Silver-Russell syndrome with unusual clinical features: A case report
|
|
|
- Francis Norris
- 5 years ago
- Views:
Transcription
1 Silver-Russell syndrome with unusual clinical features: A case report Nagalo K 1,2*, Douamba S 2,3, Kaboré A 2,3, Turgeon J 4,5, Laberge JM 4,6, Yé D 2,3 1 Service of Paediatrics, El Fateh-Suka Clinic, Ouagadougou, Burkina Faso 2 UFR/SDS, Ouaga I Pr. Joseph Ki - Zerbo University of Ouagadougou, Ouagadougou, Burkina Faso 3 Service of Medical Paediatrics, Charles de Gaulle Paediatric University Teaching Hospital of Ouagadougou, Ouagadougou, Burkina Faso 4 Mission Sourire d Afrique", Montreal, Canada 5 Department of Paediatrics, Sainte Justine University Teaching Hospital, University of Montreal, Montreal, Canada 6 Departement of Paediatric Surgery, The Montreal Children s Hospital, McGill University, Montreal, Canada Abstract The Silver-Russell syndrome (SRS) is a rare heterogeneous genetic disorder whose pathogenesis remains controversial. The diagnosis is mainly based on the clinical association of characteristic signs, including intrauterine growth retardation, postnatal short stature, relative macrocephaly, triangular facies, clinodactyly of the fifth finger and asymmetry of the body. In this case report, we focused on a patient with SRS, who was spotted during a routine paediatric plastic surgery campaign in Ouagadougou, Burkina Faso (West Africa). The propositus is a young male with evident poor weight gain, relative macrocephaly, large and fibrous anterior fontanel, triangular facies, frontal bossing, hypertelorism, kypho-lordosis, clinodactyly and camptodactyly. The specific SRS features in this patient included flat feet and clubbing digit. In the subsequent follow-up, the patient revealed a few alterations in the craniofacial anomalies, but with heightened intellectual and psychological issues. The diagnosis, evolution and prognosis of this syndrome are discussed in the report, including the necessity for a clinical diagnostic score for SRS and other congenital malformations to aid clinicians in developing countries that are deprived of access to molecular or genetic diagnostics. Citation: Nagalo K, Douamba S, Kaboré A, Turgeon J, Laberge JM, Yé D (2018) Silver-russell syndrome with unusual clinical features: A case report. Adv Pediatr Res 5:7. doi: /apr Received date: Feb 10, 2018; Accepted date: June 3, 2018; Published date: June 15, 2018 Copyright: 2018 Nagalo et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Competing interests: The authors have declared that no competing interests exist. Sources of funding: There is no source of funding for this article. * kiki_nagalo@yahoo.fr Introduction Silver Russell syndrome (SRS) (OMIM #180860) [1] is defined as a distinct syndromic growth disorder in which prenatal and postnatal growth failure are associated with other characteristic features, including relative macrocephaly at birth, protruding forehead in the early life, body asymmetry and substantial feeding difficulties. Almost all children with SRS are born small for gestational age (SGA). Postnatal catch up growth is uncommon in most of the children with SRS. [2]. This rare genetic disease ranks Q87.1 in the International Statistical Classification of Diseases and Related Health Problems 10th Revision [3], and it is estimated to affect 1 30/100,000 individuals, with a prevalence of 1 9/1,000,000 live births. Globally, only around 400 cases have been reported until date [4]. The disease equally affects all races [5-7] and both the sexes [8]. Historically, in 1953, Silver et al. [9] first described this disease, followed by Russell in 1954 [10]. Silver et al. [9] described two children with congenital hemi-hypertrophy, low birth weight, short stature and increased urinary gonadotropins. Russell [10], however, reported five children with intrauterine growth retardation and anomalies of the skull and face. Even as both the authors believed they were describing two different conditions, the two phenotypes were later identified as a single entity and the disease was thus classified as SRS, using both their names [11]. From the perspective of heredity, transmission is observed to be sporadic or autosomal dominant, Advances in Pediatric Research 1
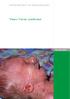
2 although some alternate routes of inheritance have been reported [4]. At present, the two genotypic anomalies clearly recognisable in the initial stage of the disease include loss of methylation (LOM) on chromosome 11p15, imprinting the centre region 1 (ICR1) [12] and the maternal uniparental chromosome 7 disomy (upd(7)mat) [13]. The 11p15 ICR1 bears the genes responsible for the growth-regulating proteins, and the LOM in this region induces characteristic growth retardation in SRS. In fact, 44.6% (15-64%) of the SRS phenotypes show LOM, and the upd(7)mat accounts for 4.5% ( %) of the phenotypes. Besides SRS, there have been rather very rare reports of other duplications (1-2%) and chromosomal aberrations (1%) [14-16], which leaves around 50% of the SRS cases with unknown aetiology. Great interest and numerous reasons are accorded to the understanding of this polymalformative syndrome and of this present case of SRS. First, SRS is relatively uncommon [4], with only very limited cases recorded in Africa [6,17], and the present instance is, to the best of our knowledge, the first case of SRS reported in Burkina Faso (West Africa). The clinical diagnosis of SRS is quite difficult, as several other syndromes show similar phenotypical characteristics [3,18-20]. The patient in this study reveals peculiarities not catalogued in the characteristics of SRS. Finally, although as a congenital affliction, there is no cure for SRS, prevention through genetic counselling is useful in familial cases of SRS. Case Report T.I. visited the Canadian Humanitarian Paediatric Surgery Mission Sourires d Afrique ( for consultation on 29 November, T.I was 11-year-old and manifested delayed closure of the anterior fontanel, spinal deformity and short stature. According to his medical history, T.I. was the outcome of a normal mono-foetal pregnancy without any complications that culminated in normal delivery at term. At birth, his weight was 2480 g and body length 48 cm, with the head circumference (HC) of 32 cm and thoracic perimeter of 31 cm. Referring to the WHO child growth standards charts, the HC-for-age was comprised between 0 and +1 z-score, height-for-age was comprised between -1 and -2 z-score, weightfor-age equal to -2 z-score, weight-for-height was comprised between -2 and -3 z-score, and BMI-forage is kg/m ² comprised between -2 and -3 z- score. The Apgar score was 6, 8 and 10, respectively, at 1, 5 and 10 min. The growthmonitoring chart showed a gradual shift in weight from 5 months of age, leaving the corridor of normal weight-for-age and entry into under nutrition area at 8 months of age without catchingup to the 21 months of age. During the course of interrogation, it was revealed that the patient suffered from language and cognition development delay. His biological parents are not in a consanguineous marriage; his father is a trader aged 29 years, and the mother is a housewife of age 20 years, G4 P3, with a stillborn due to malaria. T.I. is the eldest of the three siblings, with both the younger sisters in apparently good health. He is enrolled in the elementary school, grade two and has encountered learning difficulties. Figure 1. The Silver Russell syndrome in the patient T. I., showing the triangular facies characteristic with relative macrocephaly, frontal bossing, mandibular hypoplasia and small chin (Photograph by B. Fougères). On physical examination, the patient showed a general good condition, a weight of 18.5 kg, HC of 52 cm, height of 119 cm and a weight-to-height comprised between -1 and -2 z-score. His BMI of 13.1 kg/m² was comprised between -2 and -3 z- Advances in Pediatric Research 2
3 score, indicating thinness. His skull and face examination revealed triangular facies with relative macrocephaly, prominent broad forehead with large bumps, mandibular hypoplasia and micrognathia (Figure 1). The anterior fontanel was broad, fibrous and non-pulsatile. Kypho-lordosis was evident, with the scapular spines showing detachment (Figure 2). The hands showed a clubbing digit, bilateral clinodactyly of the fifth finger and camptodactyly of the fifth right finger (Figure 3). Both his feet were flat. The rest of the examination was normal. Figure 3. The Silver Russell syndrome in the patient T. I. having clinodactyly, camptodactyly, and clubbing digit (Photograph by B. Fougères). On examination, the patient weight was 45 kg, height cm with a BMI of 20.7 kg/m², indicating a normal weight. The HC was 55 cm and the mid-parental height was 184 cm or 84.4% height percentile. The patient had strong muscles, the anterior fontanel was closed, but the craniofacial, skeletal, spinal anomalies (Figures 4 and 5) and extremities anomalies remain unchanged. Figure 2. The Silver Russell syndrome in the patient T. I. showing kypho-lordosis and scapular spines detachment (Photograph by B. Fougères). No cytogenetic or molecular investigations were performed. The set of clinical signs observed facilitated the diagnosis of SRS. No growth hormone treatment was performed. When the second examination was performed on 20 June, 2017, T.I. was of age 20 years and 6 months. His complaints, according to the mother, included his short stature and absence of weight gain despite having a good appetite. The young man also reported excess sweating. Figure 4. The Silver Russell syndrome in the patient T. I. His craniofacial pattern at 20 and 6 months of age (Photograph by K. Nagalo). A sort of claudication approach was evident; the pelvic right limb was 88-cm long, the left one being 91 cm, giving a difference of 3 cm in length. The palate was high arched and the teeth showed decay, with the pubertal development and language ability appearing normal. Intellectually, the patient Advances in Pediatric Research 3
4 experienced memory lapses with academic delay; he is currently in secondary school, grade five and repeating each class. Psychologically, he feels ostracised by his classmates, which has given him a complex. He sometimes has outbursts of unjustified and excessive anger and uses both alcohol and tobacco. The count of blood cells, glycaemia, serum electrolytes (calcium and phosphorus) were normal. Table 1 summarises the phenotype presented by the patient, and Figure 6 shows the growth chart through two follow-up visits. Relative macrocephaly at birth + Protruding forehead + Body asymmetry + Feeding difficulties and/or low BMI + Associated signs Triangular face + Fifth finger clinodactyly + Shoulder dimples + Micrognathia + Low muscle mass - Excessive sweating + Low-set and/or posteriorly rotated ears - Down-turned mouth - High-pitched squeaky voice gold - Prominent heels + Delayed closure of fontanel + Male genital anomalies - Speech delay + Irregular or crowded teeth + Motor delay - Syndactyly of toes - Hypoglycaemia - Figure 5. The Silver Russell syndrome in the patient T. I. His craniofacial and spine anomalies at 20 and 6 months of age (Photograph by K. Nagalo). Table 1. Summary of the phenotype of the Silver Russell syndrome in the patient T.I. Clinical signs * Major characteristics Small for gestational age + Patient Scoliosis and/or kyphosis + Peculiar signs Flat feet + Clubbing digit + * Adapted from Wakeling et al [2] + present; - absent. Postnatal growth failure + Advances in Pediatric Research 4
5 Figure 6. The follow-up of the growth of the patient T.I. presenting with the Silver-Russell syndrome. Table 2. Frequency of the main clinical signs of the Silver-Russell syndrome. Clinical sign Frequency Netchine, 2007 [22] Kotzot, 2008 [23] Wakeling, 2011 [24] Growth Birth weight -2 SD Height at examination -2 SD Relative macrocephaly Body asymmetry Development Global retardation Skull and face Triangular facies Bulging forehead Micro/retrognathia Dental anomalies Advances in Pediatric Research 5
6 Down-turned corners of the mouth Low-set ears Other clinical sign Clinodactyly 5th finger Syndactyly 2/3 toes Camptodactyly Arthrogryposis 0-11 Café-au-lait spots Other aspects Feeding difficulties Sweating Hypoglycaemia Gastro-oesophageal reflux Delayed closure of fontanel Associated congenital malformations Myoclonus-dystonia 0-15 Table 3. The diagnosis of the Silver-Russell syndrome in the patient T.I. according to the NH-CSS criteria. NH-CSS criteria Small for gestational age + Postnatal growth failure + Relative macrocephaly at birth Protruding forehead + Body asymmetry + Feeding difficulties and/or low BMI + present; -absent Patient + + Table 4. Differential diagnosis of the Silver-Russell syndrome. Microcephaly Bloom syndrome Nijmegen breakage syndrome MOPD II Meier-Gorlin syndrome IGF1R mutation or deletion IGF1 mutation Foetal alcohol syndrome Normocephaly or 3-M syndrome macrocephaly Mulibrey nanism SHORT syndrome Floating-Harbor syndrome IMAGe syndrome Other Osteogenesis imperfect Rickets Advances in Pediatric Research 6
7 Discussion The place of congenital anomalies and SRS in developing countries In the working conditions of a hospital in a developing country, we encountered several deformities, but the lack of amenities, of a geneticist and of a Human Genetics Unit made these anomalies remain underdiagnosed with accuracy. In the light of the high-impact conditions of neonatal morbidity and mortality, such as neonatal sepsis, perinatal asphyxia, and prematurity, congenital anomalies are largely neglected by both health authorities and health professionals. This is true even for SRS presented in this case study, the diagnosis of which was made fortuitously during a Canadian Humanitarian Mission for Paediatric Plastic Surgery in Burkina Faso. The diagnosis of SRS The historic cardinal clinical signs of SRS include intra-uterine growth retardation without postnatal catch-up, relative macrocephaly, a prominent forehead with large bumps and hypoplasia of the jaws that ends in a point by a micrognathia, which altogether give the face a triangular appearance [9,10]. Body asymmetry, a clinodactyly of the fifth finger and more recently feeding disorders have been associated with SRS [14,18,21]. The main clinical signs and their frequency in some studies are listed in Table 2. Infrequent, uncommon, or rare anomalies may be associated with SRS, such as endocrine [25], urogenital, skin [6,26], heart [26 28], eye [19,25,29], neurological [25,30,31] and psychiatric [32] anomalies, besides the appearance of tumours [1,4]. To minimise the risk of over/underestimation of SRS cases and enable easier diagnosis, several clinical scores have been proposed [5,8,22,33,34]. At present, the diagnosis of SRS is based on the Netchine Harbinson clinical scoring system (NH-CSS). When compared to other scores, NH- CSS offers the advantage of high sensitivity (97.9%), low specificity (36.4%) and high negative (88.9%) and positive (76.7%) predictive values in addition to being easy to use. The NH-CSS was proposed by Azzi et al. [35] and includes six criteria: (1) prenatal growth retardation; (2) postnatal growth retardation; (3) relative macrocephaly at birth; (4) protruding forehead; (5) body asymmetry; and (6) feeding difficulties and/or low BMI. Table 3 summarises the signs of SRS in patients with reference to the NH-CSS criteria. The patient met all NH-CSS six criteria and was therefore considered as a clinical SRS. Even though none of the scores were perfect, they are definitely useful in diagnosing SRS for clinicians in developing countries, who are generally unfamiliar with SRS and lack access to specialised laboratories for genetic and molecular tests. Molecular tests can confirm the diagnosis of SRS in around 60% of patients [22]. This means that a negative result does not exclude the diagnosis of SRS. Hence, the experts recommend that the diagnosis of SRS remains essentially clinical, as molecular tests are used for confirmation and classification of patients in the sub-groups (level A +++ recommendation); therefore, the NH CSS flow chart must be adopted for the diagnosis of SRS (level A ++ recommendation) [2]. Singular aspects observed in this patient include flat feet and clubbing digit. Even when these signs are minor clinical signs, our literature review did not reveal flat feet in SRS. Similarly, clubbing digit has not been reported among signs associated with SRS. After excluding obvious causes akin to cyanogen heart disease or chronic respiratory failure, clubbing has been related to SRS. The diagnosis of SRS is difficult due to its phenotypic similarity with other syndromes [3,18-20] and the highly heterogeneous clinical forms that this disease presents. The diagnosis is more difficult in our situation; we discussed the other similar syndromes and withheld the diagnosis of clinical SRS according to the recommendations of the consensus statement on SRS [2]. The syndromes used to differentiate SRS in a child with intrauterine growth retardation, short stature and craniofacial anomalies are listed in Table 4. Because of the lack of funding and essential facilities, we could not perform molecular tests. Burkina Faso is a developing country that lacks the availability of laboratories for molecular tests. Advances in Pediatric Research 7
8 According to our experience, we considered sending the samples to advanced countries for analysis and accurate examination. However, even if such facilities were locally available, the costs incurred in doing so would have been exorbitant and out of limit of the considered patient s parents. The accessibility for such genetic tests must necessarily be made locally; given the protean presentation of SRS, clinicians will require performing confirmatory tests to facilitate the diagnosis when they encounter patients exhibiting signs that indicate this syndrome [2,24]. The correlation between SRS phenotype and the genetic anomaly responsible is well established. In LOM, patients have phenotypic characteristics of the SRS, although the signs are moderated in upd(7)mat [7,8,14,22,24,35]. In the present case, the dysmorphic features and other clinical signs exhibited by the patient direct to the hypothesis of 11p15 LOM. On the other hand, however, the patient manifested intellectual disorders that are especially described in upd(7)mat [7,24]. We unfortunately could not collect molecular test evidence to confirm the genotype of the SRS in this patient. Evolution and prognosis of SRS One of the distinct features of SRS is the attenuation of the signs over a period of time, which impedes the clinical diagnosis even more in older children and adults. If treatment with growth hormones is not administered, the final adult height gets reduced to cm in males and cm in females [30]. In the current case, the dysmorphic signs remain constant. A height of cm is under mid-parental height, albeit quite close to the adult height reported for the disease. SRS, however, has a comparatively good prognosis. In fact, Russell described a patient in 1954 [10] who was doing satisfactorily well at 69 years of age despite having type 2 diabetes, hypercholesterolemia, hypogonadism and osteopenia [36]. Normally, while fatality is the exception, rather than the rule in SRS, Africa has recorded cases of sudden infant deaths [6]. These deaths, explained as sudden by the family members, most often carry the suspicion of infanticide, which is a common occurrence with infants having congenital malformations [37]. We propose that the main drawback with the present patient was that his intellectual deficit will continue throughout his lifetime. Although most children with SRS show normal intelligence level [5,18], 37 50% of them encounter intellectual difficulties [33,38], with some type of moderate, but significant decline in the intelligence quotient, reading performance, arithmetic ability and learning skill [15,39]. Therefore, these children require specific educational needs, like this young man who is at present facing academic failure. However, continuous education in a speciality centre may train him and improve his options of working toward successfully integrating into his society. Conclusion SRS ranks among the cosmopolitan polymalformative syndromes, and similar to other congenital malformations, continues to remain underdiagnosed in the developing countries. Therefore, in these countries, clinical diagnostic scores are highly beneficial for diagnosis. Hence, we have described uncommon clinical signs of SRS, which were distinguished by flat feet and clubbing digit. References Wakeling EL, Brioude F, Lokulo-Sodipe O, O Connell SM, Salem J, Bliek J, et al. Diagnosis and management of Silver Russell syndrome: first international consensus statement. Nature Rev Endocrinol. 2017;13: Lng=FR&Expert= Price S, Stanhope R, Garrett C, Preece M, Trembath R. The spectrum of Silver Russell syndrome: a clinical and molecular genetic study and new diagnostic criteria. J Med Genet. 1999;36: Johnson AW, Mokuolu OA. Russell Silver Syndrome in a Nigerian infant with intrauter-ine growth retardation. J Natl Med Assoc. 2001;93: Fuke T, Mizuno S, Nagai T, Hasegawa T, Horikawa R, Miyoshi Y, et al. Molecular and clinical studies in 138 Japanese patients with Silver Russell Syndrome. PLoS ONE. 2013;8:e Bartholdi D, Krajewska-Walasek M, Ounap K, Gaspar H, Chrzanowska KH, Ilyana H, et al. Epigenetic mutations of the imprinted IGF2-H19 domain in Silver Russell syndrome (SRS): results from a large cohort of patients with SRS and SRS-like phenotypes. J Med Genet. 2008;46: Silver HK, Kiyasu W, George J, Deamer WC. Syndrome of congenital hemihypertrophy, shortness of stature, and elevated urinary gonadotropins. Pediatr. 1953;12: Russell A. A syndrome of Intra-uterine dwarfism recognizable at birth with cranio-facial dysostosis, Advances in Pediatric Research 8
9 disproportionately short arms, and other anomalies (5 examples). Proc R Soc Med. 1954;47: Tanner JM, Lejarraga H, Cameron N. The natural history of the Silver Russell syndrome: a longitudinal study of thirty-nine cases. Pediatr Res. 1975;9: Gicquel C, Rossignol S, Cabrol S, Houang M, Steunou V, Barbu V, et al. Epimutation of the telomeric imprinting center region on chromosome 11p15 in Silver Russell syndrome. Nat Genet. 2005;37: Kotzot D, Schmitt S, Bernasconi F, Robinson WP, Lurie IW, Ilyina H, et al. Uniparental disomy 7 in Silver Russell syndrome and primordial growth retardation. Hum Mol Genet. 1995;4: Eggermann T. Russell Silver syndrome. Am J Med Genet C Semin Med Genet. 2010;154C: Coutton C, Devillard F, Vieville G, Amblard F, Lopez G, Jouk P-S, et al. 17p13.1 microduplication in a boy with Silver Russell syndrome features and intellectual disability. Am J Med Genet A. 2012;158A: Fokstuen S, Kotzot D. Chromosomal rearrangements in patients with clinical features of Silver Russell syndrome. Am J Med Genet A. 2014;164: Lamzouri A, Ratbi I, Sefiani A. Syndrome de Silver Russell: à propos de 3 cas et revue de la littérature. Pan Afr Med J. 2013; 14: Patton MA. Russell Silver syndrome. J Med Genet. 1988;25: Varma SK, Varma B. Clinical spectrum of Silver Russell syndrome. Contemp Clin Dent. 2013;4: Şıklar Z, Berberoğlu M. Syndromic disorders with short stature. J Clin Res Pediatr Endocrinol. 2014;6: Prasad D, Navarette V, Naganathan S. Infant with growth failure body asymmetry and dysmorphic features. Pediatr Rev. 2013;34(5):e Netchine I, Rossignol S, Dufourg M-N, Azzi S, Rousseau A, Perin L, et al. 11p15 Imprinting Center Region 1 loss of methylation is a common and specific cause of typical Russell Silver Syndrome: clinical scoring system and epigenetic-phenotypic correlations. J Clin Endocrinol Metab. 2007;92: Kotzot D. Maternal uniparental disomy 7 and Silver Russell syndrome Clinical update and comparison with other subgroups. Eur J Med Genet. 2008;51: Wakeling EL. Silver Russell syndrome. Arch Dis Child. 2011;96: Stark Z, Ryan MM, Bruno DL, Burgess T, Savarirayan R. Atypical Silver Russell phenotype resulting from maternal uniparental disomy of chromosome 7. Am J Med Genet A. 2010;152A: Fuke-Sato T, Yamazawa K, Nakabayashi K, Matsubara K, Matsuoka K, Hasegawa T, et al. Mosaic upd(7)mat in a patient with Silver Russell syndrome. Am J Med Genet A. 2012;158A: Ghanim M, Rossignol S, Delobel B, Irving M, Miller O, Devisme L, et al. Possible association between complex congenital heart defects and 11p15 hypomethylation in three patients with severe Silver-Russell syndrome. Am J Med Genet A. 2013;161: Ryan TD, Gupta A, Gupta D, Goldenberg P, Taylor MD, Lorts A, et al. Dilated cardio-myopathy in a 32-year-old woman with Russell Silver syndrome. Cardiovasc Pathol. 2014;23: Grönlund MA, Dahlgren J, Aring E, Kraemer M, Hellstrom A. Ophthalmological findings in children and adolescents with Silver Russell syndrome. Br J Ophthalmol. 2011;95: Wakeling EL, Amero SA, Alders M, Bliek J, Forsythe E, Kumar S, et al. Epigenotype-phenotype correlations in Silver Russell syndrome. J Med Genet. 2010;47: Abdelhedi F, El Khattabi L, Cuisset L, Tsatsaris V, Viot G, Druart L, et al. Neonatal Silver Russell Syndrome with maternal uniparental heterodisomy, trisomy 7 mosaicism, and dysplasia of the cerebellum. Am J Clin Pathol. 2014;142: Inoue K, Natsuyama T, Miyaoka H. Case report of schizophrenia in adolescent with Russell Silver syndrome. Psychiatry Clin Neurosci. 2014;68: Laï K, Skuse D, Stanhope R, Hindmarsh P. Cognitive abilities associated with the Silver Russell syndrome. Arch Dis Chilhood. 1994;71: Dias RP, Nightingale P, Hardy C, Kirby G, Tee L, Price S, et al. Comparison of the clinical scoring systems in Silver Russell syndrome and development of modified diagnostic criteria to guide molecular genetic testing. J Med Genet. 2013;50: Azzi S, Salem J, Thibaud N, Chantot-Bastaraud S, Lieber E, Netchine I, et al. A prospective study validating a clinical scoring system and demonstrating phenotypicalgenotypical correlations in Silver Russell syndrome. J Med Genet. 2015;52: Searle C, Johnson D. Russel Silver syndrome: a historical note and comment on an older adult. Am J Med Genet A. 2016;170: DOI Nagalo K, Laberge JM, Nguyen V, Laberge-Caouette L, Turgeon J. Syndrome de Goltz chez un nouveau-né avec fente labio-palatine. Arch Pediatr. 2012;19: Wollmann HA, Kirchner T, Enders H, Preece MA, Ranke MB. Growth and symptoms in Silver Russell syndrome: review on the basis of 386 patients. Eur J Pediatr. 1995;154: Noeker M, Wollmann HA. Cognitive development in Silver Russell syndrome: a sibling-controlled study. Dev Med Child Neurol. 2004;46: Advances in Pediatric Research 9
Silver-Russell syndrome
 Silver-Russell syndrome Emma Wakeling Consultant in Clinical Genetics North West Thames Regional Genetic Centre (Kennedy-Galton Centre) London, UK Silver-Russell syndrome Clinical features Genetic heterogeneity
Silver-Russell syndrome Emma Wakeling Consultant in Clinical Genetics North West Thames Regional Genetic Centre (Kennedy-Galton Centre) London, UK Silver-Russell syndrome Clinical features Genetic heterogeneity
Epigenetic mutations in 11p15 in Silver-Russell syndrome are restricted to the telomeric imprinting domain
 JMG Online First, published on October 19, 2005 as 10.1136/jmg.2005.038687 1 Epigenetic mutations in 11p15 in Silver-Russell syndrome are restricted to the telomeric imprinting domain Thomas Eggermann
JMG Online First, published on October 19, 2005 as 10.1136/jmg.2005.038687 1 Epigenetic mutations in 11p15 in Silver-Russell syndrome are restricted to the telomeric imprinting domain Thomas Eggermann
Perthes disease in a child with Silver-Russell syndrome
 ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 7 Number 1 Perthes disease in a child with Silver-Russell syndrome V Kakar, R Botchu, M Katchburian Citation V Kakar, R Botchu, M Katchburian.
ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 7 Number 1 Perthes disease in a child with Silver-Russell syndrome V Kakar, R Botchu, M Katchburian Citation V Kakar, R Botchu, M Katchburian.
Mosaic UPD(7q)mat in a patient with silver Russell syndrome
 Su et al. Molecular Cytogenetics (2017) 10:36 DOI 10.1186/s13039-017-0337-1 CASE REPORT Open Access Mosaic UPD(7q)mat in a patient with silver Russell syndrome Jiasun Su 1*, Jin Wang 1, Xin Fan 1, Chunyun
Su et al. Molecular Cytogenetics (2017) 10:36 DOI 10.1186/s13039-017-0337-1 CASE REPORT Open Access Mosaic UPD(7q)mat in a patient with silver Russell syndrome Jiasun Su 1*, Jin Wang 1, Xin Fan 1, Chunyun
Design and Setting: A longitudinal study. Participants: Sixty-two SRS and 227 non-srs subjects.
 ORIGINAL ARTICLE Long-Term Results of GH Treatment in Silver-Russell Syndrome (SRS): Do They Benefit the Same as Non-SRS Short-SGA? C. C. J. Smeets, G. R. J. Zandwijken, J. S. Renes, and A. C. S. Hokken-Koelega
ORIGINAL ARTICLE Long-Term Results of GH Treatment in Silver-Russell Syndrome (SRS): Do They Benefit the Same as Non-SRS Short-SGA? C. C. J. Smeets, G. R. J. Zandwijken, J. S. Renes, and A. C. S. Hokken-Koelega
APPROACH TO A DYSMORPHIC INDIVIDUAL. Denise LM Goh
 APPROACH TO A DYSMORPHIC INDIVIDUAL Denise LM Goh Contents The dysmorphic child Incidence of congenital anomalies Suspicion for diagnosis Approach to the dysmorphic child Problem analysis history hysical
APPROACH TO A DYSMORPHIC INDIVIDUAL Denise LM Goh Contents The dysmorphic child Incidence of congenital anomalies Suspicion for diagnosis Approach to the dysmorphic child Problem analysis history hysical
First Genetic Screening for Maternal Uniparental Disomy of Chromosome 7 in Turkish Silver-Russell Syndrome Patients
 Original Article Iran J Pediatr Dec 2012; Vol 22 (No 4), Pp: 445-451 First Genetic Screening for Maternal Uniparental Disomy of Chromosome 7 in Turkish Silver-Russell Syndrome Patients Emin Karaca* 1,
Original Article Iran J Pediatr Dec 2012; Vol 22 (No 4), Pp: 445-451 First Genetic Screening for Maternal Uniparental Disomy of Chromosome 7 in Turkish Silver-Russell Syndrome Patients Emin Karaca* 1,
For Affected Individuals, Families and Caregivers
 For Affected Individuals, Families and Caregivers HIGHLIGHTS and SUMMARY of Diagnosis and Management of Silver Russell Syndrome: First International Consensus Statement Condensed by Jennifer B. Salem,
For Affected Individuals, Families and Caregivers HIGHLIGHTS and SUMMARY of Diagnosis and Management of Silver Russell Syndrome: First International Consensus Statement Condensed by Jennifer B. Salem,
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on the Approach to Pediatric Anemia and Pallor. These podcasts are designed to give medical students an overview of key
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on the Approach to Pediatric Anemia and Pallor. These podcasts are designed to give medical students an overview of key
Cleidocranial Dysplasia
 BRIEF REPORTS Cleidocranial Dysplasia Anita Sharma Rohtash Yadav Kuldip Ahlawat Cleidocranial dysplasia (CCD), is characterized by short stature, typical facial features and variable degree of pan-skeletal
BRIEF REPORTS Cleidocranial Dysplasia Anita Sharma Rohtash Yadav Kuldip Ahlawat Cleidocranial dysplasia (CCD), is characterized by short stature, typical facial features and variable degree of pan-skeletal
Robinow syndrome without mesomelic 'brachymelia': a report of five cases
 Journal of Medical Genetics 1986, 23, 350-354 Robinow syndrome without mesomelic 'brachymelia': a report of five cases M D BAIN*, R M WINTERt, AND J BURNt From *the Section of Perinatal and Child Health,
Journal of Medical Genetics 1986, 23, 350-354 Robinow syndrome without mesomelic 'brachymelia': a report of five cases M D BAIN*, R M WINTERt, AND J BURNt From *the Section of Perinatal and Child Health,
Lab #10: Karyotyping Lab
 Lab #10: Karyotyping Lab INTRODUCTION A karyotype is a visual display of the number and appearance of all chromosomes from a single somatic cell. A normal human karyotype would reveal 46 chromosomes (22
Lab #10: Karyotyping Lab INTRODUCTION A karyotype is a visual display of the number and appearance of all chromosomes from a single somatic cell. A normal human karyotype would reveal 46 chromosomes (22
Russell-Silver syndrome (RSS)
 GENETIC DIAGNOSTIC LABORATORY Russell-Silver syndrome (RSS) Background: Russell-Silver syndrome (RSS, OMIM 103280, 180860) is a growth disorder characterized by intrauterine and postnatal growth retardation,
GENETIC DIAGNOSTIC LABORATORY Russell-Silver syndrome (RSS) Background: Russell-Silver syndrome (RSS, OMIM 103280, 180860) is a growth disorder characterized by intrauterine and postnatal growth retardation,
SWISS SOCIETY OF NEONATOLOGY. Raine syndrome: clinical and radiological features of a case from the United Arab Emirates
 SWISS SOCIETY OF NEONATOLOGY Raine syndrome: clinical and radiological features of a case from the United Arab Emirates December 2014 2 Abu Asbeh J, Bystricka A, Qadir M, Nikolay M, Khan J, Neonatal Intensive
SWISS SOCIETY OF NEONATOLOGY Raine syndrome: clinical and radiological features of a case from the United Arab Emirates December 2014 2 Abu Asbeh J, Bystricka A, Qadir M, Nikolay M, Khan J, Neonatal Intensive
Unifactorial or Single Gene Disorders. Hanan Hamamy Department of Genetic Medicine and Development Geneva University Hospital
 Unifactorial or Single Gene Disorders Hanan Hamamy Department of Genetic Medicine and Development Geneva University Hospital Training Course in Sexual and Reproductive Health Research Geneva 2011 Single
Unifactorial or Single Gene Disorders Hanan Hamamy Department of Genetic Medicine and Development Geneva University Hospital Training Course in Sexual and Reproductive Health Research Geneva 2011 Single
Dysmorphology. Sue White. Diagnostic Dysmorphology, Aase. Victorian Clinical Genetics Services
 Dysmorphology Sue White www.rch.unimelb.edu.au/nets/handbook Diagnostic Dysmorphology, Aase Dysmorphology Assessment Algorithm no Are the features familial? yes Recognised syndrome yes no AD/XL syndrome
Dysmorphology Sue White www.rch.unimelb.edu.au/nets/handbook Diagnostic Dysmorphology, Aase Dysmorphology Assessment Algorithm no Are the features familial? yes Recognised syndrome yes no AD/XL syndrome
22q11.2 DELETION SYNDROME. Anna Mª Cueto González Clinical Geneticist Programa de Medicina Molecular y Genética Hospital Vall d Hebrón (Barcelona)
 22q11.2 DELETION SYNDROME Anna Mª Cueto González Clinical Geneticist Programa de Medicina Molecular y Genética Hospital Vall d Hebrón (Barcelona) Genomic disorders GENOMICS DISORDERS refers to those diseases
22q11.2 DELETION SYNDROME Anna Mª Cueto González Clinical Geneticist Programa de Medicina Molecular y Genética Hospital Vall d Hebrón (Barcelona) Genomic disorders GENOMICS DISORDERS refers to those diseases
Seven cases of intellectual disability analysed by genomewide SNP analysis. Rodney J. Scott
 Seven cases of intellectual disability analysed by genomewide SNP analysis Rodney J. Scott Ability to interrogate Genomic Material ~1930 Crude analyses 2012 Highly precise analyses A (very) brief history
Seven cases of intellectual disability analysed by genomewide SNP analysis Rodney J. Scott Ability to interrogate Genomic Material ~1930 Crude analyses 2012 Highly precise analyses A (very) brief history
ISSN CHROMOSOME STUDY IN SUSPECTED CASES OF TURNER S SYNDROME FROM JAMMU REGION OF JAMMU & KASHMIR
 J. Adv. Zool. 2018: 39(1): 32-36 ISSN-0253-7214 CHROMOSOME STUDY IN SUSPECTED CASES OF TURNER S SYNDROME FROM JAMMU REGION OF JAMMU & KASHMIR Wahied Khawar Balwan and Neelam Saba *Department of Zoology,
J. Adv. Zool. 2018: 39(1): 32-36 ISSN-0253-7214 CHROMOSOME STUDY IN SUSPECTED CASES OF TURNER S SYNDROME FROM JAMMU REGION OF JAMMU & KASHMIR Wahied Khawar Balwan and Neelam Saba *Department of Zoology,
What is Craniosynostosis?
 What is Craniosynostosis? Craniosynostosis is defined as the premature closure of the cranial sutures (what some people refer to as soft spots). This results in restricted and abnormal growth of the head.
What is Craniosynostosis? Craniosynostosis is defined as the premature closure of the cranial sutures (what some people refer to as soft spots). This results in restricted and abnormal growth of the head.
Journal of Medical Genetics 1989, 26, syndrome
 Severe Silver-Russell syndrome Journal of Medical Genetics 1989, 26, 447-451 D DONNAI*, E THOMPSONt, J ALLANSONt, AND M BARAITSERt From *the Regional Genetic Service, St Mary's Hospital, Manchester M13
Severe Silver-Russell syndrome Journal of Medical Genetics 1989, 26, 447-451 D DONNAI*, E THOMPSONt, J ALLANSONt, AND M BARAITSERt From *the Regional Genetic Service, St Mary's Hospital, Manchester M13
CHROMOSOMAL MICROARRAY (CGH+SNP)
 Chromosome imbalances are a significant cause of developmental delay, mental retardation, autism spectrum disorders, dysmorphic features and/or birth defects. The imbalance of genetic material may be due
Chromosome imbalances are a significant cause of developmental delay, mental retardation, autism spectrum disorders, dysmorphic features and/or birth defects. The imbalance of genetic material may be due
The basic methods for studying human genetics are OBSERVATIONAL, not EXPERIMENTAL.
 Human Heredity Chapter 5 Human Genetics 5:1 Studying Human Genetics Humans are not good subjects for genetic research because: 1. Humans cannot ethically be crossed in desired combinations. 2. Time between
Human Heredity Chapter 5 Human Genetics 5:1 Studying Human Genetics Humans are not good subjects for genetic research because: 1. Humans cannot ethically be crossed in desired combinations. 2. Time between
chromosomal anomalies and mental pdf Chapter 8: Chromosomes and Chromosomal Anomalies (PDF) Chromosomal abnormalities -A review - ResearchGate
 DOWNLOAD OR READ : CHROMOSOMAL ANOMALIES AND MENTAL RETARDATION FROM GENOTYPES TO NEUROPSYCHOLOGICAL PHENOTYPES OF GENETIC SYNDROMES AT HIGH INCIDENCEGENOTYPE TO PHENOTYPE PDF EBOOK EPUB MOBI Page 1 Page
DOWNLOAD OR READ : CHROMOSOMAL ANOMALIES AND MENTAL RETARDATION FROM GENOTYPES TO NEUROPSYCHOLOGICAL PHENOTYPES OF GENETIC SYNDROMES AT HIGH INCIDENCEGENOTYPE TO PHENOTYPE PDF EBOOK EPUB MOBI Page 1 Page
When to suspect Prader Willi Syndrome and how to diagnose it?
 When to suspect Prader Willi Syndrome and how to diagnose it? Dr Chirita-Emandi Adela Dr Dobrescu Andreea Victor Babes University of Medicine and Pahrmacy Timisoara Emergency Hospital for Children Louis
When to suspect Prader Willi Syndrome and how to diagnose it? Dr Chirita-Emandi Adela Dr Dobrescu Andreea Victor Babes University of Medicine and Pahrmacy Timisoara Emergency Hospital for Children Louis
Prevention Diagnosis
 Prevention and Management of Positional Skull Deformities in Infants John Persing, MD, Hector James, MD, Jack Swanson, MD, John Kattwinkel, MD, Committee on Practice and Ambulatory Medicine, Section on
Prevention and Management of Positional Skull Deformities in Infants John Persing, MD, Hector James, MD, Jack Swanson, MD, John Kattwinkel, MD, Committee on Practice and Ambulatory Medicine, Section on
Epigenetic contribution to birth defects. David Amor 20 th June 2011
 Epigenetic contribution to birth defects David Amor 20 th June 2011 Genomic imprinting Genomic imprinting is the biological process whereby a gene or genomic domain is biochemically marked with information
Epigenetic contribution to birth defects David Amor 20 th June 2011 Genomic imprinting Genomic imprinting is the biological process whereby a gene or genomic domain is biochemically marked with information
UNIT IX: GENETIC DISORDERS
 UNIT IX: GENETIC DISORDERS Younas Masih Lecturer New Life College Of Nursing Karachi 3/4/2016 1 Objectives By the end of this session the Learners will be able to, 1. Know the basic terms related genetics
UNIT IX: GENETIC DISORDERS Younas Masih Lecturer New Life College Of Nursing Karachi 3/4/2016 1 Objectives By the end of this session the Learners will be able to, 1. Know the basic terms related genetics
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name OMIM number for disease 147920 Disease alternative names Please provide any alternative
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name OMIM number for disease 147920 Disease alternative names Please provide any alternative
CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE. Dr. Bahar Naghavi
 2 CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE Dr. Bahar Naghavi Assistant professor of Basic Science Department, Shahid Beheshti University of Medical Sciences, Tehran,Iran 3 Introduction Over 4000
2 CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE Dr. Bahar Naghavi Assistant professor of Basic Science Department, Shahid Beheshti University of Medical Sciences, Tehran,Iran 3 Introduction Over 4000
Approach to Mental Retardation and Developmental Delay. SR Ghaffari MSc MD PhD
 Approach to Mental Retardation and Developmental Delay SR Ghaffari MSc MD PhD Introduction Objectives Definition of MR and DD Classification Epidemiology (prevalence, recurrence risk, ) Etiology Importance
Approach to Mental Retardation and Developmental Delay SR Ghaffari MSc MD PhD Introduction Objectives Definition of MR and DD Classification Epidemiology (prevalence, recurrence risk, ) Etiology Importance
Intrauterine Growth Retardation or Small Gestational Age. Series N.14
 Intrauterine Growth Retardation or Small Gestational Age Series N.14 Patient s Guide Average Readability Leaflet Intrauterine Growth Retardation- Series 14 (Revised August 2006) This leaflet was produced
Intrauterine Growth Retardation or Small Gestational Age Series N.14 Patient s Guide Average Readability Leaflet Intrauterine Growth Retardation- Series 14 (Revised August 2006) This leaflet was produced
Prior Authorization Criteria Form This form applies to Paramount Commercial Members Only. Non-Preferred Growth Hormone Products
 Prior Authorization Criteria Form This form applies to Paramount Commercial Members Only Criteria: P0078 Approved: 3/2017 Reviewed: Non-Preferred Growth Hormone Products Complete/review information, sign
Prior Authorization Criteria Form This form applies to Paramount Commercial Members Only Criteria: P0078 Approved: 3/2017 Reviewed: Non-Preferred Growth Hormone Products Complete/review information, sign
A. Definitions... CD-157. B. General Information... CD-158
 CD Part 10 Multiple Body System Disorders A. Definitions... CD-157 B. General Information... CD-158 C. Specific Listings and Residual Functional Capacity... CD-158 1. Listing 10.06: Non-Mosaic Down Syndrome
CD Part 10 Multiple Body System Disorders A. Definitions... CD-157 B. General Information... CD-158 C. Specific Listings and Residual Functional Capacity... CD-158 1. Listing 10.06: Non-Mosaic Down Syndrome
To Be Your Local Expert A General Pediatrician s Story
 To Be Your Local Expert A General Pediatrician s Story DDC Clinic mission: To enhance the quality of life for people with special needs caused by rare genetic disorders What Does It Take to Be Your Local
To Be Your Local Expert A General Pediatrician s Story DDC Clinic mission: To enhance the quality of life for people with special needs caused by rare genetic disorders What Does It Take to Be Your Local
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names you wish listed) (A)-Testing
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names you wish listed) (A)-Testing
(i) Family 1. The male proband (1.III-1) from European descent was referred at
 1 Supplementary Note Clinical descriptions of families (i) Family 1. The male proband (1.III-1) from European descent was referred at age 14 because of scoliosis. He had normal development. Physical evaluation
1 Supplementary Note Clinical descriptions of families (i) Family 1. The male proband (1.III-1) from European descent was referred at age 14 because of scoliosis. He had normal development. Physical evaluation
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names you wish listed) (A)-Testing
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names you wish listed) (A)-Testing
AMERICAN BOARD OF MEDICAL GENETICS AND GENOMICS
 AMERICAN BOARD OF MEDICAL GENETICS AND GENOMICS Logbook Guidelines for Certification in Clinical Genetics and Genomics for the 2017 Examination as of 10/5/2015 Purpose: The purpose of the logbook is to
AMERICAN BOARD OF MEDICAL GENETICS AND GENOMICS Logbook Guidelines for Certification in Clinical Genetics and Genomics for the 2017 Examination as of 10/5/2015 Purpose: The purpose of the logbook is to
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier/Additional Provider
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier/Additional Provider TEST DISORDER/CONDITION POPULATION TRIAD Submitting laboratory: Exeter RGC Approved: Sept 2013 1. Disorder/condition
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier/Additional Provider TEST DISORDER/CONDITION POPULATION TRIAD Submitting laboratory: Exeter RGC Approved: Sept 2013 1. Disorder/condition
Epigenetics and Chromatin Remodeling
 Epigenetics and Chromatin Remodeling Bradford Coffee, PhD, FACMG Emory University Atlanta, GA Speaker Disclosure Information Grant/Research Support: none Salary/Consultant Fees: none Board/Committee/Advisory
Epigenetics and Chromatin Remodeling Bradford Coffee, PhD, FACMG Emory University Atlanta, GA Speaker Disclosure Information Grant/Research Support: none Salary/Consultant Fees: none Board/Committee/Advisory
Abstract. Introduction
 Med. J. Cairo Univ., Vol. 77, No. 1, September: 453-458, 2009 www.medicaljournalofcairouniversity.com Sanjad-Sakati Syndrome: A Rare Autosomal Recessive Disorder of Congenital Hypoparathyroidism-Microcephaly-Mental
Med. J. Cairo Univ., Vol. 77, No. 1, September: 453-458, 2009 www.medicaljournalofcairouniversity.com Sanjad-Sakati Syndrome: A Rare Autosomal Recessive Disorder of Congenital Hypoparathyroidism-Microcephaly-Mental
Faravareh Khordadpoor (PhD in molecular genetics) 1- Tehran Medical Genetics Laboratory 2- Science and research branch, Islamic Azad University
 Faravareh Khordadpoor (PhD in molecular genetics) 1- Tehran Medical Genetics Laboratory 2- Science and research branch, Islamic Azad University 1395 21 مشاوره ژنتیک و نقش آن در پیش گیری از معلولیت ها 20
Faravareh Khordadpoor (PhD in molecular genetics) 1- Tehran Medical Genetics Laboratory 2- Science and research branch, Islamic Azad University 1395 21 مشاوره ژنتیک و نقش آن در پیش گیری از معلولیت ها 20
IGF2/H19 hypomethylation in a patient with very low birthweight, preocious pubarche and insulin resistance
 Murphy et al. BMC Medical Genetics 2012, 13:42 RESEARCH ARTICLE Open Access IGF2/H19 hypomethylation in a patient with very low birthweight, preocious pubarche and insulin resistance Rinki Murphy 1*, Lourdes
Murphy et al. BMC Medical Genetics 2012, 13:42 RESEARCH ARTICLE Open Access IGF2/H19 hypomethylation in a patient with very low birthweight, preocious pubarche and insulin resistance Rinki Murphy 1*, Lourdes
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names Osteogenesis Imperfecta
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name and description (please provide any alternative names Osteogenesis Imperfecta
R.C.P.U. NEWSLETTER. Beckwith Wiedemann Syndrome Carrie Crain, B.S.
 R.C.P.U. NEWSLETTER Editor: Heather J. Stalker, M.Sc. Director: Roberto T. Zori, M.D. R.C. Philips Research and Education Unit Vol. XIX No. 1 A statewide commitment to the problems of mental retardation
R.C.P.U. NEWSLETTER Editor: Heather J. Stalker, M.Sc. Director: Roberto T. Zori, M.D. R.C. Philips Research and Education Unit Vol. XIX No. 1 A statewide commitment to the problems of mental retardation
IGF-II is a peptide hormone and a member of the IGF family. IGF-I and
 The new england journal of medicine Brief Report Paternally Inherited IGF2 Mutation and Growth Restriction Matthias Begemann, Ph.D., Birgit Zirn, M.D., Ph.D., Gijs Santen, M.D., Ph.D., Elisa Wirthgen,
The new england journal of medicine Brief Report Paternally Inherited IGF2 Mutation and Growth Restriction Matthias Begemann, Ph.D., Birgit Zirn, M.D., Ph.D., Gijs Santen, M.D., Ph.D., Elisa Wirthgen,
CLINICAL INFORMATION SHEET NEUROFIBROMATOSIS (NF)
 CLINICAL INFORMATION SHEET NEUROFIBROMATOSIS (NF) NNFF International NF1 Genetic Mutation Analysis Consortium Submission Form FORM USE Name of investigator (required field): Institution (required field):
CLINICAL INFORMATION SHEET NEUROFIBROMATOSIS (NF) NNFF International NF1 Genetic Mutation Analysis Consortium Submission Form FORM USE Name of investigator (required field): Institution (required field):
Genetics Questions: There are 15 questions in total. The answers can be found on the accompanying document
 Page 1 Genetics Questions: These questions are aimed at medical and allied health professionals and they are designed to show where genetics has a role in clinical practice. There are 15 questions in total
Page 1 Genetics Questions: These questions are aimed at medical and allied health professionals and they are designed to show where genetics has a role in clinical practice. There are 15 questions in total
Chapter 2. Study population, MRI studies & neuropsychological evaluation
 Chapter 2 Study population, MRI studies & neuropsychological evaluation Study population, MRI studies & neuropsychological evaluation 21 Study population For the current studies we included children born
Chapter 2 Study population, MRI studies & neuropsychological evaluation Study population, MRI studies & neuropsychological evaluation 21 Study population For the current studies we included children born
Corporate Medical Policy
 Corporate Medical Policy Genetic Testing for FMR1 Mutations Including Fragile X Syndrome File Name: Origination: Last CAP Review Next CAP Review Last Review genetic_testing_for_fmr1_mutations_including_fragile_x_syndrome
Corporate Medical Policy Genetic Testing for FMR1 Mutations Including Fragile X Syndrome File Name: Origination: Last CAP Review Next CAP Review Last Review genetic_testing_for_fmr1_mutations_including_fragile_x_syndrome
City: Person Completing this Form (if not patient): Relation to patient: Reason for Appointment:
 Ball State University Speech and Audiology Clinic Family Medical History Form : Date: Birthdate: Sex: Address: City: State: ZIP: Home Phone: ( ) Other Phone: ( ) Email: Primary Care Physician: Maternal
Ball State University Speech and Audiology Clinic Family Medical History Form : Date: Birthdate: Sex: Address: City: State: ZIP: Home Phone: ( ) Other Phone: ( ) Email: Primary Care Physician: Maternal
FASD Diagnosis, Intervention, & Prevention
 FASD Diagnosis, Intervention, & Prevention Susan Astley PhD Professor Director Washington State FAS Diagnostic & Prevention Network University of Washington Seattle WA, U.S.A fasdpn.org 07 WA State FAS
FASD Diagnosis, Intervention, & Prevention Susan Astley PhD Professor Director Washington State FAS Diagnostic & Prevention Network University of Washington Seattle WA, U.S.A fasdpn.org 07 WA State FAS
Hypermobile Ehlers-Danlos syndrome (heds) vs. Hypermobility Spectrum Disorders (HSD): What s the Difference?
 Hypermobile Ehlers-Danlos syndrome (heds) vs. Hypermobility Spectrum Disorders (HSD): What s the Difference? There has been a major revision in the approach to joint hypermobility (JH) as a whole. To recognize
Hypermobile Ehlers-Danlos syndrome (heds) vs. Hypermobility Spectrum Disorders (HSD): What s the Difference? There has been a major revision in the approach to joint hypermobility (JH) as a whole. To recognize
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012
 Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
Klinefelter syndrome ( 47, XXY )
 Sex Chromosome Abnormalities, Sex Chromosome Aneuploidy It has been estimated that, overall, approximately one in 400 infants have some form of sex chromosome aneuploidy. A thorough discussion of sex chromosomes
Sex Chromosome Abnormalities, Sex Chromosome Aneuploidy It has been estimated that, overall, approximately one in 400 infants have some form of sex chromosome aneuploidy. A thorough discussion of sex chromosomes
The Essential Role of Growth Deficiency in the Diagnosis of FASD
 The Essential Role of Growth Deficiency in the Diagnosis of FASD Susan Astley PhD Julia Bledsoe MD Julian Davies MD Members of the FAS DPN FASD Diagnostic Team University of Washington Seattle WA Published
The Essential Role of Growth Deficiency in the Diagnosis of FASD Susan Astley PhD Julia Bledsoe MD Julian Davies MD Members of the FAS DPN FASD Diagnostic Team University of Washington Seattle WA Published
Alcohol and Pregnancy: What Have We Learned in 37 Years?
 Alcohol and Pregnancy: What Have We Learned in 37 Years? Kenneth Lyons Jones, M.D. Professor of Pediatrics University of California, San Diego School of Medicine La Jolla, CA Generalizations About Phenotype
Alcohol and Pregnancy: What Have We Learned in 37 Years? Kenneth Lyons Jones, M.D. Professor of Pediatrics University of California, San Diego School of Medicine La Jolla, CA Generalizations About Phenotype
NYEIS Version 4.3 (ICD) ICD - 10 Codes Available in NYEIS at time of version launch (9/23/2015)
 D82.1 Di George's syndrome E63.9 Nutritional deficiency, unspecified E70.21 Tyrosinemia E70.29 Other disorders of tyrosine metabolism E70.30 Albinism, unspecified E70.5 Disorders of tryptophan metabolism
D82.1 Di George's syndrome E63.9 Nutritional deficiency, unspecified E70.21 Tyrosinemia E70.29 Other disorders of tyrosine metabolism E70.30 Albinism, unspecified E70.5 Disorders of tryptophan metabolism
Orofacial function of persons having. Report from questionnaires. Turner syndrome
 Orofacial function of persons having Turner syndrome Report from questionnaires The survey comprises questionnaires. Estimated occurrence: : girls born. Etiology: Girls with Turner syndrome are either
Orofacial function of persons having Turner syndrome Report from questionnaires The survey comprises questionnaires. Estimated occurrence: : girls born. Etiology: Girls with Turner syndrome are either
DR. SHAHJADA SELIM. Growth Hormone Deficiency. Subdivisions of Growth Hormone Deficiency. General Discussion. Signs & Symptoms
 Growth Hormone Deficiency NORD gratefully acknowledges Joe Head, NORD Intern and Richard A. Levy, MD, Director of Pediatric Endocrinology Section, Rush University, for their assistance in the preparation
Growth Hormone Deficiency NORD gratefully acknowledges Joe Head, NORD Intern and Richard A. Levy, MD, Director of Pediatric Endocrinology Section, Rush University, for their assistance in the preparation
Myoclonus-dystonia and Silver Russell syndrome resulting from maternal uniparental disomy of chromosome 7
 Clin Genet 2013: 84: 368 372 Printed in Singapore. All rights reserved Short Report 2012 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd CLINICAL GENETICS doi: 10.1111/cge.12075 Myoclonus-dystonia
Clin Genet 2013: 84: 368 372 Printed in Singapore. All rights reserved Short Report 2012 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd CLINICAL GENETICS doi: 10.1111/cge.12075 Myoclonus-dystonia
Basic Facts About PWS:
 Phone: 800-926-4797 or 941-312-0400 Your membership provides this website - Join Today! Basic Facts About PWS: A Diagnosis and Reference Guide for Physicians and Other Health Professionals What is Prader-Willi
Phone: 800-926-4797 or 941-312-0400 Your membership provides this website - Join Today! Basic Facts About PWS: A Diagnosis and Reference Guide for Physicians and Other Health Professionals What is Prader-Willi
Atlas of Genetics and Cytogenetics in Oncology and Haematology
 Atlas of Genetics and Cytogenetics in Oncology and Haematology Genetic Counseling I- Introduction II- Motives for genetic counseling requests II-1. Couple before reproduction II-2. Couple at risk III-
Atlas of Genetics and Cytogenetics in Oncology and Haematology Genetic Counseling I- Introduction II- Motives for genetic counseling requests II-1. Couple before reproduction II-2. Couple at risk III-
Diagnosing Growth Disorders. PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health
 Diagnosing Growth Disorders PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health Content Normal pattern of growth and its variation Using growth charts Interpreting auxological
Diagnosing Growth Disorders PE Clayton School of Medical Sciences, Faculty of Biology, Medicine & Health Content Normal pattern of growth and its variation Using growth charts Interpreting auxological
Orofacial function of persons having. Report from questionnaires. Silver-Russell syndrome
 Orofacial function of persons having Silver-Russell syndrome Report from questionnaires The survey comprises 7 questionnaires. Synonyms: Russell-Silver syndrome, Silver syndrome. Estimated occurrence:
Orofacial function of persons having Silver-Russell syndrome Report from questionnaires The survey comprises 7 questionnaires. Synonyms: Russell-Silver syndrome, Silver syndrome. Estimated occurrence:
22q11 deletion syndrome Report from observation charts
 Orofacial function of persons having 22q11 deletion syndrome Report from observation charts The survey comprises 147 observation charts. Synonyms: CATCH 22, Di George syndrome, Velocardiofacial syndrome
Orofacial function of persons having 22q11 deletion syndrome Report from observation charts The survey comprises 147 observation charts. Synonyms: CATCH 22, Di George syndrome, Velocardiofacial syndrome
PROTOCOLS. Osteogenesis imperfecta. Principal investigator. Co-investigators. Background
 Osteogenesis imperfecta Principal investigator Leanne M. Ward, MD, FRCPC, paediatric endocrinologist Division of Endocrinology and Metabolism, Children s Hospital of Eastern Ontario, 401 Smyth Rd., Ottawa
Osteogenesis imperfecta Principal investigator Leanne M. Ward, MD, FRCPC, paediatric endocrinologist Division of Endocrinology and Metabolism, Children s Hospital of Eastern Ontario, 401 Smyth Rd., Ottawa
Visual Vignette EP VISUAL VIGNETTE
 ENDOCRINE PRACTICE Rapid Electronic Article in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited, typeset
ENDOCRINE PRACTICE Rapid Electronic Article in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited, typeset
Section F: Discussing the diagnosis and developing a management plan
 Section E: Formulating a diagnosis Information collected during the diagnostic assessment should be reviewed, ideally in a multi-disciplinary team context, to evaluate the strength of evidence to: Support
Section E: Formulating a diagnosis Information collected during the diagnostic assessment should be reviewed, ideally in a multi-disciplinary team context, to evaluate the strength of evidence to: Support
Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 2 nd Week Dr. Zakariya Al-Akri Common and Uncommon Conditions
 Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 2 nd Week Dr. Zakariya Al-Akri Common and Uncommon Conditions - Case (1): sunset eye appearance which occurs with increased intracranial pressure
Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 2 nd Week Dr. Zakariya Al-Akri Common and Uncommon Conditions - Case (1): sunset eye appearance which occurs with increased intracranial pressure
I have no disclosures
 I have no disclosures Provide an overview of the spectrum of congenital upper extremity anomalies Describe the key imaging findings of these abnormalities Discuss the important clinical features of these
I have no disclosures Provide an overview of the spectrum of congenital upper extremity anomalies Describe the key imaging findings of these abnormalities Discuss the important clinical features of these
A New Method for Maturity Determination in Newborn Infants
 A New Method for Maturity Determination in Newborn Infants by Charles Osayande Eregie Institute of Child Health, University of Benin, Benin City, Nigeria Summary A two-part study was conducted in several
A New Method for Maturity Determination in Newborn Infants by Charles Osayande Eregie Institute of Child Health, University of Benin, Benin City, Nigeria Summary A two-part study was conducted in several
a Genetics Unit, Department of Paediatrics, Faculty of Medicine, University of Received 29 June 2004 Accepted 3 November 2004
 Original article 1 Further delineation of Al-Gazali syndrome (multiple skeletal abnormalities with anterior segment anomalies of the eye and early lethality) in a Malaysian family Meow-Keong Thong a, Lee-Gaik
Original article 1 Further delineation of Al-Gazali syndrome (multiple skeletal abnormalities with anterior segment anomalies of the eye and early lethality) in a Malaysian family Meow-Keong Thong a, Lee-Gaik
UNIVERSITY OF WASHINGTON
 UNIVERSITY OF WASHINGTON THE FETAL ALCOHOL SYNDROME DIAGNOSTIC AND PREVENTION NETWORK (FAS DPN) Center for Human Development and Disability Dear Sir or Madam, Thank you very much for your request for an
UNIVERSITY OF WASHINGTON THE FETAL ALCOHOL SYNDROME DIAGNOSTIC AND PREVENTION NETWORK (FAS DPN) Center for Human Development and Disability Dear Sir or Madam, Thank you very much for your request for an
Chapter 13. DiGeorge Syndrome
 Chapter 13 DiGeorge Syndrome DiGeorge Syndrome is a primary immunodeficiency disease caused by abnormal migration and development of certain cells and tissues during fetal development. As part of the developmental
Chapter 13 DiGeorge Syndrome DiGeorge Syndrome is a primary immunodeficiency disease caused by abnormal migration and development of certain cells and tissues during fetal development. As part of the developmental
New Patient Information Form
 New Patient Information Form Patient Identification Prenatal Alcohol & Drug Exposure Clinic FASD CLINIC Patient s OHIP N. Female Male Race Patient s Name Birth Date Age First Middle Last Patient s Address
New Patient Information Form Patient Identification Prenatal Alcohol & Drug Exposure Clinic FASD CLINIC Patient s OHIP N. Female Male Race Patient s Name Birth Date Age First Middle Last Patient s Address
Supplementary Information. Mutations in the Pre-Replication Complex cause Meier-Gorlin syndrome
 Supplementary Information Mutations in the Pre-Replication Complex cause Meier-Gorlin syndrome Louise S. Bicknell, Ernie M.H.F. Bongers, Andrea Leitch, Stephen Brown, Jeroen Schoots, Margaret E. Harley,
Supplementary Information Mutations in the Pre-Replication Complex cause Meier-Gorlin syndrome Louise S. Bicknell, Ernie M.H.F. Bongers, Andrea Leitch, Stephen Brown, Jeroen Schoots, Margaret E. Harley,
4/23/2015. Pediatric Growth Hormone Deficiency: Identification, Diagnosis, & Management. Conflict of Interest. Objectives THANK YOU!
 Pediatric Growth Hormone Deficiency: Identification, Diagnosis, & Management Kent Reifschneider, MD CHKD / EVMS Norfolk, VA Conflict of Interest Speaker bureau and advisor for Pfizer Board member of The
Pediatric Growth Hormone Deficiency: Identification, Diagnosis, & Management Kent Reifschneider, MD CHKD / EVMS Norfolk, VA Conflict of Interest Speaker bureau and advisor for Pfizer Board member of The
Birth mother Foster carer Other
 PATIENT DETAILS NAME Sex Female Male Other Date of birth (DD/MM/YYYY) / / Age at assessment: Racial/ ethnic background Preferred language Hospital number (if applicable) Referral source, date, provider
PATIENT DETAILS NAME Sex Female Male Other Date of birth (DD/MM/YYYY) / / Age at assessment: Racial/ ethnic background Preferred language Hospital number (if applicable) Referral source, date, provider
PRIMARY HYPERPARATHYROIDISM WITH RICKETS. KRITHIKA.P Dr.L.N.Padmasani Unit 1 Sri Ramachandra Medical College
 PRIMARY HYPERPARATHYROIDISM WITH RICKETS KRITHIKA.P Dr.L.N.Padmasani Unit 1 Sri Ramachandra Medical College Presenting Complaints v 17 year old developmentally normal adolescent boy, first of a twin pregnancy,
PRIMARY HYPERPARATHYROIDISM WITH RICKETS KRITHIKA.P Dr.L.N.Padmasani Unit 1 Sri Ramachandra Medical College Presenting Complaints v 17 year old developmentally normal adolescent boy, first of a twin pregnancy,
and duodenal atresia. Two other families reported may have had the same syndrome. Case reports CASE 1 (III.8, FAMILY 1)
 JMedGenet 1991; 28: 389-394 Autosomal dominant inheritance of abnormalities of the hands and feet with short palpebral fissures, variable microcephaly with learning disability, and oesophageal/duodenal
JMedGenet 1991; 28: 389-394 Autosomal dominant inheritance of abnormalities of the hands and feet with short palpebral fissures, variable microcephaly with learning disability, and oesophageal/duodenal
SWISS SOCIETY OF NEONATOLOGY. Yunis-Varon syndrome
 SWISS SOCIETY OF NEONATOLOGY Yunis-Varon syndrome January 2003 2 Heyland K, Hodler C, Bänziger O, Neonatology, University Children s Hospital of Zurich, Switzerland Swiss Society of Neonatology, Thomas
SWISS SOCIETY OF NEONATOLOGY Yunis-Varon syndrome January 2003 2 Heyland K, Hodler C, Bänziger O, Neonatology, University Children s Hospital of Zurich, Switzerland Swiss Society of Neonatology, Thomas
Growth Hormones DRUG.00009
 Market DC Growth Hormones DRUG.00009 Override(s) Prior Authorization Quantity Limit Approval Duration WPM PAB Center: Thirty (30) day exception for recently expired (within the past 45 days) growth hormone
Market DC Growth Hormones DRUG.00009 Override(s) Prior Authorization Quantity Limit Approval Duration WPM PAB Center: Thirty (30) day exception for recently expired (within the past 45 days) growth hormone
Investigation of chromosomal abnormalities and microdeletions in 50 patients with multiple congenital anomalies
 Investigation of chromosomal abnormalities and microdeletions in 50 patients with multiple congenital anomalies Akbar Mohammadzadeh MD, PhD candidate in Medical Genetics Genetics Research Center University
Investigation of chromosomal abnormalities and microdeletions in 50 patients with multiple congenital anomalies Akbar Mohammadzadeh MD, PhD candidate in Medical Genetics Genetics Research Center University
Common Genetic syndromes. Dr. E.M. Honey Department Genetics Division Human Genetics University of Pretoria
 Common Genetic syndromes Dr. E.M. Honey Department Genetics Division Human Genetics University of Pretoria Definitions Deformation Malformation Disruption Dysplasia Syndrome Associations Complex Sequences
Common Genetic syndromes Dr. E.M. Honey Department Genetics Division Human Genetics University of Pretoria Definitions Deformation Malformation Disruption Dysplasia Syndrome Associations Complex Sequences
2. Has this plan authorized this medication in the past for this member (i.e., previous authorization is on file under this plan)?
 Pharmacy Prior Authorization AETA BETTER HEALTH KETUCK Growth Hormone (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign and
Pharmacy Prior Authorization AETA BETTER HEALTH KETUCK Growth Hormone (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign and
Lab Activity 36. Principles of Heredity. Portland Community College BI 233
 Lab Activity 36 Principles of Heredity Portland Community College BI 233 Terminology of Chromosomes Homologous chromosomes: A pair, of which you get one from mom, and one from dad. Example: the pair of
Lab Activity 36 Principles of Heredity Portland Community College BI 233 Terminology of Chromosomes Homologous chromosomes: A pair, of which you get one from mom, and one from dad. Example: the pair of
Aberrant genomic imprinting in chromosome 11p15-associated congenital growth disorders : consequences for DNA-diagnostics Bliek, H.J.
 UvA-DARE (Digital Academic Repository) Aberrant genomic imprinting in chromosome 11p15-associated congenital growth disorders : consequences for DNA-diagnostics Bliek, H.J. Link to publication Citation
UvA-DARE (Digital Academic Repository) Aberrant genomic imprinting in chromosome 11p15-associated congenital growth disorders : consequences for DNA-diagnostics Bliek, H.J. Link to publication Citation
treacher collins syndrome
 a guide to understanding treacher collins syndrome a publication of children s craniofacial association a guide to understanding treacher collins syndrome this parent s guide to Treacher Collins syndrome
a guide to understanding treacher collins syndrome a publication of children s craniofacial association a guide to understanding treacher collins syndrome this parent s guide to Treacher Collins syndrome
Height- Weight Growth of Cleft Children,
 Height- Weight Growth of Cleft Children, Birth to Six Years DENNIS N. RANALLI, D.D.S.* MOHAMMAD MAZAHERI, D.D.S., M.Sc. Lancaster, Pennsylvania 17602 In 1960 the Toronto Research Institute of the Hospital
Height- Weight Growth of Cleft Children, Birth to Six Years DENNIS N. RANALLI, D.D.S.* MOHAMMAD MAZAHERI, D.D.S., M.Sc. Lancaster, Pennsylvania 17602 In 1960 the Toronto Research Institute of the Hospital
Objectives See course web page for full objectives Read : , (not Bayes theorem section)
 An Approach to Birth Defects: Perspectives in Dysmorphology Cassatt children, Mary Cassatt Adam and Eve Romulus Vuia (1922) Elizabeth M. Petty, MD Associate Professor Molecular Medicine and Genetics epetty@umich.edu
An Approach to Birth Defects: Perspectives in Dysmorphology Cassatt children, Mary Cassatt Adam and Eve Romulus Vuia (1922) Elizabeth M. Petty, MD Associate Professor Molecular Medicine and Genetics epetty@umich.edu
Approach to the Genetic Diagnosis of Neurological Disorders
 Approach to the Genetic Diagnosis of Neurological Disorders Dr Wendy Jones MBBS MRCP Great Ormond Street Hospital for Children National Hospital for Neurology and Neurosurgery What is a genetic diagnosis?
Approach to the Genetic Diagnosis of Neurological Disorders Dr Wendy Jones MBBS MRCP Great Ormond Street Hospital for Children National Hospital for Neurology and Neurosurgery What is a genetic diagnosis?
Hypoglycemia. Objectives. Glucose Metabolism
 Hypoglycemia Instructor: Janet Mendis, MSN, RNC-NIC, CNS Outline: Janet Mendis, MSN, RNC-NIC, CNS Summer Morgan, MSN, RNC-NIC, CPNP UC San Diego Health System Objectives State the blood glucose level at
Hypoglycemia Instructor: Janet Mendis, MSN, RNC-NIC, CNS Outline: Janet Mendis, MSN, RNC-NIC, CNS Summer Morgan, MSN, RNC-NIC, CPNP UC San Diego Health System Objectives State the blood glucose level at
Thymic hypoplaisa/aplasia, very small thymus gland or none at all, increased risk of infection C
 Orofacial function of persons having q deletion syndrome Report from questionnaires The survey comprises questionnaires. Synonyms: CATCH, Di George syndrome, Velocardiofacial syndrome Estimated incidence:
Orofacial function of persons having q deletion syndrome Report from questionnaires The survey comprises questionnaires. Synonyms: CATCH, Di George syndrome, Velocardiofacial syndrome Estimated incidence:
Formal Genetics of Humans: Modes of Inheritance. Dr. S Hosseini-Asl
 Formal Genetics of Humans: Modes of Inheritance Dr. S Hosseini-Asl 1 Autosomal dominant (AD) a: Wild type (Wt) allele A: Mutant allele aa: Normal phenotype Aa: Affected (heterozygous) AA: Affected (homozygous)
Formal Genetics of Humans: Modes of Inheritance Dr. S Hosseini-Asl 1 Autosomal dominant (AD) a: Wild type (Wt) allele A: Mutant allele aa: Normal phenotype Aa: Affected (heterozygous) AA: Affected (homozygous)
By: Dr. Doaa Khater Yassin, MM and M.D Paed Sr. specialist of Pediatrics SQUH
 By: Dr. Doaa Khater Yassin, MM and M.D Paed Sr. specialist of Pediatrics SQUH Born SGA with birth weight of 2.4 kg, had IUGR Hospitalized at the age of 2 month with severe dehydration Diagnosed as DKA
By: Dr. Doaa Khater Yassin, MM and M.D Paed Sr. specialist of Pediatrics SQUH Born SGA with birth weight of 2.4 kg, had IUGR Hospitalized at the age of 2 month with severe dehydration Diagnosed as DKA
World Health Organization Growth Standards. First Nations and Inuit Health Alberta Region: Training Module May 2011
 World Health Organization Growth Standards First Nations and Inuit Health Alberta Region: Training Module May 2011 Acknowledgements First Nation and Inuit Health Alberta Region would like to thank the
World Health Organization Growth Standards First Nations and Inuit Health Alberta Region: Training Module May 2011 Acknowledgements First Nation and Inuit Health Alberta Region would like to thank the
