Effect of Pressure Ulcers on the Survival of Long-Term Care Residents
|
|
|
- Ferdinand Lloyd
- 6 years ago
- Views:
Transcription
1 Journal of Gerontology: MEDICAL SCIENCES Vol. 52A. No. 2. MI06-M110 In the Public Domain Effect of Pressure Ulcers on the Survival of Long-Term Care Residents Dan R. Berlowitz, 12 Gary H. Brandeis, 13 Jennifer Anderson, 1 Wei Du, 12 and Harriet Brand 1 'Edith Nourse Rogers Memorial Veterans Hospital, Bedford, Massachusetts. 2 Section of General Internal Medicine and 'Geriatrics Section, Boston University Medical Center. Background. Past studies have emphasized that patients with pressure ulcers are at high risk of dying. However, it remains unclear whether this increased risk is related to the ulcer or to coexisting conditions. In this study we examined the independent effect of pressure ulcers on the survival of long-term care residents. Methods. We evaluated all 19,981 long-term care residents institutionalized in Department of Veterans Affairs (VA) long-term care facilities as of April 1, Baseline resident characteristics and survival status were obtained by merging data from five existing VA data bases. Survival experience over a 6-month period was described using a proportional hazards model. Results., Pressure ulcers were present in 1,539 (7.7%) long-term care residents. Residents with pressure ulcers had a relative risk of 2.37 (95% CI = 2.13, 2.64) for dying as compared to those without ulcers. After adjusting for 16 other measures of clinical and functional status, the relative risk associated with pressure ulcers decreased to 1.45 (95% Cl = 1.30, 1.65). No increased risk of death was noted for residents with deeper ulcers. Conclusions. Pressure ulcers are a significant marker for long-term care residents at risk of dying. After adjusting for clinical and functional status, however, the independent risk associated with pressure ulcers declines considerably. The fact that larger ulcers are not associated with greater risk suggests that other unmeasured clinical conditions may also be contributing to the increased mortality associated with pressure ulcers. PRESSURE ulcers are a serious medical condition that significantly affects the morbidity and mortality of longterm care residents (1). Past studies have emphasized that pressure ulcers are common in the terminal stages of disease (2) and that as many as 70% of pressure ulcer patients will die within a short time (3,4). Among residents newly admitted to a nursing home, 92% of those dying within 12 weeks had developed a pressure ulcer during the first 3 weeks of institutionalization (5). In recent work, using data from both a chronic care hospital (6) and a large nursing home chain (7), we have confirmed that pressure ulcer patients have a two- to threefold increased risk of dying compared to patients without an ulcer. Faced with this poor prognosis, clinicians may conclude that aggressive care of pressure ulcers is unlikely to result in prolonged patient benefit. For example, Bennett et al. (8) observed such high mortality among pressure ulcer patients treated with an airfluidized bed that they recommended limiting this expensive treatment only to those patients surviving beyond 30 days of institutionalization. However, since the use of such specialized beds is effective in promoting the healing of ulcers (9,10), clinicians may be unsure how to proceed and patients may be deprived of a beneficial intervention. Pressure ulcers are a common source of infection in the nursing home (11,12), and bacteremia resulting from a pressure ulcer is associated with a 50% mortality (13,14). This suggests a likely mechanism by which pressure ulcers may result in patient death. However, patients with pressure ulcers often have serious coexisting illnesses and are functionally dependent (15-17). We have previously suggested that these coexisting conditions, and not the pressure ulcer, may be causing this increased mortality (6). These results were limited, though, by small sample size, incomplete follow-up of discharged patients, and a lack of information on other predictors of survival. Thus, the independent effect of pressure ulcers on the survival of long-term care residents remained poorly defined. The purpose of this study is to examine the effect of pressure ulcers on survival in a national sample of long-term care residents institutionalized at Department of Veterans Affairs (VA) hospitals and nursing homes. METHODS Data Base Descriptions We used information from five separate VA data bases to identify long-term care residents, determine their baseline status, and describe their survival over a 6-month time period. Our primary source of information was the Patient Assessment File (PAF) (18), an administrative data base developed for case-mix based reimbursements in long-term care, and based on Resource Utilization Groups (RUGs II) (19). PAF data, which describe individual long-term care residents, are collected by nursing staff at each VA facility semiannually on April 1 and October 1, as well as at the time of admission or transfer to a nursing home or intermediate medicine unit. The PAF documents the stage of the deepest M106
2 EFFECT OF PRESSURE ULCERS ON SURVIVAL M107 pressure ulcer, if present, on the evaluation date. Staging of pressure ulcers is on a 1 to 5 scale: a stage 1 ulcer consists of erythematous skin; a stage 2 ulcer consists of a superficial layer of broken or blistered skin; a stage 3 ulcer involves the subcutaneous tissues; and a stage 4 ulcer extends to muscle or bone. Stage 5 ulcers are stage 4 ulcers without a treatment plan documented in the medical record; in this study we combined stages 4 and 5. Additional information included in the PAF are patient demographics including age and gender; specific diagnoses such as multiple sclerosis, urinary tract infection, hemiplegia, or quadriplegia; medical treatments being received such as oxygen therapy and dialysis; and activities of daily living, consisting of eating, mobility, transfer, and toileting ability, each rated on a 1 to 5 scale (20). The presence of a terminal illness, defined as a condition likely to result in death within 3 months, is also recorded in the PAF. The Patient Treatment File (PTF) has a record for each discharge from VA inpatient care during a fiscal year (21). Included are the date of discharge, whether the patient was discharged alive, and specific ICD-9-CM codes relating to the hospitalization. Separate files exist for episodes of care at VA medical centers; episodes of non-va care provided at military or private hospitals under contract; and extended care episodes in domiciliaries, VA nursing homes, or community contract nursing homes. No record is present, though, for long-staying patients not discharged during the fiscal year. The Outpatient Clinic File (OPC) has a record specific to each individual visit to a VA outpatient clinic (21). Non-VA outpatient care is not captured. The Annual Census File contains information on all patients in VA hospitals and extended care facilities on September 30 of each year (21). The Beneficiary Identification and Record Locator Subsystem (BIRLS) records all veterans who are receiving benefits (21). Information about the date of death of veterans is included, as death benefits are available to surviving family members. We merged records from these five data bases through a common social security number. As the BIRLS file uses veterans' real social security numbers, while the other data bases use scrambled social security numbers, existing conversion files were used in relating BIRLS to these other data bases. Study Cohort We used the PAF to identify all veterans residing in VA nursing homes or intermediate medicine units on April 1, An intermediate medical unit serves residents with a variety of needs, including short courses of rehabilitation, and long-term interventions more intensive than provided in the nursing home setting. Our study cohort consists of the resulting 19,981 long-term care residents. Characteristics of the population are described in Table 1. Selection of Study Variables The outcome event was resident survival over the 6-month period between April 1 and September 30, For patients dying during this time period, the date of death was recorded from the PTF or BIRLS. In the rare situation that Table 1. Characteristics of the Study Population All With Without Patients Ulcer Ulcer (N = 19,981) (/i = 1,539) (n = 18,442) Age (mean ± SD) 71.2 ± ± ±11.4 Male gender (%) Dependent in mobility* (% requiring assistance) Dependent in transferring* (% requiring assistance) Incontinent of urine* orfeces(%) Terminal illness (%)* *p<.001. the dates from these two files did not match, the date from the PTF was used in our analyses. The relationship of pressure ulcers to 6-month survival was examined with pressure ulcer status on April 1, 1993 coded both dichotomously (present/not present) and by stage. As stage 1 pressure ulcers (erythematous lesions of intact skin) are difficult to recognize clinically (22), patients with only stage 1 ulcers were considered ulcer-free. We selected 26 additional potential predictors of survival from among resident characteristics available in the PAF entry from April 1, Candidate variables included demographic items such as gender and residence in either nursing home or intermediate medicine units; variables shown in past studies to be associated with survival of nursing home residents, including age and measures of functional dependence (23,24); and variables with a clinically plausible association with survival, such as receiving dialysis or radiation therapy. These variables are listed in Table 2. Information on age and functional dependence was available on the entire study sample. All other variables were considered absent unless specifically identified as present in the data base. Analyses We sequentially searched these data bases for episodes of health care utilization after September 30, 1993, indicating that the resident was alive as of that date; or an indication that the resident had died between April 1 and September 30, Long-term care residents were designated as having survived the 6-month period if any of the following conditions were met: (a) a PAF entry existed between October 1, 1993 and April 1, 1994; (b) an Annual Census record existed from September 30, 1993; (c) an Outpatient Clinic File entry during the one-year period following September 30, 1993; (d) a PTF entry from either the main VA file, the non-va hospital file, or the extended care file, indicating a hospital discharge after September 30, 1993; or (e) a BIRLS entry indicating resident death after September 30, Residents were considered to have died if there was no indication that they were alive after September 30, 1993, and either the PTF or BIRLS indicated that the patient had died during the 6 months preceding that date. Patients who could not be labeled as either dead or alive were excluded from the analyses.
3 M108 BERLOWITZ ET AL. Variable Table 2. Factors From the Proportional Hazards Model That Are Independently Associated (p <.05) With Dying During a 6-month Follow-up Period Pressure ulcer present Terminal illness Oxygen therapy* Radiation therapy* Dialysis* Blood transfusion* Male gender Residence on intermediate medical unit Dehydration Age (for each 10 years of increasing age) Dependence in transferring! Dependence in mobilityt Dependence in eatingt Hemiplegia Quadriplegia Tracheostomy Multiple sclerosis Relative Risk (95% Confidence Interval) 1.45(1.30, 1.63) 4.66(4.21,5.17) 2.76 (2.48, 3.07) 2.07(1.69,2.55).87(1.35,2.58).84(1.31,2.60).64(1.26,2.15).34(1.23,.45).32(1.14,.53).23(1.18,.28).13(1.06, 19).13(1.08,.19).07(1.03,.11) 0.71(0.63,0.80) 0.62 (0.48, 0.79) 0.58 (0.46, 0.74) 0.43 (0.29, 0.66) Note: Other variables significant on the log-rank test and entered into the model include chemotherapy, coma, gastrointestinal bleeding, urinary tract infection, incontinence, ventilator dependence, stasis ulcer, non-pressure ulcer wound care, and parenteral feeding. Treatment provided during the 4 weeks preceding the assessment and (for new admissions) anticipated to be provided in the future. trelative risk for each step on a 5-point scale. Statistical analyses were performed using the Statistical Analysis System (SAS Institute, Cary, NC). We performed bivariate testing, including chi-square tests for categorical variables, Mantel-Haenszel chi-square tests for ordinal variables, and Mests for continuous variables, to compare baseline characteristics of patients with and without pressure ulcers on April 1, The association of pressure ulcers, and the other candidate predictor variables, with survival during the 6-month period following April 1, 1993 was assessed using the log-rank test; unadjusted hazard ratios for each variable were obtained by Cox proportional hazards regression. The log-log survival curves for subjects with and without pressure ulcers were parallel, supporting the assumption of proportional hazards for these data. All candidate variables were then entered into a stepwise proportional hazards model to identify factors independently associated (p ^.05) with resident survival. Separate models were examined with pressure ulcers classified as present/not present and by stage. Additionally, as the presence of an ulcer may affect whether patients are designated as having a terminal illness, modeling was repeated with this explanatory variable excluded, as well as with the inclusion of an interaction term for the presence of an ulcer in a terminally ill patient. The estimated survival curves for the no-ulcer and ulcer stage groups were plotted both with and without adjustment for the significant additional factors. The adjusted curves represent survival within groups at the mean of each adjustment factor. RESULTS The study sample consisted of 19,981 residents of 141 VA long-term care facilities. Pressure ulcers were present in 1,539 (7.7%) residents; 45.6% of the ulcers were stage 2, 31.5% stage 3, and 22.9% stage 4. Pressure ulcer patients were of similar age and gender than patients without an ulcer, but they were more likely to be functionally dependent or have a terminal illness. We could not locate information on survival status in any of the data bases for 311 (1.6%) long-term care residents. For an additional 51 (0.2%) residents, we were unable to unscramble their social security numbers and use the BIRLS file. Consequently, 362 residents were excluded from the survival analyses. Excluded veterans were younger (68.0 ± 11.5 vs 71.2 ± 11.4 years), more likely to reside on an intermediate medicine unit, and less dependent in each of their activities of daily living (p <.001 for all analyses). Of the remaining 19,619 residents, 2,579 (13.1%) died during the 6-month follow-up period. Among residents with a pressure ulcer, 26.0% died, compared with 12.1% of those without an ulcer (p <.001). The relative risk (RR) of dying for pressure ulcer patients was 2.37 (95% CI = 2.13,2.64). Each of the ordinal dependence in activities of daily living (ADL) variables (transferring, mobility, and eating) showed a strongly ordered association in bivariate trend testing with dying. We chose to include them parsimoniously in the modeling as if they were continuous. Stepwise proportional hazards regression using the 26 potential explanatory variables selected from the PAF, including the ADL measures, resulted in the retention of 17 variables that were significant atp <.05 (model x 2 = 2380) (Table 2). After adjusting for these other resident characteristics, pressure ulcers, while still significant, were a weaker predictor of dying (RR = 1.45, 95% CI = 1.30, 1.65). Among the other variables significantly associated with dying and included in the full model were the presence of a terminal illness (RR = 4.66), as well as receiving oxygen therapy (RR = 2.76), radiation therapy (RR = 2.07), dialysis (RR = 1.87), and blood transfusions (RR = 1.84) during the preceding 4 weeks. The presence of hemiplegia, quadriplegia, multiple sclerosis, and a tracheostomy were all protective in this model. Additional characteristics individually associated with dying on the log-rank test, but not significant independent predictors in the model, include receiving chemotherapy, coma, recent gastrointestinal bleeding, incontinence, and recent urinary tract infections. Excluding terminal illness from the model did not affect overall conclusions. Pressure ulcers remained a weaker, but still significant predictor of dying in this new model (RR = 1.62, 95% CI = 1.45, 1.81). In the model that included both terminal illness and the interaction of this variable with the presence of an ulcer, no additional risk was noted for residents with both characteristics. Residents with superficial pressure ulcers were not less likely to die than residents with deeper ulcers. Using the unadjusted rates (Figure 1), the risk of dying was similar for residents with either stage 2 or stage 4 ulcers; residents with stage 3 ulcers had a lower risk (p =.05). The addition of indicator variables for each stage of pressure ulcers to the full risk-adjustment model increased the model chi-square marginally (x 2 = 2383). The relative risk of dying was 1.60 for residents with stage 2 ulcers, as compared to 1.34 and 1.33 for stages 3 and 4, respectively (p = n.s.) (Figure 2).
4 EFFECT OF PRESSURE ULCERS ON SURVIVAL M ] 1.0CH 0.95-j j ; Stage j Weeks Figure I. Proportional hazards estimates of the proportion of patients surviving, by weeks from baseline, for the no pressure ulcer and the ulcer stages 2,3, and 4 subject groups, without adjustment for other factors. Weeks Figure 2. Proportional hazards estimates of the proportion of patients surviving, by weeks from baseline, for the no pressure ulcer and the ulcer stages 2,3, and 4 subject groups, after adjustment for other factors. DISCUSSION Patients with pressure ulcers have a markedly increased risk of dying. This poor prognosis has resulted in recommendations to temporarily limit the use of air-fluidized beds, an effective intervention for promoting ulcer healing (8). Other effective but expensive interventions may be similarly withheld. However, it remains uncertain whether the increased mortality is a direct result of the pressure ulcer or is explained by coexisting conditions. We have therefore made use of the extensive information available from VA data bases to examine this association between pressure ulcers and survival of long-term care residents. Pressure ulcers are a significant marker of death during a 6-month follow-up period. The unadjusted relative risk of dying for pressure ulcer patients was 2.37 in the present study, results similar to those we reported in past studies. For example, among new admissions to a chronic care hospital, we previously noted a relative risk of 1.9 (6). Among a national sample of predominantly female nursing home residents, 38.8% of residents with a pressure ulcer, and 15.4% of those without an ulcer, died over one year (7), as compared to 6-month rates of 26.0% and 12.1%, respectively, in the present study. By using VA administrative data bases to obtain detailed information on residents' clinical and functional status that was lacking in these previous studies, we have been able to examine the independent effect of pressure ulcers on survival. Pressure ulcers are a weaker predictor of dying after adjusting for the presence of these other conditions. The relative risk associated with the presence of an ulcer decreased from the unadjusted value of 2.37, to 1.45 in the full model. Other variables included in the model, such as functional status and age, have been shown to be important predictors in previous studies of survival in nursing home residents (23,24); or, as for dialysis, radiation therapy, or oxygen, are clinically plausible predictors of dying. We are unsure why the presence of multiple sclerosis, hemiplegia, quadriplegia, and tracheostomy were associated with increased survival in this model. Stage 4 ulcers, which are deeper and likely more prone to serious infections that could result in death, were not associated with an increased risk of dying when compared to stage 2 and 3 ulcers in the proportional hazards model. This suggests that the presence of a pressure ulcer may be a marker for other unmeasured clinical factors that are not included in our model. Inclusion of these factors in the model could result in a further lowering of the relative risk associated with the presence of an ulcer. Strengths of this study should be emphasized. First, the large sample size obtained by using all VA long-term care residents allowed us to calculate stable estimates of the relative risk associated with pressure ulcers with narrow 95% confidence intervals. Second, detailed information on the clinical status of long-term care residents, including functional status, specific diagnoses, and therapies, was available from the PAF. Third, information on survival was available on nearly all veterans. Even though long-term care residents may be lost to follow-up through discharges home, transfers to acute care settings, or placement on contract in private nursing homes, the application of different data bases allowed follow-up information on 98.2% of our sample. Residents for whom no follow-up information was available tended to be younger and less functionally dependent, suggesting that they may have been discharged from long-term care and not required subsequent VA outpatient care. Limitations should also be noted. Administrative data, as used in this study, may contain errors. Studies evaluating the different data bases used in this study have been limited. For the PAF, a study at three VA nursing homes indicated that pairs of registered nurses have a Pearson reliability coefficient of greater than 0.90 when evaluating residents on their wards (25). Errors in the date of discharge and whether patients died during the admission are infrequent in the PTF (21). This study has important clinical implications. Decisions regarding the use of diagnostic and therapeutic interventions in long-term care patients should be guided by their overall medical condition, as well as patient preferences, and should not be based on simple criteria such as whether the patient
5 MHO BERLOWITZ ET AL. has a pressure ulcer and on the stage of the ulcer. This emphasizes the need for comprehensive assessments of these complex patients. We have demonstrated that while patients with pressure ulcers are more likely to die, this increased risk is largely related to their frailty and high disease burden, and not a direct result of the ulcer. These results do not imply that pressure ulcers may be ignored. Rather, our results demonstrate that with usual care, pressure ulcers have at most a modest independent effect on resident survival. ACKNOWLEDGMENTS This project was supported by the Department of Veterans Affairs HSR&D Service, grant Dr. Berlowitz was supported by a Department of Veterans Affairs HSR&D Career Development Award. Dr. Brandeis was supported by a Clinical Investigator Award from the National Institute on Aging. The authors wish to thank Dr. Gene Stollerman and Dr. Mark Moskowitz for their helpful comments during preparation of the manuscript. Address correspondence and reprint requests to Dr. Dan Berlowitz, HSR&D Field Program, Bedford VA Medical Center, Bedford, MA REFERENCES 1. Allman RM. Pressure ulcers among the elderly. N Engl J Med 1989;320: Howell TH. Some terminal aspects of disease in old age: a clinical study of 300 patients. J AmGeriatrSoc 1969;17: Michocki RJ, Lamy PP. The problem of pressure sores in a nursing home population: statistical data. J Am Geriatr Soc 1976;24: Reed JW. Pressure ulcers in the elderly: prevention and treatment utilizing the team approach. Maryland State Med J 1981;30: Bergstrom N, Braden B. A prospective study of pressure sore risk among institutionalized elderly. J Am Geriatr Soc 1992;40: Berlowitz DR, Wilking SVB. The short-term outcome of pressure sores. J Am Geriatr Soc 1990;38: Brandeis GH, Morris JN, Nash DJ, Lipsitz LA. The epidemiology and natural history of pressure ulcers in elderly nursing home residents. JAMA l990;264: Bennett RG, Bellantoni MF, Ouslander JG. Air-fiuidized bed treatment of nursing home patients with pressure sores. J Am Geriatr Soc 1989;37: Ferrell BA, Osterweil D, Christenson P. A randomized trial of low-airloss beds for treatment of pressure ulcers. JAMA 1993;269: Allman RM, Walker JM, Hart MK, et al. Air-fiuidized beds or conventional therapy for pressure sores. Ann Intern Med 1987; 107: Scheckler WE, Peterson PJ. Infections and infection control among residents of eight rural Wisconsin nursing homes. Arch Intern Med 1986:146: Garibaldi RA, Brodine S, Matsumiya S. Infections among patients in nursing homes. N Engl J Med 1981 ;305: Bryan CS, Dew CE, Reynolds KL. Bacteremia associated with decubitus ulcers. Arch Intern Med 1983; 143: Galpin J, Ghow A, Bayer A, Guze L. Sepsis associated with decubitus ulcers. Am J Med 1976;61: Allman RM, Laprade CA, Noel LB, et al. Pressure sores among hospitalized patients. Ann Intern Med 1986; 105: Berlowitz DR, Wilking SVB. Risk factors for pressure sores: a comparison of cross-sectional and cohort-derived data. J Am Geriatr Soc 1989;37: Spector WD, Kapp MC, Tucker RJ, Sternberg J. Factors associated with presence of decubitus ulcers at admission to nursing homes. Gerontologist 1988;28:83O Rudman D, Abbasi AA, Tourky GM, Rudman IW, Mattson DE. Easily measurable adverse outcome indicators in a Veterans Affairs nursing home. QRB 1990; 16: Schneider DP, Fries BE, Foley WJ, Desmond M, Gormely WJ. Case mix for nursing home payment: Resource Utilization Groups, version II. Health Care Financing Rev 1988;10(Suppl): Rudman D, McCormack J, Cuisinier M, Mattson DE. A simple method to quantify the changes in activities of daily living of long-stay nursing home populations. Am J Phys Med Rehabil 1993;72: Beattie MC, Swindle RW, Tomko LA. Department of Veterans Affairs databases resource guide. Palo Alto, CA: HSR&D Center for Health Care Evaluation, National Pressure Ulcer Advisory Panel. Pressure ulcers' prevalence, cost, and risk assessment: consensus development conference statement. Decubitus 1989;2: Lewis MA, Kane RL, Cretin S, Clark V. The immediate and subsequent outcomes of nursing home care. Am J Public Health 1985;75: Lichtenstein MJ, Federspiel CF, Schaffner W. Factors associated with early demise in nursing home residents. J Am Geriatr Soc 1985;33: Rudman D, Slater EJ, Richardson TJ, Mattson DE. The occurrence of pressure ulcers in three nursing homes. J Gen Intern Med 1993;8: Received March 15, 1996 Accepted July 27, 1996
Supplementary Online Content
 Supplementary Online Content Pham B, Stern A, Chen W, et al. Preventing pressure ulcers in long-term care: a costeffectiveness analysis. Arch Intern Med. Published online September 26, 2011. doi:10.1001/archinternmed.2011.473
Supplementary Online Content Pham B, Stern A, Chen W, et al. Preventing pressure ulcers in long-term care: a costeffectiveness analysis. Arch Intern Med. Published online September 26, 2011. doi:10.1001/archinternmed.2011.473
Differences between Briefs 1
 Differences between Briefs 1 Comparisons on the Use of Disposable and Reusable Briefs in Long-Term Care: Skin Integrity of Residents and Burden on Staff by Peter Brink, Michael Stones, Wendy Kirkpatrick
Differences between Briefs 1 Comparisons on the Use of Disposable and Reusable Briefs in Long-Term Care: Skin Integrity of Residents and Burden on Staff by Peter Brink, Michael Stones, Wendy Kirkpatrick
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Inappropriate use of urinary catheters: A prospective observational study
 Inappropriate use of urinary catheters: A prospective observational study Manish M. Tiwari, MD, PhD, MPH, a Mary E. Charlton, PhD, a James R. Anderson, PhD, a Elizabeth D. Hermsen, PharmD, b and Mark E.
Inappropriate use of urinary catheters: A prospective observational study Manish M. Tiwari, MD, PhD, MPH, a Mary E. Charlton, PhD, a James R. Anderson, PhD, a Elizabeth D. Hermsen, PharmD, b and Mark E.
Surgery in Frail Elders. Emily Finlayson, MD, MS Department of Surgery University of California, San Francisco September, 2011
 Surgery in Frail Elders Emily Finlayson, MD, MS Department of Surgery University of California, San Francisco September, 2011 What we re going to cover Mortality after surgery in the elderly Fact v Fantasy
Surgery in Frail Elders Emily Finlayson, MD, MS Department of Surgery University of California, San Francisco September, 2011 What we re going to cover Mortality after surgery in the elderly Fact v Fantasy
Chapter 5: Acute Kidney Injury
 Chapter 5: Acute Kidney Injury In 2015, 4.3% of Medicare fee-for-service beneficiaries experienced a hospitalization complicated by Acute Kidney Injury (AKI); this appears to have plateaued since 2011
Chapter 5: Acute Kidney Injury In 2015, 4.3% of Medicare fee-for-service beneficiaries experienced a hospitalization complicated by Acute Kidney Injury (AKI); this appears to have plateaued since 2011
Retention in HIV care predicts subsequent retention and predicts survival well after the first year of care: a national study of US Veterans
 Retention in HIV care predicts subsequent retention and predicts survival well after the first year of care: a national study of US Veterans Thomas P. Giordano, MD, MPH, Jessica A. Davila, PhD, Christine
Retention in HIV care predicts subsequent retention and predicts survival well after the first year of care: a national study of US Veterans Thomas P. Giordano, MD, MPH, Jessica A. Davila, PhD, Christine
Case Review of Inpatient Rehabilitation Hospital Patients Not Suited for Intensive Therapy
 U.S. DEPARTMENT OF HEALTH & HUMAN SERVICES OFFICE OF INSPECTOR GENERAL Case Review of Inpatient Rehabilitation Hospital Patients Not Suited for Intensive Therapy OEI-06-16-00360 DECEMBER 2016 SUZANNE MURRIN
U.S. DEPARTMENT OF HEALTH & HUMAN SERVICES OFFICE OF INSPECTOR GENERAL Case Review of Inpatient Rehabilitation Hospital Patients Not Suited for Intensive Therapy OEI-06-16-00360 DECEMBER 2016 SUZANNE MURRIN
The prognosis of falls in elderly people living at home
 Age and Ageing 1999; 28: 121 125 The prognosis of falls in elderly people living at home IAN P. D ONALD, CHRISTOPHER J. BULPITT 1 Elderly Care Unit, Gloucestershire Royal Hospital, Great Western Road,
Age and Ageing 1999; 28: 121 125 The prognosis of falls in elderly people living at home IAN P. D ONALD, CHRISTOPHER J. BULPITT 1 Elderly Care Unit, Gloucestershire Royal Hospital, Great Western Road,
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
MAKING THE NSQIP PARTICIPANT USE DATA FILE (PUF) WORK FOR YOU
 MAKING THE NSQIP PARTICIPANT USE DATA FILE (PUF) WORK FOR YOU Hani Tamim, PhD Clinical Research Institute Department of Internal Medicine American University of Beirut Medical Center Beirut - Lebanon Participant
MAKING THE NSQIP PARTICIPANT USE DATA FILE (PUF) WORK FOR YOU Hani Tamim, PhD Clinical Research Institute Department of Internal Medicine American University of Beirut Medical Center Beirut - Lebanon Participant
The Geriatrician in the Trauma Service. Trauma Quality Improvement Program (TQIP) Annual Scientific Meeting and Training 2013
 The Geriatrician in the Trauma Service Trauma Quality Improvement Program (TQIP) Annual Scientific Meeting and Training 2013 Challenges of the Geriatric Trauma Patient Challenges of the Geriatric Patient
The Geriatrician in the Trauma Service Trauma Quality Improvement Program (TQIP) Annual Scientific Meeting and Training 2013 Challenges of the Geriatric Trauma Patient Challenges of the Geriatric Patient
Hospice and Palliative Care: Value-Based Care Near the End of Life
 Hospice and Palliative Care: Value-Based Care Near the End of Life Mary Dittrich, MD, FASN Senior Medical Director, Remedy Partners Joseph W. Shega, MD National Medical Director, VITAS Healthcare 2017
Hospice and Palliative Care: Value-Based Care Near the End of Life Mary Dittrich, MD, FASN Senior Medical Director, Remedy Partners Joseph W. Shega, MD National Medical Director, VITAS Healthcare 2017
Hospice and Palliative Care: Value-Based Care Near the End of Life
 Hospice and Palliative Care: Value-Based Care Near the End of Life Mary Dittrich, MD, FASN Senior Medical Director, Remedy Partners Joseph W. Shega, MD National Medical Director, VITAS Healthcare 2017
Hospice and Palliative Care: Value-Based Care Near the End of Life Mary Dittrich, MD, FASN Senior Medical Director, Remedy Partners Joseph W. Shega, MD National Medical Director, VITAS Healthcare 2017
The Long-term Prognosis of Delirium
 The Long-term Prognosis of Jane McCusker, MD, DrPH, Professor, Epidemiology and Biostatistics, McGill University; Head, Clinical Epidemiology and Community Studies, St. Mary s Hospital, Montreal, QC. Nine
The Long-term Prognosis of Jane McCusker, MD, DrPH, Professor, Epidemiology and Biostatistics, McGill University; Head, Clinical Epidemiology and Community Studies, St. Mary s Hospital, Montreal, QC. Nine
NeuroPI Case Study: Palliative Care Counseling and Advance Care Planning
 Case: An 86 year-old man presents to your office after recently being diagnosed as having mild dementia due to Alzheimer s disease, accompanied by his son who now runs the family business. At baseline
Case: An 86 year-old man presents to your office after recently being diagnosed as having mild dementia due to Alzheimer s disease, accompanied by his son who now runs the family business. At baseline
Age as a Predictor of Functional Outcome in Anoxic Brain Injury
 Age as a Predictor of Functional Outcome in Anoxic Brain Injury Mrugeshkumar K. Shah, MD, MPH, MS Samir Al-Adawi, PhD David T. Burke, MD, MA Department of Physical Medicine and Rehabilitation, Spaulding
Age as a Predictor of Functional Outcome in Anoxic Brain Injury Mrugeshkumar K. Shah, MD, MPH, MS Samir Al-Adawi, PhD David T. Burke, MD, MA Department of Physical Medicine and Rehabilitation, Spaulding
Geriatrics and Cancer Care
 Geriatrics and Cancer Care Roger Wong, BMSc, MD, FRCPC, FACP Postgraduate Dean of Medical Education Clinical Professor, Division of Geriatric Medicine UBC Faculty of Medicine Disclosure No competing interests
Geriatrics and Cancer Care Roger Wong, BMSc, MD, FRCPC, FACP Postgraduate Dean of Medical Education Clinical Professor, Division of Geriatric Medicine UBC Faculty of Medicine Disclosure No competing interests
THE POTENTIAL IMPACT OF VITALSTIM THERAPY ON HEALTHCARE COSTS: A White PaperVitalStim Therapy has significant
 Dysphagia THE POTENTIAL IMPACT OF VITALSTIM THERAPY ON HEALTHCARE COSTS: A White PaperVitalStim Therapy has significant Contents potential to dramatically impact the health care costs arising from oropharyngeal
Dysphagia THE POTENTIAL IMPACT OF VITALSTIM THERAPY ON HEALTHCARE COSTS: A White PaperVitalStim Therapy has significant Contents potential to dramatically impact the health care costs arising from oropharyngeal
Research Report. Key Words: Functional status; Orthopedics, general; Treatment outcomes. Neva J Kirk-Sanchez. Kathryn E Roach
 Research Report Relationship Between Duration of Therapy Services in a Comprehensive Rehabilitation Program and Mobility at Discharge in Patients With Orthopedic Problems Background and Purpose. The purpose
Research Report Relationship Between Duration of Therapy Services in a Comprehensive Rehabilitation Program and Mobility at Discharge in Patients With Orthopedic Problems Background and Purpose. The purpose
Appendix Identification of Study Cohorts
 Appendix Identification of Study Cohorts Because the models were run with the 2010 SAS Packs from Centers for Medicare and Medicaid Services (CMS)/Yale, the eligibility criteria described in "2010 Measures
Appendix Identification of Study Cohorts Because the models were run with the 2010 SAS Packs from Centers for Medicare and Medicaid Services (CMS)/Yale, the eligibility criteria described in "2010 Measures
The Effect of Depression on Social Engagement in Newly Admitted Dutch Nursing Home Residents
 The Gerontologist Vol. 43, No. 2, 213 218 Copyright 2003 by The Gerontological Society of America The Effect of Depression on Social Engagement in Newly Admitted Dutch Nursing Home Residents Wilco Achterberg,
The Gerontologist Vol. 43, No. 2, 213 218 Copyright 2003 by The Gerontological Society of America The Effect of Depression on Social Engagement in Newly Admitted Dutch Nursing Home Residents Wilco Achterberg,
Identification Information.
 Section A. Identification Information. A1200. Marital Status. 1. Never married. 2. Married. 3. Widowed. 4. Separated. 5. Divorced. A1300. Optional Resident Items. A. Medical record number: B. Room number:
Section A. Identification Information. A1200. Marital Status. 1. Never married. 2. Married. 3. Widowed. 4. Separated. 5. Divorced. A1300. Optional Resident Items. A. Medical record number: B. Room number:
QM Reports Technical Specifications: Version 1.0
 Exhibit 271 Introduction The measures contained on the Quality Measure (QM) Reports are calculated in two major steps. In the first step, two samples of assessments are selected: a long-stay sample and
Exhibit 271 Introduction The measures contained on the Quality Measure (QM) Reports are calculated in two major steps. In the first step, two samples of assessments are selected: a long-stay sample and
The Risks of Hip Fracture in Older People from Private Homes and Institutions
 Age and Ageing 1996:25:381-385 The Risks of Hip Fracture in Older People from Private Homes and Institutions MEG BUTLER, ROBYN NORTON, TREVOR LEE-JOE, ADA CHENG, A. JOHN CAMPBELL Summary This study aimed
Age and Ageing 1996:25:381-385 The Risks of Hip Fracture in Older People from Private Homes and Institutions MEG BUTLER, ROBYN NORTON, TREVOR LEE-JOE, ADA CHENG, A. JOHN CAMPBELL Summary This study aimed
9 Diabetes care. Back to contents
 Back to contents Diabetes is a major risk factor for the development of peripheral vascular disease and 349/628 (55.6%) of the patients in this study had diabetes. Hospital inpatients with diabetes are
Back to contents Diabetes is a major risk factor for the development of peripheral vascular disease and 349/628 (55.6%) of the patients in this study had diabetes. Hospital inpatients with diabetes are
SEPSIS: IT ALL BEGINS WITH INFECTION. Theresa Posani, MS, RN, ACNS-BC, CCRN M/S CNS/Sepsis Coordinator Texas Health Harris Methodist Ft.
 SEPSIS: IT ALL BEGINS WITH INFECTION Theresa Posani, MS, RN, ACNS-BC, CCRN M/S CNS/Sepsis Coordinator Texas Health Harris Methodist Ft. Worth 1 2 3 OBJECTIVES Review the new Sepsis 3 definitions of sepsis
SEPSIS: IT ALL BEGINS WITH INFECTION Theresa Posani, MS, RN, ACNS-BC, CCRN M/S CNS/Sepsis Coordinator Texas Health Harris Methodist Ft. Worth 1 2 3 OBJECTIVES Review the new Sepsis 3 definitions of sepsis
End of Life Care in Dementia. Dr Rosie Lockwood Consultant Geriatrician Sheffield Teaching Hospitals
 End of Life Care in Dementia Dr Rosie Lockwood Consultant Geriatrician Sheffield Teaching Hospitals Rosie.Lockwood@sth.nhs.uk Agenda Some facts and figures What are the challenges? What is good care? How
End of Life Care in Dementia Dr Rosie Lockwood Consultant Geriatrician Sheffield Teaching Hospitals Rosie.Lockwood@sth.nhs.uk Agenda Some facts and figures What are the challenges? What is good care? How
ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS
 R2 (REVISED MANUSCRIPT BLUE 200208-877OC) ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS Mario Castro, M.D., M.P.H. Nina A. Zimmermann R.N. Sue
R2 (REVISED MANUSCRIPT BLUE 200208-877OC) ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS Mario Castro, M.D., M.P.H. Nina A. Zimmermann R.N. Sue
Pattern of Functional Change During Rehabilitation of Patients With Hip Fracture
 111 ORIGINAL ARTICLE Pattern of Functional Change During Rehabilitation of Patients With Hip Fracture Nancy K. Latham, PhD, PT, Diane U. Jette, DSc, PT, Reg L. Warren, PhD, Christopher Wirtalla, BA ABSTRACT.
111 ORIGINAL ARTICLE Pattern of Functional Change During Rehabilitation of Patients With Hip Fracture Nancy K. Latham, PhD, PT, Diane U. Jette, DSc, PT, Reg L. Warren, PhD, Christopher Wirtalla, BA ABSTRACT.
Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications
 MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
COGNITIVE IMPAIRMENT IN
 COGNITIVE IMPAIRMENT IN THE HOSPITAL SETTING Professor Len Gray April 2014 Some key questions How common is cognitive impairment among hospitalised older patients? Which cognitive syndromes are associated
COGNITIVE IMPAIRMENT IN THE HOSPITAL SETTING Professor Len Gray April 2014 Some key questions How common is cognitive impairment among hospitalised older patients? Which cognitive syndromes are associated
Chapter 5: Acute Kidney Injury
 Chapter 5: Acute Kidney Injury Introduction In recent years, acute kidney injury (AKI) has gained increasing recognition as a major risk factor for the development of chronic kidney disease (CKD). The
Chapter 5: Acute Kidney Injury Introduction In recent years, acute kidney injury (AKI) has gained increasing recognition as a major risk factor for the development of chronic kidney disease (CKD). The
Geriatric screening in acute care wards a novel method of providing care to elderly patients
 Geriatric screening in acute care wards a novel method of providing care to elderly patients JKH Luk, T Kwok, J Woo Objective. To assess a nurse-implemented geriatric screening system. Design. Descriptive
Geriatric screening in acute care wards a novel method of providing care to elderly patients JKH Luk, T Kwok, J Woo Objective. To assess a nurse-implemented geriatric screening system. Design. Descriptive
Withholding & Withdrawing Life Sustaining Treatment: A Lifespan Approach
 Withholding & Withdrawing Life Sustaining Treatment: A Lifespan Approach Kenneth Brummel-Smith, M.D. Charlotte Edwards Maguire Professor, Department of Geriatrics FSU College of Medicine Basic Concepts
Withholding & Withdrawing Life Sustaining Treatment: A Lifespan Approach Kenneth Brummel-Smith, M.D. Charlotte Edwards Maguire Professor, Department of Geriatrics FSU College of Medicine Basic Concepts
Delirium in the Elderly
 Delirium in the Elderly ELITE 2015 Mamata Yanamadala M.B.B.S, MS Division of Geriatrics Why should we care about delirium? It is: common associated with high mortality associated with increased morbidity
Delirium in the Elderly ELITE 2015 Mamata Yanamadala M.B.B.S, MS Division of Geriatrics Why should we care about delirium? It is: common associated with high mortality associated with increased morbidity
Medical conditions as risk factors for pressure ulcers in an outpatient setting
 Age and Ageing 2003; 32: 259 264 # Age and Ageing Vol. 32 No. 3 # 2003, British Geriatrics Society. All rights reserved. Medical conditions as risk factors for pressure ulcers in an outpatient setting
Age and Ageing 2003; 32: 259 264 # Age and Ageing Vol. 32 No. 3 # 2003, British Geriatrics Society. All rights reserved. Medical conditions as risk factors for pressure ulcers in an outpatient setting
24 09:29:46 EDT 2008 QIES
 Wed Sep 24 9:29:46 EDT 28 QIES Workbench Record Layout Report For Job: OASIS Dump of Everything for dictionary ( 23927.1 ) Report Name: OASIS Dump of Everything for dictionary Data Type Offset Length DP
Wed Sep 24 9:29:46 EDT 28 QIES Workbench Record Layout Report For Job: OASIS Dump of Everything for dictionary ( 23927.1 ) Report Name: OASIS Dump of Everything for dictionary Data Type Offset Length DP
Supplementary Online Content
 Supplementary Online Content Schnabel RB, Aspelund T, Li G, et al. Validation of an atrial fibrillation risk algorithm in whites and African Americans. Arch Intern Med. 2010;170(21):1909-1917. eappendix.
Supplementary Online Content Schnabel RB, Aspelund T, Li G, et al. Validation of an atrial fibrillation risk algorithm in whites and African Americans. Arch Intern Med. 2010;170(21):1909-1917. eappendix.
SHORT COMMUNICATION. G. Joshy & P. Dunn & M. Fisher & R. Lawrenson
 Diabetologia (2009) 52:1474 1478 DOI 10.1007/s00125-009-1380-1 SHORT COMMUNICATION Ethnic differences in the natural progression of nephropathy among diabetes patients in New Zealand: hospital admission
Diabetologia (2009) 52:1474 1478 DOI 10.1007/s00125-009-1380-1 SHORT COMMUNICATION Ethnic differences in the natural progression of nephropathy among diabetes patients in New Zealand: hospital admission
Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
 Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Attendance rates and outcomes of cardiac rehabilitation in Victoria, 1998
 Attendance rates and outcomes of cardiac rehabilitation in Victoria, 1998 CARDIOVASCULAR DISEASE is the leading cause of death in Australia, causing more than 40% of all deaths in 1998. 1 Cardiac rehabilitation
Attendance rates and outcomes of cardiac rehabilitation in Victoria, 1998 CARDIOVASCULAR DISEASE is the leading cause of death in Australia, causing more than 40% of all deaths in 1998. 1 Cardiac rehabilitation
Do Elderly Men Have Increased Mortality Following Hip Fracture?
 Do Elderly Men Have Increased Mortality Following Hip Fracture? Excess Mortality in Men Compared With Women Following a Hip Fracture. National Analysis of Comedications, Comorbidity and Survival. Kannegaard
Do Elderly Men Have Increased Mortality Following Hip Fracture? Excess Mortality in Men Compared With Women Following a Hip Fracture. National Analysis of Comedications, Comorbidity and Survival. Kannegaard
Michal Boyd, 1,2,3 Joanna B Broad, 1 Xian (Tony) Zhang, 1 Ngaire Kerse, 4 and Martin J Connolly 1,3
 NZACA Annual Conference - Wellington 15 October 2014 Michal Boyd, 1,2,3 Joanna B Broad, 1 Xian (Tony) Zhang, 1 Ngaire Kerse, 4 and Martin J Connolly 1,3 1 Freemasons Department of Geriatric Medicine, The
NZACA Annual Conference - Wellington 15 October 2014 Michal Boyd, 1,2,3 Joanna B Broad, 1 Xian (Tony) Zhang, 1 Ngaire Kerse, 4 and Martin J Connolly 1,3 1 Freemasons Department of Geriatric Medicine, The
The COLLaboration on AGEing (COLLAGE)
 The COLLaboration on AGEing (COLLAGE) Professor D. William Molloy University College Cork, Ireland. The Lessons from Europe Seminar 23-09-15 Overview Exemplars within COLLAGE: 1. What is COLLAGE? 2. The
The COLLaboration on AGEing (COLLAGE) Professor D. William Molloy University College Cork, Ireland. The Lessons from Europe Seminar 23-09-15 Overview Exemplars within COLLAGE: 1. What is COLLAGE? 2. The
Chapter 2: Identification and Care of Patients with CKD
 Chapter 2: Identification and Care of Patients with CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients with CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Risk Adjustment for Clinicians. Risk Adjustment Resource. Logistic Regression Models 4/2/2012
 Risk Adjustment for Clinicians Teresa Northcutt RN BSN COS C HCS D Missouri Alliance for Home Care Annual Conference 2012 Risk Adjustment Resource Home Health Agency Quality Measures: Logistic Regression
Risk Adjustment for Clinicians Teresa Northcutt RN BSN COS C HCS D Missouri Alliance for Home Care Annual Conference 2012 Risk Adjustment Resource Home Health Agency Quality Measures: Logistic Regression
Prolonged Mechanical Ventilation
 Prolonged Mechanical Ventilation Shannon S. Carson, MD Associate Professor and Chief Pulmonary and Critical Care Medicine University of North Carolina AJRCCM 2010 Projected Growth of Prolonged Acute MV
Prolonged Mechanical Ventilation Shannon S. Carson, MD Associate Professor and Chief Pulmonary and Critical Care Medicine University of North Carolina AJRCCM 2010 Projected Growth of Prolonged Acute MV
Appendix. Potentially Preventable Complications (PPCs) identify. complications that can occur during an admission. There are 64
 Calikoglu S, Murray R, Feeney D. Hospital pay-for-performance programs in Maryland produced strong results, including reduced hospital-acquired infections. Health Aff (Millwood). 2012;31(12). Appendix
Calikoglu S, Murray R, Feeney D. Hospital pay-for-performance programs in Maryland produced strong results, including reduced hospital-acquired infections. Health Aff (Millwood). 2012;31(12). Appendix
Is laparoscopic sleeve gastrectomy safer than laparoscopic gastric bypass?
 Is laparoscopic sleeve gastrectomy safer than laparoscopic gastric bypass? A comparison of 30-day complications using the MBSAQIP data registry Sandhya B. Kumar MD, Barbara C. Hamilton MD, Soren Jonzzon,
Is laparoscopic sleeve gastrectomy safer than laparoscopic gastric bypass? A comparison of 30-day complications using the MBSAQIP data registry Sandhya B. Kumar MD, Barbara C. Hamilton MD, Soren Jonzzon,
Stability of Choices about Life-sustaining Treatments Marion Danis, MD; Joanne Garrett, PhD; Russell Harris, MD; and Donald L.
 Stability of Choices about Life-sustaining Treatments Marion Danis, MD; Joanne Garrett, PhD; Russell Harris, MD; and Donald L. Patrick, PhD Objective: To examine the stability of patients' choices for
Stability of Choices about Life-sustaining Treatments Marion Danis, MD; Joanne Garrett, PhD; Russell Harris, MD; and Donald L. Patrick, PhD Objective: To examine the stability of patients' choices for
No Association between Calcium Channel Blocker Use and Confirmed Bleeding Peptic Ulcer Disease
 American Journal of Epidemiology Copyright 1998 by The Johns Hopkins University School of Hygiene and Public Health All rights reserved Vol. 148, No. 4 Printed in U.S.A. A BRIEF ORIGINAL CONTRIBUTION No
American Journal of Epidemiology Copyright 1998 by The Johns Hopkins University School of Hygiene and Public Health All rights reserved Vol. 148, No. 4 Printed in U.S.A. A BRIEF ORIGINAL CONTRIBUTION No
Delirium in the Elderly
 Delirium in the Elderly ELITE 2017 Liza Genao, MD Division of Geriatrics Why should we care about delirium? It is: common associated with high mortality associated with increased morbidity Very much under-recognized
Delirium in the Elderly ELITE 2017 Liza Genao, MD Division of Geriatrics Why should we care about delirium? It is: common associated with high mortality associated with increased morbidity Very much under-recognized
HOMES AND SENIORS SERVICES. APPROVAL DATE: February 2011 REVISION DATE: July 2018
 Page 1 of 7 POLICY: Each resident s level of nutrition and hydration risk will be identified by the Registered Dietitian during the RAI-MDS Admission Assessment and thereafter during the quarterly, significant
Page 1 of 7 POLICY: Each resident s level of nutrition and hydration risk will be identified by the Registered Dietitian during the RAI-MDS Admission Assessment and thereafter during the quarterly, significant
MDS 3.0 Quality Measures USER S MANUAL
 MDS 3.0 Quality Measures USER S MANUAL Effective April 1, 2017 Prepared for: The Centers for Medicare & Medicaid Services under Contract No. HHSM500-2013- 13015I (HHSM-500-T0001). (RTI Project Number 0214077.001.001)
MDS 3.0 Quality Measures USER S MANUAL Effective April 1, 2017 Prepared for: The Centers for Medicare & Medicaid Services under Contract No. HHSM500-2013- 13015I (HHSM-500-T0001). (RTI Project Number 0214077.001.001)
Approaches to Predictive Modeling for Palliative or Hospice Care Management
 Approaches to Predictive Modeling for Palliative or Hospice Care Management Donald L. Libby, PhD and Stephen Saunders, MD Fourth National Predictive Modeling Summit September 15-16, 2010 Presenters Donald
Approaches to Predictive Modeling for Palliative or Hospice Care Management Donald L. Libby, PhD and Stephen Saunders, MD Fourth National Predictive Modeling Summit September 15-16, 2010 Presenters Donald
The elderly in residential care: mortality in relation to functional capacity
 Journal of Epidemiology and Community Health, 1980, 34, 96-101 The elderly in residential care: mortality in relation to functional capacity L. J. DONALDSON, D G CLAYTON, AND MICHAEL CLARKE From the Department
Journal of Epidemiology and Community Health, 1980, 34, 96-101 The elderly in residential care: mortality in relation to functional capacity L. J. DONALDSON, D G CLAYTON, AND MICHAEL CLARKE From the Department
Exposure to potentially inappropriate medications among long-term care residents with cognitive impairment in Ontario:
 Exposure to potentially inappropriate medications among long-term care residents with cognitive impairment in Ontario: Is there an association with frailty? Laura Maclagan, Jun Guan, Sima Gandhi, Colleen
Exposure to potentially inappropriate medications among long-term care residents with cognitive impairment in Ontario: Is there an association with frailty? Laura Maclagan, Jun Guan, Sima Gandhi, Colleen
a guide to Reimbursement of Intermittent Catheters Know your options M2116N 04.08
 a guide to Reimbursement of Intermittent Catheters 1 Know your options Coloplast Corp. Minneapolis, MN 55411 1.800.533.0464 usmedweb@coloplast.com www.us.coloplast.com is a registered trademark of Coloplast
a guide to Reimbursement of Intermittent Catheters 1 Know your options Coloplast Corp. Minneapolis, MN 55411 1.800.533.0464 usmedweb@coloplast.com www.us.coloplast.com is a registered trademark of Coloplast
Rehabilitation/Geriatrics ADMISSION CRITERIA. Coordinated Entry System
 Rehabilitation/Geriatrics ADMISSION CRITERIA Coordinated Entry System Table of Contents Rehabilitation and Geriatric Service Sites 3 Overview of Coordinated Entry System...4 Geriatric Rehabilitation Service
Rehabilitation/Geriatrics ADMISSION CRITERIA Coordinated Entry System Table of Contents Rehabilitation and Geriatric Service Sites 3 Overview of Coordinated Entry System...4 Geriatric Rehabilitation Service
Palliative Care for Older Adults in the United States
 Palliative Care for Older Adults in the United States Nathan Goldstein, MD Associate Professor Hertzberg Palliative Care Institute Brookdale Department of Geriatrics and Palliative Medicine Icahn School
Palliative Care for Older Adults in the United States Nathan Goldstein, MD Associate Professor Hertzberg Palliative Care Institute Brookdale Department of Geriatrics and Palliative Medicine Icahn School
Water Works. The Value of Water
 Water Works The Value of Water The Value of Water Water Works Water is vital for the body Accounting for roughly 60% of body weight, water is the largest component of the human body and the major constituent
Water Works The Value of Water The Value of Water Water Works Water is vital for the body Accounting for roughly 60% of body weight, water is the largest component of the human body and the major constituent
Financial & Management Aspects of OASIS C2
 Financial & Management Aspects of OASIS C2 Presented By: Melinda A. Gaboury, COS C Healthcare Provider Solutions, Inc. 615 399 7499 info@healthcareprovidersolutions.com WHAT DOES OASIS C2 IMPACT? HHRG/HIPPS
Financial & Management Aspects of OASIS C2 Presented By: Melinda A. Gaboury, COS C Healthcare Provider Solutions, Inc. 615 399 7499 info@healthcareprovidersolutions.com WHAT DOES OASIS C2 IMPACT? HHRG/HIPPS
JAMA, January 11, 2012 Vol 307, No. 2
 JAMA, January 11, 2012 Vol 307, No. 2 Dementia is associated with increased rates and often poorer outcomes of hospitalization Worsening cognitive status Adequate chronic disease management is more difficult
JAMA, January 11, 2012 Vol 307, No. 2 Dementia is associated with increased rates and often poorer outcomes of hospitalization Worsening cognitive status Adequate chronic disease management is more difficult
Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts Future Cardiovascular Events
 Diabetes Care Publish Ahead of Print, published online May 28, 2008 Chronotropic response in patients with diabetes Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts
Diabetes Care Publish Ahead of Print, published online May 28, 2008 Chronotropic response in patients with diabetes Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts
Chapter 2: Identification and Care of Patients With CKD
 Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Adam D. Marks, MD MPH Assistant Professor of Medicine University of Michigan Health System
 Adam D. Marks, MD MPH Assistant Professor of Medicine University of Michigan Health System The truth will set you free but first it will piss you off - Gloria Steinem Life expectancy is up dramatically
Adam D. Marks, MD MPH Assistant Professor of Medicine University of Michigan Health System The truth will set you free but first it will piss you off - Gloria Steinem Life expectancy is up dramatically
Evaluating Functional Status in Hospitalized Geriatric Patients. UCLA-Santa Monica Geriatric Medicine Didactic Lecture Series
 Evaluating Functional Status in Hospitalized Geriatric Patients UCLA-Santa Monica Geriatric Medicine Didactic Lecture Series Case 88 y.o. woman was admitted for a fall onto her hip. She is having trouble
Evaluating Functional Status in Hospitalized Geriatric Patients UCLA-Santa Monica Geriatric Medicine Didactic Lecture Series Case 88 y.o. woman was admitted for a fall onto her hip. She is having trouble
In each hospital-year, we calculated a 30-day unplanned. readmission rate among patients who survived at least 30 days
 Romley JA, Goldman DP, Sood N. US hospitals experienced substantial productivity growth during 2002 11. Health Aff (Millwood). 2015;34(3). Published online February 11, 2015. Appendix Adjusting hospital
Romley JA, Goldman DP, Sood N. US hospitals experienced substantial productivity growth during 2002 11. Health Aff (Millwood). 2015;34(3). Published online February 11, 2015. Appendix Adjusting hospital
Hospital at Home. Frailty and Hospital at Home. 17 th March Pam Livingstone and Gwyneth Thom
 Hospital at Home Frailty and Hospital at Home 17 th March 2016 Pam Livingstone and Gwyneth Thom National Definition of Hospital at Home December 2013 An episode of specialist care delivered at home as
Hospital at Home Frailty and Hospital at Home 17 th March 2016 Pam Livingstone and Gwyneth Thom National Definition of Hospital at Home December 2013 An episode of specialist care delivered at home as
Finland and Sweden and UK GP-HOSP datasets
 Web appendix: Supplementary material Table 1 Specific diagnosis codes used to identify bladder cancer cases in each dataset Finland and Sweden and UK GP-HOSP datasets Netherlands hospital and cancer registry
Web appendix: Supplementary material Table 1 Specific diagnosis codes used to identify bladder cancer cases in each dataset Finland and Sweden and UK GP-HOSP datasets Netherlands hospital and cancer registry
Quality Care for the Hospitalized Older Adult
 Quality Care for the Hospitalized Older Adult Quality Care for the Hospitalized Older Adult Shelley R McDonald, DO, PhD May 19 th, 2018 Objectives To define why the hospital is a dangerous place for older
Quality Care for the Hospitalized Older Adult Quality Care for the Hospitalized Older Adult Shelley R McDonald, DO, PhD May 19 th, 2018 Objectives To define why the hospital is a dangerous place for older
Understanding and Assessing for Frailty
 Understanding and Assessing for Frailty Dr Gloria Yu Clinical Head of Bexley Integrated Care Consultant Physician in Elderly, General and Stroke Medicine 8 July 2015 Learning objectives What is frailty?
Understanding and Assessing for Frailty Dr Gloria Yu Clinical Head of Bexley Integrated Care Consultant Physician in Elderly, General and Stroke Medicine 8 July 2015 Learning objectives What is frailty?
Predictors of Outcomes of Community Acquired Pneumonia in Egyptian Older Adults
 Original Contribution/Clinical Investigation Predictors of Outcomes of Community Acquired Pneumonia in Egyptian Older Adults Hossameldin M. M. Abdelrahman Amal E. E. Elawam Ain Shams University, Faculty
Original Contribution/Clinical Investigation Predictors of Outcomes of Community Acquired Pneumonia in Egyptian Older Adults Hossameldin M. M. Abdelrahman Amal E. E. Elawam Ain Shams University, Faculty
Original Article. Japanese Journal of Comprehensive Rehabilitation Science (2011)
 77 Japanese Journal of Comprehensive Rehabilitation Science (2011) Original Article Relationship between the intensity of stroke rehabilitation and outcome: A survey conducted by the Kaifukuki Rehabilitation
77 Japanese Journal of Comprehensive Rehabilitation Science (2011) Original Article Relationship between the intensity of stroke rehabilitation and outcome: A survey conducted by the Kaifukuki Rehabilitation
How Can Palliative Care Help Your Patient Get Home Sooner?
 How Can Palliative Care Help Your Patient Get Home Sooner? Annette T. Carron, D.O. Director Geriatrics and Palliative Care Botsford Hospital OMED 2014 Patient Care Issues That Can Delay Your Day/ Pain
How Can Palliative Care Help Your Patient Get Home Sooner? Annette T. Carron, D.O. Director Geriatrics and Palliative Care Botsford Hospital OMED 2014 Patient Care Issues That Can Delay Your Day/ Pain
(Facility Name and Address) (1D) Surveillance of Urinary Tract Infections in the Long-Term Care Setting
 Policy Number: 1D Date: 4/16/14 Version: 1 (1D) Surveillance of Urinary Tract Infections in the Long-Term Care Setting Introduction: One-quarter of the older adult population in the United States will
Policy Number: 1D Date: 4/16/14 Version: 1 (1D) Surveillance of Urinary Tract Infections in the Long-Term Care Setting Introduction: One-quarter of the older adult population in the United States will
Pancreatitis Is a Risk Factor for Pancreatic Cancer
 GASTROENTEROLOGY 1995;109:247-251 Pancreatitis Is a Risk Factor for Pancreatic Cancer PRADEEP BANSAL and AMNON SONNENBERG Division of Gastroenterology and Division of Epidemiology, Department of Veterans
GASTROENTEROLOGY 1995;109:247-251 Pancreatitis Is a Risk Factor for Pancreatic Cancer PRADEEP BANSAL and AMNON SONNENBERG Division of Gastroenterology and Division of Epidemiology, Department of Veterans
EPO-144 Patients with Morbid Obesity and Congestive Heart Failure Have Longer Operative Time and Room Time in Total Hip Arthroplasty
 SESUG 2016 EPO-144 Patients with Morbid Obesity and Congestive Heart Failure Have Longer Operative Time and Room Time in Total Hip Arthroplasty ABSTRACT Yubo Gao, University of Iowa Hospitals and Clinics,
SESUG 2016 EPO-144 Patients with Morbid Obesity and Congestive Heart Failure Have Longer Operative Time and Room Time in Total Hip Arthroplasty ABSTRACT Yubo Gao, University of Iowa Hospitals and Clinics,
Critical Review Form Clinical Prediction or Decision Rule
 Critical Review Form Clinical Prediction or Decision Rule Development and Validation of a Multivariable Predictive Model to Distinguish Bacterial from Aseptic Meningitis in Children, Pediatrics 2002; 110:
Critical Review Form Clinical Prediction or Decision Rule Development and Validation of a Multivariable Predictive Model to Distinguish Bacterial from Aseptic Meningitis in Children, Pediatrics 2002; 110:
Recovery trajectories following critical illness: Can we really modify them? Tim Walsh Professor of Critical Care, Edinburgh University
 Recovery trajectories following critical illness: Can we really modify them? Tim Walsh Professor of Critical Care, Edinburgh University Considerations What is the problem? What is the current evidence
Recovery trajectories following critical illness: Can we really modify them? Tim Walsh Professor of Critical Care, Edinburgh University Considerations What is the problem? What is the current evidence
NIH Public Access Author Manuscript World J Urol. Author manuscript; available in PMC 2012 February 1.
 NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
The Geography of Medicare Beneficiary Hospitalizations 2012 Data
 The Geography of Medicare Beneficiary Hospitalizations 2012 Data Gary, PhD Mandi-Leigh Peterson, MA Alana Knudson, PhD Rural Health Reform Policy and Research Center Center for Rural Health/NORC University
The Geography of Medicare Beneficiary Hospitalizations 2012 Data Gary, PhD Mandi-Leigh Peterson, MA Alana Knudson, PhD Rural Health Reform Policy and Research Center Center for Rural Health/NORC University
Sharp HealthCare Hospice and Palliative Care
 Sharp HealthCare Hospice and Palliative Care The Continuum for Advanced Illness and End Stage Disease Management (AAC) Daniel R. Hoefer, MD CMO, Outpatient Palliative Care and Hospice Suzi K. Johnson,
Sharp HealthCare Hospice and Palliative Care The Continuum for Advanced Illness and End Stage Disease Management (AAC) Daniel R. Hoefer, MD CMO, Outpatient Palliative Care and Hospice Suzi K. Johnson,
The risk of dementia and death after delirium
 Age and Ageing 1999; 28: 551 556 The risk of dementia and death after delirium KENNETH ROCKWOOD, SYLVIA COSWAY, DANIEL CARVER, PAMELA JARRETT, KAREN STADNYK, JOHN FISK Division of Geriatric Medicine, Dalhousie
Age and Ageing 1999; 28: 551 556 The risk of dementia and death after delirium KENNETH ROCKWOOD, SYLVIA COSWAY, DANIEL CARVER, PAMELA JARRETT, KAREN STADNYK, JOHN FISK Division of Geriatric Medicine, Dalhousie
Rates and patterns of participation in cardiac rehabilitation in Victoria
 Rates and patterns of participation in cardiac rehabilitation in Victoria Vijaya Sundararajan, MD, MPH, Stephen Begg, MS, Michael Ackland, MBBS, MPH, FAPHM, Ric Marshall, PhD Victorian Department of Human
Rates and patterns of participation in cardiac rehabilitation in Victoria Vijaya Sundararajan, MD, MPH, Stephen Begg, MS, Michael Ackland, MBBS, MPH, FAPHM, Ric Marshall, PhD Victorian Department of Human
Describe the 2017 expectations of NPSG Effectively evaluate compliance with NPSG
 DRAFT Surveyor Education Module Nursing Care Center (NCC) Accreditation Program National Patient Safety Goal on Catheter-Associated Urinary Tract Infections Effective Date: January 2017 Introduction This
DRAFT Surveyor Education Module Nursing Care Center (NCC) Accreditation Program National Patient Safety Goal on Catheter-Associated Urinary Tract Infections Effective Date: January 2017 Introduction This
Course Handouts & Post Test
 STROKE/COMA: DISEASE TRAJECTORY AND HOSPICE ELIGIBILITY Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Hospice Education Network Course Handouts & Post Test To download presentation
STROKE/COMA: DISEASE TRAJECTORY AND HOSPICE ELIGIBILITY Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Hospice Education Network Course Handouts & Post Test To download presentation
Death by Bedrest: The Perils of The Hospital
 Death by Bedrest: The Perils of The Hospital Mindy Fain, MD Professor of Clinical Medicine Director, Arizona Reynolds Program of Applied Geriatrics Section Head, Geriatrics & Gerontology University of
Death by Bedrest: The Perils of The Hospital Mindy Fain, MD Professor of Clinical Medicine Director, Arizona Reynolds Program of Applied Geriatrics Section Head, Geriatrics & Gerontology University of
Value of Hospice Benefit to Medicaid Programs
 One Pennsylvania Plaza, 38 th Floor New York, NY 10119 Tel 212-279-7166 Fax 212-629-5657 www.milliman.com Value of Hospice Benefit May 2, 2003 Milliman USA, Inc. New York, NY Kate Fitch, RN, MEd, MA Bruce
One Pennsylvania Plaza, 38 th Floor New York, NY 10119 Tel 212-279-7166 Fax 212-629-5657 www.milliman.com Value of Hospice Benefit May 2, 2003 Milliman USA, Inc. New York, NY Kate Fitch, RN, MEd, MA Bruce
Delirium. A Geriatric Syndrome. Jonathan McCaleb, MD, CMD, HMDC UNSOM, Assistant Professor of Medicine Geriatrics / Hospice & Palliative Medicine
 Delirium A Geriatric Syndrome Jonathan McCaleb, MD, CMD, HMDC UNSOM, Assistant Professor of Medicine Geriatrics / Hospice & Palliative Medicine Introduction Common Serious Unrecognized: a medical emergency
Delirium A Geriatric Syndrome Jonathan McCaleb, MD, CMD, HMDC UNSOM, Assistant Professor of Medicine Geriatrics / Hospice & Palliative Medicine Introduction Common Serious Unrecognized: a medical emergency
Continence, falls and the frailty syndrome. Anne Foley - BGS Bladders and Bowel Health 2012
 Continence, falls and the frailty syndrome Outline Frailty Geriatric syndromes and giants Aetiology What can be done? The future Frailty Frailty Frailty (noun): The state of being weak in health or body
Continence, falls and the frailty syndrome Outline Frailty Geriatric syndromes and giants Aetiology What can be done? The future Frailty Frailty Frailty (noun): The state of being weak in health or body
A Competing Risk Analysis of Men Age Years at Diagnosis Managed Conservatively for Clinically Localized Prostate Cancer
 A Competing Risk Analysis of Men Age 55-74 Years at Diagnosis Managed Conservatively for Clinically Localized Prostate Cancer Peter C. Albertsen, MD 1 James A. Hanley, PhD 2 Donald F.Gleason, MD, PhD 3
A Competing Risk Analysis of Men Age 55-74 Years at Diagnosis Managed Conservatively for Clinically Localized Prostate Cancer Peter C. Albertsen, MD 1 James A. Hanley, PhD 2 Donald F.Gleason, MD, PhD 3
Geriatr Gerontol Int 2016; 16: ORIGINAL ARTICLE: EPIDEMIOLOGY, CLINICAL PRACTICE AND HEALTH
 bs_bs_banner Geriatr Gerontol Int 2016; 16: 1324 1331 ORIGINAL ARTICLE: EPIDEMIOLOGY, CLINICAL PRACTICE AND HEALTH Lower body function as a predictor of mortality over 13 years of follow up: Findings from
bs_bs_banner Geriatr Gerontol Int 2016; 16: 1324 1331 ORIGINAL ARTICLE: EPIDEMIOLOGY, CLINICAL PRACTICE AND HEALTH Lower body function as a predictor of mortality over 13 years of follow up: Findings from
Objectives. Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers
 Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers August 22, 2017 Objectives Understand the basics of the hospital specific MSPB data files and reports Review the factors
Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers August 22, 2017 Objectives Understand the basics of the hospital specific MSPB data files and reports Review the factors
Geriatric Grand Rounds
 Geriatric Grand Rounds Prevalence and Risk Factors of Delirium in Older Patients Admitted to a Community Based Acute Care Hospital Tuesday, October 27, 2009 12:00 noon Dr. Bill Black Auditorium Glenrose
Geriatric Grand Rounds Prevalence and Risk Factors of Delirium in Older Patients Admitted to a Community Based Acute Care Hospital Tuesday, October 27, 2009 12:00 noon Dr. Bill Black Auditorium Glenrose
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Influenza Vaccine Effectiveness among the Elderly Monto et al. Influenza Vaccine Effectiveness among Elderly Nursing Home Residents: A Cohort Study
 American Journal of Epidemiology Copyright 2001 by the Johns Hopkins University Bloomberg School of Public Health All rights reserved Vol. 154, No. 2 Printed in U.S.A. Influenza Vaccine Effectiveness among
American Journal of Epidemiology Copyright 2001 by the Johns Hopkins University Bloomberg School of Public Health All rights reserved Vol. 154, No. 2 Printed in U.S.A. Influenza Vaccine Effectiveness among
CHF Longitudinal Workgroup. Addressing readmissions from SNFs and other PAC settings 3/2/17
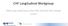 CHF Longitudinal Workgroup Addressing readmissions from SNFs and other PAC settings 3/2/17 Readmission Rate (%) Readmission Rate from SNF by Hospital (CHF) 16 14 13.6% 12 10 8 6 4 2 0 Mean = 6.3% 0% 0
CHF Longitudinal Workgroup Addressing readmissions from SNFs and other PAC settings 3/2/17 Readmission Rate (%) Readmission Rate from SNF by Hospital (CHF) 16 14 13.6% 12 10 8 6 4 2 0 Mean = 6.3% 0% 0
Home Health Prospective Payment System. Overview
 Overview Version 6117 January 2017 PBL-046 Java is a registered trademark of Oracle and/or its affiliates. Table of Contents Overview of the... 5 Background and versioning... 5 Changes for this version...
Overview Version 6117 January 2017 PBL-046 Java is a registered trademark of Oracle and/or its affiliates. Table of Contents Overview of the... 5 Background and versioning... 5 Changes for this version...
