Rehabilitation Guidelines for Patients Undergoing Precice Nail Lengthening. Joint Academic Committee. Holly Doyle. Aresh Nejad. Clinical 19/04/2021
|
|
|
- Clyde Bartholomew Hicks
- 5 years ago
- Views:
Transcription
1 Rehabilitation Guidelines for Patients Undergoing Precice Nail Lengthening Date Approved 19/04/2018 Ratifying Body Related Documents Joint Academic Committee Physiotherapy rehabilitation guidelines Author Owner (Executive Director) Directorate Superseded Documents Subject Holly Doyle Aresh Nejad Clinical N/A N/A Review Date Keywords and Phrases External References Consultation Group/Approving Bodies Readership CQC Outcomes 19/04/2021 Rehabilitation, physiotherapy, limb deformity surgery, complications, outcomes, milestones, function, treatment, exercise, pain relief, restrictions, limitations, sport, fitness, postural awareness, pain education, mobility, goals, precautions, compliance, knee pain, leg pain e.g. NHSLA RNOH Limb Reconstruction service Clinical staff only Outcome 1: Respecting and involving people who use services Outcome 4: Care and welfare of people who use services Outcome 6: Cooperating with other providers Outcome16: Assessing and monitoring the quality of service provision Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 1
2 NHSLA General Standards 4.1 Patient information & consent 4.2 Patient information 4.4 Screening Procedures 4.7 Physical assessment & examination of patients 4.14 Transfer of patients 4.15 Discharge of patients 5.6 Analysis 5.7 Improvement 5.8 Best practice - NICE Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 2
3 Table of Contents 1. Introductions and aims of guideline Sub heading 2... Error! Bookmark not defined. 2. Definitions Sub heading 2... Error! Bookmark not defined. 3. Duties and Responsibilities Sub heading 2... Error! Bookmark not defined. 4. Body of guideline Sub heading 2... Error! Bookmark not defined. 5. Monitoring and the effectiveness of this guideline Sub heading 2... Error! Bookmark not defined. Appendix 1: Glossary of Terms Appendix 2: Other linked trust policies and guidelines Appendix 3: Extra sources of information and support Appendix 4: Privacy Impact Assessment and Equality Analysis Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 3
4 1. Introductions and aims of guideline Please note that this is advisory information only. Your experiences may differ from those described. All exercises must be demonstrated to a patient by a fully qualified physiotherapist. We cannot be held liable for the outcome of you undertaking any of the exercises shown here independently of direct supervision from the RNOH. As a specialist orthopaedic hospital we recognise that our broad and often complex patient group needs an individualised rehabilitation approach. Our emphasis is on patient-specific rehabilitation, which encourages recognition of those patients who may progress slower than others. These rehabilitation guidelines are therefore milestone driven and designed to provide an equitable rehabilitation service to all our patients. They will also limit unnecessary visits to the outpatient clinic at RNOHT by helping the patient and therapist to identify when specialist review is required. 2. Definitions See Section 4 3. Duties and Responsibilities This section N/A for this guideline 4. Body of guideline Indications for Surgery The main indication for Precice Nail surgery is limb length discrepancy. The aim of surgery is to grow new bone and change the length of the limb. Possible Complications Infection Bleeding Nerve and blood vessel damage Deep vein thrombosis Joint stiffness and soft tissue tightness Pulmonary embolism Persistent / Recurrent pain Joint instability Failure to gain length Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 4
5 Delayed union of bone Loosening of the nail Re-fracture Surgical Techniques A Precice nail is a device, surgically placed within the bone, which is used to grow new bone and change the length of the limb. The nail contains a magnet and a gear system, this enables the nail to lengthen or shorten. It is activated when a programmed external handset is placed on the limb. The operation involves the nail being inserted into the centre of the bone to be lengthened and secured with screws. The bone is also divided in a specific place. The patient will have surgical wounds where the nail and screws are inserted and also in the area where the bone has been divided. After 1 week, the division in the bone will be in the early stages of healing, this is when lengthening should commence. As the bone is pulled apart using the nail, new bone starts to form along a line of tension created by the device and then continues to grow in the gap. Expected Outcome The bone is normally lengthened at the rate of 1mm/day and the patient is nonweight bearing during the lengthening process. The bone needs to harden (consolidate) before the nail is removed. The nail will most likely be in place for months. Every patient is different and the amount of lengthening and time to lengthen may differ between patients. Whilst lengthening they will attend clinic every 2 weeks and have x-rays to confirm that new bone is forming. Based on the x- rays and the soft tissue length can define if lengthening is slowed down or sped up. Correction of the deformity. Pre-operatively The patient may be seen pre-operatively, and with consent, the following can be assessed: Current functional levels General Health Social / Work / Hobbies Functional range of movement Balance / Proprioception Gait / mobility, including walking aids, orthoses Multidisciplinary approach with psychologists, pain management, nursing and Physiotherapy (guide to stretches) Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 5
6 Post-operative expectations, commitment to exercises and maintaining protocol. Patient information leaflet issued Post-operative management explained Post-operatively Always check the operation notes, and the post-operative instructions. Discuss any deviation from routine guidelines with the team concerned. INITIAL REHABILITATION PHASE: In-patient Stay (Usually 6-8 days) Goals To be safely and independently mobile with appropriate walking aid/s, adhering to non-weight bearing status. To be independent with home exercise programme. To understand self-management / monitoring. Maintaining full range of Hip/knee/ankle ROM- Achieve 90 degrees of knee/hip flexion prior to discharge. Minimal swelling Restrictions If sedentary employment, may be able to return to work from 2-4 weeks postoperatively, as long as provisions are made to elevate leg, remain non-weight bearing and no complications. Children may be able to return to school if adaptations are made possible with classrooms and mobility. Treatment Pain-relief: Ensure adequate analgesia. Advice / Education: Teach how to monitor sensation, colour, circulation, temperature, swelling, and advise on scar tissue expectations and advise what to do if concerned. Teach protection, rest, and elevation. Advice on maintaining good postures for muscles that could be compromised by lengthening process (ie. If Tibial lengthening do not let foot rest in equinus all day) and on implications of contracture if do not complete stretches. Swelling management. Exercises: Example exercises AROM exercises for hip/knee/ankle to ensure maintaining range despite NWB Stretches for relevant muscle groups for nail position: Femoral nail: Quads, hamstrings, ITB, adductors and glutes Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 6
7 Tibial Nail: Gastrocs, Soleus, TA and tibialis anterior 5 sets of stretching daily-stretching prior to lengthening in the morning, then 1hr after lengthening (usually 3 x daily) and then once more in evening once lengthening for the day is complete. Emphasis on stretching the more pennate or posterior/lateral muscle groups especially gastrocs, hamstrings and ITB. These muscle groups are more likely to lead to contractures. Stretch to the point of pain and hold for 30 seconds 3 x each muscle group, with 15 seconds rest in between each stretching exercise. Gait re-education: Ensure safely and independently mobile non weight bearing with walking aid/s Stretches taught rigorously in preparation for lengthening phase. Focus on correct stretching technique non weight bearing of Gastrocs/hamstrings/quads/adductors/ITB/soleus, combined with education on stretching to point of tolerance. Exercises: Some example exercises: Precice tibial exercise sheet (TBC) Precice Femoral exercise sheet (TBC) Hamstrings-Ankle raised with knee unsupported-gravity assisted stretch Prone foot hangs over edge of bed. Quads- heel to bottom stretch ITB- Adduction past the midline using a non-elastic band for assistance Adductors: Abduction with forward lean in sitting Gastrocs: With band around forefoot. Knee/hip and ankle range of movement exercises Strengthening- Maintain non weight bearing muscle strength, isometric and open chain quads and hamstrings, hip flexion, ankle dorsiflexion and plantarflexion. Pacing advice as appropriate. Mobility: Ensure patient is independent with transfers and mobility, including stairs if necessary. Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 7
8 On discharge from the ward Independent and safe mobilising with appropriate walking aid/s, including safety on stairs if appropriate. Independent and safe with home exercise programme. Maintaining hip/(knee at least 90 degrees flexion) /ankle range of movement Independent with swelling management Ongoing out-patient physiotherapy arranged for within 2 weeks post op Milestones to progress to lengthening phase Achieving and maintaining full ROM of hip/knee/ankle Safe with non-weight bearing mobilisation Minimal effusion Ideally full quadriceps activation (full isometric contraction and ideally no quads lag on SLR when assessed by physiotherapist) LENGTHENING PHASE: Day 6/7- up to 80 days (1mm a day, depends on length of bone patient needs to achieve). Goals Maintain full range of hip/knee and ankle Maintain non-weight bearing throughout lengthening stage Monitor closely for first signs of contracture and stop lengthening immediately. Lengthening 3 x daily (femoral nail), 2 x daily (tibial nail) Pain controlled. Restrictions If sedentary employment, may be able to return to work from 2-4 weeks postoperatively, as long as provisions are made to elevate leg, and no complications. Driving: unable to drive whilst weight-bearing status restricted. Maintain non-weight bearing status. Complications: The data we have collected shows the most vulnerable period for contractures to develop is around day 30 (seen at 3cm through hip musculature, 2 cm through knee musculature). Implant failure of nail or gear box. Wound infection. Nerve damage. See above Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 8
9 Treatment Options Pain Relief: Ensure adequate analgesia and taken prior to lengthening Advice / Education: Comprehensive education and instruction on restrictions and on carrying out activities of daily living to manage pain and swelling Posture advice / education. Swelling management. Gait re-education. Mobility: Ensure safely and independently mobile with walking aid/s progressing to safe and independently mobile without mobility aid/s. Exercises: Example exercises Strengthening- Maintaining quads, glutes and hamstring strength in nonweight bearing Stretches- As previously discussed, and consistent re-evaluation and monitoring of range to identify tight muscle groups. Main Issues: From our data collection patients with short stature and congenital short femur had a higher risk of knee contractures with a retrograde femoral nail. Retrograde femoral nail- the median length at which ROM decreased was 3.25cm of lengthening. Antegrade femoral nail-the median length at which ROM decreased was 3cm of lengthening. Antegrade tibial nail-most soft tissue issues are observed from 2cm of lengthening. Retrograde tibial nail-85% of patients had knee stiffness with a retrograde nail which occurred from 1.5cm of lengthening. Hydrotherapy if appropriate (available), once wounds healed and to help improve range of movement if contractures develop etc. Pacing advice as appropriate. Milestones to progress to next phase No evidence of contractures Good bony consolidation on X-ray Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 9
10 POST LENGTHENING REHABILITATION PHASE: Goals Return to full weight bearing as per consultant guidelines. Commence loading programme Restrictions Ensure patient follows Consultant s instructions on weight bearing status week by week, if no complications and good consolidation then 25% week 1 after cessation of lengthening, 50% week 2, 75% week 3 and 100% by week 4. Treatment Pain Relief: Ensure adequate analgesia Advice / Education: Comprehensive education and instruction on restrictions and on carrying out activities of daily living to manage pain and swelling. Posture advice / education. Swelling management. Mobility: Ensure safely and independently mobile without walking aid (if applicable). Exercises Example exercises: Cycling, Cross trainer Alter-G treadmill (If available) especially relevant at 25%-75% weight bearing as can start normalisation of loading tissues and bone at weight bearing status. Balance / Proprioception progress weight shift exercises to single leg balance and ultimately proprioceptive exercises. Strengthening of muscles stabilising the knee, hip and ankle. Strengthening of other muscle groups as appropriate. Core stability and gluteal control work Stretches maintain stretches as appropriate to ensure normal flexibility of quadriceps, hamstrings and calf muscles in weight bearing position. Review lower limb biomechanics and kinetic chain, addressing issues as appropriate. Biofeedback may be used if altered sequencing of muscles. Manual therapy: o Soft tissue techniques as appropriate. o Joint mobilisations as appropriate. Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 10
11 Hydrotherapy (if available)- especially relevant at 25%-75% weight bearing as can start normalisation of loading tissues and bone at weight bearing status. Pacing advice as appropriate. Milestones for discharge Good proprioceptive control dynamically. Return to normal functional level. Achieved patient goals. Failure to meet milestones Refer back to team / Discuss with team. Continue with outpatient physiotherapy if still progressing and appropriate goals. Failure to progress If a patient is failing to progress, then consider the following: 5. Monitoring and the effectiveness of this guideline POSSIBLE PROBLEM Swelling ACTION Ensure elevating leg regularly. Use ice as appropriate if normal skin sensation and no contraindications. Pacing. Use walking aids. Circulatory exercises. Modify exercise programme as appropriate. If does not decrease over a few days, refer back to surgical team Pain Decrease activity. Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 11
12 Ensure adequate analgesia. Elevate regularly. Reduce amount of lengthening (liaise with surgeon) Pacing discussion and modify exercise programme as appropriate. Should continue isometric work at all times. If persists, refer back to surgical team. Breakdown of wound e.g. inflammation, bleeding, infection Contracture Refer to surgical/cns team. Identify reduced range of movement as soon as possible and alert surgical team. Stop lengthening process with approval from surgical team, until soft tissue length catches up to bone length. Re-enforce importance of stretches// increase daily number. Consider local anaesthetic or botox injections with surgical team. Varus deformity (mainly tibias) Alert surgical team immediately Appendix 1: Please add text here. Glossary of Terms Appendix 2: Other linked trust policies and guidelines Other orthopaedic rehabilitation guidelines for knee surgery would sit here Link to rehabilitation guidelines for all other teams Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 12
13 Appendix 3: Extra sources of information and support Summary of evidence for physiotherapy guidelines A comprehensive literature search was carried out to identify research relating to rehabilitation following Precice Nail surgery. However due Precice nail surgery being an innovative new surgical practice, there is no research currently available on rehabilitation after Precice Nail surgery. Therefore we reviewed other lengthening methods and results of stretching programmes on normal muscles as well as effects of lengthening in animal models. After reviewing the articles and information, and discussion with the consultants and therapists at the RNOH, the physiotherapy guidelines were produced on the best available evidence. References: Apostolopoulos, N., Metsios, G., Flouris, A., Koutedakis, Y. and Wyon, M. (2015) The relevance of stretch intensity and position a systematic review, Frontiers in Psychology, 6. Blazevich, A., Cannavan, D., Waugh, C., Miller, S., Thorlund, J., Aagaard, P. and Kay, A. (2014) Range of motion, neuromechanical, and architectural adaptations to plantar flexor stretch training in humans, Journal of Applied Physiology, 117(5), pp Cabido, C.E.T., Bergamini, J.C., Andrade, A.G.P., Lima, F.V., Menzel, H.J. and Chagas, M.H. (2013) ACUTE EFFECT OF CONSTANT TORQUE AND ANGLE STRETCHING ON RANGE OF MOTION, MUSCLE PASSIVE PROPERTIES, AND STRETCH DISCOMFORT PERCEPTION, Journal of Strength and Conditioning Research, 28(4), p Calder, P., Laubscher, M. and Goodier, W. (2017) The role of the intramedullary implant in limb lengthening, Injury, 48, pp.s52-s58. Calder, P.R., McGrath, M., Timms, A., and Goodier, W.D. (2013) The precice intramedullary limb lengthening system- Early results, The Journal of Bone and Joint research, 95, pp1-2. Cipriani, D.J., Terry, M.E., Haines, M.A., Tabibnia, A.P., Lyssanova, O. (2012) Effect of stretch frequency and sex on the rate of gain and rate of loss in muscle flexibility during a hamstring-stretching program: a randomized single-blind longitudinal study, Journal of Strength and Conditioning Research, 26(8), pp Demoulin, C., Wolfs, S., Chevalier, M., Granado, C., Grosdent, S., Depas, Y., Roussel, N., Hage, R. and Vanderthommen, M. (2016) A comparison of two stretching programs for hamstring muscles: A randomized controlled assessor-blinded study, Physiotherapy Theory and Practice, 32(1), pp Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 13
14 Freitas, S. and Mil-Homens, P. (2015) Effect of 8-Week High-Intensity Stretching Training on Biceps Femoris Architecture, Journal of Strength and Conditioning Research, 29(6), pp Gajdosik, R.L. (2001) Passive extensibility of skeletal muscle: review of the literature with clinical implications, Clinical Biomechanics, 16, pp Gajdosik, R. (1991) Effects of Static Stretching on the Maximal Length and Resistance to Passive Stretch of Short Hamstring Muscles, Journal of Orthopaedic & Sports Physical Therapy, 14(6), pp Makarov, M., Birch, J., and Samchukov, M. (2009) The Role of Variable Muscle Adaptation to Limb Lengthening in the Development of Joint Contractures Journal of Paediatric Orthopaedics, 29(2), pp Puentedura, E., Huijbregts, P., Celeste, S., Edwards, D., In, A., Landers, M. and Fernandez-de-las-Penas, C. (2011) Immediate effects of quantified hamstring stretching: Hold-relax proprioceptive neuromuscular facilitation versus static stretching, Physical Therapy in Sport, 12(3), pp Schiedel, F., Vogt, B., Tretow, H., Schuhknecht, B., Gosheger, G., Horter, M. and Rödl, R. (2014 How precise is the PRECICE compared to the ISKD in intramedullary limb lengthening? Acta Orthopaedica, 85(3), pp Yuktasir, B. and Kaya, F. (2009) Investigation into the long-term effects of static and PNF stretching exercises on range of motion and jump performance Journal of Bodywork and Movement Therapies, 13(1), pp Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 14
15 Appendix 4: Privacy Impact Assessment and Equality Analysis Please add text here.this guideline is available on request in large print and alternative languages. It is a manager s responsibility to ensure employees are aware of these options. * The following policies must be sent for review to the Local Counter Fraud Specialist: Fraud and Bribery Standard Financial Instructions Declaration of Interests Gifts and Hospitality Whistleblowing Disciplinary IT Anti-Money Laundering Managing Sickness Absence Secondary Employment Expenses Overpayment Financial Redress TOIL (Time off in Lieu) Code of Conduct/Standards of Business Conduct Data Protection Lone Worker Patient Transport Commercial Sponsorship Overseas Visitors Disclosure Rehabilitation Guidelines for patients undergoing Precice Nail Lengthening Page 15
Foot and ankle fractures
 Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Bunion (hallux valgus deformity) surgery
 Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
INITIAL REHABILITATION PHASE 0-4 weeks. Posterolateral Corner Injury
 Posterolateral Corner Injury Indications for Surgery The main indication of PLC reconstruction surgery is symptomatic instability following PLC injury. The aim of PLC reconstruction surgery is to restore
Posterolateral Corner Injury Indications for Surgery The main indication of PLC reconstruction surgery is symptomatic instability following PLC injury. The aim of PLC reconstruction surgery is to restore
Foot and ankle. Achilles tendon rupture repair. After surgery
 Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Total ankle replacement
 Total ankle replacement Initial rehabilitation phase 0-4 weeks To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise
Total ankle replacement Initial rehabilitation phase 0-4 weeks To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise
Rehabilitation guidelines for patients undergoing Anterior Ankle Arthroscopy
 Rehabilitation guidelines for patients undergoing Anterior Ankle Arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We
Rehabilitation guidelines for patients undergoing Anterior Ankle Arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We
Ankle instability surgery
 Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Post Operative Total Hip Replacement Protocol Brian J. White, MD
 Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Adam N. Whatley, M.D Main St., STE Zachary, LA Phone(225) Fax(225)
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Knee Arthroplasty Protocol: The intent of this protocol is to provide the clinician with a guideline
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Knee Arthroplasty Protocol: The intent of this protocol is to provide the clinician with a guideline
Guidance for the Physiotherapy Management of Patients Undergoing Limb Reconstruction with a Circular Frame External Fixator.
 Guidance for the Physiotherapy Management of Patients Undergoing Limb Reconstruction with a Circular Frame External Fixator. Table of Contents INTRODUCTION... 2 TARGET AUDIENCE... 2 KEY CHANGES FROM PREVIOUS
Guidance for the Physiotherapy Management of Patients Undergoing Limb Reconstruction with a Circular Frame External Fixator. Table of Contents INTRODUCTION... 2 TARGET AUDIENCE... 2 KEY CHANGES FROM PREVIOUS
Sports Rehabilitation & Performance Center Medial Patellofemoral Ligament Reconstruction Guidelines * Follow physician s modifications as prescribed
 The following MPFL guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital for Special Surgery. Progression is based on healing constraints, functional progression
The following MPFL guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital for Special Surgery. Progression is based on healing constraints, functional progression
Post-Operative Meniscus Repair Protocol Brian J.White, MD
 Post-Operative Meniscus Repair Protocol Brian J.White, MD www.western-ortho.com (This protocol should be used with combined a ACL Reconstruction and meniscus repair) The intent of this protocol is to provide
Post-Operative Meniscus Repair Protocol Brian J.White, MD www.western-ortho.com (This protocol should be used with combined a ACL Reconstruction and meniscus repair) The intent of this protocol is to provide
Anterior Cruciate Ligament (ACL) Reconstruction
 Further information Information on who to contact, i.e. web sites / telephone numbers of other departments / organisations which may be of help. How to contact us Watford General Hospital West Hertfordshire
Further information Information on who to contact, i.e. web sites / telephone numbers of other departments / organisations which may be of help. How to contact us Watford General Hospital West Hertfordshire
Post Operative ACL Reconstruction Protocol Brian J. White, MD
 Post Operative ACL Reconstruction Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve as
Post Operative ACL Reconstruction Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve as
Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol
 Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol Progression is based on healing constraints, functional progression specific to the patient. Phases and time frames are designed
Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol Progression is based on healing constraints, functional progression specific to the patient. Phases and time frames are designed
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Brennen Lucas, M.D. Advanced Orthopaedic Associates
 Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Advice following Anterior Cruciate Ligament (ACL) reconstruction
 Advice following Anterior Cruciate Ligament (ACL) reconstruction Information for patients Mobilisation As soon as you feel well enough after the operation you will be able to get up and mobilise. You will
Advice following Anterior Cruciate Ligament (ACL) reconstruction Information for patients Mobilisation As soon as you feel well enough after the operation you will be able to get up and mobilise. You will
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS)
 Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Information and exercises following a proximal femoral replacement
 Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Proximal Medial Gastrocnemius Release (PMGR)
 Proximal Medial Gastrocnemius Release (PMGR) Physiotherapy and Orthopaedic Department Patient information leaflet Date: Name of Patient: Name of Physiotherapist: Telephone: 01483 464153 This leaflet has
Proximal Medial Gastrocnemius Release (PMGR) Physiotherapy and Orthopaedic Department Patient information leaflet Date: Name of Patient: Name of Physiotherapist: Telephone: 01483 464153 This leaflet has
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT 12+ weeks, no
ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT 12+ weeks, no
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
ACL REHABILITATION PROTOCOL
 Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Mr Paul Y F Lee All in side - ACL Reconstruction Version 2.2. Sports Knee Surgery. Rehabilitation protocol. ACL Reconstruction.
 Sports Knee Surgery Rehabilitation protocol ACL Reconstruction ACL Repair Meniscus Repair Surgeon: Paul Y F Lee MBBch, MFSEM, MSc, PhD, FRCS (T&O) Why ACL Reconstruction? The ACL helps to stabilize the
Sports Knee Surgery Rehabilitation protocol ACL Reconstruction ACL Repair Meniscus Repair Surgeon: Paul Y F Lee MBBch, MFSEM, MSc, PhD, FRCS (T&O) Why ACL Reconstruction? The ACL helps to stabilize the
Protocol for the Management of Hip Arthroscopy Surgery
 Overall Aims of Surgery To decrease pain To increase range of motion (ROM) To increase hip/pelvis and lumbar stability To enable return to activities of daily living and sport Initial Post-operative Objectives
Overall Aims of Surgery To decrease pain To increase range of motion (ROM) To increase hip/pelvis and lumbar stability To enable return to activities of daily living and sport Initial Post-operative Objectives
GALLAND/KIRBY PCL RECONSTRUCTION POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY PCL RECONSTRUCTION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue TED Hose
GALLAND/KIRBY PCL RECONSTRUCTION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue TED Hose
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
Femoral Condyle Rehabilitation Guidelines
 Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Ankle Fracture Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Anterior Cruciate Ligament (ACL) Reconstruction Protocol. Hamstring Autograft, Allograft, or Revision
 Anterior Cruciate Ligament (ACL) Reconstruction Protocol Hamstring Autograft, Allograft, or Revision As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp,
Anterior Cruciate Ligament (ACL) Reconstruction Protocol Hamstring Autograft, Allograft, or Revision As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp,
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon
 Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
ARTHROSCOPIC MENISECTOMY PROTOCOL
 REHABILITATION PROGRESSION ARTHROSCOPIC MENISECTOMY PROTOCOL The following are guidelines for rehabilitation progression following menisectomy, loose body removed, or debridement etc. Progression through
REHABILITATION PROGRESSION ARTHROSCOPIC MENISECTOMY PROTOCOL The following are guidelines for rehabilitation progression following menisectomy, loose body removed, or debridement etc. Progression through
A patient s guide to. Inferior Heel Pain
 A patient s guide to Inferior Heel Pain The Foot & Ankle Unit at the Royal National Orthopaedic Hospital is made up of a multi-disciplinary team. The team consists of four specialist orthopaedic foot and
A patient s guide to Inferior Heel Pain The Foot & Ankle Unit at the Royal National Orthopaedic Hospital is made up of a multi-disciplinary team. The team consists of four specialist orthopaedic foot and
REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol
 REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol Phase I (Days 1 7) WEIGHTBEARING STATUS 1- Two crutches, weightbearing as tolerated. Exercises 1- Heel slides/wall
REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol Phase I (Days 1 7) WEIGHTBEARING STATUS 1- Two crutches, weightbearing as tolerated. Exercises 1- Heel slides/wall
Post-operative information Total knee replacement
 Post-operative information Total knee replacement Day of operation You will arrive on the ward following your surgery. You may have had a spinal anaesthetic which will wear off after a couple of hours.
Post-operative information Total knee replacement Day of operation You will arrive on the ward following your surgery. You may have had a spinal anaesthetic which will wear off after a couple of hours.
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction
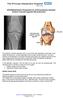 GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
CAPPAGH NATIONAL ORTHOPAEDIC HOSPITAL, FINGLAS, DUBLIN 11. The Sisters of Mercy. Hip Arthroscopy
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Rehabilitation Phase 1 (Day 1
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Rehabilitation Phase 1 (Day 1
Microfracture of Knee Joint
 Microfracture of Knee Joint Post-op Precautions: The patient will ambulate with crutches for 4 weeks or more after surgery. The physician will base weightbearing status upon the location of the lesion.
Microfracture of Knee Joint Post-op Precautions: The patient will ambulate with crutches for 4 weeks or more after surgery. The physician will base weightbearing status upon the location of the lesion.
GUIDELINES FOR REHABILITATION Arthroscopic Meniscectomy/Loose Body Removal/Debridement
 GENERAL GUIDELINES Cryotherapy: Change ice packs or apply cryocuff every 4 hours while awake for first 72 hrs. GENERAL PROGRESSION OF ACTIVITIES OF DAILY LIVING Patients may begin the following activities
GENERAL GUIDELINES Cryotherapy: Change ice packs or apply cryocuff every 4 hours while awake for first 72 hrs. GENERAL PROGRESSION OF ACTIVITIES OF DAILY LIVING Patients may begin the following activities
Anterior Cruciate Ligament Reconstruction
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
MATRIX-INDUCED AUTOLOGOUS CHONDROCYTE IMPLANTATION PHYSICAL THERAPY PRESCRIPTION
 UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
GALLAND/KIRBY TOTAL KNEE AND UNI-COMPARTMENT ARTHROPLASTY POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY TOTAL KNEE AND UNI-COMPARTMENT ARTHROPLASTY POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 7 TED Hose x 6 weeks Walker or crutches: Primary Weight bearing as tolerated (WBAT) Revision
GALLAND/KIRBY TOTAL KNEE AND UNI-COMPARTMENT ARTHROPLASTY POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 7 TED Hose x 6 weeks Walker or crutches: Primary Weight bearing as tolerated (WBAT) Revision
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT. Brace E-Z Wrap locked at zero degree extension, sleep in Brace
 Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
ACL Reconstruction Protocol (Allograft)
 ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
Meniscal Repair Protocol-Dr. McClung
 Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Meniscal Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in full extension for ambulation and sleeping but drop-locked for sitting and knee ROM. Patients
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
ACL REHABILITATION. Key to Success
 ACL REHABILITATION The overall rehabilitation plan emphasises the importance of pre-operative exercises followed post operatively by early control of swelling and regaining full extension (straightening)
ACL REHABILITATION The overall rehabilitation plan emphasises the importance of pre-operative exercises followed post operatively by early control of swelling and regaining full extension (straightening)
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol
 Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Dr Schock High Tibial Osteotomy
 Dr Schock High Tibial Osteotomy Goals for phase 1 Control pain Control edema Initiate ROM and quad strengthening Maintain WB restrictions Appropriate brace wear Criteria for progression to Phase 2 Edema
Dr Schock High Tibial Osteotomy Goals for phase 1 Control pain Control edema Initiate ROM and quad strengthening Maintain WB restrictions Appropriate brace wear Criteria for progression to Phase 2 Edema
Therapy following a neck of femur fracture
 INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
MENISCAL REPAIR ACCELERATED REHABILITATION GUIDELINES
 MENISCAL REPAIR ACCELERATED REHABILITATION GUIDELINES MIHAI VIOREANU MD, MCH, FRCSI (TR&ORTH) www.mrmv.ie MR. VIOREANU, WHERE POSSIBLE, WILL TRY TO PRESERVE AND REPAIR THE MENISCUS. Recent research has
MENISCAL REPAIR ACCELERATED REHABILITATION GUIDELINES MIHAI VIOREANU MD, MCH, FRCSI (TR&ORTH) www.mrmv.ie MR. VIOREANU, WHERE POSSIBLE, WILL TRY TO PRESERVE AND REPAIR THE MENISCUS. Recent research has
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
High Tibial Osteotomy (HTO) Rehabilitation Protocols
 High Tibial Osteotomy (HTO) Rehabilitation Protocols Targets Upon Discharge from Hospital Protected weight-bearing (feather-weight -bearing) Ambulating with crutches Rehab brace without range of motion
High Tibial Osteotomy (HTO) Rehabilitation Protocols Targets Upon Discharge from Hospital Protected weight-bearing (feather-weight -bearing) Ambulating with crutches Rehab brace without range of motion
ACL RECONSTRUCTION PROTOCOL
 ACL RECONSTRUCTION PROTOCOL Name of Protocol/Regime ACL Reconstruction Consultant Updated On Updated By Review Date Mr Dawson 5/5/16 Barbara Pinguey/ Rachael Edgar 6/18 Please note that surgeons may have
ACL RECONSTRUCTION PROTOCOL Name of Protocol/Regime ACL Reconstruction Consultant Updated On Updated By Review Date Mr Dawson 5/5/16 Barbara Pinguey/ Rachael Edgar 6/18 Please note that surgeons may have
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft
 Sports Medicine and Rehabilitation Center Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation
Sports Medicine and Rehabilitation Center Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation
9180 KATY FREEWAY, STE. 200 (713)
 AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015
 PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015 REHABILITATION PROGRAM PHASE 1: WEEKS 0-6: PHASE I GOALS: Protect the surgical graft(s) 0-60 ROM Regain adequate quadriceps control CRUTCHES:
PCL/PLC RECONSTRUCTION REHABILITATION Revised OCTOBER 2015 REHABILITATION PROGRAM PHASE 1: WEEKS 0-6: PHASE I GOALS: Protect the surgical graft(s) 0-60 ROM Regain adequate quadriceps control CRUTCHES:
Sports Rehabilitation & Performance Center Rehabilitation Guidelines for Non-operative Treatment of Patellofemoral Instability *
 Sports Rehabilitation & Performance Center Rehabilitation Guidelines for Non-operative Treatment of The following guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital
Sports Rehabilitation & Performance Center Rehabilitation Guidelines for Non-operative Treatment of The following guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital
Post-operative information ACL reconstruction
 Post-operative information ACL reconstruction On discharge: Ensure you are steady on your crutches at the time of hospital discharge. Feel free to put your full weight on your operated knee, and bend the
Post-operative information ACL reconstruction On discharge: Ensure you are steady on your crutches at the time of hospital discharge. Feel free to put your full weight on your operated knee, and bend the
Hip Arthroscopy Labral Repair Protocol
 Hip Arthroscopy Labral Repair Protocol Applicability: Physician Practices Date Effective: 09/2013 Department: Rehabilitation Services Date Last Reviewed: 1/2018 Supersedes: n/a Administration Approval:
Hip Arthroscopy Labral Repair Protocol Applicability: Physician Practices Date Effective: 09/2013 Department: Rehabilitation Services Date Last Reviewed: 1/2018 Supersedes: n/a Administration Approval:
Medial Collateral Ligament Repair Protocol-Dr. McClung
 Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
Medial Collateral Ligament Repair Protocol-Dr. McClung Brace: Normally patients will be wearing post-op knee brace locked in 30 degrees for ambulation and sleeping but drop-locked for sitting and knee
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: - POD 1: Debulk dressing, TED Hose in place - POD 2: Change
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: - POD 1: Debulk dressing, TED Hose in place - POD 2: Change
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: MENISCAL REPAIR: 1. General Guidelines: Time lines in this rehabilitation protocol are approximate. If the
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: MENISCAL REPAIR: 1. General Guidelines: Time lines in this rehabilitation protocol are approximate. If the
Periarticular knee osteotomy
 Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE
 PHYSICAL THERAPY SECTION WILLIAM BEAUMONT ARMY MEDICAL CENTER 5005 N. PIEDRAS ST EL PASO, TEXAS 79920 KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE Revised August 2008 Post-op Days 1 14 Dressing POD
PHYSICAL THERAPY SECTION WILLIAM BEAUMONT ARMY MEDICAL CENTER 5005 N. PIEDRAS ST EL PASO, TEXAS 79920 KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE Revised August 2008 Post-op Days 1 14 Dressing POD
ACHILLES TENDON REPAIR REHAB GUIDELINES
 ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
Patient Guide. Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening
 Patient Guide Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening Introduction You have decided to have a limb lengthening operation. The surgery you have chosen uses a device
Patient Guide Intramedullary Skeletal Kinetic Distractor For Tibial and Femoral Lengthening Introduction You have decided to have a limb lengthening operation. The surgery you have chosen uses a device
Total Knee Replacement
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Pre-Operative... 3 7.2 Post-Operative...
Anterior Cruciate Ligament Reconstruction Standard Rehabilitation Protocol Dr. Mark Adickes
 Anterior Cruciate Ligament Reconstruction Standard Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction
Anterior Cruciate Ligament Reconstruction Standard Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction
Knee PCL Reconstruction Rehabilitation Program
 The Gundersen Health System Sports Medicine PCL Reconstruction Rehabilitation Program is an evidencebased and soft tissue healing dependent program allowing patients to progress to vocational and sports-related
The Gundersen Health System Sports Medicine PCL Reconstruction Rehabilitation Program is an evidencebased and soft tissue healing dependent program allowing patients to progress to vocational and sports-related
FOOT AND ANKLE ARTHROSCOPY
 FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
Patellar Tendon Debridement & Repair Rehabilitation Protocol
 Patellar Tendon Debridement & Repair Rehabilitation Protocol PREOPERATIVE PHASE Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore voluntary muscle
Patellar Tendon Debridement & Repair Rehabilitation Protocol PREOPERATIVE PHASE Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore voluntary muscle
Physiotherapy following peri acetabular osteotomy (PAO) surgery
 Physiotherapy following peri acetabular osteotomy (PAO) surgery This leaflet explains more about returning to your everyday activities after your peri acetabular osteotomy (PAO). It explains the exercises
Physiotherapy following peri acetabular osteotomy (PAO) surgery This leaflet explains more about returning to your everyday activities after your peri acetabular osteotomy (PAO). It explains the exercises
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
Human anatomy reference:
 Human anatomy reference: Weak Glut Activation Weak gluteal activation comes from poor biomechanics, poor awareness when training or prolonged exposure in deactivated positions such as sitting. Weak Glut
Human anatomy reference: Weak Glut Activation Weak gluteal activation comes from poor biomechanics, poor awareness when training or prolonged exposure in deactivated positions such as sitting. Weak Glut
Postoperative Days 1-7
 ACL RECONSTRUCTION REHABILITATION PROTOCOL Postoperative Days 1-7 *IT IS EXTREMELY IMPORTANT THAT YOU WORK ON EXTENSION IMMEDIATELY Goals: * Control pain and swelling * Care for the knee and dressing *
ACL RECONSTRUCTION REHABILITATION PROTOCOL Postoperative Days 1-7 *IT IS EXTREMELY IMPORTANT THAT YOU WORK ON EXTENSION IMMEDIATELY Goals: * Control pain and swelling * Care for the knee and dressing *
GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline
 Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for
Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY
 A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
A PATIENT S GUIDE TO REHABILITATION POST KNEE REPLACEMENT SURGERY Georgia Bouffard Student Physiotherapist Colin Walker Orthopaedic Knee Specialist Frank Gilroy BSc MSCP 1 CONTENTS Anatomy of the knee
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL
 ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
ANATOMIC ACL RECONSTRUCTION RECOVERY & REHABILITATION PROTOCOL PREOPERATIVE: If you have suffered an acute ACL injury and surgery is planned, the time between injury and surgery should be used to regain
GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
Glossary. WZWA Wheeled zimmer walking aid. ZF Zimmer frame. E/C Elbow crutches. A/C Axillary crutches. MUA Manipulation under anaesthetic
 WZWA Wheeled zimmer walking aid ZF Zimmer frame E/C Elbow crutches A/C Axillary crutches MUA Manipulation under anaesthetic ORIF Open reduction internal fixation DHS Dynamic hip screw IM Nail Intramedullary
WZWA Wheeled zimmer walking aid ZF Zimmer frame E/C Elbow crutches A/C Axillary crutches MUA Manipulation under anaesthetic ORIF Open reduction internal fixation DHS Dynamic hip screw IM Nail Intramedullary
