Investigation of the Feasibility of an Intervention to Manage Fall Risk in Wheeled Mobility Device Users with Multiple Sclerosis
|
|
|
- Audrey Cooper
- 5 years ago
- Views:
Transcription
1 Investigation of the Feasibility of an Intervention to Manage Fall Risk in Wheeled Mobility Device Users with Multiple Sclerosis Laura A. Rice, PhD, MPT, ATP; Zadok Isaacs, MS; Cherita Ousley, MS; Jacob Sosnoff, PhD Background: Falls are a common concern for wheeled mobility device users with multiple sclerosis (MS); however, no evidence-based fall prevention programs have been developed to meet the specific needs of the population. We examine the preliminary feasibility of a fall management intervention in wheeled mobility device users with MS. Methods: Study participants were exposed to an intervention program targeting risk factors for falls, including transfer skills and seated postural control. The feasibility of the program was evaluated by assessing participant perspectives, cost, recruitment rates, study adherence, participant retention, safety, and the ability to collect primary and secondary outcomes, including fall frequency, concerns about falling, transfer quality, and seated postural control. Results: 16 wheeled mobility device users completed the program, which was found to be feasible and was positively evaluated by participants. No adverse events were experienced. After exposure to the intervention, fall frequency significantly decreased (P <.001) and transfer quality (P =.001) and seated postural control (P =.002) significantly improved. No significant differences were found regarding concerns about falling (P =.728). Conclusions: This study examined the feasibility of an intervention program to manage fall risk in wheeled mobility device users with MS. The program was found to be feasible, and preliminary results showed the intervention to be effective in decreasing fall frequency. Additional testing is needed to further examine the efficacy and long-term impact of the intervention. Int J MS Care. 2018;20: Falls are a common concern in persons affected by multiple sclerosis (MS). Falls may result in physical injury that requires hospitalization 1 and/or development of a dysfunctional fear of falling. 2 Approximately two-thirds of the MS population report concerns about falling 3 that might result in self-imposed activity curtailment, loss of confidence, difficulty performing From the Department of Kinesiology and Community Health, College of Applied Health Sciences, University of Illinois at Urbana- Champaign, Champaign, USA. Correspondence: Laura Rice, PhD, MPT, ATP, 116 Huff Hall, 1206 S. Fourth St., Champaign, IL 61820; ricela@illinois.edu. Note: Supplementary material for this article is available at ijmsc.org. DOI: / Consortium of Multiple Sclerosis Centers. typical societal roles, loss of independence, and physiologic deconditioning. 4 Ultimately, this disuse-disability cycle may place individuals at greater risk for falls. The adverse physical and psychosocial impact of falls has led to a growing amount of research examining prevention strategies to decrease the frequency of falls in ambulatory individuals. 5 Overall, this work has highlighted that some fall risk factors, such as impaired balance and functional mobility, are modifiable, and there is great potential to prevent falls in people with MS using targeted rehabilitation interventions. 6 Unfortunately, most research in the MS population thus far has focused almost exclusively on community ambulators. This focus ignores the approximately 25% of the MS population who use a wheeled mobility device (manual wheelchair, power wheelchair, scooter, etc.) as their primary means of community mobility. 7 Owing 121
2 Rice et al. older than 18 years, self-reported Patient-Determined Disease Steps 10 level of 7 (ie, main form of mobility is via a wheeled mobility device), self-reported inability to ambulate outside the home, and self-reported ability to transfer with moderate assistance (participant expends 50%-74% of the effort) or less. Exclusion criteria included an MS exacerbation in the past 30 days and unable to sit upright for at least 1 hour. After participants were enrolled in the study and signed an institutional review board approved informed consent form, a baseline assessment was performed, as described herein. After collection of baseline data, an intervention program to manage fall risk and concerns about falling was implemented. Details regarding the content of the intervention are provided herein. All the participants were reevaluated 12 weeks later using the same protocol performed during the baseline assessment. Feasibility As suggested by Thabane et al., 11 feasibility outcomes include the assessment of cost, recruitment and retention rates, adherence to the proposed program, safety, and the ability to collect primary and secondary outcomes. The cost of the study was calculated by summing all of the direct costs associated with performance of the study. Indirect costs to support administrative activities were not included. The recruitment rate was assessed by calculating the percentage of participants who enrolled in the study from the pool of known participants who were exposed to the recruitment materials. Study adherence was evaluated by assessing the number of self-reported exercise sessions performed by participants and the number of times participants self-reported that they reviewed the transfer education materials. The retention rate was calculated as a percentage of the number of participants who completed both study visits and engaged in the intervention program. Safety was evaluated by assessing the number of adverse events self-reported by participants. Finally, the ability to collect primary and secondary outcomes was assessed by evaluating the amount of missing data that occurred during each assessment and examination of the outcome assessments performed. Participant Perspectives Participant perspectives on the study were evaluated by asking direct questions about the content of the intervention program. Perspectives were examined in a one-on-one interview during the postintervention assessment. Participants were asked whether they found the transfer education to be helpful, whether they significantly changed the way they performed their transfers, and whether they felt that the exercise program signifito the differences in physical characteristics (eg, muscle strength, balance impairments) and functional mobility limitations (eg, assistive devices used) between ambulatory and wheeled mobility device users with MS, individualized investigation of unique strategies to prevent falls is needed. Indeed, there is evidence that approximately 45% of individuals with MS who use a wheeled mobility device as their primary means of mobility report at least one fall per 6-month period, and approximately 30% of those fallers report frequent falls. 8 A recent literature review of wheeled mobility device users with various disabilities evaluated factors related to fall risk. 9 Results indicate that transfers (ie, moving from a wheelchair/scooter to another surface, such as a bed or chair) were found to be associated with falls in 54.5% of the studies reviewed and impaired seated balance control was associated with falls in 36.3% of the studies evaluated. A lack of fall prevention interventions for wheeled mobility device users was also noted. Importantly, there were no fall prevention programs specifically for individuals with MS who use wheeled mobility devices. 9 Therefore, the purpose of this article is to describe an intervention program designed to prevent falls and concerns about falling by targeting risk factors associated with falls in wheeled mobility device users, to describe the preliminary feasibility of the program, and to report preliminary results. To our knowledge, this is the first study to describe the implementation of an intervention program to manage falls and concerns about falling in wheeled mobility device users with MS. It was hypothesized that the program will be feasible and that, after exposure to the intervention program, participants will display improved transfer quality and seated postural control and a decreased frequency of falls and concerns about falling. Methods Study Design A single-group interventional study was performed to examine the preliminary feasibility and efficacy of an intervention program to decrease fall frequency and concerns about falling in wheeled mobility device users with MS. All study-related procedures were approved by the institutional review board of the University of Illinois at Urbana-Champaign. A sample of convenience of 16 participants was recruited through the North American Research Committee on Multiple Sclerosis (NAR- COMS) research registry, posting of flyers, and word of mouth. Individuals were invited to participate if they met the following inclusion criteria: a diagnosis of MS, 122
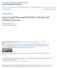
3 Managing Fall Risk in Wheeled Mobility Device Users cantly improved their sitting balance abilities. Finally, participants were asked to provide any other feedback they had about the program. Outcome Assessments During the baseline assessment, participants completed a general demographic questionnaire and were asked information about the length of time they had had MS, wheeled mobility use, and the frequency of falls in the previous 6 months. A fall was defined as unintentionally coming to rest on the ground or lower level. 12 Participants were also asked to complete the Spinal Cord Injury Falls Concern Scale (SCI-FCS). 13 The SCI-FCS examines concerns about falling by asking participants to rate the level of concern they have about falling on a 4-point scale ranging from 1 = not at all concerned to 4 = very concerned when performing 16 common activities of daily living. Total scores range from 16 to 64. The SCI-FCS has not been validated in individuals with MS but evaluates activities pertinent to a variety of nonambulatory individuals. In the spinal cord injury population, the SCI-FCS has excellent internal and testretest reliability (Cronbach α = 0.92, intraclass correlation coefficient = 0.93). 13 There is currently no validated tool available to evaluate fall concerns during functional activities in individuals with MS who use a wheeled mobility device. 9 After completion of the surveys, participants were asked to perform up to four transfers to and from a solid mat table. Participants were instructed to perform the transfers as they normally would at home, and they could use any type of assistive device, such as a transfer board, as preferred. Participants could also receive assistance from a caregiver, if necessary. Transfer quality was objectively evaluated using the Transfer Assessment Instrument (TAI) 14 by a trained researcher. Items such as hand placement or the distance from the target surface are assessed, not how much assistance the participant requires. A final score is given ranging from 0 = very poor transfer quality to 10 = excellent transfer quality. The TAI has been found to be valid and reliable in fulltime wheelchair users, including individuals with MS. 15 Seated postural control was evaluated using a Bertec force plate (model FP ; Bertec Inc, Columbus, OH). Per the protocol established by Shin and Sosnoff, 16 seated postural control was assessed by having participants sit with their arms resting in their lap with both their feet and back unsupported for 30 seconds. After the quiet sitting trial, participants were instructed to lean as far forward, backward, and side-to-side as possible in a circular pattern for 30 seconds to assess the functional boundary of stability. The functional boundary of stability examines how far a participant is capable of leaning without loss of balance. From the force plate data obtained, virtual time to contact was calculated. 17 Virtual time to contact quantifies the temporal proximity of an individual to their functional stability boundary 16 and takes into consideration the relationship between center of pressure and the borders of the functional base of support, 18 as described in Figure 1. Per Slobounov et al., 17 virtual time to contact was calculated using a position vector of the center of pressure on a virtual trajectory, τ i (t), determined for each moment in time, t i during static sitting, on the basis of the instantaneous center of pressure velocity and acceleration: x, y(τ) = r xi,yi (t i ) + v xi,yi (t i )τ + a xi,yi (t i )τ 2 2 where r xi,yi (t i ) is the instantaneous position vector, v xi,yi (t i ) is the instantaneous velocity vector, and a xi,yi (t i ) is the instantaneous acceleration vector in the x and y directions. Higher values indicate increased stability. The entire assessment performed at the baseline study visit was repeated at the 12-week study visit. After completion of the 12-week study visit, participants were asked a series of questions to examine their perceived functional changes as a result of the intervention program. Intervention Program After completing the baseline assessment, participants were exposed to an education intervention focused on improving the quality of transfer skills and seated postural control to decrease fall frequency and concerns about falling. The education was provided to study participants in individual sessions by a physical therapist COP Virtual Trajectory Functional Stability Boundary Figure 1. Visual representation of the functional boundary of stability and center of pressure (COP) 123
4 Rice et al. during a single session that lasted approximately 45 minutes. The education was implemented in a private room with a height-adjustable mat table with sufficient room for participants to perform transfers and seated exercises. The intervention was developed by a physical therapist (L.A.R.) with more than 10 years of experience providing instruction to wheeled mobility device users. Transfer Quality First, participants received instruction on transfer quality focused on how to perform transfers in a safe manner to reduce the frequency of falls and concerns about falling. The information presented was informed from previous research describing the circumstances of falls among wheeled mobility device users with other disabilities 19 and transfer biomechanics. 20 To our knowledge, there are currently no other peer-reviewed fall prevention interventions designed for wheeled mobility device users with MS. 9 During the intervention, participants were individually shown a 9-minute video describing how to correctly perform a transfer. The video broke down the performance of a transfer into three phases: setup, flight, and end phases. For example, participants were educated to place their feet on the floor, whenever possible, to create a solid base of support during the flight phase of the transfer. Paper handouts that mirrored the information presented in the video were also given to participants. Separate materials were developed for participants performing independent and assisted transfers (Appendix S1 [parts a and b], which is published in the online version of this article at ijmsc. org). As the video played, the physical therapist would frequently stop the video to discuss specific aspects of the transfer that the participant had difficulty performing during the baseline assessment or to answer questions posed by the participant. After completion of the video, the participant was given an opportunity to practice the transfers. Feedback on performance was provided and individual technique was fine-tuned by the physical therapist. Participants were given a copy of the paper handouts and video to take home. Participants were instructed to review the materials at least once every other week. Exercise Protocol Next, participants were instructed on exercises designed to improve seated postural control. The protocol was designed by a physical therapist (L.A.R.) using exercises described by Kisner and Colby 21 to be performed in the participant s home without any equipment. Participants were individually instructed on how to perform the exercises and were given a paper handout describing exercise techniques (Appendix S2). After instruction, participants were given an opportunity to practice the exercises and received feedback on their performance by the physical therapist. If needed, the exercises were modified for individual participants based on their strength impairments and other limitations. Participants were instructed to perform the exercises three times per week. Participant Monitoring Between the baseline and 12-week study visits, participants were called every other week to inquire about their adherence to the intervention program. Participants were asked whether they had any questions about the transfer techniques and to remind them to watch the instructional transfer video every other week. Participants were also asked how well they were tolerating the exercise program. If participants reported that the exercises were too easy, they were instructed to increase the frequency of performance, and to reduce the frequency if too difficult. Participants were also asked to report the frequency of their falls during the past 2 weeks. To ensure that the frequency of falls was collected in an objective, nonbiased manner, a standardized script was used. Data Analysis Data were analyzed using IBM SPSS Statistics for Windows, version 22.0 (IBM Corp, Armonk, NY). Descriptive statistics were used to evaluate feasibility. To evaluate program outcomes, general exploratory analysis was performed, and Shapiro-Wilk testing found virtual time to contact to be normally distributed. All other variables of interest were found to be nonnormally distributed or used ordinal data. To examine the differences before and after exposure to the intervention, paired t tests (normally distributed data) and a generalized linear model (nonnormally distributed/ordinal data) were used. Effect sizes (d) were calculated using Cohen s d z. Per Lakens, 22 Cohen s d z values were calculated by examining the differences in mean scores between assessment points divided by the SD of the difference scores and were interpreted as small (d 0.2), moderate (d ~ 0.5), or large (d 0.8). Significance was set a priori at P =.05. Due to the pilot nature of the study, no corrections were made for multiple comparisons. Results Study Participants Between May 1, 2014, and May 31, 2015, 16 participants were enrolled and tested (Figure 2). All the participants completed both study visits. Participants 124
5 Did not meet inclusion criteria (n = 3) Reasons: Recent MS exacerbation (n = 1) Performance of a dependent transfer (n = 2) had a mean ± SD age of 58.1 ± 11.9 years and duration of diagnosis of MS of 16.9 ± 8.7 years. At the start of the study, 75% of participants reported at least one fall in the past 6 months, with a mean ± SD fall frequency of 1.7 ± 2.7 per month (Table 1). Feasibility Based on the criteria established by Thabane et al., 11 the study was found to be feasible but requires modifications. All the participants who started the study completed both assessment sessions and the intervention program, and no participants reported injuries or impairments associated with the intervention program. The direct costs associated with the study were approximately $30,000 ($1875 per participant) and included salary support for personnel ($25,000), development Table 1. Demographic and baseline data for the 16 study participants Variable Value Age, mean ± SD, y 58.1 ± 11.9 Sex, No. (%) Female 11 (69) Male 5 (31) Type of MS, No. (%) Relapsing-remitting 6 (37.5) Primary progressive 2 (12.5) Secondary progressive 7 (43.8) Progressive relapsing 1 (6.3) Time with MS, mean ± SD, y 16.9 ± 8.7 Falls per month, mean ± SD, No. 1.7 ± 2.7 Type of wheeled mobility device, No. (%) Power wheelchair 6 (37.5) Manual wheelchair 9 (56.3) Scooter 1 (6.3) Abbreviation: MS, multiple sclerosis. Participants responding to recruitment materials (n = 29) Declined to participate (n = 10) Reasons: Unable to travel to testing location (n = 5) Unable to schedule testing session (n = 5) Figure 2. Participant recruitment MS, multiple sclerosis 125 Managing Fall Risk in Wheeled Mobility Device Users and production of transfer education videos ($800), general materials to support the study (including participant handouts) ($500), participant payments ($2000), and recruitment expenses ($1700). In addition, a $10,000 force platform was used to evaluate seated postural control that was previously owned by the research team. Study recruitment materials were sent to 137 individuals within an approximately 3-hour driving distance from the research laboratory, and 29 (21%) responded. Of the 29 people who responded, 16 (55%) were enrolled in the study, 10 (35%) declined to participate after learning more about the study, and 3 (10%) did not meet the inclusion criteria (Figure 2). Participants self-reported viewing the transfer education video a mean ± SD of 3.5 ± 2.7 times and performing the exercises a mean ± SD of 2.86 ± 1.92 times per week. Regarding data collection, missing data occurred for two participants during collection of the SCI-FCS data, and one participant did not complete the patient perspective questions. No missing data occurred for the other outcomes of interest. Participant-Perceived Improvements The intervention was well-tolerated, and no participants reported injuries or impairments associated with the intervention. When asked Did you find the transfer education helpful? most participants (n = 14 [87.5%]) reported that they did. Twelve of 15 participants (80%; one participant did not provide a response) responded in a positive manner when asked Did you significantly change the way you perform your transfers? When asked to describe the changes that were made, six participants reported that they changed how they positioned their body, five changed how they positioned their chair, four reported changing their overall technique, and four reported taking more precautions during their transfers. Regarding the exercises, when asked Do you feel that the exercises significantly improved your sitting balance, 13 of 15 participants (86.7%; one participant did not provide a response) reported significant improvements. In response to the question Do you have any other comments about the transfer and exercise education? eight participants provided a response. Regarding the structure of the education materials, two participants thought the materials were organized well, and one participant did Enrolled in study (n = 16)
6 Rice et al. not like the materials (but did not specify why). Regarding the difficulty of the exercises, two participants felt that the exercises were too hard, and one felt that they were too easy. Finally, one participant wished that the materials were more specific to individuals with MS, and one thought that the monitoring was helpful. Fall Frequency and Concerns About Falling Fall frequency was found to be nonnormally distributed (Shapiro-Wilk P <.001), and the SCI-FCS score is measured on an ordinal scale; therefore, nonparametric statistics were used to evaluate both variables. At the 12-week study visit, participants reported a significant mean ± SD reduction in fall frequency (preintervention: 1.7 ± 2.7 falls/mo; postintervention: 1.0 ± 1.2 falls/mo; P <.001, d z = 0.26) (Table 2). No significant differences were found in mean ± SD SCI-FCS scores (preintervention: ± 7.5, postintervention: 32.8 ± 11.3, P =.728, d z = 0.01). Transfer Quality Transfer quality, as measured by the TAI, is ordinal in nature; therefore, nonparametric statistics were used. After exposure to the intervention, participants showed significant improvements in mean ± SD TAI scores (preintervention: 6.1 ± 2.3, postintervention: 8.0 ± 2.3, P =.001, d z = 0.97) (Table 2). Seated Postural Control Seated postural control, as evaluated by virtual time to contact, was found to be normally distributed (Shapiro-Wilk P =.553). After exposure to the intervention, mean ± SD values of virtual time to contact significantly improved (preintervention: 1.2 ± 0.3, postintervention: 1.3 ± 0.4, P =.002, d z = 0.83) (Table 2). Discussion The primary results of this feasibility study indicate that an intervention program designed to decrease fall frequency and concerns about falling by providing Table 2. Differences in outcomes preintervention to postintervention Outcome Preintervention Postintervention P value Effect size (Cohen s d z ) Fall frequency, 1.7 ± ± 1.2 <.001 a 0.26 No./mo SCI-FCS score ± ± TAI score 6.1 ± ± a 0.97 VTC value 1.2 ± ± a 0.83 Note: Unless otherwise indicated, data are given as mean ± SD. Abbreviations: SCI-FCS, Spinal Cord Injury Falls Concern Scale; TAI, Transfer Assessment Instrument; VTC, virtual time to contact. a P <.05. education on methods to improve transfer quality and exercises to improve seated postural control was feasible to perform, well tolerated, and received in a positive manner by study participants. Subjectively, most participants reported that they significantly changed the way they performed their transfers and that the exercises significantly improved sitting balance. Objectively, fall frequency significantly decreased and transfer quality and seated postural control significantly improved after exposure to the intervention. No significant differences were found regarding concerns about falling. Further testing is needed to examine the long-term impact of the intervention in a larger group of wheeled mobility device users with MS. Due to the complex nature of falls, a longer follow-up period with additional study participants is necessary to examine the full impact of the intervention. The results of the feasibility and subjective analysis indicate that the intervention is possible, well tolerated, and perceived to be beneficial by study participants. The cost of the study is an area of concern. The direct costs associated with the study totaled approximately $40,000, including the cost of the force plate ($10,000), which, although not excessive, requires considerable resources. To reduce cost, future studies may consider use of the Function In Sitting Test 23 to assess seated postural control instead of using a force plate. Our research team recently assessed the reliability and validity of the tool in nonambulatory individuals with MS and found it to be reliable and valid. 24 Funds to support the salaries of the study investigators developing the study protocol may also be reduced in future iterations of the study. To perform the study intervention using the currently developed materials, we anticipate the cost to be approximately $12,200. These costs would include general study materials, including participant handouts, DVDs, etc. ($500); participant payments ($2000: $100/participant plus travel expenses); recruitment expenses ($1700); and payment of a research assistant to implement the study intervention ($8000). The recruitment rate of study participants is also an area of concern. Five of the ten participants who declined to participate did so due to transportation limitations. Independent transportation is particularly difficult for individuals who would meet the inclusion criteria. Also, the study was performed in a rural area with limited accessible public transportation. In the future, researchers should consider performing the study in a metropolitan area in which participants can use an extensive network of accessible public or paratransit resources. In addition, future studies should examine 126
7 Managing Fall Risk in Wheeled Mobility Device Users the feasibility and validity of converting the intervention program into an Internet-based program with the capacity to remotely evaluate transfer and exercise performance for individuals with limited resources to participate in in-person therapeutic activities. After exposure to the education intervention, preliminary results showed that transfer quality significantly improved, and a large effect size was noted. Such improvements are noteworthy as transfers are frequently associated with falls. 9 Improving quality, therefore, has a good potential to positively influence fall frequency. Improvements in functional mobility and community participation may also be seen as a result of improved transfer quality, however further testing is needed to examine these concepts. Similar results were found by Rice et al. 25 in an examination of full-time wheelchair users with spinal cord injury who received a structured transfer education intervention during acute inpatient rehabilitation. In this previous study, however, the program had a greater impact on participants who required assistance to transfer. The present results, however, found the program to be effective among participants performing independent transfers. In addition to transfers, impaired seated postural control has previously been found to be associated with falls in wheeled mobility device users. 9 Thus, the significant improvements seen in seated postural control potentially had an influence on fall frequency. To our knowledge, no previous studies have examined the impact of an exercise program targeting improvements in seated postural control on fall frequency. A recent study in older ambulatory adults with MS by Sosnoff et al. 26 found similar results that indicate that a home-based exercise program can reduce fall risk. In addition to the potential effect on fall frequency, improvements in seated postural control are important because impaired balance can affect a variety of functional activities necessary for performing activities of daily living. Not only does impaired balance affect an individual s ability to transfer and remain upright when sitting unsupported, necessary functional activities such as cooking, bathing, and dressing are also negatively affected. Further investigation is needed to examine the long-term impact of the intervention program and to determine whether differences exist in a larger group of participants over a longer period. After exposure to the intervention, fall frequency significantly decreased, although a small effect size was found. Programs designed to prevent falls from occur- ring are important because falls can result in substantial physical 1 and psychological impairments. 2 A recent study by Bisson et al. 27 found that after a fall, 27.6% of individuals with MS lay on the floor or ground for more than 10 minutes and 4.7% were on the ground for more than an hour. Such wait times can result in further development of a fear of falling and decreased participation in activities of daily living. 28 Thus, the development of programs to prevent falls is important for the overall health and well-being of wheeled mobility device users with MS. To our knowledge, there are currently no interventions focused on fall prevention in wheeled mobility device users with MS and few available for wheeled mobility device users in general. 9 Dyer et al. 29 examined the impact of an intervention program designed to decrease fall frequency in individuals after amputation of a lower-extremity limb. After implementation of the intervention, fall frequency decreased by 5%. In comparison, the intervention in the present study resulted in a 41.2% decrease in fall incidence. Although a significant difference was found in fall frequency, the effect size was small (d z = 0.26). In addition, no significant difference and a small effect size were found regarding concerns about falling. As a result of the complex nature of falls and concerns about falling, it is likely that longer follow-up is necessary to fully assess the impact of the program on this important outcome. Making a significant change regarding the concerns that people feel about falling may require several months of a reduction in fall frequency for the individual to feel increased confidence. There are several limitations associated with this study that require consideration. The small sample size (N = 16) may reduce the generalizability of the results to a larger group of individuals with MS who use a wheeled mobility device as their primary means of mobility. Another limitation is the limited follow-up period. Participants were evaluated 3 months after implementation PRACTICE POINTS Falls are common in wheeled mobility device users with MS; however, few peer-reviewed intervention programs are available that are designed to decrease fall risk and enhance functional mobility. The preliminary investigation of a home-based intervention program designed to reduce fall frequency was found to be feasible to perform, was well received by study participants, and resulted in a significant reduction in fall frequency. 127
8 Rice et al. of the intervention, thus limiting our ability to investigate the long-term impact of these findings. Future studies with longer follow-up are needed to examine the long-term impact of the intervention on fall frequency and concerns about falling. It is likely that changes in fall frequency and concerns about falling require more than 3 months to fully manifest. Finally, the homebased nature of the study limits our ability to determine whether participants were performing the exercises and reviewing the transfer materials, as instructed. Although follow-up telephone calls were made to participants every other week to inquire about their adherence to the program, participants may have misreported what actually occurred. In conclusion, this preliminary feasibility study evaluated the impact of an intervention on fall frequency, concerns about falling, transfer skills, and seated postural control of wheeled mobility device users with MS. Preliminary results indicate that the educational intervention was well tolerated by participants and was found to be helpful. In addition, the preliminary assessment indicates that fall frequency decreased but concerns about falling did not. Transfer quality and seated postural control significantly improved. Although the findings of the study are preliminary, such results are noteworthy because this seems to be the first research study to examine methods to manage fall frequency in wheeled mobility device users with MS. The improvements found in transfer quality and seated postural control may have an added benefit of improving functional mobility and community participation. Use of such an intervention may be of benefit to wheeled mobility device users with MS and has the potential to be used in a clinical setting by occupational and physical therapists. Further investigation is needed to examine the long-term impact of the intervention on concerns about falling and other MS-related symptoms. o Financial Disclosures: The authors have no conflicts of interest to disclose. Funding/Support: This study was funded by the National Multiple Sclerosis Society Pilot Project (grant PP2185). NARCOMS is supported in part by the Consortium of Multiple Sclerosis Centers (CMSC) and the Foundation of the CMSC. Prior Presentation: Aspects of this study have been presented in abstract form at the 33rd International Seating Symposium; March 2-4, 2017; Nashville, TN. References 1. Cameron MH, Poel AJ, Haselkorn JK, Linke A, Bourdette D. Falls requiring medical attention among veterans with multiple sclerosis: a cohort study. J Rehabil Res Dev. 2011;48: Finlayson ML, Peterson EW. Falls, aging, and disability. Phys Med Rehabil Clin N Am. 2010;21: Matsuda PN, Shumway-Cook A, Ciol MA, Bombardier CH, Kartin DA. Understanding falls in multiple sclerosis: association of mobility status, concerns about falling, and accumulated impairments. Phys Ther. 2012;92: Peterson EW, Cho CC, Finlayson ML. Fear of falling and associated activity curtailment among middle aged and older adults with multiple sclerosis. Mult Scler. 2007;13: Sosnoff JJ, Finlayson M, McAuley E, Morrison S, Motl RW. Homebased exercise program and fall-risk reduction in older adults with multiple sclerosis: phase 1 randomized controlled trial. Clin Rehabil. 2014;28: Cattaneo D, Jonsdottir J, Zocchi M, Regola A. Effects of balance exercises on people with multiple sclerosis: a pilot study. Clin Rehabil. 2007;21: Einarsson U, Gottberg K, Fredrikson S, Bergendal G, von Koch L, Holmqvist LW. Multiple sclerosis in Stockholm County: a pilot study exploring the feasibility of assessment of impairment, disability and handicap by home visits. Clin Rehabil. 2003;17: Coote S, Hogan N, Franklin S. Falls in people with multiple sclerosis who use a walking aid: prevalence, factors, and effect of strength and balance interventions. Arch Phys Med Rehabil. 2013;94: Rice LA, Ousley C, Sosnoff JJ. A systematic review of risk factors associated with accidental falls, outcome measures and interventions to manage fall risk in non-ambulatory adults. Disabil Rehabil. 2015;37: Learmonth YC, Motl RW, Sandroff BM, Pula JH, Cadavid D. Validation of patient determined disease steps (PDDS) scale scores in persons with multiple sclerosis. BMC Neurol. 2013;13: Thabane L, Ma J, Chu R, et al. A tutorial on pilot studies: the what, why and how. BMC Med Res Methodol. 2010;10: Al-Faisal W, Beattie L, Fu H, et al. WHO Global Report on Falls Prevention in Older Age. Geneva, Switzerland: World Health Organization; Boswell-Ruys CL, Harvey LA, Delbaere K, Lord SR. A Falls Concern Scale for people with spinal cord injury (SCI-FCS). Spinal Cord. 2010;48: Tsai CY, Rice LA, Hoelmer C, Boninger ML, Koontz AM. Basic psychometric properties of the transfer assessment instrument (version 3.0). Arch Phys Med Rehabil. 2013;94: McClure LA, Boninger ML, Ozawa H, Koontz A. Reliability and validity analysis of the transfer assessment instrument. Arch Phys Med Rehabil. 2011;92: Shin S, Sosnoff JJ. Spinal cord injury and time to instability in seated posture. Arch Phys Med Rehabil. 2013;94: Slobounov S, Cao C, Jaiswal N, Newell KM. Neural basis of postural instability identified by VTC and EEG. Exp Brain Res. 2009;199: Cattaneo D, Ferrarin M, Jonsdottir J, Montesano A, Bove M. The virtual time to contact in the evaluation of balance disorders and prediction of falls in people with multiple sclerosis. Disabil Rehabil. 2012;34: Chen WY, Jang Y, Wang JD, et al. Wheelchair-related accidents: relationship with wheelchair-using behavior in active community wheelchair users. Arch Phys Med Rehabil. 2011;92: Gagnon D, Koontz A, Mulroy S, et al. Biomechanics of sitting pivot transfers among individuals with spinal cord injury: a review of the current knowledge. Top Spinal Cord Inj Rehabil. 2009;15: Kisner C, Colby L. Therapeutic Exercise: Foundations and Techniques. 4th ed. Philadelphia, PA: FA Davis; Lakens D. Calculating and reporting effect sizes to facilitate cumulative science: a practical primer for t-tests and ANOVAs. Front Psychol. 2013;4: Gorman SL, Radtka S, Melnick ME, Abrams GM, Byl NN. Development and validation of the Function In Sitting Test in adults with acute stroke. J Neurol Phys Ther. 2010;34: Sung JH, Ousley C, Shen S, Issacs Z, Sosnoff J, Rice LA. Reliability and validity of the function in sitting test in non-ambulatory individuals with multiple sclerosis. Int J Rehabil Res. 2016;39: Rice LA, Smith I, Kelleher AR, Greenwald K, Hoelmer C, Boninger ML. Impact of the clinical practice guideline for preservation of upper limb function on transfer skills of persons with acute spinal cord injury. Arch Phys Med Rehabil. 2013;94: Sosnoff JJ, Moon Y, Wajda DA, et al. Fall risk and incidence reduction in high risk individuals with multiple sclerosis: a pilot randomized control trial. Clin Rehabil. 2015;29: Bisson EJ, Peterson EW, Finlayson M. Delayed initial recovery and long lie after a fall among middle-aged and older people with multiple sclerosis. Arch Phys Med Rehabil. 2015;96: Fleming J, Brayne C; Cambridge City over-75s Cohort (CC75C) study collaboration. Inability to get up after falling, subsequent time on floor, and summoning help: prospective cohort study in people over 90. BMJ. 2008;337:a Dyer D, Bouman B, Davey M, Ismond KP. An intervention program to reduce falls for adult in-patients following major lower limb amputation. Healthc Q. 2008;11:
Whom to Target for Falls-Prevention Trials
 Whom to Target for Falls-Prevention Trials Recommendations from the International MS Falls Prevention Research Network Michelle Cameron, MD, PT, MCR; Susan Coote, PhD, PT; Jacob J. Sosnoff, PhD Effective
Whom to Target for Falls-Prevention Trials Recommendations from the International MS Falls Prevention Research Network Michelle Cameron, MD, PT, MCR; Susan Coote, PhD, PT; Jacob J. Sosnoff, PhD Effective
Short Term Influences of Transfer Training Among Full Time Pediatric Wheelchair Users: A Randomized Trial
 Short Term Influences of Transfer Training Among Full Time Pediatric Wheelchair Users: A Randomized Trial Laura A Rice, Jennifer Dysterheft, Ethan Sanders & Ian Rice Department of Kinesiology and Community
Short Term Influences of Transfer Training Among Full Time Pediatric Wheelchair Users: A Randomized Trial Laura A Rice, Jennifer Dysterheft, Ethan Sanders & Ian Rice Department of Kinesiology and Community
PhD Rehabilitation Science and Technology 2010 University of Pittsburgh Human Engineering Research Laboratories
 Rice vitae 1 Laura A. Rice (McClure), PhD, MPT, ATP Department of Kinesiology and Community Health University of Illinois at Urbana- Champaign 2003 Huff Hall, (M/C 586) 1206 S. Fourth St. Champaign, IL
Rice vitae 1 Laura A. Rice (McClure), PhD, MPT, ATP Department of Kinesiology and Community Health University of Illinois at Urbana- Champaign 2003 Huff Hall, (M/C 586) 1206 S. Fourth St. Champaign, IL
Cleveland Clinic Mellen Center for Multiple Sclerosis. Mellen Center Approaches: Falls and Fall Prevention in MS. Q: What is a fall?
 Mellen Center Approaches: Falls and Fall Prevention in MS Q: What is a fall? A: A fall can be defined as an unplanned change in position resulting in the individual resting on the ground or a lower level.
Mellen Center Approaches: Falls and Fall Prevention in MS Q: What is a fall? A: A fall can be defined as an unplanned change in position resulting in the individual resting on the ground or a lower level.
Multiple sclerosis (MS) impairs cognition, Community Delivery of a Comprehensive Fall-Prevention Program in People with Multiple Sclerosis
 Community Delivery of a Comprehensive Fall-Prevention Program in People with Multiple Sclerosis A Retrospective Observational Study Cinda L. Hugos, MS, PT; Debra Frankel, MS, OT; Sara A. Tompkins, PhD;
Community Delivery of a Comprehensive Fall-Prevention Program in People with Multiple Sclerosis A Retrospective Observational Study Cinda L. Hugos, MS, PT; Debra Frankel, MS, OT; Sara A. Tompkins, PhD;
DOUGLAS A. WAJDA. M.S., Mechanical Engineering 2012
 DOUGLAS A. WAJDA Department of Kinesiology University of Illinois 906 S Goodwin Ave Urbana, IL 61801 Telephone: (330) 883-7149 E-mail: wajda2@illinois.edu EDUCATION Completed Degrees: The University of
DOUGLAS A. WAJDA Department of Kinesiology University of Illinois 906 S Goodwin Ave Urbana, IL 61801 Telephone: (330) 883-7149 E-mail: wajda2@illinois.edu EDUCATION Completed Degrees: The University of
Fall Incidence as the Primary Outcome in Multiple Sclerosis Falls-Prevention Trials
 Fall Incidence as the Primary Outcome in Multiple Sclerosis Falls-Prevention Trials Recommendation from the International MS Falls Prevention Research Network Susan Coote, PhD, PT; Jacob J. Sosnoff, PhD;
Fall Incidence as the Primary Outcome in Multiple Sclerosis Falls-Prevention Trials Recommendation from the International MS Falls Prevention Research Network Susan Coote, PhD, PT; Jacob J. Sosnoff, PhD;
Overview The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and dynamic balance.
 Core Measure: Berg Balance Scale (BBS) Overview The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and dynamic balance. Number of Test Items The BBS consists of
Core Measure: Berg Balance Scale (BBS) Overview The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and dynamic balance. Number of Test Items The BBS consists of
Multiple Sclerosis and Falls An Evolving Tale
 Multiple Sclerosis and Falls An Evolving Tale Jacob J Sosnoff, 1 Robert W Motl 1 and Steven Morrison 2 1. Associate Professor, Department of Kinesiology and Community Health, College of Applied Health
Multiple Sclerosis and Falls An Evolving Tale Jacob J Sosnoff, 1 Robert W Motl 1 and Steven Morrison 2 1. Associate Professor, Department of Kinesiology and Community Health, College of Applied Health
Mellen Center Approaches Exercise in MS
 Mellen Center Approaches Exercise in MS Framework: Physical exercise is generally recommended to promote fitness and wellness in individuals with or without chronic health conditions. Implementing and
Mellen Center Approaches Exercise in MS Framework: Physical exercise is generally recommended to promote fitness and wellness in individuals with or without chronic health conditions. Implementing and
Transfer Assessment Instrument 4.0 Independent Transfers
 Transfer Assessment Instrument 4. Independent Transfers This tool is designed to objectively unassisted transfers. The tool breaks down the transfer into three components: wheelchair setup, body set up,
Transfer Assessment Instrument 4. Independent Transfers This tool is designed to objectively unassisted transfers. The tool breaks down the transfer into three components: wheelchair setup, body set up,
CORE MEASURE: CORE MEASURE: BERG BALANCE SCALE (BBS)
 OVERVIEW NUMBER OF TEST ITEMS SCORING EQUIPMENT TIME (NEW CLINICIAN) TIME (EXPERIENCED CLINICIAN) COST o The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and
OVERVIEW NUMBER OF TEST ITEMS SCORING EQUIPMENT TIME (NEW CLINICIAN) TIME (EXPERIENCED CLINICIAN) COST o The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and
CURRICULUM VITAE Brian M. Sandroff
 CURRICULUM VITAE Brian M. Sandroff Institutional Address Brian M. Sandroff, Ph.D. Assistant Professor, Department of Physical Therapy School of Health Professions The University of Alabama at Birmingham
CURRICULUM VITAE Brian M. Sandroff Institutional Address Brian M. Sandroff, Ph.D. Assistant Professor, Department of Physical Therapy School of Health Professions The University of Alabama at Birmingham
Participation as an Outcome in Multiple Sclerosis Falls-Prevention Research
 Participation as an Outcome in Multiple Sclerosis Falls-Prevention Research Consensus Recommendation from the International MS Falls Prevention Research Network Marcia Finlayson, PhD, OT Reg (Ont), OTR;
Participation as an Outcome in Multiple Sclerosis Falls-Prevention Research Consensus Recommendation from the International MS Falls Prevention Research Network Marcia Finlayson, PhD, OT Reg (Ont), OTR;
A qualitative study of a home-based DVD exercise intervention in older adults with multiple sclerosis
 A qualitative study of a home-based DVD exercise intervention in older adults with multiple sclerosis HUBBARD EA, LEARMONTH YC, KINNETT-HOPKINS DL, WOJCICKI T, ROBERTS S, FANNING J, MCAULEY E, AND MOTL
A qualitative study of a home-based DVD exercise intervention in older adults with multiple sclerosis HUBBARD EA, LEARMONTH YC, KINNETT-HOPKINS DL, WOJCICKI T, ROBERTS S, FANNING J, MCAULEY E, AND MOTL
Kathryn D. Mitchell, PT, DPT, NCS, MSCS; Han Chen, MD, MPH; Sheri P. Silfies, PT, PhD
 Test-Retest Reliability, Validity, and Minimal Detectable Change of the Balance Evaluation Systems Test to Assess Balance in Persons with Multiple Sclerosis Kathryn D. Mitchell, PT, DPT, NCS, MSCS; Han
Test-Retest Reliability, Validity, and Minimal Detectable Change of the Balance Evaluation Systems Test to Assess Balance in Persons with Multiple Sclerosis Kathryn D. Mitchell, PT, DPT, NCS, MSCS; Han
Telephone: (217) Department of Kinesiology
 Yaejin Moon ===================================================================== University of Illinois at Urbana Champaign Telephone: (217) 898-5026 Department of Kinesiology E-mail: ymoon9@illinois.edu
Yaejin Moon ===================================================================== University of Illinois at Urbana Champaign Telephone: (217) 898-5026 Department of Kinesiology E-mail: ymoon9@illinois.edu
Static posturography across the EDSS scale in people with multiple sclerosis: a cross sectional study
 Kalron et al. BMC Neurology (2016) 16:70 DOI 10.1186/s12883-016-0603-6 RESEARCH ARTICLE Open Access Static posturography across the EDSS scale in people with multiple sclerosis: a cross sectional study
Kalron et al. BMC Neurology (2016) 16:70 DOI 10.1186/s12883-016-0603-6 RESEARCH ARTICLE Open Access Static posturography across the EDSS scale in people with multiple sclerosis: a cross sectional study
Balance and mobility impairments, leg weakness,
 Frequency of and Factors Associated with a Proxy for Critical Falls Among People Aging with Multiple Sclerosis An Exploratory Study Etienne J. Bisson, PhD; Elizabeth W. Peterson, PhD; Marcia Finlayson,
Frequency of and Factors Associated with a Proxy for Critical Falls Among People Aging with Multiple Sclerosis An Exploratory Study Etienne J. Bisson, PhD; Elizabeth W. Peterson, PhD; Marcia Finlayson,
Lara A. Pilutti, Ph.D.
 Institutional Address: Department of Kinesiology and Community Health University of Illinois at Urbana-Champaign 906 S Goodwin Ave, Room 213, Urbana, IL, 61801 Tel: 217-333-6126 email: lpilutti@illinois.edu
Institutional Address: Department of Kinesiology and Community Health University of Illinois at Urbana-Champaign 906 S Goodwin Ave, Room 213, Urbana, IL, 61801 Tel: 217-333-6126 email: lpilutti@illinois.edu
Functional Ability Screening Tools for the Clinic
 Functional Ability Screening Tools for the Clinic Shelley Hockensmith,, P.T., NCS Objectives Review screening tools for physical or functional ability including Five Times Sit to Stand, Walking Speed,
Functional Ability Screening Tools for the Clinic Shelley Hockensmith,, P.T., NCS Objectives Review screening tools for physical or functional ability including Five Times Sit to Stand, Walking Speed,
Quality of life defined
 Psychometric Properties of Quality of Life and Health Related Quality of Life Assessments in People with Multiple Sclerosis Learmonth, Y. C., Hubbard, E. A., McAuley, E. Motl, R. W. Department of Kinesiology
Psychometric Properties of Quality of Life and Health Related Quality of Life Assessments in People with Multiple Sclerosis Learmonth, Y. C., Hubbard, E. A., McAuley, E. Motl, R. W. Department of Kinesiology
The study of physical activity behavior and its
 Most Common Types of Physical Activity Self-Selected by People with Multiple Sclerosis Madeline Weikert, BS; Deirdre Dlugonski, BS; Swathi Balantrapu, BS; Robert W. Motl, PhD The promotion of physical
Most Common Types of Physical Activity Self-Selected by People with Multiple Sclerosis Madeline Weikert, BS; Deirdre Dlugonski, BS; Swathi Balantrapu, BS; Robert W. Motl, PhD The promotion of physical
Improving Balance and Mobility in People with Multiple Sclerosis
 University of Massachusetts Medical School escholarship@umms UMass Center for Clinical and Translational Science Research Retreat 2014 UMass Center for Clinical and Translational Science Research Retreat
University of Massachusetts Medical School escholarship@umms UMass Center for Clinical and Translational Science Research Retreat 2014 UMass Center for Clinical and Translational Science Research Retreat
Exercise, Physical Therapy and Fall Prevention
 Exercise, Physical Therapy and Fall Prevention University of Davis Medical Center Rosy Chow Neuro Clinical Specialist Physical Therapist Outline of Talk Role of Physical Therapy in care of people with
Exercise, Physical Therapy and Fall Prevention University of Davis Medical Center Rosy Chow Neuro Clinical Specialist Physical Therapist Outline of Talk Role of Physical Therapy in care of people with
Wheelchair/Scooter/Stroller Seating Assessment Form (CCP/Home Health Services) ( pages)
 Wheelchair/Scooter/Stroller Seating Assessment Form (CCP/Home Health Services) ( pages) Instructions A current wheelchair/scooter/stroller seating assessment conducted by a physician or a physical or occupational
Wheelchair/Scooter/Stroller Seating Assessment Form (CCP/Home Health Services) ( pages) Instructions A current wheelchair/scooter/stroller seating assessment conducted by a physician or a physical or occupational
Benefits and Safety of Exercise
 Capitalising on the Interaction Between Patients and Healthcare Providers; A Qualitative Study to Explore the Exercise Promotion of MS Patients Learmonth, Y. C. 1, Adamson, B.C. 1, Balto, J.M. 1, Chiu,
Capitalising on the Interaction Between Patients and Healthcare Providers; A Qualitative Study to Explore the Exercise Promotion of MS Patients Learmonth, Y. C. 1, Adamson, B.C. 1, Balto, J.M. 1, Chiu,
Equipment Stopwatch A clear pathway of at least 10 m (32.8 ft) in length in a designated area over solid flooring 2,3.
 Core Measure: 10 Meter Walk Test (10mWT) Overview The 10mWT is used to assess walking speed in meters/second (m/s) over a short distance. Number of Test Items 1 item Scoring The total time taken to ambulate
Core Measure: 10 Meter Walk Test (10mWT) Overview The 10mWT is used to assess walking speed in meters/second (m/s) over a short distance. Number of Test Items 1 item Scoring The total time taken to ambulate
Please demonstrate each task and/or give instructions as written. When scoring, please record the lowest response category that applies for each item.
 Berg Balance Test Name Date Location Rater GENERAL INSTRUCTIONS Please demonstrate each task and/or give instructions as written. When scoring, please record the lowest response category that applies for
Berg Balance Test Name Date Location Rater GENERAL INSTRUCTIONS Please demonstrate each task and/or give instructions as written. When scoring, please record the lowest response category that applies for
Berg Balance Scale. CVA, Parkinson Disease, Pediatrics
 CVA, Parkinson Disease, Pediatrics CVA Highly recommended for inpatient and outpatient rehabilitation Recommended for acute care Parkinson s Disease Recommended for H and Y stages 2 and 3 G code-changing
CVA, Parkinson Disease, Pediatrics CVA Highly recommended for inpatient and outpatient rehabilitation Recommended for acute care Parkinson s Disease Recommended for H and Y stages 2 and 3 G code-changing
Falls and Multiple Sclerosis (MS)
 6/9/14 Balance Based Torso Weighting Results in Fall Reduction during Sensory Organization Test for People with Multiple Sclerosis Kristin Horn BS, Cynthia Gibson Horn PT, Diane D Allen PhD, PT, Gail L
6/9/14 Balance Based Torso Weighting Results in Fall Reduction during Sensory Organization Test for People with Multiple Sclerosis Kristin Horn BS, Cynthia Gibson Horn PT, Diane D Allen PhD, PT, Gail L
FES Standing: The Effect of Arm Support on Stability and Fatigue During Sit-to-Stand Manoeuvres in SCI Individuals
 FES Standing: The Effect of Arm Support on Stability and Fatigue During Sit-to-Stand Manoeuvres in SCI Individuals Musfirah Abd Aziz and Nur Azah Hamzaid Abstract Functional Electrical Stimulation (FES)
FES Standing: The Effect of Arm Support on Stability and Fatigue During Sit-to-Stand Manoeuvres in SCI Individuals Musfirah Abd Aziz and Nur Azah Hamzaid Abstract Functional Electrical Stimulation (FES)
Functional Activity and Mobility
 Functional Activity and Mobility Documentation for Hospitalized Adult The Johns Hopkins University and The Johns Hopkins Health System Corporation Goals for Documentation of Activity and Mobility To develop
Functional Activity and Mobility Documentation for Hospitalized Adult The Johns Hopkins University and The Johns Hopkins Health System Corporation Goals for Documentation of Activity and Mobility To develop
Occupational Therapy: INTERVENTION AND INDEPENDENCE
 Occupational Therapy: INTERVENTION AND INDEPENDENCE What is Occupational Therapy? A therapy to help people find ways to do things that matter to them Dressing, bathing, toileting Housekeeping Leisure Community
Occupational Therapy: INTERVENTION AND INDEPENDENCE What is Occupational Therapy? A therapy to help people find ways to do things that matter to them Dressing, bathing, toileting Housekeeping Leisure Community
C-MILL PRE-TRAINING MATERIAL
 4 C-MILL PRE-TRAINING MATERIAL 1 Background information The ability to adjust gait to the requirements of the environment is related to fall risk. Someone must be able to avoid a doorstep, puddle of water
4 C-MILL PRE-TRAINING MATERIAL 1 Background information The ability to adjust gait to the requirements of the environment is related to fall risk. Someone must be able to avoid a doorstep, puddle of water
Physical and Occupational Therapy after Spine Surgery. Preparation for your surgery
 Physical and Occupational Therapy after Spine Surgery Preparation for your surgery Agenda Pre-Operative Exercises What to Expect Post-Operative Plan Spinal Precautions Post-Discharge Plan S A I N T LU
Physical and Occupational Therapy after Spine Surgery Preparation for your surgery Agenda Pre-Operative Exercises What to Expect Post-Operative Plan Spinal Precautions Post-Discharge Plan S A I N T LU
Mobile, Virtual Enhancements for Rehabilitation (MOVER)
 Charles River Analytics Quarterly Progress Report No. R1219812 Reporting Period: Jun 1, 2014 Aug 28, 2015 Government Contract No. N00014-13-C-0359 Total Award Value: $767,388 Charles River Analytics Contract
Charles River Analytics Quarterly Progress Report No. R1219812 Reporting Period: Jun 1, 2014 Aug 28, 2015 Government Contract No. N00014-13-C-0359 Total Award Value: $767,388 Charles River Analytics Contract
7 Element Order. elsewhere classified, Spinal stenosis, lumbar region, without neurogenic claudication. Physician signature:
 7 Element Order Medicare national and local policy specify that following completion of the face-to-face examination, the physician or treating practitioner must complete a written order containing seven
7 Element Order Medicare national and local policy specify that following completion of the face-to-face examination, the physician or treating practitioner must complete a written order containing seven
Incorporating Balance, Resistance, and Aerobic Training into Therapy Sessions with a Patient who has MS: A Case Report
 Doctor of Physical Therapy Program Case Reports 2017 Incorporating Balance, Resistance, and Aerobic Training into Therapy Sessions with a Patient who has MS: A Case Report Eric Callahan University of Iowa
Doctor of Physical Therapy Program Case Reports 2017 Incorporating Balance, Resistance, and Aerobic Training into Therapy Sessions with a Patient who has MS: A Case Report Eric Callahan University of Iowa
CSHCN Services Program Benefits Have Changed for Some Durable Medical Equipment (DME) CSHCN Services Program Documentation of Receipt
 CSHCN Services Program Benefits Have Changed for Some Durable Medical Equipment (DME) Information posted February 6, 2009 Effective for dates of service on or after April 1, 2009, benefit criteria for
CSHCN Services Program Benefits Have Changed for Some Durable Medical Equipment (DME) Information posted February 6, 2009 Effective for dates of service on or after April 1, 2009, benefit criteria for
Intelligent Sensor Systems for Healthcare: A Case Study of Pressure Ulcer TITOLO. Prevention and Treatment TESI. Rui (April) Dai
 Intelligent Sensor Systems for Healthcare: A Case Study of Pressure Ulcer TITOLO Prevention and Treatment TESI Rui (April) Dai Assistant Professor Department of Computer Science North Dakota State University
Intelligent Sensor Systems for Healthcare: A Case Study of Pressure Ulcer TITOLO Prevention and Treatment TESI Rui (April) Dai Assistant Professor Department of Computer Science North Dakota State University
Mary Fitzpatrick, ANP, MSCN Michelle Cameron, MD, PT
 Mary Fitzpatrick, ANP, MSCN Michelle Cameron, MD, PT This continuing education activity is managed and accredited by Professional Education Service Group. The material presented in this activity represents
Mary Fitzpatrick, ANP, MSCN Michelle Cameron, MD, PT This continuing education activity is managed and accredited by Professional Education Service Group. The material presented in this activity represents
JEFFERSON COLLEGE COURSE SYLLABUS. PTA 120 PTA Principles and Procedures I. 3 Credit Hours
 JEFFERSON COLLEGE COURSE SYLLABUS PTA 120 PTA Principles and Procedures I 3 Credit Hours Prepared by: Bridget B. Webb, PT, MPT, CEEAA Physical Therapist Assistant Program Director October 12, 2011 Elizabeth
JEFFERSON COLLEGE COURSE SYLLABUS PTA 120 PTA Principles and Procedures I 3 Credit Hours Prepared by: Bridget B. Webb, PT, MPT, CEEAA Physical Therapist Assistant Program Director October 12, 2011 Elizabeth
Slide 1. Slide 2 Disclosure. Slide 3 Objectives. Functional Mobility and Activities of Daily Living: Assessing and Treating Patients in Rehabilitation
 Slide 1 Functional Mobility and Activities of Daily Living: Assessing and Treating Patients in Rehabilitation Terry Carolan, MSPT, NCS Slide 2 Disclosure Terry Carolan has no industry disclosures to make
Slide 1 Functional Mobility and Activities of Daily Living: Assessing and Treating Patients in Rehabilitation Terry Carolan, MSPT, NCS Slide 2 Disclosure Terry Carolan has no industry disclosures to make
Chapter 1. Overview. General Description. Test Developers. Purpose and Use. Qualifications of Users. Limitations. Communication. General Description
 Chapter 1: Overview Chapter 1 Overview General Description Test Developers Purpose and Use Qualifications of Users Limitations Communication General Description The research version of the Seated Postural
Chapter 1: Overview Chapter 1 Overview General Description Test Developers Purpose and Use Qualifications of Users Limitations Communication General Description The research version of the Seated Postural
William C Miller, PhD, FCAOT Professor Occupational Science & Occupational Therapy University of British Columbia Vancouver, BC, Canada
 William C Miller, PhD, FCAOT Professor Occupational Science & Occupational Therapy University of British Columbia Vancouver, BC, Canada THE L TEST MANUAL Version: November 2014 Table of Contents Introduction...
William C Miller, PhD, FCAOT Professor Occupational Science & Occupational Therapy University of British Columbia Vancouver, BC, Canada THE L TEST MANUAL Version: November 2014 Table of Contents Introduction...
An Intervention Program to Reduce Falls for Adult In-Patients Following Major Lower Limb Amputation
 Improving Care at the Front Lines An Intervention Program to Reduce Falls for Adult In-Patients Following Major Lower Limb Amputation David Dyer, Bonnie Bouman, Monique Davey and Kathleen P. Ismond Abstract
Improving Care at the Front Lines An Intervention Program to Reduce Falls for Adult In-Patients Following Major Lower Limb Amputation David Dyer, Bonnie Bouman, Monique Davey and Kathleen P. Ismond Abstract
Reducing Computer Workstation Hazards Through Proper Set-up and Design
 PPT Presentation page 1 Reducing Computer Workstation Hazards Through Proper Set-up and Design Presented by the NYS Public Employees Federation Paige Engelhardt PEF Health & Safety Trainer www.pef.org
PPT Presentation page 1 Reducing Computer Workstation Hazards Through Proper Set-up and Design Presented by the NYS Public Employees Federation Paige Engelhardt PEF Health & Safety Trainer www.pef.org
What is Occupational Therapy?
 Introduction to Occupational Therapy Services What is Occupational Therapy? Alice Chan, OTI Tai Po Hospital a health profession that focuses on promoting health and well being through engagement in meaningful
Introduction to Occupational Therapy Services What is Occupational Therapy? Alice Chan, OTI Tai Po Hospital a health profession that focuses on promoting health and well being through engagement in meaningful
Mobile, Virtual Enhancements for Rehabilitation (MOVER)
 Charles River Analytics Quarterly Progress Report No. R1219809 Reporting Period: Dec 1, 2014 Feb 28, 2015 Government Contract No. N00014-13-C-0359 Total Award Value: $767,388 Charles River Analytics Contract
Charles River Analytics Quarterly Progress Report No. R1219809 Reporting Period: Dec 1, 2014 Feb 28, 2015 Government Contract No. N00014-13-C-0359 Total Award Value: $767,388 Charles River Analytics Contract
GENERAL EXERCISES YOGA BMW MANUFACTURING CO. PZ-AM-G-US I July 2017
 GENERAL EXERCISES YOGA BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to be
GENERAL EXERCISES YOGA BMW MANUFACTURING CO. PZ-AM-G-US I July 2017 Disclosure: The exercises, stretches, and mobilizations provided in this presentation are for educational purposes only are not to be
Heidi Sanders, OTR/L. Amy Shuckra, MPT
 Adaptive Equipment Heidi Sanders, OTR/L University of New Mexico Health Sciences Center, Los Pasos Program Amy Shuckra, MPT Shriners Hospitals for Children Salt Lake City, Utah What is Adaptive Equipment?
Adaptive Equipment Heidi Sanders, OTR/L University of New Mexico Health Sciences Center, Los Pasos Program Amy Shuckra, MPT Shriners Hospitals for Children Salt Lake City, Utah What is Adaptive Equipment?
Sensitivity and Specificity of the Minimal Chair Height Standing Ability Test: A Simple and Affordable Fall-Risk Screening Instrument
 Sensitivity and Specificity of the Minimal Chair Height Standing Ability Test: A Simple and Affordable Fall-Risk Screening Instrument By: Nadia C. Reider, MSc ; Patti-Jean Naylor, PhD ; Catherine Gaul,
Sensitivity and Specificity of the Minimal Chair Height Standing Ability Test: A Simple and Affordable Fall-Risk Screening Instrument By: Nadia C. Reider, MSc ; Patti-Jean Naylor, PhD ; Catherine Gaul,
Changes in Functional Mobility Outcomes of Individuals Receiving a New Seating/Mobility Device
 Changes in Functional Mobility Outcomes of Individuals Receiving a New Seating/Mobility Device Virginia Fly Miranda Law Stacey Lindsley Lacey Little Spence Tomlinson Penny Powers, PT, ATP Renee Brown,
Changes in Functional Mobility Outcomes of Individuals Receiving a New Seating/Mobility Device Virginia Fly Miranda Law Stacey Lindsley Lacey Little Spence Tomlinson Penny Powers, PT, ATP Renee Brown,
Interventions, Effects, and Outcomes in Occupational Therapy
 Interventions, Effects, and Outcomes in Occupational Therapy ADULTS AND OLDER ADULTS Instructor s Manual Learning Activities Mary Law, PhD, FCAOT Professor and Associate Dean Rehabilitation Science McMaster
Interventions, Effects, and Outcomes in Occupational Therapy ADULTS AND OLDER ADULTS Instructor s Manual Learning Activities Mary Law, PhD, FCAOT Professor and Associate Dean Rehabilitation Science McMaster
Tuesday, May 1, Elizabeth W. Peterson, PhD OTR/L FAOTA THIS WEBINAR IS BEING RECORDED. THE SLIDE DECK AND RECORDING WILL BE
 Interdisciplinary and Evidence-based Approaches to Supporting Management of Diverse Fall Risk Factors among Community-dwelling People with Multiple Sclerosis Tuesday, May 1, 2018 Elizabeth W. Peterson,
Interdisciplinary and Evidence-based Approaches to Supporting Management of Diverse Fall Risk Factors among Community-dwelling People with Multiple Sclerosis Tuesday, May 1, 2018 Elizabeth W. Peterson,
Education B.P.H.E., Physical and Health Education, Queen s University, Kingston, ON. Academic Positions
 LARA A. PILUTTI, Ph.D. University of Illinois at Urbana-Champaign 906 S Goodwin Ave, Room 213, Urbana, IL, 61801 Tel: 217-333-6126 email: lpilutti@illinois.edu Education 2006-2012 Ph.D., Kinesiology, McMaster
LARA A. PILUTTI, Ph.D. University of Illinois at Urbana-Champaign 906 S Goodwin Ave, Room 213, Urbana, IL, 61801 Tel: 217-333-6126 email: lpilutti@illinois.edu Education 2006-2012 Ph.D., Kinesiology, McMaster
A Study of the Effects of a Video-Observed Home Exercise Program on Improving the Motor Skills of Chronic Stroke Patients
 NEUROTHERAPY 2 0 1 6 Ho-Jin Lee, Woo-Nam 대한신경치료학회지 Jang, Eun-Ja 제20권제Kim 1호 A Study of the Effects of a Video-Observed Home Exercise Program on Improving the Motor Skills of Chronic Stroke Patients Ho-Jin
NEUROTHERAPY 2 0 1 6 Ho-Jin Lee, Woo-Nam 대한신경치료학회지 Jang, Eun-Ja 제20권제Kim 1호 A Study of the Effects of a Video-Observed Home Exercise Program on Improving the Motor Skills of Chronic Stroke Patients Ho-Jin
VISTA400 REMOVABLE FOOT PLATE. Instructions For Use. Step on yellow pedals to close and open legs to go around chairs & ambulate.
 VISTA400 Instructions For Use Squeeze the yellow bar & push down/pull up to activate pneumatic stand assist. Step on yellow pedals to close and open legs to go around chairs & ambulate. Pull yellow levers
VISTA400 Instructions For Use Squeeze the yellow bar & push down/pull up to activate pneumatic stand assist. Step on yellow pedals to close and open legs to go around chairs & ambulate. Pull yellow levers
Course Descriptions for Courses in the Entry-Level Doctorate in Occupational Therapy Curriculum
 Course Descriptions for Courses in the Entry-Level Doctorate in Occupational Therapy Curriculum Course Name Therapeutic Interaction Skills Therapeutic Interaction Skills Lab Anatomy Surface Anatomy Introduction
Course Descriptions for Courses in the Entry-Level Doctorate in Occupational Therapy Curriculum Course Name Therapeutic Interaction Skills Therapeutic Interaction Skills Lab Anatomy Surface Anatomy Introduction
Co-morbidities and Exercise with Parkinson s Disease (COPE) Exercise Manual
 Name: Date: Co-morbidities and Exercise with Parkinson s Disease (COPE) Exercise Manual This program is organized into 6 themed stations done like a circuit to address the specific difficulties that a
Name: Date: Co-morbidities and Exercise with Parkinson s Disease (COPE) Exercise Manual This program is organized into 6 themed stations done like a circuit to address the specific difficulties that a
JEFFERSON COLLEGE COURSE SYLLABUS. PTA 120 PTA Principles and Procedures I. 3 Credit Hours
 JEFFERSON COLLEGE COURSE SYLLABUS PTA 120 PTA Principles and Procedures I 3 Credit Hours Prepared by: Bridget B. Webb, PT, MPT, CEEAA Physical Therapist Assistant Program Director October 12, 2011 Elizabeth
JEFFERSON COLLEGE COURSE SYLLABUS PTA 120 PTA Principles and Procedures I 3 Credit Hours Prepared by: Bridget B. Webb, PT, MPT, CEEAA Physical Therapist Assistant Program Director October 12, 2011 Elizabeth
The influence of Belt Use on Reach and Push Function in Active Wheelchair Users
 2/24/13 The influence of Belt Use on Reach and Push Function in Active Wheelchair Users 29th International Seating Symposium 8 March 2013 Study Question Why Do Active Wheelchair Riders Use Belts In Wheelchair
2/24/13 The influence of Belt Use on Reach and Push Function in Active Wheelchair Users 29th International Seating Symposium 8 March 2013 Study Question Why Do Active Wheelchair Riders Use Belts In Wheelchair
Home Office Solutions By: Laura Cervantes QAS 515 3/26/03
 Home Office Solutions By: Laura Cervantes QAS 515 3/26/03 Working from home is becoming more of an option for employees today. The type of work usually entails working from the home computer work station.
Home Office Solutions By: Laura Cervantes QAS 515 3/26/03 Working from home is becoming more of an option for employees today. The type of work usually entails working from the home computer work station.
Electrical stimulation to reduce the overload in upper limbs on SPT
 Electrical stimulation to reduce the overload in upper limbs during sitting pivot transfer in paraplegic: a preliminary study Ana Claudia G. Lopes (1,2), Claudia Ochoa-Diaz (3), Roberto S. Baptista (3),
Electrical stimulation to reduce the overload in upper limbs during sitting pivot transfer in paraplegic: a preliminary study Ana Claudia G. Lopes (1,2), Claudia Ochoa-Diaz (3), Roberto S. Baptista (3),
Reliability of time to stabilization in single leg standing
 Northern Michigan University The Commons Conference Papers in Published Proceedings 2009 Reliability of time to stabilization in single leg standing Randall L. Jensen Northern Michigan University Follow
Northern Michigan University The Commons Conference Papers in Published Proceedings 2009 Reliability of time to stabilization in single leg standing Randall L. Jensen Northern Michigan University Follow
Physical exercise in MS / Tallinn Anders Romberg, PhD, Physical Therapist Neuro Society / Masku Neurological Rehabilitation Centre
 Physical exercise in MS 20.3.2015 / Tallinn Anders Romberg, PhD, Physical Therapist Neuro Society / Masku Neurological Rehabilitation Centre 2 Finnish Neuro Society Content; 5 perspectives 1) Historical
Physical exercise in MS 20.3.2015 / Tallinn Anders Romberg, PhD, Physical Therapist Neuro Society / Masku Neurological Rehabilitation Centre 2 Finnish Neuro Society Content; 5 perspectives 1) Historical
Program Evaluation Results of a Structured Group Exercise Program in Individuals with Multiple Sclerosis
 Program Evaluation Results of a Structured Group Exercise Program in Individuals with Multiple Sclerosis Mary E. Charlton, PhD; Kelley Pettee Gabriel, PhD; Terry Munsinger, RN, BSN; Lorene Schmaderer,
Program Evaluation Results of a Structured Group Exercise Program in Individuals with Multiple Sclerosis Mary E. Charlton, PhD; Kelley Pettee Gabriel, PhD; Terry Munsinger, RN, BSN; Lorene Schmaderer,
products, education, and rehabilitation solutions FREEDOM FOR THERAPISTS INDEPENDENCE FOR PATIENTS
 products, education, and rehabilitation solutions FREEDOM FOR THERAPISTS INDEPENDENCE FOR PATIENTS The Original Partial-Weight-Bearing Gait Therapy Device LiteGait is a gait training device that simultaneously
products, education, and rehabilitation solutions FREEDOM FOR THERAPISTS INDEPENDENCE FOR PATIENTS The Original Partial-Weight-Bearing Gait Therapy Device LiteGait is a gait training device that simultaneously
Modified Parkinson Activity Scale
 Modified Parkinson Activity Scale Chair transfers Analyses: Instruction: Chair with 40 cm seat height, or, when at the patient's home, the chair that causes the greatest problems to the patient and is
Modified Parkinson Activity Scale Chair transfers Analyses: Instruction: Chair with 40 cm seat height, or, when at the patient's home, the chair that causes the greatest problems to the patient and is
Singapore s Telerehabilitation Experience: Its Basis and How It Works
 Singapore s Telerehabilitation Experience: Its Basis and How It Works Clinical Care Education Research What is Telemedicine? Telemedicine is the use of medical information exchanged from one site to another
Singapore s Telerehabilitation Experience: Its Basis and How It Works Clinical Care Education Research What is Telemedicine? Telemedicine is the use of medical information exchanged from one site to another
Most Dangerous Man! FACTS ON STREGNTH. Session #627 Functionally Fit Seniors
 FACTS ON STREGNTH We lose strength as we age. Over a 5 year study, Men experienced a 16.1% loss of muscle torque (isometric strength) and women saw a 13.4% loss. (1) Session #627 Functionally Fit Seniors
FACTS ON STREGNTH We lose strength as we age. Over a 5 year study, Men experienced a 16.1% loss of muscle torque (isometric strength) and women saw a 13.4% loss. (1) Session #627 Functionally Fit Seniors
Goal Attainment Scaling Clinical Utility and Training Methods
 Goal Attainment Scaling Clinical Utility and Training Methods Jen Angeli, Karen Harpster, Amber Sheehan FINANCIAL DISCLOSURE AACPDM 72 nd Annual Meeting October 9-13, 2018 Speaker Names: Amber Sheehan,
Goal Attainment Scaling Clinical Utility and Training Methods Jen Angeli, Karen Harpster, Amber Sheehan FINANCIAL DISCLOSURE AACPDM 72 nd Annual Meeting October 9-13, 2018 Speaker Names: Amber Sheehan,
lntertester and lntratester Reliability of a Dynamic Balance Protocol Using the Biodex Stability System
 Journal of Sport Rehabilitation, 1998, 7, 95-101 0 1998 Human Kinetics Publishers, Inc. lntertester and lntratester Reliability of a Dynamic Balance Protocol Using the Biodex Stability System Randy Schmitz
Journal of Sport Rehabilitation, 1998, 7, 95-101 0 1998 Human Kinetics Publishers, Inc. lntertester and lntratester Reliability of a Dynamic Balance Protocol Using the Biodex Stability System Randy Schmitz
Created in January 2005 Duration: approx. 20 minutes
 1 1 The Timed Up and Go Test Created in January 2005 Duration: approx. 20 minutes 2 Credits 2005 Stein Gerontological Institute. All rights reserved. Principal medical contributors: Alan Katz, MD Francois
1 1 The Timed Up and Go Test Created in January 2005 Duration: approx. 20 minutes 2 Credits 2005 Stein Gerontological Institute. All rights reserved. Principal medical contributors: Alan Katz, MD Francois
ATTENTION TRAINING EXERCISES USING BRAINWAVE-R
 ATTENTION TRAINING EXERCISES USING BRAINWAVE-R Aim To understand why attention training is needed by some service users. To be able to safely and effectively carry out prescribed attention training exercises
ATTENTION TRAINING EXERCISES USING BRAINWAVE-R Aim To understand why attention training is needed by some service users. To be able to safely and effectively carry out prescribed attention training exercises
07/13/2017. Introduction. What Does Bariatric Mean? Learning Objectives. Bariatric vs Heavy Duty
 Introduction Bariatric Manual Wheelchairs Cindy Duff PT, ATP/SMS July 18, 2017 Cindy Duff, PT, ATP/SMS cynthia.duff@dhha.org 29 years as a physical therapist; at Denver Health, a level one trauma, safety
Introduction Bariatric Manual Wheelchairs Cindy Duff PT, ATP/SMS July 18, 2017 Cindy Duff, PT, ATP/SMS cynthia.duff@dhha.org 29 years as a physical therapist; at Denver Health, a level one trauma, safety
Treating MS is Not Easy!
 Utilizing Technology to Improve Patient Adherence and Professional Patient Monitoring for At-home Exercise Programs in Patients with Multiple Sclerosis: HUNTER VINCENT TOURO COLLEGE OF OSTEOPATHIC MEDICINE,
Utilizing Technology to Improve Patient Adherence and Professional Patient Monitoring for At-home Exercise Programs in Patients with Multiple Sclerosis: HUNTER VINCENT TOURO COLLEGE OF OSTEOPATHIC MEDICINE,
Title: The effects of videogames therapy on balance and attention in chronic ambulatory traumatic brain injury: an exploratory study.
 Author s response to reviews Title: The effects of videogames therapy on balance and attention in chronic ambulatory traumatic brain injury: an exploratory study. Authors: sofia straudi (s.straudi@ospfe.it)
Author s response to reviews Title: The effects of videogames therapy on balance and attention in chronic ambulatory traumatic brain injury: an exploratory study. Authors: sofia straudi (s.straudi@ospfe.it)
Clinical Problem Solving 1: Using the Short Form Berg Balance Scale to Detect Change in Post Acute Stroke Patients
 Clinical Problem Solving 1: Using the Short Form Berg Balance Scale to Detect Change in Post Acute Stroke Patients By Caroline Owen November 12, 2015 Purpose 1. To present the physical therapy evaluation
Clinical Problem Solving 1: Using the Short Form Berg Balance Scale to Detect Change in Post Acute Stroke Patients By Caroline Owen November 12, 2015 Purpose 1. To present the physical therapy evaluation
Evaluate the Effectiveness of a Home Safety Screening Tool to Assess Fall Risk at Home for Elderly with Fragility Fracture
 Evaluate the Effectiveness of a Home Safety Screening Tool to Assess Fall Risk at Home for Elderly with Fragility Fracture Validation and Application of the Chinese HOME Falls and Accidents Screening Tool
Evaluate the Effectiveness of a Home Safety Screening Tool to Assess Fall Risk at Home for Elderly with Fragility Fracture Validation and Application of the Chinese HOME Falls and Accidents Screening Tool
LINKING EVIDENCE AND PRACTICE. Exercise for Managing the Symptoms of Multiple Sclerosis Parminder K. Padgett, Susan L. Kasser
 Exercise for Managing the Symptoms of Multiple Sclerosis Parminder K. Padgett, Susan L. Kasser LEAP LINKING EVIDENCE AND PRACTICE highlights the findings and application of Cochrane reviews and
Exercise for Managing the Symptoms of Multiple Sclerosis Parminder K. Padgett, Susan L. Kasser LEAP LINKING EVIDENCE AND PRACTICE highlights the findings and application of Cochrane reviews and
Healthcare Technology Letters
 Page 1 of 6 The effect of technique and transfer board use on the performance of wheelchair transfers Giulia Barbareschi 1, Tsu-Jui Cheng 2 and Catherine Holloway 1 1 University College London Interaction
Page 1 of 6 The effect of technique and transfer board use on the performance of wheelchair transfers Giulia Barbareschi 1, Tsu-Jui Cheng 2 and Catherine Holloway 1 1 University College London Interaction
Kinematics of Lateral Transfers: A Pilot Study. Sharon Sonenblum, ScM Thursday, August 4 th, 2005
 Kinematics of Lateral Transfers: A Pilot Study Sharon Sonenblum, ScM Thursday, August 4 th, 2005 What is a lateral transfer? Background Lateral transfers are very important to the independent function
Kinematics of Lateral Transfers: A Pilot Study Sharon Sonenblum, ScM Thursday, August 4 th, 2005 What is a lateral transfer? Background Lateral transfers are very important to the independent function
Lift it, Shift it, Twist it
 Lift it, Shift it, Twist it Optimizing Movement to Avoid Workplace Injury Dr. Amanda Williamson, PT, DPT, CSCS Dr. Constanza Aranda, PT, DPT, MSPH Disclosures We present on behalf of the Florida Physical
Lift it, Shift it, Twist it Optimizing Movement to Avoid Workplace Injury Dr. Amanda Williamson, PT, DPT, CSCS Dr. Constanza Aranda, PT, DPT, MSPH Disclosures We present on behalf of the Florida Physical
Understanding Tilt-in-Space Use in Shepherd Center Clients
 Understanding Tilt-in-Space Use in Shepherd Center Clients Sharon Eve Sonenblum, ScM Monday, August 18th, 2008 Shepherd Center In-service What DO we know about Tilt-in-Space? Seating clinic prescribed
Understanding Tilt-in-Space Use in Shepherd Center Clients Sharon Eve Sonenblum, ScM Monday, August 18th, 2008 Shepherd Center In-service What DO we know about Tilt-in-Space? Seating clinic prescribed
eappendix 1. Exercise Instruction Sheet for the Strengthening and Optimal Movements for Painful Shoulders (STOMPS) Trial in Chronic Spinal Cord Injury
 Exercise Instruction Sheet for the Strengthening and Optimal Movements for Painful Shoulders (STOMPS) Trial in Chronic Spinal Cord Injury Instructions: Exercises are to be performed 3 times per week. Allow
Exercise Instruction Sheet for the Strengthening and Optimal Movements for Painful Shoulders (STOMPS) Trial in Chronic Spinal Cord Injury Instructions: Exercises are to be performed 3 times per week. Allow
Validation of the 2-Minute Walk Test with the 6-Minute Walk Test and Other Functional. Measures in Persons with Multiple Sclerosis.
 Validation of the 2-Minute Walk Test with the 6-Minute Walk Test and Other Functional Measures in Persons with Multiple Sclerosis David A. Scalzitti, PhD; Kenneth J. Harwood, PhD; Joyce R. Maring, EdD;
Validation of the 2-Minute Walk Test with the 6-Minute Walk Test and Other Functional Measures in Persons with Multiple Sclerosis David A. Scalzitti, PhD; Kenneth J. Harwood, PhD; Joyce R. Maring, EdD;
University of Manitoba - MPT: Neurological Clinical Skills Checklist
 Name: Site: Assessment Skills Observed Performed Becoming A. Gross motor function i. Describe movement strategies (quality, devices, timeliness, independence): supine sidelying sit stand supine long sitting
Name: Site: Assessment Skills Observed Performed Becoming A. Gross motor function i. Describe movement strategies (quality, devices, timeliness, independence): supine sidelying sit stand supine long sitting
American Council on Exercise
 American Council on Exercise February 23, 2015 Fitnovatives Blog Exercise Progressions for Clients Who Are Overweight or Are Affected by Obesity While there is no single right way to train clients who
American Council on Exercise February 23, 2015 Fitnovatives Blog Exercise Progressions for Clients Who Are Overweight or Are Affected by Obesity While there is no single right way to train clients who
Scoring The score of the test is the distance a patient walks in 6 minutes (measured in meters and can round to the nearest decimal point).
 Core Measure: Six Minute Walk Test (6MWT) Overview The 6MWT is a sub-maximal exercise test used to assess walking endurance and aerobic capacity. Participants will walk around the perimeter of a set circuit
Core Measure: Six Minute Walk Test (6MWT) Overview The 6MWT is a sub-maximal exercise test used to assess walking endurance and aerobic capacity. Participants will walk around the perimeter of a set circuit
Assessments of the Reliability of the Iranian Version of the Berg Balance Scale in Patients with Multiple Sclerosis
 22 Assessments of the Reliability of the Iranian Version of the Berg Balance Scale in Patients with Multiple Sclerosis Akram Azad, Ghorban Taghizadeh, Arash Khaneghini Abstract- Purpose: Because of the
22 Assessments of the Reliability of the Iranian Version of the Berg Balance Scale in Patients with Multiple Sclerosis Akram Azad, Ghorban Taghizadeh, Arash Khaneghini Abstract- Purpose: Because of the
Outcome Measures for Hip Fracture Care Pathway
 Outcome Measures for Hip Fracture Care Pathway Summary of Outcome Measures for Hip Fracture PRE-OP CARE: Braden, Confusion Assessment Method (CAM), Morse, Numeric Pain Rating Scale (NPRS) ACUTE CARE: Braden,
Outcome Measures for Hip Fracture Care Pathway Summary of Outcome Measures for Hip Fracture PRE-OP CARE: Braden, Confusion Assessment Method (CAM), Morse, Numeric Pain Rating Scale (NPRS) ACUTE CARE: Braden,
Version February 2016
 Version 3.1 29 February 2016 Health and Safety Unit 1 Table of Contents 1. Setting up your computer workstation... 3 Step 1: Adjusting yourself to the correct height... 3 Step 2 Adjusting your Chair...
Version 3.1 29 February 2016 Health and Safety Unit 1 Table of Contents 1. Setting up your computer workstation... 3 Step 1: Adjusting yourself to the correct height... 3 Step 2 Adjusting your Chair...
Value of Physical Therapy TINA DUONG PARENT PROJECT MUSCULAR DYSTROPHY ANNUAL CONFERENCE 28JUN2018
 Value of Physical Therapy TINA DUONG PARENT PROJECT MUSCULAR DYSTROPHY ANNUAL CONFERENCE 28JUN2018 Disclosures Scientific Advisory Board: Biogen, Cytokinetics, Roche, Acceleron Consultation: Roche, Audentes,
Value of Physical Therapy TINA DUONG PARENT PROJECT MUSCULAR DYSTROPHY ANNUAL CONFERENCE 28JUN2018 Disclosures Scientific Advisory Board: Biogen, Cytokinetics, Roche, Acceleron Consultation: Roche, Audentes,
Multiple sclerosis (MS) is a chronic, frequently progressive disease of the central nervous
 National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Occupational Therapy in Multiple Sclerosis Rehabilitation by Marcia Finlayson,
National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Occupational Therapy in Multiple Sclerosis Rehabilitation by Marcia Finlayson,
Focusing on the Fundamental Movement Skill of Balancing in a Gymnastics lesson
 Sample Lesson Plan Focusing on the Fundamental Movement Skill of Balancing in a Gymnastics lesson Class Level Strand Strand Unit Curriculum Objectives Learning outcomes Fundamental Movement Skill Resources
Sample Lesson Plan Focusing on the Fundamental Movement Skill of Balancing in a Gymnastics lesson Class Level Strand Strand Unit Curriculum Objectives Learning outcomes Fundamental Movement Skill Resources
Blood Flow and Pressure Changes that Occur with Tilt-in- Space
 RESNA Blood Flow and Pressure Changes that Occur with Tilt-in- Space Journal: RESNA 2010 Annual Conference Manuscript ID: Draft Submission Type: Student Scientific Paper Topic Area: Seating (S) Note: The
RESNA Blood Flow and Pressure Changes that Occur with Tilt-in- Space Journal: RESNA 2010 Annual Conference Manuscript ID: Draft Submission Type: Student Scientific Paper Topic Area: Seating (S) Note: The
Therapy following a neck of femur fracture
 INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
A THESIS SUBMITTED TO THE GRADUATE DIVISION OF THE UNIVERSITY OF HAWAI I AT MĀNOA IN PARTIAL FULFILLMENT OF THE REQUIREMENTS FOR THE DEGREE OF
 PRELIMINARY INVESTIGATION OF THE EFFICACY OF CLINICALLY PRACTICAL DUAL-TASK TESTS AS A CONCUSSION ASSESSMENT TOOL: A COMPARISON OF SINGLE- AND DUAL-TASK TESTS ON HEALTHY YOUNG ADULTS A THESIS SUBMITTED
PRELIMINARY INVESTIGATION OF THE EFFICACY OF CLINICALLY PRACTICAL DUAL-TASK TESTS AS A CONCUSSION ASSESSMENT TOOL: A COMPARISON OF SINGLE- AND DUAL-TASK TESTS ON HEALTHY YOUNG ADULTS A THESIS SUBMITTED
