Urinary System Basics
|
|
|
- Grace Cole
- 6 years ago
- Views:
Transcription
1 Urinary William A. Olexik Urinary System Basics A. Concept 1. Kidneys 2. Ureters 3. Urinary bladder 4. Urethra INTRODUCTION B. Importance Homeostasis 1. General meaning -- maintenance of life requirements within narrow tolerance limits, given continual variable influences. 2. Specific urinary application -- overall homeostasis of body fluids a. Direct -- blood & ECF b. Indirect -- ICF, from contact with ECF C. Functions 1. Fluid balance [details later ] a. Volume maintenance b. Solute amounts c. Acid-base maintenance d. Transport between ECF & ICF -- osmotic context 2. Excretion a. Fluid balance -- in order to maintain homeostasis, elimination of excesses required b. Toxicity -- elimination of toxins
2 Urinary -- 2 Excretion A. Meaning 1. Separation from body fluids & ejection out of body of metabolic waste products 2. Must have been involved in metabolic reactions to be an excretion B. Systems Represented 1. Urinary -- full-time, primary function 2. Integumentary -- part-time, but very significant function 3. Respiratory -- part-time, significant function 4. Digestive -- part-time, secondary function C. Substances Excreted 1. General a. Due to varying homeostatic needs, some substances which are considered valuable metabolites may at times be excreted b. Other, usually toxic, substances are always excreted in greater quantities 2. Water -- from ingestion & cellular respiration a. Urine ml/day Less in hot weather & strenuous exercise b. Skin, via sweat glands & diffusion ml/day Up to 10x more in hot weather & exercise c. Expired as water vapor ml/day May double during exercise d. Feces ml/day under all conditions
3 Urinary CO 2 -- from cellular respiration a. Overwhelming majority expired b. Some via urine, feces & sweat -- CaCO 3 4. Nitrogenous organic compounds a. From amino acid metabolism in the liver General Most via urine Some via bile & sweat Urea -- 90% of total Urate (uric acid) Ammonia (NH 3 ) -- quite toxic Excess amino acids -- only 1-2 g/day b. From muscle metabolism -- creatinine From unique high energy creatine-po 4 Some excreted via urine c. From benzoic acid detoxification Hippuric acid -- benzoic acid + glycine Via urine 5. Non-nitrogenous organic compounds a. General Most via urine Slight via sweat & oil glands, & feces Quite variable in types & amounts b. Glucose -- barely perceptible amounts c. Ketone bodies From fatty acid metabolism
4 Urinary -- 4 Minute amounts d. Oxalates -- small amounts e. Citrate -- small amounts f. Vitamins -- excess water soluble g. Hormones h. Enzymes -- only a few 6. Inorganic salts (electrolytes) 7. Heat a. General Most via urine -- exceptions noted Some in sweat & feces b. In decreasing amount: Chloride Sodium Potassium Sulfate Phosphate Calcium -- more via feces Magnesium -- more via feces a. Not a chemical substance, but there is elimination of the excess not utilized to maintain body temperature b. From cellular respiration c. Most via skin Sweat carries away more heat than dry skin Extra vessels deliver more heated blood d. Some via urine, feces & expired air D. Basic Processes [ all details later ] 1. Filtration a. Removes majority of substances from blood b. Substances now in space which eventually leads outside of
5 Urinary -- 5 the body 2. Reabsorption a. Removal of most components from what was filtered & return to body fluids b. Selectivity is its importance 3. Secretion a. Addition of extra amounts of some substances to what was filtered b. From body fluids via different route Gross Kidney Structure [ details from lab ] A. Regions 1. Cortex a. Outer b. Columns 2. Medulla a. Inner b. Pyramids Divisions Apex -- papilla B. Urine Collecting Structures 1. Calyces a. Minor One per pyramid -- funnel-shaped Receives urine from papillary ducts [ later ] b. Major -- confluence of several minor
6 Urinary Pelvis -- receives major calyces 3. Ureter a. Tube from narrowing of pelvis b. Exits kidney through hilus c. Represents duct for entire kidney d. Takes urine to bladder C. Blood vessels 1. Renal artery & vein 2. Interlobar arteries & veins a. Branches from renals b. Run through columns 3. Arcuate arteries & veins a. Perpendicular branches from interlobars b. Run along cortical-medullary border 4. Interlobular arteries & veins a. Perpendicular branches from arcuates b. Run through cortex outwardly 5. Other branches from interlobulars a. Run through cortex and under capsule b. Example -- intralobulars Microscopic Kidney Structure A. Nephron 1. General a. Basic structural & functional unit b. 1.5 million per kidney
7 Urinary -- 7 c. Essentially a tubular glandular unit d. 2 types Cortical Majority Shorter mm Mostly within cortex Juxtamedullary Longer mm 2. Bowman's (renal) capsule Over half its length runs through pyramid, almost to apex (papilla) a. Double-walled rounded cup-like b. 200 μm across c. Squamous parietal wall d. Visceral wall of unique podocytes -- cling to & follow contours of enclosed glomerulus [ not part of nephron per se -- later ] e. Beginning portion 3. Proximal convoluted tubule a. About 15 mm (L) x 60 μm (D) b. Simple cuboidal cells with microvilli c. Completely within cortex 4. Thick descending (straight proximal) tubule a. About 2 mm (L) x 30 μm (D) b. Low cuboidal cells with microvilli c. Enters medulla in juxtamedullary nephrons 5. Loop of Henle (thin portions)
8 Urinary -- 8 a. General About 5-15 mm (L) x 15 μm (D) Longer in juxtamedullary nephrons Squamous cells b. Descending portion -- longer c. Ascending portion -- shorter 6. Thick ascending (straight distal) tubule a. About 7 mm (L) x 60 μm (D) b. Cuboidal cells with short microvilli c. Runs back into cortex 7. Distal convoluted tubule a. About 10 mm (L) x 60 μm (D) b. Cuboidal cells with sparse (beginning ) to no microvilli (end) c. Last portion of nephron B. Excretory Ducts 1. General a. Take liquid from nephron b. Chemical adjustments to produce final urine c. Pass urine to minor calyces d. Total length of one pathway of this highly branched & interconnected complex mm 2. Collecting tubule a. Begins at end of distal convoluted tubule b. Same diameter as DCT c. Simple cuboidal cells 3. Collecting ducts
9 Urinary -- 9 a. Smallest formed by confluence of several collecting tubules b. Several levels of branching to larger ducts c. Up to 100 μm diameter d. Cells from simple cuboidal to simple columnar 4. Papillary duct (of Bellini) a. Largest ducts -- confluence of several of largest collecting ducts b. 200 μm diameter c per papilla of a pyramid d. Final ducts - empty into minor calyx C. Capillaries & Arterioles 1. General a. Supply nephron with blood for filtering b. Receptacle for reabsorbed substances c. Source for secreted substances 2. Glomerulus a. Balled-up capillary bed b. Nestled within Bowman's capsule -- tightly adherent to visceral wall c. Special lining squamous cells -- fenestrated & extremely permeable 3. Afferent arteriole a. Branches from other arteries after interlobular b. Joins glomerulus 4. Efferent arteriole a. Joins opposite end of glomerulus b. Carries blood from glomerulus
10 Urinary c. Exception to venule draining capillaries d. Smaller than afferent 5. Peritubular capillaries a. Capillary bed surrounding cortical nephron portions b. Variations in 2 nephron types Cortical -- around straight proximal & distal, & most of thin loop of Henle Juxtamedullary -- only around convoluted portions c. Receive blood from efferent arterioles d. Join venules which eventually lead to interlobular vein 6. Vasa recta a. Only in association with juxtamedullary nephrons b. Origin from efferent arterioles, just like peritubular c. Descend into medulla, paralleling straight tubule portions & thin loop of Henle d. Hairpin turn, just like loop of Henle e. Lateral interconnections among vasa recta form plexuses in medulla e. Join same venules as peritubular capillaries D. Renal (Malpighian) Corpuscle 1. Concept -- term applied to glomerulus & the attached Bowman' capsule which surrounds it 2. Significance -- represents vital link between nephron & its initial blood supply
11 URINE FORMATION Urinary Filtration A. Introduction 1. Location -- renal corpuscles 2. Concept a. Filtration (diffusion under pressure) of substances from blood circulating through glomerulus into capsular space of nephron. b. Involves passage through glomerular endothelium, a basement membrane & the capsule's visceral wall of podocytes. 3. Significance a. Rapid removal of diffusible substances from blood b. No selectivity as to importance -- basically just size c. Later, more leisurely selective processes in other parts of nephron B. Ultrafiltrate 1. Concept -- filtrate contains same concentration of substances as blood 2. Significance -- this direct quantitative reflection permits kidneys to accurately determine the homeostatic fates of the various substances 3. Exclusions -- non-permeable materials a. Formed elements b. Plasma proteins c. Lipids -- e.g. cyclomicrons C. Physical Mechanisms 1. Glomerular endothelium
12 Urinary a. Many large fenestrations b. Only formed elements not permeable 2. Basement membrane a. Ionized -- highly negative b. Repels plasma proteins -- negatively ionized 3. Visceral wall of capsule a. Podocytes Branching major & minor processes -- wrap around glomerulus Terminals -- feet (pedicels) Feet from different podocytes interdigitate b. Diffusion through gaps between feet D. Pressures Responsible 1. Blood a. Glomerular hydrostatic (blood) pressure at afferent arteriolar end about 60 mmhg b. Much higher than body's other capillaries c. This force necessary to drive filtration 2. Colloid osmotic a. From blood's non-diffusible plasma proteins -- about 25 mmhg b. Opposes blood pressure & filtration 3. Capsular hydrostatic a. From filtrate constantly within capsule, between visceral & parietal walls -- about 10 mmhg b. Opposes filtration 4. Net filtration pressure a. Blood - (colloid osmotic + capsular) b. 60 mmhg - (25 mmhg + 10 mmhg) = 25 mmhg
13 Urinary E. Rate 1. Basic a. 125 ml/min from all nephrons in both kidneys b. 180 L per day c. Represents 20% of the plasma 2. Variations a. Sex -- lower in women b. Variable under different conditions in same person F. Unique Variables 1. General -- necessary to form sufficient filtrate quickly 2. To maintain high net filtration pressure a. Glomerulus between 2 arterioles Only place in body Efferent (2nd) arteriole's resistance helps maintain higher pressure than venule would b. Difference in afferent/efferent diameters Efferent smaller Increased resistance to flow raises pressure c. Renal blood pressure -- higher than other organs 3. Permeability -- glomerular endothelium 100x more than other capillaries Reabsorption A. Introduction 1. Concept -- selective removal of substances from filtrate 2. Amount -- of 180 L/day filtrate, only L urine
14 Urinary Locations a. From filtrate in rest of nephron & collecting lumen -- mostly proximal b. To interstitial (tissue) fluid around nephron c. Into peritubular capillaries & vasa recta to be carried away 4. Significance a. Filtration was massive, but nonselective b. Reabsorption determines urine composition -- mostly [ secretion later ] c. Not inefficient, despite having to reverse most of filtration -- [ evidence later -- counter-current ] B. Water 1. General a. Normally 97-99% reabsorbed from filtrate b. 65% from proximal convoluted & straight 2. Obligatory a. This must be reabsorbed b. Majority -- from proximal c. Passive -- from osmotic gradient created by reabsorption of solutes from filtrate [ details later ] 3. Facultative a. Variable amounts, depending on homeostatic needs b. From distal convoluted & collecting c. Controlled by ADH Permeability in direct proportion Reason for osmotic gradient [later -- counter-current] d. Diabetes insipidus Absence of ADH
15 Urinary Excretion of L/day of mostly aqueous urine 4. Membrane mechanisms a. Aquaporins water channels b. Membrane proteins all body cells have these c. 4 subunits with channel between d. 8 distinct types some also handle small solutes (e.g. glycerol) e. Cells of proximal convoluted and straight, and descending just thin follow sodium gradient f. Collecting duct cells regulated by ADH C. Minerals 1. Sodium a. 99% reabsorbed from filtrate b. Mechanisms Actively transported from tubule cell cytoplasm into interstitial fluid Concentration gradient causes diffusion from tubule lumen -- most facilitated by carrier, which makes it more efficient c. Significance Its movement is basis for co-transport of other solutes & part of osmotic reabsorption of water Central role in counter-current mechanism [ later ] d. Variations in nephron segments Proximal -- as described above Distal -- variable Less permeable cell membranes Hormonal control -- aldosterone
16 Urinary Chloride a. 99% reabsorbed b. Mechanisms 3. Potassium Most directly follows sodium, to maintain electrical balance Some by co-transport a. Some reabsorbed b. Mechanisms 4. Calcium Due to Na + /K + pump, transported opposite sodium -- into tubule cells from interstitial fluid Tends to diffuse back out through sides at intercellular junctions, though a. Most reabsorbed b. Mechanism -- co-transport 5. Magnesium a. Some reabsorbed b. Mechanism -- co-transport 6. Bicarbonate a. Almost all reabsorbed b. Mechanism -- complicated 7. Others Tubule lumen -- CO 2 diffuses out In cell -- CO 2 + H 2 O = H 2 CO 3 = H + + HCO 3 - Bicarbonate into interstitium by co-transport a. Phosphate, sulfate & nitrate -- some reabsorbed b. Mechanism -- co-transport
17 Urinary D. Nitrogenous Wastes 1. Urea a. 50% reabsorbed b. Mechanism -- passive, follows water 2. Urate a. 98% reabsorbed b. Mechanism -- co-transport 3. Creatinine a. None is reabsorbed b. [ see below -- secretion ] E. Organic Nutrients 1. General a. Glucose, amino acids, vitamins (water soluble), & ketone bodies b. Normal amounts completely reabsorbed -- vital c. Mechanisms 2. Proteins Co-transport from lumen into tubule cells Facilitated diffusion from cells into interstitium a. Completely reabsorbed b. Mechanism -- special handling, since non-permeable From tubule lumen by pinocytosis Hydrolyzed into amino acids -- now handled as already described
18 Urinary Sucrose, oxalates & citrates None reabsorbed Secretion A. Introduction 1. Concept a. Addition to filtrate of substances which were not filtered b. Opposite direction from reabsorption 2. Locations From peritubular capillary blood Into interstitial fluid Enters tubule lumen a. Distal convoluted tubule b. Collecting tubule & duct 3. Significance a. Permits maximum excretion of certain substances, making up for ultrafiltrate inadequacy b. Some toxic substances cannot be filtered B. Substances 1. Ammonia a. Too toxic for body fluids b. NH 3 + glutamic acid = glutamine (nontoxic) c. DCT reverses reaction d. Excreted as ammonium ion NH 3 + H + + = NH 4 2. Hippuric acid a. Benzoates -- toxic
19 Urinary b. Benzoic acid (e.g.) + glycine = hippuric acid (nontoxic) c. DCT reverses reaction 3. Creatinine a. None was reabsorbed -- secretion adds to amount excreted in urine b. Mechanism -- active transport 4. Potassium & hydrogen a. DCT & collecting tubules b. Mechanisms 5. Others Counter-transport -- earlier portions From active sodium reabsorption More negative tubule lumen attracts positive ions Active transport -- latter portions K + -- aldosterone control H + -- special cells, for ph homeostasis a. e.g. -- organic acids & bases; neurotransmitters b. Mechanism -- active transport 6. Abnormal a. e.g. -- drugs b. Mechanism -- active transport
20 Counter-current Mechanism A. Introduction Urinary Urine/filtrate difference a. Urine typically hyperosmotic to original filtrate b. Most water usually needed in body fluids 2. Progressive concentration a. Would seem to occur from capsule to collecting b. Not possible Would require active transport of water Osmotic gradient 900x greater than exists 3. Variable filtrate osmotic conditions [ all will be compared with original capsular filtrate] a. Isosmotic (no change) -- PCT & thick descending b. Hyperosmotic (more concentrated) -- loop of Henle c. Isosmotic (same as filtrate) -- thick ascending d. Hypoosmotic (more dilute) -- DCT e. Hyperosmotic -- latter DCT & collecting 4. Significance a. Permits concentration of solute wastes b. Conserves water c. Accomplished via simple fluid principles d. Variable due to hormonal influences -- more dilute urine can be produced if excess water excretion needed [ later ] B. Underlying Principles 1. Concentration gradients
21 Urinary a. Increased when gong from cortex into medulla b. Decreased when going from medulla into cortex 2. Innate behavior from physical relationships a. Physical setup Parallel tubes Hairpin connections Solution flowing in opposite directions Semipermeable walls Fluid surrounding tubes b. Results Setup will cause a small concentration difference to be multiplied continuously through the tubes Must be this type of setup for production of concentrated urine -- straight, or differently configured tubes would work poorly or not at all 3. Gradient maintenance a. Loop of Henle Establishes gradient From descending/ascending differences [ later ] b. Vasa recta Maintains gradient established by loop Own separate counter-current multiplier -- coordinated with nephron/collecting, though c. Collecting tubule & ducts Finish the process, producing final urine Variable, due to ADH [ later ] 4. Osmotic counter currents a. Entire mechanism based on osmotic currents
22 Urinary b. Created by continuously circulating filtrate, interstitial fluid & blood -- form positive feedback loops c. Opposite currents in descending & collecting as compared with ascending d. Opposite currents in ascending & descending limbs of vasa recta C. Mechanisms of Action 1. Proximal convoluted tubule a. Results 65 + % volume reduction of capsular filtrate Proportional, though -- isosmotic to filtrate b. Events Active sodium (with chloride) reabsorption Passive osmosis of water -- follows sodium 2. Ascending thin & thick a. This is the next logical step Filtrate itself is next in descending portions Ascending events control those in descending b. Results Change to isosmotic -- was hyper- at bottom of loop Hypoosmotic by DCT c. Events Active chloride (with sodium) transport out No osmosis follows -- impermeable to water 3. Descending thick & thin a. Results -- very hyperosmotic by bottom of loop b. Events Sodium diffuses in
23 Urinary Water diffuses out by osmosis c. Cause -- hyperosmotic medullary fluid [ later ] 4. Distal convoluted & collecting tubules a. Results Progressively less hypoosmotic Variable -- from hypo- to hyperosmotic b. Events Osmosis out -- no longer impermeable ADH responsible for variable amount -- direct proportion c. Causes Active sodium (with chloride) transport out Hyperosmotic medullary fluid attracts water 5. Medullary tissue fluid a. Result Perpetually kept hyperosmotic More hyperosmotic higher to lower b. Causes 6. Vasa recta Active salt transport out of thick ascending Active salt transport out of collecting Passive salt transport out of thin descending Passive urea transport out of collecting -- follows water, from ADH increase Vasa recta leaves behind excess sodium [ later ] a. Result -- prevents medullary blood from removing excess solutes
24 Urinary b. Causes Sluggish blood flow -- only 1-2% of kidney total Counter-current exchange mechanism Removes excess water from medulla -- recall diffusion from descending Leaves behind excess sodium D. Summary 1. Production of concentrated urine a. Basic counter-current mechanism b. Increased ADH 2. Production of dilute urine a. Basic counter-current mechanism b. Decreased ADH MICTURITION A. Concept 1. Expulsion of urine from the bladder 2. Commonly termed urination or voiding B. Mechanisms 1. Muscles a. Detrusor -- general smooth muscle of bladder wall b. Internal urethral sphincter Smooth muscle Around beginning of urethra
25 Urinary c. External urethral sphincter Skeletal muscle Below internal sphincter d. Rectus abdominis 2. Volumes a ml -- threshold for initiation b. 500 ml 3. Pressure receptors Total effective capacity Very little ability to retain more without considerable discomfort a. Within bladder wall b. Respond to stretch from filling c. Impulses to sacral segments of spinal cord d. Initiate reflex muscle responses eventually leading to micturition e. May completely occur locally -- brain may intervene 4. Muscle responses a. Detrusor Parasympathetic impulses from spinal cord Wave-like rhythmic contractions b. Internal sphincter Towards urethral outlet Periodic & widespread until maximum capacity reached Remains contracted via sacral reflex to prevent micturition Relaxation under different conditions <500 ml -- only when external sphincter relaxed
26 Urinary c. External sphincter >500 ml -- from intense detrusor contractions Remains contracted via sacral reflex -- inhibition causes relaxation Relaxation under different conditions d. Rectus abdominis <500 ml -- conscious decision >500 ml -- unconscious, along with internal sphincter Contracted to increase intra-abdominal pressure Pressure on full bladder assists 5. Brain centers a. Cerebral cortex Responsible for learned reflex which contracts external sphincter Initiates conscious relaxation of external sphincter for micturition Can override spinal micturition reflex, if volume not extreme b. Brainstem Pons & medulla Unconscious facilitation or inhibition of spinal reflex C. Pathology 1. Incontinence a. Concept Loss of bladder control From slight to inability to retain any urine
27 Urinary b. Normal in infants -- insufficient development of nervous pathways between brain & sacral cord c. Abnormal 2. Retention Several sites of damage -- bladder, cord or brain Would determine severity a. Concept -- inability to void b. Causes Obstruction Spasmodic sphincter contraction Nerve damage Psychological factors -- e.g. stress FLUID BALANCE & DYNAMICS Blood Pressure Regulation -- Urinary Related A. Autonomic Nervous Control 1. General a. Affects kidneys only -- rest of body unaffected b. Sympathetic division alone -- parasympathetic not utilized to produce opposite effects 2. Pressure increase a. Moderate impulse level b. Afferent & efferent constricted proportionately c. Vasoconstriction raises glomerular pressure 3. Pressure decrease a. Intense impulse level
28 Urinary b. Afferent more constricted than efferent c. Arteriolar diameters closer to the same d. Pressure lowered -- size disparity negated B. Autoregulation 1. General a. Local -- not from outside (e.g. nervous) influences b. Purpose -- maintains constant effective filtration rate c. Mechanism Involves nephron & arterioles Accomplished chemically d. Significance More important than nervous More attuned to needs More effective (accurate) 2. Structure -- juxtaglomerular apparatus (JGA) or complex a. Indistinct -- merger of 3 parts of larger structures First part of distal convoluted tubule Afferent arteriole Efferent arteriole b. Each JGA from parts of same nephron/corpuscle c. Modified cells in wall of contact areas Macula densa -- distal tubule Juxtaglomerular cells -- arterioles 3. Mechanisms a. Sodium & chloride levels monitored -- distal filtrate
29 Urinary Too low if insufficient filtration pressure -- too much reabsorption in ascending Too high if excessive filtration pressure -- insufficient reabsorption in ascending b. To increase pressure & filtration rate Afferent arteriole dilated by macula densa Efferent arteriole constricted by juxtaglomerular cells -- indirect Increased renin secretion into blood Plasma angiotensinogen converted to angiotensin Angiotensin targets efferent arteriole c. To decrease pressure & filtration rate Afferent arteriole constricted Efferent arteriole dilated C. Systemic Control 1. General a. Overall BP changes throughout body b. Kidneys affected as well c. Sympathetic & autoregulation can counteract 2. Causes a. Cardiac output influences on BP b. Peripheral resistance -- e.g. widespread autonomic c. Respiratory needs requiring BP adjustments
30 Osmotic Pressure Regulation A. Scope Urinary Affects the entire body 2. Important homeostatic mechanism -- controls ECF/ICF interchanges 3. Intricate & interrelated -- very simple consideration here B. Increases 1. Concept -- hyperosmotic condition in body fluids 2. Causes a. Solute retention Ingestion -- more salt (solute) intake Kidney diseases -- excessive reabsorption Hormonal b. Water loss Hyperglycemia Aldosterone hypersecretion & no ADH change -- usually vary together Ingestion -- too little intake Fluid loss -- solutes lost as well, but water causes more dramatic effects Diarrhea Vomiting Excess sweating Hormonal Hyperglycemia -- water drawn from tissues Hyposecretion of ADH -- diabetes insipidus
31 Urinary C. Decreases 1. Concept -- hypoosmotic condition in body fluids 2. Causes a. Solute loss Ingestion -- insufficient salt (solute) intake Kidney infection -- e.g. glomerulonephritis Hormonal Hypoglycemia Aldosterone hyposecretion b. Water retention Ingestion -- excess intake Kidney failure Hormonal -- ADH hypersecretion D. Control Mechanisms 1. Osmoreceptors a. Within hypothalamus b. Monitor osmotic pressure of body fluids c. Activity level Hyperosmotic causes more activity Hypoosmotic causes less activity 2. Antidiuretic hormone (ADH) a. Secreted by hypothalamus b. Stored within pars nervosa c. Amounts More from increased osmoreceptor activity
32 Urinary Water reabsorption Less from decreased osmoreceptor activity a. In DCT & collecting tubules/ducts b. Direct proportion with ADH amount 4. Drinking center More reabsorption dilutes hyperosmotic body fluids Less reabsorption excretes excess water from hypoosmotic body fluids a. Within hypothalamus b. Controls thirst c. Precise amount needed consumed Immediate relief -- prevents further desire Takes 30 + min. for ingested water to actually dilute body fluids, though Extracellular Fluid Volume Regulation A. Scope [ same as for osmotic pressure ] Not any particular component of fluids as in osmotic changes -- the water is of critical importance, though B. Increases 1. General -- all produce solute and water retention 2. Ingestion a. Increased solutes & water
33 Urinary b. Malnutrition 3. Hormonal -- aldosterone & ADH hypersecretion 4. Kidney diseases -- e.g. chronic renal failure (insufficiency) 5. Cardiovascular diseases a. Hypertension b. Congestive heart failure 6. Drugs a. All would increase ADH b. e.g. -- nicotine, morphine, barbiturates, anesthetics C. Decreases 1. General -- caused by any general body fluid loss 2. Ingestion -- general decrease (e.g. undernourishment) 3. Hormonal -- aldosterone &/or ADH hyposecretion 4. Diseases a. Kidney reabsorptive deficiencies b. Systemic infections 5. Fluid losses a. Excessive sweating or severe burns b. Vomiting or diarrhea c. Hyperventilation 6. Drugs a. All diuretics b. e.g. -- alcohol, caffeine, lithium
34 Urinary D. Control Mechanisms [ Example of fluid volume decrease ] 1. Sodium reabsorption a. Renin -- secretion from JGA b. Angiotensin I -- renin converts from angiotensinogen c. Angiotensin II More active form Derived from angiotensin I Converted by lung enzyme d. Aldosterone Secretion stimulated by angiotensin II Increased sodium/chloride reabsorption e. Atrial natriuretic factor Secreted by heart wall Proportionate with blood volume Inhibits sodium/chloride reabsorption f. Salt appetite Hypothalamic center Regulates desire to consume salt More active under 2 body fluid conditions Less sodium concentration Decreased fluid volume 2. Water reabsorption a. Osmoreceptors Detect hyperosmotic body fluids Gradient purposely caused by sodium/chloride reabsorption
35 Urinary b. ADH Secretion increased Water reabsorption increased Counteracts hyperosmolality Increases body fluids -- ultimate goal Electrolyte Balance A. General 1. Scope a. Principal ions only b. Others important -- e.g. phosphate, sulfate 2. General effects a. Determine water distribution in body b. Acid-base balance c. Cell membrane irritability -- nerve & muscle B. Potassium 1. Functions -- principal intracellular cation a. Cytoplasmic osmotic pressure maintenance b. Membrane electrical potentials -- nerve & muscle c. Enzyme activation 2. Influences upon potassium a. Aldosterone Sodium reabsorption causes potassium secretion Excess potassium increases aldosterone b. ph
36 Urinary Acidosis causes more K + reabsorption To cause secretion of H + via ion exchange c. Sodium Basically moves opposite from potassium Kidneys handle Na + better -- if both low, it is more reabsorbed C. Sodium 1. Functions -- principal extracellular cation a. Extracellular osmotic pressure maintenance -- tissue fluid & blood b. Sodium pump Establishes basic membrane gradients Permits transport of other substances c. Membrane electrical potentials -- nerve & muscle 2. Influences upon sodium a. Aldosterone -- [ previously covered ] b. Atrial natriuretic factor -- [ previously covered ] c. Glomerular filtration rate (GFR) Indirect proportion for GFR : sodium excretion Conserves sodium when filtration in excess d. Other solutes -- glucose (e.g.) Hyperglycemia leads to glycosuria Sodium displaced by glucose More sodium excretion than desirable
37 Urinary D. Calcium 1. Functions -- most abundant cation (most in bones) a. Stabilizes membranes b. Regulates muscle contraction -- intracellularly c. Enzyme regulation -- as co-factor d. Adherence of adjacent cells 2. Influences upon calcium a. Hormonal PTH -- [ previously covered ] Thyrocalcitonin -- [ previously covered ] b. Digestive absorption Vitamin D enhances Phosphates inhibit c. Excretion Most via feces -- vitamin D & phosphate control Some via urine -- handled like sodium, under PTH influence E. Magnesium 1. Functions -- equally distributed a. Membrane stabilization -- nerve & muscle b. Enzyme co-factor -- e.g. ATPase & peptidases c. Calcium antagonist -- often 2. Influences upon magnesium a. Hormonal T 3, T 4, GH & PTH -- [ previously covered ] Via movements in/out of cells & bones
38 Urinary b. Excretion Most reabsorbed -- PTH control Direct nephron effect -- excess excreted F. Chloride 1. Functions -- principal extracellular anion a. Counteracts cations b. Osmotic pressure maintenance c. Acid-base balance -- usually via HCl 2. Influences upon chloride a. Sodium -- follow each other (except nerve/muscle) b. Digestive -- part of gastric HCl c. Bicarbonate Normally balance each other Excess Cl - loss (e.g.) -- alkalosis Acid-Base Balance A. Extracellular Buffering System 1. Dual function -- absorbs excess ions of opposite types a. Acidic -- H + b. Basic -- e.g. OH - 2. Systems utilized a. Bicarbonate -- mixture of H 2 CO 3 & NaHCO 3 b. Phosphate c. Protein 3. Mechanism -- using bicarbonate system a. Acid buffering
39 Urinary HCL + NaHCO 3 = H 2 CO 3 + NaCl b. Basic buffering NaOH + H 2 CO 3 = NaHCO 3 + H 2 O B. Lung Excretion 1. Frees CO 2 from blood in carbonic acid form 2. Dysfunctions a. Respiratory acidosis From hypoventilation Normal correction -- breathing control system increases ventilation b. Respiratory alkalosis From hyperventilation Uncommon C. Kidney Excretion 1. Bicarbonate -- adjusted by varying reabsorption 2. Hydrogen a. Exchanged for sodium [ previously covered ] b. Secondary frees bicarbonate which was utilized for neutralizing H + in body fluids c. H + neutralized within urine Combined with phosphate Combines with ammonia -- ties up potentially harmful ammonia as well
Urinary System Basics
 Urinary _ 1 INTRODUCTION 2002 William A. Olexik Urinary System Basics A. Concept 1. Kidneys 2. Ureters 3. Urinary bladder 4. Urethra B. Importance Homeostasis 1. General meaning _ maintenance of life requirements
Urinary _ 1 INTRODUCTION 2002 William A. Olexik Urinary System Basics A. Concept 1. Kidneys 2. Ureters 3. Urinary bladder 4. Urethra B. Importance Homeostasis 1. General meaning _ maintenance of life requirements
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Urinary System BIO 250. Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat. Routes of Waste Elimination
 Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
CHAPTER 25 URINARY. Urinary system. Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1. functions
 CHAPTER 25 URINARY Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1 fluid waste elimination secretion of wastes control blood volume and BP control blood ph electrolyte levels RBC levels hormone production
CHAPTER 25 URINARY Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1 fluid waste elimination secretion of wastes control blood volume and BP control blood ph electrolyte levels RBC levels hormone production
Chapter 25: Urinary System
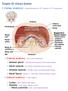 Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden
 Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden The urinary system is important because it performs vital excretory functions Takes blood from renal arteries into the kidney to filtrate
Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden The urinary system is important because it performs vital excretory functions Takes blood from renal arteries into the kidney to filtrate
Urinary system. Urinary system
 INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
Excretory Lecture Test Questions Set 1
 Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph
 The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
Chapter 23. The Nephron. (functional unit of the kidney
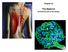 Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Chapter 17: Urinary System
 Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Urinary System and Fluid Balance. Urine Production
 Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Functions of the Urinary System
 The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Regulate aspects of homeostasis Water balance Electrolytes Acid-base balance in the blood
The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Regulate aspects of homeostasis Water balance Electrolytes Acid-base balance in the blood
Urinary bladder provides a temporary storage reservoir for urine
 Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Lab Activity 31. Anatomy of the Urinary System. Portland Community College BI 233
 Lab Activity 31 Anatomy of the Urinary System Portland Community College BI 233 Urinary System Organs Kidneys Urinary bladder: provides a temporary storage reservoir for urine Paired ureters: transport
Lab Activity 31 Anatomy of the Urinary System Portland Community College BI 233 Urinary System Organs Kidneys Urinary bladder: provides a temporary storage reservoir for urine Paired ureters: transport
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
Figure 26.1 An Introduction to the Urinary System
 Chapter 26 Figure 26.1 An Introduction to the Urinary System Components of the Urinary System Kidney Produces urine Ureter Transports urine toward the urinary bladder Urinary Bladder Temporarily stores
Chapter 26 Figure 26.1 An Introduction to the Urinary System Components of the Urinary System Kidney Produces urine Ureter Transports urine toward the urinary bladder Urinary Bladder Temporarily stores
The Urinary System. Copyright 2003 Pearson Education, Inc. publishing as Benjamin Cummings
 The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Functions of the Urinary System Regulate aspects of homeostasis Water balance Electrolytes
The Urinary System Functions of the Urinary System Elimination of waste products Nitrogenous wastes Toxins Drugs Functions of the Urinary System Regulate aspects of homeostasis Water balance Electrolytes
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
Other Factors Affecting GFR. Chapter 25. After Filtration. Reabsorption and Secretion. 5 Functions of the PCT
 Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System. BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College
 Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
BIOLOGY - CLUTCH CH.44 - OSMOREGULATION AND EXCRETION.
 !! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
!! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Kidney Structure. Renal Lobe = renal pyramid & overlying cortex. Renal Lobule = medullary ray & surrounding cortical labryinth.
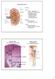 Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Urinary System kidneys, ureters, bladder & urethra
 Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
Urine Formation. Urinary Physiology Urinary Section pages Urine Formation. Glomerular Filtration 4/24/2016
 Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question.
 Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Urinary System kidneys, ureters, bladder & urethra
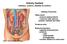 Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
I. Metabolic Wastes Metabolic Waste:
 I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
Essentials of Anatomy and Physiology, 5e (Martini/Nath) Chapter 18 The Urinary System. Multiple-Choice Questions
 Essentials of Anatomy and Physiology, 5e (Martini/Nath) Chapter 18 The Urinary System Multiple-Choice Questions 1) The urinary system A) regulates plasma concentrations of electrolytes. B) regulates blood
Essentials of Anatomy and Physiology, 5e (Martini/Nath) Chapter 18 The Urinary System Multiple-Choice Questions 1) The urinary system A) regulates plasma concentrations of electrolytes. B) regulates blood
Chapter 26 The Urinary System
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Excretion and Waste Management. Biology 30S - Miss Paslawski
 Excretion and Waste Management Biology 30S - Miss Paslawski Lesson 1 Waste Products and Organs 2 3 Excretion Excretion: Process by which dissolved metabolic wastes are separated from body fluids and removed
Excretion and Waste Management Biology 30S - Miss Paslawski Lesson 1 Waste Products and Organs 2 3 Excretion Excretion: Process by which dissolved metabolic wastes are separated from body fluids and removed
19. RENAL PHYSIOLOGY ROLE OF THE URINARY SYSTEM THE URINARY SYSTEM. Components and function. V BS 122 Physiology II 151 Class of 2011
 19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
organs of the urinary system
 organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
General Anatomy of Urinary System
 General Anatomy of Urinary System URINARY SYSTEM ORGANS Kidneys (2) Ureters (2) Urinary bladder Urethra KIDNEY FUNCTIONS Control blood volume and composition KIDNEY FUNCTIONS Filter blood plasma, eliminate
General Anatomy of Urinary System URINARY SYSTEM ORGANS Kidneys (2) Ureters (2) Urinary bladder Urethra KIDNEY FUNCTIONS Control blood volume and composition KIDNEY FUNCTIONS Filter blood plasma, eliminate
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
28/04/2013 LEARNING OUTCOME C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS STUDENT ACHIEVEMENT INDICATORS URINARY SYSTEM & EXCRETION
 LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
The Excretory System. Biology 20
 The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
The functions of the kidney:
 The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
Histology Urinary system
 Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Unit 15 - The Urinary System 1
 Unit 15 - The Urinary System 1 I. Unit 15: The Urinary System A. Functions of the Urinary System 1. Elimination of waste products a) Nitrogenous wastes b) Toxins c) Drugs 2. Regulate aspects of homeostasis
Unit 15 - The Urinary System 1 I. Unit 15: The Urinary System A. Functions of the Urinary System 1. Elimination of waste products a) Nitrogenous wastes b) Toxins c) Drugs 2. Regulate aspects of homeostasis
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
Chapter 16 Lecture Outline
 Chapter 16 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Chapter 16 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Unit 15: The Urinary System
 Unit 15: The Urinary System I. Functions of the Urinary System A. Elimination of waste products 1. Nitrogenous wastes 2. Toxins 3. Drugs B. Regulate aspects of homeostasis 1. Water balance 2. Electrolytes
Unit 15: The Urinary System I. Functions of the Urinary System A. Elimination of waste products 1. Nitrogenous wastes 2. Toxins 3. Drugs B. Regulate aspects of homeostasis 1. Water balance 2. Electrolytes
Urinary System Review Questions:
 Urinary System Review Questions: 1. This system would be lined with what type of membrane? 2. What type of epithelial tissue would line the opening of the urethra (the exit of the tract)? 3. What type
Urinary System Review Questions: 1. This system would be lined with what type of membrane? 2. What type of epithelial tissue would line the opening of the urethra (the exit of the tract)? 3. What type
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
The Urinary System. Jim Swan
 The Urinary System Jim Swan These slides are from class presentations, reformatted for static viewing. The content contained in these pages is also in the Class Notes pages in a narrative format. Best
The Urinary System Jim Swan These slides are from class presentations, reformatted for static viewing. The content contained in these pages is also in the Class Notes pages in a narrative format. Best
P215 Spring 2018: Renal Physiology Chapter 18: pp , Chapter 19: pp ,
 P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
Chapter 24: The Urinary System
 Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System)
 NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
The Urinary System 15PART B. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART B Ureters Slender tubes attaching the kidney to the bladder Continuous with
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART B Ureters Slender tubes attaching the kidney to the bladder Continuous with
Urinary System (Anatomy & Physiology)
 Urinary System (Anatomy & Physiology) IACLD CME, Monday, February 20, 2012 Mohammad Reza Bakhtiari, DCLS, PhD Iranian Research Organization for Science & Technology (IROST) Tehran, Iran The Urinary System
Urinary System (Anatomy & Physiology) IACLD CME, Monday, February 20, 2012 Mohammad Reza Bakhtiari, DCLS, PhD Iranian Research Organization for Science & Technology (IROST) Tehran, Iran The Urinary System
Lecture 16: The Nephron
 Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
Lecture 16: The Nephron Reading: OpenStax A&P Text Chapter 25 Primary functions of the kidneys 1. Regulating osmolarity (blood concentration!) A. Regulating blood pressure B. Maintaining ion balance C.
Class XI Chapter 19 Excretory Products and their Elimination Biology
 Class XI Chapter 19 Excretory Products and their Elimination Biology Question 1: Define Glomerular Filtration Rate (GFR) Glomerular filtration rate is the amount of glomerular filtrate formed in all the
Class XI Chapter 19 Excretory Products and their Elimination Biology Question 1: Define Glomerular Filtration Rate (GFR) Glomerular filtration rate is the amount of glomerular filtrate formed in all the
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
The Urinary System 15PART A. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART A Functions of the Urinary System Elimination of waste products Nitrogenous
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART A Functions of the Urinary System Elimination of waste products Nitrogenous
Chapter 26 The Urinary System. Overview of Kidney Functions. External Anatomy of Kidney. External Anatomy of Kidney
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Waste Products & Kidney Function
 Waste Products & Kidney Function urinary system principal means of metabolic waste removal urinary system is closely associated with reproductive system urogenital system share embryonic development share
Waste Products & Kidney Function urinary system principal means of metabolic waste removal urinary system is closely associated with reproductive system urogenital system share embryonic development share
Functions of the kidney
 Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
November 30, 2016 & URINE FORMATION
 & URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
& URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX
 One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
Unit #4 Waste and Excretion. The Kidneys
 Unit #4 Waste and Excretion The Kidneys Renal Hilus (Hilus) the doorway of the kidney Ureter leaves this region blood and lymphatic vessels enter and exit here Renal Capsule (Capsule) smooth fibrous tissue
Unit #4 Waste and Excretion The Kidneys Renal Hilus (Hilus) the doorway of the kidney Ureter leaves this region blood and lymphatic vessels enter and exit here Renal Capsule (Capsule) smooth fibrous tissue
URINARY SYSTEM. Urinary System
 URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
URINARY SYSTEM Urinary System Kidney Functions Excretion Regulation of blood volume and pressure Regulation of electrolyte and ph levels Kidney Structure Gross Anatomy Fibrous Capsule Renal Cortex Renal
Collin College. BIOL Anatomy & Physiology WEEK 12. Urinary System INTRODUCTION. Main functions of the kidneys are
 Collin College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 INTRODUCTION Main functions of the kidneys are regulate blood volume, water content regulate blood composition e..g. Na, Cl, K, ph
Collin College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 INTRODUCTION Main functions of the kidneys are regulate blood volume, water content regulate blood composition e..g. Na, Cl, K, ph
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
1. The Fibrous Capsule covers the outside of the kidney. It is made of fat and fibers.
 Slide 2 The kidney has a number of functions. First is the excretion of toxic metabolic waste through urine production. The kidneys filter blood plasma and as a result of filtering blood, the kidneys help
Slide 2 The kidney has a number of functions. First is the excretion of toxic metabolic waste through urine production. The kidneys filter blood plasma and as a result of filtering blood, the kidneys help
Waste. Urinary System Anatomy Urinary Section pages 5-8. Urinary System. Urinary System. Nitrogenous Wastes. Nitrogenous Wastes 4/22/2016
 Waste Urinary System Anatomy Urinary Section pages 5-8 Metabolism produces waste products What is the primary waste product of cellular respiration? How does the body dispose of it? Urinary System Urinary
Waste Urinary System Anatomy Urinary Section pages 5-8 Metabolism produces waste products What is the primary waste product of cellular respiration? How does the body dispose of it? Urinary System Urinary
A. Incorrect! The urinary system is involved in the regulation of blood ph. B. Correct! The urinary system is involved in the synthesis of vitamin D.
 Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
I. Anatomy of the Urinary System A. Kidneys 1. Right lower than Left* 2. Retroperitoneal 3. Layers that secure kidneys in the abdominal cavity a.
 I. Anatomy of the Urinary System A. Kidneys 1. Right lower than Left* 2. Retroperitoneal 3. Layers that secure kidneys in the abdominal cavity a. Renal fascia b. Perinephric fat (Adipose) capsule c. Fibrous
I. Anatomy of the Urinary System A. Kidneys 1. Right lower than Left* 2. Retroperitoneal 3. Layers that secure kidneys in the abdominal cavity a. Renal fascia b. Perinephric fat (Adipose) capsule c. Fibrous
Histology / First stage The Urinary System: Introduction. Kidneys
 The Urinary System: Introduction The urinary system consists of the paired kidneys and ureters, the bladder, and the urethra. This system helps maintain homeostasis by a complex combination of processes
The Urinary System: Introduction The urinary system consists of the paired kidneys and ureters, the bladder, and the urethra. This system helps maintain homeostasis by a complex combination of processes
