Confident, modern dysphagia practice. Goals of evaluation. Goals of dysphagia management 1/5/2016. Jay Rosenbek, PhD
|
|
|
- Priscilla Eaton
- 6 years ago
- Views:
Transcription
1 Confident, modern dysphagia practice Jay Rosenbek, PhD Goals of evaluation Discover if anything is wrong Why its wrong if it is What to do about it, when and with whom For how long With what expectations Goals of dysphagia management Safe nutrition Adequate nutrition Enjoyable nutrition Alone or in combinations 1
2 Managing these goals Achieving all three is our dream Often incapable of achieving all three Achieving one may frustrate others So need to be rank ordered for the individual patient In the easiest case the pt will have set the course with advanced directives But many don t have advanced directives One challenge Not all the compensatory or rehabilitative approaches are compatible with all three goals Thickeners may threaten adequacy, enjoyment and even safety Tubes in some may threaten all three Enjoyment may come at the potential expense of safety or adequacy Safety may come at expense of others What s to be done? Run screaming into the night MBA Continue to seek the most solid, data based approach to individual decisions available Self examination of degree to which personal beliefs influence decisions And learn tolerance for ambiguity 2
3 Time to add another Neuroprotection exercises to Slow appearance of signs Slow deterioration Should be standard of practice in many neurodegenerative diseases Here are some specifics Neuroprotection Even in PD results are not unanimous, of course But it looks too promising for us at UF to ignore References Suchowersky et al. (2006). Neurology Smith & Zigmond. (2003). Exper Neurol Yacoubian et al. (2010). Cell death Dis Thus at time of diagnosis referral to SLP for discussion and home program as pt desires is the norm Four parts Our program General exercise such as walking Modest swallow mechanism strengthening As can be done with Expiratory muscle strength training Maximum performance training Range of motion Skill training (target practice) 3
4 Goals for clinicians become trainers of cells Principles Use it or lose it Use it right and improve it Specificity matters Salience matters Time matters Age matters Intensity matters Repetition matters Interference Transference And for muscles must OVERLOAD References Kleim & Jones (2008). Principles of experience dependent neural plasticity: Implications for rehabilitation after brain damage. JSLHR, 51, S225 S238 Rothi et al (2008). Neuroplasticity and rehabilitation research for speech, language, and swallowing. JSLHR, 51, S222 S224 Ludlow et al (2008). Translating principles of neural plasticity into research on speech motor control Raymer et al (2008). Translational research in aphasia: fromneuroscience to neurorehabilitation. JSLHR, 51, S259 S275 Robbins et al (2008). Swallowing and dysphagia rehabilitation: translating principles of neural plasticity into clinically oriented evidence. JSLHR, 51, S276 S300 Conference the brain child of Leslie Gonzalez Rothi Ganguly & Mu ming (2013). Activity dependent neural plasticity from bench to bedside. Neuron, 80, Cramer et al (2011). Harnessing nueroplasticity for clinical applications. Brain, 134, US pitiful shape One patient 254 professional responses Few standardized assessments mostly selfgenerated 47 different treatment suggestions for pt And 90 different treatment combinations Carnaby & Harenberg (2013). Dysphagia, 28,
5 But maybe not hopeless Recent survey of US SLPs 206 SLPs responded with evaluation and treatment recommendations for two patients One with UES dysfunction only Second with UES and pharyngeal weakness Jones et al (2014). Dysphagia, 29, Treatments recommendations 64% for 1 and 88% for two recommended rehabilitation? The milder the less likely to receive rehab? OOOOOPS For one in order of most frequently recommended Shaker Effortful swallow Mendelsohn For two Effortful Shaker Tongue hold So What do you think? Shaker Hard swallow Mendelsohn Make some sense right? Lets look at a patient 5
6 However Hard swallow may be the least direct Traditional covered Head raise Mendelswohn Newer methods Towel tuck Chin tuck against resistance Pt sample for discussion UES relaxes Normal UES opening Anterior superior movement of hyolaryngeal complex in part responsible for opening Intrabolus pressure also critical Reason why tiny boluses sometimes mislead 6
7 Selected muscles including mylohyoid, geniohyoid and anterior belly of diagastric elevate the hyolaryngeal complex Laryngeal structures anterior attachment of UES Comic strip Result With movement of hyolaryngeal complex opening of the UES occurs Failure of this movement compromises UES opening Other forces such as failure to relax can also influence of course Can only infer mechanism with fluoro unless combined with manometry Muscles to treat 7
8 Head raise: The exercise Purpose strengthen the suprahyoid muscles to elevate the hyolaryngeal complex The exercise is described as an isometric/isokinetic exercise Isometric: Strengthening by pushing against another body part or fixed object little lengthening of muscle Isokinetic: Strengthening in which length changes while resistance remains relatively the same biceps curl is classic example Head raise portion fits the definition HERE IS THE WELL KNOWN POSTURE Three, one minute head raises with hold followed by 30 quick raises Candidates Those with failed opening of the UES because of inadequate relaxation Those with inadequate opening of UES because of inadequate movement of hyolaryngeal complex Included are brainstem patients And any neurodegenerative disease in which weakness especially of pharygeal and upper esophageal muscles is present Dystrophy is a classic example 8
9 The technique Lie flat with shoulders against a firm but not uncomfortable surface and then elevate head (only) and look at your feet Then one of two variations Do one to three times in groups of 30 followed by 3 one minute holds separated by one minute Or do the three minute holds followed by 30 quick elevations The technique Duration is six weeks (min) Practice is every day Intensity can vary from one total set per day to three If possible for the pt three sets is preferred In general we do not prescribe the right intensities The data First in normals 31 healthy geriatric volunteers randomized to shaker or sham The Shaker group after six weeks got improved opening of UES and in laryngeal excursion 9
10 More data 19 patients with pyriform residual and aspiration because of reduced UES opening 17 of 19 got good enough to move to oral nutrition from tube Effects were apparently retained And more Another group of mixed patients N=27 tube fed patients 6 weeks of tx All improved All maintained improvement at 12 months Spectacular results The group calls for RCT The group calls for RCT Yep And its now been done on a small basis Logemann et al (2009). A randomized comparison of Shaker exercise with traditional therapy: A preliminary study. Dysphagia, 24,
11 The study N=19 stroke and head neck cancer All aspirating for at least three months Randomized into 6 weeks of Shaker (30 followed by three one minute) Or traditional Supersupraglottic swallow, Mendelsohn Yawn and hold; retract tongue and hold Practiced 5 minutes 10 times/day Results Greatest changes in aspiration in Shaker group Many and significant changes in swallowing physiology (duration measurements primarily) in the other group Study recommendations If aspirating use Shaker If reduced range of pharyngeal movements but no aspiration use the other package 11
12 Even a systematic review Antunes & Lunet (2012). Gerontology, epub Strong support for tx Systematic review Influences Increased anterior movement of larynx UES opening Elimination of several signs of dysphagia Permutations Modifications including modifying the decline Using light padded weights on head to increase the load But no data for either Frailty Challenges Cervical and other spinal issues Cardiac abnormalities Weakness, severe 12
13 Mendelsohn the method Logemann Swallow normally and when you feel your voice box go up grab it with your throat muscles for a count of three before relaxing So is that your instruction? One quick clinical test to see if it is going to be helpful Manually elevate the pts larynx during a swallow Mendelsohn permutations Clinician executes the maneuver while pt is feeling clinicians throat Pt and Cl monitor pt s throats during attempt Cl provides knowledge of performance Repeat and redemonstrate if necessary Use semg Manual resistance may add a strengthening component Mendelsohn when When UES opening is reduced in extent and/or duration When dangerous residual in pyriforms Primarily secondary to reduced anterior and posterior hyolaryngeal movement 13
14 Goals May increase endurance Probably primarily a skill task at first but if done intensively and for a long period of time probably strengthens Resist laryngeal elevation and may turn it into a strengthening task Selected data Bryant (1991). Biofeedback in the treatment of a selected dysphagic patient. Dysphagia, 6, Huckabee & Cannito (1999). Outcomes of swallowing rehabilitation in chronic brainstem dysphagia Dysphagia, 14, Crary et al (2004). Functional benefits of dysphagia therapy Dysphagia, 19, These studies all report semg assisted biofeedback as part of procedure Recent data McCullough et al (2012). Effects of Mendelsohn maneuver post stroke. Top Stroke Rehab, 19, N=18 randomized to Two weeks of treatment followed by two weeks of no treatment Or the reverse Treated twice daily for 45 to 60 minutes with attempt to get 40 and settle for 30 swallows per session 14
15 Findings Duration of hyolaryngeal movement increased during tx and decreased during no treatment Same with duration of UES opening Extent of UES opening increased but not significantly No change in pyriform sinus residuals or aspiration OOOPS Lesson Mendelsohn has physiologic effects But some of the assumed signs of reduced hyolaryngeal and UES activity such as residual may not Thus rethinking the interpretation of some signs in some pts is necessary And combining with other methods may be useful Such as hard swallow, Masako Follow up McCullough & Kim (2013), Dysphagia. Epub ahead of print With same cohort of patients demonstrated improved coordination of swallow structures Peck et al (2010). Cortical activation Laryngoscope, 120, Confirm greater activation of cortical swallowing structures during Mendelsohn and effortful 15
16 Cortical swallow centers Towel tuck Developed clinically a decade ago and seeking money to study Roll up a bath towel Place up against neck under chin SQUEEZE DOWN (isokinetic) Swallow hard Can add Effortful laryngeal valve (grunt) Or get one of these Created as alternative to the more difficult head raise Effects The squeeze may strengthen the suprahyoid muscles critical to opening of UES The hard swallow may condition oral and pharyngeal muscles The valsalva with breath hold may condition larynx 16
17 The method Swallow sip of water if safe Place towel under chin and try to hold it with squeeze and not with hands Swallow hard Rest for seconds Repeat Try for 100 repetitions per day in groups of 4 Six days per week For as long as it takes Sip of water Quick valsalva SQUEEZE Swallow HARD Rest Repeat If adding valsalva How to know if it is working First you pick some symptoms that you know the frequency or severity of We use SWAL QOL symptom profile You make sure pt and caregiver are tuned in You have them keep a diary of instances Usually if method is going to work you will see results in one to six weeks 17
18 Permutation Yoon et al (2014). Chin Tuck Against Resistance. Dysphagia, 29, Effects They say significantly greater muscle activity measured with semg during CTAR than during Shaker Admit to many weaknesses of their study But variations of it may be more appropriate to many frail men and women with dysphagia Now to prepare for other treatments What are requirements for contemporary confident practice? Using the previous case as an example throughout 18
19 Modern practice depends upon Training If extensive And not from the 70s Psyche Tolerance for ambiguity Humility Curiosity Depends on Knowing principles of neruomuscular plasticity Knowing what the methods accomplish Knowing the pattern of swallowing difficulty to be txd Knowing the treatment data Several collections of data Frymark et al (2009). Evidence based systematic review.jrrd, 46, Discussion of their procedures in collecting and evaluating data Wheeler Hegland et al (2009). JRRD, 46, Review of the data on normal Normal groups often used in early days of tx development 19
20 Data in dysphagia Ashford et al (2009). JRRD, 2, Neurologic populations Evidence in support of Chin tuck Side lying Head rotation Mendelsohn Supraglottic Less strong evidence for Effortful Supersupraglottic Other special populations Prophylactic exercise during chemoradiation Can reduce negative effects on muscle and movement Now the standard practice in most advanced medical centers Kotz et al (2012). Arch Otolaryngology The usual package contains the usual suspects Hard swallow, Mendelsohn, Supraglottic, and so on How to judge your education If it emphasized The SLP as a trainer of cells Rehabilitate rather than compensate unless rehab ABSOLUTELY IMPOSSIBLE OR CONTRAINDICATED There are no bad SLPs only bad training 20
21 What would you have done? 55 year old person with PD admitted for infection Referred for swallow and was aspirating Someone recommended feeding tube and not given any rehab or even plan for follow up Not best decision most times A tube is not a treatment A tube will not prevent aspiration A tube once in is very hard to d/c A tube without concomitant rehab even if it is only very gentle is a dangerously incomplete approach to management Compensations Thickened liquids most frequent strategy for managing aspiration risk Garcia et al (2005). Thickened liquids AJSLP, 14, 4 13 Texture modifications are unpalatable and pts are likely to be dehydrated and have reduced nutritional intake Sharpe et al (2007). Thickened fluids.dysphagia, 22,
22 On compensations Need to recognize that our frequent use of compensations such as postures and thickeners Has convinced many non SLPs that they can just use these and save the referral Nothing could be farther from truth Read Logemann et al (2008). JSLHR, 51, That study showed In groups of demented, IPD and demented IPD, that chin tuck and nectar and honey thick were unlikely to reduce aspiration And that individual patients from all three categories reacted idiosyncratically One half of pts received no benefit from any of these compensations Leading authors to recommend we look for other treatments Hear Hear Try rehabilitation and we will talk about other methods including EMST But wait, people say, dementia makes such treatments impossible Depending on amount of dementia yes For active txs but some of our treatments are passive Sensory stimulation in its various forms May be the best choice for the more severely demented 22
23 NPO NPO and tubes or thickened coffee and pureed prunes were the 1970s If pt aspirated on exam Even if pt was at risk for aspiration NOW Know that tubes have risks Altered diets have risks Aspirators will aspirate So its about judging relative risk Clinician s psyche Can never know for sure even about something we once thought was so clear Consider aspiration Not all aspirators get sick So who does and who doesn t Who gets sick? Relationship of aspiration and pneumonia is tentative Martin et al. Dysphagia, 1994 Not all aspirators get sick Only 5 of 26 aspirators got sick Schmidt et al, Dysphagia,
24 Langmore s data Langmore et al, Dysphagia, 1998 Dependent for oral care Number of decayed teeth Number of medications Tube feeding Dependent for feeding Now smoking Multiple medical diagnoses Said another way Risk factors are Cognitive impairment Dependence Lack of mobility Pulmonary and cough compromise Malnutrition/dehydration Immune system compromise Multiple medical diagnoses Use of these in clinic Can include an analysis in your report of the number of these risks pt has Thus providing a data base for decision making And as a way of showing you know that aspiration is a necessary but incomplete reason for pulmonary complications 24
25 Aspirators will aspirate Remember Dysphagia with aspiration necessary but incomplete explanation for most pulmonary illness Making patients NPO will not prevent aspiration Despite all we ve been taught Diet recommendations Clinicians act are taught they know how to choose diet But they do not with any confidence Groher recognized this in the 80s but was ignored Reliability has been confused with validity Two clinicians can often agree on what THEY think a diet should be The proper diet is not what we say it is It is what pt wants and can tolerate Thus Need tolerance for ambiguity More likely to be unsure than sure Unless you ignore the pt and just do what you ve been taught Need to be humble Chance of making a mistake is very high 25
26 Here is a place for confronting ambiguity Decision triggers for NPO Risk of aspiration Aspiration observed on exam Risk of illness from aspiration Illness from aspiration Way to evaluate your practice The first is obviously very conservative The fourth is extreme in the other direction One trigger does not fit all Even for a given pt at different times in course of illness And you can never be for sure you are doing the right thing Modern, confident practice depends on Knowing patient s disease An hypothesis about why each patient is having a swallowing problem based on what you know about disease And about how pulmonary status protection mechanisms might be influenced as rehab is underway or if it is impossible Characteristics of swallowing deficit And how the characteristics of each disease will influence response to treatment And about what method(s) from our substantial array can be expected to address that hypothesized condition or those conditions 26
27 Confine to neurologic disease More than 600 If any one of them alters bulbar or respiratory function then dysphagia can result So how do you cope with several hundred etiologies? You look for commonalities What causes the dysphagia Weakness leading to reduced range and force of movement Abnormal (too much or too little) tone leading to reduced range and force of movement Dyscoordination leading to unpredictable movement control Altered rate (too fast, two slow, too variable) leading to impired timing of movement Adventitious or irregular, unpredictable movements as in chorea leading to poor control of movement Airway protection Two of most critical are tight and timely airway closure And cough 27
28 Characteristics of the dysphagia Highly variable across patients and diseases In most will have some mix of Inadequate bolus flow Misdirection of bolus flow Abnormal timing of bolus flow Characteristics influencing response to treatment Of course severity of dysphagia is one Others are related to Cognition Affect General health Social supports Return to our classification of treatments Treatments can be divided into Compensation and rehabilitation Rehabilitative ones change STRENGTH/ENDURANCE SKILL COMBINATION 28
29 Appropriateness of compensations When rehab is impossible When it will be protracted When patient requests When the effects of a compensation may be superior to those for rehab Useful metaphors for strength, endurance and skill training Strength and endurance txs are the equivalent of weight lifting Skill txs are equivalent to learning to ride a bike Clinical significance Why care? Influences timing of what you expect Influences prognosis And need for and type of follow up 29
30 So lets put all this together to create another treatment plan Lets chose PD cause it is so common and easy to generalize from Wait, wait you say I very seldom see PD Not a problem its mostly not about the disease But the reason(s) for dysphagia which are similar across many different conditions For example, reduced force and range of movement in PD lead to residuals, aspiration and likelihood of aspiration pneumonia Parkinson s disease Caused by loss of dopaminergic neurons in the substantia nigra pars compacta of the basal ganglia Classic characteristics summarized as TRAP Tremor impaired steadiness Rigidity increased tone Akinesia (slow or reduced movement) altered timing Postural instability + weakness although controversial Disease begins in brain stem and ascends the neuroaxis to end in cortex Ref: Braak et al (2004). Cell Tissue Res. Aspiration pneumonia one of three major causes of death 30
31 So called non motor signs Apathy Depression Reduced sense of smell Fatiguability Impaired ability to attend to and evaluate internal cues All can influence response to treatment Signs of dysphagia and reasons Dysphagia usually not an early sign but present in nearly 100% in course of disorder Oral stage inefficiencies in preparing and moving bolus posteriorly Diffuse residual throughout pharynx Oral stage more impaired than pharyngeal until late Penetration/Aspiration Caused by rigidity leading to reduced range and force of movement Compounded by apathy, depression, executive dysfunction, poor ability to monitor So what treatments Specific cause of dysphagia Reduced endurance, sometimes weakness Certainly reduced range of motion What methods do we have to rehabilitate? 31
32 First These patients, like all patients, deserve attempted rehabilitation If you send these patients home with a bunch of compensations you deserve any criticism that comes your way Actually your teachers probably do, because most clinical failures are related to failed education What rehab programs seem best? Respiratory muscle training The tools for accomplishing this training are probably at least in part if done lone and intensively enough strengthening programs Maximum performance training Probably part strengthening and part skill training Furthermore EMST and IMST are the two most likely forms of respiratory muscle training May be along with LSVT or other maximum performance training the most likely methods to be simultaneously helpful for both swallowing and speech Especially if done simultaneously 32
33 EMST Pt blows into a device fitted with a one way spring loaded, pressure release valve Amount of pressure can be controlled Training based on 70% 80% of maximum expiratory pressure Or on clinical judgement Another view This is a good diagram of the device At left end (in this view) is the cap that can be tightened or loosened to influence pressure Training load Can measure maximum inspiratory and expiratory pressures and train at 70 80% of max Using a spirometer Or can set clinically 33
34 Cheek lip press Critical to maximize flow thru mouth Minimize through nose Enhance lip seal Treatment EMST set at 75% of MEP (or clinically) Nose clip and cheek/lip press 25 trials per day in five groups of five I prefer more reps in two groups Five sessions per day is burdensome Five days per week I prefer 6 Five weeks and I prefer 3 months Expiratory Muscle Strength Training (EMST) (e.g., Sapienza, Davenport, & Martin, 2002; Sapienza et al., 2011) 34
35 The Rationale Quiet Breathing Resting Palate Hyoid at rest Device in mouth Elevated Palate Hyoid elevation (Wheeler et al., 2007; Wheeler Hegland et al., 2008) Randomized clinical trial EMST Randomized, prospective, double blinded trial with Hoehn and Yahr 2 4 stages Troche, Okun, Rosenbek, et al (2010) Neurology, 75, Methods Participant Demographics n = 60 Variable Experimental Sham p value Age (8.90) (10.31) Sex 1.17 (0.38) 1.27 (0.45) =male, 2=female 25(M), 5(F) 22(M), 8(F) Hoehn & Yahr 7 (Stage 2) 8 (Stage 2.5) 14 (Stage 3) 1 (Stage 4) 5 (Stage 2) 13 (Stage 2.5) 8 (Stage 3) 4 (Stage 4) UPDRS III Motor (Total) (9.15) (8.51)
36 Methods: Design 4 WKS INTERVENTION Consent Baseline1 EMST n =30 sham n =30 Post measures Prospective, blinded, randomized, sham controlled, clinical trial Randomly assigned to active or sham treatment group Baseline swallow assessment followed by 4 weeks of EMST/sham intervention Post intervention assessment followed completion of treatment arm Outcomes: Maximum Expiratory Pressures Swallowing function Voluntary cough function Results: Swallowing Measures PA Score * EMST SHAM EMST sham 1 Pre Post 1 Pre Post DISPLACEMENT: EMST group: hyoid displacement increased at all measured swallow events significant at: UES opening, UES widest, UES closure Additionally SWAL QOL scores increased significantly for both groups, p=.007 Maximum Expiratory Pressure Results: Maximum Expiratory Pressures cm H2O Experimental Sham Pre Pre Post Post 36
37 Results in words P A scores significantly improved for the tx group 3 tx pts had decline in PA in tx group and 16 in sham SWAL QOL increased in both and most in tx Conclusions Device can be used to treat swallowing in PD Has physiologic and quality of life implications One of first randomized controlled trials in dysphagia, called Level I evidence Don t know durability of results Strengthening likely to require maintenance Especially in degenerative disease Did not use with most severe stage PD Interesting feature Penetration aspiration events were decreased by a tx ostensibly focused on respiratory mechanism Why? Respiratory mechanism bigger contributor to P A than traditionally thought Wider influence of blowing than hypothesized Maybe one active ingredient is effort 37
38 Cough in PD Pitts et al (2009) Utilizing voluntary cough to predict penetration and aspiration Chest, 135, Two findings Voluntary cough predicts penetrating and aspirating PD pts Voluntary cough competence is improved by EMST at the previously discussed frequency and duration Masked facies Data showing that computerized images of facial expression reflect improvement in masked face In mild and moderate patients with PD With caregivers and patients reporting improved communication IMST used Unpublished data by Bowers (2013) Our program one more time 75% of maximum expiratory effort 25 reps divided among at least two sessions Six days per week For 4 to 12 weeks, OR LONGER, depending on response Visit clinic once per week for adjustment and drill 38
39 Contraindications Untreated cardiac abnormalities Untreated HTN Till MD approves post surgery anywhere in body RECALL: this is real exercise Remember the three Three pts had declines in PA performance What do they teach us? Working that out Possibly had too much overload or the wrong duration of tx Had different underlying pathophysiology For now gives us something to say to men and women with PD 90% of a sample got better Need rehab programs Because medical surgical txs often do not help and may hurt Menezes & Melo (2009). J Clin Pharm Ther, 34, Meta analysis, N=5 studies with aspiration as major outcome Levodopa not associated with swallow improvement Merola et al (2011). Brain, 134, of 19 patients developed worsening dysphagia after DBS 39
40 However All these conclusions are in need of replication Wanted to give you a heads up, however Devices being used in vent units to aid weaning Used in voice clinics In professional singing programs With asthmatics And in other environments and populations This train has left the station Worry About The future SLPs are hearing about this Trying it sometimes even unsuccessfully on themselves Are unsuccessful and reject the method Or try unguided with a patient, fail, and reject the method Or they try it without transfer techniques and person gets stronger but nothing else changes Recommendation EMST is not a cure all Will have to be joined by one or more skill treatments But it is a powerful new tool Including for reduced cough, a common sign in a variety of neurodegenerative diseases Because of Neurology publication going to spread into clinics rapidly Clinician training can be accomplished in one day 40
41 IMST Inhalatory muscle strength training Some say this is the preferred modality for those with reduced respiratory support Diaphragm is main muscle Inhalation has substantial influence on exhalation Amount of air and to a degree control of flow For now for sure in cases of diaphragm weakness IMST DEVICE Order from: This device is calibrated for 0 to 40 cm of H2o So good for very weak Use of IMT Notion is to get quick, smooth, deep inhalation using diaphragm Followed by long controlled exhalation These two actions roughly parallel speech breathing especially by some treated dysarthric speakers Need to inhibit exaggerated shoulder raising and other maladaptive responses Use nose plug Systematically increase resistance based on pt performance 41
42 Maximum performance training also appropriate LSVT the most popular but must be certified Exhortation and practice to be loud during production of progressively longer productions of ah Another critical exercise is the increasingly competent and extended production of pitch change on ah or its equivalent, from the lowest to the highest possible pitch Variations of this pitch change idea are part of McNeal Dysphagia Program developed by Crary and colleagues Also requires certification so can t teach LSVT another permutation Farley et al describe the development of a treatment that emphasizes not only getting louder but also making bigger reaching and walking movements They are calling this treatment Big and Loud. It, too, requires certification training The essence of the method is that patients are given intensive practice in walking, reaching and other daily tasks with much extended amplitudes A small N study In PD Decreased oral transit time and reduced tongue rocking Reduced residual in oral stage Improved swallow efficiency El Sharkawi et al (2002). Swallowing and voice effects.j Neuro, Neurosurg Psychia, 72,
43 Interpretation of these findings May have increased range of motion although this was not measured directly Authors say improved nueromuscular control of entire upper aerodigestive tract Also say some oral stage effects may reflect an overflow of effort from the habitual increase in phonatory effort Maximum performance training May influence both skill (learning to use enhanced effort) and endurance The idea is simple: have pt perform quality maximum performance tasks An absolute minimum of 25 per day, five and preferably six days per week Our steps Get pt in best posture usually sitting upright Have pt increase background of effort valsalva Have pt get to best size appropriate inhalation Check that inhalation Then start maximum duration of vowel With attention to consistent airflow, loudness and quality Repeat 43
44 Steps, cont. Cue pt to the sound and feel of this maximum performance mode Carefully monitor for laryngeal hyperfunction, pain, dizziness, other discomfort Have pt get a timer URGE maximum, consistent performance Try to transfer the same intensity and effort to speech using short sentences heavy on plosives Caveat Purely mechanical treatments for dysphagia in both degenerative and non degenerative disease will be less than maximally successful in the long run UNLESS COGNITIVE TASKS ARE INCLUDED THROUGHOUT Treatment is not motor it is cognitive motor How to make cognitive Most important is helping pt become own, best clinician Means planning, evaluating and selfcorrecting Clinician who takes responsibility for these slows patient progress and limits generalization 44
45 Transition Those are the newest of the treatments Lets end with a discussion of tube feeding Some thoughts on tubes Two NHs in South Carolina with 41.8 % of residents on tube in one and 10.7 in other Low Homelike atmosphere Food important part of socialization Trained staff at mealtimes who valued hand feeding Advance care planning with family Palliative care options Mouth as environment Especially important in swallowing Martin DRS, 2012 on both society and Mouth cares Good dentition aids general health and function As does adequate saliva 45
46 Its often most about oral health Yoneyama et al (2002). Oral care reduces pneumonia in older patients in nursing homes. J Am Ger Soc, 50, Prandial aspiration and pneumonia Read Feinberg et al: Dysphagia, 1996 Studied 152 frail, elderly NH residents for up to three years All pts had VFSE and those with objective difficulty had the range of treatment Conclusion Most pneumonae in the institutionalized elderly are believed to be secondary to mircoaspiration of oropharyngeal secretions that have been pathologically colonized Authors specifically say that they do not think those selected for tube feeding were more debilitated than others in the study 46
47 Generalization Prandial aspiration should not be the assumed cause of pneumonia in any patient Among the other causes are aspiration of oral bacteria Aspiration of refluxed or vomited stomach contents Aspiration of blood Colonization may occur in 70 75% of critically ill Evaluation suggestions GERD history, including how well controlled History of vomiting in relation to pulmonary complications Oral health including condition of dentition Whether saliva reduced Quality of oral hygiene Interpretation Make the data convince you that prandial aspiration is the villain 47
48 Treatment Aggressive oral care in both oral and tube fed patients A typical protocol Tooth, tongue and oral mucosa brushing using sponge brush and 0.2% chlorhexidine solution Moisturizing mouth with Biotene OralBalance Salivary gland massage Salivary glands Massage 48
49 Effect 63 elderly bedridden, tube fed in oral care or standard of care (no protocol nor rigid schedule of oral care)..the results of the present study suggest that daily oral care for tube fed patients who do not receive nutrition by mouth reduced the incidence of pneumonia (p. 616) Maeda & Akagi (2014). Dysphagia, 29, Furthermore Similar results for non tube fed and for a variety of different populations Azarpazhooh & Leake (2006). Systematic review of the association between respiratory diseases and oral health. J Peridontol, 77, Also maintaining oral nutrition is a factor STRATEGIES FOR INCREASING ORAL Use strong flavors Use varying types of foods Liquid supplements 2 hours before meal rather than with meal Make food available Lengthen meal time Keep supplements at bedside Pleasant eating environment Ina. Amer Family Phy, 2002, 65,
50 Criteria for tube in elderly Read: Ciocon, Dysphagia, 1990 Malnutrition for five days despite above and attempted finger food delivery Severe dysphagia This may be more acceptable to many practitioners But even here need consent to use non oral ANOTHER APPROACH Marik & Kaplan Chest. Emphasis should be on prevention especially with those having dysphagia Approach Aggressive rehab of the swallow and compensations as appropriate and necessary Aggressive oral hygiene Yoshino et al. JAMA, 2001 Tx cont Tube feeding, short term if significant improvement is expected Ace inhibitors to prevent breakdown of substance P Arai et al, Lancet, 1998 Avoid sedative medication if at all possible 50
51 SLPs and risk N=731 US SLPs queried about tube feeding in dementia Results 42.1 said moderately or well trained 22% knew TF unlikely to prevent aspiration pneumonia 70% still willing to recommend because of presumed limited risk Vitale et al (2011). J. Pain Symptom Management. But here are the potential complications Infection Tube disintegration Clogging Leakage Ileus Larson et al. Gastro, 1987 Aspiration Peritonitis Premature removal Buried button syndrome Gastrocolocutaneous fistula Necrotizing fasciitis Hemorrhage Loser et al, Dig Dis Sci, 1998 Thus there are NO risk free options in dysphagia and that is one reason dysphagia makes for such interesting practice 51
52 Practice is evolving Time to quit The most evolved are most likely to help patients simultaneously toward all three of our swallowing goals And it is only going to get better 52
Main Aspects of the Management of Neurogenic Dysphagia
 Main Aspects of the Management of Neurogenic Dysphagia Mario Prosiegel/München German Society of Neurology (DGN) prosiegel@t-online.de DYSPHAGIA October 8-10, 2015 Pavia, Italy Overview Diagnosis Causal
Main Aspects of the Management of Neurogenic Dysphagia Mario Prosiegel/München German Society of Neurology (DGN) prosiegel@t-online.de DYSPHAGIA October 8-10, 2015 Pavia, Italy Overview Diagnosis Causal
Daniels SK & Huckabee ML (2008). Dysphagia Following Stroke. Muscles of Deglutition. Lateral & Mesial Premotor Area 6. Primary Sensory
 An Overview of Dysphagia in the Stroke Population Stephanie K. Daniels, PhD Michael E. DeBakey VA Medical Center PM & R, Baylor College of Medicine Communication Sciences and Disorders, University of Houston
An Overview of Dysphagia in the Stroke Population Stephanie K. Daniels, PhD Michael E. DeBakey VA Medical Center PM & R, Baylor College of Medicine Communication Sciences and Disorders, University of Houston
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
2013, Bouchat-Laird, N.
 Critical Review: The Effect of Expiratory Muscle Strength Training (EMST) on Dysphagia in individuals with Idiopathic Parkinson s disease. Natasha Bouchat-Laird M.Cl.Sc (SLP) Candidate University of Western
Critical Review: The Effect of Expiratory Muscle Strength Training (EMST) on Dysphagia in individuals with Idiopathic Parkinson s disease. Natasha Bouchat-Laird M.Cl.Sc (SLP) Candidate University of Western
The Clinical Swallow Evaluation: What it can and cannot tell us. Introduction
 The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
Expiratory Muscle Strength Training. (EMST) and Dysphagia
 Expiratory Muscle Strength Training 2015 Adult Swallowing Group NSW Speech Pathology Evidence Based Practice Network Christian Wiley and Kylie Draper Hans Bogaardt - Academic Member (EMST) and Dysphagia
Expiratory Muscle Strength Training 2015 Adult Swallowing Group NSW Speech Pathology Evidence Based Practice Network Christian Wiley and Kylie Draper Hans Bogaardt - Academic Member (EMST) and Dysphagia
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล
 Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
5 Things I Want You to Know About Dysphagia. Prof Maggie-Lee Huckabee The University of Canterbury Rose Centre for Stroke Recovery and Research
 5 Things I Want You to Know About Dysphagia Prof Maggie-Lee Huckabee The University of Canterbury Rose Centre for Stroke Recovery and Research 5 things 1) Why we can t diagnose dysphagia at bedside. 2)
5 Things I Want You to Know About Dysphagia Prof Maggie-Lee Huckabee The University of Canterbury Rose Centre for Stroke Recovery and Research 5 things 1) Why we can t diagnose dysphagia at bedside. 2)
MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring Patricia Bednarik, MS, CCC-SLP, MSCS
 Page 1 MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring, MS, CCC-SLP, MSCS >>Kate Milliken: Welcome to MS Learn Online. I am Kate Milliken. Swallowing is something
Page 1 MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring, MS, CCC-SLP, MSCS >>Kate Milliken: Welcome to MS Learn Online. I am Kate Milliken. Swallowing is something
Dysphagia Treatment: What are We Doing, and Why?
 Dysphagia Treatment: What are We Doing, and Why? ASHA Convention, 2014; Orlando James L. Coyle, Ph.D., CCC SLP, BCS S University of Pittsburgh jcoyle@pitt.edu 1 Treatment 2 Aims, targets and ingredients
Dysphagia Treatment: What are We Doing, and Why? ASHA Convention, 2014; Orlando James L. Coyle, Ph.D., CCC SLP, BCS S University of Pittsburgh jcoyle@pitt.edu 1 Treatment 2 Aims, targets and ingredients
Communication and Swallowing with PSP/CBD. Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist
 Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016
 Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Clinical Swallowing Exam
 Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
SWALLOWING DIFFICULTIES IN HD
 Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Management of Chronic Obstructive Lung Disease
 Management of Chronic Obstructive Lung Disease 慢性阻塞性肺病的治療與護理 Chapter Three Put Yourself in Control LEARNING HELPFUL WAYS TO BREATHE Learning helpful ways to breathe means learning to use your lungs smarter
Management of Chronic Obstructive Lung Disease 慢性阻塞性肺病的治療與護理 Chapter Three Put Yourself in Control LEARNING HELPFUL WAYS TO BREATHE Learning helpful ways to breathe means learning to use your lungs smarter
Airway Protection: Clinical Management of Dysphagia and Dystussia in Neurodegenerative disease
 Airway Protection: Clinical Management of Dysphagia and Dystussia in Neurodegenerative disease Alexandra E. Brandimore, Ph.D. CCC/SLP MESPA Conference April 13, 2019 No conflicts of interest or disclosure
Airway Protection: Clinical Management of Dysphagia and Dystussia in Neurodegenerative disease Alexandra E. Brandimore, Ph.D. CCC/SLP MESPA Conference April 13, 2019 No conflicts of interest or disclosure
NIH T-32 Post-Doctoral Fellow, University of Florida, Departments of Neurology and Physiological Sciences (Fall 2008 Fall 2009)
 KAREN WHEELER HEGLAND, PH.D. WORK ADDRESS: University of Florida Department of Speech Language and Hearing Sciences Box 117420 Gainesville, FL 32611 EDUCATIONAL BACKGROUND: University of Florida, Undergraduate
KAREN WHEELER HEGLAND, PH.D. WORK ADDRESS: University of Florida Department of Speech Language and Hearing Sciences Box 117420 Gainesville, FL 32611 EDUCATIONAL BACKGROUND: University of Florida, Undergraduate
Dysphagia as a Geriatric Syndrome Assessment and Treatment. Ashton Galyen M.A., CCC-SLP St. Vincent Indianapolis Acute Rehabilitation Unit
 Dysphagia as a Geriatric Syndrome Assessment and Treatment Ashton Galyen M.A., CCC-SLP St. Vincent Indianapolis Acute Rehabilitation Unit March 16, 2018 Ashton Galyen, M.A., CCC-SLP Master s degree in
Dysphagia as a Geriatric Syndrome Assessment and Treatment Ashton Galyen M.A., CCC-SLP St. Vincent Indianapolis Acute Rehabilitation Unit March 16, 2018 Ashton Galyen, M.A., CCC-SLP Master s degree in
2013 Charleston Swallowing Conference
 Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Critical Review: Is a chin-down posture more effective than thickened liquids in eliminating aspiration for patients with Parkinson s disease?
 Critical Review: Is a chin-down posture more effective than thickened liquids in eliminating aspiration for patients with Parkinson s disease? Nadia Torrieri, M.Cl.Sc. (SLP) Candidate The Unversity of
Critical Review: Is a chin-down posture more effective than thickened liquids in eliminating aspiration for patients with Parkinson s disease? Nadia Torrieri, M.Cl.Sc. (SLP) Candidate The Unversity of
Swallowing problems. Patient information. Name: Date: Speech and Language Therapist: Reviewed: May 2016 Next review: June 2017 Version 1
 Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
When Eating Becomes A Challenge Dysphagia
 When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
Supporting information leaflet (6): Chest Physiotherapy: Lung Volume Recruitment Techniques and Cough Augmentation (Assisted Cough Techniques)
 Acute Services Division Supporting information leaflet (6): Chest Physiotherapy: Lung Volume Recruitment Techniques and Cough Augmentation (Assisted Cough Techniques) Introduction For many people with
Acute Services Division Supporting information leaflet (6): Chest Physiotherapy: Lung Volume Recruitment Techniques and Cough Augmentation (Assisted Cough Techniques) Introduction For many people with
Sapienza, C.M. (2008, invited). Respiratory muscle strength training. Current Opinion in Otolaryngology and Head and Neck Surgery, 16, 3,
 Pitts, T., Bolser, D., Rosenbek, J., Troche, M., & Sapienza, C. (2008). Voluntary cough production and swallow dysfunction in Parkinson's disease. Dysphagia, 23, 3, 297-301. Epub ahead of print. Cough
Pitts, T., Bolser, D., Rosenbek, J., Troche, M., & Sapienza, C. (2008). Voluntary cough production and swallow dysfunction in Parkinson's disease. Dysphagia, 23, 3, 297-301. Epub ahead of print. Cough
TRANSCRIPT LESSON 01: WHO TAKES THIS COURSE & WHY
 PNMEDICAL PULMONARY AND SPEECH DEVICES 1 of 10 THE BREATHER TM ONE DEVICE MANY THERAPIES TRANSCRIPT LESSON 01: WHO TAKES THIS COURSE & WHY Hi everyone. My name is Carrie. I'll be your guide through this
PNMEDICAL PULMONARY AND SPEECH DEVICES 1 of 10 THE BREATHER TM ONE DEVICE MANY THERAPIES TRANSCRIPT LESSON 01: WHO TAKES THIS COURSE & WHY Hi everyone. My name is Carrie. I'll be your guide through this
Surgical Effects on Swallowing DYSPHAGIA AFTER TREATMENT FOR HNC: WHAT CAUSES IT? WHAT TREATMENT WORKS? Surgical Effects on Swallowing
 Susan Langmore, PhD, CCC-SLP, BRS-S Professor, BUMC, BU September 27, 2010 DYSPHAGIA AFTER TREATMENT FOR HNC: WHAT CAUSES IT? WHAT TREATMENT WORKS? Incidence of dysphagia after XRT VA study (Wolf; Terrell
Susan Langmore, PhD, CCC-SLP, BRS-S Professor, BUMC, BU September 27, 2010 DYSPHAGIA AFTER TREATMENT FOR HNC: WHAT CAUSES IT? WHAT TREATMENT WORKS? Incidence of dysphagia after XRT VA study (Wolf; Terrell
Understanding and Managing Your Chronic Obstructive Pulmonary Disease (COPD)* *Includes chronic bronchitis and emphysema.
 Understanding and Managing Your Chronic Obstructive Pulmonary Disease (COPD)* *Includes chronic bronchitis and emphysema. 2 LIVING WITH COPD You may have been told that you have COPD. It is a lung disease
Understanding and Managing Your Chronic Obstructive Pulmonary Disease (COPD)* *Includes chronic bronchitis and emphysema. 2 LIVING WITH COPD You may have been told that you have COPD. It is a lung disease
How Speech and Swallowing are Affected with ALS
 Patient Education How Speech and Swallowing are Affected with ALS This handout describes how ALS affects speech and swallowing. For speech issues it covers tips for listeners and speakers and what can
Patient Education How Speech and Swallowing are Affected with ALS This handout describes how ALS affects speech and swallowing. For speech issues it covers tips for listeners and speakers and what can
ORAL HYGIENE SESSION 2
 ORAL HYGIENE SESSION 2 BSCS_flipchart_session2.indd 1 dental FLOSS Floss is a special string used to clean between your teeth. This is a very hard space to get clean Floss can get to small spaces your
ORAL HYGIENE SESSION 2 BSCS_flipchart_session2.indd 1 dental FLOSS Floss is a special string used to clean between your teeth. This is a very hard space to get clean Floss can get to small spaces your
Speech and Language Therapy. Kerrie McCarthy Senior Speech and Language Therapist
 Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Review of dysphagia in poststroke
 Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
Moments of Joy: It s What YOU Choose to Do as a Caregiver. Teepa Snow
 Moments of Joy: It s What YOU Choose to Do as a Caregiver Teepa Snow Laughing VS Surviving My goal for you Understanding of what s happening with the person with dementia Support so you can survive Insight
Moments of Joy: It s What YOU Choose to Do as a Caregiver Teepa Snow Laughing VS Surviving My goal for you Understanding of what s happening with the person with dementia Support so you can survive Insight
Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
 National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
Applied physiology. 7- Apr- 15 Swallowing Course/ Anatomy and Physiology
 Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
Relaxation Techniques
 Relaxation is needed for good health. It gives your body and mind a chance to rest and recover from high-stress situations. Your heart rate slows down, blood pressure decreases and muscles relax. Relaxation
Relaxation is needed for good health. It gives your body and mind a chance to rest and recover from high-stress situations. Your heart rate slows down, blood pressure decreases and muscles relax. Relaxation
Respiratory Compromise and Swallowing
 Speech Pathology and Respiratory Care April 11, 2013 By Angela Parcaro-Tucker, MA, CCC-SLP, LSVT How can Speech Therapy help? 1 Respiratory Compromise and Swallowing Swallowing is a complex sequence of
Speech Pathology and Respiratory Care April 11, 2013 By Angela Parcaro-Tucker, MA, CCC-SLP, LSVT How can Speech Therapy help? 1 Respiratory Compromise and Swallowing Swallowing is a complex sequence of
Feeding and Oral Hygiene: How to Address the Challenges
 Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Oral care & swallowing
 Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
How to Reduce Test Anxiety
 How to Reduce Test Anxiety To reduce math test anxiety, you need to understand both the relaxation response and how negative self-talk undermines your abilities. Relaxation Techniques The relaxation response
How to Reduce Test Anxiety To reduce math test anxiety, you need to understand both the relaxation response and how negative self-talk undermines your abilities. Relaxation Techniques The relaxation response
ORAL HYGIENE SESSION 2
 ORAL HYGIENE SESSION 2 BSCS_flipchart_session2.indd 1 dental FLOSS Floss is a special string used to clean between your teeth. This is a very hard space to get clean Floss can get to small spaces your
ORAL HYGIENE SESSION 2 BSCS_flipchart_session2.indd 1 dental FLOSS Floss is a special string used to clean between your teeth. This is a very hard space to get clean Floss can get to small spaces your
Understanding your child s videofluoroscopic swallow study report
 Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
1. With your toothbrush brush the top and sides of your tongue, while your tongue is sitting on the floor of your mouth.
 EXERCISES FOR THE TONGUE TONGUE BRUSHING 1. With your toothbrush brush the top and sides of your tongue, while your tongue is sitting on the floor of your mouth. 2. Repeat the individual sections 5 times
EXERCISES FOR THE TONGUE TONGUE BRUSHING 1. With your toothbrush brush the top and sides of your tongue, while your tongue is sitting on the floor of your mouth. 2. Repeat the individual sections 5 times
Now to the opportunities. Explanation. Opportunities, cont 3/31/2018. More clarification than ground breaking for the sophisticated Canadian audience
 Now to the opportunities More clarification than ground breaking for the sophisticated Canadian audience Explanation Opportunities, as used here, was meant to include some recent violations of traditional
Now to the opportunities More clarification than ground breaking for the sophisticated Canadian audience Explanation Opportunities, as used here, was meant to include some recent violations of traditional
Dysphagia Management in TCP. Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012
 Dysphagia Management in TCP Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012 The role of the Speech Pathologist To assess swallowing status To provide management and
Dysphagia Management in TCP Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012 The role of the Speech Pathologist To assess swallowing status To provide management and
VOICE LESSON #6. Resonance: Creating Good Vocal Vibes. The Soft Palate
 VOICE LESSON #6 Resonance: Creating Good Vocal Vibes Voice Lesson #6 - Resonance Page 1 of 7 RESONANCE is the amplification and enrichment of tones produced by the voice. When we talk about resonance,
VOICE LESSON #6 Resonance: Creating Good Vocal Vibes Voice Lesson #6 - Resonance Page 1 of 7 RESONANCE is the amplification and enrichment of tones produced by the voice. When we talk about resonance,
Screening. James L. Coyle, Ph.D., CCC-SLP, BRS-S University of Pittsburgh. J. Coyle 1
 Screening James L. Coyle, Ph.D., CCC-SLP, BRS-S University of Pittsburgh J. Coyle 1 Disclosure University of Pittsburgh (salary) Continuing education Northern Speech Services State Conferences and Conventions
Screening James L. Coyle, Ph.D., CCC-SLP, BRS-S University of Pittsburgh J. Coyle 1 Disclosure University of Pittsburgh (salary) Continuing education Northern Speech Services State Conferences and Conventions
Laryngeal Cancer. Understanding your diagnosis cancer.ca
 Laryngeal Cancer Understanding your diagnosis 1 888 939-3333 cancer.ca Laryngeal Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be
Laryngeal Cancer Understanding your diagnosis 1 888 939-3333 cancer.ca Laryngeal Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be
Exercise- Based Approaches to Dysphagia Rehabilitation
 Interventions Cichero J, Clavé P (eds): Stepping Stones to Living Well with Dysphagia. Nestlé Nutr Inst Workshop Ser, vol 72, pp 109 117, Nestec Ltd., Vevey/S. Karger AG., Basel, 2012 Exercise- Based Approaches
Interventions Cichero J, Clavé P (eds): Stepping Stones to Living Well with Dysphagia. Nestlé Nutr Inst Workshop Ser, vol 72, pp 109 117, Nestec Ltd., Vevey/S. Karger AG., Basel, 2012 Exercise- Based Approaches
Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST
 Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST Objectives Gain a general understanding of normal swallowing Gain
Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST Objectives Gain a general understanding of normal swallowing Gain
Safe swallowing strategies
 Learning Guide Safe swallowing strategies 27468 Apply safe swallowing strategies in a health or wellbeing setting Level 3 5 credits Name: Workplace: Issue 2.0 Copyright 2017 Careerforce All rights reserved.
Learning Guide Safe swallowing strategies 27468 Apply safe swallowing strategies in a health or wellbeing setting Level 3 5 credits Name: Workplace: Issue 2.0 Copyright 2017 Careerforce All rights reserved.
Asthma. & Older Adults. A guide to living with asthma for people aged 65 years and over FOR PATIENTS & CARERS
 Asthma & Older Adults A guide to living with asthma for people aged 65 years and over FOR PATIENTS & CARERS what is Asthma? Asthma is a disease of the airways, the small tubes which carry air in and out
Asthma & Older Adults A guide to living with asthma for people aged 65 years and over FOR PATIENTS & CARERS what is Asthma? Asthma is a disease of the airways, the small tubes which carry air in and out
BETTER SPIROMETRY. Marijke Currie (CRFS) Care Medical Ltd Phone: Copyright CARE Medical ltd
 BETTER SPIROMETRY Marijke Currie (CRFS) Care Medical Ltd Phone: 0800 333 808 Email: sales@caremed.co.nz What is spirometry Spirometry is a physiological test that measures the volume of air an individual
BETTER SPIROMETRY Marijke Currie (CRFS) Care Medical Ltd Phone: 0800 333 808 Email: sales@caremed.co.nz What is spirometry Spirometry is a physiological test that measures the volume of air an individual
Benefits of Weight bearing increased awareness of the involved side decreased fear improved symmetry regulation of muscle tone
 From the information we have gathered during our Evaluation, the Clinical Reasoning we used to identify key problem areas and the Goals Established with functional outcomes we now have enough information
From the information we have gathered during our Evaluation, the Clinical Reasoning we used to identify key problem areas and the Goals Established with functional outcomes we now have enough information
Vocal Hygiene. How to Get The Best Mileage From Your Voice
 Vocal Hygiene How to Get The Best Mileage From Your Voice Speech and Voice Production Speech and voice are the result of a complex interplay of physical and emotional events. The first event is in the
Vocal Hygiene How to Get The Best Mileage From Your Voice Speech and Voice Production Speech and voice are the result of a complex interplay of physical and emotional events. The first event is in the
Vocal Hygiene. How to Get The Best Mileage From Your Voice. Provincial Voice Care Resource Program Vancouver General Hospital
 Vocal Hygiene How to Get The Best Mileage From Your Voice Provincial Voice Care Resource Program Vancouver General Hospital Gordon & Leslie Diamond Health Care Centre Vancouver General Hospital 4th Floor,
Vocal Hygiene How to Get The Best Mileage From Your Voice Provincial Voice Care Resource Program Vancouver General Hospital Gordon & Leslie Diamond Health Care Centre Vancouver General Hospital 4th Floor,
1 Pause and Practice: Facilitating Trunk and Shoulder Control with the Therapy Ball
 1 Pause and Practice: Facilitating Trunk and Shoulder Control with the Therapy Ball This is an example of Facilitating Combinations of Movements and Active Assist. Starting Position Have your patient sit
1 Pause and Practice: Facilitating Trunk and Shoulder Control with the Therapy Ball This is an example of Facilitating Combinations of Movements and Active Assist. Starting Position Have your patient sit
The Role of the Speech Language Pathologist & Spinal Cord Injury
 The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
15/11/2011. Swallowing
 Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Swallow-respiratory coordination. Liza Bergström, Leg. logoped.
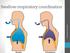 Swallow-respiratory coordination Liza Bergström, Leg. logoped. Biological timeshare When we breathe, we don t swallow When we swallow, we don t breathe Body will always choose to breathe over anything
Swallow-respiratory coordination Liza Bergström, Leg. logoped. Biological timeshare When we breathe, we don t swallow When we swallow, we don t breathe Body will always choose to breathe over anything
How to Cope with Anxiety
 How to Cope with Anxiety A PUBLICATION OF CBT PROFESSIONALS TABLE OF CONTENTS 1 Coping Skills for Anxiety 2 Breathing Exercise 3 Progressive Muscle Relaxation 4 Psychological Treatments for Anxiety 2 1.
How to Cope with Anxiety A PUBLICATION OF CBT PROFESSIONALS TABLE OF CONTENTS 1 Coping Skills for Anxiety 2 Breathing Exercise 3 Progressive Muscle Relaxation 4 Psychological Treatments for Anxiety 2 1.
Swallowing Strategies
 Department of Head and Neck Surgery Section of Speech Pathology & Audiology M.D. Anderson Cancer Center (713) 792-6525 Swallowing Strategies 1) POSTURAL CHANGES: a) Chin Tuck: (1) Delayed onset pharyngeal
Department of Head and Neck Surgery Section of Speech Pathology & Audiology M.D. Anderson Cancer Center (713) 792-6525 Swallowing Strategies 1) POSTURAL CHANGES: a) Chin Tuck: (1) Delayed onset pharyngeal
Stay Fit While You Sit: 10 Simple Exercises for Sewers
 Published on Sew4Home Stay Fit While You Sit: 10 Simple Exercises for Sewers Editor: Liz Johnson Friday, 05 May 2017 1:00 There is a lot of sitting involved in sewing, which can lead to aches and pains
Published on Sew4Home Stay Fit While You Sit: 10 Simple Exercises for Sewers Editor: Liz Johnson Friday, 05 May 2017 1:00 There is a lot of sitting involved in sewing, which can lead to aches and pains
COPD. Helen Suen & Lexi Smith
 COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
Common complaints included: "No one can hear me!" "My voice wears out too quickly." "My throat feels so tight and strained."
 PART ONE OF THREE ARTICLES The George Washington University Speech and Hearing Center in Washington DC has treated clients with voice problems since the 1970 s. One of the most common vocal issues that
PART ONE OF THREE ARTICLES The George Washington University Speech and Hearing Center in Washington DC has treated clients with voice problems since the 1970 s. One of the most common vocal issues that
WHAT IS A SOCIAL CONSEQUENCE OF USING TOBACCO?
 WHAT IS A SOCIAL CONSEQUENCE OF USING TOBACCO? Essential Standards 6.ATOD.2 - Understand the health risks associated with alcohol, tobacco, and other drug use. Clarifying Objectives: 6.ATOD.2.1 - Explain
WHAT IS A SOCIAL CONSEQUENCE OF USING TOBACCO? Essential Standards 6.ATOD.2 - Understand the health risks associated with alcohol, tobacco, and other drug use. Clarifying Objectives: 6.ATOD.2.1 - Explain
RELAXATION EXERCISES
 RELAXATION EXERCISES Relaxation technique 1: Breathing meditation for stress relief With its focus on full, cleansing breaths, deep breathing is a simple, yet powerful, relaxation technique. It s easy
RELAXATION EXERCISES Relaxation technique 1: Breathing meditation for stress relief With its focus on full, cleansing breaths, deep breathing is a simple, yet powerful, relaxation technique. It s easy
Swallowing after a Total Laryngectomy
 Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA
 TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA ANNE URIKO SPORTS MEDICINE AND REHABILITATION CLINIG OF TARTU UNIVERSITY HOSPITAL 17.09.2010 DYSPHAGIA DIFFICULTY MOVING FOOD FROM MOUTH TO STOMACH
TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA ANNE URIKO SPORTS MEDICINE AND REHABILITATION CLINIG OF TARTU UNIVERSITY HOSPITAL 17.09.2010 DYSPHAGIA DIFFICULTY MOVING FOOD FROM MOUTH TO STOMACH
Pediatric Modified Barium Swallow Studies. Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015
 Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS. Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis
 DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis Suiter, ASHA, 2012 Diagnostic Tests vs. Screening Diagnostic tests are used when a
DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis Suiter, ASHA, 2012 Diagnostic Tests vs. Screening Diagnostic tests are used when a
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Patient Information Series
 A M E R I C A N T H O R A C I C S O C I E T Y Patient Information Series What Is Vocal Cord Dysfunction (VCD)? Vocal Cord Dysfunction means that your vocal cords do not act normally. With VCD, instead
A M E R I C A N T H O R A C I C S O C I E T Y Patient Information Series What Is Vocal Cord Dysfunction (VCD)? Vocal Cord Dysfunction means that your vocal cords do not act normally. With VCD, instead
DISCLAIMER - PLEASE READ!
 DISCLAIMER - PLEASE READ! This e-book and the information contained in it are not meant for the treatment or prevention of disease, nor as a substitute for medical treatment, nor as an alternative to medical
DISCLAIMER - PLEASE READ! This e-book and the information contained in it are not meant for the treatment or prevention of disease, nor as a substitute for medical treatment, nor as an alternative to medical
Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease
 Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease Medicare Newsletter Spring 2012 Getting Rid of Mold There are many types of molds. Molds will not grow without water
Asthma and COPD Awareness breathe with ease sm and Chronic Obstructive Pulmonary Disease Medicare Newsletter Spring 2012 Getting Rid of Mold There are many types of molds. Molds will not grow without water
The Effects of Specific Respiratory Muscle Training on the Speech Intelligibility of a Patient with Parkinson s Disease
 The Effects of Specific Respiratory Muscle Training on the Speech Intelligibility of a Patient with Parkinson s Disease Vaneysa Hansen, M.A., SLP (C) & Barbara Mathers-Schmidt, PhD, SLP-CCC Western Washington
The Effects of Specific Respiratory Muscle Training on the Speech Intelligibility of a Patient with Parkinson s Disease Vaneysa Hansen, M.A., SLP (C) & Barbara Mathers-Schmidt, PhD, SLP-CCC Western Washington
Managing Other Medical Conditions
 Managing Other Medical Conditions When Dementia is Part of the Picture Terms You Will NEED to Know - Advanced directives - Living Will - DNR orders - Durable HC-POA - Palliative care - Hospice care - Comfort
Managing Other Medical Conditions When Dementia is Part of the Picture Terms You Will NEED to Know - Advanced directives - Living Will - DNR orders - Durable HC-POA - Palliative care - Hospice care - Comfort
Workbook. Apply safe swallowing strategies as a health assistant in an aged care, health or disability context. US Level 4 Credits 4. Name...
 Workbook Apply safe swallowing strategies as a health assistant in an aged care, health or disability context US 27468 Level 4 Credits 4 Name... US 27468 Level 4 Credits 4 All rights reserved. Careerforce
Workbook Apply safe swallowing strategies as a health assistant in an aged care, health or disability context US 27468 Level 4 Credits 4 Name... US 27468 Level 4 Credits 4 All rights reserved. Careerforce
DEMENTIA Dementia is NOT a normal part of aging Symptoms of dementia can be caused by different diseases Some symptoms of dementia may include:
 DEMENTIA Dementia is NOT a normal part of aging Symptoms of dementia can be caused by different diseases Some symptoms of dementia may include: 1. Memory loss The individual may repeat questions or statements,
DEMENTIA Dementia is NOT a normal part of aging Symptoms of dementia can be caused by different diseases Some symptoms of dementia may include: 1. Memory loss The individual may repeat questions or statements,
Copyright Cardiff University
 This exercise programme has been developed by physiotherapists specifically for people with movement disorders. Exercise is not without its risks and this or any other exercise programme has potential
This exercise programme has been developed by physiotherapists specifically for people with movement disorders. Exercise is not without its risks and this or any other exercise programme has potential
Introduction to Standard Esophageal Speech. Texas Laryngectomy Association 2018
 Introduction to Standard Esophageal Speech Texas Laryngectomy Association 2018 Disclosure Objectives At the end of this presentation the participant will be able to: Describe the production of standard
Introduction to Standard Esophageal Speech Texas Laryngectomy Association 2018 Disclosure Objectives At the end of this presentation the participant will be able to: Describe the production of standard
Your Guide to a Smoke Free Future
 Your Guide to a Smoke Free Future If you smoke, or if you have quit within the past 2 months, then ask for our detailed handout which provides information on how to begin and maintain a smoke-free lifestyle.
Your Guide to a Smoke Free Future If you smoke, or if you have quit within the past 2 months, then ask for our detailed handout which provides information on how to begin and maintain a smoke-free lifestyle.
EXERCISE FOR PARKINSON S RECOMMENDATIONS FOR MANAGING SYMPTOMS
 EXERCISE FOR PARKINSON S RECOMMENDATIONS FOR MANAGING SYMPTOMS INSIDE THIS GUIDE EXERCISE FOR PARKINSON S OVERVIEW 3 RECOMMENDATIONS FOR EXERCISE FOR PARKINSON S 4 EXERCISE FOR PARKINSON S PRINCIPLES 5
EXERCISE FOR PARKINSON S RECOMMENDATIONS FOR MANAGING SYMPTOMS INSIDE THIS GUIDE EXERCISE FOR PARKINSON S OVERVIEW 3 RECOMMENDATIONS FOR EXERCISE FOR PARKINSON S 4 EXERCISE FOR PARKINSON S PRINCIPLES 5
Validation Techniques in a Real World By Alisa Tagg, BA ACC/EDU AC-BC CADDCT CDP CDCS NAAP President
 What is Validation? This therapy was developed to attempt understanding what emotions patients with Alzheimer s disease are expressing and respond in a way that allows patients to express their emotions
What is Validation? This therapy was developed to attempt understanding what emotions patients with Alzheimer s disease are expressing and respond in a way that allows patients to express their emotions
Standardisation of Videofluoroscopy: Where is it taking us?
 Standardisation of Videofluoroscopy: Where is it taking us? Jodi Allen, Senior Speech and Language Therapist, The National Hospital for Neurology and Neurosurgery If somebody asked you. What do you start
Standardisation of Videofluoroscopy: Where is it taking us? Jodi Allen, Senior Speech and Language Therapist, The National Hospital for Neurology and Neurosurgery If somebody asked you. What do you start
COMMUNICATION AND SWALLOWING DISORDERS IN PARKINSON S DISEASE Challenges, Treatments, and Resources
 COMMUNICATION AND SWALLOWING DISORDERS IN PARKINSON S DISEASE Challenges, Treatments, and Resources Rosemary B. Loftin, M.S. CCC/SLP Supervisor of Speech Pathology Services Mayo Clinic Hospital Arizona
COMMUNICATION AND SWALLOWING DISORDERS IN PARKINSON S DISEASE Challenges, Treatments, and Resources Rosemary B. Loftin, M.S. CCC/SLP Supervisor of Speech Pathology Services Mayo Clinic Hospital Arizona
SWALLOWING: HOW CAN WE HELP
 SWALLOWING: HOW CAN WE HELP Carol Romero-Clark, M.S., CCC-SLP University of New Mexico Hospital Speech Pathology Department November 10, 2017 What happens when you swallow? Mouth (Oral Phase) Your tongue
SWALLOWING: HOW CAN WE HELP Carol Romero-Clark, M.S., CCC-SLP University of New Mexico Hospital Speech Pathology Department November 10, 2017 What happens when you swallow? Mouth (Oral Phase) Your tongue
Progressive Muscle Relaxation
 Module 3 Progressive Muscle Relaxation Introduction 2 Progressive Muscle Relaxation 3 Preparing for Relaxation 3 Relaxation Technique 4 The Calming Technique: Body and Breath 6 Difficulties with Relaxation
Module 3 Progressive Muscle Relaxation Introduction 2 Progressive Muscle Relaxation 3 Preparing for Relaxation 3 Relaxation Technique 4 The Calming Technique: Body and Breath 6 Difficulties with Relaxation
Table Of Contents. Complete Guide To Muscle Building MUSCLE BUILDING INTRODUCTION... 3 TRAINING EXERCISES...
 Table Of Contents MUSCLE BUILDING INTRODUCTION... 3 TRAINING EXERCISES... 7 EXTENSIVE WORKOUTS... 21 POWER FOODS DEFINED... 29 MEAL PLANS: PRINT OUT... 48 RESTED PERFORMANCE... 71 THE TRUTH ABOUT SUPPLEMENTS...
Table Of Contents MUSCLE BUILDING INTRODUCTION... 3 TRAINING EXERCISES... 7 EXTENSIVE WORKOUTS... 21 POWER FOODS DEFINED... 29 MEAL PLANS: PRINT OUT... 48 RESTED PERFORMANCE... 71 THE TRUTH ABOUT SUPPLEMENTS...
Efficacy of breathing exercises and relaxation techniques for patients with neurological disorders
 Efficacy of breathing exercises and relaxation techniques for patients with neurological disorders Delphine Herrmann Rachael Katz Svetlana Piliavsky Shelley Rice ASHA 2008-CHICAGO WHAT IS THE BENEFIT OF
Efficacy of breathing exercises and relaxation techniques for patients with neurological disorders Delphine Herrmann Rachael Katz Svetlana Piliavsky Shelley Rice ASHA 2008-CHICAGO WHAT IS THE BENEFIT OF
relaxation and nervous system regulation exercises
 relaxation and nervous system regulation exercises Objectives to provide a range of simple exercises that encourage the regular practice of relaxation and to help build resilience with increased awareness
relaxation and nervous system regulation exercises Objectives to provide a range of simple exercises that encourage the regular practice of relaxation and to help build resilience with increased awareness
Disclosures. Common feature in current rehab approaches: Dysphagia Management: In the Beginning 11/28/18
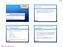 Disclosures Ê ML Huckabee is employed by the University of Canterbury, who is the owner and manufacturer of the BiSSkiT software that will be discussed. Skill based swallowing training Can the pharyngeal
Disclosures Ê ML Huckabee is employed by the University of Canterbury, who is the owner and manufacturer of the BiSSkiT software that will be discussed. Skill based swallowing training Can the pharyngeal
Coach on Call. Letting Go of Stress. A healthier life is on the line for you! How Does Stress Affect Me?
 Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
Stroke. Objectives: After you take this class, you will be able to:
 Stroke Objectives: After you take this class, you will be able to: 1. Describe the signs of a stroke and how a stroke happens. 2. Discuss stroke risk factors. 3. Detail the care and rehabilitation of a
Stroke Objectives: After you take this class, you will be able to: 1. Describe the signs of a stroke and how a stroke happens. 2. Discuss stroke risk factors. 3. Detail the care and rehabilitation of a
Sources. Taking Charge of Your Asthma. Asthma Action Plan (to be completed with your doctor) UnitedHealthcare Insurance Company
 Asthma Action Plan (to be completed with your doctor) Green Zone: (80 to 00% of my personal best) Peak Flow between and (00% = personal best) You can do all the things you usually do. Your asthma medicine
Asthma Action Plan (to be completed with your doctor) Green Zone: (80 to 00% of my personal best) Peak Flow between and (00% = personal best) You can do all the things you usually do. Your asthma medicine
COPD & Managing Your Disease at Home
 COPD & Managing Your Disease at Home Oxygen and Activity The importance of activity: Activity is important for everyone. When you have COPD your activity level may be low because breathing is difficult
COPD & Managing Your Disease at Home Oxygen and Activity The importance of activity: Activity is important for everyone. When you have COPD your activity level may be low because breathing is difficult
For carers and relatives of people with frontotemporal dementia and semantic dementia. Newsletter
 For carers and relatives of people with frontotemporal dementia and semantic dementia Newsletter AUGUST 2008 1 Welcome Welcome to the August edition of our CFU Support Group Newsletter. Thanks to all of
For carers and relatives of people with frontotemporal dementia and semantic dementia Newsletter AUGUST 2008 1 Welcome Welcome to the August edition of our CFU Support Group Newsletter. Thanks to all of
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE
 EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
Muscular Strength and Endurance:
 PE 1- Assignment #5 6 1 Name: Per: Date: Teacher: STRESS BREAK Participating in physical activities that improve your self-esteem is a great way to deal with stress. The better you feel about yourself,
PE 1- Assignment #5 6 1 Name: Per: Date: Teacher: STRESS BREAK Participating in physical activities that improve your self-esteem is a great way to deal with stress. The better you feel about yourself,
Breathing and pulmonary function
 EXPERIMENTAL PHYSIOLOGY EXPERIMENT 5 Breathing and pulmonary function Ying-ying Chen, PhD Dept. of Physiology, Zhejiang University School of Medicine bchenyy@zju.edu.cn Breathing Exercise 1: Tests of pulmonary
EXPERIMENTAL PHYSIOLOGY EXPERIMENT 5 Breathing and pulmonary function Ying-ying Chen, PhD Dept. of Physiology, Zhejiang University School of Medicine bchenyy@zju.edu.cn Breathing Exercise 1: Tests of pulmonary
