Deep brain stimulation for camptocormia in dystonia and Parkinson s disease
|
|
|
- Joleen Dixon
- 6 years ago
- Views:
Transcription
1 J Neurol (2011) 258: DOI /s ORIGINAL COMMUNICATION Deep brain stimulation for camptocormia in dystonia and Parkinson s disease Hans-Holger Capelle Christoph Schrader Christian Blahak Wolfgang Fogel Thomas M. Kinfe Hansjoerg Baezner Joachim K. Krauss Received: 18 December 2009 / Revised: 20 July 2010 / Accepted: 28 July 2010 / Published online: 28 August 2010 Ó Springer-Verlag 2010 Abstract Camptocormia, or bent spine syndrome, may occur in various movement disorders such as primary dystonia or idiopathic Parkinson s disease (PD). Although deep brain stimulation (DBS) is an established treatment in refractory primary dystonia and advanced PD, few data are available on the effect of DBS on camptocormia comparing these two conditions. Seven patients (4 with dystonia, 3 with PD; mean age 60.3 years at surgery, range years) with camptocormia were included in the study. Five patients underwent bilateral GPi DBS and two patients underwent bilateral STN DBS guided by CT-stereotactic surgery and microelectrode recording. Pre- and postoperative motor assessment included the BFM in the dystonia patients and the UPDRS in the PD patients. Severity of camptocormia was assessed by the BFM subscore for the trunk at the last available follow-up at a mean of 17.3 months (range 9 36 months). There were no surgical complications. In the four patients with dystonia there was a mean improvement of 53% in the BFM motor score (range 41 79%) and of 63% (range 50 67%) in the BFM H.-H. Capelle T. M. Kinfe J. K. Krauss (&) Department of Neurosurgery, Medical School Hannover, MHH, Carl-Neuberg-Straße 1, Hannover, Germany krauss.joachim@mh-hannover.de C. Schrader Department of Neurology, Medical School Hannover, MHH, Hannover, Germany C. Blahak H. Baezner Department of Neurology, University Hospital Mannheim, Mannheim, Germany W. Fogel Department of Neurology, Deutsche Klinik für Diagnostik, Wiesbaden, Germany subscore for the trunk at the last available follow-up (mean 14.3 months, range 9 18 months). In the three patients with camptocormia in PD who underwent bilateral STN DBS (2 patients) or pallidal DBS (1 patient), the PD symptoms improved markedly (mean improvement in the UPDRS motor subscore stimulation on/medication off 55%, range 49 61%), but there was no or only mild improvement of camptocormia in the two patients who underwent STN DBS, and only moderate improvement in the patient with GPi DBS at the last available follow-up (mean 21 months, range months). GPi DBS is an effective treatment for camptocormia in dystonia. The response of camptocormia to chronic STN or GPi DBS in PD is more heterogenous. The latter may be due to a variety of causes and needs further clarification. Keywords Camptocormia Deep brain stimulation Dystonia Parkinson s disease Introduction Camptocormia, or bent spine syndrome, is defined as a forced posture with a forward-bent trunk which increases during standing or walking and vanishes in the recumbent position [1]. Azher and Jankovic [1] recently proposed classifying camptocormia according to etiology. Camptocormia may occur in movement disorders, most frequently in Parkinson s disease (PD) and in primary dystonia [2, 3]; it may be a sequel of stroke, spine deformities, spine surgery, or of psychogenic origin [4, 5]; and, finally, it can develop due to myopathic changes, including inflammatory or metabolic mitochondrial myopathies of the erector spinae muscle [6]. This etiologic classification is important, since treatment options for camptocormia depend crucially
2 J Neurol (2011) 258: on the etiology. For camptocormia in PD and primary dystonia, drugs including levodopa, anticholinergics, muscle relaxants and tetrabenazine are frequently tried, however, in most cases only minimal or no effect at all is achieved. Chronic deep brain stimulation (DBS) of the posteroventral lateral globus pallidus internus (GPi) and the subthalamic nucleus (STN) has been established as a powerful tool in the treatment of refractory primary dystonia and of advanced PD [7 13]. There are few data available, however, on the effect of DBS on camptocormia in dystonia or in PD [1, 14 17]. Here, we report a series of seven patients with camptocormia in dystonia or in PD to evaluate the effect of chronic DBS and to determine whether the therapeutic response depends on etiology. s and methods Seven patients with disabling camptocormia were included in this prospective study. Mean age at surgery was 60.3 years (range years). s were included only when camptocormia constituted a component of significant disability and a primary indication for surgery. All patients were assessed according to a standard protocol and video tape recording which included the Burke Fahn Marsden (BFM) scale in dystonia and the unified Parkinson s disease rating scale (UPDRS) in PD preoperatively and at scheduled follow-up investigations. To assess the severity of camptocormia and to evaluate the effect of DBS, the BFM motor subscore for the trunk was used (range 0 16 points). In addition, pre- and postoperative low back pain scores (visual analogue scale, range 0 10; with 0 = no pain, 10 = worst pain) and postoperative patient s self rating scores (0 100%; with 0% = no effect, 100% = excellent improvement) for the effect of DBS on their camptocormia were ascertained. Three patients had camptocormia embedded in a clinical picture of segmental or generalized dystonia (2 m/l f, mean age 50 years at surgery, years). Oral medication including trihexiphenidyl, levodopa and benzodiazepines, as well as repeated botulinum toxin (BTX) injections did not yield therapeutic benefit for their camptocormia. 4 (f, 69 years old) presented with disabling camptocormia without other dystonic features or PD symptoms. In this patient, histological examination of a biopsy of the erector trunci muscle which was performed 2 years earlier had shown findings consistent with a myopathy. Since she suffered markedly but her camptocormia was refractory to medication with biperiden and levodopa, as well as to extensive physiotherapy, DBS was offered to her as an optional treatment. s 1 4 were scheduled for bilateral GPi DBS. Demographic and clinical data are summarized in Table 1. Three patients suffered from advanced idiopathic PD according to UK brain bank criteria (3 men, mean age 67.3 years at surgery, years; see Table 1). None of Table 1 Diagnostic and clinical data of seven patients with camptocormia in dystonia or in PD Age/sex Disorder Duration of movement disorder Medication preoperative (LEDD) Medication postoperative at last available follow-up 1 72/F Segmental dystonia 25 years Levodopa Clonazepam Trihexiphenidyl Tetrabenazine Clonazepam Bromazepam Botulinum toxine A injections 2 39/M Segmental dystonia 13 years Trihexiphenidyl None Botulinum toxine A injections 3 40/M Generalized dystonia 15 years Trihexiphenidyl Trihexiphenidyl Levodopa 4 69/F Isolated dystonic camptocormia 5 years Biperiden None (associated with myopathy) Levodopa 5 73/M Parkinson s disease 12 years LEDD 1100 mg LEDD 900 mg 6 65/M Parkinson s disease 15 years LEDD 570 mg LEDD 570 mg Amantadin Baclofen Baclofen 7 64/M Parkinson s disease 10 years LEDD 800 mg LEDD 800 mg LEDD levodopa equivalent daily dose
3 98 J Neurol (2011) 258: them showed signs of psychosis or had cognitive deficits according to the preoperative assessments. Dopaminergic medication improved the cardinal symptoms of their PD, yet it was ineffective for camptocormia. All three patients had marked degenerative spinal disorders including multilevel osteochondrosis and spondylarthrosis. s 5 and 6 suffered also from motor fluctuations and were therefore scheduled for bilateral STN DBS. 7 was scheduled for DBS of the posteroventral lateral GPi. The target for implantation of the DBS electrodes was defined by MR imaging and CT-stereotactic imaging as described in detail elsewhere [18]. The preliminary target for the GPi was 20 mm lateral to and 4 mm below the intercommissural line, and 2 3 mm anterior to the intercommissural midpoint. The preliminary target for the STN was 12 mm lateral to and 4 mm below the intercommissural line, and 4 mm posterior to the intercommissural midpoint. All patients, except for patient 4, were operated under local anaesthesia. The detailed surgical procedure has been reported elsewhere [18]. Microelectrode recordings (MER) were performed to delineate the target in the GPi or STN further. MER for the pallidum started at 15 mm above the target. To place the electrodes into the sensorimotor part of the GPi, passive movements of the contralateral joints were conducted intraoperatively and were linked to the response in the MER. Based on the mapping of neurons and the response to passive movements, the DBS electrode was implanted so that contact 1 and 2 (electrode 3387, Medtronic) were placed within the sensorimotor part of the GPi. Macrostimulation was used to assess the thresholds for visual phosphenes or capsular responses. For localization of the STN, MER started at 10 mm above target. Again, passive movements of the contralateral joints were performed intraoperatively along the trajectory to locate the dorsolateral part of the STN. The DBS electrode (model 3389, Medtronic, Minneapolis, MN, USA) was placed so that contact 2 was in the dorsolateral portion of the nucleus and contact 3 at the border to or in the zona incerta. Macrostimulation was used to assess thresholds for paraesthesias and capsular responses. Electrode localizations were controlled by postoperative stereotactic CT scans. Additionally, the stereotactic CT scans were matched with the preoperative MR scans to determine the morphological position of the electrodes inside the GPi or STN. Postoperative programming of the stimulator settings were performed as described elsewhere in detail [18]. For the GPi we routinely used a bipolar configuration with contact 1 as the cathode and contact 2 as the anode. In the beginning of stimulation the frequency was set at 130 Hz, and pulse width at 210 ls, but could subsequently be adjusted to other settings to achieve optimal efficacy. In the following 6 8 weeks the amplitude was increased stepwise up to V in case there were no stimulation-induced side effects, such as hypokinetic dysarthria. If satisfactory clinical improvement occurred, the amplitude was not further increased. Otherwise, the amplitude was increased up to 6 V. At this stage, monopolar stimulation via single contacts was also evaluated. For the STN we routinely started stimulation in a unipolar setting with contact 2 as the cathode. The frequency was set at 130 Hz, and pulse width at 60 ls. The amplitude was adapted according to the effect on the PD symptoms and occurrence of stimulationinduced side effects. Impedances of all electrode contacts were checked routinely at follow-up visits. Localization of the electrodes and their contacts within the target region was confirmed in all patients. Two single channel pacemakers were used in five patients (Soletra, Medtronic) and a dual channel pacemaker in two (Kinetra, Medtronic). The percentage of improvement for the pre- and postoperative BFM motor scores, the BFM motor subscores for the trunk, and for the low back pain scores was calculated as follows: [(score preoperative-score postoperative)/score preoperative] The statistical analysis was performed using a paired t-test. In case of failed normality test of data, the Wilcoxon signed-rank test was used for analysis. For statistical analysis of two independent groups an unpaired t-test was used; in case of failed normality test of data the Wilcoxon rank sum test was used (SigmaStat Software; SPSS Inc., Chicago, IL, USA). For patients self rating the percentage of improvement was used for the statistical analysis. Results There were no surgery-related complications in any instance. All patients experienced sustained benefit of dystonia or of the cardinal PD symptoms, respectively (Table 2; Fig. 1). In the four patients with dystonia, there was a mean improvement by 53% (range, 41 79%; p = 0.135) according to the BFM motor score after a mean follow-up period of 14.3 months (range, 9 18 months). The three patients with PD who underwent bilateral STN DBS (2 patients) or GPi DBS (1 patient) showed a mean of 55% improvement (range, 49 61%; p \ 0.001) in the UPDRS motor subscore medication off/stimulation on, compared to the preoperative medication off state at the last available follow-up at a mean of 21 months (range, months). The pre- and postoperative BFM and UPDRS motor scores are summarized in Table 2. Camptocormia was improved in six of the seven patients. The mean change in all seven patients was 44% (range, 0 67%, p = 0.007) according to the BFM motor
4 J Neurol (2011) 258: Table 2 Pre- and postoperative BFM motor (patients with dystonia) and UPDRS motor scores (patients with Parkinson s disease) and BFM motor subscores for the trunk BFM motor subscore trunk at last available FU (provoking 9 severity factor) BFM motor last available FU Last available follow-up in months BFM motor subscore trunk preoperative (provoking 9 severity factor) BFM motor preoperative Target of DBS 1 GPi (4 9 3) (2 9 2) 2 GPi (4 9 3) (2 9 2) 3 GPi (4 9 3) (2 9 2) 4 GPi (4 9 3) (3 9 2) BFM motor subscore trunk at last available FU (provoking 9 severity factor) UPDRS III (med off/stim on) last available FU Last available follow-up in months BFM motor subscore trunk preoperative (provoking 9 severity factor) UPDRS III preoperative (med off/on) Target of DBS 5 STN 43/21 8 (4 9 2) (3 9 2) 6 STN 36/15 12 (4 9 3) (4 9 3) 7 GPi 47/25 9 (3 9 3) (2 9 3) Summarized pre- and postoperative BFM motor (patients with dystonia) and UPDRS motor scores (patients with Parkinson s disease) of the seven patients at the last available follow-up at a mean of 17.3 months (range, 9 36 months). The second score for all patients shows the BFM motor subscore for the trunk to assess camptocormia UPDRS unified Parkinson s disease rating scale; BFM Burke Fahn Marsden dystonia rating scale Relative improvement of BFM or UPDRS motor score (%) Relative improvement of BFM motor subscore for the trunk (%) Fig. 1 Relative improvement of the BFM motor scores and the BFM motor subscores for the trunk in dystonia patients (patients 1 4) and PD patients (patients 5 7) at the last available follow-up. The left columns show the improvement (in % as compared to baseline) of the BFM or UPDRS motor scores, the right columns show the improvement (in % as compared to baseline) of the BFM motor subscore for the trunk as a measurement for camptocormia subscore for the trunk at the last available follow-up at a mean of 17.3 months (range, 9 36 months). In the patients with dystonia, pallidal DBS yielded marked and sustained improvement of their camptocormia. Compared to the preoperative BFM motor subscore for the trunk, patients with camptocormia in dystonia showed a mean improvement of 63% (range, 50 67%; p = 0.125) at the last available follow-up at a mean of 14.3 months (range, 9 18 months). 4 initially experienced a more unstable benefit with no improvement of her camptocormia after initiation of stimulation but reported more marked improvement at 18 months after changing stimulation frequency, which was reflected by 50% improvement in the BFM subscore for the trunk. Figure 2 shows pre- and postoperative video stills at the last follow-up (Fig. 2). In the four dystonia patients, scores for low back pain improved by a mean of 42% (range, 33 50%; p = 0.03) (Fig. 3). The effect of DBS as estimated by the patients self rating score indicated a 58% mean improvement as compared to baseline (range, 50 70%; p = 0.001) at the last available follow-up. The three PD patients experienced improvement of camptocormia by a mean of 19% (range, 0 33%; p = 0.199) according to the BFM subscore for the trunk at the last available follow-up at a mean of 21 months (range,
5 100 J Neurol (2011) 258: Fig. 2 Video stills of patient 4 preoperatively and at 18-month follow-up with stimulation frequency set to 60 Hz A Visual Analogue Scale B Effect on camptocormia % Low back pain score preoperative Low back pain score postoperative s self rating scores: Effect of DBS on camptocormia % Fig. 3 a Pre- and postoperative low back pain scores. b s self rating scores on the effect of DBS on camptocormia. VAS, visual analogue scale; patients self rating: range 0 100%; 0%, no effect, 100%, excellent improvement months). 7, who underwent GPi DBS, showed the most pronounced improvement of his camptocormia among the PD patients by 33% at 36 months followup. The UPDRS motor subscore was improved by 49%. Dopaminergic medication was nearly equivalent to preoperative levels in all three patients at the last follow-up. Scores for low back pain changed according to the preoperative VAS by a mean of 13% (range, 0 25%; p = 0.225) (Fig. 3). s self rating score showed a mean change of 20% (range, 0 40%; p = 0.225) at the last follow-up. In the patients with dystonia, the camptocormia improvement was more pronounced than in the patients with PD (p = 0.057), comparing the BFM motor subscore for the trunk at baseline and at the last available follow-up (Fig. 1). The patients self rating scores in the dystonia patients were higher at the last available follow-up than were those of the PD patients (mean improvement of 58 vs. 20%; p = 0.057) (see Fig. 3). Stimulation settings at the last follow-up were as follows. s 1 3 were on bipolar stimulation (cathode contact 1, anode contact 2): mean amplitude 4.2 V, pulse width 210 ls, frequency 130 Hz. 4 had no benefit of camptocormia at 12 months postoperatively but developed shuffling gait with difficulty walking while on bipolar stimulation at 7 V and 130 Hz. After setting the frequency to 60 Hz, the gait disorder disappeared and there was consistent improvement of camptocormia at 3 V. At the last follow-up, the PD patient with GPi DBS was on bipolar stimulation with contact 1 set negative and 2 positive, the patients with STN DBS were on unipolar stimulation with contact 2 negative and the impulse generator positive. In STN DBS mean amplitude was 3.1 V, pulse width 60 ls, and frequency 130 Hz. In the patient with GPi DBS the amplitude was 3.5 V, pulse width 210 ls, and frequency 130 Hz. 7 presented with deterioration of his camptocormia due to battery depletion at 24 months postoperatively. After changing the pacemakers, camptocormia improved within days to the same extent as before. Discussion Our prospective study on the effect of DBS on camptocormia in seven patients presents the largest systematic
6 J Neurol (2011) 258: long-term follow-up study thus far. It demonstrates clearly that chronic DBS of the posteroventral lateral GPi yields sustained improvement in patients with camptocormia due to dystonia. The effect on camptocormia with pallidal DBS is comparable with the range of improvement for dystonia in general [7, 8, 11, 19, 20]. Changes of objective measurements for camptocormia were paralleled by patients self rating indices postoperatively. Furthermore, subjective improvement of back pain was in a similar range. The experience with pallidal DBS for camptocormia in dystonia is limited. Only a few patients had been reported earlier [14, 15, 21]. The results are summarized in Table 3. The beneficial effect of DBS was demonstrated first by Nandi and colleagues in a patient with tardive dystonia with sustained improvement at 6 months postoperatively. Fukaya et al. [15] mentioned three patients with camptocormia in a series of 36 patients with primary dystonia undergoing bilateral GPi DBS. They observed substantial improvement in camptocormia which was more pronounced than improvement of other dystonic symptoms. Camptocormia, however, was not assessed with a specific score. The postoperative course of patient 4 who was diagnosed as having a myopathy is puzzling. While myopathy has been thought by some to be the actual cause of camptocormia, it should also be considered that the focal myopathic changes in the truncal muscles might rather be a secondary phenomenon [22]. While chronic stimulation at 130 Hz yields good improvement of dystonia in the majority of patients with primary dystonia, recent observations indicate that mild parkinsonian symptoms might occur in a subset of patients [23, 24]. This is also reflected in the appearance of micrographia in patients with segmental dystonia upon chronic pallidal DBS [25]. It is somehow unusual that a parkinsonian gait disorder became manifest in our patient at 130 Hz stimulation without any Table 3 DBS for camptocormia: literature review Author/year, age Etiology of camptocormia Improvement of camptocormia Procedure Follow-up (months) Nandi et al. (2002) 1 patient, 39 Camptocormia in dystonia (tardive) Marked improvement 6 months Micheli et al. (2005) 1 patient, 62 Camptocormia in Parkinson s disease 90% 14 months Azher and Jankovic 1 patient, n.a. Camptocormia in Parkinson s disease No improvement of camptocormia (2005) Bilateral STN DBS PD symptoms improved Hellman et al. 1 patient, 53 Camptocormia in Parkinson s disease Marked improvement (2006) Bilateral STN DBS 10 months Fukaya et al. (2006) 3 patients out of 36 patients with Idiopathic camptocormia, camptocormia in 92.2% (±5.3%) primary dystonia dystonia 14 months Yamada et al. (2006) 1 patient, 71 Camptocormia in Parkinson s disease 75% Bilateral STN DBS 20 months Sako et al. (2009) O Riordan et al. (2009) 6 patients, mean age 60, range patients, mean age 64, range Capelle et al. (2010) 7 patients, mean age 60, range Camptocormia in Parkinson s disease Bilateral STN DBS Camptocormia in dystonia [1] Camptocormia in Parkinson s disease [2] 78% (±9.1%), Improvement of thoracolumbar angle 17 months Marked improvement of camptocormia in dystonia 60 months No improvement/modest improvement in PD 6 months Camptocormia in dystonia [4] 63% (range, 50 67%) 14.3 months Camptocormia in Parkinson s disease [3] 19% (range, 0 33%) 21 months Bilateral STN DBS [2] [1]
7 102 J Neurol (2011) 258: improvement of camptocormia. The concept that stimulation with 60 Hz or lower might be more valuable in some dystonia patients than high-frequency stimulation has been introduced only recently [26]. It may be that an altered balance between neuronal inhibition and orthodromic and antidromic fibre stimulation of pallidal pathways underlies the differential effects, both on improvement of dystonia and the manifestation of bradykinetic symptoms. The effects of chronic DBS on camptocormia in PD were less gratifying. GPi DBS appeared to be more effective then STN DBS. Similar to the occurrence of foot dystonia in PD patients not treated with levodopa, camptocormia may be a unique form of a secondary segmental dystonia in PD [27]. Others have thought that camptocormia in PD is an extreme form of stooped posture which may be linked to dysfunction of the caudate nucleus or the external pallidum [22, 28]. These considerations may explain why our patient 7, who underwent GPi DBS, experienced the most benefit. In another series, pallidal DBS has been described as resulting in moderate improvement in one PD patient, and as ineffective in another [21]. Micheli et al. [29] also reported a PD patient in whom bilateral GPi DBS showed beneficial and sustained improvement of PD symptoms and of camptocormia by 90%. Although bilateral STN DBS resulted in satisfactory improvement in motor symptoms,as shown by changes in the UPDRS III scores, this was not paralleled by improvement of camptocormia. Data on the effect of DBS on camptocormia in PD published thus far have yielded quite variable results (see Table 3). While STN DBS resulted in limited benefit or had no effect on camptocormia in some patients, marked improvement was noted in others [1, 16, 30]. The only multipatient series was published by Sako et al. [17] recently. In this series of six patients, improvement of camptocormia was described in all patients after STN DBS. Improvement was defined as a change in the thoracolumbar angle which was sustained at a mean follow-up period of 17 months. A limitation of our study is that we did not systematically test contacts other than the contact located at the dorsal STN for chronic stimulation in the two patients with STN DBS to achieve a better effect on camptocormia. Since camptocormia usually does not respond to levodopa treatment [31] and STN DBS is thought to be effective mainly for the dopa-responsive symptoms of PD, the mechanisms by which STN DBS improves camptocormia in some patients while not in others remain unclear. Note that camptocormia has also been considered a form of off-period dystonia in some instances [16]. Apart from methodological differences such as study design, the use of various rating scales and duration of disease, other patient-specific variables that did not receive attention might be relevant. While all three patients included in our study had marked degenerative spinal disorders at the thoracolumbar level, there is very limited information available on that in previous reports. The absence of improvement of camptocormia in patient 6 may also be due to severe degenerative changes of his lumbar spine. This is also reflected by the minimal change in the low-back pain level postoperatively. Further study on the effect of chronic DBS on camptocormia in PD is needed to clarify if the responsiveness of camptocormia to dopaminergic medication might be a predictive positive factor. Regarding such differences in responsiveness to levodopa, pallidal DBS might be reconsidered in some PD patients with camptocormia. Conclusions Pallidal DBS provides beneficial improvement for camptocormia as a symptom of segmental or generalized dystonia. The response to DBS of camptocormia in PD patients is more heterogeneous. More studies are needed in the latter in order to define those patients who will benefit from DBS surgery. References 1. Azher SN, Jankovic J (2005) Camptocormia: pathogenesis, classification, and response to therapy. Neurology 65: Lepoutre AC, Devos D, Blanchard-Dauphin A, Pardessus V, Maurage CA, Ferriby D, Hurtevent JF, Cotten A, Destée A, Defebvre L (2006) A specific clinical pattern of camptocormia in Parkinson s disease. J Neurol Neurosurg Psychiatry 77: Tolosa E, Compta Y (2006) Dystonia in Parkinson s disease. J Neurol 253(Suppl 7):VII7 VII13 4. Duman I, Baklaci K, Tan AK, Kalyon TA (2008) Unusual case of camptocormia triggered by lumbar disc herniation. Clin Rheumatol 27: Skidmore F, Anderson K, Fram D, Weiner W (2007) Psychogenic camptocormia. Mov Disord 22: Gómez-Puerta JA, Peris P, Grau JM, Martinez MA, Guañabens N (2007) Camptocormia as a clinical manifestation of mitochondrial myopathy. Clin Rheumatol 26: Krauss JK, Pohle T, Weber S, Ozdoba C, Burgunder JM (1999) Bilateral stimulation of globus pallidus internus for treatment of cervical dystonia. Lancet 354: Krauss JK, Loher TJ, Weigel R, Capelle HH, Weber S, Burgunder JM (2003) Chronic stimulation of the globus pallidus internus for treatment of non-dyt1 generalized dystonia and choreoathetosis: 2-year follow up. J Neurosurg 98: Krack P, Pollak P, Limousin P, Hoffmann D, Xie J, Benazzouz A, Benabid AL (1998) Subthalamic nucleus or internal pallidal stimulation in young onset Parkinson s disease. Brain 121: Capelle HH, Weigel R, Krauss JK (2003) Bilateral pallidal stimulation for blepharospasm-oromandibular dystonia (Meige syndrome). Neurology 60:
8 J Neurol (2011) 258: Vidailhet M, Vercueil L, Houeto JL, Krystkowiak P, Benabid AL, Cornu P et al (2005) French Stimulation du Pallidum Interne dans la Dystonie (SPIDY) Study Group. Bilateral deep-brain stimulation of the globus pallidus in primary generalized dystonia. N Engl J Med 352: Blahak C, Wöhrle JC, Capelle HH, Bäzner H, Grips E, Weigel R, Hennerici MG, Krauss JK (2007) Tremor reduction by subthalamic nucleus stimulation and medication in advanced Parkinson s disease. J Neurol 254: Capelle HH, Krauss JK (2009) Neuromodulation in dystonia: Current aspects of deep brain stimulation. Neuromodulation 12: Nandi D, Parkin S, Scott R, Winter JL, Joint C, Gregory R et al (2002) Camptocormia treated with bilateral pallidal stimulation. J Neurosurg 97: Fukaya C, Otaka T, Obuchi T, Kano T, Nagaoka T, Kobayashi K et al (2006) Pallidal high-frequency deep brain stimulation for camptocormia: an experience of three cases. Acta Neurochir Suppl 99: Yamada K, Goto S, Matsuzaki K, Tamura T, Murase N, Shimazu H, Nagahiro S, Kuratsu J, Kaji R (2006) Alleviation of camptocormia by bilateral subthalamic nucleus stimulation in a patient with Parkinson s disease. Parkinsonism Relat Disord 12: Sako W, Nishio M, Maruo T, Shimazu H, Matsuzaki K, Tamura T, Mure H, Ushio Y, Nagahiro S, Kaji R, Goto S (2009) Subthalamic nucleus deep brain stimulation for camptocormia associated with Parkinson s disease. Mov Disord 24: Krauss JK, Grossman RG (2001) Principles and techniques of movement disorders surgery. In: Krauss JK, Jankovic J, Grossman RG (eds) Surgery for Parkinson s disease and movement disorders. Lippincott Williams & Wilkins, Philadelphia, pp Loher TJ, Capelle HH, Kaelin-Lang A, Weber S, Weigel R, Burgunder JM, Krauss JK (2008) Deep brain stimulation for dystonia: outcome at long-term follow-up (3 years or longer). J Neurol 255: Wöhrle JC, Blahak C, Kekelia K, Capelle HH, Baezner HJ, Weigel R, Krauss JK (2009) Chronic deep brain stimulation for segmental dystonia. Stereotact Funct Neurosurg 87: O Riordan S, Paluzzi A, Liu X, Aziz TZ, Nandi D, Bain PG (2009) Camptocormia response to bilateral globus pallidus interna stimulation in three patients. Mov Disord 24(Suppl 1):489 (Abstract) 22. Melamed E, Djaldetti R (2006) Camptocormia in Parkinson s disease. J Neurol 253(Suppl. 7):VII14 VII Berman BD, Starr PA, Marks WJ Jr, Ostrem JL (2009) Induction of bradykinesia with pallidal deep brain stimulation in patients with cranial-cervical dystonia. Stereotact Funct Neurosurg 87: Zauber SE, Watson N, Comella CL, Bakay RA, Metman LV (2009) Stimulation-induced parkinsonism after posteroventral deep brain stimulation of the globus pallidus internus for craniocervical dystonia. J Neurosurg 110: Blahak C, Capelle HH, Bäzner H, Kinfe T, Hennerici MG, Krauss JK (2009) Micrographia induced by bilateral pallidal deep brain stimulation for segmental dystonia. Mov Disord 24(Suppl 1):481 (Abstract) 26. Alterman RL, Miravite J, Weisz D, Shils JL, Bressman SB, Tagliati M (2007) Sixty hertz pallidal deep brain stimulation for primary torsion dystonia. Neurology 69: Stawek J, Derejko M, Lass P (2003) Camptocormia as a form of dystonia in Parkinson s disease. Eur J Neurol 10: Nieves AV, Miyasaki JM, Lang AE (2001) Acute onset dystonic camptocormia caused by lenticular lesions. Mov Disord 16: Micheli F, Cersósimo MG, Piedimonte F (2005) Camptocormia in a patient with Parkinson disease: beneficial effects of pallidal deep brain stimulation. J Neurosurg 103: Hellmann MA, Djaldetti R, Israel Z, Melamed E (2006) Effect of deep brain subthalamic stimulation on camptocormia and postural abnormalities in idiopathic Parkinson s disease. Mov Disord 21: Benatru I, Vaugoyeau M, Azulay JP (2008) Postural disorders in Parkinson s disease. Neurophysiol Clin 38:
Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
 Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
Deep Brain Stimulation: Patient selection
 Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Surgical Neurology International
 Surgical Neurology International SNI: Stereotactic, a supplement to Surgical Neurology International OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor Antonio A.
Surgical Neurology International SNI: Stereotactic, a supplement to Surgical Neurology International OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor Antonio A.
Effect of Neurostimulation on Camptocormia in Parkinson s Disease Depends on Symptom Duration
 RESEARCH ARTICLE Effect of Neurostimulation on Camptocormia in Parkinson s Disease Depends on Symptom Duration Walter J. Schulz-Schaeffer, MD, 1 * Nils G. Margraf, MD, 2 Sari Munser, MD, 2 Arne Wrede,
RESEARCH ARTICLE Effect of Neurostimulation on Camptocormia in Parkinson s Disease Depends on Symptom Duration Walter J. Schulz-Schaeffer, MD, 1 * Nils G. Margraf, MD, 2 Sari Munser, MD, 2 Arne Wrede,
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor
 Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration
 doi:10.1093/brain/awn120 Brain (2008), 131,1895^1902 Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration Ioannis U. Isaias, 1 Ron L. Alterman 2 and
doi:10.1093/brain/awn120 Brain (2008), 131,1895^1902 Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration Ioannis U. Isaias, 1 Ron L. Alterman 2 and
Surgical Treatment of Movement Disorders. Surgical Treatment of Movement Disorders. New Techniques: Procedure is safer and better
 Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
P rimary generalised dystonia (PGD) is a movement disorder
 1314 PAPER Effect of electrode contact location on clinical efficacy of pallidal deep brain stimulation in primary generalised dystonia S Tisch, L Zrinzo, P Limousin, K P Bhatia, N Quinn, K Ashkan, M Hariz...
1314 PAPER Effect of electrode contact location on clinical efficacy of pallidal deep brain stimulation in primary generalised dystonia S Tisch, L Zrinzo, P Limousin, K P Bhatia, N Quinn, K Ashkan, M Hariz...
Pallidal stimulation for acquired dystonia due to cerebral palsy: beyond 5 years
 ORIGINAL ARTICLE Pallidal stimulation for acquired dystonia due to cerebral palsy: beyond 5 years L. M. Romito a,b, *, G. Zorzi a, *, C. E. Marras c, A. Franzini a, N. Nardocci a and A. Albanese a,b a
ORIGINAL ARTICLE Pallidal stimulation for acquired dystonia due to cerebral palsy: beyond 5 years L. M. Romito a,b, *, G. Zorzi a, *, C. E. Marras c, A. Franzini a, N. Nardocci a and A. Albanese a,b a
Review Article Dystonia and the Role of Deep Brain Stimulation
 International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 193718, 5 pages doi:10.5402/2011/193718 Review Article Dystonia and the Role of Deep Brain Stimulation Thomas L. Ellis Wake
International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 193718, 5 pages doi:10.5402/2011/193718 Review Article Dystonia and the Role of Deep Brain Stimulation Thomas L. Ellis Wake
Deep Brain Stimulation: Indications and Ethical Applications
 Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
doi: /brain/awt009 Brain 2013: 136; Bilateral pallidal stimulation in cervical dystonia: blinded evidence of benefit beyond 5 years
 doi:10.1093/brain/awt009 Brain 2013: 136; 761 769 761 BRAIN A JOURNAL OF NEUROLOGY Bilateral pallidal stimulation in cervical dystonia: blinded evidence of benefit beyond 5 years Richard A. Walsh, 1,2
doi:10.1093/brain/awt009 Brain 2013: 136; 761 769 761 BRAIN A JOURNAL OF NEUROLOGY Bilateral pallidal stimulation in cervical dystonia: blinded evidence of benefit beyond 5 years Richard A. Walsh, 1,2
ORIGINAL CONTRIBUTION. Acute Deep-Brain Stimulation of the Internal and External Globus Pallidus in Primary Dystonia
 ORIGINAL CONTRIBUTION Acute Deep-Brain Stimulation of the Internal and External Globus Pallidus in Primary Dystonia Functional Mapping of the Pallidum Jean-Luc Houeto, MD, PhD; Jérôme Yelnik, MD, PhD;
ORIGINAL CONTRIBUTION Acute Deep-Brain Stimulation of the Internal and External Globus Pallidus in Primary Dystonia Functional Mapping of the Pallidum Jean-Luc Houeto, MD, PhD; Jérôme Yelnik, MD, PhD;
F unctional stereotactic surgery is now well established for
 PAPER Effect of chronic pallidal deep brain on off period dystonia and sensory symptoms in advanced Parkinson s disease T J Loher, J-M Burgunder, S Weber, R Sommerhalder, J K Krauss... See end of article
PAPER Effect of chronic pallidal deep brain on off period dystonia and sensory symptoms in advanced Parkinson s disease T J Loher, J-M Burgunder, S Weber, R Sommerhalder, J K Krauss... See end of article
Troubleshooting algorithms for common DBS related problems in tremor and dystonia
 Troubleshooting algorithms for common DBS related problems in tremor and dystonia Elena Moro, MD, PhD, FEAN, FAAN Movement Disorder Center, CHU Grenoble, Grenoble Alpes University, INSERM U1216, Grenoble,
Troubleshooting algorithms for common DBS related problems in tremor and dystonia Elena Moro, MD, PhD, FEAN, FAAN Movement Disorder Center, CHU Grenoble, Grenoble Alpes University, INSERM U1216, Grenoble,
ORIGINAL CONTRIBUTION. Subthalamic Stimulation in Parkinson Disease
 Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Supplementary Online Content
 Supplementary Online Content Miocinovic S, de Hemptinne C, Qasim S, Ostrem JL, Starr PA. Patterns of cortical synchronization in isolated dystonia compared with Parkinson disease. JAMA Neurol. Published
Supplementary Online Content Miocinovic S, de Hemptinne C, Qasim S, Ostrem JL, Starr PA. Patterns of cortical synchronization in isolated dystonia compared with Parkinson disease. JAMA Neurol. Published
Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech?
 Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech? Jana Zalmanowitz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences
Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech? Jana Zalmanowitz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences
ORIGINAL CONTRIBUTION. Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement
 ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
Parkinson's Disease Center and Movement Disorders Clinic
 Parkinson's Disease Center and Movement Disorders Clinic 7200 Cambridge Street, 9th Floor, Suite 9A Houston, Texas 77030 713-798-2273 phone www.jankovic.org Dystonia Diagnosis Dystonia is a neurologic
Parkinson's Disease Center and Movement Disorders Clinic 7200 Cambridge Street, 9th Floor, Suite 9A Houston, Texas 77030 713-798-2273 phone www.jankovic.org Dystonia Diagnosis Dystonia is a neurologic
10/13/2017. Disclosures. Deep Brain Stimulation in the Treatment of Movement Disorders. Deep Brain Stimulation: Objectives.
 Deep Brain Stimulation in the Treatment of Movement Disorders Disclosures None Eleanor K Orehek, M.D. Movement Disorders Specialist Noran Neurological Clinic 1 2 Objectives To provide an overview of deep
Deep Brain Stimulation in the Treatment of Movement Disorders Disclosures None Eleanor K Orehek, M.D. Movement Disorders Specialist Noran Neurological Clinic 1 2 Objectives To provide an overview of deep
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD
 PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
Deep Brain Stimulation and Movement Disorders
 Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep Brain Stimulation Surgery for Parkinson s Disease
 Deep Brain Stimulation Surgery for Parkinson s Disease Demystifying Medicine 24 January 2012 Kareem A. Zaghloul, MD, PhD Staff Physician, Surgical Neurology Branch NINDS Surgery for Parkinson s Disease
Deep Brain Stimulation Surgery for Parkinson s Disease Demystifying Medicine 24 January 2012 Kareem A. Zaghloul, MD, PhD Staff Physician, Surgical Neurology Branch NINDS Surgery for Parkinson s Disease
Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology
 Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Citation for published version (APA): Contarino, M. F. (2013). Improving surgical treatment for movement disorders
 UvA-DARE (Digital Academic Repository) Improving surgical treatment for movement disorders Contarino, M.F. Link to publication Citation for published version (APA): Contarino, M. F. (2013). Improving surgical
UvA-DARE (Digital Academic Repository) Improving surgical treatment for movement disorders Contarino, M.F. Link to publication Citation for published version (APA): Contarino, M. F. (2013). Improving surgical
SUPPLEMENTAL DIGITAL CONTENT
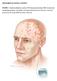 SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak, MD, PhD D.
 ARTICLES STN-DBS frequency effects on freezing of gait in advanced Parkinson disease C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak,
ARTICLES STN-DBS frequency effects on freezing of gait in advanced Parkinson disease C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak,
Deep Brain Stimulation: Surgical Process
 Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging
 J Neurosurg 103:949 955, 2005 Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging SIMONE HEMM, PH.D, GÉRARD
J Neurosurg 103:949 955, 2005 Deep brain stimulation in movement disorders: stereotactic coregistration of two-dimensional electrical field modeling and magnetic resonance imaging SIMONE HEMM, PH.D, GÉRARD
Case Report. Annals of Rehabilitation Medicine INTRODUCTION
 Case Report Ann Rehabil Med 2015;39(1):128-132 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.1.128 Annals of Rehabilitation Medicine Correction of Camptocormia Using a Cruciform
Case Report Ann Rehabil Med 2015;39(1):128-132 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.1.128 Annals of Rehabilitation Medicine Correction of Camptocormia Using a Cruciform
Treatment of Dystonia with Deep Brain Stimulation
 Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics Treatment of Dystonia with Deep Brain Stimulation Jill L. Ostrem* and Philip A. Starr *Department of Neurology,
Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics Treatment of Dystonia with Deep Brain Stimulation Jill L. Ostrem* and Philip A. Starr *Department of Neurology,
Parkinson disease: Parkinson Disease
 Surgical Surgical treatment treatment for for Parkinson disease: Parkinson Disease the Present and the Future the Present and the Future Olga Klepitskaya, MD Associate Professor of Neurology Co-Director,
Surgical Surgical treatment treatment for for Parkinson disease: Parkinson Disease the Present and the Future the Present and the Future Olga Klepitskaya, MD Associate Professor of Neurology Co-Director,
Subthalamic nucleus deep brain stimulation for severe idiopathic dystonia: impact on severity, neuropsychological status, and quality of life
 J Neurosurg 107:29 36, 2007 Subthalamic nucleus deep brain stimulation for severe idiopathic dystonia: impact on severity, neuropsychological status, and quality of life GALIT KLEINER-FISMAN, M.D., 1 GRACE
J Neurosurg 107:29 36, 2007 Subthalamic nucleus deep brain stimulation for severe idiopathic dystonia: impact on severity, neuropsychological status, and quality of life GALIT KLEINER-FISMAN, M.D., 1 GRACE
Dystonia: Title. A real pain in the neck. in All the Wrong Places
 Focus on CME at the University of Western Ontario Dystonia: Title in All the Wrong Places A real pain in the neck By Mandar Jog, MD, FRCPC and; Mary Jenkins, MD, FRCPC What is dystonia? Dystonia is a neurologic
Focus on CME at the University of Western Ontario Dystonia: Title in All the Wrong Places A real pain in the neck By Mandar Jog, MD, FRCPC and; Mary Jenkins, MD, FRCPC What is dystonia? Dystonia is a neurologic
Department of Physical Medicine and Rehabilitation, National Health Insurance Service Ilsan Hospital, Goyang, Korea
 Original Article Ann Rehabil Med 2017;41(4):677-685 pissn: 2234-0645 eissn: 2234-0653 https://doi.org/10.5535/arm.2017.41.4.677 Annals of Rehabilitation Medicine Back Extensor Strengthening Exercise and
Original Article Ann Rehabil Med 2017;41(4):677-685 pissn: 2234-0645 eissn: 2234-0653 https://doi.org/10.5535/arm.2017.41.4.677 Annals of Rehabilitation Medicine Back Extensor Strengthening Exercise and
Ablative procedures for the treatment of Parkinson s disease
 Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
EMERGING TREATMENTS FOR PARKINSON S DISEASE
 EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
The motor regulator. 1) Basal ganglia/nucleus
 The motor regulator 1) Basal ganglia/nucleus Neural structures involved in the control of movement Basal Ganglia - Components of the basal ganglia - Function of the basal ganglia - Connection and circuits
The motor regulator 1) Basal ganglia/nucleus Neural structures involved in the control of movement Basal Ganglia - Components of the basal ganglia - Function of the basal ganglia - Connection and circuits
A lthough levodopa treatment remains the gold standard
 1640 PAPER Stimulation of the subthalamic nucleus in Parkinson s disease: a 5 year follow up W M M Schüpbach, N Chastan, M L Welter, J L Houeto, V Mesnage, A M Bonnet, V Czernecki, D Maltête, A Hartmann,
1640 PAPER Stimulation of the subthalamic nucleus in Parkinson s disease: a 5 year follow up W M M Schüpbach, N Chastan, M L Welter, J L Houeto, V Mesnage, A M Bonnet, V Czernecki, D Maltête, A Hartmann,
The phenomenology and treatment of idiopathic adult-onset truncal dystonia: a retrospective review
 Ehrlich and Frucht Journal of Clinical Movement Disorders (2016) 3:15 DOI 10.1186/s40734-016-0044-9 RESEARCH ARTICLE Open Access The phenomenology and treatment of idiopathic adult-onset truncal dystonia:
Ehrlich and Frucht Journal of Clinical Movement Disorders (2016) 3:15 DOI 10.1186/s40734-016-0044-9 RESEARCH ARTICLE Open Access The phenomenology and treatment of idiopathic adult-onset truncal dystonia:
Dystonia is characterized by sustained muscle
 This article has been updated from its originally published version to replace Figure 2 and update the legend. See the corresponding erratum notice, DOI: 10.3171/10.3171/ 2013.11.JNS13844a, for full details.
This article has been updated from its originally published version to replace Figure 2 and update the legend. See the corresponding erratum notice, DOI: 10.3171/10.3171/ 2013.11.JNS13844a, for full details.
The oscillatory activity in the Parkinsonian subthalamic nucleus investigated using the macro-electrodes for deep brain stimulation
 Clinical Neurophysiology 113 (2002) 1 6 www.elsevier.com/locate/clinph The oscillatory activity in the Parkinsonian subthalamic nucleus investigated using the macro-electrodes for deep brain stimulation
Clinical Neurophysiology 113 (2002) 1 6 www.elsevier.com/locate/clinph The oscillatory activity in the Parkinsonian subthalamic nucleus investigated using the macro-electrodes for deep brain stimulation
DBS Programming. Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18
 DBS Programming Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18 Disclosure The University of Maryland has received research funding form InSightec and the Focused Ultrasound
DBS Programming Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18 Disclosure The University of Maryland has received research funding form InSightec and the Focused Ultrasound
Functional neurosurgery for the treatment of movement. Deep Brain Stimulation REVIEW ARTICLE. Drew S. Kern, MS,* and Rajeev Kumar, MD, FRCPC
 REVIEW ARTICLE Deep Brain Stimulation Drew S. Kern, MS,* and Rajeev Kumar, MD, FRCPC Background: Deep brain stimulation (DBS) for the treatment of neurologic diseases has markedly increased in popularity
REVIEW ARTICLE Deep Brain Stimulation Drew S. Kern, MS,* and Rajeev Kumar, MD, FRCPC Background: Deep brain stimulation (DBS) for the treatment of neurologic diseases has markedly increased in popularity
DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici
 DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici TECNICHE DI NEUROMODULAZIONE Invasiva: odeep Brain Stimulation Non Invasiva: o Transcranial Magnetic Stimulation (TMS) o Transcranial
DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici TECNICHE DI NEUROMODULAZIONE Invasiva: odeep Brain Stimulation Non Invasiva: o Transcranial Magnetic Stimulation (TMS) o Transcranial
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS)
 Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
No Financial Disclosures
 Deep Brain Stimulation: A Physician and Patient Perspective Jessica McClure Warren Marks, MD Cook Children s Medical Center Cook Children s Health Foundation Endowed Chair in Neurosciences Department of
Deep Brain Stimulation: A Physician and Patient Perspective Jessica McClure Warren Marks, MD Cook Children s Medical Center Cook Children s Health Foundation Endowed Chair in Neurosciences Department of
Dr Barry Snow. Neurologist Auckland District Health Board
 Dr Barry Snow Neurologist Auckland District Health Board Dystonia and Parkinson s disease Barry Snow Gowers 1888: Tetanoid chorea Dystonia a movement disorder characterized by sustained or intermittent
Dr Barry Snow Neurologist Auckland District Health Board Dystonia and Parkinson s disease Barry Snow Gowers 1888: Tetanoid chorea Dystonia a movement disorder characterized by sustained or intermittent
Patient selection for surgery: Hyperkinetic movement disorders
 Patient selection for surgery: Hyperkinetic movement disorders Alfons Schnitzler, MD, PhD Dept. of Neurology, Movement Disorder and Neuromodulation, Heinrich-Heine-University Düsseldorf, Germany Hyperkinetic
Patient selection for surgery: Hyperkinetic movement disorders Alfons Schnitzler, MD, PhD Dept. of Neurology, Movement Disorder and Neuromodulation, Heinrich-Heine-University Düsseldorf, Germany Hyperkinetic
COGNITIVE SCIENCE 107A. Motor Systems: Basal Ganglia. Jaime A. Pineda, Ph.D.
 COGNITIVE SCIENCE 107A Motor Systems: Basal Ganglia Jaime A. Pineda, Ph.D. Two major descending s Pyramidal vs. extrapyramidal Motor cortex Pyramidal system Pathway for voluntary movement Most fibers originate
COGNITIVE SCIENCE 107A Motor Systems: Basal Ganglia Jaime A. Pineda, Ph.D. Two major descending s Pyramidal vs. extrapyramidal Motor cortex Pyramidal system Pathway for voluntary movement Most fibers originate
Basal ganglia motor circuit
 Parkinson s Disease Basal ganglia motor circuit 1 Direct pathway (gas pedal) 2 Indirect pathway (brake) To release or augment the tonic inhibition of GPi on thalamus Direct pathway There is a tonic inhibition
Parkinson s Disease Basal ganglia motor circuit 1 Direct pathway (gas pedal) 2 Indirect pathway (brake) To release or augment the tonic inhibition of GPi on thalamus Direct pathway There is a tonic inhibition
Long-term follow up of subthalamic nucleus stimulation in Parkinson s disease
 oped parallel to a progressive cerebral disease. These findings are supported by other recent reports showing that EDS correlates with more advanced PD. 9 The close correlation between persistent and new
oped parallel to a progressive cerebral disease. These findings are supported by other recent reports showing that EDS correlates with more advanced PD. 9 The close correlation between persistent and new
Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease
 CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
Professor Tim Anderson
 Professor Tim Anderson Neurologist University of Otago Christchurch 11:00-11:55 WS #91: Shakes Jerks and Spasms - Recognition and Differential Diagnosis 12:05-13:00 WS #102: Shakes Jerks and Spasms - Recognition
Professor Tim Anderson Neurologist University of Otago Christchurch 11:00-11:55 WS #91: Shakes Jerks and Spasms - Recognition and Differential Diagnosis 12:05-13:00 WS #102: Shakes Jerks and Spasms - Recognition
Professor Tim Anderson
 Professor Tim Anderson Neurologist University of Otago Christchurch 11:00-11:55 WS #91: Shakes Jerks and Spasms - Recognition and Differential Diagnosis 12:05-13:00 WS #102: Shakes Jerks and Spasms - Recognition
Professor Tim Anderson Neurologist University of Otago Christchurch 11:00-11:55 WS #91: Shakes Jerks and Spasms - Recognition and Differential Diagnosis 12:05-13:00 WS #102: Shakes Jerks and Spasms - Recognition
DEEP BRAIN STIMULATION
 DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
As clinical experience with deep-brain stimulation (DBS) of
 ORIGINAL RESEARCH K.V. Slavin K.R. Thulborn C. Wess H. Nersesyan Direct Visualization of the Human Subthalamic Nucleus with 3T MR Imaging BACKGROUND AND PURPOSE: Electrical stimulation of the subthalamic
ORIGINAL RESEARCH K.V. Slavin K.R. Thulborn C. Wess H. Nersesyan Direct Visualization of the Human Subthalamic Nucleus with 3T MR Imaging BACKGROUND AND PURPOSE: Electrical stimulation of the subthalamic
E ssential tremor is a commonly diagnosed movement
 684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence
684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence
Bilateral Deep-Brain Stimulation of the Globus Pallidus in Primary Generalized Dystonia
 original article Bilateral Deep-Brain Stimulation of the Globus Pallidus in Primary Generalized Dystonia Marie Vidailhet, M.D., Ph.D., Laurent Vercueil, M.D., Jean-Luc Houeto, M.D., Ph.D., Pierre Krystkowiak,
original article Bilateral Deep-Brain Stimulation of the Globus Pallidus in Primary Generalized Dystonia Marie Vidailhet, M.D., Ph.D., Laurent Vercueil, M.D., Jean-Luc Houeto, M.D., Ph.D., Pierre Krystkowiak,
Deep brain stimulation: What can patients expect from it?
 MEDICAL GRAND ROUNDS ANDRE MACHADO, MD, PhD* Director, Center for Neurological Restoration, Neurological Institute, Cleveland Clinic HUBERT H. FERNANDEZ, MD Section Head, Movement Disorders, Center for
MEDICAL GRAND ROUNDS ANDRE MACHADO, MD, PhD* Director, Center for Neurological Restoration, Neurological Institute, Cleveland Clinic HUBERT H. FERNANDEZ, MD Section Head, Movement Disorders, Center for
Which patients with dystonia benefit from deep brain stimulation? A metaregression of individual patient outcomes
 1 Lysholm Department of Neuroradiology, National Hospital for Neurology & Neurosurgery, London, UK 2 Unit of Functional Neurosurgery, Sobell Department of Motor Neuroscience, UCL Institute of Neurology,
1 Lysholm Department of Neuroradiology, National Hospital for Neurology & Neurosurgery, London, UK 2 Unit of Functional Neurosurgery, Sobell Department of Motor Neuroscience, UCL Institute of Neurology,
Where a licence is displayed above, please note the terms and conditions of the licence govern your use of this document.
 Deep brain stimulation for tremor resulting from acquired brain injury Sitsapesan, H A; Holland, P; Oliphant, Z; De Pennington, N; Brittain, John-Stuart; Jenkinson, Ned ; Joint, C; Aziz, T Z; Green, A
Deep brain stimulation for tremor resulting from acquired brain injury Sitsapesan, H A; Holland, P; Oliphant, Z; De Pennington, N; Brittain, John-Stuart; Jenkinson, Ned ; Joint, C; Aziz, T Z; Green, A
Linköping University Post Print. Patient-specific models and simulations of deep brain stimulation for postoperative follow-up
 inköping University Post Print Patient-specific models and simulations of deep brain stimulation for postoperative follow-up Mattias Åström, Elina Tripoliti, Irene Martinez-Torres, udvic U. Zrinzo, Patricia
inköping University Post Print Patient-specific models and simulations of deep brain stimulation for postoperative follow-up Mattias Åström, Elina Tripoliti, Irene Martinez-Torres, udvic U. Zrinzo, Patricia
Deep Brain Stimulation (DBS)
 Deep Brain Stimulation (DBS) [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr go to Comunicados a Proveedores, and click Cartas Circulares.] Medical Policy:
Deep Brain Stimulation (DBS) [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr go to Comunicados a Proveedores, and click Cartas Circulares.] Medical Policy:
Deep brain stimulation for dystonia
 1 AP-HP, Department of Neurology, Groupe Hospitalier Pitié-Salpêtrière, Paris, France 2 Centre de Recherche de l Institut du Cerveau et de la Moelle épinière (CRICM), CNRS UMR 7225, UPMC Université Paris
1 AP-HP, Department of Neurology, Groupe Hospitalier Pitié-Salpêtrière, Paris, France 2 Centre de Recherche de l Institut du Cerveau et de la Moelle épinière (CRICM), CNRS UMR 7225, UPMC Université Paris
POSTOPERATIVE PATIENT MANAGEMENT
 POSTOPERATIVE PATIENT MANAGEMENT INTRODUCTION Deep brain stimulation of the internal globus pallidus (GPi) or the subthalamic nucleus (STN) effectively reduces parkinsonian motor symptoms and alleviates
POSTOPERATIVE PATIENT MANAGEMENT INTRODUCTION Deep brain stimulation of the internal globus pallidus (GPi) or the subthalamic nucleus (STN) effectively reduces parkinsonian motor symptoms and alleviates
I n 1991 Benabid et al introduced deep brain stimulation
 PAPER Multicentre European study of thalamic stimulation in essential tremor: a six year follow up O Sydow, S Thobois, F Alesch, J D Speelman, study collaborators... See Editorial Commentary, pp1361 2
PAPER Multicentre European study of thalamic stimulation in essential tremor: a six year follow up O Sydow, S Thobois, F Alesch, J D Speelman, study collaborators... See Editorial Commentary, pp1361 2
Pallidal Deep Brain Stimulation
 Pallidal Deep Brain Stimulation Treatment for Dystonia Dystonia Dystonia is a neurological disorder characterized by involuntary muscle contractions resulting in abnormal postures. These movements may
Pallidal Deep Brain Stimulation Treatment for Dystonia Dystonia Dystonia is a neurological disorder characterized by involuntary muscle contractions resulting in abnormal postures. These movements may
Clinical and programming pattern of patients with impending deep brain stimulation power failure: a retrospective chart review
 Mehanna et al. Journal of Clinical Movement Disorders 2014, 1:6 RESEARCH Open Access Clinical and programming pattern of patients with impending deep brain stimulation power failure: a retrospective chart
Mehanna et al. Journal of Clinical Movement Disorders 2014, 1:6 RESEARCH Open Access Clinical and programming pattern of patients with impending deep brain stimulation power failure: a retrospective chart
Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic surgery
 ISPUB.COM The Internet Journal of Neuromonitoring Volume 7 Number 1 Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic
ISPUB.COM The Internet Journal of Neuromonitoring Volume 7 Number 1 Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic
Deep Brain Stimulation
 Deep Brain Stimulation Policy Number: 7.01.63 Last Review: 8/2017 Origination: 8/2001 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for deep brain
Deep Brain Stimulation Policy Number: 7.01.63 Last Review: 8/2017 Origination: 8/2001 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for deep brain
Scott J Sherman MD, PhD The University of Arizona PARKINSON DISEASE
 Scott J Sherman MD, PhD The University of Arizona PARKINSON DISEASE LEARNING OBJECTIVES The Course Participant will: 1. Be familiar with the pathogenesis of Parkinson s Disease (PD) 2. Understand clinical
Scott J Sherman MD, PhD The University of Arizona PARKINSON DISEASE LEARNING OBJECTIVES The Course Participant will: 1. Be familiar with the pathogenesis of Parkinson s Disease (PD) 2. Understand clinical
Deep brain s,mula,on refers to implan,ng electrodes into specific areas of the brain and hooking the electrodes up to pacemaker- like devices in
 1 Deep brain s,mula,on refers to implan,ng electrodes into specific areas of the brain and hooking the electrodes up to pacemaker- like devices in order to send signals into the brain to jam the abnormal
1 Deep brain s,mula,on refers to implan,ng electrodes into specific areas of the brain and hooking the electrodes up to pacemaker- like devices in order to send signals into the brain to jam the abnormal
Deep Brain Stimulation. Is It Right for You?
 Deep Brain Stimulation Is It Right for You? Northwestern Medicine Deep Brain Stimulation What is DBS? Northwestern Medicine Central DuPage Hospital is a regional destination for the treatment of movement
Deep Brain Stimulation Is It Right for You? Northwestern Medicine Deep Brain Stimulation What is DBS? Northwestern Medicine Central DuPage Hospital is a regional destination for the treatment of movement
Deep brain stimulation for the treatment of Parkinson s disease: subthalamic nucleus versus globus pallidus internus
 464 Department of Neurology, University of Heidelberg, INF 4, 6912 Heidelberg, Germany M Krause W Fogel W Hacke Department of Neurosurgery A Heck M Bonsanto V Tronnier Max Planck Institute of Psychiatry,
464 Department of Neurology, University of Heidelberg, INF 4, 6912 Heidelberg, Germany M Krause W Fogel W Hacke Department of Neurosurgery A Heck M Bonsanto V Tronnier Max Planck Institute of Psychiatry,
Surgical Treatment: Patient Edition
 Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Effect of Subthalamic Deep Brain Stimulation on Levodopa-Induced Dyskinesia in Parkinson s Disease
 Original Article Yonsei Med J 2015 Sep;56(5):1316-1321 pissn: 0513-5796 eissn: 1976-2437 Effect of Subthalamic Deep Brain Stimulation on Levodopa-Induced Dyskinesia in Parkinson s Disease Ji Hee Kim, Won
Original Article Yonsei Med J 2015 Sep;56(5):1316-1321 pissn: 0513-5796 eissn: 1976-2437 Effect of Subthalamic Deep Brain Stimulation on Levodopa-Induced Dyskinesia in Parkinson s Disease Ji Hee Kim, Won
Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Value Units
 Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Units The American Academy of Neurology (AAN) presents the following case studies to help you understand
Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Units The American Academy of Neurology (AAN) presents the following case studies to help you understand
DEEP BRAIN STIMULATION (DBS) is a standard treatment
 1320 ORIGINAL ARTICLE Fast-Track Programming and Rehabilitation Model: A Novel Approach to Postoperative Deep Brain Stimulation Patient Care David B. Cohen, MD, Michael Y. Oh, MD, Susan M. Baser, MD, Cindy
1320 ORIGINAL ARTICLE Fast-Track Programming and Rehabilitation Model: A Novel Approach to Postoperative Deep Brain Stimulation Patient Care David B. Cohen, MD, Michael Y. Oh, MD, Susan M. Baser, MD, Cindy
Surgical Management of Parkinson s Disease
 Surgical Management of Parkinson s Disease Shyamal H. Mehta MD, PhD Assistant Professor of Neurology, Movement Disorders Division Mayo Clinic College of Medicine Mayo Clinic, Arizona 2016 MFMER slide-1
Surgical Management of Parkinson s Disease Shyamal H. Mehta MD, PhD Assistant Professor of Neurology, Movement Disorders Division Mayo Clinic College of Medicine Mayo Clinic, Arizona 2016 MFMER slide-1
Indications. DBS for Tremor. What is the PSA? 6/08/2014. Tremor. 1. Tremor. 2. Gait freezing/postural instability. 3. Motor fluctuations
 Indications Deep brain stimulation for Parkinson s disease A Tailored Approach 1. Tremor 2. Gait freezing/postural instability Wesley Thevathasan FRACP DPhil.Oxf 3. Motor fluctuations Consultant Neurologist,
Indications Deep brain stimulation for Parkinson s disease A Tailored Approach 1. Tremor 2. Gait freezing/postural instability Wesley Thevathasan FRACP DPhil.Oxf 3. Motor fluctuations Consultant Neurologist,
Deep brain stimulation in the treatment of dyskinesia and dystonia
 Neurosurg Focus 17 (1):E2, 2004, Click here to return to Table of Contents Deep brain stimulation in the treatment of dyskinesia and dystonia HIROKI TODA, M.D., PH.D., CLEMENT HAMANI, M.D., PH.D., AND
Neurosurg Focus 17 (1):E2, 2004, Click here to return to Table of Contents Deep brain stimulation in the treatment of dyskinesia and dystonia HIROKI TODA, M.D., PH.D., CLEMENT HAMANI, M.D., PH.D., AND
Palladotomy and Pallidal Deep Brain Stimulation
 Palladotomy and Pallidal Deep Brain Stimulation Parkinson s disease Parkinson s Disease is a common neurodegenerative disorder that affects about 1:100 individuals over the age of 60. In a small percentage
Palladotomy and Pallidal Deep Brain Stimulation Parkinson s disease Parkinson s Disease is a common neurodegenerative disorder that affects about 1:100 individuals over the age of 60. In a small percentage
Outcomes after stereotactically guided pallidotomy for advanced Parkinson s disease
 J Neurosurg 90:197 202, 1999 Outcomes after stereotactically guided pallidotomy for advanced Parkinson s disease DOUGLAS KONDZIOLKA, M.D., F.R.C.S.(C), EUGENE BONAROTI, M.D., SUSAN BASER, M.D., FRAN BRANDT,
J Neurosurg 90:197 202, 1999 Outcomes after stereotactically guided pallidotomy for advanced Parkinson s disease DOUGLAS KONDZIOLKA, M.D., F.R.C.S.(C), EUGENE BONAROTI, M.D., SUSAN BASER, M.D., FRAN BRANDT,
Diagnosis and treatment of dystonia
 Diagnosis and treatment of dystonia Professor Tom Warner, Reta Lila Weston Institute of Neurological Studies UCL Institute of Neurology National Hospital for Neurology and Neurosurgery Queen Square What
Diagnosis and treatment of dystonia Professor Tom Warner, Reta Lila Weston Institute of Neurological Studies UCL Institute of Neurology National Hospital for Neurology and Neurosurgery Queen Square What
Deep brain stimulation (DBS) has been
 TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Do Stable Patients With a Premorbid Depression History Have a Worse Outcome After Deep Brain Stimulation for Parkinson Disease? Michael
TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Do Stable Patients With a Premorbid Depression History Have a Worse Outcome After Deep Brain Stimulation for Parkinson Disease? Michael
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL Policy Number: MP.108.MH Last Review Date: 05/10/2018 Effective Date: 07/01/2018
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.0108.MH Deep Brain and Dorsal Column (Spinal Cord) This policy applies to the following lines of business: MedStar Employee (Select) MedStar CareFirst
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.0108.MH Deep Brain and Dorsal Column (Spinal Cord) This policy applies to the following lines of business: MedStar Employee (Select) MedStar CareFirst
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA.
 Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
Long-Term Results of a Multicenter Study on Subthalamic and Pallidal Stimulation in Parkinson s Disease
 Movement Disorders Vol. 25, No. 5, 2010, pp. 578 586 Ó 2010 Movement Disorder Society Long-Term Results of a Multicenter Study on Subthalamic and Pallidal Stimulation in Parkinson s Disease Elena Moro,
Movement Disorders Vol. 25, No. 5, 2010, pp. 578 586 Ó 2010 Movement Disorder Society Long-Term Results of a Multicenter Study on Subthalamic and Pallidal Stimulation in Parkinson s Disease Elena Moro,
Intraoperative microelectrode recording (MER) for targeting during deep brain stimulation (DBS) procedures 巴黎第六大学医学院生理学
 Intraoperative microelectrode recording (MER) for targeting during deep brain stimulation (DBS) procedures 巴黎第六大学医学院生理学 Paris 6 University (Pierre-et-Marie-Curie) Medical school physiology department 皮度
Intraoperative microelectrode recording (MER) for targeting during deep brain stimulation (DBS) procedures 巴黎第六大学医学院生理学 Paris 6 University (Pierre-et-Marie-Curie) Medical school physiology department 皮度
Deep brain stimulation for dystonia
 Hu and Stead Translational Neurodegeneration 2014, 3:2 Translational Neurodegeneration REVIEW Deep brain stimulation for dystonia Wei Hu * and Matt Stead * Open Access Abstract Deep brain stimulation (DBS)
Hu and Stead Translational Neurodegeneration 2014, 3:2 Translational Neurodegeneration REVIEW Deep brain stimulation for dystonia Wei Hu * and Matt Stead * Open Access Abstract Deep brain stimulation (DBS)
Patient selection for surgery: Parkinson s disease
 Patient selection for surgery: Parkinson s disease Dr. María C. Rodríguez-Oroz Neurology and Neuroscience. University Hospital Donostia, Research Institute BioDonostia, Ikerbasque Senior Researcher San
Patient selection for surgery: Parkinson s disease Dr. María C. Rodríguez-Oroz Neurology and Neuroscience. University Hospital Donostia, Research Institute BioDonostia, Ikerbasque Senior Researcher San
Overweight after deep brain stimulation of the subthalamic nucleus in Parkinson disease: long term follow-up
 1 CHU Clermont-Ferrand, Department of Neurology, Gabriel Montpied Hospital, Clermont-Ferrand, France; 2 Univ Clermont 1, UFR Medecine, Clermont-Ferrand, France; 3 INRA, Centre Clermont-Ferrand Theix, Unite
1 CHU Clermont-Ferrand, Department of Neurology, Gabriel Montpied Hospital, Clermont-Ferrand, France; 2 Univ Clermont 1, UFR Medecine, Clermont-Ferrand, France; 3 INRA, Centre Clermont-Ferrand Theix, Unite
Supplementary Information for Decreased activity of single subthalamic nucleus neurons in Parkinson patients responding to placebo
 Supplementary Information for Decreased activity of single subthalamic nucleus neurons in Parkinson patients responding to placebo Fabrizio Benedetti, 1,2 Luana Colloca, 1,2 Elena Torre, 1 Michele Lanotte,
Supplementary Information for Decreased activity of single subthalamic nucleus neurons in Parkinson patients responding to placebo Fabrizio Benedetti, 1,2 Luana Colloca, 1,2 Elena Torre, 1 Michele Lanotte,
Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II
 Parkinsonism and Related Disorders 13 (2007) 399 405 www.elsevier.com/locate/parkreldis Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II A. Haffenden, U.
Parkinsonism and Related Disorders 13 (2007) 399 405 www.elsevier.com/locate/parkreldis Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II A. Haffenden, U.
Diagnosis and treatment of dystonia
 Diagnosis and treatment of dystonia Professor Tom Warner, Reta Lila Weston Institute of Neurological Studies UCL Institute of Neurology National Hospital for Neurology and Neurosurgery Queen Square What
Diagnosis and treatment of dystonia Professor Tom Warner, Reta Lila Weston Institute of Neurological Studies UCL Institute of Neurology National Hospital for Neurology and Neurosurgery Queen Square What
