The Effect of Hippotherapy on Postural Control in Sitting for Children with Cerebral Palsy
|
|
|
- Easter Adams
- 5 years ago
- Views:
Transcription
1 The Effect of Hippotherapy on Postural Control in Sitting for Children with Cerebral Palsy Darrell Hamill Kathleen Washington Owen R. White ABSTRACT. The purpose of this single subject research study was to examine the effects of a once weekly, 10-week hippotherapy program for three children, ages months, with cerebral palsy. Participants were rated as Level V on the Gross Motor Function Classification System. The Sitting Dimension of the Gross Motor Function Measure was used to establish a baseline of sitting abilities, and was administered every 2 weeks during intervention. The Sitting Assessment Scale and the Gross Motor Function Measure were administered before, after, and 4 weeks postintervention. Parental perceptions of the hippotherapy intervention were assessed using questionnaires. None of the children made gains on any of the standardized outcome measures. Parental perceptions were very Darrell Hamill, MS, PT, HPCS, is Physical Therapist, Squak Mountain Therapy and Federal Way School District, Issaquah, WA. Kathleen Washington, PT, PhD, is Clinical Associate Professor, Department of Rehabilitation Medicine, Division of Physical Therapy, University of Washington, Seattle, WA. Owen R. White, PhD, is Professor, College of Education, Special Education Area, University of Washington, Seattle, WA. Address correspondence to: Kathleen Washington, Clinical Associate Professor, Department of Rehabilitation Medicine, Division of Physical Therapy, Box , University of Washington, Seattle, WA ( kwpt@u.washington.edu). Physical & Occupational Therapy in Pediatrics, Vol. 27(4) 2007 Available online at by The Haworth Press, Inc. All rights reserved. doi: /j006v27n04_03 23
2 24 PHYSICAL & OCCUPATIONAL THERAPY IN PEDIATRICS positive, with reported improvements in range of motion and head control. doi: /j006v27n04_03 [Article copies available for a fee from The Haworth Document Delivery Service: HAWORTH. address: <docdelivery@ haworthpress.com> Website: < by The Haworth Press, Inc. All rights reserved.] KEYWORDS. Hippotherapy, cerebral palsy, children, sitting, gross motor function Hippotherapy is the use of a horse as part of an integrated treatment strategy for children and adults with movement dysfunction. Unlike therapeutic horseback riding, where riding skills are taught to individuals with disabilities, hippotherapy is a treatment strategy performed by health professionals, such as physical and occupational therapists, in which the horse is used as a therapeutic intervention (NARHA, 1998). The goals of hippotherapy are to improve the client s posture, balance, mobility, and function. The back of the walking horse imparts a threedimensional movement to the pelvis of the rider that is thought to be similar to the human s pelvic movement during gait (Fleck, 1992). The therapist directs the movements of the horse while analyzing the client s responses. Modifications in the terrain, the horse s speed or direction, or the rider s position, or functional tasks can be made to provide an appropriate movement challenge. As indicated by the American Hippotherapy Association ( persons who may benefit from hippotherapy include those with diagnoses of cerebral palsy (CP), developmental delay, Down syndrome, and traumatic brain injury. According to a systems theory of postural control, The task of postural control involves the body s position in space for (a) stability, defined as controlling the center of body mass within the base of support, and (b) orientation, defined as the ability to maintain an appropriate relationship between the body segments and between the body and the environment for a task (Shumway-Cook & Woollacott, 2001, p. 190). Putting a child with movement dysfunction on a horse provides myriad opportunities for the child to respond to the movement of the horse while performing functional tasks like reaching. The rider must maintain the head, trunk, and arms (body mass) over the base of support (the pelvis), when sitting on a horse, and is presumed to be practicing postural control in the sitting position. The rider is an active participant who makes continuous
3 Hamill, Washington, and White 25 adjustments to maintain postural control on a dynamic surface. Responding to the movements of the horse requires both reactive and anticipatory postural adjustments, both of which can be impaired in children with CP (Shumway-Cook, Hutchinson, Kartin, Price, & Woollacott, 2003; Liu, Zaino, & Westcott, 2000). There are many reported benefits of hippotherapy for children with CP including improvements in standing posture (Bertoti, 1988), symmetry of muscle activity (Benda, McGibbon, & Grant, 2003), gross motor function (Casady & Nichols-Larsen, 2004; Haehl, Guiliani, & Lewis, 1999), and self-perception (MacKinnon et al., 1995). Decreases in energy expenditure during ambulation have also been reported (Mc- Gibbon, Andrade, Widener, & Cintas, 1998). Several studies have indicated that hippotherapy may lead to improvements in standing balance, energy expenditure, and mobility skills for ambulatory children with CP (Bertoti, 1988; Casady & Nichols-Larsen, 2004; Haehl, Guiliani, & Lewis, 1999). However, results are mixed for children with CP with more severe levels of involvement, such as children who are non-ambulatory (Sterba, Rogers, France, & Vokes, 2002). Bertoti (1988) conducted the first data-based study in the area of hippotherapy. Using a scale developed for the study, Bertoti examined posture in 11 children ages 2 years 4 months to 9 years 5 months with spastic diplegia or quadriplegia. The children participated in one-hour hippotherapy sessions conducted by the author twice weekly for 10 weeks. A repeated measures design with two baseline measurements taken 10 weeks apart and a post-test after the riding program was used. Three physical therapists observed and independently rated each child in standing, with the author providing support to the child as needed. A Friedman test between the three median scores was significant (df = 2, p <.05), with 8 of the 11 children demonstrating improvement in standing postural control. Subjective improvements in balance were also reported by parents and therapists. This study suggests a trend of greater improvement with the younger, less severely involved children with CP. MacPhail et al. (1998) quantified postural reactions while riding in 6 children with CP (mean age 6.7 years) and seven children without CP (mean age 8.1 years). Children were videotaped in the frontal plane while riding the same horse at a walk. Children with CP showed significantly (p <.001) greater and more variable lateral trunk deviation than the children who were typically developing. Children with diplegia averaged smaller lateral movements (mean = 8.3 degrees) when compared to the children with quadriplegia (mean = 12 degrees) and responded with normal postural reactions more frequently (65-75% of the
4 26 PHYSICAL & OCCUPATIONAL THERAPY IN PEDIATRICS time) than children with quadriplegia (10-35% of the time). In this study children were allowed to stabilize their trunks with their hands, and possible changes in postural reactions over time were not evaluated. In 1999, Haehl et al. developed a kinematic tool to assess postural reactions in the sagittal plane in 2 subjects with CP, a 9 1/2-year-old child with spastic athetoid quadriplegic, a power wheelchair user, and a 4-year-old child who ambulated with a reverse walker. Both subjects were videotaped at the beginning of five one-hour hippotherapy sessions throughout their 12-week, once weekly, individualized hippotherapy program. While both children demonstrated improved postural reactions, only the child who was ambulatory showed significant (greater than 2 standard errors) gains in the Mobility and Social Function domains of the Pediatric Evaluation of Disability Inventory (Haley, Coster, Ludlow, Haltivanger, & Andrellos, 1992) after the riding program. In 2002, Sterba et al. examined the effects of a one-hour-per-week, 18-week riding program using the Gross Motor Function Measure-88 item version (GMFM-88) (Russell et al., 1993). Seventeen children with a diagnosis of CP (12 with spastic diplegia, 3 with spastic quadriplegia, and 2 with spastic hemiplegia) with a mean age of 9 years, 10 months participated. Participants served as their own controls. Assessments were performed 6 weeks before riding began, at the onset of riding, every 6 weeks during the riding program, and 6 weeks following the riding program. There was a significant (p < 0.04) improvement in total GMFM-88 scores during intervention, and a significant (p < 0.03) change in the GMFM Dimension E (walking, running, and jumping) that lasted six weeks post-intervention. The five children who were non-ambulatory, however, did not demonstrate changes in total GMFM scores. Sterba et al. recommended further studies that include larger numbers of children with more severe disabilities. Several limitations were identified in the research on hippotherapy. In all the studies, sample sizes were small and only one study (MacKinnon et al., 1995) utilized a control group. Content of the hippotherapy intervention was not always adequately described to allow for replication and tended not to be standardized across subjects. Descriptions for classifying subjects into groups were very general (e.g., ambulatory versus non-ambulatory) and did not necessarily provide homogeneity of groups. One important variable that was not always described was whether children were allowed to use their hands to stabilize their trunks, or how much support was given to the child to keep them safely positioned on the horse during hippotherapy. The task demands on the rider are dramatically changed if
5 Hamill, Washington, and White 27 the hands are not used for stabilization or if external support is not given while on horseback. Although they often participate in hippotherapy programs, little research has been done on children with CP who require external support to maintain a sitting position. The purpose of this single subject research study was to examine the effects of hippotherapy for three young children with CP classified in Level V on the Gross Motor Function Classification System (GMFCS) (Palisano et al., 1997). Participants and Settings METHODS A convenience sample of three children, months of age, with a diagnosis of CP participated in this study. All participants met the following inclusion criteria: (1) age between 20 months and 5 years with a diagnosis of quadriplegia as confirmed by physician, (2) Level V on the GMFCS, (3) no previous participation in a hippotherapy or therapeutic riding program, (4) postural instability in all sitting positions as defined by obtaining a minimum score of 10% but less than 25% on the GMFM Dimension B (Sitting), (5) parental commitment to the study, and (6) no contraindications excluding them from involvement in a hippotherapy program (NARHA, 1998). For safety reasons, children with uncontrolled seizures or who were unable to wear a helmet were excluded from participating. Characteristics of participants (with pseudonyms) are given in Table 1. TABLE 1. Participant Characteristics Child Gender Age Diagnosis GMFCS* Level Roger M 4 yrs. 6 mo. Mixed quadriplegic CP Beth F 3 yrs. 6 mo. Hypotonic quadriplegic CP Sam M 2 yrs. 3 mo. Dystonic quadriplegic CP Concurrent Therapies Initial GMFM** Score (Dimension B) V OT, PT, 15% Speech V OT, PT 18% V OT, PT 16% *Gross Motor Function Classification System for Cerebral Palsy (Palisano et al., 1997). **Gross Motor Function Measure (Russell et al., 1993).
6 28 PHYSICAL & OCCUPATIONAL THERAPY IN PEDIATRICS Roger could indicate yes and no reliably with head movement, and communicated using single words. He was able to follow simple directions. Beth and Sam communicated using eye gaze to indicate wants, but did not respond to verbal directions. Sam was motivated to reach for desired objects. All participants could sit for 4-5 seconds in ring sitting on the floor while propping on their hands. All three children had manual wheelchairs with modifications including head, trunk, pelvis, and foot supports. Children were recruited following referral to the hippotherapy program sponsored by a local birth-to-three center. When a child who met the inclusion criteria was referred, an informational flyer was mailed to their home, and the parent was instructed to contact the first author if they wished inclusion or if they had questions about the study. When parents contacted the first author and agreed to participate, a home visit was arranged. Informed consent was obtained and a screening conducted in the child s home to insure all inclusion criteria were met before baseline data were collected. All hippotherapy sessions were conducted at a therapeutic riding center. This study was approved by the Institutional Review Board at the University of Washington. Measures The two standardized outcome measures utilized were the Gross Motor Function Measure-88 item version (GMFM-88) (Russell et al., 1993); and the Sitting Assessment Scale (SAS) (Myhr, 1993). Two parent questionnaires were developed, one for pre-intervention and one for post-intervention. Response options utilized a Likert scale and openended questions (described in Results section) were included to assess anticipated and perceived effects and perceived value of the hippotherapy program. The GMFM-88 is an evaluative measure designed to quantify changes in gross motor function in children with cerebral palsy. It is divided into the five following dimensions: (A) lying and rolling, (B) sitting, (C) crawling and kneeling, (D) standing, and (E) walking, running, and jumping. Items are scored on a 4-point ordinal scale. Dimension scores and the total score is expressed as a percentage of the maximum score for that dimension (0-100%). A total score is obtained by adding the percentage for each dimension and dividing by 5. Several studies have documented reliability and validity (Bjornson, Graubert, McLaughlin, Kerfeld, & Clark, 1998; Russell et al., 1989, 1998, 2000; Trahan & Malouin, 1999),
7 including when scoring videotaped assessments (Nordmark, Haggland, & Jarnlo, 1997). The SAS was designed to assess postural control and functional control of arms and hands for different sitting positions in children with CP. A 4-point ordinal scale is used for each of five areas (head control, trunk control, foot control, arm function, hand function) with a 1 indicating no control/function to a 4 indicating good control/function. Using Spearman s rank order correlation coefficients, inter-rater reliability coefficients on the SAS ranged from.78 to 1.0 for individual scale area scores, with intra-rater reliability coefficients ranging from.57 to 1.0 for inexperienced raters (Myhr, von Wendt, & Sandberg, 1993). No validity studies were found. Baseline and Intervention Measurements Hamill, Washington, and White 29 As it was not possible to start all children in the study at the same time, a non-concurrent multiple baseline design was used (Watson & Workman, 1981). Baseline data were collected across randomly assigned periods of two, three, or four weeks. The GMFM Dimension B (Sitting) was administered three times for baseline data collection in the child s home, every two weeks during the intervention phase at the riding center, and at a follow-up assessment four to six weeks post-intervention. The entire GMFM and the SAS were administered at home on the first and last days of the intervention phase, and at the follow-up assessment. Follow-up data were collected with some variability due to vacation schedules. The first author administered all measures throughout the study period. Written pre-intervention and post-intervention questionnaires were completed by the participants parents. One parent was present during all testing sessions. The GMFM and SAS were administered by the first author in the standardized manner described in the manuals, and a checklist was used to insure procedural reliability. Additional standardized procedures for the SAS for each child included placing blocks under the feet of two of the children (Beth and Sam) to provide stability, and an insert placed behind one child s (Beth) back to promote an upright trunk. The parent was allowed to closely guard and give support to the child for safety, when appropriate, and any assistance given was noted and recorded. Table height was adjusted to just below the level of the elbows. All data collection sessions were videotaped with a camcorder mounted on a tripod.
8 30 PHYSICAL & OCCUPATIONAL THERAPY IN PEDIATRICS Inter-Rater Agreement Three phases of inter-rater agreement were established using percentage of agreement calculated as the number of agreements divided by the total number of agreements plus disagreements multiplied by 100 (Kazdin, 1982). Prior to data collection and following a training session using videotapes, the first author reached a minimum of 90% inter-rater agreement with an expert physical therapist who had 9 years experience using the GMFM in a research setting. To examine inter-rater percentage of agreement for items on the GMFM, the expert physical therapist and first author scored from videotape one GMFM for each child. Percentage of agreement between the first author and the expert was 81.0% on the last data collection for Roger, 78.2% for Beth, and 83.8% for Sam. Three occupational therapists with pediatric experience (Rater 1 = 4 years, Rater 2 = 25 years, Rater 3 = 3 years) scored videotapes for GMFM Dimension B and the SAS. Following a training period, each rater reached a minimum of 90% inter-rater agreement on the GMFM Dimension B and 100% inter-rater agreement on the SAS with the first author. After inter-rater agreement was established, each rater took the randomly ordered videotapes for one child home, and was instructed to complete the scoring of all tapes within one week. Raters were unaware of the purpose of the study and each independently scored one child s videotapes. When a rater s score differed from the first author on a specific item, an average of the two scores was used as final data. Because the participants were unable to attempt many of the more challenging items, inter-rater agreement between the first author and the three raters on the GMFM Dimension B was calculated in two ways: (1) based on all possible items (20 items), and (2) based on the number of items attempted. Inter-rater agreements based on all possible items in Dimension B were acceptable (Kazdin, 1982) for all scores for all three children (Table 2). Agreements based on items attempted were slightly lower. Inter-rater agreement results for the Sitting Assessment Scale (SAS) were lower (range = ) than for the GMFM Dimension B. Since there were only 5 items to score, a difference of one score lowered the percentage of agreement dramatically. Hippotherapy Intervention Following baseline, each participant began a 50-minute session of hippotherapy once weekly for 10 weeks. Sessions were conducted in an
9 Hamill, Washington, and White 31 TABLE 2. Item by Item Inter-Rater Agreement (Number of Agreements Divided by Total Number of Agreements Plus Disagreements Multiplied by 100) Based on All Items in Dimension GMFM Dimension B* Based on Items Attempted Sitting Assessment Scale** Roger mean median low/high Beth mean median low/high Sam mean median low/high *Gross Motor Function Measure (Russell et al., 1993). **Sitting Assessment Scale (Myhr, 1993). indoor arena and on outdoor trails as weather permitted. The same horse was used for all children for all sessions. All children used a saddle pad, lightweight approved helmet, and safety belt. Three people were needed to conduct all hippotherapy sessions; a physical therapist (first author) who conducted the session, a side walker, and a horse handler who led the horse according to the therapist s directions. The physical therapist had five years experience providing hippotherapy, was registered with the North American Riding for the Handicapped Association (NARHA), and was working toward her Hippotherapy Clinical Specialist credentialing through the American Hippotherapy Association. Attempts were made to keep the participants positioned in midline on the horse. Riders were visually inspected on the horse from the posterior aspect every 5 minutes, and corrections were made by the physical therapist and side walker to manually align the midline of the horse and child as closely as visual inspection would allow. The horse handler was given instructions by the physical therapist as to changes of speed and direction in order to provide an appropriate challenge to the child. The North American Riding for the Handicapped (NARHA, 1998) contraindications, precautions, and safety rules were observed at all times.
10 32 PHYSICAL & OCCUPATIONAL THERAPY IN PEDIATRICS A procedural checklist was developed prior to the sessions to insure as much consistency as possible. A log was kept of each session recording specifics of how much support was given, activities performed, attendance, and any other current relevant issues such as illness. The hippotherapy intervention was individualized according to each child s abilities. (See descriptions below.) Children were given adequate support to insure safety and an optimal position on the horse. The physical therapist provided manual support as low as possible on the child s trunk to maximize the child s own postural responses. Due to the poor sitting abilities of the participants, all three children required external support given by the physical therapist to maintain an upright seated posture on the horse. All participants attended 100% of their intervention sessions. Participant 1: Roger The physical therapist stabilized Roger s trunk at the lower ribcage. Additionally, Roger held on to handles on a strap around the horse s girth during part of his sessions. His trunk control improved while reaching up for a ring or toy, enabling the therapist to withdraw manual trunk support for a few seconds at a time. This activity was repeated many times during a session to encourage trunk control. Roger tolerated facing forward, sideways, and backward on the horse. The horse was led at a moderate walking speed with gentle turns. Parents reported Roger became very ill between sessions five and six and lost 8 pounds. He appeared much less engaged in the hippotherapy sessions six through eight. Participant 2: Beth The physical therapist provided manual support at Beth s mid-torso. Beth worked on head control during sessions, especially holding her head up and looking to the right. She was able to prop on her arms with assistance. She tolerated facing forward, sideways, and backward on the horse and gentle turns. Beth was never able to sit without support of the physical therapists s hands around her torso at any time during any session. Participant 3: Sam Sam often needed manual support by the physical therapist at his mid-torso because of his tendency to hyperextend his trunk. He was very motivated to reach for objects and required less support at the trunk
11 when reaching up for toys and rings. This strategy was employed often in sessions to increase activity of trunk muscles as well as to work on reaching and grasping toys and reaching toward midline. He tolerated facing forward and sideways on the horse. The horse was led at a medium walk with gentle turns. Data Analysis Percentage scores for the GMFM-88 Dimension B, GMFM-88 total score, and the SAS raw scores were first put in tabular format. The results of the GMFM Dimension B were graphed for visual inspection and comparison. Parental questionnaires were summarized and results of the parental rating scale were reported as descriptive data. GMFM-88 Dimension B RESULTS Baseline data for Roger and Sam ranged from 15 to 22.5%, Beth s scores were less variable (Figure 1). During intervention, all participants scores were fairly stable with no trend change. When looking at participants scores on an item-by-item basis, improvement on any given item did not change more than a single point, indicating stable performance. Visual inspection of the graphs shows no trend change during follow-up. GMFM-88 Total Scores For Roger, there was a slight upward trend between the pre- and post-intervention GMFM-88 total score, with a slight decline on followup testing (Table 3). Beth s scores reflected a slight downward trend from pre- to post-intervention. Sam s scores were very stable across all three testing sessions. Sitting Assessment Scale (SAS) Hamill, Washington, and White 33 Roger s scores across sessions showed a slight downward trend between pre- and post-intervention with a return toward baseline with the follow-up test (Table 4). A similar trend was noted for Sam. Results for Beth show almost identical scores across the three testing sessions.
12 34 PHYSICAL & OCCUPATIONAL THERAPY IN PEDIATRICS FIGURE 1. Percent Scores for Sitting Dimension of Gross Motor Function Measure (88 item)
13 Hamill, Washington, and White 35 TABLE 3. Gross Motor Function Measure (GMFM-88) Total Percentage Scores of the Three Subjects Child Pre-Score Post-Score Follow-Up Score Roger 14.6% 17.8% 16.9% Beth 12.7% 9.7% 9.4% Sam 11.4% 10.9% 12.0% TABLE 4. Mean Raw Scores for the Sitting Assessment Scale (SAS) Child Pre-Score Post-Score Follow-Up Score Roger Beth Sam Raw scores for the SAS vary from 4 to 20. Parent Questionnaires Parents comments indicated they had a good understanding of what hippotherapy was prior to the program starting. Their answers to the question What do you believe hippotherapy is? included the following: A therapy that will help exercise his trunk muscles while on a horse, (Roger s mother); It is a child learning to move with the movement of the horse, (Beth s mother); and A therapy to help the child to have more control of his body (trunk and head) (Sam s mother). When asked what effects they anticipated for their child through involvement in a hippotherapy program, all mothers mentioned improved trunk control or improved sitting, Roger and Beth s mothers mentioned improved head control, and Roger s mother added increased happiness and enthusiasm. When asked to describe the effects the hippotherapy program had on their child, all three mothers felt their children had improved trunk control. Sam s mother talked about how her son s looser legs and better trunk control made handling him and assisting him in play much easier for her. Roger s mother felt her son was better at following directions such as chin down, and sit up. When asked, Did what you thought would happen (in terms of how the program ran and how it affected your child) match what actually
14 36 PHYSICAL & OCCUPATIONAL THERAPY IN PEDIATRICS happened? Sam s mother wrote, I had hoped to see improvement in his trunk muscles, which I did. I was happily surprised with the improvements in the flexibility in his legs. Roger s mother wrote, My son is more happy. He feels secure and he is receiving more therapy which is helping his body to have better development. Beth s mother wrote, She liked riding and I could see her working to hold her head up and try to sit up tall. Using a 5-point Likert scale with 1 representing very negative effect and 5 representing very positive effect, parents were asked to rate the effects that hippotherapy would have on their child both before and after the intervention. Parents ratings increased from a 4 (positive effect) on the pre-hippotherapy questionnaire to a 5 (very positive effect) on the post-hippotherapy questionnaire. All parents scored a 5 ( absolutely worth the time and effort ) in response to the question Was involvement in a hippotherapy program worth the time and effort? DISCUSSION The purpose of this study was to examine the effects of hippotherapy on three young children with CP who were unable to sit alone without external support. None of the children showed significant improvement on the SAS, GMFM-88 total score, or the GMFM-88 Dimension B. These findings support other studies (Bertoti, 1988; MacPhail et al., 1998; Sterba et al., 2002) suggesting that hippotherapy is less effective in improving overall gross motor function for children classified in Level V on the GMFCS. One variable which could have affected the results of this study was that all children required support at the trunk or used their arms to support themselves in order to ensure safe and effective positioning on the horse. Attempts were made throughout the sessions to lessen the support given by adjusting the movement of the horse and having the child reach up for objects. These techniques were utilized with varying degrees of success, but the three participants were supported most of the sessions by the therapist or by their own upper extremities while holding handles or propping on arms. It is possible that beneficial effects of hippotherapy are related to the amount of time the child can actively make anticipatory and reactive adjustments to the horse s movement without external support. This possibility was hinted at in the study by
15 Hamill, Washington, and White 37 MacPhail et al. (1998) which looked at postural reactions of children with diplegic and quadriplegic CP. Children with quadriplegia hung on to handles and they performed less frequent postural adjustments in response to the horse s movement compared to children with diplegia. Thus, one possible predictor for hippotherapy efficacy may be the amount of trunk support a child requires. Another variable which was not measured but may have had an effect is the cognitive ability of the child. This idea was discussed with a pediatric therapist who has been involved in hippotherapy for 18 years (B. Burtucio, personal communication, January 12, 2005). She felt that if a child could follow directions or requests made by the treating therapist, the chances for improvement were greater. Roger, the one child who did show some slight objective improvement, was the child who was most able to follow verbal directions. This ability to follow verbal instructions was not measured but might have been an important variable. Assessment of parental perceptions of the hippotherapy intervention was included as a measure of social validity. Typically social validity measures evaluate whether the change produced in the target behavior has been sufficient to actually improve the life of the subject, and evaluate the acceptability or viability of the intervention for consumers, in this case, parents (Schwartz & Baer, 1991). Parents rated hippotherapy positively whereas objective measures failed to show any change in motor function. These results are consistent with the findings of MacKinnon et al. (1995) where parents reported improvements in functional motor skills such as walking, activities of daily living, and social skills despite lack of improvement on a variety of standardized measures. There may be several reasons to explain this discrepancy between parental perceptions and objective findings. First, horseback riding is a recreational activity in which children who are typically developing participate. Perhaps seeing their child engage in an activity that children who are typically developing participate in is a positive experience for the parent. All the parents reported to the first author that their child liked the experience of horseback riding, including interacting with the animal, the movement of the horse, and going out on the trails. They also seemed to enjoy the attention of several adults during sessions. Since the hippotherapy sessions were covered by insurance, parents were able to provide an activity their child enjoyed at relatively low cost. Parents wanted their children to continue in the hippotherapy program, indicating that it was worth the time and effort. From their comments, it is possible the mothers observed functional improvements that were not measured. Beth was learning how to drive a power chair and
16 38 PHYSICAL & OCCUPATIONAL THERAPY IN PEDIATRICS her mother felt Beth improved in her ability to turn her head to the right and scan with her eyes to the right. Beth s mother felt this skill had significant functional implications for Beth because of the goal of becoming independent in driving a power wheelchair with a head switch. It is difficult to tell if head turning and visual tracking actually improved as they were not specifically measured. However, Beth s scores on the portions of the SAS and GMFM-88 which address head in midline actually declined. Roger s mother also cited head control as one of the improvements for her child. Roger did show some improvement in the GMFM-88 total score with the most improvement shown in Lying and Rolling (Dimension A) on pre- and post-intervention testing. Sam s mother was very pleased about the fact that Sam s legs were much looser after therapy. She stated this benefit made handling and playing with Sam much easier. She also stated that reduction of tone in his legs would often last for several hours after a session and felt that there was a general reduction in tone over time. Limitations One threat to external validity is the fact that this study included only three children. The small number of participants limits generalizability of the results. There were some uncontrolled factors during the course of this study which could have affected outcome. Roger became very ill between the fourth and fifth week of intervention and lost eight pounds. Roger was less energetic and appeared to put less effort into the sessions for three to four weeks after his illness. A potential limitation was the testing effect the repeated measure (GMFM-88 Dimension B) may have had on the individual children s performance during evaluation sessions. All three children s mothers felt that the repetitive evaluations had a positive or negative effect on their children but for different reasons. Beth s mother felt Beth gave her best performance on the early evaluation due to the novelty of the examiner and that she became less and less motivated to perform with each session. This child was the most severely involved child functionally and voluntary movement took the most effort for her to perform. Roger, on the other hand, became more and more comfortable with the examiner and would throw himself backward and laugh when asked to sit independently. He knew he would be caught and enjoyed this activity. However, he would become upset if asked to not play around and would cry. Evaluations became more and more difficult to do because
17 of this. As evaluations progressed, Sam became more fearful of feeling unsupported in sitting, and his startle reflex seemed to become more pronounced. Another possible threat to internal validity is raised by Nordmark et al. (2000). The authors used both the PEDI and the GMFM to measure change 6 and 12 months post dorsal rhizotomy for children with CP. Both instruments detected change in children with milder severity, but only the PEDI showed change in children in the more severe group. These authors suggest that both the PEDI and the GMFM be used as outcome measures for children with CP and are complementary measures. However, the PEDI may not be the most sensitive measure of change for individuals at GMFCS Level V, since many items in the mobility domain of the PEDI, such as performing transfers and stair climbing, are beyond their physical capabilities. All three raters in this study commented about the difficulty they had scoring the SAS, citing lack of clarity in definitions for scoring criteria. Although acceptable levels of inter-rater agreement were obtained for two of the three raters, the third rater s levels were lower, ranging from.60 to.80. Lower reliability and lack of evidence of validity are limitations for research purposes. Implications for Practice and Research Hamill, Washington, and White 39 To date, there is little evidence to indicate that children with CP who are non-ambulatory make improvements in their gross motor skills from the use of a horse as a treatment strategy. This is especially true for children who need external trunk support, and are not actively responding to the horse s movements. Potential changes in gross motor function were measured in this study by the GMFM-88, an evaluative tool designed specifically for children with CP. However, the GMFM-88 may have limited sensitivity in detecting change in children with severe limitations in motor function (Nordmark et al., 2000). An alternative method of measuring clinically important changes over time for children at GMFCS Level V may be goal attainment scaling (GAS) (Brown, Effgen, & Palisano, 1998). This individualized, client-centered system incorporates the components of the behavioral objective, and can evaluate levels of activity and participation. Examples of criteria for measuring participation in meaningful activities can relate to consistency, efficiency of the activity, use of assistive devices, or degree of caregiver assistance. GAS has been shown to be responsive to change in individualized motor goals for infants with motor delays
18 40 PHYSICAL & OCCUPATIONAL THERAPY IN PEDIATRICS (Palisano, Haley, & Brown, 1992). However, in a study of 24 individuals with severely limited physical and cognitive abilities, Brown et al. (1998) found that while goal attainment scaling (GAS) scores for gross motor goals improved in the therapy setting, these improvements did not transfer to recess and home settings. Generalization of motor skills across settings should be an important consideration both for therapists conducting research and those providing hippotherapy to children with significantly limited physical abilities. The length of hippotherapy intervention reported in research varies from 8 weeks to 6 months. A survey conducted by McGibbon (2003) asked therapists registered with the American Hippotherapy Association to review their notes and estimate how long it took treating with a hippotherapy program to produce functional changes off the horse. Based on treatment notes from 95 patients with CP, the average length of time to produce notable changes was weeks. Since clinicians typically are expected to document objective changes for insurance companies every three months, a treatment time of 12 weeks would be a reasonable amount of time to use as a standard for children with CP. More research is needed that includes children with CP with limited motor function. As the task demands affect the amount of postural control required by the child, a quantifiable way to measure external support is needed. Researchers may gain valuable insights into selecting meaningful outcomes by consulting with family members when designing studies. Identifying goals that are functionally and contextually relevant to the primary caregiver and that incorporate GAS may prove a more responsive measure of change. REFERENCES Benda, W., McGibbon, N., & Grant, K. (2003). Improvements in muscle symmetry in children with cerebral palsy after equine-assisted therapy (hippotherapy). The Journal of Alternative and Complementary Medicine, 9(10), Bertoti, D. (1988). Effects of therapeutic horseback riding on posture in children with cerebral palsy. Physical Therapy, 68(10), Bjornson, K.F., Graubert, C.S., McLaughlin, J.F., Kerfeld, C.I., & Clark, E.M. (1998). Test-retest reliability of the Gross Motor Function Measure in children with cerebral palsy. Physical and Occupational Therapy in Pediatrics, 18 (2), Brown, D. A., Effgen, S. A., & Palisano, R. J. (1998). Performance following abilityfocused physical therapy intervention in individuals with severely limited physcal and cognitive abilities. Physical Therapy, 78(9),
19 Hamill, Washington, and White 41 Casady, R. L., & Nichols-Larsen, D. S. (2004). The effect of hippotherapy on ten children with cerebral palsy. Pediatric Physical Therapy, 16(3), Fleck, C. (1992). Hippotherapy: Mechanics of human walking and horseback riding. In: Eagle, B. T., Ed. Rehab With the Aid of the Horse: A Collection of Studies, Haehl, V., Giuliani, C., & Lewis, C. (1999). Influence of hippotherapy on the kinematics and functional performance of two children with cerebral palsy. Pediatric Physical Therapy, 11, Haley, S., Coster, W., Ludlow, L., Haltivanger, J., & Andrellos, P. (1992). The Pediatric Evaluation of Disability Inventory (PEDI). Published by the New England Medical Center Hospital. Kazdin, A. E., (1982). Single-case research designs: Methods for clinical and applied settings. New York: Oxford University Press. Liu, W. Y., Zaino, C. A., & Westcott, S.L. (2000). Anticipatory postural adjustments in children with cerebral palsy and children with typical development during functional reaching: A center of pressure (COP) study. Pediatric Physical Therapy, 12, MacKinnon, J., Noh, S., Lariviere, J., MacPhail, A., Allan, D., & Laliberte, D. (1995). A study of therapeutic effects of horseback riding for children with cerebral palsy. Physical and Occupational Therapy in Pediatrics, 15, MacPhail, H., Edwards, J., Golding, J., Miller, K., Mosier, C., & Zwiers, T. (1998). Trunk postural reactions in children with and without cerebral palsy during therapeutic horseback riding. Pediatric Physical Therapy, 10, McGibbon, N., Andrade, C., Widener, G., & Cintas, H. (1998). Effect of an equinemovement therapy program on gait, energy expenditure, and motor function in children with spastic cerebral palsy: a pilot study. Developmental Medicine and Child Neurology, 40, McGibbon, N. (2003). A retrospective study of hippotherapy patients responses to treatment. American Hippotherapy News, Spring, Myhr, U. (1993). Manual for the Sitting Assessment Scale. Boden University College of Health Sciences, S , Boden, Sweden. Myhr, U., von Wendt, L., & Sandberg, K. (1993). Assessment of sitting in children with cerebral palsy from videofilm: a reliability study. Physical and Occupational Therapy in Pediatrics, 12(4), Nordmark, E., Haggland, G., & Jarnlo, G. (1997). Reliability of the gross motor function measure in cerebral palsy. Scandinavian Journal of Rehabilitation Medicine, 29, North American Riding for the Handicapped Association (N.AR.H.A) (1998). North American Riding for the Handicapped Association, P.O.Box 33150, Denver, Colorado, Palisano, R. J., Haley, S. M., & Brown, D. D. Goal attainment scaling as a measure of change in infants with motor delays. Physical Therapy, 72, Palisano, R. J., Rosenbaum P., Walter, S., Russell, D., Wood, E., & Galuppi, B. (1997). Gross motor function classification system for cerebral palsy. Developmental Medicine and Child Neurology, 39,
20 42 PHYSICAL & OCCUPATIONAL THERAPY IN PEDIATRICS Russell, D., Rosenbaum, P., Cadman, D., Gowland, C., Hardy, S., & Jarvis, S. (1989). The gross motor function measure: a means to evaluate the effects of physical therapy. Developmental Medicine and Child Neurology, 31, Russell, D., Rosenbaum, P., Gowland, C., Hardy, S., Lane M., Plews, N., McGavin, H., Cadman, D., & Jarvis, S. (1993). Gross motor function measure manual 2 nd Ed. Hamilton, Ont. McMaster University Press. Russell, D., Palisano, R., Walter, S., Rosenbaum, P., Gemus, M., Gowland, C., et al. (1998). Evaluating motor function in children with Down syndrome: validity of the GMFM. Developmental Medicine and Child Neurology, 40(10), Russell, D., Palisano, R., Hanna, S., Rosenbaum, P., Walter, S., Wood, E, et al. (2000). Validation of a model of gross motor function for children with cerebral palsy. Physical Therapy, 80 (10), Schwartz, I. S., & Baer, D. M. (1991). Social validity assessments: Is current practice state of the art? Journal of Applied Behavior Analysis, 24, Shumway-Cook,A., Hutchinson, S., Kartin, D., Price, R., & Woollacott, M. (2003). Effect of balance training on recovery of stability in children with crerbral palsy. Developmental Medicine and Child Neurology, 45:, Shumway-Cook, A., & Woollacott, M. (2001). Motor Control Theory and Practical Applications (2 nd Ed.) Lippincott Williams & Wilkins. Sterba, J., Rogers, B., France, A., & Vokes, D. (2002). Horseback riding in children with cerebral palsy: Effect on gross motor function. Developmental Medicine & Child Neurology, 44, Trahan, J., Malouin, F. (1999). Changes in the gross motor function measure in children with different types of cerebral palsy: an eight-month follow-up study. Developmental Medicine and Child Neurology, 44 (4), Watson, P. J., & Workman, E. A. (1981). The nonconcurrent multiple baseline across-individuals design:an extension of the traditional multiple baseline design. Journal of Behavioral Therapy and Experimental Psychiatry, 12, doi: /j006v27n04_03
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Kwon, J. Y., Chang, H. J., Yi, S. H., Lee, J. Y., Shin, H. Y., & Kim, Y. H. (2015). Effect of hippotherapy on gross motor function in children with cerebral palsy: A randomized
CRITICALLY APPRAISED PAPER (CAP) Kwon, J. Y., Chang, H. J., Yi, S. H., Lee, J. Y., Shin, H. Y., & Kim, Y. H. (2015). Effect of hippotherapy on gross motor function in children with cerebral palsy: A randomized
Case History Report Form
 Child details ( * required) Name (first name only) or *Code John *Chronological age (CA) Actual age since birth *Diagnosis and/or presenting problems 18-27 mos Joubert Syndrome - a rare brain malformation
Child details ( * required) Name (first name only) or *Code John *Chronological age (CA) Actual age since birth *Diagnosis and/or presenting problems 18-27 mos Joubert Syndrome - a rare brain malformation
An Introduction to Occupational Therapy, Physical Therapy, and Speech-Language Pathology Incorporating Hippotherapy in Clinical Practice
 An Introduction to Occupational Therapy, Physical Therapy, and Speech-Language Pathology Incorporating Hippotherapy in Clinical Practice Provided by the American Hippotherapy Association, Inc. www.americanhippotherapyassociation.org
An Introduction to Occupational Therapy, Physical Therapy, and Speech-Language Pathology Incorporating Hippotherapy in Clinical Practice Provided by the American Hippotherapy Association, Inc. www.americanhippotherapyassociation.org
What is Hippotherapy
 HIPPOTHERAPY Mission Statement Angel Paths mission is to improve the body, mind and spirits of individuals with physical and mental disabilities through high-quality therapeutic programs, specializing
HIPPOTHERAPY Mission Statement Angel Paths mission is to improve the body, mind and spirits of individuals with physical and mental disabilities through high-quality therapeutic programs, specializing
Purpose: To advance hippotherapy and therapeutic riding professions by increasing
 Abstract Purpose: To advance hippotherapy and therapeutic riding professions by increasing awareness about the programs, the staff backgrounds, and the business aspects of a hippotherapy and therapeutic
Abstract Purpose: To advance hippotherapy and therapeutic riding professions by increasing awareness about the programs, the staff backgrounds, and the business aspects of a hippotherapy and therapeutic
Department of Rehabilitation Medicine, CHA Bundang Medical Center, CHA University, Seongnam, Korea
 Original Article Ann Rehabil Med 2015;39(4):624-629 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.4.624 Annals of Rehabilitation Medicine Gross Motor Function Outcome After Intensive
Original Article Ann Rehabil Med 2015;39(4):624-629 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.4.624 Annals of Rehabilitation Medicine Gross Motor Function Outcome After Intensive
Trunk control. Outline 13/09/2014. Hilde Feys. Disclosure of Relevant Financial Relationships
 Disclosure Information AACPDM 6 th Annual Meeting September 10-13, 2014 Evaluation of trunk in children with cerebral palsy: The Trunk Control Measurement Scale Dr. Lieve HEYRMAN Prof. Dr. Hilde FEYS Speaker
Disclosure Information AACPDM 6 th Annual Meeting September 10-13, 2014 Evaluation of trunk in children with cerebral palsy: The Trunk Control Measurement Scale Dr. Lieve HEYRMAN Prof. Dr. Hilde FEYS Speaker
Standing in children with bilateral spastic cerebral palsy: Aspects of muscle strength, vision and motor function
 Standing in children with bilateral spastic cerebral palsy: Aspects of muscle strength, vision and motor function Cecilia Lidbeck, PT, PhD Department of Women s and Children s Health Karolinska Institutet
Standing in children with bilateral spastic cerebral palsy: Aspects of muscle strength, vision and motor function Cecilia Lidbeck, PT, PhD Department of Women s and Children s Health Karolinska Institutet
Inter-Rater Reliability of the Gross Motor Penonnance Measure
 KAUTPT Vol. 10 No. 4 2003. Inter-Rater Reliability of the Gross Motor Penonnance Measure Yi Chung-hwi, Ph.D., P.T. Dept. of Physical Therapy, College of Health Science, Y onsei University Institute of
KAUTPT Vol. 10 No. 4 2003. Inter-Rater Reliability of the Gross Motor Penonnance Measure Yi Chung-hwi, Ph.D., P.T. Dept. of Physical Therapy, College of Health Science, Y onsei University Institute of
HEALTH CARE PROVIDERS are being challenged to
 697 Rasch Analysis of the Gross Motor Function Measure: Validating the Assumptions of the Rasch Model to Create an Interval-Level Measure Lisa M. Avery, BEng, Dianne J. Russell, MSc, Parminder S. Raina,
697 Rasch Analysis of the Gross Motor Function Measure: Validating the Assumptions of the Rasch Model to Create an Interval-Level Measure Lisa M. Avery, BEng, Dianne J. Russell, MSc, Parminder S. Raina,
Gross Motor Performance Measure (GMPM) 대구보건대학교고주연 PhD. RPT in NY, USA
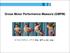 Gross Motor Performance Measure (GMPM) 대구보건대학교고주연 PhD. RPT in NY, USA GMPM Purpose Age range To evaluate change over time in gross motor performance (quality of movement) in CP children o CP children from
Gross Motor Performance Measure (GMPM) 대구보건대학교고주연 PhD. RPT in NY, USA GMPM Purpose Age range To evaluate change over time in gross motor performance (quality of movement) in CP children o CP children from
Sensory. Physical. Cognitive. Language 4/12/2016 LEARNING OBJECTIVES AT ASSESSMENT: SKILLS EVALUATION OVERVIEW
 ASSISTIVE TECHNOLOGY ASSESSMENT: SEATING AND POSITIONING FOR ACCESS Anne Cronin 2016 LEARNING OBJECTIVES Describe the principles related to assessment and intervention in assistive technology (AT) service
ASSISTIVE TECHNOLOGY ASSESSMENT: SEATING AND POSITIONING FOR ACCESS Anne Cronin 2016 LEARNING OBJECTIVES Describe the principles related to assessment and intervention in assistive technology (AT) service
Considerations in the selection of patients for Selective Dorsal Rhizotomy
 Considerations in the selection of patients for Selective Dorsal Rhizotomy The best and the worst surgery I have ever been associated with. A therapist's perspective Dean Morgan, PT Disclosure Statement
Considerations in the selection of patients for Selective Dorsal Rhizotomy The best and the worst surgery I have ever been associated with. A therapist's perspective Dean Morgan, PT Disclosure Statement
Introduction to Hippotherapy
 Introduction to Hippotherapy By Barbara Heine, PT Reprinted from NARHA Strides magazine, April 1997 (Vol. 3, No. 2) By its very nature, therapeutic riding influences the whole person and the effect on
Introduction to Hippotherapy By Barbara Heine, PT Reprinted from NARHA Strides magazine, April 1997 (Vol. 3, No. 2) By its very nature, therapeutic riding influences the whole person and the effect on
Gross Motor Outcomes After Dynamic Weight- Bearing in 2 Children With Trunk Hypotonia: A Case Series
 University of St Augustine for Health Sciences SOAR @ USA Physical Therapy Faculty and Staff Research 0-0 Gross Motor Outcomes After Dynamic Weight- Bearing in Children With Trunk Hypotonia: A Case Series
University of St Augustine for Health Sciences SOAR @ USA Physical Therapy Faculty and Staff Research 0-0 Gross Motor Outcomes After Dynamic Weight- Bearing in Children With Trunk Hypotonia: A Case Series
Normal development & reflex
 Normal development & reflex Definition of Development : acquisition & refinement of skills 1 대근육운동발달 2 소근육운동발달 3 대인관계및사회성발달 4 적응능력혹은비언어성발달 5 의사소통및언어발달 6 학습, 청각, 시각의발달 Department of Rehabilitation Medicine,
Normal development & reflex Definition of Development : acquisition & refinement of skills 1 대근육운동발달 2 소근육운동발달 3 대인관계및사회성발달 4 적응능력혹은비언어성발달 5 의사소통및언어발달 6 학습, 청각, 시각의발달 Department of Rehabilitation Medicine,
Building Better Balance
 Building Better Balance The Effects of MS on Balance Individuals with MS experience a decline in their balance due to various MS related impairments. Some of these impairments can be improved with exercise
Building Better Balance The Effects of MS on Balance Individuals with MS experience a decline in their balance due to various MS related impairments. Some of these impairments can be improved with exercise
Chapter 4B: Reliability Trial 2. Chapter 4B. Reliability. General issues. Inter-rater. Intra - rater. Test - Re-test
 Chapter 4B: Reliability Trial 2 Chapter 4B Reliability General issues Inter-rater Intra - rater Test - Re-test Trial 2 The second clinical trial was conducted in the spring of 1992 using SPCM Draft 6,
Chapter 4B: Reliability Trial 2 Chapter 4B Reliability General issues Inter-rater Intra - rater Test - Re-test Trial 2 The second clinical trial was conducted in the spring of 1992 using SPCM Draft 6,
Module Goals. An Introduction to Seating and Positioning for Individuals Who Use Assistive Technology. To answer the following questions:
 An Introduction to Seating and Positioning for Individuals Who Use Assistive Technology Aileen Costigan, MSc-OT Communication Sciences and Disorders The Pennsylvania State University fac3@psu.edu Module
An Introduction to Seating and Positioning for Individuals Who Use Assistive Technology Aileen Costigan, MSc-OT Communication Sciences and Disorders The Pennsylvania State University fac3@psu.edu Module
HBOT IN CEREBRAL PALSY an observational longitudinal study
 HBOT IN CEREBRAL PALSY an observational longitudinal study Dr. Pierre Marois, MD, F.R.C.P.(c) Dr. Michel Vanasse,, MD, F.R.C.P.(c) Dr. Jean Lambert, PhD. Pilot study (McGill 1999) 25 children with spastic
HBOT IN CEREBRAL PALSY an observational longitudinal study Dr. Pierre Marois, MD, F.R.C.P.(c) Dr. Michel Vanasse,, MD, F.R.C.P.(c) Dr. Jean Lambert, PhD. Pilot study (McGill 1999) 25 children with spastic
Forskning inden for truncus postural kontrol. CPOP DAG 22. maj What difference does trunk postural control make to function?
 Forskning inden for truncus postural kontrol CPOP DAG 22. maj 2014 Derek Curtis PT MSc Phd stud. Hvidovre Hospital Københavns Universitet What difference does trunk postural control make to function? Clinical
Forskning inden for truncus postural kontrol CPOP DAG 22. maj 2014 Derek Curtis PT MSc Phd stud. Hvidovre Hospital Københavns Universitet What difference does trunk postural control make to function? Clinical
HIP DYSPLASIA AND HYPOTONIA CAN STANDING IN ABDUCTION HELP?
 HIP DYSPLASIA AND HYPOTONIA CAN STANDING IN ABDUCTION HELP? Written by: MARY MILES, PT, DPT, ATP THIS CASE STUDY IS SPONSORED BY ALTIMATE MEDICAL Standing with hips in abduction has evolved as the new
HIP DYSPLASIA AND HYPOTONIA CAN STANDING IN ABDUCTION HELP? Written by: MARY MILES, PT, DPT, ATP THIS CASE STUDY IS SPONSORED BY ALTIMATE MEDICAL Standing with hips in abduction has evolved as the new
Randomized controlled trial of physiotherapy in 56 children with cerebral palsy followed for 18 months
 Randomized controlled trial of physiotherapy in 56 children with cerebral palsy followed for 18 months E Bower* PhD MCSP, Senior Research Fellow; D Michell BSc MCSP, Research Associate; M Burnett BSc,
Randomized controlled trial of physiotherapy in 56 children with cerebral palsy followed for 18 months E Bower* PhD MCSP, Senior Research Fellow; D Michell BSc MCSP, Research Associate; M Burnett BSc,
RESEARCH: Past Future How far have we come? How far have we to go? By Kathy Splinter-Watkins, MOT, OTR/L
 RESEARCH: Past Future How far have we come? How far have we to go? By Kathy Splinter-Watkins, MOT, OTR/L It takes rare gifts and talents and rare personalities to be real pathfinders in this work. Adolf
RESEARCH: Past Future How far have we come? How far have we to go? By Kathy Splinter-Watkins, MOT, OTR/L It takes rare gifts and talents and rare personalities to be real pathfinders in this work. Adolf
DoD Ergonomics Working Group NEWS
 DoD Ergonomics Working Group NEWS Issue 128, July/August 2012 Back Injury Prevention for Childcare Providers If you are taking care of infants and toddlers, you need to take care of your back. The U.S.
DoD Ergonomics Working Group NEWS Issue 128, July/August 2012 Back Injury Prevention for Childcare Providers If you are taking care of infants and toddlers, you need to take care of your back. The U.S.
Selective Motor Control Assessment of the Lower Extremity in Patients with Spastic Cerebral Palsy
 Overview Selective Motor Control Assessment of the Lower Extremity in Patients with Spastic Cerebral Palsy Marcia Greenberg MS, PT* Loretta Staudt MS, PT* Eileen Fowler PT, PhD Selective Motor Control
Overview Selective Motor Control Assessment of the Lower Extremity in Patients with Spastic Cerebral Palsy Marcia Greenberg MS, PT* Loretta Staudt MS, PT* Eileen Fowler PT, PhD Selective Motor Control
Exercise, Physical Therapy and Fall Prevention
 Exercise, Physical Therapy and Fall Prevention University of Davis Medical Center Rosy Chow Neuro Clinical Specialist Physical Therapist Outline of Talk Role of Physical Therapy in care of people with
Exercise, Physical Therapy and Fall Prevention University of Davis Medical Center Rosy Chow Neuro Clinical Specialist Physical Therapist Outline of Talk Role of Physical Therapy in care of people with
By: Griffin Smith & Eric Foch
 By: Griffin Smith & Eric Foch What is Cerebral Palsy? Non progressive neurodevelopmentalcondition Signs: Spasticity Ataxia Muscle rigidity idit Athetosis Tremor Distribution Among Limbs Why study cerebral
By: Griffin Smith & Eric Foch What is Cerebral Palsy? Non progressive neurodevelopmentalcondition Signs: Spasticity Ataxia Muscle rigidity idit Athetosis Tremor Distribution Among Limbs Why study cerebral
Test Administration Instructions for the Fullerton Advanced Balance (FAB) Scale 10
 The Interactive Health Partner Wellness Program addresses fall prevention with assessments, outcomes tracking in an easy to use, comprehensive online system. Website: www.interactivehealthpartner.com Email:
The Interactive Health Partner Wellness Program addresses fall prevention with assessments, outcomes tracking in an easy to use, comprehensive online system. Website: www.interactivehealthpartner.com Email:
Effect of intensive neurodevelopmental treatment in gross motor function of children with cerebral palsy
 Effect of intensive neurodevelopmental treatment in gross motor function of children with cerebral palsy Nikos Tsorlakis* MSc PT, Physical Educator, Hellenic Society for Care and Rehabilitation of Children
Effect of intensive neurodevelopmental treatment in gross motor function of children with cerebral palsy Nikos Tsorlakis* MSc PT, Physical Educator, Hellenic Society for Care and Rehabilitation of Children
University of Manitoba - MPT: Neurological Clinical Skills Checklist
 Name: Site: Assessment Skills Observed Performed Becoming A. Gross motor function i. Describe movement strategies (quality, devices, timeliness, independence): supine sidelying sit stand supine long sitting
Name: Site: Assessment Skills Observed Performed Becoming A. Gross motor function i. Describe movement strategies (quality, devices, timeliness, independence): supine sidelying sit stand supine long sitting
CORE MEASURE: CORE MEASURE: BERG BALANCE SCALE (BBS)
 OVERVIEW NUMBER OF TEST ITEMS SCORING EQUIPMENT TIME (NEW CLINICIAN) TIME (EXPERIENCED CLINICIAN) COST o The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and
OVERVIEW NUMBER OF TEST ITEMS SCORING EQUIPMENT TIME (NEW CLINICIAN) TIME (EXPERIENCED CLINICIAN) COST o The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and
ORIGINAL ARTICLE. Effects of Neurodevelopmental Therapy on Gross Motor Function in Children with Cerebral Palsy. Introduction. Abstract Objective
 ORIGINAL ARTICLE Effects of Neurodevelopmental Therapy on Gross Motor Function in Children with Cerebral Palsy How to Cite This Article: labaf S, Shamsoddini A, Hollisaz MT, Sobhani V, Shakibaee A. Effects
ORIGINAL ARTICLE Effects of Neurodevelopmental Therapy on Gross Motor Function in Children with Cerebral Palsy How to Cite This Article: labaf S, Shamsoddini A, Hollisaz MT, Sobhani V, Shakibaee A. Effects
Chapter 1. Overview. General Description. Test Developers. Purpose and Use. Qualifications of Users. Limitations. Communication. General Description
 Chapter 1: Overview Chapter 1 Overview General Description Test Developers Purpose and Use Qualifications of Users Limitations Communication General Description The research version of the Seated Postural
Chapter 1: Overview Chapter 1 Overview General Description Test Developers Purpose and Use Qualifications of Users Limitations Communication General Description The research version of the Seated Postural
Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual
 Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual 2nd Edition Isabelle M. Bohman, M.S., P.T., NDT Coordinator Instructor TM Published by Clinician s View Albuquerque, NM 505-880-0058
Handling Skills Used in the Management of Adult Hemiplegia: A Lab Manual 2nd Edition Isabelle M. Bohman, M.S., P.T., NDT Coordinator Instructor TM Published by Clinician s View Albuquerque, NM 505-880-0058
Evaluation of the Family - Rated Kinder Infant Development Scale (KIDS) for Disabled Children
 Jikeikai Med J 2012 ; 59 : 5-10 Evaluation of the Family - Rated Kinder Infant Development Scale (KIDS) for Disabled Children Keiji Hashimoto, Naoko Matsui, Hidemi Yakuwa, and Kohei Miyamura Division of
Jikeikai Med J 2012 ; 59 : 5-10 Evaluation of the Family - Rated Kinder Infant Development Scale (KIDS) for Disabled Children Keiji Hashimoto, Naoko Matsui, Hidemi Yakuwa, and Kohei Miyamura Division of
Body Mechanics When caring for a client
 Body Mechanics When caring for a client If assistance is needed, find out the client's strengths and weaknesses. Often one side of the body is stronger. The stronger side should be transferred first. When
Body Mechanics When caring for a client If assistance is needed, find out the client's strengths and weaknesses. Often one side of the body is stronger. The stronger side should be transferred first. When
Overview The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and dynamic balance.
 Core Measure: Berg Balance Scale (BBS) Overview The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and dynamic balance. Number of Test Items The BBS consists of
Core Measure: Berg Balance Scale (BBS) Overview The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and dynamic balance. Number of Test Items The BBS consists of
Active-Assisted Stretches
 1 Active-Assisted Stretches Adequate flexibility is fundamental to a functional musculoskeletal system which represents the foundation of movement efficiency. Therefore a commitment toward appropriate
1 Active-Assisted Stretches Adequate flexibility is fundamental to a functional musculoskeletal system which represents the foundation of movement efficiency. Therefore a commitment toward appropriate
On The Road. Training Manual
 On The Road Training Manual ST - 1 Standing External Rotation Strength Training Injury prevention Strengthening the rotator cuff Attach the tubing to a secure location like a fence or the net post. Start
On The Road Training Manual ST - 1 Standing External Rotation Strength Training Injury prevention Strengthening the rotator cuff Attach the tubing to a secure location like a fence or the net post. Start
Agenda and Objectives
 Agenda and Objectives Session 2 Handout: Activity Session One 1. Welcome & outline review today s agenda 2. Benefits of and barriers to regular exercise 3. Review of exercise homework and planning ahead
Agenda and Objectives Session 2 Handout: Activity Session One 1. Welcome & outline review today s agenda 2. Benefits of and barriers to regular exercise 3. Review of exercise homework and planning ahead
KAATSU training in a case of patients with periventricular leukomalacia (PVL)
 CASE REPORT KAATSU training in a case of patients with periventricular leukomalacia (PVL) H. Iwashita, T. Morita, Y. Sato, T. Nakajima Int. J. KAATSU Training Res. 2014; 10: 7-11 Correspondence to: H.
CASE REPORT KAATSU training in a case of patients with periventricular leukomalacia (PVL) H. Iwashita, T. Morita, Y. Sato, T. Nakajima Int. J. KAATSU Training Res. 2014; 10: 7-11 Correspondence to: H.
Heidi Sanders, OTR/L. Amy Shuckra, MPT
 Adaptive Equipment Heidi Sanders, OTR/L University of New Mexico Health Sciences Center, Los Pasos Program Amy Shuckra, MPT Shriners Hospitals for Children Salt Lake City, Utah What is Adaptive Equipment?
Adaptive Equipment Heidi Sanders, OTR/L University of New Mexico Health Sciences Center, Los Pasos Program Amy Shuckra, MPT Shriners Hospitals for Children Salt Lake City, Utah What is Adaptive Equipment?
CommonKnowledge. Pacific University. Leah Rybolt Pacific University. Recommended Citation. Notice to Readers
 Pacific University CommonKnowledge PT Critically Appraised Topics School of Physical Therapy 2014 A comparison of strength training to standard care at Khayelitsha Special School in improving motor function
Pacific University CommonKnowledge PT Critically Appraised Topics School of Physical Therapy 2014 A comparison of strength training to standard care at Khayelitsha Special School in improving motor function
Universal Exercise Unit for Treatment of a Child Following Hemispherectomy: A Case Report
 Doctor of Physical Therapy Program Case Reports 2017 Universal Exercise Unit for Treatment of a Child Following Hemispherectomy: A Case Report Abbie Wooten University of Iowa Copyright 2017 Abbie Wooten
Doctor of Physical Therapy Program Case Reports 2017 Universal Exercise Unit for Treatment of a Child Following Hemispherectomy: A Case Report Abbie Wooten University of Iowa Copyright 2017 Abbie Wooten
COPYRIGHTED MATERIAL COMPONENTS OF A GOOD SEAT. Developing a Good Seat
 1 COMPONENTS OF A GOOD SEAT The seat is the rider s primary and most important point of influence with the horse.the rider s weight in the seat and the pressure of his legs on the horse are considered
1 COMPONENTS OF A GOOD SEAT The seat is the rider s primary and most important point of influence with the horse.the rider s weight in the seat and the pressure of his legs on the horse are considered
The Complex Rehab Technology Company. Focused on Providing Specialized Products and Related Services to People with Disabilities
 The Complex Rehab Technology Company Focused on Providing Specialized Products and Related Services to People with Disabilities The Complex Rehab Technology Company What is Complex Rehab Technology and
The Complex Rehab Technology Company Focused on Providing Specialized Products and Related Services to People with Disabilities The Complex Rehab Technology Company What is Complex Rehab Technology and
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) De Brito Brandao, M., Gordon, A. M., & Mancini, M. C. (2012). Functional impact of constraint therapy and bimanual training in children with cerebral palsy: A randomized
CRITICALLY APPRAISED PAPER (CAP) De Brito Brandao, M., Gordon, A. M., & Mancini, M. C. (2012). Functional impact of constraint therapy and bimanual training in children with cerebral palsy: A randomized
Hippotherapy. Policy Number: Last Review: 7/2014 Origination: 7/2008 Next Review: 1/2015
 Hippotherapy Policy Number: 8.03.12 Last Review: 7/2014 Origination: 7/2008 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for Hippotherapy. This
Hippotherapy Policy Number: 8.03.12 Last Review: 7/2014 Origination: 7/2008 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for Hippotherapy. This
Exercise Program WARNING: DO NOT USE THIS OR ANY OTHER EXERCISE PROGRAM WITHOUT FIRST BEING CLEARED BY YOUR DOCTOR.
 Exercise Program WARNING: DO NOT USE THIS OR ANY OTHER EXERCISE PROGRAM WITHOUT FIRST BEING CLEARED BY YOUR DOCTOR. Things you MUST know before you begin Posture It is absolutely critical to maintain proper
Exercise Program WARNING: DO NOT USE THIS OR ANY OTHER EXERCISE PROGRAM WITHOUT FIRST BEING CLEARED BY YOUR DOCTOR. Things you MUST know before you begin Posture It is absolutely critical to maintain proper
1. Can self-propel, or use their foot to push (punt), a standard manual wheelchair 1 and be safe and able to do essential daily tasks.
 Disability Support Services Equipment and Modifications Competency Framework Wheeled Mobility and Postural Management Introduction The Wheeled Mobility and Postural Management Credential recognises that
Disability Support Services Equipment and Modifications Competency Framework Wheeled Mobility and Postural Management Introduction The Wheeled Mobility and Postural Management Credential recognises that
DEEP SQUAT. Upper torso is parallel with tibia or toward vertical Femur below horizontal Knees are aligned over feet Dowel aligned over feet
 APPENDIX 9 SCORING CRITERIA DEEP SQUAT Upper torso is parallel with tibia or toward vertical Femur below horizontal Knees are aligned over feet Dowel aligned over feet Upper torso is parallel with tibia
APPENDIX 9 SCORING CRITERIA DEEP SQUAT Upper torso is parallel with tibia or toward vertical Femur below horizontal Knees are aligned over feet Dowel aligned over feet Upper torso is parallel with tibia
How to Apply for a Constraint-Induced Movement Therapy (CIMT) Program
 How to Apply for a Constraint-Induced Movement Therapy (CIMT) Program Constraint-Induced Movement Therapy (CI Therapy, or CIMT): Two Programs There are two programs offered it the Taub Therapy Clinic for
How to Apply for a Constraint-Induced Movement Therapy (CIMT) Program Constraint-Induced Movement Therapy (CI Therapy, or CIMT): Two Programs There are two programs offered it the Taub Therapy Clinic for
Commonwealth Health Corporation NEXT
 Commonwealth Health Corporation This computer-based learning (CBL) module details important aspects of musculoskeletal disorders, body mechanics and ergonomics in the workplace. It examines: what causes
Commonwealth Health Corporation This computer-based learning (CBL) module details important aspects of musculoskeletal disorders, body mechanics and ergonomics in the workplace. It examines: what causes
Review of Selected Physical Therapy Interventions for School Age Children with Disabilities
 Review of Selected Physical Therapy Interventions for School Age Children with Disabilities Prepared for the Center on Personnel Studies in Special Education EXECUTIVE SUMMARY by Susan K. Effgen University.
Review of Selected Physical Therapy Interventions for School Age Children with Disabilities Prepared for the Center on Personnel Studies in Special Education EXECUTIVE SUMMARY by Susan K. Effgen University.
GENERAL EXERCISES YOGA BMW MANUFACTURING CO. PZ-AM-G-US I July 2017
 GENERAL EXERCISES YOGA BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to be
GENERAL EXERCISES YOGA BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to be
Lifting and Moving Patients
 1. Which of the following factors should be considered before lifting any patient? a. The weight of the patient b. Your physical limitations c. Communications 2. When lifting a patient, a basic principle
1. Which of the following factors should be considered before lifting any patient? a. The weight of the patient b. Your physical limitations c. Communications 2. When lifting a patient, a basic principle
Please demonstrate each task and/or give instructions as written. When scoring, please record the lowest response category that applies for each item.
 Berg Balance Test Name Date Location Rater GENERAL INSTRUCTIONS Please demonstrate each task and/or give instructions as written. When scoring, please record the lowest response category that applies for
Berg Balance Test Name Date Location Rater GENERAL INSTRUCTIONS Please demonstrate each task and/or give instructions as written. When scoring, please record the lowest response category that applies for
A Collection of Brief, Reliable and Valid Instruments to Obtain a Holistic Picture of Children with Cerebral Palsy: Products of the Move & PLAY Study
 A Collection of Brief, Reliable and Valid Instruments to Obtain a Holistic Picture of Children with Cerebral Palsy: Products of the Move & PLAY Study Move & PLAY Study Team Lehmann Day May 2013 Movement
A Collection of Brief, Reliable and Valid Instruments to Obtain a Holistic Picture of Children with Cerebral Palsy: Products of the Move & PLAY Study Move & PLAY Study Team Lehmann Day May 2013 Movement
CLINICAL TEST CONCEPT
 CLINICAL TEST CONCEPT Alu Rehab AS Bedriftsvegen 23 4353 Klepp Stasjon Norway T: +47 51 78 62 20 F: +47 51 42 58 25 post@my-netti.com Org.nr: NO 941 181 953 MVA Bank: 9688 05 00047 29.09.2015 Edited by;
CLINICAL TEST CONCEPT Alu Rehab AS Bedriftsvegen 23 4353 Klepp Stasjon Norway T: +47 51 78 62 20 F: +47 51 42 58 25 post@my-netti.com Org.nr: NO 941 181 953 MVA Bank: 9688 05 00047 29.09.2015 Edited by;
The Chailey Levels of Ability Assessment Charts
 The Chailey Levels of Ability Assessment Charts Assessment details NAME D.O.B. DIAGNOSIS DATE OF ASSESSMENT ASSESSMENT CENTRE NAME OF ASSESSOR Notes CHAILEY HERITAGE CLINICAL SERVICES Beggars Wood Road
The Chailey Levels of Ability Assessment Charts Assessment details NAME D.O.B. DIAGNOSIS DATE OF ASSESSMENT ASSESSMENT CENTRE NAME OF ASSESSOR Notes CHAILEY HERITAGE CLINICAL SERVICES Beggars Wood Road
Wheelchair/Scooter/Stroller Seating Assessment Form (CCP/Home Health Services) ( pages)
 Wheelchair/Scooter/Stroller Seating Assessment Form (CCP/Home Health Services) ( pages) Instructions A current wheelchair/scooter/stroller seating assessment conducted by a physician or a physical or occupational
Wheelchair/Scooter/Stroller Seating Assessment Form (CCP/Home Health Services) ( pages) Instructions A current wheelchair/scooter/stroller seating assessment conducted by a physician or a physical or occupational
Pediatric Physical Therapy Therapeutic Taping in CP 245
 RESEARCH REPORT The Effects of Therapeutic Taping on Gross Motor Function in Children with Cerebral Palsy Cheryl Burditt Footer, PhD, PT Department of Physical Therapy, Regis University, Denver, Colorado
RESEARCH REPORT The Effects of Therapeutic Taping on Gross Motor Function in Children with Cerebral Palsy Cheryl Burditt Footer, PhD, PT Department of Physical Therapy, Regis University, Denver, Colorado
William C Miller, PhD, FCAOT Professor Occupational Science & Occupational Therapy University of British Columbia Vancouver, BC, Canada
 William C Miller, PhD, FCAOT Professor Occupational Science & Occupational Therapy University of British Columbia Vancouver, BC, Canada THE L TEST MANUAL Version: November 2014 Table of Contents Introduction...
William C Miller, PhD, FCAOT Professor Occupational Science & Occupational Therapy University of British Columbia Vancouver, BC, Canada THE L TEST MANUAL Version: November 2014 Table of Contents Introduction...
Functional Ability Screening Tools for the Clinic
 Functional Ability Screening Tools for the Clinic Shelley Hockensmith,, P.T., NCS Objectives Review screening tools for physical or functional ability including Five Times Sit to Stand, Walking Speed,
Functional Ability Screening Tools for the Clinic Shelley Hockensmith,, P.T., NCS Objectives Review screening tools for physical or functional ability including Five Times Sit to Stand, Walking Speed,
BIOFEEDBACK AND HIPPOTHERAPY, FROM THE BOBATHCONCEPT, AS. HYPERTHERAPY WITH CONGENITAL HEMIPARESIS. (Daniël BENS, Belgium)
 BIOFEEDBACK AND HIPPOTHERAPY, FROM THE BOBATHCONCEPT, AS HYPERTHERAPY WITH CONGENITAL HEMIPARESIS. (Daniël BENS, Belgium) Many techniques of treatment for the child with cerebral palsy have developed over
BIOFEEDBACK AND HIPPOTHERAPY, FROM THE BOBATHCONCEPT, AS HYPERTHERAPY WITH CONGENITAL HEMIPARESIS. (Daniël BENS, Belgium) Many techniques of treatment for the child with cerebral palsy have developed over
A QUALITATIVE STUDY OF THE PERCEIVED HEALTH BENEFITS OF A THERAPEUTIC RIDING PROGRAM FOR CHILDREN WITH AUTISM SPECTRUM DISORDERS
 University of Kentucky UKnowledge University of Kentucky Doctoral Dissertations Graduate School 2010 A QUALITATIVE STUDY OF THE PERCEIVED HEALTH BENEFITS OF A THERAPEUTIC RIDING PROGRAM FOR CHILDREN WITH
University of Kentucky UKnowledge University of Kentucky Doctoral Dissertations Graduate School 2010 A QUALITATIVE STUDY OF THE PERCEIVED HEALTH BENEFITS OF A THERAPEUTIC RIDING PROGRAM FOR CHILDREN WITH
Physical Therapy throughout the Life Span. Tina Duong Stanford University Leslie Vogel, MSPT Seattle Children s Hospital
 Physical Therapy throughout the Life Span Tina Duong Stanford University Leslie Vogel, MSPT Seattle Children s Hospital Lifetime Goals for Physical Therapy Maximize Participation in school, work, community
Physical Therapy throughout the Life Span Tina Duong Stanford University Leslie Vogel, MSPT Seattle Children s Hospital Lifetime Goals for Physical Therapy Maximize Participation in school, work, community
Somatic Adaptation in Cerebral Palsy LINKING ASSESSMENT WITH TREATMENT: AN NDT PERSPECTIVE. By W. Michael Magrun, M.S., OTR/L
 Somatic Adaptation in Cerebral Palsy LINKING ASSESSMENT WITH TREATMENT: AN NDT PERSPECTIVE By W. Michael Magrun, M.S., OTR/L INTRODUCTION Somatic adaptation is one of the primary functions of the central
Somatic Adaptation in Cerebral Palsy LINKING ASSESSMENT WITH TREATMENT: AN NDT PERSPECTIVE By W. Michael Magrun, M.S., OTR/L INTRODUCTION Somatic adaptation is one of the primary functions of the central
Equipment Stopwatch A clear pathway of at least 10 m (32.8 ft) in length in a designated area over solid flooring 2,3.
 Core Measure: 10 Meter Walk Test (10mWT) Overview The 10mWT is used to assess walking speed in meters/second (m/s) over a short distance. Number of Test Items 1 item Scoring The total time taken to ambulate
Core Measure: 10 Meter Walk Test (10mWT) Overview The 10mWT is used to assess walking speed in meters/second (m/s) over a short distance. Number of Test Items 1 item Scoring The total time taken to ambulate
Gait Assessment & Implications in Geriatric Rehabilitation
 Gait Assessment & Implications in Geriatric Rehabilitation Therapy Network Seminars, Inc. Nicole Dawson, PT, PhD, GCS Learning Objectives Following completion of this webinar, participants will be able
Gait Assessment & Implications in Geriatric Rehabilitation Therapy Network Seminars, Inc. Nicole Dawson, PT, PhD, GCS Learning Objectives Following completion of this webinar, participants will be able
American Council on Exercise
 American Council on Exercise February 23, 2015 Fitnovatives Blog Exercise Progressions for Clients Who Are Overweight or Are Affected by Obesity While there is no single right way to train clients who
American Council on Exercise February 23, 2015 Fitnovatives Blog Exercise Progressions for Clients Who Are Overweight or Are Affected by Obesity While there is no single right way to train clients who
A Gillette Center of Excellence. Center for Gait and Motion Analysis. at Gillette Children s Specialty Healthcare
 A Gillette Center of Excellence Center for Gait and Motion Analysis at Gillette Children s Specialty Healthcare Centers of Excellence at Gillette Children s Specialty Healthcare Treating people who have
A Gillette Center of Excellence Center for Gait and Motion Analysis at Gillette Children s Specialty Healthcare Centers of Excellence at Gillette Children s Specialty Healthcare Treating people who have
RESEARCH ARTICLE THE EFFECTS OF FUNCTIONAL THERAPY ON MOTOR DEVELOPMENT IN CHILDREN WITH CEREBRAL PALSY
 RESEARCH ARTICLE THE EFFECTS OF FUNCTIONAL THERAPY ON MOTOR DEVELOPMENT IN CHILDREN WITH CEREBRAL PALSY Akbari A. PhD 1, Javad zadeh M. MD, Shahraki S. Bsc 3, Jahanshahi Javaran P. Bsc 3 1. Associate Professor
RESEARCH ARTICLE THE EFFECTS OF FUNCTIONAL THERAPY ON MOTOR DEVELOPMENT IN CHILDREN WITH CEREBRAL PALSY Akbari A. PhD 1, Javad zadeh M. MD, Shahraki S. Bsc 3, Jahanshahi Javaran P. Bsc 3 1. Associate Professor
CLINICIANS CORNER So Is NDT Just Everything, Then? The Answers to Three Questions Pinpoint the NDT Approach
 From NDTA Network on the Net, 2006 CLINICIANS CORNER So Is NDT Just Everything, Then? The Answers to Three Questions Pinpoint the NDT Approach By Marcia Stamer, PT As an NDTA instructor, I learn a lot
From NDTA Network on the Net, 2006 CLINICIANS CORNER So Is NDT Just Everything, Then? The Answers to Three Questions Pinpoint the NDT Approach By Marcia Stamer, PT As an NDTA instructor, I learn a lot
20944_Exercise Diary:20944_Exercise Diary 7/10/09 09:46 Page 1 Exercise Diary
 Exercise Diary Name: Hospital number: Contact number for renal unit: Contents Page Introduction 4 Your clothing and trainers 5 Diet and fluid management 6 Starting your exercise programme 6 Tips for succeeding
Exercise Diary Name: Hospital number: Contact number for renal unit: Contents Page Introduction 4 Your clothing and trainers 5 Diet and fluid management 6 Starting your exercise programme 6 Tips for succeeding
MODULE 10: Breaking down the Exercises - Stability Exercises
 MODULE 10: Breaking down the Exercises - Stability Exercises Stability is a core component of the Ridefit program, because so much of riding is dependent on the stability of the rider s body in the saddle.
MODULE 10: Breaking down the Exercises - Stability Exercises Stability is a core component of the Ridefit program, because so much of riding is dependent on the stability of the rider s body in the saddle.
 Too Early for Mobility? The Benefits of Early Mobility on Pediatric Development Disclosures Julie Cagney, PT, DPT Sarah Murdoch, PT, DPT, ATP Kaitlin MacDonald, MOT, OTR/L Have no financial or non-financial
Too Early for Mobility? The Benefits of Early Mobility on Pediatric Development Disclosures Julie Cagney, PT, DPT Sarah Murdoch, PT, DPT, ATP Kaitlin MacDonald, MOT, OTR/L Have no financial or non-financial
Improving quality of life! INNOWALK Up, Stand and Move
 Improving quality of life! INNOWALK Up, Stand and Move UP, STAND AND MOVE Children usually move into a standing position at 9 12 months of age. An upright standing position with the possibility of movement,
Improving quality of life! INNOWALK Up, Stand and Move UP, STAND AND MOVE Children usually move into a standing position at 9 12 months of age. An upright standing position with the possibility of movement,
Quick Reference Guide
 Quick Reference Guide Quick Reference Guide Products for life from people who care. Page The Rifton Title TRAM Quick Reference Guide Contents Introduction 1 Importance of Proper Positioning 2 Key Components
Quick Reference Guide Quick Reference Guide Products for life from people who care. Page The Rifton Title TRAM Quick Reference Guide Contents Introduction 1 Importance of Proper Positioning 2 Key Components
Canadian Stroke Best Practices Table 3.3A Screening and Assessment Tools for Acute Stroke
 Canadian Stroke Best Practices Table 3.3A Screening and s for Acute Stroke Neurological Status/Stroke Severity assess mentation (level of consciousness, orientation and speech) and motor function (face,
Canadian Stroke Best Practices Table 3.3A Screening and s for Acute Stroke Neurological Status/Stroke Severity assess mentation (level of consciousness, orientation and speech) and motor function (face,
Starting a Strength Training Program
 MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Starting a Strength Training Program About This Kit The key to improving strength is applying resistance to the muscle
MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Starting a Strength Training Program About This Kit The key to improving strength is applying resistance to the muscle
HIPPOTHERAPY AND CEREBRAL PALSY ADDUCTOR ACTIVITY, McGibbon 967 motor function, 11,12 walking energy expenditure, 11 and trunk postural coordination.
 966 ORIGINAL ARTICLE Immediate and Long-Term Effects of Hippotherapy on Symmetry of Adductor Muscle Activity and Functional Ability in Children With Spastic Cerebral Palsy Nancy H. McGibbon, MS, PT, HPCS,
966 ORIGINAL ARTICLE Immediate and Long-Term Effects of Hippotherapy on Symmetry of Adductor Muscle Activity and Functional Ability in Children With Spastic Cerebral Palsy Nancy H. McGibbon, MS, PT, HPCS,
Table 3.1: Canadian Stroke Best Practice Recommendations Screening and Assessment Tools for Acute Stroke Severity
 Table 3.1: Assessment Tool Number and description of Items Neurological Status/Stroke Severity Canadian Neurological Scale (CNS)(1) Items assess mentation (level of consciousness, orientation and speech)
Table 3.1: Assessment Tool Number and description of Items Neurological Status/Stroke Severity Canadian Neurological Scale (CNS)(1) Items assess mentation (level of consciousness, orientation and speech)
MANUAL THE ANKLE TRAINER. Movement-Enabling Rehab Equipment
 Movement-Enabling Rehab Equipment MANUAL THE ANKLE TRAINER Neurogym Technologies Inc. 2016 100-1050 Morrison Drive, Ottawa, ON, Canada neurogymtech.com ? FOR SERVICE OR PART INFORMATION CALL: + 1.877.523.4148
Movement-Enabling Rehab Equipment MANUAL THE ANKLE TRAINER Neurogym Technologies Inc. 2016 100-1050 Morrison Drive, Ottawa, ON, Canada neurogymtech.com ? FOR SERVICE OR PART INFORMATION CALL: + 1.877.523.4148
Range of motion and positioning
 Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY
 Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Functional Strength Exercise Guide
 Functional Strength Exercise Guide Fast, convenient weight training that helps you look better, feel better and perform better during everyday activities. Welcome to Functional Strength Training from Horizon
Functional Strength Exercise Guide Fast, convenient weight training that helps you look better, feel better and perform better during everyday activities. Welcome to Functional Strength Training from Horizon
Chapter 9 PHYSICAL ACHIEVEMENT TRAINING IN THE ARMY CADET FORCE
 General Chapter 9 PHYSICAL ACHIEVEMENT TRAINING IN THE ARMY CADET FORCE SECTION 1. INTRODUCTION 0901. As part of the APC syllabus cadets are required to pass simple physical achievement tests at 1-, 2-,
General Chapter 9 PHYSICAL ACHIEVEMENT TRAINING IN THE ARMY CADET FORCE SECTION 1. INTRODUCTION 0901. As part of the APC syllabus cadets are required to pass simple physical achievement tests at 1-, 2-,
EXERCISE AND CYSTIC FIBROSIS: MY EXERCISE RECORD
 EXERCISE AND CYSTIC FIBROSIS: MY EXERCISE RECORD My exercise goals Name What is my target heart rate? What is the maximum heart rate I should not exceed? What is my target rating of perceived exertion?
EXERCISE AND CYSTIC FIBROSIS: MY EXERCISE RECORD My exercise goals Name What is my target heart rate? What is the maximum heart rate I should not exceed? What is my target rating of perceived exertion?
TheraSuit Orthosis I. The History and Development of TheraSuit :
 -- www.genius4kids.com -- TheraSuit Orthosis I. The History and Development of TheraSuit : TheraSuit, a soft, dynamic, proprioceptive orthotic, is a full-featured dynamic correction clothing. The invention
-- www.genius4kids.com -- TheraSuit Orthosis I. The History and Development of TheraSuit : TheraSuit, a soft, dynamic, proprioceptive orthotic, is a full-featured dynamic correction clothing. The invention
MUST BE SUBMITTED BY PHONE
 Neurodevelopmental Program: PT Therapy Clinical Worksheet Required for all Neurodevelopmental Conditions Please use this fax form for NON-URGENT requests only. Failure to provide all relevant information
Neurodevelopmental Program: PT Therapy Clinical Worksheet Required for all Neurodevelopmental Conditions Please use this fax form for NON-URGENT requests only. Failure to provide all relevant information
Evaluating Fundamental
 12 Locomotor Lab 12.1 Evaluating Fundamental Skills Purpose Practice in learning to observe and evaluate locomotor skills from video performance. Procedures Listed below are several websites showing children
12 Locomotor Lab 12.1 Evaluating Fundamental Skills Purpose Practice in learning to observe and evaluate locomotor skills from video performance. Procedures Listed below are several websites showing children
Shining Hope Farms. Annual Report Based on Fiscal Year 2017
 Shining Hope Farms Annual Report Based on Fiscal Year 2017 is a 501(c)(3) organization whose mission is to enable children and adults with disabilities to achieve functional goals through the use of equine
Shining Hope Farms Annual Report Based on Fiscal Year 2017 is a 501(c)(3) organization whose mission is to enable children and adults with disabilities to achieve functional goals through the use of equine
You may begin these exercises in the Intensive Care Unit. Complete
 Exercises for Patients After Open Heart Surgery You may begin these exercises in the Intensive Care Unit. Complete the exercises in a sitting position. Sit upright looking straight ahead with your chin
Exercises for Patients After Open Heart Surgery You may begin these exercises in the Intensive Care Unit. Complete the exercises in a sitting position. Sit upright looking straight ahead with your chin
2017 COS ANNUAL MEETING AND EXHIBITION HOME EXERCISES
 UPPER BODY Push Up From a push up position. Lower whole body down to floor. Press up to return to start position. Maintain abdominal hollow and neutral spinal alignment throughout movement. Note: Perform
UPPER BODY Push Up From a push up position. Lower whole body down to floor. Press up to return to start position. Maintain abdominal hollow and neutral spinal alignment throughout movement. Note: Perform
EXERCISE AND CYSTIC FIBROSIS: MY EXERCISE RECORD
 EXERCISE AND CYSTIC FIBROSIS: MY EXERCISE RECORD My exercise goals Name What is my target heart rate? What is the maximum heart rate I should not exceed? What is my target rating of perceived exertion?
EXERCISE AND CYSTIC FIBROSIS: MY EXERCISE RECORD My exercise goals Name What is my target heart rate? What is the maximum heart rate I should not exceed? What is my target rating of perceived exertion?
Evaluating Movement Posture Disorganization
 Evaluating Movement Posture Disorganization A Criteria-Based Reference Format for Observing & Analyzing Motor Behavior in Children with Learning Disabilities By W. Michael Magrun, MS, OTR 3 R D E D I T
Evaluating Movement Posture Disorganization A Criteria-Based Reference Format for Observing & Analyzing Motor Behavior in Children with Learning Disabilities By W. Michael Magrun, MS, OTR 3 R D E D I T
Physical and Occupational Therapy after Spine Surgery. Preparation for your surgery
 Physical and Occupational Therapy after Spine Surgery Preparation for your surgery Agenda Pre-Operative Exercises What to Expect Post-Operative Plan Spinal Precautions Post-Discharge Plan S A I N T LU
Physical and Occupational Therapy after Spine Surgery Preparation for your surgery Agenda Pre-Operative Exercises What to Expect Post-Operative Plan Spinal Precautions Post-Discharge Plan S A I N T LU
The ENERGI Product Line as a Strength and Flexibility Builder
 The ENERGI Product Line as a Strength and Flexibility Builder Ian Proud & Elizabeth Ingraham November 2009 Page 1 of 11 Contents Summary.. 3 Test & Sample Description.. 3 Observations Upper Body Strength
The ENERGI Product Line as a Strength and Flexibility Builder Ian Proud & Elizabeth Ingraham November 2009 Page 1 of 11 Contents Summary.. 3 Test & Sample Description.. 3 Observations Upper Body Strength
