PfP Quality Metrics: Readmissions, Value-Based Purchasing and Beyond
|
|
|
- Allyson Weaver
- 5 years ago
- Views:
Transcription
1 PfP Quality Metrics: Readmissions, Value-Based Purchasing and Beyond Presented to ASHNHA Alaska Partnership for Patients Advisory Group February 4, 2015 Gloria Kupferman
2 Readmissions Calculation methods Agenda 3M compared to Medicare (CMS) Sample reporting tool Medicare Value-Based Purchasing Maintaining PfP momentum with data collection and reporting
3 Readmissions
4 What is a Readmission? A readmission is a return hospitalization to an acute care hospital that follows a prior admission from an acute care hospital within the specified readmission time interval The time interval can vary depending upon the purpose of the review Many methodologies exist to identify and quantify readmissions
5 Methodologies 3M Potentially Preventable Readmissions Some States Medicaid Penalties CMS Hospital Readmissions Reduction Program Hospital-Level 30-Day Risk-Standardized Readmission Measures for specific conditions AMI, HF, PNEU, COPD, THA/TKA, CABG Readmissions in the BPCI and ACO Initiatives Others developed by QIOs, health departments, etc.
6 3M PPR Methodology
7 3M PPR Methodology Index admissions and readmissions for conditions that are not considered preventable are globally excluded e.g. major or metastatic malignancies, multiple trauma and burns, etc. Some admissions are considered non-events and are considered at risk admissions e.g. same day transfer to an acute care hospital for non-acute care, etc.
8 Observed PPR Rate
9 Expected PPR Rate
10 Observed to Expected Ratio
11 Overview of the Current CMS Methodology All-cause readmissions Current focus areas Heart Failure (HF) patients Heart Attack (AMI) patients Pneumonia (PN) patients Chronic Obstructive Pulmonary Disease (COPD) Total hip and knee replacements (THA/TKA) CABG in FFY 2017 What hospitals are included? All acute care PPS hospitals CAHs are exempt Hospital must have 25 discharges within a disease category over the 3 year reporting period
12 Inclusions Medicare Fee-for-Service patients, at least 65 years of age, with a principal diagnosis of AMI, HF, or PN 12 full months of enrollment in parts A and B FFS prior to the index admission FFS Medicare Part A at the time of the index admission One full month of enrollment in Parts A and B FFS post discharge
13 Exclusions Incomplete Medicare enrollment data Under age 65 Length of stay greater than one year Discharged against medical advice In hospital deaths Transfers out Same day readmissions for the same condition to the same hospital Disease category specific exclusions Some recognition of planned readmissions
14 Risk Adjustment Methodology Developed by a team of clinical and statistical experts from Yale and Harvard universities Each disease category has an individual risk adjustment model Adjust for variables that are clinically relevant and have strong relationships with the outcome Demographics, disease severity indicators, indicators of frailty Example for HF: age, sex, history of CABG, cancer, diabetes, asthma, COPD, pneumonia, renal failure, etc.
15 Risk Standardized Readmission Rate (RSRR) RSRR= Predicted Rate National Expected Rate Unadjusted Rate Predicted Rate (similar to observed rate) the number of readmissions within 30 days predicted on the basis of the hospital's performance with its observed case mix Expected Rate the number of readmissions expected on the basis of the nation s performance (US average hospital performance) with that hospital s case mix.
16 Predicted to Expected Ratio P/E less than 1 = Lower than expected readmission rate Better quality, no penalty P/E greater than 1= Higher than expected readmission rate Lower quality, subject to penalty
17 Live Tour Readmissions Diagnostic Tool 17
18 Takeaways You can t evaluate and address issues without data You need an analytic tool that can identify and track readmissions Let the CMO, Dept. Chairs, Nurse Leads... Play with it Formally analyze Provide feedback Share with MD/RN and other key clinicians Use for focus groups... What goes well and where are the opportunities
19 Medicare Value-Based Purchasing
20 Value-Based Purchasing Overview Mandated by the ACA The only Medicare quality program that actually rewards good performance Funded by Medicare payment carve-outs Complex scoring methodology looks at quality metrics in several domains Scores reflect performance compared to national standards and individual improvement Domains, metrics and standards change annually
21 General VBP Program Trends Continuously evolving program Program rules established well in advance Increasing program exposure Increasing weight towards Outcomes & Efficiency Measures Domain Weight 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% 30% 25% 20% 25% 70% 45% 30% 20% 30% 30% 10% 25% 40% 25% 25% 5% 20% 25% Program Contribution Amount 2.00% 1.75% 1.50% 1.25% 1.00% 0.75% 0.50% 0.25% 0.00%
22 FFY 2015 VBP Program Overview 1.5% program contribution Outcomes domain measure expansion PSI-90 Safety Indicator Composite CLABSI Standardized Infection Ratio New Efficiency Domain SPP_1 (Medicare Spending Per Beneficiary) Overlap with FFY 2015 HAC Reduction Program PSI-90 Composite CLABSI 30% 20% Process Domain Patient Experience Domain 30% 20% Patient Outcomes Domain Efficiency Domain
23 FFY 2015 VBP Program Overview First Year of Proportional Reweighting Impacts program eligibility Process Domain Unweighted Domain Score Original Domain Weight Proportionally Reweighted Domain Weight * 63.33% 20.00% 28.57% 29% Process Domain Patient Experience Domain Patient Experience Domain Patient Outcomes Domain 96.00% 30.00% 42.86% Not Eligible 30.00% Not Elgible 43% 29% Patient Outcomes Domain Efficiency Domain 90.00% 20.00% 28.57% Efficiency Domain Hospital Counts Scored on 2 Domains % Scored on 3 Domains % Scored on 4 Domains % Total Number of Insiders* % *Based on 4Q2013 DataGen Estimate
24 Tracking VBP Performance Measure and Domain Score Comparison FFY 2013 Program ACTUAL Performance Hospital FFY 2014 Program ACTUAL Performance Hospital FFY 2015 Program ESTIMATED Performance VBP Measure Score VBP Measure Score Hospital Performance VBP Measure Score Performance Performance Program Eligibility Eligible Eligible Projected to be Eligible AMI-7a N/A N/A N/A N/A N/A N/A AMI-8a N/A N/A 100.0% % 6 HF % % % 6 PN-3b 100.0% % % 10 PN % % % 10 SCIP-Inf % % % 10 Process of Care SCIP-Inf % % % 10 SCIP-Inf % % % 10 SCIP-Inf-4 N/A N/A N/A N/A N/A N/A SCIP-Inf-9 Measure Not Evaluated for VBP % % 6 SCIP-Card % % % 5 SCIP-VTE % % 10 Measure Not Evaluated for VBP 2015 SCIP-VTE % % % 10 Unweighted Domain Score 85.6% 93.6% 83.0% Patient Experience of Care Communication with Nurses % 1 Communication with Doctors % 0 Responsiveness of Hospital Staff % 0 Pain Management % 0 Not Provided By Not Provided By Communication about Medicines CMS 6 CMS % 3 Cleanliness and Quietness of Hospital Environment % 3 Discharge Information % 7 Overall Rating of Hospital % 2 HCAHPS Consistency Score Not Applicable 19 Unweighted Domain Score 51.0% 35.0% 35.0% Patient Outcomes MORT-30-AMI 85.0% 2 N/A N/A MORT-30-HF 85.8% % 0 Domain Not Evaluated MORT-30-PN for VBP % % 0 PSI Measure Not Evaluated for VBP 2014 HAI_1 N/A N/A Unweighted Domain Score 30.0% 0.0% Efficiency SPP_1 Domain Not Evaluated for VBP 2013 Domain Not Evaluated for VBP Unweighted Domain Score 100.0% Reweighting factor 1 TPS and Payment Impact Comparison FFY 2013 ACTUAL Program Performance Unweighted Domain X Domain Weight = FFY 2014 ACTUAL Program Performance Unweighted Domain X Domain Weight = FFY 2015 ESTIMATED Program Performance Unweighted Domain Score Process of Care Domain 85.6% X 70.0% = 59.9% 93.6% X 45.0% = 42.1% 83.0% X 20.0% = Patient Experience of Care Domain 51.0% X 30.0% = 15.3% 35.0% X 30.0% = 10.5% 35.0% X 30.0% = Patient Outcomes Domain 30.0% X 25.0% = 7.5% 0.0% X 30.0% = Not Applicable Efficiency Domain Not Applicable 100.0% X 20.0% = Weighted Score Weighted Score X Domain Weight = Weighted Score 16.6% 10.5% 0.0% 20.0% Total Performance Score (TPS) 75.2% 60.1% 47.1%
25 PfP Data Collection and Reporting
26 Maintain Momentum Sample data collection / reporting tool Sample summary workbook
27 Questions? Gloria Kupferman Vice President, DataGen
Mandatory Elements of Healthcare Reform Walter Coleman. healthcare consulting
 Mandatory Elements of Healthcare Reform Walter Coleman 1 Agenda ACA Mandatory Elements of Reform Value Based Purchasing Readmission Reduction Program Hospital Acquired Conditions Best practices to analyze
Mandatory Elements of Healthcare Reform Walter Coleman 1 Agenda ACA Mandatory Elements of Reform Value Based Purchasing Readmission Reduction Program Hospital Acquired Conditions Best practices to analyze
Medicare Value Based Purchasing Andrew B. Wheeler Vice President of Federal Finance
 Medicare Value Based Purchasing - 101 Andrew B. Wheeler Vice President of Federal Finance What is Medicare s VBP System? Incentive program to improve outcomes, safety, patient satisfaction, and efficiency
Medicare Value Based Purchasing - 101 Andrew B. Wheeler Vice President of Federal Finance What is Medicare s VBP System? Incentive program to improve outcomes, safety, patient satisfaction, and efficiency
Measure Applications Partnership. Hospital Workgroup In-Person Meeting Follow- Up Call
 Measure Applications Partnership Hospital Workgroup In-Person Meeting Follow- Up Call December 21, 2016 Feedback on Current Measure Sets for IQR, HACs, Readmissions, and VBP 2 Previously Identified Crosscutting
Measure Applications Partnership Hospital Workgroup In-Person Meeting Follow- Up Call December 21, 2016 Feedback on Current Measure Sets for IQR, HACs, Readmissions, and VBP 2 Previously Identified Crosscutting
2016 Hospital Measures
 2016 Hospital Measures Vicki Tang Olson, Stratis Health Statewide Quality Reporting and Measurement System (SQRMS) Annual Forum June 22, 2015 Objectives Share the process used for 2016 hospital measures
2016 Hospital Measures Vicki Tang Olson, Stratis Health Statewide Quality Reporting and Measurement System (SQRMS) Annual Forum June 22, 2015 Objectives Share the process used for 2016 hospital measures
CMS Hospital IQR Program Measure Comparison Tables FY 2018 (CY 2016) Measures Required to Meet Hospital IQR APU Requirements NHSN Submission
 CMS IQR Program Measure Comparison Tables (CY 2016) NHSN Submission CLABSI Central Line-Associated Bloodstream Infection (CLABSI) Required NHSN CAUTI Catheter-Associated Urinary Tract Infection (CAUTI)
CMS IQR Program Measure Comparison Tables (CY 2016) NHSN Submission CLABSI Central Line-Associated Bloodstream Infection (CLABSI) Required NHSN CAUTI Catheter-Associated Urinary Tract Infection (CAUTI)
Appendix G Explanation/Clarification Summary
 Appendix G Explanation/Clarification Summary Summary of Changes for Recommendations Alignment of measures with VBP by fiscal year Measures and service dates were adjusted to be consistent with the FY2016
Appendix G Explanation/Clarification Summary Summary of Changes for Recommendations Alignment of measures with VBP by fiscal year Measures and service dates were adjusted to be consistent with the FY2016
The Centers for Medicare & Medicaid Services (CMS) Acute Care Hospital Fiscal Year (FY) 2018 Quality Improvement Program Measures
 ID M easure Name NQF # H os pital M easurement Period H os pital H os pital Value-Bas ed Purchas ing M easurement Period H os pital H ealth Record (EH R) Incentive M easurement Period H os pital H os pital-
ID M easure Name NQF # H os pital M easurement Period H os pital H os pital Value-Bas ed Purchas ing M easurement Period H os pital H ealth Record (EH R) Incentive M easurement Period H os pital H os pital-
CMS Hospital Inpatient Quality Reporting (IQR) Program Measures for the FY 2020 Payment Update
 CMS Inpatient Quality Reporting (IQR) Program Measures for the Payment Update Measures Required to Meet IQR Program APU Requirements Healthcare-Associated Infection on CAUTI National Healthcare Safety
CMS Inpatient Quality Reporting (IQR) Program Measures for the Payment Update Measures Required to Meet IQR Program APU Requirements Healthcare-Associated Infection on CAUTI National Healthcare Safety
CMS Measures - Fiscal Year 2019
 ID Me asure Name NQF # Value- (VBP) - (HACRP) (HRRP) ID Me asure Name NQF # Value- (VBP) - (HACRP) (HRRP) CMS s - Fiscal Year 2019 ID Name NQF # The Centers for Medicare & Medicaid Services (CMS) Improvement
ID Me asure Name NQF # Value- (VBP) - (HACRP) (HRRP) ID Me asure Name NQF # Value- (VBP) - (HACRP) (HRRP) CMS s - Fiscal Year 2019 ID Name NQF # The Centers for Medicare & Medicaid Services (CMS) Improvement
Performance Measure. Inpatient Clinical Process of Care Measures
 Acute Myocardial Infarction (AMI) 's Maryland Hospital Performance Evaluation System: Inpatient s Quality Based Reimbursement () Measures Highlighted in Green (02/27/2014) Inpatient Clinical Process of
Acute Myocardial Infarction (AMI) 's Maryland Hospital Performance Evaluation System: Inpatient s Quality Based Reimbursement () Measures Highlighted in Green (02/27/2014) Inpatient Clinical Process of
CMS Hospital Inpatient Quality Reporting (IQR) Program Measures for the FY 2019 Payment Update
 CMS Inpatient Quality Reporting (IQR) Program Measures for the Update Measures Required to Meet IQR Program APU Requirements NHSN Submission CAUTI National Healthcare Safety Network (NHSN) Catheter-Associated
CMS Inpatient Quality Reporting (IQR) Program Measures for the Update Measures Required to Meet IQR Program APU Requirements NHSN Submission CAUTI National Healthcare Safety Network (NHSN) Catheter-Associated
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
State of the State: Hospital Performance in Pennsylvania August 2010
 State of the State: Hospital Performance in Pennsylvania August 2010 Measuring Progress in PA Hospital Performance: Process Measures Quality Measures Analysis We reviewed the latest year-over-year changes
State of the State: Hospital Performance in Pennsylvania August 2010 Measuring Progress in PA Hospital Performance: Process Measures Quality Measures Analysis We reviewed the latest year-over-year changes
Advancing Care Coordination through Episode Payment Models (EPMs): Summary of the Proposed Rule
 Advancing Care Coordination through Episode Payment Models (EPMs): Summary of the Proposed Rule Overview Three new mandatory Episode Payment Models (EPMs) Cardiac Rehabilitation (CR) Incentive Payment
Advancing Care Coordination through Episode Payment Models (EPMs): Summary of the Proposed Rule Overview Three new mandatory Episode Payment Models (EPMs) Cardiac Rehabilitation (CR) Incentive Payment
Nancy Hailpern, Director, Regulatory Affairs K Street, NW, Suite 1000 Washington, DC 20005
 Summary of Infection Prevention Issues in the Centers for Medicare & Medicaid Services (CMS) FY 2014 Inpatient Prospective Payment System (IPPS) Final Rule Hospital Readmissions Reduction Program-Fiscal
Summary of Infection Prevention Issues in the Centers for Medicare & Medicaid Services (CMS) FY 2014 Inpatient Prospective Payment System (IPPS) Final Rule Hospital Readmissions Reduction Program-Fiscal
Patient Navigator Program: Focus MI Diplomat Hospital Metrics
 Patient Navigator Program: Focus MI Diplomat Hospital Metrics Goal Statement: To reduce avoidable hospital readmissions for patients discharged with acute myocardial infarction (AMI) by supporting a culture
Patient Navigator Program: Focus MI Diplomat Hospital Metrics Goal Statement: To reduce avoidable hospital readmissions for patients discharged with acute myocardial infarction (AMI) by supporting a culture
End-Stage Renal Disease Quality Incentive Program (ESRD QIP) Status Type NQF Measure Title
 End-Stage Renal Disease Quality Incentive Program (ESRD QIP) Status Type NQF Measure Title NQF Status ID Implemented Outcome 1454 Proportion of patients with hypercalcemia 0256 Vascular Access Type Catheter
End-Stage Renal Disease Quality Incentive Program (ESRD QIP) Status Type NQF Measure Title NQF Status ID Implemented Outcome 1454 Proportion of patients with hypercalcemia 0256 Vascular Access Type Catheter
State of the State: Hospital Performance in Pennsylvania September 2012
 State of the State: Hospital Performance in Pennsylvania September 2012 Measuring Progress in PA Hospital Performance: Process Measures 1 PA Hospital Performance: Process Measures We examined the latest
State of the State: Hospital Performance in Pennsylvania September 2012 Measuring Progress in PA Hospital Performance: Process Measures 1 PA Hospital Performance: Process Measures We examined the latest
COOK COUNTY HEALTH Meaningful Metrics
 COOK COUNTY HEALTH Meaningful Metrics 2018-2019 Ronald Wyatt MD MHA January 18, 2019 2 Meaningful Measures 3 Meaningful Measures Framework Meaningful Measure Areas Achieve: High quality healthcare Meaningful
COOK COUNTY HEALTH Meaningful Metrics 2018-2019 Ronald Wyatt MD MHA January 18, 2019 2 Meaningful Measures 3 Meaningful Measures Framework Meaningful Measure Areas Achieve: High quality healthcare Meaningful
Appendix Identification of Study Cohorts
 Appendix Identification of Study Cohorts Because the models were run with the 2010 SAS Packs from Centers for Medicare and Medicaid Services (CMS)/Yale, the eligibility criteria described in "2010 Measures
Appendix Identification of Study Cohorts Because the models were run with the 2010 SAS Packs from Centers for Medicare and Medicaid Services (CMS)/Yale, the eligibility criteria described in "2010 Measures
Troubleshooting Audio
 Welcome Audio for this event is available via ReadyTalk Internet streaming. No telephone line is required. Computer speakers or headphones are necessary to listen to streaming audio. Limited dial-in lines
Welcome Audio for this event is available via ReadyTalk Internet streaming. No telephone line is required. Computer speakers or headphones are necessary to listen to streaming audio. Limited dial-in lines
HEART FAILURE QUALITY IMPROVEMENT. American Heart Association Shawni Smith Regional Director, Quality & Systems Improvement
 HEART FAILURE QUALITY IMPROVEMENT American Heart Association Shawni Smith Regional Director, Quality & Systems Improvement 1 DISCLOSURES NONE 2 3 WHY IS THIS IMPORTANT? WHY? Heart Failure Currently, an
HEART FAILURE QUALITY IMPROVEMENT American Heart Association Shawni Smith Regional Director, Quality & Systems Improvement 1 DISCLOSURES NONE 2 3 WHY IS THIS IMPORTANT? WHY? Heart Failure Currently, an
Final Recommendation for Updating the Quality Based Reimbursement Program
 Final Recommendation for Updating the Quality Based Reimbursement Program for FY 2018 October 14, 2015 Health Services Cost Review Commission 4160 Patterson Avenue Baltimore, Maryland 21215 (410) 764 2605
Final Recommendation for Updating the Quality Based Reimbursement Program for FY 2018 October 14, 2015 Health Services Cost Review Commission 4160 Patterson Avenue Baltimore, Maryland 21215 (410) 764 2605
SCORES FOR 4 TH QUARTER, RD QUARTER, 2014
 SCORES FOR 4 TH QUARTER, 2013 3 RD QUARTER, 2014 PATIENT SATISFACTION SCORES (HCAHPS): 4 STARS OUT OF 5 (ONLY 4 AREA ACUTE CARE HOSPITALS RECEIVED A 4-STAR RATING. NONE ACHIEVED 5-STARS). STRUCTURAL MEASURES:
SCORES FOR 4 TH QUARTER, 2013 3 RD QUARTER, 2014 PATIENT SATISFACTION SCORES (HCAHPS): 4 STARS OUT OF 5 (ONLY 4 AREA ACUTE CARE HOSPITALS RECEIVED A 4-STAR RATING. NONE ACHIEVED 5-STARS). STRUCTURAL MEASURES:
Risk Mitigation in Bundled Payment
 Risk Mitigation in Bundled Payment When to Hold Them and When To Fold Them Lily Pazand, MPH NYU Langone Medical Center Jonathan Pearce, MBA, CPA, FHFMA Singletrack Analytics Jessica Walradt, MS Association
Risk Mitigation in Bundled Payment When to Hold Them and When To Fold Them Lily Pazand, MPH NYU Langone Medical Center Jonathan Pearce, MBA, CPA, FHFMA Singletrack Analytics Jessica Walradt, MS Association
50198 Federal Register / Vol. 75, No. 157 / Monday, August 16, 2010 / Rules and Regulations
 50198 Federal Register / Vol. 75, No. 157 / Monday, August 16, 2010 / Rules and Regulations mstockstill on DSKH9S0YB1PROD with RULES2 VerDate Mar2010 17:02 Aug 13, 2010 Jkt 220001 PO 00000 Frm 00158
50198 Federal Register / Vol. 75, No. 157 / Monday, August 16, 2010 / Rules and Regulations mstockstill on DSKH9S0YB1PROD with RULES2 VerDate Mar2010 17:02 Aug 13, 2010 Jkt 220001 PO 00000 Frm 00158
Stratis Health
 2017 Hospital Measure Summary Minnesota Statewide Quality eporting & Measurement System (SQMS) and FY2019 for Center for Medicare & Medicaid Services (CMS) Contents Key... 1 Chart Abstracted Measures...
2017 Hospital Measure Summary Minnesota Statewide Quality eporting & Measurement System (SQMS) and FY2019 for Center for Medicare & Medicaid Services (CMS) Contents Key... 1 Chart Abstracted Measures...
Rehospitalization Data: A Primer for Clinicians Prepared for Project STAAR
 1 Rehospitalization Data: A Primer for Clinicians Prepared for Project STAAR Stephen F. Jencks, M.D., M.P.H. Consultant in Healthcare Safety and Quality 410-708-1134 443-801-8348 steve.jencks@comcast.net
1 Rehospitalization Data: A Primer for Clinicians Prepared for Project STAAR Stephen F. Jencks, M.D., M.P.H. Consultant in Healthcare Safety and Quality 410-708-1134 443-801-8348 steve.jencks@comcast.net
FY X Time (48 hrs for cardiac surgery) SCIP-Inf-4 Cardiac Surgery Patients With Controlled 6 A.M. Postoperative Blood
 Valuebased 2013 Hospital Measure Summary Data Collection for Inpatient Quality Reporting FY2015 and Outpatient Reporting CY2014 January 2013 Key: = Required by both CMS and State of Minnesota = Required
Valuebased 2013 Hospital Measure Summary Data Collection for Inpatient Quality Reporting FY2015 and Outpatient Reporting CY2014 January 2013 Key: = Required by both CMS and State of Minnesota = Required
SUNY Downstate Medical Center/University Hospital Oct - Dec 2013 (Q4)
 Value Based Purchasing-Clinical Process of Care Measures Denom Observed VBP VBP Benchmark Standard Denom Observed VBP VBP Benchmark Standard N Percent x/n N Percent x/n SCIP-Inf-9 Urinary catheter removed
Value Based Purchasing-Clinical Process of Care Measures Denom Observed VBP VBP Benchmark Standard Denom Observed VBP VBP Benchmark Standard N Percent x/n N Percent x/n SCIP-Inf-9 Urinary catheter removed
Medicare Hospital Acquired Conditions Reduction Program Andrew B. Wheeler Vice President of Federal Finance
 Medicare Hospital Acquired Conditions Reduction Program - 201 Andrew B. Wheeler Vice President of Federal Finance Value-Based Hospital Acquired Purchasing Conditions FFY 2018 FFY -2016 2020 AHRQ Claims
Medicare Hospital Acquired Conditions Reduction Program - 201 Andrew B. Wheeler Vice President of Federal Finance Value-Based Hospital Acquired Purchasing Conditions FFY 2018 FFY -2016 2020 AHRQ Claims
BPCI Advanced Episode Selection
 BPCI Advanced Episode Selection Analytic Framework and Strategies from Northwestern Medicine Presented June 7, 2018 to: Insert relevant presenter information Calibri 16pt Presented Jessica Walradt on:
BPCI Advanced Episode Selection Analytic Framework and Strategies from Northwestern Medicine Presented June 7, 2018 to: Insert relevant presenter information Calibri 16pt Presented Jessica Walradt on:
UCLA Health System Apr - Jun 2013 (Q2)
 Denom Observed VBP Standard VBP Benchmark Denom Observed VBP Standard VBP Benchmark N Percent x/n N Percent x/n Value Based Purchasing-Clinical Process of Care Measures (%) SCIP-Inf-9 Urinary catheter
Denom Observed VBP Standard VBP Benchmark Denom Observed VBP Standard VBP Benchmark N Percent x/n N Percent x/n Value Based Purchasing-Clinical Process of Care Measures (%) SCIP-Inf-9 Urinary catheter
NEW JERSEY 2012 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES
 NEW JERSEY 2012 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES New Jersey Department of Health Health Care Quality Assessment June 2013 NEW JERSEY
NEW JERSEY 2012 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES New Jersey Department of Health Health Care Quality Assessment June 2013 NEW JERSEY
Quality Reporting for CAHs and Rural PPS Hospitals: The Potential Impact of Composite Measures
 UpperMidwest Rural Health Research Center www.uppermidwestrhrc.org July 202 Policy Brief Quality Reporting for CAHs and Rural PPS Hospitals: The Potential Impact of Composite Measures Michelle Casey MS,
UpperMidwest Rural Health Research Center www.uppermidwestrhrc.org July 202 Policy Brief Quality Reporting for CAHs and Rural PPS Hospitals: The Potential Impact of Composite Measures Michelle Casey MS,
Medicare Shared Savings Program Quality Measure Benchmarks for the 2014 and 2015 Reporting Years
 Medicare Shared Savings Program Quality Measure Benchmarks for the 2014 and 2015 Reporting Years Introduction This document describes methods for calculating the quality performance benchmarks for Accountable
Medicare Shared Savings Program Quality Measure Benchmarks for the 2014 and 2015 Reporting Years Introduction This document describes methods for calculating the quality performance benchmarks for Accountable
APPENDIX EXHIBITS. Appendix Exhibit A2: Patient Comorbidity Codes Used To Risk- Standardize Hospital Mortality and Readmission Rates page 10
 Ross JS, Bernheim SM, Lin Z, Drye EE, Chen J, Normand ST, et al. Based on key measures, care quality for Medicare enrollees at safety-net and non-safety-net hospitals was almost equal. Health Aff (Millwood).
Ross JS, Bernheim SM, Lin Z, Drye EE, Chen J, Normand ST, et al. Based on key measures, care quality for Medicare enrollees at safety-net and non-safety-net hospitals was almost equal. Health Aff (Millwood).
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Fiscal Year (FY) 2019 Hospital Inpatient Proposed Rule Interventional Cardiology, Peripheral Interventions & Rhythm Management
 Fiscal Year (FY) 2019 Hospital Inpatient Proposed Rule Interventional Cardiology, Peripheral Interventions & Rhythm Management On April 24, 2018, the Centers for Medicare & Medicaid Services (CMS) released
Fiscal Year (FY) 2019 Hospital Inpatient Proposed Rule Interventional Cardiology, Peripheral Interventions & Rhythm Management On April 24, 2018, the Centers for Medicare & Medicaid Services (CMS) released
Commercial Bundling. National Bundled Payment Summit Integrated Healthcare Association. George Washington University, Washington, DC.
 Commercial Bundling National Bundled Payment Summit Integrated Healthcare Association George Washington University, Washington, DC June 12, 2012 Copyright 2012. This presentation as a whole and all of
Commercial Bundling National Bundled Payment Summit Integrated Healthcare Association George Washington University, Washington, DC June 12, 2012 Copyright 2012. This presentation as a whole and all of
COMMUNITY ONCOLOGY ALLIANCE YOU WON T BELIEVE WHAT CMS WILL BE REPORTING ON YOUR ONCOLOGISTS
 COMMUNITY ONCOLOGY ALLIANCE YOU WON T BELIEVE WHAT CMS WILL BE REPORTING ON YOUR ONCOLOGISTS Community Oncology Alliance 2 Physician Ratings Consumers want information about quality Have become used to
COMMUNITY ONCOLOGY ALLIANCE YOU WON T BELIEVE WHAT CMS WILL BE REPORTING ON YOUR ONCOLOGISTS Community Oncology Alliance 2 Physician Ratings Consumers want information about quality Have become used to
Core = Core required measures for all CAH nationally r = Required by State of Minnesota X = Additional for MBQIP
 Key: 2016 Hospital Measure Summary Minnesota Statewide Quality eporting and Measurement System (SQMS) and FY2018 for Center for Medicare and Medicaid Services () January 2016 = equired by Core = Core required
Key: 2016 Hospital Measure Summary Minnesota Statewide Quality eporting and Measurement System (SQMS) and FY2018 for Center for Medicare and Medicaid Services () January 2016 = equired by Core = Core required
Kansas Care Coordination Quarterly Report October 2018
 Kansas Care Coordination Quarterly Report October 2018 Background Communities across the Great Plains Quality Innovation Network (QIN) region are collaborating to improve care coordination and medication
Kansas Care Coordination Quarterly Report October 2018 Background Communities across the Great Plains Quality Innovation Network (QIN) region are collaborating to improve care coordination and medication
The Future of Cardiac Care: Managing Our Patients Together
 The Future of Cardiac Care: Managing Our Patients Together Charles R. Caldwell, MD, FACC Disclosures: iheartdoc,inc. Telemedicine 1 MACRA Medicare Access and CHIP Reauthorization Act of 2015 Repealed the
The Future of Cardiac Care: Managing Our Patients Together Charles R. Caldwell, MD, FACC Disclosures: iheartdoc,inc. Telemedicine 1 MACRA Medicare Access and CHIP Reauthorization Act of 2015 Repealed the
Dana L. Gilbert Chief Operating Officer Sharon Rudnick Vice President Outpatient Care Management
 Ambulatory Sensitive Admissions Dana L. Gilbert Chief Operating Officer Sharon Rudnick Vice President Outpatient Care Management 1 Sites Of Care Advocate Health Care 12 Hospitals 10 acute care hospitals
Ambulatory Sensitive Admissions Dana L. Gilbert Chief Operating Officer Sharon Rudnick Vice President Outpatient Care Management 1 Sites Of Care Advocate Health Care 12 Hospitals 10 acute care hospitals
Objectives. Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers
 Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers August 22, 2017 Objectives Understand the basics of the hospital specific MSPB data files and reports Review the factors
Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers August 22, 2017 Objectives Understand the basics of the hospital specific MSPB data files and reports Review the factors
THE NATIONAL QUALITY FORUM
 THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
THE NATIONAL QUALITY FORUM National Voluntary Consensus Standards for Patient Outcomes Table of Measures Submitted-Phase 1 As of March 5, 2010 Note: This information is for personal and noncommercial use
Key Findings. Mortality Rates
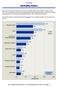 Mortality Rates Statewide in-hospital mortality rates showed a statistically significant decrease from to in nine of the 15 conditions reported. The largest decrease was in, where the mortality rate decreased
Mortality Rates Statewide in-hospital mortality rates showed a statistically significant decrease from to in nine of the 15 conditions reported. The largest decrease was in, where the mortality rate decreased
Quality & Hospital Acquired Conditions
 Quality & Hospital Acquired Conditions Rebecca Armbruster, DO, MS, FACOI Medical Director Resource Management Patricia Heys, BS Director of Infection Prevention & Control Sally Hinkle, DNP, MPA, RN Director
Quality & Hospital Acquired Conditions Rebecca Armbruster, DO, MS, FACOI Medical Director Resource Management Patricia Heys, BS Director of Infection Prevention & Control Sally Hinkle, DNP, MPA, RN Director
Supplementary Online Content
 Supplementary Online Content Dharmarajan K, Wang Y, Lin Z, et al. Association of changing hospital readmission rates with mortality rates after hospital discharge. JAMA. doi:10.1001/jama.2017.8444 etable
Supplementary Online Content Dharmarajan K, Wang Y, Lin Z, et al. Association of changing hospital readmission rates with mortality rates after hospital discharge. JAMA. doi:10.1001/jama.2017.8444 etable
2011 Measures Maintenance Technical Report: Acute Myocardial Infarction, Heart Failure, and Pneumonia 30 Day Risk Standardized Readmission Measures
 2011 Measures Maintenance Technical Report: Acute Myocardial Infarction, Heart Failure, and Pneumonia 30 Day Risk Standardized Readmission Measures Submitted By Yale New Haven Health Services Corporation
2011 Measures Maintenance Technical Report: Acute Myocardial Infarction, Heart Failure, and Pneumonia 30 Day Risk Standardized Readmission Measures Submitted By Yale New Haven Health Services Corporation
Table 1. Proposed Measures for Use in Establishing Quality Performance Standards that ACOs Must Meet for Shared Savings
 CMS-1345-P 174 Table 1. Proposed Measures for Use in Establishing Quality Performance Standards that ACOs Must Meet for Shared Savings AIM: Better Care for Individuals 1. Patient/Care Giver Experience
CMS-1345-P 174 Table 1. Proposed Measures for Use in Establishing Quality Performance Standards that ACOs Must Meet for Shared Savings AIM: Better Care for Individuals 1. Patient/Care Giver Experience
Improving Quality of Care for Medicare Patients: Accountable Care Organizations
 DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services Room 352-G 200 Independence Avenue, SW Washington, DC 20201 Office of Media Affairs MEDICARE FACT SHEET FOR IMMEDIATE RELEASE
DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services Room 352-G 200 Independence Avenue, SW Washington, DC 20201 Office of Media Affairs MEDICARE FACT SHEET FOR IMMEDIATE RELEASE
The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis
 Client Report Milliman Client Report The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis Prepared by Kathryn Fitch, RN, MEd Principal and Healthcare
Client Report Milliman Client Report The Cost Burden of Worsening Heart Failure in the Medicare Fee For Service Population: An Actuarial Analysis Prepared by Kathryn Fitch, RN, MEd Principal and Healthcare
Reporting Period and Reliability of AHRQ, CMS 30-day and HAC Quality Measures - Revised
 MEMORANDUM TO: Sophia Chan SUBJECT: Reporting Period and Reliability of AHRQ, CMS 30-day and HAC Quality Measures - Revised Reliability of an outcome measure is the extent to which variation in the measure
MEMORANDUM TO: Sophia Chan SUBJECT: Reporting Period and Reliability of AHRQ, CMS 30-day and HAC Quality Measures - Revised Reliability of an outcome measure is the extent to which variation in the measure
2016 HCPro, a division of BLR. All rights reserved. These materials may not be duplicated without express written permission.
 CDI and Hospital Readmissions: What Impact Can You Have? Kim Charland, BA, RHIT, CCS Senior Vice President Clinical Innovation & Publisher of VBPmonitor Michelle A. Leonard Mays, RN, MSN, CCDS Senior Healthcare
CDI and Hospital Readmissions: What Impact Can You Have? Kim Charland, BA, RHIT, CCS Senior Vice President Clinical Innovation & Publisher of VBPmonitor Michelle A. Leonard Mays, RN, MSN, CCDS Senior Healthcare
Bundled Payments in Post Acute Care: Put on Your Crash Helmets or Fasten Your Seatbelts
 Bundled Payments in Post Acute Care: Put on Your Crash Helmets or Fasten Your Seatbelts Presented by: Rodney Farley, Vice President of Post Acute Services 5925 Stevenson Avenue Suite G Harrisburg, PA 17112
Bundled Payments in Post Acute Care: Put on Your Crash Helmets or Fasten Your Seatbelts Presented by: Rodney Farley, Vice President of Post Acute Services 5925 Stevenson Avenue Suite G Harrisburg, PA 17112
Statewide Statistics and Key Findings 1
 % s, 30 Days PHC4 s for Same Condition Jan 03 through Aug 04 Data Statewide information about readmissions and the key findings of this report are presented in this section. The study examines hospitalizations
% s, 30 Days PHC4 s for Same Condition Jan 03 through Aug 04 Data Statewide information about readmissions and the key findings of this report are presented in this section. The study examines hospitalizations
Publicly Reported Quality Measures
 Publicly Reported Quality Measures Five-Star Quality Rating System As part of the initiative to add five-star quality ratings to its Compare Web sites, the Centers for Medicare & Medicaid Services (CMS)
Publicly Reported Quality Measures Five-Star Quality Rating System As part of the initiative to add five-star quality ratings to its Compare Web sites, the Centers for Medicare & Medicaid Services (CMS)
A Physician Leader s Role In Becoming A High Performing Health System
 A Physician Leader s Role In Becoming A High Performing Health System Byron C. Scott, MD, MBA Associate Chief Medical Officer, Truven Health Analytics Truven Health Analytics Inc. All Rights Reserved.
A Physician Leader s Role In Becoming A High Performing Health System Byron C. Scott, MD, MBA Associate Chief Medical Officer, Truven Health Analytics Truven Health Analytics Inc. All Rights Reserved.
Writing Committee. ACP Performance Measurement Committee Members*
 Performance Measurement Coronary Artery Bypass Graft Surgery: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem,
Performance Measurement Coronary Artery Bypass Graft Surgery: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem,
Real World Patients: The Intersection of Real World Evidence and Episode of Care Analytics
 PharmaSUG 2018 - Paper RW-05 Real World Patients: The Intersection of Real World Evidence and Episode of Care Analytics David Olaleye and Youngjin Park, SAS Institute Inc. ABSTRACT SAS Institute recently
PharmaSUG 2018 - Paper RW-05 Real World Patients: The Intersection of Real World Evidence and Episode of Care Analytics David Olaleye and Youngjin Park, SAS Institute Inc. ABSTRACT SAS Institute recently
IASIS Focus on Quality
 IASIS Focus on Quality Patients and their families know and understand the meaning of quality healthcare. The attitude and responsiveness of their nurse, the doctor s bedside manner, the overall appearance
IASIS Focus on Quality Patients and their families know and understand the meaning of quality healthcare. The attitude and responsiveness of their nurse, the doctor s bedside manner, the overall appearance
Supplementary Online Content
 Supplementary Online Content Khera R, Dharmarajan K, Wang Y, et al. Association of the hospital readmissions reduction program with mortality during and after hospitalization for acute myocardial infarction,
Supplementary Online Content Khera R, Dharmarajan K, Wang Y, et al. Association of the hospital readmissions reduction program with mortality during and after hospitalization for acute myocardial infarction,
Hospice Metrics Using Medicare Data to Measure Access and Performance for Hospice and Palliative Care
 Hospice Metrics Using Medicare Data to Measure Access and Performance for Hospice and Palliative Care 1 Outline What are the Medicare data? What are the important metrics? Why hospitals matter so much
Hospice Metrics Using Medicare Data to Measure Access and Performance for Hospice and Palliative Care 1 Outline What are the Medicare data? What are the important metrics? Why hospitals matter so much
NEW JERSEY 2011 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES
 NEW JERSEY 2011 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES New Jersey Department of Health and Senior Services Health Care Quality Assessment
NEW JERSEY 2011 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES New Jersey Department of Health and Senior Services Health Care Quality Assessment
Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments
 Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments Prepared for: American Hospital Association April 4, 2019 Berna Demiralp,
Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments Prepared for: American Hospital Association April 4, 2019 Berna Demiralp,
Fifth Annual National ACO Summit
 Fifth Annual National ACO Summit June 18 20, 2014 Follow us on Twitter at @ACO_LN and use #ACOsummit The Engelberg Center for Health Care Reform at Brookings The Dartmouth Institute Track One: Performance
Fifth Annual National ACO Summit June 18 20, 2014 Follow us on Twitter at @ACO_LN and use #ACOsummit The Engelberg Center for Health Care Reform at Brookings The Dartmouth Institute Track One: Performance
Publicly Reported Quality Measures
 Publicly Reported Quality Measures Five-Star Quality Rating System As part of the initiative to add five-star quality ratings to its Compare Web sites, the Centers for Medicare & Medicaid Services (CMS)
Publicly Reported Quality Measures Five-Star Quality Rating System As part of the initiative to add five-star quality ratings to its Compare Web sites, the Centers for Medicare & Medicaid Services (CMS)
Quality Payment Program: A Closer Look at the Proposed Rule for Year 3
 Quality Payment Program: A Closer Look at the Proposed Rule for Year 3 Sandy Swallow and Michelle Brunsen August 21, 2018 1 This material was prepared by Telligen, the Medicare Quality Innovation Network
Quality Payment Program: A Closer Look at the Proposed Rule for Year 3 Sandy Swallow and Michelle Brunsen August 21, 2018 1 This material was prepared by Telligen, the Medicare Quality Innovation Network
Key Findings. Mortality Rates
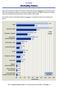 Mortality Rates Statewide in-hospital mortality rates showed a statistically significant decrease from federal fiscal year to federal fiscal year in 12 of the 15 conditions reported. The largest decrease
Mortality Rates Statewide in-hospital mortality rates showed a statistically significant decrease from federal fiscal year to federal fiscal year in 12 of the 15 conditions reported. The largest decrease
Absent: Director Layla P. Suleiman Gonzalez, PhD, JD (1)
 Minutes of the meeting of the Quality and Patient Safety Committee of the Board of Directors of the Cook County Health and Hospitals System held Friday, January 18, 2019 at the hour of 10:00 A.M. at 1950
Minutes of the meeting of the Quality and Patient Safety Committee of the Board of Directors of the Cook County Health and Hospitals System held Friday, January 18, 2019 at the hour of 10:00 A.M. at 1950
Heart Attack Readmissions in Virginia
 Heart Attack Readmissions in Virginia Schroeder Center Statistical Brief Research by Mitchell Cole, William & Mary Public Policy, MPP Class of 2017 Highlights: In 2014, almost 11.2 percent of patients
Heart Attack Readmissions in Virginia Schroeder Center Statistical Brief Research by Mitchell Cole, William & Mary Public Policy, MPP Class of 2017 Highlights: In 2014, almost 11.2 percent of patients
Quality Outcomes and Financial Benefits of Nutrition Intervention. Tracy R. Smith, PhD, RD, LD Senior Clinical Manager, Abbott Nutrition
 Quality Outcomes and Financial Benefits of Nutrition Intervention Tracy R. Smith, PhD, RD, LD Senior Clinical Manager, Abbott Nutrition January 28, 2016 SHIFTING MARKET DYNAMICS PROVIDE AN OPPORTUNITY
Quality Outcomes and Financial Benefits of Nutrition Intervention Tracy R. Smith, PhD, RD, LD Senior Clinical Manager, Abbott Nutrition January 28, 2016 SHIFTING MARKET DYNAMICS PROVIDE AN OPPORTUNITY
Appendix 1: Supplementary tables [posted as supplied by author]
![Appendix 1: Supplementary tables [posted as supplied by author] Appendix 1: Supplementary tables [posted as supplied by author]](/thumbs/81/83505567.jpg) Appendix 1: Supplementary tables [posted as supplied by author] Table A. International Classification of Diseases, Ninth Revision, Clinical Modification Codes Used to Define Heart Failure, Acute Myocardial
Appendix 1: Supplementary tables [posted as supplied by author] Table A. International Classification of Diseases, Ninth Revision, Clinical Modification Codes Used to Define Heart Failure, Acute Myocardial
The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO
 The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO ACO-1 ACO-2 Getting Timely Care, Appointments, and Information How Well Your Providers
The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO ACO-1 ACO-2 Getting Timely Care, Appointments, and Information How Well Your Providers
Quality Performance Measurement and Use of Health Information Technology in Critical Access Hospitals
 Quality Performance Measurement and Use of Health Information Technology in Critical Access Hospitals Michelle Casey University of Minnesota Rural Health Research Center Flex Monitoring Team 2006 National
Quality Performance Measurement and Use of Health Information Technology in Critical Access Hospitals Michelle Casey University of Minnesota Rural Health Research Center Flex Monitoring Team 2006 National
Diagnosis Coding is About to be Much More Important. Matthew Menendez
 Diagnosis Coding is About to be Much More Important Matthew Menendez Agenda What is CMS doing with MACRA? What is an HCC code and why should I care? Brief MIPS overview How does risk adjustment impact
Diagnosis Coding is About to be Much More Important Matthew Menendez Agenda What is CMS doing with MACRA? What is an HCC code and why should I care? Brief MIPS overview How does risk adjustment impact
CAH Payment Reform: Defining Value and Sustainability. MN Rural Health Conference June 20, 2016
 CAH Payment Reform: Defining Value and Sustainability MN Rural Health Conference June 20, 2016 Minnesota s CAH Landscape 143 Hospitals / 132 General Acute Hospitals 17 Health Systems with 44 CAHs 78 Minnesota
CAH Payment Reform: Defining Value and Sustainability MN Rural Health Conference June 20, 2016 Minnesota s CAH Landscape 143 Hospitals / 132 General Acute Hospitals 17 Health Systems with 44 CAHs 78 Minnesota
The Relationship between Multimorbidity and Concordant and Discordant Causes of Hospital Readmission at 30 Days and One Year
 The Relationship between Multimorbidity and Concordant and Discordant Causes of Hospital Readmission at 30 Days and One Year Arlene S. Bierman, M.D., M.S Professor, University of Toronto and Scientist,
The Relationship between Multimorbidity and Concordant and Discordant Causes of Hospital Readmission at 30 Days and One Year Arlene S. Bierman, M.D., M.S Professor, University of Toronto and Scientist,
Understanding Hierarchical Condition Categories (HCC)
 Understanding Hierarchical Condition Categories (HCC) How hierarchical condition category coding will impact your practice and how you can use these codes to increase quality, improve the patient experience,
Understanding Hierarchical Condition Categories (HCC) How hierarchical condition category coding will impact your practice and how you can use these codes to increase quality, improve the patient experience,
Hypoglycemia and Quality Measurement
 Hypoglycemia and Quality Measurement Sam Stolpe Senior Director The Triple Aim Affordable Care Better Care Healthy People/ Communities 1 Comprehensive Overview of CMS Quality Programs Hospital Quality
Hypoglycemia and Quality Measurement Sam Stolpe Senior Director The Triple Aim Affordable Care Better Care Healthy People/ Communities 1 Comprehensive Overview of CMS Quality Programs Hospital Quality
QIOs: Partners for Quality Improvement Under the Medicare Drug Benefit
 QIOs: Partners for Quality Improvement Under the Medicare Drug Benefit Presentation to The 2 nd Annual National Medicare Prescription Drug Congress David Schulke Executive Vice President The American Health
QIOs: Partners for Quality Improvement Under the Medicare Drug Benefit Presentation to The 2 nd Annual National Medicare Prescription Drug Congress David Schulke Executive Vice President The American Health
Evolution of Heart Failure Disease Management at a Large VA Medical Center. Richard S. Schofield MD, FACC North Florida/South Georgia VHS
 Evolution of Heart Failure Disease Management at a Large VA Medical Center Richard S. Schofield MD, FACC North Florida/South Georgia VHS Disclosures None 2 1,000,000 Increasing VA Burden: Outpatient Encounters
Evolution of Heart Failure Disease Management at a Large VA Medical Center Richard S. Schofield MD, FACC North Florida/South Georgia VHS Disclosures None 2 1,000,000 Increasing VA Burden: Outpatient Encounters
Policy Brief June 2014
 Policy Brief June 2014 Which Medicare Patients Are Transferred from Rural Emergency Departments? Michelle Casey MS, Jeffrey McCullough PhD, and Robert Kreiger PhD Key Findings Among Medicare beneficiaries
Policy Brief June 2014 Which Medicare Patients Are Transferred from Rural Emergency Departments? Michelle Casey MS, Jeffrey McCullough PhD, and Robert Kreiger PhD Key Findings Among Medicare beneficiaries
Hospital Compare Quality Measures: 2011 National and Tennessee Results for Critical Access Hospitals
 March 2013 Hospital Compare Quality Measures: 2011 National and Results for Critical Access Michelle Casey, MS, Peiyin Hung, MSPH, Maeve McClellan, BS, Ira Moscovice, PhD, University of Minnesota Rural
March 2013 Hospital Compare Quality Measures: 2011 National and Results for Critical Access Michelle Casey, MS, Peiyin Hung, MSPH, Maeve McClellan, BS, Ira Moscovice, PhD, University of Minnesota Rural
APR DRG Data Discovery
 APR DRG Data Discovery Henry Johnson MD, MPH Midas+ Vice President and Medical Director Vanessa Dorr RN MSN Midas+ DataVision Clinical Consultant Review: Agenda 3M APR DRG Methodology DataVision: Web and
APR DRG Data Discovery Henry Johnson MD, MPH Midas+ Vice President and Medical Director Vanessa Dorr RN MSN Midas+ DataVision Clinical Consultant Review: Agenda 3M APR DRG Methodology DataVision: Web and
Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians
 Performance Measurement Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem, MD,
Performance Measurement Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem, MD,
MIPS TIPS What is HCC and How Does It Impact the MIPS Cost Category? Oct. 25, 2018
 MIPS TIPS What is HCC and How Does It Impact the MIPS Cost Category? Oct. 25, 2018 Presented by HealthInsight and Mountain Pacific Quality Health Tina Morishima, CPC, Mountain-Pacific Practice Consultant
MIPS TIPS What is HCC and How Does It Impact the MIPS Cost Category? Oct. 25, 2018 Presented by HealthInsight and Mountain Pacific Quality Health Tina Morishima, CPC, Mountain-Pacific Practice Consultant
Quality Committee Core Measures Report AMI. Acute Myocardial Infarction
 AMI 2011 Acute Myocardial Infarction ASPIRIN AT ARRIVAL: A higher number is better. This measure shows the percentage of heart attack patients who receive aspirin within 24 hrs of arrival at hospital.
AMI 2011 Acute Myocardial Infarction ASPIRIN AT ARRIVAL: A higher number is better. This measure shows the percentage of heart attack patients who receive aspirin within 24 hrs of arrival at hospital.
NATIONAL QUALITY FORUM
 TO: NQF Members and Public FR: NQF Staff RE: Pre-comment review of an addendum to National Voluntary Consensus Standards: Cardiovascular Endorsement Maintenance 2010: A Consensus Report DA: October 6,
TO: NQF Members and Public FR: NQF Staff RE: Pre-comment review of an addendum to National Voluntary Consensus Standards: Cardiovascular Endorsement Maintenance 2010: A Consensus Report DA: October 6,
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Massachusetts Medicaid pediatric high-risk asthma bundled payment pilot
 University of Massachusetts Medical School escholarship@umms Commonwealth Medicine Publications Commonwealth Medicine 9-28-2011 Massachusetts Medicaid pediatric high-risk asthma bundled payment pilot Katharine
University of Massachusetts Medical School escholarship@umms Commonwealth Medicine Publications Commonwealth Medicine 9-28-2011 Massachusetts Medicaid pediatric high-risk asthma bundled payment pilot Katharine
Yale New Haven Health Services Corporation/Center for Outcomes Research and Evaluation (YNHHSC/CORE)
 701 Pennsylvania Avenue, Ste. 800 Washington, DC 20004 2654 Tel: 202 783 8700 Fax: 202 783 8750 www.advamed.org July 8, 2011 Yale New Haven Health Services Corporation/Center for Outcomes Research and
701 Pennsylvania Avenue, Ste. 800 Washington, DC 20004 2654 Tel: 202 783 8700 Fax: 202 783 8750 www.advamed.org July 8, 2011 Yale New Haven Health Services Corporation/Center for Outcomes Research and
At the completion of this educational activity, the learner will be able to understand:
 Claims vs. Submission: Understanding the Difference Sonia Trepina, MPA Director, Risk Adjustment & Ambulatory CDI Services Enjoin Asheville, NC Brett Senor, MD, CRC, CCDS Physician Associate, CDI Quality
Claims vs. Submission: Understanding the Difference Sonia Trepina, MPA Director, Risk Adjustment & Ambulatory CDI Services Enjoin Asheville, NC Brett Senor, MD, CRC, CCDS Physician Associate, CDI Quality
2016 Condition-Specific Measures Updates and Specifications Report Hospital-Level 30-Day Risk-Standardized Readmission Measures
 2016 Condition-Specific Measures Updates and Specifications Report Hospital-Level 30-Day Risk-Standardized Readmission Measures Acute Myocardial Infarction Version 9.0 Chronic Obstructive Pulmonary Disease
2016 Condition-Specific Measures Updates and Specifications Report Hospital-Level 30-Day Risk-Standardized Readmission Measures Acute Myocardial Infarction Version 9.0 Chronic Obstructive Pulmonary Disease
The Challenge. Bill Frist, M.D.!
 The Challenge 5% of U.S. Population Spend 50% of Healthcare Dollars % of Healthcare Spending % of U.S. Population 5% of Medicare beneficiaries die each year accounting for 27.4% of Medicare expenditures
The Challenge 5% of U.S. Population Spend 50% of Healthcare Dollars % of Healthcare Spending % of U.S. Population 5% of Medicare beneficiaries die each year accounting for 27.4% of Medicare expenditures
Achieving Quality and Value in Chronic Care Management
 The Burden of Chronic Disease One of the greatest burdens on the US healthcare system is the rapidly growing rate of chronic disease. These statistics illustrate the scope of the problem: Nearly half of
The Burden of Chronic Disease One of the greatest burdens on the US healthcare system is the rapidly growing rate of chronic disease. These statistics illustrate the scope of the problem: Nearly half of
HQID Hospital Performance Update & Analysis of Quality, Cost and Mortality Trends Fact Sheet
 HQID Hospital Performance Update & Analysis of Quality, Cost and Mortality Trends Fact Sheet I.) Performance of Hospitals in the Hospital Quality Incentive Demonstration over 15 Quarters* (pages 2-5) Launched
HQID Hospital Performance Update & Analysis of Quality, Cost and Mortality Trends Fact Sheet I.) Performance of Hospitals in the Hospital Quality Incentive Demonstration over 15 Quarters* (pages 2-5) Launched
Surgical Care, Pneumonia, Immunizations and Emergency Department Core Measures
 Surgical Care, Pneumonia, Immunizations and Emergency Department Core Measures Audrey Paulman, MD, MMM Principal Clinical Coordinator & Jackie Trojan, RN, BSN Quality Improvement Advisor This material
Surgical Care, Pneumonia, Immunizations and Emergency Department Core Measures Audrey Paulman, MD, MMM Principal Clinical Coordinator & Jackie Trojan, RN, BSN Quality Improvement Advisor This material
