Overview. Nature of Soft Tissue Healing and Repair. Terms. Principles of Physiotherapy Interventions for Common Sport Injuries
|
|
|
- Jocelin Bridges
- 5 years ago
- Views:
Transcription
1 Principles of Physiotherapy Interventions for Common Sport Injuries Sport Injuries PT Mx Nature of Healing and Repair Injury Identification Rehabilitation Principles Tan Yee Siong Sport Physiotherapist TYS Physio On Wheel Overview Wound Damage/disruption of normal anatomical structure and functions Nature of Soft Tissue Healing and Repair Healing A coordinated series of events in response to an injury/wound resulting in partial or complete repair and regeneration of the lost part Repair - The process of synthesizing connective tissues and its subsequent maturation into scar tissues Regeneration The exact replacement of the lost cells by cells of the same type Connective Tissues A group of wide variation cells that provide the structural framework, supports, transport and energy storage within the body Terms Connective Tissue Proper [Areolar Tissue] The Normal Healing Cascade 1
2 Local tissue reactions to injury, sometimes known as the demolition phase/clean-up process. Preserve and restore homeostasis, ie returning normal tissues condition and cells environment. 4 cardinal signs: rubor, tumor, dolor, calor [Celsus AD35] + loss of function described by Virchow Suffix of itis Prerequisite for repair and regeneration Acute Inflammation Acute Inflammation Seen in lower vertebrates eg earthworm up to complex organism eg human. Human s organs /tissues regenerative powers varies and limited. Certain discrepancies between the amount of regeneration and repair. Epithelial, connective tissues (except cartilage), smooth muscles tissues usually regenerate well. Muscle and neural tissues regenerate poorly. Possible Response after Injury Regeneration { Local { Disturbed demolition phase Vascularity Excess movements Foreign material Infection/irradiation Systemic Malnutrition Corticosteroids Jaundice Rate of Healing Factors Influencing Wound healing 2
3 Identification of Injury Stress-Strain Curve Excellent in the treatment and management of MS dysfunction can only be obtained as a result of the application of a logical, systematic, careful and intellectual examination and assessment strategy. Petty & Moore 1999 I know that you believe you understand what I said, but I am not sure you realize that what you heard is not what I meant. Maitland 1986 Why Examination and Ax? Always listen to what patient has to say. What are the mechanisms of injury? Which structures could be the source of the symptom/site of injury? What is the nature of the injury/condition? What others factors need to be examined? Is the condition severe and/or irritable? Key Identification from the Subjective Ax Systematic and goal-oriented. Every piece of information gather is just a clue, not the truth by itself. Do not test for the sake of testing. The value of examination/tests carried out must be weighted. Keep and open-mind, think logically rather quickly jumping into conclusion. Establish comparable sign. Strain Sprain Dislocation Subluxation Muscle/tendon rupture Tendinoathy/Tendinosi s Synovitis Hemarthrosis Contusion Bursitis Synovitis Ganglion RSI Key Points in Physical Examination Common MS Lesions 3
4 Synovial Fluid Quality Time Lapse Colour Viscosity 2 weeks Bloody red Watery 5 weeks Apricot orange Loose salivary 4 months Clear light yellow Loose salivary 8 months Clear light yellow Thick salivary years Clear light yellow Thick mucus Cartilage Flakes White colour fragmented debris suspended in the synovial fluid. Differential Dx of Soft Tissues Disorder Synovial Fluid Inspection Degree of Injury Grade 1 Grade 2 Grade 3 Pain Mild Moderate Severe Playability Able Unable Unable Stress Response Structural Integrity ERP ERP Nil Preserved Joint play increased Laxity/ Instability Principles of Rehabilitation Severity of Tissue Injury Return to Sport Sorts Specific Training Neuromuscular relearning Specific Sport Drills Plyometric and Agility Neuromuscular Control 3 Aerobic & Endurance ROM Muscular Strength Proprioception The Initial Guide where Everything Started CR Capacity Muscles Strength and Endurance Neuromuscular Control 2 Protection and Healing ROM and Muscle activation Weight Bearing and Mobility Neuromuscular Control 1 LL Rehabilitation RoadMap 4
5 Sorts Specific Training Strength 3 [task specific] Neuromuscular Control 3 [closed-chain stabilization] Functional 2 [Eccentric-plyo, Total body] ROM 2 Strength and Endurance [dynamic] Neuromuscular Control 2 [ST and GH] Functional 1 [ADL] Nature of Injury Healing Process Timing Wilhelm Roux Law of functional adaptation Mechanics (movement & position) Passive and Active Stability Associated Injuries Protection and Healing ROM 1 and Muscle activation [static isometric] Neuromuscular Control 1 [postural] Shoulder Rehabilitation RoadMap Governing Factors in Rehabilitation progression Acute Stage (Inflammatory Reaction) Management Guidelines Motor Tasks Taxonomy [Gentile 2000] Characteristic (< 7days unless insult is perpetuated) Vascular reaction Exudation of cells and chemicals Clot formation Phagocytic, neutralization of irritants Early fibroblastic activity Goals Provide reassurance and understanding Control the effects of inflammation Maintain soft tissue and joint integrity Maintain function of associated areas (ROM, Muscle performance, Circulation, Function) The initial inflammatory response is critical to the entire healing process. If this response does not accomplish what it is suppose to or if it does not subside, normal healing cannot take place. Any movement tolerated at this stage is beneficial, but it must not increase the inflammation or pain. Stretching and resistance exercises should not be performed over the lesion site. Active movement is usually contraindicated. In an injured structure that is not rested and is subjected to unnecessary external stress and strains, the healing process will never really get a chance to begin. 5
6 Subacute Stage (Repair and Healing) Management Guidelines Characteristics (2 3 weeks after injury, up to 6 weeks in tissue with limited circulation) Decreasing or absent of inflammation Removal of noxious stimuli Angiogenesis Exudate replacement by collagen formation Tissue granulation Myofibroblastic activity Goals Encourage patient to return to normal activities that do not exacerbate the symptoms. Help them to adapt to their work and recreational activities. Monitor healing tissue response to exercise Restore soft tissue, muscle and joint mobility and flexibility Develop neuromuscular control, strength and endurance (including proper mechanics) Wound closure takes 5 to 8 days in muscle and skin and up to 6 weeks in tendons and ligaments. Exercises and activities should be within the tolerance of the healing tissues. (non-destructive motion) Criteria for initiating active exercises and stretching include decreased swelling, intermittent pain and pain that are not exacerbated by motion in the available range. During this stage, the immature connective tissue is thin and unorganized. Yet proper growth and alignment can be stimulated by appropriate tensile loading in the line of normal stress of the tissue. Patient response is the best guide to how quickly or vigorously to progress. Any abnormal response might be the sign of chronic inflammation and intensity of exercises should be tuned-down. Muscle weakness will set in even in the absence of muscle pathology because of restricted use of the injured region. Be certain patient is using the correct motor pattern without substitution. Chronic Stage (Maturation and Remodeling) Management Guidelines Characteristic (up to 6 months and continues ) No inflammatory sign Balance between synthesis and degradation of collagen Collagen oriented and increase in tensile strength in response to stresses placed on them Adhesions and contractures Goals Instruct patient in biomechanically safe progression of resistance and stretching exs and how to monitor for signs of excessive stress. Increase soft tissue, muscle and joint mobility including joint play. Improve neuromuscular control, strength and endurance. Improve cardiovascular endurance. Progress functional activities. 6
7 Immature collagen molecules are held together with hydrogen bonding and can be easily remodeled in response to the stresses placed for up to 10 weeks with gentle but persistent treatment. At 14 weeks, the scar tissue has changed to covalent bonding and is unresponsive to remodeling. Treatment under these conditions requires either adaptive lengthening in the tissue surrounding the scar or surgical release. The progressively increasing in tensile quality may continue for 12 to 18 months. It is important to use controlled forces that duplicate the normal stresses on the tissue. Joint motion without adequate muscle support causes trauma to the joint as proposed by Zohn and Mennell, who recommended a muscle test grade of 4 in LL musculature before discontinuing use of assistive devices for ambulation. Joint dynamics, muscle strength and flexibility should be balanced. Soreness that does not decrease after 4 hours and is not resolved after 24 hours. Pain that comes on earlier or is increased over the previous session. Progressive stiffness and decrease in ROM. Inflammatory signs. Progressive weakness. Decreased in functional usage. McKenzie Traffic Light Procedure If symptom increase RED Light STOP If symptom unclear but not worse AMBER Light Try a little bit further If symptom improve GREEN Light Move On Monitoring Signs Monitoring System Ensuring Safety Protect athlete from further harm/danger Keep the athlete calm Athlete Positioning Comfortable and injured part supported. For seriously injured athlete, only move unless is necessary Equipment Removal Only remove if it will not cause further injury, use proper cutter if needed Before Injury Assessment In The Field 7
8 R.I.C.E, P.R.I.C.E, P.O.L.I.C.E, P.R.I.C.E.M.M. Only 5% level 1 evidence. Based on expert opinion and clinical reasoning. In The Field Formula for Treatments? High cost incur for ACL injuries in overseas. Only 53% of the patient return back to sport post trauma 3 4 years (Kvist 2005) 94% of football players went back to sport within a year. Probable reasons for the above rehab / conditioning lack: Failure to mimic the complexity of the sport movements during rehab. Condition in rehabilitation is over controlled. Gap between the rehab knowledge and athletic expertise Outcome measures are not up to the athletic level. What is the nature of the sport? How would you judge the current level of practice / training in compare to the pre-injury level? How appropriate with the outcome measures used in relation to the sport before discharging from training / conditioning / rehab? How do you feel during the first practice / competition and why so? Has the rehabilitation brought patient back to the normal practice routine? Questions to Ponder in Sports Rehab Questions to Ponder in Sports Rehab Kisner C, Colby LA (2007), Soft Tissue Injury, Repair and Management: Chapter 10, in Kisner C, Therapeutic Exercise Foundation and Techniques (5 th Edition, pp ), USA, F.A. Davis Company Robert FD, Melissa CE (2004), Wound Healing: An Overview of Acute, Fibrotic and Delayed Healing. Frontiers in Bioscience (9), pp , Virginia US Martini FH (2006), The Tissue Level of Organization: Chapter 4, in Fundamentals of Anatomy and physiology (7 th Edition, pp ), USA, Pearson Cummings Spector TD, Axford JS (1999), Healing and Repair: Chapter 15, in An Introduction to General Pathology (4 th Edition, pp ), Churchill Livingstone Bleakley CM (2013), Acute Soft Tissue Injury Management: Past, resent and Future. Physical Therapy in Sort 14 (2013), 73 74, Elsevier UK Suun A et al (2010), Introduction to Sort Injuries Management: Chapter 1, in Sorts Injuries, pp 1 6, Open University Malaysia, Meteor Doc PEtty NJ, Moore AP (2001), Subjective and Physical Examination: Chapter 2 3, in Neuromusculoskeletal Examination nd Assessment A Handbook for Therapist, (2 th Edition, pp ), Churchill Livingstone Dr Arshad Puji, Sport Physician, ASIU, Orthopedic Institute HKL Dr Goh Siew Li, Sport Physician, ASIU, Orthopedic Institute HKL Dr Siti Hawa, Orthopedic Surgeon ASIU, Orthopedic Institute HKL Dr Bazam, Orthopedic Surgeon, ASIU, Orthopedic Institute HKL Mr Zahari Afandi, Sport Physiotherapist, Physiotherapy Department HKL References 8
Treatment, Rehabilitation and Reconditioning Physiology of Tissue Repair
 Treatment, Rehabilitation and Reconditioning Physiology of Tissue Repair PHYSIOLOGY OF TISSUE REPAIR Knowing when it is appropriate to begin rehabilitation and when it is acceptable to return to practice
Treatment, Rehabilitation and Reconditioning Physiology of Tissue Repair PHYSIOLOGY OF TISSUE REPAIR Knowing when it is appropriate to begin rehabilitation and when it is acceptable to return to practice
McKenzie Extremity Talk.
 McKenzie Extremity Talk www.fisiokinesiterapia.biz New Zealand Physical Therapist Robin McKenzie Robin McKenzie was made an Officer of the Most Excellent Order of the British Empire in 1990 and appointed
McKenzie Extremity Talk www.fisiokinesiterapia.biz New Zealand Physical Therapist Robin McKenzie Robin McKenzie was made an Officer of the Most Excellent Order of the British Empire in 1990 and appointed
9/14/16 PHASES OF HEALING. Mandatory Knowledge LEARNING OBJECTIVE. Understand Phases of Healing in Musculoskeletal Trauma
 Mandatory Knowledge LEARNING OBJECTIVE Understand Phases of Healing in Musculoskeletal Trauma LEARNING OBJECTIVE Apply Phases of Healing knowledge in the evaluation and treatment of musculoskeletal complaints
Mandatory Knowledge LEARNING OBJECTIVE Understand Phases of Healing in Musculoskeletal Trauma LEARNING OBJECTIVE Apply Phases of Healing knowledge in the evaluation and treatment of musculoskeletal complaints
HIGH PERFORMANCE CENTRE FOR SPORTS RECOVERY
 HIGH PERFORMANCE CENTRE FOR SPORTS RECOVERY EDMONTON BREWERY DISTRICT DOWNTOWN Edmonton s First Boutique Physiotherapy Clinic WHAT SETS US APART? NO ATHLETE IS TRULY TESTED UNTIL THEY VE STARED INJURY
HIGH PERFORMANCE CENTRE FOR SPORTS RECOVERY EDMONTON BREWERY DISTRICT DOWNTOWN Edmonton s First Boutique Physiotherapy Clinic WHAT SETS US APART? NO ATHLETE IS TRULY TESTED UNTIL THEY VE STARED INJURY
ULNAR COLLATERAL LIGAMENT (UCL) RECONSTRUCTION REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Sprains. Initially the ankle is swollen, painful, and may turn eccyhmotic (bruised). The bruising, and the initial swelling, is due to ruptured
 Sprains Introduction An ankle sprain is a common injury and usually results when the ankle is twisted, or inverted. The term sprain signifies injury to the soft tissues, usually the ligaments, of the ankle.
Sprains Introduction An ankle sprain is a common injury and usually results when the ankle is twisted, or inverted. The term sprain signifies injury to the soft tissues, usually the ligaments, of the ankle.
Trauma and Immobilization SCAR. Summary: Acute Inflammation & Healing. TRAUMA Wound Healing: Three Phases
 Upper Extremity Stiffness and Contracture After Trauma Phil PT, PhD, FAPTA mcclure@arcadia.edu Trauma and Immobilization SCAR TRAUMA Wound Healing: Three Phases Inflammation (0-5 days) Fibroplasia (Repair,
Upper Extremity Stiffness and Contracture After Trauma Phil PT, PhD, FAPTA mcclure@arcadia.edu Trauma and Immobilization SCAR TRAUMA Wound Healing: Three Phases Inflammation (0-5 days) Fibroplasia (Repair,
Objectives. Sprains, Strains, and Musculoskeletal Maladies. Sprains. Sprains. Sprains. Physical Exam 5/5/2010
 Objectives, Strains, and Musculoskeletal Maladies Robert Hosey, MD University of Kentucky Sports Medicine Define sprains and strains Systematically evaluate and manage joint / muscle injuries When to refer
Objectives, Strains, and Musculoskeletal Maladies Robert Hosey, MD University of Kentucky Sports Medicine Define sprains and strains Systematically evaluate and manage joint / muscle injuries When to refer
Foot and ankle. Achilles tendon rupture repair. After surgery
 Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
SHOULDER ARTHROSCOPY WITH ANTERIOR STABILIZATION / CAPSULORRHAPHY REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Shoulder Arthroscopy with Rotator Cuff Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
KNEE INJURIES IN SPORTS MEDICINE
 KNEE INJURIES IN SPORTS MEDICINE Irving Raphael, MD June 13, 2014 RSM Medical Associates Head Team Physician Syracuse University Outline Meniscal Injuries anatomy Exam Treatment ACL Injuries Etiology Physical
KNEE INJURIES IN SPORTS MEDICINE Irving Raphael, MD June 13, 2014 RSM Medical Associates Head Team Physician Syracuse University Outline Meniscal Injuries anatomy Exam Treatment ACL Injuries Etiology Physical
Vivekananda University Free Lance Language Editor. Ghoshal
 C14 M 6.1: Introduction and Classification of Therapeutic Exercise Role Name Affiliation Principal Investigator Dr. Asis Goswami Ramakrishna Mission Vivekananda University Co-Principal Investigator Dr.
C14 M 6.1: Introduction and Classification of Therapeutic Exercise Role Name Affiliation Principal Investigator Dr. Asis Goswami Ramakrishna Mission Vivekananda University Co-Principal Investigator Dr.
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Robert Klitzman
 Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Robert Klitzman This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Robert Klitzman This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
ACL Rehabilitation and Return To Play
 ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
August 12, Sports Med Critical Question 4.notebook. Critical Question 4. How is injury rehabilitation managed?
 Critical Question 4 How is injury rehabilitation managed? 1 2 Syllabus 3 Big Heading: Critical Questions 4: How is injury rehabilitation managed Heading: Rehabilitation Procedures Rehabilitation after
Critical Question 4 How is injury rehabilitation managed? 1 2 Syllabus 3 Big Heading: Critical Questions 4: How is injury rehabilitation managed Heading: Rehabilitation Procedures Rehabilitation after
Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab
 1 Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab Thomas Clennell, PT, DPT, SCS Physical Therapist UCSF Benioff Children s Hospital Oakland Sports Medicine
1 Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab Thomas Clennell, PT, DPT, SCS Physical Therapist UCSF Benioff Children s Hospital Oakland Sports Medicine
Shoulder Arthroscopy with Posterior Labral Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Anterior Cruciate Ligament Injuries
 Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
ACL REHABILITATION. Key to Success
 ACL REHABILITATION The overall rehabilitation plan emphasises the importance of pre-operative exercises followed post operatively by early control of swelling and regaining full extension (straightening)
ACL REHABILITATION The overall rehabilitation plan emphasises the importance of pre-operative exercises followed post operatively by early control of swelling and regaining full extension (straightening)
Dr. Huff Modified Brostrom Repair Rehabilitation Protocol:
 Dr. Huff Modified Brostrom Repair Rehabilitation Protocol: The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient who has undergone
Dr. Huff Modified Brostrom Repair Rehabilitation Protocol: The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient who has undergone
Acute Injuries. Learning Objectives. 1. Definition
 Acute Injuries Learning Objectives 1. Distinguish between intrinsic and 2. List the major acute injuries according to tissue type 3. Discuss common examples of how acute injuries present - GP role 4. Preview
Acute Injuries Learning Objectives 1. Distinguish between intrinsic and 2. List the major acute injuries according to tissue type 3. Discuss common examples of how acute injuries present - GP role 4. Preview
A Patient s Guide to Elbow Dislocation
 A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL. WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches.
 REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
Rehabilitation Guidelines for Large Rotator Cuff Repair
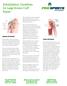 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Following Unilateral Patellar Tendon Repair
 Rehabilitation Following Unilateral Patellar Tendon Repair I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate
Rehabilitation Following Unilateral Patellar Tendon Repair I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
9180 KATY FREEWAY, STE. 200 (713)
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Achilles Tendonitis and Tears
 Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
Chinese Proverb. He who asks a question is a fool for five minutes; he who does not ask a question remains a fool forever. What do we Fix?
 Robert H. Rowe, PT, DPT, DMT, MHS, FAAOMPT Director Brooks Institute of Higher Learning Chinese Proverb He who asks a question is a fool for five minutes; he who does not ask a question remains a fool
Robert H. Rowe, PT, DPT, DMT, MHS, FAAOMPT Director Brooks Institute of Higher Learning Chinese Proverb He who asks a question is a fool for five minutes; he who does not ask a question remains a fool
Anterior Cruciate Ligament Reconstruction Delayed Rehab Protocol
 Anterior Cruciate Ligament Reconstruction Delayed Rehab Protocol Clarkstown Division This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction with other surgical
Anterior Cruciate Ligament Reconstruction Delayed Rehab Protocol Clarkstown Division This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction with other surgical
Anterior Cruciate Ligament (ACL) Reconstruction- Delayed Rehabilitation Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Cruciate Ligament (ACL) Reconstruction- Delayed Rehabilitation Protocol This rehabilitation
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Cruciate Ligament (ACL) Reconstruction- Delayed Rehabilitation Protocol This rehabilitation
dressing, immobilization most commonly avoided or neglected after spraining injuries, puncture, pharmacotherapy and physiotherapy, rehabilitation.
 Many people take up physical exercises, often excessing their efficiency and soft tissue endurance, due to living in a hurry, lack of motoric ativity and esthetic standards of the world today. In addition,
Many people take up physical exercises, often excessing their efficiency and soft tissue endurance, due to living in a hurry, lack of motoric ativity and esthetic standards of the world today. In addition,
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the
 The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
An Introduction to Scandinavian Mobilization Therapy
 An Introduction to Scandinavian Mobilization Therapy Page 1 Definition Scandinavian Mobilization Therapy is based upon Contemporary Naprapathic Manual Medicine, therapeutic passive exercise, and the American
An Introduction to Scandinavian Mobilization Therapy Page 1 Definition Scandinavian Mobilization Therapy is based upon Contemporary Naprapathic Manual Medicine, therapeutic passive exercise, and the American
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL ARTHROSCOPIC SLAP LESION REPAIR (TYPE II) BENJAMIN J. DAVIS, MD
 I. Phase I Immediate Postoperative Phase Restrictive Motion (Day 1 to Week 6) Goals: Protect the anatomic repair Prevent negative effects of immobilization Promote dynamic stability Diminish pain and inflammation
I. Phase I Immediate Postoperative Phase Restrictive Motion (Day 1 to Week 6) Goals: Protect the anatomic repair Prevent negative effects of immobilization Promote dynamic stability Diminish pain and inflammation
Location of Pain/Symptoms Where do you feel the pain/symptoms? Can you point with one finger to location of pain? Is the pain general or localized?
 Injury Evaluation History A complete and accurate medical history is one of the most important and useful parts of the clinical examination. A complete history consists of past history and a history of
Injury Evaluation History A complete and accurate medical history is one of the most important and useful parts of the clinical examination. A complete history consists of past history and a history of
COMMON KNEE AND SHOULDER INJURIES IN THE YOUNG ATHLETE. Outline 5/11/2017
 COMMON KNEE AND SHOULDER INJURIES IN THE YOUNG ATHLETE IRVING RAPHAEL MD Syracuse Orthopedic Specialists Former S.U. Head Team Physician May 19, 2017 Meniscal Injuries anatomy Exam Treatment ACL Injuries
COMMON KNEE AND SHOULDER INJURIES IN THE YOUNG ATHLETE IRVING RAPHAEL MD Syracuse Orthopedic Specialists Former S.U. Head Team Physician May 19, 2017 Meniscal Injuries anatomy Exam Treatment ACL Injuries
Patellar Tendon Repair Rehabilitation Guideline
 Patellar Tendon Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Patellar Tendon Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
CERVICAL STRAIN AND SPRAIN (Whiplash)
 CERVICAL STRAIN AND SPRAIN (Whiplash) Description time and using proper technique decrease the frequency of Whiplash is an injury to the neck caused when it is forcefully whipped or forced backward or
CERVICAL STRAIN AND SPRAIN (Whiplash) Description time and using proper technique decrease the frequency of Whiplash is an injury to the neck caused when it is forcefully whipped or forced backward or
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Sprained Ankle An ankle sprain occurs when the strong ligaments that support the ankle stretch beyond their limits and tear. Ankle sprains are common injuries that occur among people of all ages. They
Sprained Ankle An ankle sprain occurs when the strong ligaments that support the ankle stretch beyond their limits and tear. Ankle sprains are common injuries that occur among people of all ages. They
CERVICAL STRAIN AND SPRAIN
 CERVICAL STRAIN AND SPRAIN Description Cervical strain/sprain is an injury to the neck caused when it is forcefully whipped or forced backward or forward. The structures involved are the muscles, ligaments,
CERVICAL STRAIN AND SPRAIN Description Cervical strain/sprain is an injury to the neck caused when it is forcefully whipped or forced backward or forward. The structures involved are the muscles, ligaments,
Athletic Preparation ACL Reconstruction - Accelerated Rehabilitation. Autologous Bone-Tendon-Bone, Patella Tendon Graft
 Orthopaedic Sports Specialists, P.C. Michael E. Joyce, M.D. 84 Glastonbury Blvd., Suite 101, Glastonbury, Connecticut 06033 Voice: 860-652-8883, Fax: 860-652-8887 Athletic Preparation ACL Reconstruction
Orthopaedic Sports Specialists, P.C. Michael E. Joyce, M.D. 84 Glastonbury Blvd., Suite 101, Glastonbury, Connecticut 06033 Voice: 860-652-8883, Fax: 860-652-8887 Athletic Preparation ACL Reconstruction
UNIT 2.- SPORT INJURIES: SYMPTOMS AND TREATMENT
 UNIT 2.- SPORT INJURIES: SYMPTOMS AND TREATMENT Every year, millions of teenagers participate in high school sports. An injury to a high school athlete can be a significant disappointment for the teen,
UNIT 2.- SPORT INJURIES: SYMPTOMS AND TREATMENT Every year, millions of teenagers participate in high school sports. An injury to a high school athlete can be a significant disappointment for the teen,
When are athletes ready for return to sports??? Functional Testing for Return to Sports. Important Factors Involved in Return to Sport
 Functional Testing for Return to Sports Meg Jacobs PT Momentum Physical Therapy and Sports Rehab Mjacobs@wegetyouhealthy.com When are athletes ready for return to sports??? Post ACL reconstruction, average
Functional Testing for Return to Sports Meg Jacobs PT Momentum Physical Therapy and Sports Rehab Mjacobs@wegetyouhealthy.com When are athletes ready for return to sports??? Post ACL reconstruction, average
Superior Labrum Repair Protocol - SLAP
 Superior Labrum Repair Protocol - SLAP Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain
Superior Labrum Repair Protocol - SLAP Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain
Ankle instability surgery
 Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Latarjet Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
Site: College of Rehabilitation Sciences Department of Physical Therapy NEUROMUSCULOSKELETAL CLINICAL SKILLS CHECKLIST
 Name: Site: College of Rehabilitation Sciences Department of Physical Therapy NEUROMUSCULOSKELETAL CLINICAL SKILLS CHECKLIST ASSESSMENT PROCESS / TECHNIQUE Opportunity to review and integrate A. Information
Name: Site: College of Rehabilitation Sciences Department of Physical Therapy NEUROMUSCULOSKELETAL CLINICAL SKILLS CHECKLIST ASSESSMENT PROCESS / TECHNIQUE Opportunity to review and integrate A. Information
Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521 DISTAL BICEPS TENDON REPAIR PROTOCOL This rehabilitation protocol
Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521 DISTAL BICEPS TENDON REPAIR PROTOCOL This rehabilitation protocol
Rehabilitation Guidelines for Shoulder Arthroscopy
 Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
BANKART REPAIR PROTOCOL
 BANKART REPAIR PROTOCOL Clarkstown Division This rehabilitation protocol has been developed for the patient following Bankart surgical procedure for anterior shoulder instability. The protocol is divided
BANKART REPAIR PROTOCOL Clarkstown Division This rehabilitation protocol has been developed for the patient following Bankart surgical procedure for anterior shoulder instability. The protocol is divided
These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at if you have any questions.
 OSU Sports Medicine Knee Microfracture Rehabilitation Guidelines These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at 614-293-2385 if you have any questions. Rehabilitation
OSU Sports Medicine Knee Microfracture Rehabilitation Guidelines These are rehabilitation guidelines for OSU Sports Medicine patients. Please contact us at 614-293-2385 if you have any questions. Rehabilitation
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline
 Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Key words: Laser, sprain, strain, lameness, tendon
 MLS Master Class - Veterinary Imaging Presented by CelticSMR Ltd Free Phone (UK): 0800 279 9050 International: +44 (0) 1646 603150 AUTHOR DETAILS Carl Gorman BVSc MRCVS PUBLISHER DETAILS Mike Howe B Vet
MLS Master Class - Veterinary Imaging Presented by CelticSMR Ltd Free Phone (UK): 0800 279 9050 International: +44 (0) 1646 603150 AUTHOR DETAILS Carl Gorman BVSc MRCVS PUBLISHER DETAILS Mike Howe B Vet
Post-op / Pre-op Page (ALREADY DONE)
 Post-op / Pre-op Page (ALREADY DONE) We offer individualized treatment plans based on your physician's recommendations, our evaluations, and your feedback. Most post-operative and preoperative rehabilitation
Post-op / Pre-op Page (ALREADY DONE) We offer individualized treatment plans based on your physician's recommendations, our evaluations, and your feedback. Most post-operative and preoperative rehabilitation
A Patient s Guide to Adult-Acquired Flatfoot Deformity
 A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
Arthroscopic Bankart Repair Rehabilitation Protocol Dr. Mark Adickes
 Arthroscopic Bankart Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following an arthroscopic Bankart (anteroinferior labral
Arthroscopic Bankart Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following an arthroscopic Bankart (anteroinferior labral
DOWNLOAD PDF ON-FIELD EVALUATION AND TREATMENT OF COMMON ATHLETIC INJURIES
 Chapter 1 : On Field Evaluation And Treatment Of Common Athletic Injuries, 1e Medical Books On Field Evaluation And Treatment Of Common Athletic Injuries, 1e Three of today's leading orthopedic specialists
Chapter 1 : On Field Evaluation And Treatment Of Common Athletic Injuries, 1e Medical Books On Field Evaluation And Treatment Of Common Athletic Injuries, 1e Three of today's leading orthopedic specialists
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
PROM is not stretching!
 Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Joshua D. Stein, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX (903)
 Joshua D. Stein, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX 75701 (903) 510-8840 Anterior Cruciate Ligament Reconstruction Delayed Rehab This rehabilitation protocol has
Joshua D. Stein, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX 75701 (903) 510-8840 Anterior Cruciate Ligament Reconstruction Delayed Rehab This rehabilitation protocol has
ARTHROSCOPIC SLAP LESION REPAIR (TYPE II) WITH THERMAL CAPSULAR SHRINKAGE
 ARTHROSCOPIC SLAP LESION REPAIR (TYPE II) WITH THERMAL CAPSULAR SHRINKAGE I. Phase I Immediate Postoperative Phase Restrictive Motion (Day 1 to Week 6) Goals: Protect the anatomic repair Prevent negative
ARTHROSCOPIC SLAP LESION REPAIR (TYPE II) WITH THERMAL CAPSULAR SHRINKAGE I. Phase I Immediate Postoperative Phase Restrictive Motion (Day 1 to Week 6) Goals: Protect the anatomic repair Prevent negative
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol
 Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Clarkstown Division This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Clarkstown Division This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning
KNEE REHABILITATION PROGRAMME. Patient Information & Exercise Folder
 KNEE REHABILITATION PROGRAMME Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon BOSTONIAN PRIVATE WING Pilgrim Hospital, Boston Lincolnshire PE21
KNEE REHABILITATION PROGRAMME Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon BOSTONIAN PRIVATE WING Pilgrim Hospital, Boston Lincolnshire PE21
Anterior Cruciate Ligament (ACL) Reconstruction Hamstring Graft/PTG-Accelerated Rehabilitation Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Cruciate Ligament (ACL) Reconstruction Hamstring Graft/PTG-Accelerated Rehabilitation
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Cruciate Ligament (ACL) Reconstruction Hamstring Graft/PTG-Accelerated Rehabilitation
Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521 ELBOW S/P LOOSE BODY REMOVAL PROTOCOL This rehabilitation protocol
Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521 ELBOW S/P LOOSE BODY REMOVAL PROTOCOL This rehabilitation protocol
Acute Low Back Pain. North American Spine Society Public Education Series
 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
3rd MuscleTech Network Workshop. Muscle injuries and repair: Current trends in research.
 3rd MuscleTech Network Workshop. Muscle injuries and repair: Current trends in research. CONCLUSIONS AND CLOSING REMARKS Dr. Carles Pedret MUSCLE AND TENDON WORKSHOP HEALTH AND GENERAL POPULATION SPORTS
3rd MuscleTech Network Workshop. Muscle injuries and repair: Current trends in research. CONCLUSIONS AND CLOSING REMARKS Dr. Carles Pedret MUSCLE AND TENDON WORKSHOP HEALTH AND GENERAL POPULATION SPORTS
A Patient s Guide to Trochanteric Bursitis of the Hip
 A Patient s Guide to Trochanteric Bursitis of the Hip Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
A Patient s Guide to Trochanteric Bursitis of the Hip Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can
Rehabilitation of an ACL injury in a 29 year old male with closed kinetic chain exercises: A case study
 Abstract Objective: This paper will examine a rehabilitation program for a healthy 29 year old male who sustained an incomplete tear of the left ACL. Results: Following a 9 week treatment plan focusing
Abstract Objective: This paper will examine a rehabilitation program for a healthy 29 year old male who sustained an incomplete tear of the left ACL. Results: Following a 9 week treatment plan focusing
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Stephanie Gould Pht, Naudira Stewart P.R.T. i000
 Return to Sport After ACL in the Young Athlete Stephanie Gould Pht, Naudira Stewart P.R.T i000 The ACL epidemic In youth aged 6-18 y.o., ACL injuries occur at a rate of 130/100,000 people per year Rate
Return to Sport After ACL in the Young Athlete Stephanie Gould Pht, Naudira Stewart P.R.T i000 The ACL epidemic In youth aged 6-18 y.o., ACL injuries occur at a rate of 130/100,000 people per year Rate
Introduction. Anatomy
 the patella is called the quadriceps mechanism. Though we think of it as a single device, the quadriceps mechanism has two separate tendons, the quadriceps tendon on top of the patella and the patellar
the patella is called the quadriceps mechanism. Though we think of it as a single device, the quadriceps mechanism has two separate tendons, the quadriceps tendon on top of the patella and the patellar
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Sprains and Strains. The Medical Disability Advisor: Workplace Guidelines for Disability Duration
 Sample Topic Sprains and Strains The Medical Disability Advisor: Workplace Guidelines for Disability Duration Fifth Edition Presley Reed, MD Editor-in-Chief The Most Widely-Used Duration Guidelines in
Sample Topic Sprains and Strains The Medical Disability Advisor: Workplace Guidelines for Disability Duration Fifth Edition Presley Reed, MD Editor-in-Chief The Most Widely-Used Duration Guidelines in
Principles of Treatment. Case Studies. Principles of Treatment. Clinical Perspectives for the GP
 Principles of Treatment Clinical Perspectives for the GP Case Studies 1. Jumping athlete with an acute exacerbation of chronic patellar tendinopathy major competition in 9 days time 2 week tournament 2.
Principles of Treatment Clinical Perspectives for the GP Case Studies 1. Jumping athlete with an acute exacerbation of chronic patellar tendinopathy major competition in 9 days time 2 week tournament 2.
Shoulder Arthroscopy: Postop Instructions. Activites & Advice for in the Hospital and while at Home
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
Proximal Hamstring Rupture: Physical Therapy Protocol
 Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment.
Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment.
Anterior Cruciate Ligament (ACL) Tears
 WASHINGTON UNIVERSITY ORTHOPEDICS Anterior Cruciate Ligament (ACL) Tears Knowing what to expect for ACL surgery is key for a healthy surgery and recovery. Our sports medicine specialists are committed
WASHINGTON UNIVERSITY ORTHOPEDICS Anterior Cruciate Ligament (ACL) Tears Knowing what to expect for ACL surgery is key for a healthy surgery and recovery. Our sports medicine specialists are committed
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 ROTATOR CUFF REPAIR PROTOCOL This rehabilitation protocol has been
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 ROTATOR CUFF REPAIR PROTOCOL This rehabilitation protocol has been
REGENETEN Bioinductive Implant. Rehabilitation Protocol. for REGENETEN partial thickness tears without repair
 REGENETEN Bioinductive Implant Rehabilitation Protocol for REGENETEN partial thickness tears without repair Let s get you back to YOU. We must emphasize that this protocol is recommended ONLY for partial
REGENETEN Bioinductive Implant Rehabilitation Protocol for REGENETEN partial thickness tears without repair Let s get you back to YOU. We must emphasize that this protocol is recommended ONLY for partial
Type II SLAP lesions are created when the biceps anchor has pulled away from the glenoid attachment.
 Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Chapter 16: Using Therapeutic Exercise in Rehabilitation
 Chapter 16: Using Therapeutic Exercise in Rehabilitation Athletic Trainer s Approach to Rehabilitation Begins immediately after injury Initial first aid has a substantial impact on the injury One of ATC
Chapter 16: Using Therapeutic Exercise in Rehabilitation Athletic Trainer s Approach to Rehabilitation Begins immediately after injury Initial first aid has a substantial impact on the injury One of ATC
Bunion (hallux valgus deformity) surgery
 Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Hands on Sports Therapy KNOWLEDGE REVIEW QUESTIONS 2004 Thomson Learning. Q1: What are the main areas of focus in the field of sports injuries?
 CHAPTER 05 Knowledge Review Q1: What are the main areas of focus in the field of sports injuries? A1: The 4 main areas of sports injury management are: aetiology [causes]; assessment and diagnosis; treatment
CHAPTER 05 Knowledge Review Q1: What are the main areas of focus in the field of sports injuries? A1: The 4 main areas of sports injury management are: aetiology [causes]; assessment and diagnosis; treatment
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations
 SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
Latissimus dorsi tendon transfer protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the physical therapist with a guideline/treatment protocol for the postoperative rehabilitation management
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the physical therapist with a guideline/treatment protocol for the postoperative rehabilitation management
Anterior Cruciate Ligament (ACL)
 Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
ACL Reconstruction Protocol (Allograft)
 ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
