Inborn error of metabolism
|
|
|
- Dorothy Anthony
- 5 years ago
- Views:
Transcription
1
2 Inborn error of metabolism The lecture is given by Dr Kefah Al qa qa, Consultant metabolic pediatrician, in Queen Rania Al Abdulla children hospital, on Thursday 11/12/2014. Let s tart Metabolism: refers to all biochemical processes and pathways in the body. 1. Catabolism (Breaking down): is the set of metabolic pathways that break down molecules into smaller units and release energy. 2. Anabolism (Building up): is the set of metabolic pathways that construct molecules from smaller units. These reactions require energy *Enzymes play an important role in facilitating the process by serving as catalysts in the conversion of one chemical (metabolite) to another Inborn errors of metabolism are usually caused by a single gene defect that causes a block in metabolic pathways; it may lead to abnormality in a receptor, transport vehicle, membrane pump and structural element. Not necessary the inborn error to be an enzyme deficiency, it can be in anything that the DNA code of that protein. All inborn error of metabolic disease is autosomal recessive except those ones which are x-linked: 1- Lesch Nyhan syndrome: it has an association with uric acid metabolism leads to very high uric acid. The baby born healthy, after a period the mother will notice developmental delay. The thing that distinguish them is that they after awhile is self-mutilating behaviors, characterized by lip and finger biting. 2- OTC deficiency(ornithine transcarbamylase deficiency): it is urea cycle defect.it cause primary hyperammonimia usually leads to death bcz it is very difficult to treat. 3- Fabry s disease has an association with joints 4- Hunter s syndrome: mucopolysscaridosis type 2 storage diseases. 5- Menke s disease: it has defect in cupper metabolism; they come with developmental delay, abnormal hair (kinky). It involves renal system, and usually they die. It affects males mainly. Trial to their treatment is cupper supplement but it is not approved yet The principle of inborn error Metabolism Substrate(A) Other substance(b) Enzyme, cofactor "vitamin or mineral" Intermediate metabolite (C)
3 In normal conditions substrate(a) will metabolite to substance (B) in the presence of an enzyme and a cofactor.in IBEOM there will be deficiency in the enzyme or/& the cofactor and this will lead to: 1- accumulation of substrate(a) (mechanism of action of group 3 IBOM) 2- Deficiency of the product (B) 3- The body on trying to get rid of the accumulated substrate it will go to other metabolic pathway so there will be new metabolite and accumulation of them; we call them intermediate metabolite (C). These intermediate metabolite are toxic to the body bcz normally they aren't present in the body. 4- Intermediate metabolite will block another metabolic pathways in the body as urea cycle 5- Toxic metabolite has high affinity to other substance in the body called carnitine which leads to secondary carnitine deficiency. So we give them carnitine maintenance dose to prevent sec deficiency carnitine is carrier for long chain fatty acid to transport them from cytoplasm to mitochondria to metabolite them there is a benefit to this affinity bcz when the metabolite bind to carnitine they become water soluble and can be excreted in urine and this is imp in the treatment when the patient in acute decompansation we increase the dose from 100 to 300g/kg/day In Organic academia and aminoacidopathies the intermediate metabolite will block another metabolic pathways in the body as urea cycle (which detoxify ammonia, converting it to urea excreted in the urine), by inhibition to one of the enzymes that are catalyzing the urea cycle leading to secondary hyperammonemia Before proceeding note that the doctor was showing some pics and she said notes about them, I wrote the notes that the doctor said about each one Group 1: disorders that gives rise to intoxication This group includes inborn errors of metabolism that lead to an acute or progressive intoxication from the accumulation of toxic compounds proximal to the metabolic block (accumulation of substrate or intermediate metabolite) All the conditions in this group share clinical similarities: They do not interfere with the embryo fetal development (not dysmorphic). They present with a symptom-free interval.(born normal 4-5d then started to have hypoactivity, poor feeding. we think of sepsis,and we do septic workup, given IV antibiotic,but the pt continue to deteriorate. in the fetal life they get rid of toxic metabolites by placenta and they need time to build up these toxic again. What determine the time of presentation and severity of s&s is the level of enzyme deficiency. It includes: 1- Amino acid catabolism disorder 2- organic academia 3- congenital urea cycle defect 4- Sugar intolerance (galactosemia). 5- Metal intoxication (menke's diseases) 6- porphyria phenylketonuria *In phenylketonuria the pt may come first with intractable seizure which leads to neuro damage *in phenylketonuria if the patient strict in low protein diet he will not deteriorate. * U can do antenatal detection for the infant and manage the problem
4 Tyrosenimea it has 3 types. In the first type there will be triad "jaundice, rickittis, coagulopathy" but there will not be any dysmorphic features We treat them by one drug nitisinone which inhibits an enzyme (succinyl acetone), in the metabolic pathway of tyrosine on step before production of the toxic metabolite. It is very effective but it is lifelong treatment and it is expensive. It come as capsule 2mg, 26 JOD each. The coagulopathy will improve in 24 h, liver back to normal in 48 h maple syrup urine disease also called branched chain ketoaciduria affect brach chained amin acids (leucine, isolucine, valine) ** may cause encephalopathy Most of the organioacacedime cause encephalopathy due to accumulation of ammonia except this one which cause encephalopathy due to Lucien accumulation And it is difficult to treat. Tyrosinemia 2 *We call it oculocutaneous *They came with sensitivity to light and hyperkeratic lesion on the sole, palms. In the past was diagnosed herpetic keratitis but herpetic keratitis is unilateral while tyrosinemia is bilateral We put them in low phynelalanin and tyrosine diet they improve in 2-10 w for the eye manifestation but skin manifestation takes months Clinical signs of intoxication may be: 1- Acute: *vomiting. *Coma. *liver failure. *thromboembolic complications. 2- Chronic: *failure to thrive. * developmental delay. *ectopia lentis. *cardiomyopathy Acute decompansation **It means increase catabolic rate, which leads to increase substrate accumulation >>more toxic metabolites >> more inhibition to urea cycle >>> more deficiency of carnitine. This is important in the treatment; bcz the treatment goal is to stop catabolism. **It is usually provoked by (stress): 1- Fever. 2- intercurrent illness. 3- Food intake. **Most of these disorders are treatable and require the emergency removal of the toxin. **Nutritional therapy is the backbone of the treatment in this group. **Pharmacological doses of vitamins have also shown remarkable efficiency in vitamin-responsive disorders: Ex: Propionic acidemia >>we add (V.B 7) which is the cofactor, Methylmalonic acidemia >> (B12).if I don t know the diagnose I give multi vitamins
5 Group 2: Disorders involving energy metabolism (most difficult group) These consist of inborn errors of metabolism with symptoms due to a deficiency in energy production or utilization within liver, myocardium, muscle, brain or other tissues. This group can be divided into: 1- Mitochondrial defects: -most severe -diff to diagnose -present at any age -usually untreateble. -involve any system in the body -no specific s&s They include: -Congenital lactic acidemias:(pc,pd,). -Mitochondrial resp chain defects. -Fatty acid oxidation defects. -Ketone body defects 2- Cytoplasmic energy defects: Usually less severe. - Could be: 1- treatable : disorders of glycolysis,gsd (glycogen storage ), gluconeogenesis and hyperinsulinism. 2-partly treatable: creatine metabolism. 3- untreatable: pentose phosphate pathway Common symptoms include: 1-hypoglycemia. 2-Hyperlactatemia. 3- Hepatomegaly. 4- Hypotonia. 5-Myopathy and cardiomyopathy. 6- FTT. 7- Sudden un expected death. 8-Some mitochondrial may interfer with embryo-fetal development leading to dysmorphism.(but not for diagnosis) Biotin deficiency **Symptoms include: Loss of hair, severe eczema, academia, seizure **"Anticonvulsant therapy: Prolonged use of certain drugs, may lead to biotin deficiency; however, valproic acid therapy is less likely to cause this condition. Some anticonvulsant inhibit biotin transport across the intestinal mucosa. Evidence suggests that these anticonvulsants accelerate biotin catabolism. Therefore, supplemental biotin, in addition to the usual minimum daily requirements, has been suggested for patients who are treated with anticonvulsants that have been linked to biotin deficiency".wiki but some are said by the doctor **treated by given Biotine 5mg *2!!
6 Glycogen storage disease type1 Clinical picture: *Recurrent hypoglycemia, huge hepatomegaly, Elevate liver enzyme but not as in hepatitis, Hyperlipedimia, triglycridemia, hyperlactetimia *Recurrent attack of nasal bledding >>defect in platelet function not number *PT, PTT, INR is normal unless the patient is septic *The bleeding time is prolonged *They are short stature, but we don t give them growth hormone, bcz it is not effective *Liable to hyperthyroidism! Treated by: 1- lactose, glucose, fructose free 2- uncooked corn starch ( bcz they are catabolized to glucose slowly ) 3- Liver transplant not effect (We do transplant to type 4 only) There are 2 forms of type 1: -A -B>> u find neutropenia Group 3: Disorders involving complex molecules This group involves cellular organelles and includes diseases that disturb the synthesis or the catabolism of complex molecules. Symptoms are: 1- progressive. 2- permanent. 3- Independent of intercurrent events (not affected by current infections >> not go to acute decompansation) 4- Unrelated to food intake. This group includes: 1- All lysosomal storage disorders. 2- Peroxisomal disorders. 3- α1-antitrypsin. 4- Carbohydrate deficient glycoprotein (CDG) syndrome. 5- Inborn errors of cholesterol synthesis. Treatment for some of these disorders is available: 1- Enzyme replacement therapy: for several lysosomal disorders such as Gaucher and Fabry diseases and MPS. 2- Organ transplantation.(bone marrow) 3- Gene therapy. Mucoplysacaridosis Type 1(hurler) *They have: Hypertelorism, depressed nasal bridge, Short stature broad flexion deformity *After awhile excess body Hair, The eye's cornea often becomes cloudy from intracellular storage. Type6: Maroteaux-lamy syndrome They die bcz of cardiopulmonary complication Treatment: enzyme replacement. But it is expensive, lifelong (every week given an injection)
7 Clinical pointers towards an underlying IEM include: Deterioration after a period of apparent normalcy. Parental consanguinity. Family history of neonatal deaths. (cp) Rapidly progressive encephalopathy and seizures of unexplained cause Severe metabolic acidosis Persistent vomiting with metabolic acidosis bcz in other problems they be with alkalosis Special smells to some disorders: Musty or Mousy: PKU Boiled Cabbage Tyrosinemia or hypermethioninemia Maple Syrup maple syrup urine disease(most ccc) Sweaty feet: isovaleric acidemia or glutaric acidemia type II Cat urine multiple carboxylase deficiencies (Biotin deficiency) Times when presentation of inherited metabolic disease is more likely (when there are metabolic stress): 1- Neonatal period 2- Weaning Increased oral intake for example, increased protein load. First exposure to new diet component for example, fructose. 3- End of first year Slowing in growth rate means more protein is catabolised for same Protein intake, thus putting greater load on these pathways. 4- Infection Increased metabolic stress often associated with decreased intake for example, vomiting, diarrhoea. 5- Puberty Alterations in growth rate, hormonal changes. 6- Postnatal Urea cycle defect previously asymptomatic - involution of placenta equates to a signifi cant protein load. Inborn error can be divided into: -treatable (to start medication as early as possible) -untreatable (genetic counseling) First line investigations (metabolic screen): The following tests should be obtained in all babies with suspected IEM. 1- Complete blood count: (neutropenia and thrombocytopenia ).(acidosis>>bone marrow supression>>pancytopnia) 2- Arterial blood gases and electrolytes.(with chloride and electrolyte to calculate anion gap) 3- ammonia, lactate diarrhea normal anion gap: renal tubular acidosis Metabolic acidosis ketoacidosis increased anion gap (usually lactic acidosis organic acidopathy
8 Other things that those patients will have: Hypoglycemia -definition: Blood glucose < 2.6 mmol/l (45 mg/dl) at all ages To approach hypoglycemia we need critical sample",in this sample we ll take things that would help us in diagnose * for endocrine causes : Growth hormone, cortisone, ACTH, insulin, C-peptide *and we should also look for ketone bodies : I-high ketone bodies ( ketotic hypoglycemia ), found in : 1. GSD 1 ( glycogen storage disease type 1 ) 2. Gluconeogenetic defect 3. Carbohydrate intolerance 4. Organic academia 5. Adrenal / pituitary problems II-not-ketotic hypoglycemia, found in : 1. Hyperinsulism 2. Fat oxidation defect *** if it s negative for ketone bodies, then I should look for the level of insulin: if high hyperinsulinemia. normal fatty acid oxidation defect (FAOD). at first : I prepare glucose 10% and I give it for the patient to prevent convulsions. Hyperammonemia We should know the normal values of Plasma ammonia NH3 1-Neonates: -Healthy<110μmol/l -Sick ( septic) up to 180 μmol/l : but when the pt. recover we should recheck it to make sure that it s back to normal -Suspect metabolic disease >200 umol/l 2-After the neonatal period : μmol/l at any time if it s >100 then we should role out IEOM. -Suspect metabolic disease >100 umol/l Hyperlactemia CAUSES OF HYPERAMMONEMIA: 1-primary = Urea cycle defect. 2-secondary : A- wrong sampling : the most important one because ammonia concentration inside the cells is 10x the ammonia conc. in the serum.so if the sample was taken improperly (didn t put it in ice, water) there will be hemolysis of the RBCs > ammonia is out of the cells > gives false high reading. B-liver disease. C- metabolic diseases e.g. organic acidemias and FAOD. D - Sepsis. - Arterial blood lactate Normal values: * Blood <2.1 mmol/l (<19 mg/dl) * CSF <1.8 mmol/l (<16 mg/dl).-> ( sometimes we are highly suspicious that there is mitochondrial disease in which you ll find lactic acidemia, absence of it doesn t rule out mitochondrial diseases but the lactate in the CSF will be high in patients with mitochondrial disease ). Primary lactic acidosis Remember that they are in general metabolic diseases: Amino acid disorders. Organic acidemias. Urea cycle defects. Pyruvate metabolism defects. Krebs cycle defects. Mitochondrial OXPHOS disorders. Fatty acid oxidation disorders. Disorders of liver glycogen metabolism. Disorders of liver gluconeogenesis. Biotinidase deficiency - if a patient has convulsion we don t do investigations if he still uncontrolled,because the convulsion is an exercise so it will raise the lactate level Secondary lactic acidosis Remember-> anything that cause decrease in perfusion or decrease in oxygenation: Poor collection technique. Exercise. *Hypoxia Hypotension Shock Sepsis Cardiac failure/cardiomyopathy Renal failure Short bowel syndrome (D-lactate) Thiamine deficiency.
9 Other tests: -Liver function tests : like in glycogen disease, liver enzymes will be high + hyperlipidemia. -Urine ketones - Urine reducing substances : for galactosemia. - Serum uric acid (low in molybdenum cofactor deficiency). Second line investigations 1-blood: -Aminoacid -chromatography. -Acylcarnitine profile. -Lactate /pyruvate ratio. -VLCFA( very long chain fatty acid ) 3-Enzyme assay: This is required for definitive diagnosis, but we can t do it for all patients because it needs skin fibroblasts or liver biopsy for enzyme assay. 2-Urine: *Ketones *DNPH (Dinitrophenylhydrazine) : this test is important for patients of maple syrup urine disease -if the mother felt that her son isn t doing well, she uses a dipstick and put it in a urine sample from her son so as to know if he is started to have acute decompansation or not. *reducing substances. *Organic acid chromatography. *Orotic acid : important to distinguish between the types of enzyme deficiency in the urea cycle. 8-CSF : 1-Aminoacid analysis: CSF Glycine levels are elevated in NKH. 2- CSF glucose to plasma glucose ratio for the diagnosis of GLUT defects. 3-CSF lactate. 4- GABA and other neurotransmitters : some metabolic disorders will cause defect in the neurotransmitters 4-Neuroimaging: MRI may provide helpful pointers towards etiology while results of definitive investigations are pending. - for patients with leukodystrophy,because most of the metabolic diseases cause leukodystrophy. Some IEM may be associated with structural malformations such as Agenesis of corpus callosum brainstem and cerebellar edema, basal ganglia signal change, subdural hematoma and frontotemporal atrophys. 5-Magnetic resonance spectroscopy (MRS): -similar to MRI -they use the spectroscope that can detect the concentration of certain metabolites like : 1- lactate peak elevated in mito-chondrial disorders. 2- leucine peak elevated in MSUD (maple syrup urine disease). 6-Electroencephalography (EEG): some EEG abnormalities may be suggestive of particular IEM e.g. : 1-Comb-like rhythm in MSUD. 2- Burst suppression in : NKH (non-ketotic hyperglycemia). Holocarboxylase synthetase deficiency 7-Mutation analysis when available: to know the types of mutations that we have, to do perinatal diagnosis.. so we ll be anticipating that we ll have affected newborn if the family decided to keep the baby (didn t choose abortion ), so I ll do tests immediately, start him on treatment so as to prevent convulsions, encephalopathy and neurological deficit
10 And now test yourself - Urea cycle defect is the only one of IEOM IE to come with respiratory alkalosis, but if the pt. had brain hypoxia and he came with th sepsis,it might change to metabolic alkalosis because of Hyperlactemia due to hyperperfusion or hypo-oxygenation oxygenation. - Hyperinsulinemia won t come with metabolic acidosis. * Notes : -Limitation Limitation of substrate intake : In aminoacidopathies, organic academia and galactosemia we give the patients formula that doesn t have the substrate that causes the problems. - or we give the enzyme ( as a drug or by organ transplant ). - Supplement product: like in Biotinidase deficiency.. We give biotin in as a treatment. - Gene therapy: it s on the enzyme..but but there are only studies, still there is no prove on it. - If the toxic metabolites causes inhibition of other pathways, we give a treatment to suppress this inhibition. The end شكرا جزيال 9 yaqeen
INBORN ERRORS OF METABOLISM (IEM) IAP UG Teaching slides
 INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
Metabolic Disorders. Chapter Thomson - Wadsworth
 Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
The spectrum and outcome of the. neonates with inborn errors of. metabolism at a tertiary care hospital
 The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
Inborn Errors of Metabolism (IEM)
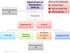 Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition
 Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Training Syllabus CLINICAL SYLLABUS
 Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
Training Syllabus CLINICAL SYLLABUS SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated July 2006 This syllabus is intended as a guide. Whilst the training should be comprehensive,
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis)
 Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Metabolic Changes in ASD. Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius
 Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet
 Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet Website:www.tipn.org.tw Telephone:(02)85962050 Ext. 401-403 Service line:(02)85962065 Fax:(02)85962067
Newborn screening for congenital metabolic diseases Optional out-of-pocket tests Information Sheet Website:www.tipn.org.tw Telephone:(02)85962050 Ext. 401-403 Service line:(02)85962065 Fax:(02)85962067
Module : Clinical correlates of disorders of metabolism Block 3, Week 2
 Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Medical Foods for Inborn Errors of Metabolism
 Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE
 SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
SYLLABUS FOR TRAINING IN CLINICAL PAEDIATRIC METABOLIC MEDICINE Updated December 2014: Vassili Valayannopoulos and Andrew Morris Paediatrics is an independent medical specialty based on the knowledge and
Inborn Errors of Metabolism in the Emergency Department. Will Davies June 2014
 Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children
 National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD
 Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology
 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology 1 PBL SEMINAR ACUTE & CHRONIC ETHANOL EFFECTS An Overview Sites
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology 1 PBL SEMINAR ACUTE & CHRONIC ETHANOL EFFECTS An Overview Sites
HEREDITARY METABOLIC DISEASES
 HEREDITARY METABOLIC DISEASES Particular risk factors are: Advanced maternal age (e.g. Down's syndrome) Family history of inherited diseases (e.g. fragile X syndrome, Huntington's chorea) Previous child
HEREDITARY METABOLIC DISEASES Particular risk factors are: Advanced maternal age (e.g. Down's syndrome) Family history of inherited diseases (e.g. fragile X syndrome, Huntington's chorea) Previous child
Introduction to Organic Acidemias. Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.
 Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism
 Indian J Pediatr (July 2011) 78(7):854 859 DOI 10.1007/s12098-011-0422-0 SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika
Indian J Pediatr (July 2011) 78(7):854 859 DOI 10.1007/s12098-011-0422-0 SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Acute Management of Sick Infants with Suspected Inborn Errors of Metabolism Neerja Gupta Madhulika
Metabolic diseases of the liver
 Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
ACUTE & CHRONIC ETHANOL EFFECTS An Overview
 ACUTE & CHRONIC ETHANOL EFFECTS An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Clinical Biochemistry: PBL Seminar MBBS Yr 4 VJ Temple
ACUTE & CHRONIC ETHANOL EFFECTS An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Clinical Biochemistry: PBL Seminar MBBS Yr 4 VJ Temple
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting
 Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Inborn errors of metabolism
 ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism
 Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Fatty Acid Oxidation Disorders
 Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social
Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social
Inborn Errors of Metabolism Clinical Approach to Diagnosis and Treatment
 Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
Case Scenario: 15 year old girl presented in ED with aggressive behaviour and hallucinations. No associated fever, vomiting, seizures or developmental concerns Previously well Inborn Errors of Metabolism
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE
 THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT
 Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Newborn Screening: Blood Spot Disorders
 Newborn Screening: Blood Spot Disorders Arizona s Newborn Screening Program Program Overview Panel of Disorders Disorder Descriptions Program Components Hospitals ADHS Lab ADHS Follow-up ADHS Billing Medical
Newborn Screening: Blood Spot Disorders Arizona s Newborn Screening Program Program Overview Panel of Disorders Disorder Descriptions Program Components Hospitals ADHS Lab ADHS Follow-up ADHS Billing Medical
7 Medical Genetics. Hemoglobinopathies. Hemoglobinopathies. Protein and Gene Structure. and Biochemical Genetics
 SESSION 7 Medical Genetics Hemoglobinopathies and Biochemical Genetics J a v a d F a s a J a m s h i d i U n i v e r s i t y o f M e d i c a l S c i e n c e s, N o v e m b e r 2 0 1 7 Hemoglobinopathies
SESSION 7 Medical Genetics Hemoglobinopathies and Biochemical Genetics J a v a d F a s a J a m s h i d i U n i v e r s i t y o f M e d i c a l S c i e n c e s, N o v e m b e r 2 0 1 7 Hemoglobinopathies
Urea Cycle Defects. Dr Mick Henderson. Biochemical Genetics Leeds Teaching Hospitals Trust. MetBioNet IEM Introductory Training
 Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese. DOI: /neo.
 Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese Neoreviews 2008;9;e291 DOI: 10.1542/neo.9-7-e291 The online version of this article, along
Testing Strategy for Inborn Errors of Metabolism in the Neonate Aditi I. Dagli, Roberto T. Zori and Bryce A. Heese Neoreviews 2008;9;e291 DOI: 10.1542/neo.9-7-e291 The online version of this article, along
Childhood epilepsy: the biochemical epilepsies. Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary
 Childhood epilepsy: the biochemical epilepsies Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary Definitions Epileptic Seizure Manifestation(s) of epileptic (excessive and/or
Childhood epilepsy: the biochemical epilepsies Dr Colin D Ferrie Consultant Paediatric Neurologist Leeds General Infirmary Definitions Epileptic Seizure Manifestation(s) of epileptic (excessive and/or
Newborn Screening in Manitoba. Information for Health Care Providers
 Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up
 HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
Glycogen Storage Disease
 Glycogen Storage Disease 1 Introduction The food we eat is usually used for growth, tissue repair and energy. The body stores what it does not use. Excess sugar, or glucose, is stored as glycogen in the
Glycogen Storage Disease 1 Introduction The food we eat is usually used for growth, tissue repair and energy. The body stores what it does not use. Excess sugar, or glucose, is stored as glycogen in the
Methylmalonic aciduria
 Methylmalonic aciduria Introductory information Written by: F. Hörster, S. Kölker & P. Burgard Reviewed & Revised for North America by: S. van Calcar Methylmalonic aciduria MMA 2 Methylmalonic aciduria
Methylmalonic aciduria Introductory information Written by: F. Hörster, S. Kölker & P. Burgard Reviewed & Revised for North America by: S. van Calcar Methylmalonic aciduria MMA 2 Methylmalonic aciduria
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
So Much More Than The PKU Test
 Newborn Metabolic Screening So Much More Than The PKU Test Sarah Viall, MSN, PPCNP BC Newborn Screening Program Coordinator Division of Genetics & Metabolism Conflicts of Interest I have no conflicts of
Newborn Metabolic Screening So Much More Than The PKU Test Sarah Viall, MSN, PPCNP BC Newborn Screening Program Coordinator Division of Genetics & Metabolism Conflicts of Interest I have no conflicts of
Inborn Errors of Metabolism
 30 Inborn Errors of Metabolism Inborn errors of metabolism (IEM) are disorders in which there is a block in the normal metabolic pathway that is caused by a genetic defect of a specific enzyme. The number
30 Inborn Errors of Metabolism Inborn errors of metabolism (IEM) are disorders in which there is a block in the normal metabolic pathway that is caused by a genetic defect of a specific enzyme. The number
Metabolic Emergencies and the Pediatrician
 Metabolic Emergencies and the Pediatrician Stephen G. Kahler, MD Professor of Pediatrics Section of Genetics and Metabolism, UAMS and ACH Hot Springs, AR March 8, 2012 INHERITED METABOLIC DISORDERS HOW
Metabolic Emergencies and the Pediatrician Stephen G. Kahler, MD Professor of Pediatrics Section of Genetics and Metabolism, UAMS and ACH Hot Springs, AR March 8, 2012 INHERITED METABOLIC DISORDERS HOW
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE. Bwee Tien Poll-The Amsterdam UMC The Netherlands
 CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
Presentation and investigation of mitochondrial disease in children
 Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Inborn Error Of Metabolism :
 Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
Inborn Error Of Metabolism : Inborn Error Of Metabolism inborn error of metabolism are a large group of hereditary biochemical diseases in which specific gene mutation cause abnormal or missing proteins
THIAMINE TRANSPORTER TYPE 2 DEFICIENCY
 THIAMINE TRANSPORTER TYPE 2 DEFICIENCY WHAT IS THE THIAMINE TRANSPORTER TYPE 2 DEFICIENCY (hthtr2)? The thiamine transporter type 2 deficiency (hthtr2) is a inborn error of thiamine metabolism caused by
THIAMINE TRANSPORTER TYPE 2 DEFICIENCY WHAT IS THE THIAMINE TRANSPORTER TYPE 2 DEFICIENCY (hthtr2)? The thiamine transporter type 2 deficiency (hthtr2) is a inborn error of thiamine metabolism caused by
Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff
 Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
Training Syllabus LABORATORY SYLLABUS Syllabus for Training in Inborn Errors of Metabolism for Scientists and Medically Qualified Laboratory Staff This syllabus is intended as a guide. Whilst the training
ANATOMY OF A METABOLIC CRISIS: FAOD-style. Mark S. Korson, MD Tufts Medical Center Boston, MA
 ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
Nutritional Management of Inborn Errors of Metabolism. Kay Davis, RD, CSP Esther Berenhaut, RD, CSP, CSR Aug 28, 2017
 Nutritional Management of Inborn Errors of Metabolism Kay Davis, RD, CSP Esther Berenhaut, RD, CSP, CSR Aug 28, 2017 OBJECTIVES Brief overview of newborn screening of metabolic disorders, inheritance patterns.
Nutritional Management of Inborn Errors of Metabolism Kay Davis, RD, CSP Esther Berenhaut, RD, CSP, CSR Aug 28, 2017 OBJECTIVES Brief overview of newborn screening of metabolic disorders, inheritance patterns.
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015
 Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review -
 Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
The laboratory investigation of lactic acidaemia. J Bonham/T Laing
 The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center
 Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center Kefah Al-Qa qa MD*, Wajdi Amayreh MD*, Ali Al-Hawamdeh MD* ABSTRACT Objective: To describe the different
Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center Kefah Al-Qa qa MD*, Wajdi Amayreh MD*, Ali Al-Hawamdeh MD* ABSTRACT Objective: To describe the different
Nutritional Interventions in Primary Mitochondrial Disorders
 Nutritional Interventions in Primary Mitochondrial Disorders Carolyn J Ellaway MBBS PhD FRACP CGHGSA Genetic Metabolic Disorders Service Sydney Children s Hospital Network Disciplines of Child and Adolescent
Nutritional Interventions in Primary Mitochondrial Disorders Carolyn J Ellaway MBBS PhD FRACP CGHGSA Genetic Metabolic Disorders Service Sydney Children s Hospital Network Disciplines of Child and Adolescent
NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA
 NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS NEONATAL HYPOGLYCEMIA? Glucose concentration low enough to cause signs and symptoms of impaired brain
NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS NEONATAL HYPOGLYCEMIA? Glucose concentration low enough to cause signs and symptoms of impaired brain
The breakdown of fats to provide energy occurs in segregated membrane-bound compartments
 CPT1a deficiency The breakdown of fats to provide energy occurs in segregated membrane-bound compartments of the cell known as mitochondria. Carnitine palmitoyltransferase Ia (CPT1a) is a protein that
CPT1a deficiency The breakdown of fats to provide energy occurs in segregated membrane-bound compartments of the cell known as mitochondria. Carnitine palmitoyltransferase Ia (CPT1a) is a protein that
ESPEN Congress Madrid 2018
 ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable
 Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable Marshall L. Summar, M.D. Chief, Division of Genetics and Metabolism Children s National Medical Center Washington, DC, USA Disclosure
Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable Marshall L. Summar, M.D. Chief, Division of Genetics and Metabolism Children s National Medical Center Washington, DC, USA Disclosure
Isovaleric Acidemia: Quick reference guide
 Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Fatty Acid Oxidation Disorders
 Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social
Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social
Metabolism. Chapter 5. Catabolism Drives Anabolism 8/29/11. Complete Catabolism of Glucose
 8/29/11 Metabolism Chapter 5 All of the reactions in the body that require energy transfer. Can be divided into: Cell Respiration and Metabolism Anabolism: requires the input of energy to synthesize large
8/29/11 Metabolism Chapter 5 All of the reactions in the body that require energy transfer. Can be divided into: Cell Respiration and Metabolism Anabolism: requires the input of energy to synthesize large
For Your Baby s Health Department of Health
 Newborn Screening For Your Baby s Health Department of Health Why is my baby tested? To help make sure your baby will be as healthy as possible. The blood test provides important information about your
Newborn Screening For Your Baby s Health Department of Health Why is my baby tested? To help make sure your baby will be as healthy as possible. The blood test provides important information about your
Paediatric Clinical Chemistry
 Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Paediatric Clinical Chemistry Dr N Oosthuizen Dept Chemical Pathology UP 2011 Paediatric biochemistry The child is not a miniature adult Physiological development Immature organ systems Growing individual
Hypoglycaemia of the neonate. Dr. L.G. Lloyd Dept. Paediatrics
 Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Overview. o Limitations o Normal regulation of blood glucose o Definition o Symptoms o Clinical forms o Pathophysiology o Treatment.
 Pål R. Njølstad MD PhD KG Jebsen Center for Diabetes Research University of Bergen, Norway Depertment of Pediatrics Haukeland University Hospital Broad Institute of Harvard & MIT Cambridge, MA, USA Hypoglycemia
Pål R. Njølstad MD PhD KG Jebsen Center for Diabetes Research University of Bergen, Norway Depertment of Pediatrics Haukeland University Hospital Broad Institute of Harvard & MIT Cambridge, MA, USA Hypoglycemia
PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS
 PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS SPECIFIC WAYS OF AMINO ACID CATABOLISM After removing of amino group the carbon skeletons of amino acids are transformed into metabolic
PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS SPECIFIC WAYS OF AMINO ACID CATABOLISM After removing of amino group the carbon skeletons of amino acids are transformed into metabolic
Fatty Acid Oxidation Disorders Organic Acid Disorders
 Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial,
Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial,
Fatty Acid Oxidation Disorders- an update. Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London
 Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Metabolism of pentoses, glycogen, fructose and galactose. Jana Novotna
 Metabolism of pentoses, glycogen, fructose and galactose Jana Novotna 1. The Pentose Phosphate Pathway The pentose phosphate pathway (PPP): (hexose monophosphate or 6-phosphogluconate patway) Process that
Metabolism of pentoses, glycogen, fructose and galactose Jana Novotna 1. The Pentose Phosphate Pathway The pentose phosphate pathway (PPP): (hexose monophosphate or 6-phosphogluconate patway) Process that
Hypoglycemia in congenital hyperinsulinism
 How a normal body works: Our body is constantly at work. Our cells need a source of energy, and this source of energy is called glucose. The process is quite simple; think of it like an assembly line.
How a normal body works: Our body is constantly at work. Our cells need a source of energy, and this source of energy is called glucose. The process is quite simple; think of it like an assembly line.
BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona
 BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona BIOTIN (BIOTINIDASE) DEFICIENCY biotin in the body is recycled by its removal from carboxylase enzymes to which it is attached
BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona BIOTIN (BIOTINIDASE) DEFICIENCY biotin in the body is recycled by its removal from carboxylase enzymes to which it is attached
Neonatal Guidelines. Chapter 10: Metabolic V Date Revised : January 2017 Ratified 6 th February Date for Review: 1 st of March 2021
 Neonatal Guidelines Chapter 10: Metabolic V2017.1 Specialty: Neonatal Medicine Revised by: Jean Matthes Date Revised : January 2017 Ratified 6 th February 2017 Approved by: ABMU Joint Perinatal Forum Date
Neonatal Guidelines Chapter 10: Metabolic V2017.1 Specialty: Neonatal Medicine Revised by: Jean Matthes Date Revised : January 2017 Ratified 6 th February 2017 Approved by: ABMU Joint Perinatal Forum Date
Prevalence of selected disorders of inborn errors of metabolism in suspected cases at a Tertiary Care Hospital in Karachi
 Original Article Prevalence of selected disorders of inborn errors of metabolism in suspected cases at a Tertiary Care Hospital in Karachi Hema Satwani, 1 Jamal Raza, 2 Junji Hanai, 3 Shosuke Nomachi 4
Original Article Prevalence of selected disorders of inborn errors of metabolism in suspected cases at a Tertiary Care Hospital in Karachi Hema Satwani, 1 Jamal Raza, 2 Junji Hanai, 3 Shosuke Nomachi 4
UREA CYCLE DISORDERS - The What, Why, How and When
 UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
Lipid Metabolism. Remember fats?? Triacylglycerols - major form of energy storage in animals
 Remember fats?? Triacylglycerols - major form of energy storage in animals Your energy reserves: ~0.5% carbs (glycogen + glucose) ~15% protein (muscle, last resort) ~85% fat Why use fat for energy? 1 gram
Remember fats?? Triacylglycerols - major form of energy storage in animals Your energy reserves: ~0.5% carbs (glycogen + glucose) ~15% protein (muscle, last resort) ~85% fat Why use fat for energy? 1 gram
ESPEN Congress Madrid 2018
 ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Inborn errors of carbohydrate metabolism G. Pintos (ES) INBORN ERRORS OF METABOLISM INBORN ERRORS OF CARBOHYDRATE METABOLISM Guillem Pintos-Morell,
ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Inborn errors of carbohydrate metabolism G. Pintos (ES) INBORN ERRORS OF METABOLISM INBORN ERRORS OF CARBOHYDRATE METABOLISM Guillem Pintos-Morell,
Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when
 CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
Summary. Syndromic versus Etiologic. Definitions. Why does it matter? ASD=autism
 Summary It is becoming clear that multiple genes with complex interactions underlie autism spectrum (ASD). A small subset of people with ASD, however, actually suffer from rare single-gene Important to
Summary It is becoming clear that multiple genes with complex interactions underlie autism spectrum (ASD). A small subset of people with ASD, however, actually suffer from rare single-gene Important to
The Digestive System and Body Metabolism
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Digestive System and Body Metabolism 14PART D Metabolism Chemical reactions necessary to maintain
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Digestive System and Body Metabolism 14PART D Metabolism Chemical reactions necessary to maintain
Current Management and Future Developments in Metabolic Disease
 Current Management and Future Developments in Metabolic Disease APAGBI Annual Scientific Meeting Friday 15 th May 2015 Dr Saikat Santra Birmingham Children s Hospital, UK Outline Metabolic disorders in
Current Management and Future Developments in Metabolic Disease APAGBI Annual Scientific Meeting Friday 15 th May 2015 Dr Saikat Santra Birmingham Children s Hospital, UK Outline Metabolic disorders in
Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine
 Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine Harvey Levy, MD Mark Korson, MD Piero Rinaldo, MD, PhD Larry Sweetman, PhD K. Michael Gibson, PhD Charlie Roe, MD Jerry
Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine Harvey Levy, MD Mark Korson, MD Piero Rinaldo, MD, PhD Larry Sweetman, PhD K. Michael Gibson, PhD Charlie Roe, MD Jerry
Metabolic Disorders Screened Overseas but not Screened in Australia Condition Features Inherited Diagnosis Treatment Newborn Screen
 Metabolic Disorders ed Overseas but not ed in Australia Biotinidase Deficiency Severe form causes seizures & delay Biotin can prevent complications NZ, USA Tyrosinaemia Type I Coma & death before age 10
Metabolic Disorders ed Overseas but not ed in Australia Biotinidase Deficiency Severe form causes seizures & delay Biotin can prevent complications NZ, USA Tyrosinaemia Type I Coma & death before age 10
Organic Acid Disorders
 Genetic Fact Sheets for Parents Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
Genetic Fact Sheets for Parents Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
Physiology 12. Metabolism. Metabolism. Cellular metabolism. The synthesis and Breakdown of organic molecules required for cell structure and function
 Physiology 12 Cellular metabolism Germann Ch3 Metabolism The synthesis and Breakdown of organic molecules required for cell structure and function Metabolism Anabolism = Synthesis Catabolism = Breaking
Physiology 12 Cellular metabolism Germann Ch3 Metabolism The synthesis and Breakdown of organic molecules required for cell structure and function Metabolism Anabolism = Synthesis Catabolism = Breaking
Understanding metabolic disease
 Understanding metabolic disease Let s build a restaurant Chris Hendriksz Birmingham Children s Hospital 2006 The Task Let s build a restaurant! 2 Partners join to draw the plan. How can we change the
Understanding metabolic disease Let s build a restaurant Chris Hendriksz Birmingham Children s Hospital 2006 The Task Let s build a restaurant! 2 Partners join to draw the plan. How can we change the
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion , version 1.1
 EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
Most common metabolic disorders in childhood. Neonatal screening and diagnostic approach to the. Inborn errors of metabolism (IEM)
 Department of Pediatrics and Developmental Disorders Medical University of Bialystok Most common metabolic disorders in childhood. Neonatal screening and diagnostic approach to the inborn errors of metabolism
Department of Pediatrics and Developmental Disorders Medical University of Bialystok Most common metabolic disorders in childhood. Neonatal screening and diagnostic approach to the inborn errors of metabolism
BIOB111 - Tutorial activity for Session 25
 BIOB111 - Tutorial activity for Session 25 General topics for week 14 Session 25 The metabolism of proteins Students are asked to draw the concept map showing all details of protein metabolism 1 Instructions:
BIOB111 - Tutorial activity for Session 25 General topics for week 14 Session 25 The metabolism of proteins Students are asked to draw the concept map showing all details of protein metabolism 1 Instructions:
Fatty acid oxidation. Naomi Rankin
 Fatty acid oxidation Naomi Rankin Fatty acid oxidation Provides energy to muscles from lipid stores, spares glucose for the brain Lipolysis of triglycerides results in FFA, mainly C16 and C18 FA oxidation
Fatty acid oxidation Naomi Rankin Fatty acid oxidation Provides energy to muscles from lipid stores, spares glucose for the brain Lipolysis of triglycerides results in FFA, mainly C16 and C18 FA oxidation
MSUD. Maple Syrup Urine Disease. TEMPLE Tools Enabling Metabolic Parents LEarning. Information for families after a positive newborn screening
 Maple Syrup Urine Disease MSUD Information for families after a positive newborn screening ADAPTED Adapted by BY the THE Dietitians DIETITIANS Group GROUP BIMDG British Inherited Metabolic Diseases Group
Maple Syrup Urine Disease MSUD Information for families after a positive newborn screening ADAPTED Adapted by BY the THE Dietitians DIETITIANS Group GROUP BIMDG British Inherited Metabolic Diseases Group
Amino Acid Oxidation and the Urea Cycle
 Amino Acid Oxidation and the Urea Cycle Amino Acids: Final class of biomolecules whose oxidation contributes significantly to the generation of energy Undergo oxidation in three metabolic circumstances
Amino Acid Oxidation and the Urea Cycle Amino Acids: Final class of biomolecules whose oxidation contributes significantly to the generation of energy Undergo oxidation in three metabolic circumstances
Hompes Method Lesson 29 Organic Acids Part One
 Hompes Method Lesson 29 Organic Acids Part One Health for the People Ltd not for reuse without expressed permission Organic Acids - Introduction The ultimate tool for laboratory evaluations in nutritional
Hompes Method Lesson 29 Organic Acids Part One Health for the People Ltd not for reuse without expressed permission Organic Acids - Introduction The ultimate tool for laboratory evaluations in nutritional
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM
 LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
A. History Urinalysis is the oldest lab test still being performed today
 III. THE ROUTINE URINALYSIS A. History Urinalysis is the oldest lab test still being performed today 1. Cave man noted change in urine properties associated with disease 2. Babylonians and Egyptians noted
III. THE ROUTINE URINALYSIS A. History Urinalysis is the oldest lab test still being performed today 1. Cave man noted change in urine properties associated with disease 2. Babylonians and Egyptians noted
Chemistry 1120 Exam 4 Study Guide
 Chemistry 1120 Exam 4 Study Guide Chapter 12 12.1 Identify and differentiate between macronutrients (lipids, amino acids and saccharides) and micronutrients (vitamins and minerals). Master Tutor Section
Chemistry 1120 Exam 4 Study Guide Chapter 12 12.1 Identify and differentiate between macronutrients (lipids, amino acids and saccharides) and micronutrients (vitamins and minerals). Master Tutor Section
NBCE Mock Board Questions Biochemistry
 1. Fluid mosaic describes. A. Tertiary structure of proteins B. Ribosomal subunits C. DNA structure D. Plasma membrane structure NBCE Mock Board Questions Biochemistry 2. Where in the cell does beta oxidation
1. Fluid mosaic describes. A. Tertiary structure of proteins B. Ribosomal subunits C. DNA structure D. Plasma membrane structure NBCE Mock Board Questions Biochemistry 2. Where in the cell does beta oxidation
Most common is the congenital adrenogenital syndrome (AGS) or congenital adrenal hyperplasia (CAH) due to 21-hydroxylase deficiency.
 Newborn Screening Examination parameters: TSH-neonatal (hypothyreosis), 17-OH progesterone (AGS), galactose (galactosemia), galactose-uridyl transferase (galacto semia), biotinidase (biotinidase ), phenylalanine
Newborn Screening Examination parameters: TSH-neonatal (hypothyreosis), 17-OH progesterone (AGS), galactose (galactosemia), galactose-uridyl transferase (galacto semia), biotinidase (biotinidase ), phenylalanine
Glycogen Storage Disease Type III, VI and IX - basics -
 Glycogen Storage Disease Type III, VI and IX - basics - Wyboston Lakes 10.10.2015 Urike Steuerwald Tórshavn / Hannover usteuerwald@web.de GSD III, VI and IX - Questions What goes wrong in glycogen storage
Glycogen Storage Disease Type III, VI and IX - basics - Wyboston Lakes 10.10.2015 Urike Steuerwald Tórshavn / Hannover usteuerwald@web.de GSD III, VI and IX - Questions What goes wrong in glycogen storage
Enzymes Topic 3.6 & 7.6 SPEED UP CHEMICAL REACTIONS!!!!!!!
 Enzymes Topic 3.6 & 7.6 SPEED UP CHEMICAL REACTIONS!!!!!!! Key Words Enzyme Substrate Product Active Site Catalyst Activation Energy Denature Enzyme-Substrate Complex Lock & Key model Induced fit model
Enzymes Topic 3.6 & 7.6 SPEED UP CHEMICAL REACTIONS!!!!!!! Key Words Enzyme Substrate Product Active Site Catalyst Activation Energy Denature Enzyme-Substrate Complex Lock & Key model Induced fit model
Very-long-chain acyl-coa dehydrogenase deficiency
 Very-long-chain acyl-coa dehydrogenase deficiency Introductory information Written by: V. Prietsch & P. Burgard Reviewed & Revised for North America by: S. van Calcar Very-long-chain acyl-coa dehydrogenase
Very-long-chain acyl-coa dehydrogenase deficiency Introductory information Written by: V. Prietsch & P. Burgard Reviewed & Revised for North America by: S. van Calcar Very-long-chain acyl-coa dehydrogenase
