Charlotte Shoulder Institute
|
|
|
- Maximilian Murphy
- 6 years ago
- Views:
Transcription
1 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC (Office) (Fax) DISCHARGE INSTRUCTIONS & PHYSICAL THERAPY INSTRUCTIONS FOR SHOULDER HEMI- OR TOTAL SHOULDER ARTHROPLASTY Initial recovery after shoulder surgery entails healing, controlling swelling and discomfort and regaining some shoulder motion. The following instructions are intended as a guide to help you achieve these goals until your 1 st postoperative visit. A. Comfort: Although surgery uses small incisions around the shoulder joint, swelling and discomfort can be present. To minimize discomfort, please do the following: 1. Ice- Ice controls swelling and discomfort by slowing down the circulation in your shoulder. Place crushed ice in cloth covered plastic bag over your shoulder for no more than 20 minutes, 3 times a day. 2. Pain Medication- Take medications as prescribed, but only as often as necessary. Avoid alcohol and driving if you are taking pain medication. 3. Sling- A sling has been provided for your comfort and should be worn as described below. 4. Driving Driving is NOT permitted as long as the sling is necessary. B. Activities: 1. You are immobilized with a sling and abductor pillow, full time, for approximately one month. Your doctor can tell you when you can discontinue use of the sling at your 1 st postoperative visit. The sling may be removed for exercises and for hygiene. 2. Your sling may be removed for gentle PASSIVE range-of-motion (PROM) exercises. (SOMEONE ELSE MOVES YOUR SHOULDER). This should be done 3x a day /15 repetitions (ABDUCTION ONLY away from your body). 1
2 3. Active range-of motion (AROM you move your shoulder) should be performed for shoulder internal/external rotation. Keep elbow positioned at the side and flexed at 90 so forearm is parallel to the floor. This should be done within a comfortable range until you feel slight pain (3x a day for 15 repetitions). You can shrug your shoulders. 4. While your sling is off you should flex and extend your elbow and wrist (3x a day for 15 repetitions) to avoid elbow stiffness. 5. Handball squeezes should be done in the sling (3x a day for 15 squeezes). 6. You may NOT move your shoulder by yourself in certain directions. NO active flexion (lifting arm up) or abduction (lifting arm away from body) until Dr. Romanowski or your therapist gives permission. These exercises must be done by someone else (Passive Range of Motion). 7. Physical therapy will begin approximately 3-4 weeks after surgery. Make an appointment with a therapist of your choice for this period of time. You will be given a prescription and instructions for therapy at your 1 st post op or 1 month visit. Please take these with you to your first therapy visit. 8. Athletic activities such as throwing, lifting, swimming, bicycling, jogging, running, and stop-and-go sports should be avoided until cleared by Dr. Romanowski. C. Wound Care: 1. Keep the dressing on, clean and dry until your 1 week post op follow up appointment. 2. Should your dressing come off, you may apply band-aids to the small incisions around your shoulder. 3. You may shower the first day after surgery with the dressings in place. 4. Bathing, swimming, and soaking should be avoided for two weeks after your surgery. D. Eating: Your first few meals after surgery should include light, easily digestible foods and plenty of liquids, as some people experience slight nausea as a temporary reaction to anesthesia. C. Call your physician if: 1. Pain persists or worsens in the first few days after surgery. 2. Excessive redness or drainage of cloudy or bloody material from the wounds. (Clear red tinted fluid and some mild drainage should be expected). Drainage of any kind 5 days after surgery should be reported to the doctor. 3. Temperature elevation greater than Pain, swelling, or redness in your arm or hand. 5. Numbness or weakness in your arm or hand. 6. Chest pain or difficulty breathing. 2
3 D. Return to the office Your first return to the office should be within the first 1-2 weeks after your surgery. Call Dr. Romanowski s office to make your first postoperative appointment. 3
4 DISCHARGE INSTRUCTIONS & PHYSICAL THERAPY INSTRUCTIONS FOR SHOULDER HEMI- OR TOTAL SHOULDER ARTHROPLASTY The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone a total shoulder arthroplasty (TSA) or hemiarthroplasty (humeral head replacement, HHR). It is not intended to be a substitute for appropriate clinical decision-making regarding the progression of a patient s postoperative course. The actual post surgical physical therapy management must be based on the surgical approach, physical exam/findings, individual progress, and/or the presence of postoperative complications. If a clinician requires assistance in the progression of a patient postsurgery, consult with the referring surgeon. Please Note: Patients with a concomitant repair of a rotator cuff tear and/or a TSA/HHR secondary to fracture or cuff arthropathy should be progressed to the next phase based on meeting the clinical criteria (not based on the postoperative time frames) as appropriate in collaboration with the referring surgeon. The given time frames are an approximate guide for progression, achieving the clinical criteria should guide the clinician and patient through this protocol. Joint Specific Outcome Measure: Upon the start of postoperative care the patient and therapist complete the Simple Shoulder Test and the American Shoulder and Elbow Surgeon s Shoulder Evaluation Short Form during their first ambulatory visit. These assessment measures are then completed every 30 days and upon discharge from physical therapy, in conjunction with routine reevaluations to assist in assessing progress. Passive Range of Motion (PROM): PROM for all patients having undergone a TSA/HHR should be defined as ROM that is provided by an external source (therapist, instructed family member, or other qualified personnel) with the intent to gain ROM without placing undue stress on either soft tissue structures and/or the surgical repair. PROM is not stretching!!!!!!! Phase I Immediate Post Surgical Phase: Goals: Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM) of shoulder; restore active range of motion (AROM) of elbow/wrist/hand Reduce pain and inflammation Reduce muscular inhibition Independent with activities of daily living (ADLs) with modifications while maintaining the integrity of the replaced joint. 4
5 Precautions: Sling should be worn continuously for 3-4 weeks While lying supine, a small pillow or towel roll should be placed behind the elbow to avoid shoulder hyperextension / anterior capsule stretch / subscapularis stretch. (When lying supine patient should be instructed to always be able to visualize their elbow. This ensures they are not extending their shoulder past neutral.) This should be maintained for 6-8 weeks post-surgically. Avoid shoulder AROM. No lifting of objects No excessive shoulder motion behind back, especially into internal rotation (IR) No excessive stretching or sudden movements (particularly external rotation (ER)) No supporting of body weight by hand on involved side Keep incision clean and dry (no soaking for 2 weeks) No driving for 3 weeks Post-Operative Day (POD) #1 (in hospital): Passive forward flexion in supine to tolerance Gentle ER in scapular plane to available PROM (as documented in operative note) usually around 30 (Attention: DO NOT produce undue stress on the anterior joint capsule, particularly with shoulder in extension) Passive IR to chest Active distal extremity exercise (elbow, wrist, hand) Pendulum exercises Frequent cryotherapy for pain, swelling, and inflammation management Patient education regarding proper positioning and joint protection techniques Early Phase I: (out of hospital) Continue above exercises Begin scapula musculature isometrics / sets (primarily retraction) Continue active elbow ROM Continue cryotherapy as much as able for pain and inflammation management Late Phase I: Continue previous exercises Continue to progress PROM as motion allows Begin assisted flexion, elevation in the plane of the scapula, ER, IR in the scapular plane Progress active distal extremity exercise to strengthening as appropriate Criteria for progression to the next phase (II): 5
6 If the patient has not reached the below ROM, forceful stretching and mobilization/manipulation is not indicated. Continue gradual ROM and gentle mobilization (i.e. Grade I oscillations), while respecting soft tissue constraints. Tolerates PROM program Has achieved at least 90 PROM forward flexion and elevation in the scapular plane. Has achieved at least 45 PROM ER in plane of scapula Has achieved at least 70 PROM IR in plane of scapula measured at 30 of abduction Phase II Early Strengthening Phase (Not to begin before 4-6 Weeks post-surgery to allow for appropriate soft tissue healing): Goals: Restore full passive ROM Gradually restore active motion Control pain and inflammation Allow continue healing of soft tissue Do not overstress healing tissue Re-establish dynamic shoulder stability Precautions: Sling should only be used for sleeping and removed gradually over the course of the next 2 weeks, for periods throughout the day. While lying supine a small pillow or towel should be placed behind the elbow to avoid shoulder hyperextension / anterior capsule stretch. In the presence of poor shoulder mechanics avoid repetitive shoulder AROM exercises/activity against gravity in standing. No heavy lifting of objects (no heavier than coffee cup) No supporting of body weight by hand on involved side No sudden jerking motions Early Phase II: Continue with PROM, active assisted range of motion (AAROM) Begin active flexion, IR, ER, elevation in the plane of the scapula pain free ROM AAROM pulleys (flexion and elevation in the plane of the scapula) as long as greater than 90 of PROM Begin shoulder sub-maximal pain-free shoulder isometrics in neutral Scapular strengthening exercises as appropriate Begin assisted horizontal adduction Progress distal extremity exercises with light resistance as appropriate Gentle glenohumeral and scapulothoracic joint mobilizations as indicated Initiate glenohumeral and scapulothoracic rhythmic stabilization 6
7 Continue use of cryotherapy for pain and inflammation. Late Phase II: Progress scapular strengthening exercises Criteria for progression to the next phase (III): If the patient has not reached the below ROM, forceful stretching and mobilization/manipulation is not indicated. Continue gradual ROM and gentle mobilization (i.e. Grade I oscillations), while respecting soft tissue constraints. Tolerates P/AAROM, isometric program Has achieved at least 140 PROM forward flexion and elevation in the scapular plane. Has achieved at least 60+ PROM ER in plane of scapula Has achieved at least 70 PROM IR in plane of scapula measured at 30 of abduction Able to actively elevate shoulder against gravity with good mechanics to 100. Phase III Moderate strengthening (Not to begin before 6 Weeks post-surgery to allow for appropriate soft tissue healing and to ensure adequate ROM): Goals: Gradual restoration of shoulder strength, power, and endurance Optimize neuromuscular control Gradual return to functional activities with involved upper extremity Precautions: No heavy lifting of objects (no heavier than 3 kg.) No sudden lifting or pushing activities No sudden jerking motions Early Phase III: Progress AROM exercise / activity as appropriate Advance PROM to stretching as appropriate Continue PROM as needed to maintain ROM Initiate assisted shoulder IR behind back stretch Resisted shoulder IR, ER in scapular plane Begin light functional activities Wean from sling completely Begin progressive supine active elevation strengthening (anterior deltoid) with light weights ( kg.) at variable degrees of elevation Late Phase III: Resisted flexion, elevation in the plane of the scapula, extension (therabands / sport cords) 7
8 Continue progressing IR, ER strengthening Progress IR stretch behind back from AAROM to AROM as ROM allows (Pay particular attention as to avoid stress on the anterior capsule.) Criteria for progression to the next phase (IV): If the patient has not reached the below ROM, forceful stretching and mobilization/manipulation is not indicated. Continue gradual ROM and gentle mobilization (i.e. Grade I oscillations), while respecting soft tissue constraints. Tolerates AA/AROM/strengthening Has achieved at least 140 AROM forward flexion and elevation in the scapular plane supine. Has achieved at least 60+ AROM ER in plane of scapula supine Has achieved at least 70 AROM IR in plane of scapula supine in 30 of abduction Able to actively elevate shoulder against gravity with good mechanics to at least 120. Note: (If above ROM are not met then patient is ready to progress if their ROM is consistent with outcomes for patients with the given underlying pathology). Phase IV Advanced strengthening phase (Not to begin before 12 Weeks to allow for appropriate soft tissue healing and to ensure adequate ROM, and initial strength): Goals: Maintain non-painful AROM Enhance functional use of upper extremity Improve muscular strength, power, and endurance Gradual return to more advanced functional activities Progress weight bearing exercises as appropriate Precautions: Avoid exercise and functional activities that put stress on the anterior capsule and surrounding structures. (Example: no combined ER and abduction above 80 of abduction.) Ensure gradual progression of strengthening Early Phase IV: Typically patient is on a home exercise program by this point to be performed 3-4 times per week. Gradually progress strengthening program Gradual return to moderately challenging functional activities. Late Phase IV (Typically 4-6 months post-op): Return to recreational hobbies, gardening, sports, golf, doubles tennis 8
9 Criteria for discharge from skilled therapy: Patient able to maintain non-painful AROM Maximized functional use of upper extremity Maximized muscular strength, power, and endurance Patient has returned to advanced functional activitie 9
TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY
 Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
PROM is not stretching!
 Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Total Shoulder Arthroplasty / Hemiarthroplasty Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol
 Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty
 Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Total Shoulder Rehab Protocol Dr. Payne
 Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Orthopedic Surgery and Sports Medicine FL License:
 Reverse Shoulder Arthroplasty Protocol: The intent of this protocol is to provide the therapist with a guideline for the post-operative rehabilitation course of a patient that has undergone a Reverse Shoulder
Reverse Shoulder Arthroplasty Protocol: The intent of this protocol is to provide the therapist with a guideline for the post-operative rehabilitation course of a patient that has undergone a Reverse Shoulder
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Christopher K. Jones, MD Colorado Springs Orthopaedic Group
 Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Rehab protocol. Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits. Goals:
 Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY
 TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY Philosophy The following is an outline of the standard post-operative rehabilitation program following total shoulder arthroplasty.
TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY Philosophy The following is an outline of the standard post-operative rehabilitation program following total shoulder arthroplasty.
WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C
 WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C Post-Operative Rehabilitation Guidelines for Total Shoulder Arthroplasty (TSA) The intent of this protocol is to provide the physical therapist with a guideline/treatment
WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C Post-Operative Rehabilitation Guidelines for Total Shoulder Arthroplasty (TSA) The intent of this protocol is to provide the physical therapist with a guideline/treatment
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
DISCHARGE INSTRUCTIONS & PHYSICAL THERAPY PROTOCOL: Arthroscopic Rotator Cuff Repair With or Without Biceps Tenodesis
 DISCHARGE INSTRUCTIONS & PHYSICAL THERAPY PROTOCOL: Arthroscopic Rotator Cuff Repair With or Without Biceps Tenodesis Initial recovery after shoulder surgery entails healing, controlling swelling and discomfort
DISCHARGE INSTRUCTIONS & PHYSICAL THERAPY PROTOCOL: Arthroscopic Rotator Cuff Repair With or Without Biceps Tenodesis Initial recovery after shoulder surgery entails healing, controlling swelling and discomfort
REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL Shoulder
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Reverse Total Shoulder Protocol
 Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) REHABILITATION AFTER REVERSE SHOULDER ARTHROPLASTY
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Jennifer L. Cook, MD Stephen A. Hanff, MD. Rotator Cuff Type I Repair (Small Large Tear)
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD
 General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
(PROTOCOL #18) REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
 The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
Arthroscopic Rotator Cuff Repair Protocol:
 Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
DISCHARGE INSTRUCTIONS & PHYSICAL THERAPY PROTOCOL: Biceps Tenodesis
 DISCHARGE INSTRUCTIONS & PHYSICAL THERAPY PROTOCOL: Biceps Tenodesis Initial recovery after shoulder surgery entails healing, controlling swelling and discomfort and regaining some shoulder motion. The
DISCHARGE INSTRUCTIONS & PHYSICAL THERAPY PROTOCOL: Biceps Tenodesis Initial recovery after shoulder surgery entails healing, controlling swelling and discomfort and regaining some shoulder motion. The
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
AC reconstruction Protocol: Dr. Rolf
 AC reconstruction Protocol: Dr. Rolf The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient that has undergone a AC reconstruction
AC reconstruction Protocol: Dr. Rolf The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient that has undergone a AC reconstruction
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Rehabilitation following Arthroscopic Rotator Cuff Repair: Medium Tears Phase I: Immediate Postsurgical Phase (Days 10-14) Precautions: No lifting of objects; No excessive arm motions; No excessive external
Rehabilitation following Arthroscopic Rotator Cuff Repair: Medium Tears Phase I: Immediate Postsurgical Phase (Days 10-14) Precautions: No lifting of objects; No excessive arm motions; No excessive external
Biceps Tenodesis Protocol
 Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Biceps Tenotomy Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
TALLGRASS ORTHOPEDIC & SPORTS MEDICINE. Phase I Immediate Post-Surgical Phase (Weeks 0-2) Date: Maintain/protect integrity of the repair
 TALLGRASS ORTHOPEDIC & SPORTS MEDICINE Name: Date of Surgery: Patient Flow Sheet Arthroscopic Rotator Cuff Repair Small to Medium Tears Benedict Figuerres, MD Phase I Immediate Post-Surgical Phase (Weeks
TALLGRASS ORTHOPEDIC & SPORTS MEDICINE Name: Date of Surgery: Patient Flow Sheet Arthroscopic Rotator Cuff Repair Small to Medium Tears Benedict Figuerres, MD Phase I Immediate Post-Surgical Phase (Weeks
Biceps Tenotomy Protocol
 Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
Biceps Tenodesis Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Anterior Stabilization of the Shoulder: Distal Tibial Allograft
 Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
James R. Romanowski, M.D.
 James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery. Phase 1: Immediate postoperative period (weeks 0-6) Goals
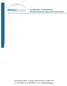 The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery Phase 1: Immediate postoperative period (weeks 0-6) Maintain/protect integrity of repair Gradually increase PROM Diminish
The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery Phase 1: Immediate postoperative period (weeks 0-6) Maintain/protect integrity of repair Gradually increase PROM Diminish
Reverse Total Shoulder
 Rehabilitation Protocol: Reverse Total Shoulder Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Reverse Total Shoulder Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Latissimus dorsi tendon transfer protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the physical therapist with a guideline/treatment protocol for the postoperative rehabilitation management
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the physical therapist with a guideline/treatment protocol for the postoperative rehabilitation management
Rotator Cuff Repair +/- Acromioplasty/Mumford. Phase I: 0 to 2 weeks after surgery
 Rotator Cuff Repair +/- Acromioplasty/Mumford 2. Ensure wound healing Phase I: 0 to 2 weeks after surgery 1. Sling: Use your sling all of the time. 2. Use of the affected arm: You may use your hand on
Rotator Cuff Repair +/- Acromioplasty/Mumford 2. Ensure wound healing Phase I: 0 to 2 weeks after surgery 1. Sling: Use your sling all of the time. 2. Use of the affected arm: You may use your hand on
Progression to the next phase based on Clinic Criteria and or Time Frames as Appropriate
 Bicep Tenodesis D. WATTS, M.D. Progression to the next phase based on Clinic Criteria and or Time Frames as Appropriate PHASE I PASSIVE RANG OF MOTION PHASE (STARTS APPROXIMATELY POST OP WEEKS 1-2) Minimize
Bicep Tenodesis D. WATTS, M.D. Progression to the next phase based on Clinic Criteria and or Time Frames as Appropriate PHASE I PASSIVE RANG OF MOTION PHASE (STARTS APPROXIMATELY POST OP WEEKS 1-2) Minimize
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft
 Day of Surgery Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft A. Relax. Diet as tolerated. B. Icing is important for the first 5-7 days post-op. While the post-op
Day of Surgery Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft A. Relax. Diet as tolerated. B. Icing is important for the first 5-7 days post-op. While the post-op
Shoulder Arthroscopy: Postop Instructions. Activites & Advice for in the Hospital and while at Home
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol:
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol: General Information:
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol: General Information:
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm)
 Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm) Therapist Phone I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity
Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm) Therapist Phone I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 1 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 1 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol. Phase 1 Maximum Protection (0-4 weeks)
 Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol Goals for phase 1 Minimize Pain and inflammation Protect integrity of repair Initiate shoulder PROM Reduce muscular inhibition Maintain AROM of elbow,
Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol Goals for phase 1 Minimize Pain and inflammation Protect integrity of repair Initiate shoulder PROM Reduce muscular inhibition Maintain AROM of elbow,
Shoulder Arthroscopy with Posterior Labral Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Rehabilitation Protocol: Massive Rotator Cuff Tear Repair
 Rehabilitation Protocol: Massive Rotator Cuff Tear Repair Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey
Rehabilitation Protocol: Massive Rotator Cuff Tear Repair Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey
SHOULDER ARTHROSCOPY WITH ANTERIOR STABILIZATION / CAPSULORRHAPHY REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
James R. Romanowski, M.D.
 James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
Total Shoulder Arthroplasty
 1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Latarjet Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
Type II SLAP lesions are created when the biceps anchor has pulled away from the glenoid attachment.
 Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Phase I: 0 to 3 weeks after surgery
 Dx: Right Left RTC (Massive) Repair Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: 2. Ensure wound healing Phase I:
Dx: Right Left RTC (Massive) Repair Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: 2. Ensure wound healing Phase I:
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL BENJAMIN J. DAVIS, MD Type Two Rotator Cuff Repair
 I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity of the Repair Gradually Increase Passive Range of Motion Diminish Pain and Inflammation Prevent Muscular Inhibition Passive
I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity of the Repair Gradually Increase Passive Range of Motion Diminish Pain and Inflammation Prevent Muscular Inhibition Passive
Limited Goals Program (Examples Include: Cuff Tear Arthropathy, Massive Irrepairable Rotator Cuff Tear, Selected Revision Surgeries)
 Limited Goals Program (Examples Include: Cuff Tear Arthropathy, Massive Irrepairable Rotator Cuff Tear, Selected Revision Surgeries) All information contained in this protocol is to be used as general
Limited Goals Program (Examples Include: Cuff Tear Arthropathy, Massive Irrepairable Rotator Cuff Tear, Selected Revision Surgeries) All information contained in this protocol is to be used as general
Progression to the next phase based on clinical criteria and time frames as appropriate
 Indications Reverse total shoulder replacement is indicated for use in grossly rotator cuff deficient joints with severe arthropathy, or for use when a previous joint replacement has failed with a grossly
Indications Reverse total shoulder replacement is indicated for use in grossly rotator cuff deficient joints with severe arthropathy, or for use when a previous joint replacement has failed with a grossly
Important rehabilitation management concepts to consider for a postoperative physical therapy RSA program are:
 : General Information: Reverse or Inverse Shoulder Arthroplasty (RSA) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff damage,
: General Information: Reverse or Inverse Shoulder Arthroplasty (RSA) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff damage,
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline
 Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMIAL DECOMPRESSION) Dr. Carson
 REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMIAL DECOMPRESSION) Dr. Carson The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMIAL DECOMPRESSION) Dr. Carson The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
SHOULDER RESURFACING
 MGH Sports Medicine Center 175 Cambridge St., 4th floor Boston, MA 02114 http://orthodoc.aaos.org/mdprice SHOULDER RESURFACING The shoulder is a ball and socket joint that enables you to raise, twist,
MGH Sports Medicine Center 175 Cambridge St., 4th floor Boston, MA 02114 http://orthodoc.aaos.org/mdprice SHOULDER RESURFACING The shoulder is a ball and socket joint that enables you to raise, twist,
Arthroscopic Anterior Stabilization Rehab
 Arthroscopic Anterior Stabilization Rehab Phase I (0-3weeks) Sling immobilization-md directed Codmans/Pendulum exercises Wrist/Elbow ROM Gripping exercises FF-AAROM (supine)-limit to 90 o ER to 0 o Sub
Arthroscopic Anterior Stabilization Rehab Phase I (0-3weeks) Sling immobilization-md directed Codmans/Pendulum exercises Wrist/Elbow ROM Gripping exercises FF-AAROM (supine)-limit to 90 o ER to 0 o Sub
Mini Open Rotator Cuff Repair Small Tears < 1 cm
 Mini Open Rotator Cuff Repair Small Tears < 1 cm **It is the treating therapist s responsibility along with the referring physician s guidance to determine the actual progression of the patient within
Mini Open Rotator Cuff Repair Small Tears < 1 cm **It is the treating therapist s responsibility along with the referring physician s guidance to determine the actual progression of the patient within
Shoulder Arthroscopy with Rotator Cuff Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Anterior Labrum Repair Protocol
 Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
REGENETEN Bioinductive Implant. Rehabilitation Protocol. for REGENETEN partial thickness tears without repair
 REGENETEN Bioinductive Implant Rehabilitation Protocol for REGENETEN partial thickness tears without repair Let s get you back to YOU. We must emphasize that this protocol is recommended ONLY for partial
REGENETEN Bioinductive Implant Rehabilitation Protocol for REGENETEN partial thickness tears without repair Let s get you back to YOU. We must emphasize that this protocol is recommended ONLY for partial
REVERSE SHOULDER ARTHROPLASTY
 William J. Robertson, MD TMI Sports Medicine 3533 Matlock Rd Arlington, TX 76015 Office: (817) 419-0303 Fax: (817) 468-5963 www.billrobertsonmd.com www.hipkneepreservation.com REVERSE SHOULDER ARTHROPLASTY
William J. Robertson, MD TMI Sports Medicine 3533 Matlock Rd Arlington, TX 76015 Office: (817) 419-0303 Fax: (817) 468-5963 www.billrobertsonmd.com www.hipkneepreservation.com REVERSE SHOULDER ARTHROPLASTY
Rotator Cuff Repair Therapy Protocol
 Bart Eastwood D.O. 825 Davis st Blacksburg, VA 24060 540-951-6000 All information contained in this protocol is to be used as general guidelines only. Specific variations may be appropriate for each patient
Bart Eastwood D.O. 825 Davis st Blacksburg, VA 24060 540-951-6000 All information contained in this protocol is to be used as general guidelines only. Specific variations may be appropriate for each patient
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer
 Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
ROTATOR CUFF REPAIR REHAB PROTOCOL
 Jayesh K. Patel, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX 75701 (903) 510-8840 ROTATOR CUFF REPAIR REHAB PROTOCOL This rehabilitation protocol has been developed for
Jayesh K. Patel, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX 75701 (903) 510-8840 ROTATOR CUFF REPAIR REHAB PROTOCOL This rehabilitation protocol has been developed for
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) Arthroscopic Posterior Labral Repair
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Arthroscopic
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Arthroscopic
Diagnosis: s/p ( LEFT / RIGHT ) AC Joint Reconstruction -- Surgery Date:
 UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
No Financial Disclosures
 Rehabilitation Following Total and Reverse Shoulder Arthroplasty, PT, DPT, SCS, CSCS No Financial Disclosures Total Shoulder Arthroplasty Arthritic shoulder increasing in prevalence More active as we age
Rehabilitation Following Total and Reverse Shoulder Arthroplasty, PT, DPT, SCS, CSCS No Financial Disclosures Total Shoulder Arthroplasty Arthritic shoulder increasing in prevalence More active as we age
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines
 Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
REHABILITATION FOLLOWING OPEN AND MINI-OPEN ROTATOR CUFF REPAIR
 REHABILITATION FOLLOWING OPEN AND MINI-OPEN ROTATOR CUFF REPAIR Post-Operative Physical Therapy Protocol Philip A. Davidson M.D. Phase I Immediate Post-Surgical Phase (Week 1-2) Maintain integrity of the
REHABILITATION FOLLOWING OPEN AND MINI-OPEN ROTATOR CUFF REPAIR Post-Operative Physical Therapy Protocol Philip A. Davidson M.D. Phase I Immediate Post-Surgical Phase (Week 1-2) Maintain integrity of the
Superior Labrum Repair Protocol - SLAP
 Superior Labrum Repair Protocol - SLAP Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain
Superior Labrum Repair Protocol - SLAP Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain
Mini Open Rotator Cuff Repair Large (3 5 cm)
 Mini Open Rotator Cuff Repair Large (3 5 cm) Size: small = < 1 cm, medium = 1 3 cm, large 3 5 cm, massive = > 5 cm **It is the treating therapist s responsibility along with the referring physician s guidance
Mini Open Rotator Cuff Repair Large (3 5 cm) Size: small = < 1 cm, medium = 1 3 cm, large 3 5 cm, massive = > 5 cm **It is the treating therapist s responsibility along with the referring physician s guidance
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Overview a. Begin passive shoulder ROM after surgery (beginning week 1) b. Active assist ROM beginning week 7 after surgery (weeks 7-8) c. Active ROM beginning week 9 after
Rotator Cuff Repair Protocol Overview a. Begin passive shoulder ROM after surgery (beginning week 1) b. Active assist ROM beginning week 7 after surgery (weeks 7-8) c. Active ROM beginning week 9 after
Rehabilitation Guidelines for Large Rotator Cuff Repair
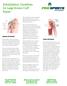 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Rotator Cuff Tears The shoulder is a ball and socket joint
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Rotator Cuff Tears The shoulder is a ball and socket joint
Small Rotator Cuff Repair
 Small Rotator Cuff Repair 1. Defined a. Surgical repair of the rotator cuff (most commonly supraspinatus muscle) utilizing sutures b. May be done arthroscopically or open. c. May be done in conjunction
Small Rotator Cuff Repair 1. Defined a. Surgical repair of the rotator cuff (most commonly supraspinatus muscle) utilizing sutures b. May be done arthroscopically or open. c. May be done in conjunction
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are
Rotator Cuff Repair Protocol
 Protocol This rehabilitation protocol has been developed for the patient following a rotator cuff surgical procedure. This protocol will vary in length and aggressiveness depending on factors such as:
Protocol This rehabilitation protocol has been developed for the patient following a rotator cuff surgical procedure. This protocol will vary in length and aggressiveness depending on factors such as:
Large/Massive Rotator Cuff Repair
 Large/Massive Rotator Cuff Repair 1. Defined a. Suturing of tears within the rotator cuff (most commonly supraspinatus muscle). Massive RCR usually involve more than the supraspinatus. b. May be done arthroscopically
Large/Massive Rotator Cuff Repair 1. Defined a. Suturing of tears within the rotator cuff (most commonly supraspinatus muscle). Massive RCR usually involve more than the supraspinatus. b. May be done arthroscopically
 Appendix A: The American Society Of Shoulder And Elbow Therapists Arthroscopic Rotator Cuff Repair Rehabilitation Guide Phase 1 (POD 1 to ~ POW 6) GOALS: Maintain integrity of repair Minimize pain and
Appendix A: The American Society Of Shoulder And Elbow Therapists Arthroscopic Rotator Cuff Repair Rehabilitation Guide Phase 1 (POD 1 to ~ POW 6) GOALS: Maintain integrity of repair Minimize pain and
Pectorlais Major Tendon Repair
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Pectorlais Major Tendon Repair The pectoralis major muscle
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Pectorlais Major Tendon Repair The pectoralis major muscle
Reverse Total Shoulder Rehabilitation Protocol
 Reverse Total Shoulder Rehabilitation Protocol The Reverse Ball and Socket Arthroplasty is a new implant design for severely damaged shoulders. It is generally used for rotator cuff tear arthropathy, and
Reverse Total Shoulder Rehabilitation Protocol The Reverse Ball and Socket Arthroplasty is a new implant design for severely damaged shoulders. It is generally used for rotator cuff tear arthropathy, and
