HOMES AND SENIORS SERVICES. APPROVAL DATE: August 1985 REVISION DATE: January 2015 REVIEW DATE: May 2018
|
|
|
- Stephen Hawkins
- 5 years ago
- Views:
Transcription
1 POLICY: Page 1 of 10 Residents who experience signs and symptoms associated with dysphagia will have their nutrition and hydration needs met in a safe, coordinated manner as managed by the interdisciplinary care team. OBJECTIVES: To ensure timely access to a swallowing assessment for those residents identified with swallowing problems To ensure an optimal nutrition and hydration intake for residents identified with dysphagia. To ensure that residents with dysphagia receive their foods and fluids in a manner that promotes their safety. To promote the role of the Registered Dietitian as part of an interdisciplinary care team in the screening, assessment, treatment and ongoing management of dysphagia within the Long Term Care Home setting To prevent or minimize the significant consequences or complications/adverse effects associated with dysphagia. PROCEDURE: 1. As part of the admission nutrition assessment, the Registered Dietitian (RD) evaluates the swallowing ability of all newly admitted residents, noting any past swallowing difficulties and including observation of the resident swallowing foods and fluids. 2. Based on the admission nutrition assessment, the RD verifies that the admission diet order and texture meets the swallowing needs of the resident or makes the necessary changes and creates the Nutrition Care Plan.
2 Page 2 of Recognizing the high percentage of residents with swallowing problems in Long Term Care Homes, all members of the interdisciplinary care team receive relevant in-service education and are familiar with the signs and symptoms of swallowing problems (dysphagia). See below 4. All residents are monitored on an ongoing basis by the interdisciplinary care team for any signs/symptoms of dysphagia, which may include but are not limited to, the following: SIGNS/SYMPTOMS of DYSPHAGIA resident choosing to avoid eating all or certain textures complaints of food getting stuck refusal to eat weight loss, especially 1.5 kg in 7 days choking or coughing drooling, excessive secretions difficulty chewing frequent upper respiratory infections gurgling in throat poor air intake very slow eating, resident complains of taste of food food or drink running from the nose chronic constipation dehydration signs of malnutrition pocketing of food in cheeks 5. The RD is informed by any member of the interdisciplinary care team involved with feeding residents of any resident whom they believe: is exhibiting signs/symptoms of dysphagia; needs a reassessment of their food texture and/or fluid consistency modification; has a change in health status which is affecting their ability to chew and/or swallow foods and fluids
3 Page 3 of All residents experiencing acute signs and symptoms of a stroke are kept NPO until their swallowing ability has been assessed; all such residents are referred to the RD. 7. Upon receiving the referral for assessment/ reassessment, the RD observes the resident for at least 10 minutes as resident eats a meal and completes the Dysphagia Assessment and Identification Tool. (See Registered Dietitians Dysphagia Identification and Assessment Tool). The RD attempts tests to determine severity of resident s condition and strategies to improve resident s intake. Input from Registered Nurse and front line staff is essential. (See tests to determine severity of conditions) 8. The RD develops the Nutrition Care Plan, including goals and interventions for safe food and fluid consumption, informs all staff of the treatment strategies, discusses the need for interventions with the resident/substitute Decision Maker (SDM) and reviews any changes in food texture and fluid consistency with the MSS; the MSS informs/instructs Dietary staff, as required, and ensures that the Dietary kardex is updated. 9. Choking incidents must be documented in the progress notes by staff in order to identify specific foods/fluids that are problematic and that may require modification or elimination from the resident s diet. 10. The RD reviews the interventions and treatment strategies on a regular basis and, in consultation with the physician, makes a referral, when required, to a Speech Language Pathologist for further recommendations and follow up [in Ontario, services of a SLP are usually arranged through the Community Care Access Centre]. When possible, the SLP visits are coordinated with days when the RD is in the Home. 11. To maximize resident independence, residents are referred to the Restorative Feeding Program, as appropriate 12. Food brought in from outside the Home is assessed by the Registered staff to determine suitability and safety for the resident. At the time of the admission and annual care conferences, family members/substitute Decision Makers (SDMs) are kept informed regarding any texture modification of foods and fluids that are required by residents.
4 Page 4 of Family members/sdms who disagree with texture modification needs, as assessed by the interdisciplinary care team, agree to take responsibility (as documented in writing in the resident s chart) for any adverse consequences that result from providing residents with foods or fluids in a texture that is considered to be unsafe. All known incidents of the resident/sdm or family providing a different texture/consistency of food/fluid other than what is considered safe are documented in the progress notes by the RD, with the team, including the MD, being aware of such incidents. Resources, References and Regulations: Ontario Regulation 79/10 made under the Long-Term Care Homes Act, 2007, Sections 68 and 71 A Randomized Study of Three Interventions for Aspiration of Thin Liquids in Patients with Dementia or Parkinson s Disease, Logemann, J. A. et al Texture-Modified Foods and Thickened Fluids as Used for Individuals with Dysphagia: Australian Standardised Labels and Definitions, Nutrition and Dietetics Scope of Practice for Registered Dietitians Caring for Clients with Dysphagia in Ontario, College of Dietitians of Ontario, February 2016 Texture Modified Foods: A Manual for Food Production in Long Term Care Facilities, Wendy Dahl, Dietitians of Canada, 2008 Management of Dysphagia in Acute Stroke, Heart and Stroke Foundation of Ontario 2006 Defining the Role of the Dietitian in Dysphagia Assessment and Management, Dietitians of Canada March Dysphagia Manual - Helping People Who Have Difficulty Swallowing, Riverview Health Centre 2002 Dysphagia Manual for Long -Term Care, Jerrilyn Platt, 2001 BB&A Policy: Dysphagia Diet - Thickened Fluids and BB&A Policy: Restorative Feeding
5 Page 5 of 10 Registered Dietitian s Dysphagia Identification and Assessment Tool Resident Information: Name: Room: Current Diet/Texture/Fluid Consistency: Current Food/Fluid Intake: Nourishment/Supplement: Current Weight: IBW/Usual BW: BMI: Weight changes: Medical History: Respiratory or Dysphagia Hx: History / Observations: Is resident alert enough to be assessed (awake during whole meal): Yes No Is resident able to sit upright during meals with neck upright: Yes No Is resident able to communicate/follow commands, either orally or visually: Yes No If answer to the above questions is no, try another meal or another day. Visual Assessment Before Meal: Condition of Mouth Condition of Dentures Fit of Dentures Condition of Teeth/Gums moist good U / L good U / L healthy gums dry poor U / L poor U / L cracked lips drooling broken U / L red or bleeding gums missing U / L broken teeth not worn oral hygiene/condition Observation during Meal: Meal Observed: Breakfast / Lunch / Supper Texture of meal provided: Head Position Body Position Hand Coordination Seating
6 Page 6 of 10 head upright sitting upright able to hold cutlery chair/wheelcha head tilted R L body leaning R hand steady tray on chair chin tucked body leaning L hand shaking gerichair head arched back body leaning forward neck extended restless Difficulty Chewing Difficulty Swallowing Tongue Movement Food in Mouth good mastication swallows well moves food in mouth no pocketing poor mastication clears throat tongue thrusting yes, left spitting hesitation no movement yes, right change in breathing pattern residue in mout holding food in mouth after swallowing obvious difficulty Choking/Coughing Voice Quality Lip Seal Self-Feeding Skills not observed clear good lip seal independent motor skil coughing/choking eating wet oral spillage R L eating coughing/choking drinking gurgly during meal drooling drinking nasal regurgitation gurgly after meal hand dominance: R/L watery eyes Intake of solids: 100% 75% 50% 25% Intake of liquids: ml Length of time to complete meal: Assistive devices required: Other Findings: Summary of Observation:
7 Page 7 of 10 Treatment Plan: Signature: Date: Revised from the original developed by: Dietitians of Canada Long Term Care Action Group, January 2006 STRATEGIES FOR MANAGING RESIDENTS WITH DYSPHAGIA PROBLEM/CONDITION SIGNS AND SYMPTOMS DIETARY CONSIDERATIONS Oral Preparation Phase Reduced cheek or lip tone, Decreased lip closure Poor tongue control Food is pocketed Poor bolus formation Food or liquid leaks from mouth Maintain semi-solid textures tha form a cohesive bolus Poor rotary jaw movement Reduced tongue movement Reduced jaw range Slow oral transit time with solids Choking during or after swallow Particles remain lodged in throat Maintain semi-solid or chopped textures Use moist, well-lubricated food
8 Reduced tongue movement Reduced oral sensation or awareness Preferences to taste: sweet/sa hot/cold Dry mouth due to: medication cancer treatments Oral Transit Phase Delayed or absent swallow ref Reduced coordination due to neuromuscular disease Limited ability to form bolus and push f to back of throat Bolus separates, food particles fall into throat before swallow Food lodges in areas with reduced sensitivity Excessive or thick saliva, difficulty lubricating and manipulating food, gagging, spittin Page 8 of 10 Use foods that form cohesive bo Close supervision to assess abilit manipulate foods/liquids and saf swallow Use moist, well-lubricated foods Add gravies, sauces, margarine Use artificial saliva or juice to thi secretions, avoid milk Pooling and overflow of food and liquiduse cohesive foods into the airway Possible use of highly seasoned a extreme temperature foods Use thickened liquids Avoid sticky or bulky foods Pharyngeal Transit Phase Reduced airway closure Aspiration before the swallow Use cohesive foods that do not fall apart Reduced or slowed movement through the pharynx Decreased laryngeal elevation Esophageal Transit Phase Weakened closure of airway and pharynx Reduced esophageal peristalsis Food residue remains at base of tongue, particles may fall into airway Food remains on top of airway and falls into airway when it opens to restore breathing Food material returns from the esophagus into the pharynx and spills into the airway Food bolus remains in esophagus Use moist, well-lubricated foods that maintain a cohesive bolus Use soft solids and thick to spoon-thick liquids Avoid sticky, bulky foods that fall apart Use semi-solid moist foods that maintain a cohesive bolus Avoid sticky and dry foods Try dense foods followed by
9 Esophageal obstruction Narrowing of esophageal passageway Reference: Manual of Clinical Dietetics, 6 th edition, page Page 9 of 10 liquid Use thin liquids and pureed or soft foods Avoid sticky, dry foods TESTS TO DETERMINE SEVERITY OF CONDITIONS PROBLEM/CONDITION TEST FOR SEVERITY RESULT AND IMPLICATION Suspected poor tongue control Oral cavity poorly hydrated Poor swallowing Poor mouth opening Holds jaw slack or in open position. Drooling from slack jaw. Ask resident to touch tongue to nose Ask resident to touch tongue to chin Place small amount of honey or smooth jam on upper or lower lip or corners of mouth Place tongue depressor flat on tongue and press lightly Put spoon in mouth and press lightly on tongue Put spoon into ice water. Press gently onto tongue and remove quickly. Ask resident to mimic your open mouth Try to open mouth with tongue depressor. Place small amount of food on inside of lower lip Ask resident to mimic you as you close your mouth. Place your hand under jaw and gently Assess ability to move tongue around inside mouth to manipulate food and to clean oral cavity with tongue Tongue depressor comes off tongue dry if poorly hydrated Comes off easily and wet if tongue is well-hydrated Light pressure should stimulate first swallow. Put food on spoon and press again. Alternate empty spoon and spoon with food to feed resident. If swallowing is successful, keep three spoons in ice and rotate use. Apply heat to jaw to relax muscles. Resident is able to open mouth and lick food. Continue until resident opens mouth enough to be fed. Prop resident s hand under jaw with elbow on table to control jaw closed between spoons of food.
10 Page 10 of 10 try to close mouth. Poor lip control Ask resident to mimic you as you close and open your lips. Ask resident to smile and then to blow out a match. Coughing while drinking Check head positioning. Maintain head in neutral position. Use nosey cup so resident can drink Choking on solids Give resident soft solids without extra additional liquid. Reference: Canadian Nursing Home1:2, May/June 1990 without tilting head. Change eating pattern so that solids are fed first and liquids follow at end of meal Possible texture change.
SWALLOWING DIFFICULTIES IN HD
 Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Dysphagia Management in TCP. Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012
 Dysphagia Management in TCP Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012 The role of the Speech Pathologist To assess swallowing status To provide management and
Dysphagia Management in TCP Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012 The role of the Speech Pathologist To assess swallowing status To provide management and
When Eating Becomes A Challenge Dysphagia
 When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
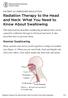 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Dysphagia Identification and Management
 Dysphagia Identification and Management Presented By Speech-Language Pathologist Developmental Disabilities Administration DC Department on Disability Services Training Objectives After this training session
Dysphagia Identification and Management Presented By Speech-Language Pathologist Developmental Disabilities Administration DC Department on Disability Services Training Objectives After this training session
Review of dysphagia in poststroke
 Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
Clinical Swallowing Exam
 Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
Safe swallowing strategies
 Learning Guide Safe swallowing strategies 27468 Apply safe swallowing strategies in a health or wellbeing setting Level 3 5 credits Name: Workplace: Issue 2.0 Copyright 2017 Careerforce All rights reserved.
Learning Guide Safe swallowing strategies 27468 Apply safe swallowing strategies in a health or wellbeing setting Level 3 5 credits Name: Workplace: Issue 2.0 Copyright 2017 Careerforce All rights reserved.
Swallowing problems. Patient information. Name: Date: Speech and Language Therapist: Reviewed: May 2016 Next review: June 2017 Version 1
 Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
Feeding and Oral Hygiene: How to Address the Challenges
 Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
The Role of the Speech Language Pathologist & Spinal Cord Injury
 The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล
 Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016
 Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE
 EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
Workbook. Apply safe swallowing strategies as a health assistant in an aged care, health or disability context. US Level 4 Credits 4. Name...
 Workbook Apply safe swallowing strategies as a health assistant in an aged care, health or disability context US 27468 Level 4 Credits 4 Name... US 27468 Level 4 Credits 4 All rights reserved. Careerforce
Workbook Apply safe swallowing strategies as a health assistant in an aged care, health or disability context US 27468 Level 4 Credits 4 Name... US 27468 Level 4 Credits 4 All rights reserved. Careerforce
Swallowing Awareness Day
 awareness for youth and adults INSIDE: Facts about eating and drinking checklist General information 9, 2011 Facts for youth and adults on swallowing issues Dysphagia is the medical term for any difficulty
awareness for youth and adults INSIDE: Facts about eating and drinking checklist General information 9, 2011 Facts for youth and adults on swallowing issues Dysphagia is the medical term for any difficulty
Dysphagia and Swallowing. Jan Adams, DNP, MPA, RN and Karen Kern
 Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Communication and Swallowing with PSP/CBD. Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist
 Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Role of Dining Services and Dietary Needs of the Resident, 2014
 Role of Dining Services and Dietary Needs of the Resident, 2014 It is the dining services role to provide quality meals and service to all residents that is as home-like as possible. This will be done
Role of Dining Services and Dietary Needs of the Resident, 2014 It is the dining services role to provide quality meals and service to all residents that is as home-like as possible. This will be done
Pediatric Modified Barium Swallow Studies. Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015
 Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
Reluctance or refusal to feed or eat. Understanding Feeding Aversion in a City Full of Foodies. Presentation Outline. Learning Objectives
 Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
The Clinical Swallow Evaluation: What it can and cannot tell us. Introduction
 The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
SWALLOWING: HOW CAN WE HELP
 SWALLOWING: HOW CAN WE HELP Carol Romero-Clark, M.S., CCC-SLP University of New Mexico Hospital Speech Pathology Department November 10, 2017 What happens when you swallow? Mouth (Oral Phase) Your tongue
SWALLOWING: HOW CAN WE HELP Carol Romero-Clark, M.S., CCC-SLP University of New Mexico Hospital Speech Pathology Department November 10, 2017 What happens when you swallow? Mouth (Oral Phase) Your tongue
Speech and Language Therapy. Kerrie McCarthy Senior Speech and Language Therapist
 Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Quick Death, Slow Death, Hopefully No Death
 Quick Death, Slow Death, Hopefully No Death Collaborative presentation on learning from choking and nutrition incidents in RWT. Introduction of IDDSI for food and fluids Why there is an NPSA Alert Safe
Quick Death, Slow Death, Hopefully No Death Collaborative presentation on learning from choking and nutrition incidents in RWT. Introduction of IDDSI for food and fluids Why there is an NPSA Alert Safe
Chapter 20. Assisting With Nutrition and Fluids
 Chapter 20 Assisting With Nutrition and Fluids Food and water: Are physical needs Basics of Nutrition Are necessary for life A poor diet and poor eating habits: Increase the risk for diseases and infection
Chapter 20 Assisting With Nutrition and Fluids Food and water: Are physical needs Basics of Nutrition Are necessary for life A poor diet and poor eating habits: Increase the risk for diseases and infection
Chapter 19. Nutrition and Fluids. All items and derived items 2015, 2011 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved.
 Chapter 19 Nutrition and Fluids Nutrition Nutrition--processes involved in the ingestion, digestion, absorption & use of foods & fluids by the body. The person s diet affects physical & mental wellbeing
Chapter 19 Nutrition and Fluids Nutrition Nutrition--processes involved in the ingestion, digestion, absorption & use of foods & fluids by the body. The person s diet affects physical & mental wellbeing
MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring Patricia Bednarik, MS, CCC-SLP, MSCS
 Page 1 MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring, MS, CCC-SLP, MSCS >>Kate Milliken: Welcome to MS Learn Online. I am Kate Milliken. Swallowing is something
Page 1 MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring, MS, CCC-SLP, MSCS >>Kate Milliken: Welcome to MS Learn Online. I am Kate Milliken. Swallowing is something
Section K Swallowing/ Nutritional Status
 Instructor Guide Section K Swallowing/ Nutritional Status Objectives State the intent of Section K Swallowing and Nutritional Status. Describe how to conduct an assessment of a resident s nutritional status.
Instructor Guide Section K Swallowing/ Nutritional Status Objectives State the intent of Section K Swallowing and Nutritional Status. Describe how to conduct an assessment of a resident s nutritional status.
Chapter 27 & 28. Key Terms. Digestive System. Fig. 27-1, p. 443 Also known as the Gastrointestinal System (GI system)
 Chapter 27 & 28 Nutrition & Fluids Key Terms Aspiration Dehydration Edema Dysphagia Gastrostomy tube Intravenous therapy (IV) Digestive System Fig. 27-1, p. 443 Also known as the Gastrointestinal System
Chapter 27 & 28 Nutrition & Fluids Key Terms Aspiration Dehydration Edema Dysphagia Gastrostomy tube Intravenous therapy (IV) Digestive System Fig. 27-1, p. 443 Also known as the Gastrointestinal System
COMMUNICATION. Communication and Swallowing post Tracheostomy. Role of SLT. Impact of Tracheostomy. Normal Speech. Facilitating Communication
 Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
Dysphagia (swallowing problems)
 Dysphagia (swallowing problems) Speech and Language Therapy Department Patient Information Leaflet Introduction This leaflet is for people who have dysphagia. It gives information on what this condition
Dysphagia (swallowing problems) Speech and Language Therapy Department Patient Information Leaflet Introduction This leaflet is for people who have dysphagia. It gives information on what this condition
Chapter 23. Nutrition Needs. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 23 Nutrition Needs Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 23.1 Define the key terms and key abbreviations in this chapter. Explain the purpose and use of the MyPlate symbol.
Chapter 23 Nutrition Needs Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 23.1 Define the key terms and key abbreviations in this chapter. Explain the purpose and use of the MyPlate symbol.
The importance of eating and drinking for people living in care homes
 The importance of eating and drinking for people living in care homes Aims of the training What is malnutrition Reasons for malnutrition Consequences of malnutrition and dehydration Food First and food
The importance of eating and drinking for people living in care homes Aims of the training What is malnutrition Reasons for malnutrition Consequences of malnutrition and dehydration Food First and food
1. With your toothbrush brush the top and sides of your tongue, while your tongue is sitting on the floor of your mouth.
 EXERCISES FOR THE TONGUE TONGUE BRUSHING 1. With your toothbrush brush the top and sides of your tongue, while your tongue is sitting on the floor of your mouth. 2. Repeat the individual sections 5 times
EXERCISES FOR THE TONGUE TONGUE BRUSHING 1. With your toothbrush brush the top and sides of your tongue, while your tongue is sitting on the floor of your mouth. 2. Repeat the individual sections 5 times
Oral care & swallowing
 Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
NUTRITION CARE ALERTS
 APPENDIX 10 A NUTRITION CARE ALERTS and for Caregivers in Nursing Facilities or at Home Proper nutrition care is vital to the health and well-being of nursing facility residents and seniors living in their
APPENDIX 10 A NUTRITION CARE ALERTS and for Caregivers in Nursing Facilities or at Home Proper nutrition care is vital to the health and well-being of nursing facility residents and seniors living in their
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Feeding Assistant Training Session #2
 Feeding Assistant Training Session #2 Dr. Heidi J. Silver, PhD, RDN Mrs. Abbie Hudson, BS, RDN Vanderbilt Center for Quality Aging & Qsource Vanderbilt Center for Human Nutrition Why is Nutrition Important?
Feeding Assistant Training Session #2 Dr. Heidi J. Silver, PhD, RDN Mrs. Abbie Hudson, BS, RDN Vanderbilt Center for Quality Aging & Qsource Vanderbilt Center for Human Nutrition Why is Nutrition Important?
How Speech and Swallowing are Affected with ALS
 Patient Education How Speech and Swallowing are Affected with ALS This handout describes how ALS affects speech and swallowing. For speech issues it covers tips for listeners and speakers and what can
Patient Education How Speech and Swallowing are Affected with ALS This handout describes how ALS affects speech and swallowing. For speech issues it covers tips for listeners and speakers and what can
DEPARTMENT OF HEALTH AND HUMAN SERVICES CENTERS FOR MEDICARE & MEDICAID SERVICES Dental Status and Services Critical Element Pathway
 Use this pathway for a resident having oral/dental problems such as broken, carious, or loose teeth; inflamed gums; mouth sores or mouth pain; denture problems; or chewing problems. If mouth or facial
Use this pathway for a resident having oral/dental problems such as broken, carious, or loose teeth; inflamed gums; mouth sores or mouth pain; denture problems; or chewing problems. If mouth or facial
PATIENT COMPLIANCE TIP SHEET Dietary Guidelines Following a Stroke
 PATIENT COMPLIANCE TIP SHEET Dietary Guidelines Following a Stroke A stroke may be very frightening to both the patient and family. It helps to remember that stroke survivors usually have at least some
PATIENT COMPLIANCE TIP SHEET Dietary Guidelines Following a Stroke A stroke may be very frightening to both the patient and family. It helps to remember that stroke survivors usually have at least some
Laryngoscopy Examinations
 Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Video Fluoroscopic Swallowing Exam (VFSE)
 Scan for mobile link. Video Fluoroscopic Swallowing Exam (VFSE) A video fluoroscopic swallowing exam (VFSE) uses a form of real-time x-ray called fluoroscopy to evaluate a patient s ability to swallow
Scan for mobile link. Video Fluoroscopic Swallowing Exam (VFSE) A video fluoroscopic swallowing exam (VFSE) uses a form of real-time x-ray called fluoroscopy to evaluate a patient s ability to swallow
New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol
 New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol Steven B. Leder, Ph.D. Yale University School of Medicine New Haven, Connecticut Debra M. Suiter, Ph.D. VA Medical Center-Memphis
New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol Steven B. Leder, Ph.D. Yale University School of Medicine New Haven, Connecticut Debra M. Suiter, Ph.D. VA Medical Center-Memphis
Nutricia. Nutrition and Dysphagia
 Nutricia Nutrition and Dysphagia 1 Introduction What is Dysphagia? The inability to swallow normally or freely. Disorder in the swallowing process that does not allow safe passing of food from the mouth
Nutricia Nutrition and Dysphagia 1 Introduction What is Dysphagia? The inability to swallow normally or freely. Disorder in the swallowing process that does not allow safe passing of food from the mouth
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA
 RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
Post Operative Instructions: Wisdom Teeth
 The removal of impacted teeth is a serious surgical procedure. Post-operative care is very important. Unnecessary pain and the complications of infection and swelling can be minimized if the instructions
The removal of impacted teeth is a serious surgical procedure. Post-operative care is very important. Unnecessary pain and the complications of infection and swelling can be minimized if the instructions
Chef Rick Schmitt, CDM, CFPP Assistant Dining Director/Executive Chef Westminster Towers Rock Hill, SC
 Chef Rick Schmitt, CDM, CFPP Assistant Dining Director/Executive Chef Westminster Towers Rock Hill, SC Water/Hydration Food/Nutrition Shelter/Security Love/Acceptance/Belonging Definition A chronic or
Chef Rick Schmitt, CDM, CFPP Assistant Dining Director/Executive Chef Westminster Towers Rock Hill, SC Water/Hydration Food/Nutrition Shelter/Security Love/Acceptance/Belonging Definition A chronic or
Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
 National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
Dysphagia. A Problem Swallowing Foods or Liquids
 Dysphagia A Problem Swallowing Foods or Liquids What Is Dysphagia? If you have a problem swallowing foods or liquids, you may have dysphagia. It has a number of causes. Your doctor can find out what is
Dysphagia A Problem Swallowing Foods or Liquids What Is Dysphagia? If you have a problem swallowing foods or liquids, you may have dysphagia. It has a number of causes. Your doctor can find out what is
Patient and Family Resource Guide to ALS. Section 6. Nutritional Support
 Patient and Family Resource Guide to ALS Section 6 Nutritional Support 6 5550 W. Touhy Avenue, Skokie IL, 60077 847 679 3311 lesturnerals.org info@lesturnerals.org Nutritional Support Many factors can
Patient and Family Resource Guide to ALS Section 6 Nutritional Support 6 5550 W. Touhy Avenue, Skokie IL, 60077 847 679 3311 lesturnerals.org info@lesturnerals.org Nutritional Support Many factors can
Orofacial function of persons having
 Orofacial function of persons having Report from questionnaires 24 questionnaires Synonym There are 186 (July 2013) different types of (ED), of which hypohidrotic ectodermal dysplasia (HED) is the most
Orofacial function of persons having Report from questionnaires 24 questionnaires Synonym There are 186 (July 2013) different types of (ED), of which hypohidrotic ectodermal dysplasia (HED) is the most
MDS 3.0. Acronyms. Terminology & Definitions 8/22/2016 CAA CAT ADL BMI BIMS PT/OT/ST QI QM MDS RAI OMRA (SOT) OBRA RUG CMS COT OMRA ARD
 MDS 3.0 Acronyms MDS RAI OMRA (SOT) OBRA RUG CMS COT OMRA ARD CAA CAT ADL BMI BIMS PT/OT/ST QI QM Terminology & Definitions Active Disease Diagnosis Acute Change in Mental Status Period Reference Date
MDS 3.0 Acronyms MDS RAI OMRA (SOT) OBRA RUG CMS COT OMRA ARD CAA CAT ADL BMI BIMS PT/OT/ST QI QM Terminology & Definitions Active Disease Diagnosis Acute Change in Mental Status Period Reference Date
Applied physiology. 7- Apr- 15 Swallowing Course/ Anatomy and Physiology
 Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
Management of Dysphagia in Stroke. An Educational Manual for the Dysphagia Screening Professional in the Long-Term Care Setting
 Management of Dysphagia in Stroke An Educational Manual for the Dysphagia Screening Professional in the Long-Term Care Setting Management of Dysphagia in Stroke: An Educational Manual for the Dysphagia
Management of Dysphagia in Stroke An Educational Manual for the Dysphagia Screening Professional in the Long-Term Care Setting Management of Dysphagia in Stroke: An Educational Manual for the Dysphagia
Puree Diet. Patient Information Leaflet.
 Information Prescriptions Information Prescriptions are a quick and easy way to provide information about your condition and local services. www.nhs.uk/ips How can I help reduce healthcare associated infections?
Information Prescriptions Information Prescriptions are a quick and easy way to provide information about your condition and local services. www.nhs.uk/ips How can I help reduce healthcare associated infections?
Understanding your child s videofluoroscopic swallow study report
 Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Eating and drinking in dementia
 Eating and drinking in dementia Patient infomation Nutrition and dietetics Clinical and diagnostic services centre This leaflet offers practical advice on how you can help someone with early stage dementia
Eating and drinking in dementia Patient infomation Nutrition and dietetics Clinical and diagnostic services centre This leaflet offers practical advice on how you can help someone with early stage dementia
Surgical Instructions. Wisdom Tooth TREASURE VALLEY ORAL & FACIAL SURGERY
 TREASURE VALLEY ORAL & FACIAL SURGERY Surgical Instructions Wisdom Tooth 1000 North Curtis Road, Suite 103 Boise, ID 83706 Phone: 208-343-0909 Fax: 208-343-6282 TREASURE VALLEY ORAL & FACIAL SURGERY AFTER
TREASURE VALLEY ORAL & FACIAL SURGERY Surgical Instructions Wisdom Tooth 1000 North Curtis Road, Suite 103 Boise, ID 83706 Phone: 208-343-0909 Fax: 208-343-6282 TREASURE VALLEY ORAL & FACIAL SURGERY AFTER
Dementia Care A Practical Guide to Swallowing Problems
 Nutrition and Dietetics Dementia Care A Practical Guide to Swallowing Problems People with dementia can experience difficulties with chewing and swallowing as their condition progresses. This may affect
Nutrition and Dietetics Dementia Care A Practical Guide to Swallowing Problems People with dementia can experience difficulties with chewing and swallowing as their condition progresses. This may affect
Pediatric Feeding and Swallowing Center Intake Form
 Inova Loudoun Hospital Pediatric Feeding and Swallowing Center Intake Form Patient Name: Form Completed by: Today s Date: Relationship to client: Feeding Concerns What is your major feeding concern? Please
Inova Loudoun Hospital Pediatric Feeding and Swallowing Center Intake Form Patient Name: Form Completed by: Today s Date: Relationship to client: Feeding Concerns What is your major feeding concern? Please
Documentation ASSOCIATION OF NUTRITION AND FOOD PROFESSIONALS. Amber Gordon RD LD Consultant Dietitian, Carolina Nutrition Consultants
 Documentation ASSOCIATION OF NUTRITION AND FOOD PROFESSIONALS Amber Gordon RD LD Consultant Dietitian, Carolina Nutrition Consultants Objective Review nutrition documentation with focus on individualization
Documentation ASSOCIATION OF NUTRITION AND FOOD PROFESSIONALS Amber Gordon RD LD Consultant Dietitian, Carolina Nutrition Consultants Objective Review nutrition documentation with focus on individualization
Nutrition and Feeding
 Nutrition and Feeding Introduction Within Neuromuscular conditions there can be a range of issues with feeding and nutrition. This may vary with different diagnoses. Normal, healthy growth is measured
Nutrition and Feeding Introduction Within Neuromuscular conditions there can be a range of issues with feeding and nutrition. This may vary with different diagnoses. Normal, healthy growth is measured
Swallowing after a Total Laryngectomy
 Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
SAFETYNET LEARNING TOOLS
 SAFETYNET LEARNING TOOLS Topic: Respiratory Illness Use the materials in this document to help others learn more about respiratory illness. LEARNING TOOLS: 1. Understanding Respiratory Illness PowerPoint
SAFETYNET LEARNING TOOLS Topic: Respiratory Illness Use the materials in this document to help others learn more about respiratory illness. LEARNING TOOLS: 1. Understanding Respiratory Illness PowerPoint
Short-Term Side Effects from Head and Neck Radiation
 PATIENT EDUCATION patienteducation.osumc.edu Short-Term Side Effects from Head and Neck Radiation Side effects are problems caused by radiation therapy. These problems are different for each person and
PATIENT EDUCATION patienteducation.osumc.edu Short-Term Side Effects from Head and Neck Radiation Side effects are problems caused by radiation therapy. These problems are different for each person and
Dysphagia goes International
 Sponsor Disclosure: Support for this presentation was provided by the Foodservice Express division of Med-Diet, Inc. The material herein is for educational purposes only. Reproduction or distribution of
Sponsor Disclosure: Support for this presentation was provided by the Foodservice Express division of Med-Diet, Inc. The material herein is for educational purposes only. Reproduction or distribution of
Dysphagia goes International
 Sponsor Disclosure: Support for this presentation was provided by the Foodservice Express division of Med-Diet, Inc. The material herein is for educational purposes only. Reproduction or distribution of
Sponsor Disclosure: Support for this presentation was provided by the Foodservice Express division of Med-Diet, Inc. The material herein is for educational purposes only. Reproduction or distribution of
 - speech-~echanism Assessment tion, a small dental mirror and gauze pads may be necessary. Before putting the gloves on, clean the table with disinfectant and wash your hands thoroughly with antibacterial
- speech-~echanism Assessment tion, a small dental mirror and gauze pads may be necessary. Before putting the gloves on, clean the table with disinfectant and wash your hands thoroughly with antibacterial
Throat and Jaw Exercise Training to Treat Obstructive Sleep Apnea
 Throat and Jaw Exercise Training to Treat Obstructive Sleep Apnea Department of Health and Nutritional Science South Dakota State University, Brookings, SD This video was prepared by the Exercise Science
Throat and Jaw Exercise Training to Treat Obstructive Sleep Apnea Department of Health and Nutritional Science South Dakota State University, Brookings, SD This video was prepared by the Exercise Science
Nutrition and Fluid Balance
 90 14 Nutrition and Fluid Balance 1. Define important words in this chapter 2. Describe common nutritional problems of the elderly and the chronically ill 3. Describe cultural factors that influence food
90 14 Nutrition and Fluid Balance 1. Define important words in this chapter 2. Describe common nutritional problems of the elderly and the chronically ill 3. Describe cultural factors that influence food
Feeding and Swallowing Problems in the Child with Special Needs
 Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Also there may be some increased saliva production by the autonomic nervous system.
 Introduction Possible problems What can be done? Too much saliva Too little saliva Thick saliva Further help Saliva Control Introduction This fact sheet is aimed at those affected by MSA and experiencing
Introduction Possible problems What can be done? Too much saliva Too little saliva Thick saliva Further help Saliva Control Introduction This fact sheet is aimed at those affected by MSA and experiencing
Developments on the International Dysphagia Diet Standardisation Initiative, IDDSI
 Developments on the International Dysphagia Diet Standardisation Initiative, IDDSI Dr Ben Hanson, University College London UCL 1. Where we are now timeline and what s happening 2. IDDSI: What? and Why?
Developments on the International Dysphagia Diet Standardisation Initiative, IDDSI Dr Ben Hanson, University College London UCL 1. Where we are now timeline and what s happening 2. IDDSI: What? and Why?
Dysphagia Diet Texture B Thin Puree
 The Clatterbridge Cancer Centre NHS Foundation Trust Dysphagia Diet Texture B Thin Puree Rehabilitation & Support A guide for patients and carers Contents Swallowing...1 Swallowing problems...1 Who can
The Clatterbridge Cancer Centre NHS Foundation Trust Dysphagia Diet Texture B Thin Puree Rehabilitation & Support A guide for patients and carers Contents Swallowing...1 Swallowing problems...1 Who can
2.3 Managing Symptoms of PSP: Swallowing, Eating Difficulties and Saliva Control
 2.3 Managing Symptoms of PSP: Swallowing, Eating Difficulties and Saliva Control This Help Sheet gives further information about the swallowing, eating and saliva control problems experienced by people
2.3 Managing Symptoms of PSP: Swallowing, Eating Difficulties and Saliva Control This Help Sheet gives further information about the swallowing, eating and saliva control problems experienced by people
1 ANIMALS Digestive System Oral Cavity and Esophagus.notebook January 06, 2016
 The Human Digestive System 1 The Human Digestive System 2 You are a tube inside a tube 3 The Digestive System The Four Stages of Food Processing 1. Ingestion the taking in or eating of food 2. Digestion
The Human Digestive System 1 The Human Digestive System 2 You are a tube inside a tube 3 The Digestive System The Four Stages of Food Processing 1. Ingestion the taking in or eating of food 2. Digestion
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices OPTICS
 OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version June 16 2014 Page 1 of 11 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version June 16 2014 Page 1 of 11 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices OPTICS
 OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version April 26 th 2016 Page 1 of 12 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version April 26 th 2016 Page 1 of 12 This information booklet was originally
WILTSHIRE FARM FOODS
 WILTSHIRE FARM FOODS WILTSHIRE FARM FOODS NACC South West Specialised Nutrition Presentation December 2018 What is IDDSI? Why IDDSI? What does it mean? Nutrition Labels Timescales WILTSHIRE Agenda FARM
WILTSHIRE FARM FOODS WILTSHIRE FARM FOODS NACC South West Specialised Nutrition Presentation December 2018 What is IDDSI? Why IDDSI? What does it mean? Nutrition Labels Timescales WILTSHIRE Agenda FARM
What is Dysphagia? An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION What is Dysphagia? An information guide What is Dysphagia? If someone has dysphagia, this means they have difficulty in swallowing. Dysphagia
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION What is Dysphagia? An information guide What is Dysphagia? If someone has dysphagia, this means they have difficulty in swallowing. Dysphagia
Oesophageal and gastric stents Patient Information leaflet
 Oesophageal and gastric stents Patient Information leaflet Why have you been given this leaflet? This leaflet has been written to help you understand why it has been recommended that you have a stent.
Oesophageal and gastric stents Patient Information leaflet Why have you been given this leaflet? This leaflet has been written to help you understand why it has been recommended that you have a stent.
Anal Atresia FACTS: There is no known cause for anal atresia. Children with anal atresia can lead very happy lives post surgery!
 Anal Atresia FACTS: Anal atresia affects 1 in 5,000 births and is slightly more common in boys. There is no known cause for this condition. With anal atresia, any of the following can occur: The anal passage
Anal Atresia FACTS: Anal atresia affects 1 in 5,000 births and is slightly more common in boys. There is no known cause for this condition. With anal atresia, any of the following can occur: The anal passage
For all the places our children have meal times.
 Donna Edwards, MA CCC SLP, BCS S Board Certified Specialist in Swallowing and Swallowing Disorders ASHA Fellow Dayton Children s Hospital Dayton, OH For Children! For Parents! For Professionals! For the
Donna Edwards, MA CCC SLP, BCS S Board Certified Specialist in Swallowing and Swallowing Disorders ASHA Fellow Dayton Children s Hospital Dayton, OH For Children! For Parents! For Professionals! For the
Nasogastric Tube Patient Passport
 Nutrition and Dietetics Department Nasogastric Tube Patient Passport Please bring this booklet with you for all tube changes Patient Information If you need this information in another format or language
Nutrition and Dietetics Department Nasogastric Tube Patient Passport Please bring this booklet with you for all tube changes Patient Information If you need this information in another format or language
2013 Charleston Swallowing Conference
 Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Nutrition and the Teeth for Patients receiving Radiotherapy to the Head and Neck
 Nutrition and the Teeth for Patients receiving Radiotherapy to the Head and Neck Name: Date: Provided by: Contact: Introduction The aim of this booklet is to ensure your dental and general health is as
Nutrition and the Teeth for Patients receiving Radiotherapy to the Head and Neck Name: Date: Provided by: Contact: Introduction The aim of this booklet is to ensure your dental and general health is as
Long Term Toxicities of Head & Neck Cancer Therapies. Faith Mutale Abramson Cancer Center University of Pennsylvania
 Long Term Toxicities of Head & Neck Cancer Therapies Faith Mutale Abramson Cancer Center University of Pennsylvania Head & Neck Cancer 2-3% of all cancers 1-2% of all cancer deaths Incidence includes:
Long Term Toxicities of Head & Neck Cancer Therapies Faith Mutale Abramson Cancer Center University of Pennsylvania Head & Neck Cancer 2-3% of all cancers 1-2% of all cancer deaths Incidence includes:
Module 2: Facilitator instructions for Airway & Breathing Skills Station
 Module 2: Facilitator instructions for Airway & Breathing Skills Station 1. Preparation a. Assemble equipment beforehand. b. Make sure that you have what you need and that it is functioning properly. 2.
Module 2: Facilitator instructions for Airway & Breathing Skills Station 1. Preparation a. Assemble equipment beforehand. b. Make sure that you have what you need and that it is functioning properly. 2.
Guidance for Oral Nutritional Support in patients with disease related malnutrition
 Guidance for Oral Nutritional Support in patients with disease related malnutrition NICE (CG3, 6) define oral nutrition support (ONS) as the modification of food and fluid by: fortifying food with protein,
Guidance for Oral Nutritional Support in patients with disease related malnutrition NICE (CG3, 6) define oral nutrition support (ONS) as the modification of food and fluid by: fortifying food with protein,
Filling the Nutritional Gap in Dysphagia
 Filling the Nutritional Gap in Dysphagia Krystel Ouaijan, RDN, MSc Nutrition Support Dietitian in Saint George Hospital UMC PhD in University of Geneva Krystel Ouaijan - Dubai -2018 1 Patient Profiles
Filling the Nutritional Gap in Dysphagia Krystel Ouaijan, RDN, MSc Nutrition Support Dietitian in Saint George Hospital UMC PhD in University of Geneva Krystel Ouaijan - Dubai -2018 1 Patient Profiles
The Digestive System or tract extends from the mouth to the anus.
 The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
The Digestive System or tract extends from the mouth to the anus. FUNCTION The Digestive System breaks down and absorbs food materials e.g. amino acids, glucose DEFINITIONS: Ingestion: Ingestion is the
Feeding Evaluation Case History Form
 Feeding Evaluation Case History Form Child s Name: Date of Birth: Current Age: Person Completing Form & Relationship to patient: Date: The following information will be read by the therapist who is performing
Feeding Evaluation Case History Form Child s Name: Date of Birth: Current Age: Person Completing Form & Relationship to patient: Date: The following information will be read by the therapist who is performing
Having a PEG tube inserted
 Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
TABLE OF CONTENTS TABLE OF CONTENTS... 1 ORAL HEALTH IS AN IMPORTANT PART OF TOTAL HEALTH... 2 DENTAL DECAY... 2
 TABLE OF CONTENTS TABLE OF CONTENTS... 1 ORAL HEALTH IS AN IMPORTANT PART OF TOTAL HEALTH... 2 DENTAL DECAY... 2 PRIMARY TEETH (BABY TEETH, DECIDUOUS TEETH)... 2 EARLY CHILDHOOD TOOTH DECAY... 2 CAREGIVER
TABLE OF CONTENTS TABLE OF CONTENTS... 1 ORAL HEALTH IS AN IMPORTANT PART OF TOTAL HEALTH... 2 DENTAL DECAY... 2 PRIMARY TEETH (BABY TEETH, DECIDUOUS TEETH)... 2 EARLY CHILDHOOD TOOTH DECAY... 2 CAREGIVER
How to look after your mouth. Cancer Services Information for patients
 How to look after your mouth Cancer Services Information for patients i Is my mouth at risk? There are many things that can affect your mouth. If you answer yes to any of the following, you may be at risk
How to look after your mouth Cancer Services Information for patients i Is my mouth at risk? There are many things that can affect your mouth. If you answer yes to any of the following, you may be at risk
Nutrition at the Bedside
 Nutrition at the Bedside Linda Varnell, RD, LDN Clinical Dietitian February 26, 2010 Objectives Identify risk factors for malnutrition in the older adult Recognize physical signs of malnutrition Gain skills
Nutrition at the Bedside Linda Varnell, RD, LDN Clinical Dietitian February 26, 2010 Objectives Identify risk factors for malnutrition in the older adult Recognize physical signs of malnutrition Gain skills
Dysphagia. What is Dysphagia? Diagnosis and Treatment
 Dysphagia C A R E & M A N AG E M E N T S O L U T I O N S What is Dysphagia? Diagnosis and Treatment 1 Diagnosis contents and Treatment 2What is Dysphagia? 3 What is Dysphagia? KAPITEX are specialists in
Dysphagia C A R E & M A N AG E M E N T S O L U T I O N S What is Dysphagia? Diagnosis and Treatment 1 Diagnosis contents and Treatment 2What is Dysphagia? 3 What is Dysphagia? KAPITEX are specialists in
