Long-Term Results of a Multicenter Study on Subthalamic and Pallidal Stimulation in Parkinson s Disease
|
|
|
- Easter Harmon
- 6 years ago
- Views:
Transcription
1 Movement Disorders Vol. 25, No. 5, 2010, pp Ó 2010 Movement Disorder Society Long-Term Results of a Multicenter Study on Subthalamic and Pallidal Stimulation in Parkinson s Disease Elena Moro, MD, PhD, 1 * Andres M. Lozano, MD, PhD, 2 Pierre Pollak, MD, 3 Yves Agid, MD, 4 Stig Rehncrona, MD, 5 Jens Volkmann, MD, PhD, 6 Jaime Kulisevsky, MD, 7 Jose A. Obeso, MD, 8 Alberto Albanese, MD, PhD, 9,10 Marwan I. Hariz, MD, 11,12 Niall P. Quinn, MD, 11 Jans D. Speelman, MD, 13 Alim L. Benabid, MD, PhD, 3 Valerie Fraix, MD, 3 Alexandre Mendes, MD, 3 Marie-Laure Welter, MD, 4 Jean-Luc Houeto, MD, 4,14 Philippe Cornu, MD, 4 Didier Dormont, MD, 4 Annalena L. Tornqvist, RN, 5 Ron Ekberg, MD, 5 Alfons Schnitzler, MD, 15 Lars Timmermann, MD, 15,16 Lars Wojtecki, MD, 15 Andres Gironell, MD, 7 Maria C. Rodriguez-Oroz, MD, PhD, 8 Jorge Guridi, MD, 8 Anna R. Bentivoglio, MD, PhD, 10 Maria F. Contarino, MD, 10,13 Luigi Romito, MD, 9 Massimo Scerrati, MD, 10,17 Marc Janssens, PhD, 18 and Anthony E. Lang, MD, 1 1 Toronto Western Hospital, Movement Disorders Center, University of Toronto and University Health Network, Toronto, Ontario, Canada 2 Division of Neurosurgery, University of Toronto and University Health Network, Toronto, Ontario, Canada 3 Service de Neurologie, CHU de Grenoble, Grenoble, France 4 Hôpital de la Salpêtrière, Fédération de Neurologie, Paris, France 5 Neurosurgery Service, Lund University Hospital, Lund, Sweden 6 Neurologische Klinik der Christian-Albrect-Universitat, Kiel, Germany 7 Department of Neurology, Sant Pau Hospital, Autonomous University of Barcelona, CIBERNED, Barcelona, Spain 8 Department of Neurology and Neurosurgery, Clinica Universitaria and Medical School, University of Navarra, CIBERNED, Pamplona, Spain 9 Istituto Nazionale Neurologico C. Besta and Università Cattolica, Milano, Italy 10 Dipartimento di Neuroscienze, Università Cattolica del Sacro Cuore, Roma, Italy 11 Institute of Neurology, Queen Square, London, UK 12 Department of Neurosurgery, University Hospital of Northern Sweden, Umeå, Sweden 13 Department of Neurology, Academic Medical Center, Amsterdam, The Netherlands 14 Service de Neurologie, CHU de Poitiers, University of Poitiers, Poitiers, France 15 Department of Neurology and Institute of Clinical Neurosciences, Heinrich-Heine-Universitat Duesseldorf, Duesseldorf, Germany 16 Department of Neurology, University Hospital, Cologne, Germany 17 Dipartimento di Neuroscienze, Sezione di Neurochirurgia, Università Politecnica delle Marche, Ancona, Italy 18 Bakken Research Center, Maastricht, The Netherlands Additional Supporting Information may be found in the online version of this article. *Correspondence to: Dr. Elena Moro, Toronto Western Hospital, Movement Disorders Center, 399 Bathurst Street McL7-402, University of Toronto and University Health Network, Toronto, Ontario, M5T 2S8 Canada elena.moro@uhn.on.ca Potential conflict of interest: None reported. Received 14 December 2008; Revised 13 April 2009; Accepted 8 July 2009 Published online 8 March 2010 in Wiley InterScience (www. interscience.wiley.com). DOI: /mds
2 STUDY ON SUBTHALAMIC AND PALLIDAL STIMULATION 579 Abstract: We report the 5 to 6 year follow-up of a multicenter study of bilateral subthalamic nucleus (STN) and globus pallidus internus (GPi) deep brain stimulation (DBS) in advanced Parkinson s disease (PD) patients. Thirty-five STN patients and 16 GPi patients were assessed at 5 to 6 years after DBS surgery. Primary outcome measure was the stimulation effect on the motor Unified Parkinson s Disease Rating Scale (UPDRS) assessed with a prospective cross-over double-blind assessment without medications (stimulation was randomly switched on or off). Secondary outcomes were motor UPDRS changes with unblinded assessments in offand on-medication states with and without stimulation, activities of daily living (ADL), anti-pd medications, and dyskinesias. In double-blind assessment, both STN and GPi DBS were significantly effective in improving the motor UPDRS scores (STN, P < , 45.4%; GPi, P , 20.0%) compared with off-stimulation, regardless of the sequence of stimulation. In open assessment, both STN- and GPi-DBS significantly improved the off-medication motor UPDRS when compared with before surgery (STN, P < 0.001, 50.5%; GPi, P , 35.6%). Dyskinesias and ADL were significantly improved in both groups. Anti-PD medications were significantly reduced only in the STN group. Adverse events were more frequent in the STN group. These results confirm the long-term efficacy of STN and GPi DBS in advanced PD. Although the surgical targets were not randomized, there was a trend to a better outcome of motor signs in the STN-DBS patients and fewer adverse events in the GPi-DBS group. Ó 2010 Movement Disorder Society Key words: deep brain stimulation; globus pallidus internus; Parkinson s disease; subthalamic nucleus Significant improvements in quality of life and motor function have been obtained in the short-term and long-term with both subthalamic nucleus (STN) and globus pallidus internus (GPi) deep brain stimulation (DBS) in Parkinson s disease (PD). 1 9 In relatively short-term follow-up studies, trends to both less motor improvement and fewer complications have been observed with GPi-DBS, 1,10,11 findings which were supported by preliminary 12-month follow-up data from a randomized study of pallidal vs. STN stimulation 12 and by a comparison of the effects of bilateral STN- vs. bilateral GPi-DBS in patients operated on both targets. 13 In the long-term, a multicenter DBS study reported significant benefits with both targets at 4 years. 2 The only study with 5-year follow-up data in patients with GPi-DBS reported a progressive loss of initial benefit in 11 bilateral GPi-DBS patients, leading to subsequent successful bilateral STN-DBS implantation in 4 of them. 14 In contrast, the larger number of studies with STN-DBS suggests that these patients continue to obtain a significant benefit in the longterm These observations emphasize the importance of long-term follow-up studies for both targets. This article reports 5- to 6-year follow-up data of the previously reported multicenter DBS trial 1,2,18 on STN- and GPi-DBS in advanced PD. PATIENTS AND METHODS Patients The main aim of this study was to evaluate the effects of bilateral STN- and GPi-DBS in patients with advanced PD followed for a minimum of five and a maximum of 6 years. Of 160 patients with PD initially recruited from 18 centers as part of a nonrandomized, multicenter study, patients were implanted with bilateral STN- or GPi-DBS between January 1996 and July Criteria of inclusion and exclusion, initial outcome at 3- and 6-month follow-up and the surgical procedure have previously been reported. 1 One hundred and five patients from eight surgical centers later agreed to participate in the extension (up to 5 6 years) of the initial study. The results of 69 patients with bilateral STN (49 patients) and GPi (20 patients) DBS at 3 to 4 year follow-up have also been reported earlier. 2,18 Fifty-one patients (35 with STN-DBS and 16 with GPi-DBS) were available at the 5 to 6 year follow-up. The Figure 1 illustrates the steps of the trial and the reasons for the subsequent drop outs. The study was approved by each local ethics boards and all patients gave written informed consent to the study extension. Study Design The study was initially designed as an open, nonrandomized, prospective multicenter clinical trial aimed at evaluating safety and effectiveness of bilateral STN and GPi stimulation in patients with advanced PD. 1 The study planned a randomized double-blind evaluation with cross-over on the second day of the 3-month follow-up visit and unblinded assessments at 1-, 6-, and 12-month follow-up. A subsequent extension of the study was performed to obtain data from the long-term (3 4 years and 5 6 years) and from a double-blind randomized crossover assessment at 5 6 years.
3 580 E. MORO ET AL. on for 2 hours and then stimulation turned off for another 2 hours, sequence B). Patients were assessed using the Unified Parkinson s Disease Rating Scale (UPDRS) 20 and a dyskinesia rating scale. 21,22 Only the UPDRS part II (activities of daily living, ADL) and III (motor) and some UPDRS- III and IV subscores (see later) were analyzed in this study. For the double-blind assessments, only the UPDRS motor score was analyzed. Anti-PD medications required before and after surgery were recorded and converted to L-dopa equivalent daily dose (LEDD). 2 Adverse events (AEs) were defined and recorded as previously described. 1,2,18 FIG. 1. The overall study profile. As previously reported, 1,2 the patients were assessed before surgery in the defined off anti-pd medications (meds) condition (after 12-hour medication withdrawal) and in the defined on meds condition 19 after an acute levodopa (L-dopa) challenge. The same preoperative dose of L-dopa was used for all the postoperative assessments in on meds condition. At each postsurgery follow-up, patients were assessed using the previously reported four-condition schedule: off meds/off stimulation (stim) and on meds/off stim (after minutes stim off), off meds/on stim and on meds/on stim (after minutes stim on). 2 In contrast with the 3 to 4 years assessment, the patients were also evaluated in a double-blind fashion with cross-over 1 or 2 days after the open 5 to 6 year follow-up assessment, using the same protocol used for the 3-month assessment. 1 After overnight discontinuation of both anti-pd medications and stimulation, patients were randomly assigned to have motor assessments with stimulation off for another 2 hours and after 2 hours after switching stimulation on (sequence A) or to the reverse sequence (first stimulation turned Statistics The primary outcome measure was the differences between the UPDRS motor scores in the off meds condition with and without stimulation in the double-blind crossover assessment. A mixed linear model was used to evaluate the effect of sequence, period, and stimulation. The analysis of the sequence effect and period effects assessed whether the stimulation intervention in the first assessment influenced the results acquired in the second. Secondary outcome measurements included changes in the UPDRS part II and III scores in the stim on condition between preoperative (baseline) and postoperative follow-up at 3 to 4 and 5 to 6 years in off and on meds conditions. Some subscores of the motor UPDRS were analyzed separately: speech (item 18), tremor (items 20 and 21), rigidity (item 22), akinesia (items 23 26), postural stability (item 28), and gait (item 29). Other secondary outcomes were changes in dyskinesia scores (UPDRS-IV, items 32, 33, 34, and 35) and changes in the LEDD compared with before surgery and at the two latest follow-ups and changes of the parameters of stimulation between 3 to 4 and 5 to 6 years. As normality could not be assumed in the relatively small STN and GPi groups of patients, nonparametric testing was used. The type 1 error limit was set to to account for multiple comparisons. Regression analysis was performed to assess possible preoperative factors predictive of benefit or failure in both STN and GPi patients. Stepwise model-selection multiple-regression method was used to predict motor scores on the basis of four independent variables: preoperative L-dopa response, surgical target, age, and disease duration at time of surgery. Data are presented as both medians (and quartiles) and means (with Standard Errors). All P-values are
4 STUDY ON SUBTHALAMIC AND PALLIDAL STIMULATION 581 TABLE 1. Main baseline clinical characteristics of the patients with PD involved in the long-term study STN (n 5 35) GPi (n 5 16) Gender, M/F 17/18 11/5 Age at surgery (yr) 59.6 ( ); 59.3 (1.6) 54.4 ( ); 56.0 (2.1) Duration of follow-up (yr) 5.2 ( ); 5.3 (0.1) 5.5 ( ); 5.6 (0.1) Duration of PD since onset (yr) 13.5 ( ); 15.3 (1.1) 13.2 ( ); 15.1 (1.5) Duration of PD since diagnosis (yr) 12.6 ( ); 14.1 (1.0) 12.6 ( ); 14.0 (1.3) UPDRS-II Off medication 32.5 ( ); 30.0 (1.3) 26.8 ( ); 26.7 (2.3) On medication 8.5 ( ); 10.4 (1.1) 9.8 ( ); 12.0 (1.6) UPDRS-III Off medications 56.5 ( ); 56.0 (2.7) 52.5 ( ); 52.2 (3.5) On medication 24.5 ( ); 22.9 (1.8) 16.5 ( ); 18.5 (2.8) Hoehn & Yahr, off medications 5.0 ( ); 4.4 (0.1) 4.0 ( ); 3.9 (0.2) Dyskinesias a Off dystonia 0.5 ( ); 1.0 (0.2) 0.0 ( ); 0.6 (0.3) On dyskinesia 2.0 ( ); 2.1 (0.2) 3.0 ( ); 2.8 (0.3) LEDD (mg) 1,475 (1,025 2,050); 1,709.3 (166.8) 1,275 (913 1,998); 1,417.8 (153.0) a Using the Dyskinesia Scale from Langston 21 and Goetz. 22 Data are presented as both median (values in parentheses are lower and upper quartiles) and mean (values in parenthesis are the standard errors). LEDD, levodopa equivalent daily dose. two-tailed. The analysis was performed using SAS release RESULTS Evaluations were performed between March 2001 and September The median follow-up for all patients was 5.3 ( ) years. The main clinical characteristics at time of surgery of the 51 patients with PD with 5 to 6 year follow-up are summarized in Table 1. Fifty-four (51.4%) of the initial 105 patients were lost to follow-up at the 5 to 6 year period (Fig. 1). Details about patient drop out during the first 3 to 4 year follow-up have been published. 2,18 Compared with the 3 to 4 year evaluation, 18 more patients exited the study before the 5 to 6 year assessment (Fig. 1). Among these patients, 10 STN patients died (1 of a stroke, 1 after fracture, 8 for unknown reasons), 3 STN patients were lost to follow-up, 1 STN and 1 GPi patient withdrew their consent, 1 GPi patient with suboptimal clinical benefit underwent bilateral STN-DBS, 1 bilateral GPi-DBS patient remained with unilateral stimulation, and 1 GPi patient had leads and batteries explanted and not replaced. Long-Term STN Stimulation Data were available on the 5 to 6 year doubleblinded evaluation in 31 of 35 patients and nonblinded assessments in all 35. The electrical parameters of stimulation were unchanged compared with the 3 to 4 year follow-up. 2 Fourteen patients (40%) had battery replacement (bilateral replacement in 11 patients and unilateral in 3 patients) between the two time points, with a mean battery lifetime of years. Double-Blind Evaluation (Cross-Over) Table 2 shows the main results of the assessments at 5 to 6 years compared with the 3-month follow-up. The UPDRS motor scores at 5 to 6 years remained significantly improved (45.4%; P < ) comparing the on and the off stim conditions. There were no significant sequence effects or carry-over effects (P ). Unblinded Evaluation Table 3 and Supporting Information Table 1 show the main results of the unblinded assessments at 5 to 6 years. In the off meds condition, the total UPDRS motor scores were significantly (P < 0.001) improved by stimulation (50.5%) when compared with baseline. However, there was a significant decline in this benefit when compared with the 3 to 4 year follow-up scores (Table 3). Overall, stimulation at 5 to 6 years significantly improved the main off meds UPDRS-III subscores (tremor by 81.1%, rigidity by 59.1%, akinesia by 30.8%, postural stability by 66.6%, and gait by 33.3%), with the exception of speech (Supporting Information Table 1). Akinesia subscores improvement declined significantly when compared with the 3 to 4 year follow-up. The UPDRS-II total scores and early morning dystonia scores also significantly improved at
5 582 E. MORO ET AL. TABLE 2. UPDRS motor scores in double-blind randomization using sequence evaluations at 3-month and 5 6 year follow-up for STN and GPi patients (off medications) Motor scores STN (31 patients) GPi (15 patients) 3 months 5 6 years 3 months 5 6 years Off stimulation 54.0 ( ) 55.0 ( ) 49.0 ( ) 35.0 ( ) 51.5 (3.1) 52.7 (3.2) 48.7 (4.8) 43.9 (4.6) On stimulation 21.0 ( ) 30.0 ( ) 27.0 ( ) 28.0 ( ) 23.7 (2.2) 30.1 (2.5) 32.3 (3.9) 32.6 (4.6) P-value < < Data are presented as both median (values in parentheses are lower and upper quartiles) and mean (values in parenthesis are the standard errors). Using a mixed linear model, sequence, and period effects were not significant, thus the comparison was made between on and off stimulation. The 3-month data are presented on only those patients undergoing 5 6 years evaluation. 5 to 6 years (49.2%) compared with baseline, without any change with respect to the 3 to 4 year follow-up (Table 3). There was no significant worsening of the motor UPDRS scores over the years in off meds/ off stim condition when compared with baseline (Table 3). In the on meds condition, stimulation did not further improve the motor UPDRS scores at 5 to 6 years when compared with baseline and there was a significant decrease in the improvement achieved at 3 to 4 year follow-up (Table 3). Among the UPDRS motor subscores, only rigidity was significantly improved by 5 to 6 year stimulation (25.0%) when compared with baseline, whereas speech and gait showed a significant worsening (Supporting Information Table 1). No change was observed in the other subscores. Initial improvement in akinesia and gait scores declined significantly at 5 to 6 years when compared with the 3 to 4 year time point. There was a significant worsening of the total UPDRS-II scores when compared with both baseline and 3 to 4 year follow-up (Table 3). Dyskinesia scores (total, duration, and disability) were significantly improved at 5 to 6 years compared with baseline (by 83.3%, 75%, and 100%, respectively) and unchanged when compared with 3 to 4 years (Supporting Information Table 1). Although in the on meds and off stim condition the motor UPDRS scores significantly deteriorated over the years, stimulation added a significant benefit to the total on meds motor scores at 5 to 6 years (26.0%, P ) (Table 3). LEDD was significantly reduced at 5 to 6 years compared with baseline (29.7%) (Supporting Information Table 1). Only the preoperative L-dopa response (i.e., the difference between on and off meds UPDRS motor scores during the acute L-dopa challenge) was positively correlated with the motor improvement at the 5 to 6 year follow-up (P ). Adverse Events Three hardware-related AEs were observed: one lead was replaced in 2 patients and one battery plus extension was replaced in another. Table 4 shows the number and type of non-hardware-related AEs reported as unresolved at the last follow-up. Long-Term GPi Stimulation Data related to the double-blind evaluations at 5 to 6 years were available for 15 of 16 patients and open assessments in all 16. The electrical parameters of stimulation and the electrode contacts of stimulation were unchanged at 5 to 6 years when compared with the 3 to 4 year follow-up 2 and 8 (50%) patients had battery replacement (7 bilateral and 1 unilateral replacements), with a mean battery lifetime of years. Double-Blind Evaluation Table 2 shows the main results of the UPDRS motor assessments at 5 to 6 years compared with the 3-month follow-up in the same group of patients. The UPDRS motor scores improvement between off and on stim conditions was significant (20.0%; P ). There were no significant sequence effects or carry-over effects (P ). Unblinded Evaluation Table 3 and Supporting Information Table 2 show the main results of the unblinded assessments at 5 to 6 years. In the off meds condition, the total UPDRS motor scores were significantly improved by stimulation at 5 to 6 years compared with baseline (35.6%). This improvement was stable when compared with the 3 to 4 year scores (Table 3). However, tremor and rigidity subscores were the only motor UPDRS items
6 STUDY ON SUBTHALAMIC AND PALLIDAL STIMULATION 583 TABLE 3. Main results of STN and GPi stimulation on the total scores of the UPDRS part II and III in off and on medication conditions (unblinded evaluations) UPDRS-III total scores P-value Target and condition Baseline 3 4-years 5 6 years 5 6 years vs. baseline 5 6 years vs. 3 4 years STN (n 5 35) Off medication UPDRS-II total 32.5 ( ) 15.0 ( ) 16.5 ( ) < (1.3) 17.3 (1.6) 18.7 (1.4) UPDRS-III total Off stimulation 56.5 ( ) 57.0 ( ) 57.0 ( ) (2.7) 54.7 (2.9) 54.3 (3.0) On stimulation 26.0 ( ) 28.0 ( ) <0.001 < (2.7) 30.8 (2.9) On medication UPDRS-II total 8.5 (5 14) 11.0 ( ) 14.0 ( ) < (1.2) 12.7 (1.6) 14.7 (1.3) UPDRS-III total Off stimulation 24.5 ( ) 21.5 ( ) 29.0 ( ) < (2.0) 28.1 (3.8) 32.9 (3.8) On stimulation 15.0 ( ) 23.0 ( ) < (2.6) 24.6 (2.9) GPi (n 5 16) Off medication UPDRS-II total 26.8 ( ) 17.5 ( ) 17.0 ( ) (2.3) 17.3 (2.1) 19.8 (2.8) UPDRS-III total Off stimulation 52.5 ( ) 44.0 ( ) 47.0 ( ) (3.5) 48.4 (2.9) 48.8 (3.5) On stimulation 29.5 ( ) 33.0 ( ) (3.1) 33.9 (4.4) On medication UPDRS-II total 9.8 ( ) 10.0 ( ) 12.0 ( ) (1.6) 10.9 (2.0) 14.5 (2.5) UPDRS-III total Off stimulation 16.5 ( ) 19.0 ( ) 20.0 ( ) (2.8) 21.7 (3.9) 26.0 (3.9) On stimulation 16.5 ( ) 19.5 ( ) (3.0) 21.6 (3.2) Data are presented as both median (values in parentheses are lower and upper quartiles) and mean (values in parenthesis are the standard errors). The P-values were calculated using the Wilcoxon signed rank test. Bonferroni correction was used to issue testing multiplicity. Type 1 error was set to significantly improved at 5 to 6 years (Supporting Information Table 2) (65.5% and 41.7%, respectively). The UPDRS-II total scores were significantly improved at 5 to 6 years (36.7%) and stable compared with the previous 3 to 4 year scores (Table 3). No difference was observed in early morning dystonia scores. There was no significant worsening of the motor UPDRS scores over the years in off meds/off stim conditions. In the on meds condition, stimulation did not further improve the motor UPDRS at 5 to 6 years when compared with baseline and there was a significant worsening between the scores at the 3 to 4 and 5 to 6 year time points (Table 3). None of the UPDRS motor subscores showed further improvement with stimulation (Supporting Information Table 2), whereas speech showed a significant worsening at 5 to 6 years compared with baseline and the 3 to 4 year follow-up. Although there was no significant worsening of the total UPDRS-II scores at 5 to 6 years compared with baseline, the difference was significant when compared with the 3 to 4 year followup (Table 3). Dyskinesia scores were significantly improved at 5 to 6 year stimulation compared with baseline (total 75.0%, duration 75.0%, and disability 100%), with no loss of this sustained benefit compared with 3 to 4 years (Supplementary Table 2). There was a significant worsening of the motor UPDRS scores over the years in on meds/off stim conditions (Table 3) and no additional benefit was seen when stimulation was added. LEDD was not significantly reduced at 5 to 6 years compared with baseline (Supporting Information Table 2).
7 584 E. MORO ET AL. TABLE 4. Unresolved AEs present at 5-year follow-up in both STN and GPi patients STN (n 5 35) GPi (n 5 16) No of patients with AEs 26 8 Total no of AEs Cognitive decline 8 2 Depression/anxiety 7 2 Hypersexuality 1 2 Speech difficulties 10 2 Balance disturbances 5 1 Gait disorders 9 1 Motor fluctuations 3 Sleep disorders 4 Only the preoperative L-dopa response was positively correlated with the motor improvement at 5 to 6 year stimulation (P ). Adverse Events One hardware-related AE and a lead fracture that required surgery were observed. Table 4 shows the number and the type of non-hardware-related AEs reported as unresolved at 5 to 6 years. DISCUSSION These long-term follow-up results of bilateral DBS in patients with advanced PD confirm the effectiveness of both STN- and GPi-DBS in improving L-dopa-responsive PD signs, L-dopa-induced dyskinesias, and ADL up to 5.7 years after surgery and show that the preoperative response to L-dopa predicts long-term benefit with both targets. Both the double-blind and the open label clinical assessments documented a significant treatment effect of bilateral STN-DBS on the motor scores in off meds conditions. All the UPDRS motor subscores (except speech), the off-meds ADL, the early morning dystonia, and dyskinesias were also markedly improved and LEDD was greatly reduced. Some of the clinical benefit of STN DBS declined between 3 to 4 and 5 to 6 year follow-up, as previously reported, 2,15 17 probably related to a combination of the natural progression of PD and the parallel reduction of the L-dopa response. Bilateral GPi-DBS was also significantly effective in improving motor PD signs in both the blinded and unblinded assessments. In particular, tremor and rigidity were significantly improved by stimulation in off meds condition, as were off meds ADL and dyskinesia scores. LEDD was unchanged at 5 to 6 years compared with before surgery. There was no significant difference in stimulation benefit between the 3- and 5-year follow-up. However, as previous reported, 14 one patient (Fig. 1), who lost the DBS motor benefit between the 3 to 4 and 5 to 6 year follow-up, subsequently underwent successful bilateral STN DBS surgery. Although the reasons for this loss of GPi-DBS benefit are unclear, one possible explanation may be a suboptimal placement of the electrode inside the pallidum, which is larger than the STN and has more functional segregation. 14 Both STN- and GPi-DBS patients showed deterioration of the L-dopa response at 5 to 6 years, suggesting a relationship more with the progression of PD 2,15,17 rather than with the target of stimulation, stimulation parameters, or medication dose reduction. 23 Although the lack of initial randomization between the two target sites prevents direct comparison and possibly represents the major limitation of the study, treatment-related AEs were proportionally more frequent in the STN patients compared with the GPi patients over the 5 to 6 year evaluation period. A recent separate article has specifically addressed the DBS associated AEs at 3 to 4 years in this same group of patients. 18 Most of these AEs were unresolved at the 5 to 6 year follow-up. Although over the 6-year duration of the study about 50% of the patients were lost to follow-up for various reasons, this is not an uncommon problem in clinical trials with patients with PD. 24 Proportionally more patients died in the STN group than in the GPi group. Although the reason for the mortality differences is unclear, no difference in mortality rate between patients with PD with and without STN-DBS has been reported. 25 In summary, both STN and GPi DBS have been shown to be effective in improving motor PD signs with sustained benefit at the 5 to 6 year follow-up. STN-DBS patients obtained relatively greater benefit as measured by the magnitude and quality of the motor benefit and improvement in ADL, whereas GPi-DBS patients experienced fewer AEs. However, it is important to emphasize that this study was not designed to enable comparison between STN- and GPi-DBS in patients with advanced PD. Acknowledgments: The authors thank Carin Wensing, Jo Lissens, and Alan Cohen from Medtronic for their assistance as project managers during the study. They also thank Abdallah Abouihia for his assistance in the statistical analysis. Financial disclosures: All authors (with the exception of A.L. Tornqvist) have occasionally received honoraria from Medtronic for lecturing at meetings. The three members of
8 STUDY ON SUBTHALAMIC AND PALLIDAL STIMULATION 585 the ad hoc AE Committee (M.I. Hariz, N.P. Quinn, J.D. Speelman) were reimbursed by Medtronic for their time spent analyzing the AE data, but not for preparing this paper. Author Roles: E. Moro has contributed to execution of the research project, has had a major role in the design, review, and critique of statistical analysis and has written the first draft of the manuscript. She has also had full access to the data and takes responsibility for the integrity of the data and the accuracy of the data analysis. A.M. Lozano has had a major role in the conception and execution of the research project and has contributed to the review and critique of the statistical analysis and the first draft of the manuscript. P. Pollak has had a major role in the conception and execution of the research project and has contributed to the review and critique of the statistical analysis and the first draft of the manuscript. Y. Agid has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. S. Rehncrona has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. J. Volkmann has contributed to execution of the analysis, and to the first draft of the manuscript. J. Kulisevsky has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. J.A. Obeso has had a major role in the conception and execution of the research project and has contributed to the review and critique of the statistical analysis, and to the first draft of the manuscript. A. Albanese has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. M.I. Hariz has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. N.P. Quinn has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. J.D. Speelman has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. A.L. Benabid has had a major role in the conception of the research project and has contributed to the review and critique of the statistical analysis and to the first draft of the manuscript. V. Fraix has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. A. Mendes has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. M. Welter has contributed to execution of the analysis, and to the first draft of the manuscript. J.L. Houeto has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. P. Cornu has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. D. Dormont has contributed to execution of the analysis, and to the first draft of the manuscript. A.L. Tornqvist has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. R. Ekberg has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. A. Schnitzler has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. L. Timmermann has contributed to execution of the analysis, and to the first draft of the manuscript. L. Wojtecki has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. A. Gironell has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. M.C. Rodriguez-Oroz has contributed to execution of the analysis, and to the first draft of the manuscript. J. Guridi has contributed to the analysis and interpretation of the data, the execution of the research project, the review and critique of the statistical analysis, and the first draft of the manuscript. A.R. Bentivoglio has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. M.F. Contarino has contributed to execution of the analysis, and to the first draft of the manuscript. L. Romito has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. M. Scerrati has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. M. Janssens has contributed to the design and has performed the statistical analysis. He has also contributed to the review and critique of the first draft of the manuscript. He has also had full access to the data and takes responsibility for the integrity of the data and the accuracy of the data analysis. He has conducted the statistical analysis. A.E. Lang has contributed to execution of the research project, to the review and critique of the statistical analysis, and to the first draft of the manuscript. REFERENCES 1. The Deep Brain Stimulation for Parkinson s Disease Study Group. Deep brain stimulation of the subthalamic nucleus or the pars interna of the globus pallidus in Parkinson s disease. N Engl J Med 2001;345: Rodriguez-Oroz MC, Obeso JA, Lang AE, et al. Bilateral deep brain stimulation in Parkinson s disease: a multicenter study with 4 years follow-up. Brain 2005;128: Kleiner-Fisman G, Herzog J, Fisman DN, et al. Subthalamic nucleus deep brain stimulation: summary and meta-analysis of outcomes. Mov Disord 2006;21(Suppl. 14):S290 S Ghika J, Villemure JG, Fankhauser H, et al. Efficiency and safety of bilateral contemporaneous pallidal stimulation (deep brain stimulation) in levodopa-responsive patients with Parkinson s disease with severe motor fluctuations: a 2-year follow-up review. J Neurosurg 1998;89: Durif F, Lemaire JJ, Debilly B, Dordain G. Long-term follow-up of globus pallidus chronic stimulation in advanced Parkinson s disease. Mov Disord 2002;
9 586 E. MORO ET AL. 6. Diamond A, Jankovic J. The effect of deep brain stimulation on quality of life in movement disorders. J Neurol Neurosurg Psychiatry 2005;76: Lyons KE, Pahwa R. Long-term benefits in quality of life provided by bilateral subthalamic stimulation in patients with Parkinson disease. J Neurosurg 2005;103: Deuschl G, Schade-Brittinger C, Krack P, et al. A randomized trial of deep-brain stimulation for Parkinson s disease. N Engl J Med 2006;355: Pahwa R, Factor SA, Lyons KE, et al. Practice parameters: treatment of Parkinson disease with motor fluctuations and dyskinesia (an evidence-based review). Report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology 2006;66: Krack P, Pollak P, Hoffmann D, Xie J, Benazzouz A, Benabid AL. Subthalamic nucleus or internal pallidal stimulation in young onset Parkinson s disease. Brain 1998;121: Volkmann J, Allert N, Voges J, Weiss PH, Sturm V. Safety and efficacy of pallidal or subthalamic nucleus stimulation in advanced Parkinson s disease. Neurology 2001;56: Anderson VC, Burchiel KJ, Hogarth P, Favre J, Hammerstad JP. Pallidal vs subthalamic nucleus deep brain stimulation in Parkinson s disease. Arch Neurol 2005;62: Peppe A, Pierantozzi M, Bassi A, et al. Stimulation of the subthalamic nucleus compared to the globus pallidus internus in patients with Parkinson s disease. J Neurosurg 2004;101: Volkmann J, Allert N, Voges J, Sturm V, Schnitzler A, Freund HJ. Long-term results of bilateral pallidal stimulation in Parkinson s disease. Ann Neurol 2004;55: Krack P, Batir A, Van Blercom N, et al. Five-year follow-up of bilateral stimulation of the subthalamic nucleus in advanced Parkinson s disease. N Engl J Med 2003;349: Schupbach WM, Chastan N, Welter ML, et al. Stimulation of the subthalamic nucleus in Parkinson s disease: a 5 year follow up. J Neurol Neurosurg Psychiatry 2005;76: Piboolnurak P, Lang AE, Lozano AM, et al. Levodopa-response in long-term bilateral subthalamic stimulation in Parkinson s disease. Mov Disord 2007;22: Hariz MI, Rehncrona S, Quinn N, Speelman JD, Wensing C,and the Multicenter Advanced Parkinson s Disease Deep Brain Stimulation Group. Multicenter study on deep brain stimulation in Parkinson s disease: an independent assessment of reported adverse events at 4 years. Mov Disord 2008;23: Defer GL, Widner H, Marie RM,and the Conference Participants. Core Assessment Program for Surgical Interventional Therapies in Parkinson s Disease (CAPSIT-PD). Mov Disord 1999;14: Fahn SE, RL. Unified Parkinson s Disease Rating Scale. Florham Park, NJ: Macmillan Health Care Information; Langston JW, Widner H, Goetz C, et al. Core assessment program for intracerebral transplantation (CAPIT). Mov Disord 1992;7: Goetz C, Stebbins GT, Shale HM, et al. Utility of an objective dyskinesia rating scale for Parkinson s disease: inter- and intrarater reliability assessment. Mov Disord 1994;9: Moro E, Esselink RJ, Benabid AL, Pollak P. Response to levodopa in parkinsonian patients with bilateral subthalamic nucleus stimulation. Brain 2002;125: Rascol O, Brooks DJ, Korczyn AD, et al. A five year study of the incidence of dyskinesia in patients with early Parkinson s disease who were treated with ropinirole or levodopa. 056 Study Group. N Engl J Med 2000;342: Schupbach WM, Welter ML, Bonnet AM, et al. Mortality in patients with Parkinson s disease treated by stimulation of the subthalamic nucleus. Mov Disord 2007;22:
Long-term follow up of subthalamic nucleus stimulation in Parkinson s disease
 oped parallel to a progressive cerebral disease. These findings are supported by other recent reports showing that EDS correlates with more advanced PD. 9 The close correlation between persistent and new
oped parallel to a progressive cerebral disease. These findings are supported by other recent reports showing that EDS correlates with more advanced PD. 9 The close correlation between persistent and new
Bilateral deep brain stimulation in Parkinson s disease: a multicentre study with 4 years follow-up
 doi:10.1093/brain/awh571 Brain (2005), 128, 2240 2249 Bilateral deep brain stimulation in Parkinson s disease: a multicentre study with 4 years follow-up M. C. Rodriguez-Oroz, 1 J. A. Obeso, 1 A. E. Lang,
doi:10.1093/brain/awh571 Brain (2005), 128, 2240 2249 Bilateral deep brain stimulation in Parkinson s disease: a multicentre study with 4 years follow-up M. C. Rodriguez-Oroz, 1 J. A. Obeso, 1 A. E. Lang,
Replacement of Dopaminergic Medication with Subthalamic Nucleus Stimulation in Parkinson s Disease: Long-Term Observation
 Movement Disorders Vol. 24, No. 4, 2009, pp. 557 563 Ó 2008 Movement Disorder Society Replacement of Dopaminergic Medication with Subthalamic Nucleus Stimulation in Parkinson s Disease: Long-Term Observation
Movement Disorders Vol. 24, No. 4, 2009, pp. 557 563 Ó 2008 Movement Disorder Society Replacement of Dopaminergic Medication with Subthalamic Nucleus Stimulation in Parkinson s Disease: Long-Term Observation
ORIGINAL CONTRIBUTION. Subthalamic Stimulation in Parkinson Disease
 Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
ORIGINAL CONTRIBUTION. Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement
 ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
A lthough levodopa treatment remains the gold standard
 1640 PAPER Stimulation of the subthalamic nucleus in Parkinson s disease: a 5 year follow up W M M Schüpbach, N Chastan, M L Welter, J L Houeto, V Mesnage, A M Bonnet, V Czernecki, D Maltête, A Hartmann,
1640 PAPER Stimulation of the subthalamic nucleus in Parkinson s disease: a 5 year follow up W M M Schüpbach, N Chastan, M L Welter, J L Houeto, V Mesnage, A M Bonnet, V Czernecki, D Maltête, A Hartmann,
C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak, MD, PhD D.
 ARTICLES STN-DBS frequency effects on freezing of gait in advanced Parkinson disease C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak,
ARTICLES STN-DBS frequency effects on freezing of gait in advanced Parkinson disease C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak,
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor
 Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
Overweight after deep brain stimulation of the subthalamic nucleus in Parkinson disease: long term follow-up
 1 CHU Clermont-Ferrand, Department of Neurology, Gabriel Montpied Hospital, Clermont-Ferrand, France; 2 Univ Clermont 1, UFR Medecine, Clermont-Ferrand, France; 3 INRA, Centre Clermont-Ferrand Theix, Unite
1 CHU Clermont-Ferrand, Department of Neurology, Gabriel Montpied Hospital, Clermont-Ferrand, France; 2 Univ Clermont 1, UFR Medecine, Clermont-Ferrand, France; 3 INRA, Centre Clermont-Ferrand Theix, Unite
I n 1991 Benabid et al introduced deep brain stimulation
 PAPER Multicentre European study of thalamic stimulation in essential tremor: a six year follow up O Sydow, S Thobois, F Alesch, J D Speelman, study collaborators... See Editorial Commentary, pp1361 2
PAPER Multicentre European study of thalamic stimulation in essential tremor: a six year follow up O Sydow, S Thobois, F Alesch, J D Speelman, study collaborators... See Editorial Commentary, pp1361 2
Deep-brain stimulation of the subthalamic nucleus or the pars interna of the globus pallidus in Parkinson's disease
 Article Deep-brain stimulation of the subthalamic nucleus or the pars interna of the globus pallidus in Parkinson's disease Deep-Brain Stimulation for Parkinson's Disease Study Group KRACK, Paul (Collab.)
Article Deep-brain stimulation of the subthalamic nucleus or the pars interna of the globus pallidus in Parkinson's disease Deep-Brain Stimulation for Parkinson's Disease Study Group KRACK, Paul (Collab.)
Five-Year Follow-up of Bilateral Stimulation of the Subthalamic Nucleus in Advanced Parkinson s Disease
 The new england journal of medicine original article Five-Year Follow-up of Bilateral Stimulation of the Subthalamic Nucleus in Advanced Parkinson s Disease Paul Krack, M.D., Ph.D., Alina Batir, M.D.,
The new england journal of medicine original article Five-Year Follow-up of Bilateral Stimulation of the Subthalamic Nucleus in Advanced Parkinson s Disease Paul Krack, M.D., Ph.D., Alina Batir, M.D.,
Deep Brain Stimulation: Patient selection
 Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Comparison of Subthalamic Nucleus vs. Globus Pallidus Interna Deep Brain Stimulation in Terms of Gait and Balance; A Two Year Follow-Up Study
 DOI: 10.5137/1019-5149.JTN.22614-18.3 Received: 23.01.2018 / Accepted: 13.06.2018 Published Online: 26.10.2018 Turk Neurosurg, 2018 qr code Original Investigation Comparison of Subthalamic Nucleus vs.
DOI: 10.5137/1019-5149.JTN.22614-18.3 Received: 23.01.2018 / Accepted: 13.06.2018 Published Online: 26.10.2018 Turk Neurosurg, 2018 qr code Original Investigation Comparison of Subthalamic Nucleus vs.
B ilateral chronic subthalamic nucleus stimulation
 PAPER Functional improvement after subthalamic stimulation in Parkinson s disease: a non-equivalent controlled study with 12 24 month follow up M Capecci, R A Ricciuti, D Burini, V G Bombace, L Provinciali,
PAPER Functional improvement after subthalamic stimulation in Parkinson s disease: a non-equivalent controlled study with 12 24 month follow up M Capecci, R A Ricciuti, D Burini, V G Bombace, L Provinciali,
Evidence compendium. Research study summaries supporting the use of Medtronic deep brain stimulation (DBS) for Parkinson s disease
 Evidence compendium Research study summaries supporting the use of Medtronic deep brain stimulation (DBS) for Parkinson s disease CONTENTS Introduction... 4 Index of study summaries... 6 Parkinson s disease
Evidence compendium Research study summaries supporting the use of Medtronic deep brain stimulation (DBS) for Parkinson s disease CONTENTS Introduction... 4 Index of study summaries... 6 Parkinson s disease
Deep Brain Stimulation: Indications and Ethical Applications
 Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
Pallidal stimulation in Parkinson s patients with contraindications to subthalamic target: A 3 years follow-up
 Pallidal stimulation in Parkinson s patients with contraindications to subthalamic target: A 3 years follow-up Julien Bonenfant, Sophie Drapier, Jean François Houvenaghel, Florian Naudet, Claire Haegelen,
Pallidal stimulation in Parkinson s patients with contraindications to subthalamic target: A 3 years follow-up Julien Bonenfant, Sophie Drapier, Jean François Houvenaghel, Florian Naudet, Claire Haegelen,
F unctional stereotactic surgery is now well established for
 PAPER Effect of chronic pallidal deep brain on off period dystonia and sensory symptoms in advanced Parkinson s disease T J Loher, J-M Burgunder, S Weber, R Sommerhalder, J K Krauss... See end of article
PAPER Effect of chronic pallidal deep brain on off period dystonia and sensory symptoms in advanced Parkinson s disease T J Loher, J-M Burgunder, S Weber, R Sommerhalder, J K Krauss... See end of article
doi: /brain/awq221 Brain 2010: 133;
 doi:10.1093/brain/awq221 Brain 2010: 133; 2664 2676 2664 BRAIN A JOURNAL OF NEUROLOGY Motor and cognitive outcome in patients with Parkinson s disease 8 years after subthalamic implants Alfonso Fasano,
doi:10.1093/brain/awq221 Brain 2010: 133; 2664 2676 2664 BRAIN A JOURNAL OF NEUROLOGY Motor and cognitive outcome in patients with Parkinson s disease 8 years after subthalamic implants Alfonso Fasano,
Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II
 Parkinsonism and Related Disorders 13 (2007) 399 405 www.elsevier.com/locate/parkreldis Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II A. Haffenden, U.
Parkinsonism and Related Disorders 13 (2007) 399 405 www.elsevier.com/locate/parkreldis Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II A. Haffenden, U.
EMERGING TREATMENTS FOR PARKINSON S DISEASE
 EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
Basal ganglia motor circuit
 Parkinson s Disease Basal ganglia motor circuit 1 Direct pathway (gas pedal) 2 Indirect pathway (brake) To release or augment the tonic inhibition of GPi on thalamus Direct pathway There is a tonic inhibition
Parkinson s Disease Basal ganglia motor circuit 1 Direct pathway (gas pedal) 2 Indirect pathway (brake) To release or augment the tonic inhibition of GPi on thalamus Direct pathway There is a tonic inhibition
Effect of Subthalamic Deep Brain Stimulation on Levodopa-Induced Dyskinesia in Parkinson s Disease
 Original Article Yonsei Med J 2015 Sep;56(5):1316-1321 pissn: 0513-5796 eissn: 1976-2437 Effect of Subthalamic Deep Brain Stimulation on Levodopa-Induced Dyskinesia in Parkinson s Disease Ji Hee Kim, Won
Original Article Yonsei Med J 2015 Sep;56(5):1316-1321 pissn: 0513-5796 eissn: 1976-2437 Effect of Subthalamic Deep Brain Stimulation on Levodopa-Induced Dyskinesia in Parkinson s Disease Ji Hee Kim, Won
Deep brain stimulation in the GPi or the STN is a. Site of deep brain stimulation and jaw velocity in Parkinson disease.
 J Neurosurg 115:985 994, 2011 Site of deep brain stimulation and jaw velocity in Parkinson disease Clinical article Lee T. Robertson, Ph.D., 1 Rebecca J. St George, Ph.D., 2 Patricia Carlson-Kuhta, Ph.D.,
J Neurosurg 115:985 994, 2011 Site of deep brain stimulation and jaw velocity in Parkinson disease Clinical article Lee T. Robertson, Ph.D., 1 Rebecca J. St George, Ph.D., 2 Patricia Carlson-Kuhta, Ph.D.,
Factors Related to Outcomes of Subthalamic Deep Brain Stimulation in Parkinson s Disease
 online ML Comm www.jkns.or.kr http://dx.doi.org/0.3340/jkns.203.54.2.8 J Korean Neurosurg Soc 54 : 8-24, 203 Print ISSN 2005-3 On-line ISSN 598-8 Copyright 203 The Korean Neurosurgical Society Clinical
online ML Comm www.jkns.or.kr http://dx.doi.org/0.3340/jkns.203.54.2.8 J Korean Neurosurg Soc 54 : 8-24, 203 Print ISSN 2005-3 On-line ISSN 598-8 Copyright 203 The Korean Neurosurgical Society Clinical
Patient selection for surgery: Parkinson s disease
 Patient selection for surgery: Parkinson s disease Dr. María C. Rodríguez-Oroz Neurology and Neuroscience. University Hospital Donostia, Research Institute BioDonostia, Ikerbasque Senior Researcher San
Patient selection for surgery: Parkinson s disease Dr. María C. Rodríguez-Oroz Neurology and Neuroscience. University Hospital Donostia, Research Institute BioDonostia, Ikerbasque Senior Researcher San
DEEP BRAIN STIMULATION (DBS) is a standard treatment
 1320 ORIGINAL ARTICLE Fast-Track Programming and Rehabilitation Model: A Novel Approach to Postoperative Deep Brain Stimulation Patient Care David B. Cohen, MD, Michael Y. Oh, MD, Susan M. Baser, MD, Cindy
1320 ORIGINAL ARTICLE Fast-Track Programming and Rehabilitation Model: A Novel Approach to Postoperative Deep Brain Stimulation Patient Care David B. Cohen, MD, Michael Y. Oh, MD, Susan M. Baser, MD, Cindy
Deep brain stimulation (DBS) is now well established
 Pallidal Stimulation in Parkinson s Disease Does Not Induce Apathy Clément Lozachmeur, M.D. Sophie Drapier, M.D. Gabriel Robert, M.D., Ph.D. Thibaut Dondaine Bruno Laviolle, M.D., Ph.D. Paul Sauleau, M.D.
Pallidal Stimulation in Parkinson s Disease Does Not Induce Apathy Clément Lozachmeur, M.D. Sophie Drapier, M.D. Gabriel Robert, M.D., Ph.D. Thibaut Dondaine Bruno Laviolle, M.D., Ph.D. Paul Sauleau, M.D.
Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients
 J Neurosurg 98:779 784, 2003 Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients ATSUSHI UMEMURA, M.D., JURG L. JAGGI, PH.D., HOWARD I. HURTIG, M.D., ANDREW D. SIDEROWF,
J Neurosurg 98:779 784, 2003 Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients ATSUSHI UMEMURA, M.D., JURG L. JAGGI, PH.D., HOWARD I. HURTIG, M.D., ANDREW D. SIDEROWF,
Surgical Treatment of Movement Disorders. Surgical Treatment of Movement Disorders. New Techniques: Procedure is safer and better
 Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Coordinated Reset Neuromodulation for Parkinson s Disease: Proof-of-Concept Study
 BRIEF REPORT Coordinated Reset Neuromodulation for Parkinson s Disease: Proof-of-Concept Study Ilya Adamchic, MD, 1 Christian Hauptmann, PhD, 1 Utako Brigit Barnikol, MD, 1,2,3,4 Norbert Pawelczyk, 1 Oleksandr
BRIEF REPORT Coordinated Reset Neuromodulation for Parkinson s Disease: Proof-of-Concept Study Ilya Adamchic, MD, 1 Christian Hauptmann, PhD, 1 Utako Brigit Barnikol, MD, 1,2,3,4 Norbert Pawelczyk, 1 Oleksandr
Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology
 Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Deep Brain Stimulation
 Deep Brain Stimulation Patient and caregiver education Valérie Fraix, MD, PhD and Emmanuelle Schmitt Neurology Department, Grenoble-Alpes University Hospital Grenoble-Alpes University, INSERM U1216 F-38000
Deep Brain Stimulation Patient and caregiver education Valérie Fraix, MD, PhD and Emmanuelle Schmitt Neurology Department, Grenoble-Alpes University Hospital Grenoble-Alpes University, INSERM U1216 F-38000
Deep brain stimulation (DBS) has been shown to be
 clinical article J Neurosurg 124:908 916, 2016 Clinical outcomes using ClearPoint interventional MRI for deep brain stimulation lead placement in Parkinson s disease Jill L. Ostrem, MD, 1 Nathan Ziman,
clinical article J Neurosurg 124:908 916, 2016 Clinical outcomes using ClearPoint interventional MRI for deep brain stimulation lead placement in Parkinson s disease Jill L. Ostrem, MD, 1 Nathan Ziman,
D eep brain stimulation of the subthalamic nucleus (STN
 PAPER Disease progression continues in patients with advanced Parkinson s disease and effective subthalamic nucleus stimulation R Hilker*, A T Portman*, J Voges, M J Staal, L Burghaus, T van Laar, A Koulousakis,
PAPER Disease progression continues in patients with advanced Parkinson s disease and effective subthalamic nucleus stimulation R Hilker*, A T Portman*, J Voges, M J Staal, L Burghaus, T van Laar, A Koulousakis,
MRI-guided STN DBS in Parkinson s disease without microelectrode recording: efficacy and safety
 MRI-guided STN DBS in Parkinson s disease without microelectrode recording: efficacy and safety T Foltynie, L Zrinzo,,2 I Martinez-Torres, 3 E Tripoliti, E Petersen, 4 E Holl,,5 I Aviles-Olmos, M Jahanshahi,
MRI-guided STN DBS in Parkinson s disease without microelectrode recording: efficacy and safety T Foltynie, L Zrinzo,,2 I Martinez-Torres, 3 E Tripoliti, E Petersen, 4 E Holl,,5 I Aviles-Olmos, M Jahanshahi,
DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici
 DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici TECNICHE DI NEUROMODULAZIONE Invasiva: odeep Brain Stimulation Non Invasiva: o Transcranial Magnetic Stimulation (TMS) o Transcranial
DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici TECNICHE DI NEUROMODULAZIONE Invasiva: odeep Brain Stimulation Non Invasiva: o Transcranial Magnetic Stimulation (TMS) o Transcranial
Deep Brain Stimulation and Movement Disorders
 Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Long-term outcome of subthalamic nucleus deep brain stimulation for Parkinson s disease using an MRI-guided and MRI-verified approach
 RESEARCH PAPER Long-term outcome of subthalamic nucleus deep brain stimulation for Parkinson s disease using an MRI-guided and MRI-verified approach Iciar Aviles-Olmos, Zinovia Kefalopoulou, Elina Tripoliti,
RESEARCH PAPER Long-term outcome of subthalamic nucleus deep brain stimulation for Parkinson s disease using an MRI-guided and MRI-verified approach Iciar Aviles-Olmos, Zinovia Kefalopoulou, Elina Tripoliti,
Therapeutic efficacy of unilateral subthalamotomy in Parkinson s disease: results in 89 patients followed for up to 36 months
 See Editorial Commentary, p 939 1 Movement Disorders, Functional Neurosurgery and Neurophysiology Units, Centro Internacional de Restauración Neurológica (CIREN), La Habana, Cuba; 2 Department of Neurology
See Editorial Commentary, p 939 1 Movement Disorders, Functional Neurosurgery and Neurophysiology Units, Centro Internacional de Restauración Neurológica (CIREN), La Habana, Cuba; 2 Department of Neurology
Pallidal versus Subthalamic Deep-Brain Stimulation for Parkinson s Disease
 original article Pallidal versus Subthalamic Deep-Brain for Parkinson s Disease Kenneth A. Follett, M.D., Ph.D., Frances M. Weaver, Ph.D., Matthew Stern, M.D., Kwan Hur, Ph.D., Crystal L. Harris, Pharm.D.,
original article Pallidal versus Subthalamic Deep-Brain for Parkinson s Disease Kenneth A. Follett, M.D., Ph.D., Frances M. Weaver, Ph.D., Matthew Stern, M.D., Kwan Hur, Ph.D., Crystal L. Harris, Pharm.D.,
Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease
 CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE
 11 th Bienniel Speech Motor Control Conference, Colonial Williamsburg, Virginia, 2002. THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE Steven Barlow,
11 th Bienniel Speech Motor Control Conference, Colonial Williamsburg, Virginia, 2002. THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE Steven Barlow,
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Bilateral deep brain stimulation (DBS) has become
 technical note J Neurosurg 125:85 89, 2016 Simultaneous bilateral stereotactic procedure for deep brain stimulation implants: a significant step for reducing operation time Erich Talamoni Fonoff, MD, PhD,
technical note J Neurosurg 125:85 89, 2016 Simultaneous bilateral stereotactic procedure for deep brain stimulation implants: a significant step for reducing operation time Erich Talamoni Fonoff, MD, PhD,
ELECTRICAL STIMULATION OF THE SUBTHALAMIC NUCLEUS IN ADVANCED PARKINSON S DISEASE
 ELECTRICAL OF THE SUBTHALAMIC NUCLEUS IN ADVANCED PARKINS S DISEASE ELECTRICAL OF THE SUBTHALAMIC NUCLEUS IN ADVANCED PARKINS S DISEASE PATRICIA LIMOUSIN, M.D., PAUL KRACK, M.D., PIERRE POLLAK, M.D., ABDELHAMID
ELECTRICAL OF THE SUBTHALAMIC NUCLEUS IN ADVANCED PARKINS S DISEASE ELECTRICAL OF THE SUBTHALAMIC NUCLEUS IN ADVANCED PARKINS S DISEASE PATRICIA LIMOUSIN, M.D., PAUL KRACK, M.D., PIERRE POLLAK, M.D., ABDELHAMID
doi: /brain/awr121 Brain 2011: 134;
 doi:10.1093/brain/awr121 Brain 2011: 134; 2074 2084 2074 BRAIN A JOURNAL OF NEUROLOGY Parkinson s disease progression at 30 years: a study of subthalamic deep brain-stimulated patients Aristide Merola,
doi:10.1093/brain/awr121 Brain 2011: 134; 2074 2084 2074 BRAIN A JOURNAL OF NEUROLOGY Parkinson s disease progression at 30 years: a study of subthalamic deep brain-stimulated patients Aristide Merola,
Neurobehavioral disturbances constitute an important
 Differential Effects of L-Dopa and Subthalamic Stimulation on Depressive Symptoms and Hedonic Tone in Parkinson s Disease Karsten Witt, M.D. Christine Daniels, M.D. Jan Herzog, M.D. Delia Lorenz, M.D.
Differential Effects of L-Dopa and Subthalamic Stimulation on Depressive Symptoms and Hedonic Tone in Parkinson s Disease Karsten Witt, M.D. Christine Daniels, M.D. Jan Herzog, M.D. Delia Lorenz, M.D.
SUPPLEMENTAL DIGITAL CONTENT
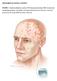 SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
Deep Brain Stimulation
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Expectation and the Placebo Effect in Parkinson s Disease Patients With Subthalamic Nucleus Deep Brain Stimulation
 EXPECTATION AND PLACEBO EFFECT 1457 Expectation and the Placebo Effect in Parkinson s Disease Patients With Subthalamic Nucleus Deep Brain Stimulation Rodrigo Mercado, MD, 1 Constantine Constantoyannis,
EXPECTATION AND PLACEBO EFFECT 1457 Expectation and the Placebo Effect in Parkinson s Disease Patients With Subthalamic Nucleus Deep Brain Stimulation Rodrigo Mercado, MD, 1 Constantine Constantoyannis,
Indications. DBS for Tremor. What is the PSA? 6/08/2014. Tremor. 1. Tremor. 2. Gait freezing/postural instability. 3. Motor fluctuations
 Indications Deep brain stimulation for Parkinson s disease A Tailored Approach 1. Tremor 2. Gait freezing/postural instability Wesley Thevathasan FRACP DPhil.Oxf 3. Motor fluctuations Consultant Neurologist,
Indications Deep brain stimulation for Parkinson s disease A Tailored Approach 1. Tremor 2. Gait freezing/postural instability Wesley Thevathasan FRACP DPhil.Oxf 3. Motor fluctuations Consultant Neurologist,
Rapid assessment of gait and speech after subthalamic deep brain stimulation
 SNI: Stereotactic, a supplement to Surgical Neurology International OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor Antonio A. F. DeSalles, MD University of California,
SNI: Stereotactic, a supplement to Surgical Neurology International OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor Antonio A. F. DeSalles, MD University of California,
POSTOPERATIVE PATIENT MANAGEMENT
 POSTOPERATIVE PATIENT MANAGEMENT INTRODUCTION Deep brain stimulation of the internal globus pallidus (GPi) or the subthalamic nucleus (STN) effectively reduces parkinsonian motor symptoms and alleviates
POSTOPERATIVE PATIENT MANAGEMENT INTRODUCTION Deep brain stimulation of the internal globus pallidus (GPi) or the subthalamic nucleus (STN) effectively reduces parkinsonian motor symptoms and alleviates
Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic surgery
 ISPUB.COM The Internet Journal of Neuromonitoring Volume 7 Number 1 Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic
ISPUB.COM The Internet Journal of Neuromonitoring Volume 7 Number 1 Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic
Deep brain stimulation (DBS) has been
 TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Do Stable Patients With a Premorbid Depression History Have a Worse Outcome After Deep Brain Stimulation for Parkinson Disease? Michael
TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Do Stable Patients With a Premorbid Depression History Have a Worse Outcome After Deep Brain Stimulation for Parkinson Disease? Michael
WHAT DEFINES YOPD? HANDLING UNIQUE CONCERNS REBECCA GILBERT, MD, PHD VICE PRESIDENT, CHIEF SCIENTIFIC OFFICER, APDA MARCH 14, 2019
 WHAT DEFINES YOPD? HANDLING UNIQUE CONCERNS REBECCA GILBERT, MD, PHD VICE PRESIDENT, CHIEF SCIENTIFIC OFFICER, APDA MARCH 14, 2019 YOUNG ONSET PARKINSON S DISEASE Definition: Parkinson s disease diagnosed
WHAT DEFINES YOPD? HANDLING UNIQUE CONCERNS REBECCA GILBERT, MD, PHD VICE PRESIDENT, CHIEF SCIENTIFIC OFFICER, APDA MARCH 14, 2019 YOUNG ONSET PARKINSON S DISEASE Definition: Parkinson s disease diagnosed
10/13/2017. Disclosures. Deep Brain Stimulation in the Treatment of Movement Disorders. Deep Brain Stimulation: Objectives.
 Deep Brain Stimulation in the Treatment of Movement Disorders Disclosures None Eleanor K Orehek, M.D. Movement Disorders Specialist Noran Neurological Clinic 1 2 Objectives To provide an overview of deep
Deep Brain Stimulation in the Treatment of Movement Disorders Disclosures None Eleanor K Orehek, M.D. Movement Disorders Specialist Noran Neurological Clinic 1 2 Objectives To provide an overview of deep
2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Measure #294: Parkinson s Disease: Parkinson s Disease Medical and Surgical Treatment Options Reviewed National Quality Strategy Domain: Communication and Care Coordination 2017 OPTIONS FOR INDIVIDUAL
Measure #294: Parkinson s Disease: Parkinson s Disease Medical and Surgical Treatment Options Reviewed National Quality Strategy Domain: Communication and Care Coordination 2017 OPTIONS FOR INDIVIDUAL
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
A major aim in the management of advanced Parkinson s
 396 PAPER Use and interpretation of on/off diaries in Parkinson s disease J Reimer, M Grabowski, O Lindvall, P Hagell... See end of article for authors affiliations... Correspondence to: Peter Hagell,
396 PAPER Use and interpretation of on/off diaries in Parkinson s disease J Reimer, M Grabowski, O Lindvall, P Hagell... See end of article for authors affiliations... Correspondence to: Peter Hagell,
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS)
 Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
E ssential tremor is a commonly diagnosed movement
 684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence
684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence
Deep Brain Stimulation. Is It Right for You?
 Deep Brain Stimulation Is It Right for You? Northwestern Medicine Deep Brain Stimulation What is DBS? Northwestern Medicine Central DuPage Hospital is a regional destination for the treatment of movement
Deep Brain Stimulation Is It Right for You? Northwestern Medicine Deep Brain Stimulation What is DBS? Northwestern Medicine Central DuPage Hospital is a regional destination for the treatment of movement
Deep Brain Stimulation
 Deep Brain Stimulation Policy Number: 7.01.63 Last Review: 8/2017 Origination: 8/2001 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for deep brain
Deep Brain Stimulation Policy Number: 7.01.63 Last Review: 8/2017 Origination: 8/2001 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for deep brain
Intraoperative microelectrode recording (MER) for targeting during deep brain stimulation (DBS) procedures 巴黎第六大学医学院生理学
 Intraoperative microelectrode recording (MER) for targeting during deep brain stimulation (DBS) procedures 巴黎第六大学医学院生理学 Paris 6 University (Pierre-et-Marie-Curie) Medical school physiology department 皮度
Intraoperative microelectrode recording (MER) for targeting during deep brain stimulation (DBS) procedures 巴黎第六大学医学院生理学 Paris 6 University (Pierre-et-Marie-Curie) Medical school physiology department 皮度
Over the last 20 years, Deep Brain Stimulation (DBS)
 Deep Brain Stimulation in Parkinson s Disease: Past, Present, and Future Though it has been underutilized over the past two decades, deep brain stimulation is an effective intervention for many individuals
Deep Brain Stimulation in Parkinson s Disease: Past, Present, and Future Though it has been underutilized over the past two decades, deep brain stimulation is an effective intervention for many individuals
Deep brain stimulation in Parkinson s disease
 Therapeutic Advances in Neurological Disorders Review Deep brain stimulation in Parkinson s disease S. J. Groiss, L. Wojtecki, M. Südmeyer and A. Schnitzler Abstract: During the last 15 years deep brain
Therapeutic Advances in Neurological Disorders Review Deep brain stimulation in Parkinson s disease S. J. Groiss, L. Wojtecki, M. Südmeyer and A. Schnitzler Abstract: During the last 15 years deep brain
Short term surgical complications after subthalamic deep brain stimulation for Parkinson s disease: does old age matter?
 Levi et al. BMC Geriatrics (2015) 15:116 DOI 10.1186/s12877-015-0112-2 RESEARCH ARTICLE Open Access Short term surgical complications after subthalamic deep brain stimulation for Parkinson s disease: does
Levi et al. BMC Geriatrics (2015) 15:116 DOI 10.1186/s12877-015-0112-2 RESEARCH ARTICLE Open Access Short term surgical complications after subthalamic deep brain stimulation for Parkinson s disease: does
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Deep brain stimulation for the treatment of Parkinson s disease: subthalamic nucleus versus globus pallidus internus
 464 Department of Neurology, University of Heidelberg, INF 4, 6912 Heidelberg, Germany M Krause W Fogel W Hacke Department of Neurosurgery A Heck M Bonsanto V Tronnier Max Planck Institute of Psychiatry,
464 Department of Neurology, University of Heidelberg, INF 4, 6912 Heidelberg, Germany M Krause W Fogel W Hacke Department of Neurosurgery A Heck M Bonsanto V Tronnier Max Planck Institute of Psychiatry,
Citation for the original published paper (version of record):
 http://www.diva-portal.org This is the published version of a paper published in Journal of Parkinson's Disease. Citation for the original published paper (version of record): Hariz, M. (2017) My 25 Stimulating
http://www.diva-portal.org This is the published version of a paper published in Journal of Parkinson's Disease. Citation for the original published paper (version of record): Hariz, M. (2017) My 25 Stimulating
Unilateral Subthalamic Nucleus Stimulation in the Treatment of Asymmetric Parkinson s Disease with Early Motor Complications
 DOI: 10.5137/1019-5149.JTN.14894-15.0 Received: 09.05.2015 / Accepted: 08.07.2015 Published Online: 13.04.2016 Original Investigation Unilateral Subthalamic Nucleus Stimulation in the Treatment of Asymmetric
DOI: 10.5137/1019-5149.JTN.14894-15.0 Received: 09.05.2015 / Accepted: 08.07.2015 Published Online: 13.04.2016 Original Investigation Unilateral Subthalamic Nucleus Stimulation in the Treatment of Asymmetric
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD
 PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
Cell transplantation in Parkinson s disease
 Cell transplantation in Parkinson s disease Findings by SBU Alert Published September 18, 2001 Revised November 7, 2003 Version 2 Technology and target group: In Parkinsons disease, the brain cells that
Cell transplantation in Parkinson s disease Findings by SBU Alert Published September 18, 2001 Revised November 7, 2003 Version 2 Technology and target group: In Parkinsons disease, the brain cells that
What contributes to quality of life in patients with Parkinson s disease?
 308 Department of Neurology, Institute of Neurology, Queen Square, London WC1N 3BG, UK A Schrag M Jahanshahi N Quinn Correspondence to: Professor NP Quinn n.quinn@ion.ucl.ac.uk Received 2 Sepyember 1999
308 Department of Neurology, Institute of Neurology, Queen Square, London WC1N 3BG, UK A Schrag M Jahanshahi N Quinn Correspondence to: Professor NP Quinn n.quinn@ion.ucl.ac.uk Received 2 Sepyember 1999
A Funkiewiez, C Ardouin, E Caputo, P Krack, V Fraix, H Klinger, S Chabardes, K Foote, A-L Benabid, P Pollak...
 834 PAPER Long term effects of bilateral subthalamic nucleus stimulation on cognitive function, mood, and behaviour in Parkinson s disease A Funkiewiez, C Ardouin, E Caputo, P Krack, V Fraix, H Klinger,
834 PAPER Long term effects of bilateral subthalamic nucleus stimulation on cognitive function, mood, and behaviour in Parkinson s disease A Funkiewiez, C Ardouin, E Caputo, P Krack, V Fraix, H Klinger,
Topic: Deep Brain Stimulation Date of Origin: April Section: Surgery Approved Date: April Policy No: 84 Effective Date: July 1, 2014
 Medical Policy Manual Topic: Deep Brain Stimulation Date of Origin: April 1998 Section: Surgery Approved Date: April 2014 Policy No: 84 Effective Date: July 1, 2014 IMPORTANT REMINDER Medical Policies
Medical Policy Manual Topic: Deep Brain Stimulation Date of Origin: April 1998 Section: Surgery Approved Date: April 2014 Policy No: 84 Effective Date: July 1, 2014 IMPORTANT REMINDER Medical Policies
Neurosurgery 61[ONS Suppl 2]:ONS346 ONS357, 2007
![Neurosurgery 61[ONS Suppl 2]:ONS346 ONS357, 2007 Neurosurgery 61[ONS Suppl 2]:ONS346 ONS357, 2007](/thumbs/91/105469457.jpg) Yasin Temel, M.D., Ph.D. Department of Neurosurgery, University Hospital Maastricht, and European Graduate School of Neuroscience, Poldi Wilbrink, M.D. Department of Neurosurgery, University Hospital Maastricht,
Yasin Temel, M.D., Ph.D. Department of Neurosurgery, University Hospital Maastricht, and European Graduate School of Neuroscience, Poldi Wilbrink, M.D. Department of Neurosurgery, University Hospital Maastricht,
The effects of deep brain stimulation on sleep in Parkinson s disease
 Therapeutic Advances in Neurological Disorders Review The effects of deep brain stimulation on sleep in Parkinson s disease Amy W. Amara, Ray L. Watts and Harrison C. Walker Ther Adv Neurol Disord (2011)
Therapeutic Advances in Neurological Disorders Review The effects of deep brain stimulation on sleep in Parkinson s disease Amy W. Amara, Ray L. Watts and Harrison C. Walker Ther Adv Neurol Disord (2011)
NEUROLOGICAL REVIEW SECTION EDITOR: DAVID E. PLEASURE, MD. Deep Brain Stimulation for Parkinson Disease
 NEUROLOGICAL REVIEW ONLINE FIRST SECTION EDITOR: DAVID E. PLEASURE, MD Deep Brain Stimulation for Parkinson Disease An Expert Consensus and Review of Key Issues Jeff M. Bronstein, MD, PhD; Michele Tagliati,
NEUROLOGICAL REVIEW ONLINE FIRST SECTION EDITOR: DAVID E. PLEASURE, MD Deep Brain Stimulation for Parkinson Disease An Expert Consensus and Review of Key Issues Jeff M. Bronstein, MD, PhD; Michele Tagliati,
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA.
 Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
Clinimetrics, clinical profile and prognosis in early Parkinson s disease Post, B.
 UvA-DARE (Digital Academic Repository) Clinimetrics, clinical profile and prognosis in early Parkinson s disease Post, B. Link to publication Citation for published version (APA): Post, B. (2009). Clinimetrics,
UvA-DARE (Digital Academic Repository) Clinimetrics, clinical profile and prognosis in early Parkinson s disease Post, B. Link to publication Citation for published version (APA): Post, B. (2009). Clinimetrics,
Trajectory of Quality of Life in Advanced Parkinson's Patients Receiving Bilateral Subthalamic Nucleus Deep Brain Stimulation
 University of Denver Digital Commons @ DU Electronic Theses and Dissertations Graduate Studies 8-1-2009 Trajectory of Quality of Life in Advanced Parkinson's Patients Receiving Bilateral Subthalamic Nucleus
University of Denver Digital Commons @ DU Electronic Theses and Dissertations Graduate Studies 8-1-2009 Trajectory of Quality of Life in Advanced Parkinson's Patients Receiving Bilateral Subthalamic Nucleus
MRI guided STN DBS in Parkinson s disease without microelectrode recording: efficacy and safety.
 MRI guided STN DBS in Parkinson s disease without microelectrode recording: efficacy and safety. Thomas Foltynie, Ludvic Zrinzo, Irene Martinez-Torres, Elina Tripoliti, Erika Petersen, Etienne Holl, Iciar
MRI guided STN DBS in Parkinson s disease without microelectrode recording: efficacy and safety. Thomas Foltynie, Ludvic Zrinzo, Irene Martinez-Torres, Elina Tripoliti, Erika Petersen, Etienne Holl, Iciar
Surgical Treatment: Patient Edition
 Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Name of Policy: Deep Brain Stimulation
 Name of Policy: Deep Brain Stimulation Policy #: 347 Latest Review Date: June 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross and
Name of Policy: Deep Brain Stimulation Policy #: 347 Latest Review Date: June 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross and
Deep Brain Stimulation for Parkinson s Disease: Recent Trends and Future Direction
 REVIEW ARTICLE Neurol Med Chir (Tokyo) 55, 422 431, 2015 doi: 10.2176/nmc.ra.2014-0446 Online April 28, 2015 Deep Brain Stimulation for Parkinson s Disease: Recent Trends and Future Direction Chikashi
REVIEW ARTICLE Neurol Med Chir (Tokyo) 55, 422 431, 2015 doi: 10.2176/nmc.ra.2014-0446 Online April 28, 2015 Deep Brain Stimulation for Parkinson s Disease: Recent Trends and Future Direction Chikashi
Deep Brain Stimulation of the Subthalamic Nucleus and Cognitive Functions in Parkinson s Disease
 315) Deep Brain Stimulation of the Subthalamic Nucleus and Cognitive Functions in Parkinson s Disease Klempířová O. 1,2, Jech R. 1, Urgošík D. 3, Klempíř J. 1, Špačková N. 1, Roth J. 1, Růžička E. 1 1
315) Deep Brain Stimulation of the Subthalamic Nucleus and Cognitive Functions in Parkinson s Disease Klempířová O. 1,2, Jech R. 1, Urgošík D. 3, Klempíř J. 1, Špačková N. 1, Roth J. 1, Růžička E. 1 1
Activa RC and Activa PC
 Activa RC and Activa PC neurostimulators for deep brain stimulation From the company with the most experience in DBS The Activa Family Innovative programming platform More choices for patients With the
Activa RC and Activa PC neurostimulators for deep brain stimulation From the company with the most experience in DBS The Activa Family Innovative programming platform More choices for patients With the
Validity and Efficacy of Screening Algorithms for Assessing Deep Brain Stimulation Candidacy in Parkinson s Disease
 RESEARCH ARTICLE CLINICAL PRACTICE Validity and Efficacy of Screening Algorithms for Assessing Deep Brain Stimulation Candidacy in Parkinson s Disease Robert R. Coleman, MD, 1,2 Vikas Kotagal, MD, MS,
RESEARCH ARTICLE CLINICAL PRACTICE Validity and Efficacy of Screening Algorithms for Assessing Deep Brain Stimulation Candidacy in Parkinson s Disease Robert R. Coleman, MD, 1,2 Vikas Kotagal, MD, MS,
Deep brain stimulation for Parkinson s disease :Panikar D, Kishore A, Neurololy India
 Page 1 of 10 Home REVIEW ARTICLE Year : 2003 Volume : 51 Issue : 2 Page : 167--175 Deep brain stimulation for Parkinson s disease Panikar D, Kishore A Comprehensive Care Center for Movement Disorders,
Page 1 of 10 Home REVIEW ARTICLE Year : 2003 Volume : 51 Issue : 2 Page : 167--175 Deep brain stimulation for Parkinson s disease Panikar D, Kishore A Comprehensive Care Center for Movement Disorders,
Ablative procedures for the treatment of Parkinson s disease
 Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association.
 Deep Brain Stimulation Page 1 of 31 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association. Title: Deep Brain Stimulation Professional Institutional Original Effective Date:
Deep Brain Stimulation Page 1 of 31 Medical Policy An Independent Licensee of the Blue Cross and Blue Shield Association. Title: Deep Brain Stimulation Professional Institutional Original Effective Date:
Deep Brain Stimulation for Parkinson s Disease and Other Movement Disorders
 Ontario Health Technology Assessment Series 005; Vol. 5, No. Deep Brain Stimulation for Parkinson s Disease and Other Movement Disorders An Evidence-Based Analysis March 005 Medical Advisory Secretariat
Ontario Health Technology Assessment Series 005; Vol. 5, No. Deep Brain Stimulation for Parkinson s Disease and Other Movement Disorders An Evidence-Based Analysis March 005 Medical Advisory Secretariat
Deep brain stimulation in the treatment of dyskinesia and dystonia
 Neurosurg Focus 17 (1):E2, 2004, Click here to return to Table of Contents Deep brain stimulation in the treatment of dyskinesia and dystonia HIROKI TODA, M.D., PH.D., CLEMENT HAMANI, M.D., PH.D., AND
Neurosurg Focus 17 (1):E2, 2004, Click here to return to Table of Contents Deep brain stimulation in the treatment of dyskinesia and dystonia HIROKI TODA, M.D., PH.D., CLEMENT HAMANI, M.D., PH.D., AND
Deep Brain Stimulation
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Linköping University Post Print. Patient-specific models and simulations of deep brain stimulation for postoperative follow-up
 inköping University Post Print Patient-specific models and simulations of deep brain stimulation for postoperative follow-up Mattias Åström, Elina Tripoliti, Irene Martinez-Torres, udvic U. Zrinzo, Patricia
inköping University Post Print Patient-specific models and simulations of deep brain stimulation for postoperative follow-up Mattias Åström, Elina Tripoliti, Irene Martinez-Torres, udvic U. Zrinzo, Patricia
ASSFN Clinical Case: Bilateral STN DBS Implant for Parkinson s Disease
 ASSFN Clinical Case: Bilateral STN DBS Implant for Parkinson s Disease Parkinson s Disease Cardinal Signs: Resting tremor Rigidity Bradykinesia Postural instability Other Symptoms Dystonia Dysphagia Autonomic
ASSFN Clinical Case: Bilateral STN DBS Implant for Parkinson s Disease Parkinson s Disease Cardinal Signs: Resting tremor Rigidity Bradykinesia Postural instability Other Symptoms Dystonia Dysphagia Autonomic
