INFORMATION FOR PATIENTS WITH LIMB INJURIES
|
|
|
- Charity Grant
- 5 years ago
- Views:
Transcription
1 Hammersmith Hospitals ma NHS Trust Charing Cross Lower Limb Trauma Unit INFORMATION FOR PATIENTS WITH LIMB INJURIES Mr Adam Topping December Review: December SUW O Hammemmith Hospitals NHS Trust
2 This booklet has been provided to help answer some of the questions you may have about your injury and how it may be treated during your stay at Charing Cross Hospital. All the health care professionals involved in your care will be happy to answer any queries or concerns you may have. The Lower Limb Trauma Team Welcome to the Lower Limb Trauma Unit at Charing Cross Hospital. We specialise in the type of injuries that you have. You have been brought here for one of the following reasons: 1. You have an injury to your involving either broken bones or open joints. 2. You have a wound that cannot be closed because it is too big. 3. You have damage either to the blood vessels or to the nerves of your leg(s). Prof. Jagdeep Nanchahal Mr Simon Mr Adam Topping Orthopaedic Surgeons will treat your broken bones or open joints; Plastic Surgeons will look after your skin and soft tissue damage, which includes the nerves and blood vessels. The two groups of surgeons work together if you have both broken bones and soft tissue damage. Consultant Orthopaedic Surgeons Senior mllysiother~-'-t Senior L'mm-se The nursing staff on the ward will provide daily care and you will also see the physiotherapists, particularly after your operation(s), who will help with your mobilising (moving around). Mr Dinesh Nathwani Mr Michael Pearse ira Morgan
3 A general outline of your treatment plan I. Admission to hospital. 2. Seen by Orthopaedic Surgeons and I or Plastic Surgeons 3. First operation This is to clean and inspect the wound. You may need a second operation approximately 48 hours later to repeat this until the wound is clean. 4. Discussion with Orthopaedic Surgeons and Plastic Surgeons How can the injured leg be reconstructed? Is the wound too severe for the leg to be reconstructed? 6. Main operation Leg Is reconstructed if possible. Orthopaedic Surgeons fix the bones if needed Plastic Surgeons cover the wound with soft tissue. 6. Rehabilitation - physiotherapy What happens now? The first thing we need to do is to get an idea as to the extent of your injuries. We will do this in the operating theatre whilst you sleep under a general anaesthetic. The surgeon will explain the procedure to you in detail before asking you to sign a consent form. This is to make sure that you understand the risks and benefits of having the operation. The anaesthetist who will be putting you to sleep for the operation. will also see you to discuss the type of anaesthetic you will have before asking for your written consent. Slhe may prescribe a 'pre-med' for you to take 1 hour before surgery to help you relax and make you sleepy. During the operation, the wound will be cleaned by taking away any dead or dirty soft tissue as well as any dead or dirty pieces of bone if that is broken..this is done to help prevent the wound from becoming infected. Your wound will then be washed out thoroughly with saline solution and if required, the bone will be held together using one of the methods below, if this has not been done already. Please note, sometimes the fixation device that was used to hold the bone together immediately after your injury will need to be changed. 7.. Discharge home and follow-up in clinic The length of your stay will depend on your injury: If the operation is relatively simple, you will need to stay in hospital for 3 or 4 days to recover. More complex procedures will mean a stay of up to 2 weeks or more, depending on the surgery and amount of rehabilitation required afterwards.
4 Fixation can be either by Using a metal bar outside the leg (usually an 'external fixator') or by a metal plate or a nail within the bone (see illustration). Will I need any medication? We will give you antibiotics to prevent wound infection, especially if you have a broken bone as well. These medications will be given intravenously (via a vein), which gives a higher dose. You will also have daily anti-coagulant (blood thinning) injections to prevent thrombosis (blood clots) in your calves and be measured for special stockings (sometimes known as 'TEDS') to help the flow of blood in your uninjured leg. Incisions How will my pain be controlled? We will give you standard painkillers to start with, but some people can react differently to these and some types may not work for you. If this happens, we can change them for you. We also have a 'Pain Team' who are here to help and can also advise about painkillers. Remember - if you are in pain, then tell a member of the nursing staff and your tablets can be adjusted. Your wound will then be sealed using a special 'vacuum dressing'. This is attached to a machine that gently sucks on the wound to keep the wound clean and controlled (not messy). Is there anything I can do to help myself? Your injured leg must be elevated (raised) at all times to reduce the swelling. This will also reduce your pain and improve the flow of blood through your leg. If you are a smoker - NOW IS THE TIME TO QUIT! Nicotine in cigarettes will prevent healing and will damage any reconstruction that can be done to encourage - your leg - to heal. This could result in amputation of your leg. Your body will be trying to heal itself. This takes a lot of energy and you will need to eat and drink plenty to help it to repair. The nurses will give you energy drinks as this will help your body to heal.
5 What happens after the first operation? We should know at this stage what the extent of damage is and what needs to be done. The Orthopaedic Surgeons and the Plastic surgeons will know if the damage is too great to be repaired and whether an amputation is the best way forward. We will come and talk to you about all the possibilities, including amputation. Please be assured that we will not perform an amputation without having spoken to you about it first. What about further surgery? This can be one of the following options, which will be fully discussed with you. Please note these operations are all done under a general anaesthetic. 1. With major injuries to soft tissues, it may be that you need to go back for further surgery to make sure the wound is clean. It can sometimes be difficult to see whether muscle is actually alive or not and rather than take it all away, we prefer to wait and see what survives. This will usually be within 48 hours of the first operation. Only when we are happy that the wound is clean will we be able to decide what to do. 2. When the wound is clean and healthy, not too deep and no bones broken, we may be able to close the wound with a skin graft Sheet of skin harvested (see illustration opposite). 1 Expanded with machine (meshed) Injured leg + This is where a very thin piece of skin is taken from your thigh and then placed onto the wound. The area where the skin was removed is like a graze and will heal on its own after around 2 weeks. 'string-vest' Where the skin graft is covering the wound, it will initially be covered with a dressing. We will ask you to remain in hospital for about 5 days before we check the graft to see whether it has 'taken' (survived). If all is well, then you will be able to go home with dressings over the wound. 3. Deeper wounds to the leg that have tendons or bare bone exposed require covering with a 'flap'. The difference between a flap and a graft is that the flap has its own blood supply, whereas the graft needs to get its blood supply from the wound. A graft cannot survive on bare bone or bare tendon.
6 A flap can be either a piece of skin, a muscle or both. Flaps can be of 2 kinds: a) 'Local' flaps (see illustrations below) -where the flap is planned next to the wound and can be moved across to cover the wound. In reality, the damage to the surrounding tissues usually prevents us from using this method. 'Local' skin flap / / b) 'Free' flaps (see illustrations below and on the page opposite) - where a piece of skin or muscle is detached from somewhere on the body, either the thigh, the back or the abdomen (tummy), complete with its artery and vein which supply it with blood. Using a microscope, the artery and vein are then connected to the main artery and vein in the leg, so that the flap can receive the blood supply it needs to keep it alive. The flap (piece of skin or muscle) is then used to cover the wound in your leg. If we have used a piece of muscle, this will need a skin graft over the top to cover it. This is complex surgery and can take up to 6 hours to complete (see the section headed 'Other investigations' on page 12). 'Free' skin flap taken from the leg 'Local' muscle flap Muscle tunnelled under skin Incision Calf muscle Skin graft on top of muscle 9
7 Alternative sites for removal of skin for a 'free' flap Other investigations You may need an angiogram before your reconstructive surgery. This is a special x-ray examination of the blood vessels in your injured leg via your groin and is done under local anaesth&ic. A dye (known as 'contrast medium') is injected into the artery supplying your leg using a catheter (a fine, plastic tube). The dye allows detailed images (pictures) of the blood vessels to be seen using x-rays. We can then see if the blood vessels in your leg are in good enough condition for us to stitch the blood vessels from a piece of tissue or muscle to form a 'flap'. You will be awake during the test and although you may feel some pressure or pushing at the insertion site to begin with, this should not be painful. be made depending on your specific wound. Certain flaps work better Is some areas than others and this will be discussed with you by your surgeon... If your leg is severely damaged and we cannot repair it, then we will talk to you about the prospect of an amputation. At Charing Cross Hospital, we have the Holderness Centre, which is a unit purely for the rehabilitation of patients who have had amputations. One of the staff from the Centre will also visit and if you wish, slhe can arrange for you to talk with a patient who has already had an amputation. What about the broken bone or open joint? If you havea broken bone and have come to us from another hospital, then this might have been held together already. If it has not been fixed or the fixator that was used is a temporary one, then the Orthopaedic Surgeons will need to change this. How the fracture is held together depends on several things: 1. How badly damaged the bone is and the pattern of the break. 2. How much bone has been lost in the injury. 3. How clean the wound is and whether there is infection present. Limb prostheses (artificial limbs) are very good and very realistic these days and can return you to a lifestyle very similar, if not the same, as the one you had before your injury. People do very well after amputations - cycling and even running marathons1
8 More simple fractures that are not infected involving the middle part of bone can be fixed.together using a long nail that passes down the inside of the bone (see illustration opposite). This nail will remain permanently inside your leg within the bone, even after it has healed. Breaks around the ankle can be fixed using metal plates and screws which are also buried under the skin and will also be left there permanently. Incision Sometimes we use a special fixator, which consists of rings around the legs and wires that pass through the bone (see illustration opposite). Pin sites Open fracture Pin sites Complex fractures that are in several pieces or those where infection is present, need to be held by an 'external fixator (see illustration opposite). This is where 4 metal pins or more are placed into the bone on either side of the break. The pins are then connected together outside of the leg by bars and this holds the break in the correct position. The pins and bars are removed when the bone has healed. This is called an 'Ilizarov frame' after the surgeon who invented it and gives greater control of the break. It can also be used at a later date to slowly lengthen the bone, if a lot of bone has been lost in the original injury. This will bring the leg back to its normal length. Please note The fixation of the bone is usually done by the Orthopaedic Surgeons at the same time that the fracture is covered with soft tissue by the Plastic Surgeons.
9 What are the risks associated with reconstructive surgery? With this type of surgery, the risks depend on: 1. The extent of the injury you have suffered, including injuries to other parts of your body 2. The type of reconstruction you will need 3. How fit and healthy you are normally as well as general risks such as wound infection (5-8%), bleeding after the operation (approximately 2%) and thrombosis (blood clots) In the leg (approximately 2%). Reconstruction with a 'free' flap has a fallure rate (where the new flap does not survive at its new site) of up to 5%. Long-term complications include failure of the bone to heal initially or not healing in the correct position (approximately 10%). If this happens, then an operation may be required to either adjust the metalwork (fixation device) or to take some bone from your hip to place around the break, as this will encourage the fracture to heal. There will also be risks specific to your particular operation. These mainly centre around the reconstruction not working or failing. If this happens, a different option may have to be taken. Your surgeon will discuss this with you in detail before any operation. What happens after the operation? You will wake up in the Recovery Room before you are taken back to the ward. If all is well, you will be able to eat and drink the day after your operation. Please tell us if you are in pain or feel sick. We have tablets1 injections that we can give you as and when required, so that you remain comfortable and pain free. However, you may have a device which you can use to control any pain yourself. This is known as a 'PCA' (Patient Controlled Analgesia) pump and you will be shown how to use it. You may feel light-headed or sleepy after the operation. This is due to the anaesthetic and may continue until the next morning. It is also common to have a sore throat for 2 or 3 days after having a general anaesthetic. This sometimes happens because the anaesthetist (specialist doctor) has to pass a tube down your windpipe to give you the anaesthetic gases that keep you asleep during the operation. The nurses will take your temperature, pulse and blood pressure at regular intewals to check your recovery and it will sometimes be necessary to wake you up to do this. It is very important that we monitor your progress after your operation, so please be patient with the nursing staff during this time. A catheter (tube) will be inside your bladder to drain urine away and to allow the nurses to closely monitor your urine output after the operation. The amount of urine you produce each hour is a good measurement of whether you are dehydrated or not and we can give you more fluids if needed. The tube will be removed when your condition is stable and you are able to move around.
10 A 'drip' (also known as a 'line') will be attached to a needle in your arm or neck to provide you with fluids and prevent dehydration. 'Drains" (tubes) are sometimes used to remove any fluid that collects in the wounds either at the injury site or the area where the flap has been taken from for the reconstruction. The drains will be removed when they are no longer collecting any fluid. However, sometimes fluid can re-accumulate after the drain has been taken out. We can usually remove this fluid using a syringe and needle. 1. Recovery after direct wound closure If we were able to close your wound with stitches, the physiotherapists will visit you the day after surgery and help you to start moving around (known as 'mobilising'). We will ask you to keep your leg elevated (raised) the rest of the time. If all is well, you could be home within 3 days of having the operation. 2. Recovery after wound closure with a skin graft If your wound had a skin graft, you can sit out of bed the next day, but you must keep your leg elevated (raised). We may have put a plaster of Paris cast on your leg to keep it still and help the graft to heal. We will inspect the graft approximately 5 days after surgery. At this stage, you should be able to get up and start to move around with the assistance of the physiotherapists. This is known as 'mobilisation'. 3. Recovery after wound closure with a local flap and skin graft This is similar to recovery after a skin graft alone (see above). The flap will be checked regularly by both doctors and nurses. About 5 days after surgery, the graft will be inspected and your mobilisation will begin. 4. Free flap reconstruction You will be cared for on the HDU (High Dependency Unit) and the flap checked every hour for the first 3 days after your operation. You will have a special warming blanket on to encourage blood flow within the flap. This will keep the reconstruction alive. On the 4th day after surgery, most of the lines and the catheter will be removed. You will be able to sit out of bed and begin to 'dangle' the flap. This means hanging your leg over the bed or letting your foot drop to the floor for 10 minutes at a time. This gets the reconstruction used to its new position. Approximately 5 days after your operation, you may be able to get up and start to move around with the assistance of the physiotherapists. You may then need to stay in hospital for up to 2 weeks or more, depending in your recovery. 5. Recovery after amputation If you and the doctors have agreed that an amputation is required, then the Holderness Centre team will have seen you before your operation. Depending on the extent of damage, usually you will able to attend physiotherapy and the gym within 5 days after surgery. Your length of stay in hospital will be dependent on how long it takes to manufacture your prosthesis (artificial limb) and how comfortable you are with moving around. If you wish, you can go home at weekends during this time.
11 A 'drip' (also known as a 'line') will be attached to a needle in your arm or neck to provide you with fluids and prevent dehydration. 'Drains' (tubes) are sometimes used to remove any fluid that collects in the wounds either at the injury site or the area where the flap has been taken from for the reconstruction. The drains will be removed when they are no longer collecting any fluid. However, sometimes fluid can re-accumulate after the drain has been taken out. We can usually remove this fluid using a syringe and needle. 1. Recovery after direct wound closure If we were able to close your wound with stitches, the physiotherapists will visit you the day after surgery and help you to start moving around (known as 'mobilising'). We will ask you to keep your leg elevated (raised) the rest of the time. If all is well, you could be home within 3 days of having the operation. 2. Recovery after wound closure with a skin graft If your wound had a skin graft, you can sit out of bed the next day, but you must keep your leg elevated (raised). We may have put a plaster of Paris cast on your leg to keep it still and help the graft to heal. We will inspect the graft approximately 5 days after surgery. At this stage, you should be able to get up and start to move around with the assistance of the physiotherapists. This is known as 'mobilisation'. 3. Recovery after wound closure with a local flap and skin graft This is similar to recovery after a skin graft alone (see above). The flap will be checked regularly by both doctors and nurses. About 5 days after surgery, the graft will be inspected and your mobilisation will begin. 4. Free flap reconstruction You will be cared for on the HDU (High Dependency Unit) and the flap checked every hour for the first 3 days after your operation. You will have a special warming blanket on to encourage blood flow within the flap. This will keep the reconstruction alive. On the 4th day after surgery, most of the lines and the catheter will be removed. You will be able to sit out of bed and begin to 'dangle' the flap. This means hanging your leg over the bed or letting your foot drop to the floor for 10 minutes at a time. This gets the reconstruction used to its new position. Approximately 5 days after your operation, you may be able to get up and start to move around with the assistance of the physiotherapists. You may then need to stay in hospital for up to 2 weeks or more, depending in your recovery. 5. Recovery after amputation If you and the doctors have agreed that an amputation is required, then the Holderness Centre team will have seen you before your operation. Depending on the extent of damage, usually you will able to attend physiotherapy and the gym within 5 days after surgery. Your length of stay in hospital will be dependent on how long it takes to manufacture your prosthesis (artificial limb) and how comfortable you are with moving around. If you wish, you can go home at weekends during this time.
12 When can I go home? This depends on the type of surgery you have had. A skin graft or 'local' flap will mean you will need to stay in hospital for 5-7 days. If you have had more complex surgery, then you will need to be closely monitored for up to 4 days after the operation. You may then need to stay in hospital for up to 2 weeks or more, depending on your recovery. If you have had an amputation, then on average, your stay could be up to 5 weeks from the date of your admission to hospital. If possible, please arrange for someone to come and collect you by car on the day of your discharge home, as you will not be able to drive yourself or travel on public transport. It is important that you make the necessary arrangements for going home unless your doctor feels that there are special reasons why you need hospital transport. We will give you a 2-week supply of medication to take home with you. Any further medication will need to be prescribed by your GP. Please make sure that you arrange this before the 2-week supply runs out. How will I cope at home? We will not discharge you until you are safe to leave hospital and your home circumstances are suitable for you. We are keen for you to get home as soon as you feel able to do so and we are happy that you will be able to cope. We have a Discharge Nurse who will liaise with your doctors and physiotherapists and social care packages will be arranged to make sure everything is ready for you. Note for patients going home with an external fixator You may find it difficult to wear your normal trousers over the frame on your leg. Tracksuit bottoms that have zips or buttons at the heel are ideal, as are stretchy pyjama bottoms or yoga pants. Alternatively, you may wish to alter an old pair of trousers by sewing a triangle of material into the seam to make them flare out. Will I need to visit the hospital again? Yes. We will either give you an appointment before you leave or post one to you. If you have any queries or concerns about your reconstruction whilst at home, please do not hesitate to contact the Lower Limb Team on How do I make a comment about my treatment? We aim to provide the best possible treatment and staff will be happy to answer any questions you may have. If you have any suggestions or comments about your stay, please either speak to a member of staff; fill in a comment card or contact the Patient Advice and Liaison Service (PALS) on or PALS staff are able to listen to your concerns, suggestions or queries and help sort out problems on your behalf. Alternatively, you may wish to express your concerns in writing to: The Chief Executive Hammersmith Hospitals NHS Trust, Hammersmith Hospital, Du Cane Road, London W12 OHS
Complex Limb Injury. Exceptional healthcare, personally delivered
 Complex Limb Injury Exceptional healthcare, personally delivered Complex Limb Injuries Introduction This information booklet aims to help you to understand the nature, treatment and outcome of your limb
Complex Limb Injury Exceptional healthcare, personally delivered Complex Limb Injuries Introduction This information booklet aims to help you to understand the nature, treatment and outcome of your limb
Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet
 Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet Originator: Mr Jayatunga, Consultant Vascular surgeon. Joy Lewis, Vascular Nurse Specialist Date: October 2011 Version: 1 Date
Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet Originator: Mr Jayatunga, Consultant Vascular surgeon. Joy Lewis, Vascular Nurse Specialist Date: October 2011 Version: 1 Date
Femoropopliteal/distal. bypass grafts. Vascular Surgery Patient Information Leaflet
 Femoropopliteal/distal bypass grafts Vascular Surgery Patient Information Leaflet Femoro-popliteal/distal bypass grafts This leaflet tells you about the operation known as a femoropopliteal bypass graft.
Femoropopliteal/distal bypass grafts Vascular Surgery Patient Information Leaflet Femoro-popliteal/distal bypass grafts This leaflet tells you about the operation known as a femoropopliteal bypass graft.
Varicoceles can cause various problems, including subfertility.
 This leaflet has been provided to help answer some of the questions you or those who care for you may have about percutaneous abscess drainage. It is not meant to replace the consultation between you and
This leaflet has been provided to help answer some of the questions you or those who care for you may have about percutaneous abscess drainage. It is not meant to replace the consultation between you and
Crossover bypass graft surgery Vascular Surgery Patient Information Leaflet
 Crossover bypass graft surgery Vascular Surgery Patient Information Leaflet Crossover bypass graft surgery Information for patients from the Vascular Surgery Service This leaflet tells you about the operation
Crossover bypass graft surgery Vascular Surgery Patient Information Leaflet Crossover bypass graft surgery Information for patients from the Vascular Surgery Service This leaflet tells you about the operation
Tibial shaft fracture surgery (tibial nailing)
 Tibial shaft fracture surgery (tibial nailing) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we
Tibial shaft fracture surgery (tibial nailing) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we
Gynaecology Department Patient Information Leaflet
 Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Dynamic hip screw (sliding hip screw)
 Dynamic hip screw (sliding hip screw) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a dynamic hip screw, sometimes also known as a sliding hip
Dynamic hip screw (sliding hip screw) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a dynamic hip screw, sometimes also known as a sliding hip
Femoral shaft fracture surgery (femoral nailing)
 Femoral shaft fracture surgery (femoral nailing) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Femoral shaft fracture surgery (femoral nailing) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that
Dynamic Hip Screw - DHS
 Dynamic Hip Screw - DHS Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2017. Document for issue as handout. Procedure Alternative procedure The hip is an important ball and socket joint.
Dynamic Hip Screw - DHS Turnberg Building Orthopaedics 0161 206 4898 All Rights Reserved 2017. Document for issue as handout. Procedure Alternative procedure The hip is an important ball and socket joint.
Patient information. Total Ankle Replacement Trauma and Orthopaedic Directorate PIF 1335 V2
 Patient information Total Ankle Replacement Trauma and Orthopaedic Directorate PIF 1335 V2 Your Consultant has advised you that you are suitable to have a total ankle replacement. The aim of surgery is
Patient information Total Ankle Replacement Trauma and Orthopaedic Directorate PIF 1335 V2 Your Consultant has advised you that you are suitable to have a total ankle replacement. The aim of surgery is
Surgery. In this fact sheet. Surgery: English
 Surgery: English Surgery This information is about surgery (having an operation). Any words that are underlined are explained in the glossary at the end. Many people with cancer will have surgery as part
Surgery: English Surgery This information is about surgery (having an operation). Any words that are underlined are explained in the glossary at the end. Many people with cancer will have surgery as part
Femoral Neck (Hip) Fracture
 Patient Information Leaflet Femoral Neck (Hip) Fracture Produced By: Orthopaedic Department September 2013 Review due September 2016 1 If you require this leaflet in another language, large print or another
Patient Information Leaflet Femoral Neck (Hip) Fracture Produced By: Orthopaedic Department September 2013 Review due September 2016 1 If you require this leaflet in another language, large print or another
ARTERIAL BYPASS GRAFTS IN THE LEG
 The Christchurch Department of Vascular Surgery is actively involved in research projects aimed at improving treatment for patients with arterial disease. Marilyn Ollett Department of Surgery Christchurch
The Christchurch Department of Vascular Surgery is actively involved in research projects aimed at improving treatment for patients with arterial disease. Marilyn Ollett Department of Surgery Christchurch
Elbow fracture surgery (adult) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Elbow fracture surgery (adult) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Elbow fracture surgery (adult) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Inguinal hernias may be present from birth but may not become evident until later in life. They are usually more common in men.
 This booklet is designed to give you information about inguinal hernia repair done under general anaesthesia. We hope it will answer some of the questions that you or those who care for you may have at
This booklet is designed to give you information about inguinal hernia repair done under general anaesthesia. We hope it will answer some of the questions that you or those who care for you may have at
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft
 Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft Why do you need this operation? You need this operation because you have either pain in your legs or a leg ulcer
Department of Vascular Surgery Femoral to Femoral or Iliac to Femoral Crossover Bypass Graft Why do you need this operation? You need this operation because you have either pain in your legs or a leg ulcer
Your anaesthetic for heart surgery
 Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
Patient Information for Consent
 Patient Information for Consent OS12 Femoral Shaft Fracture Surgery (Femoral Nailing) Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your
Patient Information for Consent OS12 Femoral Shaft Fracture Surgery (Femoral Nailing) Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
information The Enhanced Recovery Programme for Total Hip Replacement (1 of 6) What will happen before I come into hospital?
 information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
AN INFORMATION LEAFLET
 LAPAROSCOPIC NEPHRECTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside: 0161 922 6696/6698 Website: www.tameside.nhs.uk
LAPAROSCOPIC NEPHRECTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: www.stockport.nhs.uk Tameside: 0161 922 6696/6698 Website: www.tameside.nhs.uk
ABDOMINAL PERINEAL RESECTION. Patient information Leaflet
 ABDOMINAL PERINEAL RESECTION Patient information Leaflet April 2017 WHAT IS AN ABDOMINAL PERINEAL RESECTION? This is an operation which involves removing the lower end of your large bowel along with the
ABDOMINAL PERINEAL RESECTION Patient information Leaflet April 2017 WHAT IS AN ABDOMINAL PERINEAL RESECTION? This is an operation which involves removing the lower end of your large bowel along with the
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
Ankle fracture surgery. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Ankle fracture surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Ankle fracture surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Ankle arthroscopy. If you have any further questions, please speak to a doctor or nurse caring for you
 Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Ankle arthroscopy This leaflet aims to answer your questions about having an ankle arthroscopy. It explains the benefits, risks and alternatives, as well as what you can expect when you come to hospital.
Internal fixation of a hip fracture. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Internal fixation of a hip fracture Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
Internal fixation of a hip fracture Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained
Ankle Fracture Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Subcapital hip fracture surgery. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Subcapital hip fracture surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the
Subcapital hip fracture surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the
Department of Vascular Surgery Femoral-Popliteal and Femoral-Distal Bypass Grafts
 Department of Vascular Surgery Femoral-Popliteal and Femoral-Distal Bypass Grafts Why do you need the operation? You need this operation because you have either pain in your legs or a leg ulcer or gangrene
Department of Vascular Surgery Femoral-Popliteal and Femoral-Distal Bypass Grafts Why do you need the operation? You need this operation because you have either pain in your legs or a leg ulcer or gangrene
Hemiarthroplasty (half hip replacement)
 Hemiarthroplasty (half hip replacement) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a half hip replacement. It gives information about the
Hemiarthroplasty (half hip replacement) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a half hip replacement. It gives information about the
Aortobifemoral bypass graft Vascular Surgery Patient Information Leaflet
 Aortobifemoral bypass graft Vascular Surgery Patient Information Leaflet This information sheet includes extracts reproduced with permission from the Circulation Foundation. www.circulationfoundation.org.uk
Aortobifemoral bypass graft Vascular Surgery Patient Information Leaflet This information sheet includes extracts reproduced with permission from the Circulation Foundation. www.circulationfoundation.org.uk
PERCUTANEOUS NEPHROLITHOTOMY
 PERCUTANEOUS NEPHROLITHOTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport Tel: 0161 419 5698 Website: www.stockport.nhs.uk Tameside Tel: 0161 922 6696/6698 Website: www.tameside.nhs.uk
PERCUTANEOUS NEPHROLITHOTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport Tel: 0161 419 5698 Website: www.stockport.nhs.uk Tameside Tel: 0161 922 6696/6698 Website: www.tameside.nhs.uk
Kelly procedure. How does the urinary system work? What is a Kelly procedure and why does my child need one?
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
About your graft for dialysis. Information for patients Sheffield Kidney Institute (Renal Unit)
 About your graft for dialysis Information for patients Sheffield Kidney Institute (Renal Unit) page 2 of 12 You will have discussed with your doctor that your kidney condition means that you need to have
About your graft for dialysis Information for patients Sheffield Kidney Institute (Renal Unit) page 2 of 12 You will have discussed with your doctor that your kidney condition means that you need to have
Knee joint arthroscopy
 Critical Care, Theatres & Diagnostics Knee joint arthroscopy Information for patients This booklet answers some of the questions you may have about having a knee joint arthroscopy. It explains the risks
Critical Care, Theatres & Diagnostics Knee joint arthroscopy Information for patients This booklet answers some of the questions you may have about having a knee joint arthroscopy. It explains the risks
Free flaps and Pedicled flaps in lower limb reconstruction
 Free flaps and Pedicled flaps in lower limb reconstruction UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Free flaps and Pedicled flaps in lower limb reconstruction UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Information for patients. Vena Cava Filters. Sheffield Vascular Institute. Northern General Hospital
 Information for patients Vena Cava Filters Sheffield Vascular Institute Northern General Hospital You have been given this leaflet because you need a procedure known as Vena Cava Filter insertion. This
Information for patients Vena Cava Filters Sheffield Vascular Institute Northern General Hospital You have been given this leaflet because you need a procedure known as Vena Cava Filter insertion. This
HARTMANNS PROCEDURE. Patient information Leaflet
 HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
Enhanced Recovery Programme
 Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Hip Fracture Orthopaedic Department Patient Information Leaflet
 riginator: Anne Flavall Professional Development Lead, Mr Marsh and Mr Quraishi Orthopaedic Consultant Surgeons Date: March 2012 Version: 2 Date for Review: March 2015 DGOH Ref No: DGOH/PIL/00611 Hip Fracture
riginator: Anne Flavall Professional Development Lead, Mr Marsh and Mr Quraishi Orthopaedic Consultant Surgeons Date: March 2012 Version: 2 Date for Review: March 2015 DGOH Ref No: DGOH/PIL/00611 Hip Fracture
Your anaesthetic for major surgery
 Your anaesthetic for major surgery with planned high dependency care or intensive care afterwards Information for patients and families First Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet is for
Your anaesthetic for major surgery with planned high dependency care or intensive care afterwards Information for patients and families First Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet is for
This booklet has been provided to help answer some of the questions you may have about RFA of liver tumours.
 This booklet has been provided to help answer some of the questions you may have about RFA of liver tumours. RFA of tumours is a minimally invasive procedure used to treat liver tumours (growth or mass
This booklet has been provided to help answer some of the questions you may have about RFA of liver tumours. RFA of tumours is a minimally invasive procedure used to treat liver tumours (growth or mass
Hindfoot/Midfoot Fusion (Arthrodesis)
 Hindfoot/Midfoot Fusion (Arthrodesis) There are often three reasons why this operation is performed: Pain - from osteoarthritis (OA) and rheumatoid arthritis (RA). Change of shape of foot or deformity.
Hindfoot/Midfoot Fusion (Arthrodesis) There are often three reasons why this operation is performed: Pain - from osteoarthritis (OA) and rheumatoid arthritis (RA). Change of shape of foot or deformity.
Having a nephrostomy tube inserted
 Having a nephrostomy tube inserted Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been advised to have a nephrostomy tube inserted. It includes information
Having a nephrostomy tube inserted Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been advised to have a nephrostomy tube inserted. It includes information
Angiogram, angioplasty and stenting
 Angiogram, angioplasty and stenting Who is this leaflet for? This leaflet is for people who are having: an angiogram angioplasty (with or without a stent) An angiogram (also called an arteriogram or angiography)
Angiogram, angioplasty and stenting Who is this leaflet for? This leaflet is for people who are having: an angiogram angioplasty (with or without a stent) An angiogram (also called an arteriogram or angiography)
Total ankle replacement. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Total ankle replacement Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Total ankle replacement Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Angiogram and angioplasty
 Angiogram and angioplasty The femoral arteries run from the groin to the thigh, delivering blood to your legs. When there is a narrowing or blockage in these arteries, the blood supply to the legs is reduced,
Angiogram and angioplasty The femoral arteries run from the groin to the thigh, delivering blood to your legs. When there is a narrowing or blockage in these arteries, the blood supply to the legs is reduced,
Mr Sanjeev Sarin MS FRCS. Aortic Aneurysms Patient Information Sheet
 Aortic Aneurysms Patient Information Sheet The aim of this information sheet is to ensure that you understand the nature of the treatment you wish to undertake. Please read it carefully and discuss any
Aortic Aneurysms Patient Information Sheet The aim of this information sheet is to ensure that you understand the nature of the treatment you wish to undertake. Please read it carefully and discuss any
Northumbria Healthcare NHS Foundation Trust. Knee Arthroscopy. Issued by the Orthopaedic Department
 Northumbria Healthcare NHS Foundation Trust Knee Arthroscopy Issued by the Orthopaedic Department Introduction This guide has been produced to provide you with information regarding your knee arthroscopy
Northumbria Healthcare NHS Foundation Trust Knee Arthroscopy Issued by the Orthopaedic Department Introduction This guide has been produced to provide you with information regarding your knee arthroscopy
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Having a diagnostic catheter angiogram
 Having a diagnostic catheter angiogram This information leaflet will explain what an angiogram is and why you have been sent for one. Please read this leaflet carefully. If you have any questions or concerns
Having a diagnostic catheter angiogram This information leaflet will explain what an angiogram is and why you have been sent for one. Please read this leaflet carefully. If you have any questions or concerns
Bunion Surgery. Patient information Leaflet
 Bunion Surgery Patient information Leaflet April 2017 What is a bunion? A bunion is a bony lump on the side of your foot at the base of your big toe (see figure 1). This may be an isolated problem but
Bunion Surgery Patient information Leaflet April 2017 What is a bunion? A bunion is a bony lump on the side of your foot at the base of your big toe (see figure 1). This may be an isolated problem but
PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE)
 PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
Arthroscopy of the knee joint Orthopaedic Department Patient Information Leaflet
 Arthroscopy of the knee joint Orthopaedic Department Patient Information Leaflet Page 1 Arthroscopy of the knee joint Welcome to the Dudley Group NHS Foundation Trust Orthopaedic Department. This booklet
Arthroscopy of the knee joint Orthopaedic Department Patient Information Leaflet Page 1 Arthroscopy of the knee joint Welcome to the Dudley Group NHS Foundation Trust Orthopaedic Department. This booklet
Surgery to reconstruct the anterior cruciate ligament of the knee (ACL reconstruction)
 Surgery to reconstruct the anterior cruciate ligament of the knee (ACL reconstruction) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery
Surgery to reconstruct the anterior cruciate ligament of the knee (ACL reconstruction) Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery
Arch Angiography. Exceptional healthcare, personally delivered
 Exceptional healthcare, personally delivered This leaflet has been prepared to tell you about arch angiography. It will explain what will happen during this procedure and we hope that it will answer some
Exceptional healthcare, personally delivered This leaflet has been prepared to tell you about arch angiography. It will explain what will happen during this procedure and we hope that it will answer some
Information about Your Anaesthetic and Pain Control After Surgery
 Information about Your Anaesthetic and Pain Control After Surgery Information for patients Specialist Support If you require this leaflet in another language, large print or another format, please contact
Information about Your Anaesthetic and Pain Control After Surgery Information for patients Specialist Support If you require this leaflet in another language, large print or another format, please contact
The Leeds Teaching Hospitals NHS Trust Catheter directed thrombolysis and pelvic venous stenting for ilio-femoral DVT
 n The Leeds Teaching Hospitals NHS Trust Catheter directed thrombolysis and pelvic venous stenting for ilio-femoral DVT Information for patients Catheter directed thrombolysis and pelvic venous stenting
n The Leeds Teaching Hospitals NHS Trust Catheter directed thrombolysis and pelvic venous stenting for ilio-femoral DVT Information for patients Catheter directed thrombolysis and pelvic venous stenting
Laparoscopic partial removal of the kidney
 Laparoscopic partial removal of the kidney Department of Urology 2 Patient Information What evidence is this information based on? This booklet includes advice from consensus panels, the British Association
Laparoscopic partial removal of the kidney Department of Urology 2 Patient Information What evidence is this information based on? This booklet includes advice from consensus panels, the British Association
Retroperineal Lymph Node Dissection (RPLND)
 Acute Services Division Information for patients about Retroperineal Lymph Node Dissection (RPLND) Introduction This booklet gives you information about surgery to remove the residual lymph nodes at the
Acute Services Division Information for patients about Retroperineal Lymph Node Dissection (RPLND) Introduction This booklet gives you information about surgery to remove the residual lymph nodes at the
Leg artery bypass (fem-pop bypass)
 Leg artery bypass (fem-pop bypass) The femoral artery runs down from the groin and into the thigh. This artery delivers blood to your legs. When the femoral artery reaches the back of the knee it becomes
Leg artery bypass (fem-pop bypass) The femoral artery runs down from the groin and into the thigh. This artery delivers blood to your legs. When the femoral artery reaches the back of the knee it becomes
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Femoral endarterectomy
 Femoral endarterectomy The femoral arteries run from the groin to the thigh delivering blood to your legs. When there is a narrowing or blockage in these arteries, the blood supply to the legs is reduced,
Femoral endarterectomy The femoral arteries run from the groin to the thigh delivering blood to your legs. When there is a narrowing or blockage in these arteries, the blood supply to the legs is reduced,
Procedure Information Guide
 Procedure Information Guide Breast reconstruction with abdominal tissue flap Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every
Procedure Information Guide Breast reconstruction with abdominal tissue flap Brought to you in association with EIDO and endorsed by the The Royal College of Surgeons of England Discovery has made every
Femoro-popliteal bypass surgery. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Femoro-popliteal bypass surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the
Femoro-popliteal bypass surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the
Hindfoot / Midfoot Fusion (Arthrodesis) Orthopeadic Department Patient Information Leaflet
 Hindfoot / Midfoot Fusion (Arthrodesis) Orthopeadic Department Patient Information Leaflet There are often three reasons why this operation is performed: Pain - from osteoarthritis (OA) and rheumatoid
Hindfoot / Midfoot Fusion (Arthrodesis) Orthopeadic Department Patient Information Leaflet There are often three reasons why this operation is performed: Pain - from osteoarthritis (OA) and rheumatoid
The organs and tissues of the body are made up of tiny building blocks called cells. Cancer is a disease of these cells.
 Surgery: English Surgery This fact sheet is about surgery for cancer. This is when someone has an operation to remove part of the body where the cancer is growing. It is also used to help diagnose cancer.
Surgery: English Surgery This fact sheet is about surgery for cancer. This is when someone has an operation to remove part of the body where the cancer is growing. It is also used to help diagnose cancer.
Total elbow replacement. Information for patients Orthopaedics - Upper Limb
 Total elbow replacement Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation you
Total elbow replacement Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation you
Insertion of a Haemodialysis Catheter
 Insertion of a Haemodialysis Catheter Exceptional healthcare, personally delivered Introduction This leaflet is about the procedure required to put in a temporary dialysis catheter. It is intended to give
Insertion of a Haemodialysis Catheter Exceptional healthcare, personally delivered Introduction This leaflet is about the procedure required to put in a temporary dialysis catheter. It is intended to give
Caring for a Nephrostomy and what is Ureteric Stenting
 Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Radical Orchidectomy. Department of Urology. Patient Information
 Radical Orchidectomy Department of Urology 2 Patient Information This leaflet answers some of the questions people ask about a radical orchidectomy operation. If any further questions are raised after
Radical Orchidectomy Department of Urology 2 Patient Information This leaflet answers some of the questions people ask about a radical orchidectomy operation. If any further questions are raised after
Femoropopliteal bypass graft
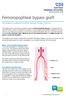 Femoropopliteal bypass graft Information for patients from the Vascular Surgery Service This leaflet tells you about the operation known as femoropopliteal bypass; it explains what is involved before,
Femoropopliteal bypass graft Information for patients from the Vascular Surgery Service This leaflet tells you about the operation known as femoropopliteal bypass; it explains what is involved before,
Endovascular repair for abdominal aortic aneurysm (EVAR) Information for patients Sheffield Vascular Institute
 Endovascular repair for abdominal aortic aneurysm (EVAR) Information for patients Sheffield Vascular Institute page 2 of 12 You have been diagnosed as having an Abdominal Aortic Aneurysm (AAA) and it has
Endovascular repair for abdominal aortic aneurysm (EVAR) Information for patients Sheffield Vascular Institute page 2 of 12 You have been diagnosed as having an Abdominal Aortic Aneurysm (AAA) and it has
Shoulder replacement surgery
 Shoulder replacement surgery Information for patients The aim of this leaflet is to answer some of the questions you may have about having shoulder replacement surgery. It explains the risks and benefits
Shoulder replacement surgery Information for patients The aim of this leaflet is to answer some of the questions you may have about having shoulder replacement surgery. It explains the risks and benefits
Leg Bypass Surgery Includes:
 Leg Bypass Surgery Includes: Ilio-femoral bypass Femoro-popliteal bypass Femoro-distal bypass Femoro-femoro crossover Vascular Surgery Patient Information Leaflet This information sheet includes extracts
Leg Bypass Surgery Includes: Ilio-femoral bypass Femoro-popliteal bypass Femoro-distal bypass Femoro-femoro crossover Vascular Surgery Patient Information Leaflet This information sheet includes extracts
Arthroscopy of the ankle. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Arthroscopy of the ankle Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Arthroscopy of the ankle Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Your visit to theatre
 Your visit to theatre Information for you about your anaesthetic and your visit to the operating theatre This leaflet provides information about coming into hospital for your operation It explains anaesthetic
Your visit to theatre Information for you about your anaesthetic and your visit to the operating theatre This leaflet provides information about coming into hospital for your operation It explains anaesthetic
Hernia Operations. What is a hernia? What does the operation involve? What are the benefits of an operation?
 Hernia Operations Hernia Operations What is a hernia? The abdomen (the medical word for the tummy) contains many organs such as the liver spleen and intestines (the medical word for insides ) and these
Hernia Operations Hernia Operations What is a hernia? The abdomen (the medical word for the tummy) contains many organs such as the liver spleen and intestines (the medical word for insides ) and these
Radiology department. Vena cava filter
 Radiology department Vena cava filter Introduction This leaflet tells you about the procedure known as vena cava filter insertion. It explains what is involved and what the benefits and risks are. It may
Radiology department Vena cava filter Introduction This leaflet tells you about the procedure known as vena cava filter insertion. It explains what is involved and what the benefits and risks are. It may
Esophagectomy Surgery
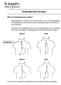 Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Inferior Vena Cava (IVC) filter insertion. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Inferior Vena Cava (IVC) filter insertion An information guide Inferior Vena Cava (IVC) Filter Insertion Introduction This leaflet tells
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Inferior Vena Cava (IVC) filter insertion An information guide Inferior Vena Cava (IVC) Filter Insertion Introduction This leaflet tells
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet February 2018 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used
Epidural Continuous Infusion Patient information Leaflet February 2018 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used
Open repair of Abdominal Aortic Aneurysms (AAA)
 Open repair of Abdominal Aortic Aneurysms (AAA) Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling us
Open repair of Abdominal Aortic Aneurysms (AAA) Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling us
Managing Pain and Sickness after Surgery
 Managing Pain and Sickness after Surgery This pamphlet explains about pain relief after surgery. There are many effective treatments to help keep you comfortable after your operation. The different ways
Managing Pain and Sickness after Surgery This pamphlet explains about pain relief after surgery. There are many effective treatments to help keep you comfortable after your operation. The different ways
Information for Patients having Total Knee Replacement Surgery
 Information for Patients having Total Knee Replacement Surgery Hello You will be coming into hospital for your surgery and we hope your stay will be pleasant. We have written this booklet to give you information
Information for Patients having Total Knee Replacement Surgery Hello You will be coming into hospital for your surgery and we hope your stay will be pleasant. We have written this booklet to give you information
Why do I need a kidney biopsy?
 Page 1 of 6 Renal biopsy Introduction Your doctor has referred you for a renal (kidney) biopsy. This leaflet aims to answer some of your questions about having a kidney biopsy. The leaflet also explains
Page 1 of 6 Renal biopsy Introduction Your doctor has referred you for a renal (kidney) biopsy. This leaflet aims to answer some of your questions about having a kidney biopsy. The leaflet also explains
Having an Anaesthetic Your Questions Answered
 PATIENT INFORMATION Having an Anaesthetic Your Questions Answered This leaflet explains what you can expect when having an anaesthetic for a planned operation. What is anaesthesia? Anaesthesia means loss
PATIENT INFORMATION Having an Anaesthetic Your Questions Answered This leaflet explains what you can expect when having an anaesthetic for a planned operation. What is anaesthesia? Anaesthesia means loss
REVERSAL OF ILEOSTOMY. Patient information Leaflet
 REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
Ankle, sub-talar or mid-foot joint fusion
 Ankle, sub-talar or mid-foot joint fusion This leaflet aims to answer your questions about having an ankle, sub-talar or mid-foot joint fusion. It explains the benefits, risks and alternatives, as well
Ankle, sub-talar or mid-foot joint fusion This leaflet aims to answer your questions about having an ankle, sub-talar or mid-foot joint fusion. It explains the benefits, risks and alternatives, as well
WEB device for treating brain (intracranial) aneurysms
 WEB device for treating brain (intracranial) aneurysms This leaflet explains more about the WEB device, including the benefits, risks and any alternatives and what you can expect when you come to hospital.
WEB device for treating brain (intracranial) aneurysms This leaflet explains more about the WEB device, including the benefits, risks and any alternatives and what you can expect when you come to hospital.
This leaflet is available in other formats including large print, audio tape, CD and braille, and in languages other than English, upon request.
 Information for inpatients This leaflet is available in other formats including large print, audio tape, CD and braille, and in languages other than English, upon request. Med/304.1 (2012) Page 1 of 8
Information for inpatients This leaflet is available in other formats including large print, audio tape, CD and braille, and in languages other than English, upon request. Med/304.1 (2012) Page 1 of 8
Bunion surgery. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Bunion surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information in this
Bunion surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information in this
Posterior Cervical Decompression
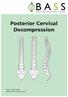 Posterior Cervical Decompression Issue 5: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a narrowing of your
Posterior Cervical Decompression Issue 5: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a narrowing of your
Cerebral angiography. Information for families. Great Ormond Street Hospital for Children NHS Foundation Trust
 Cerebral angiography Information for families Great Ormond Street Hospital for Children NHS Foundation Trust This leaflet explains about the cerebral angiography procedure and what to expect when your
Cerebral angiography Information for families Great Ormond Street Hospital for Children NHS Foundation Trust This leaflet explains about the cerebral angiography procedure and what to expect when your
Foot and Ankle Surgery
 Information about Foot and Ankle Surgery Statement of Use The information in this leaflet is intended solely for the person to whom it was given by the health care team and is provided as a general information
Information about Foot and Ankle Surgery Statement of Use The information in this leaflet is intended solely for the person to whom it was given by the health care team and is provided as a general information
Having an operation on the pancreas
 Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Advice to patients having an angioplasty
 What is an angioplasty? Advice to patients having an angioplasty An angioplasty is an x ray procedure to open a narrowed or blocked artery in order to improve blood flow. It involves inserting a long tube
What is an angioplasty? Advice to patients having an angioplasty An angioplasty is an x ray procedure to open a narrowed or blocked artery in order to improve blood flow. It involves inserting a long tube
Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation
 Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation Plastic Surgery Department Leaflet Number 2 Produced: October 2007 Review date: October 2010
Lancashire Teaching Hospitals NHS Foundation Trust Information for Patients having a Breast Reduction Operation Plastic Surgery Department Leaflet Number 2 Produced: October 2007 Review date: October 2010
