Comparative Effectiveness of Linezolid and Vancomycin among a National Cohort of Patients Infected with Methicillin-Resistant Staphylococcus aureus
|
|
|
- William Johns
- 5 years ago
- Views:
Transcription
1 University of Rhode Island Pharmacy Practice Faculty Publications Pharmacy Practice 2010 Comparative Effectiveness of Linezolid and Vancomycin among a National Cohort of Patients Infected with Methicillin-Resistant Staphylococcus aureus Aisling R. Caffrey University of Rhode Island, aisling_caffrey@uri.edu Brian J. Quilliam bquilliam@uri.edu See next page for additional authors Follow this and additional works at: Terms of Use All rights reserved under copyright. Citation/Publisher Attribution Caffrey, Aisling R., Brian J. Quilliam and Kerry L. LaPlante "Comparative Effectiveness of Linezolid and Vancomycin Among a National Cohort of Patients Infected With Methicillin-Resistant Staphylococcus aureus." Antimicrobial Agents and Chemotherapy. 54(10): Available at: This Article is brought to you for free and open access by the Pharmacy Practice at DigitalCommons@URI. It has been accepted for inclusion in Pharmacy Practice Faculty Publications by an authorized administrator of DigitalCommons@URI. For more information, please contact digitalcommons@etal.uri.edu.
2 Authors Aisling R. Caffrey, Brian J. Quilliam, and Kerry L. LaPlante PharmD This article is available at
3 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 2010, p Vol. 54, No /10/$12.00 doi: /aac Copyright 2010, American Society for Microbiology. All Rights Reserved. Comparative Effectiveness of Linezolid and Vancomycin among a National Cohort of Patients Infected with Methicillin-Resistant Staphylococcus aureus Aisling R. Caffrey, 1,2 Brian J. Quilliam, 2 and Kerry L. LaPlante 1,2,3 * Veterans Affairs Medical Center, Infectious Diseases Research Program, Providence, Rhode Island 1 ; University of Rhode Island, Department of Pharmacy Practice, Kingston, Rhode Island 2 ; and Warren Alpert Medical School of Brown University, Division of Infectious Diseases, Providence, Rhode Island 3 Received 12 February 2010/Returned for modification 30 April 2010/Accepted 21 July 2010 While newer antibiotics play a key role in treating methicillin-resistant Staphylococcus aureus (MRSA) infections, knowledge of their real-world clinical impact is limited. We sought to quantify the effectiveness of linezolid compared to that of vancomycin among MRSA-infected patients. This national retrospective cohort study included adult patients admitted to all Veterans Affairs hospitals between January 2002 and June 2008, infected with MRSA, and treated with either linezolid (oral or intravenous [i.v.]) or vancomycin (i.v.). Patients were followed from their treatment initiation date until the event of interest, discharge, death, or December Utilizing propensity score methods, we estimated the treatment effects of linezolid primarily on time to discharge and secondarily on time to all-cause in-hospital mortality, therapy discontinuation, and all-cause 90-day readmission with Cox proportional-hazard models. We identified 20,107 patients treated with linezolid (3.2%) or vancomycin (96.8%). Baseline covariates were well balanced by treatment group within propensity score quintiles and between propensity score matched patients (626 pairs). The discharge rate was significantly higher among patients treated with linezolid, representing a decreased length of stay, in both the propensity score adjusted (hazard ratio [HR], 1.38; 95% confidence interval [95% CI], 1.27 to 1.50) and matched (HR, 1.70; 95% CI, 1.44 to 2.00) analyses. A significantly decreased rate of therapy discontinuation, indicating longer therapy duration, was observed in the linezolid group (adjusted HR, 0.64; 95% CI, 0.54 to 0.75; matched HR, 0.49; 95% CI, 0.36 to 0.65). In this clinical population of MRSA-infected patients, linezolid therapy was as effective as vancomycin therapy with respect to in-hospital survival and readmission. Limited treatment options exist for patients infected with methicillin-resistant Staphylococcus aureus (MRSA). Vancomycin has served as the gold standard of care for many years (16, 28). However, the emergence of bacteria with decreased vancomycin susceptibility has prompted the need for novel antibiotics (16, 32). Linezolid, an oxazolidinone antibiotic, was approved by the Food and Drug Administration in April While a limited number of clinical trials have reported linezolid superiority, many have found efficacy equivalent to that of vancomycin for the treatment of MRSA infections (10, 14, 30, 31, 33, 35 37). The few studies demonstrating significantly higher clinical cure and survival rates with linezolid therapy have been criticized for their limitations and conclusions, particularly the claim of linezolid superiority based on MRSA subgroup analyses (3, 10, 11, 21, 22). Additionally, there are conflicting data regarding length of stay decreases and length of therapy when comparing linezolid and vancomycin therapies (7, 15, 18 20, 30, 36). Though randomized clinical trials provide key efficacy data on newly approved agents, insight regarding their effectiveness in clinical practice, particularly among diverse patient populations, and their effectiveness compared to that of standard * Corresponding author. Mailing address: Veterans Affairs Medical Center (151), Research Building #35, 830 Chalkstone Avenue, Providence, RI Phone: (401) , ext Fax: (401) KerryTedesco@uri.edu. Published ahead of print on 26 July therapies is often lacking. Due to the increasing complexity of treating MRSA infections, knowledge of the real-world clinical impact of newer agents is needed for informed decision making. We therefore sought to quantify the effectiveness of linezolid compared to that of vancomycin on clinical outcomes among a national cohort of MRSA-infected patients admitted to Veterans Affairs (VA) facilities. (This work was presented in part at the 25th International Conference on Pharmacoepidemiology and Therapeutic Risk Management in Providence, RI, on 19 August 2009.) MATERIALS AND METHODS Data sources. We utilized standardized Veterans Health Administration national inpatient datasets, which contain International Classification of Diseases, 9th ed. (ICD-9), discharge diagnosis (up to 13 entries per admission) and procedure (up to 5 entries per day) codes (17). National extracts of inpatient and outpatient records for prescriptions, laboratory tests, and select laboratory results were also included. This study was reviewed and approved by the Providence Veterans Affairs Medical Center and University of Rhode Island institutional review boards. Study design and population identification. We conducted a retrospective cohort study among adult ( 18 years of age) patients admitted to VA hospitals between 1 January 2002 and 30 June 2008 with a MRSA infection diagnosis code (ICD-9 V09.0). If patients had more than one admission with a MRSA diagnosis code, the first admission occurring during the study period was selected for inclusion. We excluded patients with a concomitant diagnosis code for vancomycin-resistant enterococcus (ICD-9 V09.8) or endocarditis (ICD , 421.1, 421.9, or ), due to vancomycin nonutilization with the former and reported linezolid treatment failure with the latter (26). From this eligible population, we identified two groups of patients initiating therapy during the admission: those receiving oral or intravenous (i.v.) linezolid (exposed group), as the oral formu- 4394
4 VOL. 54, 2010 LINEZOLID & VANCOMYCIN EFFECTIVENESS IN MRSA INFECTION 4395 lation is 100% bioavailable, and those treated with i.v. vancomycin (comparison group). Patients receiving greater than one dose of linezolid or vancomycin therapy, but not both, during the admission were selected for inclusion. Figure 1 illustrates the inclusion and exclusion criteria applied for the identification of the final study population. Outcome definitions. The primary outcome of interest was time to discharge, and the secondary endpoints evaluated were time to all-cause in-hospital mortality, therapy discontinuation, and all-cause 90-day readmission. Therapy initiation was used to define the index date of treatment. Time calculations were made from the index date to the event date for each endpoint. Patients who died during the admission were censored on their date of death, and those alive were censored on their date of discharge. If the end of inpatient therapy occurred on the date of discharge or death, patients were censored at these time points. Patients who died during the index admission (n 1,537) were not included in the follow-up for all-cause 90-day readmission to a medical unit in a VA hospital. Patients without readmission records were censored on their date of death, 90 days from their discharge date, or on 31 December Propensity score development. The Charlson comorbidity index and chronic comorbidities were captured from ICD-9 codes in the year prior to admission and during the index admission (23). Infection type was defined by the following ICD-9 codes: bacteremia, , , , 038.8, 038.9, and 790.7; pneumonia, , , , , 482.9, 484.8, 485, 486, 510.0, 510.9, 513.0, and 513.1; and skin and soft tissue, to 680.9, to , , , 681.9, to 682.9, 684, 686.9, 704.8, to 707.9, , , , , and (8). To assess baseline differences between the two study groups, we utilized Fisher s exact or the 2 test for categorical data. For continuous variables of interest, we used a t test for normally distributed data, and the nonparametric Wilcoxon rank-sum test was used otherwise. We employed propensity score methods, where the predicted probability of treatment with linezolid was derived from unconditional logistic regression utilizing a manual backward-elimination approach (1, 5, 25). Propensity scores provide a means of balancing baseline covariates predictive of treatment, mitigating the unequal chance of receiving linezolid versus vancomycin, and are an efficient method to control for confounding in pharmacoepidemiologic analyses (1, 25). Our final model demonstrated fit (Hosmer and Lemeshow, P 0.477), discrimination (C statistic, 0.784), and an absence of multicollinearity (5). Propensity score stratification into quintiles and 1:1 matching within a 0.01 propensity score caliper range were implemented, related assumptions were assessed, and subsequent covariate balance was reviewed. Time-to-event analyses. We developed separate Cox proportional-hazard regression models to quantify the effect of linezolid therapy compared to that of vancomycin therapy for each of the aforementioned outcomes. In propensity score adjustment, indicators of propensity score quintile (reference lowest quintile) were included in the Cox models, while propensity score matching accounted for matched linezolid- and vancomycin-treated pairs. We evaluated Cox proportional-hazard model assumptions, including that of proportionality, with formal tests and graphical displays (6). A hazard ratio (HR) greater than 1 indicated an increased probability of the event occurring sooner in the linezolid group than in the reference vancomycin group. In terms of the study outcomes, an HR greater than 1 would represent higher rates of discharge, mortality, therapy discontinuation, and readmission among patients treated with linezolid. In subgroup analyses, we assessed variations by infection type (24). We evaluated various follow-up periods for all-cause readmission (30, 60, 180, and 365 days) in sensitivity analyses. All analyses were performed using SAS software (version 9.1; SAS Institute Inc., Cary, NC). RESULTS FIG. 1. Study inclusion and exclusion criteria applied for sample identification. a, Patients aged 18 years and older, admitted to medical units in Veterans Affairs hospitals between 1 January 2002 and 30 June 2008, with a MRSA diagnosis code. b, If a patient had multiple admissions with a MRSA diagnosis during the study period, only the first admission was included. c, Patients who received both vancomycin (i.v.) and linezolid (i.v. or oral) during the admission. VRE, vancomycin-resistant enterococcus. We identified 20,107 patients treated with linezolid (3.2%) or vancomycin (96.8%). The majority of MRSA infections occurred in Southern facilities. Several significant variations in demographics and comorbidities, including gender, race, amputation, and para- or quadriplegia, were observed by treat- TABLE 1. Demographics and comorbid conditions by treatment group Covariate Result a for patients treated with: Linezolid (n 637) Vancomycin (n 19,470) P value b Age in yr, mean (SD c ) 65.1 (14.0) 64.2 (13.6) Race White 371 (58.2) 11,250 (57.8) African-American 72 (11.3) 2,955 (15.2) Other 7 (1.1) 186 (0.9) Unknown/missing 187 (29.4) 5,079 (26.1) Gender Male 611 (95.9) 18,992 (97.5) Female 26 (4.1) 478 (2.5) Charlson comorbidity index, median (IQR d ) 2 (1 4) 2 (1 4) Comorbid condition Diabetes 251 (39.4) 7,966 (40.9) Renal disease 191 (30.0) 5,214 (26.8) Chronic respiratory disease 186 (29.2) 5,255 (27.0) Coronary heart disease 185 (29.0) 5,464 (28.1) Heart failure 127 (19.9) 3,774 (19.4) Cancer 93 (14.6) 2,405 (12.4) Amputation 48 (7.5) 1,013 (5.2) Para- or quadriplegia 43 (6.8) 914 (4.7) Hepatic disease 36 (5.7) 961 (4.9) Cerebrovascular disease 32 (5.0) 1,322 (6.8) HIV/AIDS 12 (1.9) 438 (2.3) Transplant 9 (1.4) 193 (1.0) Burns 4 (0.6) 83 (0.4) a Data represent numbers of subjects, with percentages in parentheses, unless otherwise indicated. b Determined by t test, 2 test, Fisher s exact test, or Wilcoxon rank-sum test as appropriate. c SD, standard deviation. d IQR, interquartile range.
5 4396 CAFFREY ET AL. ANTIMICROB. AGENTS CHEMOTHER. TABLE 2. Health care and antibiotic exposures and hospitalizationrelated characteristics by treatment group Covariate Result a for patients treated with: Linezolid (n 637) Vancomycin (n 19,470) P value b Previous hospitalization c 380 (59.7) 10,935 (56.2) Previous surgery d 164 (25.8) 4,481 (23.0) Previous antibiotics e, mean 1.9 (2.2) 1.4 (1.7) no. (SD) Previous linezolid or vancomycin Linezolid 22 (3.5) 58 (0.3) Vancomycin 163 (25.6) 6,039 (31.0) Linezolid and vancomycin 80 (12.6) 225 (1.2) Origin of admission Home 518 (81.3) 16,149 (82.9) Hospital 60 (9.4) 1,438 (7.4) Nursing home 59 (9.3) 1,883 (9.7) Region of facility f North 78 (12.2) 1,948 (10.0) South 307 (48.2) 7,995 (41.1) Midwest 105 (16.5) 4,351 (22.3) West 147 (23.1) 5,176 (26.6) Procedure during hospitalization Surgery 146 (22.9) 5,705 (29.3) Catheterization 93 (14.6) 6,062 (31.1) Mechanical ventilation 47 (7.4) 1,593 (8.2) Dialysis 27 (4.2) 1,010 (5.2) MRSA infection type Bacteremia 82 (12.9) 4,498 (23.1) Pneumonia 126 (19.8) 2,718 (14.0) Skin and soft tissue 232 (36.4) 6,965 (35.8) Other/not specified 197 (30.9) 5,289 (27.1) Treating specialty Intensive care 82 (12.9) 2,985 (15.3) Surgery 96 (15.1) 2,032 (10.4) General medicine 362 (56.8) 11,384 (58.5) Other 97 (15.2) 3,069 (15.8) Treatment initiation 3 days g 390 (61.2) 14,802 (76.0) Yr of treatment (29.0) 7,665 (39.4) (36.6) 6,352 (32.6) (34.4) 5,453 (28.0) a Data represent numbers of subjects, with percentages in parentheses, unless otherwise indicated. b Determined by 2 test or Wilcoxon rank-sum test as appropriate. c All-cause hospitalization to a Veterans Affairs medical unit in the previous year. d Any surgical procedure in the previous year. e Previous exposures to unique antibiotics, at least one dose, in the 90 days before admission. f U.S. Census Bureau-defined regions. g Treatment initiated within 3 days of the admission date. ment group (Table 1). Patients treated with linezolid were exposed to a greater number of unique antibiotics in the 90 days before admission than those treated with vancomycin. Linezolid use was more common in recent years, with concurrent decreases in vancomycin utilization over time. Previous antibiotic exposure, facility region, surgery during the hospitalization, presence of a catheter while hospitalized, infection type, time to treatment initiation, and treating specialty also varied significantly between the linezolid and vancomycin treatment groups (Table 2). No differences in baseline white blood cell count, blood urea nitrogen, serum creatinine, or creatinine clearance were observed by treatment group. The propensity score was derived from an unconditional logistic regression model controlling for age, gender, race, region of facility, renal disease, amputation, para- or quadriplegia, cerebrovascular disease, previous linezolid and/or vancomycin exposure, catheterization, surgery, infection type, treating specialty, treatment year, time to treatment initiation, age by renal disease, age by previous linezolid and/or vancomycin exposure, age by infection type, age by treatment year, age by time to treatment initiation, race by region, race by treating specialty, race by time to treatment initiation, region by amputation, region by previous linezolid and/or vancomycin exposure, region by treating specialty, amputation by time to treatment initiation, catheter by infection type, catheter by treating specialty, infection type by treatment year, infection type by time to treatment initiation, and treatment year by time to treatment initiation. Propensity score overlap between the linezolid and vancomycin treatment groups was observed within quintiles. Propensity score matching yielded 626 matched pairs, identifying a vancomycin-treated match for 98.3% of linezolidtreated patients. Baseline covariates were well balanced by treatment group within propensity score quintiles and between the matched linezolid- and vancomycin-treated pairs. The results of propensity score adjusted and propensity score matched analyses were comparable for each study outcome (Fig. 2). Based on unadjusted Kaplan-Meier estimates of event-free distribution functions, the median time to discharge from treatment initiation was 6 days in the linezolid group and 9 days in the vancomycin group (likelihood ratio test, P 0.001). The discharge rate was significantly higher among patients treated with linezolid in both the propensity score adjusted (HR, 1.38; 95% confidence interval [95% CI], 1.27 to 1.50) and matched (HR, 1.70; 95% CI, 1.44 to 2.00) analyses. The median time to therapy discontinuation was 16 days in the linezolid group and 13 days in the vancomycin group (P 0.001). A significantly decreased rate of therapy discontinuation was observed in the linezolid group (adjusted HR, 0.64; 95% CI, 0.54 to 0.75; matched HR, 0.49; 95% CI, 0.36 to 0.65). In the overall population, 7.6% of patients died during the hospitalization. The median survival times (P 0.381) and 90-day readmission event-free days (P 0.677) did not differ significantly by treatment group. No associations between treatment group and time to death or time to 90-day readmission were observed. These findings were consistent in sensitivity analyses of all-cause readmission, including 30-, 60-, 180-, and 365-day follow-up periods. Of the total patients followed after discharge, 9.2% had a MRSA infection diagnosis code listed in a readmission occurring within the year after discharge (9.2% for the linezolid group and 9.2% for the vancomycin group). In subgroup analyses by infection type (Fig. 3), no associations between treatment group and any of the study outcomes were observed among patients with bacteremia. In the pneumonia subgroup, the discharge rate was significantly higher for
6 VOL. 54, 2010 LINEZOLID & VANCOMYCIN EFFECTIVENESS IN MRSA INFECTION 4397 FIG. 2. Hazard ratios of study outcomes for linezolid compared to vancomycin therapy. 1, Adjusted by propensity score quintiles (reference quintile I). 2, Propensity score matched within a 0.01 caliper range. linezolid-treated patients in propensity adjusted (HR, 1.60; 95% CI, 1.33 to 1.94) but not matched (HR, 1.85; 95% CI, 0.94 to 3.63) analyses. The therapy discontinuation rate among those with skin and soft tissue infections was significantly higher for linezolid-treated patients in propensity adjusted (HR, 0.59; 95% CI, 0.42 to 0.82) but not matched (HR, 0.42; 95% CI, 0.15 to 1.18) analyses. In propensity score matched analyses among patients with other/not specified infection types, the 90-day readmission rate was significantly higher in the linezolid group (HR, 4.60; 95% CI, 1.75 to 12.10). DISCUSSION We assessed the real-world effectiveness of linezolid compared to that of vancomycin for the treatment of MRSA infections among a large cohort of patients admitted to VA hospitals. To our knowledge, this is the first national observational cohort study evaluating the impact of linezolid therapy on time to discharge, in-hospital mortality, therapy discontinuation, and readmission. Time-to-event analyses revealed significant differences between the linezolid and vancomycin treatment groups in two of the outcomes evaluated. Compared to vancomycin therapy, we found linezolid therapy to be associated with a decreased length of stay after treatment initiation, as indicated by the significantly higher discharge rate. While length of stay was generally lower (1.0 to 3.5 days) for patients treated with linezolid compared to vancomycin in randomized controlled trials, it was uncertain whether these decreases would be experienced in clinical practice, particularly due to the small efficacy trial sample sizes and MRSA subgroup analyses (7, 15, 18, 19, 30). In our pharmacoepidemiologic effectiveness study of patients hospitalized with MRSA infections in VA facilities throughout the country, the median length of stay was 3 days shorter among those treated with linezolid compared to those treated with vancomycin. We observed a decreased rate of therapy discontinuation in the linezolid group, representing an increased length of therapy. The reasons behind longer therapy duration in the linezolid group compared to the vancomycin group are not clear but may be related to prescribing practices as patients transition out of the hospital. Interpreting survival with linezolid treatment compared to vancomycin in clinical trials has been complicated by conflicting results, subgroup analyses, and small study populations (14, 31, 33, 35, 37). Two trials reported similar death rates by treatment group in the overall study population but did not describe the mortality rates in the MRSA subset (33, 35). A MRSA subgroup analysis of two nosocomial pneumonia clinical trials reported a higher survival rate among patients treated with linezolid compared to those treated with vancomycin (60/75 versus 54/85, P 0.030), which was not observed in the overall study population (37). Alternatively, MRSA bacteremia survival did not vary by treatment group in a pooled analysis of five randomized S. aureus bacteremia trials (odds ratio [OR], 1.08; 95% CI, 0.41 to 2.85) (31). In our retrospective cohort study, treatment with linezolid therapy did not significantly reduce the risk of death. Readmission rates were similar by treatment group in clinical trials, although few studies reported such rates with very short follow-up times ( 35 days) (7, 19). In the overall MRSA cohort and subgroups of pneumonia, skin and soft tissue infections, and bacteremia, we did not find readmission rates to vary by treatment group. This study has several limitations. There is always the potential for residual confounding by unobserved covariates. While the propensity score methodology successfully balanced the baseline covariates assessed, it does not ensure subsequent balance of unobserved covariates. In sensitivity analyses of residual confounding, strong confounders, with a significant confounder-outcome association and unequal distribution by treatment group, could change the lower 95% confidence limit of the hazard ratio to include one for the primary outcome. The therapeutic impact of vancomycin could not be determined in this study, as peak and trough results were not avail-
7 4398 CAFFREY ET AL. ANTIMICROB. AGENTS CHEMOTHER. FIG. 3. Hazard ratios of study outcomes by infection type for linezolid compared to vancomycin therapy. able for evaluation. The mean baseline creatinine clearance in the vancomycin group was 59 ml/min, suggesting that a typical dosing regimen of 1 g every 12 h would be sufficient to achieve a therapeutic trough (12, 27). Additionally, we expect the average MIC of our national VA cohort to correspond with the national average MIC of 1 mg/liter (9, 27, 34). Patients receiving both linezolid and vancomycin during the admission were excluded, as patients failing treatment with vancomycin may have been switched to linezolid. We identified patients with MRSA infections from the V09.0
8 VOL. 54, 2010 LINEZOLID & VANCOMYCIN EFFECTIVENESS IN MRSA INFECTION 4399 ICD-9 code, as microbiological culture results could not be obtained. Little information regarding the accuracy of this diagnosis code exists. Despite this limitation, the code is used in research to identify MRSA infections with a reportedly high positive predictive value (92%) (2, 4, 29). Further, increased sensitivity is expected when antibiotic treatment is taken into account and when greater numbers of diagnosis entries are available (4, 13, 29). While the possibility of MRSA infection underascertainment exists, differential variation by treatment group is doubtful. MRSA infections requiring inpatient treatment may be captured with more consistency, which would indicate better ascertainment among those treated with anti- MRSA therapies. In our study population, linezolid was utilized much less frequently than vancomycin (3.2% versus 96.8%). In the linezolid group, few patients died during the hospitalization (37/ 637) and subgroup analyses by infection type resulted in small numbers, which affected our ability to discern differences by treatment group. As more patients are treated with linezolid in the future, a clearer picture of its effectiveness by infection type and its impact on mortality will emerge. The generalizability of this study is limited to VA patients. In summary, linezolid was associated with a significantly shorter length of stay and significantly longer duration of therapy compared to vancomycin for the treatment of MRSA infections. Among our national cohort of MRSA-infected patients, linezolid was as effective as vancomycin, with similar in-hospital survival and readmission rates by treatment group. Future research should include comprehensive pharmacoeconomic analyses assessing costs related to length of stay and duration of therapy comparing linezolid and vancomycin. ACKNOWLEDGMENTS We gratefully acknowledge the Center on Systems, Outcomes and Quality in Chronic Disease and Rehabilitation, a REAP of the Health Services Research and Development Service, Providence Veterans Affairs Medical Center Research Service, for data storage and software assistance. The views expressed are those of the authors and do not necessarily reflect the position or policy of the United States Department of Veterans Affairs. No financial support for this study was received. After the completion of this study and manuscript, A.R.C., K.L.L., and B.J.Q. received collaborative research funding from Pfizer Inc., makers of linezolid, for separate research. K.L.L. has received unrestricted investigator initiated research grants and/or served on a drug advisory board for Astellas, Cubist, Forrest, Merck, and Pfizer. B.J.Q. has received research funding from Takeda Pharmaceuticals North America. REFERENCES 1. D Agostino, R. B., Jr Propensity score methods for bias reduction in the comparison of a treatment to a non-randomized control group. Stat. Med. 17: Elixhauser, A., and C. Steiner Infections with methicillin-resistant Staphylococcus aureus (MRSA) in U.S. hospitals, Healthcare Cost and Utilization Project (HCUP) statistical brief no. 35. Agency for Healthcare Research and Quality, Rockville, MD Estes, L., and R. Orenstein Cost-effectiveness analysis of linezolid compared with vancomycin for the treatment of nosocomial pneumonia caused by methicillin-resistant Staphylococcus aureus. Clin. Ther. 29: Gerber, J. S., S. E. Coffin, S. A. Smathers, and T. E. Zaoutis Trends in the incidence of methicillin-resistant Staphylococcus aureus infection in children s hospitals in the United States. Clin. Infect. Dis. 49: Hosmer, D. W., and S. Lemeshow Applied logistic regression, 2nd ed. John Wiley & Sons, Inc., New York, NY. 6. Hosmer, D. W., and S. Lemeshow Applied survival analysis: regression modeling of time to event data. John Wiley & Sons, Inc., New York, NY. 7. Itani, K. M., J. Weigelt, J. Z. Li, and S. Duttagupta Linezolid reduces length of stay and duration of intravenous treatment compared with vancomycin for complicated skin and soft tissue infections due to suspected or proven methicillin-resistant Staphylococcus aureus (MRSA). Int. J. Antimicrob. Agents 26: Jhung, M. A., S. N. Banerjee, S. Fridkin, F. C. Tenover, and L. C. McDonald Enhanced detection of Staphylococcus aureus-related hospitalizations using administrative databases, United States th Annu. Sci. Meet. Soc. Healthcare Epidemiol. Am., Orlando, FL. /ncidod/dhqp/shea_enhandetecs_aureus_textonly.html. 9. Jones, R. N Microbiological features of vancomycin in the 21st century: minimum inhibitory concentration creep, bactericidal/static activity, and applied breakpoints to predict clinical outcomes or detect resistant strains. Clin. Infect. Dis. 42(Suppl. 1):S13 S Kalil, A. C., S. Puumala, and J. Stoner Is linezolid superior to vancomycin for complicated skin and soft tissue infections due to methicillinresistant Staphylococcus aureus? Antimicrob. Agents Chemother. 50: Kalil, A. C., S. E. Puumala, and J. Stoner Unresolved questions with the use of linezolid vs vancomycin for nosocomial pneumonia. Chest 125: Karam, C. M., P. S. McKinnon, M. M. Neuhauser, and M. J. Rybak Outcome assessment of minimizing vancomycin monitoring and dosing adjustments. Pharmacotherapy 19: Klompas, M., and D. S. Yokoe Automated surveillance of health care-associated infections. Clin. Infect. Dis. 48: Kollef, M. H., J. Rello, S. K. Cammarata, R. V. Croos-Dabrera, and R. G. Wunderink Clinical cure and survival in Gram-positive ventilatorassociated pneumonia: retrospective analysis of two double-blind studies comparing linezolid with vancomycin. Intensive Care Med. 30: Li, Z., R. J. Willke, L. A. Pinto, B. E. Rittenhouse, M. J. Rybak, A. M. Pleil, C. W. Crouch, B. Hafkin, and H. A. Glick Comparison of length of hospital stay for patients with known or suspected methicillin-resistant Staphylococcus species infections treated with linezolid or vancomycin: a randomized, multicenter trial. Pharmacotherapy 21: Lodise, T. P., Jr., and P. S. McKinnon Burden of methicillin-resistant Staphylococcus aureus: focus on clinical and economic outcomes. Pharmacotherapy 27: Maynard, C., and M. K. Chapko Data resources in the Department of Veterans Affairs. Diabetes Care 27(Suppl. 2):B22 B McCollum, M., S. V. Sorensen, and L. Z. Liu A comparison of costs and hospital length of stay associated with intravenous/oral linezolid or intravenous vancomycin treatment of complicated skin and soft-tissue infections caused by suspected or confirmed methicillin-resistant Staphylococcus aureus in elderly US patients. Clin. Ther. 29: McKinnon, P. S., S. V. Sorensen, L. Z. Liu, and K. M. Itani Impact of linezolid on economic outcomes and determinants of cost in a clinical trial evaluating patients with MRSA complicated skin and soft-tissue infections. Ann. Pharmacother. 40: Mullins, C. D., A. Kuznik, F. T. Shaya, N. A. Obeidat, A. R. Levine, L. Z. Liu, and W. Wong Cost-effectiveness analysis of linezolid compared with vancomycin for the treatment of nosocomial pneumonia caused by methicillin-resistant Staphylococcus aureus. Clin. Ther. 28: Powers, J. H., D. Lin, and D. Ross FDA evaluation of antimicrobials: subgroup analysis. Chest 127: Powers, J. H., D. B. Ross, D. Lin, and J. Soreth Linezolid and vancomycin for methicillin-resistant Staphylococcus aureus nosocomial pneumonia: the subtleties of subgroup analyses. Chest 126: Quan, H., V. Sundararajan, P. Halfon, A. Fong, B. Burnand, J. C. Luthi, L. D. Saunders, C. A. Beck, T. E. Feasby, and W. A. Ghali Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med. Care 43: Rassen, J. A., M. A. Brookhart, and S. Schneeweiss Applying propensity scores estimated in a full cohort to achieve balance in subgroup analyses. Pharmacoepidemiol. Drug Saf. 18(Suppl. 1):S Rubin, D. B Estimating causal effects from large data sets using propensity scores. Ann. Intern. Med. 127: Ruiz, M. E., I. C. Guerrero, and C. U. Tuazon Endocarditis caused by methicillin-resistant Staphylococcus aureus: treatment failure with linezolid. Clin. Infect. Dis. 35: Rybak, M., B. Lomaestro, J. C. Rotschafer, R. Moellering, Jr., W. Craig, M. Billeter, J. R. Dalovisio, and D. P. Levine Therapeutic monitoring of vancomycin in adult patients: a consensus review of the American Society of Health-System Pharmacists, the Infectious Diseases Society of America, and the Society of Infectious Diseases Pharmacists. Am. J. Health Syst. Pharm. 66: Sakoulas, G., and R. C. Moellering, Jr Increasing antibiotic resistance among methicillin-resistant Staphylococcus aureus strains. Clin. Infect. Dis. 46(Suppl. 5):S360 S Schaefer, M., K. Ellingson, C. Conover, A. Genisca, S. Fridkin, D. Currie, T.
9 4400 CAFFREY ET AL. ANTIMICROB. AGENTS CHEMOTHER. Esposito, L. Pantilla, P. Ruesto, K. Martin, D. Cronin, M. Costello, S. Sokalski, and A. Srinivasan Evaluation of ICD-9 codes as a mechanism for surveillance of methicillin-resistant Staphylococcus aureus infections in Illinois United States, 2007, abstr Abstr. 18th Annu. Sci. Meet. Soc. Healthcare Epidemiol. Am., Orlando, FL. 30. Sharpe, J. N., E. H. Shively, and H. C. Polk, Jr Clinical and economic outcomes of oral linezolid versus intravenous vancomycin in the treatment of MRSA-complicated, lower-extremity skin and soft-tissue infections caused by methicillin-resistant Staphylococcus aureus. Am. J. Surg. 189: Shorr, A. F., M. J. Kunkel, and M. Kollef Linezolid versus vancomycin for Staphylococcus aureus bacteraemia: pooled analysis of randomized studies. J. Antimicrob. Chemother. 56: Sievert, D. M., J. T. Rudrik, J. B. Patel, L. C. McDonald, M. J. Wilkins, and J. C. Hageman Vancomycin-resistant Staphylococcus aureus in the United States, Clin. Infect. Dis. 46: Stevens, D. L., D. Herr, H. Lampiris, J. L. Hunt, D. H. Batts, and B. Hafkin Linezolid versus vancomycin for the treatment of methicillin-resistant Staphylococcus aureus infections. Clin. Infect. Dis. 34: Tenover, F. C., and R. C. Moellering, Jr The rationale for revising the Clinical and Laboratory Standards Institute vancomycin minimal inhibitory concentration interpretive criteria for Staphylococcus aureus. Clin. Infect. Dis. 44: Weigelt, J., K. Itani, D. Stevens, W. Lau, M. Dryden, and C. Knirsch Linezolid versus vancomycin in treatment of complicated skin and soft tissue infections. Antimicrob. Agents Chemother. 49: Weigelt, J., H. M. Kaafarani, K. M. Itani, and R. N. Swanson Linezolid eradicates MRSA better than vancomycin from surgical-site infections. Am. J. Surg. 188: Wunderink, R. G., J. Rello, S. K. Cammarata, R. V. Croos-Dabrera, and M. H. Kollef Linezolid vs vancomycin: analysis of two double-blind studies of patients with methicillin-resistant Staphylococcus aureus nosocomial pneumonia. Chest 124:
Pharmacy Practice Faculty Publications
 University of Rhode Island DigitalCommons@URI Pharmacy Practice Faculty Publications Pharmacy Practice 2014 Comparative Effectiveness of Linezolid and Vancomycin Among a National Veterans Affairs Cohort
University of Rhode Island DigitalCommons@URI Pharmacy Practice Faculty Publications Pharmacy Practice 2014 Comparative Effectiveness of Linezolid and Vancomycin Among a National Veterans Affairs Cohort
Changing epidemiology of methicillin-resistant Staphylococcus aureus in the Veterans Affairs Healthcare System,
 University of Rhode Island DigitalCommons@URI Pharmacy Practice Faculty Publications Pharmacy Practice 2012 Changing epidemiology of methicillin-resistant Staphylococcus aureus in the Veterans Affairs
University of Rhode Island DigitalCommons@URI Pharmacy Practice Faculty Publications Pharmacy Practice 2012 Changing epidemiology of methicillin-resistant Staphylococcus aureus in the Veterans Affairs
ORIGINAL ARTICLE DOI: (e) ISSN Online: (p) ISSN Print: Anand Kumar Singh 1, Poonam Verma 2. Sciences, Dehradun
 ORIGINAL ARTICLE CLINICAL ASSESSMENT OF NEPHROTOXICITY ASSOCIATED WITH VANCOMYCIN TROUGH CONCENTRATIONS DURING TREATMENT OF DEEP-SEATED INFECTIONS: A RETROSPECTIVE ANALYSIS Anand Kumar Singh 1, Poonam
ORIGINAL ARTICLE CLINICAL ASSESSMENT OF NEPHROTOXICITY ASSOCIATED WITH VANCOMYCIN TROUGH CONCENTRATIONS DURING TREATMENT OF DEEP-SEATED INFECTIONS: A RETROSPECTIVE ANALYSIS Anand Kumar Singh 1, Poonam
D DAVID PUBLISHING. Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within a Therapeutic Range. 1.
 Journal of Pharmacy and Pharmacology 2 (2014) 713-721 doi: 10.17265/2328-2150/2014.12.004 D DAVID PUBLISHING Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within
Journal of Pharmacy and Pharmacology 2 (2014) 713-721 doi: 10.17265/2328-2150/2014.12.004 D DAVID PUBLISHING Evaluation of the Effectiveness of a Vancomycin Nomogram at Predicting Trough Levels within
D DAVID PUBLISHING. 1. Introduction. Kathryn Koliha 1, Julie Falk 1, Rachana Patel 1 and Karen Kier 2
 Journal of Pharmacy and Pharmacology 5 (2017) 607-615 doi: 10.17265/2328-2150/2017.09.001 D DAVID PUBLISHING Comparative Evaluation of Pharmacist-Managed Vancomycin Dosing in a Community Hospital Following
Journal of Pharmacy and Pharmacology 5 (2017) 607-615 doi: 10.17265/2328-2150/2017.09.001 D DAVID PUBLISHING Comparative Evaluation of Pharmacist-Managed Vancomycin Dosing in a Community Hospital Following
Evaluation of Vancomycin Continuous Infusion in Trauma Patients
 OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
Supplementary Online Content
 Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Supplementary Online Content Toyoda N, Chikwe J, Itagaki S, Gelijns AC, Adams DH, Egorova N. Trends in infective endocarditis in California and New York State, 1998-2013. JAMA. doi:10.1001/jama.2017.4287
Clinical Guidelines for Use of Antibiotics. VANCOMYCIN (Adult)
 VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
Running head: REDUCING HOSPITAL- ACQUIRED INFECTIONS 1
 Running head: REDUCING HOSPITAL- ACQUIRED INFECTIONS 1 Reducing Hospital-Acquired Infections Corinne Showalter University of South Florida REDUCING HOSPITAL- ACQUIRED INFECTIONS 2 Abstract Clinical Problem:
Running head: REDUCING HOSPITAL- ACQUIRED INFECTIONS 1 Reducing Hospital-Acquired Infections Corinne Showalter University of South Florida REDUCING HOSPITAL- ACQUIRED INFECTIONS 2 Abstract Clinical Problem:
Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia
 Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia Brandon Dionne, PharmD, BCPS, AAHIVP Assistant Clinical Professor Northeastern University Seth Housman, PharmD, MPA Clinical Assistant
Superhero or Superzero? Vancomycin vs. Linezolid for MRSA Pneumonia Brandon Dionne, PharmD, BCPS, AAHIVP Assistant Clinical Professor Northeastern University Seth Housman, PharmD, MPA Clinical Assistant
Higher Daptomycin Dose Associated with Improved Survival in Methicillin-Resistant Staphylococcus aureus Bacteremia
 University of Rhode Island DigitalCommons@URI Pharmacy Practice Faculty Publications Pharmacy Practice 2017 Higher Daptomycin Dose Associated with Improved Survival in Methicillin-Resistant Staphylococcus
University of Rhode Island DigitalCommons@URI Pharmacy Practice Faculty Publications Pharmacy Practice 2017 Higher Daptomycin Dose Associated with Improved Survival in Methicillin-Resistant Staphylococcus
Supplementary Online Content
 Supplementary Online Content Lee JS, Nsa W, Hausmann LRM, et al. Quality of care for elderly patients hospitalized for pneumonia in the United States, 2006 to 2010. JAMA Intern Med. Published online September
Supplementary Online Content Lee JS, Nsa W, Hausmann LRM, et al. Quality of care for elderly patients hospitalized for pneumonia in the United States, 2006 to 2010. JAMA Intern Med. Published online September
Zhao Y Y et al. Ann Intern Med 2012;156:
 Zhao Y Y et al. Ann Intern Med 2012;156:560-569 Introduction Fibrates are commonly prescribed to treat dyslipidemia An increase in serum creatinine level after use has been observed in randomized, placebocontrolled
Zhao Y Y et al. Ann Intern Med 2012;156:560-569 Introduction Fibrates are commonly prescribed to treat dyslipidemia An increase in serum creatinine level after use has been observed in randomized, placebocontrolled
Proton-pump inhibitors do not influence clinical outcomes in patients with Staphylococcus aureus bacteremia
 834273TAG0010.1177/1756284819834273Therapeutic Advances in GastroenterologyAR Caffrey research-article20192019 Therapeutic Advances in Gastroenterology Original Research Proton-pump inhibitors do not influence
834273TAG0010.1177/1756284819834273Therapeutic Advances in GastroenterologyAR Caffrey research-article20192019 Therapeutic Advances in Gastroenterology Original Research Proton-pump inhibitors do not influence
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING
 EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
Clinical Safety & Effectiveness Cohort # 10
 1 Clinical Safety & Effectiveness Cohort # 10 Improving Weight-Based Vancomycin Dosing and Monitoring DATE Educating for Quality Improvement & Patient Safety 2 Financial Disclosure lizabeth A. Walter,
1 Clinical Safety & Effectiveness Cohort # 10 Improving Weight-Based Vancomycin Dosing and Monitoring DATE Educating for Quality Improvement & Patient Safety 2 Financial Disclosure lizabeth A. Walter,
Rates and patterns of participation in cardiac rehabilitation in Victoria
 Rates and patterns of participation in cardiac rehabilitation in Victoria Vijaya Sundararajan, MD, MPH, Stephen Begg, MS, Michael Ackland, MBBS, MPH, FAPHM, Ric Marshall, PhD Victorian Department of Human
Rates and patterns of participation in cardiac rehabilitation in Victoria Vijaya Sundararajan, MD, MPH, Stephen Begg, MS, Michael Ackland, MBBS, MPH, FAPHM, Ric Marshall, PhD Victorian Department of Human
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
VANCOMYCIN DOSING AND MONITORING GUIDELINES
 VANCOMYCIN DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee Approved: May 2017 GENERAL COMMENTS Vancomycin is a glycopeptide antibiotic with bactericidal
VANCOMYCIN DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee Approved: May 2017 GENERAL COMMENTS Vancomycin is a glycopeptide antibiotic with bactericidal
Full title of guideline INTRAVENOUS VANCOMYCIN PRESCRIBING AND MONITORING GUIDELINE FOR ADULT PATIENTS. control
 Full title of guideline Author: Contact Name and Job Title Division and specialty Scope Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis) Changes
Full title of guideline Author: Contact Name and Job Title Division and specialty Scope Explicit definition of patient group to which it applies (e.g. inclusion and exclusion criteria, diagnosis) Changes
Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry
 doi: 10.1111/j.1742-1241.2008.01824.x ORIGINAL PAPER Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry W. J. Martone, K. C. Lindfield, D. E. Katz OnlineOpen: This
doi: 10.1111/j.1742-1241.2008.01824.x ORIGINAL PAPER Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry W. J. Martone, K. C. Lindfield, D. E. Katz OnlineOpen: This
Finland and Sweden and UK GP-HOSP datasets
 Web appendix: Supplementary material Table 1 Specific diagnosis codes used to identify bladder cancer cases in each dataset Finland and Sweden and UK GP-HOSP datasets Netherlands hospital and cancer registry
Web appendix: Supplementary material Table 1 Specific diagnosis codes used to identify bladder cancer cases in each dataset Finland and Sweden and UK GP-HOSP datasets Netherlands hospital and cancer registry
Clinical Therapeutics/Volume 35, Number 6, 2013 Antimicrobial Stewardship
 Clinical Therapeutics/Volume 35, Number 6, 2013 Antimicrobial Stewardship A Stewardship Program s Retrospective Evaluation of Vancomycin AUC 24 /MIC and Time to Microbiological Clearance in Patients with
Clinical Therapeutics/Volume 35, Number 6, 2013 Antimicrobial Stewardship A Stewardship Program s Retrospective Evaluation of Vancomycin AUC 24 /MIC and Time to Microbiological Clearance in Patients with
Methicillin-Resistant Staphylococcus aureus (MRSA) S urveillance Report 2008 Background Methods
 Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance Report 2008 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services
Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance Report 2008 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services
Cubicin A Guide to Dosing
 Cubicin A Guide to Dosing Cubicin (Daptomycin) powder for solution for injection or infusion Indications (see SmPC) 1 : Cubicin is indicated for the treatment of the following infections (see sections
Cubicin A Guide to Dosing Cubicin (Daptomycin) powder for solution for injection or infusion Indications (see SmPC) 1 : Cubicin is indicated for the treatment of the following infections (see sections
In each hospital-year, we calculated a 30-day unplanned. readmission rate among patients who survived at least 30 days
 Romley JA, Goldman DP, Sood N. US hospitals experienced substantial productivity growth during 2002 11. Health Aff (Millwood). 2015;34(3). Published online February 11, 2015. Appendix Adjusting hospital
Romley JA, Goldman DP, Sood N. US hospitals experienced substantial productivity growth during 2002 11. Health Aff (Millwood). 2015;34(3). Published online February 11, 2015. Appendix Adjusting hospital
Care Guideline DRAFT for review cycle 08/02/17 CARE OF THE ADULT PNEUMONIA PATIENT
 Care Guideline DRAFT for review cycle 08/02/17 CARE OF THE ADULT PNEUMONIA PATIENT Target Audience: All MHS employed providers within Primary Care, Urgent Care, and In-Hospital Care. The secondary audience
Care Guideline DRAFT for review cycle 08/02/17 CARE OF THE ADULT PNEUMONIA PATIENT Target Audience: All MHS employed providers within Primary Care, Urgent Care, and In-Hospital Care. The secondary audience
Augmented Renal Clearance: Let s Get the Discussion Flowing
 Augmented Renal Clearance: Let s Get the Discussion Flowing Terry Makhoul, PharmD PGY-2 Emergency Medicine Pharmacy Resident University of Rochester Medical Center Strong Memorial Hospital Disclosures
Augmented Renal Clearance: Let s Get the Discussion Flowing Terry Makhoul, PharmD PGY-2 Emergency Medicine Pharmacy Resident University of Rochester Medical Center Strong Memorial Hospital Disclosures
Nephrotoxicity. Pros and Cons of the article: Relationship between Initial Vancomycin
 Pros and Cons of the article: Relationship between Initial Vancomycin Nephrotoxicity among Hospitalized Patients Diane M. Cappelletty, Pharm.D. Associate Professor Pharmacy Practice The University of Toledo
Pros and Cons of the article: Relationship between Initial Vancomycin Nephrotoxicity among Hospitalized Patients Diane M. Cappelletty, Pharm.D. Associate Professor Pharmacy Practice The University of Toledo
GSK Medicine: Study Number: Title: Rationale: Study Period: Objectives: Indication: Study Investigators/Centers: Research Methods: Data Source
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
DIABETES ASSOCIATED WITH ANTIPSYCHOTIC USE IN VETERANS WITH SCHIZOPHRENIA
 DIABETES ASSOCIATED WITH ANTIPSYCHOTIC USE IN VETERANS WITH SCHIZOPHRENIA Fran Cunningham, Pharm.D. Department of Veterans Affairs* University of Illinois at Chicago Bruce Lambert, Ph.D. University of
DIABETES ASSOCIATED WITH ANTIPSYCHOTIC USE IN VETERANS WITH SCHIZOPHRENIA Fran Cunningham, Pharm.D. Department of Veterans Affairs* University of Illinois at Chicago Bruce Lambert, Ph.D. University of
Epidemiology of Pneumococcal Disease in a National Cohort of Older Adults
 University of Rhode Island DigitalCommons@URI Pharmacy Practice Faculty Publications Pharmacy Practice 2014 Epidemiology of Pneumococcal Disease in a National Cohort of Older Adults Haley J. Morrill University
University of Rhode Island DigitalCommons@URI Pharmacy Practice Faculty Publications Pharmacy Practice 2014 Epidemiology of Pneumococcal Disease in a National Cohort of Older Adults Haley J. Morrill University
Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia
 Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia Amanda Guth 1 Amy Slenker MD 1,2 1 Department of Infectious Diseases, Lehigh Valley Health Network
Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia Amanda Guth 1 Amy Slenker MD 1,2 1 Department of Infectious Diseases, Lehigh Valley Health Network
Supplementary Online Content
 1 Supplementary Online Content Friedman DJ, Piccini JP, Wang T, et al. Association between left atrial appendage occlusion and readmission for thromboembolism among patients with atrial fibrillation undergoing
1 Supplementary Online Content Friedman DJ, Piccini JP, Wang T, et al. Association between left atrial appendage occlusion and readmission for thromboembolism among patients with atrial fibrillation undergoing
BIOSTATISTICAL METHODS
 BIOSTATISTICAL METHODS FOR TRANSLATIONAL & CLINICAL RESEARCH PROPENSITY SCORE Confounding Definition: A situation in which the effect or association between an exposure (a predictor or risk factor) and
BIOSTATISTICAL METHODS FOR TRANSLATIONAL & CLINICAL RESEARCH PROPENSITY SCORE Confounding Definition: A situation in which the effect or association between an exposure (a predictor or risk factor) and
Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications
 MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
Received 24 August 2010/Returned for modification 7 November 2010/Accepted 7 February 2011
 JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 2011, p. 1583 1587 Vol. 49, No. 4 0095-1137/11/$12.00 doi:10.1128/jcm.01719-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Clinical and
JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 2011, p. 1583 1587 Vol. 49, No. 4 0095-1137/11/$12.00 doi:10.1128/jcm.01719-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Clinical and
Trust Guideline for the Use of Parenteral Vancomycin and Teicoplanin in Adults
 A clinical guideline recommended for use: In: By: For: Division responsible for document: Key words: Names of document authors: Job titles of document authors: Name of document author s Line Manager: Job
A clinical guideline recommended for use: In: By: For: Division responsible for document: Key words: Names of document authors: Job titles of document authors: Name of document author s Line Manager: Job
CARE OF THE ADULT PNEUMONIA PATIENT
 Care Guideline CARE OF THE ADULT PNEUMONIA PATIENT Target Audience: The target audience for this Care Guideline is all MultiCare providers and staff, including those associated with our clinically integrated
Care Guideline CARE OF THE ADULT PNEUMONIA PATIENT Target Audience: The target audience for this Care Guideline is all MultiCare providers and staff, including those associated with our clinically integrated
Risk Factors for Failure of OPAT (Outpatient Parenteral Antimicrobial Therapy) in Veterans with Staphylococcus aureus Bacteremia
 Journal of Pharmacy and Pharmacology 4 (2016) 241-247 doi: 10.17265/2328-2150/2016.06.001 D DAVID PUBLISHING Risk Factors for Failure of OPAT (Outpatient Parenteral Antimicrobial Therapy) in Veterans with
Journal of Pharmacy and Pharmacology 4 (2016) 241-247 doi: 10.17265/2328-2150/2016.06.001 D DAVID PUBLISHING Risk Factors for Failure of OPAT (Outpatient Parenteral Antimicrobial Therapy) in Veterans with
Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure
 Journal of Medical Microbiology (2016), 65, 195 199 DOI 10.1099/jmm.0.000211 Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure Michael A. Lorenz, 1,2 Ryan P. Moenster
Journal of Medical Microbiology (2016), 65, 195 199 DOI 10.1099/jmm.0.000211 Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure Michael A. Lorenz, 1,2 Ryan P. Moenster
Open Forum Infectious Diseases MAJOR ARTICLE
 Open Forum Infectious Diseases MAJOR ARTICLE Efficacy and Safety of Oritavancin Relative to Vancomycin for Patients with Acute Bacterial Skin and Skin Structure Infections (ABSSSI) in the Outpatient Setting:
Open Forum Infectious Diseases MAJOR ARTICLE Efficacy and Safety of Oritavancin Relative to Vancomycin for Patients with Acute Bacterial Skin and Skin Structure Infections (ABSSSI) in the Outpatient Setting:
Chapter 5: Acute Kidney Injury
 Chapter 5: Acute Kidney Injury In 2015, 4.3% of Medicare fee-for-service beneficiaries experienced a hospitalization complicated by Acute Kidney Injury (AKI); this appears to have plateaued since 2011
Chapter 5: Acute Kidney Injury In 2015, 4.3% of Medicare fee-for-service beneficiaries experienced a hospitalization complicated by Acute Kidney Injury (AKI); this appears to have plateaued since 2011
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sutton M, Nikolova S, Boaden R, Lester H, McDonald R, Roland
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sutton M, Nikolova S, Boaden R, Lester H, McDonald R, Roland
Outcomes: Initially, our primary definitions of pneumonia was severe pneumonia, where the subject was hospitalized
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Retention in HIV care predicts subsequent retention and predicts survival well after the first year of care: a national study of US Veterans
 Retention in HIV care predicts subsequent retention and predicts survival well after the first year of care: a national study of US Veterans Thomas P. Giordano, MD, MPH, Jessica A. Davila, PhD, Christine
Retention in HIV care predicts subsequent retention and predicts survival well after the first year of care: a national study of US Veterans Thomas P. Giordano, MD, MPH, Jessica A. Davila, PhD, Christine
Supplementary Online Content
 Supplementary Online Content Gershengorn HB, Scales DC, Kramer A, Wunsch H. Association between overnight extubations and outcomes in the intensive care unit. JAMA Intern Med. Published online September
Supplementary Online Content Gershengorn HB, Scales DC, Kramer A, Wunsch H. Association between overnight extubations and outcomes in the intensive care unit. JAMA Intern Med. Published online September
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Vancomycin Drug Class 1
 Drug Class 1 Antibiotic glycopeptide Spectrum 1 Cross Sensitivities / Allergies 1 Refer to product monograph for complete spectrum Gram positive pathogens (e.g., S. aureus, Enterococcus, S. viridans, methicillinresistant
Drug Class 1 Antibiotic glycopeptide Spectrum 1 Cross Sensitivities / Allergies 1 Refer to product monograph for complete spectrum Gram positive pathogens (e.g., S. aureus, Enterococcus, S. viridans, methicillinresistant
Serious MRSA infection: anything new?
 Serious MRSA infection: anything new? Professor Mark H. Wilcox Leeds Teaching Hospitals & University of Leeds, UK Public Health England & NHS Improvement Potential Conflicts of Interest I have received:
Serious MRSA infection: anything new? Professor Mark H. Wilcox Leeds Teaching Hospitals & University of Leeds, UK Public Health England & NHS Improvement Potential Conflicts of Interest I have received:
Role of Pharmacoepidemiology in Drug Evaluation
 Role of Pharmacoepidemiology in Drug Evaluation Martin Wong MD, MPH School of Public Health and Primary Care Faculty of Medicine Chinese University of Hog Kong Outline of Content Introduction: what is
Role of Pharmacoepidemiology in Drug Evaluation Martin Wong MD, MPH School of Public Health and Primary Care Faculty of Medicine Chinese University of Hog Kong Outline of Content Introduction: what is
Disclosures. Evidence Based Medicine. Infections in SLE and LN Patients. Aim
 Serious Infection Rates among Patients with Systemic Lupus Erythematosus Receiving Corticosteroids and Immunosuppressants None Disclosures Candace H. Feldman, MD, MPH 1,2 Linda T. Hiraki, MD, SM, ScD 3
Serious Infection Rates among Patients with Systemic Lupus Erythematosus Receiving Corticosteroids and Immunosuppressants None Disclosures Candace H. Feldman, MD, MPH 1,2 Linda T. Hiraki, MD, SM, ScD 3
Vancomycin: A 50-something-yearold antibiotic we still don t understand
 Current Drug Therapy CME CREDIT EDUCATIONAL OBJECTIVES: Readers will use vancomycin appropriately Amy Schilling, PharmD Department of Pharmacy, The University of Texas Medical Branch, Galveston Elizabeth
Current Drug Therapy CME CREDIT EDUCATIONAL OBJECTIVES: Readers will use vancomycin appropriately Amy Schilling, PharmD Department of Pharmacy, The University of Texas Medical Branch, Galveston Elizabeth
The University of Mississippi School of Pharmacy
 LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
The impact of vancomycin trough concentrations on outcomes in non-deep seated infections: a retrospective cohort study
 Wan et al. BMC Pharmacology and Toxicology (2018) 19:47 https://doi.org/10.1186/s40360-018-0236-z RESEARCH ARTICLE The impact of vancomycin trough concentrations on outcomes in non-deep seated infections:
Wan et al. BMC Pharmacology and Toxicology (2018) 19:47 https://doi.org/10.1186/s40360-018-0236-z RESEARCH ARTICLE The impact of vancomycin trough concentrations on outcomes in non-deep seated infections:
Abstract. Introduction
 ORIGINAL ARTICLE Comparison of vancomycin and linezolid in patients with peripheral vascular disease and/or diabetes in an observational European study of complicated skin and soft-tissue infections due
ORIGINAL ARTICLE Comparison of vancomycin and linezolid in patients with peripheral vascular disease and/or diabetes in an observational European study of complicated skin and soft-tissue infections due
Population based studies in Pancreatic Diseases. Satish Munigala
 Population based studies in Pancreatic Diseases Satish Munigala 1 Definition Population-based studies aim to answer research questions for defined populations 1 Generalizable to the whole population addressed
Population based studies in Pancreatic Diseases Satish Munigala 1 Definition Population-based studies aim to answer research questions for defined populations 1 Generalizable to the whole population addressed
PubH 7405: REGRESSION ANALYSIS. Propensity Score
 PubH 7405: REGRESSION ANALYSIS Propensity Score INTRODUCTION: There is a growing interest in using observational (or nonrandomized) studies to estimate the effects of treatments on outcomes. In observational
PubH 7405: REGRESSION ANALYSIS Propensity Score INTRODUCTION: There is a growing interest in using observational (or nonrandomized) studies to estimate the effects of treatments on outcomes. In observational
ESCMID Online Lecture Library. by author
 Hospital Universitario Virgen Macarena, Seville New drugs against MRSA and VRE L. Eduardo López Cortés Seville, 8th July Tedizolid Oxazolidinone Ceftaroline // Ceftobiprole 5 th gen cephalosporin Overview
Hospital Universitario Virgen Macarena, Seville New drugs against MRSA and VRE L. Eduardo López Cortés Seville, 8th July Tedizolid Oxazolidinone Ceftaroline // Ceftobiprole 5 th gen cephalosporin Overview
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Chapter 5: Acute Kidney Injury
 Chapter 5: Acute Kidney Injury Introduction In recent years, acute kidney injury (AKI) has gained increasing recognition as a major risk factor for the development of chronic kidney disease (CKD). The
Chapter 5: Acute Kidney Injury Introduction In recent years, acute kidney injury (AKI) has gained increasing recognition as a major risk factor for the development of chronic kidney disease (CKD). The
GSK Medicine: salmeterol, Salmeterol+Fluticasone proprionate, fluticasone propionate, beclomethasone
 GSK Medicine: salmeterol, Salmeterol+Fluticasone proprionate, fluticasone propionate, beclomethasone Study No.: WWE111984/WEUSRTP2640/EPI40528 Title: The Asthma Death Case Control Study (ADCCS): Association
GSK Medicine: salmeterol, Salmeterol+Fluticasone proprionate, fluticasone propionate, beclomethasone Study No.: WWE111984/WEUSRTP2640/EPI40528 Title: The Asthma Death Case Control Study (ADCCS): Association
Learning Objectives 9/9/2013. Hypothesis Testing. Conflicts of Interest. Descriptive statistics: Numerical methods Measures of Central Tendency
 Conflicts of Interest I have no conflict of interest to disclose Biostatistics Kevin M. Sowinski, Pharm.D., FCCP Last-Chance Ambulatory Care Webinar Thursday, September 5, 2013 Learning Objectives For
Conflicts of Interest I have no conflict of interest to disclose Biostatistics Kevin M. Sowinski, Pharm.D., FCCP Last-Chance Ambulatory Care Webinar Thursday, September 5, 2013 Learning Objectives For
Linezolid for treatment of ventilator-associated pneumonia: a cost-effective alternative to vancomycin Shorr A F, Susla G M, Kollef M H
 Linezolid for treatment of ventilator-associated pneumonia: a cost-effective alternative to vancomycin Shorr A F, Susla G M, Kollef M H Record Status This is a critical abstract of an economic evaluation
Linezolid for treatment of ventilator-associated pneumonia: a cost-effective alternative to vancomycin Shorr A F, Susla G M, Kollef M H Record Status This is a critical abstract of an economic evaluation
The Clinical Management of Hospital Acquired Pneumonia. NHS Ayrshire & Arran
 The Clinical Management of Hospital Acquired Pneumonia Dr R G Masterton NHS Ayrshire & Arran What s new in HAP/VAP? Care bundles MRSA VAP Improving outcomes with current antimicrobial New antimicrobials
The Clinical Management of Hospital Acquired Pneumonia Dr R G Masterton NHS Ayrshire & Arran What s new in HAP/VAP? Care bundles MRSA VAP Improving outcomes with current antimicrobial New antimicrobials
Is Hospital Admission Useful for Syncope Patients? Preliminary Results of a Multicenter Cohort
 Is Hospital Admission Useful for Syncope Patients? Preliminary Results of a Multicenter Cohort F. Dipaola, E. Pivetta, G. Costantino, G. Casazza, M.J. Reed, B. Sun, M. Solbiati, F. Barbic, D. Shiffer,
Is Hospital Admission Useful for Syncope Patients? Preliminary Results of a Multicenter Cohort F. Dipaola, E. Pivetta, G. Costantino, G. Casazza, M.J. Reed, B. Sun, M. Solbiati, F. Barbic, D. Shiffer,
Chapter 2: Identification and Care of Patients with CKD
 Chapter 2: Identification and Care of Patients with CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients with CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Searching for Clues in Infectious Diseases
 Disclosure Searching for Clues in Infectious Diseases The speaker has no financial conflicts to disclose as relates to the content of this presentation John Esterly, PharmD, BCPS Northwestern Memorial
Disclosure Searching for Clues in Infectious Diseases The speaker has no financial conflicts to disclose as relates to the content of this presentation John Esterly, PharmD, BCPS Northwestern Memorial
D DAVID PUBLISHING. 1. Introduction. Shannon Inglet 1, Michael Curcio 2 and Lada Radetic 3
 Journal of Pharmacy and Pharmacology 6 (2018) 197-201 doi: 10.17265/2328-2150/2018.03.001 D DAVID PUBLISHING Evaluation of Opioid Reversal with Naloxone before and after Implementation of a Computerized
Journal of Pharmacy and Pharmacology 6 (2018) 197-201 doi: 10.17265/2328-2150/2018.03.001 D DAVID PUBLISHING Evaluation of Opioid Reversal with Naloxone before and after Implementation of a Computerized
Challenges in Therapeutic Drug Monitoring:
 Challenges in Therapeutic Drug Monitoring: Focus on Vancomycin Pharmacodynamics and Pharmacokinetics Katherine Gallaga, PharmD PGY1 Pharmacy Practice Resident CHRISTUS Spohn Health System 1 Pharmacist
Challenges in Therapeutic Drug Monitoring: Focus on Vancomycin Pharmacodynamics and Pharmacokinetics Katherine Gallaga, PharmD PGY1 Pharmacy Practice Resident CHRISTUS Spohn Health System 1 Pharmacist
Assessment of Therapeutic Drug Monitoring of Vancomycin in Elderly Patients According to New Guidelines
 Original Article Clinical Chemistry Ann Lab Med 2014;34:1-6 http://dx.doi.org/10.3343/alm.2014.34.1.1 ISSN 2234-3806 eissn 2234-3814 Assessment of Therapeutic Drug Monitoring of Vancomycin in Elderly Patients
Original Article Clinical Chemistry Ann Lab Med 2014;34:1-6 http://dx.doi.org/10.3343/alm.2014.34.1.1 ISSN 2234-3806 eissn 2234-3814 Assessment of Therapeutic Drug Monitoring of Vancomycin in Elderly Patients
BIOSTATISTICAL METHODS AND RESEARCH DESIGNS. Xihong Lin Department of Biostatistics, University of Michigan, Ann Arbor, MI, USA
 BIOSTATISTICAL METHODS AND RESEARCH DESIGNS Xihong Lin Department of Biostatistics, University of Michigan, Ann Arbor, MI, USA Keywords: Case-control study, Cohort study, Cross-Sectional Study, Generalized
BIOSTATISTICAL METHODS AND RESEARCH DESIGNS Xihong Lin Department of Biostatistics, University of Michigan, Ann Arbor, MI, USA Keywords: Case-control study, Cohort study, Cross-Sectional Study, Generalized
Supplementary Online Content
 Supplementary Online Content Pincus D, Ravi B, Wasserstein D. Association between wait time and 30-day mortality in adults undergoing hip fracture surgery. JAMA. doi: 10.1001/jama.2017.17606 eappendix
Supplementary Online Content Pincus D, Ravi B, Wasserstein D. Association between wait time and 30-day mortality in adults undergoing hip fracture surgery. JAMA. doi: 10.1001/jama.2017.17606 eappendix
Guess or get it right?
 Guess or get it right? Antimicrobial prescribing in the 21 st century Robert Masterton Traditional Treatment Paradigm Conservative start with workhorse antibiotics Reserve more potent drugs for non-responders
Guess or get it right? Antimicrobial prescribing in the 21 st century Robert Masterton Traditional Treatment Paradigm Conservative start with workhorse antibiotics Reserve more potent drugs for non-responders
Original Article INTRODUCTION. Acute Medicine & Surgery 2018; 5: doi: /ams2.316
 Acute Medicine & Surgery 2018; 5: 140 145 doi: 10.1002/ams2.316 Original Article Adherence rate of quality-of-care indicators for Staphylococcus aureus bacteremia is extremely low in Japanese emergency
Acute Medicine & Surgery 2018; 5: 140 145 doi: 10.1002/ams2.316 Original Article Adherence rate of quality-of-care indicators for Staphylococcus aureus bacteremia is extremely low in Japanese emergency
Chapter 2: Identification and Care of Patients With CKD
 Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
9/4/2013. Decision Errors. Hypothesis Testing. Conflicts of Interest. Descriptive statistics: Numerical methods Measures of Central Tendency
 Conflicts of Interest I have no conflict of interest to disclose Biostatistics Kevin M. Sowinski, Pharm.D., FCCP Pharmacotherapy Webinar Review Course Tuesday, September 3, 2013 Descriptive statistics:
Conflicts of Interest I have no conflict of interest to disclose Biostatistics Kevin M. Sowinski, Pharm.D., FCCP Pharmacotherapy Webinar Review Course Tuesday, September 3, 2013 Descriptive statistics:
Therapeutic Dose Monitoring for Linezolid in a Patient with MRSA Pneumonia with Bacteremia in Diabetes Insipidus
 Infect Dis Ther (2016) 5:81 87 DOI 10.1007/s40121-015-0100-z CASE REPORT Therapeutic Dose Monitoring for Linezolid in a Patient with MRSA Pneumonia with Bacteremia in Diabetes Insipidus Yoshihiko Nakamura.
Infect Dis Ther (2016) 5:81 87 DOI 10.1007/s40121-015-0100-z CASE REPORT Therapeutic Dose Monitoring for Linezolid in a Patient with MRSA Pneumonia with Bacteremia in Diabetes Insipidus Yoshihiko Nakamura.
Service Line: Rapid Response Service Version: 1.0 Publication Date: October 25, 2017 Report Length: 60 Pages
 CADTH RAPID RESPONSE REPORT: PEER REVIEW WITH CRITICAL APPRAISAL Linezolid for the Treatment of Infections: A Review of the Clinical and Cost- Effectiveness Service Line: Rapid Response Service Version:
CADTH RAPID RESPONSE REPORT: PEER REVIEW WITH CRITICAL APPRAISAL Linezolid for the Treatment of Infections: A Review of the Clinical and Cost- Effectiveness Service Line: Rapid Response Service Version:
ICU Volume 11 - Issue 3 - Autumn Series
 ICU Volume 11 - Issue 3 - Autumn 2011 - Series Impact of Pharmacokinetics of Antibiotics in ICU Clinical Practice Introduction The efficacy of a drug is mainly dependent on its ability to achieve an effective
ICU Volume 11 - Issue 3 - Autumn 2011 - Series Impact of Pharmacokinetics of Antibiotics in ICU Clinical Practice Introduction The efficacy of a drug is mainly dependent on its ability to achieve an effective
Regional Density Of Cardiologists And Mortality For Acute Myocardial Infarction And Heart Failure
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2014 Regional Density Of Cardiologists And Mortality For Acute
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2014 Regional Density Of Cardiologists And Mortality For Acute
Tuning Epidemiological Study Design Methods for Exploratory Data Analysis in Real World Data
 Tuning Epidemiological Study Design Methods for Exploratory Data Analysis in Real World Data Andrew Bate Senior Director, Epidemiology Group Lead, Analytics 15th Annual Meeting of the International Society
Tuning Epidemiological Study Design Methods for Exploratory Data Analysis in Real World Data Andrew Bate Senior Director, Epidemiology Group Lead, Analytics 15th Annual Meeting of the International Society
ADJUVANT TIGECYCLINE FOR SEVERE CLOSTRIDIUM DIFFICILE-ASSOCIATED DIARRHEA
 ADJUVANT TIGECYCLINE FOR SEVERE CLOSTRIDIUM DIFFICILE-ASSOCIATED DIARRHEA Candace Marr, DO Catholic Health System University at Buffalo, NY Kevin Shiley, MD Catholic Health System Buffalo, NY FINANCIAL
ADJUVANT TIGECYCLINE FOR SEVERE CLOSTRIDIUM DIFFICILE-ASSOCIATED DIARRHEA Candace Marr, DO Catholic Health System University at Buffalo, NY Kevin Shiley, MD Catholic Health System Buffalo, NY FINANCIAL
Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches
 Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ. Disclosures I have served as a consultant to, researcher/investigator
Optimizing Antibiotic Therapy in the ICU For Pneumonia Current and Future Approaches Andrew F. Shorr, MD, MPH Washington Hospital Center Georgetown Univ. Disclosures I have served as a consultant to, researcher/investigator
Pharmacist and Physician Collaborative Practice Model Improves Vancomycin Dosing in an Intensive Care Unit
 International Journal of Clinical Medicine, 2016, 7, 675-684 http://www.scirp.org/journal/ijcm ISSN Online: 2158-2882 ISSN Print: 2158-284X Pharmacist and Physician Collaborative Practice Model Improves
International Journal of Clinical Medicine, 2016, 7, 675-684 http://www.scirp.org/journal/ijcm ISSN Online: 2158-2882 ISSN Print: 2158-284X Pharmacist and Physician Collaborative Practice Model Improves
RESEARCH. Katrina Wilcox Hagberg, 1 Hozefa A Divan, 2 Rebecca Persson, 1 J Curtis Nickel, 3 Susan S Jick 1. open access
 open access Risk of erectile dysfunction associated with use of 5-α reductase inhibitors for benign prostatic hyperplasia or alopecia: population based studies using the Clinical Practice Research Datalink
open access Risk of erectile dysfunction associated with use of 5-α reductase inhibitors for benign prostatic hyperplasia or alopecia: population based studies using the Clinical Practice Research Datalink
RESEARCH. What is already known about this subject
 RESEARCH Comparative Treatment Patterns, Resource Utilization, and Costs in Stimulant-Treated Children with ADHD Who Require Subsequent Pharmacotherapy with Atypical Antipsychotics Versus Non-Antipsychotics
RESEARCH Comparative Treatment Patterns, Resource Utilization, and Costs in Stimulant-Treated Children with ADHD Who Require Subsequent Pharmacotherapy with Atypical Antipsychotics Versus Non-Antipsychotics
had non-continuous enrolment in Medicare Part A or Part B during the year following initial admission;
 Effectiveness and cost-effectiveness of implantable cardioverter defibrillators in the treatment of ventricular arrhythmias among Medicare beneficiaries Weiss J P, Saynina O, McDonald K M, McClellan M
Effectiveness and cost-effectiveness of implantable cardioverter defibrillators in the treatment of ventricular arrhythmias among Medicare beneficiaries Weiss J P, Saynina O, McDonald K M, McClellan M
A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY. Helen Mari Parsons
 A Culture of Quality? Lymph Node Evaluation for Colon Cancer Care A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Helen Mari Parsons IN PARTIAL FULFILLMENT
A Culture of Quality? Lymph Node Evaluation for Colon Cancer Care A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Helen Mari Parsons IN PARTIAL FULFILLMENT
Supplementary Methods
 Supplementary Materials for Suicidal Behavior During Lithium and Valproate Medication: A Withinindividual Eight Year Prospective Study of 50,000 Patients With Bipolar Disorder Supplementary Methods We
Supplementary Materials for Suicidal Behavior During Lithium and Valproate Medication: A Withinindividual Eight Year Prospective Study of 50,000 Patients With Bipolar Disorder Supplementary Methods We
Incidence per 100,000
 Streptococcus pneumoniae Surveillance Report 2005 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services Updated: March 2007 Background
Streptococcus pneumoniae Surveillance Report 2005 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services Updated: March 2007 Background
Risk of serious skin & soft tissue infections in rheumatoid arthritis patients taking anti-tnf drugs.
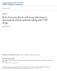 Oregon Health & Science University OHSU Digital Commons Scholar Archive July 2010 Risk of serious skin & soft tissue infections in rheumatoid arthritis patients taking anti-tnf drugs. Ngoc J. Wasson Follow
Oregon Health & Science University OHSU Digital Commons Scholar Archive July 2010 Risk of serious skin & soft tissue infections in rheumatoid arthritis patients taking anti-tnf drugs. Ngoc J. Wasson Follow
An introduction to Quality by Design. Dr Martin Landray University of Oxford
 An introduction to Quality by Design Dr Martin Landray University of Oxford Criteria for a good trial Ask an IMPORTANT question Answer it RELIABLY Quality Quality is the absence of errors that matter to
An introduction to Quality by Design Dr Martin Landray University of Oxford Criteria for a good trial Ask an IMPORTANT question Answer it RELIABLY Quality Quality is the absence of errors that matter to
Optimized Use of Vancomycin
 E-Newsletter #1 Optimized Use of Vancomycin FROM THE EDITOR S DESK Methicillin-resistant Staphylococcus aureus (MRSA) is a serious concern for clinicians managing infectious diseases in the healthcare
E-Newsletter #1 Optimized Use of Vancomycin FROM THE EDITOR S DESK Methicillin-resistant Staphylococcus aureus (MRSA) is a serious concern for clinicians managing infectious diseases in the healthcare
Hospital Transition Management. Barbara Wood, BSN, MBA
 Hospital Transition Management Barbara Wood, BSN, MBA Director, Embedded Care Management Programs OBJECTIVES Improve health care quality for our patients by streamlining care transitions Reduce avoidable
Hospital Transition Management Barbara Wood, BSN, MBA Director, Embedded Care Management Programs OBJECTIVES Improve health care quality for our patients by streamlining care transitions Reduce avoidable
Senior Vice President, Medical Affairs and Health Outcomes, 150 South Saunders Road, Lake Forest, IL 60045, Horizon Pharma USA, Inc, USA
 Research Hyperammonemic crises in patients with urea cycle disorders on chronic nitrogen scavenger therapy with either sodium phenylbutyrate or glycerol phenylbutyrate Jeffrey D Kent 1, Robert J Holt,2
Research Hyperammonemic crises in patients with urea cycle disorders on chronic nitrogen scavenger therapy with either sodium phenylbutyrate or glycerol phenylbutyrate Jeffrey D Kent 1, Robert J Holt,2
Community Acquired & Nosocomial Pneumonias
 Community Acquired & Nosocomial Pneumonias IDSA/ATS 2007 & 2016 Guidelines José Luis González, MD Clinical Assistant Professor of Medicine Outline Intro - Definitions & Diagnosing CAP treatment VAP & HAP
Community Acquired & Nosocomial Pneumonias IDSA/ATS 2007 & 2016 Guidelines José Luis González, MD Clinical Assistant Professor of Medicine Outline Intro - Definitions & Diagnosing CAP treatment VAP & HAP
Risk of serious infections associated with use of immunosuppressive agents in pregnant women with autoimmune inflammatory conditions: cohor t study
 Risk of serious infections associated with use of immunosuppressive agents in pregnant women with autoimmune inflammatory conditions: cohor t study BMJ 2017; 356 doi: https://doi.org/10.1136/bmj.j895 (Published
Risk of serious infections associated with use of immunosuppressive agents in pregnant women with autoimmune inflammatory conditions: cohor t study BMJ 2017; 356 doi: https://doi.org/10.1136/bmj.j895 (Published
Online Supplementary Material
 Section 1. Adapted Newcastle-Ottawa Scale The adaptation consisted of allowing case-control studies to earn a star when the case definition is based on record linkage, to liken the evaluation of case-control
Section 1. Adapted Newcastle-Ottawa Scale The adaptation consisted of allowing case-control studies to earn a star when the case definition is based on record linkage, to liken the evaluation of case-control
