Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese. DOI: /neo.
|
|
|
- Kathleen Watkins
- 6 years ago
- Views:
Transcription
1 Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese Neoreviews 2008;9;e291 DOI: /neo.9-7-e291 The online version of this article, along with updated information and services, is located on the World Wide Web at: Neoreviews is the official journal of the American Academy of Pediatrics. A monthly publication, it has been published continuously since. Neoreviews is owned, published, and trademarked by the American Academy of Pediatrics, 141 Northwest Point Boulevard, Elk Grove Village, Illinois, Copyright 2008 by the American Academy of Pediatrics. All rights reserved. Print ISSN:.
2 Testing Strategy for Inborn Errors of Metabolism in the Neonate Article genetics Aditi I. Dagli, MD,* Roberto T. Zori, MD,* Bryce A. Heese, MD* Author Disclosure Drs Dagli, Zori, and Heese have disclosed no financial relationships relevant to this article. This commentary does not contain a discussion of an unapproved/ investigative use of a commercial product/ device. Objectives After completing this article, readers should be able to: 1. List the initial appropriate screening tests when a neonate is suspected of having an inborn error of metabolism. 2. Describe common neonatal presentations of. 3. Interpret the initial screening test results to formulate a differential diagnosis. 4. Recognize the pitfalls to avoid while ordering metabolic tests. Abstract Early detection and management of (IEMs) can improve the affected infant s prognosis. Initial screening tests can provide a general overview of the infant s metabolic status and suggest potential IEMs. Among the clinical findings seen in many IEMs are encephalopathy, hypoglycemia, jaundice and liver disease, cardiac arrhythmias, cardiomyopathy, hypotonia, dysmorphic features, and nonimmune hydrops. Confirmatory testing (enzyme analysis or molecular DNA testing) are required to make the diagnosis. Clinicians should be aware of specific requirements for such testing to obtain the desired results. Introduction Many IEMs present in the newborn period, and early detection and management can improve an infant s prognosis substantially. The advent of extended newborn screening has made presymptomatic diagnosis of a number of these disorders possible. However, not all IEMs are identified on an extended newborn screen, and in some instances, an infant who has an IEM may become ill before the results of newborn screening become available. It is, therefore, important for the neonatologist to consider an inborn error of metabolism in the differential diagnosis for an acutely sick neonate and initiate appropriate testing. Sudden deterioration after a period of apparent normalcy is highly suggestive of a metabolic disorder. A neonate who has an IEM may present with symptoms that frequently are attributed to more common neonatal conditions, such as sepsis or gastrointestinal pathology, which may lead to a delayed or missed diagnosis. Signs such as an unusual odor (as in maple syrup urine disease), posturing (as in glutaric acidemia type 1), or apnea (as in nonketotic hyperglycinemia) can indicate an IEM. Parental consanguinity or a family history of neonatal death also should alert the physician to the possibility of a genetic disorder. In this review, we discuss the laboratory testing strategy that may be considered in the initial evaluation of a possible IEM. Discussion of the treatment of metabolic disorders is beyond the scope of this review. Initial Testing Strategy All of the tests listed in Table 1 should be obtained for neonates suspected of having IEMs. Understandably, an acutely ill neonate in metabolic crisis requires immediate management, but it is crucial to set aside samples (at least 5 ml plasma and 5 ml urine) before attempting to correct metabolic abnormalities. This is important for certain diseases where abnormal metabolites that are critical in providing a diagnosis are detected only in times of acute decompensation. The initial test results can provide a general overview of the *Division of Genetics and Metabolism, Department of Pediatrics, University of Florida, Gainesville, Fla. NeoReviews Vol.9 No.7 July 2008 e291
3 Table 1. Initial Tests for Evaluation of Possible Inborn Error of Metabolism General Laboratory Tests Blood gas Serum electrolytes Blood urea nitrogen and creatinine Blood glucose Liver function tests Creatine kinase Ammonia Serum uric acid Serum lactate Urine ketones Urinalysis Metabolic Screening Tests Plasma amino acids Plasma acylcarnitine profile Urine organic acids metabolic status of the neonate and suggest IEMs that might be considered in the differential diagnosis (Table 2). Some IEMs have characteristic presentations, but initial test results are normal. These presentations and appropriate testing are discussed in the relevant sections of this article. Encephalopathy An infant who has encephalopathy can present with seizures, lethargy, or poor feeding that may be associated with metabolic abnormalities such as hyperammonemia and metabolic acidosis. Occasionally, an infant who has encephalopathy and an IEM may present with no other supporting laboratory abnormalities. Encephalopathy associated with hyperammonemia can be a feature of several inborn errors, which can be differentiated based on initial test results (Fig. 1). Elevated ammonia concentration within 24 hours of birth with normal plasma amino acids values suggests the diagnosis of transient hyperammonemia of newborn, a Table 2. Key Laboratory Findings for Neonates Who Have Inborn Errors of Metabolism Tests Key Finding IEM Consideration Complete blood count with differential count Neutropenia Hemolytic anemia OA, GSD I G6PD deficiency, pyruvate kinase deficiency Blood gas Metabolic acidosis Respiratory alkalosis OA, Mito, PDH, PC, FAO UCD Blood glucose 2 FAO, GSD I, Galac, OA, HFI, Tyr 1 Blood urea nitrogen 2 UCD Serum lactate 1 Mito, PDH, PC, FAO, GSD I Blood ammonia 1 UCD, OA, FAO, PDH, PC Serum uric acid 1 2 GSD I Molybdenum cofactor deficiency Creatine kinase 1 FAO Ketones 2 (with hypoglycemia) 1 FAO OA Plasma acylcarnitine profile FAO, OA Plasma (free and total) carnitine FAO, OA Plasma amino acids UCD, OA Urine organic acids OA, FAO, Mito, PDH, PC Urine reducing substances Galac, HFI, Tyr 1 Very long-chain fatty acids Peroxisomal disorders Urine mucopolysaccharides Lysosomal storage disorders Urine oligosaccharides Lysosomal storage disorders 7-dehydrocholesterol Smith-Lemli-Opitz syndrome Serum transferrin glycoforms CDG CDG congenital disorder of glycosylation, FAO fatty acid oxidation defect, Galac galactosemia, GSD I glycogen storage disease type I, G6PD glucose- 6-phosphate dehydrogenase, HFI hereditary fructose intolerance, IEM inborn error of metabolism, Mito mitochondrial energy metabolism defects, OA organic aciduria, PC pyruvate carboxylase deficiency, PDH pyruvate dehydrogenase deficiency, Tyr 1 tyrosinemia type 1, UCD urea cycle defect e292 NeoReviews Vol.9 No.7 July 2008
4 Lactic acidosis metab. defects Pyruvate metab. defects Mitochondrial energy Metabolic acidosis Abnormal urine organic acids Organic acidemias Hyperammonemia No acidosis Abnormal plasma amino acids Urea cycle defect poorly understood condition that is believed to have a nongenetic cause. Encephalopathy associated with metabolic acidosis due to usually is characterized by an increased anion gap. It is important to determine the source of this increase. Lactic acidosis is encountered commonly and if mild, usually is due to cardiovascular compromise. Unexplained elevation of lactic acid requires the consideration of a metabolic disorder (Fig. 2). In addition, an acylcarnitine profile can aid in the diagnosis of fatty acid oxidation disorders and organic acidemias. Some IEMs can present with an encephalopathic picture without hyperammonemia or metabolic acidosis. Maple syrup urine disease (MSUD) is caused by an inability to break down branched-chain amino acids such as leucine, isoleucine, and valine, and a plasma amino acid profile is diagnostic. Ketoacidosis is observed in MSUD but may be absent at initial presentation. Nonketotic hyperglycinemia is caused by an inability to breakdown glycine in the liver and is characterized by a severe encephalopathy with no other associated abnormalities. Plasma amino acids may show an elevated glycine, and supporting laboratory results may be noncontributory. In this clinical scenario, it is essential to obtain cerebrospinal fluid to measure glycine concentrations, which can be diagnostic. Pyridoxine-dependent seizures present as severe, intractable seizures within the first few hours of birth. This Early onset and normal amino acids Transient hyperammonemia of the newborn Figure 1. Algorithm for evaluation of hyperammonemia in a neonate who has a suspected inborn error of metabolism. metab. metabolism. disorder is marked by a dramatic response to vitamin B6 administration. Severe seizures and encephalopathy usually developing in the first postnatal week also can suggest molybdenum cofactor deficiency. This is associated with combined deficiencies of the two enzymes that depend on molybdenum: xanthine oxidase and sulfite oxidase. In xanthine oxidase deficiency, uric acid is markedly decreased (not seen in isolated sulfite oxidase deficiency). The presence of sulfite in a fresh urine sample using a special dipstick test may be suggestive of this condition. However, elevated S-sulfocysteine concentrations in urine are more definitive. Hypoglycemia Hypoglycemia is a relatively common neonatal concern. Unexplained hypoglycemia may be caused by IEMs due to defects in carbohydrate metabolism and fatty acid oxidation. Occasionally, protein metabolism defects can have associated hypoglycemia, but other metabolic disturbances predominate. The tests listed in Table 1 should be ordered, with the addition of urine for reducing substances (Fig. 3). If nonglucose reducing substances are present in the urine, galactosemia, hereditary fructose intolerance, or tyrosinemia should be considered. Abnormally low ketones in the presence of hypoglycemia may be indicative of a fatty acid oxidation disorder. Fatty acid oxidation disorders are important because of their relatively high prevalence and usually are identified based on acylcarnitine profile abnormalities. Affected infants have an impaired capacity to use stored fats in periods of extended fasting. The presentation may be similar to Reye syndrome, with metabolic acidosis, hyperammonemia, and elevated liver enzymes, particularly transaminases. Hepatic glycogen storage diseases (GSDs), especially type I, cause hypoglycemia during periods of fasting. The diagnosis of GSD type I may be missed in the neonatal period because the hypoglycemia resolves when regular feeding is established. The liver is mildly enlarged in the first 2 postnatal days but can be markedly enlarged by the end of the first week. Abnormal laboratory study results that indicate the diagnosis of GSD type I include lactic acidosis, hyperuricemia, and hypoglycemia. NeoReviews Vol.9 No.7 July 2008 e293
5 Normal Lactate/pyruvate ratio Hypoglycemia Glycogen storage disease I Hereditary fructose intolerance Lactate Normal glucose Pyruvate metabolism defects Metabolic acidosis Lactate/pyruvate ratio Mitochondrial energy metabolism defects Pyruvate carboxylase def. Jaundice and Liver Disease Unconjugated hyperbilirubinemia may be seen in inborn errors of erythrocyte and bilirubin metabolism. Glucose- 6-phosphate dehydrogenase (G6PD) deficiency and pyruvate kinase deficiency can present in the newborn period with unconjugated hyperbilirubinemia due to hemolysis. Nonspherocytic hemolytic anemia, as noted on peripheral smear, helps in diagnosis, which can be confirmed by enzymatic analysis. Disorders of bilirubin metabolism, such as Gilbert, Crigler Najjar, Dubin- Johnson, and Lucey Driscoll syndromes, present with unconjugated hyperbilirubinemia and normal values for other liver function tests. Most of these disorders are benign. However, hyperbilirubinemia in type I Crigler Najjar syndrome may be severe enough to cause kernicterus. Most newborn screening programs include evaluation for classic galactosemia. It presents in the neonatal period with hyperbilirubinemia that is unconjugated in the early stages and predominantly conjugated in the later stages. If the neonate continues to be fed lactose-containing formula or human milk, the jaundice Normal lactate Abnormal urine organic acids Organic acidemias Fatty acid oxidation dis. Figure 2. Algorithm for evaluation of metabolic acidosis in a neonate who has a suspected inborn error of metabolism. def. deficiency, dis. disorders. worsens, hepatomegaly appears, transaminases become elevated, and coagulopathy and hypoalbuminemia can occur. When classic galactosemia is suspected, urine and blood samples should be reserved for confirmatory testing, and the patient should be switched to a nongalactose-containing soy formula. The collected urine should be tested simultaneously with Benedict solution and a glucose oxidase method (urine dipsticks). A negative glucose oxidase test result and positive Benedict reagent reaction suggests the presence of a nonglucose reducing substance, and confirmatory testing can be undertaken. Aminoacidopathies such as tyrosinemia type 1 and citrullinemia type 2 may present with severe liver disease and an abnormal plasma amino acid profile. Excretion of succinylacetone in the urine is diagnostic for tyrosinemia type 1. Fatty acid oxidation disorders also may present with hepatocellular dysfunction and are diagnosed based on an abnormal acylcarnitine profile. Traditionally, hereditary fructose intolerance does not present in the neonatal period. However, affected infants who are exposed to fructose-containing feedings (as in sucrose-containing soy formulas) may develop acute hepatocellular failure, lactic acidosis, hyperuricemia, hyperchloremia, hypophosphatemia, and metabolic acidosis. Alpha-1-antitrypsin deficiency presents with jaundice and cholestasis that may resolve spontaneously by 2 months of age only to present later with cirrhosis. The disorder is identified by low plasma concentrations of alpha-1-antitrypsin and is confirmed by protein phenotyping and mutation analysis. The perinatal form of GSD type IV presents with fetal hydrops and severe hypotonia. It often is rapidly fatal and is diagnosed by a liver biopsy. Niemann-Pick disease type C is a progressive neurodegenerative disease that can involve self-resolving jaundice and hepatomegaly in the neonatal period. Diagnosis often requires specialized studies on fibroblast cultures. Neonatal hemochromatosis can cause rapidly progressive liver failure and requires a liver biopsy for diagnosis. e294 NeoReviews Vol.9 No.7 July 2008
6 Abnormal plasma amino acids Hypoglycemia Abnormal acylcarnitine profile Hypotonia Newborns who have metabolic disorders may exhibit hypotonia and generally have associated clinical features such as encephalopathy, metabolic acidosis, cardiomyopathy, or dysmorphic features. In addition to the initial tests, relevant additional metabolic tests include measurement of very long-chain fatty acids for peroxisomal disorders, urine oligosaccharides for Pompe disease, and transferrin isoforms for congenital disorders of glycosylation. Elevated lactate values suggest a mitochondrial disorder or pyruvate metabolism defects. Urine non-glucose reducing substances Galactosemia Hereditary fructose intolerance Tyrosinemia type 1 Disorders of amino acid metabolism Abnormal urine organic acids Organic acidemias Fatty acid oxidation disorders Cardiac Presentation In the newborn period, cardiac presentations of IEM include cardiac arrhythmias and cardiomyopathy. Neonates who have fatty acid oxidation disorders may present with an arrhythmia or cardiomyopathy. An abnormal plasma acylcarnitine profile establishes the diagnosis. Primary and secondary carnitine deficiency can result in a cardiomyopathy. Free and total carnitine concentrations can be diagnostic. In rare cases, abnormally low carnitine values lead to false-negative acylcarnitine profile results. Cardiomyopathy with elevated plasma lactate and abnormal lactate/pyruvate ratios suggests a mitochondrial electron transport chain disorder. Pompe disease may present in the neonatal period with significant hypotonia and cardiomyopathy. Initial testing shows a characteristic pattern on electrocardiography, an abnormal pattern of oligosaccharides in urine, and vacuolated lymphocytes. Enzyme analysis confirms diagnosis. Glycogen Storage Disease I Hereditary fructose intolerance Ketones Serum lactate Figure 3. Algorithm for evaluation of hypoglycemia in a neonate who has a suspected inborn error of metabolism. Dysmorphic Features Subtle or overt dysmorphic features are observed in several metabolic disorders. Some disorders have a constellation of findings that can be diagnostic. Smith-Lemli-Opitz syndrome is a disorder of cholesterol synthesis associated with dysmorphic features, cleft palate, congenital heart disease, hypospadias, polydactyly, and syndactyly of the second and third toe. Serum cholesterol concentrations may be abnormally low or normal. An elevated plasma 7-dehydrocholesterol value is diagnostic. Zellweger syndrome is a peroxisomal disorder. Newborns have flat, expressionless faces with epicanthal folds and can be suspected initially to have Down syndrome. Hypotonia, cataracts, camptodactyly, and stippled epiphyses and patellae are observed. Zellweger syndrome, neonatal adrenoleukodystrophy, and other peroxisomal disorders are diagnosed by abnormal plasma very longchain fatty acid values. Congenital disorders of glycosylation are rare conditions caused by abnormalities in glycoprotein synthesis. Several different types are described and have varying clinical features involving multiple organ systems. Type 1a is characterized by a broad nasal bridge, prominent jaw and forehead, and large ears as well as abnormal fat distribution, especially of the buttocks and thighs. The diagnosis is based on an isoelectric focusing pattern of transferrin isoforms. Menkes disease is an X-linked disorder that should be suspected in a neonate who has hypothermia, hypotonia, jaundice, and characteristic facial features. Infants have macrocephaly with high foreheads and large anterior fontanelles. The hair is sparse and has a steely, kinky appearance. Skeletal radiographs show wormian bones, osteopenia, and metaphyseal widening. Copper and ceruloplasmin concentrations are decreased. NeoReviews Vol.9 No.7 July 2008 e295
7 Certain organic acidemias may be associated with multiple dysmorphic features. Neonates who have glutaric acidemia type II can have dysmorphic features, cerebral malformations, and cystic renal disease. Newborns affected by pyruvate dehydrogenase deficiency may have the facial features of fetal alcohol syndrome, agenesis of the corpus callosum, and cerebral atrophy. Because abnormal eye findings are seen in IEMs, an eye examination by an ophthalmologist is recommended. Nonimmune Hydrops Several disorders, including a number of IEMs, have been associated with nonimmune hydrops (Table 3). It is important to note that in spite of a thorough evaluation, the cause of hydrops often is not identified. Table 3. Inborn Errors of Metabolism Associated With Hydrops Fetalis Disorder Hematologic Abnormality G6PD deficiency Pyruvate kinase deficiency Lysosomal Storage Disease Mucopolysaccharidoses, sphingolipidoses, mucolipidoses Disorders of Steroid Metabolism Smith-Lemli-Opitz syndrome Mevalonic aciduria Other Zellweger syndrome Congenital disorders of glycosylation Mitochondrial disorders Glycogen storage disease type IV G6PD glucose-6-phosphate dehydrogenase Test Complete blood count with peripheral smear for hemolytic anemia Urine screen for mucopolysaccharides and oligosaccharides Lysosomal enzyme studies 7-dehydrocholesterol Urine organic acids Plasma very long-chain fatty acids Serum transferrin isoforms Serum lactate Enzyme studies, liver biopsy Confirmatory Testing Although metabolic screening tests are highly sensitive and specific for a particular diagnosis, confirmatory testing may be necessary. This often includes enzyme analysis or molecular DNA testing. Enzyme testing can be performed in various tissues such as leukocytes, skin fibroblasts, muscle, or liver. Prior to obtaining and sending out samples, it is important to review special criteria for collection and transport. Molecular testing to identify mutations in the gene coding for the enzyme may be available for certain disorders. Molecular testing is not always essential for making the diagnosis, but this information may help identify specific disease-causing mutations and aid in clinical correlation. Molecular testing is also useful in genetic counseling for at-risk family members and prenatal diagnosis. Potential Testing Pitfalls 1. Although acutely ill neonates in metabolic crisis need immediate management, it is imperative to remember that the event provides a window of opportunity for optimal metabolic testing. At least 5 ml plasma and 5 ml urine should be set aside before correction of metabolic abnormalities. Blood spots dropped onto a filter paper (such as newborn screening cards), completely dried and stored with a desiccant, also may be saved for further analysis. 2. Expanded newborn screening provides valuable information but is still only a screen. When a metabolic disorder is suspected, the newborn screen results should not be the sole diagnostic evaluation; more definitive testing should be initiated. 3. When studies such as plasma amino acids, plasma acylcarnitine profile, and urine organic acids need to be sent to a specialized laboratory, they should be sent by overnight courier. Delay can affect results. 4. When ordering measurements of plasma amino acids, it is important to ask for a quantitative analysis. Analysis of amino acids generally is more informative in plasma rather than urine. Therefore, care must be taken to specify plasma amino acid analysis. 5. Free and total carnitine measurements often are ordered erroneously instead of the plasma acylcarnitine profile. The profile provides necessary information on different acylcarnitine moieties that can aid in diagnosis of fatty acid oxidation disorders. 6. Ammonia values can be significantly elevated if the sample is not immediately rushed on ice to the laboratory and analyzed. Accurate results rely on collecting a freeflowing blood sample and avoiding the use of a tight tourniquet. 7. Lactate and pyruvate concentrations must be obtained simultaneously for comparison. The same phlebotomy precautions should be taken as described for ammonia measurement. e296 NeoReviews Vol.9 No.7 July 2008
8 Table 4. Samples That Should Be Collected in a Dying Neonate Who Has an Undiagnosed Inborn Error of Metabolism Samples Set Aside for Future Testing Plasma (at least 5 ml) frozen Urine (at least 5 ml) frozen Dried blood spot on a newborn screening filter paper card Skin biopsy in sterile saline or in culture medium at room temperature. (Caution: Povidone-iodine is toxic to cell growth) With Proper Consent, Postmortem Samples Liver tissue unfixed, immediately frozen below 20 C Muscle biopsy, immediately frozen below 20 C Skin biopsy if not obtained previously help the process flow smoothly. When it is not feasible to retrieve such samples, a blood spot, dried on filter paper as described previously, should be obtained for possible metabolic or genetic testing. It is important to make every attempt to establish a diagnosis in a terminal newborn because such information is very important to the family for making future reproductive decisions. Conclusion Diagnosis of IEMs can be challenging. The testing strategy presented in this review aims to simplify the initial clinical approach to the diagnosis of these disorders. A clinical geneticist should be involved when the initial test results are suggestive of a particular IEM to provide valuable assistance for confirmatory testing and management. 8. When the clinical condition of a neonate suspected of having a metabolic disorder deteriorates significantly and death is imminent, various samples should be set aside for future testing (Table 4). This can present a stressful situation for the medical staff and family members, and a protocol should be established to Suggested Reading Clark JTR. A Clinical Guide to Inherited Metabolic Diseases. 3rd ed. Cambridge, United Kingdom: Cambridge University Press; 2006 Scriver CR, Beaudet AL, Sly S, Valle D. The Metabolic and Molecular Bases of Inherited Disease. 8th ed. New York, NY: McGraw- Hill Publications; 1996 NeoReviews Vol.9 No.7 July 2008 e297
9 NeoReviews Quiz 4. A neonate who has an inborn error of metabolism may present with symptoms and signs that often are nonspecific and attributed to other, more common neonatal disorders such as sepsis. However, specific symptoms and signs may distinguish specific. Of the following, abnormal posturing is most likely to indicate: A. Fatty acid oxidation defect. B. Glutaric acidemia type I. C. Maple syrup urine disease. D. Nonketotic hyperglycinemia. E. Pyruvate kinase deficiency. 5. A 48-hour-old term male newborn is lethargic and feeding poorly. He has had a brief episode of generalized tonic-clonic seizures. Physical examination reveals obtunded consciousness, generalized hypotonia, and depressed reflexes. Laboratory data include normal values for blood gases, blood counts, and C-reactive protein. Cultures of blood, urine, and cerebrospinal fluid are pending. Antibiotics are administered and other supportive care is offered. Metabolic studies reveal a markedly elevated blood ammonia concentration and a highly abnormal plasma amino acid profile. Of the following, the most likely inborn error of metabolism in this infant is: A. Mitochondrial energy disorder. B. Organic acidemia. C. Pyruvate metabolism defect. D. Transient hyperammonemia of the newborn. E. Urea cycle defect. 6. A 7-day-old term female newborn is lethargic and feeding poorly. Her blood glucose concentration is 7.0 mg/dl (0.39 mmol/l). Other laboratory tests reveal mild metabolic acidosis, elevated liver enzymes and blood ammonia, low urine ketones, and an abnormal plasma acylcarnitine profile. Chest radiography reveals a markedly enlarged heart. Of the following, the most likely inborn error of metabolism in this infant is: A. Fatty acid oxidation defect. B. Galactosemia. C. Glycogen storage disease. D. Hereditary fructose intolerance. E. Organic acidemia. e298 NeoReviews Vol.9 No.7 July 2008
10 Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese Neoreviews 2008;9;e291 DOI: /neo.9-7-e291 Updated Information & Services Subspecialty Collections Permissions & Licensing Reprints including high resolution figures, can be found at: This article, along with others on similar topics, appears in the following collection(s): Fetus and Newborn Infant orn_infant Genetics/Dysmorphology smorphology Metabolic Disorders isorders Information about reproducing this article in parts (figures, tables) or in its entirety can be found online at: /site/misc/permissions.xhtml Information about ordering reprints can be found online: /site/misc/reprints.xhtml
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition
 Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
INBORN ERRORS OF METABOLISM (IEM) IAP UG Teaching slides
 INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
The spectrum and outcome of the. neonates with inborn errors of. metabolism at a tertiary care hospital
 The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD
 Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
Metabolic Disorders. Chapter Thomson - Wadsworth
 Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Inborn Errors of Metabolism (IEM)
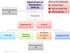 Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Dysmorphology Guy Besley
 Dysmorphology Guy Besley Willink Biochemical Genetics Unit, Manchester Children s s Hospital Dysmorphic presentation Congenital malformation Disorder of embryogenesis Intrauterine insult infection; chromosomal/genetic
Dysmorphology Guy Besley Willink Biochemical Genetics Unit, Manchester Children s s Hospital Dysmorphic presentation Congenital malformation Disorder of embryogenesis Intrauterine insult infection; chromosomal/genetic
Metabolic Changes in ASD. Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius
 Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis)
 Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Introduction to Organic Acidemias. Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.
 Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Inborn Errors of Metabolism in the Emergency Department. Will Davies June 2014
 Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Medical Foods for Inborn Errors of Metabolism
 Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up
 HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism
 Indian J Pediatr (July 2011) 78(7):854 859 DOI 10.1007/s12098-011-0422-0 SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika
Indian J Pediatr (July 2011) 78(7):854 859 DOI 10.1007/s12098-011-0422-0 SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika
Module : Clinical correlates of disorders of metabolism Block 3, Week 2
 Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE
 THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when
 CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
So Much More Than The PKU Test
 Newborn Metabolic Screening So Much More Than The PKU Test Sarah Viall, MSN, PPCNP BC Newborn Screening Program Coordinator Division of Genetics & Metabolism Conflicts of Interest I have no conflicts of
Newborn Metabolic Screening So Much More Than The PKU Test Sarah Viall, MSN, PPCNP BC Newborn Screening Program Coordinator Division of Genetics & Metabolism Conflicts of Interest I have no conflicts of
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children
 National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet
 Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet Website:www.tipn.org.tw Telephone:(02)85962050 Ext. 401-403 Service line:(02)85962065 Fax:(02)85962067
Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet Website:www.tipn.org.tw Telephone:(02)85962050 Ext. 401-403 Service line:(02)85962065 Fax:(02)85962067
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review -
 Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Training Syllabus CLINICAL SYLLABUS
 Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
Presentation and investigation of mitochondrial disease in children
 Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Metabolic diseases of the liver
 Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Genetics
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Genetics 1. GOAL: Understand the role of the pediatrician in preventing genetic disease, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Genetics 1. GOAL: Understand the role of the pediatrician in preventing genetic disease, and in counseling and screening
Paediatric Clinical Chemistry
 Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Inborn Errors of Metabolism
 30 Inborn Errors of Metabolism Inborn errors of metabolism (IEM) are disorders in which there is a block in the normal metabolic pathway that is caused by a genetic defect of a specific enzyme. The number
30 Inborn Errors of Metabolism Inborn errors of metabolism (IEM) are disorders in which there is a block in the normal metabolic pathway that is caused by a genetic defect of a specific enzyme. The number
Newborn Screening in Manitoba. Information for Health Care Providers
 Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
7 Medical Genetics. Hemoglobinopathies. Hemoglobinopathies. Protein and Gene Structure. and Biochemical Genetics
 SESSION 7 Medical Genetics Hemoglobinopathies and Biochemical Genetics J a v a d F a s a J a m s h i d i U n i v e r s i t y o f M e d i c a l S c i e n c e s, N o v e m b e r 2 0 1 7 Hemoglobinopathies
SESSION 7 Medical Genetics Hemoglobinopathies and Biochemical Genetics J a v a d F a s a J a m s h i d i U n i v e r s i t y o f M e d i c a l S c i e n c e s, N o v e m b e r 2 0 1 7 Hemoglobinopathies
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE
 SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting
 Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Best Practice Guidelines for the Biochemical Investigation of Patients with Foetal and Neonatal Hydrops
 National Metabolic Biochemistry Network Best Practice Guidelines for the Biochemical Investigation of Patients with Foetal and Neonatal Hydrops INTRODUCTION Hydrops is defined as the presence of skin oedema
National Metabolic Biochemistry Network Best Practice Guidelines for the Biochemical Investigation of Patients with Foetal and Neonatal Hydrops INTRODUCTION Hydrops is defined as the presence of skin oedema
Dr Rodney Itaki Lecturer Anatomical Pathology Discipline. University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology
 Fetal & Neonatal Pathology Dr Rodney Itaki Lecturer Anatomical Pathology Discipline University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology Self-Directed Reading Topics
Fetal & Neonatal Pathology Dr Rodney Itaki Lecturer Anatomical Pathology Discipline University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology Self-Directed Reading Topics
Neonatal Guidelines. Chapter 10: Metabolic V Date Revised : January 2017 Ratified 6 th February Date for Review: 1 st of March 2021
 Neonatal Guidelines Chapter 10: Metabolic V2017.1 Specialty: Neonatal Medicine Revised by: Jean Matthes Date Revised : January 2017 Ratified 6 th February 2017 Approved by: ABMU Joint Perinatal Forum Date
Neonatal Guidelines Chapter 10: Metabolic V2017.1 Specialty: Neonatal Medicine Revised by: Jean Matthes Date Revised : January 2017 Ratified 6 th February 2017 Approved by: ABMU Joint Perinatal Forum Date
Nutritional Management of Inborn Errors of Metabolism. Kay Davis, RD, CSP Esther Berenhaut, RD, CSP, CSR Aug 28, 2017
 Nutritional Management of Inborn Errors of Metabolism Kay Davis, RD, CSP Esther Berenhaut, RD, CSP, CSR Aug 28, 2017 OBJECTIVES Brief overview of newborn screening of metabolic disorders, inheritance patterns.
Nutritional Management of Inborn Errors of Metabolism Kay Davis, RD, CSP Esther Berenhaut, RD, CSP, CSR Aug 28, 2017 OBJECTIVES Brief overview of newborn screening of metabolic disorders, inheritance patterns.
Inborn error of metabolism
 Inborn error of metabolism The lecture is given by Dr Kefah Al qa qa, Consultant metabolic pediatrician, in Queen Rania Al Abdulla children hospital, on Thursday 11/12/2014. Let s tart Metabolism: refers
Inborn error of metabolism The lecture is given by Dr Kefah Al qa qa, Consultant metabolic pediatrician, in Queen Rania Al Abdulla children hospital, on Thursday 11/12/2014. Let s tart Metabolism: refers
HEREDITARY METABOLIC DISEASES
 HEREDITARY METABOLIC DISEASES Particular risk factors are: Advanced maternal age (e.g. Down's syndrome) Family history of inherited diseases (e.g. fragile X syndrome, Huntington's chorea) Previous child
HEREDITARY METABOLIC DISEASES Particular risk factors are: Advanced maternal age (e.g. Down's syndrome) Family history of inherited diseases (e.g. fragile X syndrome, Huntington's chorea) Previous child
NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA
 NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS NEONATAL HYPOGLYCEMIA? Glucose concentration low enough to cause signs and symptoms of impaired brain
NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS NEONATAL HYPOGLYCEMIA? Glucose concentration low enough to cause signs and symptoms of impaired brain
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012
 Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
The laboratory investigation of lactic acidaemia. J Bonham/T Laing
 The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
Childhood epilepsy: the biochemical epilepsies. Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary
 Childhood epilepsy: the biochemical epilepsies Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary Definitions Epileptic Seizure Manifestation(s) of epileptic (excessive and/or
Childhood epilepsy: the biochemical epilepsies Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary Definitions Epileptic Seizure Manifestation(s) of epileptic (excessive and/or
Metabolic Liver Disease
 Metabolic Liver Disease Peter Eichenseer, MD No relationships to disclose. Outline Overview Alpha-1 antitrypsin deficiency Wilson s disease Hereditary hemochromatosis Pathophysiology Clinical features
Metabolic Liver Disease Peter Eichenseer, MD No relationships to disclose. Outline Overview Alpha-1 antitrypsin deficiency Wilson s disease Hereditary hemochromatosis Pathophysiology Clinical features
Inborn Errors of Metabolism Clinical Approach to Diagnosis and Treatment
 Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
Positive Newborn Screens: What do you do next?
 Positive Newborn Screens: What do you do next? James B. Gibson, MD, Ph.D. Biochemical Geneticist at Specially for Children Clinical Associate Professor of Pediatrics UTHSCSA Carla R. Scott, MD Pediatric
Positive Newborn Screens: What do you do next? James B. Gibson, MD, Ph.D. Biochemical Geneticist at Specially for Children Clinical Associate Professor of Pediatrics UTHSCSA Carla R. Scott, MD Pediatric
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism
 Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital
 e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
Inborn errors of metabolism
 ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
Proceedings of a Consensus Conference for the
 Proceedings of a Consensus Conference for the Management of Patients with Urea Cycle Disorders Marshall Summar, MD, and Mendel Tuchman, MD In an effort to develop standards for the treatment of patients
Proceedings of a Consensus Conference for the Management of Patients with Urea Cycle Disorders Marshall Summar, MD, and Mendel Tuchman, MD In an effort to develop standards for the treatment of patients
Glycogen Storage Disease Type III, VI and IX - basics -
 Glycogen Storage Disease Type III, VI and IX - basics - Wyboston Lakes 10.10.2015 Urike Steuerwald Tórshavn / Hannover usteuerwald@web.de GSD III, VI and IX - Questions What goes wrong in glycogen storage
Glycogen Storage Disease Type III, VI and IX - basics - Wyboston Lakes 10.10.2015 Urike Steuerwald Tórshavn / Hannover usteuerwald@web.de GSD III, VI and IX - Questions What goes wrong in glycogen storage
Detection of inborn errors of metabolism in the newborn
 Arch Dis Child Fetal Neonatal Ed 2001;84:F205 F210 F205 REVIEW Willink Biochemical Genetics Unit, Manchester M27 4HA, UK A Chakrapani M A Cleary J E Wraith Correspondence to: Dr Cleary maureen@willink.demon.co.uk
Arch Dis Child Fetal Neonatal Ed 2001;84:F205 F210 F205 REVIEW Willink Biochemical Genetics Unit, Manchester M27 4HA, UK A Chakrapani M A Cleary J E Wraith Correspondence to: Dr Cleary maureen@willink.demon.co.uk
BCM 317 LECTURE OJEMEKELE O.
 BCM 317 LECTURE BY OJEMEKELE O. JAUNDICE Jaundice is yellowish discoloration of the skin, sclera and mucous membrane, resulting from an increased bilirubin concentration in the body fluid. It is usually
BCM 317 LECTURE BY OJEMEKELE O. JAUNDICE Jaundice is yellowish discoloration of the skin, sclera and mucous membrane, resulting from an increased bilirubin concentration in the body fluid. It is usually
The breakdown of fats to provide energy occurs in segregated membrane-bound compartments
 CPT1a deficiency The breakdown of fats to provide energy occurs in segregated membrane-bound compartments of the cell known as mitochondria. Carnitine palmitoyltransferase Ia (CPT1a) is a protein that
CPT1a deficiency The breakdown of fats to provide energy occurs in segregated membrane-bound compartments of the cell known as mitochondria. Carnitine palmitoyltransferase Ia (CPT1a) is a protein that
Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center
 Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center Kefah Al-Qa qa MD*, Wajdi Amayreh MD*, Ali Al-Hawamdeh MD* ABSTRACT Objective: To describe the different
Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center Kefah Al-Qa qa MD*, Wajdi Amayreh MD*, Ali Al-Hawamdeh MD* ABSTRACT Objective: To describe the different
Summary. Syndromic versus Etiologic. Definitions. Why does it matter? ASD=autism
 Summary It is becoming clear that multiple genes with complex interactions underlie autism spectrum (ASD). A small subset of people with ASD, however, actually suffer from rare single-gene Important to
Summary It is becoming clear that multiple genes with complex interactions underlie autism spectrum (ASD). A small subset of people with ASD, however, actually suffer from rare single-gene Important to
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA
 UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
Newborn Screening: Blood Spot Disorders
 Newborn Screening: Blood Spot Disorders Arizona s Newborn Screening Program Program Overview Panel of Disorders Disorder Descriptions Program Components Hospitals ADHS Lab ADHS Follow-up ADHS Billing Medical
Newborn Screening: Blood Spot Disorders Arizona s Newborn Screening Program Program Overview Panel of Disorders Disorder Descriptions Program Components Hospitals ADHS Lab ADHS Follow-up ADHS Billing Medical
Disorders of Carbohydrates. Disorders of Galactose Metabolism Glycogen Storage Diseases Diabetes Mellitus
 Disorders of Carbohydrates Metabolism Disorders of Galactose Metabolism Glycogen Storage Diseases Diabetes Mellitus Disorders of Galactose Metabolism GALACTOSE Galactose is a sugar that is found mainly
Disorders of Carbohydrates Metabolism Disorders of Galactose Metabolism Glycogen Storage Diseases Diabetes Mellitus Disorders of Galactose Metabolism GALACTOSE Galactose is a sugar that is found mainly
INBORN ERRORS OF METABOLISM: REVIEW AND DATA FROM A TERTIARY CARE CENTER
 Indian Journal of Clinical Biochemistry, 2009 / 24 (3) 215-222 REVIEW ARTICLE INBORN ERRORS OF METABOLISM: REVIEW AND DATA FROM A TERTIARY CARE CENTER Ananth N Rao, J Kavitha, Minakshi Koch and Suresh
Indian Journal of Clinical Biochemistry, 2009 / 24 (3) 215-222 REVIEW ARTICLE INBORN ERRORS OF METABOLISM: REVIEW AND DATA FROM A TERTIARY CARE CENTER Ananth N Rao, J Kavitha, Minakshi Koch and Suresh
Isovaleric Acidemia: Quick reference guide
 Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Neonatal Hypotonia. Encephalopathy acute No encephalopathy. Neurology Chapter of IAP
 The floppy infant assumes a frog legged position. On ventral suspension, the baby can not maintain limb posture against gravity and assumes the position of a rag doll. Encephalopathy acute No encephalopathy
The floppy infant assumes a frog legged position. On ventral suspension, the baby can not maintain limb posture against gravity and assumes the position of a rag doll. Encephalopathy acute No encephalopathy
Metabolic Emergencies and the Pediatrician
 Metabolic Emergencies and the Pediatrician Stephen G. Kahler, MD Professor of Pediatrics Section of Genetics and Metabolism, UAMS and ACH Hot Springs, AR March 8, 2012 INHERITED METABOLIC DISORDERS HOW
Metabolic Emergencies and the Pediatrician Stephen G. Kahler, MD Professor of Pediatrics Section of Genetics and Metabolism, UAMS and ACH Hot Springs, AR March 8, 2012 INHERITED METABOLIC DISORDERS HOW
UREA CYCLE DISORDERS - The What, Why, How and When
 UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
Inborn Error Of Metabolism :
 Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff
 Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
Selective newborn screening of amino acid, fatty acid and organic acid disorders in the Kingdom of Bahrain.
 Selective newborn screening of amino acid, fatty acid and organic acid disorders in the Kingdom of Bahrain. Jamal Golbahar PhD Associate Professor of Molecular Medicine, Department of Molecular Medicine,
Selective newborn screening of amino acid, fatty acid and organic acid disorders in the Kingdom of Bahrain. Jamal Golbahar PhD Associate Professor of Molecular Medicine, Department of Molecular Medicine,
Diabetic Ketoacidosis
 Diabetic Ketoacidosis Definition: Diabetic Ketoacidosis is one of the most serious acute complications of diabetes. It s more common in young patients with type 1 diabetes mellitus. It s usually characterized
Diabetic Ketoacidosis Definition: Diabetic Ketoacidosis is one of the most serious acute complications of diabetes. It s more common in young patients with type 1 diabetes mellitus. It s usually characterized
Most common metabolic disorders in childhood. Neonatal screening and diagnostic approach to the. Inborn errors of metabolism (IEM)
 Department of Pediatrics and Developmental Disorders Medical University of Bialystok Most common metabolic disorders in childhood. Neonatal screening and diagnostic approach to the inborn errors of metabolism
Department of Pediatrics and Developmental Disorders Medical University of Bialystok Most common metabolic disorders in childhood. Neonatal screening and diagnostic approach to the inborn errors of metabolism
Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT
 Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Metabolism of pentoses, glycogen, fructose and galactose. Jana Novotna
 Metabolism of pentoses, glycogen, fructose and galactose Jana Novotna 1. The Pentose Phosphate Pathway The pentose phosphate pathway (PPP): (hexose monophosphate or 6-phosphogluconate patway) Process that
Metabolism of pentoses, glycogen, fructose and galactose Jana Novotna 1. The Pentose Phosphate Pathway The pentose phosphate pathway (PPP): (hexose monophosphate or 6-phosphogluconate patway) Process that
A Guide for Prenatal Educators
 A Guide for Prenatal Educators Why Teach Newborn Screening This booklet is designed to make it easy for you, a prenatal educator, to effectively inform expectant parents about newborn screening. All of
A Guide for Prenatal Educators Why Teach Newborn Screening This booklet is designed to make it easy for you, a prenatal educator, to effectively inform expectant parents about newborn screening. All of
Pediatric metabolic bone diseases
 Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Management. (By the World Health Organization according to the magnitude of the enzyme deficiency and the severity of hemolysis)
 Glucose-6-Phosphate Dehydrogenase (G6PD) Deficiency Management Definition: Glucose-6-phosphate dehydrogenase (G6PD) deficiency is an inherited disorder caused by a genetic defect in the red blood cell
Glucose-6-Phosphate Dehydrogenase (G6PD) Deficiency Management Definition: Glucose-6-phosphate dehydrogenase (G6PD) deficiency is an inherited disorder caused by a genetic defect in the red blood cell
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE. Bwee Tien Poll-The Amsterdam UMC The Netherlands
 CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
NEWBORN METABOLIC SCREEN, MINNESOTA
 Lab Dept: Test Name: Chemistry NEWBORN METABOLIC SCREEN, MINNESOTA General Information Lab Order Codes: Synonyms: CPT Codes: Test Includes: PKUN Newborn Screen for Hyopothyroidism, Phenylketonuria (PKU),
Lab Dept: Test Name: Chemistry NEWBORN METABOLIC SCREEN, MINNESOTA General Information Lab Order Codes: Synonyms: CPT Codes: Test Includes: PKUN Newborn Screen for Hyopothyroidism, Phenylketonuria (PKU),
Pediatrics. Pyruvate Kinase Deficiency (PKD) Symptoms and Treatment. Definition. Epidemiology of Pyruvate Kinase Deficiency.
 Pediatrics Pyruvate Kinase Deficiency (PKD) Symptoms and Treatment See online here Pyruvate kinase deficiency is an inherited metabolic disorder characterized by a deficiency in the enzyme "pyruvate kinase"
Pediatrics Pyruvate Kinase Deficiency (PKD) Symptoms and Treatment See online here Pyruvate kinase deficiency is an inherited metabolic disorder characterized by a deficiency in the enzyme "pyruvate kinase"
Glycogen Storage Disease Type III also known as Cori or Forbe s Disease/Debrancher Enzyme Deficiency
 Glycogen Storage Disease Type III also known as Cori or Forbe s Disease/Debrancher Enzyme Deficiency What is GSDIII? Glycogen Storage Disease type 3 is an inherited condition caused by a defect in a gene
Glycogen Storage Disease Type III also known as Cori or Forbe s Disease/Debrancher Enzyme Deficiency What is GSDIII? Glycogen Storage Disease type 3 is an inherited condition caused by a defect in a gene
Methylmalonic aciduria
 Methylmalonic aciduria Introductory information Written by: F. Hörster, S. Kölker & P. Burgard Reviewed & Revised for North America by: S. van Calcar Methylmalonic aciduria MMA 2 Methylmalonic aciduria
Methylmalonic aciduria Introductory information Written by: F. Hörster, S. Kölker & P. Burgard Reviewed & Revised for North America by: S. van Calcar Methylmalonic aciduria MMA 2 Methylmalonic aciduria
Fatty Acid Oxidation Disorders
 Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social
Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social
TRANSAMINATION AND UREA CYCLE
 TRANSAMINATION AND UREA CYCLE USMAN SUMO FRIEND TAMBUNAN ARLI ADITYA PARIKESIT SEPTIANA BIOINFORMATICS GROUP DEPARTEMENT OF CHEMISTRY FACULTY OF MATHEMATIC AND SCIENCE UNIVERSITY OF INDONESIA What is transamination?
TRANSAMINATION AND UREA CYCLE USMAN SUMO FRIEND TAMBUNAN ARLI ADITYA PARIKESIT SEPTIANA BIOINFORMATICS GROUP DEPARTEMENT OF CHEMISTRY FACULTY OF MATHEMATIC AND SCIENCE UNIVERSITY OF INDONESIA What is transamination?
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015
 Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS
 PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS SPECIFIC WAYS OF AMINO ACID CATABOLISM After removing of amino group the carbon skeletons of amino acids are transformed into metabolic
PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS SPECIFIC WAYS OF AMINO ACID CATABOLISM After removing of amino group the carbon skeletons of amino acids are transformed into metabolic
ANATOMY OF A METABOLIC CRISIS: FAOD-style. Mark S. Korson, MD Tufts Medical Center Boston, MA
 ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
Glycogen Storage Disease
 Glycogen Storage Disease 1 Introduction The food we eat is usually used for growth, tissue repair and energy. The body stores what it does not use. Excess sugar, or glucose, is stored as glycogen in the
Glycogen Storage Disease 1 Introduction The food we eat is usually used for growth, tissue repair and energy. The body stores what it does not use. Excess sugar, or glucose, is stored as glycogen in the
Genetic Testing FOR DISEASES OF INCREASED FREQUENCY IN THE ASHKENAZI JEWISH POPULATION
 Carrier Screening and Diagnostic Testing for the Ashkenazi Jewish Population Genetic Testing FOR DISEASES OF INCREASED FREQUENCY IN THE ASHKENAZI JEWISH POPULATION Our Science. Your Care. An extensive
Carrier Screening and Diagnostic Testing for the Ashkenazi Jewish Population Genetic Testing FOR DISEASES OF INCREASED FREQUENCY IN THE ASHKENAZI JEWISH POPULATION Our Science. Your Care. An extensive
Inborn Errors of Metabolism. Metabolic Pathway. Digestion and Fasting. How is Expanded Newborn Screening Different? MS/MS. The body is a factory.
 Inborn Errors of Metabolism The body is a factory. Inborn errors of metabolism are rare genetic disorders in which the body cannot properly turn food into energy. The disorders are usually caused by defects
Inborn Errors of Metabolism The body is a factory. Inborn errors of metabolism are rare genetic disorders in which the body cannot properly turn food into energy. The disorders are usually caused by defects
NEONATAL MUSCULAR HYPOTONIA
 NEONATAL MUSCULAR HYPOTONIA Differential Diagnosis Systemic causes of neonatal hypotonia should be identified rapidly as they are usually transient if treated appropriately. Major differential diagnoses
NEONATAL MUSCULAR HYPOTONIA Differential Diagnosis Systemic causes of neonatal hypotonia should be identified rapidly as they are usually transient if treated appropriately. Major differential diagnoses
Hereditary disorders of peroxisomal metabolism.
 Hereditary disorders of peroxisomal metabolism http://www.cytochemistry.net/cell-biology/perox.jpg Peroxisomes single membrane organelles from less than 100 to more than 1000 per eukaryotic cell more than
Hereditary disorders of peroxisomal metabolism http://www.cytochemistry.net/cell-biology/perox.jpg Peroxisomes single membrane organelles from less than 100 to more than 1000 per eukaryotic cell more than
Clinical evaluation Jaundice skin and mucous membranes
 JAUNDICE Framework The definition of Neonatal Jaundice Billirubin Metabolism Special characteristic in neonates Dangerous of the Hyperbillirubinemia The diseases in relation with Neonatal Jaundice Objectives:
JAUNDICE Framework The definition of Neonatal Jaundice Billirubin Metabolism Special characteristic in neonates Dangerous of the Hyperbillirubinemia The diseases in relation with Neonatal Jaundice Objectives:
Fatty Acid Oxidation Disorders- an update. Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London
 Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology
 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology 1 PBL SEMINAR ACUTE & CHRONIC ETHANOL EFFECTS An Overview Sites
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology 1 PBL SEMINAR ACUTE & CHRONIC ETHANOL EFFECTS An Overview Sites
MEDICAL GENETICS CLINICAL CARE ROTATION
 Medical Genetics Clinical Care Rotation 1 MEDICAL GENETICS CLINICAL CARE ROTATION Overview: The Medical Genetics Clinical Care Rotation (MGC) is the backbone of the clinical genetics experience for the
Medical Genetics Clinical Care Rotation 1 MEDICAL GENETICS CLINICAL CARE ROTATION Overview: The Medical Genetics Clinical Care Rotation (MGC) is the backbone of the clinical genetics experience for the
Hereditary disorders of peroxisomal metabolism.
 Hereditary disorders of peroxisomal metabolism http://www.cytochemistry.net/cell-biology/perox.jpg Peroxisomes single membrane organelles from less than 100 to more than 1000 per eucaryotic cell more than
Hereditary disorders of peroxisomal metabolism http://www.cytochemistry.net/cell-biology/perox.jpg Peroxisomes single membrane organelles from less than 100 to more than 1000 per eucaryotic cell more than
Alvaro Serrano Russi MD University of Iowa Hospitals and Clinics
 Retrospective Analysis of the Region 4 Post Analytical Tool and Confirmatory Testing for Long Chain Fatty Acid Oxidation Disorders Screened in the State of Iowa Alvaro Serrano Russi MD University of Iowa
Retrospective Analysis of the Region 4 Post Analytical Tool and Confirmatory Testing for Long Chain Fatty Acid Oxidation Disorders Screened in the State of Iowa Alvaro Serrano Russi MD University of Iowa
Paediatric Hypoglycaemia and the Laboratory. AACB Webinar, 8 th April 2015 Tina Yen
 Paediatric Hypoglycaemia and the Laboratory AACB Webinar, 8 th April 2015 Tina Yen Synopsis Definition and classification Newborn and Neonatal Hypoglycaemia Transient Persistant Hypoglycaemia in infants
Paediatric Hypoglycaemia and the Laboratory AACB Webinar, 8 th April 2015 Tina Yen Synopsis Definition and classification Newborn and Neonatal Hypoglycaemia Transient Persistant Hypoglycaemia in infants
CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE. Dr. Bahar Naghavi
 2 CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE Dr. Bahar Naghavi Assistant professor of Basic Science Department, Shahid Beheshti University of Medical Sciences, Tehran,Iran 3 Introduction Over 4000
2 CURRENT GENETIC TESTING TOOLS IN NEONATAL MEDICINE Dr. Bahar Naghavi Assistant professor of Basic Science Department, Shahid Beheshti University of Medical Sciences, Tehran,Iran 3 Introduction Over 4000
11/8/12. KERNICTERUS: The reason we have to care about bilirubin. MANAGING JAUNDICE IN THE BREASTFEEDING INFANT AKA: Lack of Breastfeeding Jaundice
 MANAGING JAUNDICE IN THE BREASTFEEDING INFANT AKA: Lack of Breastfeeding Jaundice November 16, 2012 Orange County Lawrence M. Gartner, M.D. University of Chicago and Valley Center, California KERNICTERUS:
MANAGING JAUNDICE IN THE BREASTFEEDING INFANT AKA: Lack of Breastfeeding Jaundice November 16, 2012 Orange County Lawrence M. Gartner, M.D. University of Chicago and Valley Center, California KERNICTERUS:
ACUTE & CHRONIC ETHANOL EFFECTS An Overview
 ACUTE & CHRONIC ETHANOL EFFECTS An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Clinical Biochemistry: PBL Seminar MBBS Yr 4 VJ Temple
ACUTE & CHRONIC ETHANOL EFFECTS An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Clinical Biochemistry: PBL Seminar MBBS Yr 4 VJ Temple
Case Reports. Neonatal Seizure: A Rare Aetiology Easily Missed by Routine Metabolic Screening LY SIU, L KWONG, SN WONG, NS KWONG
 HK J Paediatr (new series) 2009;14:37-41 Case Reports Neonatal Seizure: A Rare Aetiology Easily Missed by Routine Metabolic Screening LY SIU, L KWONG, SN WONG, NS KWONG Abstract Key words We present the
HK J Paediatr (new series) 2009;14:37-41 Case Reports Neonatal Seizure: A Rare Aetiology Easily Missed by Routine Metabolic Screening LY SIU, L KWONG, SN WONG, NS KWONG Abstract Key words We present the
بنام خدا هیپوگلیسمی درنوزادان و گاالکتوزمی دکتر انتظاری
 بنام خدا هیپوگلیسمی درنوزادان و گاالکتوزمی دکتر انتظاری Serum glucose< 35 mg/dl 1-3 hr of life < 40 mg/dl 3-24 hr < 45 mg/dl after 24 hr 10% NL newborns can t maintain BS>30 if delayed feeding >3-6 hrs
بنام خدا هیپوگلیسمی درنوزادان و گاالکتوزمی دکتر انتظاری Serum glucose< 35 mg/dl 1-3 hr of life < 40 mg/dl 3-24 hr < 45 mg/dl after 24 hr 10% NL newborns can t maintain BS>30 if delayed feeding >3-6 hrs
