A new surgical technique for scleral fixation using a knot ball for scleral-fixated intraocular lenses: impact on clinical outcomes
|
|
|
- Rose Kelley
- 5 years ago
- Views:
Transcription
1 Original Article A r q u i v o s b r a s i l e i r o s d e A new surgical technique for scleral fixation using a knot ball for scleral-fixated intraocular lenses: impact on clinical outcomes Uma nova técnica cirúrgica para fixação escleral usando um nó esférico (knot ball) para lentes ıntraoculares para fixação escleral: impacto nos resultados clínicos Alper Mete 1, Sabit Kimyon 1, Oguzhan Saygılı 1, Yusuf Koçluk 2, Iffet Yarımağa Kaçarlar 1, Kıvanç Güngör 1, Mithat Temizer 3 1. Department of Ophthalmology, School of Medicine, Gaziantep University, Gaziantep, Turkey. 2. Department of Ophthalmology, Adana Numune Training and Research Hospital, Adana, Turkey. 3. Turkish Public Health Institute, Public Health Center, Gaziantep, Turkey. ABSTRACT Purpose: Scleral fixation surgery is a pivotal procedure that depends on the availability of robust and innovative surgical fixation methods. There continues to be a need for innovation in suture fixation techniques, particularly for intraocular lens implantation. Methods: We conceived and designed a knot ball scleral fixation technique for suture burial in a retrospective sample of 108 patients with primary (n=40) or secondary (n=68) scleral-fixated intraocular lens. Importantly, our technique did not require additional scleral flap or tunnel procedures. We evaluated pre- and postoperative best-corrected visual aquity (BCVA) and postoperative complications. All data were analyzed and compared between groups. Results: The preoperative mean BCVA improved significantly in both groups using the knot ball fixation technique (p<0.01). The extent of the improvement in the best-corrected visual acuity and late complications one month post-surgery were not significantly different between the groups (p>0.05). These clinical outcomes were consistent with those described in the ophthalmology literature. Conclusion: A knot ball scleral fixation technique is reported; to the best of our knowledge, this is the first report of such a technique, which offers a less invasive and simplified surgical procedure for transscleral fixation of scleral-fixated intraocular lenses. Moreover, the technique appears to display Submitted for publication: October 18, 2017 Accepted for publication: January 8, 2018 Funding: No specific financial support was available for this study. Disclosure of potential conflicts of interest: None of the authors have any potential conflict of interest to disclose. Corresponding author: Alper Mete. Gaziantep University Hospital. Department of Ophthalmology - Gaziantep Turkey - dralpermete@hotmail.com Approved by the following research ethics committee: Gaziantep University Hospital (#187/2015). similar effectiveness and safety compared with existing scleral fixation techniques. We suggest that the knot ball technique warrants further research focus and clinical evaluation in future studies. Keywords: Sclera/surgery; Lens implantation; Intraocular; Aphakia; Sutures techniques RESUMO Objetivo: A cirurgia de fixação escleral é um pro - cedimento fundamental que depende da disponibilidade de métodos robustos e inovadores de fixação cirúrgica. No entanto, existe uma necessidade de inovação nas técnicas de fixação de sutura, particularmente para a implantação de lentes intraoculares. Métodos: Concebemos e desenhamos uma técnica de fixação escleral utilizando um nó esférico para o encerramento da sutura em uma amostra retrospectiva de 108 pacientes com lente intraocular de fixação escleral (SF-IOL) primária (n=40) e secundária (n=68). Importante considerar que nossa técnica não exigiu procedimentos adicionais de aleta escleral ou de túnel. Observamos a melhor acuidade visual corrigida (MAVC) pré e pós-operatória e as complicações pós-operatórias. Todos os dados foram analisados entre os grupos. Resultados: A melhor acuidade visual corrigida média pré-operatória (logmar) melhorou significativamente em ambos os grupos com a utilização da técnica de fixação do nó esférico (p<0,01). A extensão da melhora melhor acuidade visual corrigida e as complicações tardias, um mês após a cirurgia, não foram significativamente diferentes entre os grupos (p>0,05). Esses resultados clínicos foram, em geral, comparáveis aos publicados na literatura de oftalmologia. Conclusão: Até onde sabemos, a técnica de fixação escleral de nó esférico é relatada pela primeira vez na li teratura e representa um procedimento cirúrgico promissor, menos invasivo e simplificado para a fixação transescleral de SF-IOLs. Além disso, a técnica parece exibir eficácia e segurança comparáveis às técnicas de fixação escleral existentes. Sugerimos This content is licensed under a Creative Commons Attributions 4.0 International License. 302 Arq Bras Oftalmol. 2018;81(4):
2 Mete A, et al. que a técnica do nó esférico receba mais atenção e avaliações clínicas no futuro. Descritores: Esclera/cirurgia; Implante de lente intraocular; Afacia; Técnicas de sutura INTRODUCTION Innovation in ophthalmic surgery is an area of intense research in which new technologies or procedural improvements might offer the promise of improved clinical outcomes. In this context, scleral fixation surgery is a crucial procedure which depends on the availability of robust scleral fixation methods. There is a particular need for new approaches in suture fixation techniques for intraocular lens implantation to make the procedures less invasive. In the absence of sufficient capsular support, scleral-fixated (SF) posterior chamber intraocular lenses (IOLs), anterior chamber IOLs (ACIOLs), iris-claw IOLs, or iris-sutured posterior chamber IOLs are used for surgical treatment of aphakia (1). Previous studies have suggested that transscleral fixation of posterior chamber IOLs has significant advantages over other implantation techniques in the context of prevention of various complications, including corneal endothelial damage, pupillary block glaucoma, hyphemia, uveitis, iris damage, IOL dislocation, and pseudophakodonesis (2-4). Transscleral fixation of posterior chamber IOLs can be performed using suture or sutureless techniques (5). Suture techniques need to cover, bury, or rotate suture knots to prevent suture-related complications (2,3). Numerous techniques have been described for avoiding suture exposure and suture-related complications such as creating a scleral flap for suture knots (6), suturing into a scleral groove (7) or pocket (8), burying the suture ends into a scleral tunnel (9), direct suture burial without a flap, tunnel, incision, or groove (10), covering the suture knots with fascia lata, tenon s capsule (11), cornea, or scleral autograft (12), knotless Z-suture techniques (13), sutureless techniques using fibrin glue, and trocar- or needle-assis ted techniques (14-16). The ideal transscleral fixation techni que should be simple, quick, minimally invasive, safe, effective, and offer easy management of potential surgical complications. Here, we present a simple, quick, minimally invasive, and effective alternative technique, a new knot ball scleral fixation technique for burying ball-shaped suture knots directly into the sclera for transscleral fixation of SFIOL; we compared the visual outcomes and complications in primary and secondary implantations using our technique. METHODS Subjects We retrospectively analyzed the medical records of 108 patients (65 males, 43 females; 108 eyes) who underwent SFIOL implantation surgery with our new knot ball scleral fixation technique without creating a scleral flap, groove, or tunnel. The study and analysis were conducted at the Gaziantep University Hospital between March 2014 and October This study was approved by the institutional research ethics board and adhered to the tenets of the Declaration of Helsinki. All patients had a complete preoperative evaluation, including best-corrected visual acuity (BCVA) and IOP measurements, and slit-lamp and fundus examinations. Subjects were informed about the procedure, potential complications, and possible need for secondary surgery The indications for SFIOL implantation were extensive capsular deficiency, crystalline lens subluxation preventing safe and stable IOL implantation in the bag or sulcus, corneal decompensation due to ACIOL, IOL su bluxation due to trauma, or pseudoexfoliation syndrome. The decision regarding primary or secondary implantation was made based on the preference of the surgeon depending on the type of anesthesia, comfort, and general medical condition of the patient. All surgeries were performed using the new knot ball suture fixation technique by two experienced surgeons (O.S. and A.M.). Patients who were followed up for at least nine months were included in the study. Intraoperative and postoperative complications and visual outcomes were noted. All data were compared between groups. The knot ball scleral fixation technique Figure 1 and 2 show the steps involved in SFIOL implantation using our technique. In brief, the procedure comprised the following steps and details. Preoperatively, IOL power was calculated using the Sanders-Retzlaff-Kraff II formula. Pupils were dilated with 1% tropicamide, 2.5% phenylephrine hydrochloride, and 1% cyclopentolate. The periocular area and eye were cleaned with 5% povidone iodine. In the primary implantation group, the procedure was initiated as a standard phacoemulsification or extracapsular cataract extraction surgery with a corneal incision at the 12 o clock meridian. If there were any posterior capsule or lens zonule complications during cataract surgery, corneal incision was enlarged to approximately 6.5 to 7.0 mm, and lens fragments were explanted. In the secondary implantation group (aphakic Arq Bras Oftalmol. 2018;81(4):
3 A new surgical technique for scleral fixation using a knot ball for scleral-fixated intraocular lenses: impact on clinical outcomes or pseudophakic), a 6.5 to 7.0 mm clear corneal incision was created at the 12 o clock meridian, and any subluxated IOL or ACIOL was explanted in pseudophakic cases. Surgeries in both groups were continued as following. Limbus-parallel conjunctival peritomies (~2 mm) were created at 3 o clock and 9 o clock meridians 2 mm behind the limbus. The sclera was not cauterized and only cotton buds were used for bleeding control in all patients. Next, triamcinolone acetonide (0.5 cc) was injected into the anterior chamber to stain the vitreous for direct visualization and anterior vitrectomy was performed using a 20-gauge vitrectomy cutter. The 10-0 closed-loop polypropylene suture (PC-9, ALCON, Fort Worth, Texas or MANI Inc., Togichi, Japan) ends were attached to the haptics of a PSV 651 single piece polymethylmethacrylate SFIOL (FREEDOM, Tamil Nadu, India). Subsequently, half of the curved needle was passed directly through the sclera approximately 2 mm behind the limbus at the 3 o clock meridian. A micro hole was made at the sclera-curved needle junction using the tip of a 20-gauge microvitreoretinal (MVR) blade under a high magnification surgical microscope (Figure 1F-H, Figure 3A). Next, the same procedure was performed on the opposite side (i.e., 9 o clock meridian). While implanting each haptic of the SFIOL into the posterior chamber, the curved needle was gently pulled. A B C D E F G H Figure 1. A-B) We planned phacoemulsification cataract surgery in this case. However, we performed extracapsular cataract extraction due to posterior and anterior capsule deficiency during surgery. C-D) Next, limbus-parallel conjunctival peritomies (~2 mm) were created at 3 o clock and 9 o clock meridians 2 mm behind the limbus, and anterior vitrectomy was performed. E) The 10-0 closed-loop polypropylene suture ends were attached to the haptics of the SFIOL. F-H) After half of the curved needle was passed directly through the sclera approximately 2 mm behind the limbus, we made a micro hole at the sclera-curved needle junction using the tip of a 20-gauge MVR blade under a high magnification surgical microscope. Next, the same procedure was performed for the second haptic and the SFIOL was implanted into the posterior chamber. A B C D E F G H Figure 2. A-D) The closed-loop suture was cut at a distance of approximately cm from the needle perforation in the sclera. Thus, two fibers were formed from the closed-loop suture, and we separated these fibers. Subsequently, the knot ball was created in a fashion using both suture fibers of the 10 0 closed-loop polypropylene suture. We buried the knot ball directly into the steep scleral tunnel formed by the curved needle and the tip of the 20-gauge MVR blade without any additional procedures. Next, we cut the suture ends using 20-G microscissors under a high magnification surgical microscope. E-G) The same fixation procedure was performed for the opposite side. H) The corneal incision was closed with three 10/0 cornea-scleral sutures and conjunctival peritomies were closed using 8/0 vicryl sutures. 304 Arq Bras Oftalmol. 2018;81(4):302-9
4 Mete A, et al. After implantation, the closed-loop suture was cut approximately 1.5 to 2.0 cm away from the needle-per forated scleral point so that two fibers were formed from the closed-loop suture; these fibers were separated for suturing (Figure 3B). The knot was tied in a fashion using both suture fibers of the 10-0 closed-loop polypropylene suture to create a ball-shaped knot for scleral fixation (Figure 3C). We buried the knot ball directly into the steep scleral tunnel which was formed by the curved- -needle and the tip of a 20-gauge MVR blade without any additional procedures (Figure 3D). The IOL manipulator was used for achieving centralization of the SFIOL and checking the burial of the ball-shaped suture knot. The corneal incision was closed using 10-0 monofilament nylon sutures and conjunctival pe ritomies were closed using 8-0 absorbable sutures. Finally, an antibiotic was delivered into the anterior chamber. Postoperatively, topical antibiotic and steroid drops were administered six times a day for four weeks and anti-glaucomatous drops were administered when required. Follow-up examinations were performed on the first day, the first week, and then monthly after the surgical procedure. Figure 4 shows the postoperative status of two patients. Patient demographics, preoperative and postoperative BCVAs, follow-up periods, preoperative lens status of eyes, and postoperative complications were noted. The BCVAs were measured in decimal units and converted into logarithms of the minimal angle of resolution (logmar) units for analysis. Visual acuities of hand movement and light perception were converted into equivalents of 1.7 and 1.8 logmar units, respectively (17,18). Statistical analyses The software SPSS 16.0 for Windows (SPSS Inc, Chicago, IL, USA) was used to analyze outcomes and changes in the study endpoints. Patient demographics, follow-up periods, and postoperative complications were compared between primary and secondary SFIOL implanted groups using Chi-squared tests. Preoperative and postope rative BCVAs were statistically analyzed using paired samples t-tests. A p-value less than 0.05 was considered significant. A C Figure 3. A) After half of the curved needle was passed directly through the sclera approximately 2 mm behind the limbus, we made a micro hole at the sclera-curved needle junction using the tip of a 20-gauge MVR blade under a high magnification surgical microscope. B) The closed-loop suture was cut at a distance of approximately cm from the needle perforation in the sclera. Thus, two fibers were formed from the closed-loop suture and we separated these fibers. C) The knot ball was created in a fashion using both suture fibers of the 10-0 closed-loop polypropylene suture. D) We buried the knot ball directly into the steep scleral tunnel formed by the curved needle and the tip of the 20-gauge MVR blade without any additional procedures. B D RESULTS We performed the knot ball technique in 40 eyes (37.1%) with primary implantation (the primary group) and in 68 eyes (62.9%) with secondary implantation (the secondary group). Patient characteristics, length of the follow-up period, and preoperative and postoperative BCVAs are summarized in table 1. There were no statistically significant differences between the study groups in age, gender, duration of follow-up, preoperative BCVA, or postoperative BCVA (p>0.05 for all analyses). Indications for SFIOL implantation and preoperative lens status of cases are summarized in table 2. A B C D E Figure 4. A) Postoperative 9 th month follow-up anterior segment photograph of a 54-year-old woman who underwent primary SFIOL implantation due to complicated cataract surgery. B.C.D.E) Postoperative 2 nd month follow-up anterior segment photographs of a 7-year-old boy who underwent secondary SFIOL implantation surgery due to dislocation of a previously implanted PCIOL. Arq Bras Oftalmol. 2018;81(4):
5 A new surgical technique for scleral fixation using a knot ball for scleral-fixated intraocular lenses: impact on clinical outcomes The preo perative mean BCVAs (logmar) were 1.13 ± 0.41 in the primary group and 1.14 ± 0.31 in the secondary group. Postoperative mean BCVAs were 0.55 ± 0.32 in the primary group and 0.65 ± 0.34 in the secondary group. There were no statistically significant Table 1. Clinical and demographic characteristics of patients Primary Secondary P* value Gender 0.108* Male 20 (50) 45 (66.2) Female 20 (50) 23 (33.8) Age, years 0.691* Mean + SD 51.4 ± 21.5 Range (5-79) 53.2 ± 24.1 (5-82) Follow-up period, months 0.083* Mean + SD 11.5 ± 2.3 Range (9-18) BCVA (logmar) Preoperative BCVA (Mean + SD) Range Postoperative BCVA (Mean + SD) Range 1.13 ± 0.41 ( ) 0.55 ± 0.32 ( ) 10.7 ± 1.9 (9-17) 1.14 ± 0.31 ( ) 0.65 ± 0.34 ( ) 0.840* 0.127* SD= Standard deviation; BCVA= best-corrected visual acuity; logmar= Logarithm of the minimum angle of resolution; *= Chi-squared test was used; = BCVA of a patient who had no perception of light after surgery was excluded from the statistical analyses in the primary group. differences in preoperative and postoperative mean BCVAs between the groups (p=0.840 and p=0.127, respectively). In the primary group, BCVA improved in 33 (82.5%) eyes and remained unchanged in three (7.5%), while in the secondary group, BCVA improved in 60 (88.2%) eyes and remained unchanged in six (8.8%). The postoperative BCVA improved statistically significantly compared with the preoperative BCVA in both groups (p<0.01 for both groups). Deterioration of vision occurred in four (10%) eyes (suprachoroidal hemorrhage, n=1; retinal detachment, n=1; cystoid macular edema, n=1; endophthalmia, n=1) in the primary group and in two (2.9%) eyes (cystoid ma cular edema, n=1; IOL dislocation, n=1) in the secondary group. Postoperative complications are summarized in table 3. During the early postoperative period, complications occurred in 20 (50%) and 13 (19.1%) eyes in the primary and secondary groups, respectively. There was a statistically significant difference between groups in incidence of early complications (p=0.02). Transient IOP elevation and transient corneal edema were the most common complications in both groups during the early period. These patients were treated successfully using anti-glaucomatous and steroid drops in both groups. In the primary group, four (10%) eyes required secondary Table 3. Summary of postoperative complications Table 2. Preoperative lens status of eyes Phakic Primary Secondary Complicated phacoemulsification 25 (62.5) - Complicated ECCE 05 (12.5) - Subluxated lens due to pseudoexfoliation syndrome 05 (12.5) - Marfan Syndrome 05 (12.5) - Aphakic Complicated phacoemulsification - 15 (22.1) Complicated ECCE - 05 (07.4) Previous severe trauma - 23 (33.8) Dislocated previously implanted PCIOL - 09 (13.2) Removal of PCIOL as a result of endophthalmitis Pseudophakic - 01 (01.5) Dislocated previously implanted PCIOL - 12 (17.6) Complicated ACIOL - 03 (04.4) ECCE= extracapsular cataract extraction; PCIOL= posterior chamber intraocular lens; ACIOL= anterior chamber intraocular lens. Early period complications (within one month) Primary Secondary Transient IOP elevation 06 (15.0) 3 (4.4) Transient corneal edema 05 (12.5) 4 (5.9) Pupil distortion 04 (10.0) 3 (4.4) Anterior chamber hemorrhage 02 (05.0) 1 (1.5) IOL dislocation 03 (07.5) 2 (2.9) Vitreous hemorrhage 01 (02.5) 1 (1.5) Suprachoroidal hemorrhage 01 (02.5) - Endophthalmia 01 (02.5) - Late period complications (after one month) Glaucoma 04 (10.0) 2 (2.9) Suture exposure 02 (05.0) 2 (2.9) IOL decentration 01 (02.5) 2 (2.9) Conjunctival cyst due to suture 02 (05.0) 2 (2.9) Cystoid macular edema 01 (01.5) 1 (1.4) Retinal detachment 01 (02.5) - P* value 0.02* 0.139* IOP= intraocular pressure; IOL= intraocular lenses; *= Chi-square test was used. 306 Arq Bras Oftalmol. 2018;81(4):302-9
6 Mete A, et al. surgical intervention due to early period complications (IOL dislocation, n=2; suprachoroidal hemorrhage, n=1; endophthalmitis, n=1). Eyes with IOL dislocation were treated successfully and an increase in visual acuity was attained after the secondary intervention. The BCVA deteriorated only in two patients. One patient (with fungal endophthalmitis) had no perception of light, and another patient (with suprachoroidal hemorrhage) had light perception following secondary surgical interventions. Endophthalmitis occurred two days after surgery, indicating that it may be related to intraoperative contamination. In the secondary group, secondary surgical intervention was not required for any patient. There was no statistically significant difference between groups in the incidence of late postoperative period complications (p=0.139). Late postoperative period complications were observed in 11 (27.5%) and nine (13.2%) eyes in the primary and secondary groups, respectively. Glaucoma (four eyes) was the most common late postoperative period complication in the primary group. These patients were successfully treated using anti-glaucomatous drops. In the secondary group, one of the glaucoma cases was treated with anti-glaucomatous drops, while the other one was treated using surgical intervention. We observed IOL decentration in one eye in the primary group and in two eyes in the secondary group. We performed secondary surgical intervention in these three eyes due to deteriorated vision. Suture exposure occurred in two (5%) eyes in the primary group and in two (2.9%) eyes in the secondary group. We treated all these cases using cauterization (14). Retinal detachment occurred in one patient (2.5%) in the primary group who required secondary surgical intervention. Overall, eight (20%) eyes in the primary group and five (7.4%) eyes in the secondary group required secondary surgical interventions due to postoperative complications. Our outcomes showed that there was no significant difference between groups in the requirement of secondary surgical intervention (p=0.159). We observed cystoid macular edema in one patient in the primary group (1.5%) and in one patient (1.4%) in the secondary group, with spontaneous resolution occurring in both cases. DISCUSSION There have been several methods of transscleral fixation of posterior chamber intraocular lenses (PCIOLs). Among these, the triangular scleral flap is one of the most commonly used techniques worldwide. However, this technique extends surgery duration, requires more scleral bleeding control during surgery, and atrophy in scleral flaps may occur over time (20). Hoffman et al. (8) described a minimally invasive technique without conjunctival dissection, in which scleral pockets were created through peripheral clear corneal incisions. However, this technique requires passing twice through the sclera for each haptic fixation and corneal incision. Additionally, Hoffman s technique presents a potential risk of astigmatism compared with other techniques. Some authors have reported the use of scleral grooves instead of scleral flaps for transscleral fixation (21-23). The scleral groove technique and its modifications reduce surgery duration and the rate of suture-related complications. However, the scleral groove technique and its modifications require at least two passes through the sclera, additional incisions for scleral grooves, additional sutures for grooves, and risk of vitreous hemorrhage due to scleral passes remains. Kir et al. (9) have described a scleral tunnel technique for burying suture ends into the scleral tunnel without creating a scleral flap pocket or grooves. However, this technique requires additional suturing procedures for free suture ends. Some surgeons have described graft or tissue-dependent techniques such as covering the suture knots with fascia lata, tenon s capsule (11), or corneal or scleral autograft (12) ; however, these techniques present disadvantages, including the requirement of additional surgical procedures and prolonged surgery duration. Baykara (10) has described a technique for suture knot burying into the sclera without flaps, tunnels, or grooves. The new technique we developed and described in this report, the knot ball scleral fixation approach, displays some similarities to the Baykara s direct suture burial technique. Yet, there are also important distinctions in that we pass only once through the sclera for each haptic and we create a ball-shaped suture knot ball, which is then embedded into the steep scleral tunnel formed by the passage of the curved suture needle and the tip of a 20-gauge MVR blade, without any additional procedures. Some surgeons have described knotless techniques for transscleral fixation of PCIOLs. Kongsap (1) described knotless zigzag scleral fixation for PCIOLs. This technique is a safe and viable option that reduces surgery duration and postoperative suture-re lated complications. However, Kongsap s technique re quires multiple passes through the sclera for each haptic. Sutureless techniques for scleral fixation of PCIOLs have become increasingly popular (14-16,24,25). Gabor and Pavlidis (24) introduced su tureless transscleral fixation of a three-piece PCIOL. Arq Bras Oftalmol. 2018;81(4):
7 A new surgical technique for scleral fixation using a knot ball for scleral-fixated intraocular lenses: impact on clinical outcomes Agarwal et al. (14) presented a fibrin glue-assisted technique in which the intrascleral haptic of a PCIOL is fixed into a scleral tunnel. Totan and Karadağ (15) presented a trocar-assisted sutureless transscleral fixation technique, and Yamane et al. (16) presented a 27-gauge needle-assisted transscleral fixation technique. However, these sutureless techniques have the potential risk of haptic exposure and require scleral flaps, tunnels, or fibrin glue. Ohta et al. (25) described a sutureless Y-fixation technique that was used to fix a PCIOL without large lamellar scleral flaps or fibrin glue. This technique eliminates the risk of haptic exposure without creating large scleral flaps or using fibrin glue. However, scleral incisions and mini flaps are needed for this technique. We thought that transscleral suture fixation techniques are safer than sutureless techniques because current commercially available IOLs are specially designed for transscleral suture fixation. Our outcomes showed that the rate of early and late postoperative complications and postoperative visual outcomes were similar to those in previous reports (6,26). Lee et al. (26) performed transscleral PCIOL fixation in 55 patients using an ab externo sulcus fixation technique, which was described by Lewis in 1991 (27). They reported that early-period complications occurred in 25 (83.3%) eyes in the primary group and in 16 (64%) eyes in the secondary group. They showed that early-period complications were statistically significantly higher in the primary group. Late-period postoperative complications occurred in 21 (70.0%) eyes in the primary group and in 13 (52.0%) eyes in the secondary group, with no significant differences between the groups regarding late-period complications. Yalniz-Akkaya et al. (6) performed transscleral SFIOL fixation using a triangular scleral flap technique; they reported that early-period postoperative complications occurred in 13 (35.1%) eyes in the primary group and in 17 (28.8%) eyes in the secondary group. The authors showed that late-period postoperative complications occurred in 30 (81.0%) eyes in the primary group and in 40 (67.9%) eyes in the secondary group. They reported no statistically significant differences between groups in early or late postoperative complications. In our study, early postoperative complications occurred in 20 (50%) eyes in the primary group and in 13 (19.1%) eyes in the secondary group. We showed a statistically significant difference between the groups regarding incidence of early postoperative complications (p=0.02). Early postoperative complications mostly occurred in the primary group, but late postoperative complication rates were not significantly different between the primary and secondary implantation groups. Moreover, there was no significant difference in visual outcomes between the groups. We suggest that the decision regarding primary or secondary implantation should be made based on patient characteristics and experience of the surgeon. Lee et al. (26) showed that the mean postoperative logmar BCVA was 0.50 and 0.36 in the primary and secondary groups, respectively. Akkaya et al. (6) reported that the mean postoperative logmar BCVA in the primary group was 0.50 and that in the secondary group was 0.5. In both studies, the authors showed no statistically significant difference between the groups in terms of visual outcomes. Similarly, there was no significant difference between the groups in mean postoperative logmar BCVA in our study. The knot ball scleral-fixation technique we describe eliminates risky maneuvers such as creating scleral flaps, tunnels, grooves, or two or more scleral perforations for fixation of each haptic. Moreover, this technique provides sufficient IOL centration, minimizes postoperative com plications, and reduces surgery time and scleral he morrhage during surgery. Our technique is especially helpful in treatment of IOL dislocations because it is less invasive and is easier than other methods. The dislocated IOL haptic can easily be refixated with only one pass through the sclera. However, our modified technique involves some critical steps. First, the burial extent of the first three loop-like sutures of the knot is the first critical step, which needs experience; if the suture knot is excessively buried, this may cause IOL decentration and dislocation due to the short steep scleral tunnel formed by the curved needle and the tip of the 20-gauge MVR blade. On the other hand, insufficient burial of the suture knot may cause suture-related complications. The second critical step in our technique is the cutting of the suture ends to make them as short as possible. We performed this step very carefully under a high magni fication surgical microscope using 20- or 23-gauge mi croscissors. Thus, potential suture-related complications can be substantially prevented. Our study had some limitations due to the development of a new scleral-fixation technique: its retrospective nature, the variable duration of follow-up, and the heterogeneous preoperative indications. Scleral-fixation techniques need to cover, bury, or rotate suture knots to prevent overlying conjunctival erosion and suture-related complications. The knot ball scleral-fixation technique is a simple, less invasive, safe, and 308 Arq Bras Oftalmol. 2018;81(4):302-9
8 Mete A, et al. effective alternative method for transscleral fixation of SFIOLs. Our results were based on a short-term follow-up period. Prospective, randomized studies with longer follow-up periods are required to verify the safety and efficacy of primary and secondary SFIOL implantations using our new technique. REFERENCES 1. Kongsap P. A knotless, one-haptic fixation of posterior chamber intraocular lenses: one-year results. Int J Ophthalmol. 2015;18;8(1): Wagoner MD, Cox TA, Ariyasu RG, Jacobs DS, Karp CL; American Academy of Ophthalmology. Intraocular lens implantation in the absence of capsular support: a report by the American Academy of Ophthalmology. Ophthalmology. 2003;110(4): McAllister AS, Hirst LW. Visual outcomes and complications of scleral fixated posterior chamber intraocular lenses. J Cataract Refract Surg. 2011;37(7): Comment in: J Catarct Refract Surg. 2011;37(11): Apple D, Mamalis N, Loftfield K, Googe JM, Novak LC, Kavka-Van Norman D, et al. Complications of intraocular lenses: a historical and histopathological review. Surv Ophthalmol. 1984;29(1):l Sindal MD, Nakhwa CP, Sengupta S. Comparison of sutured versus sutureless scleral-fixated intraocular lenses. J Cataract Refract Surg. 2016;42(1): Yalniz-Akkaya Z, Burcu A, Uney GO, Abay I, Eksioglu U, Acar MA, et al. Primary and secondary implantation of scleral-fixated posterior chamber intraocular lenses in adult patients. Middle East Afr J Ophthalmol. 2014;21(1):44-9. Comment in: Middle East Afr J Ophthalmol. 2014;21(4): Lin CP, Tseng HY. Suture fixation technique for poste rior chamber intraocular lenses. J Cataract Refract Surg. 2004;30(7): Hoffman RS, Fine IH, Packer M. Scleral fixation without conjunctival dissection. J Cataract Refract Surg. 2006; 32(11): Kir E, Kocaturk T, Dayanir V, Ozkan SB, Dündar SO, Aktunç TO. Prevention of suture exposure in transscleral intraocular lens fixation: an original technique. Can J Ophthalmol. 2008;43(6): Baykara M. Suture burial technique in scleral fixation. J Cataract Refract Surg. 2004;30(5): Bashshur Z, Ma luf R, Najjar D, Noureddin B. Scleral fixation of posteriorchamber intraocular lenses using fascia lata to cover the knots. Ophthalmic Surg Lasers. 2002;33(6): Bucci FA Jr, Holland EJ, Lindstrom RL. Corneal auto grafts for externalknots in transsclerally sutured posterior chamber lenses. Am J Ophthalmol. 1991;112(3): Szurman P, Petermeier K, Aisenbrey S, Spitzer MS, Jaissle GB. Z-suture: a new knotless technique for transscleral suture fixation of intraocular implants. Br J Ophthalmol. 2010;94(2): Agarwal A, Kumar DA, Jacob S, Baid C, Agarwal A, Srinivasan S. Fibrin glue assisted sutureless posterior chamber intraocular lens implantation in eyes with deficient posterior capsules. J Cataract Refract Surg. 2008;34(9): Comment in: J Cataract Refract Surg. 2009;35(5):795; author reply Totan Y, Karadag R. Trocar-assisted sutureless intrascleral posterior chamber foldable intra-ocular lens fixation. Eye (Lond). 2012; 26(6): Yamane S, Inoue M, Arakawa A, Kadonosono K. Sutureless 27-gauge needle-guided intrascleral intraocular lens implantation with lamellar scleral dissection. Oph thalmology. 2014;121(1):61-6. Comment in: Ophthalmology. 2014;121(8):e42-3. Ophthalmology. 2014;121(8):e Chan TC, Lam JK, Jhanji V, Li EY. Comparison of outcomes of primary anterior chamber versus secondary scleral-fixated intraocular lens implantation in complicated cataract surgeries. Am J Ophthalmol. 2015;159(2):221-6.e2. Comment in: Am J Ophthal mol. 2015; 160(1): Am J Ophthalmol. 2015;160(1): Luk AS, Young AL, Cheng LL. Long-term outcome of scleral-fixated intraocular lens implantation. Br J Ophthalmol. 2013;97(10): Hu XT, Zhang ZD, Zhou R, Pan QT. Cauterization technique for suture erosion in transscleral fixation of intraocular lenses. Int J Ophthalmol. 2013;18;6(6): Por YM, Lavin MJ. Techniques of intraocular lens suspension in the absence of capsular/zonular support. Surv Ophthalmol. 2005; 50(5): Friedberg MA, Berler DK. Scleral fixation of posterior chamber intraocular lenses combined with vitrectomy. Ophthalmic Surg. 1992; 23(1): Almashad GY, Abdelrahman AM, Khattab HA, Samir A. Four-point scleral fixation of posterior chamber intraocular lenses without scleral flaps. Br J Ophthalmol. 2010;94(6): Lin CP, Tseng HY. Suture fixation technique for posterior chamberintraocular lenses. J Cataract Refract Surg. 2004;30(7): Gabor SG, Pavlidis MM. Sutureless intrascleral posterior chamber intraocular lens fixation. J Cataract Refract Surg. 2007;33(11): Comment in: Retina. 2014; 34(4): Ohta T, Toshida H, Murakami A. Simplified and safe method of sutureless intrascleral posterior chamber intraocular lens fixation: Y-fixation technique. J Cataract Refract Surg. 2014;40(1):2-7. Comment in: J Cataract Refract Surg. 2014;40(5): Lee VY, Yuen HK, Kwok AK. Comparison of outcomes of primary and secondary implantation of scleral fixated posterior chamber intraocular lens. Br J Ophthalmol. 2003;87(12): Lewis JS. Ab externo sulcus fixation. Ophthalmic Surg. 1991;22(11): Arq Bras Oftalmol. 2018;81(4):
Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular Lens in Previous Vitrectomized Eyes
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(2):181-185 http://dx.doi.org/10.3341/kjo.2014.28.2.181 Case Report Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(2):181-185 http://dx.doi.org/10.3341/kjo.2014.28.2.181 Case Report Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular
Visual outcome and early complications of sutureless and glueless scleral fixated intraocular lens
 Original article Visual outcome and early complications of sutureless and glueless scleral fixated intraocular lens Lalit Agarwal, Nisha Agrawal, Rajya Laxmi Gurung, Rahul Chaubey, Bhaskar kumar Jha, Bishwa
Original article Visual outcome and early complications of sutureless and glueless scleral fixated intraocular lens Lalit Agarwal, Nisha Agrawal, Rajya Laxmi Gurung, Rahul Chaubey, Bhaskar kumar Jha, Bishwa
Yong Un Shin, 1,2 Mincheol Seong, 1,2 Hee Yoon Cho, 1,2 and Min Ho Kang 1,2. 1. Introduction
 Hindawi Ophthalmology Volume 2017, Article ID 2683415, 4 pages https://doi.org/10.1155/2017/2683415 Research Article Novel Technique to Overcome the Nonavailability of a Long Needle 9-0 Polypropylene Suture
Hindawi Ophthalmology Volume 2017, Article ID 2683415, 4 pages https://doi.org/10.1155/2017/2683415 Research Article Novel Technique to Overcome the Nonavailability of a Long Needle 9-0 Polypropylene Suture
2/26/2017. Sameh Galal. M.D, FRCS Glasgow. Lecturer of Ophthalmology Research Institute of Ophthalmology
 Sameh Galal M.D, FRCS Glasgow Lecturer of Ophthalmology Research Institute of Ophthalmology No financial interest in the subject presented 1 Managing cataracts in children remains a challenge. Treatment
Sameh Galal M.D, FRCS Glasgow Lecturer of Ophthalmology Research Institute of Ophthalmology No financial interest in the subject presented 1 Managing cataracts in children remains a challenge. Treatment
Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support
 European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 714-719 Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support R.A. AZNABAYEV, I.S. ZAIDULLIN, M.S.H.
European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 714-719 Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support R.A. AZNABAYEV, I.S. ZAIDULLIN, M.S.H.
Optometric Postoperative Cataract Surgery Management
 Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Brijesh Takkar 1, Shorya Vardhan Azad 1, Neelima Aron 1, Ravi Bypareddy 1, Rajvardhan Azad 2. Introduction
 Original Article Page 1 of 7 Combined pars plana vitrectomy and suture less scleral fixation of foldable intraocular lens: single surgery visual rehabilitation of dislocated lens/intraocular lens Brijesh
Original Article Page 1 of 7 Combined pars plana vitrectomy and suture less scleral fixation of foldable intraocular lens: single surgery visual rehabilitation of dislocated lens/intraocular lens Brijesh
Temporary Haptic Externalization and Four-point Fixation of Intraocular Lens in Scleral Fixation to Enhance Stability
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(1):23-28 https://doi.org/10.3341/kjo.2017.0038 Original Article Temporary Haptic Externalization and Four-point Fixation of Intraocular Lens
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(1):23-28 https://doi.org/10.3341/kjo.2017.0038 Original Article Temporary Haptic Externalization and Four-point Fixation of Intraocular Lens
Clinical Study The Balanced Two-String Technique for Sulcus Intraocular Lens Implantation in the Absence of Capsular Support
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 2015, Article ID 153963, 5 pages http://dx.doi.org/10.1155/2015/153963 Clinical Study The Balanced Two-String Technique for Sulcus Intraocular
Hindawi Publishing Corporation Journal of Ophthalmology Volume 2015, Article ID 153963, 5 pages http://dx.doi.org/10.1155/2015/153963 Clinical Study The Balanced Two-String Technique for Sulcus Intraocular
Combined 23-gauge transconjunctival vitrectomy and scleral fixation of intraocular lens without conjunctival dissection in managing lens complications
 Yeung et al. BMC Ophthalmology (2018) 18:108 https://doi.org/10.1186/s12886-018-0776-4 RESEARCH ARTICLE Open Access Combined 23-gauge transconjunctival vitrectomy and scleral fixation of intraocular lens
Yeung et al. BMC Ophthalmology (2018) 18:108 https://doi.org/10.1186/s12886-018-0776-4 RESEARCH ARTICLE Open Access Combined 23-gauge transconjunctival vitrectomy and scleral fixation of intraocular lens
SURGICAL OUTCOME OF SIMULTANEOUS INTRAOCULAR LENS RESCUE AND SUTURELESS INTRASCLERAL TUNNEL FIXATION OF DISLOCATED INTRAOCULAR LENSES
 SURGICAL OUTCOME OF SIMULTANEOUS INTRAOCULAR LENS RESCUE AND SUTURELESS INTRASCLERAL TUNNEL FIXATION OF DISLOCATED INTRAOCULAR LENSES MIN KIM, MD,* DONG H. LEE, MD,* HYOUNG J. KOH, MD,* SUNG C. LEE, MD,
SURGICAL OUTCOME OF SIMULTANEOUS INTRAOCULAR LENS RESCUE AND SUTURELESS INTRASCLERAL TUNNEL FIXATION OF DISLOCATED INTRAOCULAR LENSES MIN KIM, MD,* DONG H. LEE, MD,* HYOUNG J. KOH, MD,* SUNG C. LEE, MD,
Modified Technique of Four Point Scleral Sutured Posterior Chamber Intraocular Lens Without Scleral Flaps
 Original Article Modified Technique of Four Point Scleral Sutured Posterior Chamber Intraocular Lens Without Scleral Flaps Haroon Tayyab, Muhammad Ali Haider, Tehmina Jahangir Sana Jahangir, Samina Jahangir,
Original Article Modified Technique of Four Point Scleral Sutured Posterior Chamber Intraocular Lens Without Scleral Flaps Haroon Tayyab, Muhammad Ali Haider, Tehmina Jahangir Sana Jahangir, Samina Jahangir,
Navigating the Options for the Treatment of Intraocular Lens Malposition
 Incorporating current trials and technology into clinical practice Howard F. Fine Practical Retina Co-Editor There has been a wave of new and innovative techniques for vitreoretinal surgeons in the management
Incorporating current trials and technology into clinical practice Howard F. Fine Practical Retina Co-Editor There has been a wave of new and innovative techniques for vitreoretinal surgeons in the management
84 Year Old with Rosacea
 84 Year Old with Rosacea S/p tap and injection of intravitreal vancomycin, ceftazidime, dexamethasone Post-injection day#1 Va HM IOP 14 mmhg Post-injection week#3 BCVA 20/20-3 (plano +0.50 x 180) IOP 23
84 Year Old with Rosacea S/p tap and injection of intravitreal vancomycin, ceftazidime, dexamethasone Post-injection day#1 Va HM IOP 14 mmhg Post-injection week#3 BCVA 20/20-3 (plano +0.50 x 180) IOP 23
In the absence of capsular support, the ophthalmic
 SECTION CO-EDITORS: ROHIT ROSS LAKHANPAL, MD; AND THOMAS ALBINI, MD A print & video series from the Vit-Buckle Society IOL Fixation Techniques BY EFREM D. MANDELCORN, MD, FRCSC; JONATHAN PRENNER, MD; AND
SECTION CO-EDITORS: ROHIT ROSS LAKHANPAL, MD; AND THOMAS ALBINI, MD A print & video series from the Vit-Buckle Society IOL Fixation Techniques BY EFREM D. MANDELCORN, MD, FRCSC; JONATHAN PRENNER, MD; AND
Late Intraocular Lens Subluxation in Patients with Uveitis
 Late Intraocular Lens Subluxation in Patients with Uveitis LR Steeples, NP Jones Manchester Royal Eye Hospital Introduction Late in-the-bag IOL subluxation is an unusual complication of phacoemulsification
Late Intraocular Lens Subluxation in Patients with Uveitis LR Steeples, NP Jones Manchester Royal Eye Hospital Introduction Late in-the-bag IOL subluxation is an unusual complication of phacoemulsification
Net technique for intraocular lens support in aphakia without capsular support
 DOI 10.1186/s40942-017-0085-8 International Journal of Retina and Vitreous ORIGINAL ARTICLE Open Access Net technique for intraocular lens support in aphakia without capsular support Fernando José De Novelli
DOI 10.1186/s40942-017-0085-8 International Journal of Retina and Vitreous ORIGINAL ARTICLE Open Access Net technique for intraocular lens support in aphakia without capsular support Fernando José De Novelli
Pediatric traumatic cataract Presentation and Management. Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017
 Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
Original Article. Address for Correspondance Dr. Charu Mithal Upgraded Dept. of Ophthalmology, LLRM Medical College Meerut.
 Original Article EVALUATION OF THE VISUAL OUTCOME AND COMPLICATION OF SECONDARY IMPLANTATION OF OPEN-LOOP ANTERIOR CHAMBER, SULCUS FIXATED POSTERIOR CHAMBER AND SCLERAL FIXATED POSTERIOR CHAMBER INTRAOCULAR
Original Article EVALUATION OF THE VISUAL OUTCOME AND COMPLICATION OF SECONDARY IMPLANTATION OF OPEN-LOOP ANTERIOR CHAMBER, SULCUS FIXATED POSTERIOR CHAMBER AND SCLERAL FIXATED POSTERIOR CHAMBER INTRAOCULAR
COURSE DESCRIPTION BASIC FUNDAMENTALS
 TACKLING POSTERIOR CAPSULE RUPTURE AND IOL IMPLANTATION: A VIDEO BASED COURSE TUESDAY - 29 th APRIL, 2014: 1.00 PM-2.30 PM, BCEC, ROOM 258 A ; SESSION 29-308 COURSE DESCRIPTION BASIC FUNDAMENTALS Early
TACKLING POSTERIOR CAPSULE RUPTURE AND IOL IMPLANTATION: A VIDEO BASED COURSE TUESDAY - 29 th APRIL, 2014: 1.00 PM-2.30 PM, BCEC, ROOM 258 A ; SESSION 29-308 COURSE DESCRIPTION BASIC FUNDAMENTALS Early
SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: Continuous curvilinear capsulorhexis, phacoemulsification and in-the-bag placement of
 SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: ETIOLOGY, RISK FACTORS, PREVENTION, AND MANAGEMENT Session: 21-205 ASCRS San Francisco 2013 Date/Time: April 21, 2013 from 10:00 AM to 11:30 AM INTRODUCTION
SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: ETIOLOGY, RISK FACTORS, PREVENTION, AND MANAGEMENT Session: 21-205 ASCRS San Francisco 2013 Date/Time: April 21, 2013 from 10:00 AM to 11:30 AM INTRODUCTION
SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: ETIOLOGY, RISK FACTORS, PREVENTION, AND MANAGEMENT
 SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: ETIOLOGY, RISK FACTORS, PREVENTION, AND MANAGEMENT Session: 21-205 ASCRS San Francisco 2013 Date/Time: April 21, 2013 from 10:00 AM to 11:30 AM EXCHANGE FOR
SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: ETIOLOGY, RISK FACTORS, PREVENTION, AND MANAGEMENT Session: 21-205 ASCRS San Francisco 2013 Date/Time: April 21, 2013 from 10:00 AM to 11:30 AM EXCHANGE FOR
Capsule fixation device for cataract surgery
 European Journal of Ophthalmology / Vol. 19 no. 1, 2009 / pp. 143-146 SHORT COMMUNICATIONS & CASE REPORTS Capsule fixation device for cataract surgery N.M. SERGIENKO 1, Y.N. KONDRATENKO 1, A.K. YAKIMOV
European Journal of Ophthalmology / Vol. 19 no. 1, 2009 / pp. 143-146 SHORT COMMUNICATIONS & CASE REPORTS Capsule fixation device for cataract surgery N.M. SERGIENKO 1, Y.N. KONDRATENKO 1, A.K. YAKIMOV
Cataract surgery is the leading cause of malpractice claims (OMIC) Complicated CE/IOL: Choices the anterior segment surgeon can make
 Posterior Segment Complications and Management of Retained Lens Material Jay M. Stewart, MD Cataract surgery is the leading cause of malpractice claims (OMIC) Complicated CE/IOL: Choices the anterior segment
Posterior Segment Complications and Management of Retained Lens Material Jay M. Stewart, MD Cataract surgery is the leading cause of malpractice claims (OMIC) Complicated CE/IOL: Choices the anterior segment
Electronic poster presentations
 Electronic poster presentations Cataract Surgery E-00002 Blue-light exposure in an animal model of uveal melanoma B.F. Fernandes, S. Di Cesare, S. Maloney, J.-C. Marshall, W. Dawson, M.N. Burnier, Jr.
Electronic poster presentations Cataract Surgery E-00002 Blue-light exposure in an animal model of uveal melanoma B.F. Fernandes, S. Di Cesare, S. Maloney, J.-C. Marshall, W. Dawson, M.N. Burnier, Jr.
Original Article Capsular tension ring implantation after lens extraction for management of subluxated cataracts
 Int J Clin Exp Pathol 2014;7(7):3733-3738 www.ijcep.com /ISSN:1936-2625/IJCEP0000754 Original Article Capsular tension ring implantation after lens extraction for management of subluxated cataracts Xiao
Int J Clin Exp Pathol 2014;7(7):3733-3738 www.ijcep.com /ISSN:1936-2625/IJCEP0000754 Original Article Capsular tension ring implantation after lens extraction for management of subluxated cataracts Xiao
Available online at Int. J. Modn. Res. Revs. Volume 3, Issue 10, pp , October, 2015
 IJMRR ISSN: 2347-8314 Available online at www.journalijmrr.com Int. J. Modn. Res. Revs. Volume 3, Issue 10, pp 870-875, October, 2015 ORIGINAL ARTICLE VARIOUS TECHNIQUES AND RECENT INNOVATIONS IN SCLERAL
IJMRR ISSN: 2347-8314 Available online at www.journalijmrr.com Int. J. Modn. Res. Revs. Volume 3, Issue 10, pp 870-875, October, 2015 ORIGINAL ARTICLE VARIOUS TECHNIQUES AND RECENT INNOVATIONS IN SCLERAL
Capture of intraocular lens optic by residual capsular opening in secondary implantation: long-term follow-up
 Tian et al. BMC Ophthalmology (2018) 18:84 https://doi.org/10.1186/s12886-018-0741-2 RESEARCH ARTICLE Open Access Capture of intraocular lens optic by residual capsular opening in secondary implantation:
Tian et al. BMC Ophthalmology (2018) 18:84 https://doi.org/10.1186/s12886-018-0741-2 RESEARCH ARTICLE Open Access Capture of intraocular lens optic by residual capsular opening in secondary implantation:
IOL Subluxation Top 5 Pearls for Management. Disclosure. David G. Hwang, MD, FACS. Shire Consultant. Not relevant to this talk.
 IOL Subluxation Top 5 Pearls for Management David G. Hwang, MD, FACS Professor and Vice Chair Kimura Endowed Chair in Ophthalmology Director, Cornea Service and Refractive Surgery Services University of
IOL Subluxation Top 5 Pearls for Management David G. Hwang, MD, FACS Professor and Vice Chair Kimura Endowed Chair in Ophthalmology Director, Cornea Service and Refractive Surgery Services University of
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Clinical Study Air Bubble Technique for Fundus Visualization during Vitrectomy in Aphakia
 Hindawi Ophthalmology Volume 2017, Article ID 4721540, 5 pages https://doi.org/10.1155/2017/4721540 Clinical Study Air Bubble Technique for Fundus Visualization during Vitrectomy in Aphakia Mahmoud Mohamed
Hindawi Ophthalmology Volume 2017, Article ID 4721540, 5 pages https://doi.org/10.1155/2017/4721540 Clinical Study Air Bubble Technique for Fundus Visualization during Vitrectomy in Aphakia Mahmoud Mohamed
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Clinical Evaluation of the BunnyLens IOL
 Clinical Evaluation of the BunnyLens IOL Introduction: BunnyLens is a foldable Hydrophlic Acrylic IOL with four ear shaped haptic design. The lens design offers many advantages in terms of: 1. Centration
Clinical Evaluation of the BunnyLens IOL Introduction: BunnyLens is a foldable Hydrophlic Acrylic IOL with four ear shaped haptic design. The lens design offers many advantages in terms of: 1. Centration
Comparing safety and efficiency of two closed-chamber techniques for iridodialysis repair - a retrospective clinical study
 Wan et al. BMC Ophthalmology (2018) 18:311 https://doi.org/10.1186/s12886-018-0984-y RESEARCH ARTICLE Open Access Comparing safety and efficiency of two closed-chamber techniques for iridodialysis repair
Wan et al. BMC Ophthalmology (2018) 18:311 https://doi.org/10.1186/s12886-018-0984-y RESEARCH ARTICLE Open Access Comparing safety and efficiency of two closed-chamber techniques for iridodialysis repair
Subnormal Vision in Uneventful Cataract Surgery after 6 Weeks Hospital Based Study
 ISSN 2231-4261 ORIGINAL ARTICLE Subnormal Vision in Uneventful Cataract Surgery after 6 Weeks Hospital Based Study 1* 1 1 V. H. Karambelkar, Ankit Sharma, Viraj Pradhan 1 Department of Ophthalmology, Krishna
ISSN 2231-4261 ORIGINAL ARTICLE Subnormal Vision in Uneventful Cataract Surgery after 6 Weeks Hospital Based Study 1* 1 1 V. H. Karambelkar, Ankit Sharma, Viraj Pradhan 1 Department of Ophthalmology, Krishna
Clear Lens Extraction for Correction of High Myopia
 Original Article Clear Lens Extraction for Correction of High Myopia Abbas Abolhasani 1, MD; Mostafa Heidari *2, MS; Ahmad Shojaei 1, MD; Seyed Hashem Khoee 1, MD; Mahmoud Rafati 1, MD; Ali Moradi 1, MS
Original Article Clear Lens Extraction for Correction of High Myopia Abbas Abolhasani 1, MD; Mostafa Heidari *2, MS; Ahmad Shojaei 1, MD; Seyed Hashem Khoee 1, MD; Mahmoud Rafati 1, MD; Ali Moradi 1, MS
Surgery for COEXISTING CATARACT AND GLAUCOMA:
 Surgery for COEXISTING CATARACT AND GLAUCOMA: UNEASY RELATIONSHIP Session: 20-107 Monday, April 20, 2015 Time: 8:00 AM-9:30 AM Room 7B (San Diego Convention Center) Course Instructors Ahmad K Khalil Alan
Surgery for COEXISTING CATARACT AND GLAUCOMA: UNEASY RELATIONSHIP Session: 20-107 Monday, April 20, 2015 Time: 8:00 AM-9:30 AM Room 7B (San Diego Convention Center) Course Instructors Ahmad K Khalil Alan
Non Phaco Sutureless Cataract Surgery with Small Scleral Tunnel Incision Using Rigid PMMA IOLS
 Original Article Non Phaco Sutureless Cataract Surgery with Small Scleral Tunnel Incision Using Rigid PMMA IOLS Muhammad Hashim Qureshi Pak J Ophthalmol 2007, Vol. 23 No.1.......................................................................................
Original Article Non Phaco Sutureless Cataract Surgery with Small Scleral Tunnel Incision Using Rigid PMMA IOLS Muhammad Hashim Qureshi Pak J Ophthalmol 2007, Vol. 23 No.1.......................................................................................
ABSTRACT. Sorath Noorani Siddiqui, FCPS; Ayesha Khan, FCPS, FRCS
 Visual Outcome and Changes in Corneal Endothelial Cell Density Following Aphakic Iris-Fixated Intraocular Lens Implantation in Pediatric Eyes With Subluxated Lenses Sorath Noorani Siddiqui, FCPS; Ayesha
Visual Outcome and Changes in Corneal Endothelial Cell Density Following Aphakic Iris-Fixated Intraocular Lens Implantation in Pediatric Eyes With Subluxated Lenses Sorath Noorani Siddiqui, FCPS; Ayesha
No-Touch Technique and a New Donor Adjuster for Descemet s Stripping Automated Endothelial Keratoplasty
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Cataract Surgery in Patients with Uveitis
 Cataract Surgery in Patients with Uveitis Chris Kalogeropoulos MD, PhD, FEBO Professor of Ophthalmology Faculty of Medicine, University of Ioannina President of Hellenic Society for the Study of Ocular
Cataract Surgery in Patients with Uveitis Chris Kalogeropoulos MD, PhD, FEBO Professor of Ophthalmology Faculty of Medicine, University of Ioannina President of Hellenic Society for the Study of Ocular
We describe a new surgical technique for treating traumatic aniridia with aphakia
 SURGICAL TECHNIQUE A New Technique for Treating Posttraumatic Aniridia With Aphakia First Results of Haptic Fixation of a Foldable Intraocular Lens on a Foldable and Custom-Tailored Iris Prosthesis Martin
SURGICAL TECHNIQUE A New Technique for Treating Posttraumatic Aniridia With Aphakia First Results of Haptic Fixation of a Foldable Intraocular Lens on a Foldable and Custom-Tailored Iris Prosthesis Martin
Learn Connect Succeed. JCAHPO Regional Meetings 2017
 Learn Connect Succeed JCAHPO Regional Meetings 2017 Cataract Surgery in 2017 DARBY D. MILLER, MD MPH CORNEA, CATARACT AND REFRACTIVE SURGERY ASSISTANT PROFESSOR OF OPHTHALMOLOGY MAYO CLINIC FLORIDA Natural
Learn Connect Succeed JCAHPO Regional Meetings 2017 Cataract Surgery in 2017 DARBY D. MILLER, MD MPH CORNEA, CATARACT AND REFRACTIVE SURGERY ASSISTANT PROFESSOR OF OPHTHALMOLOGY MAYO CLINIC FLORIDA Natural
BAG-TO-THE-WALL TECHNIQUE FOR A SUBLUXATED LENS
 AG-TO-THE-WALL TECHNIQUE FOR A SULUXATED LENS A one-piece foldable lens is implanted in an eye after blunt trauma created a large zonular tear. Y CYRES KEIKI MEHTA, MS(Ophth), MCH(Ophth) This article describes
AG-TO-THE-WALL TECHNIQUE FOR A SULUXATED LENS A one-piece foldable lens is implanted in an eye after blunt trauma created a large zonular tear. Y CYRES KEIKI MEHTA, MS(Ophth), MCH(Ophth) This article describes
Secondary Intraocular Lens Implantation in University Hospital l, Kuala Lumpur
 Secondary Intraocular Lens Implantation in University Hospital l, Kuala Lumpur Fathilah Jaais, MRCOphth, Department of Ophthalmology, Faculty of Medicine, University of Malaya, Lembah Pantai, 50603 Kuala
Secondary Intraocular Lens Implantation in University Hospital l, Kuala Lumpur Fathilah Jaais, MRCOphth, Department of Ophthalmology, Faculty of Medicine, University of Malaya, Lembah Pantai, 50603 Kuala
Complication and Visual Outcome after Peadiatric Cataract Surgery with or Without Intra Ocular Lens Implantation
 Original Article Complication and Visual Outcome after Peadiatric with or Without Intra Ocular Lens Implantation Mazhar-ul-Hasan, Umair A. Qidwai, Aziz-ur-Rehman, Nasir Bhatti, Rashid H. Alvi Pak J Ophthalmol
Original Article Complication and Visual Outcome after Peadiatric with or Without Intra Ocular Lens Implantation Mazhar-ul-Hasan, Umair A. Qidwai, Aziz-ur-Rehman, Nasir Bhatti, Rashid H. Alvi Pak J Ophthalmol
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (9), Page
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (9), Page 5290-5297 Retropupillary Fixation of Iris-Claw Intraocular Lens versus Trans-Scleral Suturing Fixation for Aphakic Eyes without Capsular
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (9), Page 5290-5297 Retropupillary Fixation of Iris-Claw Intraocular Lens versus Trans-Scleral Suturing Fixation for Aphakic Eyes without Capsular
Publication list of Dr. Alfred T S Leung
 Publication list of Dr. Alfred T S Leung No. of journal articles: 51 (as of January 2012) 1. Lam DS, Fan DS, Chan WM, Tam BS, Kwok AK, Leung AT, Parsons H. Prevalence and characteristics of peripheral
Publication list of Dr. Alfred T S Leung No. of journal articles: 51 (as of January 2012) 1. Lam DS, Fan DS, Chan WM, Tam BS, Kwok AK, Leung AT, Parsons H. Prevalence and characteristics of peripheral
Original article. Amon M Pediatric micro-incision cataract surgery Nepal J Ophthalmol 2011;3(5):3-8
 Original article Surgical management challenges and clinical results of bimanual micro-incision phacoemulsification cataract surgery in children with congenital cataract Department of Ophthalmology and
Original article Surgical management challenges and clinical results of bimanual micro-incision phacoemulsification cataract surgery in children with congenital cataract Department of Ophthalmology and
Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
 European Journal of Ophthalmology / Vol. 18 no. 5, 2008 / pp. 848-851 SHORT COMMUNICATIONS & CASE REPORTS Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
European Journal of Ophthalmology / Vol. 18 no. 5, 2008 / pp. 848-851 SHORT COMMUNICATIONS & CASE REPORTS Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
INTRODUCTION. Trans Am Ophthalmol Soc 2007:105:
 HANGING BY A THREAD: THE LONG-TERM EFFICACY AND SAFETY OF TRANSSCLERAL SUTURED INTRAOCULAR LENSES IN CHILDREN (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS) BY Edward G. Buckley MD ABSTRACT Purpose: To
HANGING BY A THREAD: THE LONG-TERM EFFICACY AND SAFETY OF TRANSSCLERAL SUTURED INTRAOCULAR LENSES IN CHILDREN (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS) BY Edward G. Buckley MD ABSTRACT Purpose: To
Innovative Iris Repair
 UNC Eye Symposium April 2, 2016 Chapel Hill, NC Innovative Iris Repair D Mark A. Terry, MD Director, Corneal Services Devers Eye Institute Scientific Director Lions VisionGift Research Lab Portland, Oregon,
UNC Eye Symposium April 2, 2016 Chapel Hill, NC Innovative Iris Repair D Mark A. Terry, MD Director, Corneal Services Devers Eye Institute Scientific Director Lions VisionGift Research Lab Portland, Oregon,
Inadvertent trypan blue staining of posterior capsule during cataract surgery associated with "Argentinian flag" event
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 Inadvertent trypan blue staining of posterior capsule during cataract surgery associated with "Argentinian
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 Inadvertent trypan blue staining of posterior capsule during cataract surgery associated with "Argentinian
Clinical study of traumatic cataract and its management
 Clinical study of traumatic cataract and its management Original article Manjula Mangane, M.R. Pujari, Chethan N. Murthy Department of Ophthalmology, Basaweshwar Teaching and General Hospital, Gulbarga,
Clinical study of traumatic cataract and its management Original article Manjula Mangane, M.R. Pujari, Chethan N. Murthy Department of Ophthalmology, Basaweshwar Teaching and General Hospital, Gulbarga,
In-bag dislocation of intraocular lens in patients with uveitis: a case series
 Tao and Hall Journal of Ophthalmic Inflammation and Infection (2015) 5:10 DOI 10.1186/s12348-015-0036-1 ORIGINAL RESEARCH Open Access In-bag dislocation of intraocular lens in patients with uveitis: a
Tao and Hall Journal of Ophthalmic Inflammation and Infection (2015) 5:10 DOI 10.1186/s12348-015-0036-1 ORIGINAL RESEARCH Open Access In-bag dislocation of intraocular lens in patients with uveitis: a
Long-term Outcomes of Vitreous Floaters Management with 23-Gauge Transconjunctival Sutureless Vitrectomy
 Long-term Outcomes of Vitreous Floaters Management with 23-Gauge Transconjunctival Sutureless Vitrectomy Malhar 1Consultant 1 Soni, Minas G 2 Georgopoulos, Adriana 2 Kovakova Vitreo-Retinal Surgeon, London,
Long-term Outcomes of Vitreous Floaters Management with 23-Gauge Transconjunctival Sutureless Vitrectomy Malhar 1Consultant 1 Soni, Minas G 2 Georgopoulos, Adriana 2 Kovakova Vitreo-Retinal Surgeon, London,
STAB INCISION GLAUCOMA SURGERY (SIGS)
 STAB INCISION GLAUCOMA SURGERY (SIGS) Dr. Soosan Jacob, MS, FRCS, DNB Senior Consultant Ophthalmologist, Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Videos available in Youtube channel:
STAB INCISION GLAUCOMA SURGERY (SIGS) Dr. Soosan Jacob, MS, FRCS, DNB Senior Consultant Ophthalmologist, Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Videos available in Youtube channel:
VISUAL OUTCOME AFTER MICROCOAXIAL PHACOEMULSIFICATION WITH MICRIOL PLUS LENS IMPLANTATION. of Corresponding Author:
 VISUAL OUTCOME AFTER MICROCOAXIAL PHACOEMULSIFICATION WITH MICRIOL PLUS IJCRR Vol 04 issue 23 Section: Healthcare Category: Research Received on: 12/10/12 Revised on: 06/11/12 Accepted on: 27/11/12 Mohd
VISUAL OUTCOME AFTER MICROCOAXIAL PHACOEMULSIFICATION WITH MICRIOL PLUS IJCRR Vol 04 issue 23 Section: Healthcare Category: Research Received on: 12/10/12 Revised on: 06/11/12 Accepted on: 27/11/12 Mohd
Complete Visual Rehabilitation in a Patient with No Light Perception after Surgical Management of a Penetrating Open-Globe Injury: A Case Report
 Published online: June 23, 2015 1663 2699/15/0062 0204$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: June 23, 2015 1663 2699/15/0062 0204$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
ORIGINAL ARTICLE. HIGH VOLUME CAMP SURGERIES A CLINICAL STUDY D. N. Prakash, K, Sathish, Sankalp Singh Sharma, Soujanya. K, Savitha Patil.
 HIGH VOLUME CAMP SURGERIES A CLINICAL STUDY D. N. Prakash, K, Sathish, Sankalp Singh Sharma, Soujanya. K, Savitha Patil. 1. Assistant Professor. Department of Ophthalmology, MMC & RI, Mysore, 2. Associate
HIGH VOLUME CAMP SURGERIES A CLINICAL STUDY D. N. Prakash, K, Sathish, Sankalp Singh Sharma, Soujanya. K, Savitha Patil. 1. Assistant Professor. Department of Ophthalmology, MMC & RI, Mysore, 2. Associate
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg
 An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
An Injector s Guide to OZURDEX (dexamethasone intravitreal implant) 0.7 mg This guide is intended to provide injectors with information on the recommended injection technique and the important risks related
Immersion Vs Contact Biometery for Axial Length Measurement before Phacoemulsification
 Original Article Immersion Vs Contact Biometery for Axial Length Measurement before Phacoemulsification with Foldable IOL Irum Abbas, Atif Mansoor Ahmad, Tahir Mahmood Pak J Ophthalmol 2009, Vol. 25 No.
Original Article Immersion Vs Contact Biometery for Axial Length Measurement before Phacoemulsification with Foldable IOL Irum Abbas, Atif Mansoor Ahmad, Tahir Mahmood Pak J Ophthalmol 2009, Vol. 25 No.
Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk cases
 European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
The Ultima foldable scleral fixation intraocular lens: A 2-year follow-up
 European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 895-902 The Ultima foldable scleral fixation intraocular lens: A 2-year follow-up G. MIGLIORATI, P. BRUSINI Department of Ophthalmology, Santa
European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 895-902 The Ultima foldable scleral fixation intraocular lens: A 2-year follow-up G. MIGLIORATI, P. BRUSINI Department of Ophthalmology, Santa
ORIGINAL ARTICLE. SURGICAL RESULTS OF PARS PLANA VITRECTOMY COMBINED WITH SMALL INCISION CATARACT SURGERY V.D. Karthigeyan 1
 SURGICAL RESULTS OF PARS PLANA VITRECTOMY COMBINED WITH SMALL INCISION CATARACT SURGERY V.D. Karthigeyan 1 HOW TO CITE THIS ARTICLE: VD Karthigeyan. Surgical results of pars plana vitrectomy combined with
SURGICAL RESULTS OF PARS PLANA VITRECTOMY COMBINED WITH SMALL INCISION CATARACT SURGERY V.D. Karthigeyan 1 HOW TO CITE THIS ARTICLE: VD Karthigeyan. Surgical results of pars plana vitrectomy combined with
Synchrony AIOL Key Features
 Synchrony AIOL Key Features Spacers Provide consistent separation distance at emmetropia Prevent lens adhesion Synchrony AIOL Key Features Spring Haptics Bias the system open Provide consistent separation
Synchrony AIOL Key Features Spacers Provide consistent separation distance at emmetropia Prevent lens adhesion Synchrony AIOL Key Features Spring Haptics Bias the system open Provide consistent separation
Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients
 Asok Nataraj MS Abstract Aim: - Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients The purpose of this study was to directly compare the outcome, safety and efficacy of the 20G and
Asok Nataraj MS Abstract Aim: - Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients The purpose of this study was to directly compare the outcome, safety and efficacy of the 20G and
Objectives. Tubes, Ties and Videotape: Financial Disclosure. Five Year TVT Results IOP Similar
 Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Safety of 23 Gauge Transconjunctival Sutureless 3 Port Pars Plana Vitrectomy for Vitreoretinal Diseases
 Original Article Safety of 23 Gauge Transconjunctival Sutureless 3 Port Pars Plana Vitrectomy for Vitreoretinal Diseases Syed Raza Ali Shah, Nadeem Ahmad, Qasim Lateef Chaudry, Chaudary Nasir Ahmad, Asad
Original Article Safety of 23 Gauge Transconjunctival Sutureless 3 Port Pars Plana Vitrectomy for Vitreoretinal Diseases Syed Raza Ali Shah, Nadeem Ahmad, Qasim Lateef Chaudry, Chaudary Nasir Ahmad, Asad
DRAFT CONSENSUS STATEMENT FOR COMMENT October
 DRAFT CONSENSUS STATEMENT FOR COMMENT October 9 2015 This statement was developed as a result of breakout group recommendations from the March 24, 2014 Developing Novel Endpoints for Premium IOLs Workshop
DRAFT CONSENSUS STATEMENT FOR COMMENT October 9 2015 This statement was developed as a result of breakout group recommendations from the March 24, 2014 Developing Novel Endpoints for Premium IOLs Workshop
Astigmatic Outcomes of Temporal versus Nasal Clear Corneal Phacoemulsification
 Astigmatic Outcomes of Temporal versus Nasal Clear Corneal Phacoemulsification Mohammad Pakravan, MD; Homayoun Nikkhah, MD; Shahin Yazdani, MD Camelia Shahabi, MD; Massih Sedigh-Rahimabadi, MD Labbafinejad
Astigmatic Outcomes of Temporal versus Nasal Clear Corneal Phacoemulsification Mohammad Pakravan, MD; Homayoun Nikkhah, MD; Shahin Yazdani, MD Camelia Shahabi, MD; Massih Sedigh-Rahimabadi, MD Labbafinejad
Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization
 Original Article Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization Aimal Khan, P.S Mahar, Azfar Nafees Hanfi, Umair Qidwai Pak J Ophthalmol
Original Article Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization Aimal Khan, P.S Mahar, Azfar Nafees Hanfi, Umair Qidwai Pak J Ophthalmol
Phacoemulsification: Complications in First 300 Cases
 Original Article Phacoemulsification: Complications in First 300 Cases Abrar Ali, Tabassum Ahmed, Tahir Ahmed Pak J Ophthalmol 2007, Vol. 23 No. 2.................................................................................................
Original Article Phacoemulsification: Complications in First 300 Cases Abrar Ali, Tabassum Ahmed, Tahir Ahmed Pak J Ophthalmol 2007, Vol. 23 No. 2.................................................................................................
The Outcome Of 23 Gauge Pars Plana Vitrectomy Without Scleral Buckle For Management Of Rhegmatogenous Retinal Detachment. By:
 The Outcome Of 23 Gauge Pars Plana Vitrectomy Without Scleral Buckle For Management Of Rhegmatogenous Retinal Detachment. By: Mohamed El-Deeb, MD, M.Sc, ICO, FRCS. Vitreoretinal Consultant, Magrabi Eye
The Outcome Of 23 Gauge Pars Plana Vitrectomy Without Scleral Buckle For Management Of Rhegmatogenous Retinal Detachment. By: Mohamed El-Deeb, MD, M.Sc, ICO, FRCS. Vitreoretinal Consultant, Magrabi Eye
Title. with prior vitrectomy. Author(s) Takashi. Issue Date Wichtig Editore.
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Spontaneous dislocation of in-the-b with prior vitrectomy Matsumoto, Makiko; Yamada, Koki; Ue Azusa; Tsuiki, Eiko; Kumagami, Take Takashi European
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Spontaneous dislocation of in-the-b with prior vitrectomy Matsumoto, Makiko; Yamada, Koki; Ue Azusa; Tsuiki, Eiko; Kumagami, Take Takashi European
Cataract Surgery: Patient Information
 Cataract Surgery: Patient Information How do the Eyes Work? As light enters the eye, it first passes through the cornea the clear window of the eye. Because the cornea is curved, the light rays bend (refract).
Cataract Surgery: Patient Information How do the Eyes Work? As light enters the eye, it first passes through the cornea the clear window of the eye. Because the cornea is curved, the light rays bend (refract).
STAB INCISION GLAUCOMA SURGERY (SIGS)
 STAB INCISION GLAUCOMA SURGERY (SIGS) DR. SOOSAN JACOB Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Youtube channel*: Dr. Soosan Jacob SIGS or Stab Incision Glaucoma Surgery is a guarded
STAB INCISION GLAUCOMA SURGERY (SIGS) DR. SOOSAN JACOB Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Youtube channel*: Dr. Soosan Jacob SIGS or Stab Incision Glaucoma Surgery is a guarded
Why DMEK? EK: Complications and Controversies
 Why DMEK? EK: Complications and Controversies Quicker visual recovery Lower rejection rate Michael J. Taravella, MD Director: Cornea and Refractive Surgery University of Colorado 1 Less stroma? Potential
Why DMEK? EK: Complications and Controversies Quicker visual recovery Lower rejection rate Michael J. Taravella, MD Director: Cornea and Refractive Surgery University of Colorado 1 Less stroma? Potential
Start with ME. LEAVE A LEGACY OF EXCELLENT OUTCOMES FOR PATIENTS WITH ASTIGMATISM. TECNIS TORIC 1-PIECE IOL
 LEAVE A LEGACY OF EXCELLENT OUTCOMES FOR PATIENTS WITH ASTIGMATISM. Start with ME. TECNIS TORIC 1-PIECE IOL INDICATIONS: The TECNIS Toric 1-Piece Posterior Chamber Lens is indicated for the visual correction
LEAVE A LEGACY OF EXCELLENT OUTCOMES FOR PATIENTS WITH ASTIGMATISM. Start with ME. TECNIS TORIC 1-PIECE IOL INDICATIONS: The TECNIS Toric 1-Piece Posterior Chamber Lens is indicated for the visual correction
STAB INCISION GLAUCOMA SURGERY (SIGS) AMAR AGARWAL
 STAB INCISION GLAUCOMA SURGERY (SIGS) AMAR AGARWAL SIGS or Stab Incision Glaucoma Surgery is a guarded filtration procedure that was introduced by me and is slowly but surely becoming popular amongst many
STAB INCISION GLAUCOMA SURGERY (SIGS) AMAR AGARWAL SIGS or Stab Incision Glaucoma Surgery is a guarded filtration procedure that was introduced by me and is slowly but surely becoming popular amongst many
Ruba Alobaidy Jia Y Ng Sathish Srinivasan
 Ruba Alobaidy Jia Y Ng Sathish Srinivasan Department of Ophthalmology, University Hospital Ayr, Ayr, Scotland The authors have no financial interests to declare. Continuous curvilinear capsulorhexis (CCC)
Ruba Alobaidy Jia Y Ng Sathish Srinivasan Department of Ophthalmology, University Hospital Ayr, Ayr, Scotland The authors have no financial interests to declare. Continuous curvilinear capsulorhexis (CCC)
SECONDARY CAPSULOTOMY USING THE FEMTOSECOND LASER. Surendra Basti, MD Northwestern University Feinberg School of Medicine, Chicago, IL
 SECONDARY CAPSULOTOMY USING THE FEMTOSECOND LASER Surendra Basti, MD Northwestern University Feinberg School of Medicine, Chicago, IL SMALL PUPIL MANAGEMENT DURING FEMTO CATARACT SURGERY Surendra Basti,
SECONDARY CAPSULOTOMY USING THE FEMTOSECOND LASER Surendra Basti, MD Northwestern University Feinberg School of Medicine, Chicago, IL SMALL PUPIL MANAGEMENT DURING FEMTO CATARACT SURGERY Surendra Basti,
GLUED PC IOL IMPLANTATION WITH INTRALAMELLAR SCLERAL TUCK IN EYES WITH DEFICIENT CAPSULE
 GLUED PC IOL IMPLANTATION WITH INTRALAMELLAR SCLERAL TUCK IN EYES WITH DEFICIENT CAPSULE AMAR AGARWAL INTRODUCTION 1-2 Posterior capsular rent (PCR) can occur in early learning curve in phacoemulsification.
GLUED PC IOL IMPLANTATION WITH INTRALAMELLAR SCLERAL TUCK IN EYES WITH DEFICIENT CAPSULE AMAR AGARWAL INTRODUCTION 1-2 Posterior capsular rent (PCR) can occur in early learning curve in phacoemulsification.
Trauma. steve charles
 Trauma steve charles Pathobiology of Trauma Hypocellular Vitreous Collagen Contraction (formerly called gel contraction) Poor Names: Vitreous Bands & Vitreous Membranes (always along vitreous surface or
Trauma steve charles Pathobiology of Trauma Hypocellular Vitreous Collagen Contraction (formerly called gel contraction) Poor Names: Vitreous Bands & Vitreous Membranes (always along vitreous surface or
TRAUMATIC CATARACT DR.KHUTEJA FATIMA IIND YEAR PG DEPT OF OPHTHALMOLOGY
 TRAUMATIC CATARACT DR.KHUTEJA FATIMA IIND YEAR PG DEPT OF OPHTHALMOLOGY Traumatic cataract :Traumatic lens damage caused by mechanical injury and by physical forces (Ionising radiation,ir radiation, electrical
TRAUMATIC CATARACT DR.KHUTEJA FATIMA IIND YEAR PG DEPT OF OPHTHALMOLOGY Traumatic cataract :Traumatic lens damage caused by mechanical injury and by physical forces (Ionising radiation,ir radiation, electrical
Audit of extracapsular cataract extraction and posterior chamber lens implantation as a routine treatment for age related cataract in east Africa
 Br J Ophthalmol 1999;83:897 901 897 Kikuyu Hospital, Kenya D Yorston London School of Hygiene and Tropical Medicine, London A Foster Correspondence to: Dr Allen Foster, London School of Hygiene and Tropical
Br J Ophthalmol 1999;83:897 901 897 Kikuyu Hospital, Kenya D Yorston London School of Hygiene and Tropical Medicine, London A Foster Correspondence to: Dr Allen Foster, London School of Hygiene and Tropical
Venturi versus peristaltic pumps 33 vitrectomy dynamics 34 Fluorescein, vitreous staining 120
 Subject Index Accurus 35, 83 Aflibercept, diabetic macular edema management 167, 168 Air-forced infusion, Stellaris PC 12, 13 Alcon Constellation, see Constellation system Autoclave sterilization lens
Subject Index Accurus 35, 83 Aflibercept, diabetic macular edema management 167, 168 Air-forced infusion, Stellaris PC 12, 13 Alcon Constellation, see Constellation system Autoclave sterilization lens
Endo Optiks. Clinical Publication Summaries
 Endo Optiks Clinical Publication Summaries Effective. Safe. Simple. Four scientific studies demonstrating the proven clinical benefits of combined ECP and cataract surgery. ECP is an Effective, Safe, and
Endo Optiks Clinical Publication Summaries Effective. Safe. Simple. Four scientific studies demonstrating the proven clinical benefits of combined ECP and cataract surgery. ECP is an Effective, Safe, and
OVERVIEW OF OCULAR MANAGEMENT IN MARFAN SYNDROME
 OVERVIEW OF OCULAR MANAGEMENT IN MARFAN SYNDROME Prepared by: Deborah Alcorn, MD, Dianna Milewicz, MD, and Irene H Maumenee, MD OCULAR FEATURES OF MARFAN SYNDROME Marfan syndrome is a dominantly inherited
OVERVIEW OF OCULAR MANAGEMENT IN MARFAN SYNDROME Prepared by: Deborah Alcorn, MD, Dianna Milewicz, MD, and Irene H Maumenee, MD OCULAR FEATURES OF MARFAN SYNDROME Marfan syndrome is a dominantly inherited
Iris Claw versus Scleral Fixation Intraocular Lens Implantation during Pars Plana Vitrectomy
 Original Article Iris Claw versus Scleral Fixation Intraocular Lens Implantation during Pars Plana Vitrectomy Fereydoun Farrahi, MD; Mostafa Feghhi, MD; Foad Haghi, MD Ali Kasiri, MD; Abbas Afkari, MD;
Original Article Iris Claw versus Scleral Fixation Intraocular Lens Implantation during Pars Plana Vitrectomy Fereydoun Farrahi, MD; Mostafa Feghhi, MD; Foad Haghi, MD Ali Kasiri, MD; Abbas Afkari, MD;
Prabhu GR. Visual outcome of traumatic cataract in a tertiary care hospital, Tirupati.
 Jagannath C, Penchalaiah T, Swetha M, Prabhu GR. Visual outcome of traumatic cataract in a tertiary care hospital, Tirupati. Original Research Article Visual outcome of traumatic cataract in a tertiary
Jagannath C, Penchalaiah T, Swetha M, Prabhu GR. Visual outcome of traumatic cataract in a tertiary care hospital, Tirupati. Original Research Article Visual outcome of traumatic cataract in a tertiary
THE OUTCOME OF EXTRACAPSULAR AND PHACOEMULSIFICATION CATARACT EXTRACTIONS
 JMBR: A Peer-review Journal of Biomedical Sciences June 2012, Vol. 11 No.1 pp 123-128 THE OUTCOME OF EXTRACAPSULAR AND PHACOEMULSIFICATION CATARACT EXTRACTIONS OSITA ME and YUEN SZ Abstract This study
JMBR: A Peer-review Journal of Biomedical Sciences June 2012, Vol. 11 No.1 pp 123-128 THE OUTCOME OF EXTRACAPSULAR AND PHACOEMULSIFICATION CATARACT EXTRACTIONS OSITA ME and YUEN SZ Abstract This study
Sclerokeratoplasty David S. Chu, M.D. Cases
 Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Revitalization of the Anterior Segment: Corneal Transplantation and Secondary Lens Repair
 Revitalization of the Anterior Segment: Corneal Transplantation and Secondary Lens Repair CATHERINE REPPA, MD CORNEA SPECIALIST, ASSISTANT PROFESSOR TTUHSC DEPARTMENT OF OPHTHALMOLOGY AND VISUAL SCIENCES
Revitalization of the Anterior Segment: Corneal Transplantation and Secondary Lens Repair CATHERINE REPPA, MD CORNEA SPECIALIST, ASSISTANT PROFESSOR TTUHSC DEPARTMENT OF OPHTHALMOLOGY AND VISUAL SCIENCES
GLUED PC IOL IMPLANTATION WITH INTRALAMELLAR SCLERAL TUCK IN EYES WITH DEFICIENT CAPSULE
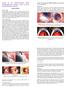 GLUED PC IOL IMPLANTATION WITH INTRALAMELLAR SCLERAL TUCK IN EYES WITH DEFICIENT CAPSULE AMAR AGARWAL INTRODUCTION 1-2 Posterior capsular rent (PCR) can occur in early learning curve in phacoemulsification.
GLUED PC IOL IMPLANTATION WITH INTRALAMELLAR SCLERAL TUCK IN EYES WITH DEFICIENT CAPSULE AMAR AGARWAL INTRODUCTION 1-2 Posterior capsular rent (PCR) can occur in early learning curve in phacoemulsification.
EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA
 EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA DR.FAISAL ALMOBARAK ASSISTANT PROFESSOR AND CONSULTANT DEPARTMENT OF OPHTHALMOLOGY COLLEGE OF MEDICINE AND KING
EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA DR.FAISAL ALMOBARAK ASSISTANT PROFESSOR AND CONSULTANT DEPARTMENT OF OPHTHALMOLOGY COLLEGE OF MEDICINE AND KING
The Visian ICL Advantages
 The Visian ICL Advantages Many vision correction procedures promise an improved level of vision, but few vision correction alternatives offer the quality and features found with the Visian ICL. These include:
The Visian ICL Advantages Many vision correction procedures promise an improved level of vision, but few vision correction alternatives offer the quality and features found with the Visian ICL. These include:
DIAGNOSTIC AND SURGICAL TECHNIQUES
 SURVEY OF OPHTHALMOLOGY VOLUME 50 NUMBER 5 SEPTEMBER OCTOBER 2005 DIAGNOSTIC AND SURGICAL TECHNIQUES MARCO ZARBIN AND DAVID CHU, EDITORS Techniques of Intraocular Lens Suspension in the Absence of Capsular/Zonular
SURVEY OF OPHTHALMOLOGY VOLUME 50 NUMBER 5 SEPTEMBER OCTOBER 2005 DIAGNOSTIC AND SURGICAL TECHNIQUES MARCO ZARBIN AND DAVID CHU, EDITORS Techniques of Intraocular Lens Suspension in the Absence of Capsular/Zonular
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens function is to focus
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
