One 8 -shaped scleral suture to treat rhegmatogenous retinal detachment: a refined procedure of minimal scleral buckling
|
|
|
- Samantha Underwood
- 6 years ago
- Views:
Transcription
1 One 8 -shaped scleral suture to treat rhegmatogenous retinal detachment: a refined procedure of minimal scleral buckling H.Y. Min, D. Chen, Y. Chen and F.T. Dong Department of Ophthalmology, Peking Union Medical College Hospital, Chinese Academy of Medical Sciences & Peking Union Medical College, Beijing, China Corresponding author: H.Y. Min hycdcn@126.com Genet. Mol. Res. 13 (3): (2014) Received May 17, 2013 Accepted October 22, 2013 Published August 28, 2014 DOI ABSTRACT. The aim of this study was to investigate the outcomes of one 8 -shaped scleral suture of minimal scleral buckling (MSB) surgery without sub-retinal drainage for rhegmatogenous retinal detachment (RRD) treatment. Thirty patients (30 eyes) with RRD were recruited. Thirty eyes with RRD were repaired by one 8 -shaped scleral suture of minimal buckling without subretinal drainage by one surgeon. The refined MSB procedure is described. Reattachment time and best-corrected visual acuity (BCVA) were observed. The age of the 30 patients ranged from 17 to 65 years (mean, 43.1 ± 8.6 years). The retinas of 19 eyes (63.3%) reattached within 12 h of the operations, and those of 11 eyes (67%) reattached within 72 h. The average time of follow-up was 10.4 ± 2.8 months. BCVAs were increased in 27 eyes (90%), whereas those of 3 eyes did not change. The mean preoperative BCVA was ± log minimal angle of resolution (MAR), and mean postoperative BCVA was ± logmar, and the difference was statistically significant (P < 0.05). The sponge for buckling in only one eye exposed from the conjunctiva was taken out,
2 H.Y. Min et al and the retina remained attached. In conclusion, an 8 -shaped scleral suture of MSB without sub-retinal drainage is an efficient procedure to treat selected RRD cases. Key words: Best-corrected visual acuity; Minimal scleral buckling; Rhegmatogenous retinal detachment INTRODUCTION Rhegmatogenous retinal detachment (RRD) is characterized by one or more breaks or tears in the neurosensory retina with drainage of fluid into the subretinal space from the vitreous cavity. RRD is the most common cause of retinal detachment and greatly threatens visual acuity. The revolutionized success of a 50% reattachment rate was achieved by Juleus Gonin based on the theory of closing the break (Rumpf, 1976). In the 1950s, Schepens and colleagues introduced the scleral buckling (SB) technique for retinal detachment, which achieved higher anatomical and functional success (Schepens, 1951; Schepens et al., 1957). This classical and well-established procedure is widely applied for treating RRD, and the average reattachment rate reaches up to 90%. However, severe complications do occur due to the wide buckle range, such as severe surgical trauma, diplopia, astigmatism, perforation of the eyeball, and infarction of the choroid, among others. Therefore, a method for decreasing the severity and high frequency of complications of SB is worth exploring. Minimal scleral buckle (MSB) without sub-retinal drainage for RRD treatment was first developed by Lincoff and Kreissig on the basis of the Custodis methods (Lincoff and Kreissig, 1972). This method has been regarded as by far the best external-route surgery for which the key point is to buckle the breach only for RRD (Rezaei and Abrams, 2005). MSB is characterized by a simplified procedure, minimal surgical trauma, less and moderate complications, and better recovery, and has therefore been gradually accepted by surgeons. However, it is difficult to define the minimal extent of MSBs. It may depend not only on the case itself, but also on the specific surgeon performing the procedure. During the operation, the surgeon always intentionally or unintentionally expands the buckle range in order to ensure that the hole or tears are on the scleral crest regardless of the size of the hole or tears (Kreissig et al., 1995; Schimel et al., 2012). Here, a refined MSB procedure without subretinal drainage was established, and the results of consecutively treating 30 eyes with RRD using this kind of surgery were investigated from January 2007 to September 2012 in the Peking Union Medical College Hospital. MATERIAL AND METHODS Study design From January 2007 to September 2012, consecutive patients were recruited in the Peking Union Medical College Hospital who matched the following criteria: 1) simple RRD with only one hole or tear, 2) no fixed retinal folds, and proliferative vitreoretinopathy (PVR) less than C1, 3) the position of the hole or tear was located within a 4 disc diameter (DD) around the equator, and 4) the size of the retinal hole or tear was less than 2 DD. Patients with
3 A refined procedure of minimal scleral buckling 6667 macular holes, giant retinal tears, retinal dialysis, multiple holes or tears, or PVR over C2 were excluded. The study was performed with approval of the Peking Union Medical College Hospital ethics committee. All patients provided informed consent before inclusion in the study and after the nature of the study had been explained. The study adhered to the tenets of the Declaration of Helsinki. Examinations After admission in the ward, antibiotic eye drops were administrated for 3 days before surgery. Bilateral lacrimal ducts were flushed with saline water. The accurate locations of the holes or tears were determined after dilation of the pupil with indirect ophthalmoscope (IO) and a three-mirror universal diagnostic lens. The sizes of the holes or tears were measured by DD. All of the retinal changes or lesions were illustrated. Surgical techniques During surgery, after retrobulbar anesthesia with lidocaine hydrochloride and bupivacaine, a T -shaped conjunctive incision was made only in the quadrant affected by the hole or tear. The sclera was exposed just enough to facilitate the location of the holes or tears. Not all of the rectus muscles were necessarily distracted by sutures. If needed, the inserted point of the muscle on the sclera was only distracted by teeth forceps to rotate the eyeball. If the hole or tears were located around the rectus muscle, it was the only one distracted by the suture in order to expose the scleral area for buckling. Using the IO, the corresponding scleral site of the retinal hole or tears was determined and marked with a Meilan marker pen. Scleral cryotherapy around the hole was applied. Subsequently, an 8 -shaped suture was tightly applied to fix the 7-mm silicone sponge buckle, which was counter-pointed to the center of the hole or tears with a 5-0 nylon stitch (Figures 1 and 2). The tie was tightened and turned to the lower edge of the sponge to prevent exposure and extrusion of the conjunctiva. Figure 1. Rhegmatogenous retinal detachment (RRD) with a round hole treated by one 8 shaped scleral suture. A. RRD with a round hole and its flap (black arrow) before surgery. B. Buckle of the 8 -shaped scleral suture intraoperatively. The 8 -shaped suture (black arrow) holds the radial short silicone sponge on the surface of the sclera behind the equator. There is about 18 mm from the location of the hole to the limbus (empty arrow). C. Retina reattaches. There are laser spots around the hole after laser photocoagulation and the flap recovers the hole (black arrow).
4 H.Y. Min et al Figure 2. Rhegmatogenous retinal detachment (RRD) with a horse-toe tear treated by one 8 shaped scleral suture. A. RRD with a 2DD tear and its flap (black arrow) before surgery. B. The 8 -shaped scleral buckle intraoperatively. The 8 -shaped suture (black arrow) holds the radial short silicone sponge on the surface of the sclera behind the equator. There is about 10 mm from the location of the hole to the limbus (empty arrow). C. Retina reattaches. The tear is located against the scleral crest. The flap of the tear re-closes by the force of the scleral indentation (black arrow). Then, reassurance of the contraposition of the hole against the scleral crest was accomplished using the IO. If the positions were far from each other or if the hole or tear was not on the crest, the silicone sponge was re-sewn or shifted according to the proper site. If the hole or tear was confirmed to be on the crest, the conjunctive incision was sewed up, and antibiotics solution and dexamethasone were injected beneath the conjunctiva. Statistical analysis For statistical analysis, Snellen visual acuity (VA) measures were converted to a logarithmic scale, i.e. logarithm of the minimum angle of resolution (logmar). Statistical analysis comparing the means of the preoperative VA and postoperative VA was performed using oneway analysis of variance. RESULTS Patients and preoperative findings There were 30 eyes (30 cases) with primary RRD that fulfilled the inclusion criteria as outlined above. The age of the patients ranged from 17 to 65 years (mean, 43.1 ± 8.6 years). There were 17 male (56.7%) and 13 female patients (43.3%) included. A total of 18 patients (60%) were operated on the right eye and 12 (40%) on the left eye. There were 16 horseshoe tears and 14 round or oval holes. All of the tears were located in the superior or superior-temporal quadrants. Six of the holes were located in the inferior-temporal quadrant, and the rest were located on the superior or superior-nasal or temporal quadrants. Anatomical results Of the 30 patients, the retinas of 15 (50%) patients reattached clinically by indirect ophthalmoscope in 24 h, those of 10 (33.3%) patients reattached in 48 h, and those of 5
5 A refined procedure of minimal scleral buckling 6669 (16.7%) patients reattached in one week. All of the breaks or tears lay against the scleral crest. The axis of the buckling sponge was radial in 21 eyes (70%) and was horizontal or arc-shaped in the others (30%). No sub-retinal fluid drainage was needed for any of the patients. Functional results After 6 months of follow-up, the best-corrected visual acuity (BCVA) in 27 eyes increased, and those of the other 3 eyes were unchanged. The mean preoperative VA (in log- MAR) was ± 0.368, and the mean postoperative BCVA (in logmar) was ± 0.278, and the difference was statistically significant (P < 0.05). Complications No significant intra-operative complications, such as sub-retinal hemorrhage or incarceration, occurred in any of the 30 eyes. Two weeks after the operation, there was only one patient whose sponge was exposed from the infra-temporal conjunctiva. Because the fundus recovered well, the sponge was taken off immediately to prevent potential infection. The retina maintained its position after 8 months of follow-up. DISCUSSION MSB, originally proposed by Lincoff and Kreissig, has been the preferred external procedure for treating RRDs for at least 40 years; however, it is hard to delineate the exact size of minimal buckling for a specific case. This depends on the case itself and on the routines of the surgeon himself (Lincoff and Kreissig, 1972; Kreissig et al., 1995; Lincoff and Kreissig, 2000; Rezaei and Abrams, 2005; Hanyi et al., 2011; Schimel et al., 2012). In general, retina specialists intentionally expand the range of the buckling to increase the rate of the first operation, and at least two sutures are favored. On the basis of our previously reported experience with MSB for RRDs (Hanyi et al., 2011), we here applied a refined MSB procedure using one 8 -shaped scleral suture to treat primary RRDs. In this series, a 7-mm wide silicone sponge was fixed with a 6-0 nylon suture in an 8 shape, and the distance between the stitch and the edge of the sponge was less than 1 mm on each side. Theoretically, the maximal diameter of the crest indenting into the vitreous cavity would be at least 7 mm. This range should cover most of the retinal breaks, which are less than 2 DD or 3 mm in diameter (Laatikainen and Tolppanen, 1985; Coffee et al., 2007; Daling et al., 2008). According to the size or the height of the retina hole or tear, the scleral depth indented or the height of the crest would be modified by the tightness of the suture, the width of the sponge, and the width of the suture. If the size of the hole or tear is large, tighter sutures would be applied to increase the height of the crest, and consequently, the diameter of the crest would increase. Furthermore, if the hole or tear is small, we could also tailor the sponge to be narrower in order to match the size. The length of the sponge can be adjusted according to the length and the axis of the hole or tears, especially for horse-toe tears. In our experience, the length of the sponge was generally less than 10 mm, which was sufficient for sealing the hole or tears. The 30 eyes of recruited patients were buckled by this procedure, and all of the retinas
6 H.Y. Min et al reattached after buckling within less than 72 h. During surgery, the surgical trauma to the eyeball was decreased substantially. First, the incision of the conjunctiva was T -shaped, which was limited to only the quadrant with the hole or tear. Second, the rectus muscles were not distracted by the sutures in order to expose the sclera. The corresponding scleral site of the hole or tear was exposed to be wide enough only by rotation of the eyeball by gently stretching the insertion of the muscles with forceps. With the application of all of these modified and refined procedures, the MSB shows merit in reducing the incidence of surgical injuries, is easier and quicker to perform, and results in more rapid recovery. In some cases, 20 min was sufficient to perform the MSB. In our review, only one scleral suture to hold the sponge against the sclera was the most refined MSB procedure to treat such an RRD, which has not been reported before. It is necessary to expand this kind of modified and refined MSB. Of course, due to the limited width of the crest by a single 8 -shaped suture, we established strict inclusion criteria, as described above. Biasing this patient sample guaranteed a higher success rate. With additional experience, the indications of a single 8 suture will be expanded to some degree. Although sub-retinal drainage procedure has not been applied for many years, the mechanism of absorption of the subretinal fluid remains controversial (Hammer, 1981; Mester et al., 2002). In two physical models, Clemens et al. (1987) and Foster et al. (2010) suggested that liquid laminar and Bernoulli effects will be formed after the hole or tears are buckled, prompting the sub-retinal fluid to flow back to the vitreous cavity. Furthermore, they indicated that rapid eye movement could help the outflow of the subretinal fluid into the vitreous cavity. It was unnecessary to fix the eyeball or limit the movement of the contra-lateral eye to promote the sub-retinal fluid absorption. In our series, no case was operated with sub-retinal drainage and the sub-retinal fluids in most of the patients were absorbed the following day. The longest duration of sub-retinal fluid was 72 h. The results showed that it was not necessary to drain the fluids below the retina or to block or seal the retinal breaks during the operation. Instead, two conditions were encountered when we performed the traditional surgery, and the intraoperative outcomes were both satisfactory. The first was that although the retina lay against the crest intra-operatively after drainage, in some RRDs, the retina detached post-operatively. The second was that the retina on the plateau of the crest stayed detached while the post-crest retina was attached. However, using this new method, neither of these conditions was encountered. The outcomes showed that the wider range of buckling or indentation did not seal or block the fluid more than that of minimal scleral buckling. Liquid laminar and/or Bernoulli effects were not formed in the former condition; therefore, the fluid could not be pumped out, and even the fluid in the vitreous cavity could flow into the sub-retinal space as before. Due to the refined procedure of MSB and the omission of sub-retinal drainage of the fluid, which is the standard operation of classical SB, the overall surgery outcome was greatly improved and the surgical time was also shortened substantially. Most of the surgical durations in our series were approximately 30 min, which is markedly less than the surgery times reported previously (Sagong and Chang, 2010). In this sense, this procedure can shorten or change the learning curve of SB. Since a primary vitrectomy with a 20 G probe was first applied for RRD in 1985, (Escoffery et al., 1985), 25 G or 27 G probes have been employed more recently for treating such RRDs. However, the primary choice, vitrectomy or MSB, remains controversial (Schwartz and Flynn, 2006; Sun et al., 2012). A recent meta-analysis (Sun et al., 2012; Soni et al., 2013)
7 A refined procedure of minimal scleral buckling 6671 found no significant differences in the proportions of primary reattachment and postoperative BCVA after 6 months or more in pseudophakic/aphakic eyes, whereas SB-treated phakic eyes showed better postoperative BCVAs after 6 months or more. In our series, besides the virtues of SB, a refined MSB protocol was established, which features a shorter surgical time, less incision size, and minimal surgical trauma. In conclusion, the refined one 8 -shaped suture of scleral buckling without sub-retinal drainage was verified to be an efficient procedure for treating selected RRDs. This procedure is an excellent example of minimally invasive segmental buckling. REFERENCES Clemens S, Kroll P, Stein E, Wagner W, et al. (1987). Experimental studies on the disappearance of subretinal fluid after episcleral buckling procedures without drainage. Graefes Arch. Clin. Exp. Ophthalmol. 225: Coffee RE, Westfall AC, Davis GH, Mieler WF, et al. (2007). Symptomatic posterior vitreous detachment and the incidence of delayed retinal breaks: case series and meta-analysis. Am. J. Ophthalmol. 144: Daling X, Wen L, Min H and Tong L (2008). Clinical observation of intravitreal dispersion of retinal pigment epithelium cells during external approach microsurgery of retinal detachment. Chin. J. Pract. Ophthalmol. 26. Escoffery RF, Olk RJ, Grand MG and Boniuk I (1985). Vitrectomy without scleral buckling for primary rhegmatogenous retinal detachment. Am. J. Ophthalmol. 99: Foster WJ, Dowla N, Joshi SY and Nikolaou M (2010). The fluid mechanics of scleral buckling surgery for the repair of retinal detachment. Graefes Arch. Clin. Exp. Ophthalmol. 248: Hammer ME (1981). Retinal re-attachment forces created by absorption of subretinal fluid. Doc. Ophthalmol. Proc. Ser. 125: Hanyi M, Jin M and Fei G (2011). Minimal scleral buckling without subretinal drainage for rhegmatogenous retinal detachment. Med. J. PUMCH 2: Kreissig I, Simader E, Fahle M and Lincoff H (1995). Visual acuity after segmental buckling and non-drainage: a 15-year follow-up. Eur. J. Ophthalmol. 5: Laatikainen L and Tolppanen EM (1985). Characteristics of rhegmatogenous retinal detachment. Acta Ophthalmol. 63: Lincoff H and Kreissig I (1972). The treatment of retinal detachment without drainage of subretinal fluid. (Modifications of the Custodis procedure. VI). Trans. Am. Acad. Ophthalmol. Otolaryngol. 76: Lincoff H and Kreissig I (2000). Changing patterns in the surgery for retinal detachment: 1929 to Klin Monbl Augenheilkd 216: Mester U, Anterist N, Kroll P and Brieden-Azvedo S (2002). The role of the vitreous in retinal detachment surgery with external buckling. Ophthalmologica 216: Rezaei KA and Abrams GW (2005). The History of Retinal Detachment Surgery. Kreissig I. Primary Retinal Detachment (option for repair). Springer, New York. Rumpf J (1976). Jules Gonin. Inventor of the surgical treatment for retinal detachment. Surv. Ophthalmol. 21: Sagong M and Chang W (2010). Learning curve of the scleral buckling operation: lessons from the first 97 cases. Ophthalmologica 224: Schepens CL (1951). Progress in detachment surgery. Trans. Am. Acad. Ophthalmol. Otolaryngol. 55: Schepens CL, Okamura ID and Brockhurst RJ (1957). The scleral buckling procedures. I. Surgical techniques and management. AMA Arch. Ophthalmol. 58: Schimel AM, Grand MG and Flynn HW, Jr. (2012). Surgery for retinal detachment: does experience matter? Retina 32: 1-3. Schwartz SG and Flynn HW (2006). Primary retinal detachment: scleral buckle or pars plana vitrectomy? Curr. Opin. Ophthalmol. 17: Soni C, Hainsworth DP and Almony A (2013). Surgical management of rhegmatogenous retinal detachment: a metaanalysis of randomized controlled trials. Ophthalmology 120: Sun Q, Sun T, Xu Y, Yang XL, et al. (2012). Primary vitrectomy versus scleral buckling for the treatment of rhegmatogenous retinal detachment: a meta-analysis of randomized controlled clinical trials. Curr. Eye Res. 37:
Scleral buckling. Surgical Treatment
 Dr. Ayman M. Khattab MD, FRCS professor of Ophthalmology Cairo University Surgical Treatment Pneumatic retinopexy. Primary pars plana vitrectomy. 1 Indications for scleral buckling. SB is used to treat
Dr. Ayman M. Khattab MD, FRCS professor of Ophthalmology Cairo University Surgical Treatment Pneumatic retinopexy. Primary pars plana vitrectomy. 1 Indications for scleral buckling. SB is used to treat
Progressive Symptomatic Retinal Detachment Complicating Retinoschisis. Initial Reporting Questionnaire
 Progressive Symptomatic Retinal Detachment Complicating Retinoschisis In association with the British Ophthalmological Surveillance Unit Ethics ref: 13/NW/0037 Initial Reporting Questionnaire Case Definition:
Progressive Symptomatic Retinal Detachment Complicating Retinoschisis In association with the British Ophthalmological Surveillance Unit Ethics ref: 13/NW/0037 Initial Reporting Questionnaire Case Definition:
Retinal dialysis. procedures. The purpose of the present paper is to report the results of treatment of 62
 Brit. J. Ophthal. (I973) 57, 572 Retinal dialysis A. H. CHIGNELL Moorfields Eye Hospital, City Road, London, E.C. i Retinal dialysis is an important cause of retinal detachment and subsequent reduction
Brit. J. Ophthal. (I973) 57, 572 Retinal dialysis A. H. CHIGNELL Moorfields Eye Hospital, City Road, London, E.C. i Retinal dialysis is an important cause of retinal detachment and subsequent reduction
The Outcome Of 23 Gauge Pars Plana Vitrectomy Without Scleral Buckle For Management Of Rhegmatogenous Retinal Detachment. By:
 The Outcome Of 23 Gauge Pars Plana Vitrectomy Without Scleral Buckle For Management Of Rhegmatogenous Retinal Detachment. By: Mohamed El-Deeb, MD, M.Sc, ICO, FRCS. Vitreoretinal Consultant, Magrabi Eye
The Outcome Of 23 Gauge Pars Plana Vitrectomy Without Scleral Buckle For Management Of Rhegmatogenous Retinal Detachment. By: Mohamed El-Deeb, MD, M.Sc, ICO, FRCS. Vitreoretinal Consultant, Magrabi Eye
Scleral Buckling under a Slit-lamp Illumination System with a Contact Wide-angle Viewing Lens Compared with an Indirect Ophthalmoscope
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(2):126-133 https://doi.org/10.3341/kjo.2017.0092 Original Article Scleral Buckling under a Slit-lamp Illumination System with a Contact Wide-angle
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(2):126-133 https://doi.org/10.3341/kjo.2017.0092 Original Article Scleral Buckling under a Slit-lamp Illumination System with a Contact Wide-angle
Failure in retinal detachment surgery
 Brit.J. Ophthal.(I 973) 57, 525 Communications Failure in retinal detachment surgery A. H. CHIGNELL, L. G. FISON, E. W. G. DAVIES, R. E. HARTLEY, AND M. F. GUNDRY Moorfields Eye Hospital, City Road, London
Brit.J. Ophthal.(I 973) 57, 525 Communications Failure in retinal detachment surgery A. H. CHIGNELL, L. G. FISON, E. W. G. DAVIES, R. E. HARTLEY, AND M. F. GUNDRY Moorfields Eye Hospital, City Road, London
Retinal Detachment PATIENT EDUCATION
 Retinal Detachment PATIENT EDUCATION What is Retinal Detachment (RD)? Retina is the light-sensitive layer at the back of the eye that converts light images into nerve impulses that are relayed to the brain
Retinal Detachment PATIENT EDUCATION What is Retinal Detachment (RD)? Retina is the light-sensitive layer at the back of the eye that converts light images into nerve impulses that are relayed to the brain
Scleral Buckling Using a Non-contact Wide-Angle Viewing System with a 25-Gauge Chandelier Endoilluminator
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(6):533-537 https://doi.org/10.3341/kjo.2017.0044 Original Article Scleral Buckling Using a Non-contact Wide-Angle Viewing System with a 25-Gauge
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(6):533-537 https://doi.org/10.3341/kjo.2017.0044 Original Article Scleral Buckling Using a Non-contact Wide-Angle Viewing System with a 25-Gauge
Encircling silicone rod without drainage
 Brit. J. Ophthal. (I 973) 57, 53 7 Encircling silicone rod without drainage for retinal detachment with giant breaks ABDEL-LATIF SIAM Ophthalmology Department, Ain Shams University, Cairo, Egypt Giant
Brit. J. Ophthal. (I 973) 57, 53 7 Encircling silicone rod without drainage for retinal detachment with giant breaks ABDEL-LATIF SIAM Ophthalmology Department, Ain Shams University, Cairo, Egypt Giant
Factors influencing anatomic and visual results in primary scleral buckling
 European Journal of Ophthalmology / Vol. 10 no. 2, 2000 / pp. 153-159 Factors influencing anatomic and visual results in primary scleral buckling H. AHMADIEH, M. ENTEZARI, M. SOHEILIAN, M. AZARMINA, M.H.
European Journal of Ophthalmology / Vol. 10 no. 2, 2000 / pp. 153-159 Factors influencing anatomic and visual results in primary scleral buckling H. AHMADIEH, M. ENTEZARI, M. SOHEILIAN, M. AZARMINA, M.H.
PLACEMENT of a scleral buckle
 CLINICAL SCIENCES Twenty-Year Follow-up for Scleral Buckling Stephen G. Schwartz, MD; Derek P. Kuhl, MD, PhD; Alice R. McPherson, MD; Eric R. Holz, MD; William F. Mieler, MD Objective: To the report 20-year
CLINICAL SCIENCES Twenty-Year Follow-up for Scleral Buckling Stephen G. Schwartz, MD; Derek P. Kuhl, MD, PhD; Alice R. McPherson, MD; Eric R. Holz, MD; William F. Mieler, MD Objective: To the report 20-year
Retinal Tear and Detachment
 Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
Liu-xue-ying Zhong, Yi Du, Wen Liu, Su-Ying Huang, and Shao-chong Zhang. Correspondence should be addressed to Wen Liu;
 BioMed Research International, Article ID 364961, 7 pages http://dx.doi.org/10.1155/2014/364961 Clinical Study Using Surgical Microscope for Sclera Buckling and Transscleral Cryopexy: An Alternative Procedure
BioMed Research International, Article ID 364961, 7 pages http://dx.doi.org/10.1155/2014/364961 Clinical Study Using Surgical Microscope for Sclera Buckling and Transscleral Cryopexy: An Alternative Procedure
Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk cases
 European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
Retinal Detachments
 Retinal Detachments What is a retinal detachment? The retina is the light sensitive layer covering the inside of the back of the eye. It is analogous to the film in a camera. The retina has many layers.
Retinal Detachments What is a retinal detachment? The retina is the light sensitive layer covering the inside of the back of the eye. It is analogous to the film in a camera. The retina has many layers.
SCLERAL BUCKLING OPERATION WITH ROLLED SCLERAL FLAP*
 Brit. J. Ophthal. (1959) 43, 361. SCLERAL BUCKLING OPERATION WITH ROLLED SCLERAL FLAP* BY V. CAVKA Belgrade, Yugoslavia AMONG the various operative procedures carried out for detachment of the retina,
Brit. J. Ophthal. (1959) 43, 361. SCLERAL BUCKLING OPERATION WITH ROLLED SCLERAL FLAP* BY V. CAVKA Belgrade, Yugoslavia AMONG the various operative procedures carried out for detachment of the retina,
Clinical Study Exclusive Use of Air as Gas Tamponade in Rhegmatogenous Retinal Detachment
 Hindawi Ophthalmology Volume 2017, Article ID 1341948, 5 pages https://doi.org/10.1155/2017/1341948 Clinical Study Exclusive Use of Air as Gas Tamponade in Rhegmatogenous Retinal Detachment Kang Yeun Pak,
Hindawi Ophthalmology Volume 2017, Article ID 1341948, 5 pages https://doi.org/10.1155/2017/1341948 Clinical Study Exclusive Use of Air as Gas Tamponade in Rhegmatogenous Retinal Detachment Kang Yeun Pak,
Scleral Buckling Surgery after Macula-Off Retinal Detachment
 Scleral Buckling Surgery after Macula-Off Retinal Detachment Worse Visual Outcome after More than 6 Days Roselie M. H. Diederen, MD, 1 Ellen C. La Heij, MD, PhD, 1 Alfons G. H. Kessels, MD, 2 Fleur Goezinne,
Scleral Buckling Surgery after Macula-Off Retinal Detachment Worse Visual Outcome after More than 6 Days Roselie M. H. Diederen, MD, 1 Ellen C. La Heij, MD, PhD, 1 Alfons G. H. Kessels, MD, 2 Fleur Goezinne,
Causes of failure of pneumatic retinopexy
 VOL. 9 NO. PHILIPPINE JOURNAL OF Ophthalmology JULY ORIGINAL ARTICLE - SEPTEMBER 00 Roberto E. Flaminiano, MD Robert T. Sy, MD Milagros H. Arroyo, MD Pearl Tamesis-Villalon, MD Department of Ophthalmology
VOL. 9 NO. PHILIPPINE JOURNAL OF Ophthalmology JULY ORIGINAL ARTICLE - SEPTEMBER 00 Roberto E. Flaminiano, MD Robert T. Sy, MD Milagros H. Arroyo, MD Pearl Tamesis-Villalon, MD Department of Ophthalmology
Late-onset Retinal Detachment Associated with Regressed Retinopathy of Prematurity
 Late-onset Retinal Detachment Associated with Regressed Retinopathy of Prematurity Hiroko Terasaki*, and Tatsuo Hirose* *Schepens Retina Associates, Schepens Eye Research Institute, Harvard Medical School,
Late-onset Retinal Detachment Associated with Regressed Retinopathy of Prematurity Hiroko Terasaki*, and Tatsuo Hirose* *Schepens Retina Associates, Schepens Eye Research Institute, Harvard Medical School,
Outcome of primary rhegmatogenous retinal detachment surgery in a tertiary referral centre in Northern Ireland A regional study
 Ulster Med J 2017;86(1):15-19 Clinical Paper Outcome of primary rhegmatogenous retinal detachment surgery in a tertiary referral centre in Northern Ireland A regional study Michael A Mikhail 1, George
Ulster Med J 2017;86(1):15-19 Clinical Paper Outcome of primary rhegmatogenous retinal detachment surgery in a tertiary referral centre in Northern Ireland A regional study Michael A Mikhail 1, George
Vitrectomy Combined with Scleral Buckling in Patients with Inferior Retinal Breaks
 Original Article Vitrectomy Combined with Scleral Buckling in Patients with Inferior Retinal Breaks Zubair Saleem, Nadeem Riaz, Muhammad Aftab, Muhammad Moin, Muhammad Irfan Karamat, Adeel Chaudhry Pak
Original Article Vitrectomy Combined with Scleral Buckling in Patients with Inferior Retinal Breaks Zubair Saleem, Nadeem Riaz, Muhammad Aftab, Muhammad Moin, Muhammad Irfan Karamat, Adeel Chaudhry Pak
The Efficacy of Fluid-Gas Exchange for the Treatment of Postvitrectomy Retinal Detachment
 Korean Journal of Ophthalmology 2009;23:253-258 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.4.253 The Efficacy of Fluid-Gas Exchange for the Treatment of Postvitrectomy Retinal Detachment Ji Hye Jang, MD,
Korean Journal of Ophthalmology 2009;23:253-258 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.4.253 The Efficacy of Fluid-Gas Exchange for the Treatment of Postvitrectomy Retinal Detachment Ji Hye Jang, MD,
Research Article Scleral Buckling for Rhegmatogenous Retinal Detachment Associated with Pars Planitis
 Ophthalmology Volume 2016, Article ID 4538193, 5 pages http://dx.doi.org/10.1155/2016/4538193 Research Article Scleral Buckling for Rhegmatogenous Retinal Detachment Associated with Pars Planitis Yong-Kyu
Ophthalmology Volume 2016, Article ID 4538193, 5 pages http://dx.doi.org/10.1155/2016/4538193 Research Article Scleral Buckling for Rhegmatogenous Retinal Detachment Associated with Pars Planitis Yong-Kyu
Follow this and additional works at:
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2003 The risk of a new retinal break or detachment following cataract surgery in eyes that had undergone repair
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2003 The risk of a new retinal break or detachment following cataract surgery in eyes that had undergone repair
Scleral buckling versus vitrectomy for primary rhegmatogenous retinal detachment
 Scleral buckling versus vitrectomy for primary rhegmatogenous retinal detachment Aditya Maitray 1, V Jaya Prakash 2 and Dhanashree Ratra 3 1 Fellow, Sri Bhagwan Mahavir Vitreoretinal Services, Sankara
Scleral buckling versus vitrectomy for primary rhegmatogenous retinal detachment Aditya Maitray 1, V Jaya Prakash 2 and Dhanashree Ratra 3 1 Fellow, Sri Bhagwan Mahavir Vitreoretinal Services, Sankara
Tractional detachments
 Retinal detachment: Surgery and post op care Tractional detachments Causes: diabetes, sickle cell, trauma, von Hippel Lindau disease. Sam S. Dahr, M.D. Retina Center of Oklahoma Key principles Remove the
Retinal detachment: Surgery and post op care Tractional detachments Causes: diabetes, sickle cell, trauma, von Hippel Lindau disease. Sam S. Dahr, M.D. Retina Center of Oklahoma Key principles Remove the
Strategy for the Management of Rhegmatogenous Retinal Detachment with Proliferative Vitreoretinopathy
 Original Article Strategy for the Management of Rhegmatogenous Retinal Detachment with Proliferative Vitreoretinopathy Tayyaba Gul Malik, Naeem Ullah, Mian Muhammad Shafiq, Muhammad Khalil Pak J Ophthalmol
Original Article Strategy for the Management of Rhegmatogenous Retinal Detachment with Proliferative Vitreoretinopathy Tayyaba Gul Malik, Naeem Ullah, Mian Muhammad Shafiq, Muhammad Khalil Pak J Ophthalmol
The Foundation. RETINA HEALTH SERIES Facts from the ASRS
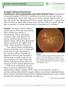 Complex Retinal Detachment: Proliferative Vitreoretinopathy and Giant Retinal Tears Proliferative vitreoretinopathy (PVR) is a condition in which retinal scar tissue, or membranes form; this may occur
Complex Retinal Detachment: Proliferative Vitreoretinopathy and Giant Retinal Tears Proliferative vitreoretinopathy (PVR) is a condition in which retinal scar tissue, or membranes form; this may occur
SCLERAL BUCKLE SURGERY FOR PRIMARY RETINAL DETACHMENT WITHOUT POSTERIOR VITREOUS DETACHMENT
 SCLERAL BUCKLE SURGERY FOR PRIMARY RETINAL DETACHMENT WITHOUT POSTERIOR VITREOUS DETACHMENT JILA NOORI, MD, RICHARD A. BILONICK, PHD, ANDREW W. ELLER, MD Purpose: To present and analyze the anatomical
SCLERAL BUCKLE SURGERY FOR PRIMARY RETINAL DETACHMENT WITHOUT POSTERIOR VITREOUS DETACHMENT JILA NOORI, MD, RICHARD A. BILONICK, PHD, ANDREW W. ELLER, MD Purpose: To present and analyze the anatomical
CLINICAL SCIENCES. for managing primary rhegmatogenous
 CLINICAL SCIENCES Pars Plana Vitrectomy Alone With Diffuse Illumination and Vitreous Dissection to Manage Primary Retinal Detachment With Unseen Breaks Vicente Martínez-Castillo, MD; Anna Boixadera, MD;
CLINICAL SCIENCES Pars Plana Vitrectomy Alone With Diffuse Illumination and Vitreous Dissection to Manage Primary Retinal Detachment With Unseen Breaks Vicente Martínez-Castillo, MD; Anna Boixadera, MD;
Intraoperative Visualization of Peripheral Retina with Wide-Angle Viewing Systems
 Intraoperative Visualization of Peripheral Retina with Wide-Angle Viewing Systems Homayoun Tabandeh, M.D., MS, Francesco Boscia, M.D. 1. Retina -Vitreous Associates Medical Group, Los Angeles, California,
Intraoperative Visualization of Peripheral Retina with Wide-Angle Viewing Systems Homayoun Tabandeh, M.D., MS, Francesco Boscia, M.D. 1. Retina -Vitreous Associates Medical Group, Los Angeles, California,
Scleral Buckling and Pars Plana Vitrectomy versus Vitrectomy alone for Primary Repair of Rhegmatogenous Retinal Detachment
 ORIGINAL ARTICLE Scleral Buckling and Pars Plana Vitrectomy versus Vitrectomy alone for Primary Repair of Rhegmatogenous Retinal Detachment MARIA MEHBOOB 1, MUHAMMAD USMAN GHANI 2, ASMA KHAN 3, MUHAMMAD
ORIGINAL ARTICLE Scleral Buckling and Pars Plana Vitrectomy versus Vitrectomy alone for Primary Repair of Rhegmatogenous Retinal Detachment MARIA MEHBOOB 1, MUHAMMAD USMAN GHANI 2, ASMA KHAN 3, MUHAMMAD
surgery Macular puckers after retinal detachment and loss of the macular reflex with a greyish appearance of the macula
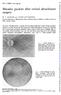 Brit. J. Ophthal. (97 ) 55, 451 Macular puckers after retinal detachment surgery W. S. HAGLER AND UPAL ATURALYA* From the Department of Ophthalmology, Emory University School of Medicine, and Emory University
Brit. J. Ophthal. (97 ) 55, 451 Macular puckers after retinal detachment surgery W. S. HAGLER AND UPAL ATURALYA* From the Department of Ophthalmology, Emory University School of Medicine, and Emory University
Note: This is an outcome measure and will be calculated solely using registry data.
 Measure #384: Adult Primary Rhegmatogenous Retinal Detachment Surgery: No Return to the Operating Room Within 90 Days of Surgery National Quality Strategy Domain: Effective Clinical Care 2017 OPTIONS FOR
Measure #384: Adult Primary Rhegmatogenous Retinal Detachment Surgery: No Return to the Operating Room Within 90 Days of Surgery National Quality Strategy Domain: Effective Clinical Care 2017 OPTIONS FOR
Comparison of Pars Planavitrectomy Versus Combined Pars Planavitrectomy + Encirclage for Primary Repair of Pseudophakic Retinal Detachment
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 1 Ver. 13 January. (2018), PP 35-41 www.iosrjournals.org Comparison of Pars Planavitrectomy
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 1 Ver. 13 January. (2018), PP 35-41 www.iosrjournals.org Comparison of Pars Planavitrectomy
Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
 European Journal of Ophthalmology / Vol. 18 no. 5, 2008 / pp. 848-851 SHORT COMMUNICATIONS & CASE REPORTS Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
European Journal of Ophthalmology / Vol. 18 no. 5, 2008 / pp. 848-851 SHORT COMMUNICATIONS & CASE REPORTS Conjunctival displacement to the corneal side for oblique-parallel insertion in 25-gauge vitrectomy
Pars Plana Vitrectomy Versus Combined Pars Plana Vitrectomy Scleral Buckle for Secondary Repair of Retinal Detachment
 CLINICAL SCIENCE Pars Plana Vitrectomy Versus Combined Pars Plana Vitrectomy Scleral Buckle for Secondary Repair of Retinal Detachment Ryan B. Rush, MD; Matthew P. Simunovic, MB, BChir, PhD; Saumil Sheth,
CLINICAL SCIENCE Pars Plana Vitrectomy Versus Combined Pars Plana Vitrectomy Scleral Buckle for Secondary Repair of Retinal Detachment Ryan B. Rush, MD; Matthew P. Simunovic, MB, BChir, PhD; Saumil Sheth,
Clinical features and surgical management of retinal detachment secondary to round retinal holes
 () 19, 9 & Nature Publishing Group All rights reserved 9-X/ $3. www.nature.com/eye Clinical features and surgical management of retinal detachment secondary to round retinal holes T Ung, MB Comer, AJS
() 19, 9 & Nature Publishing Group All rights reserved 9-X/ $3. www.nature.com/eye Clinical features and surgical management of retinal detachment secondary to round retinal holes T Ung, MB Comer, AJS
Fixing Retinal Detachments Simple and Complex. Avoiding a Dark Day in Surgery
 Fixing Retinal Detachments Simple and Complex Avoiding a Dark Day in Surgery Phakic inferior RD with hole in lattice degeneration and a demarcation line Management? Phakic macula-on RD with lattice degeneration
Fixing Retinal Detachments Simple and Complex Avoiding a Dark Day in Surgery Phakic inferior RD with hole in lattice degeneration and a demarcation line Management? Phakic macula-on RD with lattice degeneration
Late retinal reattachment
 :British Journal of Ophthalmology, 1981, 65, 142-146 Late retinal reattachment S. N. KOKOLAKIS, L. BRAVO, AND A. H. CHIGNELL From the Ophthalmic Department, St Thomas's Hospital, London SEI SUMMARY Six
:British Journal of Ophthalmology, 1981, 65, 142-146 Late retinal reattachment S. N. KOKOLAKIS, L. BRAVO, AND A. H. CHIGNELL From the Ophthalmic Department, St Thomas's Hospital, London SEI SUMMARY Six
Analysis of Changes in Corneal Shape and Refraction Following Scleral Buckling Surgery
 CLINICAL INVESTIGATIONS Analysis of Changes in Corneal Shape and Refraction Following Scleral Buckling Surgery Yuichi Okada, Seigo Nakamura, Eri Kubo, Namiki Oishi, Yukio Takahashi and Yoshio Akagi Department
CLINICAL INVESTIGATIONS Analysis of Changes in Corneal Shape and Refraction Following Scleral Buckling Surgery Yuichi Okada, Seigo Nakamura, Eri Kubo, Namiki Oishi, Yukio Takahashi and Yoshio Akagi Department
Retinal detachment When to see a doctor How retinal detachment occurs
 Retinal detachment Retinal detachment describes an emergency situation in which a thin layer of tissue (the retina) at the back of the eye pulls away from its normal position. Retinal detachment separates
Retinal detachment Retinal detachment describes an emergency situation in which a thin layer of tissue (the retina) at the back of the eye pulls away from its normal position. Retinal detachment separates
Postoperative Perfluro-N-Octane tamponade for complex retinal detachment surgery
 Bangladesh Med Res Counc Bull 2014; 40: 63-69 Postoperative Perfluro-N-Octane tamponade for complex retinal detachment surgery Reza Ali T Department of Ophthalmology (Vitreo-Retina), Bangabandhu Sheikh
Bangladesh Med Res Counc Bull 2014; 40: 63-69 Postoperative Perfluro-N-Octane tamponade for complex retinal detachment surgery Reza Ali T Department of Ophthalmology (Vitreo-Retina), Bangabandhu Sheikh
Anina Abraham, Consultant, Swarup Eye Centre, Hyderabad, India. The author has no financial interests
 Reduced Incidence of Sclerotomy Related Breaks during 23-Gauge Vitrectomy Anina Abraham, Consultant, Swarup Eye Centre, Hyderabad, India The author has no financial interests Introduction Sclerotomy related
Reduced Incidence of Sclerotomy Related Breaks during 23-Gauge Vitrectomy Anina Abraham, Consultant, Swarup Eye Centre, Hyderabad, India The author has no financial interests Introduction Sclerotomy related
Fixing Retinal Detachments Simple and Complex. Avoiding a Dark Day in Surgery
 Fixing Retinal Detachments Simple and Complex Avoiding a Dark Day in Surgery Phakic inferior RD with hole in lattice degeneration and a demarcation line Management? Phakic macula-on RD with lattice degeneration
Fixing Retinal Detachments Simple and Complex Avoiding a Dark Day in Surgery Phakic inferior RD with hole in lattice degeneration and a demarcation line Management? Phakic macula-on RD with lattice degeneration
JUVENILE RHEGMATOGENOUS RETINAL DETACHMENT IN MALAYSIA
 Med. J. Malaysia Vol. 41 No. 2 June 1986 JUVENILE RHEGMATOGENOUS RETINAL DETACHMENT IN MALAYSIA MOHINDER SINGH SUMMARY 45 patients (50 eyes) were treated for juvenile rhegmatogenous retinal detachments
Med. J. Malaysia Vol. 41 No. 2 June 1986 JUVENILE RHEGMATOGENOUS RETINAL DETACHMENT IN MALAYSIA MOHINDER SINGH SUMMARY 45 patients (50 eyes) were treated for juvenile rhegmatogenous retinal detachments
Information for Patients. Retinal Detachment
 Information for Patients Retinal Detachment Manchester Royal Eye Hospital Retinal services Your eye doctor has told you that you have a retinal detachment. This leaflet will help you understand your condition
Information for Patients Retinal Detachment Manchester Royal Eye Hospital Retinal services Your eye doctor has told you that you have a retinal detachment. This leaflet will help you understand your condition
Surgical Outcomes in Rhegmatogenous Retinal Detachment at Srinagarind Hospital
 Surgical Outcomes in Rhegmatogenous Retinal Detachment at Srinagarind Hospital Yosanan Yospaiboon MD*, Thuss Sanguansak MD*, Tanapat Ratanapakorn MD*, Suthasinee Sinawat MD* * Department of Ophthalmology
Surgical Outcomes in Rhegmatogenous Retinal Detachment at Srinagarind Hospital Yosanan Yospaiboon MD*, Thuss Sanguansak MD*, Tanapat Ratanapakorn MD*, Suthasinee Sinawat MD* * Department of Ophthalmology
Visual recovery after macula-off retinal detachment
 Eye (2002) 16, 440 446 2002 Nature Publishing Group All rights reserved 0950-222X/02 $25.00 www.nature.com/eye CAMBRIDGE OPHTHALMOLOGICAL SYMPOSIUM Department of Ophthalmology University of British Columbia
Eye (2002) 16, 440 446 2002 Nature Publishing Group All rights reserved 0950-222X/02 $25.00 www.nature.com/eye CAMBRIDGE OPHTHALMOLOGICAL SYMPOSIUM Department of Ophthalmology University of British Columbia
Impact of Age on Scleral Buckling Surgery for Rhegmatogenous Retinal Detachment
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(4):328-335 https://doi.org/10.3341/kjo.2016.0024 Original Article Impact of Age on Scleral Buckling Surgery for Rhegmatogenous Retinal Detachment
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(4):328-335 https://doi.org/10.3341/kjo.2016.0024 Original Article Impact of Age on Scleral Buckling Surgery for Rhegmatogenous Retinal Detachment
A retrospective nonrandomized study was conducted at 3
 Department of Ophthalmology, Kangbuk Samsung Hospital, Sungkyunkwan University College of Medicine 1, Seoul, Korea Hangil Eye Hospital 2, Incheon, Korea Seoul National University Bundang Hospital 3, Seongnam,
Department of Ophthalmology, Kangbuk Samsung Hospital, Sungkyunkwan University College of Medicine 1, Seoul, Korea Hangil Eye Hospital 2, Incheon, Korea Seoul National University Bundang Hospital 3, Seongnam,
Evaluation of Primary Surgical Procedures for Retinal Detachment with Macular Hole in Highly Myopic Eyes
 Evaluation of Primary Surgical Procedures for Retinal Detachment with Macular Hole in Highly Myopic Eyes A Randomized Comparison of Vitrectomy versus Posterior Episcleral Buckling Surgery Guido Ripandelli,
Evaluation of Primary Surgical Procedures for Retinal Detachment with Macular Hole in Highly Myopic Eyes A Randomized Comparison of Vitrectomy versus Posterior Episcleral Buckling Surgery Guido Ripandelli,
AIR VERSUS GAS TAMPONADE IN RHEGMATOGENOUS RETINAL DETACHMENT WITH INFERIOR BREAKS AFTER 23-GAUGE PARS PLANA VITRECTOMY
 AIR VERSUS GAS TAMPONADE IN RHEGMATOGENOUS RETINAL DETACHMENT WITH INFERIOR BREAKS AFTER 23-GAUGE PARS PLANA VITRECTOMY A Prospective, Randomized Comparative Interventional Study CHUANDI ZHOU, MD, QINGHUA
AIR VERSUS GAS TAMPONADE IN RHEGMATOGENOUS RETINAL DETACHMENT WITH INFERIOR BREAKS AFTER 23-GAUGE PARS PLANA VITRECTOMY A Prospective, Randomized Comparative Interventional Study CHUANDI ZHOU, MD, QINGHUA
Comparison of Pneumatic Retinopexy and Scleral Buckle for Primary Rhegmatogenous Retinal Detachment Repair
 CLINICAL SCIENCE Comparison of Pneumatic Retinopexy and Scleral Buckle for Primary Rhegmatogenous Retinal Detachment Repair Yannis M. Paulus, MD; Loh-Shan Leung, MD; Svetlana Pilyugina, MD; Mark S. Blumenkranz,
CLINICAL SCIENCE Comparison of Pneumatic Retinopexy and Scleral Buckle for Primary Rhegmatogenous Retinal Detachment Repair Yannis M. Paulus, MD; Loh-Shan Leung, MD; Svetlana Pilyugina, MD; Mark S. Blumenkranz,
Clinical Study Passive Removal of Silicone Oil with Temporal Head Position through Two 23-Gauge Cannulas
 Ophthalmology Volume 2016, Article ID 4182693, 4 pages http://dx.doi.org/10.1155/2016/4182693 Clinical Study Passive Removal of Silicone Oil with Temporal Head Position through Two 23-Gauge Cannulas Zhong
Ophthalmology Volume 2016, Article ID 4182693, 4 pages http://dx.doi.org/10.1155/2016/4182693 Clinical Study Passive Removal of Silicone Oil with Temporal Head Position through Two 23-Gauge Cannulas Zhong
Note: This is an outcome measure and will be calculated solely using MIPS eligible clinician, group, or third party intermediary submitted data.
 Quality ID #384: Adult Primary Rhegmatogenous Retinal Detachment Surgery: No Return to the Operating Room Within 90 Days of Surgery National Quality Strategy Domain: Effective Clinical Care Meaningful
Quality ID #384: Adult Primary Rhegmatogenous Retinal Detachment Surgery: No Return to the Operating Room Within 90 Days of Surgery National Quality Strategy Domain: Effective Clinical Care Meaningful
ARTICLE IN PRESS. Fovea-Sparing Retinal Detachments: Time to Surgery and Visual Outcomes
 Fovea-Sparing Retinal Detachments: Time to Surgery and Visual Outcomes CHARLES C. WYKOFF, WILLIAM E. SMIDDY, TAHIRA MATHEN, STEPHEN G. SCHWARTZ, HARRY W. FLYNN, JR, AND WEI SHI PURPOSE: To study the effect
Fovea-Sparing Retinal Detachments: Time to Surgery and Visual Outcomes CHARLES C. WYKOFF, WILLIAM E. SMIDDY, TAHIRA MATHEN, STEPHEN G. SCHWARTZ, HARRY W. FLYNN, JR, AND WEI SHI PURPOSE: To study the effect
Retinal detachment following surgery for congenital cataract: presentation and outcomes
 (2005) 19, 317 321 & 2005 Nature Publishing Group All rights reserved 0950-222X/05 $30.00 www.nature.com/eye Retinal detachment following surgery for congenital cataract: presentation and outcomes D Yorston,
(2005) 19, 317 321 & 2005 Nature Publishing Group All rights reserved 0950-222X/05 $30.00 www.nature.com/eye Retinal detachment following surgery for congenital cataract: presentation and outcomes D Yorston,
Incidence and Risk Factors of Cystoid Macular Edema after Vitrectomy with Silicone Oil Tamponade for Retinal Detachment
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(3):204-210 https://doi.org/10.3341/kjo.2017.0050 Original Article Incidence and Risk Factors of Cystoid Macular Edema after Vitrectomy with
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(3):204-210 https://doi.org/10.3341/kjo.2017.0050 Original Article Incidence and Risk Factors of Cystoid Macular Edema after Vitrectomy with
Comparison between 23 Gauge and 25 Gauge Pars Plana Vitrectomy for Posterior Segment Disease
 Original Article Comparison between 23 Gauge and 25 Gauge Pars Plana Vitrectomy for Posterior Segment Disease Huma Kayani, Aamir Ahmed, Kashif Jahangir, Hizb-ur-Rehman, Khurram Chauhan Pak J Ophthalmol
Original Article Comparison between 23 Gauge and 25 Gauge Pars Plana Vitrectomy for Posterior Segment Disease Huma Kayani, Aamir Ahmed, Kashif Jahangir, Hizb-ur-Rehman, Khurram Chauhan Pak J Ophthalmol
Secondary management and outcome of massive suprachoroidal hemorrhage
 European Journal of Ophthalmology / Vol. 16 no. 6, 2006 / pp. 835-840 Secondary management and outcome of massive suprachoroidal hemorrhage E. FERETIS, S. MOURTZOUKOS, G. MANGOURITSAS, S.A. KABANAROU,
European Journal of Ophthalmology / Vol. 16 no. 6, 2006 / pp. 835-840 Secondary management and outcome of massive suprachoroidal hemorrhage E. FERETIS, S. MOURTZOUKOS, G. MANGOURITSAS, S.A. KABANAROU,
Quadrantic Partial Thickness Sclerectomy for Treatment of Uveal Effusion Syndrome
 Case Report Quadrantic Partial Thickness Sclerectomy for Treatment of Uveal Effusion Syndrome Muhammad Tariq Khan, Sidrah Riaz, Zaheer ud Din Aqil Qazi Pak J Ophthalmol 2017, Vol. 33, No. 2.....................................................................................................
Case Report Quadrantic Partial Thickness Sclerectomy for Treatment of Uveal Effusion Syndrome Muhammad Tariq Khan, Sidrah Riaz, Zaheer ud Din Aqil Qazi Pak J Ophthalmol 2017, Vol. 33, No. 2.....................................................................................................
Practical Care of the Cataract Patient with Retinal Disease
 Practical Care of the Cataract Patient with Retinal Disease Brooks R. Alldredge, OD, FAAO Kelly L. Cyr, OD, FAAO The Retina Center Eye Associates of New Mexico 4411 The 25 Way NE, Suite 325 Albuquerque,
Practical Care of the Cataract Patient with Retinal Disease Brooks R. Alldredge, OD, FAAO Kelly L. Cyr, OD, FAAO The Retina Center Eye Associates of New Mexico 4411 The 25 Way NE, Suite 325 Albuquerque,
Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients
 Asok Nataraj MS Abstract Aim: - Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients The purpose of this study was to directly compare the outcome, safety and efficacy of the 20G and
Asok Nataraj MS Abstract Aim: - Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients The purpose of this study was to directly compare the outcome, safety and efficacy of the 20G and
Recurrences of retinal detachment after vitreoretinal surgery, and surgical approach
 European Journal of Ophthalmology / Vol. 11 n. 2, 2001 / pp. 166-170 Recurrences of retinal detachment after vitreoretinal surgery, and surgical approach Z. KAPRAN 1, O.M. UYAR 1, V. KAYA 2, K. ELTUTAR
European Journal of Ophthalmology / Vol. 11 n. 2, 2001 / pp. 166-170 Recurrences of retinal detachment after vitreoretinal surgery, and surgical approach Z. KAPRAN 1, O.M. UYAR 1, V. KAYA 2, K. ELTUTAR
Subretinal Fluid Bleb After Successful Scleral Buckling and Cryotherapy for Retinal Detachment
 Subretinal Fluid Bleb After Successful Scleral Buckling and Cryotherapy for Retinal Detachment SE WOONG KANG, JAE HUI KIM, WOO JAE SHIN, AND JONG IN KIM PURPOSE: To determine the characteristics of subretinal
Subretinal Fluid Bleb After Successful Scleral Buckling and Cryotherapy for Retinal Detachment SE WOONG KANG, JAE HUI KIM, WOO JAE SHIN, AND JONG IN KIM PURPOSE: To determine the characteristics of subretinal
Anatomical results and complications after silicone oil removal
 Romanian Journal of Ophthalmology, Volume 61, Issue 4, October-December 2017. pp:261-266 GENERAL ARTICLE Anatomical results and complications after silicone oil removal Brănişteanu Daniel Constantin* **,
Romanian Journal of Ophthalmology, Volume 61, Issue 4, October-December 2017. pp:261-266 GENERAL ARTICLE Anatomical results and complications after silicone oil removal Brănişteanu Daniel Constantin* **,
Surgical outcome of pars plana vitrectomy: a retrospective study in a peripheral tertiary eye care centre of Nepal
 Original article : a retrospective study in a peripheral tertiary eye care centre of Nepal Subedi S 1, Sharma MK 2, Sharma BR 2, Kansakar I 2, Dhakwa K 2, Adhikari RK 2 1.Nepal Eye Hospital, National Academy
Original article : a retrospective study in a peripheral tertiary eye care centre of Nepal Subedi S 1, Sharma MK 2, Sharma BR 2, Kansakar I 2, Dhakwa K 2, Adhikari RK 2 1.Nepal Eye Hospital, National Academy
Prophylaxis of retinal detachment
 Brit. J. Ophthal. (I973) 57, 291 Communications Prophylaxis of retinal detachment A. H. CHIGNELL AND J. SHILLING Moorfields Eye Hospital, City Road, London, E.C. i. The detection of conditions which may
Brit. J. Ophthal. (I973) 57, 291 Communications Prophylaxis of retinal detachment A. H. CHIGNELL AND J. SHILLING Moorfields Eye Hospital, City Road, London, E.C. i. The detection of conditions which may
Central serous chorioretinopathy (CSCR) was
 Case Report 777 Perfluorocarbon Liquid-Assisted External Drainage in the Management of Central Serous Chorioretinopathy with Bullous Serous Retinal Detachment Hung-Chiao Chen, MD; Jau-Der Ho, MD; San-Ni
Case Report 777 Perfluorocarbon Liquid-Assisted External Drainage in the Management of Central Serous Chorioretinopathy with Bullous Serous Retinal Detachment Hung-Chiao Chen, MD; Jau-Der Ho, MD; San-Ni
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 78/ Sept 28, 2015 Page 13570
 SAFETY AND EFFECTIVENESS OF 20G SUTURELESS PARS PLANA VITRECTOMY: A PROSPECTIVE STUDY AT SAROJINI DEVI HOSPITAL, HYDERABAD Rajalingam Vairagyam 1, Karunakar B 2, Pasyanthi B 3, B. Y. Babu Rao 4, Rita Bahadur
SAFETY AND EFFECTIVENESS OF 20G SUTURELESS PARS PLANA VITRECTOMY: A PROSPECTIVE STUDY AT SAROJINI DEVI HOSPITAL, HYDERABAD Rajalingam Vairagyam 1, Karunakar B 2, Pasyanthi B 3, B. Y. Babu Rao 4, Rita Bahadur
Vitrectomy Assisted Pneumatic Retinopexy V.A.P.
 Clinica Oculistica Azienda Ospedaliero-Universitaria Policlinico-Vittorio Emanuele-Santa Marta Catania Direttore : Prof. T. Avitabile Vitrectomy Assisted Pneumatic Retinopexy V.A.P. I. Macchi, C. Rapisarda,
Clinica Oculistica Azienda Ospedaliero-Universitaria Policlinico-Vittorio Emanuele-Santa Marta Catania Direttore : Prof. T. Avitabile Vitrectomy Assisted Pneumatic Retinopexy V.A.P. I. Macchi, C. Rapisarda,
Management of giant retinal tears with vitrectomy and perfluorocarbon liquid postoperatively as a short-term tamponade
 (2017) 31, 1290 1295 2017 Macmillan Publishers Limited, part of Springer Nature. All rights reserved 0950-222X/17 www.nature.com/eye CLINICAL STUDY Management of giant retinal tears with vitrectomy and
(2017) 31, 1290 1295 2017 Macmillan Publishers Limited, part of Springer Nature. All rights reserved 0950-222X/17 www.nature.com/eye CLINICAL STUDY Management of giant retinal tears with vitrectomy and
Repair of retinal detachments associated with giant
 Section Co-Editors: Rohit Ross Lakhanpal, MD; and Jorge A. Fortun, MD eyetube.net A print & video series from the Vit-Buckle Society Giant Retinal Tear Repair A panel discussion with members of the Vit-Buckle
Section Co-Editors: Rohit Ross Lakhanpal, MD; and Jorge A. Fortun, MD eyetube.net A print & video series from the Vit-Buckle Society Giant Retinal Tear Repair A panel discussion with members of the Vit-Buckle
Conservative management of retinal
 Brit. J. Ophthal. (1972) 56, 482 Conservative management of retinal breaks A follow-up study of subsequent retinal detachment E. NEUMANN AND S. HYAMS From the Eye Department of the Rothschild Municipal-Government
Brit. J. Ophthal. (1972) 56, 482 Conservative management of retinal breaks A follow-up study of subsequent retinal detachment E. NEUMANN AND S. HYAMS From the Eye Department of the Rothschild Municipal-Government
Safety of 23 Gauge Transconjunctival Sutureless 3 Port Pars Plana Vitrectomy for Vitreoretinal Diseases
 Original Article Safety of 23 Gauge Transconjunctival Sutureless 3 Port Pars Plana Vitrectomy for Vitreoretinal Diseases Syed Raza Ali Shah, Nadeem Ahmad, Qasim Lateef Chaudry, Chaudary Nasir Ahmad, Asad
Original Article Safety of 23 Gauge Transconjunctival Sutureless 3 Port Pars Plana Vitrectomy for Vitreoretinal Diseases Syed Raza Ali Shah, Nadeem Ahmad, Qasim Lateef Chaudry, Chaudary Nasir Ahmad, Asad
The retina is comprised of
 g Rhegmato PAMELA DALY, CST, SA-C genousretinal DETACHMENTS The retina is comprised of 1.2 million photoreceptors that are responsible for changing light rays into electrical impulses that are carried
g Rhegmato PAMELA DALY, CST, SA-C genousretinal DETACHMENTS The retina is comprised of 1.2 million photoreceptors that are responsible for changing light rays into electrical impulses that are carried
Surgical Results and Visual Outcomes of Vitreous Surgery for Advanced Stages of Retinopathy of Prematurity
 Surgical Results and Visual Outcomes of Vitreous Surgery for Advanced Stages of Retinopathy of Prematurity Toshihiro Kono, Kenji Oshima and Yuki Fuchino Department of Ophthalmology, School of Medicine,
Surgical Results and Visual Outcomes of Vitreous Surgery for Advanced Stages of Retinopathy of Prematurity Toshihiro Kono, Kenji Oshima and Yuki Fuchino Department of Ophthalmology, School of Medicine,
TYPES. Full thickness defect in the sensory retina (break) Secondary to Tumour, Inflammation or a Systemic disease
 Dr.A.Divya Introduction Definition : Retinal deatchment is the separation of the neurosensory retina(nsr) from the retinal pigment epithelium(rpe) ; results in the accumulation of subretinal fluid(srf)
Dr.A.Divya Introduction Definition : Retinal deatchment is the separation of the neurosensory retina(nsr) from the retinal pigment epithelium(rpe) ; results in the accumulation of subretinal fluid(srf)
elevations of the retina
 Brit. j. Ophthal. (I974) 58, 899 Patterns of non-rhegmatogenous elevations of the retina HARVEY LINCOFF New rork AND INGRID KREISSIG Bonn, Germany The purpose of this paper is to point out the differential
Brit. j. Ophthal. (I974) 58, 899 Patterns of non-rhegmatogenous elevations of the retina HARVEY LINCOFF New rork AND INGRID KREISSIG Bonn, Germany The purpose of this paper is to point out the differential
Full-thickness Sclerotomy for Uveal Effusion Syndrome
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(4):294-298 http://dx.doi.org/10.3341/kjo.2013.27.4.294 Full-thickness Sclerotomy for Uveal Effusion Syndrome Case Report Mingui Kong, Jae Hui
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(4):294-298 http://dx.doi.org/10.3341/kjo.2013.27.4.294 Full-thickness Sclerotomy for Uveal Effusion Syndrome Case Report Mingui Kong, Jae Hui
Research Article Surgical and Visual Outcome for Recurrent Retinal Detachment Surgery
 Ophthalmology, Article ID 810609, 6 pages http://dx.doi.org/10.1155/2014/810609 Research Article Surgical and Visual Outcome for Recurrent Retinal Detachment Surgery Constantin Pournaras, 1,2,3 Chrysanthi
Ophthalmology, Article ID 810609, 6 pages http://dx.doi.org/10.1155/2014/810609 Research Article Surgical and Visual Outcome for Recurrent Retinal Detachment Surgery Constantin Pournaras, 1,2,3 Chrysanthi
Royal Berkshire Hospital Dunedin Hospital. Prince Charles Eye Unit Pi Princess Margaret Hospital
 Vitreoretinal Surgery Mr Vaughan Tanner www.tanner-eyes.co.uk eyes Reading Royal Berkshire Hospital Dunedin Hospital Windsor Prince Charles Eye Unit Pi Princess Margaret Hospital Success rates VR surgery
Vitreoretinal Surgery Mr Vaughan Tanner www.tanner-eyes.co.uk eyes Reading Royal Berkshire Hospital Dunedin Hospital Windsor Prince Charles Eye Unit Pi Princess Margaret Hospital Success rates VR surgery
Two-Year Follow-up Study Comparing Primary Vitrectomy with Scleral Buckling for Macula-off Rhegmatogenous Retinal Detachment
 Two-Year Follow-up Study Comparing with for Macula-off Rhegmatogenous Retinal Detachment Yusuke Oshima*,, Shigeki Yamanishi*, Miki Sawa,, Masanobu Motokura*, Seiyo Harino and Kazuyuki Emi* *Department
Two-Year Follow-up Study Comparing with for Macula-off Rhegmatogenous Retinal Detachment Yusuke Oshima*,, Shigeki Yamanishi*, Miki Sawa,, Masanobu Motokura*, Seiyo Harino and Kazuyuki Emi* *Department
ORIGINAL ARTICLE. SURGICAL RESULTS OF PARS PLANA VITRECTOMY COMBINED WITH SMALL INCISION CATARACT SURGERY V.D. Karthigeyan 1
 SURGICAL RESULTS OF PARS PLANA VITRECTOMY COMBINED WITH SMALL INCISION CATARACT SURGERY V.D. Karthigeyan 1 HOW TO CITE THIS ARTICLE: VD Karthigeyan. Surgical results of pars plana vitrectomy combined with
SURGICAL RESULTS OF PARS PLANA VITRECTOMY COMBINED WITH SMALL INCISION CATARACT SURGERY V.D. Karthigeyan 1 HOW TO CITE THIS ARTICLE: VD Karthigeyan. Surgical results of pars plana vitrectomy combined with
SURGICAL VITREORETINAL FELLOWSHIP PROGRAM. UNIVERSITY OF KENTUCKY AND RETINA ASSOCIATES OF KENTUCKY Lexington, Kentucky
 SURGICAL VITREORETINAL FELLOWSHIP PROGRAM UNIVERSITY OF KENTUCKY AND RETINA ASSOCIATES OF KENTUCKY Lexington, Kentucky UK Fellowship Director P. Andrew Pearson, M.D. UK Vitreoretinal Faculty Romulo Albuquerque,
SURGICAL VITREORETINAL FELLOWSHIP PROGRAM UNIVERSITY OF KENTUCKY AND RETINA ASSOCIATES OF KENTUCKY Lexington, Kentucky UK Fellowship Director P. Andrew Pearson, M.D. UK Vitreoretinal Faculty Romulo Albuquerque,
IRIDEX MicroPulse P3: innovative cyclophotocoagulation
 Romanian Journal of Ophthalmology, Volume 61, Issue 2, April-June 2017. pp:107-111 GENERAL ARTICLE IRIDEX MicroPulse P3: innovative cyclophotocoagulation Gavris M. Monica*, Olteanu Ioana*, Kantor Erzsebet*,
Romanian Journal of Ophthalmology, Volume 61, Issue 2, April-June 2017. pp:107-111 GENERAL ARTICLE IRIDEX MicroPulse P3: innovative cyclophotocoagulation Gavris M. Monica*, Olteanu Ioana*, Kantor Erzsebet*,
The incidence of retinal redetachment after Pars plana vitrectomy with 360 endolaser.
 Research Article http://www.alliedacademies.org/case-reports-in-surgery-invasive-procedures/ The incidence of retinal redetachment after Pars plana vitrectomy with 360 endolaser. Ghislaine Peene 1, Jean-François
Research Article http://www.alliedacademies.org/case-reports-in-surgery-invasive-procedures/ The incidence of retinal redetachment after Pars plana vitrectomy with 360 endolaser. Ghislaine Peene 1, Jean-François
TWENTY-FIVE GAUGE PARS PLANA VITRECTOMY IN COMPLEX RETINAL DETACHMENTS ASSOCIATED WITH GIANT RETINAL TEAR
 TWENTY-FIVE GAUGE PARS PLANA VITRECTOMY IN COMPLEX RETINAL DETACHMENTS ASSOCIATED WITH GIANT RETINAL TEAR VINOD KUMAR, MS, DNB, MNAMS, FRCS (GLASG), DEVESH KUMAWAT, MD, ANJU BHARI, MBBS, PARIJAT CHANDRA,
TWENTY-FIVE GAUGE PARS PLANA VITRECTOMY IN COMPLEX RETINAL DETACHMENTS ASSOCIATED WITH GIANT RETINAL TEAR VINOD KUMAR, MS, DNB, MNAMS, FRCS (GLASG), DEVESH KUMAWAT, MD, ANJU BHARI, MBBS, PARIJAT CHANDRA,
Retinal Tears and Detachments
 Retinal Tears and Detachments Understanding Retinal Problems When your eyes are working well, it s easy to take them for granted. But a tear or detachment of your eye s retina (the light-sensing lining
Retinal Tears and Detachments Understanding Retinal Problems When your eyes are working well, it s easy to take them for granted. But a tear or detachment of your eye s retina (the light-sensing lining
CASE PRESENTATION. DR.Sravani 1 st yr PG Dept of Ophthalmology
 CASE PRESENTATION DR.Sravani 1 st yr PG Dept of Ophthalmology Name : X X X X X Age : 50yrs Sex : male Occupation : Farmer Residence : Mothkur CHIEF COMPLAINTS : - Diminision of vision in Right Eye since
CASE PRESENTATION DR.Sravani 1 st yr PG Dept of Ophthalmology Name : X X X X X Age : 50yrs Sex : male Occupation : Farmer Residence : Mothkur CHIEF COMPLAINTS : - Diminision of vision in Right Eye since
Comparison of External Magnet and Intraocular Forceps for Intravitreal Foreign Body Extraction
 Techniques in Ophthalmology 5(1):33 39, 2007 R E T I N A S U R G E R Y Comparison of External Magnet and Intraocular Forceps for Intravitreal Foreign Body Extraction Masoud Soheilian, MD, Abbas Abolhasani,
Techniques in Ophthalmology 5(1):33 39, 2007 R E T I N A S U R G E R Y Comparison of External Magnet and Intraocular Forceps for Intravitreal Foreign Body Extraction Masoud Soheilian, MD, Abbas Abolhasani,
Twenty-Three-Gauge Pars Plana Vitrectomy With Inferior Retinectomy and Postoperative Perfluoro-n-Octane Retention for Retinal Detachment Repair
 ORIGINAL CLINICAL STUDY Twenty-Three-Gauge Pars Plana Vitrectomy With Inferior Retinectomy and Postoperative Perfluoro-n-Octane Retention for Retinal Detachment Repair Ryan B. Rush, MD,* Matthew P. Simunovic,
ORIGINAL CLINICAL STUDY Twenty-Three-Gauge Pars Plana Vitrectomy With Inferior Retinectomy and Postoperative Perfluoro-n-Octane Retention for Retinal Detachment Repair Ryan B. Rush, MD,* Matthew P. Simunovic,
INTRODUCTION METHODS. Trans Am Ophthalmol Soc 2005;103:98-107
 VITRECTOMY FOR THE TREATMENT OF SUBMACULAR HEMORRHAGES FROM MACULAR DEGENERATION: A COMPARISON OF SUBMACULAR HEMORRHAGE/MEMBRANE REMOVAL AND SUBMACULAR TISSUE PLASMINOGEN ACTIVATOR ASSISTED PNEUMATIC DISPLACEMENT
VITRECTOMY FOR THE TREATMENT OF SUBMACULAR HEMORRHAGES FROM MACULAR DEGENERATION: A COMPARISON OF SUBMACULAR HEMORRHAGE/MEMBRANE REMOVAL AND SUBMACULAR TISSUE PLASMINOGEN ACTIVATOR ASSISTED PNEUMATIC DISPLACEMENT
Survey of Surgical Indications and Results of Primary Pars Plana Vitrectomy for Rhegmatogenous Retinal Detachments
 Survey of Surgical Indications and Results of Primary Pars Plana Vitrectomy for Rhegmatogenous Retinal Detachments Yusuke Oshima, Kazuyuki Emi, Masanobu Motokura and Shigeki Yamanishi Department of Ophthalmology,
Survey of Surgical Indications and Results of Primary Pars Plana Vitrectomy for Rhegmatogenous Retinal Detachments Yusuke Oshima, Kazuyuki Emi, Masanobu Motokura and Shigeki Yamanishi Department of Ophthalmology,
Evolution of the management of myopic macular hole retinal detachment in Egypt
 Evolution of the management of myopic macular hole retinal detachment in Egypt by Omar Rashed, M.D. Professor of Ophthalmology Ain Shams University 1 1920 Jules Gonin The father of modern retinal surgery
Evolution of the management of myopic macular hole retinal detachment in Egypt by Omar Rashed, M.D. Professor of Ophthalmology Ain Shams University 1 1920 Jules Gonin The father of modern retinal surgery
Rhegmatogenous retinal detachment (RRD) is commonly
 Air tamponade followed by fundus imaging Clinical Research Air tamponade in retinal detachment surgery followed by ultra-widefield fundus imaging system Qian-Yin Chen 1, Yun-Xia Tang 1, Yan-Qiong He 1,
Air tamponade followed by fundus imaging Clinical Research Air tamponade in retinal detachment surgery followed by ultra-widefield fundus imaging system Qian-Yin Chen 1, Yun-Xia Tang 1, Yan-Qiong He 1,
Quick Referral and Urgent Surgery to Preempt Foveal Detachment in Retinal Detachment Repair
 ORIGINAL CLINICAL STUDY Quick Referral and Urgent Surgery to Preempt Foveal Detachment in Retinal Detachment Repair Wataru Kikushima, MD,* Akira Imai, MD,* Takao Hirano, MD,* Yasuhiro Iesato, MD, PhD,*
ORIGINAL CLINICAL STUDY Quick Referral and Urgent Surgery to Preempt Foveal Detachment in Retinal Detachment Repair Wataru Kikushima, MD,* Akira Imai, MD,* Takao Hirano, MD,* Yasuhiro Iesato, MD, PhD,*
OPTIC DISC PIT Pathogenesis and Management OPTIC DISC PIT
 OPTIC DISC PIT Pathogenesis and Management Abdel-Latif Siam Ain Shams University Cairo Egypt OPTIC DISC PIT Congenital pit is an atypical coloboma usually located on the temporal edge of the disc, associated
OPTIC DISC PIT Pathogenesis and Management Abdel-Latif Siam Ain Shams University Cairo Egypt OPTIC DISC PIT Congenital pit is an atypical coloboma usually located on the temporal edge of the disc, associated
