Robot-based assessment of motor and proprioceptive function identifies biomarkers for prediction of functional independence measures
|
|
|
- Dortha Gibbs
- 6 years ago
- Views:
Transcription
1 Mostafavi et al. Journal of NeuroEngineering and Rehabilitation (2015) 12:105 DOI /s RESEARCH Robot-based assessment of motor and proprioceptive function identifies biomarkers for prediction of functional independence measures Sayyed Mostafa Mostafavi 1, Parvin Mousavi 1, Sean P. Dukelow 2 and Stephen H. Scott 3,4,5* Open Access Abstract Background: Neurological impairments following stroke impact the ability of individuals to perform daily activities, although the relative impact of individual impairments is not always clear. Recovery of sensorimotor function following stroke can vary widely, from complete recovery to modest or minimal improvements, across individuals. An important question is whether one can predict the amount of recovery based on initial examination of the individual. Robotic technologies are now being used to quantify a range of behavioral capabilities of individuals post-stroke, providing a rich set of biomarkers of sensory and motor dysfunction. The objective of the present study is to use mathematical models to identify which biomarkers best predict the ability of subjects with stroke to perform daily activities before and after rehabilitation. Methods: The Functional Independence Measure (FIM) was quantified approximately 2 weeks and three months post-stroke in 61 ischemic and 24 hemorrhagic subjects with stroke. At 2 weeks post-stroke, subjects also completed clinical assessments and robotic assessments of sensory and motor function. A computational search algorithm, known as Fast Orthogonal Search, was used to identify the robotic and clinical biomarkers that best estimated Functional Independence Measures. Results: Clinical and robot-based biomarkers were statistically similar at predicting FIM scores at 2 weeks (r = vs , respectively) and 3 months (r = vs , respectively). Importantly, robot-based biomarkers highlighted that parameters related to proprioception were influential for predicting FIM scores at 2 weeks, whereas biomarkers related to bimanual motor function were influential for predicting FIM scores at 3 months. Conclusions: The present study provides a proof of principle on the use of robot-based biomarkers of sensory and motor dysfunction to estimate present and future FIM scores. The addition of other behavioral tasks will likely increase the accuracy of these predictions, and potentially help guide rehabilitation strategies to maximize functional recovery. Keywords: Stroke assessment, Prognosis, Proprioception, Robotic assessment, Upper limb, Stroke * Correspondence: steve.scott@queensu.ca 3 Department of Biomedical and Molecular Sciences, Queen s University, Kingston, ON, Canada 4 Providence Care, St. Mary s of the Lake Hospital, Kingston, ON, Canada Full list of author information is available at the end of the article 2015 Mostafavi et al. Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
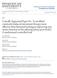
2 Mostafavi et al. Journal of NeuroEngineering and Rehabilitation (2015) 12:105 Page 2 of 12 Background A key focus of rehabilitation therapy following stroke is to regain the ability to perform daily activities. The Functional Independence Measure (FIM) is routinely used in Canada and the United States to score rehabilitation inpatients to quantify the ability to perform these daily activities following stroke using a 7-point scale for 13 motor and 5 cognitive tasks such as getting dressed, grooming and bowel control [1]. The FIM was designed to track changes in the functional status of patients prior to and following rehabilitation [2]. FIM scores have been shown to predict functional outcome following rehabilitation [3]. While FIM intake and discharge scores are correlated to some degree [4], predicting future abilities from early FIM scores is problematic - improved FIM scores following rehabilitation can reflect improved motor function in the affected limb (motor recovery), and/or acquired skills to perform motor actions unimanually with the unaffected limb (compensation) [5, 6]. The inability to perform daily activities following stroke is, of course, caused by focal damage in the brain that disrupts circuits that support various sensory, motor and cognitive processes. Several studies highlight that lesion size and location can predict motor recovery [7]. However, such predictions are not straightforward due to the close proximity of key circuits supporting various brain faculties. For example, small focal lesions near the internal capsule and thalamus can lead to varying levels of limb proprioceptive and motor impairments [8]. Another approach to predict future capabilities of daily activities is based on the underlying sensory, motor and cognitive impairments. There is an obvious link between neurological impairments and difficulties in performing daily activities. Measures of motor impairments in the affected arm generally correlate with FIM [4, 9]. As well, proprioceptive impairments also correlate with FIM scores [9, 10]. However, improvements in FIM can occur independent of the affected limb if individuals are able to perform the activity only with their unaffected limb. This unaffected arm often also shows impairments following stroke [11], and thus also potentially impacts functional recovery. The purpose of this study was to use robot and clinical biomarkers associated with upper limb function quantified in the first few days post-stroke to estimate the ability of subjects to perform daily activities at this same time point, as well as to predict their abilities at 3 months post-stroke. In particular, recent development of robot-based behavioural tasks provide a rich set of biomarkers of sensory and motor function, including performance of the affected and unaffected arms. Our interest was to observe which features of sensory and motor function were most important for predicting both FIM scores prior to and following rehabilitation. Methods Participants Subjects with stroke were recruited after admission to St. Mary s of the Lake Hospital in Kingston, Ontario, Canada, Dr. Vernon Fanning Care Centre (Calgary, AB, Canada), and Foothills Hospital, Calgary, Alberta, Canada for clinical stroke assessment and robotic evaluation. Clinical evaluation sessions were performed within approximately two weeks post-stroke. Initial FIM measurements were also completed approximately two weeks post stroke. Evaluation of the second FIM measurements were completed 3 months+/-1 month post stroke. We henceforth refer to these two FIM evaluations as FIM-2w and FIM-3 m, respectively. Inclusion criteria were the following: (a) first clinical presentation of stroke; (b) ability to understand the task instructions; and (c) sufficient range of motion to complete robotic testing. Subjects were excluded from the study if they had a history of neurological impairments not caused by stroke, any form of acute medical illness, or musculoskeletal compromise of the shoulder or elbow. Subjects received standard rehabilitation programs that were largely based on principles of motor learning as well as neurodevelopmental techniques. Rehabilitation was generally performed each weekday for 6 to 8 weeks. The study was approved by the ethics review boards of Queen s University, University of Calgary, and Providence Care, and all subjects for the study gave their informed consent. Robotic Assessment Robotic assessments were performed using the KINARM exoskeleton robotic device (BKIN Technologies, Kingston, Canada, [12]). The subject s arms were abducted into the horizontal plane. The robot provided gravitational support of the limb, monitored shoulder and elbow motion, and can apply mechanical loads at the shoulder and/or elbow. A virtual reality system aligned with the plane of the arms displayed spatial targets and visual feedback of the hand, as required by each task. Participants did not use the KINARM robot except for the clinical assessments in this study. To avoid fatigue, subjects were allowed to take a break between tasks. Figure 1 depicts a schematic view of the KINARM robot for assessment of a typical subject. Visually-Guided Reaching Task Details of this task and its associated parameters, henceforth referred to as the Reaching task, have been described elsewhere [12]. Briefly, subjects were asked to reach quickly and accurately from a central target to one of eight peripheral targets located 10 cm away, distributed around the circumference of a circle. There was no emphasis in the task instructions on either speed or accuracy to reach to the targets so each subject selected how to trade-off these task requirements. Each trial
3 Mostafavi et al. Journal of NeuroEngineering and Rehabilitation (2015) 12:105 Page 3 of 12 Fig. 1 KINARM exoskeleton robotic device used for evaluation of motor and proprioceptive deficits of subjects with stroke began with subjects holding their index finger tip at a central target for ms. Then a peripheral target was illuminated and subjects were given 3000 ms to complete the reach. Each target was presented once per block and subjects completed eight blocks for a total of 64 trials. Subjects performed this task with both their affected and unaffected arms. A total of 13 parameters were used to quantify subject performance in this task for the affected (RA) and unaffected (RU) arms (See Table 1). For each subject, the value of each measured parameter was averaged across the 64 trials. Interlimb (RI) differences in reaching performance between the two arms were also quantified. Arm-Position Matching Task Details of this task and its associated parameters, henceforth referred to as the Matching task, have been described elsewhere [13]. Briefly, subjects allowed the robot to passively move the affected hand (passive arm) to one of nine different spatial locations, arranged as a 3-by-3 square grid, with vision occluded [13]. When the robot stopped, subjects attempted to move the unaffected hand (active arm) to the mirror location in space. Subjects could continue to adjust the position of their active arm until they felt it was mirror-matched with the passive arm position. When subjects indicated they attained the mirror location, they informed the instructor and this was recorded as the final hand position, after which the next trial began. Target locations were such that the outer eight targets were separated by 10 cm. The robot randomly moved from one location to the next. Subjects did not go to a standard start position between trials. Each subject completed six blocks (target locations random within a block) for a total of 54 trials. Nine parameters quantified subject performance (See Table 1). Object Hit Task Details of this task and its associated parameters have been described elsewhere [14]. Briefly, subjects were instructed to use virtual paddles attached to the right and left hands to hit red balls that were moving towards them on the screen. The objective of the task is to hit as many balls as possible. The balls appear on the screen from 10 different (hidden) bins, and a total of 30 balls are released from each bin in random order (all 10 bins release a ball before a bin is reused). Consequently, the game consists of a total of 300 balls falling continuously on the screen. The number of balls that appear on the screen and the speed of the ball movement increases as the task progresses, such that a single ball is moving slowly (~0.01 m/s) at the beginning and up to a maximum of 16 balls moving on the screen at ~0.05 m/s towards the end of the task. The KINARM robot provides force feedback each time a paddle hits a ball. A total of 14 parameters quantified subject performance including total balls hit, as well as spatial and motor features of the task (See Table 1). Clinical Measures of Stroke The Functional Independence Measure (FIM) [15], Purdue Pegboard Test [16], Modified Ashworth Score [17], and Chedoke-McMaster assessment [18] were used for clinical evaluation of subjects with stroke. These measures have established validity and reliability [19, 20]. The FIM measures functional abilities of subjects and is a widely used measure of disability following stroke. Good construct and validity have been established for FIM [21]. The FIM evaluates 18 areas of function, which are rated on a 1 7 scale, ranging from full dependence (1) to full independence with no required assistance (7). The 18 areas of function are categorized into 13 motor items and 5 cognitive items. We refer to the scales corresponding to the 18 items and 13 items as FIM-Total and FIM-Motor, respectively. The Purdue Pegboard Test assesses manual dexterity and bimanual coordination [22]. The test involves two different abilities: gross movements of arms, hands, and fingers, and fine motor dexterity. The test consists of taking one peg at a time from a container and placing it into one of the holes on the board as quickly as possible with one hand. The score is expressed in the number of pegs placed in 30 seconds. In the present study, we use the sum of the scores for both hands (referred to as Purdue Combined). Poor Pegboard performance is a sign of deficits in complex, visually guided, or coordinated movements. The test is reported to have good test retest and inter-rater reliability [23, 24], but suffers from floor effects [21]. The Chedoke-McMaster Stroke Assessment Impairment Inventory is a measure used to assess physical
4 Mostafavi et al. Journal of NeuroEngineering and Rehabilitation (2015) 12:105 Page 4 of 12 Table 1 Abbreviations and description of robotic task parameters for three robotic tasks: visually guided reaching task, arm position matching task and ball drop object hit task Robotic Task Parameters Abbreviation Brief Description Visually Guided Reaching Reaction Time RA1* Time between illumination of the peripheral target and onset of movement First Movement Max. Speed RA2 Maximum hand speed during the participant s initial movement First Movement Distance RA3 Distance the hand traveled during the participant s initial movement First Movement Direction Error RA4 Angular deviation between (a) a straight line from the hand position at movement onset to the peripheral target and (b) a vector from the hand position at movement onset to the hand position after the initial phase of movement Total Movement Time RA5 Total time elapsed from movement onset to offset Path Length RA6 Total distance traveled by the hand between movement onset and offset Path Length Ratio RA7 Total distance traveled by the hand between movement onset and offset divided by the straight line distance. Movement Time Maximum Speed RA8 Maximum speed that the hand traveled during the entire reaching movement. Number of Movement Peaks RA9 Number of hand speed maxima between movement onset and offset Min. Max. Speed Difference RA10 Differences between local speed peaks and minima First Movement Maximum Speed Ratio RA11 Ratio of (a) the maximum hand speed during the participant s initial movement to (b) the global hand speed maximum of the trial First Movement Distance Ratio RA12 Ratio of (a) the distance the hand traveled during the participant s initial movement to (b) the distance the hand traveled between movement onset and offset Posture Speed RA13 Mean hand speed for 500 ms before peripheral target illumination Arm Position Matching Variability X (m) M1 Mean of standard deviation of the active hand s position over all target locations in the x direction Variability Y (m) M2 Mean of standard deviation of the active hand s position over all target locations in the y direction Variability XY (m) M3 Mean of standard deviation of the active hand s position over all target locations in the xy direction Contraction/expansion ratio X M4 Range/area of the workspace matched by the active hand relative to that of the passive hand in the x direction. Contraction/expansion ratio Y M5 Range/area of the workspace matched by the active hand relative to that of the passive hand in the y direction. Contraction/expansion ratio XY M6 Range/area of the workspace matched by the active hand relative to that of the passive hand in the xy direction. Shift X (m) M7 Mean of the mean error between the active and passive hands for each target location over all targets in the x direction. Shift Y (m) M8 Mean of the mean error between the active and passive hands for each target location over all targets in the y direction. Shift XY (m) M9 Mean of the mean error between the active and passive hands for each target location over all targets in the xy direction. Object Hit Total hits OH1 Number of balls that are hit and leave the display area of the subject s workspace Hits with Affected Arm OH2 Number of balls that are hit with the affected arm of stroke participants Hits with Unaffected Arm OH3 Number of balls that are hit with the unaffected arm of stroke participants Hand bias of hits OH4 Normalized difference between the total number of hits with right and left hands Miss bias OH5 Quantifies whether there was a spatial bias in position of balls missed in workspace Hand transition OH6 Line in the workspace where the participant s preference switches from one hand to the other Hand selection overlap OH7 Quantifies whether both hands share the workspace
5 Mostafavi et al. Journal of NeuroEngineering and Rehabilitation (2015) 12:105 Page 5 of 12 Table 1 Abbreviations and description of robotic task parameters for three robotic tasks: visually guided reaching task, arm position matching task and ball drop object hit task (Continued) Median error OH8 Point in the task where the participant missed half of the balls that they missed in the entire task as a percentage of the total number of balls Hand speed Affected Arm OH9 Average hand speed during the task for the affected arm of subjects with stroke Hand speed Unaffected Arm OH10 Average hand speed during the task for the unaffected arm of subjects with stroke Hand speed bias OH11 Normalized difference between mean hand speeds of the left and right hands Movement area Affected Arm OH12 Area of space used by the affected arm of subjects with stroke during the task Movement area Unaffected Arm OH13 Area of space used by the unaffected arm of subjects with stroke during the task Movement area bias OH14 Quantifies differences in the size of the workspace used by each hand *RA followed by a number is used for abbreviation of visually guided reaching task parameter on the affected arm. RU and RI followed by a number will be used for the same parameter measured on the unaffected side and the inter-limb difference, respectively impairment following stroke [18]. In the present study, we added the hand and arm impairment inventory scores, each evaluated on a 7-point scale [25] for both the affected and unaffected limbs (abbreviated to CMS- Affected and CMS-Unaffected, respectively). Spasticity at the elbow was assessed using the Modified Ashworth Scale [17]. It is an ordinal scale ([0, 1, 1+, 2, 3, 4]), with 0 representing no spasticity. The measurements were performed for the elbow at both the affected and unaffected limbs (abbreviated to MAS-Affected and MAS-Unaffected, respectively). The conventional subtests of the Behavioral Inattention Test (BIT) are basic pencil and paper measures to screen for visuospatial neglect [26]. A score at or below 129 is indicative of visuospatial neglect. Data analysis We used a normalization scheme to scale all KINARM metrics to values between 0 and 1. The minimum (x min ) and maximum (x max ) value of each metric (x) are used to obtain a normalized value, (z(x)), as follows: zx ðþ¼ x x min x max x min ð1þ This normalization procedure was previously found to result in more accurate classification results for stroke/ control subjects classification than a regime based on centering and scaling [27]. A system identification method known as Fast Orthogonal Search (FOS) [28] was used to identify the most informative clinical and robotic metrics that contribute towards prediction of FIM scores at approximately 2 weeks and 3 months post stroke. FOS allows for identification of a non-linear approximation consisting of terms with the highest contribution towards prediction of a desired target value [28]. In this study, the measured FIM score at approximately 2 weeks and 3 months post stroke, denoted by S, was used as the target value in a FOS training algorithm to form a sum of M non-linear basis functions p m (n) with coefficients a m and estimate error e(n) as follows a m m¼1 S ¼ X M p m ðnþþen ð Þ ð2þ The FOS training algorithm searches through all N input candidate basis functions, where N> > M and iteratively picks those candidates which contribute the largest mean square error (MSE) error reduction between the model estimate and the actual data (S). This method is based on the theory of Gram-Schmidt orthogonal identification, whereby orthogonal basis functions are generated from the p m (n) and coefficients are found such that the MSE of the estimate is minimized [28]. The first function selected by any model using FOS is assigned a value of 1, with a coefficient term that accounts for the constant term in the model. Following this first iteration, all subsequent basis functions are chosen from the provided pool of candidates. Non-linearity was introduced into our predicted models by including squared, cubic, sin, cosine, and logarithmic functions of the robotic metrics. A detailed description of this method is presented in [28]. FIM-related predicted measures in this study were FIM-Motor and FIM-Total at entrance to the study approximately two weeks post-stroke (FIM-Motor-2w and FIM-Total-2w) and at approximately three months poststroke (FIM-Motor-3 m and FIM-Total-3 m). If a score
6 Mostafavi et al. Journal of NeuroEngineering and Rehabilitation (2015) 12:105 Page 6 of 12 is predicted to be outside the valid range of FIM values (e.g. <18 and >126 for FIM-Total), the predicted value is adjusted to be the minimum or maximum valid score for scores below and above the valid range, respectively. Performance Measure All models were evaluated by a 10-fold cross validation procedure using 90 % of the subjects data to train the model with the remaining 10 % for model testing. Overall model performance is the average of the performance of test data over the 10 folds. To decide on the optimal number of parameters for model generalization a total of 15 models consisting of 1 to 15 basis functions were tested for each prediction. Consequently, the models that generalize best on unseen data were used as the optimal model. The addition of a higher number of basis functions results in a decrease in the models performance on unseen validation data due to model over-fitting. The optimal number of metrics for each estimated model is reported for each model. Performance of predicted clinical measures is reported as the R value between the actual and predicted values. R is a value between 0 and 1 and can be interpreted as the correlation coefficient between actual and predicted values, indicating the goodness of fit for such values. Moreover, the value of R 2 can be used to interpret the fraction of unexplained variance in data, since it compares the variance of the model s errors with the total data variance. Datasets for model generation We employed both robotic and clinical biomarkers to build predictive models. Robotic biomarkers included the Reaching task parameters recorded for the affected and unaffected arm, henceforth referred to as Reachaffected and Reach-unaffected. The set of reaching parameters describing the interlimb difference is referred to as Reach-Interlimb. A single set of data describes Matching task parameters, referred to as Match. Parameters associated with the Object Hit task are referred to as Object Hit. The last robotic dataset, All Robotic Data, contains all reaching, matching, and object hit parameters. Clinical biomarkers are comprised of FIM-2w and a set including the Chedoke-McMaster Score, Purdue Pegboard Score, BIT Score and Modified Ashworth Score. This latter set included measures for both affected and unaffected arms, henceforth referred to as Clinicalaffected and Clinical-unaffected. Another set containing both Clinical-affected and Clinical-unaffected, henceforth referred to as Clinical-All, was also used for model generation. For the case of each FIM prediction, all parameters in the above mentioned sets of biomarkers (i.e. robotic or clinical) were used as the candidate basis functions for the FOS training algorithm as described above. The FOS training algorithm then picks the parameters within each dataset based on their contribution towards minimizing the prediction error (as measured by MSE) for prediction of each FIM score. Results Participant Pool Demographics data on the participants age, gender, type of stroke, as well as the distribution of clinical scores is provided in Table 2. Clinical and robotic assessments were carried out on 85 patients with stroke (49 left- and 33 right-affected, 61 with ischemic and 24 with hemorrhagic stroke). The youngest participant was aged 25, and the oldest was 82 years old, and the average age was approximately 61 years. The range of clinical scores that are covered in this study are also presented in Table 2. Estimates of FIM-2w Scores from Robotic and non- Robotic Data Our first analysis focused on estimation of FIM-2w scores from robotic and non-robotic biomarkers. R values for estimation of FIM-Motor-2w and FIM-Total- 2w scores are shown in Table 3. Our results show that the largest R values for prediction of FIM-2w scores are Table 2 Demographics and Clinical Data Measure Quantity Number of Subjects 85 Male/Female 57/28 Affected Limb (Left-side/Right-side/Both) 49/33/3 Type of stroke (Ischemic/Hemorrhagic) 61/24 Age in years (60.6, 12.5, 25, 82) a Days since stroke to first FIM (8.1, 4.5, 1, 14) a Days since stroke to second FIM (89.6, 8.9, 68, 125) a FIM-Motor-2w score (66.5, 21.5, 13, 91) a FIM-Total-2w score (96.3, 24.3, 37, 126) a FIM-Motor-3 m score (85.9,10.1,27,91) a FIM -Motor-3 m score (118.5,12.8,45,126) a Purdue Pegboard Score - Combined (14.9, 6.0, 4, 28.5) a BIT score (133.8, 19.1, 63, 146) a Modified Ashworth Score - Affected Arm (70, 5, 4, 6, 0, 0) b Modified Ashworth Score - Unaffected Arm (83, 2, 0, 0, 0, 0) b Chedoke McMaster Score - Affected Arm (11, 9, 8, 3, 16, 8,30) c Chedoke McMaster Score - Affected Hand (14, 4, 5, 6, 16, 23, 16) c Chedoke McMaster Score - Unaffected Arm (0, 0, 0, 0, 4, 11, 70) c Chedoke McMaster Score - Unaffected Hand (0, 0, 0, 0, 3, 24, 58) c a Formatting represents (Average, Standard Deviation, Minimum, Maximum) b Formatting represents number of participants with Modified Ashworth Score of (0, 1, 1+, 2, 3, 4) c Formatting represents number of participants with Chedoke McMaster Score of (1, 2, 3, 4, 5, 6, 7)
7 Mostafavi et al. Journal of NeuroEngineering and Rehabilitation (2015) 12:105 Page 7 of 12 Table 3 R values for prediction of FIM-related scores at 2 weeks and 3 months post-stroke using clinical and robotic data (validation results) FIM-Motor-2w FIM-Total-2w FIM-Motor-3 m FIM-Total-3 m 1 Reach-Affected Reach-Unaffected Reach-Interlimb Match Object-Hit All Robotic Data FIM-2w Purdue-Combined Chedoke-Affected Chedoke-Unaffected BIT score Clinical-Affected Clinical-Unaffected Clinical-All For dataset abbreviations (rows), see the Methods section achieved using the Clinical-all dataset (0.829 and for FIM-Motor-2w and FIM-Total-2w, respectively). R values for the robotic datasets also show high correlations of and for FIM-Motor-2w and FIM- Total-2w, respectively. R values for the Object Hit dataset are almost as large as for the All Robotic Data. Table 4 displays statistical comparisons between R values obtained for some of the best datasets to predict FIM-2w scores. The difference in R values between All Robotic Data and Clinical-All is not significant (P > 0.05). Estimates of FIM-Motor-2w was better for the Clinical-All and the Clinical-Affected datasets than for the Object Hit dataset (p = for Clinical-All and p = for Clinical-Affected), but not for the FIM-Total-2w. Table 5 and 6 shows the model parameters for predictions of FIM-2w scores using All Robotic Data (top) and Clinical-All (bottom). Our models generated by FOS generalize the best using 2 basis functions for both FIM- Motor-2w and FIM-Total-2w for the Clinical-All dataset. The models performance drops on unseen validation data when including higher number of functions due to model overfitting. Basis functions are reported in Table 5 and 6 by the order in which they are selected by FOS. Thus, the first chosen basis function is the one that contributes the most to the value of the estimated model. rates for each model parameter is generated by repetitively constructing optimal models using a randomly selected 90 % subset of the original data for 100 repeats and reporting how many times each metric is picked by FOS. For FIM-Motor-2w and FIM-Total-2w, the first dominant metric contributing to the model estimation is the Chedoke-McMaster Score-Affected, and the second dominant metric is associated with the Purdue Pegboard Score. For predictions of FIM scores using robotic data, the best generated models generalize best using four and five parameters for FIM-Total-2w and FIM-Motor-2w, respectively. The first dominant metric contributing to the estimation of both FIM-Total-2w and FIM-Motor-2w is associated with the arm-position Matching task (M3: Variability XY). The second and third dominant metrics are also parameters associated with arm-position Matching task (M5: Contraction/Expansion XY) and two metrics associated with the Object-Hit task (OH11: Hand speed bias, OH14: Movement Area Bias). Table 4 P-values for comparison of R values between datasets Dataset 1 Dataset 2 FIM-Motor-2w FIM-Total-2w FIM-Motor-3 m FIM-Total-3 m 1 Object-Hit FIM-2w Object-Hit Clinical-All All Robotic Data FIM-2w All Robotic Data Clinical-All p values < 0.05 is shown in bold
8 Mostafavi et al. Journal of NeuroEngineering and Rehabilitation (2015) 12:105 Page 8 of 12 Table 5 Robotic Metrics for Prediction of FIM-related Scores and their Corresponding Rates out of 100 s for Each Model Estimation Top: predictions using robotic data Number of model parameters First Metric Second Metric Third Metric Fourth Metric Fifth Metric Sixth Metric FIM-Motor-2w 5 M3 81 OH11 26 M5 45 OH1 33 OH11 23 N/A N/A RA5 12 OH12 16 OH1 24 M5 21 RA1 16 RA9 4 OH14 15 OH12 6 OH12 8 M9 10 FIM-Total-2w 4 M3 95 M5 55 OH14 37 M9 28 N/A N/A N/A N/A RA9 5 OH6 17 OH11 22 OH1 25 OH1 12 OH12 17 M5 19 FIM-Motor-3 m 6 OH12 76 OH13 73 RA11 59 OH5 37 RA11 49 OH5 28 RA4 11 RA4 18 OH13 16 RA11 12 OH5 16 RA4 18 OH13 5 OH12 6 OH7 8 OH7 11 RA4 11 RA11 8 FIM-Total-3 m 5 OH12 75 OH13 78 RA11 63 RA7 34 M9 27 N/A N/A OH11 10 RA11 9 OH5 7 OH7 12 OH5 18 OH9 9 OH12 8 RA7 5 M9 11 M6 11 Estimates of FIM-3 m Scores from Robotic and non-robotic Data We next examined the estimation of FIM-3 m scores from robotic and non-robotic biomarkers. The best performance in terms of R values for prediction of FIM-3 m scores are achieved using the All Robotic datasets (0.694 and for FIM-Motor-3 m and FIM-Total-3 m, respectively). This is followed by the R values obtained using the Clinical-All dataset (0.626 and for FIM- Motor-3 m and FIM-Total-3 m, respectively). Also predictions of FIM-Motor-3 m and FIM-Total-3 m using the respective FIM-2w scores had R values of and 0.599, respectively. Table 4 highlights that there are no statistical differences between predictions of FIM-3 m scores generated from the Clinical-All, All Robotic Data and the FIM-2w datasets. Table 5 and 6 displays the key biomarkers that contribute to each model estimation. For FIM-Motor-3 m and FIM-Total-3 m, the dominant first and second metrics are associated with the Object Hit task for both model estimations, while the third dominant parameter is associated with the Reaching task (affected side data). This is consistent with our results in Table 3, where Object Hit parameters resulted in models that generalized better for prediction of FIM scores at both 2 weeks and three months post-stroke. The dominant Object Hit parameters include Movement Area-Affected Arm (OH12) and Movement Area-Unaffected Arm (OH13) for both Table 6 Robotic Metrics for Prediction of FIM-related Scores and their Corresponding Rates out of 100 s for Each Model Estimation Bottom: predictions using clinical data Number of model First Metric Second Metric Third Metric parameters FIM-Motor-2w 2 CM-A 100 PP 98 N/A N/A CM-U 2 FIM-Total-2w 2 CM-A 97 PP 96 N/A N/A PP 3 CM-A 3 CM-U 1 FIM-Motor-3 m 3 PP 100 CM-A 85 PP 75 CM-U 15 CM-A 16 CM-U 10 FIM-Total-3 m 3 PP 100 CM-A 89 CM-A 43 PP 7 CM-U 37 CM-U 4 PP 20 PP Purdue Pegboard Score- Combined, CM-A Chedoke-McMaster Score-Affected Arm, CM-U Chedoke-McMaster Score-Unaffected Arm For abbreviations of robotic parameters, see Table 1.
9 Mostafavi et al. Journal of NeuroEngineering and Rehabilitation (2015) 12:105 Page 9 of 12 FIM-Motor-3 m and FIM-Total-3 m predictions. Reaching task parameters used for both predictions include First Movement Direction error (RA4), First Movement Maximum Speed Ratio (RA11), and Path Length Ratio (RA7). Models that used clinical data for estimation of FIM- Motor-3 m and FIM-Total-3 m scores generalize with three parameters for both scores. Similar to predictions of scores at 2 weeks post stroke, FIM-3 m estimations are best predicted using a combination of Purdue Pegboard and Chedoke-McMaster assessment scores. However, for FIM-3 m predictions the first dominant metric is associated with the Purdue Pegboard test for both FIM-Motor-3 m and FIM-Total-3 m. The second dominant metric is associated with the Chedoke-MacMaster score, affected side. These results are consistent with our finding presented in Table 7, where both Purdue Pegboard and Chedoke MacMaster-affected side show moderate correlation values for prediction of FIM-3 m scores. Estimating Clinical Scores from Robotic Data Our next analysis examines the relationship between robotic and clinical measures of upper limb function. Table 7 shows validation results (data not used to develop the models) using robot-based tasks to estimate the traditional clinical scores using Reaching, Matching, Object Hit, and All Robotic data. R values for prediction of Purdue-Combined and CMS-Affected using Reaching task parameters show high correlations (0.778 and 0.775). Predictions using All Robotic Data are slightly improved by inclusion of Object Hit and Matching data (0.791 and 0.810). Also the predictions of BIT score using robotic data shows moderate correlations with each set of robotic task data and a relatively high R value of when using All Robotic Data. All R values except for the Chedoke-McMaster Score-Unaffected were significant at P < The correlation values for the Modified Ashworth Score are low (R = and for affected and unaffected arms, respectively). This is in line with the findings in [29] for the Modified Ashworth score, where they report R = for validation data for predictions made using robot-based kinematics. Table 7 also shows the key robotic biomarkers for prediction of these clinical scores. The dominant first and second robotic metrics for prediction of Purdue- Combined and CMS-Affected are both associated with the Reaching (RA12 and RA5) and Object Hit (OH1 and OH8) task, while there is some small contribution from the Matching task as the third metric. For prediction of BIT score, the major contributions are from the Matching (M2) and Reaching task (RA11 and RA6), with Table 7 R Values on Validation Data for Robot-Based Models to Predict Other Clinical Scores and the Robotic Metrics Associated with the Model Based on All Robotic Data Reaching Matching Object Hit All Robotic Data First Metric Second Metric Third Metric Purdue-Combined RA12 61 % OH1 48 % M9 31 % OH1 28 % RA2 24 % OH8 21 % RA5 10 % M3 17 % RA3 12 % CMS-Affected RA5 63 % RA3 46 % OH13 39 % R12 21 % OH8 31 % M1 28 % RA3 11 % RA2 13 % RA2 19 % CMS-Unaffected 0.096(NS) 0.006(NS) 0.043(NS) 0.097(NS) OH1 18 % OH2 21 % N/A N/A M8 16 % M4 13 % M4 12 % RA5 10 % MAS-Affected (NS) 0.038(NS) RA1 45 % OH8 30 % N/A N/A OH8 21 % RA9 22 % OH1 13 % M8 10 % MAS-Unaffected 0.193(NS) 0.063(NS) OH14 32 % RA12 27 % N/A N/A OH7 24 % M1 19 % RA12 11 % RA5 11 % BIT Score M2 48 % RA6 38 % OH8 31 % RA11 30 % RA3 26 % OH1 25 % RA3 14 % M2 20 % M1 17 % Matching Arm position matching task, Reaching visually-guided reaching task, affected, unaffected and interlimb parameters, Object Hit Ball drop object hit task, CMS Chedoke-MacMaster Score, MAS Modified Ashworth Score, NS Not significant for P < For abbreviations of robotic metrics see Table 1
10 Mostafavi et al. Journal of NeuroEngineering and Rehabilitation (2015) 12:105 Page 10 of 12 smaller contributions from the Object Hit tasks as the third metric. Discussion The purpose of the present study was to identify the biomarkers of sensory and motor function of the arms at approximately 2 weeks post-stroke to estimate present and future FIM scores. Our results highlight that robotic and non-robotic assessments were not statistically different when predicting FIM-2w and FIM-3 m scores. There was a general trend towards better estimates for clinical biomarkers to predict FIM-2w scores and robotic biomarkers to predict FIM-3 m scores. Importantly, robot-based biomarkers of proprioceptive function were influential for predicting FIM scores at 2 weeks, whereas biomarkers related to rapid bimanual motor function were influential for predicting FIM scores at 3months. Robot-based measures predicted Purdue Pegboard and Chedoke-McMaster Scores with high R values of ~0.8 for the affected limb within approximately 2 weeks poststroke. Our predicted R value for the Chedoke-McMaster score is statistically higher than the results obtained in [29] for robot-based estimates of the Fugl-Meyer Assessment and Motor Power (0.427 and respectively, on validation data). The fact that the prediction of these two clinical scores is attributed to robotic parameters associated with the Reaching and Object Hit tasks is in line with the observation that these two clinical tests are predominantly dependant on motor skills. Our improved estimates likely reflect two distinct factors. First, our mathematical models using FOS can consider non-linear relationships rather than simple linear regressions. Secondly, our range of robotic tasks covered a broader range of assessments of brain deficits including bimanual rapid visuomotor and proprioceptive tasks. While correlations were generated largely from measures of visual-guided reaching performance, there was some contribution from the limb matching and object hit tasks. R values associated with prediction of BIT scores are also relatively high (0.678 using all sets of robotic data). Previous studies have reported significant correlations between BIT and some robot-based metrics associated with motor function [30] (correlations as high as 0.50) and proprioceptive deficits [31] (correlations as high as -0.55) following stroke. In the present study we directly attempted to develop models to predict measures of spatial neglect using robot-based evaluation metrics for subjects with stroke. The correlation associated with BIT was attributed to measures of limb position matching and reaching performance with a smaller amount of contribution from the object hit task. This is in line with the inherent characteristics of reaching task, which quantifies reaching performance across targets at 8 different spatial locations and limb position matching task, which assesses sense of position across 9 different spatial targets. Predictions of Modified Ashworth Scores resulted in poor prediction performance for both affected and unaffected limbs (0.235 and 0.266, respectively). These results conform to the findings of [29] (0.171 on validation data), although our R values are found to be statistically significant for P < 0.005, which may be attributed to our non-linear modeling approach. The ability of non-robotic assessment measures to predict FIM-2w scores better than robot-based measures may be related to the impact of weakness on subject performance. Weakness is commonly observed post-stroke, and when severe, makes it impossible to perform any motor activity due to gravitational forces impeding goaldirect movements of the limb. This would directly impact the ability to perform daily activities as measured by FIM, as well as performance in the Purdue pegboard test and the Chedoke-McMaster test. In contrast, the robotic device provided weight support of the arms. Thus, a subject unable to lift their arms due to weakness may still be able to perform reaching and object hit movements to a certain degree. It is interesting to note that the dominant robot-based biomarker to predict FIM-2w scores was related to proprioceptive function from the arm position matching task. Our previous study using this task identified high correlation between FIM scores and matching task parameters [25]. This suggests that proprioceptive function is important to plan and control many activities of daily living, such as grooming, eating and bathing. Moreover, proprioceptive deficits in the arm and leg are correlated [32], and thus, may indirectly predict difficulties in performing lower limb activities such as locomotion. Also, it has been noted previously that proprioceptive deficits do not correlate with motor skills such as reaching post stroke [9]. This explains the presence of additional nonmatching task parameters in models for predicting FIM- 2w scores. Over the course of rehabilitation between first and second FIM measurements, the prediction of FIM-3 m scores using robot-based measures was slightly, although not statistically, better than clinical scores and FIM scores measured at 2 weeks. The dominant parameters attributed to the prediction of FIM-3 m are associated with the object hit task. The selected parameters in the robot-based models provide some insight as to the relative success of the robot-assessment to predict future abilities to perform daily activities. First, Movement Area by both affected and unaffected hands from the object hit task were the most commonly selected parameters when developing models to predict future FIM scores. This is consistent with our understanding of the ability to perform daily activities, as the wider span of hand
11 Mostafavi et al. Journal of NeuroEngineering and Rehabilitation (2015) 12:105 Page 11 of 12 movements can prove to amount to a higher level of independence during activities of daily living. In general, dominance of object hit task parameters for prediction of future FIM scores highlights the fact that weakness in moving would amount to subjects not being able to quickly move arms for success on the object hit task. Moreover, the majority of parameters on the object task have inter-rater reliability scores above the statistically accepted norm of 0.8 [14]. Second, the relative success to predict future FIM scores may be related to the fact that robot-based models commonly selected parameters that characterize differences in limb movement, measures that compared object hit performance between the affected and unaffected limb. This includes parameters such as Miss bias, Hand speed bias and Hand selection overlap. These interlimb measures neutralize differences in each subject s motor strategy, making it easier to capture differences in motor capabilities between the limbs. Third, the fact that the robot provided weight support for the limb may have reduced their ability to predict FIM-2w scores, but paradoxically may have improved its ability to predict FIM 3 m scores. Many subjects with stroke and motor deficits will improve strength with time. By alleviating weight support, the robot-based tasks assess other aspects of sensorimotor function beyond strength, allowing us to uncover other important impairments that can impact long term abilities to perform daily activities. A recent study similar in nature to the present study was performed by Krebs, et al. [33]. They used a neural network technique to construct mathematical models for prediction of a set of clinical scores including Fugl-Meyer, National Institute of Health Stroke Scale, and Motor Power based on robotic measurements. This study was performed for a group of completers (who had complete data for days 7 and 90 after stroke) and non-completers (who had some missing data on day 7 or 90). The main difference between that study and the present one is that the robotic data used for model generation for that study are collected at the same time as robotic evaluation. In contrast, our study uses data collected at day 14 to make predictive models on FIM measurements approximately 3 months post stroke. Reported R 2 values in that study range from for the non-completer group and for the completer group. Thus, our estimates of future FIM scores are relatively good given the challenge of predicting FIM scores several months in the future and following rehabilitation therapy. One of the limitations of our present study is the absence of behavioral tasks for assessment of cognitive brain function. FIM-Total is comprised of 5 items for assessment of cognition including memory, problem solving, and concentration. Robot-based predictions of FIM-Total- 2w tended to be better for than for FIM-Motor-2w, suggesting cognitive impairments likely impact performance in these tasks. Importantly, one of the advantages provided by robotic assessment is the potential to study behavioral tasks to quantify impairments in a broad range of sensory, motor and cognitive functions. We have recently developed several other tasks to assess sense of limb motion [10], ability to use sensory feedback for postural control [34] and bimanual motor function [35]. As well, we have developed more cognitively demanding tasks on the robotic system. An extension of the object hit task used in the present study is an object hit and avoid task, which requires additional cognitive processing to attend to the appropriate targets and inhibitory control to avoid distractors present in the workspace. Moreover, the pen-and-paper Trail Making test [36] that examines task switching has also been implemented on the robotic platform. When data on these tasks are added to the analysis, we expect that we will be able to make improved predictions on the ability of subjects to perform daily activities, as measured by the FIM, both at the present and in future time points. One of the advantages of using robotic technologies for prediction of FIM scores lies in the ability to discover the parameters that are most selected in the models to improve the predictions of FIM. This has the potential to ultimately lead to a better understanding of the underlying changes through the rehabilitation process that may, in turn, lead to improved patient care. Given the limited amount of available data and related studies in the use of robotic technologies for post-stroke neurorehabilitation, our collective analysis suggests that robotic technologies may enable early decision support in clinical assessment, reduce the amount of time required for assessment, and offer a reliable tool for monitoring of longitudinal changes for stroke survivors in conjunction with the current clinical scales. With addition of extra data for assessment of other areas of brain dysfunction, we expect to come up with improved decisions for patient care. The present study serves as a proof of principle, with the addition of other forms of data providing extra benefits. Conclusions The present study used biomarkers generated from a set of three behavioral robotic tasks to estimate measures of daily activities pre- and post-rehabilitation. Findings of the study highlight that robot-based metrics provide an accurate estimate of future FIM scores, in line with estimates provided by clinical scores at approximately 2 weeks post-stroke. While the findings of this study provide a proof of principle for use of robotic tools in clinical decision support, addition of other behavioral tasks on the robotic settings is expected to provide more accurate predictions in the future.
12 Mostafavi et al. Journal of NeuroEngineering and Rehabilitation (2015) 12:105 Page 12 of 12 Abbreviations FOS: fast orthogonal search; FIM: functional independence measure; FIM- 2w: functional independence measure assessed 2 weeks post-stroke; FIM- 3 m: functional independence measure assessed 3 months post-stroke; CMS: chedoke mcmaster score; MAS: modified ashworth score; BIT: behavioral inattention test; KINARM: kinseological instrument for normal and altered reaching movement. Competing interests Dr. Scott is Co-founder and Chief Scientific Officer of BKIN technologies, the company which manufactures the KINARM robotic device. The other authors have no conflicts. The other authors have no competing interests to declare. Authors contributions SMM analyzed the collected data, carried out the statistical analysis and computational modelling, and drafted the manuscript. SPD contributed to the study design, data collection and authorship of the manuscript. PM contributed to the design of the study and data analysis. SHS participated in the design of the study and robotic tasks, data analysis, and drafting of the manuscript. All authors read and approved the final manuscript. Acknowledgements We wish to thank Helen Bretzke, Kim Moore, Megan Metzler, Mark Piitz, Janice Yajure, and Justin Peterson for providing technical help with data preparation and processing for this study. This work was supported by CIHR Operating grants (MOP , MOP and NSP ), an NSERC Strategic grant ( ), a Heart and Stroke Foundation of Alberta, Northwest Territories and Nunavut Grant-in- Aid, an Ontario Research and Development Research Excellence Award, the Hotchkiss Brain Institute, a Heart and Stroke Foundation of Alberta, Northwest Territories and Nunavut Investigatorship in Stroke Rehabilitation Research to SPD and a GSK-CIHR Chair in Neuroscience to author SHS. Author details 1 School of Computing, Queen s University, Kingston, ON, Canada. 2 Hotchkiss Brain Institute, University of Calgary, Calgary, AB, Canada. 3 Department of Biomedical and Molecular Sciences, Queen s University, Kingston, ON, Canada. 4 Providence Care, St. Mary s of the Lake Hospital, Kingston, ON, Canada. 5 Centre for Neuroscience Studies, Queen s University, Kingston K7L 3N6ON, Canada. Received: 29 May 2015 Accepted: 23 November 2015 References 1. Keith RA, Granger CV, Hamilton BB, Sherwin FS. The functional independence measures: a new tool for rehabilitation. Adv Clin Rehabil. 1987;1: Heinemann AW, Linacre JM, Hamilton BB. Prediction of rehabilitation outcomes with disability measures. Arch Phys Med Rehabil. 1994;75: Chumney D, Nollinger K, Shesko K, Skop K, Spencer M, Newton RA. Ability of functional independence measure to accurately predict functional outcome of stroke-specific population: Systematic review. Journal of Rehabilitation Research & Development. 2010;47(1): Gialanella B, Santoro R. Prediction of functional outcomes in stroke patients: the role of motor patterns according to limb synergies. Aging Clin Exp Res. 2015;27(5): Levin MF, Kleim JA, Wolf SL. What do motor recovery and compensation mean in patients following stroke? Neurorehabil Neural Repair. 2009;23(4): Kwakkel G, Kollen B, Lindeman E. Understanding the pattern of functional recovery after stroke: facts and theories. Restor Neurol Neurosci. 2004;22(3): Burke Quinlan E, Dodakian L, See J, McKenzie A, Le V, Wojnowicz M, et al. Neural function, injury, and stroke subtype predict treatment gains after stroke. Ann Neurol. 2015;77: Kenzie JM, Semrau JA, Findlater SE, Herter TM, Hill MD, Scott SH, et al. Anatomical correlates of proprioceptive impairments following acute stroke: A case series. J Neurol Sci. 2014;342(1): Dukelow SP, Herter TM, Bagg SD, Scott SH. The independence of deficits in position sense and visually guided reaching following stroke. J NeuroEngineering and Rehabilitation. 2012;9: Semrau JA, Herter TM, Scott SH, Dukelow SP. Robotic identification of kinesthetic deficits after stroke. Stroke. 2013;44(12): Coderre AM, Zeid AA, Dukelow SP, Demmer MJ, Moore KD, Demers MJ, et al. Assessment of upper-limb sensorimotor function of subacute stroke patients using visually-guided reaching. Neurorehabil Neural Repair. 2010;24(6): Scott SH. Apparatus for measuring and perturbing shoulder and elbow joint positions and torques during reaching. J Neurosci Methods. 1999;89(2): Dukelow SP, Herter TM, Moore KD, Demers MJ, Glasgow JI, Bagg SD, et al. Quantitative assessment of limb position sense following stroke. Neurorehabil Neural Repair. 2010;24(2): Tyryshkin K, Coderre AM, Glasgow JI, Herter TM, Bagg SD, Dukelow SP, et al. A robotic object hitting task to quantify sensorimotor impairments in participants with stroke. J NeuroEng Rehabil. 2014;11(1): Ottenbacher K, Hsu Y, Granger C, Fiedler R. The reliability of the functional independence measure: a quantitative review. Arch Phys Med Rehabil. 1996;77(12): Strauss E. A Compendium of Neuropsychological Tests: Administration, Norms, and Commentary. New York: Oxford University Press, 2006; pp ISBN Bohannon RW, Smith MB. Inter-rater reliability of a Modified Ashworth Scale of muscle spasticity. Phys Ther. 1987;67: Gowland C, Stratford P, Ward M. Measuring physical impairment and disability with the Chedoke-McMaster Stroke Assessment. Stroke. 1993;24(1): Kidd D, Stewart G, Baldry J, Johnson J, Rossiter D, Petruckevitch A, et al. The Functional Independence Measure: a comparative validity and reliability study. Disabil Rehabil. 1995;17(1): Cohen M, Marino R. The tools of disability outcomes research functional status measures. Arch Phys Med Rehabil. 2000;81 Suppl 2:S Sunderland A, Tinson D, Bradley L, Hewer RL. Arm function after stroke. an evaluation of grip strength as a measure of recovery and a prognostic indicator. J Neurol Neurosurg Psychiatry. 1989;52(11): Bode RK, Heinemann AW, Semik P, Mallinson T. Relative importance of rehabilitation therapy characteristics on functional outcomes for persons with stroke. Stroke. 2004;35(11): Radomski MV, Trombly Latham CA. Occupational Therapy for Physical Dysfunction. Lippincott Williams & Wilkins. 2008; pp ISBN Chen HM, Chen CC, Hsueh IP, Huang SL, Hsieh CL. Test-retest reproducibility and smallest real difference of 5 hand function tests in patients with stroke. Neurorehabil Neural Repair. 2009;23(5): Brunnstrom S. Movement Therapy in Hemiplegia: A Neurolophysiological Approach. New York: Harper and Row Publishers; Wilson B, Cockburn J, Halligan P. Development of a behavioral test of visuospatial neglect. Arch Phys Med Rehabil. 1987;68: Chalmers N, Seaborn G, Jung JY, Glasgow JI, Scott SH. Recombination of common sensory-motor impairment evaluation techniques using a committee of classifiers. In: Annual conference of the IEEE of the engineering in medicine and biology society. Minneapolis, MN. 2009; Korenberg MJ. A robust orthogonal algorithm for system identification. Biol Cybern. 1989;60: Boesecker C, Dipetro L, Volpe B, Krebs HI. Kinematic robot-based evaluation scales and clinical counterparts to measure upper limb performance in patients with chronic stroke. Neurorehabil Neural Repair. 2010;24: Smith DL, Akhtar AJ, Garraway WM. Proprioception and spatial neglect after stroke. Age Ageing. 1983;12: Semrau JA, Wang JC, Herter TM, Scott SH, Dukelow SP. Relationship Between Visuospatial Neglect and Kinesthetic Deficits After Stroke. Neurorehabil Neural Repair. 2014;29(4): Busse M, Tyson SF. How many body locations need to be tested when assessing sensation after stroke? An investigation of redundancy in the Rivermead Assessment of Somatosensory Performance. Clin Rehabil. 2009;23: Krebs HI, Krams M, Agrafiotis DK, DiBernardo A, Chavez JC, Littman GS, et al. Robotic measurement of arm movements after stroke establishes biomarkers of motor recovery. Stroke. 2014;45(1): Bourke TC, Coderre AM, Bagg SD, Dukelow SP, Norman KE, Scot SH. Impaired corrective responses to postural perturbations of the arm in individuals with subacute stroke. J Neuroeng Rehabil. 2015;12(1): Lowrey CR, Jackson CPT, Bagg SD, Dukelow SP, Scott SH. A Novel Robotic Task for Assessing Impairments in Bimanual Coordination Post-Stroke. Int J Phys Med Rehabil. 2014;S3: Reitan, RM. Trail making test. Reitan Neuropsychology Laboratory, 1992.
Prediction of Stroke-related Diagnostic and Prognostic Measures Using Robot-Based Evaluation
 2013 IEEE International Conference on Rehabilitation Robotics June 24-26, 2013 Seattle, Washington USA Prediction of Stroke-related Diagnostic and Prognostic Measures Using Robot-Based Evaluation Sayyed
2013 IEEE International Conference on Rehabilitation Robotics June 24-26, 2013 Seattle, Washington USA Prediction of Stroke-related Diagnostic and Prognostic Measures Using Robot-Based Evaluation Sayyed
Evaluation of New Parameters for Assessment of Stroke Impairment
 Evaluation of New Parameters for Assessment of Stroke Impairment Kathrin Tyryshkin a, Janice I. Glasgow a and Stephen H. Scott b a School of Computing, Queen s University, Kingston, ON. Canada; b Department
Evaluation of New Parameters for Assessment of Stroke Impairment Kathrin Tyryshkin a, Janice I. Glasgow a and Stephen H. Scott b a School of Computing, Queen s University, Kingston, ON. Canada; b Department
The independence of deficits in position sense and visually guided reaching following stroke
 Dukelow et al. Journal of NeuroEngineering and Rehabilitation 12, 9:72 JOURNAL OF NEUROENGINEERING JNERAND REHABILITATION RESEARCH Open Access The independence of deficits in position sense and visually
Dukelow et al. Journal of NeuroEngineering and Rehabilitation 12, 9:72 JOURNAL OF NEUROENGINEERING JNERAND REHABILITATION RESEARCH Open Access The independence of deficits in position sense and visually
Impaired corrective responses to postural perturbations of the arm in individuals with subacute stroke
 Bourke et al. Journal of NeuroEngineering and Rehabilitation 215, 12:7 JOURNAL OF NEUROENGINEERING JNERAND REHABILITATION RESEARCH Impaired corrective responses to postural perturbations of the arm in
Bourke et al. Journal of NeuroEngineering and Rehabilitation 215, 12:7 JOURNAL OF NEUROENGINEERING JNERAND REHABILITATION RESEARCH Impaired corrective responses to postural perturbations of the arm in
Characterizing the timecourse and magnitude of sensorimotor
 Examining Differences in Patterns of Sensory and Motor Recovery After Stroke With Robotics Jennifer A. Semrau, PhD; Troy M. Herter, PhD; Stephen H. Scott, PhD; Sean P. Dukelow, MD, PhD Downloaded from
Examining Differences in Patterns of Sensory and Motor Recovery After Stroke With Robotics Jennifer A. Semrau, PhD; Troy M. Herter, PhD; Stephen H. Scott, PhD; Sean P. Dukelow, MD, PhD Downloaded from
Dominican Scholar. Dominican University of California. Jason Ichimaru Dominican University of California
 Dominican University of California Dominican Scholar Occupational Therapy Critically Appraised Papers Series Occupational Therapy 2017 Critcally Appraised Paper for: Is modified constraint-induced movement
Dominican University of California Dominican Scholar Occupational Therapy Critically Appraised Papers Series Occupational Therapy 2017 Critcally Appraised Paper for: Is modified constraint-induced movement
Characterizing the timecourse and magnitude of sensorimotor
 Examining Differences in Patterns of Sensory and Motor Recovery After Stroke With Robotics Jennifer A. Semrau, PhD; Troy M. Herter, PhD; Stephen H. Scott, PhD; Sean P. Dukelow, MD, PhD Background and Purpose
Examining Differences in Patterns of Sensory and Motor Recovery After Stroke With Robotics Jennifer A. Semrau, PhD; Troy M. Herter, PhD; Stephen H. Scott, PhD; Sean P. Dukelow, MD, PhD Background and Purpose
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION Is mirror therapy more effective in a, or individually, on sensorimotor function, activities of daily living, quality of life, and visuospatial neglect
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION Is mirror therapy more effective in a, or individually, on sensorimotor function, activities of daily living, quality of life, and visuospatial neglect
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION Is mirror therapy an effective intervention for improving function in paralyzed upper extremities after a stroke as compared to the standard therapy? Dohle,
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION Is mirror therapy an effective intervention for improving function in paralyzed upper extremities after a stroke as compared to the standard therapy? Dohle,
A Computational Framework for Quantitative Evaluation of Movement during Rehabilitation
 A Computational Framework for Quantitative Evaluation of Movement during Rehabilitation Yinpeng Chen a, Margaret Duff a,b, Nicole Lehrer a, Hari Sundaram a, Jiping He b, Steven L. Wolf c and Thanassis
A Computational Framework for Quantitative Evaluation of Movement during Rehabilitation Yinpeng Chen a, Margaret Duff a,b, Nicole Lehrer a, Hari Sundaram a, Jiping He b, Steven L. Wolf c and Thanassis
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Friedman, N., Chan, V., Reinkensmeyer, A. N., Beroukhim, A., Zambrano, G. J., Bachman, M., & Reinkensmeyer, D. J. (2014). Retraining and assessing hand movement after stroke
CRITICALLY APPRAISED PAPER (CAP) Friedman, N., Chan, V., Reinkensmeyer, A. N., Beroukhim, A., Zambrano, G. J., Bachman, M., & Reinkensmeyer, D. J. (2014). Retraining and assessing hand movement after stroke
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Huseyinsinoglu, B. E., Ozdincler, A. R., & Krespi, Y. (2012). Bobath concept versus constraint-induced movement therapy to improve arm functional recovery in stroke patients:
CRITICALLY APPRAISED PAPER (CAP) Huseyinsinoglu, B. E., Ozdincler, A. R., & Krespi, Y. (2012). Bobath concept versus constraint-induced movement therapy to improve arm functional recovery in stroke patients:
9/9/2016. By: Erica Ogilvie Rehab 540 Stroke Rehab University of Alberta Northwestern Ontario Regional Stroke Network
 By: Erica Ogilvie Rehab 540 Stroke Rehab University of Alberta Northwestern Ontario Regional Stroke Network Referred to as J.S. 60 year old Caucasian female 6 weeks post ischemic stroke Middle Cerebral
By: Erica Ogilvie Rehab 540 Stroke Rehab University of Alberta Northwestern Ontario Regional Stroke Network Referred to as J.S. 60 year old Caucasian female 6 weeks post ischemic stroke Middle Cerebral
Overview The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and dynamic balance.
 Core Measure: Berg Balance Scale (BBS) Overview The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and dynamic balance. Number of Test Items The BBS consists of
Core Measure: Berg Balance Scale (BBS) Overview The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and dynamic balance. Number of Test Items The BBS consists of
CORE MEASURE: CORE MEASURE: BERG BALANCE SCALE (BBS)
 OVERVIEW NUMBER OF TEST ITEMS SCORING EQUIPMENT TIME (NEW CLINICIAN) TIME (EXPERIENCED CLINICIAN) COST o The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and
OVERVIEW NUMBER OF TEST ITEMS SCORING EQUIPMENT TIME (NEW CLINICIAN) TIME (EXPERIENCED CLINICIAN) COST o The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and
MINERVA MEDICA COPYRIGHT
 EUR J PHYS REHABIL MED 2008;44:431-5 Robot-assisted therapy for neuromuscular training of sub-acute stroke patients. A feasibility study Aim. Several studies have described the contribution of robotics
EUR J PHYS REHABIL MED 2008;44:431-5 Robot-assisted therapy for neuromuscular training of sub-acute stroke patients. A feasibility study Aim. Several studies have described the contribution of robotics
Clinical usefulness and validity of robotic measures of reaching movement in hemiparetic stroke patients
 Otaka et al. Journal of NeuroEngineering and Rehabilitation (2015) 12:6 DOI 10.1186/s12984-015-0059-8 JOURNAL OF NEUROENGINEERING JNERAND REHABILITATION RESEARCH Clinical usefulness and validity of robotic
Otaka et al. Journal of NeuroEngineering and Rehabilitation (2015) 12:6 DOI 10.1186/s12984-015-0059-8 JOURNAL OF NEUROENGINEERING JNERAND REHABILITATION RESEARCH Clinical usefulness and validity of robotic
Akita J Med 44 : , (received 11 December 2017, accepted 18 December 2017)
 Akita J Med 44 : 111-116, 2017 (33) Takashi Mizutani 1), Toshiki Matsunaga 2), Kimio Saito 2), Takehiro Iwami 3), Satoru Kizawa 4), Toshihiko Anbo 3) and Yoichi Shimada 1) 1) Department of Orthopedic Surgery,
Akita J Med 44 : 111-116, 2017 (33) Takashi Mizutani 1), Toshiki Matsunaga 2), Kimio Saito 2), Takehiro Iwami 3), Satoru Kizawa 4), Toshihiko Anbo 3) and Yoichi Shimada 1) 1) Department of Orthopedic Surgery,
Date: December 4 th, 2012 CLINICAL SCENARIO:
 1 Title: There is strong support for the effectiveness of mcimt compared to conventional therapy in improving physical function and occupational performance of the affected upper extremity in adults 0
1 Title: There is strong support for the effectiveness of mcimt compared to conventional therapy in improving physical function and occupational performance of the affected upper extremity in adults 0
Augmented reflection technology for stroke rehabilitation a clinical feasibility study
 Augmented reflection technology for stroke rehabilitation a clinical feasibility study S Hoermann 1, L Hale 2, S J Winser 2, H Regenbrecht 1 1 Department of Information Science, 2 School of Physiotherapy,
Augmented reflection technology for stroke rehabilitation a clinical feasibility study S Hoermann 1, L Hale 2, S J Winser 2, H Regenbrecht 1 1 Department of Information Science, 2 School of Physiotherapy,
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION: Will use of low-level functional electrical stimulation improve accuracy of active reaching with the upper extremity better than traditional occupational
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION: Will use of low-level functional electrical stimulation improve accuracy of active reaching with the upper extremity better than traditional occupational
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION For stroke patients, in what ways does robot-assisted therapy improve upper extremity performance in the areas of motor impairment, muscle power, and strength?
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION For stroke patients, in what ways does robot-assisted therapy improve upper extremity performance in the areas of motor impairment, muscle power, and strength?
Table 3.1: Canadian Stroke Best Practice Recommendations Screening and Assessment Tools for Acute Stroke Severity
 Table 3.1: Assessment Tool Number and description of Items Neurological Status/Stroke Severity Canadian Neurological Scale (CNS)(1) Items assess mentation (level of consciousness, orientation and speech)
Table 3.1: Assessment Tool Number and description of Items Neurological Status/Stroke Severity Canadian Neurological Scale (CNS)(1) Items assess mentation (level of consciousness, orientation and speech)
Canadian Stroke Best Practices Table 3.3A Screening and Assessment Tools for Acute Stroke
 Canadian Stroke Best Practices Table 3.3A Screening and s for Acute Stroke Neurological Status/Stroke Severity assess mentation (level of consciousness, orientation and speech) and motor function (face,
Canadian Stroke Best Practices Table 3.3A Screening and s for Acute Stroke Neurological Status/Stroke Severity assess mentation (level of consciousness, orientation and speech) and motor function (face,
Precise evaluation of motor and non-motor dysfunction in Parkinson s disease using the KINARM
 Precise evaluation of motor and non-motor dysfunction in Parkinson s disease using the KINARM Project lead: Dr. Ron Levy Pauline Gaprielian, Dr. Stephen H. Scott, Dr. Giovanna Pari Queen s University,
Precise evaluation of motor and non-motor dysfunction in Parkinson s disease using the KINARM Project lead: Dr. Ron Levy Pauline Gaprielian, Dr. Stephen H. Scott, Dr. Giovanna Pari Queen s University,
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION For patients with acute cerebral vascular accident, is virtual reality gaming more effective than standard recreational therapy for the improvement of
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION For patients with acute cerebral vascular accident, is virtual reality gaming more effective than standard recreational therapy for the improvement of
The Hand Hub. Mary P Galea Departments of Medicine and Rehabilitation Medicine (Royal Melbourne Hospital) The University of Melbourne
 The Hand Hub Mary P Galea Departments of Medicine and Rehabilitation Medicine (Royal Melbourne Hospital) The University of Melbourne What prompted this project? 30%-60% of stroke survivors fail to regain
The Hand Hub Mary P Galea Departments of Medicine and Rehabilitation Medicine (Royal Melbourne Hospital) The University of Melbourne What prompted this project? 30%-60% of stroke survivors fail to regain
The Effects of Carpal Tunnel Syndrome on the Kinematics of Reach-to-Pinch Function
 The Effects of Carpal Tunnel Syndrome on the Kinematics of Reach-to-Pinch Function Raviraj Nataraj, Peter J. Evans, MD, PhD, William H. Seitz, MD, Zong-Ming Li. Cleveland Clinic, Cleveland, OH, USA. Disclosures:
The Effects of Carpal Tunnel Syndrome on the Kinematics of Reach-to-Pinch Function Raviraj Nataraj, Peter J. Evans, MD, PhD, William H. Seitz, MD, Zong-Ming Li. Cleveland Clinic, Cleveland, OH, USA. Disclosures:
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Shin, J., Bog Park, S., & Ho Jang, S. (2015). Effects of game-based virtual reality on healthrelated quality of life in chronic stroke patients: A randomized, controlled
CRITICALLY APPRAISED PAPER (CAP) Shin, J., Bog Park, S., & Ho Jang, S. (2015). Effects of game-based virtual reality on healthrelated quality of life in chronic stroke patients: A randomized, controlled
Optic flow in a virtual environment can impact on locomotor steering post stroke
 International Conference on Virtual Rehabilitation 2011 Rehab Week Zurich, ETH Zurich Science City, Switzerland, June 27-29, 2011 Optic flow in a virtual environment can impact on locomotor steering post
International Conference on Virtual Rehabilitation 2011 Rehab Week Zurich, ETH Zurich Science City, Switzerland, June 27-29, 2011 Optic flow in a virtual environment can impact on locomotor steering post
The potential effect of a vibrotactile glove rehabilitation system on motor recovery in chronic post-stroke hemiparesis
 Technology and Health Care 25 (2017) 1183 1187 1183 DOI 10.3233/THC-171001 IOS Press Technical Note The potential effect of a vibrotactile glove rehabilitation system on motor recovery in chronic post-stroke
Technology and Health Care 25 (2017) 1183 1187 1183 DOI 10.3233/THC-171001 IOS Press Technical Note The potential effect of a vibrotactile glove rehabilitation system on motor recovery in chronic post-stroke
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Wu, C., Huang, P., Chen, Y., Lin, K., & Yang, H. (2013). Effects of mirror therapy on motor and sensory recovery in chronic stroke: A randomized controlled trial. Archives
CRITICALLY APPRAISED PAPER (CAP) Wu, C., Huang, P., Chen, Y., Lin, K., & Yang, H. (2013). Effects of mirror therapy on motor and sensory recovery in chronic stroke: A randomized controlled trial. Archives
Angela Colantonio, PhD 1, Gary Gerber, PhD 2, Mark Bayley, MD, FRCPC 1, Raisa Deber, PhD 3, Junlang Yin, MSc 1 and Hwan Kim, PhD candidate 1
 J Rehabil Med 2011; 43: 311 315 ORIGINAL REPORT Differential Profiles for Patients with Traumatic and Non- Traumatic Brain Injury Angela Colantonio, PhD 1, Gary Gerber, PhD 2, Mark Bayley, MD, FRCPC 1,
J Rehabil Med 2011; 43: 311 315 ORIGINAL REPORT Differential Profiles for Patients with Traumatic and Non- Traumatic Brain Injury Angela Colantonio, PhD 1, Gary Gerber, PhD 2, Mark Bayley, MD, FRCPC 1,
Re-establishing establishing Neuromuscular
 Re-establishing establishing Neuromuscular Control Why is NMC Critical? What is NMC? Physiology of Mechanoreceptors Elements of NMC Lower-Extremity Techniques Upper-Extremity Techniques Readings Chapter
Re-establishing establishing Neuromuscular Control Why is NMC Critical? What is NMC? Physiology of Mechanoreceptors Elements of NMC Lower-Extremity Techniques Upper-Extremity Techniques Readings Chapter
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Kwon, J., Park, M., Yoon, I., & Park, S. (2012). Effects of virtual reality on upper extremity function and activities of daily living performance in acute stroke: A double-blind
CRITICALLY APPRAISED PAPER (CAP) Kwon, J., Park, M., Yoon, I., & Park, S. (2012). Effects of virtual reality on upper extremity function and activities of daily living performance in acute stroke: A double-blind
Relationship Between Visuospatial Neglect and Kinesthetic Deficits After Stroke
 545173NNRXXX1.1177/1545968314545173Neurorehabilitation and Neural RepairNeurorehabilitation and Neural RepairSemrau et al research-article214 Original Research Articles Relationship Between Visuospatial
545173NNRXXX1.1177/1545968314545173Neurorehabilitation and Neural RepairNeurorehabilitation and Neural RepairSemrau et al research-article214 Original Research Articles Relationship Between Visuospatial
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Wu, C. Y., Wang, T. N., Chen, Y. T., Lin, K. C., Chen, Y. A., Li, H. T., & Tsai, P. L. (2013). Effects of constraint-induced therapy combined with eye patching on functional
CRITICALLY APPRAISED PAPER (CAP) Wu, C. Y., Wang, T. N., Chen, Y. T., Lin, K. C., Chen, Y. A., Li, H. T., & Tsai, P. L. (2013). Effects of constraint-induced therapy combined with eye patching on functional
A ROBOTIC SYSTEM FOR UPPER-LIMB EXERCISES TO PROMOTE RECOVERY OF MOTOR FUNCTION FOLLOWING STROKE
 A ROBOTIC SYSTEM FOR UPPER-LIMB EXERCISES TO PROMOTE RECOVERY OF MOTOR FUNCTION FOLLOWING STROKE Peter S. Lum 1,2, Machiel Van der Loos 1,2, Peggy Shor 1, Charles G. Burgar 1,2 1 Rehab R&D Center, VA Palo
A ROBOTIC SYSTEM FOR UPPER-LIMB EXERCISES TO PROMOTE RECOVERY OF MOTOR FUNCTION FOLLOWING STROKE Peter S. Lum 1,2, Machiel Van der Loos 1,2, Peggy Shor 1, Charles G. Burgar 1,2 1 Rehab R&D Center, VA Palo
Supplementary materials for: Executive control processes underlying multi- item working memory
 Supplementary materials for: Executive control processes underlying multi- item working memory Antonio H. Lara & Jonathan D. Wallis Supplementary Figure 1 Supplementary Figure 1. Behavioral measures of
Supplementary materials for: Executive control processes underlying multi- item working memory Antonio H. Lara & Jonathan D. Wallis Supplementary Figure 1 Supplementary Figure 1. Behavioral measures of
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Smania, N., Gandolfi, M., Paolucci, S., Iosa, M., Ianes, P., Recchia, S., & Farina, S. (2012). Reduced-intensity modified constraint-induced movement therapy versus conventional
CRITICALLY APPRAISED PAPER (CAP) Smania, N., Gandolfi, M., Paolucci, S., Iosa, M., Ianes, P., Recchia, S., & Farina, S. (2012). Reduced-intensity modified constraint-induced movement therapy versus conventional
Hand of Hope. For hand rehabilitation. Member of Vincent Medical Holdings Limited
 Hand of Hope For hand rehabilitation Member of Vincent Medical Holdings Limited Over 17 Million people worldwide suffer a stroke each year A stroke is the largest cause of a disability with half of all
Hand of Hope For hand rehabilitation Member of Vincent Medical Holdings Limited Over 17 Million people worldwide suffer a stroke each year A stroke is the largest cause of a disability with half of all
Stroke Drivers Screening Assessment European Version 2012
 Stroke Drivers Screening Assessment European Version 2012 NB Lincoln, KA Radford, FM Nouri University of Nottingham Introduction The Stroke Drivers Screening Assessment (SDSA) was developed as part of
Stroke Drivers Screening Assessment European Version 2012 NB Lincoln, KA Radford, FM Nouri University of Nottingham Introduction The Stroke Drivers Screening Assessment (SDSA) was developed as part of
Comparison of Robot-Assisted Reaching to Free Reaching in Promoting Recovery From Chronic Stroke
 Comparison of Robot-Assisted Reaching to Free Reaching in Promoting Recovery From Chronic Stroke Leonard E. Kahn, M.S. 1,2, Michele Averbuch, P.T. 1, W. Zev Rymer, M.D., Ph.D. 1,2, David J. Reinkensmeyer,
Comparison of Robot-Assisted Reaching to Free Reaching in Promoting Recovery From Chronic Stroke Leonard E. Kahn, M.S. 1,2, Michele Averbuch, P.T. 1, W. Zev Rymer, M.D., Ph.D. 1,2, David J. Reinkensmeyer,
Tomoko Kitago, MD American Society of Neurorehabilitation November 10, 2016 San Diego, CA
 EARLYPATIENT RECOVERY DEMOGRAPHIC OF MOTOR CONTROL CHARACTERISTICS AFTER AND STROKE: A HUMAN LONGITUDINAL PERSPECTIVE CLINICAL DATA Tomoko Kitago, MD American Society of Neurorehabilitation November 10,
EARLYPATIENT RECOVERY DEMOGRAPHIC OF MOTOR CONTROL CHARACTERISTICS AFTER AND STROKE: A HUMAN LONGITUDINAL PERSPECTIVE CLINICAL DATA Tomoko Kitago, MD American Society of Neurorehabilitation November 10,
Restoration of Reaching and Grasping Functions in Hemiplegic Patients with Severe Arm Paralysis
 Restoration of Reaching and Grasping Functions in Hemiplegic Patients with Severe Arm Paralysis Milos R. Popovic* 1,2, Vlasta Hajek 2, Jenifer Takaki 2, AbdulKadir Bulsen 2 and Vera Zivanovic 1,2 1 Institute
Restoration of Reaching and Grasping Functions in Hemiplegic Patients with Severe Arm Paralysis Milos R. Popovic* 1,2, Vlasta Hajek 2, Jenifer Takaki 2, AbdulKadir Bulsen 2 and Vera Zivanovic 1,2 1 Institute
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Yin, C., Sien, N., Ying, L., Chung, S., & Leng, D. (2014). Virtual reality for upper extremity rehabilitation in early stroke: A pilot randomized controlled trial. Clinical
CRITICALLY APPRAISED PAPER (CAP) Yin, C., Sien, N., Ying, L., Chung, S., & Leng, D. (2014). Virtual reality for upper extremity rehabilitation in early stroke: A pilot randomized controlled trial. Clinical
Therapy Manual DO NOT PRINT
 Therapy Manual Contents 1. Shoulder 2. Shoulder and elbow a. Protraction: 1 DoF 1 b. Flexion: 1 DoF 1-6 c. Extension: 1 DoF 1-2 d. Abduction: 1 DoF 1-4 e. External rotation: 1 DoF 1-14 a. Combined shoulder
Therapy Manual Contents 1. Shoulder 2. Shoulder and elbow a. Protraction: 1 DoF 1 b. Flexion: 1 DoF 1-6 c. Extension: 1 DoF 1-2 d. Abduction: 1 DoF 1-4 e. External rotation: 1 DoF 1-14 a. Combined shoulder
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION What is the effectiveness of a modified constraint-induced therapy (mcit) intervention compared to conventional rehabilitation methods for the rehabilitation
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION What is the effectiveness of a modified constraint-induced therapy (mcit) intervention compared to conventional rehabilitation methods for the rehabilitation
SCA Functional Index Case Report Form
 SCA Functional Index Case Report Form Rater (initials): Date of examination: Proband-Pseudonym Timed walking test: 8m walk (8MW) test not performed, reason: proband unable to walk due to physical limitations
SCA Functional Index Case Report Form Rater (initials): Date of examination: Proband-Pseudonym Timed walking test: 8m walk (8MW) test not performed, reason: proband unable to walk due to physical limitations
The device for upper limb rehabilitation that supports patients during all the phases of neuromotor recovery A COMFORTABLE AND LIGHTWEIGHT GLOVE
 SINFONIA The device for upper limb rehabilitation that supports patients during all the phases of neuromotor recovery A COMFORTABLE AND LIGHTWEIGHT GLOVE The key feature of Gloreha Sinfonia is a rehabilitation
SINFONIA The device for upper limb rehabilitation that supports patients during all the phases of neuromotor recovery A COMFORTABLE AND LIGHTWEIGHT GLOVE The key feature of Gloreha Sinfonia is a rehabilitation
ASSESSMENT OF DRIVING-RELATED SKILL (ADReS)
 ASSESSMENT OF DRIVING-RELATED SKILL (ADReS) There are 3 key functions for safe driving: Vision, Cognition, and Motor Function. The ADReS assesses these 3 functions. As occupational therapists, we can perform
ASSESSMENT OF DRIVING-RELATED SKILL (ADReS) There are 3 key functions for safe driving: Vision, Cognition, and Motor Function. The ADReS assesses these 3 functions. As occupational therapists, we can perform
Clinical Study Playing Piano Can Improve Upper Extremity Function after Stroke: Case Studies
 Stroke Research and Treatment Volume 13, Article ID 159105, 5 pages http://dx.doi.org/10.1155/13/159105 Clinical Study Playing Piano Can Improve Upper Extremity Function after Stroke: Case Studies Myriam
Stroke Research and Treatment Volume 13, Article ID 159105, 5 pages http://dx.doi.org/10.1155/13/159105 Clinical Study Playing Piano Can Improve Upper Extremity Function after Stroke: Case Studies Myriam
The device for upper limb rehabilitation that supports patients during all the phases of neuromotor recovery A COMFORTABLE AND LIGHTWEIGHT GLOVE
 GLOREHA SINFONIA The device for upper limb rehabilitation that supports patients during all the phases of neuromotor recovery A COMFORTABLE AND LIGHTWEIGHT GLOVE The key feature of Gloreha Sinfonia is
GLOREHA SINFONIA The device for upper limb rehabilitation that supports patients during all the phases of neuromotor recovery A COMFORTABLE AND LIGHTWEIGHT GLOVE The key feature of Gloreha Sinfonia is
Robotic Unilateral and Bilateral Upper-Limb Movement Training for Stroke Survivors Afflicted by Chronic Hemiparesis
 2013 IEEE International Conference on Rehabilitation Robotics June 24-26, 2013 Seattle, Washington USA Robotic Unilateral and Bilateral Upper-Limb Movement Training for Stroke Survivors Afflicted by Chronic
2013 IEEE International Conference on Rehabilitation Robotics June 24-26, 2013 Seattle, Washington USA Robotic Unilateral and Bilateral Upper-Limb Movement Training for Stroke Survivors Afflicted by Chronic
Somatosensory Plasticity and Motor Learning
 5384 The Journal of Neuroscience, April 14, 2010 30(15):5384 5393 Behavioral/Systems/Cognitive Somatosensory Plasticity and Motor Learning David J. Ostry, 1,2 Mohammad Darainy, 1,3 Andrew A. G. Mattar,
5384 The Journal of Neuroscience, April 14, 2010 30(15):5384 5393 Behavioral/Systems/Cognitive Somatosensory Plasticity and Motor Learning David J. Ostry, 1,2 Mohammad Darainy, 1,3 Andrew A. G. Mattar,
EDUCATION EMPLOYMENT AWARDS
 EDUCATION DOCTOR OF PHILOSOPHY Institution: McGill University, Department of Neurology and Neurosurgery Specialization: Neurological Sciences Dissertation: Visual and saccadic processing in hemidecorticate
EDUCATION DOCTOR OF PHILOSOPHY Institution: McGill University, Department of Neurology and Neurosurgery Specialization: Neurological Sciences Dissertation: Visual and saccadic processing in hemidecorticate
Functional Independent Recovery among Stroke Patients at King Hussein Medical Center
 Functional Independent Recovery among Stroke Patients at King Hussein Medical Center Ali Al-Hadeed MD*, Amjad Banihani MD**, Tareq Al-Marabha MD* ABSTRACT Objective: To describe the functional independent
Functional Independent Recovery among Stroke Patients at King Hussein Medical Center Ali Al-Hadeed MD*, Amjad Banihani MD**, Tareq Al-Marabha MD* ABSTRACT Objective: To describe the functional independent
Expert System-Based Post-Stroke Robotic Rehabilitation for Hemiparetic Arm
 Expert System-Based Post-Stroke Robotic Rehabilitation for Hemiparetic Arm Pradeep Natarajan Department of EECS University of Kansas Outline 2 Introduction Stroke Rehabilitation Robotics Expert Systems
Expert System-Based Post-Stroke Robotic Rehabilitation for Hemiparetic Arm Pradeep Natarajan Department of EECS University of Kansas Outline 2 Introduction Stroke Rehabilitation Robotics Expert Systems
Transfer of Motor Learning across Arm Configurations
 The Journal of Neuroscience, November 15, 2002, 22(22):9656 9660 Brief Communication Transfer of Motor Learning across Arm Configurations Nicole Malfait, 1 Douglas M. Shiller, 1 and David J. Ostry 1,2
The Journal of Neuroscience, November 15, 2002, 22(22):9656 9660 Brief Communication Transfer of Motor Learning across Arm Configurations Nicole Malfait, 1 Douglas M. Shiller, 1 and David J. Ostry 1,2
Berg Balance Scale. CVA, Parkinson Disease, Pediatrics
 CVA, Parkinson Disease, Pediatrics CVA Highly recommended for inpatient and outpatient rehabilitation Recommended for acute care Parkinson s Disease Recommended for H and Y stages 2 and 3 G code-changing
CVA, Parkinson Disease, Pediatrics CVA Highly recommended for inpatient and outpatient rehabilitation Recommended for acute care Parkinson s Disease Recommended for H and Y stages 2 and 3 G code-changing
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION Is the combination of occupational therapy (OT) and mental practice (MP), from either an internal or an external perspective, an effective intervention
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION Is the combination of occupational therapy (OT) and mental practice (MP), from either an internal or an external perspective, an effective intervention
Evaluating Movement Posture Disorganization
 Evaluating Movement Posture Disorganization A Criteria-Based Reference Format for Observing & Analyzing Motor Behavior in Children with Learning Disabilities By W. Michael Magrun, MS, OTR 3 R D E D I T
Evaluating Movement Posture Disorganization A Criteria-Based Reference Format for Observing & Analyzing Motor Behavior in Children with Learning Disabilities By W. Michael Magrun, MS, OTR 3 R D E D I T
Starting a Strength Training Program
 MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Starting a Strength Training Program About This Kit The key to improving strength is applying resistance to the muscle
MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Starting a Strength Training Program About This Kit The key to improving strength is applying resistance to the muscle
Learning Classifier Systems (LCS/XCSF)
 Context-Dependent Predictions and Cognitive Arm Control with XCSF Learning Classifier Systems (LCS/XCSF) Laurentius Florentin Gruber Seminar aus Künstlicher Intelligenz WS 2015/16 Professor Johannes Fürnkranz
Context-Dependent Predictions and Cognitive Arm Control with XCSF Learning Classifier Systems (LCS/XCSF) Laurentius Florentin Gruber Seminar aus Künstlicher Intelligenz WS 2015/16 Professor Johannes Fürnkranz
Using the Kinect to Limit Abnormal Kinematics and Compensation Strategies During Therapy with End Effector Robots
 2013 IEEE International Conference on Rehabilitation Robotics June 24-26, 2013 Seattle, Washington USA Using the Kinect to Limit Abnormal Kinematics and Compensation Strategies During Therapy with End
2013 IEEE International Conference on Rehabilitation Robotics June 24-26, 2013 Seattle, Washington USA Using the Kinect to Limit Abnormal Kinematics and Compensation Strategies During Therapy with End
Title: Rotational strength, range of motion, and function in people with unaffected shoulders from various stages of life
 Author's response to reviews Title: Rotational strength, range of motion, and function in people with unaffected shoulders from various stages of life Authors: Jean-Sébastien Roy (jean-sebastien.roy.1@ulaval.ca)
Author's response to reviews Title: Rotational strength, range of motion, and function in people with unaffected shoulders from various stages of life Authors: Jean-Sébastien Roy (jean-sebastien.roy.1@ulaval.ca)
Nature Neuroscience: doi: /nn Supplementary Figure 1. Behavioral training.
 Supplementary Figure 1 Behavioral training. a, Mazes used for behavioral training. Asterisks indicate reward location. Only some example mazes are shown (for example, right choice and not left choice maze
Supplementary Figure 1 Behavioral training. a, Mazes used for behavioral training. Asterisks indicate reward location. Only some example mazes are shown (for example, right choice and not left choice maze
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Masiero, S., Boniolo, A., Wassermann, L., Machiedo, H., Volante, D., & Punzi, L. (2007). Effects of an educational-behavioral joint protection program on people with moderate
CRITICALLY APPRAISED PAPER (CAP) Masiero, S., Boniolo, A., Wassermann, L., Machiedo, H., Volante, D., & Punzi, L. (2007). Effects of an educational-behavioral joint protection program on people with moderate
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Dahl, A., Askim, T., Stock, R., Langørgen, E., Lydersen, S., & Indredavik, B. (2008). Short- and long-term outcome of constraint-induced movement therapy after stroke:
CRITICALLY APPRAISED PAPER (CAP) Dahl, A., Askim, T., Stock, R., Langørgen, E., Lydersen, S., & Indredavik, B. (2008). Short- and long-term outcome of constraint-induced movement therapy after stroke:
Original Article. Client-centred assessment and the identification of meaningful treatment goals for individuals with a spinal cord injury
 (2004) 42, 302 307 & 2004 International Society All rights reserved 1362-4393/04 $25.00 www.nature.com/sc Original Article Client-centred assessment and the identification of meaningful treatment goals
(2004) 42, 302 307 & 2004 International Society All rights reserved 1362-4393/04 $25.00 www.nature.com/sc Original Article Client-centred assessment and the identification of meaningful treatment goals
Research Strategic Plan
 Research Strategic Plan 2016-2021 VISION TO BE AN INTERNATIONAL LEADER IN THE STUDY AND ADVANCEMENT OF HUMAN MOVEMENT, SPORT, HEALTH, AND WELLNESS. MISSION TO PROVIDE EXCELLENCE IN RESEARCH, EDUCATION,
Research Strategic Plan 2016-2021 VISION TO BE AN INTERNATIONAL LEADER IN THE STUDY AND ADVANCEMENT OF HUMAN MOVEMENT, SPORT, HEALTH, AND WELLNESS. MISSION TO PROVIDE EXCELLENCE IN RESEARCH, EDUCATION,
Early Learning vs Early Variability 1.5 r = p = Early Learning r = p = e 005. Early Learning 0.
 The temporal structure of motor variability is dynamically regulated and predicts individual differences in motor learning ability Howard Wu *, Yohsuke Miyamoto *, Luis Nicolas Gonzales-Castro, Bence P.
The temporal structure of motor variability is dynamically regulated and predicts individual differences in motor learning ability Howard Wu *, Yohsuke Miyamoto *, Luis Nicolas Gonzales-Castro, Bence P.
Research Article Robotic Upper Limb Rehabilitation after Acute Stroke by NeReBot: Evaluation of Treatment Costs
 BioMed Research International, Article ID 265634, 5 pages http://dx.doi.org/10.1155/2014/265634 Research Article Robotic Upper Limb Rehabilitation after Acute Stroke by NeReBot: Evaluation of Treatment
BioMed Research International, Article ID 265634, 5 pages http://dx.doi.org/10.1155/2014/265634 Research Article Robotic Upper Limb Rehabilitation after Acute Stroke by NeReBot: Evaluation of Treatment
University of Manitoba - MPT: Neurological Clinical Skills Checklist
 Name: Site: Assessment Skills Observed Performed Becoming A. Gross motor function i. Describe movement strategies (quality, devices, timeliness, independence): supine sidelying sit stand supine long sitting
Name: Site: Assessment Skills Observed Performed Becoming A. Gross motor function i. Describe movement strategies (quality, devices, timeliness, independence): supine sidelying sit stand supine long sitting
Are randomised controlled trials telling us what rehabilitation interventions work?
 Are randomised controlled trials telling us what rehabilitation interventions work? Focus on stroke Jane Burridge March 6 th 2014 Neurorehabilitation: facts, fears and the future Overview Stroke recovery
Are randomised controlled trials telling us what rehabilitation interventions work? Focus on stroke Jane Burridge March 6 th 2014 Neurorehabilitation: facts, fears and the future Overview Stroke recovery
The following guidelines are applicable to office workers who sit at a desk and/or work on computers.
 STANDARD OPERATING PROCEDURES (SOP) FOR COMPUTER WORK, DESK TOP General Guidelines-Best Practices: The following guidelines are applicable to office workers who sit at a desk and/or work on computers.
STANDARD OPERATING PROCEDURES (SOP) FOR COMPUTER WORK, DESK TOP General Guidelines-Best Practices: The following guidelines are applicable to office workers who sit at a desk and/or work on computers.
Two 85 year olds enjoying their life on a Horseless Carriage tour - 3 years post stroke
 Stroke Rehabilitation: New Strategies for Recovery Gary Abrams MD UCSF/San Francisco VAMC U.S. Stroke Facts Stroke is 3 rd leading cause of death and leading cause of disability 730,000 new strokes/year
Stroke Rehabilitation: New Strategies for Recovery Gary Abrams MD UCSF/San Francisco VAMC U.S. Stroke Facts Stroke is 3 rd leading cause of death and leading cause of disability 730,000 new strokes/year
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION To what extent do the effects of neuromuscular electrical stimulation (NMES) on motor recovery of the upper extremity after stroke persist after the intervention
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION To what extent do the effects of neuromuscular electrical stimulation (NMES) on motor recovery of the upper extremity after stroke persist after the intervention
COGNITIVE ASSESSMENT USING THE KINARM EXOSKELETON ROBOT IN PATIENTS WITH TRANSIENT ISCHEMIC ATTACK
 COGNITIVE ASSESSMENT USING THE KINARM EXOSKELETON ROBOT IN PATIENTS WITH TRANSIENT ISCHEMIC ATTACK by Nadine Parker A research project submitted to the Department of Biomedical and Molecular Sciences In
COGNITIVE ASSESSMENT USING THE KINARM EXOSKELETON ROBOT IN PATIENTS WITH TRANSIENT ISCHEMIC ATTACK by Nadine Parker A research project submitted to the Department of Biomedical and Molecular Sciences In
The GAS-eous Tool. Goal Attainment Scaling Evaluation of Outcome for Upper-limb Spasticity. Version
 The GAS-eous Tool Goal Attainment Scaling Evaluation of Outcome for Upper-limb Spasticity Summary description: Version 1.1. 0.1.1 A semi-structured tool, designed to provide a framework for goal-setting
The GAS-eous Tool Goal Attainment Scaling Evaluation of Outcome for Upper-limb Spasticity Summary description: Version 1.1. 0.1.1 A semi-structured tool, designed to provide a framework for goal-setting
William C Miller, PhD, FCAOT Professor Occupational Science & Occupational Therapy University of British Columbia Vancouver, BC, Canada
 William C Miller, PhD, FCAOT Professor Occupational Science & Occupational Therapy University of British Columbia Vancouver, BC, Canada THE L TEST MANUAL Version: November 2014 Table of Contents Introduction...
William C Miller, PhD, FCAOT Professor Occupational Science & Occupational Therapy University of British Columbia Vancouver, BC, Canada THE L TEST MANUAL Version: November 2014 Table of Contents Introduction...
Physical Therapy/Core Strengthening Exercises
 303 91 st Ave. NE Ste. A106 Lake Stevens, WA 98258 425-377-8620 www.lakestevensanimalhospital.com Physical Therapy/Core Strengthening Exercises Dogs with osteoarthritis or those recovering from a major
303 91 st Ave. NE Ste. A106 Lake Stevens, WA 98258 425-377-8620 www.lakestevensanimalhospital.com Physical Therapy/Core Strengthening Exercises Dogs with osteoarthritis or those recovering from a major
Resting-State Functional Connectivity in Stroke Patients After Upper Limb Robot-Assisted Therapy: A Pilot Study
 Resting-State Functional Connectivity in Stroke Patients After Upper Limb Robot-Assisted Therapy: A Pilot Study N. Kinany 1,3,4(&), C. Pierella 1, E. Pirondini 3,4, M. Coscia 2, J. Miehlbradt 1, C. Magnin
Resting-State Functional Connectivity in Stroke Patients After Upper Limb Robot-Assisted Therapy: A Pilot Study N. Kinany 1,3,4(&), C. Pierella 1, E. Pirondini 3,4, M. Coscia 2, J. Miehlbradt 1, C. Magnin
/$ IEEE
 IEEE TRANSACTIONS ON NEURAL SYSTEMS AND REHABILITATION ENGINEERING, VOL. 18, NO. 4, AUGUST 2010 433 Normalized Movement Quality Measures for Therapeutic Robots Strongly Correlate With Clinical Motor Impairment
IEEE TRANSACTIONS ON NEURAL SYSTEMS AND REHABILITATION ENGINEERING, VOL. 18, NO. 4, AUGUST 2010 433 Normalized Movement Quality Measures for Therapeutic Robots Strongly Correlate With Clinical Motor Impairment
Bayesian integration in sensorimotor learning
 Bayesian integration in sensorimotor learning Introduction Learning new motor skills Variability in sensors and task Tennis: Velocity of ball Not all are equally probable over time Increased uncertainty:
Bayesian integration in sensorimotor learning Introduction Learning new motor skills Variability in sensors and task Tennis: Velocity of ball Not all are equally probable over time Increased uncertainty:
Effects of age on functional independence measure score gain in stroke patients in kaifukuki rehabilitation ward
 32 Japanese Journal of Comprehensive Rehabilitation Science (2012) Original Article Effects of age on functional independence measure score gain in stroke patients in kaifukuki rehabilitation ward Makoto
32 Japanese Journal of Comprehensive Rehabilitation Science (2012) Original Article Effects of age on functional independence measure score gain in stroke patients in kaifukuki rehabilitation ward Makoto
The UK FAM items Self-serviceTraining Course
 The UK FAM items Self-serviceTraining Course Course originator: Prof Lynne Turner-Stokes DM FRCP Regional Rehabilitation Unit Northwick Park Hospital Watford Road, Harrow, Middlesex. HA1 3UJ Background
The UK FAM items Self-serviceTraining Course Course originator: Prof Lynne Turner-Stokes DM FRCP Regional Rehabilitation Unit Northwick Park Hospital Watford Road, Harrow, Middlesex. HA1 3UJ Background
Coordination indices between lifting kinematics and kinetics
 Industrial and Manufacturing Systems Engineering Publications Industrial and Manufacturing Systems Engineering 2008 Coordination indices between lifting kinematics and kinetics Xu Xu North Carolina State
Industrial and Manufacturing Systems Engineering Publications Industrial and Manufacturing Systems Engineering 2008 Coordination indices between lifting kinematics and kinetics Xu Xu North Carolina State
Low Tolerance Long Duration (LTLD) Stroke Demonstration Project
 Low Tolerance Long Duration (LTLD) Stroke Demonstration Project Interim Summary Report October 25 Table of Contents 1. INTRODUCTION 3 1.1 Background.. 3 2. APPROACH 4 2.1 LTLD Stroke Demonstration Project
Low Tolerance Long Duration (LTLD) Stroke Demonstration Project Interim Summary Report October 25 Table of Contents 1. INTRODUCTION 3 1.1 Background.. 3 2. APPROACH 4 2.1 LTLD Stroke Demonstration Project
Estimation of the Upper Limb Lifting Movement Under Varying Weight and Movement Speed
 1 Sungyoon Lee, 1 Jaesung Oh, 1 Youngwon Kim, 1 Minsuk Kwon * Jaehyo Kim 1 Department of mechanical & control engineering, Handong University, qlfhlxhl@nate.com * Department of mechanical & control engineering,
1 Sungyoon Lee, 1 Jaesung Oh, 1 Youngwon Kim, 1 Minsuk Kwon * Jaehyo Kim 1 Department of mechanical & control engineering, Handong University, qlfhlxhl@nate.com * Department of mechanical & control engineering,
Reliability and validity of the International Spinal Cord Injury Basic Pain Data Set items as self-report measures
 (2010) 48, 230 238 & 2010 International Society All rights reserved 1362-4393/10 $32.00 www.nature.com/sc ORIGINAL ARTICLE Reliability and validity of the International Injury Basic Pain Data Set items
(2010) 48, 230 238 & 2010 International Society All rights reserved 1362-4393/10 $32.00 www.nature.com/sc ORIGINAL ARTICLE Reliability and validity of the International Injury Basic Pain Data Set items
Test Administration Instructions for the Fullerton Advanced Balance (FAB) Scale 10
 The Interactive Health Partner Wellness Program addresses fall prevention with assessments, outcomes tracking in an easy to use, comprehensive online system. Website: www.interactivehealthpartner.com Email:
The Interactive Health Partner Wellness Program addresses fall prevention with assessments, outcomes tracking in an easy to use, comprehensive online system. Website: www.interactivehealthpartner.com Email:
What is Kinesiology? Basic Biomechanics. Mechanics
 What is Kinesiology? The study of movement, but this definition is too broad Brings together anatomy, physiology, physics, geometry and relates them to human movement Lippert pg 3 Basic Biomechanics the
What is Kinesiology? The study of movement, but this definition is too broad Brings together anatomy, physiology, physics, geometry and relates them to human movement Lippert pg 3 Basic Biomechanics the
LAY LANGUAGE PROTOCOL SUMMARY
 Kinsman Conference Workshop A-3 - Responsible research: IRBs, consent and conflicts of interest Elizabeth Steiner MD, Associate Professor of Family Medicine, Co-Chair, Institutional Review Board, OHSU
Kinsman Conference Workshop A-3 - Responsible research: IRBs, consent and conflicts of interest Elizabeth Steiner MD, Associate Professor of Family Medicine, Co-Chair, Institutional Review Board, OHSU
Collaborative Research Grant Initiative: Mental Wellness in Seniors and Persons with Disabilities
 Predicting Potential for Positive Outcomes in a Slow-stream Rehabilitation Program Collaborative Research Grant Initiative: Mental Wellness in Seniors and Persons with Disabilities Ideas Fund Final Report
Predicting Potential for Positive Outcomes in a Slow-stream Rehabilitation Program Collaborative Research Grant Initiative: Mental Wellness in Seniors and Persons with Disabilities Ideas Fund Final Report
Increasing upper limb training intensity in chronic stroke using embodied virtual reality: a pilot study
 Perez-Marcos et al. Journal of NeuroEngineering and Rehabilitation (2) 4:9 DOI.86/s2984--328-9 RESEARCH Open Access Increasing upper limb training intensity in chronic stroke using embodied virtual reality:
Perez-Marcos et al. Journal of NeuroEngineering and Rehabilitation (2) 4:9 DOI.86/s2984--328-9 RESEARCH Open Access Increasing upper limb training intensity in chronic stroke using embodied virtual reality:
Integrating Sensorimotor Control Into Rehabilitation
 Integrating Sensorimotor Control Into Rehabilitation BRADY L. TRIPP, PhD, LAT, ATC Florida International University Key Points As evidence accumulates, so does our appreciation of the integral roles that
Integrating Sensorimotor Control Into Rehabilitation BRADY L. TRIPP, PhD, LAT, ATC Florida International University Key Points As evidence accumulates, so does our appreciation of the integral roles that
Robotics in the Rehabilitation of Neurological Conditions
 Robotics in the Rehabilitation of Neurological Conditions Gil J Cerros, MSHS The PRANAYAMA Research Group June 14, 2015 Clinical and Translational Research The PRANAYAMA Research Group fdsfsf Robotics
Robotics in the Rehabilitation of Neurological Conditions Gil J Cerros, MSHS The PRANAYAMA Research Group June 14, 2015 Clinical and Translational Research The PRANAYAMA Research Group fdsfsf Robotics
Predicting Recovery after a Stroke
 Predicting Recovery after a Stroke James Lynskey, PT, PhD Associate Professor, Department of Physical Therapy, A.T. Still University October 13, 2018 Wouldn t it be great if we could predict if a stroke
Predicting Recovery after a Stroke James Lynskey, PT, PhD Associate Professor, Department of Physical Therapy, A.T. Still University October 13, 2018 Wouldn t it be great if we could predict if a stroke
Dominican University of California Dominican Scholar Survey: Let us know how this paper benefits you.
 Dominican University of California Dominican Scholar Occupational Therapy Critically Appraised Papers Series Occupational Therapy 2017 Critically Appraised Paper for The Effect of Modified Constraint-Induced
Dominican University of California Dominican Scholar Occupational Therapy Critically Appraised Papers Series Occupational Therapy 2017 Critically Appraised Paper for The Effect of Modified Constraint-Induced
