HOPE. Doa'a Al Zou'bi
|
|
|
- Hester Baldwin
- 6 years ago
- Views:
Transcription
1 Anemia & Nutritional Anemia HOPE Doa'a Al Zou'bi
2 Anemia CASE : A 22 month old boy presents to your office with a chief complaint of pallor. A visiting relative who has not seen the child for 5 months told his mother that the boy appears pale. The mother brings him in for a checkup even though she notices no change in his coloring (he has always been fair skinned). On review of symptoms you find that he is an active toddler, with no recent fatigue, exercise intolerance, or increase in sleeping. He has had no blood in his diapers and no black or tarry stools. He is a picky eater, taking small amounts of chicken, pork and some vegetables, but loves milk and drinks six to eight bottles of whole milk per day. Family history reveals a distant aunt who had anemia when she was pregnant but which subsequently resolved. There is no history of splenectomy, gall stones at an early age, or other anemia in the family. Exam: VS: T 37.5, BP 90/52, P 145, RR 16, Height 85.5 cm (50th %ile), Weight 13.2 kg (75th %ile). General appearance: He is a pale appearing, active toddler, holding a bottle, tearing and eating paper from your exam table. Eyes: No scleral icterus. Pale conjunctiva. Mouth: Dental caries. Chest: Clear. Heart: Mild tachycardia as above, grade II/VI systolic ejection murmur heard best over the upper left sternal border. Abdomen: No hepatosplenomegaly. Rectal: Dark brown, soft stool, negative for occult blood. CBC: WBC 6,100, Hgb 6.2 g/dl, Hct 19.8%, Plt 589,000, MCV 54 fl, RDW 17%. Reticulocyte count is 1.8%. The lab reports microcytosis, hypochromia, mild anisocytosis and polychromasia. There is no basophilic stippling. You correctly diagnose iron deficiency anemia, start oral iron and limit his milk intake. You see him in 3 days to assure compliance and his RDW is 27% and his reticulocyte count 17%. When you see him back in two weeks his mother is amazed at his new interest in table foods. His Hgb is now 8.5 g/dl, and his MCV 64 fl. Two months later his hemoglobin has completely normalized, and you continue iron therapy for three more months. 1
3 Anemia occurs when the red blood cell mass or hemoglobin content is too low to meet a person's physiologic demands. In children, "normal" levels vary with age, gender, and geographic location (height above sea level). A summary of normal values is listed below : Lower limit (3rd %ile) of normal hemoglobin (Hgb column) and lower (3rd %ile) and upper (97th %ile) limit of normal MCV by age and sex (M=males, F=females). Age Hgb (g/dl) Lower MCV limit Upper MCV limit (F), 13(M) Over 18 12(F), 14(M) Signs of anemia : 1) pallor of the skin, conjunctiva, and mucous membranes, 2) tachycardia, 3) orthostatic hypotension, 4) heart murmur and 5) edema. Symptoms 1) fatigue, 2) headache, 3) dizziness and 4) dyspnea. Other signs and symptoms depend on the cause for anemia, such as jaundice, dark urine, or splenomegaly in hemolytic anemias. When the diagnosis of anemia is suspected based on signs and symptoms, it can quickly be confirmed by laboratory evaluation. The more difficult task is determining the etiology. Testing for all these causes at once would be 2
4 inefficient, time consuming, and expensive. It is, in fact, unnecessary because the differential diagnosis can be narrowed significantly by careful history and examination. Two classification schemes are frequently employed to narrow down the differential diagnosis in anemia. The first one uses the MCV to classify the size of the red blood cell as microcytic ( decrease MCV ), normocytic ( normal ), or macrocytic ( increased ). Since MCV values in children vary with age, the age specific MCV values must be used (See Table 1). Even so, certain conditions do not fit neatly into one category. Microcytic anemias include iron deficiency, thalassemia, chronic inflammation, lead poisoning, and sideroblastic anemia. Normocytic anemias include acute blood loss, immune hemolytic anemia, hereditary spherocytosis, G6PD deficiency, sickle cell anemia, renal disease, and transient erythroblastopenia of childhood (TEC). Macrocytic anemias include folate deficiency, B12 deficiency, liver disease, hypothyroidism, neoplasms and bone marrow failure syndromes such as aplastic anemia, Diamond-Blackfan anemia (DBA) and congenital dyserythropoietic anemia (CDEA) The anemia of inflammation/chronic disease and of lead poisoning can be microcytic or normocytic, and the anemia seen with liver failure can be normocytic or macrocytic. The second classification scheme categorizes anemia by its mechanism. If a patient's hemoglobin is low, it is due to one of three basic reasons: he/she is either not making adequate amounts (decreased production), destroying it (increased destruction), losing it from somewhere (blood loss). Increased destruction A high reticulocyte count indicates that the patient is able to adequately make red cells and is trying to compensate for the anemia, suggesting the cause to be blood loss or destruction. Signs of destruction include : jaundice, 3
5 elevated bilirubin, dark urine, splenomegaly, schistocytes and microspherocytes on peripheral smear, low serum haptoglobin, & Reticulosytosis. Increased destruction results from immune hemolytic disease, hereditary spherocytosis, G6PD deficiency, sickle cell disease, thalassemia, DIC (disseminated intravascular coagulation), mechanical heart valves, burns, PNH (paroxysmal nocturnal hemoglobinuria), and hypersplenism. Decreased production results from iron, folate, or B-12 deficiency, lead toxicity, thalassemia, aplastic anemia, chronic inflammation, neoplasms, TEC, DBA, renal disease, hypothyroidism, CDEA (congenital dyserythropoietic anemia), and sideroblastic anemia. A low reticulocyte count suggests decreased production. Blood loss results from acute hemorrhage, pulmonary hemosiderosis (pulmonary hemorrhage), Goodpasture's disease, and gastrointestinal blood loss (peptic ulcer disease, other GI conditions). ** Now,, We'll take about nutritional anemia,, other types pf anemia will be discussed in other lectures Iron Deficiency Anemia Anemia resulting from lack of sufficient iron for synthesis of hemoglobin, it is the most common hematologic disease of infancy and childhood. Infants fed cow's milk when younger than 1 year of age, toddlers fed large volumes of cow's milk, and menstruating teenage girls who are not receiving supplemental iron are at high risk for iron deficiency. Iron, the most abundant trace mineral, is used in the synthesis of hemoglobin, myoglobin, and enzyme iron. Body iron content is regulated primarily through modulation of iron absorption, which depends on the state of body iron stores, the form and amount of iron in foods, and the mixture of foods in the diet. There are two categories of iron in food. 4
6 1) Heme iron, present in hemoglobin and myoglobin, which is supplied by meat and rarely accounts for more than one fourth of the iron ingested by infants. The absorption of heme iron is relatively efficient and is not influenced by other constituents of the diet. 2) Nonheme iron, which represents the preponderance of iron intake consumed by infants and exists in the form of iron salts. The absorption of nonheme iron is influenced by the composition of consumed foods. Eitology : Enhancers of nonheme iron absorption are ascorbic acid, meat, fish, and poultry. Inhibitors are bran, polyphenols (including the tannates in tea), and phytic acid, a compound found in legumes and whole grains. In a normal term infant, there is little change in total body iron and little need for exogenous iron before 4 months of age. Iron deficiency is rare in term infants during the first 4 months, unless there has been substantial blood loss. After about 4 months of age, iron reserves become marginal, and, unless exogenous sources of iron are provided, the infant becomes progressively at risk for anemia as the iron requirement to support erythropoiesis and growth increases. Premature or low birth weight infants, have a lower amount of stored iron because : 1- Significant amounts of iron are transferred from the mother in the third trimester. 2- Their postnatal iron needs are greater because of rapid rates of growth and when frequent phlebotomy occurs ( in NICU ). Under normal circumstances, iron-fortified formula should be the only alternative to breast milk in infants younger than 1 year of age. Premature infants fed human milk may develop iron deficiency anemia earlier unless they receive iron supplements. Formula-fed preterm infants should receive iron-fortified formula. 5
7 In older children, iron deficiency may result from inadequate iron intake with excessive cow's milk intake or from intake of foods with poor iron bioavailability. >> Early introduction (at age 6 or 8 months) of whole cow's milk into the diet is clearly associated with iron deficiency anemia. This is due to three factors : 1) Cow's milk exerts a direct toxic effect on the intestinal mucosa of infants, leading to prolonged microscopic blood loss in the stools. 2) The caloric value of whole cow's milk is high due to fat content, decreasing the appetite and leading to less intake of potential iron-rich foods. 3) The bioavailability of iron in cow's milk is low (Iron is absorbed two to three times more efficiently from human milk than from cow's milk). >> The American Academy of Pediatrics recommends that cow's milk not be used in the first year of life. >> Blood loss must be considered as a possible cause in every case of iron deficiency anemia, particularly in older children. Chronic iron-deficiency anemia can be caused by occult bleeding from a lesion in the gastrointestinal tract, such as milk protein induced inflammatory colitis, peptic ulcer, Meckel diverticulum, polyp, hemangioma, or inflammatory bowel disease or blood loss because of menses. >> Hemolytic anemia generally do not lead to iron deficiency because the body reuses the freed iron. Manifestation : Anemia ( go back to anemia signs and symptoms), spoon nails, Glossitis, angular stomatitis, reduced muscle and mental performance, Pica, Irritability & Poor Appetite. Pica is characterized by an appetite for substances largely non-nutritive, such as ice, clay, chalk, soil, or sand. Pallor is the most important sign of iron deficiency. In mild to moderate iron deficiency (hemoglobin levels of 6-10 g/dl), compensatory mechanisms, including increased levels of 2,3- diphosphoglycerate (2,3-DPG) and a shift of the oxygen dissociation curve, may be so effective that few symptoms of anemia are noted, although affected children may be irritable.(( Iron deficiency may be present without anemia )) 6
8 Irritability and anorexia are characteristic of advanced cases ( Hb < 5 g/dl ) may reflect deficiency in tissue iron. Pica associated with iron deficiency increases the likelihood of ingestion of lead-contaminated items >> lead poisoning >> more anemia. Iron deficiency affects many tissues (muscle and central nervous system) in addition to producing anemia. Iron deficiency and anemia have been associated with lethargy and decreased work capacity and impaired neurocognitive development, Iron deficiency in infancy may be associated with later cognitive deficits and poor school performance,,,, deficits may be irreversible when onset is in the first 2 years of life, thus it should be recognized early and treated adequately. Gastrointestinal dysfunction, and impaired WBC and T cell function have been associated with iron deficiency. Diagnosis : Is established by the presence of a microcytic hypochromic anemia, low serum ferritin levels, low serum iron levels, reduced transferrin saturation, normal to elevated red blood cell width distribution and enhanced ironbinding capacity. The mean corpuscular volume and red blood cell indices are reduced, and the reticulocyte count is low. The red cell distribution width (RDW), a measure of the difference in size between the smallest and largest RBCs in circulation, may be elevated, denoting a dual population of cells: small (microcytic) iron deficient cells and some normocytic cells with adequate iron. A bone marrow sample stained for iron shows no iron stores. This test is most definitive, but generally unnecessary and invasive. Differential Diagnosis : Iron deficiency must be differentiated from other hypochromic microcytic anemias. The most common scenario is the need to distinguish iron deficiency from α- and β-thalassemia trait and other hemoglobinopathies, particularly those related to hemoglobin E. A simple distinguishing feature of the latter conditions is that the RBC count often is elevated above normal despite the presence of a mild anemia and microcytosis; and this is in marked contrast to iron deficiency in which the RBC count decreases along with the reduced hemoglobin and MCV. Another difference between α- and β-thalassemia trait and iron deficiency is that the RDW is elevated in iron deficiency. 7
9 The anemia of chronic disease (ACD) and infection is usually normocytic, although occasionally it may be slightly microcytic. In contrast to iron-deficiency anemia, in these inflammatory conditions both the serum iron level and ironbinding capacity (transferrin) are reduced and serum ferritin levels are normal or elevated. The serum transferrin receptor (TfR) level is useful in the distinction between iron-deficiency anemia and anemia of chronic disease because it is not affected by inflammation. The concentration of TfR is elevated in iron deficiency and is within the normal range in anemia of chronic disease. An elevation of the TfR/log ferritin ratio is especially sensitive in detecting irondeficiency anemia. Lead poisoning and iron-deficiency anemia both are associated with elevations of free erythrocyte protoporphyrins (FEP). In cases of lead poisoning associated with iron deficiency, the RBCs are morphologically similar but coarse basophilic stippling of the RBCs is frequently prominent. Elevations of blood lead, FEP, and urinary coproporphyrin levels are seen. Treatment : In an otherwise healthy child, a therapeutic trial of iron is the best diagnostic study for iron deficiency as long as the child is re-examined and a response is documented. Treatment of iron deficiency anemia includes changes in the diet to provide adequate iron and the administration of 2 to 6 mg iron/kg/24 hr. (as ferrous sulfate) divided BID or TID. ( Nelson ) A usual therapeutic dose of 4 to 6 mg/day of elemental iron induces an increase in hemoglobin of 0.25 to 0.4 g/dl/day (a 1%/day increase in hematocrit). ( Nelson ) b.i.d. or bid or BID (on prescription): b.i.d. means twice (two times) a day. It is an abbreviation for "bis in die" which in Latin means twice a day. t.i.d. or tid or TID : is three times a day ; t.i.d. stands for "ter in die" (in Latin, 3 times a day). A dose of 3 mg/kg of elemental iron for mild anemia or 6 mg/kg for severe anemia should be instituted. ( case based book ) Oral ferrous sulfate, available in liquid or pill form, the liquid can stain the teeth so it should be given in juice rather than dropped directly into the mouth. Avoid giving it with milk as milk interferes with its absorption. 8
10 The response to oral iron includes rapid subjective improvement, especially in neurologic function (within hours) and reticulocytosis (48-72 hours); increase in hemoglobin levels (4-30 days); and repletion of iron stores (in 1-3 months). It should be continued for two to three months after normalization of blood counts to replete the total body iron stores. If the hemoglobin level fails to increase within 2 weeks after institution of iron treatment, careful re-evaluation for ongoing blood loss ((( Abnormal uterine bleeding and blood loss from the GI tract are common. Blood loss in the urine is rare, and from the lungs (idiopathic pulmonary hemosiderosis) is extremly rare. ))), development of infection, poor compliance, or other causes of microcytic anemia is required. Megaloblastic Anemia (rarely seen in children) Physiology : Vitamin B12 deficiency Vitamin B12 is essential for normal lipid and carbohydrate metabolism in energy production and in protein biosynthesis and nucleic acid synthesis. In contrast to other water-soluble vitamins, absorption of vitamin B12 is complex, involving cleavage of the vitamin from dietary protein and binding to a glycoprotein called intrinsic factor, which is secreted by the gastric mucosa (parietal cells). The cobalamin-intrinsic factor complex is efficiently absorbed from the distal ileum. As vitamin B12 is absorbed into the portal circulation, it is transported bound to a specific protein, transcobalamin II. Its large stores in the liver also are unusual as a water-soluble vitamin. Efficient enterohepatic circulation normally protects from deficiency for months to years. Etiology : Dietary sources of the vitamin are animal products only. Strict vegetarians should take a vitamin B12 supplement. Most cases in childhood result from a specific defect in absorption. Such defects include congenital pernicious anemia (absent intrinsic factor), juvenile pernicious anemia (autoimmune), and deficiency of transcobalamin II transport. infection with the fish tapeworm Diphyllobothrium latum. Gastric 9
11 or intestinal resection and small bowel bacterial overgrowth also cause vitamin B12 deficiency. Exclusively breastfed infants ingest adequate vitamin B12 unless the mother is a strict vegetarian without supplementation ( mothers have Vit. B12 deficiency ) Clinical Manifestations : Nonspecific manifestations such as : weakness, fatigue, failure to thrive, or irritability. Other common findings include pallor, glossitis, vomiting, diarrhea, and jaundice ( as a result of ineffective erythropoiesis ). Neurologic symptoms : these include paresthesias, sensory deficits, hypotonia, seizures, developmental delay, developmental regression, and neuropsychiatric changes. Neurologic problems from vitamin B12 deficiency can occur in the absence of any hematologic abnormalities. Folic acid deficiency Food sources include green leafy vegetables, oranges, and whole grain. Etiology : may result from a low dietary intake, malabsorption, or vitamin-drug interactions. Folate is particularly heat labile. Heat-sterilizing home-prepared formula can decrease the folate content by half. Evaporated milk and goat's milk are low in folate. Patients with chronic hemolysis (sickle cell anemia, thalassemia) may require extra folate to avoid deficiency because of the relatively high requirement of the vitamin to support erythropoiesis. Clinical manifestation : - S & S of anemia, glossitis, jaundice ( because of ineffective erythropiosis ). Laboratory Findings of megaloblastic anemia :: elevated MCV and mean corpuscular hemoglobin. 10
12 The peripheral blood smear shows numerous macro-ovalocytes with anisocytosis and poikilocytosis. Neutrophils are large and have hypersegmented nuclei. The white cell and platelet counts are normal with mild deficiencies, but may be decreased in more severe cases. Examination of the bone marrow typically shows erythroid hyperplasia with large erythroid and myeloid precursors. The serum indirect bilirubin concentration may be slightly elevated. ** Nuclear maturation is delayed compared with cytoplasmic maturation, and erythropoiesis is ineffective. Children with vit.b12 deficiency have a low serum vitamin B12 level, but decreased levels of serum vitamin B12 may also be found in about 30% of patients with folic acid deficiency. Serum levels of metabolic intermediates (methylmalonic acid and homocysteine) may help establish the correct diagnosis. Elevated methylmalonic acid levels are consistent with vit.b12 deficiency, whereas elevated levels of homocysteine occur with both vit.b12 and folate deficiency. Patients with vitamin B12 deficiency also have increased urine levels of methylmalonic acid. Diagnosis : The diagnosis is confirmed by low serum concentration of the vitamins. B12 deficiency requires a Schilling test to determine the cause of the B12 deficiency (intrinsic factor deficiency, malabsorption due to inflammatory bowel disease, etc.). Treatment : Treatment of vit.b12 deficiency due to inadequate dietary intake is readily accomplished with oral supplementation. Most cases of vitamin B12 deficiency in infants and children are not of dietary origin and require treatment throughout life. Maintenance therapy consists of repeated monthly intramuscular injections, although a form of vitamin B12 is administered intranasally. Folic acid deficiency is treated effectively with oral folic acid in most cases. Children at risk for the development of folic acid deficiencies, such as premature infants and those with chronic hemolysis, are often given folic acid prophylactically. By this we have finished the most imp. Topics in Nutritional anemia 11
13 Questions 1. What two classification schemes can be used to narrow down the differential diagnosis of anemia in children? 2. What laboratory finding suggests that an anemia is due to a decreased production of red blood cells? 3. What elements of the history, physical, and laboratory evaluation suggest increased red cell destruction as the cause of anemia? 4. What is the best test to rule in or rule out iron deficiency? Justify your answer. 5. True/False: A child raised in a lead based paint containing home that is well maintained has a significantly lower chance of lead poisoning than if that home is in disrepair. 6. True/False: Cow's milk exerts a direct toxic effect on the intestinal mucosa of some infants, leading to microscopic blood loss and iron deficiency anemia. 7. True/False: Children with iron deficiency anemia caused by excessive cow's milk intake often have a history of black or tarry stools. 8. True/False: The iron content of cow's milk is zero or very close to zero. 9. The lab reports a patient's hemoglobin as 7 g/dl, and the reticulocyte count as 1%. The published normal value for the reticulocyte count is 0.7% to 2.0%, so the reticulocyte count is within the laboratory's normal range. How would you interpret this reticulocyte count?..... a. This reticulocyte count is normal, so the patient's bone marrow is making RBCs adequately b. This reticulocyte count is low. The laboratory's normal values are incorrect c. This reticulocyte count value is normal for a patient with a normal hemoglobin, but for a severely anemic patient, the reticulocyte count should be high. Thus, in view of this patient's severe anemia, this patient's reticulocyte count is actually low and indicative of a condition in which RBCs are not being produced. 12
14 ..... d. This reticulocyte count is too high for a low hemoglobin. Thus, this is indicative of a hemolytic etiology. Answers 1. Classification by red blood cell size (microcytic, normocytic, and macrocytic anemias) and classification by mechanism (decreased production, increased destruction, and blood loss). 2. Low reticulocyte count. 3. History: dark urine. Physical exam: jaundice, scleral icterus, splenomegaly. Lab: elevated LDH, AST, indirect bilirubin; decreased serum haptoglobin; positive direct antibody test (DAT, also known as Coombs test), high reticulocyte count. 4. Bone marrow stain for iron has the highest positive predictive value and specificity, but it is too invasive in most instances. Low serum ferritin is diagnostic of iron deficiency, but its wide range of normal values and its fluctuation with acute inflammation may make interpretation difficult. Serum iron coupled with TIBC and % iron saturation are satisfactory, but this test is subject to some laboratory fluctuation as well. Response to a therapeutic trial of iron is also acceptable as proof of iron deficiency. No actual correct answer to this question. 5. True 6. True 7. False 8. False. Cow's milk contains a modest amount of iron, but little of it is bioavailable. 9. c OSCE Style >> Take Hx and do PE for a patient with Anemia.. History 13
15 1) Has there been a sudden onset of pallor, fatigue, or exercise intolerance? Rapid onset of symptoms suggests a more acute anemia, while anemia without symptoms may indicate a more chronic process, allowing the body more time to compensate for the low hemoglobin levels. Note that the presence of symptoms does not necessarily reflect the level of anemia. A child whose Hgb drops from 14 to 10 over one week may be quite symptomatic, while the child in our case presentation ( 1 st page ) was virtually asymptomatic dropping to a Hgb of 6.2 over a period of months. Pallor unrecognized by the patient's day to day caretaker also suggests a gradual process. 2) Any history of blood loss? Obtain a menstrual history. Prolonged, heavy periods are a source for acute blood loss. Over time chronic loss can lead to iron deficiency, especially when superimposed on poor dietary iron intake. 3) Did the child have jaundice in the newborn period or episodes of jaundice in the past? Glucose-6-phosphate dehydrogenase deficiency (G6PD) and hereditary spherocytosis will cause recurrent episodes of jaundice and anemia, especially following illness or stress. 4) Describe the child's diet. When did he start whole milk? How much milk does he drink now? Excessive milk intake with inadequate dietary iron is a common cause of iron deficiency anemia. Does he eat anything unusual (paper, dirt) or chew on ice? Pica suggests iron deficiency and can predispose to lead poisoning. 5) Has anyone in the family ever had anemia or low blood counts, or ever been on iron? This may suggest a hereditable cause of anemia, but is not diagnostic. A positive response may simply reflect dietary patterns in siblings. It is quite common for families to recall at least one relative who was anemic at some time, especially during pregnancy. Ask if they are still receiving treatment or if the condition resolved. 14
16 Remember :: a negative family history does not exclude an inherited anemia. 6) Has anyone in the family ever had spleenectomy, cholecystectomy or had gallstones at an early age? Surprisingly, not all patients know the reasons for past procedures, or may have been too young when they occurred. A positive response suggests a family history of a hemolytic anemia (such as hereditary spherocytosis). A negative family Hx. does not rule out these causes. 7) What is the child's ethnic origin? Hemoglobinopathies (e.g., sickle cell anemia), thalassemias, and G6PD deficiency are more common in certain ethnic groups. 8) Hx of prolonged diarrhea? Chronic diarrhea in early childhood may be associated with considerable unrecognized blood loss and Malabsorption (e.g, celiac disease is a cause of refractory iron deficiency anemia ). Variable Comments Age Iron deficiency rare in the absence of blood loss before 6 mo or in term infants or before doubling of birth weight in preterm infants Neonatal anemia with reticulocytosis suggests hemolysis or blood loss; with reticulocytopenia, suggests bone marrow failure Sickle cell anemia and β-thalassemia appear as fetal hemoglobin disappears (4-8 mo of age) Family history and genetic considerations Nutrition X-linked: G6PD deficiency Autosomal dominant: spherocytosis Autosomal recessive: sickle cell anemia, Fanconi anemia Family member with history of cholecystectomy (for bilirubin stones) or splenectomy at an early age Ethnicity (thalassemia in persons of Mediterranean origin; G6PD deficiency in blacks, Greeks, and people of Middle Eastern origin) Race (β-thalassemia in persons of Mediterranean, African, or Asian descent; α-thalassemia in those of African and Asian descent; SC and SS in African descent) Cow's milk diet: iron deficiency Strict vegetarian: vitamin B12 deficiency Goat's milk diet: folate deficiency Pica: plumbism, iron deficiency 15
17 Drugs Diarrhea Infection Cholestasis, malabsorption: vitamin E deficiency G6PD: oxidants (e.g., nitrofurantoin, antimalarials) Immune-mediated hemolysis (e.g., penicillin) Bone marrow suppression (e.g., chemotherapy) Phenytoin, increasing folate requirements Malabsorption of vitamin B12 or E or iron Inflammatory bowel disease and anemia of inflammation (chronic disease) with or without blood loss Milk protein intolerance-induced blood loss Intestinal resection: vitamin B12 deficiency Giardia lamblia infection: iron malabsorption Intestinal bacterial overgrowth (blind loop): vitamin B12 deficiency Fish tapeworm: vitamin B12 deficiency Epstein-Barr virus, cytomegalovirus infection: bone marrow suppression, hemophagocytic syndromes Mycoplasma infection: hemolysis Parvovirus infection: bone marrow suppression HIV infection Chronic infection Endocarditis Malaria: hemolysis Hepatitis: aplastic anemia ** this table is from Nelson Essential. ** Bolded things are the most imp. Physical Examination Compare the child's color to his siblings or both parents. Is he active and playful or fatigued? Tachycardia and heart murmur are common in children with anemia, but look for signs of heart failure including tachypnea, rales, hepatomegaly or edema. Splenomegaly may indicate immune hemolytic anemia or hereditary spherocytosis. Look for any skeletal abnormalities as can be seen with the congenital bone marrow failure syndromes. System/Structure Observation Significance Skin Hyperpigmentation Fanconi anemia, dyskeratosis congenita Café au lait spots Vitiligo Partial oculocutaneous albinism Jaundice Fanconi anemia Vitamin B12 deficiency Chédiak-Higashi syndrome Hemolysis 16
18 Petechiae, purpura Bone marrow infiltration, autoimmune hemolysis with autoimmune thrombocytopenia, hemolytic uremic syndrome, hemophagocytic syndromes Erythematous rash Parvovirus or Epstein-Barr virus infection Butterfly rash SLE antibodies Bruising Bleeding disorder, nonaccidental trauma, scurvy Head Frontal bossing Thalassemia major, severe iron deficiency, chronic subdural hematoma Microcephaly Fanconi anemia Eyes Microphthalmia Fanconi anemia Retinopathy Hemoglobin SS, SC disease Optic atrophy Osteopetrosis Blocked lacrimal gland Dyskeratosis congenita Kayser-Fleischer ring Wilson disease Blue sclera Iron deficiency Ears Deafness Osteopetrosis Mouth Glossitis Vitamin B12 deficiency, iron deficiency Angular stomatitis Iron deficiency Chest Cleft lip Pigmentation Telangiectasia Leukoplakia Shield chest or widespread nipples Diamond-Blackfan syndrome Peutz-Jeghers syndrome (intestinal blood loss) Osler-Weber-Rendu syndrome (blood loss) Dyskeratosis congenita Diamond-Blackfan syndrome Murmur Endocarditis: prosthetic valve hemolysis; severe anemia Abdomen Hepatomegaly Hemolysis, infiltrative tumor, chronic disease, hemangioma, cholecystitis, extramedullary hematopoiesis Splenomegaly Hemolysis, sickle cell disease, (early) thalassemia, malaria, leukemia/lymphoma, Epstein-Barr virus, portal hypertension Nephromegaly Fanconi anemia Absent kidney Fanconi anemia Extremities Absent thumbs Fanconi anemia Triphalangeal thumb Diamond-Blackfan syndrome Spoon nails Beau line (nails) Iron deficiency Heavy metal intoxication, severe illness 17
19 Mees line (nails) Dystrophic nails Heavy metals, severe illness, sickle cell anemia Dyskeratosis congenita Rectal Hemorrhoids Portal hypertension Heme-positive stool Gastrointestinal bleeding Nerves Irritable, apathy Iron deficiency Peripheral neuropathy Dementia Ataxia, posterior column signs Stroke Deficiency of vitamins B1, B12, and E; lead poisoning Deficiency of vitamins B12 and E Vitamin B12 deficiency Sickle cell anemia, paroxysmal nocturnal hemoglobinuria General Small stature Fanconi anemia, HIV infection, malnutrition ** this table is from Nelson Essential ** important signs are BOLDED تذكر... ت ع الى ي ح ب إ ذ ا ع م ل أ ح د ك م ع م ال أ ن ي ت ق ن ه ( (إ ن للا Resources : past lec., case-based book, Nelson, Current GOOD LUCK :D Collected by Doa'a Samarah Al Zou'bi HOPE batch /
Introduction and Approach to Anemia
 2 nd lecture in Hematology by Dr.Alaa Fadhil Alwan Introduction and Approach to Anemia Anemia is defined clinically as a blood hemoglobin or hematocrit value that is below the appropriate reference range
2 nd lecture in Hematology by Dr.Alaa Fadhil Alwan Introduction and Approach to Anemia Anemia is defined clinically as a blood hemoglobin or hematocrit value that is below the appropriate reference range
Approach to a pale child
 Approach to a pale child Dr. Dafalla Ahmed Babiker Jazan university objectives Definition of anemia Classification and causes Important points in history and physical examination Investigations. Definition
Approach to a pale child Dr. Dafalla Ahmed Babiker Jazan university objectives Definition of anemia Classification and causes Important points in history and physical examination Investigations. Definition
I. Definitions. V. Evaluation A. History B. Physical Exam C. Laboratory evaluation D. Bone marrow examination E. Specialty referrals
 I. Definitions II. III. Red blood cell life cycle Iron metabolism IV. Causes of anemia A. Kinetic approach 1. decreased production 2. increased destruction 3. blood loss B. Morphologic approach 1. normocytic
I. Definitions II. III. Red blood cell life cycle Iron metabolism IV. Causes of anemia A. Kinetic approach 1. decreased production 2. increased destruction 3. blood loss B. Morphologic approach 1. normocytic
(anemia) ก hemoglobin concentration, hematocrit deviation 1 1 ก hemoglobin, hematocrit mean corpuscular volume (MCV) 2
 ก ก. ก ก.. ก (anemia) ก hemoglobin concentration, hematocrit ก ก ก 2 Standard deviation 1 1 ก hemoglobin, hematocrit mean corpuscular volume (MCV) 2 Hemoglobin hematocrit MCV (g/dl) (%) (fl) ( ) 0.5-1.9
ก ก. ก ก.. ก (anemia) ก hemoglobin concentration, hematocrit ก ก ก 2 Standard deviation 1 1 ก hemoglobin, hematocrit mean corpuscular volume (MCV) 2 Hemoglobin hematocrit MCV (g/dl) (%) (fl) ( ) 0.5-1.9
General Characterisctics
 Anemia General Characterisctics Definition: anemia is a decrease in red blood cells. Happens due to underproduction, increased destruction or loss of red cells. Diagnosis of anemia: Hgb < 135 (men) Hgb
Anemia General Characterisctics Definition: anemia is a decrease in red blood cells. Happens due to underproduction, increased destruction or loss of red cells. Diagnosis of anemia: Hgb < 135 (men) Hgb
INTERELATIONSHIP BETWEEN IDA AND VITAMIN D DEFICIENCY IS NOW ESTABLISHED
 INTERELATIONSHIP BETWEEN IDA AND VITAMIN D DEFICIENCY IS NOW ESTABLISHED Rationale for Combining Iron & Vit-D Vit D deficiency and Iron deficiency Anaemia the two most menacing disorders - are inter-related
INTERELATIONSHIP BETWEEN IDA AND VITAMIN D DEFICIENCY IS NOW ESTABLISHED Rationale for Combining Iron & Vit-D Vit D deficiency and Iron deficiency Anaemia the two most menacing disorders - are inter-related
Faculty of Medicine Dr. Tariq Aladily
 Iron deficiency anemia The most common anemia worldwide Only 10% of ingested iron is absorbed Most dietary iron occurs in meat products Absorbed in duodenum Hepcidin By inhibiting ferroportin, hepcidin
Iron deficiency anemia The most common anemia worldwide Only 10% of ingested iron is absorbed Most dietary iron occurs in meat products Absorbed in duodenum Hepcidin By inhibiting ferroportin, hepcidin
Hematopoiesis, The hematopoietic machinery requires a constant supply iron, vitamin B 12, and folic acid.
 Hematopoiesis, 200 billion new blood cells per day The hematopoietic machinery requires a constant supply iron, vitamin B 12, and folic acid. hematopoietic growth factors, proteins that regulate the proliferation
Hematopoiesis, 200 billion new blood cells per day The hematopoietic machinery requires a constant supply iron, vitamin B 12, and folic acid. hematopoietic growth factors, proteins that regulate the proliferation
Microcytic Hypochromic Anemia An Approach to Diagnosis
 Microcytic Hypochromic Anemia An Approach to Diagnosis Decreased hemoglobin synthesis gives rise to microcytic hypochromic anemias. Hypochromic anemias are characterized by normal cellular proliferation
Microcytic Hypochromic Anemia An Approach to Diagnosis Decreased hemoglobin synthesis gives rise to microcytic hypochromic anemias. Hypochromic anemias are characterized by normal cellular proliferation
Approach to the child with anemia. Nittaya Wisanuyothin,MD. Pediatrics Department, Maharat Nakhonratchasima Hospital
 Approach to the child with anemia Nittaya Wisanuyothin,MD. Pediatrics Department, Maharat Nakhonratchasima Hospital Definition of anemia Hb< 2 SD or P2.5 below the mean for a healthy of the same gender
Approach to the child with anemia Nittaya Wisanuyothin,MD. Pediatrics Department, Maharat Nakhonratchasima Hospital Definition of anemia Hb< 2 SD or P2.5 below the mean for a healthy of the same gender
The McMaster at night Pediatric Curriculum
 The McMaster at night Pediatric Curriculum Wang, M. (2016). Iron Deficiency and Other Types of Anemia in Infants and Children. American Family Physician. 93 (4): 270-278. Objectives Recognize common signs
The McMaster at night Pediatric Curriculum Wang, M. (2016). Iron Deficiency and Other Types of Anemia in Infants and Children. American Family Physician. 93 (4): 270-278. Objectives Recognize common signs
NUTRITIONAL CARE IN ANEMIA
 االله الرحمن الرحيم بسم NUTRITIONAL CARE IN ANEMIA Nutrition Departement Faculty of Medicine University of North Sumatera Definition Deficit of circulating RBC associated with diminished oxygen-carrying
االله الرحمن الرحيم بسم NUTRITIONAL CARE IN ANEMIA Nutrition Departement Faculty of Medicine University of North Sumatera Definition Deficit of circulating RBC associated with diminished oxygen-carrying
HAEMATOLOGICAL EVALUATION OF ANEMIA. Sitalakshmi S Professor and Head Department of Clinical Pathology St John s medical College, Bangalore
 HAEMATOLOGICAL EVALUATION OF ANEMIA Sitalakshmi S Professor and Head Department of Clinical Pathology St John s medical College, Bangalore Learning Objectives Laboratory tests for the evaluation of anemia
HAEMATOLOGICAL EVALUATION OF ANEMIA Sitalakshmi S Professor and Head Department of Clinical Pathology St John s medical College, Bangalore Learning Objectives Laboratory tests for the evaluation of anemia
L4-Iron Deficiency Anemia (IDA) & Biochemical Investigations
 L4-Iron Deficiency Anemia (IDA) & Biochemical Investigations 1 st Year-College of Medicine Hematology Module-Biochemistry Semester II Dr. Basil OM Saleh Objectives Identify stages in development of IDA
L4-Iron Deficiency Anemia (IDA) & Biochemical Investigations 1 st Year-College of Medicine Hematology Module-Biochemistry Semester II Dr. Basil OM Saleh Objectives Identify stages in development of IDA
Diagnostic Approach to Patients with Anemia
 J KMA Special Issue Diagnostic Approach to Patients with Anemia Seonyang Park, MD Department of Internal Medicine, Seoul National University College of Medicine E mail : seonpark@snu.ac.kr J Korean Med
J KMA Special Issue Diagnostic Approach to Patients with Anemia Seonyang Park, MD Department of Internal Medicine, Seoul National University College of Medicine E mail : seonpark@snu.ac.kr J Korean Med
THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY
 THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY INTRODUCTION TO ANEMIA Third year medical students First semester 2018/2019 Dr. RBC DISORDERS Lecturer: Dr. Tariq Al-Adaily Email: TNALADILY@ju.edu.jo
THE UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PATHOLOGY INTRODUCTION TO ANEMIA Third year medical students First semester 2018/2019 Dr. RBC DISORDERS Lecturer: Dr. Tariq Al-Adaily Email: TNALADILY@ju.edu.jo
Topic owner: Mollie Grow MD MPH, updated June 2018
 Iron deficiency Anemia UW Pediatrics Outpatient Clinical Guidelines Sources: AAP Clinical Report Diagnosis and Prevention of Iron Deficiency and Iron- Deficiency Anemia in Infants and Young Children (0
Iron deficiency Anemia UW Pediatrics Outpatient Clinical Guidelines Sources: AAP Clinical Report Diagnosis and Prevention of Iron Deficiency and Iron- Deficiency Anemia in Infants and Young Children (0
Guideline developed by Shelley Crary, MD, MS,* in collaboration with the ANGELS team. Last reviewed by Shelley Crary, MD, MS, January 19, 2017.
 Microcytic Anemia Guideline developed by Shelley Crary, MD, MS,* in collaboration with the ANGELS team. Last reviewed by Shelley Crary, MD, MS, January 19, 2017. Dr. Crary is a member of the hemophilia
Microcytic Anemia Guideline developed by Shelley Crary, MD, MS,* in collaboration with the ANGELS team. Last reviewed by Shelley Crary, MD, MS, January 19, 2017. Dr. Crary is a member of the hemophilia
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia. Abdallah Abbadi
 Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
The Evaluation and Classification of Anemia
 Case studies and research for better care To refer a patient, call. The Evaluation and Classification of Anemia A diagnostic approach BY AMANDA BRANDOW, DO, MS Anemia is defined as hemoglobin concentration
Case studies and research for better care To refer a patient, call. The Evaluation and Classification of Anemia A diagnostic approach BY AMANDA BRANDOW, DO, MS Anemia is defined as hemoglobin concentration
Types of Anaemias and their Management. S. Moncrieffe, Pharm.D., MPH, Dip.Ed., RPh. PSJ CE Mandeville Hotel April 27, 2014
 Types of Anaemias and their Management S. Moncrieffe, Pharm.D., MPH, Dip.Ed., RPh. PSJ CE Mandeville Hotel April 27, 2014 Objectives At the end of the presentations participants should be able to: 1. Define
Types of Anaemias and their Management S. Moncrieffe, Pharm.D., MPH, Dip.Ed., RPh. PSJ CE Mandeville Hotel April 27, 2014 Objectives At the end of the presentations participants should be able to: 1. Define
Anemia (3).ms Hemolytic Anemia. Abdallah Abbadi Feras Fararjeh
 Anemia (3).ms4.26.2.18 Hemolytic Anemia Abdallah Abbadi Feras Fararjeh Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k,
Anemia (3).ms4.26.2.18 Hemolytic Anemia Abdallah Abbadi Feras Fararjeh Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k,
Red cell disorder. Dr. Ahmed Hasan
 Red cell disorder Dr. Ahmed Hasan Things to be learned in this lecture Definition and clinical feature of anemia. Classification of anemia. Know some details of microcytic anemia Question of the lecture:
Red cell disorder Dr. Ahmed Hasan Things to be learned in this lecture Definition and clinical feature of anemia. Classification of anemia. Know some details of microcytic anemia Question of the lecture:
BONE MARROW PERIPHERAL BLOOD Erythrocyte
 None Disclaimer Objectives Define anemia Classify anemia according to pathogenesis & clinical significance Understand Red cell indices Relate the red cell indices with type of anemia Interpret CBC to approach
None Disclaimer Objectives Define anemia Classify anemia according to pathogenesis & clinical significance Understand Red cell indices Relate the red cell indices with type of anemia Interpret CBC to approach
Definition Aetiology
 Definition Anaemia is a fall in haemoglobin below the reference ranges for age and sex (adult female
Definition Anaemia is a fall in haemoglobin below the reference ranges for age and sex (adult female
Evaluation of Anemia. Md. Shafiqul Bari Associate professor (Medicine) SOMC
 Evaluation of Anemia Md. Shafiqul Bari Associate professor (Medicine) SOMC Definition Anemia is operationally defined as a reduction in one or more of the major RBC measurements Hemoglobin concentration
Evaluation of Anemia Md. Shafiqul Bari Associate professor (Medicine) SOMC Definition Anemia is operationally defined as a reduction in one or more of the major RBC measurements Hemoglobin concentration
Year 2003 Paper two: Questions supplied by Tricia
 QUESTION 65 A 36-year-old man presents in a post-ictal state after an observed generalised seizure. Full blood investigation shows: haemoglobin 0 g/l [128-175] mean corpuscular volume (MCV) 106 fl [80-7]
QUESTION 65 A 36-year-old man presents in a post-ictal state after an observed generalised seizure. Full blood investigation shows: haemoglobin 0 g/l [128-175] mean corpuscular volume (MCV) 106 fl [80-7]
C. treatment with Desferal (deferoxamine mesylate USP, iron-chelating agent)
 HEMOLYTIC ANEMIAS Single choice tests 1. Select the clinical manifestation that is not characteristic for the hemolytic crisis: A. decrease of the red blood cell count B. reticulocytosis C. jaundice D.
HEMOLYTIC ANEMIAS Single choice tests 1. Select the clinical manifestation that is not characteristic for the hemolytic crisis: A. decrease of the red blood cell count B. reticulocytosis C. jaundice D.
* imagine if the Hb is free ( e.g. hemolysis ) in the plasma what happens?
 In this lecture we will talk about Some characteristics of RBC. Erythrpoiesis : * During fetal & adult life. * its regulation. RBCs : - Appear under the microscope as circular,unnucleated and biconcave
In this lecture we will talk about Some characteristics of RBC. Erythrpoiesis : * During fetal & adult life. * its regulation. RBCs : - Appear under the microscope as circular,unnucleated and biconcave
LEC 6 Megaloblastic Aneamia
 LEC 6 Megaloblastic Aneamia Megaloblastosis is a generalized disorder involving most rapidly growing cells, such as gastrointestinal and uterine cervical mucosal cells. The etiology of megaloblastosis
LEC 6 Megaloblastic Aneamia Megaloblastosis is a generalized disorder involving most rapidly growing cells, such as gastrointestinal and uterine cervical mucosal cells. The etiology of megaloblastosis
Chapter 28. Media Directory. Hematopoiesis. Regulation of Hematopoiesis. Erythropoietin. Drugs for Hematopoietic Disorders
 Chapter 28 Drugs for Hematopoietic Disorders Slide 35 Media Directory Epoetin Alfa Animation Upper Saddle River, New Jersey 07458 All rights reserved. Hematopoiesis Figure 28.1 Hematopoiesis Process of
Chapter 28 Drugs for Hematopoietic Disorders Slide 35 Media Directory Epoetin Alfa Animation Upper Saddle River, New Jersey 07458 All rights reserved. Hematopoiesis Figure 28.1 Hematopoiesis Process of
Iron deficiency anemia:
 بسم هللا الرمحن الرحمي Before we start: Dr. Malik suggested for the third immunity lecture to be a continuation for the hematology pharmacology. And he will discuss the drugs for treating leukemia and
بسم هللا الرمحن الرحمي Before we start: Dr. Malik suggested for the third immunity lecture to be a continuation for the hematology pharmacology. And he will discuss the drugs for treating leukemia and
How Do I Spot Anemia in
 Focus on CME at Queen s University McMaster Queen s University How Do I Spot Anemia in By Isaac Odame, MB, ChB, MRCP, FRCPath, FRCPCH In this article: 1. What is anemia? 2. When should I refer? 3. What
Focus on CME at Queen s University McMaster Queen s University How Do I Spot Anemia in By Isaac Odame, MB, ChB, MRCP, FRCPath, FRCPCH In this article: 1. What is anemia? 2. When should I refer? 3. What
Dr Anzo William Adiga
 Anemia Dr Anzo William Adiga +256777363201 anzoism2008@gmail.com Definition of Anemia Deficiency in the oxygen-carrying capacity of the blood due to a diminished erythrocyte mass. May be due to: Erythrocyte
Anemia Dr Anzo William Adiga +256777363201 anzoism2008@gmail.com Definition of Anemia Deficiency in the oxygen-carrying capacity of the blood due to a diminished erythrocyte mass. May be due to: Erythrocyte
3 Ruba hussein Dr. ahmad Dr. ahmad
 3 Ruba hussein Dr. ahmad Dr. ahmad The arrangement of this sheet differs from that of the record. Anemia of peripheral removal in which we are losing hemoglobin and RBCs mass and the two major Causes are:
3 Ruba hussein Dr. ahmad Dr. ahmad The arrangement of this sheet differs from that of the record. Anemia of peripheral removal in which we are losing hemoglobin and RBCs mass and the two major Causes are:
Anemia. A case-based approach. David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017
 Anemia A case-based approach David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017 Recognizing trends Learning Objectives MCV, RDW, Ferritin, LDH, Reticulocytes Managing complex patients 1.
Anemia A case-based approach David B. Sykes, MD, PhD Hematology, MGH Cancer Center June 8, 2017 Recognizing trends Learning Objectives MCV, RDW, Ferritin, LDH, Reticulocytes Managing complex patients 1.
Anemia 1: Fourth year Medical Students/ October/21/ 2015/ Abdallah Abbadi.MD.FRCP Professor
 Anemia 1: Fourth year Medical Students/ October/21/ 2015/ Abdallah Abbadi.MD.FRCP Professor Email: abdalla.awidi@gmail.com Main Hematological diseases A- Benign Hematology 1- Anemias 2- Bleeding disorders
Anemia 1: Fourth year Medical Students/ October/21/ 2015/ Abdallah Abbadi.MD.FRCP Professor Email: abdalla.awidi@gmail.com Main Hematological diseases A- Benign Hematology 1- Anemias 2- Bleeding disorders
DOWNLOAD PDF MACROCYTOSIS AND MACROCYTIC ANAEMIA
 Chapter 1 : Macrocytic Anemia- Causes, Symptoms Treatment Macrocytosis is a term used to describe red blood cells that are larger than normal. Anemia is when you have low numbers of properly functioning
Chapter 1 : Macrocytic Anemia- Causes, Symptoms Treatment Macrocytosis is a term used to describe red blood cells that are larger than normal. Anemia is when you have low numbers of properly functioning
Susan Stegman, MD Medical Director AXA Equitable Life May 3, 2016
 Susan Stegman, MD Medical Director AXA Equitable Life May 3, 2016 Underwriting impact Anemia overview Classification of anemia Specific anemia topics Iron deficiency anemia Thalassemia Megaloblastic anemia
Susan Stegman, MD Medical Director AXA Equitable Life May 3, 2016 Underwriting impact Anemia overview Classification of anemia Specific anemia topics Iron deficiency anemia Thalassemia Megaloblastic anemia
Peripheral Blood Smear Examination. Momtazmanesh MD. Ped. Hematologist & Oncologist Loghman General Hospital
 1395 Peripheral Blood Smear Examination Momtazmanesh MD. Ped. Hematologist & Oncologist Loghman General Hospital Peripheral Blood Smear A peripheral blood smear is a snapshot of the cells that are present
1395 Peripheral Blood Smear Examination Momtazmanesh MD. Ped. Hematologist & Oncologist Loghman General Hospital Peripheral Blood Smear A peripheral blood smear is a snapshot of the cells that are present
Management. (By the World Health Organization according to the magnitude of the enzyme deficiency and the severity of hemolysis)
 Glucose-6-Phosphate Dehydrogenase (G6PD) Deficiency Management Definition: Glucose-6-phosphate dehydrogenase (G6PD) deficiency is an inherited disorder caused by a genetic defect in the red blood cell
Glucose-6-Phosphate Dehydrogenase (G6PD) Deficiency Management Definition: Glucose-6-phosphate dehydrogenase (G6PD) deficiency is an inherited disorder caused by a genetic defect in the red blood cell
Screening for Iron Deficiency Ann Chen Wu, Leann Lesperance and Henry Bernstein. DOI: /pir
 Screening for Iron Deficiency Ann Chen Wu, Leann Lesperance and Henry Bernstein Pediatrics in Review 2002;23;171 DOI: 10.1542/pir.23-5-171 The online version of this article, along with updated information
Screening for Iron Deficiency Ann Chen Wu, Leann Lesperance and Henry Bernstein Pediatrics in Review 2002;23;171 DOI: 10.1542/pir.23-5-171 The online version of this article, along with updated information
NUTRITIONAL ANEMIAS K Y L I E P E T E R S O N & E M I L Y S T E W A R T S A O R I S A K I T A & M A R J O R I E M I L L E R
 NUTRITIONAL ANEMIAS K Y L I E P E T E R S O N & E M I L Y S T E W A R T S A O R I S A K I T A & M A R J O R I E M I L L E R ANEMIA Anemia: a deficiency in the size/number of RBC or the amount of hemoglobin
NUTRITIONAL ANEMIAS K Y L I E P E T E R S O N & E M I L Y S T E W A R T S A O R I S A K I T A & M A R J O R I E M I L L E R ANEMIA Anemia: a deficiency in the size/number of RBC or the amount of hemoglobin
Classification of Anaemia
 Classification of Anaemia Dr Roger Pool Department of Haematology NHLS & University of Pretoria MEASUREMENT OF HAEMATOCRIT The haematocrit ratio (Hct) is the proportion of blood made up of cells - mainly
Classification of Anaemia Dr Roger Pool Department of Haematology NHLS & University of Pretoria MEASUREMENT OF HAEMATOCRIT The haematocrit ratio (Hct) is the proportion of blood made up of cells - mainly
Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust
 Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust Regional Paediatric Specialty Trainees teaching 4 th July 2017 Scope
Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust Regional Paediatric Specialty Trainees teaching 4 th July 2017 Scope
Dr. Hasan Fahmawi, MRCP (London), FRCP(Edin) Consultant Physician ANAEMIA
 Dr. Hasan Fahmawi, MRCP (London), FRCP(Edin) Consultant Physician ANAEMIA Definition Anaemia refers to a state in which haemoglobin in the blood is below the reference range appropriate for age and
Dr. Hasan Fahmawi, MRCP (London), FRCP(Edin) Consultant Physician ANAEMIA Definition Anaemia refers to a state in which haemoglobin in the blood is below the reference range appropriate for age and
Rama Nada. -Ensherah Mokheemer. 1 P a g e
 - 3 - Rama Nada -Ensherah Mokheemer - 1 P a g e Don t forget to refer to page index wherever you see * Quick revision: In the previous lecture we said that: - your body contains 4-5g of iron (4g in females
- 3 - Rama Nada -Ensherah Mokheemer - 1 P a g e Don t forget to refer to page index wherever you see * Quick revision: In the previous lecture we said that: - your body contains 4-5g of iron (4g in females
The Child with a Hematologic Alteration
 47 The Child with a Hematologic Alteration HELPFUL HINT Review the anatomy and physiology of the hematologic system in an anatomy and physiology textbook. MATCHING KEY TERMS Match the term with the correct
47 The Child with a Hematologic Alteration HELPFUL HINT Review the anatomy and physiology of the hematologic system in an anatomy and physiology textbook. MATCHING KEY TERMS Match the term with the correct
Examination Tests from Pathological Physiology. Pavel Maruna et al. Reviewed by: Prof. MUDr. Emanuel Nečas, DrSc. Prof. MUDr. Jaroslav Veselý, CSc.
 Examination Tests from Pathological Physiology Pavel Maruna et al. Reviewed by: Prof. MUDr. Emanuel Nečas, DrSc. Prof. MUDr. Jaroslav Veselý, CSc. Authors: Prof. MUDr. Pavel Maruna, CSc. Doc. MUDr. Martin
Examination Tests from Pathological Physiology Pavel Maruna et al. Reviewed by: Prof. MUDr. Emanuel Nečas, DrSc. Prof. MUDr. Jaroslav Veselý, CSc. Authors: Prof. MUDr. Pavel Maruna, CSc. Doc. MUDr. Martin
PATHOLOGY & PATHOPHYSIOLOGY
 PATHOLOGY & PATHOPHYSIOLOGY DISORDERS OF BLOOD DISORDERS OF BLOOD Disorders of Blood Infections Tumours Nutritional disorders Coagulation disorders Congenital disorders Septicaemia Leukemia Iron deficiency
PATHOLOGY & PATHOPHYSIOLOGY DISORDERS OF BLOOD DISORDERS OF BLOOD Disorders of Blood Infections Tumours Nutritional disorders Coagulation disorders Congenital disorders Septicaemia Leukemia Iron deficiency
PATHOLOGY OF THE HEMATOLYMPHOID SYSTEM 1 AND 2 -INTRODUCTION TO ANEMIA - ANEMIA OF DECREASED PRODUCTION.
 PATHOLOGY OF THE HEMATOLYMPHOID SYSTEM 1 AND 2 -INTRODUCTION TO ANEMIA - ANEMIA OF DECREASED PRODUCTION. 1 ANEMIA Anemia is defined as decrease in the RBC mass, it usually is reflected by decrease in hemoglobin
PATHOLOGY OF THE HEMATOLYMPHOID SYSTEM 1 AND 2 -INTRODUCTION TO ANEMIA - ANEMIA OF DECREASED PRODUCTION. 1 ANEMIA Anemia is defined as decrease in the RBC mass, it usually is reflected by decrease in hemoglobin
Around million aged erythrocytes/hour are broken down.
 Anemia Degradation ofheme Around 100 200 million aged erythrocytes/hour are broken down. The degradation process starts in reticuloendothelial cells in the spleen, liver, and bone marrow. [1] The tetrapyrrole
Anemia Degradation ofheme Around 100 200 million aged erythrocytes/hour are broken down. The degradation process starts in reticuloendothelial cells in the spleen, liver, and bone marrow. [1] The tetrapyrrole
THE CLASSIFICATION OF ANEMIA*
 THE CLASSIFICATION OF ANEMIA* RUSSELL L. HADEN, M.D. SUMMARY A laboratory and clinical classification of anemia has been outlined. The results of the blood study have been correlated with the clinical
THE CLASSIFICATION OF ANEMIA* RUSSELL L. HADEN, M.D. SUMMARY A laboratory and clinical classification of anemia has been outlined. The results of the blood study have been correlated with the clinical
namib la UnIVERSITY OF SCIEnCE AnD TECHnOLOGY FACULTY OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES
 namib la UnIVERSITY OF SCIEnCE AnD TECHnOLOGY FACULTY OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES QUALIFICATION: BACHELOR OF BIOMEDICAL SCIENCES QUALIFICATION CODE: SOBBMS LEVEL: 6 COURSE
namib la UnIVERSITY OF SCIEnCE AnD TECHnOLOGY FACULTY OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES QUALIFICATION: BACHELOR OF BIOMEDICAL SCIENCES QUALIFICATION CODE: SOBBMS LEVEL: 6 COURSE
Anemia 1: Fourth year Medical Students/ Feb/22/ Abdallah Awidi Abbadi.MD.FRCP.FRCPath Professor
 Anemia 1: Fourth year Medical Students/ Feb/22/ 2018 Abdallah Awidi Abbadi.MD.FRCP.FRCPath Professor Email: abdalla.awidi@gmail.com Kidney EPO O2 Sensor Blood vessel Definition: Anemia is operationally
Anemia 1: Fourth year Medical Students/ Feb/22/ 2018 Abdallah Awidi Abbadi.MD.FRCP.FRCPath Professor Email: abdalla.awidi@gmail.com Kidney EPO O2 Sensor Blood vessel Definition: Anemia is operationally
Hypochromic Anaemias
 Hypochromic Anaemias Dr Mere Kende MBBS, MMED (Path), MAACB, MACTM, MACRRM LECTURER-SMHS Anaemia LOW HEMOGLOBIN Anaemia Definition: Hb
Hypochromic Anaemias Dr Mere Kende MBBS, MMED (Path), MAACB, MACTM, MACRRM LECTURER-SMHS Anaemia LOW HEMOGLOBIN Anaemia Definition: Hb
2. Non- hemolytic anemias 3. Normocytic Normochromic Normocytic Normochromic Blood loss. (MCV<80 fl) (MCV fl) (MCV>100 fl)
 Definition of Anaemia of Anaemias Approach for diagnosis of Red cell disorders any condition resulting from a significant decrease in the total body erythrocyte mass due to decrease of Hb and or RBCs Hemoglobin
Definition of Anaemia of Anaemias Approach for diagnosis of Red cell disorders any condition resulting from a significant decrease in the total body erythrocyte mass due to decrease of Hb and or RBCs Hemoglobin
ANEMIAS OBJECTIVES. What is Anemia. A Narrow Exploration Mainly Involving Anemia Studies
 A Narrow Exploration Mainly Involving Anemia Studies ANEMIAS OBJECTIVES Definition of Anemia What Causes Anemia Signs and Symptoms Types of Anemia Case Studies What is Anemia Derived from the ancient Greek
A Narrow Exploration Mainly Involving Anemia Studies ANEMIAS OBJECTIVES Definition of Anemia What Causes Anemia Signs and Symptoms Types of Anemia Case Studies What is Anemia Derived from the ancient Greek
Nutritional anaemia. Dr J Potgieter Dept of Haematology NHLS - TAD
 Nutritional anaemia Dr J Potgieter Dept of Haematology NHLS - TAD Classification of anaemia Microcytic, hypochromic MCV < 80fl MCH > 27pg Iron deficiency Anaemia of chronic disease Thalassaemia Lead poisoning
Nutritional anaemia Dr J Potgieter Dept of Haematology NHLS - TAD Classification of anaemia Microcytic, hypochromic MCV < 80fl MCH > 27pg Iron deficiency Anaemia of chronic disease Thalassaemia Lead poisoning
Drugs Used in Anemia
 Drugs Used in Anemia Drugs of Anemia Anemia is defined as a below-normal plasma hemoglobin concentration resulting from: a decreased number of circulating red blood cells or an abnormally low total hemoglobin
Drugs Used in Anemia Drugs of Anemia Anemia is defined as a below-normal plasma hemoglobin concentration resulting from: a decreased number of circulating red blood cells or an abnormally low total hemoglobin
Instructor s Manual Chapter 26 Hematological Alterations. 1. A man and woman both test positive for the sickle cell trait. The couple asks the
 1 Instructor s Manual Chapter 26 Hematological Alterations Answers to Study Questions 1. A man and woman both test positive for the sickle cell trait. The couple asks the nurse how many of their children
1 Instructor s Manual Chapter 26 Hematological Alterations Answers to Study Questions 1. A man and woman both test positive for the sickle cell trait. The couple asks the nurse how many of their children
Assessing Iron Deficiency in Adults. Chris Theberge. Iron (Fe) deficiency remains as one of the major global public health problems for
 Assessing Iron Deficiency in Adults Chris Theberge Iron (Fe) deficiency remains as one of the major global public health problems for two reasons. It affects about one fourth of the world s population
Assessing Iron Deficiency in Adults Chris Theberge Iron (Fe) deficiency remains as one of the major global public health problems for two reasons. It affects about one fourth of the world s population
APPROACHING TO PANCYTOPENIA
 APPROACHING TO PANCYTOPENIA P A T C H A R E E K O M V I L A I S A K, M. D. A S S I S T A N T P R O F E S S O R D I V I S I O N O F P E D I A T R I C H E M A T O L O G Y O N C O L O G Y, D E P A R T M E
APPROACHING TO PANCYTOPENIA P A T C H A R E E K O M V I L A I S A K, M. D. A S S I S T A N T P R O F E S S O R D I V I S I O N O F P E D I A T R I C H E M A T O L O G Y O N C O L O G Y, D E P A R T M E
Anemia In the Insurance Applicant What do the numbers mean?
 Anemia In the Insurance Applicant What do the numbers mean? Lisa Duckett, M.D. Vice President and Medical Director September 12, 2017 Goals of the presentation Develop a consistent way to analyze Complete
Anemia In the Insurance Applicant What do the numbers mean? Lisa Duckett, M.D. Vice President and Medical Director September 12, 2017 Goals of the presentation Develop a consistent way to analyze Complete
Aplastic anamia & Sideroblastic anemia
 Hematology Lecture 7 كلية التقنيات الصحية والطبية قسم التحليالت المرضية Aplastic anamia & Sideroblastic anemia اإلعداد: ظفر جبار دهاق فؤاد APLASTIC ANEMIA What is Aplastic anemia? Aplastic anemia is a
Hematology Lecture 7 كلية التقنيات الصحية والطبية قسم التحليالت المرضية Aplastic anamia & Sideroblastic anemia اإلعداد: ظفر جبار دهاق فؤاد APLASTIC ANEMIA What is Aplastic anemia? Aplastic anemia is a
SICKLE CELL DISEASE. Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH. Assistant Professor FACULTY OF MEDICINE -JAZAN
 SICKLE CELL DISEASE Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN Objective: The student should be able: To identify the presentation, diagnosis,
SICKLE CELL DISEASE Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN Objective: The student should be able: To identify the presentation, diagnosis,
Lisa B. Weissmann, MD
 Lisa B. Weissmann, MD Anemia- Most common hematologic disorder Evaluation should be orderly Questions to ask Timing - new, old, rapidity of onset Isolated - only anemia, or other cell lines Size of cells
Lisa B. Weissmann, MD Anemia- Most common hematologic disorder Evaluation should be orderly Questions to ask Timing - new, old, rapidity of onset Isolated - only anemia, or other cell lines Size of cells
It should be noted that in the initial stage, nearly all anemias are normocytic. The major primary causes of normocytic anemia are given in Table 1.
 Normocytic Anemia JOHN R. BRILL, M.D., and DENNIS J. BAUMGARDNER, M.D., University of Wisconsin Medical School, Milwaukee Clinical Campus, Milwaukee, Wisconsin Am Fam Physician. 2000 Nov 15;62(10):2255
Normocytic Anemia JOHN R. BRILL, M.D., and DENNIS J. BAUMGARDNER, M.D., University of Wisconsin Medical School, Milwaukee Clinical Campus, Milwaukee, Wisconsin Am Fam Physician. 2000 Nov 15;62(10):2255
Physiological Role: B-vitamins are coenzymes of many enzymes systems of body metabolism. Thiamine {B 1 }
 Food Constituents [continued] Micronutrients B-Vitamins The B group of vitamin {water soluble} includes: Thiamine: vitamin B 1, ant beriberi vitamin. Riboflavin: vitamin B 2. Niacin: nicotinic acid, PP
Food Constituents [continued] Micronutrients B-Vitamins The B group of vitamin {water soluble} includes: Thiamine: vitamin B 1, ant beriberi vitamin. Riboflavin: vitamin B 2. Niacin: nicotinic acid, PP
Factors affecting oxygen dissociation curve
 P a g e 1 Factors affecting oxygen dissociation curve As you know, hemoglobin contains 4 heme molecules that bind 4 oxygen molecules (8 atoms). These 4 heme molecules, however, do not bind oxygen all at
P a g e 1 Factors affecting oxygen dissociation curve As you know, hemoglobin contains 4 heme molecules that bind 4 oxygen molecules (8 atoms). These 4 heme molecules, however, do not bind oxygen all at
Intro to Vitamins, Minerals & Water
 Intro to Vitamins, Minerals & Water 1. What is the main function of vitamins and minerals? To regulate body functions 2. What foods are a lot of the vitamins and minerals we need found in? Fruits and Vegetables
Intro to Vitamins, Minerals & Water 1. What is the main function of vitamins and minerals? To regulate body functions 2. What foods are a lot of the vitamins and minerals we need found in? Fruits and Vegetables
Objectives. But first: What s in blood? Introduction. Overview: Erythrocytes. Erythrocytes, cont. 4/21/2016
 Objectives Nutritional Deficiencies That May Cause Anemia Lee Ellen Brunson-Sicilia, MHS, MLS(ASCP) CM 1. Discuss the role that various nutrients play in red blood cell formation. 2. List sources of nutrients
Objectives Nutritional Deficiencies That May Cause Anemia Lee Ellen Brunson-Sicilia, MHS, MLS(ASCP) CM 1. Discuss the role that various nutrients play in red blood cell formation. 2. List sources of nutrients
Case # 1. RBC Loss. CASE #1 (Continued) Blood Loss Is the Most Common Cause of Anemia. AGA Definition of Occult Blood Loss
 Case # 1 A 42-yo woman with heavy menses presents with rectal bleeding. Except for pallor, exam is normal. HCT = 17.1% (normal, 36-48) HGB = 5.3 g/dl (normal, 12.0-16.0) MCV = 76 fl (normal, 82-98) RBC
Case # 1 A 42-yo woman with heavy menses presents with rectal bleeding. Except for pallor, exam is normal. HCT = 17.1% (normal, 36-48) HGB = 5.3 g/dl (normal, 12.0-16.0) MCV = 76 fl (normal, 82-98) RBC
Moath Darwish. Waseem Alhaj. Tareq Adely
 4 Moath Darwish Waseem Alhaj Tareq Adely Please refer to the slides for pictures. Iron deficiency anemia 1. Iron absorption and regulation a. only 10% of ingested iron are absorbed b. absorption of iron
4 Moath Darwish Waseem Alhaj Tareq Adely Please refer to the slides for pictures. Iron deficiency anemia 1. Iron absorption and regulation a. only 10% of ingested iron are absorbed b. absorption of iron
Deconstructing the CBC
 Deconstructing the CBC Dr. Ann M. Wexler Solano Hematology Oncology September 10, 2017 What Are the Major Components of Blood? Red Blood Cells (also called erythrocytes) White Blood Cells (also called
Deconstructing the CBC Dr. Ann M. Wexler Solano Hematology Oncology September 10, 2017 What Are the Major Components of Blood? Red Blood Cells (also called erythrocytes) White Blood Cells (also called
Kehkashan Zehra Hossain. Registered Clinical Dietitian Head of the Department SIUT
 Kehkashan Zehra Hossain Registered Clinical Dietitian Head of the Department SIUT Definition Anemia is the deficiency in the size or number of red blood cells or the amount of hemoglobin they contain Krause
Kehkashan Zehra Hossain Registered Clinical Dietitian Head of the Department SIUT Definition Anemia is the deficiency in the size or number of red blood cells or the amount of hemoglobin they contain Krause
Heme Questions and Derivatives for the USMLE Step One Exam. Winter Storm Skylar Edition
 Heme Questions and Derivatives for the USMLE Step One Exam Winter Storm Skylar Edition Howard J. Sachs, MD Howard@12DaysinMarch.com www.12daysinmarch.com Patient presents with RUQ pain. HIDA scan fails
Heme Questions and Derivatives for the USMLE Step One Exam Winter Storm Skylar Edition Howard J. Sachs, MD Howard@12DaysinMarch.com www.12daysinmarch.com Patient presents with RUQ pain. HIDA scan fails
Interpreting the CBC. Robert Miller PA Assistant Professor of Clinical Pediatrics and Family Medicine USC Keck School of Medicine Retired
 Interpreting the CBC Robert Miller PA Assistant Professor of Clinical Pediatrics and Family Medicine USC Keck School of Medicine Retired The CBC 3 Cell Lines RBCs WBCs Platelets Assess general health Make
Interpreting the CBC Robert Miller PA Assistant Professor of Clinical Pediatrics and Family Medicine USC Keck School of Medicine Retired The CBC 3 Cell Lines RBCs WBCs Platelets Assess general health Make
Pediatrics. Pyruvate Kinase Deficiency (PKD) Symptoms and Treatment. Definition. Epidemiology of Pyruvate Kinase Deficiency.
 Pediatrics Pyruvate Kinase Deficiency (PKD) Symptoms and Treatment See online here Pyruvate kinase deficiency is an inherited metabolic disorder characterized by a deficiency in the enzyme "pyruvate kinase"
Pediatrics Pyruvate Kinase Deficiency (PKD) Symptoms and Treatment See online here Pyruvate kinase deficiency is an inherited metabolic disorder characterized by a deficiency in the enzyme "pyruvate kinase"
Thalassemia Maria Luz Uy del Rosario, M.D.
 Thalassemia Maria Luz Uy del Rosario, M.D. Philippine Society of Hematology and Blood Transfusion Philippine Society of Pediatric Oncology What is Thalassemia Hereditary Hemoglobin disorder Hemolytic anemia
Thalassemia Maria Luz Uy del Rosario, M.D. Philippine Society of Hematology and Blood Transfusion Philippine Society of Pediatric Oncology What is Thalassemia Hereditary Hemoglobin disorder Hemolytic anemia
Symptoms and Signs in Hematology (2)/ 2013
 Symptoms and Signs in Hematology (2)/ 2013 Abdallah Abbadi.MD.FRCP Professor of Medicine,Hematology & Oncology University of Jordan & JUH Email: abdalla.awidi@gmail.com Case one: A 24 yr old female complains
Symptoms and Signs in Hematology (2)/ 2013 Abdallah Abbadi.MD.FRCP Professor of Medicine,Hematology & Oncology University of Jordan & JUH Email: abdalla.awidi@gmail.com Case one: A 24 yr old female complains
ASPEN MOUNTAIN MEDICAL CENTER. Lab Health Fair
 ASPEN MOUNTAIN MEDICAL CENTER Lab Health Fair GENERAL HEALTH PANEL: CMP CMP The Comprehensive Metabolic Panel is used as a broad screening tool to evaluate organ function and check for conditions such
ASPEN MOUNTAIN MEDICAL CENTER Lab Health Fair GENERAL HEALTH PANEL: CMP CMP The Comprehensive Metabolic Panel is used as a broad screening tool to evaluate organ function and check for conditions such
Case Report A Puzzle of Hemolytic Anemia, Iron and Vitamin B12 Deficiencies in a 52-Year-Old Male
 Hindawi Publishing Corporation Case Reports in Hematology Volume 2013, Article ID 708489, 5 pages http://dx.doi.org/10.1155/2013/708489 Case Report A Puzzle of Hemolytic Anemia, Iron and Vitamin B12 Deficiencies
Hindawi Publishing Corporation Case Reports in Hematology Volume 2013, Article ID 708489, 5 pages http://dx.doi.org/10.1155/2013/708489 Case Report A Puzzle of Hemolytic Anemia, Iron and Vitamin B12 Deficiencies
Anemia s. Troy Lund MSMS PhD MD
 Anemia s Troy Lund MSMS PhD MD lundx072@umn.edu Hemoglobinopathy/Anemia IOM take home points. 1. How do we identify the condtion? Smear, CBC Solubility Test (SCD) 2. How does it present clincally? 3. How
Anemia s Troy Lund MSMS PhD MD lundx072@umn.edu Hemoglobinopathy/Anemia IOM take home points. 1. How do we identify the condtion? Smear, CBC Solubility Test (SCD) 2. How does it present clincally? 3. How
Chapter 2. ERYTHROPOIESIS and ANEMIA
 Chapter 2 ERYTHROPOIESIS and ANEMIA Red Cell Production The Production of red cells, known as erythropoiesis, is a developmental system fundamentally under genetic control but modulated and regulated by
Chapter 2 ERYTHROPOIESIS and ANEMIA Red Cell Production The Production of red cells, known as erythropoiesis, is a developmental system fundamentally under genetic control but modulated and regulated by
Dr. Shiva Nazari Assistant Professor of Pediatric Oncologist & Hematologist Shahid Beheshti Medical Science University Mofid Children s Hospital
 Dr. Shiva Nazari Assistant Professor of Pediatric Oncologist & Hematologist Shahid Beheshti Medical Science University Mofid Children s Hospital Reduction in the normal red cell survival (120 days) RBC
Dr. Shiva Nazari Assistant Professor of Pediatric Oncologist & Hematologist Shahid Beheshti Medical Science University Mofid Children s Hospital Reduction in the normal red cell survival (120 days) RBC
Hematology: Challenging Cases with Your Participation COPYRIGHT
 Hematology: Challenging Cases with Your Participation Reed E. Drews, MD Beth Israel Deaconess Medical Center Harvard Medical School Boston, MA Question 1 Question 1 64-year-old man is evaluated during
Hematology: Challenging Cases with Your Participation Reed E. Drews, MD Beth Israel Deaconess Medical Center Harvard Medical School Boston, MA Question 1 Question 1 64-year-old man is evaluated during
ORIGINAL ARTICLE CLINICO PATHOLOGICAL REVIEW OF MEGALOBLASTIC ANAEMIA IN CHILDREN- A 7 YEAR PAEDIATRIC HOSPITAL EXPERIENCE
 CLINICO PATHOLOGICAL REVIEW OF MEGALOBLASTIC ANAEMIA IN CHILDREN- A 7 YEAR PAEDIATRIC HOSPITAL EXPERIENCE M.Ramani 1, D.Ranganath 2,O.H.RadhikaKrishna 3, K.Geetha 4, M.Keerthika 5, PujaDeshmukh 6, S.P.Krupani7,
CLINICO PATHOLOGICAL REVIEW OF MEGALOBLASTIC ANAEMIA IN CHILDREN- A 7 YEAR PAEDIATRIC HOSPITAL EXPERIENCE M.Ramani 1, D.Ranganath 2,O.H.RadhikaKrishna 3, K.Geetha 4, M.Keerthika 5, PujaDeshmukh 6, S.P.Krupani7,
Chapter 13. Trace Minerals
 Chapter 13 Trace Minerals Minerals in the Human Body The Trace Minerals--An Overview Needed in very small quantities in the body. Perform many essential functions important to health. Toxic levels can
Chapter 13 Trace Minerals Minerals in the Human Body The Trace Minerals--An Overview Needed in very small quantities in the body. Perform many essential functions important to health. Toxic levels can
Dairion Gatot, Soegiarto Ganie, Savita Handayani. Divisi Hematologi & Onkologi Medik Departemen Ilmu Penyakit Dalam FK-USU/RS H.Adam Malik Medan 2009
 HAEMOLYTIC ANAEMIA Dairion Gatot, Soegiarto Ganie, Savita Handayani. Divisi Hematologi & Onkologi Medik Departemen Ilmu Penyakit Dalam FK-USU/RS H.Adam Malik Medan 2009 WHEN BY THEN Hb 9 g% transfusion
HAEMOLYTIC ANAEMIA Dairion Gatot, Soegiarto Ganie, Savita Handayani. Divisi Hematologi & Onkologi Medik Departemen Ilmu Penyakit Dalam FK-USU/RS H.Adam Malik Medan 2009 WHEN BY THEN Hb 9 g% transfusion
Hemolytic anemias (2 of 2)
 Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy Mutation in the β-globin
Hemolytic anemias (2 of 2) Sickle Cell Anemia The most common familial hemolytic anemia in the world Sickle cell anemia is the prototypical (and most prevalent) hemoglobinopathy Mutation in the β-globin
Hemoglobin. Each alpha subunit has 141 amino acids, and each beta subunit has 146 amino acids.
 In the previous lecture we talked about erythropoiesis and its regulation by many vitamins like vitamin B12 and folic acid, proteins, iron and trace elements copper and cobalt. Also we talked about pernicious
In the previous lecture we talked about erythropoiesis and its regulation by many vitamins like vitamin B12 and folic acid, proteins, iron and trace elements copper and cobalt. Also we talked about pernicious
Management of anemia in CKD
 Management of anemia in CKD Pierre Cochat, MD PhD Professor of Pediatrics Chair, Pediatrics & Pediatric Surgery Department Head, Center for Rare Renal Diseases Néphrogones Hospices Civils de Lyon & University
Management of anemia in CKD Pierre Cochat, MD PhD Professor of Pediatrics Chair, Pediatrics & Pediatric Surgery Department Head, Center for Rare Renal Diseases Néphrogones Hospices Civils de Lyon & University
Objectives. But first: What s in blood? Introduction. Overview: Erythrocytes. Erythrocytes, cont. 4/10/2016
 Objectives Nutritional Deficiencies That May Cause Anemia 1. Discuss the role that various nutrients play in red blood cell formation. 2. List sources of nutrients involved in red blood cell formation.
Objectives Nutritional Deficiencies That May Cause Anemia 1. Discuss the role that various nutrients play in red blood cell formation. 2. List sources of nutrients involved in red blood cell formation.
Disorders of Blood Cells & Blood Coagulation
 Disorders of Blood Cells & Blood Coagulation HIHIM 409 WBC count RBC count WBC differential Hemoglobin (HGB) Hematocrit (HCT) % of volume occupied by RBCs CBC Red cell indices Mean cell volume (MCV) average
Disorders of Blood Cells & Blood Coagulation HIHIM 409 WBC count RBC count WBC differential Hemoglobin (HGB) Hematocrit (HCT) % of volume occupied by RBCs CBC Red cell indices Mean cell volume (MCV) average
Zahraa Muneer. Enas Ajarma. Saleem
 2 Zahraa Muneer Enas Ajarma Saleem Blood parameters: 1. RBCs count 2. Haematocrit 3. Haemoglobin content In new-born babies all three parameters of blood are higher than in normal adults. This happens
2 Zahraa Muneer Enas Ajarma Saleem Blood parameters: 1. RBCs count 2. Haematocrit 3. Haemoglobin content In new-born babies all three parameters of blood are higher than in normal adults. This happens
Year 2003 Paper two: Questions supplied by Tricia
 QUESTION 93 A 24-year-old woman, who has recently arrived in Australia from Vietnam, presents for evaluation of abnormal menstrual bleeding. There are no abnormalities on examination. Results of investigations
QUESTION 93 A 24-year-old woman, who has recently arrived in Australia from Vietnam, presents for evaluation of abnormal menstrual bleeding. There are no abnormalities on examination. Results of investigations
RBCs Disorders 1. Dr. Nabila Hamdi MD, PhD
 RBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Discuss the classification of anemia into hypochromic-microcytic, normochromicnormocytic and macrocytic. Categorize laboratory test procedures used in the
RBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Discuss the classification of anemia into hypochromic-microcytic, normochromicnormocytic and macrocytic. Categorize laboratory test procedures used in the
Genetics of Thalassemia
 Genetics of Thalassemia Submitted by : Raya Samir Al- Hayaly Sura Zuhair Salih Saad Ghassan Al- Dulaimy Saad Farouq Kassir Sama Naal Salouha Zahraa Jasim Al- Aarajy Supervised by : Dr. Kawkab Adris Mahmod
Genetics of Thalassemia Submitted by : Raya Samir Al- Hayaly Sura Zuhair Salih Saad Ghassan Al- Dulaimy Saad Farouq Kassir Sama Naal Salouha Zahraa Jasim Al- Aarajy Supervised by : Dr. Kawkab Adris Mahmod
Hematology Unit Lab 1 Review Material
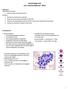 Hematology Unit Lab 1 Review Material - 2018 Objectives Laboratory instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Hematology Unit Lab 1 Review Material - 2018 Objectives Laboratory instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
