. Set aside one block of time every day to be active. When can you set aside 20 to 30 minutes to do an activity you like?
Correcting Joint Contractures
 559 Correcting Joint Contractures CHAPTER 59 In this chapter we discuss different aids used for gradually straightening limbs that have joint contractures. Information on contractures, their causes and
559 Correcting Joint Contractures CHAPTER 59 In this chapter we discuss different aids used for gradually straightening limbs that have joint contractures. Information on contractures, their causes and
orthoses Controlling Foot Movement Through Podiatric Care
 1 Controlling Foot Movement Through Podiatric Care Control Movement Control Pain Out of sight, out of mind, healthy feet are easily forgotten. But if your feet aren t moving right or you re working them
1 Controlling Foot Movement Through Podiatric Care Control Movement Control Pain Out of sight, out of mind, healthy feet are easily forgotten. But if your feet aren t moving right or you re working them
Ponseti Treatment Method for Idiopathic Clubfoot Continuing Education Module
 Ponseti Treatment Method for Idiopathic Clubfoot Continuing Education Module Michelle J. Hall, CPO, BSE 1 Ignacio V. Ponseti, MD 2 1. Certified Prosthetist Orthotist at American Prosthetics & Orthotics,
Ponseti Treatment Method for Idiopathic Clubfoot Continuing Education Module Michelle J. Hall, CPO, BSE 1 Ignacio V. Ponseti, MD 2 1. Certified Prosthetist Orthotist at American Prosthetics & Orthotics,
Plantar Fasciitis and Heel Pain
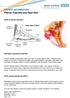 PATIENT INFORMATION Plantar Fasciitis and Heel Pain What is plantar fasciitis? Heel pain and plantar fasciitis Plantar fasciitis causes pain under your heel. It usually goes in time. Treatment may speed
PATIENT INFORMATION Plantar Fasciitis and Heel Pain What is plantar fasciitis? Heel pain and plantar fasciitis Plantar fasciitis causes pain under your heel. It usually goes in time. Treatment may speed
Lumbar Decompression GUIDELINES FOR PATIENTS HAVING A. Lumbar Decompression
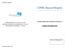 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
Information for Families. Serial Casting
 Information for Families Serial Casting Serial Casting Casting is a treatment used to provide a sustained stretch to tight muscles. Serial casting is when a series of casts are placed on the limb over
Information for Families Serial Casting Serial Casting Casting is a treatment used to provide a sustained stretch to tight muscles. Serial casting is when a series of casts are placed on the limb over
PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY
 Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Prevent Falls. with the Moore Balance Brace. Many falls can be prevented. By making minor changes, you can lower your chances of falling
 Prevent Falls with the Moore Balance Brace Many falls can be prevented. By making minor changes, you can lower your chances of falling Moore Balance Brace (MBB) Instructions for use Putting the MBB into
Prevent Falls with the Moore Balance Brace Many falls can be prevented. By making minor changes, you can lower your chances of falling Moore Balance Brace (MBB) Instructions for use Putting the MBB into
Hip Resurfacing with Precautions. Therapy Resources. xpe045 (4/2015) AHC
 Hip Resurfacing with Precautions Therapy Resources xpe045 (4/2015) AHC Hip Resurfacing Home Exercise Program - Phase I 1. Breathing Exercises Exercise can be done while sitting or lying down. Action: Place
Hip Resurfacing with Precautions Therapy Resources xpe045 (4/2015) AHC Hip Resurfacing Home Exercise Program - Phase I 1. Breathing Exercises Exercise can be done while sitting or lying down. Action: Place
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What to expect after Dupuytren's surgery and what to do to get the best possible results.
 What to expect after Dupuytren's surgery and what to do to get the best possible results. Directly after surgery: You can expect a bulky bandage covering the palm and the fingers that were operated on.
What to expect after Dupuytren's surgery and what to do to get the best possible results. Directly after surgery: You can expect a bulky bandage covering the palm and the fingers that were operated on.
TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET
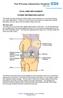 TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your knee replacement. However if you still have any concerns or queries
TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your knee replacement. However if you still have any concerns or queries
This advice and exercises have been selected to help you manage the symptoms of your arthritis
 This advice and exercises have been selected to help you manage the symptoms of your arthritis 1. GENERAL ADVICE Movement is good for your arthritic knee it helps to keep the tissue healthy, increases
This advice and exercises have been selected to help you manage the symptoms of your arthritis 1. GENERAL ADVICE Movement is good for your arthritic knee it helps to keep the tissue healthy, increases
Foot Care. Taking steps towards good FOR AT-RISK FEET. HIGH RISK of developing serious. Person with Diabetes
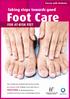 Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
ACHILLES TENDON RUPTURE
 ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
POSTNATAL EXERCISES. (Early In Patient Postnatal Days Until Six Weeks Post Delivery)
 POSTNATAL EXERCISES (Early In Patient Postnatal Days Until Six Weeks Post Delivery) Exercise Regularly This brochure is intended to educate women about mobility and exercises while as an In Patient and
POSTNATAL EXERCISES (Early In Patient Postnatal Days Until Six Weeks Post Delivery) Exercise Regularly This brochure is intended to educate women about mobility and exercises while as an In Patient and
Caring for a child in a Hip Spica cast
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Caring for a child in a Hip Spica cast Physiotherapy Department The aim of this information leaflet is to provide parents of
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Caring for a child in a Hip Spica cast Physiotherapy Department The aim of this information leaflet is to provide parents of
Foot Care. Taking steps towards good FOR AT-RISK FEET. HIGH RISK of developing serious. Person with Diabetes
 Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a HIGH RISK of developing serious problems
CARING FOR YOUR CATHETER AT HOME
 CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
Vancouver. CoastalHealth. Promoting wellness. Ensuring care. Mary Pack Arthritis Program Occupational Therapy
 Vancouver CoastalHealth Promoting wellness. Ensuring care. Mary Pack Arthritis Program Occupational Therapy O.T. IVA-9 01 12005 PATIENT EDUCATION: JOINT PROTECTION AND ENERGY CONSERVATION The goals of
Vancouver CoastalHealth Promoting wellness. Ensuring care. Mary Pack Arthritis Program Occupational Therapy O.T. IVA-9 01 12005 PATIENT EDUCATION: JOINT PROTECTION AND ENERGY CONSERVATION The goals of
Advice and exercises for managing knee and hip osteoarthritis October 2018 V1.2 April 2018 April 2021
 Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Advice: After the Removal of a Lower Leg Cast
 Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
Heather Feather s 3 Keys To Find Relief From Plantar Fasciitis Blueprint. By Heather Feather The Pain Free Feet Guide
 Heather Feather s 3 Keys To Find Relief From Plantar Fasciitis Blueprint By Heather Feather The Pain Free Feet Guide Heather Feather s 3 Keys To Kick Plantar Fasciitis To The Curb Blueprint To get the
Heather Feather s 3 Keys To Find Relief From Plantar Fasciitis Blueprint By Heather Feather The Pain Free Feet Guide Heather Feather s 3 Keys To Kick Plantar Fasciitis To The Curb Blueprint To get the
WHAT IS PLANTAR FASCIITIS?
 WHAT IS PLANTAR FASCIITIS? If you're finding when you climb out of bed each morning that your first couple steps cause your foot and heel to hurt, this might be a sign of plantar fasciitis. A common condition
WHAT IS PLANTAR FASCIITIS? If you're finding when you climb out of bed each morning that your first couple steps cause your foot and heel to hurt, this might be a sign of plantar fasciitis. A common condition
Move More Wakefield District. Active at home programme
 Move More Wakefield District Active at home programme The active at home programme has been developed to increase your activity levels in the comfort of your own home, and in turn improving your balance
Move More Wakefield District Active at home programme The active at home programme has been developed to increase your activity levels in the comfort of your own home, and in turn improving your balance
HOW TO USE NOW ROLLER MASSAGER & LACROSSE BALL - EXERCISES AND TIPS -
 HOW TO USE ROLLER MASSAGER & LACROSSE BALL - EXERCISES AND TIPS - BOOST YOUR RECOVERY NOW Thank you! Hi, it s Jeff again, Co-Founder of Maogani. Our team would like to thank you for giving us the opportunity
HOW TO USE ROLLER MASSAGER & LACROSSE BALL - EXERCISES AND TIPS - BOOST YOUR RECOVERY NOW Thank you! Hi, it s Jeff again, Co-Founder of Maogani. Our team would like to thank you for giving us the opportunity
Tips to Treat Bunion and avoid Surgery
 Tips to Treat Bunion and avoid Surgery DR JK i Important Legal Disclaimer Before beginning using any of our tips or our bunion relief products, consult your physician first to be sure it is appropriate
Tips to Treat Bunion and avoid Surgery DR JK i Important Legal Disclaimer Before beginning using any of our tips or our bunion relief products, consult your physician first to be sure it is appropriate
Posterior Total Hip Replacement with Precautions. Therapy Resources
 Posterior Total Hip Replacement with Precautions Therapy Resources The information presented is intended for general information and educational purposes. It is not intended to replace the advice of your
Posterior Total Hip Replacement with Precautions Therapy Resources The information presented is intended for general information and educational purposes. It is not intended to replace the advice of your
LETTER FROM THE AUTHOR
 LETTER FROM THE AUTHOR Included in this ebook are three fundamental exercises for improving posture. My goal for you is that you don t just go through the motions, or hope the exercises are working my
LETTER FROM THE AUTHOR Included in this ebook are three fundamental exercises for improving posture. My goal for you is that you don t just go through the motions, or hope the exercises are working my
Foot Care. Taking steps towards good FOR AT-RISK FEET. Person with Diabetes
 Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a LOW RISK of developing serious problems,
Taking steps towards good Person with Diabetes Foot Care FOR AT-RISK FEET Your healthcare professional has found that as a person with Diabetes your feet have a LOW RISK of developing serious problems,
Forefoot deformity correction
 Forefoot deformity correction This leaflet aims to answer your questions about having forefoot deformity correction surgery. It explains the benefits, risks and alternatives, as well as what you can expect
Forefoot deformity correction This leaflet aims to answer your questions about having forefoot deformity correction surgery. It explains the benefits, risks and alternatives, as well as what you can expect
ANKLE SPRAINS. Explanation. Causes. Symptoms
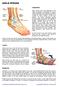 ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
How to Protect Your Joints
 Form: D-5855 How to Protect Your Joints For people with arthritis Arthritis can be painful and make every day activities difficult. This booklet will show you how to protect your joints. This can help
Form: D-5855 How to Protect Your Joints For people with arthritis Arthritis can be painful and make every day activities difficult. This booklet will show you how to protect your joints. This can help
Make sure you have properly fitting running shoes and break these in gradually. Never wear new running shoes for a race or a long run.
 Common Running Injuries We are delighted that you have decided to run in the next Bath Half Marathon and very much hope that you have good running shoes, undertake a regular training programme and don
Common Running Injuries We are delighted that you have decided to run in the next Bath Half Marathon and very much hope that you have good running shoes, undertake a regular training programme and don
Lesser toe surgery. Exceptional healthcare, personally delivered
 Lesser toe surgery Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed as needing lesser toe surgery. This leaflet
Lesser toe surgery Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed as needing lesser toe surgery. This leaflet
CUBITAL TUNNEL SYNDROME
 WHAT IS CUBITAL TUNNEL SYNDROME? SYMPTOMS Cubital tunnel syndrome is the second most commonly occurring nerve compression in the upper body It is caused by compression of the ulnar nerve at the elbow The
WHAT IS CUBITAL TUNNEL SYNDROME? SYMPTOMS Cubital tunnel syndrome is the second most commonly occurring nerve compression in the upper body It is caused by compression of the ulnar nerve at the elbow The
Knee Conditioning Program
 Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
postpartum fitness GETTING BACK IN SHAPE AFTER YOUR PREGNANCY
 postpartum fitness GETTING BACK IN SHAPE AFTER YOUR PREGNANCY While pregnancy and birth can be joyful, they also can be hard on your body. To regain the level of fitness you had before you became pregnant,
postpartum fitness GETTING BACK IN SHAPE AFTER YOUR PREGNANCY While pregnancy and birth can be joyful, they also can be hard on your body. To regain the level of fitness you had before you became pregnant,
Rehabilitation Program Following Isolated Biceps Tenodesis
 Rehabilitation Program Following Isolated Biceps Tenodesis Richard Holtby Assistant professor, Department of Surgery University of Toronto Biceps Groove Biceps tendon HOLLAND ORTHOPAEDIC & ARTHRITIC CENTRE
Rehabilitation Program Following Isolated Biceps Tenodesis Richard Holtby Assistant professor, Department of Surgery University of Toronto Biceps Groove Biceps tendon HOLLAND ORTHOPAEDIC & ARTHRITIC CENTRE
Bunion Surgery. Patient information Leaflet
 Bunion Surgery Patient information Leaflet April 2017 What is a bunion? A bunion is a bony lump on the side of your foot at the base of your big toe (see figure 1). This may be an isolated problem but
Bunion Surgery Patient information Leaflet April 2017 What is a bunion? A bunion is a bony lump on the side of your foot at the base of your big toe (see figure 1). This may be an isolated problem but
YOUR FREE COMPREHENSIVE GUIDE TO HELP RELIEVE LOWER BACK PAIN NATURALLY
 YOUR FREE COMPREHENSIVE GUIDE TO HELP RELIEVE LOWER BACK PAIN NATURALLY By: helpwithsciatica HTTPS://HELPWITHSCIATICA.COM Table of contents 1 Introduction 2 Exercise: Extensions 3 Exercise: Curl-Ups 4
YOUR FREE COMPREHENSIVE GUIDE TO HELP RELIEVE LOWER BACK PAIN NATURALLY By: helpwithsciatica HTTPS://HELPWITHSCIATICA.COM Table of contents 1 Introduction 2 Exercise: Extensions 3 Exercise: Curl-Ups 4
ANTERIOR KNEE PAIN. Explanation. Causes. Symptoms
 ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
Stretching. Knees: Rotate your knees in a circle, keeping them together and bending down slightly.
 Stretching Stretching the Major Muscle Groups Static Stretches Hamstrings: Hang down and try to reach your toes; don t push it. Keep legs and back straight. Just go down to a comfortable level for your
Stretching Stretching the Major Muscle Groups Static Stretches Hamstrings: Hang down and try to reach your toes; don t push it. Keep legs and back straight. Just go down to a comfortable level for your
Rehabilitation Program Following Shoulder Diagnostic Arthroscopy, Acromioplasty, Decompression, AC Resection, Debridement
 Rehabilitation Program Following Shoulder Diagnostic Arthroscopy, Acromioplasty, Decompression, AC Resection, Debridement Richard Holtby Assistant professor, Department of Surgery University of Toronto
Rehabilitation Program Following Shoulder Diagnostic Arthroscopy, Acromioplasty, Decompression, AC Resection, Debridement Richard Holtby Assistant professor, Department of Surgery University of Toronto
FEEL GOOD GLOW Low intensity workout
 Welcome to the low intensity workout, Feel good glow. If this is your first time doing one of our workouts, we recommend you check out the introductory video at www.healthier.qld.gov.au to get more information
Welcome to the low intensity workout, Feel good glow. If this is your first time doing one of our workouts, we recommend you check out the introductory video at www.healthier.qld.gov.au to get more information
While it s unlikely you ll meet all of us you can expect to see more than one physio during your stay in hospital.
 Introduction: This information is provided to give you and your family a basic knowledge of the total hip replacement operation, outlining the things you should know, both before and after surgery. The
Introduction: This information is provided to give you and your family a basic knowledge of the total hip replacement operation, outlining the things you should know, both before and after surgery. The
People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy.
 Form: D-5821 Treat Your Feet: Foot care for people with diabetes People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy. Diabetes raises
Form: D-5821 Treat Your Feet: Foot care for people with diabetes People with diabetes often have trouble with their feet. Read this booklet to learn 7 steps to help keep your feet healthy. Diabetes raises
1. Medications: a. A pain medicine (narcotic): b. An anti-inflammatory medicine: c. An antibiotic:
 Post Operative Instructions: 1. Medications: Three medications have been prescribed for you to make you more comfortable, decrease the swelling in the knee following surgery, and to reduce the risk of
Post Operative Instructions: 1. Medications: Three medications have been prescribed for you to make you more comfortable, decrease the swelling in the knee following surgery, and to reduce the risk of
Post Lung Transplant Exercises
 Post Lung Transplant Exercises Post Lung Transplant Physical activity improves our strength and stamina, maintains optimal functioning of our major organs and increases our vitality, energy and overall
Post Lung Transplant Exercises Post Lung Transplant Physical activity improves our strength and stamina, maintains optimal functioning of our major organs and increases our vitality, energy and overall
Knee Conditioning Program
 Knee Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Knee Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Patient and Family Education. SupER Splint. Why does my baby need a splint? What is a SupER splint and how does it work?
 Patient and Family Education SupER Splint Shoulder External Rotation and Forearm Supination Wrap Why does my baby need a splint? Your baby has been diagnosed with brachial plexus palsy. This causes your
Patient and Family Education SupER Splint Shoulder External Rotation and Forearm Supination Wrap Why does my baby need a splint? Your baby has been diagnosed with brachial plexus palsy. This causes your
General Cast and Splint Care
 General Cast and Splint Care Casts and splints provide limb support after a fracture or surgery. They may also be used to stretch the muscles in a limb. The cast or splint keeps the arm or leg in the proper
General Cast and Splint Care Casts and splints provide limb support after a fracture or surgery. They may also be used to stretch the muscles in a limb. The cast or splint keeps the arm or leg in the proper
Information and exercises following a proximal femoral replacement
 Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Information Following Ankle Injury
 Patient & Family Guide Information Following Ankle Injury 2016 www.nshealth.ca Information Following Ankle Injury Physiotherapy Department Date Physiotherapist What to expect after cast/bandage removal:
Patient & Family Guide Information Following Ankle Injury 2016 www.nshealth.ca Information Following Ankle Injury Physiotherapy Department Date Physiotherapist What to expect after cast/bandage removal:
METATARSAL FRACTURE (Including Jones and Dancer s Fractures)
 METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
Workout to Go. A Sample Exercise Routine from the National Institute on Aging at NIH
 Workout to Go A Sample Exercise Routine from the National Institute on Aging at NIH i Workout to Go Are you just starting to exercise? Getting back into a routine after a break? Wanting to keep up your
Workout to Go A Sample Exercise Routine from the National Institute on Aging at NIH i Workout to Go Are you just starting to exercise? Getting back into a routine after a break? Wanting to keep up your
Your Home Exercise Plan
 A Home Exercise Plan is designed for people who are unable to attend Pulmonary Rehabilitation classes in a community setting. This may be for a number of reasons such as travelling difficulties, personal
A Home Exercise Plan is designed for people who are unable to attend Pulmonary Rehabilitation classes in a community setting. This may be for a number of reasons such as travelling difficulties, personal
Guidelines for patients having. Achilles Tendon Repair. Achilles Tendon Repair
 Guidelines for patients having ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Achilles Tendon Repair Please stick addressograph
Guidelines for patients having ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Achilles Tendon Repair Please stick addressograph
Information for Patients having Total Knee Replacement Surgery
 Information for Patients having Total Knee Replacement Surgery Hello You will be coming into hospital for your surgery and we hope your stay will be pleasant. We have written this booklet to give you information
Information for Patients having Total Knee Replacement Surgery Hello You will be coming into hospital for your surgery and we hope your stay will be pleasant. We have written this booklet to give you information
Taking Care of Your Back
 Taking Care of Your Back Most people will feel back pain at some point in their lives, but not all back pain is the same for everyone. The good news is, most low back pain improves without any treatment
Taking Care of Your Back Most people will feel back pain at some point in their lives, but not all back pain is the same for everyone. The good news is, most low back pain improves without any treatment
Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life
 Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life. powered by WELLSTAR 360 Session 6: Overview Be Active It s Your Choice! This session focuses on how to become more physically
Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life. powered by WELLSTAR 360 Session 6: Overview Be Active It s Your Choice! This session focuses on how to become more physically
Lesson Sixteen Flexibility and Muscular Strength
 Lesson Sixteen Flexibility and Muscular Strength Objectives After participating in this lesson students will: Be familiar with why we stretch. Develop a stretching routine to do as a pre-activity before
Lesson Sixteen Flexibility and Muscular Strength Objectives After participating in this lesson students will: Be familiar with why we stretch. Develop a stretching routine to do as a pre-activity before
The In Bed Workout or the Getting Up Routine
 The In Bed Workout or the Getting Up Routine This is a great way to wake up and make good use of time. Just think, instead of lying there wasting 10 minutes thinking about getting up, you can complete
The In Bed Workout or the Getting Up Routine This is a great way to wake up and make good use of time. Just think, instead of lying there wasting 10 minutes thinking about getting up, you can complete
Golfers Stretch. for Success by Performing Exercises using the Body Bar Flex
 Golfers Stretch for Success by Performing Exercises using the Body Bar Flex Stretching before hitting your first golf ball can improve your game! Stretching before beginning in any sport can enhance your
Golfers Stretch for Success by Performing Exercises using the Body Bar Flex Stretching before hitting your first golf ball can improve your game! Stretching before beginning in any sport can enhance your
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: office@kneeclinic.info
MEDIAL TIBIAL STRESS SYNDROME (Shin Splints)
 MEDIAL TIBIAL STRESS SYNDROME (Shin Splints) Description Expected Outcome Shin splints is a term broadly used to describe pain in the lower extremity brought on by exercise or athletic activity. Most commonly
MEDIAL TIBIAL STRESS SYNDROME (Shin Splints) Description Expected Outcome Shin splints is a term broadly used to describe pain in the lower extremity brought on by exercise or athletic activity. Most commonly
BIG TOE FUSION. Patient Information
 Patient Information BIG TOE FUSION This may have been caused by an old injury, previous surgery or a long-standing bunion deformity. Pain at the joint can start to affect your daily activities and even
Patient Information BIG TOE FUSION This may have been caused by an old injury, previous surgery or a long-standing bunion deformity. Pain at the joint can start to affect your daily activities and even
Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises. Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises
 Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction Weight-bearing and resistance exercises have
Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction Weight-bearing and resistance exercises have
Ankle arthroscopy. If you have any further questions, please speak to a doctor or nurse caring for you
 Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Information about. Common conditions affecting the big toe (bunion and arthritis)
 Information about Common conditions affecting the big toe (bunion and arthritis) 2 Statement of Use The information in this leaflet is intended solely for the person to whom it was given by the health
Information about Common conditions affecting the big toe (bunion and arthritis) 2 Statement of Use The information in this leaflet is intended solely for the person to whom it was given by the health
Knee Replacement Recovery Guide
 Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
Knee Replacement Recovery Guide Table of Contents Congratulations!... 2 Recuperating At home... 2 Range of Motion... 2 Wound Care... 3 Important Signs & Symptoms... 3 Bathing and Showering... 3 Bruising...
The Complete Healthy Back System
 The Complete Healthy Back System Unlock Your Back Body s Healing The Healthy Checklist Potential Introduction Welcome to the Back to Life Healthy Back Checklist. This checklist is full of simple tips and
The Complete Healthy Back System Unlock Your Back Body s Healing The Healthy Checklist Potential Introduction Welcome to the Back to Life Healthy Back Checklist. This checklist is full of simple tips and
A Guide for People With Diabetes. Take Care of Your Feet for a
 A Guide for People With Diabetes Take Care of Your Feet for a You can take care of your feet! Do you want to avoid serious foot problems that can lead to a toe, foot, or leg amputation? Take Care of Your
A Guide for People With Diabetes Take Care of Your Feet for a You can take care of your feet! Do you want to avoid serious foot problems that can lead to a toe, foot, or leg amputation? Take Care of Your
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY
 A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
An information booklet for people using the Oswestry Standing Frame
 1 An information booklet for people using the Oswestry Standing Frame 2 Introduction A physiotherapist has visited you at home to show you how to use the standing frame. You will also have been given a
1 An information booklet for people using the Oswestry Standing Frame 2 Introduction A physiotherapist has visited you at home to show you how to use the standing frame. You will also have been given a
Shoulder Surgery Discharge Instructions
 Note: This information is provided for general educational purposes only. Because every individual is different, these instructions will not apply to every patient. Only your doctor can tell you what is
Note: This information is provided for general educational purposes only. Because every individual is different, these instructions will not apply to every patient. Only your doctor can tell you what is
Back Protection. Training Guide
 Back Protection Training Guide Use a Back Support Belt to Prevent Back Injuries Because of the incidious progression of back problems, it is always difficult to determine how a back problem began. If you
Back Protection Training Guide Use a Back Support Belt to Prevent Back Injuries Because of the incidious progression of back problems, it is always difficult to determine how a back problem began. If you
Everything you need to know to feel prepared for your walk
 Everything you need to know to feel prepared for your walk Thank you for joining Team Macmillan. We think you re amazing for having the dedication and commitment to organise your walk in aid of Macmillan.
Everything you need to know to feel prepared for your walk Thank you for joining Team Macmillan. We think you re amazing for having the dedication and commitment to organise your walk in aid of Macmillan.
Bunion surgery. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Bunion surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information in this
Bunion surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information in this
Cardiac Rehabilitation
 Cardiac Rehabilitation Home Exercise Programme Information for patients Active Programmes Patient s name: Start date: page of What is the home exercise programme? The home exercise programme can be followed
Cardiac Rehabilitation Home Exercise Programme Information for patients Active Programmes Patient s name: Start date: page of What is the home exercise programme? The home exercise programme can be followed
KNEE AND LEG EXERCISE PROGRAM
 KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
Important Safety Instructions 1-2. Maintenance 3. Features 4. Assembly Parts List 5. Assembly Instructions 6-9. Console Operation 10
 Important Safety Instructions 1-2 Maintenance 3 Features 4 Assembly Parts List 5 Assembly Instructions 6-9 Console Operation 10 Moving Machine 12 Exercise Instructions 13-18 Exploded Drawing 19 Parts List
Important Safety Instructions 1-2 Maintenance 3 Features 4 Assembly Parts List 5 Assembly Instructions 6-9 Console Operation 10 Moving Machine 12 Exercise Instructions 13-18 Exploded Drawing 19 Parts List
Knee Pain Solutions. Assess Your Pain. Make a Plan. Take Action
 Knee Pain Solutions Assess Your Pain Make a Plan Take Action By Jared Evans Certified Strength and Conditioning Specialist Giammalva Fitness Director There are many different causes of knee pain and understanding
Knee Pain Solutions Assess Your Pain Make a Plan Take Action By Jared Evans Certified Strength and Conditioning Specialist Giammalva Fitness Director There are many different causes of knee pain and understanding
RESISTANCE BANDS TOP TEN BANDS EXERCISES INSIDE
 RESISTANCE BANDS TOP TEN BANDS EXERCISES INSIDE COPYRIGHT 321 STRONG, ALL RIGHTS RESERVED http://321strong.com/ 321 STRONG Resistance Band ebook Table of Contents Welcome to the world of 321 STRONG...
RESISTANCE BANDS TOP TEN BANDS EXERCISES INSIDE COPYRIGHT 321 STRONG, ALL RIGHTS RESERVED http://321strong.com/ 321 STRONG Resistance Band ebook Table of Contents Welcome to the world of 321 STRONG...
Resistance Training Program
 Name: Resistance Training Program How to do Resistance Training: Warm up for 5 minutes before resistance training e.g., walk or cycle slowly o Avoid stretching before resistance training Do all exercises
Name: Resistance Training Program How to do Resistance Training: Warm up for 5 minutes before resistance training e.g., walk or cycle slowly o Avoid stretching before resistance training Do all exercises
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg)
 MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
Foot and Ankle Conditioning Program
 Foot and Ankle Conditioning Program Studies show, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. A program of this nature, focused
Foot and Ankle Conditioning Program Studies show, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. A program of this nature, focused
Starting a Strength Training Program
 MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Starting a Strength Training Program About This Kit The key to improving strength is applying resistance to the muscle
MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Starting a Strength Training Program About This Kit The key to improving strength is applying resistance to the muscle
Therapy following a neck of femur fracture
 INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
