CVA. Stroke. Terminology. Cerebrovascular Accident. Stroke Brain Attack
|
|
|
- Bridget Gibbs
- 6 years ago
- Views:
Transcription
1 CVA Cerebrovascular Accident Stroke Brain Attack Stroke is defined as sudden onset of neurological dysfunction resulting from abnormality in cerebral circulation (ischemic or hemorrhagic lesions in the brain) Terminology Paralysis: unable to move or feel (or both), all or part of the body Hemiplegia: paralysis on one side of the body Hemiparesis: weakness on one side of the body Paresthesias: a sensation on the skin, like tingling, prickling, creeping 1
2 CVA Categories Etiologic thrombosis, embolus, hemorrhage Management transient ischemic attack (TIA), minor stroke, major stroke, etc Anatomic specific vascular area Thrombus vs. Embolus DO NOT OVERTHINK this Thrombus originates in the body part that is damaged (i.e. cerebral artery) Embolus had to travel to get to the body part that is damaged Epidemiology CVA is the third leading cause of death in the U.S. And the most common cause of adult disability 2
3 Epidemiology incidence increases dramatically with age only 20% of CVAs occur in individuals under the age 65 incidence has declined steadily over the past 30 years Etiologic Categories Ischemic Hemorrhagic Etiologic Categories: Ischemic Lack of blood flow & oxygen to the brain Can be caused by (1) Cerebral thrombosis: blood clot (thrombus) within the cerebral arteries or their branches lead to ischemia with resulting infarction (tissue death) 3
4 Etiologic Categories (2) Cerebral embolus: bits of matter (thrombi, fat, air) that travel through the bloodstream to the cerebral arteries where they produce an occlusion and infarction associated with CV disease Etiologic Categories: Hemorrhagic Hemorrhage: abnormal bleeding due to a ruptured vessel. Tissue death results from both ischemic and mechanical injury. intracerebral hemorrhage, subarachnoid hemorrhage Hemorrhagic Stroke 4
5 Hemorrhagic Stroke Hemorrhagic Stroke Risk Factors for Stroke Hypertension Heart disease Diabetes 5
6 Stroke Prevention Preventable with modifiable risk factors Regulate blood pressure Dietary adjustments Cessation of smoking Exercise and weight control Control of diabetes and heart disease Improving public awareness of early warning signs of stroke Signs & Symptoms Beyond F.A.S.T. Other Symptoms You Should Know Sudden numbness or weakness of the leg, arm or face Sudden confusion or trouble understanding Sudden trouble seeing in one or both eyes Sudden trouble walking, dizziness, loss of balance or coordination Sudden severe headache with no known cause 6
7 Anatomy of Blood Flow Internal carotids divide into the anterior cerebral artery via anterior communicating artery middle cerebral artery via posterior communicating artery Anatomy of Blood Flow Vertebral arteries join together to form the Basilar artery Basilar artery divides into posterior cerebral artery cerebellar arteries (3 pairs) 7
8 Anatomy of Blood Flow Circle of Willis: comprised of anterior, middle, and posterior cerebral arteries anterior and posterior communicating arteries Cerebral Blood Flow Anatomy of Blood Flow Clinical relevance: the artery involved determines the area of infarct which results in the variety of signs and symptoms associated with CVAs Martin & Kessler p 284, Table
9 Blood Flow Anterior Cerebral Artery Blood Flow Middle Cerebral Artery Blood Flow Posterior Cerebral Artery 9
10 Transient Ischemic Attack (TIA) often labeled mini-stroke more accurately characterized as a warning stroke: Should be taken very seriously Stroke Syndromes Anterior Cerebral Artery Syndrome contralateral weakness and sensory loss, primarily in LE s aphasia Incontinence May have significant memory deficits, loss of behavioral inhibition May see neglect, aphasia, apraxia & agraphia Stroke Syndromes Middle Cerebral Artery Occlusion most common contralateral sensory loss and weakness in face and UE, less in LE Spastic hemiparesis homonymous hemianopsia Perceptual deficits: unilateral neglect, apraxia, and spatial disorganization Wernicke s aphasia in dominant hemisphere Flat affect in right hemisphere Impaired body schema (next slide) 10
11 Impaired Body Schema The term Body Scheme refers to a postural model of the body, including the relationship of body parts to each other and the relationship of the body to the environment This body awareness relies on tactile & proprioceptive sensations. It is considered one of the essential foundations for the performance of all purposeful motor behavior Unilateral neglect, somatoagnosia, finger agnosia, anosognosia Stroke Syndromes Vertebral-Basilar Artery occlusion Loss of consciousness Hemiplegia or tetraplegia Headache, dizziness, ataxia cranial nerve involvement locked in syndrome inability to speak alert vertical eye movement intact Treating Locked In Syndrome There is no cure for locked-in syndrome, nor is there a standard course of treatment. Neuromuscular stimulation may help activate some paralyzed muscles. Several devices to help communication are available. Other treatment is symptomatic and supportive. 11
12 Stroke Syndromes Posterior Cerebral Artery occlusion contralateral sensory loss thalamic pain syndrome memory deficit homonymous hemianopsia visual agnosia cortical blindness Stroke Syndromes Lacunar Infarct deep region of the brain common in diabetes and hypertension results in a cystic cavity after the infarct sensory loss ataxia dysarthria Other Stroke Syndromes Thalamic pain syndrome Intolerable burning pain and sensory perseveration Pusher syndrome (R CVA/ L hemiplegia) Absent/impaired tactile & kinesthetic awareness Visual deficits Truncal asymmetries Increased weight bearing on the Left Difficulties with transfers (pushing away with the uninvolved side) 12
13 Left Hemispheric Specialization Language process verbal language understand language produce written/spoken language Analytical controlled logical rational sequence and perform movements math calculations express positive emotion Characteristics of CVA Left Hemisphere Involvement Weakness, paralysis of right side Increased frustration Decreased processing Possible aphasia Possible dysphagia Possible motor apraxia Decreased discrimination between R & L Right hemianopsia Right Hemispheric Specialization Nonverbal processing process info holistically artistic General concept comprehension Hand-eye coord spatial skills kinesthetic awareness understands music nonverbal commun body image express negative emotion 13
14 Characteristics of CVA Right Hemisphere Involvement Weakness, paralysis of left side Decreased attention span Left hemianopsia Decreased awareness & judgment Left inattention Emotional lability Impulsive behaviors Decreased spatial orientation Memory deficits Direct Impairments Sensation: frequently impaired, rarely absent. Type and extent of deficit depends on location and extent of the lesion. Proprioceptive loss common Profound hemisensory loss can lead to Direct Impairments Pain CVA can result in severe headache, neck or face pain Thalamic Pain Syndrome Pain due to secondary impairments 14
15 Direct Impairments Visual deficits homonymous hemianopsia: common; blindness on nasal half of one eye and temporal half of the other. Named by the side of the defect which corresponds to the affected side (R CVA = L hemianopsia, L hemiplegia) Is Homonymous Hemianopsia reversible? Over the years it has become clear that patients may improve spontaneously. Visual field defects of vascular origin, the prognosis for spontaneous recovery is poor. Any recovery of a complete hemianopsia occurs in the first 10 days after which further recovery is unlikely. Recovery of a partial defect is usually maximal within the first 48 hours. Less than 10% of patients recover their full field, and a proportion of these will, nevertheless, continue to complain about their visual function because of coexisting parietal lobe involvement. Up to 50% show spontaneous regression of varying degrees. Direct Impairments Motor Deficits: several considerations: Sequential recovery stages: Initial flaccid stage Stage of spasticity Stage of relative recovery 15
16 Direct Impairments Motor Deficits Alterations in tone: flaccidity: usually present immediately after the CVA and short-lived spasticity: emerges in 90% of the cases and occur typically in predictable patterns Direct Impairments Motor Deficits Abnormal Synergy patterns: stereotypical movement patterns associated with spasticity The patient is unable to move an isolated segment of a limb without producing movements in the remainder of the limb 2 distinct abnormal synergy patterns have been described for each extremity Direct Impairments Motor Deficits Reflexes: become altered and depend on the stage of recovery initially, hyporeflexive middle stages of recovery (spasticity/synergy), hyperreflexive Primitive reflexes may re-emerge Associated Reactions may be present 16
17 Direct Impairments Motor Deficits Paresis: common finding. Varies considerably Direct Impairments Motor Deficits Motor programming deficits: more likely seen in patients with CVA ( hemiplegia) L hemisphere responsible for sequencing movements; so L CVA results in apraxia R hemisphere has a role in sustaining a movement or posture; R CVA may demonstrate an inability to sustain a movement or posture Direct Impairments Motor Deficits Postural Control & Balance Deficits Balance is frequently impaired following CVA Patients demo increased postural sway in standing Patients with hemiplegia typically fall in the direction of weakness 17
18 Direct Impairments Motor Deficits Speech and language disorders aphasia: general term indicating an acquired communication disorder caused by brain damage and characterized by an impairment of language comprehension, formulation, and use. Occurs in up to 40% of all patients with CVAs many types lqay Direct Impairments Motor Deficits Dysphagia Swallowing difficulty Usually delayed swallowing reflex Aspiration occurs in 1/3 of patients with dysphagia Direct Impairments Motor Deficits Perceptual deficits: includes visuospatial distortions: difficulty judging distance, size, position, rate of movement, form disturbances in body image: distorted mental and visual images of one s body that includes feelings about one s body unilateral neglect: patients are unaware of what happens on the hemiplegic side 18
19 Direct Impairments Motor Deficits Affective Disorders Lesions in Right hemisphere Impaired emotional function Lesions in Left hemisphere May experience frequent and severe depression Direct Impairments Motor Deficits Behavioral changes: vary widely L CVA: difficulty processing information in a sequential, linear manner. Negative, anxious, depressed; more cautious, insecure, and uncertain realistic in appraisal of the existing problem R CVA: difficulty in grasping the whole idea and spatial-perceptual tasks indifferent, quick, impulsive, euphoric overestimate their ability while minimizing (or denying) their problem = SAFETY CONCERNS Secondary Impairments DVT Skin Breakdown Decreased flexibility Complex Regional Pain Syndrome (CRPS) Deconditioning Shoulder subluxation & pain 19
20 Recovery Fastest in the first few weeks after onset Most measurable neurologic recovery (90%) occurs during the first 3 months Functional gains continue for up to 6 months or longer (at reduced rate) Rates of improvement vary greatly depending on the management category (minor vs. severe) Acute Rehabilitation Begins as soon as the patient is stable General goals: maintain ROM and prevent deformity Promote awareness, active movement and use of the affected side improve trunk control, symmetry, and balance improve functional mobility initiate self-care activities monitor changes associated with recovery Acute Rehabilitation Positioning: want to stimulate the patient to turn toward and engage the affected side ex. place bed so affected side faces main part of the room assume upright postures ASAP turning in bed to prevent pressure decubiti 20
21 Acute Rehabilitation AVOID these positions: lateral flexion to the affected side scapular depression & retraction, IR & add of the UE, elbow flex, FA pronation, wrist & finger flexion hip retraction & elevation, hip & knee extension with hip adduction; or hip & knee flexion with hip abduction; ankle plantarflexion Acute Rehabilitation PROMOTE these positions: supine positioning: small pillow under scapula (promotes protraction), support UE on pillow (promotes extension), pillow under pelvis (promotes anterior pelvic tilt), pillow under knee (prevents hyperextension) Acute Rehabilitation PROMOTE these positions: lying on the sound (uninvolved) side: trunk straight; pillow under rib cage (elongates affected side); pillow under the affected UE (promotes scap protraction, elbow extension, forearm neutral or supinated); pillow under the affected LE (pelvis protracted, hip extended, knee flexed, neutral rotation) 21
22 Acute Rehabilitation PROMOTE these positions: lying on the affected side: trunk straight; scapula protracted (with the UE well forward), elbow extended, forearm supinated; hip extended with knee flexed (alternate position: slight hip and knee flexion with pelvic protraction) Acute Rehabilitation PROMOTE these positions: sitting: head/trunk in midline; symmetrical WB on buttocks; hips/knees flexed to 90 degrees, feet flat; UEs resting on pillows, arm/lap board with scapula protracted and wrist/fingers in extended in a functional open position Acute Rehabilitation ROM and prevention of limb trauma: ROM: UE: can be supported in a sling during the flaccid stage, preventing joint trauma; contraindicated in the spastic stage LE: stretch plantarflexors/activate weak dorsiflexors 22
23 Acute Rehabilitation Functional mobility activities: promote use of both sides rather than just the sound side focus on: rolling (both directions) sitting up (both directions) bridging sitting Standing walking and transfers Study #1 UE TE in Acute Phase Single-blind RCT with 100 patients put in either a control group or the experimental group Experimental group received 5 days/week for 6 weeks for 30 minutes: patient in rocking chair with inflatable splint to support affected arm, shoulder in 80 flexion & slight abd, elbow ext Study #1 UE TE in Acute Phase Distal splint fixed with 2 straps in a gutter. Patient rocked for 30 minutes, using affected arm to actively push backward. This contained 3 elements: Motor Stimulation Sensory Stimulation Placement opposite of synergistic pattern 23
24 Study #1 UE TE in Acute Phase Control group: sat in rocking chair and rocked for 30 minutes with arm on cushion in lap with fake short wave therapy on the shoulder Results: experimental group did better on Brunnstrom-Fugl-Meyer (impairment test) with statistically significant differences at follow up. No effect on tests of disability level. Adding the specific intervention during the acute phase s/p CVA improved motor recovery. Feys et al (1998) Postacute Rehabilitation Continue and modify (if necessary) the treatment activities begun in the acute phase Important to monitor CV status as activities and challenges increase so as not to over-exert the patient Postacute Rehabilitation Goals: prevent/minimize secondary complications compensate for sensory and perceptual loss improve postural control and balance develop independent functional mobility skills develop independent ADLs endurance encourage socialization and motivation 24
25 Postacute Rehabilitation Motor control training: stress selective (out of synergy) movement patterns that allow success in functional tasks (feeding, dressing, gait) stress holding or eccentric contractions before concentric ones (generates more tension; hmuscle fiber recruitment) weak muscles should be activated, first in unidirectional patterns, then progressed to slow reciprocal movements (balanced agonist/antagonist interaction is crucial for normal coordination & function) Postacute Rehabilitation NDT: the patient learns to control tone & movement through the use of patterns that promote normal movements (out of synergy) PNF: PNF patterns are chosen and used while avoiding synergistic patterns. Emphasizes practice, repetition, and visual guidance. Postacute Rehabilitation Tone reduction: many techniques Elongation of spastic muscles & positioning techniques Prolonged pressure Slow rocking movements Air splints Once inhibition & ROM are achieved 25
26 Postacute Rehabilitation UE Control FIRST: pelvic/trunk/scapular alignment Early mob/rom/positioning UE WBing Scapular protraction/elbow, finger, wrist ext Emphasize wrist/finger movements independent of shoulder/elbow motions Postacute Rehabilitation LE Control: Prepares patient for gait Pregait mat activities should be out ofsynergy and promote normal gait Pelvic control Postacute Rehabilitation Balance Once initial stability control is achieved in upright postures 26
27 Balance study #1: sit to stand RCT: 32 subjects Subjects in both groups received 30 minutes of general PT 3X/week X 4 weeks. Subjects in experimental group received an additional 15 minutes of sit-to-stand training each time. Balance study #1: sit to stand Results: significant improvements in directional control anteriorly and hip extensor strength for the experimental group. Additional sit to stand training is encouraged due to effects on dynamic balance and extensor muscle strength in subjects with stroke Tung et al (2010) Balance Study #2: late after CVA RCT: 41 subjects with hemiparesis mean time after stroke (6 months) Control group: conventional stroke inpatient rehab Experimental group: 15 sessions of balance training in addition to the conventional program 27
28 Balance Study #2: late after CVA 3D computerized gait analysis system one week before and after the program Control group did not show any significant difference re: gait Experimental group: significant improvement in pelvic excursion in frontal plane and vertical ground reaction force Balance Study #2: late after CVA Balance training using force platform biofeedback in additional to conventional stroke rehab is beneficial in improving postural control and weight bearing on the paretic side while walking late after stroke. Yavuzer et al (2006) Postacute Rehabilitation Gait training: walking is initiated early Early Walking prevents Movement deficiencies will vary 28
29 Postacute Rehabilitation practice forward, backwards, sideways, braiding elevation activities different surfaces orthoses may be necessary Gait If someone has UE flexor synergy, what types of A.D. would be most appropriate? Study #1: Walking after Stroke A single-blind RCT with 97 participants recruited within 6 weeks of stroke onset, All participants received conventional rehab. Those randomly assigned to the control group also received overground gait training only and those assigned to the experimental group received gait training with body weight support on a treadmill. 29
30 Study #1: Walking after Stroke Outcomes measures used to assess the difference between the 2 groups: Motricity Index, Trunk Control Test, Barthel Index, Functional Ambulation Categories, 10-meter and 6-minute walk tests, and Walking Handicap Scale. Assessments done at baseline, after 20 treatment sessions, 2 weeks after treatment and 6 months after stroke Study #1: Walking after Stroke After treatment, all patients were able to walk. Both groups showed improvement in all outcome measures. No differences were seen between the 2 groups before, during or after treatment and follow up. Franceschini et al, 2009 Study #2: Walking After Stroke RCT: 25 subjects recruited within 90 days of stroke onset Both subjects received PT 5 days/week based on Bobath X 3 weeks. Gait training for control group: ambulate on floor surface at comfortable speed using AD, assistance and rest periods as needed. 30
31 Study #2: Walking After Stroke Gait training for experimental group: ambulating on treadmill, which was adjusted to the subject s comfortable walking speed. Subjects held horizontal bar in front or at side with the PT standing next to them assisting with hip flexion and foot placement as needed Study #2: Walking After Stroke Results: treadmill training may be more effective that conventional gait training for improving some gait parameters such as functional ambulation, stride length, percentage of paretic single stance period and gastrocnemius muscle activity Laufer et al (2001) Postacute Rehabilitation Functional training: variety of activities and postures can be utilized getting down and up from the floor varying the environment is important to ensure adaptability and generalizability training in ADL is usually directed by the OT must maintain open lines of communications between team members to direct the plan of care 31
32 Postacute Rehabilitation optimum motor learning can be achieved through: demonstration at the ideal performance speed manually guiding the patient through the movement encouraging early active participation (affected side) Postacute Rehabilitation practicing the movement on the unaffected side first simultaneous practice of similar movements on both sides visualization Patient and Family Education Provide accurate, factual information; counsel family about the patient s capabilities and limitations; avoid predictions Give only as much information as needed; be consistent and repeat information 32
33 Patient and Family Education Provide a forum for open discussion and communication Be supportive, sensitive, and maintain a hopeful manner Discharge Planning Family members should know the HEP, and proper performance of exercises Home visits Trial stays at home OP or home care may continue treatment REFERENCES Feys HM, De Weerdt WJ, et al (1998) Effect of a Therapeutic Intervention for the Hemiplegic Upper Limb in the Acute Phase After Stroke: A Single-Blind, Randomized, Controlled Multicenter Trial. Stroke 29: Franceschini M, Carda S, Agosti M, Antenucci R, MalgratiD, and Cisara C. (2009). Walking after Stroke: What Does Treadmill Training with Body Weight Supported Add to Overground Training in Patients Early After Stroke? Stroke-Journal of the American Heart Association, vol. 40, Laufer Y, Dickstein R, Chefez Y, & Marcovitz E. (2001) The Effect of Treadmill Training on the Ambulation of Stroke Survivors in the Early Stages of Rehabilitation: A Randomized Study. Journal of Rehabilitation Research and Development, 38(1): O Sullivan, S.B. & Schmitz, T.J., (2000), Physical Rehabilitation, 4 th Ed., F.A. Davis Company: Philadelphia. 33
34 REFERENCES continued Tung F, Tang Y, Lee C, Wang R. (2010) Balance Outcomes After Additional Sitto-Stand Training in Subjects with Stroke: A Randomized Controlled Trial. Clinical Rehabilitation, 24, Yavuzer, G, Eser, F et al (2006). The Effects of Balance Training on Gait Late After Stroke: A Randomized Controlled Trial. Clinical Rehabilitation. 20:
Home Exercise Program Progression and Components of the LTP Intervention. HEP Activities at Every Session Vital signs monitoring
 Home Exercise Program Progression and Components of the LTP Intervention HEP Activities at Every Session Vital signs monitoring Blood pressure, heart rate, Borg Rate of Perceived Exertion (RPE) and oxygen
Home Exercise Program Progression and Components of the LTP Intervention HEP Activities at Every Session Vital signs monitoring Blood pressure, heart rate, Borg Rate of Perceived Exertion (RPE) and oxygen
Benefits of Weight bearing increased awareness of the involved side decreased fear improved symmetry regulation of muscle tone
 From the information we have gathered during our Evaluation, the Clinical Reasoning we used to identify key problem areas and the Goals Established with functional outcomes we now have enough information
From the information we have gathered during our Evaluation, the Clinical Reasoning we used to identify key problem areas and the Goals Established with functional outcomes we now have enough information
Somatic Adaptation in Cerebral Palsy LINKING ASSESSMENT WITH TREATMENT: AN NDT PERSPECTIVE. By W. Michael Magrun, M.S., OTR/L
 Somatic Adaptation in Cerebral Palsy LINKING ASSESSMENT WITH TREATMENT: AN NDT PERSPECTIVE By W. Michael Magrun, M.S., OTR/L INTRODUCTION Somatic adaptation is one of the primary functions of the central
Somatic Adaptation in Cerebral Palsy LINKING ASSESSMENT WITH TREATMENT: AN NDT PERSPECTIVE By W. Michael Magrun, M.S., OTR/L INTRODUCTION Somatic adaptation is one of the primary functions of the central
Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual
 Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual 2nd Edition Isabelle M. Bohman, M.S., P.T., NDT Coordinator Instructor TM Published by Clinician s View Albuquerque, NM 505-880-0058
Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual 2nd Edition Isabelle M. Bohman, M.S., P.T., NDT Coordinator Instructor TM Published by Clinician s View Albuquerque, NM 505-880-0058
Evaluating Movement Posture Disorganization
 Evaluating Movement Posture Disorganization A Criteria-Based Reference Format for Observing & Analyzing Motor Behavior in Children with Learning Disabilities By W. Michael Magrun, MS, OTR 3 R D E D I T
Evaluating Movement Posture Disorganization A Criteria-Based Reference Format for Observing & Analyzing Motor Behavior in Children with Learning Disabilities By W. Michael Magrun, MS, OTR 3 R D E D I T
GLOSSARY. Active assisted movement: movement where the actions are assisted by an outside force.
 GLOSSARY The technical words used in this guide are listed here in alphabetic order. The first time one of these words is used in the guide, it is written in italics. Sometimes there is reference to a
GLOSSARY The technical words used in this guide are listed here in alphabetic order. The first time one of these words is used in the guide, it is written in italics. Sometimes there is reference to a
1 Pause and Practice: Facilitating Trunk and Shoulder Control with the Therapy Ball
 1 Pause and Practice: Facilitating Trunk and Shoulder Control with the Therapy Ball This is an example of Facilitating Combinations of Movements and Active Assist. Starting Position Have your patient sit
1 Pause and Practice: Facilitating Trunk and Shoulder Control with the Therapy Ball This is an example of Facilitating Combinations of Movements and Active Assist. Starting Position Have your patient sit
copyrighted material by PRO-ED, Inc.
 Contents Preparation for Functional Sitting Partial Pull to Sit.......................................................... 2 Pull to Sit................................................................ 3
Contents Preparation for Functional Sitting Partial Pull to Sit.......................................................... 2 Pull to Sit................................................................ 3
Hemiplegic Shoulder. Incidence & Rationale. Shoulder Pain Assessment & Treatment
 Hemiplegic Shoulder Jeane Davis Fyfe OT, Senior Therapist Incidence & Rationale Up to 72% of stroke survivors will experience shoulder pain Shoulder pain may inhibit patient participation in rehabilitation
Hemiplegic Shoulder Jeane Davis Fyfe OT, Senior Therapist Incidence & Rationale Up to 72% of stroke survivors will experience shoulder pain Shoulder pain may inhibit patient participation in rehabilitation
Scapular Protraction in Sitting
 9 Pause and Practice: Scapular Protraction in Sitting This practice lab is an example of putting muscles on length in order to achieve proper alignment of shoulder structures in preparation for facilitating
9 Pause and Practice: Scapular Protraction in Sitting This practice lab is an example of putting muscles on length in order to achieve proper alignment of shoulder structures in preparation for facilitating
University of Manitoba - MPT: Neurological Clinical Skills Checklist
 Name: Site: Assessment Skills Observed Performed Becoming A. Gross motor function i. Describe movement strategies (quality, devices, timeliness, independence): supine sidelying sit stand supine long sitting
Name: Site: Assessment Skills Observed Performed Becoming A. Gross motor function i. Describe movement strategies (quality, devices, timeliness, independence): supine sidelying sit stand supine long sitting
Active-Assisted Stretches
 1 Active-Assisted Stretches Adequate flexibility is fundamental to a functional musculoskeletal system which represents the foundation of movement efficiency. Therefore a commitment toward appropriate
1 Active-Assisted Stretches Adequate flexibility is fundamental to a functional musculoskeletal system which represents the foundation of movement efficiency. Therefore a commitment toward appropriate
Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme
 Chapter FOUR Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme Chris Higgs Cathy Chapple Daniel Pinto J. Haxby Abbott 99 n n 100 General Guidelines Knee Exercise
Chapter FOUR Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme Chris Higgs Cathy Chapple Daniel Pinto J. Haxby Abbott 99 n n 100 General Guidelines Knee Exercise
PTA 210 PTA Techniques
 PTA 210 PTA Techniques Patient Positioning and Draping INTRO Patient Positioning Must be considered before, during and after treatment AND when the patient is to be at rest for a prolonged period of time
PTA 210 PTA Techniques Patient Positioning and Draping INTRO Patient Positioning Must be considered before, during and after treatment AND when the patient is to be at rest for a prolonged period of time
Fitball and Pilates Unite Filex 2017
 Fitball and Pilates Unite Filex 2017 Lisa Westlake www.physicalbest.com Pilates, fitball and physiotherapy blend perfectly to fine tune movement and postural awareness and provide a focus on technique,
Fitball and Pilates Unite Filex 2017 Lisa Westlake www.physicalbest.com Pilates, fitball and physiotherapy blend perfectly to fine tune movement and postural awareness and provide a focus on technique,
What is Kinesiology? Basic Biomechanics. Mechanics
 What is Kinesiology? The study of movement, but this definition is too broad Brings together anatomy, physiology, physics, geometry and relates them to human movement Lippert pg 3 Basic Biomechanics the
What is Kinesiology? The study of movement, but this definition is too broad Brings together anatomy, physiology, physics, geometry and relates them to human movement Lippert pg 3 Basic Biomechanics the
Functional Movement Test. Deep Squat
 Functional Movement Test Put simply, the FMS is a ranking and grading system that documents movement patterns that are key to normal function. By screening these patterns, the FMS readily identifies functional
Functional Movement Test Put simply, the FMS is a ranking and grading system that documents movement patterns that are key to normal function. By screening these patterns, the FMS readily identifies functional
Flexibility. STRETCH: Kneeling gastrocnemius. STRETCH: Standing gastrocnemius. STRETCH: Standing soleus. Adopt a press up position
 STRETCH: Kneeling gastrocnemius Adopt a press up position Rest one knee on mat with the opposite leg straight Maintain a neutral spine position Push through arms to lever ankle into increased dorsiflexion
STRETCH: Kneeling gastrocnemius Adopt a press up position Rest one knee on mat with the opposite leg straight Maintain a neutral spine position Push through arms to lever ankle into increased dorsiflexion
Hemiplegic Shoulder Power Point for staff education sessions
 Appendix B Hemiplegic Shoulder Power Point for staff education sessions Jennifer Curry Physiotherapist, London Health Sciences Centre www.swostroke.ca Acknowledgements Maria Lung BSc (PT), MSc Train the
Appendix B Hemiplegic Shoulder Power Point for staff education sessions Jennifer Curry Physiotherapist, London Health Sciences Centre www.swostroke.ca Acknowledgements Maria Lung BSc (PT), MSc Train the
PTA 210 PTA Techniques. Patient Positioning and Draping
 PTA 210 PTA Techniques Patient Positioning and Draping Review Last Lecture 5 vital signs you are responsible for? What is patency? How do you test it? Pressing too hard with HR can cause Contraindications
PTA 210 PTA Techniques Patient Positioning and Draping Review Last Lecture 5 vital signs you are responsible for? What is patency? How do you test it? Pressing too hard with HR can cause Contraindications
Chapter 8 8/23/2016. Body Mechanics and Patient Mobility. Introduction to Body Mechanics and Patient Mobility
 Chapter 8 Body Mechanics and Patient Mobility All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Introduction to Body Mechanics and Patient Mobility
Chapter 8 Body Mechanics and Patient Mobility All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Introduction to Body Mechanics and Patient Mobility
STROKE POSITIONING, TRANSFERRING & SHOULDER MANAGEMENT IN ACUTE AND REHAB
 STROKE POSITIONING, TRANSFERRING & SHOULDER MANAGEMENT IN ACUTE AND REHAB PRESENTED BY: Francine Carrier-Stevens, PT. Natasha Uens, PT. Chelsea Foster, RN. OVERVIEW Objectives Factors affecting mobility
STROKE POSITIONING, TRANSFERRING & SHOULDER MANAGEMENT IN ACUTE AND REHAB PRESENTED BY: Francine Carrier-Stevens, PT. Natasha Uens, PT. Chelsea Foster, RN. OVERVIEW Objectives Factors affecting mobility
Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner
 Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner Eric Chaconas PT, PhD, DPT, FAAOMPT Assistant Professor and Assistant Program Director Doctor of Physical Therapy Program Eric
Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner Eric Chaconas PT, PhD, DPT, FAAOMPT Assistant Professor and Assistant Program Director Doctor of Physical Therapy Program Eric
Summary Chart 1 2 months
 NEWBORN Physiological flexion provides stability for posture & random movements Neck righting Labyrinthine righting beginning in prone & supine Primary standing reaction Movements limited by available
NEWBORN Physiological flexion provides stability for posture & random movements Neck righting Labyrinthine righting beginning in prone & supine Primary standing reaction Movements limited by available
Most hypertensive: headache, vomiting, seizures, changes in mental status, fever, changes EKG
 Wk 2. Management of Clients with Stroke 1. Stroke neurologic changes by interruption in blood supply to brain 1) Etiology Ischemia: thrombosis or embolism thrombotic strokes > embolic strokes (1) Thrombosis
Wk 2. Management of Clients with Stroke 1. Stroke neurologic changes by interruption in blood supply to brain 1) Etiology Ischemia: thrombosis or embolism thrombotic strokes > embolic strokes (1) Thrombosis
Normal development & reflex
 Normal development & reflex Definition of Development : acquisition & refinement of skills 1 대근육운동발달 2 소근육운동발달 3 대인관계및사회성발달 4 적응능력혹은비언어성발달 5 의사소통및언어발달 6 학습, 청각, 시각의발달 Department of Rehabilitation Medicine,
Normal development & reflex Definition of Development : acquisition & refinement of skills 1 대근육운동발달 2 소근육운동발달 3 대인관계및사회성발달 4 적응능력혹은비언어성발달 5 의사소통및언어발달 6 학습, 청각, 시각의발달 Department of Rehabilitation Medicine,
Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology
 Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology Activity Everyone stand up, raise your right hand, tell your neighbors your name 1 What part of the brain
Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology Activity Everyone stand up, raise your right hand, tell your neighbors your name 1 What part of the brain
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
NDTA BASIC ADULT COURSE KEY TO COURSE CONTENT
 Topic: Atypical Patterns of Movement Learning outcome(s) that pertain to occupational therapists 1. Identify the influence of atypical patterns of movement on: Postural alignment Transitional movements
Topic: Atypical Patterns of Movement Learning outcome(s) that pertain to occupational therapists 1. Identify the influence of atypical patterns of movement on: Postural alignment Transitional movements
I will explain the most important concepts of functional treatment while treating our 4 patients: Tom Clint Alice Dick
 Every step we ve covered so far, from Evaluation to Clinical Reasoning to Establishing Goals and Preparation for Function has laid the groundwork for the final step: Treatment Using Functional Activities.
Every step we ve covered so far, from Evaluation to Clinical Reasoning to Establishing Goals and Preparation for Function has laid the groundwork for the final step: Treatment Using Functional Activities.
LEAPS (Locomotor Experience Applied Post-Stroke) Home Exercise Program (HEP) Therapist Intervention Manual
 LEAPS (Locomotor Experience Applied Post-Stroke) Home Exercise Program (HEP) Therapist Intervention Manual Brooks Rehabilitation Center, Jacksonville, FL Florida Hospital, Orlando, FL Long Beach Memorial
LEAPS (Locomotor Experience Applied Post-Stroke) Home Exercise Program (HEP) Therapist Intervention Manual Brooks Rehabilitation Center, Jacksonville, FL Florida Hospital, Orlando, FL Long Beach Memorial
Osteoporosis Protocol
 PRODUCTS HELPING PEOPLE HELP THEMSELVES! Osteoporosis Protocol Rehabilitation using the Resistance Chair General Information Osteoporosis is a condition where bones gradually decrease in mass or density
PRODUCTS HELPING PEOPLE HELP THEMSELVES! Osteoporosis Protocol Rehabilitation using the Resistance Chair General Information Osteoporosis is a condition where bones gradually decrease in mass or density
MOTOR EVALUATION SCALE FOR UPPER EXTREMITY IN STROKE PATIENTS (MESUPES-arm and MESUPES-hand)
 MOTOR EVALUATION SCALE FOR UPPER EXTREMITY IN STROKE PATIENTS (MESUPES-arm and MESUPES-hand) Name patient: Test date - hour: Name examiner: Duration of the test: min Handedness: right/left Support sitting
MOTOR EVALUATION SCALE FOR UPPER EXTREMITY IN STROKE PATIENTS (MESUPES-arm and MESUPES-hand) Name patient: Test date - hour: Name examiner: Duration of the test: min Handedness: right/left Support sitting
Shoulder Exercises. Wall Press Up with Gym Ball
 Shoulder Exercises The exercises listed below are part of a treatment regime for patients attending The Police Rehabilitation Centre. They are reproduced here as an aide memoire for those patients. The
Shoulder Exercises The exercises listed below are part of a treatment regime for patients attending The Police Rehabilitation Centre. They are reproduced here as an aide memoire for those patients. The
Sensory. Physical. Cognitive. Language 4/12/2016 LEARNING OBJECTIVES AT ASSESSMENT: SKILLS EVALUATION OVERVIEW
 ASSISTIVE TECHNOLOGY ASSESSMENT: SEATING AND POSITIONING FOR ACCESS Anne Cronin 2016 LEARNING OBJECTIVES Describe the principles related to assessment and intervention in assistive technology (AT) service
ASSISTIVE TECHNOLOGY ASSESSMENT: SEATING AND POSITIONING FOR ACCESS Anne Cronin 2016 LEARNING OBJECTIVES Describe the principles related to assessment and intervention in assistive technology (AT) service
The Chailey Levels of Ability Assessment Charts
 The Chailey Levels of Ability Assessment Charts Assessment details NAME D.O.B. DIAGNOSIS DATE OF ASSESSMENT ASSESSMENT CENTRE NAME OF ASSESSOR Notes CHAILEY HERITAGE CLINICAL SERVICES Beggars Wood Road
The Chailey Levels of Ability Assessment Charts Assessment details NAME D.O.B. DIAGNOSIS DATE OF ASSESSMENT ASSESSMENT CENTRE NAME OF ASSESSOR Notes CHAILEY HERITAGE CLINICAL SERVICES Beggars Wood Road
ATHLETIC CONDITIONING ON THE ARC BARREL
 ATHLETIC CONDITIONING ON THE ARC BARREL page 1 INTRODUCTION The STOTT PILATES Athletic Conditioning stream serves as a bridge between STOTT PILATES standard repertoire and the CORE Athletic Conditioning
ATHLETIC CONDITIONING ON THE ARC BARREL page 1 INTRODUCTION The STOTT PILATES Athletic Conditioning stream serves as a bridge between STOTT PILATES standard repertoire and the CORE Athletic Conditioning
Hemiplegic Shoulder Power Point for staff education sessions
 Hemiplegic Shoulder Power Point for staff education sessions Presented by Cathy McBay and Candace Coe HHS Stroke Annual Review March 7 and 7, 2018 www.swostroke.ca Overview Structure of the Shoulder Complex
Hemiplegic Shoulder Power Point for staff education sessions Presented by Cathy McBay and Candace Coe HHS Stroke Annual Review March 7 and 7, 2018 www.swostroke.ca Overview Structure of the Shoulder Complex
2017 COS ANNUAL MEETING AND EXHIBITION HOME EXERCISES
 UPPER BODY Push Up From a push up position. Lower whole body down to floor. Press up to return to start position. Maintain abdominal hollow and neutral spinal alignment throughout movement. Note: Perform
UPPER BODY Push Up From a push up position. Lower whole body down to floor. Press up to return to start position. Maintain abdominal hollow and neutral spinal alignment throughout movement. Note: Perform
Assessment Form Post Polio Syndrome and Late Effects of Polio
 FULL NAME: DATE OF BIRTH: PHONE NUMBER: CURRENT HOME ADDRESS: EMAIL ADDRESS: THERAPIST: REFERRAL SOURCE: CURRENT GP: NEXT OF KIN: ACC/NHI NUMBER: PATIENT GOALS OF TODAY S ASSESSMENT: MAIN PROBLEMS PATIENT
FULL NAME: DATE OF BIRTH: PHONE NUMBER: CURRENT HOME ADDRESS: EMAIL ADDRESS: THERAPIST: REFERRAL SOURCE: CURRENT GP: NEXT OF KIN: ACC/NHI NUMBER: PATIENT GOALS OF TODAY S ASSESSMENT: MAIN PROBLEMS PATIENT
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol
 Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
A comparison of two patients with Guillain-Barre Syndrome J O H N C O R S I N O, S P T
 A comparison of two patients with Guillain-Barre Syndrome J O H N C O R S I N O, S P T Guillain-Barre Acute inflammatory demyelinating polyneuropathy Highly diverse presentation, course, outcome Miller-Fisher:
A comparison of two patients with Guillain-Barre Syndrome J O H N C O R S I N O, S P T Guillain-Barre Acute inflammatory demyelinating polyneuropathy Highly diverse presentation, course, outcome Miller-Fisher:
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Issues in Cerebral Palsy Part 2: Physical Handling Treatment by Christine A. Nelson, Ph.D., OTR with contribution by W. Michael Magrun, MS, OTR
 The following article is granted 1 Contact Hour/ equivalent to.15 CEU/equivalent to 1.25 PDUs. To receive CEU credit you must complete the CEU Exam after reading the article. Close the PDF file after reading
The following article is granted 1 Contact Hour/ equivalent to.15 CEU/equivalent to 1.25 PDUs. To receive CEU credit you must complete the CEU Exam after reading the article. Close the PDF file after reading
Cerebrovascular Disorders. Blood, Brain, and Energy. Blood Supply to the Brain 2/14/11
 Cerebrovascular Disorders Blood, Brain, and Energy 20% of body s oxygen usage No oxygen/glucose reserves Hypoxia - reduced oxygen Anoxia - Absence of oxygen supply Cell death can occur in as little as
Cerebrovascular Disorders Blood, Brain, and Energy 20% of body s oxygen usage No oxygen/glucose reserves Hypoxia - reduced oxygen Anoxia - Absence of oxygen supply Cell death can occur in as little as
Overview Functional Training
 Overview Functional Training Exercises with Therapist 1. Sitting 2. Standing up vs. Sitting down 3. Standing 4. Stance phase ( Static and dynamic ) 5. Swing phase 6. Gait Evaluation 7. Walking level ground
Overview Functional Training Exercises with Therapist 1. Sitting 2. Standing up vs. Sitting down 3. Standing 4. Stance phase ( Static and dynamic ) 5. Swing phase 6. Gait Evaluation 7. Walking level ground
1-Apley scratch test.
 1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
Double Knee to Chest. Lying on back with knees slightly bent. Hug both knees to chest
 Double Knee to Chest Lying on back with knees slightly bent Hug both knees to chest Flexion on the Gymnic Ball Lying on stomach over ball Drape body over ball and relax Roll back and forth to stretch out
Double Knee to Chest Lying on back with knees slightly bent Hug both knees to chest Flexion on the Gymnic Ball Lying on stomach over ball Drape body over ball and relax Roll back and forth to stretch out
General Procedure and Rules
 General Procedure and Rules PROCEDURE Description: This assessment is a measure of upper extremity (UE) and lower extremity (LE) motor and sensory impairment. Equipment: A chair, bedside table, reflex
General Procedure and Rules PROCEDURE Description: This assessment is a measure of upper extremity (UE) and lower extremity (LE) motor and sensory impairment. Equipment: A chair, bedside table, reflex
EVALUATION AND MEASUREMENTS. I. Devreux
 EVALUATION AND MEASUREMENTS I. Devreux To determine the extent and degree of muscular weakness resulting from disease, injury or disuse. The records obtained from these tests provide a base for planning
EVALUATION AND MEASUREMENTS I. Devreux To determine the extent and degree of muscular weakness resulting from disease, injury or disuse. The records obtained from these tests provide a base for planning
Clinical Information for Wheeled Mobility Page 1 of 6
 Clinical Information for Wheeled Mobility Page 1 of 6 PART A: PATIENT / PROVIDER INFORMATION - Please Print Name: Sponsor Soc. Sec. No: Address: City: St: Zip: Phone: ( ) Age: Sex: Height: Weight: Date
Clinical Information for Wheeled Mobility Page 1 of 6 PART A: PATIENT / PROVIDER INFORMATION - Please Print Name: Sponsor Soc. Sec. No: Address: City: St: Zip: Phone: ( ) Age: Sex: Height: Weight: Date
BIOFEEDBACK AND HIPPOTHERAPY, FROM THE BOBATHCONCEPT, AS. HYPERTHERAPY WITH CONGENITAL HEMIPARESIS. (Daniël BENS, Belgium)
 BIOFEEDBACK AND HIPPOTHERAPY, FROM THE BOBATHCONCEPT, AS HYPERTHERAPY WITH CONGENITAL HEMIPARESIS. (Daniël BENS, Belgium) Many techniques of treatment for the child with cerebral palsy have developed over
BIOFEEDBACK AND HIPPOTHERAPY, FROM THE BOBATHCONCEPT, AS HYPERTHERAPY WITH CONGENITAL HEMIPARESIS. (Daniël BENS, Belgium) Many techniques of treatment for the child with cerebral palsy have developed over
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
The Language of Anatomy. (Anatomical Terminology)
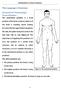 The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
An overview of posture
 An overview of posture What is posture? Posture is the description of an overall body position. This can be intentional or unintentional how we are hold our bodies, but it is the way each individual will
An overview of posture What is posture? Posture is the description of an overall body position. This can be intentional or unintentional how we are hold our bodies, but it is the way each individual will
Range of motion and positioning
 Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
DEEP SQUAT. Upper torso is parallel with tibia or toward vertical Femur below horizontal Knees are aligned over feet Dowel aligned over feet
 APPENDIX 9 SCORING CRITERIA DEEP SQUAT Upper torso is parallel with tibia or toward vertical Femur below horizontal Knees are aligned over feet Dowel aligned over feet Upper torso is parallel with tibia
APPENDIX 9 SCORING CRITERIA DEEP SQUAT Upper torso is parallel with tibia or toward vertical Femur below horizontal Knees are aligned over feet Dowel aligned over feet Upper torso is parallel with tibia
Slide 1. Slide 2. Slide 3. Intro to Physical Therapy for Neuromuscular Conditions. PT Evaluation. PT Evaluation
 Slide 1 Intro to Physical Therapy for Neuromuscular Conditions PTA 103 Introduction to Clinical Practice 2 Slide 2 Mental status: consciousness, attention, orientation, cognition Communication: speech
Slide 1 Intro to Physical Therapy for Neuromuscular Conditions PTA 103 Introduction to Clinical Practice 2 Slide 2 Mental status: consciousness, attention, orientation, cognition Communication: speech
GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017
 GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to be
GENERAL EXERCISES KNEE BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to be
Understanding Stroke
 MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Understanding Stroke About This Kit Stroke is the fourth leading cause of death in Canada after heart disease and
MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Understanding Stroke About This Kit Stroke is the fourth leading cause of death in Canada after heart disease and
Mobility sequencing!
 Mobility sequencing When practicing joint mobility drills we have the opportunity to improve our movement. The muscles associated with the joint being mobilised as well as the joint itself will improve
Mobility sequencing When practicing joint mobility drills we have the opportunity to improve our movement. The muscles associated with the joint being mobilised as well as the joint itself will improve
Do the same as above, but turn your head TOWARDS the side that you re holding on to the chair.
 Stretch 4-6 times per day and hold each stretch for a minimum of 30 seconds. Perform the stretch gently without bouncing. Discuss any problems with your Chiropractor. Sit upright with your head and shoulder
Stretch 4-6 times per day and hold each stretch for a minimum of 30 seconds. Perform the stretch gently without bouncing. Discuss any problems with your Chiropractor. Sit upright with your head and shoulder
REMEMBER GOOD POSTURE DURING ALL YOUR EXERCISES, AVOID SLOUCHING AS YOUR CURRENT PROGRAM BECOMES EASY SLOWLY INCREASE:
 REMEMBER GOOD POSTURE DURING ALL YOUR EXERCISES, AVOID SLOUCHING Apr 06, 2017 AS YOUR CURRENT PROGRAM BECOMES EASY SLOWLY INCREASE: # OF LAPS YOU ARE WALKING # OF REPITITIONS # OF SECONDS YOU HOLD A STRETCH
REMEMBER GOOD POSTURE DURING ALL YOUR EXERCISES, AVOID SLOUCHING Apr 06, 2017 AS YOUR CURRENT PROGRAM BECOMES EASY SLOWLY INCREASE: # OF LAPS YOU ARE WALKING # OF REPITITIONS # OF SECONDS YOU HOLD A STRETCH
ACE s Essentials of Exercise Science for Fitness Professionals TRUNK
 ACE s Essentials of Exercise Science for Fitness Professionals TRUNK Posture and Balance Posture refers to the biomechanical alignment of the individual body parts and the orientation of the body to the
ACE s Essentials of Exercise Science for Fitness Professionals TRUNK Posture and Balance Posture refers to the biomechanical alignment of the individual body parts and the orientation of the body to the
Taking Action for Optimal Community and Long-Term stroke Care A Resource for Healthcare Providers
 Taking Action for Optimal Community and Long-Term stroke Care A Resource for Healthcare Providers Chapter 6: Activities and Participation Section 6.2: Positioning Copyright Information The Taking Action
Taking Action for Optimal Community and Long-Term stroke Care A Resource for Healthcare Providers Chapter 6: Activities and Participation Section 6.2: Positioning Copyright Information The Taking Action
Shoulder Exercises Phase 1 Phase 2
 Shoulder Exercises Phase 1 1. Pendulum exercise Bend over at the waist and let the arm hang down. Using your body to initiate movement, swing the arm gently forward and backward and in a circular motion.
Shoulder Exercises Phase 1 1. Pendulum exercise Bend over at the waist and let the arm hang down. Using your body to initiate movement, swing the arm gently forward and backward and in a circular motion.
Stroke. Objectives: After you take this class, you will be able to:
 Stroke Objectives: After you take this class, you will be able to: 1. Describe the signs of a stroke and how a stroke happens. 2. Discuss stroke risk factors. 3. Detail the care and rehabilitation of a
Stroke Objectives: After you take this class, you will be able to: 1. Describe the signs of a stroke and how a stroke happens. 2. Discuss stroke risk factors. 3. Detail the care and rehabilitation of a
Low Back Pain Home Exercises
 Low Back Pain Home Exercises General Instructions The low back exercise program is a series of stretching exercises and strengthening exercises prescribed by your physician for your medical condition.
Low Back Pain Home Exercises General Instructions The low back exercise program is a series of stretching exercises and strengthening exercises prescribed by your physician for your medical condition.
Shoulder Exercises 2016
 Shoulder Exercises 2016 The exercises listed below are part of a treatment regime for patients attending The Police Rehabilitation Centre. They are reproduced here as an aide memoire for those patients.
Shoulder Exercises 2016 The exercises listed below are part of a treatment regime for patients attending The Police Rehabilitation Centre. They are reproduced here as an aide memoire for those patients.
DO NOT SIT WITHOUT PROPER FIT. Objectives. Recommendations 4/23/2014 CSMC Participants will be able to:
 DO NOT SIT WITHOUT PROPER FIT CSMC 2014 Presented by: Elizabeth Cole, MSPT, ATP Director of Clinical Rehab Services Objectives Participants will be able to: Match each anatomical measurement to the corresponding
DO NOT SIT WITHOUT PROPER FIT CSMC 2014 Presented by: Elizabeth Cole, MSPT, ATP Director of Clinical Rehab Services Objectives Participants will be able to: Match each anatomical measurement to the corresponding
Lower Extremity Physical Performance Testing. Return to Function (Level I): Core Stability
 Physical performance testing is completed with patients in order to collect data and make observations regarding the overall function of the limb integrated into the entire functional unit of the body,
Physical performance testing is completed with patients in order to collect data and make observations regarding the overall function of the limb integrated into the entire functional unit of the body,
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
Vascular Disorders. Nervous System Disorders (Part B-1) Module 8 -Chapter 14. Cerebrovascular disease S/S 1/9/2013
 Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Stand Tall with Osteoporosis thru Pilates
 Stand Tall with Osteoporosis thru Pilates C A S S I T E R P E N I N G P T, D P T, C S C S, C P I C H R I S R I E G E R P T U P S T A T E U N I V E R S I T Y H O S P I T A L J U N E 1 9, 2 0 1 7 Content
Stand Tall with Osteoporosis thru Pilates C A S S I T E R P E N I N G P T, D P T, C S C S, C P I C H R I S R I E G E R P T U P S T A T E U N I V E R S I T Y H O S P I T A L J U N E 1 9, 2 0 1 7 Content
Conservative Massive Rotator Cuff Tear Protocol
 SPORTS & ORTHOPAEDIC SPECIALISTS Conservative Massive Rotator Cuff Tear Protocol 3-4 visits over 4-6 weeks Emphasis is on AAROM and a high repetition, low weight free weight program Emphasize improved
SPORTS & ORTHOPAEDIC SPECIALISTS Conservative Massive Rotator Cuff Tear Protocol 3-4 visits over 4-6 weeks Emphasis is on AAROM and a high repetition, low weight free weight program Emphasize improved
Cerebrovascular Accidents
 CHAPTER 10 Cerebrovascular Accidents OBJECTIVES After reading this chapter, the student will be able to 1. Understand the etiology and clinical manifestations of stroke. 2. Identify common complications
CHAPTER 10 Cerebrovascular Accidents OBJECTIVES After reading this chapter, the student will be able to 1. Understand the etiology and clinical manifestations of stroke. 2. Identify common complications
Dynamic Flexibility All exercises should be done smoothly while taking care to maintain good posture and good technique.
 Dynamic Flexibility All exercises should be done smoothly while taking care to maintain good posture and good technique. Lying on back: Hip Crossover: Arms out in T position, feet flat on the floor, knees
Dynamic Flexibility All exercises should be done smoothly while taking care to maintain good posture and good technique. Lying on back: Hip Crossover: Arms out in T position, feet flat on the floor, knees
Neck Rehabilitation programme for Rugby players.
 Neck Rehabilitation programme for Rugby players. The programme consists of two parts, first the Therapeutic Exercise Programme to improve biomechanical function and secondly the Rehabilitation programme
Neck Rehabilitation programme for Rugby players. The programme consists of two parts, first the Therapeutic Exercise Programme to improve biomechanical function and secondly the Rehabilitation programme
E X P L A I N I N G STROKE
 EXPLAINING STROKE Introduction Explaining Stroke is a practical step-by-step booklet that explains how a stroke happens, different types of stroke and how to prevent a stroke. Many people think a stroke
EXPLAINING STROKE Introduction Explaining Stroke is a practical step-by-step booklet that explains how a stroke happens, different types of stroke and how to prevent a stroke. Many people think a stroke
EXERCISE AND CYSTIC FIBROSIS: MY EXERCISE RECORD
 EXERCISE AND CYSTIC FIBROSIS: MY EXERCISE RECORD My exercise goals Name What is my target heart rate? What is the maximum heart rate I should not exceed? What is my target rating of perceived exertion?
EXERCISE AND CYSTIC FIBROSIS: MY EXERCISE RECORD My exercise goals Name What is my target heart rate? What is the maximum heart rate I should not exceed? What is my target rating of perceived exertion?
DON T JUST PROVIDE A BAND-AID ELIZABETH COLE, MSPT, ATP U.S. Rehab / VGM
 DON T JUST PROVIDE A BAND-AID ELIZABETH COLE, MSPT, ATP U.S. Rehab / VGM Selecting the most appropriate product solutions for specific postural problems should be a thoughtful exercise in analyzing the
DON T JUST PROVIDE A BAND-AID ELIZABETH COLE, MSPT, ATP U.S. Rehab / VGM Selecting the most appropriate product solutions for specific postural problems should be a thoughtful exercise in analyzing the
OBJECTIVES. Unit 7:5 PROPERTIES OR CHARACTERISTICS OF MUSCLES. Introduction. 3 Kinds of Muscles. 3 Kinds of Muscles 4/17/2018 MUSCULAR SYSTEM
 OBJECTIVES Unit 7:5 MUSCULAR SYSTEM Compare the three main kinds of muscles by describing the action of each Differentiate between voluntary and involuntary muscles List at least three functions of muscles
OBJECTIVES Unit 7:5 MUSCULAR SYSTEM Compare the three main kinds of muscles by describing the action of each Differentiate between voluntary and involuntary muscles List at least three functions of muscles
GOLFERS TEN PROGRAM 1. SELF STRETCHING OF THE SHOULDER CAPSULE
 GOLFERS TEN PROGRAM 1. SELF STRETCHING OF THE SHOULDER CAPSULE POSTERIOR CAPSULAR STRETCH Bring your arm across your chest toward the opposite shoulder. With the opposite arm grasp your arm at your elbow.
GOLFERS TEN PROGRAM 1. SELF STRETCHING OF THE SHOULDER CAPSULE POSTERIOR CAPSULAR STRETCH Bring your arm across your chest toward the opposite shoulder. With the opposite arm grasp your arm at your elbow.
CVA. Alison Atwater PA-C
 CVA Alison Atwater PA-C Types of CVAs Ischemic strokes 80% of strokes 2/3 are thrombotic 1/3 are embolic emboli from the heart or arteries feeding the brain such as carotids, vertebral and basilar etc
CVA Alison Atwater PA-C Types of CVAs Ischemic strokes 80% of strokes 2/3 are thrombotic 1/3 are embolic emboli from the heart or arteries feeding the brain such as carotids, vertebral and basilar etc
9/26/2012. Osteokinematics (how the bones move) & Arthrokinematics (how the joints move) Planes & Axes. Planes & Axes continued
 Osteokinematics (how the bones move) & (how the joints move) Planes & Axes Planes of Action = Three fixed lines of reference along which the body is divided. Each plane is at right angles (or perpendicular)
Osteokinematics (how the bones move) & (how the joints move) Planes & Axes Planes of Action = Three fixed lines of reference along which the body is divided. Each plane is at right angles (or perpendicular)
The Golfers Ten Program. 1. Self Stretching of the Shoulder Capsule
 The Golfers Ten Program 1. Self Stretching of the Shoulder Capsule A. Posterior capsular stretch Bring your arm across your chest toward the opposite shoulder. With the opposite arm grasp your arm at your
The Golfers Ten Program 1. Self Stretching of the Shoulder Capsule A. Posterior capsular stretch Bring your arm across your chest toward the opposite shoulder. With the opposite arm grasp your arm at your
Physical Therapy/Core Strengthening Exercises
 303 91 st Ave. NE Ste. A106 Lake Stevens, WA 98258 425-377-8620 www.lakestevensanimalhospital.com Physical Therapy/Core Strengthening Exercises Dogs with osteoarthritis or those recovering from a major
303 91 st Ave. NE Ste. A106 Lake Stevens, WA 98258 425-377-8620 www.lakestevensanimalhospital.com Physical Therapy/Core Strengthening Exercises Dogs with osteoarthritis or those recovering from a major
Neurological Examination
 Neurological Examination Charles University in Prague 1st Medical Faculty and General University Hospital Neurological examination: Why important? clinical history taking and bedside examination: classical
Neurological Examination Charles University in Prague 1st Medical Faculty and General University Hospital Neurological examination: Why important? clinical history taking and bedside examination: classical
Maximal isokinetic and isometric muscle strength of major muscle groups related to age, body weight, height, and sex in 178 healthy subjects
 Maximal isokinetic and isometric muscle strength of major muscle groups related to age, body weight, height, and sex in 178 healthy subjects Test protocol Muscle test procedures. Prior to each test participants
Maximal isokinetic and isometric muscle strength of major muscle groups related to age, body weight, height, and sex in 178 healthy subjects Test protocol Muscle test procedures. Prior to each test participants
Rehab protocol. Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits. Goals:
 Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
The Bambach Saddle Seat in rehabilitation
 7 The Bambach Saddle Seat in rehabilitation The Musculo-skeletal System Good design recognises that our body has a centre of gravity (as does each limb) and maintaining posture close to the neutral centre
7 The Bambach Saddle Seat in rehabilitation The Musculo-skeletal System Good design recognises that our body has a centre of gravity (as does each limb) and maintaining posture close to the neutral centre
Bed Postioning & Mobility
 International Clinical Educators, INC. Bed Postioning & Mobility By Jan Davis, MS, OTR/L About the Author & Presenter Jan Davis, MS, OTR/L, is an internationally recognized leader in educational programs
International Clinical Educators, INC. Bed Postioning & Mobility By Jan Davis, MS, OTR/L About the Author & Presenter Jan Davis, MS, OTR/L, is an internationally recognized leader in educational programs
Training the Joint Replacement Client
 KNEE PRE-OP SAMPLE EXERCISE PLAN Quadricep: Shuttle 1 leg and 2 legs (focus on 1 leg) Leg Press 1 and 2 legs (focus on 1 leg) Sit to Stand (if no pain or compensation) Supine Circle Foam knee extension
KNEE PRE-OP SAMPLE EXERCISE PLAN Quadricep: Shuttle 1 leg and 2 legs (focus on 1 leg) Leg Press 1 and 2 legs (focus on 1 leg) Sit to Stand (if no pain or compensation) Supine Circle Foam knee extension
Commonwealth Health Corporation NEXT
 Commonwealth Health Corporation This computer-based learning (CBL) module details important aspects of musculoskeletal disorders, body mechanics and ergonomics in the workplace. It examines: what causes
Commonwealth Health Corporation This computer-based learning (CBL) module details important aspects of musculoskeletal disorders, body mechanics and ergonomics in the workplace. It examines: what causes
DPT 772 Spine Notebook Matt Kubalski, SPT
 DPT 772 Spine Notebook Matt Kubalski, SPT Table of Contents: IMPAIRMENTS/CLASSIFICATIONS PAGES Neck Pain with Mobility Deficit: Cervicalgia, Pain in thoracic spine - JOSPT 3-6 Neck Pain with Headache:
DPT 772 Spine Notebook Matt Kubalski, SPT Table of Contents: IMPAIRMENTS/CLASSIFICATIONS PAGES Neck Pain with Mobility Deficit: Cervicalgia, Pain in thoracic spine - JOSPT 3-6 Neck Pain with Headache:
Flexibility Exercises for Beginners
 Flexibility Exercises for Beginners 5 flexibility exercises that you can do anytime to give you some get up and go Hello and welcome to your free Flexibility Exercises. Flexibility is needed to perform
Flexibility Exercises for Beginners 5 flexibility exercises that you can do anytime to give you some get up and go Hello and welcome to your free Flexibility Exercises. Flexibility is needed to perform
EXERCISE AND CYSTIC FIBROSIS: MY EXERCISE RECORD
 EXERCISE AND CYSTIC FIBROSIS: MY EXERCISE RECORD My exercise goals Name What is my target heart rate? What is the maximum heart rate I should not exceed? What is my target rating of perceived exertion?
EXERCISE AND CYSTIC FIBROSIS: MY EXERCISE RECORD My exercise goals Name What is my target heart rate? What is the maximum heart rate I should not exceed? What is my target rating of perceived exertion?
Assessing the Stroke Patient. Arlene Boudreaux, MSN, RN, CCRN, CNRN
 Assessing the Stroke Patient Arlene Boudreaux, MSN, RN, CCRN, CNRN Cincinnati Pre-Hospital Stroke Scale May be done by EMS o One of many o F facial droop on one side o A arm drift (hold a pizza box, close
Assessing the Stroke Patient Arlene Boudreaux, MSN, RN, CCRN, CNRN Cincinnati Pre-Hospital Stroke Scale May be done by EMS o One of many o F facial droop on one side o A arm drift (hold a pizza box, close
Sterile gauze used at incision site. Check brace for rubbing or irritation. Compression garment at elbow to be used with physician s authorization
 ULNAR COLLATERAL LIGAMENT RECONSTRUCTION GUIDELINE Functional Outcome Measure KJOC (Appendix 1) should be completed at initial evaluation and at all identified times through guideline, Phase 1 Immediate
ULNAR COLLATERAL LIGAMENT RECONSTRUCTION GUIDELINE Functional Outcome Measure KJOC (Appendix 1) should be completed at initial evaluation and at all identified times through guideline, Phase 1 Immediate
