Clinical Therapeutics/Volume 29, Number 6, 2007
|
|
|
- Christal Little
- 6 years ago
- Views:
Transcription
1 Clinical Therapeutics/Volume 29, Number 6, 2007 A Retrospective Analysis of Possible Renal Toxicity Associated with Vancomycin in Patients with Health Care Associated Methicillin-Resistant Staphylococcus aureus Pneumonia Meghan N. Jeffres, PharmD 1 ; Warren Isakow, MD 2 ; Joshua A. Doherty, BS 3 ; Scott T. Micek, PharmD 1 ; and Marin H. Kollef, MD 2 1 Department of Pharmacy, Barnes-Jewish Hospital, St. Louis, Missouri; 2 Department of Pulmonary and Critical Care Medicine, Washington University School of Medicine, St. Louis, Missouri; and 3 Medical Informatics, BJC Healthcare, St. Louis, Missouri ABSTRACT Objective: The goal of this investigation was to determine whether more aggressive vancomycin dosing is associated with greater risk for renal toxicity in patients with health care associated pneumonia (HCAP) attributed to methicilllin-resistant Staphylococcus aureus (MRSA). Methods: This was a retrospective, single-center, observational cohort study. The following information was obtained for all study patients from automated hospital, microbiology, and pharmacy databases: age, sex, weight, serial serum creatinine (SCr), ageand sex-adjusted creatinine clearance (CrCl) during receipt of vancomycin, vancomycin serum trough concentrations, duration of vancomycin therapy, and Acute Physiology and Chronic Health Evaluation II scores. Renal toxicity was defined as either a 0.5-mg/dL increase from baseline in SCr or a 50% increase in SCr based on serial SCr measurements. Data for patients who met the definition of renal toxicity were compared with data for those who did not. Results: Ninety-four patients (mean [SD] age, 59.0 [15.6] years; 59 [62.8%] men; 73 (77.7%) white; mean baseline CrCl, 70.3 [23.0] ml/min) were identified as having MRSA HCAP. Forty (42.6%) patients developed renal toxicity. Patients who developed renal toxicity were significantly more likely than patients who did not develop renal toxicity to have greater mean vancomycin serum trough concentrations (20.8 [9.9] µg/ml vs 14.3 [6.7] µg/ml, respectively; P < 0.001), vancomycin serum trough concentrations 15 µg/ml (67.5% vs 40.7%; P = 0.01), and a prolonged duration ( 14 days) of vancomycin treatment (45.0% vs 20.4%; P = 0.011). Logistic regression analysis identified a maximum vancomycin serum trough concentration of 15 µg/ml as being independently associated with renal toxicity (adjusted odds ratio = 2.82; 95% CI, ; P = 0.045). The overall mean change in CrCl for the study population was 13.5 ( 16.0) ml/min (range, 0.0 to 62.6 ml/min). Patients with maximum measured vancomycin serum trough concentrations 15 µg/ml (n = 49) had significantly greater absolute changes in CrCl compared with patients with maximum measured vancomycin serum trough concentrations <15 µg/ml (n = 45) ( 18.9 [ 17.0] vs 7.6 [ 12.5] ml/min, respectively; P < 0.001). Conclusions: The results suggest that aggressive vancomycin dosing and prolonged vancomycin administration may be associated with greater risk for renal toxicity in patients with MRSA HCAP. However, this retrospective study cannot establish causation, and a prospective, randomized, double-blind trial is needed. (Clin Ther. 2007;29: ) Copyright 2007 Excerpta Medica, Inc. Key words: renal toxicity, Staphylococcus aureus, methicillin resistance, pneumonia. INTRODUCTION The American Thoracic Society and Infectious Diseases Society of America guidelines for the treatment of hospital-acquired, ventilator-associated, and health care associated pneumonia (HCAP) recommend a Accepted for publication April 13, doi: /j.clinthera /$32.00 Printed in the USA. Reproduction in whole or part is not permitted. Copyright 2007 Excerpta Medica, Inc. June
2 Clinical Therapeutics target vancomycin serum trough concentration of 15 to 20 µg/ml for the empiric or definitive treatment of methicillin-resistant Staphylococcus aureus (MRSA) infections. 1 This recommendation is based on the poor pulmonary distribution characteristics observed for vancomycin, with serum concentrations of 15 to 20 µg/ml potentially resulting in enhanced intrapulmonary drug delivery. 2,3 However, the efficacy of targeting increased vancomycin serum trough concentrations for the treatment of MRSA HCAP has not been established. 4 Two recent analyses failed to find improved outcomes in patients with MRSA infections, including HCAP, with target vancomycin trough concentrations of 15 to 20 µg/ml. 5,6 Vancomycin-associated renal toxicity has been a point of controversy since 1958, when Geraci et al 7 published the first case series linking the two. Since then, several studies have reported an association between vancomycin serum trough concentrations and renal toxicity However, the definition of renal toxicity, as well as the patient population and disease severity, has varied among these studies. Therefore, we performed a retrospective observational clinical study with 2 main goals: to determine the rate of renal toxicity in patients treated with vancomycin for MRSA HCAP confirmed by bronchoalveolar lavage (BAL) cultures, and to determine whether more aggressive dosing of vancomycin, resulting in serum trough concentrations 15 µg/ml, was associated with renal toxicity. PATIENTS AND METHODS Study Location and Patients This study was conducted at a university-affiliated, urban teaching hospital, Barnes-Jewish Hospital (1200 beds). During a 6.5-year period (January 1999 June 2005) all hospitalized patients with MRSA HCAP, microbiologically confirmed by BAL semiquantitative cultures, who were treated with vancomycin were eligible for this investigation. Patients with polymicrobial infection demonstrated by BAL cultures, those treated with vancomycin for <72 hours, and those with acute renal failure or requiring dialysis were excluded from evaluation. This study was approved by the Washington University School of Medicine Human Studies Committee, and informed consent was waived. Study Design and Data Collection A retrospective cohort design was employed to assess the effect of vancomycin serum trough concentrations on the occurrence of renal toxicity. The Barnes- Jewish Hospital protocol for intravenous administration of vancomycin requires measurement of steadystate trough concentrations, with a target of 15 to 20 µg/ml. Per protocol, all patients were initially treated with weight-based vancomycin, receiving 30 mg/kg in 2 divided doses during a 24-hour period. To identify potential study patients, a computerized list of all patients with MRSA HCAP who had received vancomycin and had available trough concentrations was generated by the Department of Medical Informatics through retrospective query of the microbiology, laboratory, and pharmacy databases at Barnes-Jewish Hospital (performed by J.A.D.). Patients could not be entered into the study more than once. For all study patients, the following information was recorded by one of the investigators (M.N.J.): age, sex, weight, serial serum creatinine (SCr) measurements, age- and sex-adjusted creatinine clearance (CrCl) calculated during receipt of vancomycin, measured vancomycin serum trough concentrations, duration of vancomycin therapy, and Acute Physiology and Chronic Health Evaluation (APACHE) II scores. Additionally, concomitant risk factors for renal toxicity were collected, including a diagnosis of diabetes mellitus, the ratio of blood urea nitrogen (BUN) to SCr, and administration of 1 of the following: IV contrast dye, loop diuretics, amphotericin B deoxycholate or lipid-formulation equivalent, aminoglycosides, angiotensin-converting enzyme inhibitors or angiotensin receptor blockers, cyclosporine or tacrolimus, and/or vasopressors (norepinephrine, phenylephrine, or vasopressin). Patients must have received the potentially renally toxic medication(s) while on vancomycin and before the maximum documented SCr ( ) during treatment. Vasopressor use was considered when it was initiated or maintained within 48 hours before. Definitions A clinical diagnosis of MRSA HCAP required the occurrence of new and persistent radiographic infiltrates in conjunction with 2 of the following: fever, leukocytosis, and purulent tracheal aspirate or sputum. For the purposes of this study, MRSA HCAP included patients hospitalized >2 days before a MRSApositive BAL culture was obtained, and patients with a first MRSA-positive BAL culture within 2 days of hospital admission and any of the following: admis Volume 29 Number 6
3 M.N. Jeffres et al. sion from another health care facility (including a nursing home), receipt of chronic dialysis, and previous hospitalization within 30 days. 1 A MEDLINE search was performed using the key words vancomycin, renal failure, creatinine, and creatinine clearance. Based on this literature review, renal toxicity was defined as either a 0.5-mg/dL increase from baseline in SCr or a 50% increase from baseline in SCr based on serial SCr measurements Baseline SCr and age- and sex-adjusted CrCl calculations were made before administration of vancomycin in all patients, using the following formula 15 : Estimated creatinine clearance = (140 age) (weight in kg)/(72 serum creatinine) (women only) If the patient s weight was >20% of ideal body weight (IBW), adjusted body weight (ABW) was calculated using the formula ABW = IBW + 0.4(actual body weight IBW), with IBW (men) = (inches above 60) and IBW (women) = (inches above 60). was defined as the highest SCr value during receipt of vancomycin. Minimum SCr (SCr min ) was defined as the lowest SCr value before during receipt of vancomycin or just before initiation of vancomycin. The presence of diabetes was defined as the need for insulin or an oral hypoglycemic agent before or during the patient s hospitalization. Pharmacokinetic Data Vancomycin trough concentrations were obtained from serum specimens collected 30 minutes before the administration time at steady state. Steady-state conditions were considered to be achieved after 3 doses of a particular vancomycin regimen (ie, 1 g IV q12h) based on the half-life for an individual patient, calculated as follows 15 : k e = (CrCl) Steady-state concentrations were estimated to be achieved in 65 (69%) patients within 36 hours of initiation of vancomycin, 16 (17%) patients within 48 hours of initiation, and the remaining 13 (14%) patients between 49 and 100 hours after starting vancomycin therapy. Vancomycin serum concentrations collected outside the 30-minute window were mathematically extrapolated as follows to represent a true trough concentration (n = 11) 15 : True trough = measured concentration e ([ k e time true] time actual), with time actual representing the actual time of trough assessment and time true representing the correct time of trough assessment. Statistical Analysis All comparisons were unpaired, and all tests of significance were 2-tailed. Continuous variables were compared using the Student t test for normally distributed variables and the Mann-Whitney U test for nonnormally distributed variables. The χ 2 test was used to compare categoric variables. The primary data analysis compared patients who met the study definition for renal toxicity with those who did not. Values are expressed as mean (SD) for continuous variables and as a percentage of the group from which they were derived for categoric variables. P was 2-tailed, and P 0.05 was considered statistically significant. We performed multiple logistic regression analyses using SPSS for Windows version 11.0 (SPSS Inc., Chicago, Illinois). Multivariate analysis was performed using models that were judged a priori to be clinically sound 16 ; this was prospectively determined to be necessary to avoid producing spuriously significant results with multiple comparisons. All potential risk factors that were significant at the 0.2 level in univariate analyses were entered into the model. A stepwise approach was used to enter new terms into the logistic regression model, in which renal toxicity was the dependent outcome variable and 0.05 was set as the limit for the acceptance or removal of new terms. RESULTS Patients The study cohort consisted of 94 patients. Their mean (SD) age was 59.0 (15.6) years (range, years). The mean APACHE II score was 20.2 (8.3) (range, 3 37). There were 59 (62.8%) men and 35 (37.2%) women. Seventy-three (77.7%) patients were white, and 21 (22.3%) were black, Hispanic, or Asian American. The in-hospital mortality rate for the entire cohort was 27.7%, and the mean hospital length of stay was 35.6 (27.6) days. Forty (42.6%) patients developed renal toxicity while receiving vancomycin for the treatment of MRSA HCAP. Patients developing renal toxicity did not differ significantly from those without renal toxicity in June
4 Clinical Therapeutics terms of age, SCr min and the corresponding calculated CrCl, or the presence of diabetes, but they did have significantly greater APACHE II scores (P = 0.006) (Figure 1, Table I). Patients developing renal toxicity were significantly more likely to have a measured vancomycin steady-state serum trough concentration 15 µg/ml (P = 0.010) and to receive 14 days of vancomycin therapy (P = 0.011) (Table II). Stratification of patients according to their measured vancomycin steady-state serum trough concentrations indicated a statistically significant relationship with the occurrence of renal toxicity (P = 0.002) (Figure 2). A BUN:SCr ratio >20 (P = 0.027) and administration of vasopressors (P = 0.003) were also significantly greater among patients developing renal toxicity compared with those who did not develop renal toxicity (Table III). Among patients developing renal toxicity, the was temporally observed to follow the maximum vancomycin steady-state serum trough concentration by at least 24 hours in 34 (85.0%) patients. None of the patients developing renal toxicity went on to require dialysis during their hospitalization. Twenty-nine (72.5%) patients with renal toxicity had subsequent reductions in SCr toward baseline values before hospital discharge. Patients developing renal toxicity had significantly higher in-hospital mortality rates compared with those who did not develop renal toxicity (18 [45%] vs 8 [15%], respectively; P = 0.001) and greater mean (SD) hospital lengths of stay (44.8 [28.9] vs 28.7 [24.7] days; P = 0.006). The overall increase in SCr in the study population was a mean (SD) of 0.38 (0.61) mg/dl (range, mg/dl), with a corresponding decrease in calculated CrCl of 13.5 (16.0) ml/min. The change in SCr was 47.0% (54.4%) (range, 0% 266.7%). Compared with patients with maximum measured vancomycin steady-state serum trough concentrations <15 µg/ml (n = 45), patients with maximum trough concentrations 15 µg/ml (n = 49) had significantly greater concentrations (1.1 [0.55] vs 1.7 [0.88] mg/dl, respectively; P < 0.001), absolute changes in SCr (0.24 [0.28] vs 0.61 [0.73] mg/dl; P = 0.002), and percent changes in SCr (32.4% [35.9] vs 60.3% [64.6]; P = 0.012). Correspondingly, patients with maximum measured vancomycin steady-state serum trough concentrations 15 µg/ml had a significantly greater minimum calculated CrCl compared with patients with maximum measured vancomycin steady-state serum trough concentrations <15 µg/ml (65.4 [27.2] vs 49.0 APACHE II Score Absent Renal Toxicity Present Figure 1. Box plots of Acute Physiology and Chronic Health Evaluation (APACHE) II scores. The boxes represent the 25th to 75th percentiles, with the 50th percentile represented by the solid line within the boxes. The 10th and 90th percentiles are indicated as capped bars. [19.6] ml/min, respectively; P = 0.001), absolute reduction in calculated CrCl (18.9 [17.0] vs 7.6 [12.5] ml/min; P < 0.001), and percent change in calculated CrCl ( 26.3% [21.5] vs 10.7% [15.8]; P < 0.001). A secondary analysis was performed in patients without exposure to vasopressors. Eighty (85.1%) patients did not receive vasopressor agents during the study period, 29 (36.3%) of whom developed renal toxicity (Table II). Patients developing renal toxicity were significantly more likely to receive 14 days of therapy with vancomycin (P = 0.007) and to achieve greater vancomycin steady-state serum trough concentrations (P = 0.003) (Table II). Multivariate Analysis Multiple logistic regression analysis identified achievement of a vancomycin steady-state serum trough concentration 15 µg/ml as an independent predictor of renal toxicity (Table IV). A second multivariate analysis was performed excluding patients receiving vasopressors to validate the findings of the first analysis in this subgroup. Receiving 14 days of 1110 Volume 29 Number 6
5 M.N. Jeffres et al. Table I. Baseline patient characteristics. Renal Toxicity Renal Toxicity Characteristic Absent (n = 54) Present (n = 40) P Age, mean (SD), y 57.8 (18.3) 60.6 (10.9) Male, no. (%) 31 (57.4) 28 (70.0) White, no. (%) 39 (72.2) 34 (85.0) APACHE II score, mean (SD) 18.2 (8.5) 22.9 (7.4) Diabetes mellitus, no. (%) 16 (29.6) 12 (30.0) SCr min, mean (SD), mg/dl 0.94 (0.41) 0.96 (0.43) SCr min 1.4 mg/dl, no. (%) 10 (18.5) 6 (15.0) CrCl, mean (SD), ml/min 68.4 (25.8) 72.9 (18.6) APACHE II = Acute Physiology and Chronic Health Evaluation II; SCr min = minimum serum creatinine concentration; CrCl = creatinine clearance. Table II. Vancomycin therapy and changes in renal function. Renal Toxicity Renal Toxicity Variable Absent (n = 54) Present (n = 40) P Entire cohort (N = 94) Vancomycin trough, mean (SD), µg/ml 14.3 (6.7) 20.8 (9.9) <0.001 Vancomycin trough 15 µg/ml, no. (%) 22 (40.7) 27 (67.5) Duration of vancomycin 14 d, no. (%) 11 (20.4) 18 (45.0) 0.011, mean (SD), mg/dl 1.07 (0.44) 1.80 (0.96) <0.001 SCr change, mean (SD), mg/dl 0.13 (0.12) 0.85 (0.71) <0.001 Percent change in SCr, mean (SD) 15.9 (14.1) 88.9 (60.4) <0.001 CrCl minimum, mean (SD), ml/min 63.9 (26.1) 47.4 (19.6) CrCl change, mean (SD), ml/min 4.5 (6.6) 25.5 (17.0) <0.001 Percent change in CrCl, mean (SD) 6.9 (9.1) 34.8 (21.7) <0.001 Subgroup without vasopressor exposure (n = 80)* Vancomycin trough, mean (SD), µg/ml 14.4 (6.8) 20.4 (10.7) Vancomycin trough 15 µg/ml, no. (%) 21 (41.2) 18 (62.1) Duration of vancomycin 14 d, no. (%) 10 (19.6) 14 (48.3) SCr min, mean (SD), mg/dl 0.93 (0.40) 0.94 (0.49) 0.921, mean (SD), mg/dl 1.05 (0.41) 1.59 (0.83) <0.001 SCr change, mean (SD), mg/dl 0.12 (0.11) 0.65 (0.50) <0.001 Percent change in SCr, mean (SD) 15.6 (14.4) 71.7 (44.6) <0.001 CrCl minimum, mean (SD), ml/min 64.9 (26.5) 51.8 (20.2) CrCl change, mean (SD), ml/min 4.4 (6.7) 20.0 (14.9) <0.001 Percent change in CrCl, mean (SD) 6.6 (9.0) 28.0 (18.7) <0.001 = maximum serum creatinine concentration; CrCl = creatinine clearance; SCr min = minimum SCr. *51 Without renal toxicity, 29 with renal toxicity. June
6 Clinical Therapeutics Renal Toxicity (%) <15 P = >20 Vancomycin Serum Trough Concentration (µg/ml) Figure 2. Occurrence of renal toxicity, stratified by vancomycin steady-state serum trough concentrations. vancomycin therapy was found to be the only variable independently associated with the development of renal toxicity (adjusted odds ratio = 3.33; 95% CI, ; P = 0.039). DISCUSSION Our results suggest that aggressive vancomycin dosing, as determined by maximum measured vancomycin serum trough concentrations 15 µg/ml, and prolonged vancomycin administration may be associated with renal toxicity among patients treated for MRSA HCAP. Renal toxicity is reported to be a relatively infrequent complication of vancomycin administration, occurring in ~5% of patients, and is usually reversible. 17 Acute interstitial nephritis is a rare mechanism of action for the development of vancomycin-induced renal toxicity. 18 However, vancomycin appears to potentiate the renal toxicity of other pharmacologic agents, including aminoglycosides. 19 Cimino et al 10 evaluated 229 cancer patients treated with antibiotics. The incidence of renal toxicity was similar for patients receiving an aminoglycoside, vancomycin, or the combination of an aminoglycoside and vancomycin. However, the observed occurrence of renal toxicity was greatest among patients receiving vancomycin when serum trough concentrations were 10 µg/ml compared with <10 µg/ml (18.8% vs 0%, respectively; P = 0.032). Similarly, Rybak et al 11 found <10 µg/ml that the incidence of renal toxicity was greatest for patients treated concurrently with vancomycin and an aminoglycoside. Vancomycin serum trough concentrations >10 µg/ml and >21 days of vancomycin treatment have also been associated with the development of renal toxicity. A meta-analysis of vancomycin therapy reported similar findings. 20 The occurrence of health care associated infections attributed to MRSA has steadily increased over the past 15 years. 21 This has been correlated with a similar increase in the use of vancomycin. 22 However, there has also been an increase in vancomycin treatment failures in MRSA infections as a result of an upward drift in the minimum inhibitory concentrations of isolates and the presence of heteroresistant strains. 23,24 These observations, in conjunction with the poor lung tissue penetration of vancomycin, 2,3 have resulted in recommendations for increased dosing of vancomycin in MRSA HCAP to achieve serum trough concentrations of 15 to 20 µg/ml. 1 Unfortunately, this recommendation is not based on the findings of prospective clinical studies. Rello et al 25 evaluated 75 patients with microbiologically confirmed MRSA HCAP treated with glycopeptides either teicoplanin or vancomycin (dosed to achieve serum trough concentrations of 20 µg/ml) and 75 control patients without MRSA HCAP. Despite optimization of glycopeptide therapy, the crude mortality rate in these patients was 48%. Multivariate analysis revealed that a continuous infusion of vancomycin was associated with a reduced risk of mortality in the MRSA HCAP group (P < 0.05). More recently, Jeffres et al 5 evaluated 102 patients with BAL-confirmed MRSA HCAP (mortality rate, 31.4%). Mean (SD) vancomycin trough AUC values did not differ between survivors and nonsurvivors (351 [143] and 354 [109] µg h/ml, respectively). Stratification of vancomycin trough concentrations and AUC values yielded no relationship with hospital mortality. These authors found no evidence that greater vancomycin trough concentrations or AUC values were correlated with hospital outcome in the treatment of MRSA HCAP. Based on their results, they suggested that aggressive dosing strategies for vancomycin (eg, trough concentrations 15 µg/ml) may not offer any advantages in clinical efficacy over tradition Volume 29 Number 6
7 M.N. Jeffres et al. Table III. Process-of-care variables associated with renal function. Values are no. (%). Renal Toxicity Renal Toxicity Variable Absent (n = 54) Present (n = 40) P BUN:SCr >20 24 (44.4) 27 (67.5) IV contrast dye* 10 (18.5) 14 (35.0) Loop diuretic* 24 (44.4) 25 (62.5) Amphotericin B* 3 (5.6) 2 (5.0) Aminoglycoside* 3 (5.6) 5 (12.5) ACE-I or ARB* 11 (20.4) 8 (20.0) Cyclosporine or tacrolimus* 4 (7.4) 5 (12.5) Vasopressor 3 (5.6) 11 (27.5) BUN:SCr >20 = ratio of blood urea nitrogen to serum creatinine >20; ACE-I = angiotensin-converting enzyme inhibitor; ARB = angiotensin receptor blocker. *Received before attainment of maximum serum creatinine concentration. All aminoglycosides were administered for <72 hours for empiric coverage of gram-negative bacteria before availability of culture results. Received within 48 hours before. Table IV. Multivariate analysis of independent risk factors for renal toxicity.* Adusted Odds Variable Ratio 95% CI P IV contrast dye BUN:SCr ratio > Loop diuretic Aminoglycoside Duration of vancomycin 14 d APACHE II score (1-point increments) Vasopressor administration Vancomycin trough 15 µg/ml BUN:SCr >20 = ratio of blood urea nitrogen to serum creatinine >20; APACHE II = Acute Physiology and Chronic Health Evaluation II. *The listed variables were included in the logistic regression analysis. P = 0.631, Hosmer-Lemeshow goodnessof-fit test. al targets (5 15 µg/ml) and that alternative agents should be considered Our study has several important limitations. First, we studied only BAL-confirmed cases of MRSA HCAP; therefore, our results may not be applicable to patients in whom MRSA HCAP was diagnosed using other methods. Second, we cannot exclude the possibility that some undetermined confounding factor accounted for the observed increase in renal toxicity. Patients developing renal toxicity had a greater severity of illness, as measured by APACHE II scores. Additionally, patients developing renal toxicity were significantly more likely to require vasopressors, a marker of hypotension-induced acute tubular necrosis, and to have a greater incidence of administration of IV contrast dye and loop diuretics. Any of these factors could have contributed to the greater observed occurrence of renal toxicity. Larger, randomized, controlled, blinded studies are required to determine the occurrence of renal toxicity with higher targeted van- June
8 Clinical Therapeutics comycin trough concentrations among patient groups stratified by severity of illness. Third, although we compared changes in measured SCr and CrCl with baseline values obtained before the start of vancomycin treatment, we cannot exclude the possibility that renal dysfunction unrelated to vancomycin toxicity was responsible for elevations in both SCr and vancomycin trough concentrations in some patients. It is possible that higher vancomycin serum concentrations were markers of, rather than causative factors for, renal toxicity. Finally, because of the complexity of studying the relationship between vancomycin use and renal toxicity, the study results should be viewed as hypothesis generating rather than causality proving. CONCLUSION The results of this study suggest that aggressive vancomycin dosing, as determined by vancomycin serum trough concentrations 15 µg/ml, and prolonged administration of vancomycin may be associated with renal toxicity among patients treated for MRSA HCAP. ACKNOWLEDGMENT This work, including all analyses, was funded by Washington University and Barnes-Jewish Hospital. The authors have no conflicts of interest relative to this work. REFERENCES 1. American Thoracic Society and the Infectious Diseases Society of America. Guidelines for the management of adults with hospital-acquired, ventilator-associated, and healthcare-associated pneumonia. Am J Respir Crit Care Med. 2005;171: Lamer C, de Beco V, Soler P, et al. Analysis of vancomycin entry into pulmonary lining fluid by bronchoalveolar lavage in critically ill patients. Antimicrob Agents Chemother. 1993;37: Cruciani M, Gatti G, Lazzarini L, et al. Penetration of vancomycin into human lung tissue. J Antimicrob Chemother. 1996;38: DeRyke CA, Lodise TP Jr, Rybak MJ, McKinnon PS. Epidemiology, treatment, and outcomes of nosocomial bacteremic Staphylococcus aureus pneumonia. Chest. 2005; 128: Jeffres MN, Isakow W, Doherty JA, et al. Predictors of mortality for methicillin-resistant Staphylococcus aureus health-care associated pneumonia: Specific evaluation of vancomycin pharmacokinetic indices. Chest. 2006;130: Hidayat LK, Hsu DI, Quist R, et al. High-dose vancomycin therapy for methicillin-resistant Staphylococcus aureus infections: Efficacy and toxicity. Arch Intern Med. 2006;166: Geraci JE, Heilman FR, Nichols DR, Wellman WE. Antibiotic therapy of bacterial endocarditis. VII. Vancomycin for acute micrococcal endocarditis: Preliminary report. Mayo Clin Proc. 1958;33: Kralovicova K, Spanik S, Halko J, et al. Do vancomycin serum levels predict failures of vancomycin therapy or nephrotoxicity in cancer patients? J Chemother. 1997;9: Zimmermann AE, Katona BG, Plaisance KI. Association of vancomycin serum concentrations with outcomes in patients with gram-positive bacteremia. Pharmacotherapy. 1995;15: Cimino MA, Rotstein C, Slaughter RL, Emrich LJ. Relationship of serum antibiotic concentrations to nephrotoxicity in cancer patients receiving concurrent aminoglycoside and vancomycin therapy. Am J Med. 1987;83: Rybak MJ, Albrecht LM, Boike SC, Chandrasekar PH. Nephrotoxicity of vancomycin, alone and with aminoglycoside. J Antimicrob Chemother. 1990;25: Downs NJ, Neihart RE, Dolezal JM, Hodges GR. Mild nephrotoxicity associated with vancomycin use. Arch Intern Med. 1989;149: Elting LS, Rubenstein EB, Kurtin D, et al. Mississippi mud in the 1990s: Risks and outcomes of vancomycin-associated toxicity in general oncology practice. Cancer. 1998;83: Merten GJ, Burgess WP, Gray LV, et al. Prevention of contrast-induced nephropathy with sodium bicarbonate: A randomized controlled trial. JAMA. 2004;291: Moellering RC Jr, Krogstad DJ, Greenblatt DJ. Vancomycin therapy in patients with impaired renal function: A nomogram for dosage. Ann Intern Med. 1981;94: Concato J, Feinstein AR, Holford TR. The risk of determining risk with multivariable models. Ann Intern Med. 1993;118: Farber BF, Moellering RC Jr. Retrospective study of the toxicity of preparations of vancomycin from 1974 to Antimicrob Agents Chemother. 1983;23: Bergman MM, Glew RH, Ebert TH. Acute interstitial nephritis associated with vancomycin therapy. Arch Intern Med. 1988;148: Levine DP. Vancomycin: A history. Clin Infect Dis. 2006;42(Suppl 1):S5 S Goetz MB, Sayers J. Nephrotoxicity of vancomycin and aminoglycoside therapy separately and in combination [published correction appears in J Antimicrob Chemother. 1993;32:925]. J Antimicrob Chemother. 1993;32: Volume 29 Number 6
9 M.N. Jeffres et al. 21. Lowy FD. Antimicrobial resistance: The example of Staphylococcus aureus. J Clin Invest. 2003;111: Kirst HA, Thompson DG, Nicas TI. Historical yearly usage of vancomycin. Antimicrob Agents Chemother. 1998; 42: Sakoulas G, Moise-Broder PA, Schentag J, et al. Relationship of MIC and bactericidal activity to efficacy of vancomycin for treatment of methicillin-resistant Staphylococcus aureus bacteremia. J Clin Microbiol. 2004;42: Sakoulas G, Moellering RC Jr, Eliopoulos GM. Adaptation of methicillin-resistant Staphylococcus aureus in the face of vancomycin therapy. Clin Infect Dis. 2006;42(Suppl 1): S40 S Rello J, Sole-Violan J, Sa-Borges M, et al. Pneumonia caused by oxacillin-resistant Staphylococcus aureus treated with glycopeptides. Crit Care Med. 2005;33: Kollef MH, Rello J, Cammarata SK, et al. Clinical cure and survival in Gram-positive ventilator-associated pneumonia: Retrospective analysis of two double-blind studies comparing linezolid with vancomycin. Intensive Care Med. 2004;30: Livermore DM. Tigecycline: What is it, and where should it be used? J Antimicrob Chemother. 2005;56: Schmitt-Hoffmann A, Roos B, Schleimer M, et al. Single-dose pharmacokinetics and safety of a novel broad-spectrum cephalosporin (BAL5788) in healthy volunteers. Antimicrob Agents Chemother. 2004;48: Ellis MW, Lewis JS II. Treatment approaches for community-acquired methicillin-resistant Staphylococcus aureus infections. Curr Opin Infect Dis. 2005;18: Address correspondence to: Marin H. Kollef, MD, Washington University School of Medicine, 660 South Euclid Avenue, Campus Box 8052, St. Louis, MO mkollef@im.wustl.edu June
ORIGINAL ARTICLE DOI: (e) ISSN Online: (p) ISSN Print: Anand Kumar Singh 1, Poonam Verma 2. Sciences, Dehradun
 ORIGINAL ARTICLE CLINICAL ASSESSMENT OF NEPHROTOXICITY ASSOCIATED WITH VANCOMYCIN TROUGH CONCENTRATIONS DURING TREATMENT OF DEEP-SEATED INFECTIONS: A RETROSPECTIVE ANALYSIS Anand Kumar Singh 1, Poonam
ORIGINAL ARTICLE CLINICAL ASSESSMENT OF NEPHROTOXICITY ASSOCIATED WITH VANCOMYCIN TROUGH CONCENTRATIONS DURING TREATMENT OF DEEP-SEATED INFECTIONS: A RETROSPECTIVE ANALYSIS Anand Kumar Singh 1, Poonam
Katherine E. Kollef; Richard M. Reichley, RPh; Scott T. Micek, PharmD; and Marin H. Kollef, MD, FCCP
 CHEST Original Research The Modified Score Outperforms Curb65 Pneumonia Severity Score as a Predictor of 30-Day Mortality in Patients With Methicillin- Resistant Staphylococcus aureus Pneumonia* Katherine
CHEST Original Research The Modified Score Outperforms Curb65 Pneumonia Severity Score as a Predictor of 30-Day Mortality in Patients With Methicillin- Resistant Staphylococcus aureus Pneumonia* Katherine
Evaluation of Vancomycin Continuous Infusion in Trauma Patients
 OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
Nephrotoxicity. Pros and Cons of the article: Relationship between Initial Vancomycin
 Pros and Cons of the article: Relationship between Initial Vancomycin Nephrotoxicity among Hospitalized Patients Diane M. Cappelletty, Pharm.D. Associate Professor Pharmacy Practice The University of Toledo
Pros and Cons of the article: Relationship between Initial Vancomycin Nephrotoxicity among Hospitalized Patients Diane M. Cappelletty, Pharm.D. Associate Professor Pharmacy Practice The University of Toledo
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING
 EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
D DAVID PUBLISHING. Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within a Therapeutic Range. 1.
 Journal of Pharmacy and Pharmacology 2 (2014) 713-721 doi: 10.17265/2328-2150/2014.12.004 D DAVID PUBLISHING Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within
Journal of Pharmacy and Pharmacology 2 (2014) 713-721 doi: 10.17265/2328-2150/2014.12.004 D DAVID PUBLISHING Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within
CLINICAL USE OF GLYCOPEPTIDES. Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel
 CLINICAL USE OF GLYCOPEPTIDES Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel Glycopeptides Natural Vancomycin introduced in 1958 Teicoplanin introduced in Europe
CLINICAL USE OF GLYCOPEPTIDES Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel Glycopeptides Natural Vancomycin introduced in 1958 Teicoplanin introduced in Europe
VANCOMYCIN DOSING AND MONITORING GUIDELINES
 VANCOMYCIN DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee Approved: May 2017 GENERAL COMMENTS Vancomycin is a glycopeptide antibiotic with bactericidal
VANCOMYCIN DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee Approved: May 2017 GENERAL COMMENTS Vancomycin is a glycopeptide antibiotic with bactericidal
Clinical Guidelines for Use of Antibiotics. VANCOMYCIN (Adult)
 VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
D DAVID PUBLISHING. 1. Introduction. Kathryn Koliha 1, Julie Falk 1, Rachana Patel 1 and Karen Kier 2
 Journal of Pharmacy and Pharmacology 5 (2017) 607-615 doi: 10.17265/2328-2150/2017.09.001 D DAVID PUBLISHING Comparative Evaluation of Pharmacist-Managed Vancomycin Dosing in a Community Hospital Following
Journal of Pharmacy and Pharmacology 5 (2017) 607-615 doi: 10.17265/2328-2150/2017.09.001 D DAVID PUBLISHING Comparative Evaluation of Pharmacist-Managed Vancomycin Dosing in a Community Hospital Following
Challenges in Therapeutic Drug Monitoring:
 Challenges in Therapeutic Drug Monitoring: Focus on Vancomycin Pharmacodynamics and Pharmacokinetics Katherine Gallaga, PharmD PGY1 Pharmacy Practice Resident CHRISTUS Spohn Health System 1 Pharmacist
Challenges in Therapeutic Drug Monitoring: Focus on Vancomycin Pharmacodynamics and Pharmacokinetics Katherine Gallaga, PharmD PGY1 Pharmacy Practice Resident CHRISTUS Spohn Health System 1 Pharmacist
Clinical Study Prospective Trial of a Novel Nomogram to Achieve Updated Vancomycin Trough Concentrations
 Interdisciplinary Perspectives on Infectious Diseases Volume 2013, Article ID 839456, 8 pages http://dx.doi.org/10.1155/2013/839456 Clinical Study Prospective Trial of a Novel Nomogram to Achieve Updated
Interdisciplinary Perspectives on Infectious Diseases Volume 2013, Article ID 839456, 8 pages http://dx.doi.org/10.1155/2013/839456 Clinical Study Prospective Trial of a Novel Nomogram to Achieve Updated
Guidelines for Monitoring of Vancomycin Serum Concentrations in Adult Patients
 Guidelines for Monitoring of Vancomycin Serum Concentrations in Adult Patients Guidelines developed by UWHC Department of Pharmacy Author: Cindy Gaston, RPh, PharmD Reviewed by: Antimicrobial Subcommittee,
Guidelines for Monitoring of Vancomycin Serum Concentrations in Adult Patients Guidelines developed by UWHC Department of Pharmacy Author: Cindy Gaston, RPh, PharmD Reviewed by: Antimicrobial Subcommittee,
Abstract. Background. Editor: M. Grobusch
 ORIGINAL ARTICLE INFECTIOUS DISEASES Acute renal failure associated with vancomycin and b-lactams for the treatment of osteomyelitis in diabetics: piperacillin tazobactam as compared with cefepime R. P.
ORIGINAL ARTICLE INFECTIOUS DISEASES Acute renal failure associated with vancomycin and b-lactams for the treatment of osteomyelitis in diabetics: piperacillin tazobactam as compared with cefepime R. P.
Policy: Created: 2/11/2015; Approved: Adult Pharmacokinetic Dosing and Monitoring- Vancomycin Dosing
 ProMedica Health System Clinical Interdepartmental Policy and Procedure: Section: Policy: Date: Subject: Pharmacy Created: 2/11/2015; Approved: Adult Pharmacokinetic Dosing and Monitoring- Vancomycin Dosing
ProMedica Health System Clinical Interdepartmental Policy and Procedure: Section: Policy: Date: Subject: Pharmacy Created: 2/11/2015; Approved: Adult Pharmacokinetic Dosing and Monitoring- Vancomycin Dosing
ASHP Therapeutic Position Statements 623
 ASHP Therapeutic Position Statements 623 Therapeutic Monitoring of Vancomycin in Adult Patients: A Consensus Review of the American Society of Health-System Pharmacists, the Infectious Diseases Society
ASHP Therapeutic Position Statements 623 Therapeutic Monitoring of Vancomycin in Adult Patients: A Consensus Review of the American Society of Health-System Pharmacists, the Infectious Diseases Society
Clinical Therapeutics/Volume 35, Number 6, 2013 Antimicrobial Stewardship
 Clinical Therapeutics/Volume 35, Number 6, 2013 Antimicrobial Stewardship A Stewardship Program s Retrospective Evaluation of Vancomycin AUC 24 /MIC and Time to Microbiological Clearance in Patients with
Clinical Therapeutics/Volume 35, Number 6, 2013 Antimicrobial Stewardship A Stewardship Program s Retrospective Evaluation of Vancomycin AUC 24 /MIC and Time to Microbiological Clearance in Patients with
Continuous Infusion of Antibiotics In The ICU: What Is Proven? Professor of Medicine Vice-Chairman, Department of Medicine SUNY at Stony Brook
 Continuous Infusion of Antibiotics In The ICU: What Is Proven? Michael S. Niederman, M.D. Chairman, Department of Medicine Winthrop-University Hospital Mineola, NY Professor of Medicine Vice-Chairman,
Continuous Infusion of Antibiotics In The ICU: What Is Proven? Michael S. Niederman, M.D. Chairman, Department of Medicine Winthrop-University Hospital Mineola, NY Professor of Medicine Vice-Chairman,
Full title of guideline INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS. control
 Full title of guideline Author: Contact Name and Job Title Division and specialty Scope Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis) Changes
Full title of guideline Author: Contact Name and Job Title Division and specialty Scope Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis) Changes
Cystatin C: A New Approach to Improve Medication Dosing
 Cystatin C: A New Approach to Improve Medication Dosing Erin Frazee Barreto, PharmD, MSc, FCCM Assistant Professor of Pharmacy and Medicine Kern Scholar, Center for the Science of Health Care Delivery
Cystatin C: A New Approach to Improve Medication Dosing Erin Frazee Barreto, PharmD, MSc, FCCM Assistant Professor of Pharmacy and Medicine Kern Scholar, Center for the Science of Health Care Delivery
Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure
 Journal of Medical Microbiology (2016), 65, 195 199 DOI 10.1099/jmm.0.000211 Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure Michael A. Lorenz, 1,2 Ryan P. Moenster
Journal of Medical Microbiology (2016), 65, 195 199 DOI 10.1099/jmm.0.000211 Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure Michael A. Lorenz, 1,2 Ryan P. Moenster
Evaluation of Vancomycin Dosing and Corresponding Drug Concentrations in Pediatric Patients
 RESEARCH ARTICLE Evaluation of Vancomycin Dosing and Corresponding Drug Concentrations in Pediatric Patients abstract OBJECTIVE: To describe the relationships between dosing strategy, age, and vancomycin
RESEARCH ARTICLE Evaluation of Vancomycin Dosing and Corresponding Drug Concentrations in Pediatric Patients abstract OBJECTIVE: To describe the relationships between dosing strategy, age, and vancomycin
SBUH Aminoglycoside Dosing Protocol
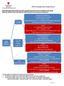 Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
Adult Inpatient Antibiogram. Antimicrobial Susceptibilities of Frequently Recovered Clinical Isolates. January to December 2016
 Adult Inpatient Antibiogram Antimicrobial Susceptibilities of Frequently Recovered Clinical Isolates January to December 2016 Department of Pathology Camille Hamula, PhD Director, Clinical Microbiology
Adult Inpatient Antibiogram Antimicrobial Susceptibilities of Frequently Recovered Clinical Isolates January to December 2016 Department of Pathology Camille Hamula, PhD Director, Clinical Microbiology
Guess or get it right?
 Guess or get it right? Antimicrobial prescribing in the 21 st century Robert Masterton Traditional Treatment Paradigm Conservative start with workhorse antibiotics Reserve more potent drugs for non-responders
Guess or get it right? Antimicrobial prescribing in the 21 st century Robert Masterton Traditional Treatment Paradigm Conservative start with workhorse antibiotics Reserve more potent drugs for non-responders
Cubicin A Guide to Dosing
 Cubicin A Guide to Dosing Cubicin (Daptomycin) powder for solution for injection or infusion Indications (see SmPC) 1 : Cubicin is indicated for the treatment of the following infections (see sections
Cubicin A Guide to Dosing Cubicin (Daptomycin) powder for solution for injection or infusion Indications (see SmPC) 1 : Cubicin is indicated for the treatment of the following infections (see sections
The Clinical Management of Hospital Acquired Pneumonia. NHS Ayrshire & Arran
 The Clinical Management of Hospital Acquired Pneumonia Dr R G Masterton NHS Ayrshire & Arran What s new in HAP/VAP? Care bundles MRSA VAP Improving outcomes with current antimicrobial New antimicrobials
The Clinical Management of Hospital Acquired Pneumonia Dr R G Masterton NHS Ayrshire & Arran What s new in HAP/VAP? Care bundles MRSA VAP Improving outcomes with current antimicrobial New antimicrobials
ICU Volume 11 - Issue 3 - Autumn Series
 ICU Volume 11 - Issue 3 - Autumn 2011 - Series Impact of Pharmacokinetics of Antibiotics in ICU Clinical Practice Introduction The efficacy of a drug is mainly dependent on its ability to achieve an effective
ICU Volume 11 - Issue 3 - Autumn 2011 - Series Impact of Pharmacokinetics of Antibiotics in ICU Clinical Practice Introduction The efficacy of a drug is mainly dependent on its ability to achieve an effective
TDM of Aminoglycoside Antibiotics
 TDM Lecture 3 5 th Stage TDM of Aminoglycoside Antibiotics The aminoglycoside antibiotics are widely used for the treatment of gram-negative infections, often in combination with a β-lactam antibiotic
TDM Lecture 3 5 th Stage TDM of Aminoglycoside Antibiotics The aminoglycoside antibiotics are widely used for the treatment of gram-negative infections, often in combination with a β-lactam antibiotic
MDR AGENTS: RISK FACTORS AND THERAPEUTIC STRATEGIES
 MDR AGENTS: RISK FACTORS AND THERAPEUTIC STRATEGIES 1 Marin H. Kollef, MD Professor of Medicine Virginia E. and Sam J. Golman Chair in Respiratory Intensive Care Medicine Washington University School of
MDR AGENTS: RISK FACTORS AND THERAPEUTIC STRATEGIES 1 Marin H. Kollef, MD Professor of Medicine Virginia E. and Sam J. Golman Chair in Respiratory Intensive Care Medicine Washington University School of
Trust Guideline for the Use of Parenteral Vancomycin and Teicoplanin in Adults
 A clinical guideline recommended for use: In: By: For: Division responsible for document: Key words: Names of document authors: Job titles of document authors: Name of document author s Line Manager: Job
A clinical guideline recommended for use: In: By: For: Division responsible for document: Key words: Names of document authors: Job titles of document authors: Name of document author s Line Manager: Job
Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center
 CA-MRSA Pneumonia Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center Professor of Clinical Medicine Weill Cornell
CA-MRSA Pneumonia Michael S. Niederman, M.D. Clinical Director Pulmonary and Critical Care Medicine New York Presbyterian Hospital Weill Cornell Medical Center Professor of Clinical Medicine Weill Cornell
Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia
 Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia Brandon Dionne, PharmD, BCPS, AAHIVP Assistant Clinical Professor Northeastern University Seth Housman, PharmD, MPA Clinical Assistant
Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia Brandon Dionne, PharmD, BCPS, AAHIVP Assistant Clinical Professor Northeastern University Seth Housman, PharmD, MPA Clinical Assistant
Adult Institutional Pharmacokinetics Protocol
 Adult Institutional Pharmacokinetics Protocol Policy Title: Clinical Pharmacokinetics (PK) Service Policy Policy Statement: It is the policy of UMHC that PK consult orders (for vancomycin or aminoglycosides)
Adult Institutional Pharmacokinetics Protocol Policy Title: Clinical Pharmacokinetics (PK) Service Policy Policy Statement: It is the policy of UMHC that PK consult orders (for vancomycin or aminoglycosides)
Counties in the top and bottom two quintiles of both diabetes and obesity, Age-adjusted percentage of adults aged 20 years who are obese, 2007
 Impact of Obesity on Medication Dosing John C. Williamson, PharmD, BCPS, AAHIVE Wake Forest University Baptist Medical Center Winston-Salem, NC Objectives Determine what constitutes the various forms of
Impact of Obesity on Medication Dosing John C. Williamson, PharmD, BCPS, AAHIVE Wake Forest University Baptist Medical Center Winston-Salem, NC Objectives Determine what constitutes the various forms of
Assessment of Therapeutic Drug Monitoring of Vancomycin in Elderly Patients According to New Guidelines
 Original Article Clinical Chemistry Ann Lab Med 2014;34:1-6 http://dx.doi.org/10.3343/alm.2014.34.1.1 ISSN 2234-3806 eissn 2234-3814 Assessment of Therapeutic Drug Monitoring of Vancomycin in Elderly Patients
Original Article Clinical Chemistry Ann Lab Med 2014;34:1-6 http://dx.doi.org/10.3343/alm.2014.34.1.1 ISSN 2234-3806 eissn 2234-3814 Assessment of Therapeutic Drug Monitoring of Vancomycin in Elderly Patients
Ping Liu 1, Blair Capitano 2, Amy Stein 3 and Ali A. El-Solh 4,5*
 Liu et al. BMC Nephrology (2017) 18:168 DOI 10.1186/s12882-017-0581-y RESEARCH ARTICLE Clinical outcomes of linezolid and vancomycin in patients with nosocomial pneumonia caused by methicillin-resistant
Liu et al. BMC Nephrology (2017) 18:168 DOI 10.1186/s12882-017-0581-y RESEARCH ARTICLE Clinical outcomes of linezolid and vancomycin in patients with nosocomial pneumonia caused by methicillin-resistant
The Pharmacokinetic and Pharmacodynamic Properties of Vancomycin
 SUPPLEMENT ARTICLE The Pharmacokinetic and Pharmacodynamic Properties of Vancomycin Michael J. Rybak Anti-Infective Research Laboratory, Department of Pharmacy Practice, College of Pharmacy and Health
SUPPLEMENT ARTICLE The Pharmacokinetic and Pharmacodynamic Properties of Vancomycin Michael J. Rybak Anti-Infective Research Laboratory, Department of Pharmacy Practice, College of Pharmacy and Health
Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients
 Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients Jan O Friedrich, MD DPhil Associate Professor of Medicine, University of Toronto Medical Director, MSICU St. Michael s Hospital,
Continuous vs Intermittent Dosing of Antibiotics in Critically-Ill Patients Jan O Friedrich, MD DPhil Associate Professor of Medicine, University of Toronto Medical Director, MSICU St. Michael s Hospital,
INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS
 Title of guideline (must include the word Guideline (not protocol, policy, procedure etc) INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS Author: Contact Name and Job Title
Title of guideline (must include the word Guideline (not protocol, policy, procedure etc) INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS Author: Contact Name and Job Title
(Max 2 g) = to nearest 250 mg
 Appendix 1 (part 1 of 8): Rubric for competency assessment of pharmacists prescribing and managing vancomycin Empiric Dosing Phase Pts Yes No Data Error OP Did the pharmacist document the indication 2
Appendix 1 (part 1 of 8): Rubric for competency assessment of pharmacists prescribing and managing vancomycin Empiric Dosing Phase Pts Yes No Data Error OP Did the pharmacist document the indication 2
Daptomycin in Clinical Practice. Paolo Grossi
 Clinica delle Malattie Infettive e Tropicali Università degli Studi dell Insubria Ospedale di Circolo e Fondazione Macchi, Varese Second Opinion Infettivologica Centro Nazionale Trapianti, ISS, Roma Daptomycin
Clinica delle Malattie Infettive e Tropicali Università degli Studi dell Insubria Ospedale di Circolo e Fondazione Macchi, Varese Second Opinion Infettivologica Centro Nazionale Trapianti, ISS, Roma Daptomycin
Optimized Use of Vancomycin
 E-Newsletter #1 Optimized Use of Vancomycin FROM THE EDITOR S DESK Methicillin-resistant Staphylococcus aureus (MRSA) is a serious concern for clinicians managing infectious diseases in the healthcare
E-Newsletter #1 Optimized Use of Vancomycin FROM THE EDITOR S DESK Methicillin-resistant Staphylococcus aureus (MRSA) is a serious concern for clinicians managing infectious diseases in the healthcare
Pharmacologyonline 1: (2010) ewsletter Singh and Kochbar. Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of
 Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of Cefoperazone Sulbactam Singh M*, Kochhar P* Medical & Research Division, Pfizer India. Summary Antimicrobial resistance is associated with
Optimizing Pharmacokinetic/Pharmacodynamics Principles & Role of Cefoperazone Sulbactam Singh M*, Kochhar P* Medical & Research Division, Pfizer India. Summary Antimicrobial resistance is associated with
without the permission of the author Not to be copied and distributed to others
 Emperor s Castle interior-prato What is the Role of Inhaled Polymyxins for Treatment of Respiratory Tract Infections? Helen Giamarellou CONCLUSIONS: Patients with Pseudomonas and Acinetobacter VAP may
Emperor s Castle interior-prato What is the Role of Inhaled Polymyxins for Treatment of Respiratory Tract Infections? Helen Giamarellou CONCLUSIONS: Patients with Pseudomonas and Acinetobacter VAP may
Vancomycin dosing in morbidly obese patients
 Eur J Clin Pharmacol (1998) 54: 621±625 Ó Springer-Verlag 1998 PHARMACOKINETICS AND DISPOSITION L. A. Bauer á D. J. Black á J. S. Lill Vancomycin dosing in morbidly obese patients Received: 9 March 1998
Eur J Clin Pharmacol (1998) 54: 621±625 Ó Springer-Verlag 1998 PHARMACOKINETICS AND DISPOSITION L. A. Bauer á D. J. Black á J. S. Lill Vancomycin dosing in morbidly obese patients Received: 9 March 1998
Supplementary Data. Supplementary Table S2. Antiretroviral Therapies Taken with Ledipasvir/Sofosbuvir
 Supplementary Data Statistical Analysis Due to the limited number of patients with acute kidney injury and concern for model overfitting, covariates included in multivariable logistic regression analyses
Supplementary Data Statistical Analysis Due to the limited number of patients with acute kidney injury and concern for model overfitting, covariates included in multivariable logistic regression analyses
Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches
 Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ. Disclosures I have served as a consultant to, researcher/investigator
Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ. Disclosures I have served as a consultant to, researcher/investigator
Original Article Mahidol Univ J Pharm Sci 2015; 42 (4), MT. Nguyen 1, TD. Dang Nguyen 1* 1
 Original Article Mahidol Univ J Pharm Sci 2015; 42 (4), 195-202 Investigation on hospital-acquired pneumonia and the association between hospital-acquired pneumonia and chronic comorbidity at the Department
Original Article Mahidol Univ J Pharm Sci 2015; 42 (4), 195-202 Investigation on hospital-acquired pneumonia and the association between hospital-acquired pneumonia and chronic comorbidity at the Department
PHA5128 Dose Optimization II Case Study 3 Spring 2013
 Use the vancomycin dosing nomogram table below: A female patient, 57 years of age, 5 6 in height and 100 in weight had an infection requiring vancomycin treatment. Her serum creatinine was 0.8 mg/d. What
Use the vancomycin dosing nomogram table below: A female patient, 57 years of age, 5 6 in height and 100 in weight had an infection requiring vancomycin treatment. Her serum creatinine was 0.8 mg/d. What
MRSA Micro Scan Pos Combo 6J DADE BEHRING VCM
 PKPD MRSA 1 1 2 1 1 2 17 1 26 17 3 16 vancomycinvcm methicillin-resistant Staphylococcus aureusmrsa 31 pharmacokineticpkparameter retrospective VCM 21 10 PK parameter Mann- Whitney U-test Cmax 37.1 µ gml29.942
PKPD MRSA 1 1 2 1 1 2 17 1 26 17 3 16 vancomycinvcm methicillin-resistant Staphylococcus aureusmrsa 31 pharmacokineticpkparameter retrospective VCM 21 10 PK parameter Mann- Whitney U-test Cmax 37.1 µ gml29.942
Aminoglycosides John A. Bosso, Pharm.D.
 AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
Clinical Safety & Effectiveness Cohort # 10
 1 Clinical Safety & Effectiveness Cohort # 10 Improving Weight-Based Vancomycin Dosing and Monitoring DATE Educating for Quality Improvement & Patient Safety 2 Financial Disclosure lizabeth A. Walter,
1 Clinical Safety & Effectiveness Cohort # 10 Improving Weight-Based Vancomycin Dosing and Monitoring DATE Educating for Quality Improvement & Patient Safety 2 Financial Disclosure lizabeth A. Walter,
Joint Trust Guideline for the Use of Intravenous Vancomycin in Paediatrics
 A clinical guideline recommended For use in: All clinical areas where vancomycin is prescribed for Children aged 1 month to 16 years By: All medical, nursing, pharmacy, microbiology and phlebotomy paediatric
A clinical guideline recommended For use in: All clinical areas where vancomycin is prescribed for Children aged 1 month to 16 years By: All medical, nursing, pharmacy, microbiology and phlebotomy paediatric
La farmacologia in aiuto
 Ferrara, 15 giugno 2018 La farmacologia in aiuto Pier Giorgio Cojutti, Federico Pea Istituto di Farmacologia Clinica Azienda Sanitaria Universitaria Integrata di Udine Therapeutic Drug Monitoring of Beta-Lactams
Ferrara, 15 giugno 2018 La farmacologia in aiuto Pier Giorgio Cojutti, Federico Pea Istituto di Farmacologia Clinica Azienda Sanitaria Universitaria Integrata di Udine Therapeutic Drug Monitoring of Beta-Lactams
Mortality Rate was unsightly!!! 4/24/2013. Sepsis Quality Improvement Project
 Libby, MT Sepsis Quality Improvement Project Barb Dumont RN, Director of Quality and Risk Management Mike Julius RN, ED Manager Cathy Wolfe RN, Chief Nursing Officer. Mortality Rate was unsightly!!! percent
Libby, MT Sepsis Quality Improvement Project Barb Dumont RN, Director of Quality and Risk Management Mike Julius RN, ED Manager Cathy Wolfe RN, Chief Nursing Officer. Mortality Rate was unsightly!!! percent
HEALTHCARE-ASSOCIATED PNEUMONIA: DIAGNOSIS, TREATMENT & PREVENTION
 HEALTHCARE-ASSOCIATED PNEUMONIA: DIAGNOSIS, TREATMENT & PREVENTION David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health Care Medical
HEALTHCARE-ASSOCIATED PNEUMONIA: DIAGNOSIS, TREATMENT & PREVENTION David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health Care Medical
Lessons from recent studies. João Gonçalves Pereira UCIP DALI
 Lessons from recent studies João Gonçalves Pereira UCIP DALI 1 Patterns of Antimicrobial Activity Concentration C max Aminoglycosides Cmax/MIC>10 Metronidazol Area under the concentration curve Azithromycin
Lessons from recent studies João Gonçalves Pereira UCIP DALI 1 Patterns of Antimicrobial Activity Concentration C max Aminoglycosides Cmax/MIC>10 Metronidazol Area under the concentration curve Azithromycin
Daily vancomycin dose requirements as a continuous infusion in obese versus non-obese SICU patients
 Lin et al. Critical Care (1) :5 DOI 1.11/s15-1-1-9 RESEARCH Daily vancomycin dose requirements as a continuous infusion in obese versus non-obese SICU patients Hsin Lin 1*, Daniel Dante Yeh and Alexander
Lin et al. Critical Care (1) :5 DOI 1.11/s15-1-1-9 RESEARCH Daily vancomycin dose requirements as a continuous infusion in obese versus non-obese SICU patients Hsin Lin 1*, Daniel Dante Yeh and Alexander
Potential Conflicts of Interests
 Potential Conflicts of Interests Research Grants Agency for Healthcare Research and Quality Akers Bioscience, Inc. Pfizer, Inc. Scientific Advisory Boards Pfizer, Inc. Cadence Pharmaceuticals Kimberly
Potential Conflicts of Interests Research Grants Agency for Healthcare Research and Quality Akers Bioscience, Inc. Pfizer, Inc. Scientific Advisory Boards Pfizer, Inc. Cadence Pharmaceuticals Kimberly
PHA Spring First Exam. 8 Aminoglycosides (5 points)
 PHA 5128 Spring 2012 First Exam 1 Aminoglycosides (5 points) 2 Aminoglycosides (10 points) 3 Basic Principles (5 points) 4 Basic Principles (5 points) 5 Bioavailability (5 points) 6 Vancomycin (5 points)
PHA 5128 Spring 2012 First Exam 1 Aminoglycosides (5 points) 2 Aminoglycosides (10 points) 3 Basic Principles (5 points) 4 Basic Principles (5 points) 5 Bioavailability (5 points) 6 Vancomycin (5 points)
Vancomycin-associated nephrotoxicity, a case control study
 Master Thesis in Medicine, Nr 859 Vancomycin-associated nephrotoxicity, a case control study Student Tutor Pr. Thierry Buclin, PD MER Div. of Clinical Pharmacology, CHUV Co-tutor Nicolas Widmer Div. of
Master Thesis in Medicine, Nr 859 Vancomycin-associated nephrotoxicity, a case control study Student Tutor Pr. Thierry Buclin, PD MER Div. of Clinical Pharmacology, CHUV Co-tutor Nicolas Widmer Div. of
PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS
 PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS SITI HIR HURAIZAH MD TAHIR Bpharm (UKM), MSc (Clinical Microbiology) (UoN) CLINICAL PHARMACIST HOSPITAL MELAKA WHY STUDY PHARMACOKINETICS (PK) AND PHARMACODYNAMICS
PHARMACOKINETIC & PHARMACODYNAMIC OF ANTIBIOTICS SITI HIR HURAIZAH MD TAHIR Bpharm (UKM), MSc (Clinical Microbiology) (UoN) CLINICAL PHARMACIST HOSPITAL MELAKA WHY STUDY PHARMACOKINETICS (PK) AND PHARMACODYNAMICS
ESCMID Online Lecture Library. by author
 Hospital Universitario Virgen Macarena, Seville New drugs against MRSA and VRE L. Eduardo López Cortés Seville, 8th July Tedizolid Oxazolidinone Ceftaroline // Ceftobiprole 5 th gen cephalosporin Overview
Hospital Universitario Virgen Macarena, Seville New drugs against MRSA and VRE L. Eduardo López Cortés Seville, 8th July Tedizolid Oxazolidinone Ceftaroline // Ceftobiprole 5 th gen cephalosporin Overview
Inadequate Empiric Antibiotic Therapy among Canadian. Hospitalized Solid-Organ Transplant Patients: Incidence and Impact on Hospital Mortality
 Inadequate Empiric Antibiotic Therapy among Canadian Hospitalized Solid-Organ Transplant Patients: Incidence and Impact on Hospital Mortality by Bassem Hamandi A thesis submitted in conformity with the
Inadequate Empiric Antibiotic Therapy among Canadian Hospitalized Solid-Organ Transplant Patients: Incidence and Impact on Hospital Mortality by Bassem Hamandi A thesis submitted in conformity with the
Consequences for the clinicians
 30th Symposium : What will change in your daily practice with the new Elewijt, 26-05-2008 EUCAST breakpoints for antibiotic susceptibility testing Consequences for the clinicians Y.Van Laethem,MD CHU St
30th Symposium : What will change in your daily practice with the new Elewijt, 26-05-2008 EUCAST breakpoints for antibiotic susceptibility testing Consequences for the clinicians Y.Van Laethem,MD CHU St
Searching for Clues in Infectious Diseases
 Disclosure Searching for Clues in Infectious Diseases The speaker has no financial conflicts to disclose as relates to the content of this presentation John Esterly, PharmD, BCPS Northwestern Memorial
Disclosure Searching for Clues in Infectious Diseases The speaker has no financial conflicts to disclose as relates to the content of this presentation John Esterly, PharmD, BCPS Northwestern Memorial
ISSUES OF THE OBESE DOSING. Janine Then, PharmD, BCPS
 ISSUES OF THE OBESE CRITICAL CARE PATIENT: DOSING Janine Then, PharmD, BCPS Learning Objectives Recognize potential limitations of some routes of administration Determine optimal dosing for anticoagulation
ISSUES OF THE OBESE CRITICAL CARE PATIENT: DOSING Janine Then, PharmD, BCPS Learning Objectives Recognize potential limitations of some routes of administration Determine optimal dosing for anticoagulation
Community Acquired & Nosocomial Pneumonias
 Community Acquired & Nosocomial Pneumonias IDSA/ATS 2007 & 2016 Guidelines José Luis González, MD Clinical Assistant Professor of Medicine Outline Intro - Definitions & Diagnosing CAP treatment VAP & HAP
Community Acquired & Nosocomial Pneumonias IDSA/ATS 2007 & 2016 Guidelines José Luis González, MD Clinical Assistant Professor of Medicine Outline Intro - Definitions & Diagnosing CAP treatment VAP & HAP
THE AMINOGLYCOSIDE ANTIBIOTICS
 4 THE AMINOGLYCOSIDE ANTIBIOTICS INTRODUCTION The aminoglycoside antibiotics are widely used for the treatment of severe gram-negative infections such as pneumonia or bacteremia, often in combination with
4 THE AMINOGLYCOSIDE ANTIBIOTICS INTRODUCTION The aminoglycoside antibiotics are widely used for the treatment of severe gram-negative infections such as pneumonia or bacteremia, often in combination with
The association between vancomycin trough concentrations and acute kidney injury in the neonatal intensive care unit
 Bhargava et al. BMC Pediatrics (2017) 17:50 DOI 10.1186/s12887-017-0777-0 RESEARCH ARTICLE Open Access The association between vancomycin trough concentrations and acute kidney injury in the neonatal intensive
Bhargava et al. BMC Pediatrics (2017) 17:50 DOI 10.1186/s12887-017-0777-0 RESEARCH ARTICLE Open Access The association between vancomycin trough concentrations and acute kidney injury in the neonatal intensive
IH Pharmacy Live Rounds
 IH Pharmacy Live Rounds Effect of Vancomycin plus Rifampicin in the Treatment of Nosocomial Methicillin-resistant Staphylococcus aureus Pneumonia Sandra Katalinic, Pharmacy Resident Kelowna General Hospital
IH Pharmacy Live Rounds Effect of Vancomycin plus Rifampicin in the Treatment of Nosocomial Methicillin-resistant Staphylococcus aureus Pneumonia Sandra Katalinic, Pharmacy Resident Kelowna General Hospital
Use ideal body weight (IBW) unless actual body weight is less. Use the following equation to calculate IBW:
 Amikacin is a partially restricted (amber) antibiotic for the treatment of infections due to gentamicin resistant Gram negative bacilli or as advised by microbiology. As with other aminoglycosides, therapeutic
Amikacin is a partially restricted (amber) antibiotic for the treatment of infections due to gentamicin resistant Gram negative bacilli or as advised by microbiology. As with other aminoglycosides, therapeutic
Vancomycin Drug Class 1
 Drug Class 1 Antibiotic glycopeptide Spectrum 1 Cross Sensitivities / Allergies 1 Refer to product monograph for complete spectrum Gram positive pathogens (e.g., S. aureus, Enterococcus, S. viridans, methicillinresistant
Drug Class 1 Antibiotic glycopeptide Spectrum 1 Cross Sensitivities / Allergies 1 Refer to product monograph for complete spectrum Gram positive pathogens (e.g., S. aureus, Enterococcus, S. viridans, methicillinresistant
Received 24 August 2010/Returned for modification 7 November 2010/Accepted 7 February 2011
 JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 2011, p. 1583 1587 Vol. 49, No. 4 0095-1137/11/$12.00 doi:10.1128/jcm.01719-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Clinical and
JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 2011, p. 1583 1587 Vol. 49, No. 4 0095-1137/11/$12.00 doi:10.1128/jcm.01719-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Clinical and
IMPROVING VANCOMYCIN DOSING AND MONITORING IN THE ABSENCE OF A FORMAL PHARMACOKINETIC SERVICE:
 IMPROVING VANCOMYCIN DOSING AND MONITORING IN THE ABSENCE OF A FORMAL PHARMACOKINETIC SERVICE: IMPACT OF A PHARMACY DEPARTMENT-WIDE APPROACH IN A COMMUNITY HOSPITAL SETTING November 2014 Monica Dorobisz,
IMPROVING VANCOMYCIN DOSING AND MONITORING IN THE ABSENCE OF A FORMAL PHARMACOKINETIC SERVICE: IMPACT OF A PHARMACY DEPARTMENT-WIDE APPROACH IN A COMMUNITY HOSPITAL SETTING November 2014 Monica Dorobisz,
Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more)
 Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more) Christian Eckmann Antibiotic Stewardship Expert ECDC Chief of Staff Department of General, Visceral and Thoracic Surgery Klinikum
Skin and soft tissue (SSTI) sepsis (surgery, antimicrobial therapy and more) Christian Eckmann Antibiotic Stewardship Expert ECDC Chief of Staff Department of General, Visceral and Thoracic Surgery Klinikum
SHC Vancomycin Dosing Guide
 SHC Vancomycin Dosing Guide A: Initial dosing considerations B. Pharmacodynamic Targets: goal AUC and troughs C. Loading dose D: Initial Vancomycin Maintenance Dosing and Serum Concentration Monitoring
SHC Vancomycin Dosing Guide A: Initial dosing considerations B. Pharmacodynamic Targets: goal AUC and troughs C. Loading dose D: Initial Vancomycin Maintenance Dosing and Serum Concentration Monitoring
Relationship of MIC and Bactericidal Activity to Efficacy of Vancomycin for Treatment of Methicillin-Resistant Staphylococcus aureus Bacteremia
 JOURNAL OF CLINICAL MICROBIOLOGY, June 2004, p. 2398 2402 Vol. 42, No. 6 0095-1137/04/$08.00 0 DOI: 10.1128/JCM.42.6.2398 2402.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved.
JOURNAL OF CLINICAL MICROBIOLOGY, June 2004, p. 2398 2402 Vol. 42, No. 6 0095-1137/04/$08.00 0 DOI: 10.1128/JCM.42.6.2398 2402.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved.
Comparison of Omadacycline and Tigecycline Pharmacodynamics in the Plasma, Epithelial Lining Fluid, and Alveolar Macrophages in Healthy Subjects
 Comparison of Omadacycline and Tigecycline Pharmacodynamics in the Plasma, Epithelial Lining Fluid, and Alveolar Macrophages in Healthy Subjects Karolyn S. Horn, Mark H. Gotfried, Judith N. Steenbergen,
Comparison of Omadacycline and Tigecycline Pharmacodynamics in the Plasma, Epithelial Lining Fluid, and Alveolar Macrophages in Healthy Subjects Karolyn S. Horn, Mark H. Gotfried, Judith N. Steenbergen,
Pneumonia Community-Acquired Healthcare-Associated
 Pneumonia Community-Acquired Healthcare-Associated Edwin Yu Clin Infect Dis 2007;44(S2):27-72 Am J Respir Crit Care Med 2005; 171:388-416 IDSA / ATS Guidelines Microbiology Principles and Practice of Infectious
Pneumonia Community-Acquired Healthcare-Associated Edwin Yu Clin Infect Dis 2007;44(S2):27-72 Am J Respir Crit Care Med 2005; 171:388-416 IDSA / ATS Guidelines Microbiology Principles and Practice of Infectious
Augmented Renal Clearance: Let s Get the Discussion Flowing
 Augmented Renal Clearance: Let s Get the Discussion Flowing Terry Makhoul, PharmD PGY-2 Emergency Medicine Pharmacy Resident University of Rochester Medical Center Strong Memorial Hospital Disclosures
Augmented Renal Clearance: Let s Get the Discussion Flowing Terry Makhoul, PharmD PGY-2 Emergency Medicine Pharmacy Resident University of Rochester Medical Center Strong Memorial Hospital Disclosures
Vancomycin Pharmacokinetics. Myrna Y. Munar, Pharm.D., BCPS Associate Professor of Pharmacy
 Vancomycin Pharmacokinetics Myrna Y. Munar, Pharm.D., BCPS Associate Professor of Pharmacy Goals Review the PK properties of vancomycin Compare and contrast methods of dosage regimen design for vancomycin
Vancomycin Pharmacokinetics Myrna Y. Munar, Pharm.D., BCPS Associate Professor of Pharmacy Goals Review the PK properties of vancomycin Compare and contrast methods of dosage regimen design for vancomycin
HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY
 HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health
HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health
Diagnosis of Ventilator- Associated Pneumonia: Where are we now?
 Diagnosis of Ventilator- Associated Pneumonia: Where are we now? Gary French Guy s & St. Thomas Hospital & King s College, London BSAC Guideline 2008 Masterton R, Galloway A, French G, Street M, Armstrong
Diagnosis of Ventilator- Associated Pneumonia: Where are we now? Gary French Guy s & St. Thomas Hospital & King s College, London BSAC Guideline 2008 Masterton R, Galloway A, French G, Street M, Armstrong
NHS Grampian Staff Guidance for the Administration of Intravenous Vancomycin in Adults via Intermittent (pulsed) Infusion
 Acute Sector NHS Grampian Staff Guidance for the Administration of Intravenous Vancomycin in Adults via Intermittent (pulsed) Infusion Co-ordinators: Gillian Macartney Fiona McDonald Specialist Antibiotic
Acute Sector NHS Grampian Staff Guidance for the Administration of Intravenous Vancomycin in Adults via Intermittent (pulsed) Infusion Co-ordinators: Gillian Macartney Fiona McDonald Specialist Antibiotic
AMINOGLYCOSIDES DOSING AND MONITORING GUIDELINES
 Approved: September 2017 AMINOGLYCOSIDES DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee GENERAL COMMENTS Aminoglycosides (AG) include gentamicin,
Approved: September 2017 AMINOGLYCOSIDES DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee GENERAL COMMENTS Aminoglycosides (AG) include gentamicin,
Vancomycin Pharmacokinetics in Normal and Morbidly Obese Subjects
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 1982, p. 575-58 66484/82/4575-6$2./ Vol. 21, No. 4 Vancomycin Pharmacokinetics in Normal and Morbidly Obese Subjects ROBERT A. BLOUIN,1 LARRY A. BAUER,3* DELWYN
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 1982, p. 575-58 66484/82/4575-6$2./ Vol. 21, No. 4 Vancomycin Pharmacokinetics in Normal and Morbidly Obese Subjects ROBERT A. BLOUIN,1 LARRY A. BAUER,3* DELWYN
Title: Incidence and predictors of nephrotoxicity associated with intravenous colistin in overweight and obese patients
 AAC Accepts, published online ahead of print on 27 February 2012 Antimicrob. Agents Chemother. doi:10.1128/aac.00028-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 TITLE PAGE
AAC Accepts, published online ahead of print on 27 February 2012 Antimicrob. Agents Chemother. doi:10.1128/aac.00028-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 TITLE PAGE
Methicillin-Resistant Staphylococcus aureus (MRSA) S urveillance Report 2008 Background Methods
 Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance Report 2008 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services
Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance Report 2008 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services
Supplementary Online Content
 Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
prophylaxis for endocarditis in patients at high risk prophylaxis for major surgical procedures
 1 Glycopeptides appropriate uses serious infections due to beta-lactam- resistant gram-positive microorganisms infections due to gram-positive microorganisms in patients with serious allergy to beta-lactam
1 Glycopeptides appropriate uses serious infections due to beta-lactam- resistant gram-positive microorganisms infections due to gram-positive microorganisms in patients with serious allergy to beta-lactam
Elevated Vancomycin Trough Concentration: Increased Efficacy and/or Toxicity?
 Iranian Journal of Pharmaceutical Research (2014), 13 (4): 1241-1247 Received: June 2013 Accepted: November 2013 Copyright 2014 by School of Pharmacy Shaheed Beheshti University of Medical Sciences and
Iranian Journal of Pharmaceutical Research (2014), 13 (4): 1241-1247 Received: June 2013 Accepted: November 2013 Copyright 2014 by School of Pharmacy Shaheed Beheshti University of Medical Sciences and
Vancomycin: A 50-something-yearold antibiotic we still don t understand
 Current Drug Therapy CME CREDIT EDUCATIONAL OBJECTIVES: Readers will use vancomycin appropriately Amy Schilling, PharmD Department of Pharmacy, The University of Texas Medical Branch, Galveston Elizabeth
Current Drug Therapy CME CREDIT EDUCATIONAL OBJECTIVES: Readers will use vancomycin appropriately Amy Schilling, PharmD Department of Pharmacy, The University of Texas Medical Branch, Galveston Elizabeth
(telavancin) Healthcare Professional s Guide. Version 2, 4 November 2014
 VIBATIV (telavancin) Healthcare Professional s Guide Version 2, 4 November 2014 1 Table of Contents Introduction... 3 About Vibativ / Therapeutic indications... 3 Antimicrobial spectrum of activity for
VIBATIV (telavancin) Healthcare Professional s Guide Version 2, 4 November 2014 1 Table of Contents Introduction... 3 About Vibativ / Therapeutic indications... 3 Antimicrobial spectrum of activity for
CAT. Dosisaanpassing van antibiotica, toepasbaarheid van beschikbare calculators. Apr. Glynis Frans Supervisor: Prof. Apr.
 CAT Dosisaanpassing van antibiotica, toepasbaarheid van beschikbare calculators Apr. Glynis Frans Supervisor: Prof. Apr. Katrien Lagrou 1. What are the current guidelines and recommendations on TDM for
CAT Dosisaanpassing van antibiotica, toepasbaarheid van beschikbare calculators Apr. Glynis Frans Supervisor: Prof. Apr. Katrien Lagrou 1. What are the current guidelines and recommendations on TDM for
Disclosures. Efficacy of the drug. Optimizing Dosing Based on PKPD- An overview. Dose Finding - The Past
 Disclosures Optimizing Dosing Based on PKPD- An overview Johan W. Mouton MD PhD FIDSA FAAM Professor pharmacokinetics and pharmacodynamics Research grants advisory boards speaker This Patient Needs Antibiotics.
Disclosures Optimizing Dosing Based on PKPD- An overview Johan W. Mouton MD PhD FIDSA FAAM Professor pharmacokinetics and pharmacodynamics Research grants advisory boards speaker This Patient Needs Antibiotics.
Supplementary Online Content
 Supplementary Online Content Torres A, Sibila O, Ferrer M, et al. Effect of corticosteroids on treatment failure among hospitalized patients with severe community-acquired pneumonia and high inflammatory
Supplementary Online Content Torres A, Sibila O, Ferrer M, et al. Effect of corticosteroids on treatment failure among hospitalized patients with severe community-acquired pneumonia and high inflammatory
Care Guideline DRAFT for review cycle 08/02/17 CARE OF THE ADULT PNEUMONIA PATIENT
 Care Guideline DRAFT for review cycle 08/02/17 CARE OF THE ADULT PNEUMONIA PATIENT Target Audience: All MHS employed providers within Primary Care, Urgent Care, and In-Hospital Care. The secondary audience
Care Guideline DRAFT for review cycle 08/02/17 CARE OF THE ADULT PNEUMONIA PATIENT Target Audience: All MHS employed providers within Primary Care, Urgent Care, and In-Hospital Care. The secondary audience
The antibiotic dose and the obese ICU patient
 The antibiotic dose and the obese ICU patient Philippe Montravers, M.D., Ph.D. Anaesthesia and Surgical ICU CHU Bichat Claude Bernard Assistance Publique-Hôpitaux de Paris INSERM UMR 1152 University Paris
The antibiotic dose and the obese ICU patient Philippe Montravers, M.D., Ph.D. Anaesthesia and Surgical ICU CHU Bichat Claude Bernard Assistance Publique-Hôpitaux de Paris INSERM UMR 1152 University Paris
