CONCUSSION GUIDELINES
|
|
|
- Merry Joseph
- 6 years ago
- Views:
Transcription
1 CONCUSSION GUIDELINES EDITION 2017
2 Table of Content 11.1 Summary Principles Introduction What is Concussion? Concussion must be taken extremely seriously What are the signs of Concussion?... 4 Table 1: Common early signs and symptoms of concussion Stage 1: Diagnosis and Management of Concussion Remember the basic rules of First Aid: Recognise and Remove If in Doubt, sit it out Continue to Monitor Medical Practitioner and/or Healthcare Professional present Examples of Memory questions Medical Practitioner and/or Healthcare Professional not present Onset of Symptoms may be DELAYED Stage 2 - Return to Play Graduated Return to Play Protocol... 8 Table 2: Graduated Return to Play Protocol Children & Adolescents... 9 Table 3: Return to School Strategy Recurrence of symptoms during GRTP process Return of Symptoms Residual Effects & Sequelae Useful Links Summary Principles Concussion must be taken extremely seriously to safeguard the long-term welfare of athletes. Athletes suspected of having concussion must be removed from play and must not resume competition or training. Athletes suspected of having concussion must be medically assessed. Athletes suspected of having concussion or diagnosed with concussion must go through a graduated return to play protocol (GRTP). Athletes must receive medical clearance before returning to play.
3 11.2 Introduction Sports Related Concussion (SRC) is considered to be among the most complex injuries in sports medicine to diagnose, assess and manage. FIS takes Athlete Welfare seriously and aims to follow the World Consensus guidance on Concussion in Sport (Zurich 2008/2012; Berlin 2017). Scientific knowledge in the field of concussion is constantly evolving and the consensus process ensures that the FIS guidance keeps pace with these changes.the guidelines were designed to be used by physicians and other health professionals as well as coaches, team managers, teachers, parents and athletes. The guidelines are set out to ensure that athletes who suffer concussion are managed effectively to protect their long-term health and welfare. FIS recommends the following concussion guidelines, which are in line with the 2017 Berlin Consensus statement. We approach this from a conservative and prescriptive angle, according to the Berlin advice. The Pocket Concussion Recognition Tool (PCRT) and Sideline Concussion Assessment Tools (SCAT) that are used to evaluate concussion injuries and guide the recovery process have been updated, and we recommend that the latest versions (SCAT5 and Child SCAT5) are used. NB The PCRT may be used by non-medical personnel; the SCAT tools are for medical personnel only. The FIS guidance is based on the latest international Consensus recommendations. Any deviation from the guidance must be supervised only by medical staff with specific expertise in this field. In practice, the outcomes are often more conservative than those directed in the guidance. For example, the median Return to Play (RTP) time across many sports is normally longer than the recommended 6/7 days. We recognise that the word lists, processes and assessments contained within the SCAT5 tools are likely to be different in different nations. Medical personnel attending to athletes are encouraged to seek appropriately translated SCAT tools if the injured athlete s main language is anything other than English What is Concussion? Concussion is a complex process caused by trauma that transmits force to the brain either directly or indirectly and results in temporary impairment of brain function. Its development and resolution are normally rapid and spontaneous. The majority of Sports Related Concussions (SRCs) occur without loss of consciousness or frank neurological signs. Concussion is associated with a graded set of clinical symptoms and signs that may evolve over time, and that resolve sequentially. Concussion reflects a functional rather than structural injury and standard neuroimaging is typically normal. Athletes participating in the FIS disciplines may be subject to both direct and indirect forces which may lead to a concussion injury.
4 Concussion must be taken extremely seriously Concussion-producing forces (both direct and indirect/transmitted) are common in snow sports; fortunately, most of these do not result in concussion. There is widespread variation in the initial effects of concussion. Recovery is spontaneous, often with rapid resolution of signs, symptoms and changes in cognition (minutes to days). This could increase the potential for athletes to ignore concussion symptoms at the time of injury or return to play prior to full recovery from a diagnosed concussion. This may result in a more serious brain injury or a prolonged recovery period. The potential for serious and prolonged injury emphasises the need for comprehensive medical assessment and follow-up until the concussion has fully resolved. Returning to play before complete resolution of the concussion exposes the athlete to an increased risk of recurrent concussions. Repeat concussion may shorten an athlete s career and has some potential to result in permanent neurological impairment. Rarely, repeat concussion may have devastating and even life-threatening consequences. Athletes must be honest with themselves and medical staff for their own protection. We emphasise that concussion is a variable and fluctuating injury, and is often characterised by evolving and delayed signs and symptoms. Athletes suspected of having a concussion injury must be monitored for 48 hours. Onset of symptoms after 48 hours is uncommon What are the signs of Concussion? The common signs and symptoms indicating that an athlete may have concussion are listed in Table 1 below. If an athlete shows any of the symptoms or signs described in the Table (as a result of a direct blow to the head, face, neck or elsewhere on the body with a force being transmitted to the head) they have suspected concussion.
5 Table 1: Common early signs and symptoms of concussion Indicator Symptoms Physical signs Behavioural changes Cognitive impairment Sleep disturbance Evidence Headache Dizziness Feeling in a fog Disorientation Double vision Vomiting Loss of consciousness (suspected or confirmed) Impact seizure; tonic posturing Inappropriate playing behaviour, unsteady on legs, No protective action when falling Blank or vacant look Slow to get up Clutching head Balance or coordination difficulties Tinnitus; light/sound sensitivity Inappropriate emotions, irritability, feeling nervous or anxious Slowed reaction times Confusion/disorientation Poor attention and concentration, Loss of memory for events up to and/or after the concussion Drowsiness
6 11.5 Stage 1: Diagnosis and Management of Concussion What happens if an athlete is injured and has suspected concussion? Remember the basic rules of First Aid: Immediate general assessment for injuries i. GCS ii. iii. Cervical spine examination Maddocks Questions (adapted for the sport, see below) If the athlete s condition gives significant cause for concern, urgent transport to the nearest hospital must be arranged Recognise and Remove If an athlete is suspected of having concussion, that athlete must be removed from the field of play and must not resume participation If in Doubt, sit it out Continue to Monitor For signs of deterioration, because concussion is often an evolving injury; the onset of signs and symptoms may be DELAYED (typically within 48 hours of the injury) Medical Practitioner and/or Healthcare Professional present Where an injury event with the potential to cause a head injury or concussion occurs and there is a Medical Practitioner or Healthcare Professional present the athlete will be examined and if any of the signs or symptoms in Table 1 are identified and/or the athlete fails to answer correctly the memory questions in the Pocket Concussion Recognition Tool (PCRT), the athlete MUST be removed from the field of play for a comprehensive medical evaluation. An assessment of the athlete s balance should form part of this off-field evaluation. The athlete MUST NOT resume participation once removed from the field of play for suspected concussion. It is preferable to remove the athlete from the field of play, or sideline, to a quiet place (e.g. Medical Room) for full assessment, including the SCAT5 assessment (medical personnel only). The athlete should be allowed a period of rest (10 minutes) prior to taking the tests. NB The SCAT5 should not, by itself, be used to make or exclude a diagnosis of concussion. An athlete may have a concussion even if his/her SCAT5 is normal Examples of Memory questions (adapted from the Maddocks questions that were written originally for team field sports): At what venue are we today? Is this the first or second run? Where were you placed after the first run? Where were you competing last week? Where were you placed in your last competition?
7 The athlete must be removed in a safe manner in accordance with general emergency management procedures. If a cervical spine injury is suspected the athlete should only be removed by emergency Healthcare Professionals with appropriate spinal care training. If a Medical Practitioner is present they can use the Sports Concussion Assessment Tool SCAT5 or other diagnostic tools to assist in the comprehensive medical evaluation of athletes with concussion or suspected concussion. Note that SCAT5 must only be used for athletes aged from 13 years and older. An athlete suspected of having concussion shall move to Stage 2, the GRTP protocol, irrespective of the subsequent diagnosis. M For the use of Medical Practitioners only, the SCAT5 concussion assessment protocol can be downloaded on 11.8 Medical Practitioner and/or Healthcare Professional not present If there is no Medical Practitioner or Healthcare Professional present, the athlete who is injured may be disorientated and must not be allowed to make a judgement about their own condition. Fellow athletes, coaches, Race Officials, team managers, administrators or parents who observe an injured athlete displaying any of the signs in Table 1 after an injury event with the potential to cause a head injury or concussion should ensure that the athlete is removed from the field of play in a safe manner. The athlete must not be left on his or her own and must not be allowed to drive a vehicle. If a medical practitioner is not available on-site the athlete must be referred to a medical practitioner for diagnosis and comprehensive assessment as soon as possible. The Pocket Concussion Recognition Tool (linked under References) can be used to assist in the identification of suspected concussion where a medical practitioner is not present at the time of the incident. Most importantly, if an athlete suffers any of the following: a. Shows any of the listed symptoms in Table 1; b. Fails to answer any of the memory questions correctly in the Pocket CRT; c. Shows a lack of balance, or any of the red flag symptoms listed in the Pocket CRT d. There are any concerns that the athlete may have been concussed If any of these are noted, these concussion management guidelines must be followed. The athlete must be removed from play and referred to a Medical Practitioner or Emergency Department for diagnosis and comprehensive assessment as soon as possible. An athlete suspected of having concussion shall move to the GRTP protocol, irrespective of the diagnosis.
8 The Pocket CRT is available on Onset of Symptoms may be DELAYED It should be noted that the symptoms of concussion may present immediately, but may also be delayed (typically in the first hours) after the incident which caused the suspected concussion. A monitoring mechanism must be set up to ensure that these delayed symptoms are not missed. All those who have suffered from a confirmed or suspected concussive injury must be repeatedly checked for development of new symptoms, or for signs of progression of symptoms Stage 2 - Return to Play FIS recommends that there should a minimum delay of return to play of 7-10 days, and that return to training should only be allowed following clearance by an appropriately experienced medical practitioner. There is insufficient evidence that rest on its own achieves recovery; after a brief period of rest (24-48 hours) it is reasonable to commence a graduated return to play (GRTP) plan. Persistent symptoms merit specialist referral: >10-14 days adult >4 weeks child (U13) In the case of delayed or abnormal recovery, the athlete must undergo formal neuropsychological testing by a concussion expert. Generally, the more severe the early symptoms, the slower the recovery. The times outlines in Table 2 below may exceptionally be expedited, but only if there is access to daily multimodal expert testing. NB There is evidence that: i. children take longer than adults to recover after concussive injuries ii. female athletes are more susceptible than males, and may also take longer to recover Graduated Return to Play Protocol The table below (Table 2) shows a suggested outline for return to play; it must be flexible; it must not be started if symptoms persist, and if symptoms recur, the injured athlete must rest for 24 hours before returning to the previous step on the pathway. It is a collaborative process between athlete and medical/coaching staff. The protocol should commence once symptom-free.the full GRTP process normally takes a minimum of one week, but often requires additional time. Science is currently incomplete, and it is recognised that clinical judgement on an individual basis is the key to management of concussion and the GRTP protocol.
9 Table 2: Graduated Return to Play Protocol Rehabilitation stage 1. No activity, minimum 24 hours following the injury where managed by a medical practitioner (otherwise minimum 14 days post-injury) 2. Light aerobic exercise during 24-hour period 3. Sport-specific exercise during 24- hour period 4. Non-contact training drills during 24- hour period Functional exercise at each stage of rehabilitation Complete physical and cognitive rest without symptoms Walking, swimming or stationary cycling keeping intensity, <70% maximum predicted heart rate. No resistance training. Symptom free during full 24-hour period. Running drills. No head impact activities. Symptom free during full 24-hour period. Progression to more complex training drills, e.g. passing drills. May start progressive resistance training. Symptom free during full 24-hour period. 5. Full Contact Practice Following medical clearance participate in normal training activities 6. After 24 hours return to Player rehabilitated play Objective of each stage Recovery Increase heart rate Add movement Exercise, coordination, and cognitive load Restore confidence and assess functional skills by coaching staff Recovered There may be extreme situations where an athlete does not have access to a Medical Practitioner to diagnose concussion or to manage the GRTP. In these situations, if an athlete has shown any signs of concussion, that athlete must be treated as having suspected concussion and must not play until at least the 21st day after the incident. An attenuated GRTP schedule should be followed. Other athletes, coaches and administrators associated with the athlete should ensure that this process is followed. Final written clearance to return to play by a Medical Practitioner should always be sought, as directed by local laws and regulations Children & Adolescents Whilst the guidelines apply to all age groups, particular care needs to be taken with
10 children and adolescents due to the potential dangers associated with concussion in the developing brain. An initial period of a few days of both physical and cognitive rest is recommended before starting the return to studies / return to play protocols. Children under 13 years of age may display unusual concussion symptoms and should be assessed by a Medical Practitioner using appropriate diagnostic tools. Children (5-12 years) and adolescents (13 18 years) with suspected concussion MUST be referred to a Medical Practitioner immediately. Additionally, they are likely to need specialist medical assessment. The Medical Practitioner responsible for the child s or adolescent s treatment will advise on the return to play process, however, a more conservative Graduated Return to Play approach is recommended this must be preceded by a graduated return to studies/school (see SCAT5 CHILD, and Table 3 below). They should complete the Return to School protocol before progressing to Stage 4 or 5 of the GRTP protocol. It is appropriate to extend the amount of time of asymptomatic rest and /or the length of the graded exertion in children and adolescents. Children and adolescents must not return to play without clearance from a Medical Practitioner. For the use of Medical Practitioners only, the SCAT5-CHILD concussion assessment protocol can be downloaded from:
11 Table 3: Return to School Strategy Stage Aim Activity Goal of each step 1 Daily activities at home that do not give the student\athlete symptoms Typical activities during the day as long as they do not increase symptoms (i.e. reading, texting, screen time). Start at 5\15 minutes at a time and gradually build up. 2 School activities Homework, reading or other cognitive activities outside of the classroom 3 Return to school part-time Gradual introduction of schoolwork. May need to start with a partial school day or with increased breaks during the day. Gradual return to typical activities Increase tolerance to cognitive work Increase academic activities 4 Return to school full-time Gradually progress Return to full academic activities and catch up on missed school work Recurrence of symptoms during GRTP process - 24 hours rest before restarting protocol at the previous step It is recognised that athletes will want to return to play as soon as possible following a concussion. Athletes, coaches, management, parents and teachers must exercise caution to: i. Ensure that all symptoms have subsided ii. iii. Ensure that the GRTP protocol is followed Ensure that the advice of Medical Practitioners is strictly adhered to In doing so, all concerned can reduce the risks to an athlete s career longevity and long term health Return of Symptoms All involved in the process of concussion management must be vigilant for the return of symptoms (including depression and other mental health issues) after a concussive incident, even if the GRTP has been successfully completed. If symptoms recur, the athlete must consult a Medical Practitioner and those involved in the process of concussion management and/or aware of the return of symptoms must do all they can to ensure that the athlete consults a Medical Practitioner as soon as possible.
12 11.15 Residual Effects & Sequelae The many and various post-concussion symptoms that are recognised include (but are not limited to) the following: i. Depression ii. Cognitive impairment iii. Anxiety iv. Headache v. Sleep dysfunction vi. Post-traumatic stress disorder (PTSD) vii. Chronic Traumatic encephalopathy (CTE) Ensuring complete recovery after any incident of concussion is the best way to lessen the risk of long-term sequelae. 12. Useful Links 1. Berlin Consensus Statement SCAT (Physicians only) 3. SCAT5 CHILD 2017 (Physicians only) 4. PCRT SCAT (Physicians only) 3. SCAT5 CHILD 2017 (Physicians only) 4. PCRT Please note that these tools are designed to be used in English speaking nations; the process of transposing them into the other major language groups is under way, and appropriate versions should be used Many sports have developed on-line resources for professional development and education in concussion, for athletes, coaches, parents and spectators, as well as for medical personnel. One of the best is: FIS Concussion Guidelines July 2013
Concussion guidance. Introduction CONCUSSION FACTS
 Introduction This World Rugby Concussion Guidance document has been developed to provide guidance and information to persons involved in the non-elite level of the game of Rugby regarding concussion and
Introduction This World Rugby Concussion Guidance document has been developed to provide guidance and information to persons involved in the non-elite level of the game of Rugby regarding concussion and
INTERNATIONAL RUGBY BOARD Putting players first
 CONCUSSION FACTS A concussion is a brain injury. All concussions are serious. Concussions can occur without loss of consciousness. All athletes with any symptoms following a head injury must be removed
CONCUSSION FACTS A concussion is a brain injury. All concussions are serious. Concussions can occur without loss of consciousness. All athletes with any symptoms following a head injury must be removed
ETA STAFF - concussion
 These guidelines are designed to be used by Referees, Coaching staff and Managers This guideline has been adapted from the Rugby Football Union (RFU) guidance, World rugby guidance and the Zurich Consensus
These guidelines are designed to be used by Referees, Coaching staff and Managers This guideline has been adapted from the Rugby Football Union (RFU) guidance, World rugby guidance and the Zurich Consensus
Concussion Policy. Guideline summary
 Guideline summary RECOGNISE AND REMOVE - learn to recognise the signs and symptoms of concussion and remove a player from the field if ANY doubt. PROTECT OUR YOUNG ATHLETES England & GB Hockey recommends
Guideline summary RECOGNISE AND REMOVE - learn to recognise the signs and symptoms of concussion and remove a player from the field if ANY doubt. PROTECT OUR YOUNG ATHLETES England & GB Hockey recommends
CONCUSSION RECOGNISING THE SIGNS STARTS WITH YOU. co.nz
 CONCUSSION RECOGNISING THE SIGNS STARTS Malcolm.Francis@acc. co.nz WITH YOU. A step-by-step guide to concussion and your role in recognising the signs, removing players from play and referring them to
CONCUSSION RECOGNISING THE SIGNS STARTS Malcolm.Francis@acc. co.nz WITH YOU. A step-by-step guide to concussion and your role in recognising the signs, removing players from play and referring them to
and present Date: Amended January 2015
 and present Concussionn Guidelines in the GAA 2013 2016 Adopted by LGFA Date: Amended January 2015 Table of Contents Summary Principles... 2 What is Concussion?... 3 Signs and Symptoms... 3 Pitch Assessment
and present Concussionn Guidelines in the GAA 2013 2016 Adopted by LGFA Date: Amended January 2015 Table of Contents Summary Principles... 2 What is Concussion?... 3 Signs and Symptoms... 3 Pitch Assessment
Concussion Guidelines in the GAA
 And present Concussion Guidelines in the GAA 2013 2016 Page 1 of 13 Position Statement Concussion Guidelines 2013 2016 Summary Principles... 3 What is Concussion?... 3 Signs and Symptoms... 3 Pitch Assessment
And present Concussion Guidelines in the GAA 2013 2016 Page 1 of 13 Position Statement Concussion Guidelines 2013 2016 Summary Principles... 3 What is Concussion?... 3 Signs and Symptoms... 3 Pitch Assessment
CONCUSSION AWARENESS, MANAGEMENT, AND ASSESSMENT FROM AN ATHLETIC TRAINER
 CONCUSSION AWARENESS, MANAGEMENT, AND ASSESSMENT FROM AN ATHLETIC TRAINER Dr. Ryan Krzyzanowicz, DAT, ATC Clinical Associate Professor Program Director - Athletic Training Education University at Buffalo
CONCUSSION AWARENESS, MANAGEMENT, AND ASSESSMENT FROM AN ATHLETIC TRAINER Dr. Ryan Krzyzanowicz, DAT, ATC Clinical Associate Professor Program Director - Athletic Training Education University at Buffalo
IF IN DOUBT, SIT THEM OUT.
 IF IN DOUBT, SIT THEM OUT. Scottish Sports Concussion Guidance: grassroots sport and general public 2018 version. Adapted from the Berlin 5th International concussion consensus statement 2016. Contents
IF IN DOUBT, SIT THEM OUT. Scottish Sports Concussion Guidance: grassroots sport and general public 2018 version. Adapted from the Berlin 5th International concussion consensus statement 2016. Contents
Australian Canoeing Limited Concussion Guidelines
 Australian Canoeing Limited Concussion Guidelines Date 5 th January 2016 Australian Canoeing PO Box 6805 Silverwater, NSW 2128 T: (02) 9763 0670 W: canoe.org.au CONTENTS 1. Overview... 1 2. Introduction...
Australian Canoeing Limited Concussion Guidelines Date 5 th January 2016 Australian Canoeing PO Box 6805 Silverwater, NSW 2128 T: (02) 9763 0670 W: canoe.org.au CONTENTS 1. Overview... 1 2. Introduction...
MANITOBA SOCCER ASSOCIATION YOUTH CONCUSSION PROTOCOL SUMMARY
 MANITOBA SOCCER ASSOCIATION YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the MANITOBA SOCCER ASSOCIATION (MSA) YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
MANITOBA SOCCER ASSOCIATION YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the MANITOBA SOCCER ASSOCIATION (MSA) YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
Director of Athletics
 3341-8-1 Concussion Management Policy. Applicability Intercollegiate Athletics Responsible Unit Policy Administrator Intercollegiate Athletics/Director of Athletics Director of Athletics (A) Policy Purpose
3341-8-1 Concussion Management Policy. Applicability Intercollegiate Athletics Responsible Unit Policy Administrator Intercollegiate Athletics/Director of Athletics Director of Athletics (A) Policy Purpose
LACROSSE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY
 LACROSSE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the Manitoba Lacrosse Association s Youth Concussion Protocol 1. All youth athletes (
LACROSSE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the Manitoba Lacrosse Association s Youth Concussion Protocol 1. All youth athletes (
May 2016 accsportsmart.co.nz
 SPORT CONCUSSION IN NEW ZEALAND: ACC NATIONAL GUIDELINES May 2016 accsportsmart.co.nz This guideline document has been produced to inform National Sports Organisations (NSOs), and recreation, education
SPORT CONCUSSION IN NEW ZEALAND: ACC NATIONAL GUIDELINES May 2016 accsportsmart.co.nz This guideline document has been produced to inform National Sports Organisations (NSOs), and recreation, education
Concussion Management Guidelines for Gaelic Games
 Concussion Management Guidelines for Gaelic Games Updated January 2018 Introduction 3 What is Concussion? 3 Summary Principles 4 Signs and Symptoms 5 Pitch Assessment / Initial Management of a Concussion
Concussion Management Guidelines for Gaelic Games Updated January 2018 Introduction 3 What is Concussion? 3 Summary Principles 4 Signs and Symptoms 5 Pitch Assessment / Initial Management of a Concussion
HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL SUMMARY
 2018-2019 HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
2018-2019 HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the HOCKEY WINNIPEG YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY
 BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the BASEBALL MANITOBA YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY
 RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL SUMMARY The following is a summary of the RINGETTE MANITOBA YOUTH CONCUSSION PROTOCOL. 1.) All youth athletes (
2017 Concussion Management Program
 2017 Concussion Management Program Michael Stuart MD Alan Ashare MD Kevin Margarucci ATC The standard of care for current medical practice and the law in most states requires that any athlete with a suspected
2017 Concussion Management Program Michael Stuart MD Alan Ashare MD Kevin Margarucci ATC The standard of care for current medical practice and the law in most states requires that any athlete with a suspected
Wisconsin Lacrosse Federation
 The purpose of this policy is to insure the safety of the players and to limit the liability of those protecting the safety of the players. The responsibility of player safety falls on everyone involved
The purpose of this policy is to insure the safety of the players and to limit the liability of those protecting the safety of the players. The responsibility of player safety falls on everyone involved
SAIL CANADA CONCUSSION PROTOCOL
 SAIL CANADA CONCUSSION PROTOCOL Sail Canada has developed the Sail Canada Concussion Protocol to help guide the management of Sailing Sport Participants (athletes, coaches, instructors, officials & volunteers)
SAIL CANADA CONCUSSION PROTOCOL Sail Canada has developed the Sail Canada Concussion Protocol to help guide the management of Sailing Sport Participants (athletes, coaches, instructors, officials & volunteers)
Sports Related Concussion. Joshua T. Williams, PT, DPT, OCS, SCS, CSCS
 Sports Related Concussion Joshua T. Williams, PT, DPT, OCS, SCS, CSCS Concussion & Traumatic Brain Injury Glasgow Coma Scale Minimal Mild Mod Severe? Sports concussion Severe GCS 8 Moderate GCS 9-12 Mild
Sports Related Concussion Joshua T. Williams, PT, DPT, OCS, SCS, CSCS Concussion & Traumatic Brain Injury Glasgow Coma Scale Minimal Mild Mod Severe? Sports concussion Severe GCS 8 Moderate GCS 9-12 Mild
Carleton College Concussion Safety Protocol
 Carleton College Introduction Carleton College is committed to ensuring the health and safety of its student-athletes. To this end, and in accordance with NCAA legislation [Division III Constitution 3.2.4.16],
Carleton College Introduction Carleton College is committed to ensuring the health and safety of its student-athletes. To this end, and in accordance with NCAA legislation [Division III Constitution 3.2.4.16],
INTERCOLLEGIATE ATHLETICS CONCUSSION MANAGEMENT PLAN
 INTERCOLLEGIATE ATHLETICS CONCUSSION MANAGEMENT PLAN I. PURPOSE In an effort to better serve the healthcare needs of its student athletes, as well as to adhere to best practices recommended by the National
INTERCOLLEGIATE ATHLETICS CONCUSSION MANAGEMENT PLAN I. PURPOSE In an effort to better serve the healthcare needs of its student athletes, as well as to adhere to best practices recommended by the National
IT S ALL IN YOUR HEAD!
 IT S ALL IN YOUR HEAD! CARING FOR CONCUSSIONS IN YOUR COMMUNITY Stephen K Stacey, DO CPT, MC, USA OUTLINE Definition Epidemiology Diagnosis Evaluation Recovery Sequelae Prevention Resources for providers
IT S ALL IN YOUR HEAD! CARING FOR CONCUSSIONS IN YOUR COMMUNITY Stephen K Stacey, DO CPT, MC, USA OUTLINE Definition Epidemiology Diagnosis Evaluation Recovery Sequelae Prevention Resources for providers
Eagle High School Lacrosse Concussion Management Plan
 ! Eagle High School Lacrosse Concussion Management Plan August 2018 Contents (1) Mandatory Parent/Athlete Meeting 1 (2) Recommended Baseline Testing 2 (3) Concussion Training for Athletic Trainers and
! Eagle High School Lacrosse Concussion Management Plan August 2018 Contents (1) Mandatory Parent/Athlete Meeting 1 (2) Recommended Baseline Testing 2 (3) Concussion Training for Athletic Trainers and
Concussion Management Protocol
 Concussion Management Protocol We at Total Sports Experience desire a safe return to play for all sick or injured athletes. Research has shown that an athlete's coordination, balance and/or cognitive functioning
Concussion Management Protocol We at Total Sports Experience desire a safe return to play for all sick or injured athletes. Research has shown that an athlete's coordination, balance and/or cognitive functioning
CONCUSSION MANAGEMENT PROTOCOL 2015
 301-333 Terminal Avenue, Vancouver, BC Canada V6A 4C1 t: 604.568.1135 f: 604.568.1639 e: info@canadasnowboard.ca www.canadasnowboard.ca CONCUSSION MANAGEMENT PROTOCOL 2015 A CONCUSSION is a disturbance
301-333 Terminal Avenue, Vancouver, BC Canada V6A 4C1 t: 604.568.1135 f: 604.568.1639 e: info@canadasnowboard.ca www.canadasnowboard.ca CONCUSSION MANAGEMENT PROTOCOL 2015 A CONCUSSION is a disturbance
1. Begin light aerobic exercise such as walking, stationary bike, etc. No resistance training.
 POLICY: Any athlete displaying signs or symptoms of a concussion, or if there is a high suspicion for concussion, an athlete will not be returned to competition or practice until they have written clearance
POLICY: Any athlete displaying signs or symptoms of a concussion, or if there is a high suspicion for concussion, an athlete will not be returned to competition or practice until they have written clearance
Page
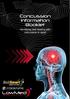 Page 2 Concussion step by step guide Name: Date 1.Education 2.Baseline testing 3.Immediate medical evaluation Post-concussion by a medical doctor 4.Follow up Computer testing 5. Return-to-play protocol
Page 2 Concussion step by step guide Name: Date 1.Education 2.Baseline testing 3.Immediate medical evaluation Post-concussion by a medical doctor 4.Follow up Computer testing 5. Return-to-play protocol
PRE-SEASON INFORMATION SHEET CONCUSSIONS
 PRE-SEASON INFORMATION SHEET CONCUSSIONS HOW TO USE THIS EDUCATION SHEET: Distribute this pre-season concussion education sheet to your athletes and their parents or legal guardians during a pre-season
PRE-SEASON INFORMATION SHEET CONCUSSIONS HOW TO USE THIS EDUCATION SHEET: Distribute this pre-season concussion education sheet to your athletes and their parents or legal guardians during a pre-season
UNIVERSITY OF MASSACHUSETTS SPORTS MEDICINE PROGRAM Concussion Management Plan
 UNIVERSITY OF MASSACHUSETTS SPORTS MEDICINE PROGRAM Concussion Management Plan University of Massachusetts Sports Medicine personnel will evaluate student-athletes with a suspected concussion as follows:
UNIVERSITY OF MASSACHUSETTS SPORTS MEDICINE PROGRAM Concussion Management Plan University of Massachusetts Sports Medicine personnel will evaluate student-athletes with a suspected concussion as follows:
Loss of consciousness (LOC) Poor recall for events prior to injury or after injury
 NAIA Championship Concussion Policy Concussions can be serious and potentially life threatening injuries in sports. Research indicates that if concussion symptoms are appropriately managed, an individual
NAIA Championship Concussion Policy Concussions can be serious and potentially life threatening injuries in sports. Research indicates that if concussion symptoms are appropriately managed, an individual
Concussion Identification, Management and Return to Play at North Hunterdon-Voorhees Regional HS District
 Concussion Identification, Management and Return to Play at North Hunterdon-Voorhees Regional HS District In tandem with the New Jersey Interscholastic Athletic Association and the National Athletic Trainers
Concussion Identification, Management and Return to Play at North Hunterdon-Voorhees Regional HS District In tandem with the New Jersey Interscholastic Athletic Association and the National Athletic Trainers
When a concussion occurs:
 When a concussion occurs: Once an athlete has experienced any type of potential head injury initiate the following checklist: 1. n Remove athlete from all activity and use the Concussion Recognition Tool
When a concussion occurs: Once an athlete has experienced any type of potential head injury initiate the following checklist: 1. n Remove athlete from all activity and use the Concussion Recognition Tool
Dhiren J. Naidu MD FRCPC Dip. Sport Med.
 Dhiren J. Naidu MD FRCPC Dip. Sport Med. Associate Professor, Division of Physical Medicine & Rehabilitation Faculty of Medicine & Dentistry Varsity Health, University of Alberta Team Physician - Oilers,
Dhiren J. Naidu MD FRCPC Dip. Sport Med. Associate Professor, Division of Physical Medicine & Rehabilitation Faculty of Medicine & Dentistry Varsity Health, University of Alberta Team Physician - Oilers,
Page I
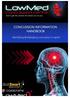 Page 2 How to manage concussion? World Rugby standard: Recognize and Remove Protocol (6Rs). RECOGNIZE - Learn the signs and symptoms of concussion so you understand when an athlete might have a concussion.
Page 2 How to manage concussion? World Rugby standard: Recognize and Remove Protocol (6Rs). RECOGNIZE - Learn the signs and symptoms of concussion so you understand when an athlete might have a concussion.
RECOVERY AND RETURN TO PLAY
 O I S S U C O C T L ADU ) E I T U O R ( S E I L E D I U G T E MAAGEM RECOVERY AD RETUR TO PLAY Concussion must be taken extremely seriously to safeguard the short and long term health and welfare of players.
O I S S U C O C T L ADU ) E I T U O R ( S E I L E D I U G T E MAAGEM RECOVERY AD RETUR TO PLAY Concussion must be taken extremely seriously to safeguard the short and long term health and welfare of players.
Concussion Assessment, Management, and Return to Play Guidelines
 Concussion Assessment, Management, and Return to Play Guidelines The following policy and procedures on neurocognitive baseline testing and subsequent assessment and management of concussions as well as
Concussion Assessment, Management, and Return to Play Guidelines The following policy and procedures on neurocognitive baseline testing and subsequent assessment and management of concussions as well as
Alberta Deaf Sports Association Concussion Protocol and Policy **BOARD APPROVED: August 27 th, 2016** 1.1 Introduction
 1.1 Introduction Alberta Deaf Sports Association Concussion Protocol and Policy **BOARD APPROVED: August 27 th, 2016** The Canadian Concussion Collaborative recommends that all recreation providers, sports
1.1 Introduction Alberta Deaf Sports Association Concussion Protocol and Policy **BOARD APPROVED: August 27 th, 2016** The Canadian Concussion Collaborative recommends that all recreation providers, sports
Concussion Information
 What is a Concussion? Concussion Information Information taken from the Sports Concussion Institute http://www.concussiontreatment.com A concussion is defined as a complex pathophysiological process that
What is a Concussion? Concussion Information Information taken from the Sports Concussion Institute http://www.concussiontreatment.com A concussion is defined as a complex pathophysiological process that
Mount Michael Benedictine Concussion Management Policy & Protocol
 Mount Michael Benedictine Concussion Management Policy & Protocol I. Definition of Concussion a. A concussion is a type of traumatic brain injury caused by a bump, blow, or jolt to the head. A concussion
Mount Michael Benedictine Concussion Management Policy & Protocol I. Definition of Concussion a. A concussion is a type of traumatic brain injury caused by a bump, blow, or jolt to the head. A concussion
Paramus Athletics. Paramus High School Athletic Department Protocol and Procedures for Management of Sports - Related Concussion
 Paramus Athletics Paramus High School Athletic Department Protocol and Procedures for Management Medical management of sports-related concussions is evolving. In recent years, there has been significant
Paramus Athletics Paramus High School Athletic Department Protocol and Procedures for Management Medical management of sports-related concussions is evolving. In recent years, there has been significant
RIDGEWOOD BOARD OF EDUCATION PROGRAM /page 1 of 8 Management of Sports-Related Concussion M Management of Sports-Related Concussion
 2431.4/page 1 of 8 M 2431.4 Medical management of sports-related concussions is evolving. In recent years, there has been significant research into sports-related concussions in high school athletes. As
2431.4/page 1 of 8 M 2431.4 Medical management of sports-related concussions is evolving. In recent years, there has been significant research into sports-related concussions in high school athletes. As
YAKIMA SCHOOL DISTRICT CONCUSSION MANAGEMENT POLICY
 YAKIMA SCHOOL DISTRICT CONCUSSION MANAGEMENT POLICY A student athlete that has sustained a concussion will be managed by the following policy described below: 1. Concussion management policy shall be in
YAKIMA SCHOOL DISTRICT CONCUSSION MANAGEMENT POLICY A student athlete that has sustained a concussion will be managed by the following policy described below: 1. Concussion management policy shall be in
Departmental Concussion Guidelines
 Concussion Plan Departmental Concussion Guidelines The following guidelines have been developed in accordance with Alabama A&M s Mission Statement and service goal of providing quality healthcare services
Concussion Plan Departmental Concussion Guidelines The following guidelines have been developed in accordance with Alabama A&M s Mission Statement and service goal of providing quality healthcare services
RECOGNISE AND REMOVE
 RECOGNISE AND REMOVE Remember the 4 R s of concussion management: RECOGNISE REMOVE RECOVER RETURN Identifying concussion is not always easy, and players may not exhibit the signs or symptoms immediately
RECOGNISE AND REMOVE Remember the 4 R s of concussion management: RECOGNISE REMOVE RECOVER RETURN Identifying concussion is not always easy, and players may not exhibit the signs or symptoms immediately
INTERCOLLEGIATE ATHLETICS CONCUSSION ACKNOWLEDGEMENT AND STATEMENT
 ACKNOWLEDGEMENT AND STATEMENT A FACT SHEET FOR STUDENT-ATHLETES WHAT IS A? A concussion is a brain injury that: Is caused by a blow to the head or body -From contact with another player, hitting a hard
ACKNOWLEDGEMENT AND STATEMENT A FACT SHEET FOR STUDENT-ATHLETES WHAT IS A? A concussion is a brain injury that: Is caused by a blow to the head or body -From contact with another player, hitting a hard
Purpose: The purpose of this policy is to establish a protocol for defining concussions, recognizing symptoms of concussions, and determining the
 Purpose: The purpose of this policy is to establish a protocol for defining concussions, recognizing symptoms of concussions, and determining the return to play of an athlete following a concussion at
Purpose: The purpose of this policy is to establish a protocol for defining concussions, recognizing symptoms of concussions, and determining the return to play of an athlete following a concussion at
Bishop Kelly High School s Concussion Management Plan
 Bishop Kelly High School s Concussion Management Plan September 2016 Contents (1) Mandatory Parent/Athlete Meeting, Parent/Athlete Consent Form... 1 (2) Baseline Testing... 2 (3) Concussion Training for
Bishop Kelly High School s Concussion Management Plan September 2016 Contents (1) Mandatory Parent/Athlete Meeting, Parent/Athlete Consent Form... 1 (2) Baseline Testing... 2 (3) Concussion Training for
SPRINGFIELD CLINIC S
 SPRINGFIELD CLINIC S HEAD INJURY MANAGEMENT GUIDE FOR PARENTS Given the complexities of concussion management, Springfield Clinic recognizes the importance of managing concussions on an individualized
SPRINGFIELD CLINIC S HEAD INJURY MANAGEMENT GUIDE FOR PARENTS Given the complexities of concussion management, Springfield Clinic recognizes the importance of managing concussions on an individualized
Concussions in Sport Definitions, Mechanisms, and Current Issues
 Concussions in Sport Definitions, Mechanisms, and Current Issues Concussions are Everyone s Responsibility! If you do not LOOK FOR IT you will not FIND IT! Paul Echlin MD CCFP, Dip. ABFM, Dip. SM, CAQSM
Concussions in Sport Definitions, Mechanisms, and Current Issues Concussions are Everyone s Responsibility! If you do not LOOK FOR IT you will not FIND IT! Paul Echlin MD CCFP, Dip. ABFM, Dip. SM, CAQSM
PEDIATRIC SPORTS RELATED CONCUSSIONS
 Anna Mazur, PhD PEDIATRIC SPORTS RELATED CONCUSSIONS Disclosure No financial interests or funding 1 Presentation Outline Prevalence Predicting recovery: Post Traumatic Amnesia and Loss of Consciousness
Anna Mazur, PhD PEDIATRIC SPORTS RELATED CONCUSSIONS Disclosure No financial interests or funding 1 Presentation Outline Prevalence Predicting recovery: Post Traumatic Amnesia and Loss of Consciousness
UPPER PERKIOMEN HIGH SCHOOL
 UPPER PERKIOMEN HIGH SCHOOL Concussion Management and Return to Play Protocol Recognizing that sport related concussions pose a significant health risk for studentathletes, the Upper Perkiomen School District
UPPER PERKIOMEN HIGH SCHOOL Concussion Management and Return to Play Protocol Recognizing that sport related concussions pose a significant health risk for studentathletes, the Upper Perkiomen School District
Lower Moreland School District: Athletic Department Protocol and Procedures for Management of Sports-Related Concussion
 Lower Moreland School District: Athletic Department Protocol and Procedures for Management of Sports-Related Concussion Preamble: Medical management of sports-related concussion is evolving. In recent
Lower Moreland School District: Athletic Department Protocol and Procedures for Management of Sports-Related Concussion Preamble: Medical management of sports-related concussion is evolving. In recent
Post Concussion Instructions and Return to Play Clearance Form. To: Parent/Guardian: Page 1. From:, at School
 Post Concussion Instructions and Return to Play Clearance Form To: Parent/Guardian: From:, at School Name of School Representative* Name of School, Position of School Representative* Phone Number of School
Post Concussion Instructions and Return to Play Clearance Form To: Parent/Guardian: From:, at School Name of School Representative* Name of School, Position of School Representative* Phone Number of School
Concussion Management Policy Overview. City School District of Albany Department of Health, Physical Education & Athletics
 Concussion Management Policy Overview City School District of Albany Department of Health, Physical Education & Athletics CSDA Concussion Management Policy After 6 months of research and development, the
Concussion Management Policy Overview City School District of Albany Department of Health, Physical Education & Athletics CSDA Concussion Management Policy After 6 months of research and development, the
University of Notre Dame Sports Medicine Department Intercollegiate Athletics Concussion Management Plan
 ! Purpose: University of Notre Dame Sports Medicine Department Intercollegiate Athletics Concussion Management Plan Head injuries can pose a significant health risk for student-athletes competing in intercollegiate
! Purpose: University of Notre Dame Sports Medicine Department Intercollegiate Athletics Concussion Management Plan Head injuries can pose a significant health risk for student-athletes competing in intercollegiate
TMPW Xplorers Basketball Concussion Management Plan
 TMPW Xplorers Basketball Concussion Management Plan November 2017 Contents (1) Mandatory Parent / Athlete Education 1 & 2 (2) Recommended Baseline Testing 3 (3) Concussion Training for Athletic Trainers
TMPW Xplorers Basketball Concussion Management Plan November 2017 Contents (1) Mandatory Parent / Athlete Education 1 & 2 (2) Recommended Baseline Testing 3 (3) Concussion Training for Athletic Trainers
Dr. JoAnne Savoie, L.Psyc. Clinical Neuropsychologist Stan Cassidy Center for Rehabilitation Fredericton, NB. October 16, 2012
 Dr. JoAnne Savoie, L.Psyc. Clinical Neuropsychologist Stan Cassidy Center for Rehabilitation Fredericton, NB October 16, 2012 Risk factors for concussion Players at all levels are at risk 5-10% of athletes
Dr. JoAnne Savoie, L.Psyc. Clinical Neuropsychologist Stan Cassidy Center for Rehabilitation Fredericton, NB October 16, 2012 Risk factors for concussion Players at all levels are at risk 5-10% of athletes
Concussions UCLA Steve Tisch BrainSPORT Clinic
 Concussions UCLA Steve Tisch BrainSPORT Clinic Concussion facts What is a concussion? A concussion is a traumatic brain injury (TBI) caused by a bump, blow or jolt to the head or by a hit to the body that
Concussions UCLA Steve Tisch BrainSPORT Clinic Concussion facts What is a concussion? A concussion is a traumatic brain injury (TBI) caused by a bump, blow or jolt to the head or by a hit to the body that
CONCUSSION BOARD POLICY 8604
 CONCUSSION BOARD POLICY 8604 Policy Concussion management and policy protocols are a standardized method of assessment to ensure an accurate diagnosis and the appropriate management of student-athlete
CONCUSSION BOARD POLICY 8604 Policy Concussion management and policy protocols are a standardized method of assessment to ensure an accurate diagnosis and the appropriate management of student-athlete
Bump to Head, Head Injury and Concussion Policy
 Bump to Head, Head Injury and Concussion Policy Policy Type Non-regulatory Last Review Summer 2018 Next Review Autumn 2018 Bump to Head, Head Injury & Concussion Policy See Appendix 1 for a flow chart
Bump to Head, Head Injury and Concussion Policy Policy Type Non-regulatory Last Review Summer 2018 Next Review Autumn 2018 Bump to Head, Head Injury & Concussion Policy See Appendix 1 for a flow chart
NEW ZEALAND RUGBY LEAGUE CONCUSSION / HEAD INJURY POLICY
 NEW ZEALAND RUGBY LEAGUE CONCUSSION / HEAD INJURY POLICY February 2015 New Zealand Rugby League Medical panel The aim of the policy is to provide information on concussion to all those involved in rugby
NEW ZEALAND RUGBY LEAGUE CONCUSSION / HEAD INJURY POLICY February 2015 New Zealand Rugby League Medical panel The aim of the policy is to provide information on concussion to all those involved in rugby
The University of Nebraska Omaha Concussion Management Plan
 Definition: The University of Nebraska Omaha Concussion Management Plan A concussion is a complex pathophysiological process affecting the brain, induced by traumatic biomechanical forces secondary to
Definition: The University of Nebraska Omaha Concussion Management Plan A concussion is a complex pathophysiological process affecting the brain, induced by traumatic biomechanical forces secondary to
CONCUSSION PROTOCOL STEPS FOR RETURN TO PLAY
 Winnacunnet High School Concussion Protocol All coaches must take the NFHS Concussion course prior to working with students in their coaching season. Coaches must retake the course on even numbered years.
Winnacunnet High School Concussion Protocol All coaches must take the NFHS Concussion course prior to working with students in their coaching season. Coaches must retake the course on even numbered years.
The Master s Academy Concussion Policy
 The Master s Academy Concussion Policy Ann Williams,M.S.N., R.N. Robert O Quinn, MS, ATC, LAT Updated 2/6/2018 Outline I. Abbreviated policy II. Introduction III. Prevention and Education IV. Recognition
The Master s Academy Concussion Policy Ann Williams,M.S.N., R.N. Robert O Quinn, MS, ATC, LAT Updated 2/6/2018 Outline I. Abbreviated policy II. Introduction III. Prevention and Education IV. Recognition
CONCUSSION INFORMATION When in Doubt, Sit Them Out!
 CONCUSSION INFORMATION When in Doubt, Sit Them Out! A concussion is a type of traumatic brain injury that interferes with normal function of the brain. All concussions are brain injuries. The WIAA recommends
CONCUSSION INFORMATION When in Doubt, Sit Them Out! A concussion is a type of traumatic brain injury that interferes with normal function of the brain. All concussions are brain injuries. The WIAA recommends
The Kansas Legislature has enacted the School Sports Head Injury Prevention Act (hereinafter the Kansas Act ) effective July 1, 2011:
 KANSAS STATE HIGH SCHOOL ACTIVITIES ASSOCIATION RECOMMENDATIONS FOR COMPLIANCE WITH THE KANSAS SCHOOL SPORTS HEAD INJURY PREVENTION ACT AND IMPLEMENTATION OF THE NATIONAL FEDERATION SPORTS PLAYING RULES
KANSAS STATE HIGH SCHOOL ACTIVITIES ASSOCIATION RECOMMENDATIONS FOR COMPLIANCE WITH THE KANSAS SCHOOL SPORTS HEAD INJURY PREVENTION ACT AND IMPLEMENTATION OF THE NATIONAL FEDERATION SPORTS PLAYING RULES
CONCUSSION POLICY AND PROCEDURES
 NORTHEAST METROPOLITAN REGIONAL VOCATIONAL SCHOOL 100 HEMLOCK ROAD WAKEFIELD, MA 01880 CONCUSSION POLICY AND PROCEDURES 1/2016 12/2017 Reviewed by Committee Members: David DiBarri Deputy Director- Principal
NORTHEAST METROPOLITAN REGIONAL VOCATIONAL SCHOOL 100 HEMLOCK ROAD WAKEFIELD, MA 01880 CONCUSSION POLICY AND PROCEDURES 1/2016 12/2017 Reviewed by Committee Members: David DiBarri Deputy Director- Principal
Excerpt from the CONCUSSION. KiT. Understanding and Managing Concussion in Youth
 Excerpt from the KiT CONCUSSION Understanding and Managing Concussion in Youth What Is a Concussion õõ A concussion is a type of brain injury. õõ A concussion is also referred to as a mild traumatic brain
Excerpt from the KiT CONCUSSION Understanding and Managing Concussion in Youth What Is a Concussion õõ A concussion is a type of brain injury. õõ A concussion is also referred to as a mild traumatic brain
CONCUSSION POLICY STATEMENT AND MANAGEMENT GUIDELINES
 INTRODUCTION It is clear that a persuasive argument can be made that a comprehensive and systematic approach to concussion injury utilizing an evidence based method holds potential benefit for both the
INTRODUCTION It is clear that a persuasive argument can be made that a comprehensive and systematic approach to concussion injury utilizing an evidence based method holds potential benefit for both the
Concussion Information any student suspected of having a concussion must be immediately removed from play.
 Concussion Information (BP/AR 6145.22) As medical management of sports-related concussion continues to evolve. Recently, there has been a significant amount of new research regarding sports-related concussions
Concussion Information (BP/AR 6145.22) As medical management of sports-related concussion continues to evolve. Recently, there has been a significant amount of new research regarding sports-related concussions
Lee County School District: Athletic Department Protocol and Procedures for Management of Sports-Related Concussion
 Lee County School District: Athletic Department Protocol and Procedures for Management of Sports-Related Concussion Medical management of sports-related concussions are evolving. In recent years, there
Lee County School District: Athletic Department Protocol and Procedures for Management of Sports-Related Concussion Medical management of sports-related concussions are evolving. In recent years, there
COS SPORTS MEDICINE CONCUSSION ASSESSMENT FORM BASELINE TEST Adapted from SCAT3
 COS SPORTS MEDICINE CONCUSSION ASSESSMENT FORM BASELINE TEST Adapted from SCAT3 Name Sport Examiner Name: Date of BASELINE TEST: Age Gender M / F COGNITIVE ASSESSMENT Orientation (1 pt each) What month
COS SPORTS MEDICINE CONCUSSION ASSESSMENT FORM BASELINE TEST Adapted from SCAT3 Name Sport Examiner Name: Date of BASELINE TEST: Age Gender M / F COGNITIVE ASSESSMENT Orientation (1 pt each) What month
Gilbert Public Schools (High School) Athletic Department Protocol and Procedures for Management of Sports-Related Concussion
 Gilbert Public Schools (High School) Athletic Department Protocol and Procedures for Management of Sports-Related Concussion Medical management of sports-related concussion is evolving. In recent years,
Gilbert Public Schools (High School) Athletic Department Protocol and Procedures for Management of Sports-Related Concussion Medical management of sports-related concussion is evolving. In recent years,
Concussion. Introduction
 Concussion Introduction Concussion is unlike most injuries that athlete s experience. As concussion is an injury to the brain, it cannot be seen and the effects can be either subtle or devastating or cumulatively
Concussion Introduction Concussion is unlike most injuries that athlete s experience. As concussion is an injury to the brain, it cannot be seen and the effects can be either subtle or devastating or cumulatively
CCYFL Concussion Information Sheet
 CCYFL Concussion Information Sheet Why am I getting this information sheet? You are receiving this information sheet about concussions because of California state law AB 2007, (effective January 1, 2017),
CCYFL Concussion Information Sheet Why am I getting this information sheet? You are receiving this information sheet about concussions because of California state law AB 2007, (effective January 1, 2017),
Idaho Amateur Hockey Association Concussion Management Plan
 Idaho Amateur Hockey Association Concussion Management Plan 1 September 2017 Contents (1) Mandatory Parent/Athlete Meeting 1 (2) Recommended Baseline Testing 2 (3) Concussion Training for Athletic Trainers
Idaho Amateur Hockey Association Concussion Management Plan 1 September 2017 Contents (1) Mandatory Parent/Athlete Meeting 1 (2) Recommended Baseline Testing 2 (3) Concussion Training for Athletic Trainers
Forney ISD Protocol and Procedures for the Management of the Sports-Related Concussion
 Forney ISD Protocol and Procedures for the Management of the Sports-Related Concussion Medical management of sports-related concussion is evolving. Recently, there has been a significant amount of research
Forney ISD Protocol and Procedures for the Management of the Sports-Related Concussion Medical management of sports-related concussion is evolving. Recently, there has been a significant amount of research
Whitnall High School 5000 South 116th St. Greenfield, WI 53228
 Concussion Information - When in Doubt, Sit Them Out! 1. Before a student may participate in practice or competition: At the beginning of a season for a youth athletic activity, the person operating the
Concussion Information - When in Doubt, Sit Them Out! 1. Before a student may participate in practice or competition: At the beginning of a season for a youth athletic activity, the person operating the
Brains are Worth It: Concussion Symposium Vancouver, BC November 10, 2010
 Brains are Worth It: Concussion Symposium Vancouver, BC November 10, 2010 Dr. Brian Hunt Co- Director ThinkFirst BC Neurological Surgeon Lions Gate Hospital, North Vancouver Dr. Shelina Babul-Wellar Associate
Brains are Worth It: Concussion Symposium Vancouver, BC November 10, 2010 Dr. Brian Hunt Co- Director ThinkFirst BC Neurological Surgeon Lions Gate Hospital, North Vancouver Dr. Shelina Babul-Wellar Associate
Neurological Effects of Sports-Related Injury
 Neurological Effects of Sports-Related Injury DAVID RUBIN, MD Disclosures Neither I nor my spouse/partner has a relevant financial relationship with a commercial interest to disclose Epidemiology 1.6 3.8
Neurological Effects of Sports-Related Injury DAVID RUBIN, MD Disclosures Neither I nor my spouse/partner has a relevant financial relationship with a commercial interest to disclose Epidemiology 1.6 3.8
Little League Concussion Information Sheet
 Little League Concussion Information Sheet Why am I getting this information sheet? You are receiving this information sheet about concussion because of California Assembly Bill 2007 (2016), which added
Little League Concussion Information Sheet Why am I getting this information sheet? You are receiving this information sheet about concussion because of California Assembly Bill 2007 (2016), which added
University of Central Arkansas Concussion Protocol and Management Plan
 University of Central Arkansas Concussion Protocol and Management Plan 5/2018 It is often reported that there is no universal agreement on the standard definition or nature of concussion; however, agreement
University of Central Arkansas Concussion Protocol and Management Plan 5/2018 It is often reported that there is no universal agreement on the standard definition or nature of concussion; however, agreement
STAMFORD CENTRAL SCHOOL CONCUSSION POLICY
 STAMFORD CENTRAL SCHOOL CONCUSSION POLICY Revised October 14, 2015 Page 1 Management of Sports-Related Concussions StamfordCentralSchool District Medical management of sports-related concussion continues
STAMFORD CENTRAL SCHOOL CONCUSSION POLICY Revised October 14, 2015 Page 1 Management of Sports-Related Concussions StamfordCentralSchool District Medical management of sports-related concussion continues
POLICY / PROCEDURE DOCUMENT Effective Date 08/19/2010. Concussion Assessment, Management, and Return to Play Guidelines
 Beacon Medical Group Sports Medicine POLICY / PROCEDURE DOCUMENT Effective Date 08/19/2010 TITLE: Document of (Entity) POLICY: PATIENT POPULATION: Concussion Assessment, Management, and Return to Play
Beacon Medical Group Sports Medicine POLICY / PROCEDURE DOCUMENT Effective Date 08/19/2010 TITLE: Document of (Entity) POLICY: PATIENT POPULATION: Concussion Assessment, Management, and Return to Play
Milford Public Schools Concussion Policy and Procedures. Department of Athletics
 Milford Public Schools Concussion Policy and Procedures Department of Athletics The mission of this document is to make known the procedures for prevention, recognition and management of MTBI (mild traumatic
Milford Public Schools Concussion Policy and Procedures Department of Athletics The mission of this document is to make known the procedures for prevention, recognition and management of MTBI (mild traumatic
What is concussion? DR MARTIN RAFTERY CHIEF MEDICAL OFFICER NOVEMBER 2016
 What is concussion? DR MARTIN RAFTERY CHIEF MEDICAL OFFICER NOVEMBER 2016 2 WHAT IS RUGBY? Short video CONCUSSION WHY IMPORTANT? 1. Can mimic more serious intra-cranial injury 2. Can lead to persistent
What is concussion? DR MARTIN RAFTERY CHIEF MEDICAL OFFICER NOVEMBER 2016 2 WHAT IS RUGBY? Short video CONCUSSION WHY IMPORTANT? 1. Can mimic more serious intra-cranial injury 2. Can lead to persistent
BRSC Concussion Policy & Protocol
 BRSC Concussion Policy & Protocol January 2018 BRSC has a full-time, certified Athletic Trainer on staff that provides immediate care for concussed athletes. BRSC also requires coaches at our competitive
BRSC Concussion Policy & Protocol January 2018 BRSC has a full-time, certified Athletic Trainer on staff that provides immediate care for concussed athletes. BRSC also requires coaches at our competitive
Concussion Management and Update. Objectives
 Concussion Management and Update Ricardo Guirola MD M Ed Pediatric Rheumatology Primary Care Sports Medicine Objectives Review definition, signs and symptoms Discuss the initial evaluation of a patient
Concussion Management and Update Ricardo Guirola MD M Ed Pediatric Rheumatology Primary Care Sports Medicine Objectives Review definition, signs and symptoms Discuss the initial evaluation of a patient
North Thurston Public Schools Concussion Information Sheet
 North Thurston Public Schools Concussion Information Sheet Definition A concussion is a brain injury that may be caused either by a direct blow to the head, face, neck or elsewhere on the body with an
North Thurston Public Schools Concussion Information Sheet Definition A concussion is a brain injury that may be caused either by a direct blow to the head, face, neck or elsewhere on the body with an
Davidson College Sports Medicine Concussion Management Policy
 Davidson College Sports Medicine Concussion Management Policy Davidson College practices concussion management care based on the most current research and consensus statements from noted concussion experts.
Davidson College Sports Medicine Concussion Management Policy Davidson College practices concussion management care based on the most current research and consensus statements from noted concussion experts.
The NOJHL Sport Concussion Policy and Management Protocol. Developed by Dr. Chris Myers, D.C., BMSc. Updated as of August 2018
 The NOJHL Sport Concussion Policy and Management Protocol Developed by Dr. Chris Myers, D.C., BMSc Updated as of August 2018 The NOJHL concussion policy and concussion management protocol have been developed
The NOJHL Sport Concussion Policy and Management Protocol Developed by Dr. Chris Myers, D.C., BMSc Updated as of August 2018 The NOJHL concussion policy and concussion management protocol have been developed
CONCUSSIONS: What You Really Need to Know Dr. Emily Dixon
 CONCUSSIONS: What You Really Need to Know Dr. Emily Dixon TriHealth Heads Count Concussion Medical Director Emily Dixon, DO Born and raised north of Kansas City, Missouri. Earned her medical degree from
CONCUSSIONS: What You Really Need to Know Dr. Emily Dixon TriHealth Heads Count Concussion Medical Director Emily Dixon, DO Born and raised north of Kansas City, Missouri. Earned her medical degree from
Jefferson County School District Protocol and Procedures for Management of Sports-Related Concussions
 Jefferson County School District 509J 390 SE 10 th St. Madras, OR 97741 Jefferson County School District Protocol and Procedures for Management of Sports-Related Concussions Medical management of a sports-related
Jefferson County School District 509J 390 SE 10 th St. Madras, OR 97741 Jefferson County School District Protocol and Procedures for Management of Sports-Related Concussions Medical management of a sports-related
Diagnosis and Management of Concussion. Dr. Kathryn Giles MD, MSc., FRCPC Cambridge Ontario
 Diagnosis and Management of Concussion Dr. Kathryn Giles MD, MSc., FRCPC Cambridge Ontario Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored,
Diagnosis and Management of Concussion Dr. Kathryn Giles MD, MSc., FRCPC Cambridge Ontario Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored,
Diagnosis and Management of Concussion. Dr. Kathryn Giles MD, MSc., FRCPC Cambridge Ontario
 Diagnosis and Management of Concussion Dr. Kathryn Giles MD, MSc., FRCPC Cambridge Ontario Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored,
Diagnosis and Management of Concussion Dr. Kathryn Giles MD, MSc., FRCPC Cambridge Ontario Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored,
NovaCare Rehabilitation Athletic Training Services
 NovaCare Rehabilitation Athletic Training Services Concussion Management Standards: Harrisburg Academy 10 Erford Rd Wormleysburg, PA 17043 Medical management of sports-related concussion is evolving. In
NovaCare Rehabilitation Athletic Training Services Concussion Management Standards: Harrisburg Academy 10 Erford Rd Wormleysburg, PA 17043 Medical management of sports-related concussion is evolving. In
CONCUSSION IN SPORT AUSTRALIA POSITION STATEMENT
 CONCUSSION IN SPORT AUSTRALIA POSITION STATEMENT An initiative of the Australian Institute of Sport, Australian Medical Association, Australasian College of Sport and Exercise Physicians and Sports Medicine
CONCUSSION IN SPORT AUSTRALIA POSITION STATEMENT An initiative of the Australian Institute of Sport, Australian Medical Association, Australasian College of Sport and Exercise Physicians and Sports Medicine
