Breathing, voice and speech
|
|
|
- Barbra Gallagher
- 6 years ago
- Views:
Transcription
1 1) Goal Set a goal for the patient (if possible together with the patient) that can be reached within the nearest future one or two weeks. The goal should be concrete and measurable. 2a) Activity If possible the intervention should always be related to a context from every-day life or end up with an activity related to breathing or voice productions The activity must be: Related to the goal Known and meaningful for the patient 2b) Environmental factors General principles for selection of environmental factors: They should be adapted to the patient and the task enabling the patient to reach the goal They should support the patient to use the affected side of the body and move as normal as possible and if relevant expand the patients movements repertoire Furniture/objects/aids should make the activity possible to complete and make the patient able to learn new movements and movement patterns They should be arranged in a way so the patient has to use more normal ways (often also with support of the therapist) instead of using already established habits that are not very supportive 2b1) Adapt location: for choosing location: A known place: Can provide confidence and safety to the patient that don t respond very well in new situations A unknown place: Can expand the patients repertoire and limit the use of old habits obstructing learning and normal movements In a niche (e.g. the patient are positioned in a corner against a wall or lying/sitting on the floor): The patient has perceptive or senso-motorical problems, disturbed bodyscheme, disturbed balance, or reduced attention to the affected side Out in the room: Patient that do not have the problems mentioned above and you may need to be able to move freely around the patient or have a plank bed or couch behind the patient A location where the patient are alone or shielded: To patients who easily becomes distracted, needs a lot and/or individual support Group situations: Can be selected if it is part of the treatment that the patient is acting and reacting in verbally in a social context, for example a cooking group or singing group 1
2 2b1) Adapt furniture s: The furniture can be essential to support and encourage a good position and postural control. They should support the patient to move selectively and normally during the treatment. Moreover they should give sufficiently support to enable the patient to sit upright against gravity, and to move actively carrying out the activity. If the furniture supports the patient too much the patient can become or remain passive. A secure active position will support the patient to achieve new experiences in movement and tactile input in relation to the body scheme and the activity (treatment) Example: The therapist work with the patient's ability to keep a tone in a standing position. To do that the patient needs sustained support to the more affected side of the body and therefore there should be a plank bed beside him, which is adjusted individually in the appropriate height 2b1) Adapt objects: Each object has to improve normal and active movements and movement-patterns Examples: You can choose confetti that the patient blows off his hand. For patients with better strength, you can choose a whistle. The patient should not compensate with associated reactions and / or mass movements. The patient should blow bubbles in water through a straw 2b1) Use of aids if: The movement is not possible for the patient; maybe because of an amputated arm They can support a movement to become more selective and make it possible for the patient to involve the affected side of the body They can support that the patient perform the activity or movement more normally Example: The patient gets a Pacing board to be reminded to speak slowly and him easier to understand in everyday life/conversation 2c) Therapeutic intervention 2.c.1. Working Level of support for breathing / voice and speech 1. Support for breathing When the patient is unable to produce sounds / voice or if he occasionally (eg. By position change when he is spoken to) spontaneously groan / moan or produce sounds (but not constant) When the patient has a rattle breathing When the patient's breathing pattern is not normal, for example if it is superficial has abnormal rhythm and frequency When there is an abnormal coordination between swallowing and breathing 2. Support for breathing and voice-coordination 2
3 When the patient's breathing pattern is not normal, for example if it is superficial has abnormal rhythm and frequency When the patient can t keep a tone longer than seconds When there is not a clear start and stop in voice in connection with the expirationphase When the patient can not adjust the pitch and volume of the voice When the patient has a rattle breathing When the patient produces voice during the inspiration phase 3. Support for breathing voice and speech When the patient can t keep a tone longer than seconds When there is not a clear start and stop in voice in connection with the expirationphase When the patient can not adjust the pitch and volume of the voice When the patient has a rattle breathing When the patient produces voice during the inspiration phase When the patient finds it difficult to coordinate the breathing, voice and articulation, e.g. he has an unclear speech, has difficulties with some sounds, he does not always has voice on the speech 2.c.3. Terapeutisk intervention Move and position Definition: All body parts (chest, pelvis, shoulders, head and neck and extremities) are put in an appropriate position towards each other, the surface, gravity and the activity. All starting positions should be without resistance, pain for the patient and safe (without risk of falling, aspiration or obstruction of the patients airway e.g. by pillow on the face or tube. It can be necessary to mobilize or guide the patient before positioning, because some neuromuscular, musculoskeletal and/or perceptive and cognitive problems makes it impossible or limits the possibility to bring the patient in a certain position. Purpose: Regulate the tonus Create a basis for selective movements in the facial-oral tract area to patients with reduced postural control of when to use of this method: Mal-alignment due to change in tonus Reduced postural control (senso-motorical problems) Perceptual problems Lack of selective movements in the facial-oral area for evaluating the patients' response: Signs of a too high a starting position: The patient's tone rises inappropriate in one or more muscles / muscle-groups 3
4 The emergence of many associated reactions when he tries to move Vegetative reactions: sweat, blood pressure and / or oxygen saturation in the blood falls, breathing rate increases The patient is unconcentrated, facial expression/movements seems tense, the patient seems worried The patient has difficulty in performing movements which he can perform in a lower position Signs of a too low starting position: The patients arousal falls The patient masters the task and moves spontaneous and selective The patient has no need of assistance The patient seems unconcentrated, because you are not working at his level, the "challenges" to his functionality is too low Mobilization: Definition: Moving body parts and / or structures which do not have full range of movement Purpose: To achieve greater range of movement (ROM), more normal tone, better proprioception, improve alignment for use of this method: Primarily when the patient has senso-motorical problems which gives a resistance or decreased ROM in a movement or an activity Mal-alignment because: Hyper / or hypo-tonus, ataxia, rigidity Reduce ROM (due to: ossification, hyper tone, condition after fracture, etc.). Abnormal sensitivity Impaired proprioception for evaluating the patients' response: Signs that mobilization has positive effects on the patient's problem: A movement becomes possible, easier ROM is increased Better alignment The patient can better feel the mobilized body part / or uses it The patient can move actively Signs that the mobilization does not have the desired effect on the patient's problem: The patient shows signs of pain No change or worsening in Rom, alignment and the possibility of moving No change in sensitivity or proprioception 4
5 Guiding: Definition: The therapist supports the patient's normal movement / movement patterns in an activity Purpose: Bringing the patient into contact with the surroundings and forming hypothesis and problemsolving processes. Moreover to perform movements that he cannot do by himself. for use of this method: The patient cannot perform a movement or an activity because of perceptive, sensomotorical or cognitive problems The patient performs the movement / activity, but only in stereotypical movement patterns without variation or only by using the non-affected body part / limb for evaluating the patients' response: Signs that guiding has positive effect on the patient's problem: The patient becomes aware of the activity or the movement The patient takes over the movement and / or pursuing the next action steps The patient can initiate and repeat the guided movement independently The Patients tone normalizes The patient's motor behavior is changes Signs that guiding does not have the desired effect on the patient's problem: The patient is not attentive towards the activity or movement Patients tension rises The patient becomes restless There is no change in behavior Facilitation: Definition: Facilitation is a technique where you most often through manual contact activate the sensory and proprioceptive afferent system. Facilitation is an active learning process that helps a person to overcome inertia, initiate, to continue and complete functional tasks. Facilitation is never passive. The therapist can choose to facilitate the patient at all times to either maintain postural control and / or perform selective movements in tasks and activities in the facial-oral tract area. The location, direction of and intensity of facilitation may vary. Purpose: Makes an activity possible, change motor behavior and ease movements for using which level: 1. All the time 5
6 The patient loses postural control at the moment the therapist takes "hands off" The patient doesn t have the idea or ability to use the movements or to initiate, conduct and/or complete a movement or activity Selective movements become mass movements The patient has associated reactions The quality of the movements becomes worse when therapeutic take "hands off" 2. Partly / in between movements, movement patterns or activities The patient can retain postural control and will not lose it over a shorter period The patient begins to take over, initiate or terminate a movement / action / activity spontaneously with sufficient quantity and quality 3. To initiate movements, functions, activities (i.e. only in the beginning) The patient has adequate postural control and can take over and complete a movement / function / activity / task The patient can move spontaneously, selective in the facial-oral tract area and can achieve the goal in the required quantity and quality for evaluating patient response: Signs that facilitation has a positive effects: Change of motor behavior (the patient becomes active and the movement becomes easier) Signs that facilitation don t have the desired effect: The patients tonus increases Motor behavior did not changed The patient is passive Elicit (produce) Definition: Elicit means to generate a response or reaction from the patient by, for example the therapist acts as a visual model, instead of encouraging the patient directly to perform the activity or movement. Objective: To induce a movement / function / activity for use of the method: The patient has no language understanding The patients tonus increases when he tries to follow the verbal requests and there are associated reactions The patient has trouble understanding the situation for evaluating patient response: Signs of eliciting has the desired effect The patient is active and performs the desired movement / function / activity 6
7 Signs of eliciting don t have the desired effect The patient tonus increases The patient does not respond or respond differently than expected 2.c.3 Working with the position and movement 1. In lying position The patient is motorical restless and / or vegetative unstable The patient has almost non or no postural control The patient may / may not move of medical reasons, for example fractures etc Lying in combination with movements The patient has almost non or no postural control The patient has a high tension in the neural structures, abnormal muscle tone, disturbed body scheme The patient is immobile / has no ability o move on his own The patient needs a "signal" that helps him to start / stop to produce sounds, this signal can be given in the form of movement (facilitated or independent) The patient has difficulty in coordinating breathing / voice / articulation and controlled movements in a starting positions with little surface 3. Sitting The patient cannot coordinate breathing / voice and articulation with movements in a starting position with little surface The patient has trouble breathing in the lying position (eg. Because of: Obesity, general hypo-tonus, heart disease, pneumonia...) Sitting position promotes postural control and / or patient's arousal Seated position promotes more normal breathing parameters (such as rhythm, frequency, location of breathing movements), voice and articulation The patient's ability to keep a tone is better in sitting than in lying position 4. Sitting in combination with movements The patient cannot coordinate breathing / voice and articulation with movements in a starting position with little surface The patient has trouble breathing in the lying position (eg. Because of: Obesity, general hypo-tonus, heart disease, pneumonia...) Sitting position promotes postural control and / or patient's arousal Seated position promotes more normal breathing parameters (such as rhythm, frequency, location of breathing movements), voice and articulation The patient can be facilitated to breathing / voice / articulation in coordination with movements, in a higher starting position 7
8 Seated position promotes more normal breathing parameters (such as rhythm, frequency, location of breathing movements), voice and articulation The patient's ability to keep a tone is better in sitting than in lying position 5. Standing The patient cannot coordinate breathing / voice and articulation with movements in positions with little surface The patient has breathing difficultis in lying or sitting (e.g. because Obesity, general hypotonus, heart disease, pneumonia) Standing position promotes postural control and / or the patient's arousal Standing position promotes more normal breathing parameters (such as rhythm, frequency, location of breathing movements), voice and articulation The patient can be facilitated to breathing / voice / articulation in coordination with movements, in a higher starting position The patient's ability to keep a tone are better than in sitting and lying position The patient's postural control is sufficient enough that he can coordinate or be facilitated by the therapist to coordinate breathing, voice / articulation in a high starting position The patient has difficulty talking when walking 6. Standing in combination with movements The patient cannot coordinate breathing / voice and articulation with movements in positions with little surface The patient has breathing difficultis in lying or sitting (e.g. because Obesity, general hypotonus, heart disease, pneumonia) Standing position promotes postural control and / or the patient's arousal Standing position promotes more normal breathing parameters (such as rhythm, frequency, location of breathing movements), voice and articulation The patient can be facilitated to breathing / voice / articulation in coordination with movements, in a higher starting position The patient's ability to keep a tone are better than in sitting and lying position The patient's postural control is sufficient enough that he can coordinate or be facilitated by the therapist to coordinate breathing, voice / articulation in a high starting position The patient has difficulty talking when walking The patient needs a "signal" that helps him to start / stop to produce sounds, this signal can be given in the form of movements (facilitated or independently) 2.c.5 Therapeutic support for the protection of airway The patient during treatment shows signs of penetration / aspiration and silent aspiration shown by rattle sounds in breathing, coughing, and clearing the throat 8
9 It should be noted that there is no specific way to train to cough or clear the throat Support for coughing When the patient coughs ineffectively (weak cough, extension pattern, lack of clearing swallowing) Can be supported using the following options: Bringing the patient forward Supporting ribs costal and sternum (possible the stomach) Avoid the patient ingest food or drink before making sure that he has free breathing Facilitate clearing swallow or spitting out Support the patient to clear the throat when: The patient has an ineffectively clearing of the throat The patient has a wet voice and does not respond to it by clearing the throat (slight coughing) Can be supported using the following options: Bringing the patient forward Support the costal and sternum (possibly the stomach) Avoid the patient ingest food or drink before making sure that he has free breathing Facilitate clearing swallow or spitting out The therapist acts as a "model" doing by demonstrating how to clearing the throat possibly together with vibrating on the patient's sternum to force expiration Support clearing swallow The patient has coughed, cleared the throat or eats without using a secondary clearing swallow Clearing swallows comes very late or is ineffective Can be supported using the following options: Stabilizing the jaw Providing tactile support to swallowing by the floor of the mouth Moving the patient Force the expiration and / or prolong the expiration phase (time) Support the use of the voice The patient shows clinical signs of penetration of saliva or food / drink. Can be facilitated or elicited by: Vibration or pressure at the ribs or sternum Maybe by support at the stomach The therapist can demonstrate how the patient should do by using own voice or try to 9
10 produce or induce a comment or an answer from the patient that is related to the context Support to cleaning the mouth The patient has residues or bits of food / drink in the mouth and does not have the senso-motorical ability to remove it. Can be supported by: Support the patient to feel the residue and swallow them or spit them out If the patient cannot be activated to swallow or spit out, the therapists removes material with gauze on the finger Support the patient to collect the remains with the tongue and either transport it to swallow or spit it out If the patient cannot be activated to collect remains of the tongue or spit out, the therapists remove material with gauze on your finger If secretions or mucus is so viscous or as large a quantity that it is inappropriate to swallow it should also be removed with gauze In special cases, it is recommended that the material is sucked out with a tube by a nurse, for example after vomiting. Support 'to come forward' It will prevent the patient from aspiration in the a treatment or eating situation or when the patient already has aspirated/penetrated Moving/leaning forward is part of the physiological protection mechanisms during normal eating and in case aspiration / penetration. Patients with extension-pattern or lack of postural control who has lost the ability to come forward. This applies to both lying, sitting and standing positions. 3. Evaluation The treatment should be evaluated by the nature of the patient's response. By answering the question: Does the patient perform the activity in a more normal way / in better quality? The question can be answered with yes or no. Whatever the answer, the therapist must adjust the treatment immediately. When adapting the treatment the therapist must always remember to change only one parameter at a time to evaluate what action is causing the effect. Even if you have a plan and the patient reacts unexpected, with e.g. pain, vomiting, then it is important to respond to patient needs and not continue the intervention. 4a. If the answer is YES, you have three options: Give less support (Important is only to change one element at a time in order to be able to evaluate the patients responds and let the patient repeat the same task) Increase requirements / the scope of the activity with use of the same level of support and see how the patient responds 10
11 Set a new goal in the same or another F.O.T.T. area NOTE: The quality or quantity parameters should not be exacerbated so there appear associated reactions or mass movements when reducing the support General principles of how to increase the demands and give less support: Level of the activity: Include more sub-actions / elements Increase the requirements to selectivity, normal movement, ROM It shall be carried out faster, over a longer time, with more repetitions of one or several elements Level of the surroundings: Room and location should be more normal and not be individually adapted The activity should be in another context that is new to the patient Surroundings should change, there should be more stimuli, sounds, and presence of other persons etc No special objects No aids Level of therapeutic support: The patient is facilitated on a lower level, for example. only partial instead of constant The therapist chooses to bring the patient in a higher starting position or decrease the support in the position he already has 4.a If you answer NO, then you have three options: To change the activity so that it demands less of the patient Give more support, this may also imply that the therapist changes approach because the patient cannot use the information / help he has received so far (e.g.: the therapist uses guiding instead of facilitation) Set a new goal, because the goal was chosen proves to be too high / unrealistic or the patient's needs have suddenly changed General principles of how to reduce demands and provide greater support: Level of the activity: Include fewer sub-actions / elements Reduce the requirements to selectivity, normal movement, ROM It shall be carried out more slowly, over a shorter time, with fewer repetitions Choose a more familiar task Level of the surroundings: 11
12 Room and location will be individually (more) adapted The activity will be performed in another, more recognizable / familiar context to the patient The patient must perform the task in a room with fewer stimuli, without the presence of other persons The furniture will be adapted to support the patient more use special items Use aids Level of the therapeutic support: The patient is facilitated on a higher level, for example. constant instead of only partial The therapist chooses to bring the patient in a lower starting position or increase the support in the position he already has (e.g. supporting both head with jaw control grip and also the patient's trunk) 4 b) Improvement? After having launched new / changed actions, you need to evaluate again the patient's response and re-adjust the treatment depending on the patient's response, with either more or less support. This process continues until this treatment-intervention is over. 5) Evaluation of the goal When the intervention is over you evaluate whether the goal for treatment has been reached and if you wish to work with this goal in further treatment sessions. At the same time you can establish a strategy for the next treatment with basis in the techniques, methods which have proved to be appropriate for the patient in this intervention. 12
Looking after your lungs
 choking awareness! Looking after your lungs Useful information and top tips Colds and chest infections can be common, especially in the autumn and winter months. It is therefore very important that you
choking awareness! Looking after your lungs Useful information and top tips Colds and chest infections can be common, especially in the autumn and winter months. It is therefore very important that you
Swallowing problems. Patient information. Name: Date: Speech and Language Therapist: Reviewed: May 2016 Next review: June 2017 Version 1
 Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
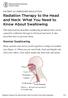 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Management of Chronic Obstructive Lung Disease
 Management of Chronic Obstructive Lung Disease 慢性阻塞性肺病的治療與護理 Chapter Three Put Yourself in Control LEARNING HELPFUL WAYS TO BREATHE Learning helpful ways to breathe means learning to use your lungs smarter
Management of Chronic Obstructive Lung Disease 慢性阻塞性肺病的治療與護理 Chapter Three Put Yourself in Control LEARNING HELPFUL WAYS TO BREATHE Learning helpful ways to breathe means learning to use your lungs smarter
Common complaints included: "No one can hear me!" "My voice wears out too quickly." "My throat feels so tight and strained."
 PART ONE OF THREE ARTICLES The George Washington University Speech and Hearing Center in Washington DC has treated clients with voice problems since the 1970 s. One of the most common vocal issues that
PART ONE OF THREE ARTICLES The George Washington University Speech and Hearing Center in Washington DC has treated clients with voice problems since the 1970 s. One of the most common vocal issues that
SWALLOWING DIFFICULTIES IN HD
 Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Scapular Protraction in Sitting
 9 Pause and Practice: Scapular Protraction in Sitting This practice lab is an example of putting muscles on length in order to achieve proper alignment of shoulder structures in preparation for facilitating
9 Pause and Practice: Scapular Protraction in Sitting This practice lab is an example of putting muscles on length in order to achieve proper alignment of shoulder structures in preparation for facilitating
Kadochnikov System. Stage I. Preparation of the body
 Kadochnikov System International Association Stage I. Preparation of the body Special methods of lower acrobatics to master the movement skills of a fighter www.kadochnikovsystem.com Stage I. Preparation
Kadochnikov System International Association Stage I. Preparation of the body Special methods of lower acrobatics to master the movement skills of a fighter www.kadochnikovsystem.com Stage I. Preparation
Benefits of Weight bearing increased awareness of the involved side decreased fear improved symmetry regulation of muscle tone
 From the information we have gathered during our Evaluation, the Clinical Reasoning we used to identify key problem areas and the Goals Established with functional outcomes we now have enough information
From the information we have gathered during our Evaluation, the Clinical Reasoning we used to identify key problem areas and the Goals Established with functional outcomes we now have enough information
Progressive Muscle Relaxation
 Module 3 Progressive Muscle Relaxation Introduction 2 Progressive Muscle Relaxation 3 Preparing for Relaxation 3 Relaxation Technique 4 The Calming Technique: Body and Breath 6 Difficulties with Relaxation
Module 3 Progressive Muscle Relaxation Introduction 2 Progressive Muscle Relaxation 3 Preparing for Relaxation 3 Relaxation Technique 4 The Calming Technique: Body and Breath 6 Difficulties with Relaxation
I will explain the most important concepts of functional treatment while treating our 4 patients: Tom Clint Alice Dick
 Every step we ve covered so far, from Evaluation to Clinical Reasoning to Establishing Goals and Preparation for Function has laid the groundwork for the final step: Treatment Using Functional Activities.
Every step we ve covered so far, from Evaluation to Clinical Reasoning to Establishing Goals and Preparation for Function has laid the groundwork for the final step: Treatment Using Functional Activities.
Chapter 21 NECK AND HEAD Upper vertebrae (mid back and neck) viewed from back
 Chapter 21 NECK AND HEAD INJURIES 319 Chapter 21 NECK AND HEAD The neck (cervical vertebrae) is the upper end of the back s vertebral column, on top of the mobile thoracic, and lumbar, and fused sacral
Chapter 21 NECK AND HEAD INJURIES 319 Chapter 21 NECK AND HEAD The neck (cervical vertebrae) is the upper end of the back s vertebral column, on top of the mobile thoracic, and lumbar, and fused sacral
BODY SYSTEMS, DRUGS, AND OBSERVATIONS SCOPE OF UNIT: This unit includes guidelines for observing and reporting.
 LESSON PLAN: 10 COURSE TITLE: UNIT: III MEDICATION TECHNICIAN BODY SYSTEMS, DRUGS, AND OBSERVATIONS SCOPE OF UNIT: This unit includes guidelines for observing and reporting. INFORMATION TOPIC: III-10 OR
LESSON PLAN: 10 COURSE TITLE: UNIT: III MEDICATION TECHNICIAN BODY SYSTEMS, DRUGS, AND OBSERVATIONS SCOPE OF UNIT: This unit includes guidelines for observing and reporting. INFORMATION TOPIC: III-10 OR
RELAXATION EXERCISES
 RELAXATION EXERCISES Relaxation technique 1: Breathing meditation for stress relief With its focus on full, cleansing breaths, deep breathing is a simple, yet powerful, relaxation technique. It s easy
RELAXATION EXERCISES Relaxation technique 1: Breathing meditation for stress relief With its focus on full, cleansing breaths, deep breathing is a simple, yet powerful, relaxation technique. It s easy
Resource: Pain Assessments
 Pain assessment is an integral part of patient care. The patient s pain should be assessed at each visit using consistent assessment tools based on the patient s ability to communicate. For all pain scales
Pain assessment is an integral part of patient care. The patient s pain should be assessed at each visit using consistent assessment tools based on the patient s ability to communicate. For all pain scales
Body Mechanics--Posture, Alignment & Core
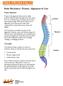 Body Mechanics--Posture, Alignment & Core Proper Alignment Proper body alignment allows you to safely perform different tasks throughout the day, and to do so in a way that does not require you to exert
Body Mechanics--Posture, Alignment & Core Proper Alignment Proper body alignment allows you to safely perform different tasks throughout the day, and to do so in a way that does not require you to exert
CHEST PHYSICAL THERAPY (CPT): CHILDREN AND ADULTS
 CHEST PHYSICAL THERAPY (CPT): CHILDREN AND ADULTS Chest Physical Therapy (CPT), also called postural drainage, is a way for you to help your child get rid of extra mucus in his lungs. This is important
CHEST PHYSICAL THERAPY (CPT): CHILDREN AND ADULTS Chest Physical Therapy (CPT), also called postural drainage, is a way for you to help your child get rid of extra mucus in his lungs. This is important
Recovering from breast reconstruction with exercise - TRAM or DIEP
 Recovering from breast reconstruction with exercise TRAM or DIEP After TRAM or DIEP flap breast reconstruction surgery, your arm movements may be limited. This fact sheet explains how to do regular exercises.
Recovering from breast reconstruction with exercise TRAM or DIEP After TRAM or DIEP flap breast reconstruction surgery, your arm movements may be limited. This fact sheet explains how to do regular exercises.
TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS
 TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS Massage: The temporalis on the side of the head is easy to locate. Press on it looking for painful nodules, massaging gently. Opening and closing
TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS Massage: The temporalis on the side of the head is easy to locate. Press on it looking for painful nodules, massaging gently. Opening and closing
Supporting information leaflet (6): Chest Physiotherapy: Lung Volume Recruitment Techniques and Cough Augmentation (Assisted Cough Techniques)
 Acute Services Division Supporting information leaflet (6): Chest Physiotherapy: Lung Volume Recruitment Techniques and Cough Augmentation (Assisted Cough Techniques) Introduction For many people with
Acute Services Division Supporting information leaflet (6): Chest Physiotherapy: Lung Volume Recruitment Techniques and Cough Augmentation (Assisted Cough Techniques) Introduction For many people with
Physiotherapy following cardiac surgery. Information for patients Cardiac Surgery
 Physiotherapy following cardiac surgery Information for patients Cardiac Surgery Physiotherapy is an essential part of your recovery from your operation. The physiotherapist will see you before you have
Physiotherapy following cardiac surgery Information for patients Cardiac Surgery Physiotherapy is an essential part of your recovery from your operation. The physiotherapist will see you before you have
Strength and Endurance
 Strength and Endurance What is strength and endurance? In practical terms, muscle strength is how strong the child is and muscular endurance is how long the child s muscles can work. In more specific terms:
Strength and Endurance What is strength and endurance? In practical terms, muscle strength is how strong the child is and muscular endurance is how long the child s muscles can work. In more specific terms:
LESSON ASSIGNMENT. Physical Assessment of the Respiratory System. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 2 Physical Assessment of the Respiratory System. LESSON ASSIGNMENT Paragraphs 2-1 through 2-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 2-1. Perform
LESSON ASSIGNMENT LESSON 2 Physical Assessment of the Respiratory System. LESSON ASSIGNMENT Paragraphs 2-1 through 2-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 2-1. Perform
the back book Your Guide to a Healthy Back
 the back book Your Guide to a Healthy Back anatomy Your spine s job is to: Support your upper body and neck Increase flexibility of your spine Protect your spinal cord There are 6 primary components of
the back book Your Guide to a Healthy Back anatomy Your spine s job is to: Support your upper body and neck Increase flexibility of your spine Protect your spinal cord There are 6 primary components of
Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises. Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises
 Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction Weight-bearing and resistance exercises have
Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction Weight-bearing and resistance exercises have
Voice. What is voice? Why is voice important?
 Voice What is voice? Voice is the sound that we hear when someone talks. It is produced by air coming from the diaphragm and lungs passing through the voice box (vocal folds) causing them to vibrate and
Voice What is voice? Voice is the sound that we hear when someone talks. It is produced by air coming from the diaphragm and lungs passing through the voice box (vocal folds) causing them to vibrate and
Anal Atresia FACTS: There is no known cause for anal atresia. Children with anal atresia can lead very happy lives post surgery!
 Anal Atresia FACTS: Anal atresia affects 1 in 5,000 births and is slightly more common in boys. There is no known cause for this condition. With anal atresia, any of the following can occur: The anal passage
Anal Atresia FACTS: Anal atresia affects 1 in 5,000 births and is slightly more common in boys. There is no known cause for this condition. With anal atresia, any of the following can occur: The anal passage
Difficulty judging body positioning in relation to objects in the environment
 ASPERGER SYNDROME & SENSORY ISSUES Accident Prone Is clumsy/accident prone; bumps into things and breaks things often Difficulty judging body positioning in relation to objects in the environment Seems
ASPERGER SYNDROME & SENSORY ISSUES Accident Prone Is clumsy/accident prone; bumps into things and breaks things often Difficulty judging body positioning in relation to objects in the environment Seems
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016
 Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Stuttering. Risk factors that predict a chronic problem rather than spontaneous recovery include:
 Stuttering PREVALENCE, INCIDENCE, AND RISK FACTORS FOR CHRONICITY About 5% of all children go through a period of stuttering that lasts six months or more. Three- quarters of those who begin to stutter
Stuttering PREVALENCE, INCIDENCE, AND RISK FACTORS FOR CHRONICITY About 5% of all children go through a period of stuttering that lasts six months or more. Three- quarters of those who begin to stutter
Taking Care of Your Back
 Taking Care of Your Back Most people will feel back pain at some point in their lives, but not all back pain is the same for everyone. The good news is, most low back pain improves without any treatment
Taking Care of Your Back Most people will feel back pain at some point in their lives, but not all back pain is the same for everyone. The good news is, most low back pain improves without any treatment
VOICE LESSON #8. Integration: Putting It All Together
 Page 1 of 6 VOICE LESSON #8 Integration: Putting It All Together I) Vocal Coordination - By now you re well aware that all of the essential elements of singing are interdependent. Breath support is dependent
Page 1 of 6 VOICE LESSON #8 Integration: Putting It All Together I) Vocal Coordination - By now you re well aware that all of the essential elements of singing are interdependent. Breath support is dependent
Laryngoscopy Examinations
 Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Pelvic floor awareness for psychosexual therapy Information for men
 Pelvic floor awareness for psychosexual therapy Information for men Yes men have pelvic floor muscles too! The pelvic floor muscles support the bottom of the pelvis and the organs inside the pelvis (lower
Pelvic floor awareness for psychosexual therapy Information for men Yes men have pelvic floor muscles too! The pelvic floor muscles support the bottom of the pelvis and the organs inside the pelvis (lower
Foundational Spine Exercises
 These exercises should only be used as a starting point to strengthen the muscles that support your back. Your physical therapist will tailor a program that fits your needs and activity level, using exercises
These exercises should only be used as a starting point to strengthen the muscles that support your back. Your physical therapist will tailor a program that fits your needs and activity level, using exercises
Precious Moments. Giving comfort and support when someone you love is dying.
 Precious Moments Giving comfort and support when someone you love is dying www.stjoes.ca When someone you love is dying When someone you love is dying, you may want to know how you can provide comfort
Precious Moments Giving comfort and support when someone you love is dying www.stjoes.ca When someone you love is dying When someone you love is dying, you may want to know how you can provide comfort
relaxation and nervous system regulation exercises
 relaxation and nervous system regulation exercises Objectives to provide a range of simple exercises that encourage the regular practice of relaxation and to help build resilience with increased awareness
relaxation and nervous system regulation exercises Objectives to provide a range of simple exercises that encourage the regular practice of relaxation and to help build resilience with increased awareness
Academy for Coaching Parents International 524 Cranbrook Drive Fort Worth, TX FULL WAVE BREATHING
 FULL WAVE BREATHING SIMPLE INFO Only the basics of Full Wave Breathing are given here. Scientific and empirical background, case studies and testimonials positively support incorporating it into your life.
FULL WAVE BREATHING SIMPLE INFO Only the basics of Full Wave Breathing are given here. Scientific and empirical background, case studies and testimonials positively support incorporating it into your life.
Physiotherapy for heart surgery
 Physiotherapy for heart surgery Patient Information Date:... Name:... Physiotherapist:... Physiotherapy Clinical Diagnostic and Support Services Centre Do only the exercise stated and shown by your physiotherapist.
Physiotherapy for heart surgery Patient Information Date:... Name:... Physiotherapist:... Physiotherapy Clinical Diagnostic and Support Services Centre Do only the exercise stated and shown by your physiotherapist.
VOICE LESSON #6. Resonance: Creating Good Vocal Vibes. The Soft Palate
 VOICE LESSON #6 Resonance: Creating Good Vocal Vibes Voice Lesson #6 - Resonance Page 1 of 7 RESONANCE is the amplification and enrichment of tones produced by the voice. When we talk about resonance,
VOICE LESSON #6 Resonance: Creating Good Vocal Vibes Voice Lesson #6 - Resonance Page 1 of 7 RESONANCE is the amplification and enrichment of tones produced by the voice. When we talk about resonance,
Rehab to Home. Stroke Recovery EDUCATION BOOKLET FOR: Care & Safety Tips. Frequently Asked Questions. Working Toward Independence. Adaptive Equipment
 Stroke Recovery Rehab to Home Care & Safety Tips Frequently Asked Questions Working Toward Independence Adaptive Equipment Summary of Progress Different Types of Therapy Personal Goals EDUCATION BOOKLET
Stroke Recovery Rehab to Home Care & Safety Tips Frequently Asked Questions Working Toward Independence Adaptive Equipment Summary of Progress Different Types of Therapy Personal Goals EDUCATION BOOKLET
Asthma. & Older Adults. A guide to living with asthma for people aged 65 years and over FOR PATIENTS & CARERS
 Asthma & Older Adults A guide to living with asthma for people aged 65 years and over FOR PATIENTS & CARERS what is Asthma? Asthma is a disease of the airways, the small tubes which carry air in and out
Asthma & Older Adults A guide to living with asthma for people aged 65 years and over FOR PATIENTS & CARERS what is Asthma? Asthma is a disease of the airways, the small tubes which carry air in and out
RESPIRATORY REHABILITATION
 RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
BACK PAIN. Spare 5 minutes to find out how to cope with back pain
 BACK PAIN Spare 5 minutes to find out how to cope with back pain You always managed your responsibilities as a wife, mother, sister, daughter, daughter in law, friend, boss, and colleague indeed managed
BACK PAIN Spare 5 minutes to find out how to cope with back pain You always managed your responsibilities as a wife, mother, sister, daughter, daughter in law, friend, boss, and colleague indeed managed
VB-MAPP Barriers Assessment
 1. Negative Behaviors 0. Does not demonstrate any significant negative behaviors 1. Engages in some minor negative behaviors weekly, but recovery is quick 2. Emits a variety of minor negative behaviors
1. Negative Behaviors 0. Does not demonstrate any significant negative behaviors 1. Engages in some minor negative behaviors weekly, but recovery is quick 2. Emits a variety of minor negative behaviors
Vocal Hygiene. How to Get The Best Mileage From Your Voice
 Vocal Hygiene How to Get The Best Mileage From Your Voice Speech and Voice Production Speech and voice are the result of a complex interplay of physical and emotional events. The first event is in the
Vocal Hygiene How to Get The Best Mileage From Your Voice Speech and Voice Production Speech and voice are the result of a complex interplay of physical and emotional events. The first event is in the
Vocal Hygiene. How to Get The Best Mileage From Your Voice. Provincial Voice Care Resource Program Vancouver General Hospital
 Vocal Hygiene How to Get The Best Mileage From Your Voice Provincial Voice Care Resource Program Vancouver General Hospital Gordon & Leslie Diamond Health Care Centre Vancouver General Hospital 4th Floor,
Vocal Hygiene How to Get The Best Mileage From Your Voice Provincial Voice Care Resource Program Vancouver General Hospital Gordon & Leslie Diamond Health Care Centre Vancouver General Hospital 4th Floor,
Chorus Study Guide Unit 1: Know Thy Voice
 Chorus Study Guide Unit 1: Know Thy Voice INSTRUCTOR: Mrs. DJ Ross Djuana.Ross@charlottelearningacademy.org Please study notes below in preparation for the unit test. www.nidcd.nih.gov Structures involved
Chorus Study Guide Unit 1: Know Thy Voice INSTRUCTOR: Mrs. DJ Ross Djuana.Ross@charlottelearningacademy.org Please study notes below in preparation for the unit test. www.nidcd.nih.gov Structures involved
Dysphagia Management in TCP. Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012
 Dysphagia Management in TCP Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012 The role of the Speech Pathologist To assess swallowing status To provide management and
Dysphagia Management in TCP Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012 The role of the Speech Pathologist To assess swallowing status To provide management and
Talk about COPD. Challenging COPD Your Action Planner. key to COPD
 Talk about COPD Challenging COPD Your Action Planner key to COPD Section 1 Welcome, Having a lifelong condition like chronic obstructive pulmonary disease (COPD) doesn t mean you have to stop doing all
Talk about COPD Challenging COPD Your Action Planner key to COPD Section 1 Welcome, Having a lifelong condition like chronic obstructive pulmonary disease (COPD) doesn t mean you have to stop doing all
Osteoporosis Exercise:
 Osteoporosis Exercise: Balance, Posture and Functional Exercises Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction You can help improve and maintain your balance, posture
Osteoporosis Exercise: Balance, Posture and Functional Exercises Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction You can help improve and maintain your balance, posture
Relax! Improve Your Playing by Releasing Tension. Dr. Liz Aleksander and Andrew Morency University of Tennessee at Martin
 Relax! Improve Your Playing by Releasing Tension Dr. Liz Aleksander and Andrew Morency University of Tennessee at Martin Tension Goal when playing: minimize tension Tension radiates to other areas Physical
Relax! Improve Your Playing by Releasing Tension Dr. Liz Aleksander and Andrew Morency University of Tennessee at Martin Tension Goal when playing: minimize tension Tension radiates to other areas Physical
Issues for Patient Discussion
 onmotor complications radykinesia Screening Tools asked PD micrographia eurodegeneration Designed for Use by Family Practitioners remor on-off opamine agonists tiffness depression ostural instability wearing
onmotor complications radykinesia Screening Tools asked PD micrographia eurodegeneration Designed for Use by Family Practitioners remor on-off opamine agonists tiffness depression ostural instability wearing
Dysphagia (swallowing problems)
 Dysphagia (swallowing problems) Speech and Language Therapy Department Patient Information Leaflet Introduction This leaflet is for people who have dysphagia. It gives information on what this condition
Dysphagia (swallowing problems) Speech and Language Therapy Department Patient Information Leaflet Introduction This leaflet is for people who have dysphagia. It gives information on what this condition
Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual
 Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual 2nd Edition Isabelle M. Bohman, M.S., P.T., NDT Coordinator Instructor TM Published by Clinician s View Albuquerque, NM 505-880-0058
Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual 2nd Edition Isabelle M. Bohman, M.S., P.T., NDT Coordinator Instructor TM Published by Clinician s View Albuquerque, NM 505-880-0058
Peer Support Meeting COMMUNICATION STRATEGIES
 Peer Support Meeting COMMUNICATION STRATEGIES Communication Think of a situation where you missed out on an opportunity because of lack of communication. What communication skills in particular could have
Peer Support Meeting COMMUNICATION STRATEGIES Communication Think of a situation where you missed out on an opportunity because of lack of communication. What communication skills in particular could have
Palliative Care Victoria The Process of Dying Page 1. The Process of Dying. What to expect and how to help
 Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
Commonwealth Health Corporation NEXT
 Commonwealth Health Corporation This computer-based learning (CBL) module details important aspects of musculoskeletal disorders, body mechanics and ergonomics in the workplace. It examines: what causes
Commonwealth Health Corporation This computer-based learning (CBL) module details important aspects of musculoskeletal disorders, body mechanics and ergonomics in the workplace. It examines: what causes
EXERCISE FOR PARKINSON S RECOMMENDATIONS FOR MANAGING SYMPTOMS
 EXERCISE FOR PARKINSON S RECOMMENDATIONS FOR MANAGING SYMPTOMS INSIDE THIS GUIDE EXERCISE FOR PARKINSON S OVERVIEW 3 RECOMMENDATIONS FOR EXERCISE FOR PARKINSON S 4 EXERCISE FOR PARKINSON S PRINCIPLES 5
EXERCISE FOR PARKINSON S RECOMMENDATIONS FOR MANAGING SYMPTOMS INSIDE THIS GUIDE EXERCISE FOR PARKINSON S OVERVIEW 3 RECOMMENDATIONS FOR EXERCISE FOR PARKINSON S 4 EXERCISE FOR PARKINSON S PRINCIPLES 5
Winter Health Tips for Vocalists
 Winter Health Tips for Vocalists The winter season is a busy time of the year for a lot of people. Along with changes in weather comes an increased potential for colds and upper respiratory ailments that
Winter Health Tips for Vocalists The winter season is a busy time of the year for a lot of people. Along with changes in weather comes an increased potential for colds and upper respiratory ailments that
Routine For: Stroke Oral Motor Routine
 GENERAL TIPS FOR PATIENTS, STUDENTS, OR CAREGIVERS GENERAL TIPS (Continued) ALWAYS wash hands before practicing. Practice while sitting in chair. Head should be in midline and chin parallel to floor Use
GENERAL TIPS FOR PATIENTS, STUDENTS, OR CAREGIVERS GENERAL TIPS (Continued) ALWAYS wash hands before practicing. Practice while sitting in chair. Head should be in midline and chin parallel to floor Use
Communication with Cognitively Impaired Clients For CNAs
 Communication with Cognitively Impaired Clients For CNAs This course has been awarded one (1.0) contact hour. This course expires on August 31, 2017. Copyright 2005 by RN.com. All Rights Reserved. Reproduction
Communication with Cognitively Impaired Clients For CNAs This course has been awarded one (1.0) contact hour. This course expires on August 31, 2017. Copyright 2005 by RN.com. All Rights Reserved. Reproduction
Sensory Processing Disorder
 Disorder 101 Ingrid M. Kanics Kanics Inclusive Design Services, LLC imkanics@mindspring.com Sensory Integration Sensory Regulation Disorder Background: A. Jean Ayres, Occupational Therapist Neuroscience
Disorder 101 Ingrid M. Kanics Kanics Inclusive Design Services, LLC imkanics@mindspring.com Sensory Integration Sensory Regulation Disorder Background: A. Jean Ayres, Occupational Therapist Neuroscience
Pilates PASSPORT. Your Guide to Movement Mastery Park Meadows Pilates and Physical Therapy
 Pilates PASSPORT Your Guide to Movement Mastery 2012 Park Meadows Pilates and Physical Therapy http://parkmeadowspilates.com 303-649-2165 This Passport Belongs To: Starting Date: My Movement Goals: 2 Welcome!
Pilates PASSPORT Your Guide to Movement Mastery 2012 Park Meadows Pilates and Physical Therapy http://parkmeadowspilates.com 303-649-2165 This Passport Belongs To: Starting Date: My Movement Goals: 2 Welcome!
Chapter 9: Exercise Instructions
 RESOURCES RESEARCHERS / MEDICAL HOW TO HELP SPONSORS GEHRIG CONNECTION MEDIA TELETHON MDA.ORG search our site Go MDA/ALS Newsmagazine Current Issue Home> Publications >Everyday Life With ALS: A Practical
RESOURCES RESEARCHERS / MEDICAL HOW TO HELP SPONSORS GEHRIG CONNECTION MEDIA TELETHON MDA.ORG search our site Go MDA/ALS Newsmagazine Current Issue Home> Publications >Everyday Life With ALS: A Practical
MOTOR EVALUATION SCALE FOR UPPER EXTREMITY IN STROKE PATIENTS (MESUPES-arm and MESUPES-hand)
 MOTOR EVALUATION SCALE FOR UPPER EXTREMITY IN STROKE PATIENTS (MESUPES-arm and MESUPES-hand) Name patient: Test date - hour: Name examiner: Duration of the test: min Handedness: right/left Support sitting
MOTOR EVALUATION SCALE FOR UPPER EXTREMITY IN STROKE PATIENTS (MESUPES-arm and MESUPES-hand) Name patient: Test date - hour: Name examiner: Duration of the test: min Handedness: right/left Support sitting
Coach on Call. Letting Go of Stress. A healthier life is on the line for you! How Does Stress Affect Me?
 Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
Understanding Dementia & Symptoms:
 Understanding Dementia & Symptoms: What is Happening? & How to Help! Teepa Snow, MS, OTR/L, FAOTA Dementia Care & Training Specialist, Positive Approach, LLC Consulting Associate, Duke University School
Understanding Dementia & Symptoms: What is Happening? & How to Help! Teepa Snow, MS, OTR/L, FAOTA Dementia Care & Training Specialist, Positive Approach, LLC Consulting Associate, Duke University School
LOW BACK PAIN. what you can do
 LOW BACK PAIN what you can do Back pain Nearly 80 percent of adults will experience back pain at some point in their life. The good news is that back pain will normally go away within four to six weeks
LOW BACK PAIN what you can do Back pain Nearly 80 percent of adults will experience back pain at some point in their life. The good news is that back pain will normally go away within four to six weeks
Home Office Solutions By: Laura Cervantes QAS 515 3/26/03
 Home Office Solutions By: Laura Cervantes QAS 515 3/26/03 Working from home is becoming more of an option for employees today. The type of work usually entails working from the home computer work station.
Home Office Solutions By: Laura Cervantes QAS 515 3/26/03 Working from home is becoming more of an option for employees today. The type of work usually entails working from the home computer work station.
Strong and Stable: Exercises for Core, Strength and Balance
 Strong and Stable: Exercises for Core, Strength and Balance Exercise and physical activity before, during and after cancer treatment are important to recovery and general quality of life. Studies show
Strong and Stable: Exercises for Core, Strength and Balance Exercise and physical activity before, during and after cancer treatment are important to recovery and general quality of life. Studies show
This Manual is copyright under the Berne Convention. In terms of the Copyright Act 98 of 1978 no part of this leaflet may be reproduced or
 Basic Ball Exercise Manual Train your Core This Manual is copyright under the Berne Convention. In terms of the Copyright Act 98 of 1978 no part of this leaflet may be reproduced or transmitted in any
Basic Ball Exercise Manual Train your Core This Manual is copyright under the Berne Convention. In terms of the Copyright Act 98 of 1978 no part of this leaflet may be reproduced or transmitted in any
Physiotherapy advice and exercises following Breast Reconstruction using a Tissue Expander. Northumbria Healthcare NHS Foundation Trust
 Northumbria Healthcare NHS Foundation Trust Physiotherapy advice and exercises following Breast Reconstruction using a Tissue Expander Issued by the Physiotherapy Department How can Physiotherapy help
Northumbria Healthcare NHS Foundation Trust Physiotherapy advice and exercises following Breast Reconstruction using a Tissue Expander Issued by the Physiotherapy Department How can Physiotherapy help
Inhale Cough and Deep Breathe Oral/Mouth Care Up - Head of Bed Up/Elevated Get out of Bed/Get moving Have a Conversation
 Preventing Pneumonia: ICOUGH Inhale Cough and Deep Breathe Oral/Mouth Care Up - Head of Bed Up/Elevated Get out of Bed/Get moving Have a Conversation Did you know anytime you are in the hospital, your
Preventing Pneumonia: ICOUGH Inhale Cough and Deep Breathe Oral/Mouth Care Up - Head of Bed Up/Elevated Get out of Bed/Get moving Have a Conversation Did you know anytime you are in the hospital, your
Functional rehab after breast reconstruction surgery
 Functional rehab after breast reconstruction surgery A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read this
Functional rehab after breast reconstruction surgery A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read this
Sportlyzer s Core Exercises
 Sportlyzer s Core Exercises Core training exercises are as important part of your training schedule as your endurance training. You need it to support your everyday running and improve your racing results.
Sportlyzer s Core Exercises Core training exercises are as important part of your training schedule as your endurance training. You need it to support your everyday running and improve your racing results.
LIPS TOGETHER AND TEETH APART
 John T. Mahoney, D.D.S. Family Dentistry 2117 Old Jeanerette Road New Iberia, LA 70563 Telephone 337-365-5865 Fax 337-365-6137 LIPS TOGETHER AND TEETH APART One of the most important steps in breaking
John T. Mahoney, D.D.S. Family Dentistry 2117 Old Jeanerette Road New Iberia, LA 70563 Telephone 337-365-5865 Fax 337-365-6137 LIPS TOGETHER AND TEETH APART One of the most important steps in breaking
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person
 Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Every 67seconds, someone will develop Alzheimer's.
 We all need a purpose and responsibilities to live a healthy life. Dementia Care 101 Corrin Campbell BS, COTA/L & Michael Urban, MS, OTR/L, MBA Every 67seconds, someone will develop Alzheimer's. http://www.alz.org
We all need a purpose and responsibilities to live a healthy life. Dementia Care 101 Corrin Campbell BS, COTA/L & Michael Urban, MS, OTR/L, MBA Every 67seconds, someone will develop Alzheimer's. http://www.alz.org
This Progressive Relaxation Procedure is yours to use and to distribute as you see fit.
 This Progressive Relaxation Procedure is yours to use and to distribute as you see fit. Jacobson s Progressive Relaxation Procedure Progressive Muscle Relaxation (PMR) Edmund Jacobson created the progressive
This Progressive Relaxation Procedure is yours to use and to distribute as you see fit. Jacobson s Progressive Relaxation Procedure Progressive Muscle Relaxation (PMR) Edmund Jacobson created the progressive
PHYSIOTHERAPY DEPARTMENT. Breathing and general exercise for the long term respiratory patient
 PHYSIOTHERAPY DEPARTMENT Breathing and general exercise for the long term respiratory patient This leaflet gives you general advice about managing your breathing. It also describes chest-clearing techniques,
PHYSIOTHERAPY DEPARTMENT Breathing and general exercise for the long term respiratory patient This leaflet gives you general advice about managing your breathing. It also describes chest-clearing techniques,
Modified Parkinson Activity Scale
 Modified Parkinson Activity Scale Chair transfers Analyses: Instruction: Chair with 40 cm seat height, or, when at the patient's home, the chair that causes the greatest problems to the patient and is
Modified Parkinson Activity Scale Chair transfers Analyses: Instruction: Chair with 40 cm seat height, or, when at the patient's home, the chair that causes the greatest problems to the patient and is
Communication and Swallowing with PSP/CBD. Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist
 Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Do s and Don ts with Low Back Pain
 Do s and Don ts with Low Back Pain Sitting Sit as little as possible and then only for short periods. Place a supportive towel roll at the belt line of the back especially when sitting in a car. When getting
Do s and Don ts with Low Back Pain Sitting Sit as little as possible and then only for short periods. Place a supportive towel roll at the belt line of the back especially when sitting in a car. When getting
Understanding and Managing Your Chronic Obstructive Pulmonary Disease (COPD)* *Includes chronic bronchitis and emphysema.
 Understanding and Managing Your Chronic Obstructive Pulmonary Disease (COPD)* *Includes chronic bronchitis and emphysema. 2 LIVING WITH COPD You may have been told that you have COPD. It is a lung disease
Understanding and Managing Your Chronic Obstructive Pulmonary Disease (COPD)* *Includes chronic bronchitis and emphysema. 2 LIVING WITH COPD You may have been told that you have COPD. It is a lung disease
Data Collection Worksheets
 Data Collection Worksheets PhenX Measure: Antipsychotic Medication Extrapyramidal Side Effects (#661600) PhenX Protocol: Antipsychotic Medication Extrapyramidal Side Effects (#661601) Date of Interview/Examination/Bioassay
Data Collection Worksheets PhenX Measure: Antipsychotic Medication Extrapyramidal Side Effects (#661600) PhenX Protocol: Antipsychotic Medication Extrapyramidal Side Effects (#661601) Date of Interview/Examination/Bioassay
Exercise: The Backbone of Spine Treatment
 Exercise: The Backbone of Spine Treatment North American Spine Society Public Education Series The Importance of Exercise Spine experts agree that physical activity is important for people with low back
Exercise: The Backbone of Spine Treatment North American Spine Society Public Education Series The Importance of Exercise Spine experts agree that physical activity is important for people with low back
YOUR FREE COMPREHENSIVE GUIDE TO HELP RELIEVE LOWER BACK PAIN NATURALLY
 YOUR FREE COMPREHENSIVE GUIDE TO HELP RELIEVE LOWER BACK PAIN NATURALLY By: helpwithsciatica HTTPS://HELPWITHSCIATICA.COM Table of contents 1 Introduction 2 Exercise: Extensions 3 Exercise: Curl-Ups 4
YOUR FREE COMPREHENSIVE GUIDE TO HELP RELIEVE LOWER BACK PAIN NATURALLY By: helpwithsciatica HTTPS://HELPWITHSCIATICA.COM Table of contents 1 Introduction 2 Exercise: Extensions 3 Exercise: Curl-Ups 4
Height: Weight: Neck Size: Does your work involve shift work? Yes No. Where did you hear about us: Physician Media Friend Other
 Personal Information Name: Date of birth: Sex: Male Female Marital Status: Nationality: MRN(for KAUH Patients): Height: Weight: Neck Size: Address: Occupation: Length of work day: Does your work involve
Personal Information Name: Date of birth: Sex: Male Female Marital Status: Nationality: MRN(for KAUH Patients): Height: Weight: Neck Size: Address: Occupation: Length of work day: Does your work involve
Stay Fit While You Sit: 10 Simple Exercises for Sewers
 Published on Sew4Home Stay Fit While You Sit: 10 Simple Exercises for Sewers Editor: Liz Johnson Friday, 05 May 2017 1:00 There is a lot of sitting involved in sewing, which can lead to aches and pains
Published on Sew4Home Stay Fit While You Sit: 10 Simple Exercises for Sewers Editor: Liz Johnson Friday, 05 May 2017 1:00 There is a lot of sitting involved in sewing, which can lead to aches and pains
Relevant Listings for Evaluating Traumatic Brain Injury at Step 3 of the Sequential Evaluation
 Relevant Listings for Evaluating Traumatic Brain Injury at Step 3 of the Sequential Evaluation I. Neurological Disorders Revised Medical Criteria for Evaluating Neurological Disorders went into effect
Relevant Listings for Evaluating Traumatic Brain Injury at Step 3 of the Sequential Evaluation I. Neurological Disorders Revised Medical Criteria for Evaluating Neurological Disorders went into effect
A guide to short relaxation exercises. Information for patients Regional Department of Neurotology
 A guide to short relaxation exercises Information for patients Regional Department of Neurotology The Regional Department of Neurotology at Sheffield Teaching Hospitals offers relaxation therapy as part
A guide to short relaxation exercises Information for patients Regional Department of Neurotology The Regional Department of Neurotology at Sheffield Teaching Hospitals offers relaxation therapy as part
Transformative Life Skills (TLS) Curriculum. Unit 4. Healthy Relationships
 Transformative Life Skills (TLS) Curriculum Unit 4. Healthy Relationships Niroga Institute Founded in 2005, Niroga is a 501(c)(3) non-profit organization that brings: Transformative Life Skills (TLS) to
Transformative Life Skills (TLS) Curriculum Unit 4. Healthy Relationships Niroga Institute Founded in 2005, Niroga is a 501(c)(3) non-profit organization that brings: Transformative Life Skills (TLS) to
Body Mechanics When caring for a client
 Body Mechanics When caring for a client If assistance is needed, find out the client's strengths and weaknesses. Often one side of the body is stronger. The stronger side should be transferred first. When
Body Mechanics When caring for a client If assistance is needed, find out the client's strengths and weaknesses. Often one side of the body is stronger. The stronger side should be transferred first. When
Do the same as above, but turn your head TOWARDS the side that you re holding on to the chair.
 Stretch 4-6 times per day and hold each stretch for a minimum of 30 seconds. Perform the stretch gently without bouncing. Discuss any problems with your Chiropractor. Sit upright with your head and shoulder
Stretch 4-6 times per day and hold each stretch for a minimum of 30 seconds. Perform the stretch gently without bouncing. Discuss any problems with your Chiropractor. Sit upright with your head and shoulder
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection
 The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
Tobacco Cessation Toolkit
 You notice physical s, like moments of dizziness, sweating, hands trembling or a mild headache. When using tobacco, nicotine increases your heart rate (by about 10 20 beats per minute) and blood pressure.
You notice physical s, like moments of dizziness, sweating, hands trembling or a mild headache. When using tobacco, nicotine increases your heart rate (by about 10 20 beats per minute) and blood pressure.
Copyright Cardiff University
 This exercise programme has been developed by physiotherapists specifically for people with movement disorders. Exercise is not without its risks and this or any other exercise programme has potential
This exercise programme has been developed by physiotherapists specifically for people with movement disorders. Exercise is not without its risks and this or any other exercise programme has potential
