post-discharge support to help prevent readmission.
|
|
|
- Katrina Davis
- 6 years ago
- Views:
Transcription
1 Retrospective Cohort Study of Medication Adherence And Risk for 30-day Hospital Readmission in a Medicare Cost Plan Angela K. Hochhalter, PhD; Rashmita Basu, PhD; Karim Prasla, PharmD; and Chanhee Jo, PhD ABSTRACT Purpose: Reducing hospital readmissions requires deploying appropriate interventions to groups at highest risk for readmission. Longterm medication adherence may indicate one s ability to manage recovery and chronic illness after discharge. If so, medication adherence also may be a predictor of hospital readmission. Design: The objective of this study was to test the association of longterm medication adherence with hospital readmission in a cohort of beneficiaries enrolled in a Medicare Cost Plan. Methodology: The study employed a retrospective cohort design using administrative pharmacy and health care claims for a sample hospitalized in Medication adherence was measured with the medication possession ratio (MPR) for the 12 months prior to the first hospitalization in The likelihood of readmission Corresponding author Angela K. Hochhalter, PhD Assistant Professor Department of Internal Medicine Scott & White Healthcare and Texas A&M Health Science Center 2401 South 31st St. (CDM) MS-34-M1254 Temple, TX (254) ahochhalter@swmail.sw.org Disclosures: All authors are employees of the health care system that includes the health plan in which participants were members. The authors report no financial or other conflicts of interest regarding the subject of this article. within 30 days from the first hospitalization in 2009 was estimated using the logistic regression model. Results: Long-term medication adherence was not associated with likelihood of 30-day hospital readmission (odds ratio [OR]=0.82, P=.71). However, older age (OR=1.07, P=.003) and longer length of hospital stay (OR=1.2, P<.001) were associated with higher likelihood of 30-day readmission, while having an office visit within 30 days of discharge (OR=0.38, P=.03) was associated with lower odds of readmission. Conclusion: Except for older age, variables associated with likelihood of readmission are difficult for clinical teams to access during a hospital stay to identify those at risk for readmission. Additional work is needed to identify indicators of readmission risk that can be utilized during hospitalization to identify patients needing post-discharge support to help prevent readmission. INTRODUCTION Transitions from hospitals back to patient homes pose risks for adverse events that lead to costly hospital readmission (Amin 2009, Boling 2009, Tsilimingrad 2008). Older adults are particularly vulnerable to hospital readmission because many have complex care needs that require careful coordination by health care providers and systems in addition to illness self-management (Jencks 2009, Ross 2009). For example, approximately half of discrepancies between medications prescribed at hospital discharge and medications elderly consumers report taking have been classified as associated with intentional or unintentional nonadherence (Coleman 2005). The majority of evidence on hospital-to-home transitions speaks to the role of health systems and practitioners. Transitional care interventions have extended the practice team s presence into patient homes or nursing homes. For example, nurses may follow patients after discharge and provide supportive care and clinical guidance (Harrison 2002, Naylor 1999), coaches may work with patients to empower self-management, or tools for improved hospital-nursing home communication may be adopted (Coleman 2006, Ouslander 2009, Parry 2009). Effective interventions incorporate support or training for patients and families to carry out tasks that are important to the success of the hospital-to-home transition (eg, watching for signs of illness exacerbation, adhering to new medication regimens, communicating with outpatient clinicians). While it is assumed that patients play an important role in successful transitions, little is known about how patients manage the challenges of transitions in care, which health behaviors are most effective for avoiding readmission, or which consumers need additional support to actively manage challenges at home. Empirical findings show that that medication management after hospital discharge is a serious challenge for many older adults. Older adults are at higher risk than other age groups for self-discontinuation of certain medications following hospitalization because they report feeling worse on the medication, feeling that medications are not helping, or being unable to JANUARY 2014 / MANAGED CARE 43
2 afford prescribed medications (Ali 2009). Li and colleagues (2004) found that after controlling for use of paid or unpaid nursing care, assistance with daily activities, and other factors, illness duration and self-reported recent medication adherence were consistent predictors of hospital readmission for elderly consumers with congestive heart failure. There is also evidence that better long-term medication adherence is associated with lower use of hospital services among populations without Medicare coverage. For example, Pitt man and colleagues (2010) reported that adults aged 18 to 63 years with hypertension and high adherence to antihypertensive medication (per administrative billing records) had lower health care costs and fewer hospitalizations for cardiovascular-related events. Medication adherence may be an indicator of overall engagement in self-management or other healthy behaviors important for mitigating vulnerability to readmission after hospital discharge. It is well documented that persons who are more adherent to medications also tend to show better health outcomes. For example, Simpson and colleagues (2006) reported lower odds of mortality for good versus poor adherence to beneficial drug therapies (pooled odds ratio [OR] =0.55) and placebo (pooled OR=0.45) in a meta-analysis of 21 studies, suggesting that persons who adhere to medication may also be healthier in general or that adherence may be a surrogate for healthy behavior in general. Given the importance of health behaviors during transitions from hospitals to homes and given evidence that long-term medication adherence is associated with use of hospital services in some populations, we hypothesized that poorer long-term medication adherence may also be associated with higher risk for hospital readmission. The purpose of TABLE 1 Member characteristics and index hospitalization characteristics Variable N Percent Study sample 721 Gender Female % Male % Age Minimum 27 Mean 77 Maximum 98 Length of stay (days) Minimum 1 Mean 3.6 Maximum 77 Office visit within 30 days Yes % No % this retrospective cohort study was therefore to examine associations between long-term medication adherence and 30-day hospital readmission in a population of Medicare Cost Plan members in Central Texas. If poorer long-term medication adherence is associated with higher risk for readmission after hospital discharge, health care providers and systems may be able to leverage this information to better-target needed intervention to reduce readmissions. METHOD Study population. Members of Scott & White Health Plan SeniorCare, a Medicare Cost Plan, 1 were eligible for study inclusion if they met the following criteria: were hospitalized at least once in 2009; if at least 1 pharmacy claim for a chronic condition 1 A Medicare Cost Plan is a type of Medicare plan that provides full coverage (usually Part A and B, sometimes also Part D). Payment is based on reasonable cost of services. Beneficiaries are not restricted to a limited network of providers. medication (see Table 1) was available for the 12 months prior to the index hospitalization in 2009; if they were continuously enrolled in the product for the full study period; and if they were discharged to home after the initial hospital admission. A total of 1243 members were identified to have at least one hospitalization in the year 2009 with the discharge status of home. Forty-nine members, who had index hospitalization after Nov. 30, 2009, and no readmission before December 2009, were excluded to avoid selection bias from truncating the time available for readmission to less than 30 days. The sample of eligible members was This sample was further reduced to 721 after linking to pharmacy claims for prescription drug utilization during a 12-month period before the index hospitalization. The study protocol was reviewed and approved by the Scott & White Healthcare Institutional Review Board. Data sources. Electronic administrative claims data for pharmacy, inpatient services, and outpatient ser- 44 MANAGED CARE / JANUARY 2014
3 vices during the study period were extracted for each eligible member. Inpatient hospital admission for any reason was identified based on the presence of a facility claim for an inpatient hospital stay (Mapel 2011). Outpatient visits were identified by CPT codes (medical evaluation and management) for new and established patients. Variables. Member characteristics included gender and age. Characteristics of the first hospitalization in 2009 the index hospitalization included length of stay and discharge disposition (routine discharge to home). The outcome variable of interest was readmission within 30 days of the index discharge. Length of stay for the index hospitalization was calculated by the difference between the admission date and the discharge date for the index hospitalization. Office visits within 30 days of discharge from the index hospitalization were identified by a date of service within 30 calendar days of the index discharge date. Office visits were treated as dichotomous (Yes, visit within 30 days or No, no documented visit within 30 days). Medication adherence for the 12 months before the admission date for the index hospitalization was measured by the medication possession ratio (MPR), a well-accepted methodology to assess medication use with administrative pharmacy claims data (Hess 2006, Steiner 1997). MPR is a ratio from 0.0 (ie, lowest) to 1.0 (perfect adherence). Values were capped at 1.0. Adherence was considered low if the MPR was less than 0.5, medium if between 0.5 and 0.79, and high if TABLE 2 Medication adherence among members in the study sample (N=721) MPR (%) Low (<0.5) Medium ( ) High (0.8 1) greater than 0.8 (Balkrishnan 2003, Lau 2004, Psaty 2001, Wei 2002). MPR was calculated for 5 classes of medication relevant to management of common chronic illnesses: antidepressant, antihyperlipidemic, antiarrhythmic, antihypertensive, and diabetes medications. The drug categories were identified based on the American Hospital Formulary Service (AHFS) codes. Each individual drug within the AHFS category was identified based on the generic code number (GCN). MPR was calculated for medications with at least 2 pharmacy claims for the same GCN. For AHFS and GCN codes, see online version of this article at com/mc1401-adherence. MPR was calculated by determining the total number of numerator and denominator days in the 12 months prior to the index hospitalization. MPR was further categorized by different drugs taken by a particular patient during the study period. Drugs were grouped based on the generic product identifier (GPI) code, excluding the last 2 digits. Denominator days were calculated by the difference between prescription filled date and the date of first hospitalization for all prescription medications in different drug categories. Finally, the sum of the maximum number of denominator days for each drug group was calculated. Numerator days of supply were calculated in 2 steps. First, we identified the total number of days of prescription medication supplied (for which claims were filed during the analysis period) for each drug category and summed the total days supplied. Second, we subtracted the carryover days of supplied drugs that fell beyond the analysis period. This gave us the total number of numerator days. The MPR was calculated by dividing the total number of numerator days by the total number of denominator days. Dose changes were treated as continuation of therapy rather than a new medication. Among 1192 patients, pharmacy claims data were identified for 722 patients during the 12-month period prior to the index hospitalization in Therefore, our analysis includes 722 patients who experienced at least 1 inpatient hospitalization in 2009 and pharmacy claims 12 months prior to the index hospitalization. Statistical analysis. Member characteristics were tabulated or summarized by mean and range. The likelihood of 30-day rehospitalization was estimated using the logistic regression technique, where rehospitalization status within 30 days was a function of age, gender, length of stay at the first hospitalization, office visits within 30 calendar days of the discharge date for the index hospitalization. Analyses were performed in SAS 9.2 (SAS Institute, Cary, NC). P values <.05 were considered statistically significant. RESULTS Table 1 shows study sample characteristics. The average age was 76 (range: years). Sixty-five percent of the sample was female. The average length of stay for the index hospitalization was 4 days (range 1 77 days). Approximately 85% of members attended an office visit within 30 days from the date of discharge from the index hospitalization. Table 2 presents the 12-month medication adherence for the study sample. About 14% of members had low medication adherence, about 30% had medium adherence, and 56% had high adherence based on MPR scores JANUARY 2014 / MANAGED CARE 45
4 prior to index hospitalization. The mean MPR was 0.78 (range ). Only 43 of 721 health plan members experienced a hospital readmission within 30 days of index hospital discharge. Table 3 shows the OR estimates for the likelihood of 30-day readmission estimated with logistic regression. Increased age (OR=1.07, P=.003) and longer length of stay for the index admission (OR=1.2, P<.001) were associated with higher likelihood of 30-day readmission. Compared with those who did not have an office visit within 30 days of the index discharge, the odds of 30- day readmission was lower for those with an office visit (OR=0.38, P=.03). Individuals with low medication adherence (MPR <0.5) were not more likely to experience 30-day readmission compared with those who had higher medication adherence (MPR >0.8). DISCUSSION Contrary to expectations, longterm medication adherence prior to the index hospitalization was not associated with likelihood of 30-day readmission in the study sample of members of a Medicare cost plan. Older age and longer length of stay were associated with higher likelihood of readmission; follow-up office visit was associated with lower likelihood of readmission. Limitations. The study sample may not be representative of all Medicare populations. Because of limitations in the available dataset, we are unable to provide detailed characteristics of the sample to include income, race/ ethnicity, marital status, and other variables that may be associated with health and health behaviors. Overall long-term medication adherence was relatively high (mean = -.78) and only 14% of the sample had low adherence based on MPR scores. In addition, the 30-day readmission rate for the group was low relative to general Medicare TABLE 3 Logistic regression model for 30-day readmission after index hospitalization in Day Readmission Parameter Odds Ratio 95% CI P-Value Age <.003 Office visits Length of stay <.001 MPR-low samples (Jencks 2009). Administrative claims data only capture information reported by providers to the cost plan payer. Pharmacy claims may miss prescriptions filled at pharmacies that do not submit claims to this payer (eg, self-paid prescription fills). The MPR measure of adherence does not capture whether members actually take medications as prescribed, but the measure has been validated and is a well-accepted method of capturing adherence (Andrade 2006, Steiner 1997). Medication errors are a wellknown contributor to safety risks and readmission following hospital discharge (Coleman 2005, Forster 2003, Marcum 2010). This study does not address how members adhered to medications in the weeks following discharge. In this study we selected classes of drugs commonly used for long-term treatment of chronic conditions. It is possible that adherence calculated on only the selected categories did not fully represent individuals long-term adherence behaviors. CONCLUSION Reducing hospital readmissions is a national health care priority. Interventions are available to help address patient needs in the time following hospital discharge, but these interventions require resources. Efficient use of those resources may be enhanced by successful identification of patient characteristics or behaviors that predict risk for readmission. To date, many of the variables that have been associated with readmission may be difficult or impossible for inpatient clinicians to easily identify before hospital discharge. For example, length of stay and attending a post-discharge office visit were associated with readmission in this study but these variables obviously are not available to clinicians who begin planning for hospital discharge arrangements early in a hospital stay (because at this point the length of stay has yet to be determined and the post-office visit has not yet occurred). In this study, long-term medication adherence was not a predictor of readmission for a sample that was relatively adherent to medications before admission and may have been generally prepared for post-discharge challenges. Additional work is needed to identify indicators of readmission risk that can be utilized during hospitalization to identify patients needing post-discharge support to help prevent readmission. REFERENCES Ali RC, Melloni C, Ou FS, Schmader K, Ohman EM, Roe MT, et al. Age and persistent use of cardiovascular medication after acute coronary syndrome: results from medication applied and sustained over time. J Am Geriatr Soc. 2009;57(11): Amin AP, Mukhopadhyay E, Nathan S, Napan S, Kelly RF. Association of medical noncompliance and longterm adverse outcomes, after myocardial infarction in a minority and 46 MANAGED CARE / JANUARY 2014
5 uninsured population. Transl Res. 2009;154(2): Andrade SE, Kahler KH, Frech F, Chan KA. Methods for evaluation of medication adherence and persistence using automated databases. Pharmacoepidemiol Drug Saf. 2006;15(8): ; discussion Balkrishnan R, Rajagopalan R, Camacho FT, Huston SA, Murray FT, Anderson RT. Predictors of medication adherence and associated health care costs in an older population with type 2 diabetes mellitus: a longitudinal cohort study. Clin Ther. 2003;25(11): Boling PA. Care transitions and home health care. Clin Geriatr Med. 2009;25(1): , viii. Coleman EA, Parry C, Chalmers S, Min SJ. The care transitions intervention: results of a randomized controlled trial. Arch Intern Med. 2006;166(17): Coleman E, Smith JD, Raha D, Min SJ. Posthospital medication discrepancies: Prevalence and contributing factors. Arch Intern Med. 2005;165: Forster AJ, Murff HJ, Peterson JF, Gandhi TK, Bates DW. The incidence and severity of adverse events affecting patients after discharge from the hospital. Ann Intern Med. 2003;138(3): Harrison MB, Browne GB, Roberts J, Tugwell P, Gafni A, Graham ID. Quality of life of individuals with heart failure: a randomized trial of the effectiveness of two models of hospital-to-home transition. Med Care. 2002;40(4): Hess LM, Raebel MA, Conner DA, Malone DC. Measurement of adherence in pharmacy administrative databases: a proposal for standard definitions and preferred measures. Ann Pharmacother. 2006;40(7 8): Jencks SF, Williams MV, Coleman EA. Rehospitalizations among patients in the Medicare fee-for-service program. N Engl J Med. 2009;360(14): Lau DT, Nau DP. Oral antihyperglycemic medication nonadherence and subsequent hospitalization among individuals with type 2 diabetes. Diabetes Care. 2004;27(9): Li H, Morrow-Howell N, Proctor EK. Postacute home care and hospital readmission of elderly patients with congestive heart failure. Health Soc Work. 2004;29(4): Mapel DW, Dutro MP, Marton JP, Woodruff K, Make B. Identifying and characterizing COPD patients in US managed care. A retrospective, crosssectional analysis of administrative claims data. BMC Health Serv Res. 2011;11:43. Marcum ZA, Handler SM, Boyce R, Gellad W, Hanlon JT. Medication misadventures in the elderly: a year in review. Am J Geriatr Pharmacother. 2010;8(1): Naylor MD, Brooten D, Campbell R, Jacobsen BS, Mezey MD, Pauly MV, et al. Comprehensive discharge planning and home follow-up of hospitalized elders. JAMA. 1999;281(7): Ouslander JG, Perloe M, Givens JH, Kluge L, Rutland T, Lamb G. Reducing potentially avoidable hospitalizations of nursing home residents: results of a pilot quality improvement project. J Am Med Dir Assoc. 2009;10(9): Parry C, Min SJ, Chugh A, Chalmers S, Coleman EA. Further application of the care transitions intervention: results of a randomized controlled trial conducted in a fee-for-service setting. Home Health Care Serv Q. 2009;28(2 3): Psaty BM, Furberg CD, Kuller LH, Cushman M, Savage PJ, Levine D et al. Association between blood pressure level and the risk of myocardial infarction, stroke, and total mortality: the cardiovascular health study. Arch Intern Med. 2001;161(9): Pittman DG, Tao Z, Chen W, Stettin GD. Antihypertensive medication adherence and subsequent healthcare utilization and costs. Am J Manag Care. 2010;16(8): Ross JS, Chen J, Lin Z, Bueno H, Curtis JP, Keenan PS, et al. Recent national trends in readmission rates after heart failure hospitalization. Circ Heart Fail. 2009;3(1): Simpson SH, Eurich DT, Majumdar SR, et al. A meta-analysis of the association between adherence to drug therapy and mortality. BMJ. 2006;333(7557):15. Steiner JF, Prochazka AV. The assessment of refill compliance using pharmacy records: methods, validity, and applications. J Clin Epidemiol. 1997;50(1): Tsilimingras D, Bates DW. Addressing postdischarge adverse events: a neglected area. Jt Comm J Qual Patient Saf. 2008;34(2): Wei L, Wang J, Thompson P, Wong S, Struthers AD, MacDonald TM. Adherence to statin treatment and readmission of patients after myocardial infarction: a six year follow up study. Heart. 2002;88(3): JANUARY 2014 / MANAGED CARE 47
CHF Longitudinal Workgroup. Addressing readmissions from SNFs and other PAC settings 3/2/17
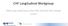 CHF Longitudinal Workgroup Addressing readmissions from SNFs and other PAC settings 3/2/17 Readmission Rate (%) Readmission Rate from SNF by Hospital (CHF) 16 14 13.6% 12 10 8 6 4 2 0 Mean = 6.3% 0% 0
CHF Longitudinal Workgroup Addressing readmissions from SNFs and other PAC settings 3/2/17 Readmission Rate (%) Readmission Rate from SNF by Hospital (CHF) 16 14 13.6% 12 10 8 6 4 2 0 Mean = 6.3% 0% 0
Robyn Tamblyn, BSCN MSc PhD May 2 nd, 2018 Baldwin Seminar Series Accreditation Council for Graduate Medical Education
 Robyn Tamblyn, BSCN MSc PhD May 2 nd, 2018 Baldwin Seminar Series Accreditation Council for Graduate Medical Education Robyn Tamblyn, BScN, MSc, PhD, CM Disclosure None of the above speakers have any conflicts
Robyn Tamblyn, BSCN MSc PhD May 2 nd, 2018 Baldwin Seminar Series Accreditation Council for Graduate Medical Education Robyn Tamblyn, BScN, MSc, PhD, CM Disclosure None of the above speakers have any conflicts
The PREDICT Trial. Prediction using a Randomized Evaluation of Data collection Integrated through Connected Technologies
 The PREDICT Trial Prediction using a Randomized Evaluation of Data collection Integrated through Connected Technologies Ogochukwu Ufio Advisors: Mitesh Patel MD, MBA, MS Caroline Carney, BA Table of Contents
The PREDICT Trial Prediction using a Randomized Evaluation of Data collection Integrated through Connected Technologies Ogochukwu Ufio Advisors: Mitesh Patel MD, MBA, MS Caroline Carney, BA Table of Contents
By 2030, the number of seniors in the United States
 Patient Characteristics and Medication Burden Affect Adherence Among Seniors Drug Trends R. Scott Leslie, MPH; Sara C. Erickson, PharmD; and Bimal V. Patel, PharmD, MS By 2030, the number of seniors in
Patient Characteristics and Medication Burden Affect Adherence Among Seniors Drug Trends R. Scott Leslie, MPH; Sara C. Erickson, PharmD; and Bimal V. Patel, PharmD, MS By 2030, the number of seniors in
H2H Early Follow-up Challenge: See You in 7. Webinar #1 Thursday, March 3, :00 pm 4:00 pm ET. Welcome
 H2H Early Follow-up Challenge: See You in 7 Webinar #1 Thursday, March 3, 2011 3:00 pm 4:00 pm ET 1 Welcome Take Home Messages Renew your H2H commitment Participate in the first H2H Challenge Help build
H2H Early Follow-up Challenge: See You in 7 Webinar #1 Thursday, March 3, 2011 3:00 pm 4:00 pm ET 1 Welcome Take Home Messages Renew your H2H commitment Participate in the first H2H Challenge Help build
Hospital Transition Management. Barbara Wood, BSN, MBA
 Hospital Transition Management Barbara Wood, BSN, MBA Director, Embedded Care Management Programs OBJECTIVES Improve health care quality for our patients by streamlining care transitions Reduce avoidable
Hospital Transition Management Barbara Wood, BSN, MBA Director, Embedded Care Management Programs OBJECTIVES Improve health care quality for our patients by streamlining care transitions Reduce avoidable
Do Elderly Men Have Increased Mortality Following Hip Fracture?
 Do Elderly Men Have Increased Mortality Following Hip Fracture? Excess Mortality in Men Compared With Women Following a Hip Fracture. National Analysis of Comedications, Comorbidity and Survival. Kannegaard
Do Elderly Men Have Increased Mortality Following Hip Fracture? Excess Mortality in Men Compared With Women Following a Hip Fracture. National Analysis of Comedications, Comorbidity and Survival. Kannegaard
METHODS RESULTS. Supported by funding from Ortho-McNeil Janssen Scientific Affairs, LLC
 PREDICTORS OF MEDICATION ADHERENCE AMONG PATIENTS WITH SCHIZOPHRENIC DISORDERS TREATED WITH TYPICAL AND ATYPICAL ANTIPSYCHOTICS IN A LARGE STATE MEDICAID PROGRAM S.P. Lee 1 ; K. Lang 2 ; J. Jackel 2 ;
PREDICTORS OF MEDICATION ADHERENCE AMONG PATIENTS WITH SCHIZOPHRENIC DISORDERS TREATED WITH TYPICAL AND ATYPICAL ANTIPSYCHOTICS IN A LARGE STATE MEDICAID PROGRAM S.P. Lee 1 ; K. Lang 2 ; J. Jackel 2 ;
HEALTH CARE EXPENDITURES ASSOCIATED WITH PERSISTENT EMERGENCY DEPARTMENT USE: A MULTI-STATE ANALYSIS OF MEDICAID BENEFICIARIES
 HEALTH CARE EXPENDITURES ASSOCIATED WITH PERSISTENT EMERGENCY DEPARTMENT USE: A MULTI-STATE ANALYSIS OF MEDICAID BENEFICIARIES Presented by Parul Agarwal, PhD MPH 1,2 Thomas K Bias, PhD 3 Usha Sambamoorthi,
HEALTH CARE EXPENDITURES ASSOCIATED WITH PERSISTENT EMERGENCY DEPARTMENT USE: A MULTI-STATE ANALYSIS OF MEDICAID BENEFICIARIES Presented by Parul Agarwal, PhD MPH 1,2 Thomas K Bias, PhD 3 Usha Sambamoorthi,
Unplanned 30-Day Readmissions in Orthopaedic Trauma
 Unplanned 30-Day Readmissions in Orthopaedic Trauma Introduction: 30-day readmission is increasingly used as a hospital quality metric. The objective of this study was to describe the patient factors associated
Unplanned 30-Day Readmissions in Orthopaedic Trauma Introduction: 30-day readmission is increasingly used as a hospital quality metric. The objective of this study was to describe the patient factors associated
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Improving Medication Adherence through Collaboration between Colleges of Pharmacy and Community Pharmacies
 Improving Medication Adherence through Collaboration between Colleges of Pharmacy and Community Pharmacies Megan Willson, PharmD, BCPS; Catrina Schwartz, PharmD, BS; Jennifer Robinson, PharmD Spokane,
Improving Medication Adherence through Collaboration between Colleges of Pharmacy and Community Pharmacies Megan Willson, PharmD, BCPS; Catrina Schwartz, PharmD, BS; Jennifer Robinson, PharmD Spokane,
ARIC Manuscript Proposal #2493. PC Reviewed: 2/10/15 Status: A Priority: 2 SC Reviewed: Status: Priority:
 ARIC Manuscript Proposal #2493 PC Reviewed: 2/10/15 Status: A Priority: 2 SC Reviewed: Status: Priority: 1. a. Full Title: Potentially inappropriate medication use in older people: Prevalence and outcomes.
ARIC Manuscript Proposal #2493 PC Reviewed: 2/10/15 Status: A Priority: 2 SC Reviewed: Status: Priority: 1. a. Full Title: Potentially inappropriate medication use in older people: Prevalence and outcomes.
Payers continue to search for effective ways to control
 At a Glance Practical Implications p 218 Author Information p 221 Full text and PDF www.ajpblive.com Value-Based Benefit Design and Healthcare Utilization in Asthma, Hypertension, and Diabetes Benefit
At a Glance Practical Implications p 218 Author Information p 221 Full text and PDF www.ajpblive.com Value-Based Benefit Design and Healthcare Utilization in Asthma, Hypertension, and Diabetes Benefit
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
The University of Mississippi School of Pharmacy
 LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
The Effect of Statin Therapy on Risk of Intracranial Hemorrhage
 The Effect of Statin Therapy on Risk of Intracranial Hemorrhage JENNIFER HANIFY, PHARM.D. PGY2 CRITICAL CARE RESIDENT UF HEALTH JACKSONVILLE JANUARY 23 RD 2016 Objectives Review benefits of statin therapy
The Effect of Statin Therapy on Risk of Intracranial Hemorrhage JENNIFER HANIFY, PHARM.D. PGY2 CRITICAL CARE RESIDENT UF HEALTH JACKSONVILLE JANUARY 23 RD 2016 Objectives Review benefits of statin therapy
Changing Patterns in Medication Use with Increasing Probability of Death for Older Medicare Beneficiaries
 Changing Patterns in Medication Use with Increasing Probability of Death for Older Medicare Beneficiaries Thomas Shaffer, MHS; Linda Simoni-Wastila, PhD, Wendy Toler, PharmD, Bruce Stuart, PhD, and Jalpa
Changing Patterns in Medication Use with Increasing Probability of Death for Older Medicare Beneficiaries Thomas Shaffer, MHS; Linda Simoni-Wastila, PhD, Wendy Toler, PharmD, Bruce Stuart, PhD, and Jalpa
GSK Medicine: Study Number: Title: Rationale: Study Period: Objectives: Indication: Study Investigators/Centers: Research Methods: Data Source
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
LAIs and the Challenge of Medication Non-Adherence The Care Transitions Network
 LAIs and the Challenge of Medication Non-Adherence The Care Transitions Network Lauren Hanna, M.D. The Zucker Hillside Hospital Northwell Health National Council for Behavioral Health Montefiore Medical
LAIs and the Challenge of Medication Non-Adherence The Care Transitions Network Lauren Hanna, M.D. The Zucker Hillside Hospital Northwell Health National Council for Behavioral Health Montefiore Medical
CLINICAL. Determinants of Compliance With Statin Therapy and Low-Density Lipoprotein Cholesterol Goal Attainment in a Managed Care Population
 Determinants of Compliance With Statin Therapy and Low-Density Lipoprotein Cholesterol Goal Attainment in a Managed Care Population Jennifer S. Schultz, PhD; John C. O Donnell, PhD; Ken L. McDonough, MD;
Determinants of Compliance With Statin Therapy and Low-Density Lipoprotein Cholesterol Goal Attainment in a Managed Care Population Jennifer S. Schultz, PhD; John C. O Donnell, PhD; Ken L. McDonough, MD;
Using claims data to investigate RT use at the end of life. B. Ashleigh Guadagnolo, MD, MPH Associate Professor M.D. Anderson Cancer Center
 Using claims data to investigate RT use at the end of life B. Ashleigh Guadagnolo, MD, MPH Associate Professor M.D. Anderson Cancer Center Background 25% of Medicare budget spent on the last year of life.
Using claims data to investigate RT use at the end of life B. Ashleigh Guadagnolo, MD, MPH Associate Professor M.D. Anderson Cancer Center Background 25% of Medicare budget spent on the last year of life.
outcome measures were adherence, medication possession ratio (MPR), persistence, prescription count, and duration of therapy.
 ORIGINAL RESEARCH Patient Adherence with HMG Reductase Inhibitor Therapy among Users of Two Types of Prescription Services by T. Jeffrey White, Pharm.D., M.S., Eunice Chang, Ph.D., Scott Leslie, M.P.H.,
ORIGINAL RESEARCH Patient Adherence with HMG Reductase Inhibitor Therapy among Users of Two Types of Prescription Services by T. Jeffrey White, Pharm.D., M.S., Eunice Chang, Ph.D., Scott Leslie, M.P.H.,
4/26/2016 DISCLOSURES BACKGROUND OBJECTIVES BACKGROUND BACKGROUND
 http://thinkprogress.org/health/01/10//1061/how-rising-health-care-costs-impact-the-national-budget/ http://www.firstaidforfree.com/wp-content/uploads/015/09/falls.jpg http://drwills.com/wp-content/uploads/015/05/drugcycle.jpg
http://thinkprogress.org/health/01/10//1061/how-rising-health-care-costs-impact-the-national-budget/ http://www.firstaidforfree.com/wp-content/uploads/015/09/falls.jpg http://drwills.com/wp-content/uploads/015/05/drugcycle.jpg
Getting Hypertension Under Control
 Getting Hypertension Under Control Learning Objectives EXPLAIN the factors involved in patient medication non-adherence. OUTLINE the results of studies focusing on medication adherence issues in patients
Getting Hypertension Under Control Learning Objectives EXPLAIN the factors involved in patient medication non-adherence. OUTLINE the results of studies focusing on medication adherence issues in patients
Performance Outcomes: Measure & Metric Details
 Performance Outcomes: Measure & Metric Details Adherence to Antipsychotic Medications for People with Schizophrenia Numerator: Number of people who remained on an antipsychotic for at least 80% of their
Performance Outcomes: Measure & Metric Details Adherence to Antipsychotic Medications for People with Schizophrenia Numerator: Number of people who remained on an antipsychotic for at least 80% of their
Parental Perception of Quality of Hospital Care for Children with Sickle Cell Disease
 Parental Perception of Quality of Hospital Care for Children with Sickle Cell Disease Jared Kam, BS; Julie A. Panepinto, MD, MSPH; Amanda M. Brandow, DO; David C. Brousseau, MD, MS Abstract Problem Considered:
Parental Perception of Quality of Hospital Care for Children with Sickle Cell Disease Jared Kam, BS; Julie A. Panepinto, MD, MSPH; Amanda M. Brandow, DO; David C. Brousseau, MD, MS Abstract Problem Considered:
Patient Safety in Older Adults
 Patient Safety in Older Adults Scott Martin Vouri, PharmD, MSCI, BCPS, BCGP, FASCP St. Louis College of Pharmacy Faculty Disclosure Dr. Vouri is funded by the Washington University Institute of Clinical
Patient Safety in Older Adults Scott Martin Vouri, PharmD, MSCI, BCPS, BCGP, FASCP St. Louis College of Pharmacy Faculty Disclosure Dr. Vouri is funded by the Washington University Institute of Clinical
Patient Safety in Older Adults
 Patient Safety in Older Adults Scott Martin Vouri, PharmD, MSCI, BCPS, BCGP, FASCP St. Louis College of Pharmacy Faculty Disclosure Dr. Vouri is funded by the Washington University Institute of Clinical
Patient Safety in Older Adults Scott Martin Vouri, PharmD, MSCI, BCPS, BCGP, FASCP St. Louis College of Pharmacy Faculty Disclosure Dr. Vouri is funded by the Washington University Institute of Clinical
Role of Pharmacoepidemiology in Drug Evaluation
 Role of Pharmacoepidemiology in Drug Evaluation Martin Wong MD, MPH School of Public Health and Primary Care Faculty of Medicine Chinese University of Hog Kong Outline of Content Introduction: what is
Role of Pharmacoepidemiology in Drug Evaluation Martin Wong MD, MPH School of Public Health and Primary Care Faculty of Medicine Chinese University of Hog Kong Outline of Content Introduction: what is
PDE File Medication Utilization; Medication Possession Ratio. Kyoungrae Jung, Ph.D. Assistant Professor Penn State University
 PDE File Medication Utilization; Medication Possession Ratio Kyoungrae Jung, Ph.D. Assistant Professor Penn State University Outline PDE variables related to medication utilization Measures of medication
PDE File Medication Utilization; Medication Possession Ratio Kyoungrae Jung, Ph.D. Assistant Professor Penn State University Outline PDE variables related to medication utilization Measures of medication
The Healthy User Effect: Ubiquitous and Uncontrollable S. R. Majumdar, MD MPH FRCPC FACP
 The Healthy User Effect: Ubiquitous and Uncontrollable S. R. Majumdar, MD MPH FRCPC FACP Professor of Medicine, Endowed Chair in Patient Health Management, Health Scholar of the Alberta Heritage Foundation,
The Healthy User Effect: Ubiquitous and Uncontrollable S. R. Majumdar, MD MPH FRCPC FACP Professor of Medicine, Endowed Chair in Patient Health Management, Health Scholar of the Alberta Heritage Foundation,
Murthy Gokula MD,CMD
 Murthy Gokula MD,CMD MEDICATIONS & LIFE EXPECTANCY DON T ROUTINELY PRESCRIBE LIPID-LOWERING MEDICATIONS IN INDIVIDUALS WITH A LIMITED LIFE EXPECTANCY: AAHPM About Choosing Wisely First conceived by the
Murthy Gokula MD,CMD MEDICATIONS & LIFE EXPECTANCY DON T ROUTINELY PRESCRIBE LIPID-LOWERING MEDICATIONS IN INDIVIDUALS WITH A LIMITED LIFE EXPECTANCY: AAHPM About Choosing Wisely First conceived by the
Quality Outcomes and Financial Benefits of Nutrition Intervention. Tracy R. Smith, PhD, RD, LD Senior Clinical Manager, Abbott Nutrition
 Quality Outcomes and Financial Benefits of Nutrition Intervention Tracy R. Smith, PhD, RD, LD Senior Clinical Manager, Abbott Nutrition January 28, 2016 SHIFTING MARKET DYNAMICS PROVIDE AN OPPORTUNITY
Quality Outcomes and Financial Benefits of Nutrition Intervention Tracy R. Smith, PhD, RD, LD Senior Clinical Manager, Abbott Nutrition January 28, 2016 SHIFTING MARKET DYNAMICS PROVIDE AN OPPORTUNITY
Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications
 MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
Improving Adherence to Chronic Medications: The Physicians Role and How 340b Can Help
 Improving Adherence to Chronic Medications: The Physicians Role and How 340b Can Help William Shrank MD MSHS Division of Pharmacoepidemiology & Pharmacoeconomics Harvard Medical School wshrank@partners.org
Improving Adherence to Chronic Medications: The Physicians Role and How 340b Can Help William Shrank MD MSHS Division of Pharmacoepidemiology & Pharmacoeconomics Harvard Medical School wshrank@partners.org
Cost-Motivated Treatment Changes in Commercial Claims:
 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non- Medical Switching August 2017 THE MORAN COMPANY 1 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non-Medical
Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non- Medical Switching August 2017 THE MORAN COMPANY 1 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non-Medical
Follow this and additional works at:
 The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2013 Factors associated with primary medication nonadherence and its effect on health service utilization among
The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2013 Factors associated with primary medication nonadherence and its effect on health service utilization among
SUPPLEMENTARY DATA. Supplementary Figure S1. Search terms*
 Supplementary Figure S1. Search terms* *mh = exploded MeSH: Medical subject heading (Medline medical index term); tw = text word; pt = publication type; the asterisk (*) stands for any character(s) #1:
Supplementary Figure S1. Search terms* *mh = exploded MeSH: Medical subject heading (Medline medical index term); tw = text word; pt = publication type; the asterisk (*) stands for any character(s) #1:
Adherence to therapy. Kamlesh Khunti University of Leicester, UK. William Polonsky University of California San Diego, USA
 Adherence to therapy Kamlesh Khunti University of Leicester, UK William Polonsky University of California San Diego, USA 1 Dualities of interest Kamlesh Khunti: Honoraria for speaking, advising or research
Adherence to therapy Kamlesh Khunti University of Leicester, UK William Polonsky University of California San Diego, USA 1 Dualities of interest Kamlesh Khunti: Honoraria for speaking, advising or research
A Prospective Comparison of Two Commercially Available Hospital Admission Risk Scores
 A Prospective Comparison of Two Commercially Available Hospital Admission Risk Scores Dale Eric Green, MD MHA FCCP: Chief Medical Information Officer, Cornerstone Health Care AMGA April, 2014 Disclosure
A Prospective Comparison of Two Commercially Available Hospital Admission Risk Scores Dale Eric Green, MD MHA FCCP: Chief Medical Information Officer, Cornerstone Health Care AMGA April, 2014 Disclosure
Background. Background. Background 3/14/2014. Conflict of Interest Statement:
 Platform Presentations Comparison of zolpidem to other drugs associated with falls in hospitalized patients Ed Rainville, MSPharm. Conflict of Interest Statement: The speaker has no conflict of interest
Platform Presentations Comparison of zolpidem to other drugs associated with falls in hospitalized patients Ed Rainville, MSPharm. Conflict of Interest Statement: The speaker has no conflict of interest
Real World Patients: The Intersection of Real World Evidence and Episode of Care Analytics
 PharmaSUG 2018 - Paper RW-05 Real World Patients: The Intersection of Real World Evidence and Episode of Care Analytics David Olaleye and Youngjin Park, SAS Institute Inc. ABSTRACT SAS Institute recently
PharmaSUG 2018 - Paper RW-05 Real World Patients: The Intersection of Real World Evidence and Episode of Care Analytics David Olaleye and Youngjin Park, SAS Institute Inc. ABSTRACT SAS Institute recently
Apurba Chakraborty MBBS, MPH Dima M. Qato PharmD, MPH, PhD Professor Mark S. Dworkin MD, MPHTM The University of Illinois at Chicago
 Less is More: The Impact of Lower Pill Burden on Adherence to Antiretroviral Therapy among Treatment-Naive Patients with HIV Infection in the United States Apurba Chakraborty MBBS, MPH Dima M. Qato PharmD,
Less is More: The Impact of Lower Pill Burden on Adherence to Antiretroviral Therapy among Treatment-Naive Patients with HIV Infection in the United States Apurba Chakraborty MBBS, MPH Dima M. Qato PharmD,
Impact of hospitalization on medication adherence estimation in claims data
 Received: 23 December 2016 Accepted: 15 February 2017 DOI: 10.1111/jcpt.12517 ORIGINAL ARTICLE Impact of hospitalization on medication adherence estimation in claims data Y.-H. Dong PhD 1,2,3 N. K. Choudhry
Received: 23 December 2016 Accepted: 15 February 2017 DOI: 10.1111/jcpt.12517 ORIGINAL ARTICLE Impact of hospitalization on medication adherence estimation in claims data Y.-H. Dong PhD 1,2,3 N. K. Choudhry
Chapter 2: Identification and Care of Patients With CKD
 Chapter 2: Identification and Care of Patients With Over half of patients from the Medicare 5% sample (restricted to age 65 and older) have a diagnosis of chronic kidney disease (), cardiovascular disease,
Chapter 2: Identification and Care of Patients With Over half of patients from the Medicare 5% sample (restricted to age 65 and older) have a diagnosis of chronic kidney disease (), cardiovascular disease,
Changes for Physician Measurement 2018
 Changes for Physician Measurement 2018 Measure Name Guidelines for Physician Measurement Effectiveness of Care Changes Revised the Systematic Sampling Methodology to require organizations to report using
Changes for Physician Measurement 2018 Measure Name Guidelines for Physician Measurement Effectiveness of Care Changes Revised the Systematic Sampling Methodology to require organizations to report using
Supplementary Online Content
 Supplementary Online Content Lee JS, Nsa W, Hausmann LRM, et al. Quality of care for elderly patients hospitalized for pneumonia in the United States, 2006 to 2010. JAMA Intern Med. Published online September
Supplementary Online Content Lee JS, Nsa W, Hausmann LRM, et al. Quality of care for elderly patients hospitalized for pneumonia in the United States, 2006 to 2010. JAMA Intern Med. Published online September
Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report. User s Guide Sixth Edition. Prepared by
 Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report User s Guide Sixth Edition Prepared by Partial Hospitalization Program Program for Evaluating Payment Patterns
Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report User s Guide Sixth Edition Prepared by Partial Hospitalization Program Program for Evaluating Payment Patterns
Preventing 30-Day Rehospitalization Among Elderly Patients: Special Focus on a Primary Care NP-Led Transition of Care Intervention
 Preventing 30-Day Rehospitalization Among Elderly Patients: Special Focus on a Primary Care NP-Led Transition of Care Intervention Katie S. Wingate, DNP, AGNP-C 2017 NPSS Asheville, NC Presentation Outline
Preventing 30-Day Rehospitalization Among Elderly Patients: Special Focus on a Primary Care NP-Led Transition of Care Intervention Katie S. Wingate, DNP, AGNP-C 2017 NPSS Asheville, NC Presentation Outline
A Systematic Review of Barriers to Medication Adherence in the Elderly: Looking Beyond Cost and Regimen Complexity
 W.F. Gellad et al. The American Journal of Geriatric Pharmacotherapy A Systematic Review of Barriers to Medication Adherence in the Elderly: Looking Beyond Cost and Regimen Complexity Walid F. Gellad,
W.F. Gellad et al. The American Journal of Geriatric Pharmacotherapy A Systematic Review of Barriers to Medication Adherence in the Elderly: Looking Beyond Cost and Regimen Complexity Walid F. Gellad,
Patient Navigator Program: Focus MI Diplomat Hospital Metrics
 Patient Navigator Program: Focus MI Diplomat Hospital Metrics Goal Statement: To reduce avoidable hospital readmissions for patients discharged with acute myocardial infarction (AMI) by supporting a culture
Patient Navigator Program: Focus MI Diplomat Hospital Metrics Goal Statement: To reduce avoidable hospital readmissions for patients discharged with acute myocardial infarction (AMI) by supporting a culture
Predictors of Rehospitalization After Admission for Pneumonia in the Veterans Affairs Healthcare System
 ORIGINAL RESEARCH Predictors of Rehospitalization After Admission for Pneumonia in the Veterans Affairs Healthcare System Victoria L. Tang, MD 1,2, Ethan A. Halm, MD, MPH 2, Michael J. Fine, MD, MSc 3,
ORIGINAL RESEARCH Predictors of Rehospitalization After Admission for Pneumonia in the Veterans Affairs Healthcare System Victoria L. Tang, MD 1,2, Ethan A. Halm, MD, MPH 2, Michael J. Fine, MD, MSc 3,
Hospice and Palliative Care: Value-Based Care Near the End of Life
 Hospice and Palliative Care: Value-Based Care Near the End of Life Mary Dittrich, MD, FASN Senior Medical Director, Remedy Partners Joseph W. Shega, MD National Medical Director, VITAS Healthcare 2017
Hospice and Palliative Care: Value-Based Care Near the End of Life Mary Dittrich, MD, FASN Senior Medical Director, Remedy Partners Joseph W. Shega, MD National Medical Director, VITAS Healthcare 2017
3/17/2017. Innovative Opportunities for Pharmacists in the Evolving World of Healthcare. Elderly represent about of our emergency medical services:
 Innovative Opportunities for Pharmacists in the Evolving World of Healthcare Christina Pornprasert, PharmD Population Health Clinical Pharmacist Hartford Healthcare Integrated Care Partners Addolorata
Innovative Opportunities for Pharmacists in the Evolving World of Healthcare Christina Pornprasert, PharmD Population Health Clinical Pharmacist Hartford Healthcare Integrated Care Partners Addolorata
Hospice and Palliative Care: Value-Based Care Near the End of Life
 Hospice and Palliative Care: Value-Based Care Near the End of Life Mary Dittrich, MD, FASN Senior Medical Director, Remedy Partners Joseph W. Shega, MD National Medical Director, VITAS Healthcare 2017
Hospice and Palliative Care: Value-Based Care Near the End of Life Mary Dittrich, MD, FASN Senior Medical Director, Remedy Partners Joseph W. Shega, MD National Medical Director, VITAS Healthcare 2017
SPECIAL ISSUE. Medicaid Prescription Drug Access Restrictions: Exploring the Effect on Patient Persistence With Hypertension Medications
 Medicaid Prescription Drug Access Restrictions: Exploring the Effect on Patient Persistence With Hypertension Medications Jerome Wilson, PhD; Kirsten Axelsen, MS; and Simon Tang, MPH Objective: To compare
Medicaid Prescription Drug Access Restrictions: Exploring the Effect on Patient Persistence With Hypertension Medications Jerome Wilson, PhD; Kirsten Axelsen, MS; and Simon Tang, MPH Objective: To compare
Innovative Opportunities for Pharmacists in the Evolving World of Healthcare
 Innovative Opportunities for Pharmacists in the Evolving World of Healthcare Christina Pornprasert, PharmD Population Health Clinical Pharmacist Hartford Healthcare Integrated Care Partners Assistant Clinical
Innovative Opportunities for Pharmacists in the Evolving World of Healthcare Christina Pornprasert, PharmD Population Health Clinical Pharmacist Hartford Healthcare Integrated Care Partners Assistant Clinical
DOES PROCESS QUALITY OF INPATIENT CARE MATTER IN POTENTIALLY PREVENTABLE READMISSION RATES?
 DOES PROCESS QUALITY OF INPATIENT CARE MATTER IN POTENTIALLY PREVENTABLE READMISSION RATES? A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Jae Young Choi,
DOES PROCESS QUALITY OF INPATIENT CARE MATTER IN POTENTIALLY PREVENTABLE READMISSION RATES? A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Jae Young Choi,
Improve the Adherence, Save the Life
 Improve the Adherence, Save the Life Park, Chang Gyu Korea University Guro Hospital Cardiovascular Center Seoul, Korea Modifiable CVD Risk Factors Obesity BMI Hypertension Cholesterol LDL HDL Diabetes
Improve the Adherence, Save the Life Park, Chang Gyu Korea University Guro Hospital Cardiovascular Center Seoul, Korea Modifiable CVD Risk Factors Obesity BMI Hypertension Cholesterol LDL HDL Diabetes
Using Evidence to Support Recovery through Comprehensive Community Services (CCS) Presentation Objectives. What is CCS? 10/17/2018
 Using Evidence to Support Recovery through Comprehensive Community Services (CCS) Chris Keenan and Tim Connor October 17, 2018 Presentation Objectives Understand the needs of CCS participants related to
Using Evidence to Support Recovery through Comprehensive Community Services (CCS) Chris Keenan and Tim Connor October 17, 2018 Presentation Objectives Understand the needs of CCS participants related to
The US Food and Drug Administration (FDA) requires that
 Prescriber Compliance With Black Box Warnings in Older Adult Patients Judith A. Ricci, ScD, MS; Charmaine Coulen, MPH; Jan E. Berger, MD, MJ; Marsha C. Moore, MD, MBA; Angela McQueen, PharmD; and Saira
Prescriber Compliance With Black Box Warnings in Older Adult Patients Judith A. Ricci, ScD, MS; Charmaine Coulen, MPH; Jan E. Berger, MD, MJ; Marsha C. Moore, MD, MBA; Angela McQueen, PharmD; and Saira
Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians
 Performance Measurement Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem, MD,
Performance Measurement Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem, MD,
The National Asthma Education and Prevention Program s
 Long-Acting b-agonist Among Children and Adults With Asthma Elizabeth A. Wasilevich, PhD, MPH; Sarah J. Clark, MPH; Lisa M. Cohn, MS; and Kevin J. Dombkowski, DrPH Managed Care & Healthcare Communications,
Long-Acting b-agonist Among Children and Adults With Asthma Elizabeth A. Wasilevich, PhD, MPH; Sarah J. Clark, MPH; Lisa M. Cohn, MS; and Kevin J. Dombkowski, DrPH Managed Care & Healthcare Communications,
Medication compliance, or. Partial Compliance and Risk of Rehospitalization Among California Medicaid Patients With Schizophrenia
 Partial Compliance and Risk of Rehospitalization Among California Medicaid Patients With Schizophrenia Peter J. Weiden, M.D. Chris Kozma, Ph.D. Amy Grogg, Pharm.D. Julie Locklear, Pharm.D., M.B.A. Objective:
Partial Compliance and Risk of Rehospitalization Among California Medicaid Patients With Schizophrenia Peter J. Weiden, M.D. Chris Kozma, Ph.D. Amy Grogg, Pharm.D. Julie Locklear, Pharm.D., M.B.A. Objective:
Bundled Payments in Orthopedic Trauma: How to Succeed
 SE 87 Bundled Payments in Orthopedic Trauma: How to Succeed Sanjit R. Konda MD Ariana Lott BA Kurtis Carlock BS Kenneth A. Egol MD Department of Orthopedic Surgery NYU Langone Orthopedic Hospital, New
SE 87 Bundled Payments in Orthopedic Trauma: How to Succeed Sanjit R. Konda MD Ariana Lott BA Kurtis Carlock BS Kenneth A. Egol MD Department of Orthopedic Surgery NYU Langone Orthopedic Hospital, New
1* 2 3. Hirva Bakeri, Dorothy Wakefield, Latha Dulipsingh. Department of Medicine, University of Connecticut Health Center, USA 2
 RESEARCH ARTICLE Is There a Role of Hemoglobin A1C in Predicting Hospital Re- Admission Rates for Patients with Diabetes? 1* 2 3 Hirva Bakeri, Dorothy Wakefield, Latha Dulipsingh 1 Department of Medicine,
RESEARCH ARTICLE Is There a Role of Hemoglobin A1C in Predicting Hospital Re- Admission Rates for Patients with Diabetes? 1* 2 3 Hirva Bakeri, Dorothy Wakefield, Latha Dulipsingh 1 Department of Medicine,
Chapter 6: Healthcare Expenditures for Persons with CKD
 Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
NON-ADHERENCE TO ADJUVANT HORMONAL TREATMENT IN EARLY BREAST CANCER
 NON-ADHERENCE TO ADJUVANT HORMONAL TREATMENT IN EARLY BREAST CANCER C. Volovat 1, C. Lupascu 2, Simona-Ruxandra Volovat 1, E. Zbranca 3 1. Center of Medical Oncology Iasi 2. I. Tanasescu Vl. Butureanu
NON-ADHERENCE TO ADJUVANT HORMONAL TREATMENT IN EARLY BREAST CANCER C. Volovat 1, C. Lupascu 2, Simona-Ruxandra Volovat 1, E. Zbranca 3 1. Center of Medical Oncology Iasi 2. I. Tanasescu Vl. Butureanu
Making the Business Case for Long-Acting Injectables
 Making the Business Case for Long-Acting Injectables David R. Swann, MA, LCAS, CCS, LPC, NCC Senior Healthcare Integration Consultant MTM Services Chief Clinical Officer Partners Behavioral Health Management
Making the Business Case for Long-Acting Injectables David R. Swann, MA, LCAS, CCS, LPC, NCC Senior Healthcare Integration Consultant MTM Services Chief Clinical Officer Partners Behavioral Health Management
Assessing Medication Adherence
 Assessing Medication Adherence Dr. Lauren Hanna and Dr. Delbert Robinson Northwell Health National Council for Behavioral Health Montefiore Medical Center Northwell Health New York State Office of Mental
Assessing Medication Adherence Dr. Lauren Hanna and Dr. Delbert Robinson Northwell Health National Council for Behavioral Health Montefiore Medical Center Northwell Health New York State Office of Mental
APPENDIX: Supplementary Materials for Advance Directives And Nursing. Home Stays Associated With Less Aggressive End-Of-Life Care For
 Nicholas LH, Bynum JPW, Iwashnya TJ, Weir DR, Langa KM. Advance directives and nursing home stays associated with less aggressive end-of-life care for patients with severe dementia. Health Aff (MIllwood).
Nicholas LH, Bynum JPW, Iwashnya TJ, Weir DR, Langa KM. Advance directives and nursing home stays associated with less aggressive end-of-life care for patients with severe dementia. Health Aff (MIllwood).
Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments
 Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments Prepared for: American Hospital Association April 4, 2019 Berna Demiralp,
Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments Prepared for: American Hospital Association April 4, 2019 Berna Demiralp,
Hospital Discharge Data
 Hospital Discharge Data West Virginia Health Care Authority Hospitalization data were obtained from the West Virginia Health Care Authority s (WVHCA) hospital discharge database. Data are submitted by
Hospital Discharge Data West Virginia Health Care Authority Hospitalization data were obtained from the West Virginia Health Care Authority s (WVHCA) hospital discharge database. Data are submitted by
Delayed or missed follow-up of laboratory tests is
 Reports from the field Follow-up of Abnormal Metanephrine and Catecholamine Testing: Chasing Missed Neuroendocrine Tumors Richard Zamore, MD, MPH, Beth Harubin, MS, Megan Sweeney, BS, and Saul N. Weingart,
Reports from the field Follow-up of Abnormal Metanephrine and Catecholamine Testing: Chasing Missed Neuroendocrine Tumors Richard Zamore, MD, MPH, Beth Harubin, MS, Megan Sweeney, BS, and Saul N. Weingart,
Study Exposures, Outcomes:
 GSK Medicine: Coreg IR, Coreg CR, and InnoPran Study No.: WWE111944/WEUSRTP3149 Title: A nested case-control study of the association between Coreg IR and Coreg CR and hypersensitivity reactions: anaphylactic
GSK Medicine: Coreg IR, Coreg CR, and InnoPran Study No.: WWE111944/WEUSRTP3149 Title: A nested case-control study of the association between Coreg IR and Coreg CR and hypersensitivity reactions: anaphylactic
had non-continuous enrolment in Medicare Part A or Part B during the year following initial admission;
 Effectiveness and cost-effectiveness of implantable cardioverter defibrillators in the treatment of ventricular arrhythmias among Medicare beneficiaries Weiss J P, Saynina O, McDonald K M, McClellan M
Effectiveness and cost-effectiveness of implantable cardioverter defibrillators in the treatment of ventricular arrhythmias among Medicare beneficiaries Weiss J P, Saynina O, McDonald K M, McClellan M
PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter
 Managing Performance Information in a Quality Driven World PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter REGULATORY UPDATE PQS Summary of Pharmacy/ Medication-Related
Managing Performance Information in a Quality Driven World PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter REGULATORY UPDATE PQS Summary of Pharmacy/ Medication-Related
Prospective Validation of Eight Different Adherence Measures for Use with Administrative Claims Data among Patients with Schizophreniavhe_
 Volume 12 Number 6 2009 VALUE IN HEALTH Prospective Validation of Eight Different Adherence Measures for Use with Administrative Claims Data among Patients with Schizophreniavhe_543 989..995 Sudeep Karve,
Volume 12 Number 6 2009 VALUE IN HEALTH Prospective Validation of Eight Different Adherence Measures for Use with Administrative Claims Data among Patients with Schizophreniavhe_543 989..995 Sudeep Karve,
eappendix A. Simulation study parameters
 eappendix A. Simulation study parameters Parameter type Notation Values or distributions Definition i {1 20} Indicator for each of 20 monitoring periods N i 500*i Number of exposed patients in each period,
eappendix A. Simulation study parameters Parameter type Notation Values or distributions Definition i {1 20} Indicator for each of 20 monitoring periods N i 500*i Number of exposed patients in each period,
Reducing the Risk of Stroke Associated With Nonvalvular Atrial Fibrillation in the VHA
 DECEMBER 21 VOL. 27 SUPPL. 1 A SUPPLEMENT TO www.fedprac.com Reducing the Risk of Stroke Associated With Nonvalvular Atrial Fibrillation in the VHA Diagnosing and Treating Atrial Fibrillation in the VHA
DECEMBER 21 VOL. 27 SUPPL. 1 A SUPPLEMENT TO www.fedprac.com Reducing the Risk of Stroke Associated With Nonvalvular Atrial Fibrillation in the VHA Diagnosing and Treating Atrial Fibrillation in the VHA
Asthma Disease Management Demonstration Project:
 Asthma Disease Management Demonstration Project: Using EMS Health Coaches May Decrease Emergency Department Revisits, Length of Hospital Admissions and Costs Michael T. Hilton, MD Jan 13, 2012 NAEMSP Annual
Asthma Disease Management Demonstration Project: Using EMS Health Coaches May Decrease Emergency Department Revisits, Length of Hospital Admissions and Costs Michael T. Hilton, MD Jan 13, 2012 NAEMSP Annual
ATRIAL FIBRILLATION AND ETHNICITY. Elsayed Z Soliman MD, MSc, MS Director, Epidemiological Cardiology Research Center (EPICARE)
 ATRIAL FIBRILLATION AND ETHNICITY Elsayed Z Soliman MD, MSc, MS Director, Epidemiological Cardiology Research Center (EPICARE) Atrial fibrillation (AF) and ethnicity The known The unknown The paradox Why
ATRIAL FIBRILLATION AND ETHNICITY Elsayed Z Soliman MD, MSc, MS Director, Epidemiological Cardiology Research Center (EPICARE) Atrial fibrillation (AF) and ethnicity The known The unknown The paradox Why
Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual
 Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual 2017 This document is a guide to the 2017 Arkansas Blue Cross and Blue Shield Patient-Centered Medical
Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual 2017 This document is a guide to the 2017 Arkansas Blue Cross and Blue Shield Patient-Centered Medical
COMMUNITY ONCOLOGY ALLIANCE YOU WON T BELIEVE WHAT CMS WILL BE REPORTING ON YOUR ONCOLOGISTS
 COMMUNITY ONCOLOGY ALLIANCE YOU WON T BELIEVE WHAT CMS WILL BE REPORTING ON YOUR ONCOLOGISTS Community Oncology Alliance 2 Physician Ratings Consumers want information about quality Have become used to
COMMUNITY ONCOLOGY ALLIANCE YOU WON T BELIEVE WHAT CMS WILL BE REPORTING ON YOUR ONCOLOGISTS Community Oncology Alliance 2 Physician Ratings Consumers want information about quality Have become used to
Antidepressant Use and Depressive Symptoms in Intensive Care Unit Survivors
 Antidepressant Use in ICU Survivors 1 Antidepressant Use and Depressive Symptoms in Intensive Care Unit Survivors Sophia Wang, MD, Chris Mosher, MD, Sujuan Gao, PhD, Kayla Kirk, MA, Sue Lasiter, PhD, RN,
Antidepressant Use in ICU Survivors 1 Antidepressant Use and Depressive Symptoms in Intensive Care Unit Survivors Sophia Wang, MD, Chris Mosher, MD, Sujuan Gao, PhD, Kayla Kirk, MA, Sue Lasiter, PhD, RN,
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Outcome High Priority
 Quality ID #355: Unplanned Reoperation within the 30 Day Postoperative Period National Quality Strategy Domain: Patient Safety Meaningful Measure Area: Admissions and Readmissions to Hospitals 2019 COLLECTION
Quality ID #355: Unplanned Reoperation within the 30 Day Postoperative Period National Quality Strategy Domain: Patient Safety Meaningful Measure Area: Admissions and Readmissions to Hospitals 2019 COLLECTION
REVIEW AND FREQUENTLY ASKED QUESTIONS (FAQ) 8/5/2015. Outline. Navigating the DSMT Reimbursement Maze in Todays Changing Environment
 Patty Telgener RN, MBA, CPC VP of Reimbursement Emerson Consultants Navigating the DSMT Reimbursement Maze in Todays Changing Environment Patty Telgener, RN, MBA, CPC VP of Reimbursement Emerson Consultants
Patty Telgener RN, MBA, CPC VP of Reimbursement Emerson Consultants Navigating the DSMT Reimbursement Maze in Todays Changing Environment Patty Telgener, RN, MBA, CPC VP of Reimbursement Emerson Consultants
Performance Analysis:
 Performance Analysis: Healthcare Utilization of CCNC- Population 2007-2010 Prepared by Treo Solutions JUNE 2012 Table of Contents SECTION ONE: EXECUTIVE SUMMARY 4-5 SECTION TWO: REPORT DETAILS 6 Inpatient
Performance Analysis: Healthcare Utilization of CCNC- Population 2007-2010 Prepared by Treo Solutions JUNE 2012 Table of Contents SECTION ONE: EXECUTIVE SUMMARY 4-5 SECTION TWO: REPORT DETAILS 6 Inpatient
Factors Affecting Use of Insulin Pens by Patients with Type 2 Diabetes
 Diabetes Care Publish Ahead of Print, published online November 26, 2007 Factors Affecting Use of Insulin Pens by Patients with Type 2 Diabetes Richard R. Rubin, PhD 1,2 Mark Peyrot, PhD 1,3 1= Department
Diabetes Care Publish Ahead of Print, published online November 26, 2007 Factors Affecting Use of Insulin Pens by Patients with Type 2 Diabetes Richard R. Rubin, PhD 1,2 Mark Peyrot, PhD 1,3 1= Department
SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES
 Summary Table of Measures, Product Lines and Changes 1 SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES General Guidelines for Data Collection and Reporting Guidelines for Calculations and Sampling
Summary Table of Measures, Product Lines and Changes 1 SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES General Guidelines for Data Collection and Reporting Guidelines for Calculations and Sampling
Functional status and social support network as risk factors for hospital readmission in Heart Failure
 Functional status and social support network as risk factors for hospital readmission in Heart Failure Sílvia Alexandra Duarte Centro Hospitalar de Trás os Montes e Alto Douro, Vila Real, Portugal CONFLICT
Functional status and social support network as risk factors for hospital readmission in Heart Failure Sílvia Alexandra Duarte Centro Hospitalar de Trás os Montes e Alto Douro, Vila Real, Portugal CONFLICT
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Chapter 2: Identification and Care of Patients With CKD
 Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Nonadherence to chronic medications contributes to
 BRIEF REPORT Pharmacy-based Interventions to Reduce Primary Medication Nonadherence to Cardiovascular Medications Michael A. Fischer, MD, MS,* Niteesh K. Choudhry, MD, PhD,* Katsiaryna Bykov, PharmD, MS,*
BRIEF REPORT Pharmacy-based Interventions to Reduce Primary Medication Nonadherence to Cardiovascular Medications Michael A. Fischer, MD, MS,* Niteesh K. Choudhry, MD, PhD,* Katsiaryna Bykov, PharmD, MS,*
medicaid and the The Role of Medicaid for People with Diabetes
 on medicaid and the uninsured The Role of for People with Diabetes November 2012 Introduction Diabetes is one of the most prevalent chronic conditions and a leading cause of death in the United States.
on medicaid and the uninsured The Role of for People with Diabetes November 2012 Introduction Diabetes is one of the most prevalent chronic conditions and a leading cause of death in the United States.
David Dosa MD, MPH Assistant Professor of Medicine and Community Health The Warren Alpert School of Medicine, Brown University Director, Primary Care
 David Dosa MD, MPH Assistant Professor of Medicine and Community Health The Warren Alpert School of Medicine, Brown University Director, Primary Care Geriatrics Clinic- Providence VAMC VA Grand Rounds
David Dosa MD, MPH Assistant Professor of Medicine and Community Health The Warren Alpert School of Medicine, Brown University Director, Primary Care Geriatrics Clinic- Providence VAMC VA Grand Rounds
DUPLICATION DISTRIBUTION PROHIBBITED AND. Utilizing Economic and Clinical Outcomes to Eliminate Health Disparities and Improve Health Equity
 General Session IV Utilizing Economic and Clinical Outcomes to Eliminate Health Disparities and Improve Health Equity Accreditation UAN 0024-0000-12-012-L04-P Participation in this activity earns 2.0 contact
General Session IV Utilizing Economic and Clinical Outcomes to Eliminate Health Disparities and Improve Health Equity Accreditation UAN 0024-0000-12-012-L04-P Participation in this activity earns 2.0 contact
Heart Attack Readmissions in Virginia
 Heart Attack Readmissions in Virginia Schroeder Center Statistical Brief Research by Mitchell Cole, William & Mary Public Policy, MPP Class of 2017 Highlights: In 2014, almost 11.2 percent of patients
Heart Attack Readmissions in Virginia Schroeder Center Statistical Brief Research by Mitchell Cole, William & Mary Public Policy, MPP Class of 2017 Highlights: In 2014, almost 11.2 percent of patients
Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach
 Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach Presented by Susan G. Haber, Sc.D 1 ; Boyd H. Gilman, Ph.D. 1 1 RTI International Presented at The 133rd Annual Meeting of
Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach Presented by Susan G. Haber, Sc.D 1 ; Boyd H. Gilman, Ph.D. 1 1 RTI International Presented at The 133rd Annual Meeting of
