JMSCR Vol 04 Issue 11 Page November 2016
|
|
|
- Thomasina Small
- 5 years ago
- Views:
Transcription
1 Impact Factor Index Copernicus Value: ISSN (e) x ISSN (p) DOI: Potentially Inappropriate Medication Use among Elderly Inpatients at a Teaching Hospital in South India Authors Dr Steve Paul Manjaly 1, Dr Geetha Francis 2, Dr Betsy Mathew 3 1 MBBS. DNB (Medicine), DGM (Geriatric Medicine), Assistant Professor, Department of Medicine, Jubilee Mission Medical College and Research Institute, Thrissur, Kerala 2 MD (Medicine), Associate Professor, Department of Medicine, St John's Medical College, Bangalore francis.geetha@gmail.com 3 MBBS MD (Medicine), DGM (Geriatric Medicine), Professor and Head, Division of Geriatric Medicine, Department of Medicine, St John's Medical College, Bangalore betsy123m@hotmail.com Corresponding Author Dr Steve Paul Manjaly MBBS. DNB (Medicine), DGM (Geriatric Medicine), Assistant Professor, Department of Medicine, Jubilee Mission Medical College and Research Institute, Thrissur, Kerala ABSTRACT BACKGROUND: Use of inappropriate medications among elderly is common. An association between potentially inappropriate medication (PIM) use in elderly and adverse outcomes such as impaired muscle strength, functional status, increased healthcare expenditure, and increased risk of hospitalization and death has been demonstrated. Yet there are few studies addressing this issue. OBJECTIVE: This study focuses on the prevalence of the use of potentially inappropriate medications in hospitalized elderly. DESIGN: A retrospective observational study was done between June and December 2012 involving 150 patients. Patient data including period of hospital stay, medical illnesses and medication list at discharge were obtained from the in-patient records. The chi-squared test for categorical variables was used to compare the characteristics of participants receiving and not receiving inappropriate medications. SETTING: The study collected data from 150 patients admitted to a teaching hospital at Bangalore, Karnataka. PATIENTS: The sample was composed of 150 patients aged > 60 years admitted with multiple co morbidities. MEASUREMENTS: The percentage of patients prescribed PIMs as defined using a modified Beers list was measured. Multivariable-adjusted odds ratios for PIM use were computed. RESULTS: Of the 150 patients, 17.3% received at least 1 PIM, and 7% received 3 or more. Most common category of PIM use were Prazosin, followed by benzodiazepines PIM use was directly associated with no: of comorbidities and Polypharmacy CONCLUSION: There is a widespread use of potentially inappropriate medications among elderly patients in the population studied. Physicians should be more aware of the Beer s criteria when treating the elderly. KEYWORDS: Potentially inappropriate medications (PIM), Beers criteria (BC), Polypharmacy, geriatric, elderly. Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14028
2 INTRODUCTION India, now home to 1.2 billion people, is projected to overtake China in about a decade to become the world s most populous country. Between 2010 and 2050, the number of those aged above 60 years is also is expected to increase from 7 percent to 14 percent of the total population. Presently we have about 100 million elderly in India. Elderly suffer from multiple illnesses both acute and chronic, requiring multiple hospital visits and medications from multiple specialists. Medications can be considered inappropriate when their risk outweighs their benefit. The pharmacokinetics and pharmacodynamics of drugs is different in elderly and knowledge of geriatric pharmacology is of utmost importance in prescribing for the elderly. The Beers criteria, named after Mark Beers, MD, lists medications that should generally be avoided in older adults. First evolved in 1991 by 13 pharmaco therapeutic and geriatric specialists as a tool for safer medication prescribing in frail older adults residing in nursing homes, it was revised in 1997 and again in 2003 to apply to all persons aged 65 years, and was most recently updated in The final updated Beers criteria encompasses fifty-three medications or medication classes, which are divided into three categories: potentially inappropriate medications (PIM) and classes to avoid in older adults, those to avoid in older adults with certain diseases and syndromes that these drugs can exacerbate, and finally medications to be used with caution in older adults. 1, I Polypharmacy (defined as the concurrent use of multiple medications) is common in the elderly and its prevalence ranges from 33% to 58%. 1, 2 Unfortunately, polypharmacy may cause problems such as drugdrug interactions, non-adherence to therapy and adverse drug effects. Objective of Study: An association between potentially inappropriate medication (PIM) use in elderly and adverse outcomes such as impaired muscle strength and functional status, increased healthcare expenditure, and increased risk of hospitalization and death has been demonstrated Use of inappropriate medications among elderly is common both in ambulatory and hospitalized settings. 6 7 Yet there are few studies addressing this issue among the elderly in India. Our objectives were to study the prevalence and predictors of the use of potentially inappropriate medications in hospitalized elderly and the associations between PIM use and comorbidities, polypharmacy, and duration of hospitalization. MATERIALS AND METHODS This is a retrospective study conducted in a 1200 bedded tertiary care teaching hospital in Karnataka, South India. 150 patients discharged from medical wards between June and December 2012 were included. Patient data including period of hospital stay, medical illnesses and medication list at discharge were obtained from the in-patient records. Wherever the medication list at discharge was unavailable, medications ordered on the last day of admission were analyzed. The medication appropriateness was decided according to Beers criteria. The number of Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14029
3 discharge medications included not only oral and parenteral medications but also inhalers, and topical medicines. Combination medications were counted separately; insulin and multivitamins were counted as a single medication. The patients were grouped according to their age into young old (65-74 yrs), old old (75-85yrs) and oldest old (>85 yrs). The presence of chronic medical illnesses like diabetes, hypertension, chronic obstructive pulmonary disease, cerebrovascular disease and ischemic heart disease were identified and the use of inappropriate medications was assessed in each group. Whenever a potentially inappropriate medicine was identified, it was classified according to the Beers criteria into the three categories mentioned above. The drugs were not counted as inappropriate if they were used in a palliative setting or if there was no other alternative to its use. Polypharmacy was considered as the administration of 5 drugs per day. Data was assessed using the statistical package for social sciences, version 16. The chi-squared test for categorical variables was used to compare the characteristics of participants receiving and not receiving inappropriate medications. A probability value of less than 0.05 was considered statistically significant. RESULTS Patient characteristics (Table 1) A total of 150 patient records were analyzed. Out of the total 150 patients, 120 (80%) were aged years (young old), 22 (14.7%) were in the age group of years (old old), and 8 (5.3%) were aged above 85 years (oldest old). The mean age of the patients in the study group was 67.8 years. Of the 150 patients, 56 (37.3%) were females and 94 (62.6%) were males. The average number of chronic co-morbid medical illnesses per patient was 4.28 (±2.235). The commonest co-morbid illnesses were hypertension (n=80) (53%) and diabetes (n=78) (52%). The average duration of hospital stay was 8.06 days (mean duration =8 days) Polypharmacy (Table 2) 110 (73.3% ) patients were subject to polypharmacy.. The mean number of medications consumed per day by the patients in the study group was 6.7 ± patients consumed <5 medications, 84 consumed between 5 to 10 medications, and 26 regularly consumed 10 medications per day. The average number of medications taken by elderly men (n=94) was 6.79 (± 3.2) per day and elderly women (n=56) were taking 6.62 (± 2.9) medications per day. The patients of the oldest old category ( 85 years n=8) had an average of 7.38 medications/day. The young old (n=120) had a mean of 6.72 medications per day and the old old (n=22) had a mean of 6.5 medications per day. The prevalence of polypharmacy was higher in those patients who had multiple co morbid illnesses. 110 patients were subject to polypharmacy. A patient who was subject to polypharmacy had an average of 4.9 comorbid illnesses, whereas the others had an average of 2.5 comorbid illnesses. Potentially inappropriate medications (Table 3) Of the total number of 150 patients in the study group, one of six (26) were taking a potentially inappropriate medication according to the Beers list. (p=0.830) Of the 26 patients taking a PIM, men constituted the majority, 17 (65.3%) compared to women, 9 (34.7%). Eighteen of them belonged to the young old (n=120), 3 of the old old (n=22) and 5 of them belonged to the oldest old category (n= 8). Nineteen (73%) were prescribed a single inappropriate medication, one of five (5) patients were prescribed 2 potentially inappropriate medicines and one of thirteen (2) were taking 3 drugs that were potentially inappropriate. Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14030
4 Among the potentially inappropriate medications, the most common ones belonged to those that acted on the cardiovascular system, (13) (50%), of which antihypertensives (prazocin) constituted the majority (6)(46%) followed by anti arrhythmic ( amiodarone)(5) (38.4%) and vasodilators (hydralazine and nitrates)(2)(15.3%). The second commonest inappropriately prescribed drugs were those that acted on the central nervous system (30%), chiefly benzodiazepines (6) ( alprazolam) followed by anticholinergics. (amitryptiline). The maximum duration of hospital stay by any patient was 55 days, (0.7%) with most patients staying on an average duration of 8.1 (range 1-55). PIM users stayed on a higher average of 8.7 days when compared to the non- PIM users. (Mean=7.93) (p=0.602) The average number of medical illnesses seen in the group inappropriately prescribed was 5.7 (4.7, 6.7), whereas the group without any inappropriate medication was 3.97 (3.6, 4.3) (p<0.001). Of the 26 PIM users, majority (22) (84.6%) were hypertensives (Odds Ratio 6.3; C.I ), 10 (38.4%) had Ischemic heart disease,( Odds ratio 3.9; C.I ), 18 (69%) had diabetes, and the proportion of patients with chronic obstructive pulmonary disease and cerebrovascular disease were 9 (34.6%) and 2 (7.6%) respectively. Of these, Hypertension, (84.6%) (p <0.001) ischemic Heart disease (38.4%) (p=0.009) were significantly associated with the use of inappropriate medications. The prevalence of PIM use varied according to the co morbid illnesses. PIM use was highest in those with ischemic heart disease (10 of 27) (37%)(p=0.009), hypertension (22 of 80) (27.5%)(p=0.000) followed by diabetes (18 of 78)(23%)(p =0.053) and chronic lung disease (2 of 13)(15%) (p=0.88) PIM and polypharmacy Of the 110 patients who were subject to polypharmacy, 21 (19.09%) were using an inappropriate medication. Of the 40 patients who were not on polypharmacy, five had PIM use. (p = 0.34) The maximum number of medications a patient was prescribed was 16. (Range 1-16, Mean 6.73 ± 3.09) 25 were prescribed 10 medicines, and 85 were prescribed 5 medicines. Of the 26 PIM users, 21 (80.7%) were subject to polypharmacy with an average of 8 medicines (mean 8.12 ± 3.36) as compared to the non PIM users (Mean 6.44 ± 2.92). DISCUSSION The study demonstrates that of the total number of patients discharged from medical wards, 17.3 % were taking at least one inappropriate medication. (p=0.830). The prevalence of PIM use was significantly associated with increasing age (p <0.001) The prevalence of PIM use was lower than in international studies conducted on the use of inappropriate medications conducted among hospitalized elderly patients in Ireland (32%) 8, France (66%), 9 Switzerland (22.1%) 10, and Taiwan (23.7%) 11. Among studies conducted in India, our results were lower compared to ones conducted in other teaching hospitals in Karnataka- Bangalore 12, Mysore 1 but comparable to studies conducted in Punjab (18%) 2. The difference could be probably due to the differences in patient and disease characteristics, prescribing patterns, study settings and availability of medications listed in BC. As in other studies, the prescription of inappropriate medication had a significant association with increasing co morbidity The average number of medical illnesses seen in the group inappropriately prescribed was 5.77, whereas the group without any inappropriate medication was 3.97 ±2.05) Hypertension, (84.6%)(p Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14031
5 <0.001) ischemic Heart disease (38.4%)( p<0.001)were significantly associated with the use of inappropriate medications Among the chronic illnesses, Essential hypertension and Ischemic heart disease increased the odds of use of PIM, similar to other studies in India 20 5 The most commonly prescribed inappropriate medication in our study were antihypertensives, chiefly prazocin (46%), antiarrhythmics, amiodarone (38%) followed by drugs acting on the CNS, benzodiazepines (19 %), and anticholinergics (15% ). This was different from other studies 19-21,23 where drugs acting on the respiratory system comprised the majority of the inappropriate medications. The difference was probably due to the increased prevalence of hypertensives (53%) in the population. As in other studies, prescription of inappropriate medications had a statistically significant association with increasing age (>84 years), 21 with 5 of 8 patients receiving inappropriately prescribed medications. (p <0.001). Contrary to other studies, 21, 22, 23 we did not find any statistically significant association with inappropriate medication use and duration of hospital stay. Studies have shown that use of inappropriate medications is significantly associated with increased duration of hospital stay. 21,22,23 We did not find such an association, This could be attributed to improved drug monitoring or other factors that could influence duration of hospital stay e.g social factors, costs of hospitalization etc. Polypharmacy Our study found a higher prevalence of polypharmacy; compared to previous studies 1 in northern India 110 (73.3%) (p<0.001). The ninety four elderly men in the study population consumed a higher average number of medications compared to that of the elderly women (mean 6.85 vs 6.53, respectively). (p >0.001) The presence of diabetes, (n=78; mean 7.26), hypertension (n=80; mean 7.9), ischemic heart disease (n=27; mean 8.07) and chronic pulmonary illness (n= 33; mean 7.97) had a statistically significant association with polypharmacy use when compared to the patients with other co morbid illnesses. Of these, hypertension appeared to be the most important predictor of polypharmacy (p<0.001) A higher prevalence of potentially inappropriate medication use was seen among those with increasing number of medications. 26 patients who were taking inappropriate medicines were prescribed a higher average number of medications (mean 8.12 ± 3.36) when compared to among the 124 non PIM users. (Mean 6.44 ± 2.92) (p <0.02) Of the 26 patients who were inappropriately prescribed, 21 (80.7% ) were subject to polypharmacy, although they formed only 19 % of the study population (p 0.346) Inappropriate prescription was directly linked to polypharmacy. The prescription of inappropriate medications increased as the number of concurrent medications increased. This was similar to studies conducted in other hospital in Karnataka 19,20. When polypharmacy was defined as the use of 5 or more drugs, this association differed markedly. Only 21 of the total 110 were prescribed more than 5 medications, which was statistically insignificant, suggesting that a quantitative definition for polypharmacy was questionable. 6 Polypharmacy was however rampant in the study group, as is known from previous studies 7, 8 and this was directly linked to morbidity in our study group. This study is important because it shows that despite the existence of Beers criteria since 1987 and its regular updation, last in 2012, it still has not found its way into mainstream practice. Hence, the elderly continue to be prescribed those medicines that are known to have adverse effects in them. Every adverse event could be misdiagnosed and another drug added to alleviate the new symptom and this leads to the Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14032
6 prescribing cascade, 9 subsequently adding to polypharmacy. Patients are at an increased risk of receiving an inappropriate medication and having an adverse drug reaction (ADR), which may impact a patient's adherence to his or her medication regimen. Polypharmacy has also been reported to increase the risk of geriatric syndromes and morbidity/ mortality. 27,10 The prevalence of the use of inappropriate medications is a concern, because studies have shown to have negative consequences such as increased risk of falls 11, impaired activities of daily living 12, non adherence to medication 13 and increased medical costs. 14 The increased prescription of inappropriate medications in patients with hypertension and diabetes points to the increased prevalence of these illnesses in the Indian elderly population. Although our study did not prove any statistical association, the use of inappropriate medications increases with the increased duration of hospital stay 23., and was known to have significant association with adverse effects such as falls 32, 15, and cognitive dysfunction 16. Our study also had certain limitations. This was a retrospective study, based on a small sample size of 150 patients, with information on drugs prescribed obtained from case records. The drug prescription was obtained from the discharge summaries, and where the same was not available, from the last day of inpatient admission. This may not have been a true representation of inappropriate medication use, since the medication list at discharge would have largely been modified to suit the chronic illness, rather than during the acute period. The prescription of inappropriate medicine among the elderly was based on the updated Beers criteria Beers criteria do not address several other important aspects of inappropriate prescribing in older people, e.g. duplicate drug class prescriptions, harmful drug-drug interactions, inappropriate duration and frequency of therapy, and perhaps most importantly, drugs that are often omitted from older people s prescriptions. Beers criteria are not organized in such a way as to make them quick and easy for the busy prescribing physician or dispensing pharmacist to use. Further, errors in prescription writing, errors of commission and omission were not looked into. Other tools for drug prescription in the elderly such as START 17, STOPP 18 and IPET 19 (Improved Prescription in the Elderly Tool) would provide more insight on the use of inappropriate prescriptions in the elderly. Our data was obtained from patients admitted and discharged from medical wards. A review of the discharge medications of patients admitted from surgical specialties would probably have shown different results. Patients with chronic illnesses like osteoarthritis, osteoporosis were not represented adequately, not only because such patients visited the orthopedic department more frequently, but also because they were probably undiagnosed in the medical wards. Adverse drug events can be a cause and effect of inappropriate medication use. There was no data obtainable from the discharge records, and hence drug related events to inappropriate medications could not be studied. CONCLUSION Pharmacotherapy in the elderly requires a balance between inappropriate medication use and undertreatment. Interventions aimed at rational medication use in elderly Indians should focus on the predictors of use of inappropriate drugs. The need of physicians trained in Geriatric medicine is rising due to the changing patient characteristics in the Indian population scenario. Geriatricians are more likely to be aware of geriatric pharmacotherapy and its effects 20. There is a great scope for conducting intense research to determine inappropriate medication use and its health-related adverse consequences in the increasing Indian elderly population. Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14033
7 REFERENCES 1. Campanelli CM. American Geriatrics Society Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults: The American Geriatrics Society 2012 Beers Criteria Update Expert Panel. J Am Geriatr Soc. 2012; 60(4): John et al, A study on polypharmacy in senior Indian population, ijpcbs 2013, 3(1), Lau DT, Kasper JD, Potter DE, Lyles A, Bennett RG. Hospitalization and death associated with potentially inappropriate medication prescriptions among elderly nursing home residents. Arch Intern Med. 2005;165: Landi F, Russo A, Liperoti R, et al. Impact of inappropriate drug use on physical performance among a frail elderly population living in the community. Eur J Clin Pharmacol. 2007;63: Fu AZ, Liu GG, Christensen DB. Inappropriate medication use and health outcomes in the elderly. J Am Geriatr Soc. 2004;52: Aparasu RR, Fliginger SE. Inappropriate medication prescribing for the elderly by office-based physicians. Ann Pharmacother 1997;31: Goulding, Inappropriate Medication Prescribing for Elderly Ambulatory Care Patients, Arch Intern Med. 2004;164(3): Barry PJ, O Keefe N, O Connor KA et al. Inappropriate prescribing in the elderly: a comparison of the Beers criteria and the improved prescribing in the elderly tool (IPET) in acutely ill elderly hospitalised patients. J Clin Pharm Ther 2006; 31: Laroche ML, Charmes JP, Nouaille Y, Fourrier A, Merle L. Impact of hospitalisation in an acute medical geriatric unit on potentially inappropriate medication use. Drugs Aging 2006;23: Egger SS, Bachmann A, Hubmann N, Schlienger RG, Krδhenbόhl S. Prevalence of potentially inappropriate medication use in elderly patients: Comparison between general medical and geriatric wards. Drugs Aging 2006;23: Lin HY, Liao CC, Cheng SH, Wang PC, Hsueh YS. Association of potentially inappropriate medication use with adverse outcomes in ambulatory elderly patients with chronic diseases: Experience in a Taiwanese medical setting. Drugs Aging 2008;25: Veena D.R, Padma L, Sapna Patil. Drug prescribing pattern in elderly patients in a teaching hospital. IOSR Journal of Dental and Medical Sciences (JDMS). Volume 1, Issue 5 (Sep-Oct. 2012), PP Harugeri A, Joseph J, Parthasarathi G, Ramesh M, Guido S. Potentially inappropriate medication use in elderly patients: A study of prevalence and predictors in two teaching hospitals. J Postgrad Med 2010;56: Mandavi, Pramil Tiwari, Vinay Kapur. Inappropriate drug prescribing identified among Indian elderly hospitalized patients, Int J Risk Saf Med 2007; 19: Klarin I,Wimo A, Fastbom J. The association of inappropriate drug use with hospitalisation and mortality: a population based study of the very old. Drugs Aging 2005; 22: Jano E, Aparasu RR. Healthcare outcomes associated with Beers criteria: A systematic review. Ann Pharmacother. 2007;41: Rothberg et al. Potentially Inappropriate Medication Use in Hospitalized Elders, J Hosp Med : Viktil et al. Polypharmacy as commonly defined is an indicator of limited value in the assessment of drug-related problems, Br J Clin Pharmacol 63 : E.R. Hajjar et al. Polypharamcy in elderly patients. Am J Geriatr Pharmacother Dec; 5(4): Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14034
8 20. Shalini, Joshi MC et al. Study of polypharmacy and associated problems among elderly patients January;7(1):35-9. Accessed Feb 19, Cooney D, Pascuzzi K. Polypharmacy in the elderly: focus on drug interactions and adherence in hypertension. Clin Geriatr Med 2009;25: Espino DV, Bazaldua OV, Palmer RF, et al. Suboptimal medication use and mortality in an older adult communitybased cohort: Results from the Hispanic EPESE Study. J Gerontol A Biol Sci Med Sci. 2006;61: Berdot et al, Inappropriate medication use and risk of falls A prospective study in a large community-dwelling elderly cohort, BMC Geriatr. 2009; 9: Magaziner J, Cadigan DA, Fedder DO, Hebel JR. Medication use and functional decline among community dwelling older women. J Aging Health. 1989;1: Marcum and Gellad. Medication Adherence to Multidrug Regimens. Clin Geriatr Med 28 (2012) Sehgal, Bajwa SJS, Vishal et al. Polypharmacy and Potentially Inappropriate Medication Use as the Precipitating Factor in Readmissions to the Hospital. J Family Med Prim Care Apr-Jun; 2(2): Stacy et al, Potentially Inappropriate Prescribing of Benzodiazepines for Older Adults and Risk of Falls During a Hospital Stay: A Descriptive Study.Can J Hosp Pharm Jul-Aug; 62(4): Tsai R, Potentially Inappropriate Medication Use in Mild Cognitive Impairment (MCI) Patients: Results from the Kerala Einstein Study. J Am Geriatr Soc July; 60(7): Barry et al, START (screening tool to alert doctors to the right treatment) an evidence-based screening tool to detect prescribing omissions in elderly patients Age and Ageing 2007; 36: Hamilton et al, Inappropriate prescribing and adverse drug events in older people. BMC Geriatrics 2009, 9:5 31. Naugler CT, Brymer C, Stolee P, Arcese ZA (2000) Development and validation of an improved prescribing for the elderly tool. The Canadian Journal of Clinical Pharmacology, 7, M. Crotty, J Halbert, D Rowett et al. An outreach geriatric medication advisory service in residential aged care: a randomised controlled trial of case conferencing. Age Ageing 2004; 33: Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14035
9 GRAPHICS Table 1: Clinical and demographic characteristics of study subjects (n=150) Characteristics 1 Frequencies Ag category > (80.0) 22 (14.7) 8 (5.3) Sex Male Female 56 (37.3) 94 (62.7) Polypharmacy Used Less than 5 More than 5 40 (26.7) 110 (73.3) Number of PIMS (82.7) 19 (12.7) 5 (3.3) 2 (1.3) PIM No Yes 124 (82.7) 26 (17.3) Presence of co-morbidities Presence of Diabetes 78 (52.0) Presence of hypertension 80 (53.3) Presence of chronic lung disease 33 (22.0) Presence of IHD 27 (18.0) Presence of BPH 13 (8.7) Presence of stroke 13 (8.7) Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14036
10 Presence of chronic kidney disease 11 (7.3) Presence of heart failure 9 (6.0) Lower urinary tract symptoms 27 (18.0) Presence of Parkinson s disease 8 (5.3) Presence of seizures 6 (4.0) Presence of peptic ulcer 3 (2.0) Presence of delirium 3 (2.0) History of falls or fractures Present 4 (2.7) Presence of Syncope 1 (0.7) Presence of dementia 1 (0.7) Presence of insomnia Absent 150 (100) Presence of urinary incontinence Absent 150 (100) Presence of constipation Absent 150 (100) Stress or mixed urinary incontinence Absent 150 (100) Duration of hospital stay* 8.1 ± (4,9) Total number of problems* 4.3 ±2.2 4(3, 6) Number of medicines Used* 6.7 ± (4, 9) 1 Reported as number within parenthesis percentages; *-mean ± SD, median (25 th & 75 th percentile) Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14037
11 Table 2: Factors associated with poly pharmacy used: Poly-pharmacy used Characteristics Less than 5 More than 5 p value n=40 n=110 Age category (80.0) 88 (80.0) (12.5) 17 (15.5) >84 3 (7.5) 4 (4.5) Sex Male 17 (42.5) 39 (35.5) 0.43 Female 23 (57l5) 71 (64.5) Number of PIMS 0 35 (87.5) 89 (80.9) 1 5 (12.5) 14 (12.7) (4.5) (1.8) Pim 0 35 (87.5) 89 (80.9) (12.5) 21 (19.1) Presence of diabetes Present 15 (37.5) 63 (57.3) 0.03 Absent 25 (62.5) 47 (42.7) Presence of hypertension Present 10 (25.0) 70 (63.6) <0.001 Absent 30 (75.0) 40 (36.4) Presence of Chronic lung disease Present Absent 3 (7.5) 37 (92.5) 30 (27.3) 80 (72.7) 0.01 Presence of IHD Present 1 (2.5) 26 (23.6) Absent 39 (97.5) 84 (76.4) Duration of hospital stay* 5.5 ±2.5 5 (4, 7) 9.0 ± (4,10) Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14038
12 Total number of problems* 2.5 ± (1, 3) Number of medicines used* 3.1 ± ± (3, 6) 8.1 ± 2.4 <0.001 < (3, 4) 7 (6, 9) Reported as number within parenthesis percentages; *-mean ± SD, median (25 th & 75 th percentile); p values using chi-square Table 3: Factors Associated With PIM: PIM OR Characteristics Yes No 95% C.I p value Age category (69.2) 102(82.3) (11.5) 19(15.3) >84 5(19.2) 3(2.4) Sex Male 18(69.2) 76(61.3) Female 8(30.8) 48(38.7) Poly pharmacy 0 5(19.2) 35(28.2) (80.8) 89(71.8) Presence of diabetes 18(69.2) 60(48.4) Present 8(30.8) 64(51.6) Absent Presence of hypertension 22(84.6) 58(46.8) 6.3 <0.001 Present 4(15.4) 66(53.2) Absent Presence of Chronic lung disease Present Absent 9(34.6) 17(65.4) 24(19.4) 100(80.6) Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14039
13 Presence of IHD 10(38.5) 17(13.7) Present 16(61.5) 107(86.3) Absent Duration of hospital stay* 8.7± (4,11) 7.9±7.65 6(4,8) Total number of problems 5.77± ±2.05 <0.001 Number of medicines used* 6.4± ± (4,8) 9(5.75,10.25) Reported as number within parenthesis percentages; *-mean ± SD, median (25 th & 75 th percentile); p values using chi-square APPENDIX I BEERS CRITERIA FOR POTENTIALLY INAPPROPRIATE MEDICATION USE IN OLDER ADULTS TABLE 1: 2012 AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults Organ System/ Therapeutic Category/Drug(s) Recommendation, Rationale, Quality of Evidence (QE) & Strength of Recommendation (SR) Anticholinergics (excludes TCAs) First-generation antihistamines (as single agent or as part of combination products) Brompheniramine Carbinoxamine Chlorpheniramine Clemastine Cyproheptadine Dexbrompheniramine Dexchlorpheniramine Diphenhydramine (oral) Doxylamine Hydroxyzine Promethazine Triprolidine Antiparkinson agents Highly anticholinergic; clearance reduced with advanced age, and tolerance develops when used as hypnotic; increased risk of confusion, dry mouth, constipation, and other anticholinergic effects/toxicity. Use of diphenhydramine in special situations such as acute treatment of severe allergic reaction may be appropriate. QE = High (Hydroxyzine and Promethazine), Moderate (All others); SR = Strong Benztropine (oral) Trihexyphenidyl Not recommended for prevention of extrapyramidal symptoms with antipsychotics; more effective agents available for treatment of Parkinson disease. Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14040
14 Antispasmodics Belladonna alkaloids Clidinium-chlordiazepoxide Dicyclomine Hyoscyamine Propantheline Scopolamine Avoid except in short-term palliative care to decrease oral secretions. Highly anticholinergic, uncertain effectiveness. Antithrombotics Dipyridamole, oral short-acting* (does not apply to the extended-release combination with aspirin) Ticlopidine* Anti-infective Nitrofurantoin Cardiovascular Alpha1 blockers Doxazosin Prazosin Terazosin May cause orthostatic hypotension; more effective alternatives available; IV form acceptable for use in cardiac stress testing. Safer, effective alternatives available. Avoid for long-term suppression; avoid in patients with CrCl <60 ml/min. Potential for pulmonary toxicity; safer alternatives available; lack of efficacy in patients with CrCl <60 ml/min due to inadequate drug concentration in the urine. Avoid use as an antihypertensive. High risk of orthostatic hypotension; not recommended as routine treatment for hypertension; alternative agents have superior risk/benefit profile. Avoid clonidine as a first-line antihypertensive. Avoid others as listed. High risk of adverse CNS effects; may cause bradycardia and orthostatic hypotension; not recommended as routine treatment for hypertension. QE = Low; SR = Strong Alpha agonists Clonidine Guanabenz* Guanfacine* Methyldopa* Reserpine (>0.1 mg/day)* Antiarrhythmic drugs (Class Ia, Ic, III) Avoid antiarrhythmic drugs as first-line treatment of atrial Amiodarone fibrillation. Dofetilide Data suggest that rate control yields better balance of benefits Dronedarone and harms than rhythm control for most older adults. Flecainide Amiodarone is associated with multiple toxicities, including Ibutilide thyroid disease, pulmonary disorders, and QT interval Procainamide prolongation. Propafenone Quinidine Sotalol Disopyramide* Disopyramide is a potent negative inotrope and therefore may induce heart failure in older adults; strongly anticholinergic; other antiarrhythmic drugs preferred. QE = Low; SR = Strong Dronedarone Avoid in patients with permanent atrial fibrillation or heart failure. Worse outcomes have been reported in patients taking dronedarone who have permanent atrial fibrillation or heart failure. In general, rate control is preferred over rhythm control for atrial fibrillation. Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14041
15 Digoxin >0.125 mg/day In heart failure, higher dosages associated with no additional benefit and may increase risk of toxicity; decreased renal clearance may increase risk of toxicity. Nifedipine, immediate release* Spironolactone >25 mg/day Central Nervous System Tertiary TCAs, alone or in combination: Amitriptyline Chlordiazepoxide- Amitriptyline Clomipramine Doxepin >6 mg/day Imipramine Perphenazine-amitriptyline Trimipramine Antipsychotics, first- (conventional) and second- (atypical) generation (see online for full list) Thioridazine Mesoridazine Barbiturates Amobarbital* Butabarbital* Butalbital Mephobarbital* Pentobarbital* Phenobarbital Secobarbital* Potential for hypotension; risk of precipitating myocardial ischemia. Avoid in patients with heart failure or with a CrCl <30 ml/min. In heart failure, the risk of hyperkalemia is higher in older adults if taking >25 mg/day. Highly anticholinergic, sedating, and cause orthostatic hypotension; the safety profile of low-dose doxepin ( 6 mg/day) is comparable to that of placebo. Avoid use for behavioral problems of dementia unless nonpharmacologic options have failed and patient is threat to self or others. Increased risk of cerebrovascular accident (stroke) and mortality in persons with dementia. Highly anticholinergic and greater risk of QT-interval prolongation. High rate of physical dependence; tolerance to sleep benefits; greater risk of overdose at low dosages. Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14042
16 Benzodiazepines Short- and intermediate-acting: Alprazolam Estazolam Lorazepam Oxazepam Temazepam Triazolam Long-acting: Chlorazepate Chlordiazepoxide Chlordiazepoxide-amitriptyline Clidinium-chlordiazepoxide Clonazepam Diazepam Flurazepam Quazepam Chloral hydrate Meprobamate Avoid benzodiazepines (any type) for treatment of insomnia, agitation, or delirium. Older adults have increased sensitivity to benzodiazepines and decreased metabolism of long-acting agents. In general, all benzodiazepines increase risk of cognitive impairment, delirium, falls, fractures, and motor vehicle accidents in older adults. May be appropriate for seizure disorders, rapid eye movement sleep disorders, benzodiazepine withdrawal, ethanol withdrawal, severe generalized anxiety disorder, periprocedural anesthesia, end-of-life care. Tolerance occurs within 10 days and risk outweighs the benefits in light of overdose with doses only 3 times the recommended dose. QE = Low; SR = Strong High rate of physical dependence; very sedating. Nonbenzodiazepine hypnotics Eszopiclone Zolpidem Zaleplon Ergot mesylates* Isoxsuprine* Endocrine Androgens Methyltestosterone* Testosterone Desiccated thyroid Estrogens with or without progestins Avoid chronic use (>90 days) Benzodiazepine-receptor agonists that have adverse events similar to those of benzodiazepines in older adults (e.g., delirium, falls, fractures); minimal improvement in sleep latency and duration. Lack of efficacy. Avoid unless indicated for moderate to severe hypogonadism. Potential for cardiac problems and contraindicated in men with prostate cancer. QE = Moderate; SR = Weak Concerns about cardiac effects; safer alternatives available. QE = Low; SR = Strong Avoid oral and topical patch. Topical vaginal cream: Acceptable to use low-dose intravaginal estrogen for the management of dyspareunia, lower urinary tract infections, and other vaginal symptoms. Evidence of carcinogenic potential (breast and endometrium); lack of cardioprotective effect and cognitive protection in older women. Evidence that vaginal estrogens for treatment of vaginal dryness is safe and effective in women with breast cancer, especially at dosages of estradiol <25 mcg twice weekly. QE = High (Oral and Patch), Moderate (Topical); SR = Strong (Oral and Patch), Weak (Topical) Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14043
17 Growth hormone Insulin, sliding scale Megestrol Sulfonylureas, long-duration Chlorpropamide Glyburide Gastrointestinal Metoclopramide Mineral oil, given orally Trimethobenzamide Avoid, except as hormone replacement following pituitary gland removal. Effect on body composition is small and associated with edema, arthralgia, carpal tunnel syndrome, gynecomastia, impaired fasting glucose. Higher risk of hypoglycemia without improvement in hyperglycemia management regardless of care setting. Minimal effect on weight; increases risk of thrombotic events and possibly death in older adults. Chlorpropamide: prolonged half-life in older adults; can cause prolonged hypoglycemia; causes SIADH Glyburide: higher risk of severe prolonged hypoglycemia in older adults. Avoid, unless for gastroparesis. Can cause extrapyramidal effects including tardive dyskinesia; risk may be further increased in frail older adults. Potential for aspiration and adverse effects; safer alternatives available. One of the least effective antiemetic drugs; can cause extrapyramidal adverse effects. QE = Moderate; SR = Stron Pain Medications Meperidine Non-COX-selective NSAIDs, oral Aspirin >325 mg/day Diclofenac Diflunisal Etodolac Fenoprofen Ibuprofen Ketoprofen Meclofenamate Mefenamic acid Meloxicam Nabumetone Naproxen Oxaprozin Piroxicam Sulindac Tolmetin Not an effective oral analgesic in dosages commonly used; may cause neurotoxicity; safer alternatives available. Avoid chronic use unless other alternatives are not effective and patient can take gastroprotective agent (proton-pump inhibitor or misoprostol). Increases risk of GI bleeding/peptic ulcer disease in high-risk groups, including those 75 years old or taking oral or parenteral corticosteroids, anticoagulants, or antiplatelet agents. Use of proton pump inhibitor or misoprostol reduces but does not eliminate risk. Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14044
18 Indomethacin Ketorolac, includes parenteral Pentazocine* Skeletal muscle relaxants Carisoprodol Chlorzoxazone Cyclobenzaprine Metaxalone Methocarbamol Orphenadrine Increases risk of GI bleeding/peptic ulcer disease in high-risk groups (See Non-COX selective NSAIDs) Of all the NSAIDs, indomethacin has most adverse effects. QE = Moderate (Indomethacin), High (Ketorolac); SR = Strong Opioid analgesic that causes CNS adverse effects, including confusion and hallucinations, more commonly than other narcotic drugs; is also a mixed agonist and antagonist; safer alternatives available. QE = Low; SR = Strong Most muscle relaxants poorly tolerated by older adults, because of anticholinergic adverse effects, sedation, increased risk of fractures; effectiveness at dosages tolerated by older adults is questionable. *Infrequently used drugs. Table 1 Abbreviations: ACEI, angiotensin converting-enzyme inhibitors; ARB, angiotensin receptor blockers; CNS, central nervous system; COX, cyclooxygenase; CrCl, creatinine clearance; GI, gastrointestinal; NSAIDs, nonsteroidal anti-inflammatory drugs; SIADH, syndrome of inappropriate antidiuretic hormone secretion; SR, Strength of Recommendation; TCAs, tricyclic antidepressants; QE, Quality of Evidence TABLE 2: 2012 AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults Due to Drug-Disease or Drug-Syndrome Interactions That May Exacerbate the Disease or Syndrome Disease or Syndrome Drug(s) Recommendation, Rationale, Quality of Evidence (QE) & Strength of Recommendation (SR) Cardiovascular Heart failure NSAIDs and COX-2 inhibitors Nondihydropyridine CCBs (avoid only for systolic heart failure) Diltiazem Verapamil Pioglitazone, rosiglitazone Cilostazol Dronedarone Potential to promote fluid retention and/or exacerbate heart failure. QE = Moderate (NSAIDs, CCBs, Dronedarone), High (Thiazolidinediones (glitazones)), Low (Cilostazol); SR = Strong Syncope Central Nervous System Chronic seizures or epilepsy Acetylcholinesterase inhibitors (AChEIs) Peripheral alpha blockers Doxazosin Prazosin Terazosin Tertiary TCAs Chlorpromazine, thioridazine, and olanzapine Bupropion Chlorpromazine Clozapine Maprotiline Olanzapine Thioridazine Thiothixene Tramadol Increases risk of orthostatic hypotension or bradycardia. QE = High (Alpha blockers), Moderate (AChEIs, TCAs and antipsychotics); SR = Strong (AChEIs and TCAs), Weak (Alpha blockers and antipsychotics) Lowers seizure threshold; may be acceptable in patients with well-controlled seizures in whom alternative agents have not been effective. Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14045
19 Delirium Dementia & cognitive impairment History of falls or fractures Insomnia Parkinson s disease All TCAs Anticholinergics Benzodiazepines Chlorpromazine Corticosteroids H2-receptor antagonist Meperidine Sedative hypnotics Thioridazine Anticholinergics Benzodiazepines H2-receptor antagonists Zolpidem Antipsychotics, chronic and asneeded use Anticonvulsants Antipsychotics Benzodiazepines Nonbenzodiazepine hypnotics Eszopiclone Zaleplon Zolpidem TCAs/SSRIs Oral decongestants Pseudoephedrine Phenylephrine Stimulants Amphetamine Methylphenidate Pemoline Theobromines Theophylline Caffeine All antipsychotics (see online publication for full list, except for quetiapine and clozapine) Antiemetics Metoclopramide Prochlorperazine Promethazine Avoid in older adults with or at high risk of delirium because of inducing or worsening delirium in older adults; if discontinuing drugs used chronically, taper to avoid withdrawal symptoms. Avoid due to adverse CNS effects. Avoid unless safer alternatives are not available; avoid anticonvulsants except for seizure. Ability to produce ataxia, impaired psychomotor function, syncope, and additional falls; shorter-acting benzodiazepines are not safer than longacting ones. CNS stimulant effects. Dopamine receptor antagonists with potential to worsen parkinsonian symptoms. Quetiapine and clozapine appear to be less likely to precipitate worsening of Parkinson disease. Gastrointestinal Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14046
20 Chronic constipation Oral antimuscarinics for urinary incontinence Darifenacin Oxybutynin (oral) Solifenacin Tolterodine Trospium Nondihydropyridine CCB Diltiazem Verapamil First-generation antihistamines as single agent or part of combination products Brompheniramine Chlorpheniramine Cyproheptadine Dexchlorpheniramine Diphenhydramine Doxylamine Hydroxyzine Promethazine Anticholinergics/antispasmodics Antipsychotics Belladonna alkaloids Clidinium-chlordiazepoxide Dicyclomine Hyoscyamine Propantheline Scopolamine Tertiary TCAs Avoid unless no other alternatives. Can worsen constipation; agents for urinary incontinence: antimuscarinics overall differ in incidence of constipation; response variable; consider alternative agent if constipation develops. QE = High (For Urinary Incontinence), Moderate/Low (All Others); SR = Strong History of gastric or duodenal ulcers Kidney/Urinary Tract Chronic kidney disease stages IV and V Urinary incontinence (all types) in women Lower urinary tract symptoms, benign prostatic hyperplasia Stress or mixed urinary incontinence Aspirin (>325 mg/day) Non COX-2 selective NSAIDs NSAIDs Triamterene (alone or in combination) Estrogen oral and transdermal (excludes intravaginal estrogen) Inhaled anticholinergic agents Strongly anticholinergic drugs, except antimuscarinics for urinary incontinence (see Table 9 for complete list). Alpha-blockers Doxazosin Prazosin Terazosin Avoid unless other alternatives are not effective and patient can take gastroprotective agent (proton-pump inhibitor or misoprostol). May exacerbate existing ulcers or cause new/additional ulcers. May increase risk of kidney injury. May increase risk of acute kidney injury. QE = Moderate (NSAIDs), Low (Triamterene); SR = Strong (NSAIDs), Weak (Triamterene) Avoid in women. Aggravation of incontinence. Avoid in men. May decrease urinary flow and cause urinary retention. (Inhaled agents), Weak (All others) Avoid in women. Aggravation of incontinence. Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14047
21 Table 2 Abbreviations: CCBs, calcium channel blockers; AChEIs, acetylcholinesterase inhibitors; CNS, central nervous system; COX, cyclooxygenase; NSAIDs, nonsteroidal anti-inflammatory drugs; SR, Strength of Recommendation; SSRIs, selective serotonin reuptake inhibitors; TCAs, tricyclic antidepressants; QE, Quality of Evidence TABLE 3: 2012 AGS Beers Criteria for Potentially Inappropriate Medications to Be Used with Caution in Older Adults Drug(s) Recommendation, Rationale, Quality of Evidence (QE) & Strength of Recommendation (SR) Aspirin for primary prevention of cardiac events Use with caution in adults 80 years old. Lack of evidence of benefit versus risk in individuals 80 years old. QE = Low; SR = Weak Dabigatran Use with caution in adults 75 years old or if CrCl <30 ml/min. Increased risk of bleeding compared with warfarin in adults 75 years old; lack of evidence for efficacy and safety in patients with CrCl <30 ml/min QE = Moderate; SR = Weak Prasugrel Use with caution in adults 75 years old. Greater risk of bleeding in older adults; risk may be offset by benefit in highest-risk older patients (eg, those with prior myocardial infarction or diabetes). QE = Moderate; SR = Weak Antipsychotics Carbamazepine Carboplatin Cisplatin Mirtazapine SNRIs SSRIs TCAs Vincristine Vasodilators Use with caution. May exacerbate or cause SIADH or hyponatremia; need to monitor sodium level closely when starting or changing dosages in older adults due to increased risk. Use with caution. May exacerbate episodes of syncope in individuals with history of syncope. QE = Moderate; SR = Weak Table 3 Abbreviations: CrCl, creatinine clearance; SIADH, syndrome of inappropriate antidiuretic hormone Dr Steve Paul Manjaly et al JMSCR Volume 4 Issue 11 November 2016 Page 14048
Potentially Inappropriate Medication Use in Older Adults 2015 Latest Research
 Home Resources Potentially Inappropriate Medication Use in Older Adults 2015 Resources Potentially Inappropriate Medication Use in Older Adults 2015 Latest Research Drugs and Categories of Drugs What these
Home Resources Potentially Inappropriate Medication Use in Older Adults 2015 Resources Potentially Inappropriate Medication Use in Older Adults 2015 Latest Research Drugs and Categories of Drugs What these
Measure #238 (NQF 0022): Use of High-Risk Medications in the Elderly National Quality Strategy Domain: Patient Safety
 Measure #238 (NQF 0022): Use of High-Risk Medications in the Elderly National Quality Strategy Domain: Patient Safety 2015 PHYSICIAN QUALITY REPTING OPTIONS F INDIVIDUAL MEASURES REGISTRY ONLY DESCRIPTION:
Measure #238 (NQF 0022): Use of High-Risk Medications in the Elderly National Quality Strategy Domain: Patient Safety 2015 PHYSICIAN QUALITY REPTING OPTIONS F INDIVIDUAL MEASURES REGISTRY ONLY DESCRIPTION:
Measure #238 (NQF 0022): Use of High-Risk Medications in the Elderly National Quality Strategy Domain: Patient Safety
 Measure #238 (NQF 0022): Use of High-Risk Medications in the Elderly National Quality Strategy Domain: Patient Safety 2016 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES REGISTRY ONLY DESCRIPTION:
Measure #238 (NQF 0022): Use of High-Risk Medications in the Elderly National Quality Strategy Domain: Patient Safety 2016 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES REGISTRY ONLY DESCRIPTION:
COMMON DRUG RELATED PROBLEMS SEEN IN PACE AND MECHANISMS TO MITIGATE RISK
 COMMON DRUG RELATED PROBLEMS SEEN IN PACE AND MECHANISMS TO MITIGATE RISK Robert L Alesiani, PharmD, CGP Chief Pharmacotherapy Officer CareKinesis, Inc. (a Tabula Rasa Healthcare Company) 2 3 4 5 Pharmacogenomics
COMMON DRUG RELATED PROBLEMS SEEN IN PACE AND MECHANISMS TO MITIGATE RISK Robert L Alesiani, PharmD, CGP Chief Pharmacotherapy Officer CareKinesis, Inc. (a Tabula Rasa Healthcare Company) 2 3 4 5 Pharmacogenomics
Measure #238 (NQF 0022): Use of High-Risk Medications in the Elderly National Quality Strategy Domain: Patient Safety
 Measure #238 (NQF 0022): Use of High-Risk Medications in the Elderly National Quality Strategy Domain: Patient Safety 2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION:
Measure #238 (NQF 0022): Use of High-Risk Medications in the Elderly National Quality Strategy Domain: Patient Safety 2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION:
Quality ID #238 (NQF 0022): Use of High-Risk Medications in the Elderly National Quality Strategy Domain: Patient Safety
 Quality ID #238 (NQF 0022): Use of High-Risk Medications in the Elderly National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION:
Quality ID #238 (NQF 0022): Use of High-Risk Medications in the Elderly National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION:
Geri-PARDY! (2015 Beers Criteria) Pharmacology Edition
 Geri-PARDY! Pharmacology Edition (2015 Beers Criteria) Aurelio Muyot, MD, AGSF, FACP Assistant Professor College of Osteopathic Medicine Touro University Nevada Objectives Review the 2015 Beers Criteria
Geri-PARDY! Pharmacology Edition (2015 Beers Criteria) Aurelio Muyot, MD, AGSF, FACP Assistant Professor College of Osteopathic Medicine Touro University Nevada Objectives Review the 2015 Beers Criteria
AGS. From THE AMERICAN GERIATRICS SOCIETY AGS 2015 BEERS CRITERIA
 From THE AMERICAN GERIATRICS SOCIETY AGS 2015 BEERS CRITERIA This guide has been developed as a tool to assist healthcare providers in improving medication safety in older adults. The role of this guide
From THE AMERICAN GERIATRICS SOCIETY AGS 2015 BEERS CRITERIA This guide has been developed as a tool to assist healthcare providers in improving medication safety in older adults. The role of this guide
Use of diphenhydramine in situations such as acute treatment of. treatment of Parkinson disease. Avoid
 From THE AMERICAN GERIATRICS SOCIETY A POCKET GUIDE TO THE AGS 2015 BEERS CRITERIA This guide has been developed as a tool to assist healthcare providers in improving medication safety in older adults.
From THE AMERICAN GERIATRICS SOCIETY A POCKET GUIDE TO THE AGS 2015 BEERS CRITERIA This guide has been developed as a tool to assist healthcare providers in improving medication safety in older adults.
American Geriatrics Society 2015 Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults
 CLINICAL INVESTIGATIONS American Geriatrics Society 2015 Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults By the American Geriatrics Society 2015 Beers Criteria Update
CLINICAL INVESTIGATIONS American Geriatrics Society 2015 Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults By the American Geriatrics Society 2015 Beers Criteria Update
American Geriatrics Society Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults
 SPECIAL ARTICLES American Geriatrics Society Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults The American Geriatrics Society 2012 Beers Criteria Update Expert Panel
SPECIAL ARTICLES American Geriatrics Society Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults The American Geriatrics Society 2012 Beers Criteria Update Expert Panel
Pennsylvania Academy of Family Physicians Foundation & UPMC 43rd Refresher Course in Family Medicine CME Conference March 10-13, 2016
 Pennsylvania Academy of Family Physicians Foundation & UPMC 43rd Refresher Course in Family Medicine CME Conference March 10-13, 2016 Disclosures: Drugs in Older Adults: Beers Criteria Heather Sakely,
Pennsylvania Academy of Family Physicians Foundation & UPMC 43rd Refresher Course in Family Medicine CME Conference March 10-13, 2016 Disclosures: Drugs in Older Adults: Beers Criteria Heather Sakely,
Objectives. Polypharmacy and the Geriatric Patient: A Primer for the Orthopedic Nurse CONFLICT OF INTEREST
 Polypharmacy and the Geriatric Patient: A Primer for the Orthopedic Nurse Presented by Eric Greenberg Pharm. D., CGP, BCPS, R.Ph. Clinical Pharmacist Hospital for Special Surgery CONFLICT OF INTEREST I
Polypharmacy and the Geriatric Patient: A Primer for the Orthopedic Nurse Presented by Eric Greenberg Pharm. D., CGP, BCPS, R.Ph. Clinical Pharmacist Hospital for Special Surgery CONFLICT OF INTEREST I
Katee Kindler, PharmD, BCACP
 Speaker Introduction Katee Kindler, PharmD, BCACP Current Practice: Clinical Pharmacy Specialist Ambulatory Care, St. Vincent Indianapolis Assistant Professor of Pharmacy Practice, Manchester University,
Speaker Introduction Katee Kindler, PharmD, BCACP Current Practice: Clinical Pharmacy Specialist Ambulatory Care, St. Vincent Indianapolis Assistant Professor of Pharmacy Practice, Manchester University,
American Geriatrics Society 2019 Updated AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults
 CLINICAL INVESTIGATION American Geriatrics Society 2019 Updated AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults By the 2019 American Geriatrics Society Beers Criteria Update
CLINICAL INVESTIGATION American Geriatrics Society 2019 Updated AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults By the 2019 American Geriatrics Society Beers Criteria Update
STOPP and START criteria October 2011
 # START and STOPP are newer criteria to identify potentially inappropriate medications in elderly, including drug drug and drug disease interactions, drugs which increase risk of falls and drugs which
# START and STOPP are newer criteria to identify potentially inappropriate medications in elderly, including drug drug and drug disease interactions, drugs which increase risk of falls and drugs which
Geriatric Pharmacology
 Geriatric Pharmacology Janice Scheufler R.Ph.,PharmD, FASCP Clinical Pharmacist Hospice of the Western Reserve Objectives List three risk factors for adverse drug events in the elderly Discuss two physiological
Geriatric Pharmacology Janice Scheufler R.Ph.,PharmD, FASCP Clinical Pharmacist Hospice of the Western Reserve Objectives List three risk factors for adverse drug events in the elderly Discuss two physiological
High-risk medications in older adults drug alternative(s)
 Antianxiety Analgesics Antihypertensive High-risk medications in older adults drug alternative(s) Guanabenz Guanfacine Methyldopa Reserpine (greater than 0.1 mg per day) High risk of adverse central nervous
Antianxiety Analgesics Antihypertensive High-risk medications in older adults drug alternative(s) Guanabenz Guanfacine Methyldopa Reserpine (greater than 0.1 mg per day) High risk of adverse central nervous
4/10/2013 DISCLOSURES
 DISCLOSURES I have no financial relationship to disclose. 2012 BEERSCRITERIA AN UPDATE FOR GERIATRIC MEDICINE Charles Mosler, PharmD, CGP, FASCP Ohio Pharmacists Association Annual Conference and Trade
DISCLOSURES I have no financial relationship to disclose. 2012 BEERSCRITERIA AN UPDATE FOR GERIATRIC MEDICINE Charles Mosler, PharmD, CGP, FASCP Ohio Pharmacists Association Annual Conference and Trade
Chronic Obstructive Pulmonary Disease (COPD) Care Management Assessment
 The questions in this brochure, based on the 2010 Global Initiative for Chronic Obstructive Lung Disease (GOLD) report, 1 are designed to help healthcare professionals (specifically case/care managers)
The questions in this brochure, based on the 2010 Global Initiative for Chronic Obstructive Lung Disease (GOLD) report, 1 are designed to help healthcare professionals (specifically case/care managers)
STOPP START Toolkit Supporting Medication Review in the Older Person
 STOPP START Toolkit Supporting Medication Review in the Older Person STOPP: Screening Tool of Older People s potentially inappropriate Prescriptions START: Screening Tool to Alert doctors to Right (appropriate,
STOPP START Toolkit Supporting Medication Review in the Older Person STOPP: Screening Tool of Older People s potentially inappropriate Prescriptions START: Screening Tool to Alert doctors to Right (appropriate,
Medications to avoid in the elderly
 Medicationstoavoidintheelderly Description Medicationstoavoid 1 (nonformularyin2016) Adversesideeffects/concerns Formularyalternatives 2,3 Alphaagonists, central Analgesics Androgen Anti anxiety guanabenz
Medicationstoavoidintheelderly Description Medicationstoavoid 1 (nonformularyin2016) Adversesideeffects/concerns Formularyalternatives 2,3 Alphaagonists, central Analgesics Androgen Anti anxiety guanabenz
1/21/2016 UPDATE ON THE AMERICAN GERIATRICS SOCIETY 2015 BEERS CRITERIA DISCLOSURE OBJECTIVES AGING GOALS BEERS CRITERIA
 UPDATE ON THE AMERICAN GERIATRICS SOCIETY 2015 BEERS CRITERIA DISCLOSURE I have no financial conflict of interest to disclose. Lacey Charbonneau, Pharm.D. PGY-1 Community Practice Resident Baptist Medical
UPDATE ON THE AMERICAN GERIATRICS SOCIETY 2015 BEERS CRITERIA DISCLOSURE I have no financial conflict of interest to disclose. Lacey Charbonneau, Pharm.D. PGY-1 Community Practice Resident Baptist Medical
Geriatric Pharmacology. Kwi Bulow, M.D. Clinical Professor of Medicine Director, Academic Geriatric Resource Center
 Geriatric Pharmacology Kwi Bulow, M.D. Clinical Professor of Medicine Director, Academic Geriatric Resource Center Silver Tsunami 2010: 40 million (13%) 2030: 72 million (20%) Baby Boomers (1946-1964)
Geriatric Pharmacology Kwi Bulow, M.D. Clinical Professor of Medicine Director, Academic Geriatric Resource Center Silver Tsunami 2010: 40 million (13%) 2030: 72 million (20%) Baby Boomers (1946-1964)
The Geriatric Assessment. Dr. Gary Mumaugh Western Physical Assessment
 The Geriatric Assessment Dr. Gary Mumaugh Western Physical Assessment Geriatric Assessment The number of elderly Americans older than 65 yrs of age could increase from 34 million in 1998 to approximately
The Geriatric Assessment Dr. Gary Mumaugh Western Physical Assessment Geriatric Assessment The number of elderly Americans older than 65 yrs of age could increase from 34 million in 1998 to approximately
Prescribing and Pharmacokinetic Considerations in the Elderly
 Prescribing and Pharmacokinetic Considerations in the Elderly Melanie A. Dodd, Pharm.D., Ph.C., BCPS Associate Professor of Pharmacy in Geriatrics College of Pharmacy The University of New Mexico OBJECTIVES
Prescribing and Pharmacokinetic Considerations in the Elderly Melanie A. Dodd, Pharm.D., Ph.C., BCPS Associate Professor of Pharmacy in Geriatrics College of Pharmacy The University of New Mexico OBJECTIVES
Maximizing Medication Safety UNIVERSITY OF HAWAII AUGUST 31, 2016
 Maximizing Medication Safety UNIVERSITY OF HAWAII AUGUST 31, 2016 Adverse Drug Events (ADE s) RISK FACTORS FOR Adverse Drug Events (ADEs) 6 or more concurrent chronic conditions 12 or more doses of drugs/day
Maximizing Medication Safety UNIVERSITY OF HAWAII AUGUST 31, 2016 Adverse Drug Events (ADE s) RISK FACTORS FOR Adverse Drug Events (ADEs) 6 or more concurrent chronic conditions 12 or more doses of drugs/day
BEERs For the Elderly
 BEERs For the Elderly February 2008 Presented by:carla Ambrosini Seniors First Clinic Pharmacist 12/05/2008 1 Objectives To highlight the overall health care impact of drug related adverse reactions and
BEERs For the Elderly February 2008 Presented by:carla Ambrosini Seniors First Clinic Pharmacist 12/05/2008 1 Objectives To highlight the overall health care impact of drug related adverse reactions and
POLYPHARMACY IN OLDER ADULTS AND BEERS CRITERIA UPDATE
 POLYPHARMACY IN OLDER ADULTS AND BEERS CRITERIA UPDATE Jeannie Kim Lee, PharmD, BCPS, CGP Clinical Pharmacy Director College of Pharmacy The University of Arizona Learning Objectives: State the risks of
POLYPHARMACY IN OLDER ADULTS AND BEERS CRITERIA UPDATE Jeannie Kim Lee, PharmD, BCPS, CGP Clinical Pharmacy Director College of Pharmacy The University of Arizona Learning Objectives: State the risks of
Medication Use in Older Adults
 Medication Use in Older Adults F. Michael Gloth, III, MD, AGSF, FACP, CMD Clinical Professor Department of Geriatrics, Florida State University College of Medicine Associate Professor of Medicine Division
Medication Use in Older Adults F. Michael Gloth, III, MD, AGSF, FACP, CMD Clinical Professor Department of Geriatrics, Florida State University College of Medicine Associate Professor of Medicine Division
Supplementary Online Content
 Supplementary Online Content Gray SL, Anderson ML, Dublin S, et al. Cumulative use of strong anticholinergics and incident dementia: a prospective cohort study. JAMA Intern Med. Published online January
Supplementary Online Content Gray SL, Anderson ML, Dublin S, et al. Cumulative use of strong anticholinergics and incident dementia: a prospective cohort study. JAMA Intern Med. Published online January
Learning Objectives 2/4/2016. Patrick Leung, Pharm.D., BCPS, PhC. Patrick Leung, Pharm.D., BCPS, PhC Davena Norris, Pharm.D., BCPS, PhC 2/20/2016
 Patrick Leung, Pharm.D., BCPS, PhC Davena Norris, Pharm.D., BCPS, PhC 2/20/2016 Learning Objectives Identify age-related pharmacokinetic and pharmacodynamic changes in older adults. Utilization the START/STOPP
Patrick Leung, Pharm.D., BCPS, PhC Davena Norris, Pharm.D., BCPS, PhC 2/20/2016 Learning Objectives Identify age-related pharmacokinetic and pharmacodynamic changes in older adults. Utilization the START/STOPP
High Risk Medications: What Can Community Pharmacists Do to Make Patients Safer?
 CONTINUING EDUCATION High Risk Medications: What Can Community Pharmacists Do to Make Patients Safer? by Sean T. Lasota, PharmD Sept. 1, 2015 (expires Sept. 1, 2018) Activity Type: Knowledge-based To earn
CONTINUING EDUCATION High Risk Medications: What Can Community Pharmacists Do to Make Patients Safer? by Sean T. Lasota, PharmD Sept. 1, 2015 (expires Sept. 1, 2018) Activity Type: Knowledge-based To earn
Guideline Summary NGC-10857
 Guideline Summary NGC-10857 Guideline Title American Geriatrics Society 2015 updated Beers Criteria for potentially inappropriate medication use in older adults. Bibliographic Source(s) American Geriatrics
Guideline Summary NGC-10857 Guideline Title American Geriatrics Society 2015 updated Beers Criteria for potentially inappropriate medication use in older adults. Bibliographic Source(s) American Geriatrics
AGS AGS 2015 BEERS CRITERIA. From THE AMERICAN GERIATRICS SOCIETY A POCKET GUIDE TO THE. PAGE 1 PAGE 2 Table 1 (continued on page 3)
 From THE AMERICAN GERIATRICS SOCIETY A POCKET GUIDE TO THE AGS 2015 BEERS CRITERIA This guide has been developed as a tool to assist healthcare providers in improving medication safety in older adults.
From THE AMERICAN GERIATRICS SOCIETY A POCKET GUIDE TO THE AGS 2015 BEERS CRITERIA This guide has been developed as a tool to assist healthcare providers in improving medication safety in older adults.
Fall Prevention in Hospice (A pharmacologic and nonpharmacologic approach)
 Fall Prevention in Hospice (A pharmacologic and nonpharmacologic approach) Chinenye Emereole, Pharm.D. Clinical Pharmacist Hospice Pharmacy Solutions Objectives Assess and identify hospice patients who
Fall Prevention in Hospice (A pharmacologic and nonpharmacologic approach) Chinenye Emereole, Pharm.D. Clinical Pharmacist Hospice Pharmacy Solutions Objectives Assess and identify hospice patients who
Medication Assessment and Quality Parameters. Norma J. Owens, PharmD, FCCP Professor of Pharmacy University of Rhode Island
 Medication Assessment and Quality Parameters Norma J. Owens, PharmD, FCCP Professor of Pharmacy University of Rhode Island Financial Disclosure None of the planners, speakers, and/or members of the CME
Medication Assessment and Quality Parameters Norma J. Owens, PharmD, FCCP Professor of Pharmacy University of Rhode Island Financial Disclosure None of the planners, speakers, and/or members of the CME
Psychotropic Medication Use in Dementia
 Psychotropic Medication Use in Dementia Marie A DeWitt, MD Diplomate of the American Board of Psychiatry and Neurology, Specialization in Psychiatry & Subspecialization in Geriatric Psychiatry Staff Physician,
Psychotropic Medication Use in Dementia Marie A DeWitt, MD Diplomate of the American Board of Psychiatry and Neurology, Specialization in Psychiatry & Subspecialization in Geriatric Psychiatry Staff Physician,
DRUGS THAT ACT IN THE CNS
 DRUGS THAT ACT IN THE CNS Anxiolytic and Hypnotic Drugs Dr Karamallah S. Mahmood PhD Clinical Pharmacology 1 OTHER ANXIOLYTIC AGENTS/ A. Antidepressants Many antidepressants are effective in the treatment
DRUGS THAT ACT IN THE CNS Anxiolytic and Hypnotic Drugs Dr Karamallah S. Mahmood PhD Clinical Pharmacology 1 OTHER ANXIOLYTIC AGENTS/ A. Antidepressants Many antidepressants are effective in the treatment
Chitra Fernando, MD March 18, 2008
 Chitra Fernando, MD March 18, 2008 Definition Statistics Risk factors Why older adults are more prone to ADE Manifestations Inappropriate medications for older adults What can be done to minimize adverse
Chitra Fernando, MD March 18, 2008 Definition Statistics Risk factors Why older adults are more prone to ADE Manifestations Inappropriate medications for older adults What can be done to minimize adverse
Aging and Geriatric Assessment March 31, 2008 Sharon Leigh, Pharm D. BCPS Providence ElderPlace
 Aging and Geriatric Assessment Page 1 Aging and Geriatric Assessment March 31, 2008 Sharon Leigh, Pharm D. BCPS Providence ElderPlace I. Aging A. Demographics Age 65+ population 3.1 million 1900 31.2 million
Aging and Geriatric Assessment Page 1 Aging and Geriatric Assessment March 31, 2008 Sharon Leigh, Pharm D. BCPS Providence ElderPlace I. Aging A. Demographics Age 65+ population 3.1 million 1900 31.2 million
Proposed Changes to Existing Measures for HEDIS : Use of High-Risk Medications in the Elderly (DAE) and
 Proposed Changes to Existing Measures for HEDIS 1 2020: Use of High-Risk Medications in the Elderly (DAE) and Potentially Harmful Drug-Disease Interactions in the Elderly (DDE) NCQA seeks comments on proposed
Proposed Changes to Existing Measures for HEDIS 1 2020: Use of High-Risk Medications in the Elderly (DAE) and Potentially Harmful Drug-Disease Interactions in the Elderly (DDE) NCQA seeks comments on proposed
START, STOPP, Beers Oh My! Navigating the World of Geriatric Pharmacy
 START, STOPP, Beers Oh My! Navigating the World of Geriatric Pharmacy Jessica DiLeo, PharmD Kate Murphy, PharmD OBJECTIVES Identify pharmacodynamic and pharmacokinetic parameters that may influence treatment
START, STOPP, Beers Oh My! Navigating the World of Geriatric Pharmacy Jessica DiLeo, PharmD Kate Murphy, PharmD OBJECTIVES Identify pharmacodynamic and pharmacokinetic parameters that may influence treatment
Reduction of High Risk Medications Using A Quality Initiative Perspective
 Reduction of High Risk Medications Using A Quality Initiative Perspective Richard Mueller PharmD, MBA, MS, Director of Pharmacy Dianne Hempel BSN, RN Quality Improvement Coordinator Objectives Learn what
Reduction of High Risk Medications Using A Quality Initiative Perspective Richard Mueller PharmD, MBA, MS, Director of Pharmacy Dianne Hempel BSN, RN Quality Improvement Coordinator Objectives Learn what
Bree Collaborative AMDG Opioid Prescribing Guidelines Workgroup. Opioid Prescribing Metrics - DRAFT
 Bree Collaborative AMDG Opioid Prescribing Guidelines Workgroup Opioid Prescribing Metrics - DRAFT Definitions: Days Supply: The total of all opioid prescriptions dispensed during the calendar quarter
Bree Collaborative AMDG Opioid Prescribing Guidelines Workgroup Opioid Prescribing Metrics - DRAFT Definitions: Days Supply: The total of all opioid prescriptions dispensed during the calendar quarter
Prescribing Drugs to the Elderly
 Answers to your questions from University of Toronto experts Prescribing Drugs to the Elderly Can drugs do more harm than good? M.A. is a 90-year-old man living at home. He has dementia and due to wandering
Answers to your questions from University of Toronto experts Prescribing Drugs to the Elderly Can drugs do more harm than good? M.A. is a 90-year-old man living at home. He has dementia and due to wandering
Falls most commonly seen in RACFs are due to tripping, slipping and stumbling (21.6%). Falling down stairs is relatively uncommon in
 This Presentation Medications and Falls Dr Peter Tenni M Pharm (Curtin), PhD (UTAS) AACPA Director, CPS A fall is an event which results in a person coming to rest inadvertently on the ground or floor
This Presentation Medications and Falls Dr Peter Tenni M Pharm (Curtin), PhD (UTAS) AACPA Director, CPS A fall is an event which results in a person coming to rest inadvertently on the ground or floor
Did you know that some medications can be harmful to people 65 years or older?
 Did you know that some medications can be harmful to people 65 years or older? What s the risk? Some medications can be dangerous to people 65 years of age or older. As we age, our bodies change. These
Did you know that some medications can be harmful to people 65 years or older? What s the risk? Some medications can be dangerous to people 65 years of age or older. As we age, our bodies change. These
There s A Pill For That (But should my patient be on it?) A Review of Tools for the Evaluation of Optimal Prescribing in Geriatric Patients
 There s A Pill For That (But should my patient be on it?) A Review of Tools for the Evaluation of Optimal Prescribing in Geriatric Patients Marilyn N. Bulloch, PharmD, BCPS Assistant Clinical Professor
There s A Pill For That (But should my patient be on it?) A Review of Tools for the Evaluation of Optimal Prescribing in Geriatric Patients Marilyn N. Bulloch, PharmD, BCPS Assistant Clinical Professor
Pharmacology in the Elderly
 Pharmacology in the Elderly James Hardy Geriatrician, Royal North Shore Hospital A recent consultation Aspirin Clopidogrel Warfarin Coloxyl with senna Clearlax Methotrexate Paracetamol Pantoprazole Cholecalciferol
Pharmacology in the Elderly James Hardy Geriatrician, Royal North Shore Hospital A recent consultation Aspirin Clopidogrel Warfarin Coloxyl with senna Clearlax Methotrexate Paracetamol Pantoprazole Cholecalciferol
Medications Contributing to Falls. Kate Niemann, PharmD BCGP AuBurn Pharmacy
 Medications Contributing to Falls Kate Niemann, PharmD BCGP AuBurn Pharmacy Why Are Falls Important? Leading cause of injury in elders Costs to the system (CDC, 2008) ER Visits: 2.2 million $28.2 billion
Medications Contributing to Falls Kate Niemann, PharmD BCGP AuBurn Pharmacy Why Are Falls Important? Leading cause of injury in elders Costs to the system (CDC, 2008) ER Visits: 2.2 million $28.2 billion
Medicine Related Falls Risk Assessment Tool (MRFRAT)
 Medicine Related Falls Risk Assessment Tool (MRFRAT) The Medicine Related Falls Risk Assessment tool (MRFRAT) in Appendix 1 is designed to help identify patients at risk of falls due to their current medicine
Medicine Related Falls Risk Assessment Tool (MRFRAT) The Medicine Related Falls Risk Assessment tool (MRFRAT) in Appendix 1 is designed to help identify patients at risk of falls due to their current medicine
Inappropriate Medication Use in the Elderly
 Inappropriate Medication Use in the Elderly Amanda Ilenin, Pharm.D. OhioHealth Dublin Methodist Hospital & OhioHealth Grady Memorial Hospital Kristian Navickas, Pharm.D. OhioHealth McConnell Heart Health
Inappropriate Medication Use in the Elderly Amanda Ilenin, Pharm.D. OhioHealth Dublin Methodist Hospital & OhioHealth Grady Memorial Hospital Kristian Navickas, Pharm.D. OhioHealth McConnell Heart Health
The Path to Geriatric Sensitive Evidence - Based Care: Medications and Older Adults Barberton Hospital. Joyce Restifo MSN, RN Geriatric CNS-BC
 The Path to Geriatric Sensitive Evidence - Based Care: Medications and Older Adults Barberton Hospital Joyce Restifo MSN, RN Geriatric CNS-BC Aging Population By 2030, older adults will make up 20% of
The Path to Geriatric Sensitive Evidence - Based Care: Medications and Older Adults Barberton Hospital Joyce Restifo MSN, RN Geriatric CNS-BC Aging Population By 2030, older adults will make up 20% of
PRESCRIBING IN THE ELDERLY. CARE HOME PHARMACY TEAM Bhavini Shah, Eleesha Pentiah & Puja Vyas
 PRESCRIBING IN THE ELDERLY CARE HOME PHARMACY TEAM Bhavini Shah, Eleesha Pentiah & Puja Vyas LEARNING OUTCOMES Medicines Optimisation The effects of aging on health and medicines. Polypharmacy Acute Kidney
PRESCRIBING IN THE ELDERLY CARE HOME PHARMACY TEAM Bhavini Shah, Eleesha Pentiah & Puja Vyas LEARNING OUTCOMES Medicines Optimisation The effects of aging on health and medicines. Polypharmacy Acute Kidney
Geriatric prescribing considerations
 Geriatric prescribing considerations Melanie A. Dodd, Pharm.D., Ph.C., BCPS Associate Professor of Pharmacy in Geriatrics Vice-chair, Department of Pharmacy Practice and Administrative Sciences College
Geriatric prescribing considerations Melanie A. Dodd, Pharm.D., Ph.C., BCPS Associate Professor of Pharmacy in Geriatrics Vice-chair, Department of Pharmacy Practice and Administrative Sciences College
Provider Toolkit PFFS/PPO
 Provider Toolkit 2014 2015 Y0067_PR_PhysTlkt_0514_IA 05/14/2014 PFFS/PPO TABLE OF CONTENTS Sample Letter from Physician to Patient...4 HEDIS Quick Reference Guide...5 High Risk Medication Formulary Alternative
Provider Toolkit 2014 2015 Y0067_PR_PhysTlkt_0514_IA 05/14/2014 PFFS/PPO TABLE OF CONTENTS Sample Letter from Physician to Patient...4 HEDIS Quick Reference Guide...5 High Risk Medication Formulary Alternative
Medication Prescribing for Older Adults
 REVIEW Medication Prescribing for Older Adults Barbara Roehl, MD, MBA, Amy Talati, PharmD, and Susan Parks, MD The frequency of chronic illness increases with age. As a result, elderly persons receive
REVIEW Medication Prescribing for Older Adults Barbara Roehl, MD, MBA, Amy Talati, PharmD, and Susan Parks, MD The frequency of chronic illness increases with age. As a result, elderly persons receive
Management of Delirium in Hospice Patients
 Presentation Objectives Management of Delirium in Hospice Patients Lynn Williams, BSPharm Clinical Pharmacist Hospice Pharmacy Solutions Identify the clinical features of delirium Understand the underlying
Presentation Objectives Management of Delirium in Hospice Patients Lynn Williams, BSPharm Clinical Pharmacist Hospice Pharmacy Solutions Identify the clinical features of delirium Understand the underlying
Appendix 3: Screening Tool of Older Persons Prescriptions (STOPP) version 2.
 STOPP/START criteria for potentially inappropriate prescribing in older people: version 2 By Denis O'Mahony, David O'Sullivan, Stephen Byrne, Marie Noelle O'Connor, Cristin Ryan and Paul Gallagher Age
STOPP/START criteria for potentially inappropriate prescribing in older people: version 2 By Denis O'Mahony, David O'Sullivan, Stephen Byrne, Marie Noelle O'Connor, Cristin Ryan and Paul Gallagher Age
Polypharmacy: Guidance for Prescribing in Frail Adults
 Polypharmacy: Guidance for Prescribing in Frail Adults Why is reviewing polypharmacy important? Medication is by far the most common form of medical intervention. Four out of five people aged over 75 years
Polypharmacy: Guidance for Prescribing in Frail Adults Why is reviewing polypharmacy important? Medication is by far the most common form of medical intervention. Four out of five people aged over 75 years
 20.9 15.4 3.1 0.1 0.2 0.2 0.3 0.4 0.6 0.9 1.5 2.2 9.6 6.1 7.3 4.2 1900 1910 1920 1930 1940 1950 1960 1970 1980 1990 2000 2010 2020 2030 2040 2050 All Ages Age 65+ Age 85+ Female 50.9% Male 49.1% Female
20.9 15.4 3.1 0.1 0.2 0.2 0.3 0.4 0.6 0.9 1.5 2.2 9.6 6.1 7.3 4.2 1900 1910 1920 1930 1940 1950 1960 1970 1980 1990 2000 2010 2020 2030 2040 2050 All Ages Age 65+ Age 85+ Female 50.9% Male 49.1% Female
Insomnia: Updates in Medical Management. Michael Newnam M.D.
 Insomnia: Updates in Medical Management Michael Newnam M.D. Sleep Neurobiology Delicate balance of excitatory and inhibitory neurotransmitters that control the switch between wakefulness and sleep Circadian
Insomnia: Updates in Medical Management Michael Newnam M.D. Sleep Neurobiology Delicate balance of excitatory and inhibitory neurotransmitters that control the switch between wakefulness and sleep Circadian
Deprescribing Unnecessary Medications: A Four-Part Process
 Deprescribing Unnecessary Medications: A Four-Part Process Scott Endsley, MD Fam Pract Manag. 2018;25(3):28-32. Abstract and Introduction Introduction www.medscape.com Ms. Horatio is a 76-year-old patient
Deprescribing Unnecessary Medications: A Four-Part Process Scott Endsley, MD Fam Pract Manag. 2018;25(3):28-32. Abstract and Introduction Introduction www.medscape.com Ms. Horatio is a 76-year-old patient
High risk medications in the elderly/ Beers criteria updates
 High risk medications in the elderly/ Beers criteria updates Date- 9/9/2016 Matt Just, Pharm.D., CGP and Jordan Wolf, Pharm.D., CGP Thrifty White Pharmacy Wi-fi Information: NETWORK: EC-CTR PASSWORD: westgate252
High risk medications in the elderly/ Beers criteria updates Date- 9/9/2016 Matt Just, Pharm.D., CGP and Jordan Wolf, Pharm.D., CGP Thrifty White Pharmacy Wi-fi Information: NETWORK: EC-CTR PASSWORD: westgate252
Deconstructing Polypharmacy. Alan B. Douglass, M.D. Director
 Deconstructing Polypharmacy Alan B. Douglass, M.D. Director Recognize this patient? Mrs. Brown- 82 years young Active Medical Problems Hypertension Hyperlipidemia Type 2 Diabetes Peripheral edema Osteoarthritis
Deconstructing Polypharmacy Alan B. Douglass, M.D. Director Recognize this patient? Mrs. Brown- 82 years young Active Medical Problems Hypertension Hyperlipidemia Type 2 Diabetes Peripheral edema Osteoarthritis
Disclosures. Use caution in the elderly: review of safe and effective medication use in older patients. Institute of Medicine. Learning Objectives
 Use caution in the elderly: review of safe and effective medication use in older patients Disclosures I have no disclosures or conflicts of interest related to this presentation John T. Holmes, PharmD,
Use caution in the elderly: review of safe and effective medication use in older patients Disclosures I have no disclosures or conflicts of interest related to this presentation John T. Holmes, PharmD,
Anxiolytic, Sedative and Hypnotic Drugs. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Anxiolytic, Sedative and Hypnotic Drugs Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Anxiolytics: reduce anxiety Sedatives: decrease activity, calming
Anxiolytic, Sedative and Hypnotic Drugs Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Anxiolytics: reduce anxiety Sedatives: decrease activity, calming
Assessment of Drug Therapy in Geriatric Patients Using Beer s Criteria
 Original Article Assessment of Drug Therapy in Geriatric Patients Using Beer s Criteria RJ Lihite *, M Lahkar **, S Roy * Abstract Aim: Inappropriate medication use (IMU) in the elderly population has
Original Article Assessment of Drug Therapy in Geriatric Patients Using Beer s Criteria RJ Lihite *, M Lahkar **, S Roy * Abstract Aim: Inappropriate medication use (IMU) in the elderly population has
America s other drug problem: How to avoid medication-related problems in older adults
 America s other drug problem: How to avoid medication-related problems in older adults Melanie A. Dodd, Pharm.D., Ph.C., BCPS Associate Professor of Pharmacy in Geriatrics Vice-Chair, Department of Pharmacy
America s other drug problem: How to avoid medication-related problems in older adults Melanie A. Dodd, Pharm.D., Ph.C., BCPS Associate Professor of Pharmacy in Geriatrics Vice-Chair, Department of Pharmacy
Inappropriate drug prescribing in older adults: the updated 2002 Beers criteria a population-based cohort study
 DOI:10.1111/j.1365-2125.2005.02391.x British Journal of Clinical Pharmacology Inappropriate drug prescribing in older adults: the updated 2002 Beers criteria a population-based cohort study Cornelis S.
DOI:10.1111/j.1365-2125.2005.02391.x British Journal of Clinical Pharmacology Inappropriate drug prescribing in older adults: the updated 2002 Beers criteria a population-based cohort study Cornelis S.
Disclosures. Outline. Epidemiology. Medication Management in the Elderly. In 2008 pts age 65 and older represented 40% of all hospitalized adults
 Medication Management in the Elderly Disclosures Melissa Stevens MD Atlanta VA Medical Center Assistant Professor Emory University Department of Medicine I have no significant financial interest or other
Medication Management in the Elderly Disclosures Melissa Stevens MD Atlanta VA Medical Center Assistant Professor Emory University Department of Medicine I have no significant financial interest or other
Update in Geriatrics: Choosing Wisely Primum Non Nocere
 Joseph G. Ouslander, M.D. Professor of Clinical Biomedical Science Senior Associate Dean for Geriatric Programs Chair, Department of Integrated Medical Science Charles E. Schmidt College of Medicine Professor
Joseph G. Ouslander, M.D. Professor of Clinical Biomedical Science Senior Associate Dean for Geriatric Programs Chair, Department of Integrated Medical Science Charles E. Schmidt College of Medicine Professor
Polypharmacy. in the Elderly. Lesley Charles, MBChB, CCFP
 Polypharmacy in the Elderly Lesley Charles, MBChB, CCFP Associate Professor and Program Director Division of Care of the Elderly Department of Family Medicine, University of Alberta March 06, 2016 1 Faculty/Presenter
Polypharmacy in the Elderly Lesley Charles, MBChB, CCFP Associate Professor and Program Director Division of Care of the Elderly Department of Family Medicine, University of Alberta March 06, 2016 1 Faculty/Presenter
Pharmaceutical Care for Geriatrics
 Continuing Professional Pharmacy Development Program Pharmaceutical Care for Geriatrics Presented by: Alla El-Awaisi; MPharm, MRPharmS, MSc Event Organizer: Dr. Nadir Kheir; PhD Disclaimer: PRESENTING
Continuing Professional Pharmacy Development Program Pharmaceutical Care for Geriatrics Presented by: Alla El-Awaisi; MPharm, MRPharmS, MSc Event Organizer: Dr. Nadir Kheir; PhD Disclaimer: PRESENTING
Condition/Procedure Measure Compliance Criteria Reference Attribution Method
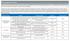 Premium Specialty: Cardiology Credentialed Specialties include: Cardiac Diagnostic, Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, and Interventional Cardiology This document is
Premium Specialty: Cardiology Credentialed Specialties include: Cardiac Diagnostic, Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, and Interventional Cardiology This document is
Beers Criteria: Practical Considerations. A Clinician Education Tool. Curt Wood, RPh, CGP, FASCP
 Beers Criteria: Practical Considerations A Clinician Education Tool Curt Wood, RPh, CGP, FASCP Objectives: u Explain the purpose of the Beers Criteria u Discuss the key concepts in applying the Beers Criteria
Beers Criteria: Practical Considerations A Clinician Education Tool Curt Wood, RPh, CGP, FASCP Objectives: u Explain the purpose of the Beers Criteria u Discuss the key concepts in applying the Beers Criteria
Potentially Harmful Drugs in the Elderly: Beers List
 PL Detail-Document #311201 This PL Detail-Document gives subscribers additional insight related to the Recommendations published in PHARMACIST S LETTER / PRESCRIBER S LETTER December 2015 Potentially Harmful
PL Detail-Document #311201 This PL Detail-Document gives subscribers additional insight related to the Recommendations published in PHARMACIST S LETTER / PRESCRIBER S LETTER December 2015 Potentially Harmful
Medicine Related Falls Risk Assessment Tool (MrFRAT) User Guide for Age Related Residential Care Facility Staff in Hawke s Bay
 Medicine Related Falls Risk Assessment Tool (MrFRAT) User Guide for Age Related Residential Care Facility Staff in Hawke s Bay (Revised edition November 2015) The Medicine Related Falls Risk Assessment
Medicine Related Falls Risk Assessment Tool (MrFRAT) User Guide for Age Related Residential Care Facility Staff in Hawke s Bay (Revised edition November 2015) The Medicine Related Falls Risk Assessment
David Dosa MD, MPH Assistant Professor of Medicine and Community Health The Warren Alpert School of Medicine, Brown University Director, Primary Care
 David Dosa MD, MPH Assistant Professor of Medicine and Community Health The Warren Alpert School of Medicine, Brown University Director, Primary Care Geriatrics Clinic- Providence VAMC VA Grand Rounds
David Dosa MD, MPH Assistant Professor of Medicine and Community Health The Warren Alpert School of Medicine, Brown University Director, Primary Care Geriatrics Clinic- Providence VAMC VA Grand Rounds
Tranquilizers & Sedative-Hypnotics
 Tranquilizers & Sedative-Hypnotics 1 Tranquilizer or anxiolytic: Drugs used therapeutically to treat agitation or anxiety Sedative-Hypnotic: drugs used to sedate and aid in sleep Original sedatives (before
Tranquilizers & Sedative-Hypnotics 1 Tranquilizer or anxiolytic: Drugs used therapeutically to treat agitation or anxiety Sedative-Hypnotic: drugs used to sedate and aid in sleep Original sedatives (before
Using the ASCP-NCOA Falls Risk Reduction Toolkit Part 1: A Companion to CDC's STEADI Toolkit
 Using the ASCP-NCOA Falls Risk Reduction Toolkit Part 1: A Companion to CDC's STEADI Toolkit Target Audience: Pharmacists ACPE#: 0202-9999-18-056-L01-P Activity Type: Application-based Disclosures Kathleen
Using the ASCP-NCOA Falls Risk Reduction Toolkit Part 1: A Companion to CDC's STEADI Toolkit Target Audience: Pharmacists ACPE#: 0202-9999-18-056-L01-P Activity Type: Application-based Disclosures Kathleen
Allergy: Levocetirizine (Xyzal) (F) Desloratadine (Clarinex) (NF) OTC Cetirizine (Zyrtec) (NF) OTC Loratadine (Claritin) (NF) Dexchlorpheniramine
 Anticholinergics Brompheniramine Carbinoxamine Chlorpheniramine Clemastine Cyproheptadine Highly anticholinergic, clearance reduced with advanced age, and tolerance develops when used as hypnotic; greater
Anticholinergics Brompheniramine Carbinoxamine Chlorpheniramine Clemastine Cyproheptadine Highly anticholinergic, clearance reduced with advanced age, and tolerance develops when used as hypnotic; greater
Conflict of interest declaration and sources of funding
 Potentially Inappropriate Prescribing immediately prior to Long-Term Care admission (PIP in LTC): Validation of tools for their future use across Ontario Bruyère CLRI Webinar March 24 th, 2016 and Bruyère
Potentially Inappropriate Prescribing immediately prior to Long-Term Care admission (PIP in LTC): Validation of tools for their future use across Ontario Bruyère CLRI Webinar March 24 th, 2016 and Bruyère
Safe Medication Use. Holly Divine, PharmD, CGP, CDE. University of Kentucky College of Pharmacy Department of Pharmacy Practice & Science
 Safe Medication Use in the Older Adult Holly Divine, PharmD, CGP, CDE Associate Professor University of Kentucky College of Pharmacy Department of Pharmacy Practice & Science Objectives Know the principles
Safe Medication Use in the Older Adult Holly Divine, PharmD, CGP, CDE Associate Professor University of Kentucky College of Pharmacy Department of Pharmacy Practice & Science Objectives Know the principles
Anthony J. Caprio, MD, CMD, AGSF 1
 Objectives 1) Discuss the dangers of polypharmacy 2) Review potentially inappropriate medications for older adults Doc, I think I am taking too many medications! 3) Develop strategies for prioritizing
Objectives 1) Discuss the dangers of polypharmacy 2) Review potentially inappropriate medications for older adults Doc, I think I am taking too many medications! 3) Develop strategies for prioritizing
Session ID: 1005 June 15, Older Adults. Director of Clinical and Educational Programs Peter Lamy Center on Drug Therapy and Aging
 Mdi Medication Misadventures in Older Adults Nicole Brandt, PharmD, CGP, BCPP, FASCP Director of Clinical and Educational Programs Peter Lamy Center on Drug Therapy and Aging AssociateProfessor Professor,
Mdi Medication Misadventures in Older Adults Nicole Brandt, PharmD, CGP, BCPP, FASCP Director of Clinical and Educational Programs Peter Lamy Center on Drug Therapy and Aging AssociateProfessor Professor,
An approach to prescribing in the elderly. Preamble
 An approach to prescribing in the elderly Dr K Outhoff Preamble Advances in medical technology, surgical procedures, medical practice and innovative drug development An increasing proportion of the population
An approach to prescribing in the elderly Dr K Outhoff Preamble Advances in medical technology, surgical procedures, medical practice and innovative drug development An increasing proportion of the population
Polypharmacy Preventing Unnecessary Medications for Older Adults
 Polypharmacy Preventing Unnecessary Medications for Older Adults Robert Sonntag MD, CMD, HMDC sonnt001@umn.edu 1 2 F329 in review Each residents drug regimen must be free from unnecessary drugs. An unnecessary
Polypharmacy Preventing Unnecessary Medications for Older Adults Robert Sonntag MD, CMD, HMDC sonnt001@umn.edu 1 2 F329 in review Each residents drug regimen must be free from unnecessary drugs. An unnecessary
De-prescribing in Older Adults. Wael Hamade, MD, FAAFP 04/08/2016
 De-prescribing in Older Adults Wael Hamade, MD, FAAFP 04/08/2016 DISCLOSURES None of the faculty, planners, speakers, providers nor CME committee has any relevant financial relationships with commercial
De-prescribing in Older Adults Wael Hamade, MD, FAAFP 04/08/2016 DISCLOSURES None of the faculty, planners, speakers, providers nor CME committee has any relevant financial relationships with commercial
Pharmacist CE LESSON. Reducing and eliminating high-risk medications in older adults 1 OCTOBER 2015
 By Tara Dymon, PharmD, BCACP, Clinical Pharmacist, Medicare Pharmacy Clinical Programs; Miranda Wilhelm, PharmD, Clinical Associate Professor, Southern Illinois University Edwardsville School of Pharmacy;
By Tara Dymon, PharmD, BCACP, Clinical Pharmacist, Medicare Pharmacy Clinical Programs; Miranda Wilhelm, PharmD, Clinical Associate Professor, Southern Illinois University Edwardsville School of Pharmacy;
When Less is More: Managing Medication for Older Adults
 When Less is More: Managing Medication for Older Adults Sunny Linnebur, PharmD, BCGP, BCPS Robert Page, PharmD, MSPH, BCGP, BCPS-AQ Cardiology Professors, University of Colorado Skaggs School of Pharmacy
When Less is More: Managing Medication for Older Adults Sunny Linnebur, PharmD, BCGP, BCPS Robert Page, PharmD, MSPH, BCGP, BCPS-AQ Cardiology Professors, University of Colorado Skaggs School of Pharmacy
Rational prescribing in the older adult. Assoc Prof Craig Whitehead
 Rational prescribing in the older adult Assoc Prof Craig Whitehead Introduction Physioloical ageing and frailty Medication risks in older adults Drug Burden Anticholinergic and sedative drug burden Cascade
Rational prescribing in the older adult Assoc Prof Craig Whitehead Introduction Physioloical ageing and frailty Medication risks in older adults Drug Burden Anticholinergic and sedative drug burden Cascade
Medication safety in vulnerable patient groups - Elderly patients -
 Woodennature/CC-BY-SA-3.0 http://theintelligence.de Medication safety in vulnerable patient groups - Elderly patients - 20th Congress of EAHP 25-27 March, 2015, Hamburg, Germany Dr. rer. nat. Beate Wickop
Woodennature/CC-BY-SA-3.0 http://theintelligence.de Medication safety in vulnerable patient groups - Elderly patients - 20th Congress of EAHP 25-27 March, 2015, Hamburg, Germany Dr. rer. nat. Beate Wickop
Anxiety Pharmacology UNIVERSITY OF HAWAI I HILO PRE -NURSING PROGRAM
 Anxiety Pharmacology UNIVERSITY OF HAWAI I HILO PRE NURSING PROGRAM NURS 203 GENERAL PHARMACOLOGY DANITA NARCISO PHARM D Learning Objectives Understand the normal processing of fear vs fear processing
Anxiety Pharmacology UNIVERSITY OF HAWAI I HILO PRE NURSING PROGRAM NURS 203 GENERAL PHARMACOLOGY DANITA NARCISO PHARM D Learning Objectives Understand the normal processing of fear vs fear processing
PRESCRIBING PRACTICE IN DELIRIUM. John Warburton Critical Care Pharmacist
 PRESCRIBING PRACTICE IN DELIRIUM John Warburton Critical Care Pharmacist Learning outcomes Modifiable medication risk factors for delirium An appreciation of contributing factors modifiable with medicines
PRESCRIBING PRACTICE IN DELIRIUM John Warburton Critical Care Pharmacist Learning outcomes Modifiable medication risk factors for delirium An appreciation of contributing factors modifiable with medicines
Hypertension (JNC-8)
 Hypertension (JNC-8) Southern California University of Health Sciences Physician Assistant Program Management and Treatment of Hypertension April 17, 2018, presented by Ezra Levy, Pharm.D.! The 8 th Joint
Hypertension (JNC-8) Southern California University of Health Sciences Physician Assistant Program Management and Treatment of Hypertension April 17, 2018, presented by Ezra Levy, Pharm.D.! The 8 th Joint
Friend or Foe? Review of the Regulations & Benefits: Risk Profiles of the Benzodiazepines
 Friend or Foe? Review of the Regulations & Benefits: Risk Profiles of the Benzodiazepines Program Learning Objectives At the conclusion of the activity, participants should be able to: Have a basic understanding
Friend or Foe? Review of the Regulations & Benefits: Risk Profiles of the Benzodiazepines Program Learning Objectives At the conclusion of the activity, participants should be able to: Have a basic understanding
Legemiddelbruk og hoftebrudd
 Legemiddelbruk og hoftebrudd Oppsummering av ph.d. GerIT 05.04.16 LIS Marit Stordal Bakken Haraldsplass Diakonale Sykehus U N I V E R S I T Y O F B E R G E N Potentially inappropriate drug use and hip
Legemiddelbruk og hoftebrudd Oppsummering av ph.d. GerIT 05.04.16 LIS Marit Stordal Bakken Haraldsplass Diakonale Sykehus U N I V E R S I T Y O F B E R G E N Potentially inappropriate drug use and hip
University of Hawaii Center on Aging
 University of Hawaii Center on Aging. Supported in part by a cooperative agreement No. 90AL0011-01-00 from the Administration on Aging, Administration for Community Living, U.S. Department of Health and
University of Hawaii Center on Aging. Supported in part by a cooperative agreement No. 90AL0011-01-00 from the Administration on Aging, Administration for Community Living, U.S. Department of Health and
