Lumbar Spine Management. Jason Zafereo, PT, OCS, FAAOMPT
|
|
|
- Brett Booth
- 6 years ago
- Views:
Transcription
1 Lumbar Spine Management Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education Are we being billed for this? 1
2 Objectives 2 Discuss the components of the ICF classification scheme Describe the treatment interventions used for the primary management of: Pain Stiffness Weakness Describe treatment considerations for rehabilitation after disc or fusion surgery
3 3 TREATMENT BY CLASSIFICATION
4 Old Classification Categories 4 Treatment-based classification (TBC) system (Delitto et al 1995) Pain-dominant treatment Specific Exercise Traction Impairment-dominant treatment Mobilization Stabilization
5 New Classification Categories ICF-based system (Delitto et al, JOSPT 2012) Pain-dominant treatment Acute LBP with referred LE pain Acute - Chronic LBP with radiating LE pain Impairment-dominant treatment Acute - Chronic LBP with mobility deficits Acute - Chronic LBP with movement impairments Acute LBP with related cognitive or affective tendencies Chronic LBP with related generalized pain 5
6 Acute LBP with Referred LE Pain 6 Often worsens with flexion Preference for lateral shift and sitting Visible frontal plane deviation of shoulders to Centralization with specific pelvis postures/rom Preference for extension Limited lumbar extension Symptoms distal to the mobility buttock Lateral trunk shift possible Symptoms centralize with lumbar extension Findings of Symptoms peripheralize subacute/chronic LBP with with lumbar flexion movement impairments Preference for traction Delitto et al, JOSPT 2012 No movements centralize symptoms Fritz et al 2007
7 Acute-Chronic LBP with Radiating Pain LE paresthesias, numbness, weakness, DTR changes possible Concordant sx with initial to mid range (acute), mid to end range (subacute), or sustained mvts/ nerve tension tests Delitto et al, JOSPT 2012 Preference for flexion Age > 50 Imaging evidence of lumbar spinal stenosis Preference for traction Signs and symptoms of nerve root compression Fritz et al
8 Acute-Chronic LBP with Mobility Deficits 8 Restricted ROM/segmental mobility of at least one of the following regions: Thoracic Lumbar Lumbopelvic Hip Concordant sx with LS PA (acute) or end range movements (subacute) Delitto et al, JOSPT 2012 Manipulation CPR Asymmetrical lateral flexion Positive Cibulka cluster Fritz et al 2007
9 Acute-Chronic LBP with Movement Impairments 9 Recurrent LBP, commonly referred Concordant sx with LS PA (acute-subacute), initial to mid range mvts (acute), mid to end range mvts (subacute), or sustained end range mvts (chronic) Hypermobile PA Stiff Thorax, Pelvis, Hips Weak Trunk, Hips Delitto et al, JOSPT 2012 Stabilization CPR Recurrent episodes with trivial onset History of lateral shift with alternating sides Prior use of manipulation for relief Trauma, pregnancy Relief with bracing Fritz et al 2007
10 Acute LBP with Related Cognitive or Affective Tendencies Chronic LBP with Related Generalized Pain 10 One or more of the following: High Fear-Avoidance or Anxiety FABQ-PA: Sum 2-5 Cutoff >14 FABQ-W: Sum 6-7, 9-12, 15 Cutoff >29 High Pain Catastrophizing Scale scores Rumination: 8-11 Magnification: 6-7,13 Helplessness:1-5,12 During the past month, have you often been bothered by feeling down, depressed, or hopeless? During the past month, have you often been bothered by little interest or pleasure in doing things? 2 no answers = -LR of 0.07 Delitto et al, JOSPT 2012
11 Classification Reliability and Utility 11 Reliability K =.60 when traction removed (paper assessment) Fritz et al 2006 K =.52 for all groups (individual assessment) Stanton et al, PT 2011 Utility Classification versus clinical practice guidelines or unmatched care Significant improvements in pain, disability, general health, satisfaction, and likelihood of returning to work in matched classification group (4 wks & 1yr) Fritz et al 2003; Brennan et al 2006
12 Prevalence Data 50% of patients meet criteria for one subgroup Of remaining 50%... 25% cannot be classified (myofascial pain?) 25% fit >1 classification 68% of these individuals fitting manipulation/specific exercise Stanton et al, PT 2011 (acute); Apeldoorn et al, Spine 2012 (chronic) c) 12
13 Beyond the old TBC 13 Classification often unclear in patients who are older, chronic, less affected by LBP (FABQ and ODI) Stanton t et al 2013 Treatment by old TBC criteria yielded equivocal outcomes to an individualized approach (Dutch LBP guidelines) (Apeldoorn et al 2012) and did not reveal a preference for matched care in the stabilization category (Henry et al 2014) in patients with CLBP New ICF guidelines represent the best attempt yet to provide considerations for directional preferences, regional interdependence, and chronic pain states
14 14 PAIN-DOMINANT TREATMENT
15 Pain-Dominant Treatment Contractile Myofascial pain syndrome Non-contractile Acute to subacute LBP with referred/radiating pain Lumbar spine stenosis Cauda equina syndrome Herniated disc HNP with radiculopathy Sciatica 15
16 Comprehensive Treatment for Pain 16 Tissue-Specific Rx Contractile Soft tissue mobilization Dry needling Submaximal isometrics Non-contractile Graded mobilization Graded spinal ROM (directional pref) Spinal traction Neural gliding/tensioning Generalized Rx Relative rest Education Modalities Short-term orthosis Exercise Relaxation/Breathing Cognitive behavioral therapy
17 Myofascial Pain Syndrome 17 Environmental/Emotional/Physical Ergonomics (short upper arms) Stress Hormone and Vitamin deficiencies Structural misalignment (legs and pelvis) Mechanical Underlying facilitated segment or thoracolumbar joint dysfunction SI joint dysfunction (Iliopsoas/Quadratus) Synergist/agonist strengthening
18 Support for Myofascial Pain Management 18 Non-specific low back pain (13 studies) Massage might be beneficial i for patients t with subacute and chronic non-specific low back pain, especially when combined with exercises and education. Furlan et al, Cochr Syst Rev 2008 Myofascial low back pain Support for multimodal treatment including massage, correction of muscle imbalance, and dry needling Malanga and Cruz, Phys Med Rehabil Clin N Am 2010 Furlan et al, Spine 2005 Currently no high quality evidence supporting the use of US for improved pain/qol Ebadi et al., 2014
19 Acute to Subacute LBP with Referred/Radiating Pain Management Disc Graded d ROM (Specific Exercise) Graded Axial distraction (Traction) Nerve Graded ROM Specific Exercise Neural gliding Painfree (Acute) Mid to end-range (Subacute) Graded Axial distraction 19
20 Specific Exercise Philosophy Achieve centralization of patient s referred pain Patient-directed approach consisting of McKenzie-based techniques Perform movements in opposite direction once movement no longer creates peripheralization 20
21 Specific Exercise - Extension Positioning Patient t prone lying or prone on elbows Useful when movement peripheralizes sx Typically acute Hold positions for minutes 21
22 Specific Exercise - Extension 22 ROM Passive movements Prone press up Standing back bends Perform in sets of 10 until sx centralization plateaus Perform as many timesasneeded during the day
23 Specific Exercise - Translocation Positioning Sidelying on the side describing the shift Pillows under thorax to encourage pelvic translocation Prone with pelvic translocation Standing lateral l shift correction Active ROM 23
24 Specific Exercise - Translocation Standing lateral shift correction Passive ROM with therapist Active-assist ROM on lat bar with manual correction Patients beginning with a translocation preference will typically favor extension at some point 24 Laslett, JMMT 2009
25 Specific Exercise - Flexion 25 Positioning Supine hook lying Supine 90/90 Seated forward bend Passive ROM Quadruped flexion Bilateral/unilateral knees to chest Active ROM Standing/Seated lumbar flexion Post pelvic tilts
26 Subacute Management of Referred/Radiating Pain Specific exercise Self treatment t t techniques should be exhausted before application of therapist-assisted assisted technique Therapist assistance provided via positioning, PA mobilization, overpressure, or soft tissue mobilization 26
27 Subacute Management of Referred/Radiating Pain 27 Extension therapist-assisted techniques Overpressure Stabilization of pelvis during prone press ups Extension mobilization PA over level l that t provides favorable response Followup with prone press ups Lateral compartment t Pelvic translocation away from pain side Maintain position during prone press ups
28 Subacute Management of Referred/Radiating Pain 28 Flexion therapistassisted techniques Soft tissue mobilization or overpressure while patient is in position of flexion Best applied in Quadruped Leaning over edge of table Sitting
29 Support for Directional Preference 29 Systemic review supports short term to intermediate benefits (Claire et al. Aust J Physiother 2004; Machado et al. Spine 2006; Surkitt et al. PT 2012) Moderate evidence DPM superior to multidirectional mid-range exercises, stretches, and advice in those with DP Conflicting evidence when DPM compared to manual therapy and strengthening Patients given exercises matched to their movement preference improved significantly in pain, med use, disability y( (Long et al, Spine 2004)
30 Support for Centralization 30 Patients centralizing with repeated movements SE and mobilization superior to stabilization for pain/disability at 1 week, disability at 4 weeks and 6 months Browder et al. JOSPT 2007 SE superior to manipulation for patient reports of success (2mos) and disability (2mos/12mos) Petersen et al 2011 Patient experiencing reduced pain levels ( 2/10) with mobilization and prone press ups demonstrated concurrent increase in disc water diffusion Beattie et al, 2010 Rates of centralization in other CPR categories Manipulation = 68% Stabilization = 80% Werneke et al, 2010
31 Spinal Traction Philosophy Achieve centralization of patient s referred pain Patient-directed Positional Maximum IVF opening with flexion, side bending contralateral, rotation ipsilateral Creighton JMMT 1993 Therapist-directed Manual Mechanical 31
32 Spinal Traction 32 Effective parameters in the literature 30-60% body weight Static or intermittent (3:1) duty cycle 12-15mins Supine or prone Cai et al 2009, Fritz et al 2007, Saunders 1993
33 Conflicting Support for Traction (General LBP) 33 Traction efficacy (pain and disability) not endorsed in systematic reviews for mixed samples of LBP Macario and Pergolizzi, Pain Pract 2006; Clark et al, Spine 2006 Physiological effects are supported Widens IVF/Stretch posterior spinal elements (Lehmann et al 1958) Creates negative intradiscal pressure (Ramos et al, J Neurosurg, 1994)
34 Support for Traction Population: Lumbar Radiculopathy Intervention: Lumbar extension exercises (6 weeks) versus lumbar extension protocol with traction (2 weeks) Significant improvements in disability and FABQ favoring traction group at two weeks Improved outcomes and sustained changes in subgroup at six weeks Positive crossed leg raise (<45deg) Lower extremity pain that peripheralized with extension Fritz et al
35 Subacute LBP with Radiating (Non- Peripheralizing) Pain Management Neural gliding Generalized PT program (aerobic exercise, global PRE, and PA mobilization) versus Generalized PT with Slump stretching (30secx5), 2x/week x 3 weeks Slump group improved disability, pain compared to control Cleland et al 2006 Nagrale et al
36 Acute to Subacute LBP with Referred/Radiating Pain Management 36 Contributing Impairments (Env.) Ergonomics Encourage positioning into specific exercise movement preference Weight bearing Wheeled walker: >250% increase in self reported walking distance in 71% of subjects Goldman et al, J Fam Pract 2008 Walking stick: no significant improvement in walking tolerance Comer et al, Arch Phys Med Rehabil 2010
37 Acute to Subacute LBP with Referred/Radiating Pain Management Contributing Impairments 37 Mechanical Mobilization of hypomobile segments above/below level Tightness opposite specific exercise movement preference Mobilization of nerve interface points Strengthening of hypotonic lumbopelvic muscles to address underlying instability Weakness into specific exercise movement preference
38 Support for Contributing ti Impairment Management 38 Population: Lumbar Spine Stenosis Intervention: Flexion-based program with progressive walking program versus manual therapy to hips and spine with PRE and unweighted treadmill ambulation (6 weeks) Significant ifi improvements in disability and pain at 6 weeks, 1 year, and 29 months in both groups Improved perceived recovery in manual therapy group (79% vs 41% at 6 weeks) Whitman et al Spine 2006
39 Support for Contributing ti Impairment Management Population: Subacute to chronic back-related LE pain (not stenosis) Intervention: ROM and stabilization exercise versus manual therapy (including thrust) with ROM and stabilization exercise (12 weeks) Significant improvements in disability, pain, medication usage, satisfaction, global improvement, and medication use at 12 weeks Maintained satisfaction, global improvement, and meds at 1 year Bronfort et al,
40 40 STIFFNESS-DOMINANT TREATMENT
41 Treatment Considerations Primary treatment for patients in Acute to Chronic LBP with Mobility Deficits category Classification for patients with undifferentiated pain May address a mixture of myofascial, joint, or neural limitations in motion Primary treatment for addressing motion loss in patients without a chief complaint of pain Reduced manual emphasis in Acute LBP with Related Cognitive or Affective Tendencies and Chronic LBP with Related Generalized Pain 41
42 Spinal Manipulative Therapy (SMT) Cochrane Reviews In general, SMT not superior to inert treatment, sham SMT, or other active treatments in acute or chronic heterogeneous LBP subjects Rubinstein et al 2013 (acute) Rubinstein et al 2011 (chronic) Thrust equal to non-thrust in CLBP (Cook et al 2013) and adults 55+ (Learman et al 2013) 42
43 Acute LBP with Mobility Deficits CPR for lumbar manipulation Duration of symptoms < 16 days * No symptoms distal to the knee * At least one hip with > 35 of IR Hypomobility with lumbar PAIVM testingti FABQ(W) < 19 4/5 criteria Posttest probability of success increased from 44% to 92% (+LR=13.2) Flynn et al, Spine 2002; Childs et al, Ann Intern Med CPR has been Validated!
44 In Patients Fitting the CPR Expect a good prognosis regarding ODI change, NPRS change, # visits, extent of recovery Cook et al, 2013 Thrust technique (lumbopelvic or lumbar rotation) does not matter Range of inferior to equal outcomes for nonthrust techniques Cleland et al, 2009; Learman et al, 2014 Equivocal outcomes between repeated end range movements and manipulation Schenk et al, 2012 End range may be what s most important! 44
45 Inability to Respond to Manipulation Longer duration of symptoms Symptoms in the buttocks or leg Absence of hypomobility/pain on mobility testing Less discrepancy in the left to right hip IR ROM Negative Gaenslen s sign Peripheralization with motion testing Fritz et al, PT
46 Chronic LBP with Mobility Deficits 46 Case series 8 patients t with chronic LBP and hip stiffness in at least 2 planes 3 visits it for hip mobilization and hip stretching 62.5% rated improvement as moderately better or higher on GROC 24.4% improvement on ODI Burns et al, JMMT 2011
47 Chronic LBP with Mobility Deficits RCT investigating non- region specific manipulation for CLBP Immediate pain reduction for T1-T5 manipulation comparable to L2-L5 manipulation De Oliveira et al., PT
48 48 PRIMARY INSTABILITY IMPAIRMENT
49 Treatment Considerations Primary treatment for patients in Acute to Chronic LBP with Movement Coordination Impairments category Classification for patients with undifferentiated pain Treatment primarily focused on contractile tissue neuromuscular re-education/strengthening at the site of pain Secondary treatment for patients in all other categories, especially Acute LBP with Referred LE Pain 49
50 Examples of Education for Joint Instability 50 Sleeping Pillow between the knees, under the lateral trunk, or anterior to trunk Medium mattress preferred to firm Sitting Kovacs et al, 2003 Foot support Lumbar support Arm support LS corsets Equivocal findings for management van Duijvenbode et al, 2008
51 Overview of Exercise Progression Strengthening of lumbar spine away from syndrome Avoids aggravation associated with loading into DSM Begin with isometrics of deep stabilizers, progress to superficial muscles Teach patient how to use lumbar region more Stretching of thoracic spine and hips spine into syndrome Motor control of lumbar spine into syndrome Ensures activation of weakest synergist(s) Teach patient how to use hip and thoracic regions more 51
52 Examples of Initial Treatment for Joint Instability Independent activation and tonic hold Pelvic floor TRA (extension syndrome) Lumbar multifidus isometrics (flexion syndrome) Glutes (rotation syndrome) 52
53 Examples of Progressive Treatment for Joint Instability 53 Integrated tonic hold Iliopsoas strengthening (flexion syndrome) Glut max and thoracic extensor strengthening (extension syndrome) Hip versus lateral trunk strengthening (rotation syndrome)
54 Recruitment of Abdominal Muscles 54 Drawing-in maneuver and Bird-dog (TRA) Posterior pelvic tilt and abdominal bracing (IO) Side plank and Abdominal crunch (Both) Urquhart et al, Man Ther 2005; Teyhen et al, JOSPT 2008 Hollowing during typical exercises increases TRA recruitment from 4-43% Bjerkefors et al, Manual Therapy 2010 Adding ankle DF to drawing-in led to greater gains in pain/function You et al, Clinical Rehabilitation, 2013
55 Recruitment of Gluteals over TFL 55 Clam Neutral (vertical) pelvis maximizes G med/max activation Gmed maximized i at 60deg hip flexion Sidestepping Unilateral bridge Quadruped hip extension with bent/straight knee Willcox & Burden, 2013; Selkowitz et al, 2013
56 Chronic LBP with Mobility Deficits A Meta Analysis and RCT 56 Motor control exercise was superior to general exercise, manual therapy, and minimal intervention for the reduction of pain and disability at variable time intervals, depending on the comparison condition First evidence suggesting widespread application of this procedure in heterogeneous samples of CLBP subjects (Bystrom et al, 2013) No added benefit to matching motor control deficit to exercise preference in CLBP using Sahrmann categories (Henry et al. 2014) Lack of evidence for matched stabilization treatment in ALBP or chronic widespread pain
57 Acute LBP with Mobility Deficits A Systematic and Cochrane Review 57 Evidence for general exercise programs Systematic Review: Acute LBP Equivocal results for exercise compared to other interventions in acute population (C) Lawrence et al, 2008 Cochrane Review Moderate quality evidence that post-treatment exercise program can prevent recurrence of low back pain Choi et al, 2010
58 Acute LBP with Mobility Deficits it Who Needs Motor Control Approach? CPR for lumbar stabilization Age < 41 years * Positive prone instability test Aberrant motion SLR > 91 3/4 criteria (LR+ = 4.0) Validation study failed to completely support CPR (underpowered?) Modified CPR of + PIT and aberrant movement may provide better predictive validity 58 Hicks et al, Arch Phys Med Rehabil 2005; Rabin et al, JOSPT, 2014
59 Motor Control Exercise in Radiographic Instability Population: Spondylolysis or spondylolisthesis Intervention: Stabilization program with TRA and multifidus focus versus treatment t t as directed d by PT (10 weeks) Significant improvements in disability and pain at 10 weeks and 30 months in stabilization group O Sullivan et al, Spine
60 Inability to Respond to Stabilization 60 Discrepancy in SLR ROM >10deg Apeldoorn et al, 2012 Negative prone instability test Hypomobility with PAIVM testing Aberrant motion absent FABQ(PA) score 9 2/4 criteria SN =.85; SP =.87 Hicks et al, Arch Phys Med Rehabil 2005
61 Summary of Recommendations: Acute-Chronic LBP with Movement Impairments 61 Education Supportive postures Ergonomic activities Temporary bracing (acute) Motor control exercise Begin with isolated contractions and holds Progress to isotonic open/closed chain loading Graded dosing: 2min total time under tension PRE Functional movements Gym-based activity Pilates Manual therapy to thoracic spine, ribs, sacrum, and hips Progression to work reintegration programs as needed Delitto et al, JOSPT 2012
62 Summary of Recommendations: Acute LBP with Related Cognitive or Affective Tendencies and Chronic LBP with Related Generalized Pain 62 Education De-emphasize pathology Emphasis on anatomical strength of spine Neuroscience of pain Overall favorable prognosis of LBP Strategies to limit fear and catastrophizing (CBT) Emphasis on increasing activity capacity, not just pain relief =4b8oB757DKc Fitness Low intensity, submaximal fitness and endurance activities for above mentioned categories Moderate to high intensity exercise for CLBP without generalized pain Exercise Graded stabilization Graded functional activity Delitto et al, JOSPT 2012
63 Graded d Functional Activities iti vs Stabilization 63 Graded functional activity versus motor control exercise No significant difference between groups at 2, 6, and 12 months Macedo et al, PT 2012 Graded stabilization program compared to general walking program 55% success (stab) versus 26% success (walk) at 12 and 36 months Rasmussen-Bar et al, Spine 2009
64 Lumbar Spine Instability Questionnaire 64 Give way or give out Self-manipulation Frequent pain in the day Back catches or locks Pain with sit to stand Pain with supine to sit Painful quick, unexpected, mild movements Need back support in chair Pain with sustained posture Worsening over time Temporary relief with corset Muscle spasms common Fearful of movement Trauma MOI in the past Long duration of problem Positive test is 9/15 Predictive of which CLBP patients respond best to motor control over graded exercise Macedo et al., 2014
65 Aquatic Therapy in CLBP 5x/w x 4w supervised 60min aquatic program to comparably dosed unsupervised land HEP Both groups improved; Statistical (not clinical) significant difference in ODI and QL scores Dundar et al, Spine x/w x 6w supervised 60min aquatic versus land program Both groups improved pain/function, no differences Sjogren, Physiother Res Int 1997 Systematic review supported benefits in CLBP and pregnancy Waller et al, Clin Rehabil
66 66 POST-SURGICAL MANAGEMENT
67 Overview 67 Pain/Pathology focus is patient dependent, usually limited Cryotherapy/TENS for post-surgical pain Impairment focus is key Stabilization Neural gliding Conditioning Spinal ROM Mobilization away from surgical site Cioppa-Mosca et al, 2006; Maxey and Magnusson 2013
68 Lumbar Fusion Types 68 Instrumented Posterolateral t l fusion Disc preserved Most common Multifidus partial denervation Anterior lumbar interbody fusion Disc resected Circumferential fusion Oblique partial denervation Cage fusion Disc resected Interbody fusion only
69 Lumbar Fusion Rehab Considerations 69 Outpatient therapy typically begins at 6-10 weeks post-opop Precautions No iliopsoas stretching until 8 weeks No lifting >10lbs or overhead until 12 weeks No lumbar standing ROM testing or iliopsoas MMT until ready for return to sport (typically 20 weeks) No US over healing fusion No end range extension for 6 months (cage)
70 Lumbar Disc Surgical Procedures 70 Disc replacement Anterior approach consistent t with cage fusion Lumbar discectomy Microscopic or open Lamina removal variable Multifidus partial denervation possible Minimally invasive percutaneous technique Chemonucleolysis Percutaneous discectomy
71 Lumbar Disc Rehab Considerations Outpatient therapy typically begins at 4-6 weeks post-opop Discectomy Precautions Limit lumbar flexion stress 71 No lumbar standing ROM or slump testing until 6 th week Running and return to sport between 8-12 weeks Replacement Precautions Limit lumbar extension stress No lumbar standing ROM or PAs until 6-8 weeks Return to sport weeks
72 Lumbar Surgery General Guidelines 72 Body mechanics Stabilization All positions Conditioning Bike, treadmill Stretching Hip and leg muscles Scar mobility Thoracic/Hip joints Neural mobilization Lumbar spine Strengthening (discectomy) Back extensors (Kulig et al 2009)
73 Support for Post-Operative PT 73 Cochrane Review: 14 trials, status post discectomy or microdiscectomy (Ostelo et al 2009) Moderate quality evidence Exercise more effective than no treatment at improving disability High intensity exercise more effective than low intensity exercise Low quality evidence + effects of exercise (regardless of intensity) on pain Negligible gg effects of neural gliding gshort-long term Home and supervised programs yield same short term results 8 week exercise program administered 2 weeks post- op discectomy (Hebert et al, 2015) No difference in general vs specific exercise programs on clinical outcomes or multifidus function at 10wks or 6mos
Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology
 Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
Lumbar Spine Applied Anatomy. Jason Zafereo, PT, OCS, FAAOMPT
 Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education 1 Objectives Apply key concepts from the cervical anatomy/kinesiology self-study to aid
Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education 1 Objectives Apply key concepts from the cervical anatomy/kinesiology self-study to aid
Lumbar Spine Applied Anatomy. Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education
 Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education Objectives Discuss concepts relevant to pathophysiology and differential diagnosis for lumbar radiculopathy
Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education Objectives Discuss concepts relevant to pathophysiology and differential diagnosis for lumbar radiculopathy
Thoracic Spine Management. Jason Zafereo, PT, OCS, FAAOMPT
 Thoracic Spine Management Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education Objectives Describe the treatment interventions used for the management of pain from contractile
Thoracic Spine Management Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education Objectives Describe the treatment interventions used for the management of pain from contractile
LUMBAR SPINE CASE 3. Property of VOMPTI, LLC. For Use of Participants Only. No Use or Reproduction Without Consent 1. L4-5, 5-S1 disc, facet (somatic)
 LUMBAR SPINE CASE 3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Richmond 2018-2019 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
LUMBAR SPINE CASE 3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Richmond 2018-2019 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT
 LUMBAR SPINE CASE #3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
LUMBAR SPINE CASE #3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
Exercise for Rehabilitation and Treatment: Summary of Research
 Exercise for Rehabilitation and Treatment: Summary of Research Summarizing research findings to evaluate the effectiveness of exercise for rehabilitation and treatment of orthopedic conditions Summary
Exercise for Rehabilitation and Treatment: Summary of Research Summarizing research findings to evaluate the effectiveness of exercise for rehabilitation and treatment of orthopedic conditions Summary
Low back pain (LBP) is the reason for seeking care in nearly 50% of
 [ clinical commentary ] Julie M. Fritz, PT, PhD, ATC 1 Joshua A. Cleland, PT, PhD, OCS, FAAOMPT 2 John D. Childs, PT, PhD, MBA, OCS, FAAOMPT 3 Subgrouping Patients With Low Back Pain: Evolution of a Classification
[ clinical commentary ] Julie M. Fritz, PT, PhD, ATC 1 Joshua A. Cleland, PT, PhD, OCS, FAAOMPT 2 John D. Childs, PT, PhD, MBA, OCS, FAAOMPT 3 Subgrouping Patients With Low Back Pain: Evolution of a Classification
DPT 772 Spine Notebook Matt Kubalski, SPT
 DPT 772 Spine Notebook Matt Kubalski, SPT Table of Contents: IMPAIRMENTS/CLASSIFICATIONS PAGES Neck Pain with Mobility Deficit: Cervicalgia, Pain in thoracic spine - JOSPT 3-6 Neck Pain with Headache:
DPT 772 Spine Notebook Matt Kubalski, SPT Table of Contents: IMPAIRMENTS/CLASSIFICATIONS PAGES Neck Pain with Mobility Deficit: Cervicalgia, Pain in thoracic spine - JOSPT 3-6 Neck Pain with Headache:
When Clinical Reasoning Overrules the Evidence
 When Clinical Reasoning Overrules the Evidence Breakout session Paul Mintken PT, DPT, OCS, FAAOMPT Kristin Carpenter PT, DPT, OCS, FAAOMPT Amy McDevitt PT, DPT, OCS, FAAOMPT Objectives Break Out Session
When Clinical Reasoning Overrules the Evidence Breakout session Paul Mintken PT, DPT, OCS, FAAOMPT Kristin Carpenter PT, DPT, OCS, FAAOMPT Amy McDevitt PT, DPT, OCS, FAAOMPT Objectives Break Out Session
Labral Repair with a Microfracture
 Labral Repair with a Microfracture This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for
Labral Repair with a Microfracture This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for
Hip Arthroscopy. Labral Repair/Debridement with Femoroplasty
 Precautions for weeks 1 4 post-op: Hip Arthroscopy Labral Repair/Debridement with Femoroplasty Patient Education o For 1 week, Assist the involved LE during all transfers o For 2 weeks, Do not sit with
Precautions for weeks 1 4 post-op: Hip Arthroscopy Labral Repair/Debridement with Femoroplasty Patient Education o For 1 week, Assist the involved LE during all transfers o For 2 weeks, Do not sit with
EXERCISE PRESCRIPTION PART 1
 EXERCISE PRESCRIPTION PART 1 Michael McMurray, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 What is MET? An active rehabilitation system based in the biopsychosocial
EXERCISE PRESCRIPTION PART 1 Michael McMurray, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 What is MET? An active rehabilitation system based in the biopsychosocial
Algorithm #1 Lumbo-Pelvic Region Examination
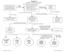 Red Screen for Potentially Serious Conditions (i.e., Red Flags) including Neurologic when indicated Positive Findings Algorithm #1 Lumbo-Pelvic Region Clinical Prediction Rule Screening: Duration of symptoms
Red Screen for Potentially Serious Conditions (i.e., Red Flags) including Neurologic when indicated Positive Findings Algorithm #1 Lumbo-Pelvic Region Clinical Prediction Rule Screening: Duration of symptoms
Role of Lumbar Stabilization Exercise and Spinal Manipulation in Low back pain. Dr. PICHET YIEMSIRI
 Role of Lumbar Stabilization Exercise and Spinal Manipulation in Low back pain Dr. PICHET YIEMSIRI Lumbar Stabilization Exercise Spinal stability Static stability Dynamic stability Stable of the back The
Role of Lumbar Stabilization Exercise and Spinal Manipulation in Low back pain Dr. PICHET YIEMSIRI Lumbar Stabilization Exercise Spinal stability Static stability Dynamic stability Stable of the back The
A Manual Therapy and Exercise Approach to Breast Cancer Rehabilitation Course
 2014 Annual Breast Cancer Rehabilitation Healthcare Provider Event A Manual Therapy and Exercise Approach to Breast Cancer Rehabilitation Course November 7 th and 8 th, 2014 Mercer University, Atlanta,
2014 Annual Breast Cancer Rehabilitation Healthcare Provider Event A Manual Therapy and Exercise Approach to Breast Cancer Rehabilitation Course November 7 th and 8 th, 2014 Mercer University, Atlanta,
Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner
 Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner Eric Chaconas PT, PhD, DPT, FAAOMPT Assistant Professor and Assistant Program Director Doctor of Physical Therapy Program Eric
Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner Eric Chaconas PT, PhD, DPT, FAAOMPT Assistant Professor and Assistant Program Director Doctor of Physical Therapy Program Eric
Thoracic Spine Mobilization for Shoulder Pain. Scott Tauferner PT, ATC
 Thoracic Spine Mobilization for Shoulder Pain Scott Tauferner PT, ATC Conflicts of Interest None 1 2 3 Participants will be able to select thoracic mobilization strategies in patients with shoulder pain.
Thoracic Spine Mobilization for Shoulder Pain Scott Tauferner PT, ATC Conflicts of Interest None 1 2 3 Participants will be able to select thoracic mobilization strategies in patients with shoulder pain.
Exercises to Correct Muscular Imbalances. presented by: Darrell Barnes, LAT, ATC, CSCS
 Exercises to Correct Muscular Imbalances presented by: Darrell Barnes, LAT, ATC, CSCS Objectives Review Functional Anatomy Identify physical imbalances that lead to injury and/or decrease performance
Exercises to Correct Muscular Imbalances presented by: Darrell Barnes, LAT, ATC, CSCS Objectives Review Functional Anatomy Identify physical imbalances that lead to injury and/or decrease performance
Internal Rotation (turning toes/knee toward other leg) 30 degree limit. limit
 Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
Travis G. - 1 Maak, - MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic Osteochondroplasty with or without Labral Repair/Debridement General Guidelines: Normalize gait pattern with brace and crutches Continuous Passive
Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic Osteochondroplasty with or without Labral Repair/Debridement General Guidelines: Normalize gait pattern with brace and crutches Continuous Passive
Lumbar Spine Differential Diagnosis. Jason Zafereo, PT, OCS, FAAOMPT
 Lumbar Spine Differential Diagnosis Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education 1 Objectives Describe the relevant findings from the history and examination indicating
Lumbar Spine Differential Diagnosis Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education 1 Objectives Describe the relevant findings from the history and examination indicating
Active-Assisted Stretches
 1 Active-Assisted Stretches Adequate flexibility is fundamental to a functional musculoskeletal system which represents the foundation of movement efficiency. Therefore a commitment toward appropriate
1 Active-Assisted Stretches Adequate flexibility is fundamental to a functional musculoskeletal system which represents the foundation of movement efficiency. Therefore a commitment toward appropriate
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
Travis G. Maak, MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 General Guidelines: Hip Arthroscopy Rehabilitation Capsular Shift with or without FAI Labral Components No external rotation greater than 30 degrees for 4 weeks No hyperextension for 4 weeks Normalize
General Guidelines: Hip Arthroscopy Rehabilitation Capsular Shift with or without FAI Labral Components No external rotation greater than 30 degrees for 4 weeks No hyperextension for 4 weeks Normalize
Movement System Diagnoses. Movement System Impairment Syndromes of the Lumbar Spine. MSI Syndrome - Assumptions. Return From Forward Bending
 Movement System Diagnoses Kinesiopathologic Pathokinesiologic Movement System Impairment Syndromes of the Lumbar Spine Shirley Sahrmann, PT, PhD, FAPTA Washington University St. Louis School of Medicine
Movement System Diagnoses Kinesiopathologic Pathokinesiologic Movement System Impairment Syndromes of the Lumbar Spine Shirley Sahrmann, PT, PhD, FAPTA Washington University St. Louis School of Medicine
Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component
 Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component ROM Restrictions: -Perform PROM in patient s PAIN FREE Range FLEXION EXTENSION EXTERNAL ROTATION 90 degrees
Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component ROM Restrictions: -Perform PROM in patient s PAIN FREE Range FLEXION EXTENSION EXTERNAL ROTATION 90 degrees
VIRGINIA ORTHOPEDIC MANUAL PHYSICAL THERAPY INSTITUTE TECHNIQUE MANUAL
 VIRGINIA ORTHOPEDIC MANUAL PHYSICAL THERAPY INSTITUTE TECHNIQUE MANUAL Lumbar and Thoracic Spine Lumbar AROM Assessment -Patient Positioning: Standing, appropriately undressed so that the lumbar and thoracic
VIRGINIA ORTHOPEDIC MANUAL PHYSICAL THERAPY INSTITUTE TECHNIQUE MANUAL Lumbar and Thoracic Spine Lumbar AROM Assessment -Patient Positioning: Standing, appropriately undressed so that the lumbar and thoracic
Precautions following Hip Arthroscopy/FAI: (Refixation/Osteochondroplasty)
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, CAM / Pincer Procedure: Labral Repair / Capsular Shift, CAM / Pincer Decompression RX: Evaluate / Treat, and follow attached protocol
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, CAM / Pincer Procedure: Labral Repair / Capsular Shift, CAM / Pincer Decompression RX: Evaluate / Treat, and follow attached protocol
Cervical Case Study. M. Benson, A. Felts, S. Kibiloski, J. Mowen, A. Rijhwani
 Cervical Case Study M. Benson, A. Felts, S. Kibiloski, J. Mowen, A. Rijhwani Medical Dx 35 y.o. female with myofascial pain No significant radiological findings other than reported flattened cervical spine,
Cervical Case Study M. Benson, A. Felts, S. Kibiloski, J. Mowen, A. Rijhwani Medical Dx 35 y.o. female with myofascial pain No significant radiological findings other than reported flattened cervical spine,
Recommended reading Christopher M Norris Back Stability edition two
 1 2 CHERRY BAKER 2017 3 Recommended reading http://www.physology.co.uk/james-tyrell-nestor/ james@physology.co.uk Christopher M Norris Back Stability edition two 4 Welcome Anatomy of the spine Vertebra
1 2 CHERRY BAKER 2017 3 Recommended reading http://www.physology.co.uk/james-tyrell-nestor/ james@physology.co.uk Christopher M Norris Back Stability edition two 4 Welcome Anatomy of the spine Vertebra
Sciatica. 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) Website: philip-bayliss.com
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353. Website: philip-bayliss.com Sciatica Nagging, burning pain radiating down the back of the leg, or dull throbbing pain in the buttocks
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353. Website: philip-bayliss.com Sciatica Nagging, burning pain radiating down the back of the leg, or dull throbbing pain in the buttocks
Microfracture. This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient.
 This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for two months (8-9 weeks). Allow to place
This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for two months (8-9 weeks). Allow to place
Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement. Normalize gait pattern with brace (if indicated) and crutches
 General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
ACE s Essentials of Exercise Science for Fitness Professionals TRUNK
 ACE s Essentials of Exercise Science for Fitness Professionals TRUNK Posture and Balance Posture refers to the biomechanical alignment of the individual body parts and the orientation of the body to the
ACE s Essentials of Exercise Science for Fitness Professionals TRUNK Posture and Balance Posture refers to the biomechanical alignment of the individual body parts and the orientation of the body to the
Proximal Hamstring Rupture: Physical Therapy Protocol
 Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment.
Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment.
Rotational Forces. : Their impact; our treatments
 Rotational Forces : Their impact; our treatments Lee Stang, LMT, LMBT, BCTMB NCBTMB Provider: 450217-06 bridgestohealthseminars.com bthseminars@gmail.com 860.985.5834 Facebook.com/BridgesToHealthSeminars
Rotational Forces : Their impact; our treatments Lee Stang, LMT, LMBT, BCTMB NCBTMB Provider: 450217-06 bridgestohealthseminars.com bthseminars@gmail.com 860.985.5834 Facebook.com/BridgesToHealthSeminars
The Lumbopelvic & Hip Region. Contents. Contents. Chapter 5 Assessment & Treatment incorporating corrective exercises/stretching. Chapter 6 Quiz T & F
 The Lumbopelvic & Hip Region Contents Chapter 1 The lumbopelvic & hip region Chapter 2 Muscle firing patterns/endurance Chapter 3 Altered biomechanics to the & hip region lumbopelvic Chapter 4 - Musculoskeletal
The Lumbopelvic & Hip Region Contents Chapter 1 The lumbopelvic & hip region Chapter 2 Muscle firing patterns/endurance Chapter 3 Altered biomechanics to the & hip region lumbopelvic Chapter 4 - Musculoskeletal
13/09/2012. Flexion. Extension
 The McKenzie Method in 2012 Mechanical Diagnosis & Therapy of the Spine & Extremities Outline Section 1 History and background Principles, evidence overview Section2 The natural history of musculoskeletal
The McKenzie Method in 2012 Mechanical Diagnosis & Therapy of the Spine & Extremities Outline Section 1 History and background Principles, evidence overview Section2 The natural history of musculoskeletal
Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer. Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement RX: Evaluate
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement RX: Evaluate
Thoracic Spine Applied Anatomy. Jason Zafereo, PT, OCS, FAAOMPT
 Thoracic Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education Objectives Discuss concepts relevant to thoracic pain of red flag origin Discuss concepts
Thoracic Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education Objectives Discuss concepts relevant to thoracic pain of red flag origin Discuss concepts
Rehabilitation Considerations Following Surgical Arthroscopy of the Hip. Joy Anderson PT, ATC, CSCS
 Rehabilitation Considerations Following Surgical Arthroscopy of the Hip Joy Anderson PT, ATC, CSCS 1 Best Rehab Program? Review of the Evidence paucity of evidence surrounding post-operative rehabilitation
Rehabilitation Considerations Following Surgical Arthroscopy of the Hip Joy Anderson PT, ATC, CSCS 1 Best Rehab Program? Review of the Evidence paucity of evidence surrounding post-operative rehabilitation
JOHN M. REDMOND, M.D.
 Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Today s session. Common Problems in Rehab. Tim Keeley B.Phty, Cred.MDT, APA Principal Physiotherapist. physiofitness.com.au facebook.
 Tim Keeley B.Phty, Cred.MDT, APA Principal Physiotherapist physiofitness.com.au facebook.com/physiofitness Today s session Essential list for the lower body Rehab starting point Focussing on activation,
Tim Keeley B.Phty, Cred.MDT, APA Principal Physiotherapist physiofitness.com.au facebook.com/physiofitness Today s session Essential list for the lower body Rehab starting point Focussing on activation,
Phase 1- Immediate Rehabilitation (1-3 weeks): Goals Precautions:
 Phase 1- Immediate Rehabilitation (1-3 weeks): Goals: Protection of the repaired tissue Prevent muscular inhibition and gait abnormalities Diminish pain and inflammation Precautions: 20 lb. flat-foot weight-bearing
Phase 1- Immediate Rehabilitation (1-3 weeks): Goals: Protection of the repaired tissue Prevent muscular inhibition and gait abnormalities Diminish pain and inflammation Precautions: 20 lb. flat-foot weight-bearing
Lumbar Stenosis Rehabilitation Using the Resistance Chair
 PRODUCTS HELPING PEOPLE HELP THEMSELVES! Lumbar Stenosis Rehabilitation Using the Resistance Chair a. Description Lumbar spinal stenosis is a term used to describe a narrowing of the spinal canal. The
PRODUCTS HELPING PEOPLE HELP THEMSELVES! Lumbar Stenosis Rehabilitation Using the Resistance Chair a. Description Lumbar spinal stenosis is a term used to describe a narrowing of the spinal canal. The
Post Operative Hip Arthroscopy Rehabilitation Protocol Dr. David Hergan Labral Repair with or without FAI Component
 Post Operative Hip Arthroscopy Rehabilitation Protocol Dr. David Hergan Labral Repair with or without FAI Component Initial Joint Protection Guidelines- (P.O. Day 1-4 wks): Joint Protection Patient education
Post Operative Hip Arthroscopy Rehabilitation Protocol Dr. David Hergan Labral Repair with or without FAI Component Initial Joint Protection Guidelines- (P.O. Day 1-4 wks): Joint Protection Patient education
Manual Manipulative Medicine: A Structural Examination for Lower Back Pain. Friday, October 2, :30 AM - 12:00 PM W116.
 Manual Manipulative Medicine: A Structural Examination for Lower Back Pain Friday, October 2, 2015 10:30 AM - 12:00 PM W116. Level: Beginner No Financial Disclosures Amir Mahajer, DO Ronald Tolchin, DO
Manual Manipulative Medicine: A Structural Examination for Lower Back Pain Friday, October 2, 2015 10:30 AM - 12:00 PM W116. Level: Beginner No Financial Disclosures Amir Mahajer, DO Ronald Tolchin, DO
Evaluation and Treatment Lumbar/Sacral Spine: Manual Therapist Approach KAMERON IHRY HODEM PT, DPT, MTC, CERT. DN
 Evaluation and Treatment Lumbar/Sacral Spine: Manual Therapist Approach KAMERON IHRY HODEM PT, DPT, MTC, CERT. DN Purpose Educate on the Evaluation of the lumbar/sacral spine using a manual therapy approach
Evaluation and Treatment Lumbar/Sacral Spine: Manual Therapist Approach KAMERON IHRY HODEM PT, DPT, MTC, CERT. DN Purpose Educate on the Evaluation of the lumbar/sacral spine using a manual therapy approach
ATHLETIC CONDITIONING ON THE ARC BARREL
 ATHLETIC CONDITIONING ON THE ARC BARREL page 1 INTRODUCTION The STOTT PILATES Athletic Conditioning stream serves as a bridge between STOTT PILATES standard repertoire and the CORE Athletic Conditioning
ATHLETIC CONDITIONING ON THE ARC BARREL page 1 INTRODUCTION The STOTT PILATES Athletic Conditioning stream serves as a bridge between STOTT PILATES standard repertoire and the CORE Athletic Conditioning
Pilates for Lumbar Spinal Fusion: Recommended Conditioning for Multilevel Spinal Fusion Rehab
 Pilates for Lumbar Spinal Fusion: Recommended Conditioning for Multilevel Spinal Fusion Rehab Maggie Curcio October 14, 2012 Summer 2012 - Chicago 1 Abstract This paper focuses on a suggested rehabilitative
Pilates for Lumbar Spinal Fusion: Recommended Conditioning for Multilevel Spinal Fusion Rehab Maggie Curcio October 14, 2012 Summer 2012 - Chicago 1 Abstract This paper focuses on a suggested rehabilitative
Double Knee to Chest. Lying on back with knees slightly bent. Hug both knees to chest
 Double Knee to Chest Lying on back with knees slightly bent Hug both knees to chest Flexion on the Gymnic Ball Lying on stomach over ball Drape body over ball and relax Roll back and forth to stretch out
Double Knee to Chest Lying on back with knees slightly bent Hug both knees to chest Flexion on the Gymnic Ball Lying on stomach over ball Drape body over ball and relax Roll back and forth to stretch out
Initial Exercises (Weeks 1-3)
 Labral Repair This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Partial weight bearing (50%) (4 weeks). Encourage, but limit hip
Labral Repair This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Partial weight bearing (50%) (4 weeks). Encourage, but limit hip
BENJAMIN G. DOMB, MD
 Physical Therapy Protocol Partial or full thickness gluteus medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Physical Therapy Protocol Partial or full thickness gluteus medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Pilates for Chronic Low Back Pain
 Pilates for Chronic Low Back Pain Julianne Bettencourt March 23, 2015 Course Year: 2014 Integrated Fitness, Visalia, CA Abstract Low back pain is an injury that affects thousands of people every day and
Pilates for Chronic Low Back Pain Julianne Bettencourt March 23, 2015 Course Year: 2014 Integrated Fitness, Visalia, CA Abstract Low back pain is an injury that affects thousands of people every day and
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Post Operative Hip Arthroscopy Procedure Form
 Post Operative Hip Arthroscopy Procedure Form Femoracetabular Impingement (FAI) Femoral Osteochondroplasty Acetabular Rim Trimming Acetabular Labrum Repair Location: o clock to o clock Debridement Articular
Post Operative Hip Arthroscopy Procedure Form Femoracetabular Impingement (FAI) Femoral Osteochondroplasty Acetabular Rim Trimming Acetabular Labrum Repair Location: o clock to o clock Debridement Articular
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) Fax: (763)
 Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
Outline. Introduction / Epidemiology. Anatomy / Pain generators. Diagnosis. Treatment. Most Important lecture!!
 Acute Low Back Pain Outline Introduction / Epidemiology. Most Important lecture!! Anatomy / Pain generators Diagnosis Treatment Course Objectives Know the RED FLAGS in history taking. Know the Pain Generators
Acute Low Back Pain Outline Introduction / Epidemiology. Most Important lecture!! Anatomy / Pain generators Diagnosis Treatment Course Objectives Know the RED FLAGS in history taking. Know the Pain Generators
2017 COS ANNUAL MEETING AND EXHIBITION HOME EXERCISES
 UPPER BODY Push Up From a push up position. Lower whole body down to floor. Press up to return to start position. Maintain abdominal hollow and neutral spinal alignment throughout movement. Note: Perform
UPPER BODY Push Up From a push up position. Lower whole body down to floor. Press up to return to start position. Maintain abdominal hollow and neutral spinal alignment throughout movement. Note: Perform
Rehabilitation of Low Back Injuries in Football Players
 Rehabilitation of Low Back Injuries in Football Players By Albi Gilmer, OCS, Cert MDT Typical Lumbar Injuries in Football Players Seen in Rehab Disc Injuries Lumbar Instability Spondylolysis and Spondylolisthesis
Rehabilitation of Low Back Injuries in Football Players By Albi Gilmer, OCS, Cert MDT Typical Lumbar Injuries in Football Players Seen in Rehab Disc Injuries Lumbar Instability Spondylolysis and Spondylolisthesis
Evidence- Based Examination of the Lumbar Spine Presented by Chad Cook, PT, PhD, MBA, FAAOMPT Practice Sessions/Skill Check- offs
 Evidence- Based Examination of the Lumbar Spine Presented by Chad Cook, PT, PhD, MBA, FAAOMPT Practice Sessions/Skill Check- offs Chapter Five: Movement Examination of the Lumbar Spine Time) (45 minutes
Evidence- Based Examination of the Lumbar Spine Presented by Chad Cook, PT, PhD, MBA, FAAOMPT Practice Sessions/Skill Check- offs Chapter Five: Movement Examination of the Lumbar Spine Time) (45 minutes
The theory and practice of getting fitter and stronger
 The theory and practice of getting fitter and stronger David Docherty, PhD, Professor Emeritus School of Exercise Science, Physical and Health Education University of Victoria All the presentations are
The theory and practice of getting fitter and stronger David Docherty, PhD, Professor Emeritus School of Exercise Science, Physical and Health Education University of Victoria All the presentations are
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Alejandro Verdugo m.d.
 Alejandro Verdugo m.d. Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Alejandro Verdugo m.d. Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Bryan T. Kelly, MD Center for Hip Pain and Preservation Hospital for Special Surgery
 Hip Arthroscopy Rehabilitation Labral refixation with or without FAI Component General Guidelines: Limited external rotation to 20 degrees (2 weeks) No hyperextension (4 weeks) Normalize gait pattern with
Hip Arthroscopy Rehabilitation Labral refixation with or without FAI Component General Guidelines: Limited external rotation to 20 degrees (2 weeks) No hyperextension (4 weeks) Normalize gait pattern with
Hip Arthroscopy Protocol
 The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
By: Sarah Van Winkle, SPT Dr. Jeff Sischo, PT, DPT, LAT, CSCS
 The Outcomes Following the Implementation of a Pelvic Floor Contraction with Lumbar Stabilization Exercises for a Patient with Low Back Pain: A Case Report By: Sarah Van Winkle, SPT Dr. Jeff Sischo, PT,
The Outcomes Following the Implementation of a Pelvic Floor Contraction with Lumbar Stabilization Exercises for a Patient with Low Back Pain: A Case Report By: Sarah Van Winkle, SPT Dr. Jeff Sischo, PT,
CORE STABILIZATION EXERCISE. Vincent J. Hudson, PhD, DPT, MBA, ATC Chief Operating Officer OAA Orthopaedic Specialists Allentown, PA
 CORE STABILIZATION EXERCISE Vincent J. Hudson, PhD, DPT, MBA, ATC Chief Operating Officer OAA Orthopaedic Specialists Allentown, PA Stepping Back What are the goals? What is the value? Is it Sport Specific
CORE STABILIZATION EXERCISE Vincent J. Hudson, PhD, DPT, MBA, ATC Chief Operating Officer OAA Orthopaedic Specialists Allentown, PA Stepping Back What are the goals? What is the value? Is it Sport Specific
Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme
 Chapter FOUR Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme Chris Higgs Cathy Chapple Daniel Pinto J. Haxby Abbott 99 n n 100 General Guidelines Knee Exercise
Chapter FOUR Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme Chris Higgs Cathy Chapple Daniel Pinto J. Haxby Abbott 99 n n 100 General Guidelines Knee Exercise
Protocol G Arthroscopic Surgery: Therapist Information
 Protocol G Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Protocol G Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Strength Essentials for Lower Back Problems. Lower Back Problems. Injury and Pain issues. Tim Keeley B.Phty, Cred.MDT, APA Principal Physiotherapist
 for Lower Back Problems Tim Keeley B.Phty, Cred.MDT, APA Principal Physiotherapist 1300 233 300 physiofitness.com.au Lower Back Problems Hyper-lordotic / kyphotic Disc Bulge and Herniation SIJ dysfunction
for Lower Back Problems Tim Keeley B.Phty, Cred.MDT, APA Principal Physiotherapist 1300 233 300 physiofitness.com.au Lower Back Problems Hyper-lordotic / kyphotic Disc Bulge and Herniation SIJ dysfunction
Functional Anatomy and Exam of the Lumbar Spine. Thomas Hunkele MPT, ATC, NASM-PES,CES Coordinator of Rehabilitation
 Functional Anatomy and Exam of the Lumbar Spine Thomas Hunkele MPT, ATC, NASM-PES,CES Coordinator of Rehabilitation Disclosure Anatomical Review Quick Review of Bony and Ligamentous structures Discal anatomy
Functional Anatomy and Exam of the Lumbar Spine Thomas Hunkele MPT, ATC, NASM-PES,CES Coordinator of Rehabilitation Disclosure Anatomical Review Quick Review of Bony and Ligamentous structures Discal anatomy
WEEKEND 1 CERVICAL SPINE
 Virginia Orthopedic Manual Physical Therapy Institute - Technique Manual WEEKEND 1 CERVICAL SPINE Cervical Active Range of Motion Testing Rotation CT Flexion Mid Cervical Flexion Extension Side-Bending
Virginia Orthopedic Manual Physical Therapy Institute - Technique Manual WEEKEND 1 CERVICAL SPINE Cervical Active Range of Motion Testing Rotation CT Flexion Mid Cervical Flexion Extension Side-Bending
Aaron Hartstein, PT, DPT, OCS, FAAOMPT A.J. Lievre, PT, DPT, OCS, CMPT
 LUMBAR SPINE CASE #2 Aaron Hartstein, PT, DPT, OCS, FAAOMPT A.J. Lievre, PT, DPT, OCS, CMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 L4-5, 5-S1 disc, facet (somatic) L4-5, 5-1
LUMBAR SPINE CASE #2 Aaron Hartstein, PT, DPT, OCS, FAAOMPT A.J. Lievre, PT, DPT, OCS, CMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 L4-5, 5-S1 disc, facet (somatic) L4-5, 5-1
Dr Schock High Tibial Osteotomy
 Dr Schock High Tibial Osteotomy Goals for phase 1 Control pain Control edema Initiate ROM and quad strengthening Maintain WB restrictions Appropriate brace wear Criteria for progression to Phase 2 Edema
Dr Schock High Tibial Osteotomy Goals for phase 1 Control pain Control edema Initiate ROM and quad strengthening Maintain WB restrictions Appropriate brace wear Criteria for progression to Phase 2 Edema
Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
Training Philosophy. There are numerous views on core conditioning.
 Abs Lab Presented by Helen Vanderburg BKin, ACE, CanFitPro, Yoga and Pilates 2005 IDEA Instructor of the Year 2006/ 1996 CanFitPro Presenter of the Year Nautilus and BOSU Fitness Education Team Introduction
Abs Lab Presented by Helen Vanderburg BKin, ACE, CanFitPro, Yoga and Pilates 2005 IDEA Instructor of the Year 2006/ 1996 CanFitPro Presenter of the Year Nautilus and BOSU Fitness Education Team Introduction
Test-retest. The therapist can perform test: retest procedures throughout the treatment session as required.
 HIP TREATMENT PROTOCOL Manual Therapy General Guidelines The goal of manual therapy: For this study, manipulative therapy includes specific manipulations (lowamplitude, high-velocity thrust techniques)
HIP TREATMENT PROTOCOL Manual Therapy General Guidelines The goal of manual therapy: For this study, manipulative therapy includes specific manipulations (lowamplitude, high-velocity thrust techniques)
3 Moves To Improve Your Lifts
 1 Each lift has three exercises outlined to help you perform at your best. Muscle strength, endurance and stability are taken into account and serves as a guide to help coordinate all of your systems.
1 Each lift has three exercises outlined to help you perform at your best. Muscle strength, endurance and stability are taken into account and serves as a guide to help coordinate all of your systems.
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES
 APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
Meniscal Repair Protocol-Dr. McClung
 Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Move Better, Feel Better: What Can Physical Therapy Do For You
 Back to Basics Move Better, Feel Better: What Can Physical Therapy Do For You Dr. Stephen Baxter, Dr. Dean Yamanuha Department of Physical Therapy and Rehabilitative Sciences 5/16/2017 Dr. Stephen Baxter
Back to Basics Move Better, Feel Better: What Can Physical Therapy Do For You Dr. Stephen Baxter, Dr. Dean Yamanuha Department of Physical Therapy and Rehabilitative Sciences 5/16/2017 Dr. Stephen Baxter
Examination of the lumbosacral spine. Dr Lucy Holtzhausen Rotorua GP CME June 2015
 Examination of the lumbosacral spine Dr Lucy Holtzhausen Rotorua GP CME June 2015 Diagnostic Algorithm Presenting symptoms Diagnostic decisions Diagnostic triage LOW BACK PAIN Mechanical NON-SPECIFIC LBP
Examination of the lumbosacral spine Dr Lucy Holtzhausen Rotorua GP CME June 2015 Diagnostic Algorithm Presenting symptoms Diagnostic decisions Diagnostic triage LOW BACK PAIN Mechanical NON-SPECIFIC LBP
Medial Collateral Ligament Repair Protocol-Dr. McClung
 Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
Session 4: Exercise Prescription for Musculoskeletal Disorders: Low Back Pain
 Session 4: Exercise Prescription for Musculoskeletal Disorders: Low Back Pain Course: Designing Exercise Prescriptions for Normal/Special Populations Presentation Created by Ken Baldwin, M.ED, ACSM-H/FI
Session 4: Exercise Prescription for Musculoskeletal Disorders: Low Back Pain Course: Designing Exercise Prescriptions for Normal/Special Populations Presentation Created by Ken Baldwin, M.ED, ACSM-H/FI
Passive Intervertebral Mobilization
 Passive Intervertebral Mobilization Terry Rose DPT, FAAOMPT, Cert, MDT Guide to Physical Therapy Practice Section 4D-Impairment/Connective Tissue Dysfunction Section 4E,4F,4G,4H,4I,4J Impaired Joint Mobility
Passive Intervertebral Mobilization Terry Rose DPT, FAAOMPT, Cert, MDT Guide to Physical Therapy Practice Section 4D-Impairment/Connective Tissue Dysfunction Section 4E,4F,4G,4H,4I,4J Impaired Joint Mobility
Movement System Impairment Syndromes Concepts Lumbar Spine Syndromes
 Movement System Impairment Syndromes Concepts Lumbar Spine Syndromes Developed by Shirley Sahrmann, PT, PhD, FAPTA Professor Emerita Washington University School of Medicine STL Program in Physical Therapy
Movement System Impairment Syndromes Concepts Lumbar Spine Syndromes Developed by Shirley Sahrmann, PT, PhD, FAPTA Professor Emerita Washington University School of Medicine STL Program in Physical Therapy
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
IFAST Assessment. Name: Date: Sport: Review Health Risk Assessment on initial consult form. List Client Goals (what brings you here?
 IFAST Assessment Name: Date: Sport: Review Health Risk Assessment on initial consult form List Client Goals (what brings you here?) Cardiovascular Measurements Blood Pressure Resting Heart Rate Body Composition
IFAST Assessment Name: Date: Sport: Review Health Risk Assessment on initial consult form List Client Goals (what brings you here?) Cardiovascular Measurements Blood Pressure Resting Heart Rate Body Composition
Anterior Cruciate Ligament (ACL) Rehabilitation
 Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation program and the
Thomas D. Rosenberg, M.D. Vernon J. Cooley, M.D. Anterior Cruciate Ligament (ACL) Rehabilitation Dear Enclosed you will find a copy of our Anterior Cruciate Ligament (ACL) Rehabilitation program and the
BENJAMIN G. DOMB, M.D.
 Arthroscopic Hip Surgery Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment. We
Arthroscopic Hip Surgery Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment. We
Dethroning the Clinical Prediction Rule WPTA Fall Conference 2017
 Course objectives 1. Understand the methodology for developing clinical prediction rules. 2. Assess clinical prediction rule methodology in prescriptive rules used in rehabilitation. 3. Discuss methods
Course objectives 1. Understand the methodology for developing clinical prediction rules. 2. Assess clinical prediction rule methodology in prescriptive rules used in rehabilitation. 3. Discuss methods
BACK SPASM. Explanation. Causes. Symptoms
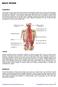 BACK SPASM Explanation A back spasm occurs when the muscles of the back involuntarily contract due to injury in the musculature of the back or inflammation in the structural spine region within the discs
BACK SPASM Explanation A back spasm occurs when the muscles of the back involuntarily contract due to injury in the musculature of the back or inflammation in the structural spine region within the discs
Physical Therapy for patients after spinal surgery with internal fixation devices.
 Physical Therapy for patients after spinal surgery with internal fixation devices www.fisiokinesiterapia.biz After spinal surgery, patients want to know when they are allowed to sit, to walk without a
Physical Therapy for patients after spinal surgery with internal fixation devices www.fisiokinesiterapia.biz After spinal surgery, patients want to know when they are allowed to sit, to walk without a
Provide movement Maintain posture/stability Generate heat
 How we move.. What do muscles do for us? Provide movement Maintain posture/stability Generate heat (skeletal muscle accounts for 40% body mass) So looking at skeletal muscles.. What do skeletal muscles
How we move.. What do muscles do for us? Provide movement Maintain posture/stability Generate heat (skeletal muscle accounts for 40% body mass) So looking at skeletal muscles.. What do skeletal muscles
Guidelines for the Trunk test for Paracanoe Athletes. Trunk test guidelines for Paracanoe
 Guidelines for the Trunk test for Paracanoe Athletes Information Please note that the purpose of the pictures is to show the position of the athlete and classifier. The classifier s job is to assess function
Guidelines for the Trunk test for Paracanoe Athletes Information Please note that the purpose of the pictures is to show the position of the athlete and classifier. The classifier s job is to assess function
Dynamic Neural Mobilization as an Adjunct Intervention for a Patient with Cervical Radiculopathy: A Case Report.
 Dynamic Neural Mobilization as an Adjunct Intervention for a Patient with Cervical Radiculopathy: A. Kara Delie, SPT Kristine Erickson, PT, MS, NCS 1 Abstract: Title: Dynamic Neural Mobilization as an
Dynamic Neural Mobilization as an Adjunct Intervention for a Patient with Cervical Radiculopathy: A. Kara Delie, SPT Kristine Erickson, PT, MS, NCS 1 Abstract: Title: Dynamic Neural Mobilization as an
Thoracolumbar Spine Conditions: Treatment and Return to Play
 Thoracolumbar Spine Conditions: Treatment and Return to Play C H R I S T O P H E R B U R K S, MD B I E N V I L L E O R T H O P A E D I C S P E C I A L I S T S O C E A N S P R I N G S, MS Thoracolumbar
Thoracolumbar Spine Conditions: Treatment and Return to Play C H R I S T O P H E R B U R K S, MD B I E N V I L L E O R T H O P A E D I C S P E C I A L I S T S O C E A N S P R I N G S, MS Thoracolumbar
Deep Inferior Epigastric Perforator Breast Flap Reconstruction Protocol:
 Deep Inferior Epigastric Perforator Breast Flap Reconstruction Protocol: DAY 5-WEEK 2: Continue home exercise program per written patient handout. Continue appropriate incision care management per MD Maintain
Deep Inferior Epigastric Perforator Breast Flap Reconstruction Protocol: DAY 5-WEEK 2: Continue home exercise program per written patient handout. Continue appropriate incision care management per MD Maintain
