Department of Health Care Services SB 1004 Medi-Cal Palliative Care Policy September 1, 2016 Update
|
|
|
- Kathlyn Cain
- 5 years ago
- Views:
Transcription
1 Department of Health Care Services SB 1004 Medi-Cal Palliative Care Policy September 1, 2016 Update This document provides an update on the Department of Health Care Services (DHCS) Medi-Cal palliative care policy as authorized by SB 1004 (Hernandez, Chapter 574, Statutes of 2014). The DHCS Medi-Cal palliative care policy will be applicable to both managed care and fee-forservice delivery systems. Due to the specific focus of SB 1004, this document is oriented toward Medi-Cal only beneficiaries enrolled in Medi-Cal Managed Care Plans (MCPs). Further guidance will be provided for Medicare Medi-Cal dually-eligible beneficiaries, and Medi-Cal only fee-forservice beneficiaries not enrolled in MCPs. Section 1: SB 1004 Medi-Cal Palliative Care, and Overall Context The Centers for Medicare and Medicaid Services (CMS) defines palliative care as: patient and family-centered care that optimizes quality of life by anticipating, preventing, and treating suffering. Palliative care throughout the continuum of illness involves addressing physical, intellectual, emotional, social, and spiritual needs and to facilitate patient autonomy, access to information, and choice. Many physicians and practitioners note that palliative care is an overall approach to the practice of medicine that is broader than end-of-life care, and is for any age and any stage of illness. For purposes of SB 1004 guidance, DHCS proposes a Medi-Cal palliative care policy that is guided by the CMS definition of palliative care and the substantial body of research on palliative care programs, and with specific definitions of eligible conditions, services, and providers. The purpose of defining Medi-Cal palliative care more narrowly for a specific set of conditions is to meet the specific requirements of SB 1004, and to recognize that long-term success in implementing a new program to improve end of life care for Medi-Cal beneficiaries is more likely to be achieved through an incremental approach. At the same time, a number of Medi-Cal managed care health plans (MCPs), hospitals and health systems, and other providers are already incorporating broader palliative care principles and strategies into their models of care. DHCS encourages those strategies to improve patient satisfaction and outcomes for Medi-Cal beneficiaries at all stages of life and illness, and to help meet the goals of Let s Get Healthy California and the DHCS Quality Strategy. Early Palliative Care At initial diagnosis of serious illness, early palliative care may accompany disease modifying care (curative care or restorative intent). Early palliative care is often advance care planning and can include palliative care consultation or pain and symptom management as needed, but may not reflect the full array of services listed below for SB 1004 palliative care. Research indicates patients and families have higher satisfaction and alignment of care with treatment wishes when advance care planning conversations occur earlier in the disease process. For example, a patient with a recent diagnosis of Stage II cancer, who is proceeding with initial chemotherapy, does not have related emergency department visits or inpatient stays, and whose condition is stable, should be offered early palliative care, but may not be eligible for SB 1004 palliative care. Hospice Care Note that hospice care also serves seriously ill patients, but is distinct from SB 1004 Medi-Cal palliative care. Hospice care is a Medi-Cal benefit that is available to both managed care and fee-for-service beneficiaries who have a medical prognosis of six months or less to live, and is
2 provided in lieu of curative treatment for the terminal condition. Palliative care may be provided concurrently with curative care while hospice care may not, and palliative care is not limited to beneficiaries with a medical prognosis for life expectancy of six months or less. Further information about hospice care in Medi-Cal can be found in the DHCS All-Plan Letter for managed care, and in Title 22 of the California Code of Regulations, Section Figure 1 * Patients with serious illness can complete a Physicians Authorization for Life-Sustaining Treatment (POLST) form with their provider. The POLST is a statewide standard form for seriously ill patients to indicate to medical personnel whether the patient desires or declines resuscitation, intubation, feeding tubes and other interventions. Figure 1 above provides an overview of the care model for SB 1004 Medi-Cal palliative care. The design is adapted from the National Consensus Project for Quality Palliative Care. At initial diagnosis of serious illness, early palliative care may accompany disease modifying care (curative care or restorative intent). Early palliative care is often advance care planning and/or palliative care consultation, and can include pain and symptom management as SB 1004 Medi-Cal Palliative Care, September 1, 2016 Page 2
3 needed. The wavy line indicates that the proportion of palliative care varies based on individual patient choices and needs. As the patient s illness progresses, those with serious illness who meet specific clinical eligibility criteria can enroll in SB 1004 palliative care programs and also continue to access disease modifying care. As the patient s illness progresses further, those who meet hospice eligibility criteria can disenroll from SB 1004 palliative care, and enroll in hospice to receive additional comfort care and forego further disease modifying care. Note that specific services for individual patients are based on medical necessity, and this figure is for general descriptive purposes only. Also, additional options are available for children. Case Example: Provision of Palliative Care and Hospice through the Course of Illness 1 Primary/Early Palliative Care Patient A is a 55 year-old woman diagnosed with stage IIA breast cancer, who is being evaluated in oncology clinic for initial treatment with chemotherapy and hormone therapy. She has been working for several years, is a single mother of 3 adult children, including one about to enter college. She reports feeling stress and anxiety in juggling work, treatment, and support for her child entering college. Considerations for early palliative care: o Psychosocial and spiritual support in coping with the diagnosis o Practical assistance with paperwork for Family Medical Leave Act, disability, etc. o Education and support for family members o Symptom management during treatment o Introduction of advance care planning and identification of surrogate decision-maker SB 1004 Palliative Care Patient A underwent mastectomy, 4 cycles of chemotherapy and hormone therapy, and seemed to have no evidence of disease progression. She returned to work and had resumed her normal activities, with some modifications, for 18 months; however, she has recently become more fatigued and has had to take days off of work to rest. She returned to see her primary care doctor for progressive back pain, which she attributed to strain while moving furniture; unfortunately, x-rays of her spine showed a lesion suspicious for a metastasis, as well as lung nodules. Patient was diagnosed with advanced cancer and referred back to her oncologist for follow-up, who presents options of palliative radiation and chemotherapy to potentially extend and improve the quality of her life. Considerations for palliative care o Psychosocial and spiritual support in coping with disease progression o Practical assistance with applying for disability and counseling regarding financial planning, insurance issues o Education and support for family members o Discussion of benefits/burdens of treatment options and goals of care o Symptom management during treatment 1 Example developed by Anne Kinderman, MD, Director of the Supportive & Palliative Care Service Program at Zuckerberg San Francisco General and Associate Professor of Medicine at the University of California San Francisco. SB 1004 Medi-Cal Palliative Care, September 1, 2016 Page 3
4 o Focused advance care planning and designation of durable power of attorney for healthcare, if not already done Hospice Care Patient A chose to undergo both palliative radiation and chemotherapy for her stage IV breast cancer, and experienced some relief from her back pain. Unfortunately, she had difficulty tolerating the chemotherapy regimen, due to fatigue and nausea. Nevertheless, she completed an additional 4 cycles of chemotherapy in the hopes that this would provide her with more time with her family. Unfortunately, on follow-up CT scans, the metastatic disease in her lungs had continued to progress, in spite of treatment. Patient A s palliative care and oncology providers discuss this bad news with her, and inform her of options to try 3 rd line chemotherapy, or enroll in hospice. Based on the difficulty she had tolerating the 2 nd line chemotherapy, she decided to enroll in hospice care at home. Considerations for hospice: o Psychosocial and spiritual support in coping with end of life o Practical assistance with caregiving services, health aides, meal services, etc. o Counseling regarding financial planning, insurance issues o Education and support for family members o Transition to inpatient hospice or skilled nursing facility if needed o Symptom management through disease progression and end of life o Focused advance care planning and designation of durable power of attorney for healthcare, if not already done o Completion of POLST form Palliative Care Options for Children Additional options for children include the Section 1915(c) Home and Community Based Services waiver known as Partners for Children (PFC), to provide hospice-like services in addition to Medi-Cal State Plan services for seriously-ill children. Also, Section 2302 of the Patient Protection and Affordable Care Act (ACA) provides authority for hospice care concurrently with curative care for beneficiaries under age 21. Information regarding the concurrent care policy for children is available in DHCS All Plan Letter , California Children s Services Numbered Letter , and Managed Care Policy Letter Concurrent care for children is a statewide benefit, and PFC waiver enrollment is available in several counties in the state. DHCS policy for SB 1004 is without regard to age, so beneficiaries under age 21 may be eligible for SB 1004 palliative care services if they meet the general and disease-specific eligibility criteria. However, both concurrent care under Section 2302 of the ACA and the PFC waiver provide additional services and broader eligibility criteria for children than SB Further, since enrollment in SB 1004 and either Section 2302 concurrent care or the PFC waiver would result in redundant services, children enrolled in either of those programs cannot enroll in SB 1004 palliative care. Section 2: Eligible Conditions DHCS proposes that eligible conditions for SB 1004 Medi-Cal palliative care include Cancer, Congestive Heart Failure (CHF), Chronic Obstructive Pulmonary Disease (COPD), or Liver Disease. Based on the significant body of national research on palliative care, and the results SB 1004 Medi-Cal Palliative Care, September 1, 2016 Page 4
5 of existing palliative care programs, these four conditions are most promising for improved patient satisfaction and health outcomes, and permit cost-effective implementation. Although DHCS initially proposed that eligibility would be limited to beneficiaries with latestage/high grade cancer with significant functional decline or limitations, stakeholder feedback suggested that this eligibility limit was too restrictive, these patients may already be hospice eligible, and palliative care is more appropriate and effective earlier in the disease progression. Based on feedback from a panel of palliative care experts, DHCS proposes that beneficiary eligibility for SB 1004 Medi-Cal palliative care be determined through a clinical review consisting of general eligibility criteria and disease-specific criteria. 2 Beneficiaries would need to meet all items in the general eligibility criteria in subsection A and at least one of the four diseasespecific criteria in subsection B below. A. General Eligibility Criteria: 1. Patient is likely to or has started to use the hospital or emergency department as a means to manage their late stage disease. This refers to unanticipated decompensation and does not include elective procedures. For example, a patient with two or more inpatient admissions or Emergency Department visits in the past six months and meeting the disease-specific criteria below should be strongly considered for palliative care assessment. 2. Patient in the late stage of illness, as defined in subsection B, with appropriate documentation of continued decline in health status, and is not eligible for or declines hospice enrollment. 3. The patient s death within a year would not be unexpected based on clinical status. 4. Patient has received appropriate patient-desired medical therapy, or for whom treatment is no longer effective. 3 Patient is not in reversible acute decompensation. For example, patient with advanced tonsillar cancer had undergone tumor debulking and neck dissection followed by adjuvant chemotherapy and external beam radiation therapy. Despite this appropriate therapy, the patient developed locally recurrent disease. This patient could pursue additional surgery and radiation therapy, likely for symptom relief, while still qualifying for SB 1004 palliative care referral and services. 5. Patient and, if applicable, family/patient-designated support person agree to both of the following: 2 The SB 1004 palliative care criteria are based on the Sharp HealthCare Transitions Guidelines for Advanced Illness Management, developed by Daniel R. Hoefer, MD, Chief Medical Officer of Outpatient Palliative Care and Hospice for Sharp HealthCare, and guidelines for the Partnership Health Plan Partners in Palliative Care Program developed by Robert Moore, MD, Chief Medical Officer. 3 This language is intended to distinguish between patients undergoing well-tolerated and effective treatment (early palliative care) and patients for whom treatment is not effective or well-tolerated (SB 1004 palliative care). Examples of this situation cited by the Advanced Illness Management (AIM) palliative care model include: ineffective chemotherapy or radiation for cancer; refractory fluid overload for CHF; severe or frequent exacerbations of COPD. Note that in lieu of appropriate patient-desired medical therapy, the Sharp Transitions Guidelines indicate that patients should have received maximum medical therapy, according to the Medicare definition of maximum medical therapy, which includes any of the following: 1) No further traditional therapy is available, 2) Patient is intolerant to further therapy, 3) Patient declines further therapy, 4) Patient repeatedly decompensates due to severe non-compliance. This criteria is also permissible under SB SB 1004 Medi-Cal Palliative Care, September 1, 2016 Page 5
6 a. Willing to attempt in-home, residential-based or outpatient disease management as recommended by the MCP Palliative Care team instead of first going to the emergency department. b. Willing to participate in Advance Care Planning discussions. B. Disease-Specific Eligibility Criteria 1. Congestive Heart Failure (CHF) a. Any patient who is hospitalized due to CHF as the primary diagnosis. No further invasive interventions planned although access to curative care is maintained, or b. NYHA III (Definition of NYHA III: Patients with cardiac disease resulting in marked limitation of physical activity. They are comfortable at rest. Less than ordinary activity causes fatigue, palpitation, dyspnea or anginal pain.) AND one of the following: a. Ejection Fraction < 30 for systolic failure b. Significant comorbidities: e.g. renal disease, diabetes, dementia, or poor biomarkers including rising BNP, pro-bnp, hscrp, BUN/ Creatinine (patient is in their best compensated state), and CAD. 2. Chronic Obstructive Pulmonary Disease (COPD): a. Severe airflow obstruction: FEV1 < 35 % predicted AND b. 24-hour oxygen requirement at less than 3L/minute OR c. 24-hour oxygen requirement at greater than or equal to 3 L/minute 3. Advanced Cancer: a. Any Stage III or IV cancer, locally advanced or metastatic cancer, leukemia or lymphoma AND one of the following: b. Karnofsky Performance Scale (KPS) score < or equal to 70 (KPS 70= Cares for self; unable to carry on normal activity or do active work) c. Being failed by two lines of standard chemotherapy. 4. Liver Disease: Irreversible Liver Damage AND BOTH of the following: 1. Albumin < INR > 1.3 PLUS one of the below a. Ascites b. Subacute bacterial peritonitis c. Hepatic encephalopathy SB 1004 Medi-Cal Palliative Care, September 1, 2016 Page 6
7 d. Hepatorenal syndrome e. Recurrent esophageal bleeds OR 1. Model for End Stage Liver Disease (MELD) score of greater than 19 To calculate MELD Score: Beneficiaries with serious illness who are receiving services under SB 1004 palliative care may choose to transition to hospice care if they meet the medical prognosis for hospice, or, if they also continue to meet the medical eligibility criteria for SB 1004, may remain in SB 1004 palliative care until their death. Beneficiaries with medical conditions that improve or stabilize, but still meet the eligibility criteria for SB 1004, may have palliative care services reduced as determined by medical necessity, but should continue to receive periodic assessments to monitor for a change in condition or needed services. Note that research supports additional conditions for palliative care referral, and some MCPs are already authorizing palliative care consults and services for patients with other medical conditions. This draft policy reflects the minimum eligibility criteria for SB 1004 palliative care patients; MCPs would continue to have discretion to authorize palliative care services for patients with other medical conditions in addition to the four listed above. Further, across existing palliative care programs in California, clinical eligibility criteria varies, and several approaches have been successful in improving patient satisfaction and health outcomes in a cost-effective manner for patients with serious illness. As a result, MCPs may propose alternative eligibility protocols for DHCS review. Those protocols may be no more restrictive, in terms of the eligible conditions, than the criteria listed above. In addition, as noted on page 1 above, research indicates that beneficiaries diagnosed with serious illness have improved patient satisfaction and receive care better aligned with their preferences when they have early palliative care services, such as advance care planning, early in the disease progression. As a result, MCPs should consider working with specialists in targeted practice areas such as oncology and cardiology, so that early palliative care, particularly advance care planning, is offered to beneficiaries diagnosed with serious illness but who are not enrolled in SB 1004 palliative care. Section 3: Services DHCS proposes that Medi-Cal palliative care include the eight services listed below, when reasonable and necessary for the palliation or management of a qualified serious illness and related conditions, when provided by a qualified provider, and when provided according to existing Medi-Cal regulations, Provider Manuals, Provider Bulletins, or All-Plan Letters for the specific service. All of the services below, except for chaplain services, are included in existing Medi-Cal benefits. Note that DHCS initially proposed that SB 1004 palliative care services include both palliative care-type services (such as advance care planning, consultation, and pain and symptom management) as well as all hospice care services. The Department has revised the list of palliative care services based on stakeholder and expert feedback, which indicated that including all hospice care services under SB 1004 palliative care was unnecessary and could delay hospice enrollment. SB 1004 Medi-Cal Palliative Care, September 1, 2016 Page 7
8 A. Palliative Care Services: 1. Advance Care Planning Advance care planning includes discussions between a physician or other qualified healthcare professional and a patient, family member, or surrogate in counseling and discussing advance directives, including POLST forms. MCPs must provide advance care planning to beneficiaries enrolled in Medi-Cal palliative care under SB Note that advance care planning is a Medi-Cal benefit available for all beneficiaries and is not limited to those with SB 1004 palliative care eligibility. 2. Palliative Care Assessment and Consultation Palliative care assessment and consultation services may be provided at the same time as advance care planning, or in subsequent patient conversations. The palliative care consultation aims to collect both routine medical data and additional personal information not regularly included in a medical history or Health Risk Assessment. In existing palliative care programs, providers usually complete an initial consultation, followed by periodic assessments. During an initial and/or subsequent palliative care consultation or assessment, topics may include, but are not limited to: Treatment plans, including palliative care and curative care Pain and medicine side effects Emotional and social challenges Spiritual concerns Patient goals Advance directives, including POLST forms 3. Plan of Care SB 1004 palliative care beneficiaries should have an individualized written plan of care. MCPs are required to develop a plan and engage the beneficiary and/or his or her representative(s) in its design. If a beneficiary already has a plan of care, that plan should be updated to reflect any changes resulting from the palliative care consultation or advance care planning discussion. 4. Pain and Symptom Management Adequate pain and symptom management is an essential component of palliative care. Prescription drugs, physical therapy and other medically necessary services may be needed to address beneficiary pain and other symptoms. The beneficiary s plan of care must include all services authorized for pain and symptom management. 5. Mental Health and Medical Social Services Counseling services must be available to the beneficiary to assist in minimizing the stress and problems that arise from the serious illness, related conditions, and the dying process. Counseling services must include, but are not limited to psychotherapy, SB 1004 Medi-Cal Palliative Care, September 1, 2016 Page 8
9 bereavement counseling, medical social services (within Home Health Agency services), and discharge planning. 6. Care Coordination The MCP s Medi-Cal palliative care program must designate a member of the Palliative Care Team to provide coordination of care, ensure continuous assessment of the patient's needs, and implement the plan of care. 7. Palliative Care Team The palliative care team is a group of individuals who work together to meet the physical, medical, psychosocial, emotional and spiritual needs of beneficiaries and their families and are able to assist in identifying sources of pain and discomfort of the beneficiary. This may include problems with breathing, fatigue, depression, anxiety, insomnia, bowel or bladder, dyspnea, nausea, etc. The palliative care team will also address other issues such as medication services and allied health. The team members must provide the care and services offered by palliative care. DHCS recommends that the Palliative Care Team include, but is not limited to: A doctor of medicine or osteopathy (Primary Care Provider if MD or DO) A registered nurse and/or nurse practitioner (Primary Care Provider if NP) A social worker A chaplain 8. Chaplain Services MCPs must provide access to chaplain services as needed as part of the palliative care team. Chaplain services provided as a palliative care service are not reimbursable through the Medi-Cal program. 9. Recommended Service: 24/7 Telephonic Palliative Care Support (separate from a routine advice line). Many palliative care programs include specialized telephonic support. This service is recommended but not required for MCPs, due to initial program development constraints. Additional notes on palliative care services: Identification of the specific palliative care services needed for an individual beneficiary is dependent on a palliative care consult and/or needs assessment process. Palliative care services should be aligned with the needs and decisions of the beneficiary. Research and discussions with palliative care experts indicate that the full range of palliative care services (physical, social, spiritual, and emotional) should be available to achieve the intended results in quality and cost-effectiveness measures. DHCS encourages MCPs and providers to provide palliative care consultations and SB 1004 Medi-Cal Palliative Care, September 1, 2016 Page 9
10 services in a manner that meets beneficiaries cultural needs. Resources and technical assistance on culturally sensitive palliative care is an emerging field, and DHCS supports further training and development in this area. B. Curative Care/Disease Modifying Care: As specified in SB 1004, beneficiaries electing not to enroll in hospice care but who meet the eligibility criteria for SB 1004 Medi-Cal palliative care may access both palliative care and curative care services that are medically necessary, as specified in current Medi-Cal statute and regulation. Essential to care coordination, the palliative care team and a plan of care will ensure coordination between curative care and palliative care services, particularly including the beneficiary s Primary Care Provider. Section 4: Providers Medi-Cal palliative care may be provided in a variety of settings, including inpatient, outpatient, or community-based, and therefore providers may vary based on the setting and needs of the patient. DHCS proposes that MCPs be provided flexibility in provider types, qualifications, and training requirements for palliative care, so long as the providers meet existing Medi-Cal regulations, Provider Bulletins, or All-Plan Letters. MCPs may contract with hospitals, long-term care facilities, clinics, hospice agencies, home health agencies, and other types of community-based providers that include licensed clinical staff. MCPs generally work with existing local providers, and may need to contract with several different types of providers depending on local provider qualifications and the need to reflect the diversity of provider types. However, palliative care services provided in a beneficiary s home must meet the applicable existing Medi-Cal requirements for in-home providers, services, and authorization, such as physician assessments, care plans, or home health agency regulations. Also, DHCS recommends that Community- Based Adult Services (CBAS) facilities be considered as a palliative care partner for facilitating advance care planning or palliative care referrals. Also, DHCS is authorized to expend up to $244,000 for palliative care provider training, and will provide further guidance on this funding and training to MCPs. In particular, DHCS recommends that providers of palliative care consultations or assessments have current palliative care training or certification. Further, results from existing palliative care programs highlight the importance of developing provider referral and education processes, as well as consumer information about palliative care. DHCS recommends that MCPs develop provider and consumer outreach plans when implementing SB 1004 palliative care programs. Section 5: Monitoring Outcomes and Performance Measures To track results from SB 1004, DHCS will require MCPs to periodically provide lists of SB 1004 palliative care beneficiary participants to the Department. Further guidance will be provided on any MCP requirements for additional data reporting, such as inpatient stays, emergency department visits, or hospice enrollment, as well as quality measures. SB 1004 Medi-Cal Palliative Care, September 1, 2016 Page 10
Partnership HealthPlan s Implementation of SB Robert Moore, MD MPH MBA. Chief Medical Officer, Partnership HealthPlan of California
 Partnership HealthPlan s Implementation of SB 1004 Robert Moore, MD MPH MBA Chief Medical Officer, Partnership HealthPlan of California Medi-Cal Managed Care Model: County Organized Health System Mission:
Partnership HealthPlan s Implementation of SB 1004 Robert Moore, MD MPH MBA Chief Medical Officer, Partnership HealthPlan of California Medi-Cal Managed Care Model: County Organized Health System Mission:
Hospice Basics and Benefits
 Hospice Basics and Benefits Goal To educate health care professionals about hospice basics and the benefits for the patient and family. 2 Objectives Describe the history and philosophy of the hospice movement
Hospice Basics and Benefits Goal To educate health care professionals about hospice basics and the benefits for the patient and family. 2 Objectives Describe the history and philosophy of the hospice movement
Palliative Care Quality Improvement Program (QIP) Measurement Specifications
 Palliative Care Quality Improvement Program (QIP) 2017-18 Measurement Specifications Developed by: QIP Team Contact: palliativeqip@partnershiphp.org Published on: October 6, 2017 Table of Contents Program
Palliative Care Quality Improvement Program (QIP) 2017-18 Measurement Specifications Developed by: QIP Team Contact: palliativeqip@partnershiphp.org Published on: October 6, 2017 Table of Contents Program
Transitions Guidelines: Chronic Illness Management. Revised 2016
 Transitions Guidelines: Chronic Illness Management Revised 2016 1 Table of Contents Introduction Transitions Program Pillars General Principles Regarding Admission Cancer Cirrhosis Congestive Heart Failure
Transitions Guidelines: Chronic Illness Management Revised 2016 1 Table of Contents Introduction Transitions Program Pillars General Principles Regarding Admission Cancer Cirrhosis Congestive Heart Failure
IEHP UM Subcommittee Approved Authorization Guidelines My Path (A Palliative Care Approach)
 UM_OTH 09 IEHP UM Subcommittee Approved Authorization Guidelines I. Policy: A. Inland Empire Health Plan (IEHP), in accordance with Senate Bill (SB) 1004, is dedicated to creating a community/home-based
UM_OTH 09 IEHP UM Subcommittee Approved Authorization Guidelines I. Policy: A. Inland Empire Health Plan (IEHP), in accordance with Senate Bill (SB) 1004, is dedicated to creating a community/home-based
Quality of Life (F309 End of Life) Interpretive Guidance Investigative Protocol
 483.25 Quality of Life (F309 End of Life) Interpretive Guidance Investigative Protocol 2 483.25 End of Life Each resident must receive and the facility must provide the necessary care and services to attain
483.25 Quality of Life (F309 End of Life) Interpretive Guidance Investigative Protocol 2 483.25 End of Life Each resident must receive and the facility must provide the necessary care and services to attain
Quality of Life (F309 End of Life) Surveyor Train the Trainer: Interpretive Guidance Investigative Protocol
 483.25 Quality of Life (F309 End of Life) Surveyor Train the Trainer: Interpretive Guidance Investigative Protocol 2 483.25 End of Life Each resident must receive and the facility must provide the necessary
483.25 Quality of Life (F309 End of Life) Surveyor Train the Trainer: Interpretive Guidance Investigative Protocol 2 483.25 End of Life Each resident must receive and the facility must provide the necessary
Objectives 2/11/2016 HOSPICE 101
 HOSPICE 101 Overview Hospice History and Statistics What is Hospice? Who qualifies for services? Levels of Service The Admission Process Why Not to Wait Objectives Understand how to determine hospice eligibility
HOSPICE 101 Overview Hospice History and Statistics What is Hospice? Who qualifies for services? Levels of Service The Admission Process Why Not to Wait Objectives Understand how to determine hospice eligibility
Life is pleasant. Death is peaceful. It s the transition that s troublesome. Isaac Asimov ( )
 Life is pleasant. Death is peaceful. It s the transition that s troublesome. Isaac Asimov (1920-1992) Objectives Palliative care versus hospice care. Admission guidelines to hospice services. Having the
Life is pleasant. Death is peaceful. It s the transition that s troublesome. Isaac Asimov (1920-1992) Objectives Palliative care versus hospice care. Admission guidelines to hospice services. Having the
Community and Mental Health Services. Palliative Care. Criteria and
 Community and Mental Health Services Specialist Palliative Care Service Referral Criteria and Guidance November 2018 Specialist Palliative Care Service Referrals These guidelines cover referrals for patients
Community and Mental Health Services Specialist Palliative Care Service Referral Criteria and Guidance November 2018 Specialist Palliative Care Service Referrals These guidelines cover referrals for patients
Coalition for Compassionate Care of California (CCCC)
 PALLIATIVE CARE FOR HEALTH HOME PROGRAM PATIENTS IN CALIFORNIA Leah Morris, RN, MPH, NP Director of Policy and Payer Relations Coalition for Compassionate Care of California. Lael Duncan, MD Medical Director
PALLIATIVE CARE FOR HEALTH HOME PROGRAM PATIENTS IN CALIFORNIA Leah Morris, RN, MPH, NP Director of Policy and Payer Relations Coalition for Compassionate Care of California. Lael Duncan, MD Medical Director
Specialist Palliative Care Service Referral Criteria and Guidance
 Specialist Palliative Care Service Referral Criteria and Guidance Specialist Palliative Care Service Referrals These guidelines cover referrals for patients with progressive terminal illness, whether
Specialist Palliative Care Service Referral Criteria and Guidance Specialist Palliative Care Service Referrals These guidelines cover referrals for patients with progressive terminal illness, whether
How Many Times? Result: an Unsatisfactory Outcome That Can Be Avoided
 Removing Obstacles to a Peaceful Death by Revising Health Professional Training and Payment Systems Professor Kathy L. Cerminara Nova Southeastern University Shepard Broad College of Law October 24, 2018
Removing Obstacles to a Peaceful Death by Revising Health Professional Training and Payment Systems Professor Kathy L. Cerminara Nova Southeastern University Shepard Broad College of Law October 24, 2018
Partners in Palliative Care Pilot Evaluation. James Cotter, MD MPH
 Partners in Palliative Care Pilot Evaluation James Cotter, MD MPH Partnership HealthPlan of California County Organized Health System 14 Northern California Counties 560,000 health plan members The Problem
Partners in Palliative Care Pilot Evaluation James Cotter, MD MPH Partnership HealthPlan of California County Organized Health System 14 Northern California Counties 560,000 health plan members The Problem
PALLIATIVE CARE IN NEW YORK STATE
 Collaborative for Palliative Care In collaboration with its partners End of Life Choices New York Finger Lakes Geriatric Education Center at the University of Rochester COLLABORATIVE FOR PALLIATIVE CARE
Collaborative for Palliative Care In collaboration with its partners End of Life Choices New York Finger Lakes Geriatric Education Center at the University of Rochester COLLABORATIVE FOR PALLIATIVE CARE
Palliative Care under a Value Based Reimbursement Model. Janet Bull MD, MBA, FAAHPM CMO Four Seasons
 Palliative Care under a Value Based Reimbursement Model Janet Bull MD, MBA, FAAHPM CMO Four Seasons Objectives o Describe palliative care o Discuss benefits of palliative care o Understand differences
Palliative Care under a Value Based Reimbursement Model Janet Bull MD, MBA, FAAHPM CMO Four Seasons Objectives o Describe palliative care o Discuss benefits of palliative care o Understand differences
Objectives. ORC Definition. Definitions of Palliative Care. CMS and National Quality Forum Definition (2013) CAPC 9/7/2017
 Objectives General overview of palliative care Define the role of palliative care Palliative Care Management and Transition Joan Hanson, Director of WRN Palliative Care, RN, CHPCA Jennifer Martnick, Team
Objectives General overview of palliative care Define the role of palliative care Palliative Care Management and Transition Joan Hanson, Director of WRN Palliative Care, RN, CHPCA Jennifer Martnick, Team
There For You. Your Compassionate Guide. World-Class Hospice Care Since 1979
 There For You Your Compassionate Guide World-Class Hospice Care Since 1979 What Is Hospice? Hospice is a type of care designed to provide support during an advanced illness. Hospice care focuses on comfort
There For You Your Compassionate Guide World-Class Hospice Care Since 1979 What Is Hospice? Hospice is a type of care designed to provide support during an advanced illness. Hospice care focuses on comfort
Palliative Care and Hospice. University of Illinois at Chicago College of Nursing
 Palliative Care and Hospice University of Illinois at Chicago College of Nursing 1 Learning Objectives Upon completion of this module, participants will be better able to: 1. Describe Palliative Care 2.
Palliative Care and Hospice University of Illinois at Chicago College of Nursing 1 Learning Objectives Upon completion of this module, participants will be better able to: 1. Describe Palliative Care 2.
Chapter 6. Hospice: A Team Approach to Care
 Chapter 6 Hospice: A Team Approach to Care Chapter 6: Hospice: A Team Approach to Care Comfort, Respect and Dignity in Dying Hospice care provides patients and family members with hope, comfort, respect,
Chapter 6 Hospice: A Team Approach to Care Chapter 6: Hospice: A Team Approach to Care Comfort, Respect and Dignity in Dying Hospice care provides patients and family members with hope, comfort, respect,
Specialist Palliative Care Referral for Patients
 Specialist Palliative Care Referral for Patients This guideline covers referrals for patients with progressive terminal illness, whether due to cancer or other disease. For many patients in the late stages
Specialist Palliative Care Referral for Patients This guideline covers referrals for patients with progressive terminal illness, whether due to cancer or other disease. For many patients in the late stages
August 16, Healthy Living Conference For Seniors and Caregivers VITAS 1. What we Know. Defining Palliative Care: Comfort. Symptom Management.
 Comfort. Symptom Management. Respect. & Hospice Care Pam Wright, LCSW Licensed Clinical Social Worker pamela.wright@vitas.com 626-918-2273 What we Know Defining : Palliative care is medical care that relieves
Comfort. Symptom Management. Respect. & Hospice Care Pam Wright, LCSW Licensed Clinical Social Worker pamela.wright@vitas.com 626-918-2273 What we Know Defining : Palliative care is medical care that relieves
What You Need To Know About Palliative Care. Natalie Wu Moy, LCSW, MSPA RUHS Medical Center Hospital Social Services Director
 What You Need To Know About Palliative Care Natalie Wu Moy, LCSW, MSPA RUHS Medical Center Hospital Social Services Director None of the faculty, planners, speakers, providers, nor CME committee members
What You Need To Know About Palliative Care Natalie Wu Moy, LCSW, MSPA RUHS Medical Center Hospital Social Services Director None of the faculty, planners, speakers, providers, nor CME committee members
Primary Palliative Care
 Primary Palliative Care Amanda Overstreet, DO October 20, 2017 No financial disclosures Objectives Discuss palliative care and how it differs from hospice Explore how to manage patients goals and expectations
Primary Palliative Care Amanda Overstreet, DO October 20, 2017 No financial disclosures Objectives Discuss palliative care and how it differs from hospice Explore how to manage patients goals and expectations
Palliative Care in the Community
 Palliative Care in the Community Carol Babcock, MFT Director Palliative Care, Navicent Health American College of Surgeons Commission on Cancer (CoC) Standard 2.4 Palliative care services are available
Palliative Care in the Community Carol Babcock, MFT Director Palliative Care, Navicent Health American College of Surgeons Commission on Cancer (CoC) Standard 2.4 Palliative care services are available
GUIDE TO PROGRAM DESIGN
 GUIDE GUIDE Palliative Care in the Home A GUIDE TO PROGRAM DESIGN PALLIATIVE CARE IN THE HOME: A GUIDE TO PROGRAM DESIGN Table of Contents Section 1 Introduction A Letter from Diane E. Meier, MD B Key
GUIDE GUIDE Palliative Care in the Home A GUIDE TO PROGRAM DESIGN PALLIATIVE CARE IN THE HOME: A GUIDE TO PROGRAM DESIGN Table of Contents Section 1 Introduction A Letter from Diane E. Meier, MD B Key
UND GERIATRIC MEDICINE FELLOWSHIP CURRICULUM HOSPICE AND PALLIATIVE CARE
 LOCATION SITE: HOSPICE OF THE RED RIVER VALLEY CONTACTS ATTENDING FACULTY: Tricia Langlois, M.D. Tricia.Langlois@hrrv.org Michelle Cooley, FNP-C Michelle.Cooley@hrrv.org SITE CONTACT: Brenda Iverson Brenda.Iverson@hrrv.org
LOCATION SITE: HOSPICE OF THE RED RIVER VALLEY CONTACTS ATTENDING FACULTY: Tricia Langlois, M.D. Tricia.Langlois@hrrv.org Michelle Cooley, FNP-C Michelle.Cooley@hrrv.org SITE CONTACT: Brenda Iverson Brenda.Iverson@hrrv.org
Founded in 1978 as Hospice of the North Shore. Know Your Choices. A Guide for People with Serious Illness
 Founded in 1978 as Hospice of the North Shore Know Your Choices A Guide for People with Serious Illness Advance Care Planning: Expressing Your Wishes In Massachusetts, all patients with serious advancing
Founded in 1978 as Hospice of the North Shore Know Your Choices A Guide for People with Serious Illness Advance Care Planning: Expressing Your Wishes In Massachusetts, all patients with serious advancing
A Quick Talk About Hospice As a Local Community Resource
 A Quick Talk About Hospice As a Local Community Resource 1 Agenda A Very Brief Overview of Hospice Care Your Local Hospice as a Greif & Bereavement Resource 2 David Stone, LCSW, ACSW, CAE Chief Executive
A Quick Talk About Hospice As a Local Community Resource 1 Agenda A Very Brief Overview of Hospice Care Your Local Hospice as a Greif & Bereavement Resource 2 David Stone, LCSW, ACSW, CAE Chief Executive
Karl Sash, MD Board Certified: Internal Medicine, Geriatrics, and Hospice and Palliative Medicine Medical Director, St Mary s Palliative Care
 Karl Sash, MD Board Certified: Internal Medicine, Geriatrics, and Hospice and Palliative Medicine Medical Director, St Mary s Palliative Care (Inpatient) Medical Director, Aseracare Hospice Evansville
Karl Sash, MD Board Certified: Internal Medicine, Geriatrics, and Hospice and Palliative Medicine Medical Director, St Mary s Palliative Care (Inpatient) Medical Director, Aseracare Hospice Evansville
Hospice and Palliative Care An Essential Component of the Aging Services Network
 Hospice and Palliative Care An Essential Component of the Aging Services Network Howard Tuch, MD, MS American Academy of Hospice and Palliative Medicine Physician Advocate, American Academy of Hospice
Hospice and Palliative Care An Essential Component of the Aging Services Network Howard Tuch, MD, MS American Academy of Hospice and Palliative Medicine Physician Advocate, American Academy of Hospice
Enabling the Transition to Hospice through Effective Palliative Care
 Enabling the Transition to Hospice through Effective Palliative Care Amber Jones, M.ED Center to Advance Palliative Care Objectives Identify continuity of care improvements to be realized by enhanced inpatient
Enabling the Transition to Hospice through Effective Palliative Care Amber Jones, M.ED Center to Advance Palliative Care Objectives Identify continuity of care improvements to be realized by enhanced inpatient
Cambia Palliative Care Metrics: Where are we and where are we going?
 Cambia Palliative Care Metrics: Where are we and where are we going? J. Randall Curtis, MD, MPH Director, Cambia Palliative Care Center of Excellence www.uwpalliativecarecenter.com Overview of System-Wide
Cambia Palliative Care Metrics: Where are we and where are we going? J. Randall Curtis, MD, MPH Director, Cambia Palliative Care Center of Excellence www.uwpalliativecarecenter.com Overview of System-Wide
Hospice & Palliative Care
 Patient-centered Medical Neighborhood Hospice & Palliative Care Our Hospice of South Central Indiana 2626 East 17th Street Columbus, IN 47201 812-314-8089 Schneck Medical Center Hospice & Palliative Care
Patient-centered Medical Neighborhood Hospice & Palliative Care Our Hospice of South Central Indiana 2626 East 17th Street Columbus, IN 47201 812-314-8089 Schneck Medical Center Hospice & Palliative Care
12/6/2016. Objective PALLIATIVE CARE IN THE NURSING HOME. Medical Care in the US. Palliative Care
 Objective PALLIATIVE CARE IN THE NURSING HOME Deborah Morris, M.D., M.H.S. Assistant Professor of Medicine The Glennan Center for Geriatrics and Gerontology Eastern Virginia Medical School Describe program
Objective PALLIATIVE CARE IN THE NURSING HOME Deborah Morris, M.D., M.H.S. Assistant Professor of Medicine The Glennan Center for Geriatrics and Gerontology Eastern Virginia Medical School Describe program
Hospice Eligibility August 2018
 Hospice Eligibility August 2018 Objectives Identify who can make a hospice referral Review hospice eligibility and disease-specific prognostic indicators Review Open Access philosophy Who Can Make A Referral
Hospice Eligibility August 2018 Objectives Identify who can make a hospice referral Review hospice eligibility and disease-specific prognostic indicators Review Open Access philosophy Who Can Make A Referral
Determining Eligibility for Hospice Care
 Determining Eligibility for Hospice Care Main Number: 203 739-8300 Toll Free Number: 888 357-3334 www.regionalhospicect.org Many people may not understand all that Regional Hospice can offer or they are
Determining Eligibility for Hospice Care Main Number: 203 739-8300 Toll Free Number: 888 357-3334 www.regionalhospicect.org Many people may not understand all that Regional Hospice can offer or they are
PART one. The Palliative Care Spectrum: Providing Care Across Settings
 PART one The Palliative Care Spectrum: Providing Care Across Settings Chapter 1 An Introduction to Palliative Pharmacy Care Jennifer M. Strickland To palliate means to alleviate. Palliative care, as the
PART one The Palliative Care Spectrum: Providing Care Across Settings Chapter 1 An Introduction to Palliative Pharmacy Care Jennifer M. Strickland To palliate means to alleviate. Palliative care, as the
Mapping Palliative Care Need and Supply in California: Methodology
 Mapping Palliative Care Need and Supply in California: Methodology February 2015 Kathleen Kerr, Kerr Healthcare Analytics Mike Rabow, MD, University of California San Francisco J. Brian Cassel, PhD, Virginia
Mapping Palliative Care Need and Supply in California: Methodology February 2015 Kathleen Kerr, Kerr Healthcare Analytics Mike Rabow, MD, University of California San Francisco J. Brian Cassel, PhD, Virginia
5/3/2012 PRESENTATION GOALS RESPIRATORY THERAPISTS ROLE IN END OF LIFE CARE FOR THE PULMONARY PATIENT
 RESPIRATORY THERAPISTS ROLE IN END OF LIFE CARE FOR THE PULMONARY PATIENT Presented by Carrie Black Bourassa, LRT, RRT PRESENTATION GOALS Define palliative care Define hospice care Discuss pulmonary hospice
RESPIRATORY THERAPISTS ROLE IN END OF LIFE CARE FOR THE PULMONARY PATIENT Presented by Carrie Black Bourassa, LRT, RRT PRESENTATION GOALS Define palliative care Define hospice care Discuss pulmonary hospice
Provider Operations Bulletin
 Provider Operations Bulletin JANUARY 2018 35 Gold Coast Health Plan Provider Operations Bulletin January 2018 35 2 Table of Contents SECTION 1: Palliative Care Update... 3 SECTION 2: Non-Emergency Medical
Provider Operations Bulletin JANUARY 2018 35 Gold Coast Health Plan Provider Operations Bulletin January 2018 35 2 Table of Contents SECTION 1: Palliative Care Update... 3 SECTION 2: Non-Emergency Medical
Palliative Care in the Community Setting. David Mandelbaum, MD Melissa Rockhill, MSN, GNP-BC Lorie Hacker, MSN, NP-C, CNE
 Palliative Care in the Community Setting David Mandelbaum, MD Melissa Rockhill, MSN, GNP-BC Lorie Hacker, MSN, NP-C, CNE Objectives 1. Discuss the framework for building a palliative care program in the
Palliative Care in the Community Setting David Mandelbaum, MD Melissa Rockhill, MSN, GNP-BC Lorie Hacker, MSN, NP-C, CNE Objectives 1. Discuss the framework for building a palliative care program in the
NeuroPI Case Study: Palliative Care Counseling and Advance Care Planning
 Case: An 86 year-old man presents to your office after recently being diagnosed as having mild dementia due to Alzheimer s disease, accompanied by his son who now runs the family business. At baseline
Case: An 86 year-old man presents to your office after recently being diagnosed as having mild dementia due to Alzheimer s disease, accompanied by his son who now runs the family business. At baseline
Hospice and Palliative Care: Value-Based Care Near the End of Life
 Hospice and Palliative Care: Value-Based Care Near the End of Life Mary Dittrich, MD, FASN Senior Medical Director, Remedy Partners Joseph W. Shega, MD National Medical Director, VITAS Healthcare 2017
Hospice and Palliative Care: Value-Based Care Near the End of Life Mary Dittrich, MD, FASN Senior Medical Director, Remedy Partners Joseph W. Shega, MD National Medical Director, VITAS Healthcare 2017
Hospice Care vs Palliative Care
 Hospice Care vs Palliative Care Easing the burden of illness, Improving quality of life Seasons Hospice and Palliative Care Cheryl Ledesma, FNP-BC Jacklyn Griffin, ACNP-BC Objectives After completing this
Hospice Care vs Palliative Care Easing the burden of illness, Improving quality of life Seasons Hospice and Palliative Care Cheryl Ledesma, FNP-BC Jacklyn Griffin, ACNP-BC Objectives After completing this
Palliative Care Series. Faculty School of Nursing
 Palliative Care Series Faculty School of Nursing Palliative Care Series The purpose of this series of education module is to provide adequate preparation and educational support for LVNs in their practice.
Palliative Care Series Faculty School of Nursing Palliative Care Series The purpose of this series of education module is to provide adequate preparation and educational support for LVNs in their practice.
Hospice and Palliative Care: Value-Based Care Near the End of Life
 Hospice and Palliative Care: Value-Based Care Near the End of Life Mary Dittrich, MD, FASN Senior Medical Director, Remedy Partners Joseph W. Shega, MD National Medical Director, VITAS Healthcare 2017
Hospice and Palliative Care: Value-Based Care Near the End of Life Mary Dittrich, MD, FASN Senior Medical Director, Remedy Partners Joseph W. Shega, MD National Medical Director, VITAS Healthcare 2017
Advocate Health Care Palliative Care Service Line
 Advocate Health Care Palliative Care Service Line Making the case for Palliative Care Approximately 90 million Americans are living with serious and life-threatening illness, and this number is expected
Advocate Health Care Palliative Care Service Line Making the case for Palliative Care Approximately 90 million Americans are living with serious and life-threatening illness, and this number is expected
Palliative Care Today. BJ Miller Zen Hospice Project May 29, 2014
 Palliative Care Today BJ Miller Zen Hospice Project May 29, 2014 Palliative Care Hospice Hospice Curative Care Palliative Care Diagnosis Death & Bereavement (Progression / Time) Existential/Spiritual Physical
Palliative Care Today BJ Miller Zen Hospice Project May 29, 2014 Palliative Care Hospice Hospice Curative Care Palliative Care Diagnosis Death & Bereavement (Progression / Time) Existential/Spiritual Physical
REPORT OF THE COUNCIL ON MEDICAL SERVICE
 REPORT OF THE COUNCIL ON MEDICAL SERVICE CMS Report -I- Subject: Presented by: Referred to: Concurrent Hospice and Curative Care (Resolution 0-I-) Peter S. Lund, MD, Chair Reference Committee J (Candace
REPORT OF THE COUNCIL ON MEDICAL SERVICE CMS Report -I- Subject: Presented by: Referred to: Concurrent Hospice and Curative Care (Resolution 0-I-) Peter S. Lund, MD, Chair Reference Committee J (Candace
Hospice Services. Prior Authorization Required: Additional Information:
 MP9299 Covered Service: Prior Authorization Required: Additional Information: Medicare Policy: BadgerCare Plus Policy: Yes when meets criteria below Yes None Prior authorization is dependent on the member
MP9299 Covered Service: Prior Authorization Required: Additional Information: Medicare Policy: BadgerCare Plus Policy: Yes when meets criteria below Yes None Prior authorization is dependent on the member
CareFirst Hospice. Health care for the end of life. CareFirst
 Hospice Health care for the end of life 1 What is Hospice? Hospice is a philosophy- When a person in end stages of an illness can no longer receive, or wants to receive, life sustaining treatment, he or
Hospice Health care for the end of life 1 What is Hospice? Hospice is a philosophy- When a person in end stages of an illness can no longer receive, or wants to receive, life sustaining treatment, he or
Trends in Hospice Utilization
 Proposed FY 2017 Hospice Wage Index and Rate Update and Hospice Quality Reporting Requirements To: NHPCO Provider Members From: Health Policy Team Date: April 25, 2016 On April 21, 2016, the Centers for
Proposed FY 2017 Hospice Wage Index and Rate Update and Hospice Quality Reporting Requirements To: NHPCO Provider Members From: Health Policy Team Date: April 25, 2016 On April 21, 2016, the Centers for
The Role of Palliative Care in Readmission Reduction Steven Z. Pantilat, MD
 The Role of Palliative Care in Readmission Reduction Steven Z. Pantilat, MD Professor of Clinical Medicine Alan M. Kates and John M. Burnard Endowed Chair in Palliative Care Director, Palliative Care Program
The Role of Palliative Care in Readmission Reduction Steven Z. Pantilat, MD Professor of Clinical Medicine Alan M. Kates and John M. Burnard Endowed Chair in Palliative Care Director, Palliative Care Program
Achieving earlier entry to hospice care: Issues and strategies. Sonia Lee, APN, GCNS-BC
 Achieving earlier entry to hospice care: Issues and strategies Sonia Lee, APN, GCNS-BC Objectives The learner will: Describe the benefits of hospice List at least barriers to early hospice care List at
Achieving earlier entry to hospice care: Issues and strategies Sonia Lee, APN, GCNS-BC Objectives The learner will: Describe the benefits of hospice List at least barriers to early hospice care List at
Session 127 PD - Palliative Care: Improving Quality While Lowering Cost. Moderator: Allison Silvers
 Session 127 PD - Palliative Care: Improving Quality While Lowering Cost Moderator: Allison Silvers Presenters: Torrie Fields Stan Hornbacher Allison Silvers SOA Antitrust Compliance Guidelines SOA Presentation
Session 127 PD - Palliative Care: Improving Quality While Lowering Cost Moderator: Allison Silvers Presenters: Torrie Fields Stan Hornbacher Allison Silvers SOA Antitrust Compliance Guidelines SOA Presentation
SANTA BARBARA COUNTY DEPARTMENT OF Behavioral Wellness A System of Care and Recovery
 Page 1 of 9 SANTA BARBARA COUNTY DEPARTMENT OF Behavioral Wellness A System of Care and Recovery Departmental Polley and Procedure Section Sub-section Alcohol and Drug Program (ADP) Effective: 7/11/2018
Page 1 of 9 SANTA BARBARA COUNTY DEPARTMENT OF Behavioral Wellness A System of Care and Recovery Departmental Polley and Procedure Section Sub-section Alcohol and Drug Program (ADP) Effective: 7/11/2018
Abby Woods, DNP, FNP Southern Illinois Healthcare Supportive Care Program END OF LIFE ISSUES IN THE CARE OF CARDIAC PATIENTS
 Abby Woods, DNP, FNP Southern Illinois Healthcare Supportive Care Program END OF LIFE ISSUES IN THE CARE OF CARDIAC PATIENTS Objectives Describe a team approach in the setting of critical illness Differentiate
Abby Woods, DNP, FNP Southern Illinois Healthcare Supportive Care Program END OF LIFE ISSUES IN THE CARE OF CARDIAC PATIENTS Objectives Describe a team approach in the setting of critical illness Differentiate
HOSPICE 101. Another choice for patients facing a terminal prognosis. De Anna Looper, RN, CHPN, CHPCA. Carrefour Associates L.L.C.
 HOSPICE 101 Another choice for patients facing a terminal prognosis. De Anna Looper, RN, CHPN, CHPCA Senior Vice President of Clinical Operations Carrefour Associates L.L.C. HOSPICE 101 Patients and their
HOSPICE 101 Another choice for patients facing a terminal prognosis. De Anna Looper, RN, CHPN, CHPCA Senior Vice President of Clinical Operations Carrefour Associates L.L.C. HOSPICE 101 Patients and their
The Palliative Home Care Program: Our Agency s Experience
 The Palliative Home Care Program: Our Agency s Experience NAHC Annual Meeting November 3, 2013 Washington, D.C. NAHC Annual Meeting November 3, 2013 Washington, D.C. Presented by: Karen Marshall Thompson,
The Palliative Home Care Program: Our Agency s Experience NAHC Annual Meeting November 3, 2013 Washington, D.C. NAHC Annual Meeting November 3, 2013 Washington, D.C. Presented by: Karen Marshall Thompson,
How Can Palliative Care Help Your Patient Get Home Sooner?
 How Can Palliative Care Help Your Patient Get Home Sooner? Annette T. Carron, D.O. Director Geriatrics and Palliative Care Botsford Hospital OMED 2014 Patient Care Issues That Can Delay Your Day/ Pain
How Can Palliative Care Help Your Patient Get Home Sooner? Annette T. Carron, D.O. Director Geriatrics and Palliative Care Botsford Hospital OMED 2014 Patient Care Issues That Can Delay Your Day/ Pain
Road Blocks in Non-Cancer Palliative Care Obstacles observed from outpatient non-cancer palliative practice.
 Road Blocks in Non-Cancer Palliative Care Obstacles observed from outpatient non-cancer palliative practice. 25th Annual Palliative Education and Research Days, West Edmonton Mall. Edmonton. 2014 Amanda
Road Blocks in Non-Cancer Palliative Care Obstacles observed from outpatient non-cancer palliative practice. 25th Annual Palliative Education and Research Days, West Edmonton Mall. Edmonton. 2014 Amanda
Case studies: palliative care in Vital Signs 2014: The State of Safety and Quality in Australian Health Care
 University of Wollongong Research Online Australian Health Services Research Institute Faculty of Business 2014 Case studies: palliative care in Vital Signs 2014: The State of Safety and Quality in Australian
University of Wollongong Research Online Australian Health Services Research Institute Faculty of Business 2014 Case studies: palliative care in Vital Signs 2014: The State of Safety and Quality in Australian
END-OF-LIFE DECISIONS HONORING THE WISHES OF A PERSON WITH ALZHEIMER S DISEASE
 END-OF-LIFE DECISIONS HONORING THE WISHES OF A PERSON WITH ALZHEIMER S DISEASE PREPARING FOR THE END OF LIFE When a person with late-stage Alzheimer s a degenerative brain disease nears the end of life
END-OF-LIFE DECISIONS HONORING THE WISHES OF A PERSON WITH ALZHEIMER S DISEASE PREPARING FOR THE END OF LIFE When a person with late-stage Alzheimer s a degenerative brain disease nears the end of life
Anne Kinderman, MD Director, Supportive & Palliative Care Service Zuckerberg San Francisco General Associate Clinical Professor of Medicine, UCSF
 Estimating the number of individuals eligible for SB1004 palliative care and appreciating baseline utilization patterns and costs in the final year of life Kathleen Kerr, BA Kerr Healthcare Analytics Anne
Estimating the number of individuals eligible for SB1004 palliative care and appreciating baseline utilization patterns and costs in the final year of life Kathleen Kerr, BA Kerr Healthcare Analytics Anne
Palliative Care for Older Adults in the United States
 Palliative Care for Older Adults in the United States Nathan Goldstein, MD Associate Professor Hertzberg Palliative Care Institute Brookdale Department of Geriatrics and Palliative Medicine Icahn School
Palliative Care for Older Adults in the United States Nathan Goldstein, MD Associate Professor Hertzberg Palliative Care Institute Brookdale Department of Geriatrics and Palliative Medicine Icahn School
Clinical Policy: Hospice Services Reference Number: PA.CP.MP.54
 Clinical Policy: Reference Number: PA.CP.MP.54 Effective Date: 01/18 Last Review Date: 10/17 Coding Implications Revision Log Description Medical necessity for hospice services. Policy It is the policy
Clinical Policy: Reference Number: PA.CP.MP.54 Effective Date: 01/18 Last Review Date: 10/17 Coding Implications Revision Log Description Medical necessity for hospice services. Policy It is the policy
There Is Something More We Can Do: An Introduction to Hospice and Palliative Care
 There Is Something More We Can Do: An Introduction to Hospice and Palliative Care presented to the Washington Patient Safety Coalition July 28, 2010 Hope Wechkin, MD Medical Director Evergreen Hospice
There Is Something More We Can Do: An Introduction to Hospice and Palliative Care presented to the Washington Patient Safety Coalition July 28, 2010 Hope Wechkin, MD Medical Director Evergreen Hospice
the sum of our parts. More than HOSPICE of the PIEDMONT
 More than the sum of our parts. HOSPICE of the PIEDMONT Hospice in-home care Hospice Home at high point grief counseling center kids path CARE CONNECTION Understanding your healthcare choices and talking
More than the sum of our parts. HOSPICE of the PIEDMONT Hospice in-home care Hospice Home at high point grief counseling center kids path CARE CONNECTION Understanding your healthcare choices and talking
Palliative Care & Hospice
 Palliative Care & Hospice Kenneth Brummel-Smith, M.D. Charlotte Edwards Maguire Professor, Department of Geriatrics Florida State University College of Medicine 1 Diane Meier, MD Director, Center to Advance
Palliative Care & Hospice Kenneth Brummel-Smith, M.D. Charlotte Edwards Maguire Professor, Department of Geriatrics Florida State University College of Medicine 1 Diane Meier, MD Director, Center to Advance
Incorporating a Dementia Stratagem into Your Practice Billing options, time management, and other considerations
 Incorporating a Dementia Stratagem into Your Practice Billing options, time management, and other considerations Steven L. Phillips, MD CEO/President Geriatric Specialty Care By permission of Johnny Hart
Incorporating a Dementia Stratagem into Your Practice Billing options, time management, and other considerations Steven L. Phillips, MD CEO/President Geriatric Specialty Care By permission of Johnny Hart
MODULE 1 PALLIATIVE NURSING CARE
 Curriculum MODULE 1 PALLIATIVE NURSING CARE Objectives Describe the role of the nurse in providing quality palliative care for patients across the lifespan. Identify the need for collaborating with interdisciplinary
Curriculum MODULE 1 PALLIATIVE NURSING CARE Objectives Describe the role of the nurse in providing quality palliative care for patients across the lifespan. Identify the need for collaborating with interdisciplinary
PALLIATIVE CARE The Relief You Need When You Have a Serious Illness
 PALLIATIVE CARE The Relief You Need When You Have a Serious Illness PALLIATIVE CARE: Improving quality of life when you re seriously ill. Dealing with any serious illness can be difficult. However, care
PALLIATIVE CARE The Relief You Need When You Have a Serious Illness PALLIATIVE CARE: Improving quality of life when you re seriously ill. Dealing with any serious illness can be difficult. However, care
SUPPLEMENTAL NOTE ON HOUSE BILL NO. 2031
 SESSION OF 2018 SUPPLEMENTAL NOTE ON HOUSE BILL NO. 2031 As Amended by Senate Committee on Public Health and Welfare Brief* HB 2031, as amended, would create the Palliative Care and Quality of Life Interdisciplinary
SESSION OF 2018 SUPPLEMENTAL NOTE ON HOUSE BILL NO. 2031 As Amended by Senate Committee on Public Health and Welfare Brief* HB 2031, as amended, would create the Palliative Care and Quality of Life Interdisciplinary
Hospice Quality Reporting Program: Specifications for the Hospice Item Set- Based Quality Measures
 April 2016 Hospice Quality Reporting Program: Specifications for the Hospice Item Set- Based Quality Measures Prepared for Center for Clinical Standards and Quality Centers for Medicare & Medicaid Services
April 2016 Hospice Quality Reporting Program: Specifications for the Hospice Item Set- Based Quality Measures Prepared for Center for Clinical Standards and Quality Centers for Medicare & Medicaid Services
Clinical Policy: Hospice Services Reference Number: CP.MP.54
 Clinical Policy: Reference Number: CP.MP.54 Effective Date: 05/13 Last Review Date: 07/16 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.54 Effective Date: 05/13 Last Review Date: 07/16 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Approved Care Model for Project 3gi: Integration of Palliative Care into the PCMH Model
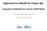 1 Approved Care Model for Project 3gi: Integration of Palliative Care into the PCMH Model OneCity Health Webinar January 13, 2016 Overview of presentation 2 Approach to care model development Project overview
1 Approved Care Model for Project 3gi: Integration of Palliative Care into the PCMH Model OneCity Health Webinar January 13, 2016 Overview of presentation 2 Approach to care model development Project overview
Three triggers that suggest that patients could benefit from a hospice palliative care approach
 Why is it important to identify people nearing the end of life? About 1% of the population dies each year. Although some deaths are unexpected, many more in fact can be predicted. This is inherently difficult,
Why is it important to identify people nearing the end of life? About 1% of the population dies each year. Although some deaths are unexpected, many more in fact can be predicted. This is inherently difficult,
The Changing Landscape of Palliative Care
 The Changing Landscape of Palliative Care KAHPC 17th Annual Conference August 2015 Brian Jones Joe Rotella Elizabeth Wessels Turner West Kay Williams Why Home-based Palliative Care? Turner West, MPH, MTS
The Changing Landscape of Palliative Care KAHPC 17th Annual Conference August 2015 Brian Jones Joe Rotella Elizabeth Wessels Turner West Kay Williams Why Home-based Palliative Care? Turner West, MPH, MTS
Understanding Hospice, Palliative Care and of-life Issues
 Understanding Hospice, Palliative Care and End-of of-life Issues Huntington's Disease Society of America June 2009 Roseanne Berry, MS, RN RBC Consulting, LLC roseanne@rbcconsultingllc.com The information
Understanding Hospice, Palliative Care and End-of of-life Issues Huntington's Disease Society of America June 2009 Roseanne Berry, MS, RN RBC Consulting, LLC roseanne@rbcconsultingllc.com The information
PATH. On the right. Suggested Websites. For Patients with a Serious Illness. PATH is a service provided by:
 On the right PATH For Patients with a Serious Illness transitional care for patients with a serious illness Suggested Websites hospicesacredheart.org seriousillness.org/nepa elderlawanswers.com caringinfo.org
On the right PATH For Patients with a Serious Illness transitional care for patients with a serious illness Suggested Websites hospicesacredheart.org seriousillness.org/nepa elderlawanswers.com caringinfo.org
Objectives. End-of-Life Exercise. Palliative Care Can Help Patients and Decrease 30-Day Hospital Readmissions.
 Palliative Care Can Help Patients and Decrease 30-Day Hospital Readmissions. Objectives Describe how palliative care meets the needs of the patient and family. Discuss how out-patient palliative care can
Palliative Care Can Help Patients and Decrease 30-Day Hospital Readmissions. Objectives Describe how palliative care meets the needs of the patient and family. Discuss how out-patient palliative care can
SENATE AND ASSEMBLY HEARING ON THE EXECUTIVE HEALTH BUDGET PROPOSAL
 2017-2018 SENATE AND ASSEMBLY HEARING ON THE EXECUTIVE HEALTH BUDGET PROPOSAL February 16, 2017 Testimony from the Hospice and Palliative Care Association of New York State Introduction The Hospice and
2017-2018 SENATE AND ASSEMBLY HEARING ON THE EXECUTIVE HEALTH BUDGET PROPOSAL February 16, 2017 Testimony from the Hospice and Palliative Care Association of New York State Introduction The Hospice and
How to Integrate Peer Support & Navigation into Care Delivery
 How to Integrate Peer Support & Navigation into Care Delivery Andrew Bertagnolli, PhD Care Management Institute Why Integrate Peer Support into the Care Delivery Pathway? Improved health Increased feelings
How to Integrate Peer Support & Navigation into Care Delivery Andrew Bertagnolli, PhD Care Management Institute Why Integrate Peer Support into the Care Delivery Pathway? Improved health Increased feelings
Palliative Care In PICU
 Palliative Care In PICU Professor Lucy Lum University Malaya Annual Scientific Meeting on Intensive Care 15 August 2015 2 Defining Palliative Care: Mistaken perception: For patients whom curative care
Palliative Care In PICU Professor Lucy Lum University Malaya Annual Scientific Meeting on Intensive Care 15 August 2015 2 Defining Palliative Care: Mistaken perception: For patients whom curative care
Module 1: Principles of Palliative Care. Part I: Dying Well. A Good Death Defined
 E L N E C End-of-Life Nursing Education Consortium Geriatric Curriculum Module 1: Principles of Palliative Care Part I: Dying Well A natural part of life Opportunity for growth Profoundly personal experience
E L N E C End-of-Life Nursing Education Consortium Geriatric Curriculum Module 1: Principles of Palliative Care Part I: Dying Well A natural part of life Opportunity for growth Profoundly personal experience
Ministry of Health and Long-Term Care. Palliative Care. Follow-Up on VFM Section 3.08, 2014 Annual Report RECOMMENDATION STATUS OVERVIEW
 Chapter 1 Section 1.08 Ministry of Health and Long-Term Care Palliative Care Follow-Up on VFM Section 3.08, 2014 Annual Report RECOMMENDATION STATUS OVERVIEW # of Status of Actions Recommended Actions
Chapter 1 Section 1.08 Ministry of Health and Long-Term Care Palliative Care Follow-Up on VFM Section 3.08, 2014 Annual Report RECOMMENDATION STATUS OVERVIEW # of Status of Actions Recommended Actions
Palliative Care to Hospice: Forging an Effective Partnership. Dennis Cox, LCSW
 Palliative Care to Hospice: Forging an Effective Partnership Dennis Cox, LCSW The Old Days Home Care or Hospice There was a clear choice Physicians needed to take a stand Have the Hospice conversation
Palliative Care to Hospice: Forging an Effective Partnership Dennis Cox, LCSW The Old Days Home Care or Hospice There was a clear choice Physicians needed to take a stand Have the Hospice conversation
Integrating Palliative and Oncology Care in Patients with Advanced Cancer
 Integrating Palliative and Oncology Care in Patients with Advanced Cancer Jennifer Temel, MD Massachusetts General Hospital Cancer Center Director, Cancer Outcomes Research Overview 1. Why should we be
Integrating Palliative and Oncology Care in Patients with Advanced Cancer Jennifer Temel, MD Massachusetts General Hospital Cancer Center Director, Cancer Outcomes Research Overview 1. Why should we be
Know Your Choices: A Guide for Patients with Serious Advancing Illness
 Know Your Choices: A Guide for Patients with Serious Advancing Illness In Massachusetts, all patients with serious advancing illness have a legal right to receive information about their medical conditions,
Know Your Choices: A Guide for Patients with Serious Advancing Illness In Massachusetts, all patients with serious advancing illness have a legal right to receive information about their medical conditions,
Transitional Care With Palliative Medicine
 Bridging The Gaps: Providing Transitional Care With Palliative Medicine Angie Hollis-Sells, RN, CHPN President AseraCare Robert Parker, RN, MSN Ed., CHPN Program Manager Bridging The Gaps: Proving Transitional
Bridging The Gaps: Providing Transitional Care With Palliative Medicine Angie Hollis-Sells, RN, CHPN President AseraCare Robert Parker, RN, MSN Ed., CHPN Program Manager Bridging The Gaps: Proving Transitional
Enhancing Care Management with a Palliative Care Partnership
 Enhancing Care Management with a Palliative Care Partnership Presented by: Brian Michaelsen, Administrator Family Hospice Care HERITAGE PROVIDER NETWORK HPN is a limited Knox Keene licensed organization
Enhancing Care Management with a Palliative Care Partnership Presented by: Brian Michaelsen, Administrator Family Hospice Care HERITAGE PROVIDER NETWORK HPN is a limited Knox Keene licensed organization
FINANCES OF PALLIATIVE CARE
 FINANCES OF PALLIATIVE CARE Andrew Molosky, MBA Vice President of Operations Seasons Hospice & Palliative Care Learning Objectives: Distinguish and identify the unique needs of one's organization as it
FINANCES OF PALLIATIVE CARE Andrew Molosky, MBA Vice President of Operations Seasons Hospice & Palliative Care Learning Objectives: Distinguish and identify the unique needs of one's organization as it
MEDICAID WAIVERS FOR PEOPLE WITH INTELLECTUAL DISABILITIES OR AUTISM
 (800) 692-7443 (Voice) (877) 375-7139 (TDD) www.disabilityrightspa.org MEDICAID WAIVERS FOR PEOPLE WITH INTELLECTUAL DISABILITIES OR AUTISM Pennsylvania s Medical Assistance ( Medicaid ) program includes
(800) 692-7443 (Voice) (877) 375-7139 (TDD) www.disabilityrightspa.org MEDICAID WAIVERS FOR PEOPLE WITH INTELLECTUAL DISABILITIES OR AUTISM Pennsylvania s Medical Assistance ( Medicaid ) program includes
Pediatric Palliative Care and Having Difficult Conversations
 Pediatric Palliative Care and Having Difficult Conversations UCSF Pediatric Neurology and Palliative Care Audrey Foster-Barber, MD, PhD Pediatric Hospital Medicine Boot Camp 6/14 Palliative Care A philosophy
Pediatric Palliative Care and Having Difficult Conversations UCSF Pediatric Neurology and Palliative Care Audrey Foster-Barber, MD, PhD Pediatric Hospital Medicine Boot Camp 6/14 Palliative Care A philosophy
Clinical Policy: Hospice Services Reference Number: CA.CP.MP.54
 Clinical Policy: Reference Number: CA.CP.MP.54 Effective Date: 05/13 Last Review Date: 01/18 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CA.CP.MP.54 Effective Date: 05/13 Last Review Date: 01/18 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
patient decision aid advanced lung cancer
 patient decision aid advanced lung cancer Introduction This aid is meant to supplement conversations with your care team. Patients who have used a decision aid like this said it helped them make care choices
patient decision aid advanced lung cancer Introduction This aid is meant to supplement conversations with your care team. Patients who have used a decision aid like this said it helped them make care choices
Hospice Approach to Caring Ellen M. Brown M.D.
 Hospice Approach to Caring Ellen M. Brown M.D. bjectives By the conclusion of this session, attendees will be able to: Explain the hospice philosophy and goals Understand what is covered by the hospice
Hospice Approach to Caring Ellen M. Brown M.D. bjectives By the conclusion of this session, attendees will be able to: Explain the hospice philosophy and goals Understand what is covered by the hospice
