WHAT YOU NEED TO KNOW ABOUT PARKINSON'S DISEASE
|
|
|
- Elvin Stafford
- 5 years ago
- Views:
Transcription
1 Definition WHAT YOU NEED TO KNOW ABOUT PARKINSON'S DISEASE Parkinson's Disease develops gradually, often starting with a barely noticeable tremor in just one hand. But while the tremor may be the most well know sign of Parkinson's Disease, the disorder also commonly causes a slowing or freezing of movement. Friends and family may notice that your face shows little or no expression and your arms don't swing when you walk. Speech often becomes soft and mumbling. Parkinson's symbols tend to worsen as the disease progresses. While there is no cure for Parkinson's Disease, many different types of medicines can treat it's symptoms. In some cases your doctor may suggest surgery. Symptoms: The symptoms of Parkinson's Disease vary from person to person. Early signs may be subtle and can go unnoticed for months or years. Symptoms typically begin on one side of the body and usually remain worse on that side. Parkinson's signs and symptoms may include: Causes Tremor- The characteristic shaking associated with Parkinson's Disease often begins in a hand. A back-andforth rubbing of your thumb and forefinger, known as pie-rolling, is common. However, many people with Parkinson's Disease do not experience substantial tremor. Slow motion (bradykinesia)- Over time, Parkinson's Disease may reduce your ability to initiate voluntary movement. This may make even the simplest tasks difficult and time-consuming. When you walk, your steps may become short and shuffling. Or your feet may freeze to the floor, making it hard to take the first step. Rigid muscles- Muscle stiffness often occurs in your limbs and neck. Sometimes the stiffness can be so severe that it limits the range of your movements and causes pain. Impaired posture and balance- Your posture may become stooped as a result of Parkinson's Disease. Imbalance is also common, although this is usually mild until the later stages of the disease. Loss of automatic movements- Blinking, smiling, and swinging your arms when you walk are all unconscious acts that are a normal part of being human. In Parkinson's Disease, these acts tend to be diminished and even lost. Some people may develop a fixed staring expression and unblinking eyes. Others my no longer gesture or seem animated when they speak. Speech changes- Many people with Parkinson's Disease have problems with speech. You may speak more softly, rapidly, or in a monotone, sometimes slurring or repeating words, or hesitating before speaking. Dementia- In the later stages of Parkinson's Disease, some people develop problems with memory and mental clarity. Alzheimer's drugs appear to alleviate some of these symptoms to a mild degree. Many symptoms of Parkinson's Disease result from the lack of a chemical messenger, called dopamine, in the brain. This occurs when the specific brain cells that produce dopamine die or become impaired. But researchers still aren't certain about what sets this chain of events in motion. Some theorize that genetic mutations or environmental toxins may play a role in Parkinson's Disease. Risk Factors Risk factors for Parkinson's Disease include: Age- Young adults very rarely experience Parkinson's Disease. It ordinarily begins in middle or late life, and the risk continues to increase with age. Heredity- Having one or more close relatives with Parkinson's increases the chances that you'll also develop the disease, although your risk is still less than 5%. Recent evidence suggests a crucial role for small contributions from many different genes that program brain architecture. Sex- Men are more likely to develop Parkinson's Disease than women are. Exposure to toxins- Ongoing exposure to herbicides and pesticides puts you at slightly increased risk of Parkinson's.
2 Complications Parkinson's Disease is often accompanied by these additional problems: Depression- This can occur even before other Parkinson's symptoms. Receiving treatment for depression can make it easier to handle the other challenges of Parkinson's Disease. Sleep problems- People with Parkinson's Disease often have trouble falling asleep and may wake up frequently throughout the night. They may also experience sudden sleep onset, called sleep attacks, during the day. Difficulty chewing and swallowing- The muscles you use to swallow may be affected in the later stages of the disease, making eating more difficult. Urinary problems- Parkinson's Disease may cause either urinary incontinence or urine retention. Certain medications used to treat Parkinson's also can make it difficult to urinate. Constipation- Many people with Parkinson's Disease develop constipation because the digestive tract works more slowly. Constipation may also be a side effect of medications used to treat the disease. Sexual dysfunction- Some people with Parkinson's Disease may notice a decrease in sexual desire. This may stem from a combination of psychological and physical factors, or it may be the result of physical factors alone. Medications for Parkinson's Disease also may cause a number of complications, including involuntary twitching or jerking movements of the arms or legs, hallucinations, sleepiness, and a drop in blood pressure when standing up. Healthy Eating Eat a nutritionally balanced diet that contains plenty of fluids, vegetables, and whole grains. These foods are high in fiber, which is important for helping prevent the constipation that is common in Parkinson's Disease. If you take a fiber supplement, such a psyllium powder, Metamucil, or Citrucel, be sure to introduce it gradually and drink plenty of fluids daily. Otherwise, your constipation may become worse. If you find that fiber helps your symptoms, use it on a regular basis for the best results. Walking With Care Parkinson's Disease can disturb your sense of balance, making it difficult to walk with a normal gait. These suggestions may help: Try not to move too quickly. Aim for your heel to strike the floor first when you're walking. If you notice yourself shuffling, stop and check your posture. It's best to stand up straight with your head over your hips and your feet eight to ten inches apart. Avoiding Falls In the later stages of the disease, you may fall more easily. That's because Parkinson's Disease affects the balance and coordination centers in the brain. In fact, you may be thrown off balance by just a small push or bump. The following suggestions may help: Don't pivot your body over your feet while turning. Instead, make a U-turn. Don't lean or reach. Keep your center of gravity over your feet. Don't carry things while walking. Avoid walking backward. Dressing Dressing can be the most frustrating of all activities for someone with Parkinson's Disease. The loss of fine-motor control makes it hard to button and zip clothes, and even to step into a pair of pants. A physical therapist can point out techniques that make daily activities easier. These suggestions also may help: Allow plenty of time so that you don't feel rushed.
3 Lay clothes nearby. Choose clothes that you can slip on easily, such as sweat pants, simple dresses, or pants with elastic waistbands. Use fabric fasteners, such as Velcro, instead of buttons. PROVIDING CARE FOR PARKINSON'S DISEASE Constant reassurance that my loved ones are supportive, patient, caring, understanding, and loving is, I believe, my greatest asset and most secure source of happiness. Dwight C. McGoon, M.D., a Mayo Clinic surgeon with Parkinson's Disease. High-fashion thermos coffee mugs, electric toothbrushes, hand-held shower heads, and yes, satin sheets- these are just a few of the items that make life easier for a person with Parkinson's Disease. Read on to learn more about providing care for a person with Parkinson's Disease. Take Charge of Parkinson's A cure hasn't yet been found, but that doesn't mean there are no effective treatments for the symptoms of Parkinson's. If one approach to treatment doesn't work, insist that others be considered. Take charge. Learn the course Parkinson's may take in the future and be prepared for changes in the level of care you will have to provide. Parkinson's is life altering, not life threatening. This means life with PD will change. All the same pleasures are out there to be enjoyed; they just need a bit of modification. If your care recipient enjoyed running, some of the same enjoyment of the outdoors comes with walking. Look for versions of the same kinds of activities to keep your care recipient active, independent and interested in life. Stress and Anxiety The symptoms of tremor, rigidity and bradykinesia (abnormal slowness of movement) are made worse by anxiety, stress, and pressure. Be a calming influence. Don't pressure your care recipient to speed up. The anxiety you create will make movement slower. Depression Up to 50% of people with Parkinson's suffer from depression. Watch for signs of depression and get treatment for your care recipient right away. Depression can affect short-term memory and concentration that will aggravate Parkinson's Disease. There is a risk of suicide. The signs of depression include: sadness suicidal ideas sleep disturbance fatigue problems concentrating weight loss or gain appetite change (usually loss) feelings of worthlessness anxiety irritability apathy unwillingness to socialize loss of interest in sex and reduced performance
4 Depression and Parkinson's Disease share the symptoms of fatigue and anxiety. The trick is to sense an unexplained increase in these symptoms that may be caused by depression. Constipation Parkinson's and it's medications combine to make constipation a problem. Take pre ventative action to avoid a crisis that will need medical attention. Increase fluid intake, especially in hot weather. Your care recipient should drink eight cups of fluid every day. High-fiber foods are traditionally recommended to prevent constipation but these may cause intestinal gas and cramping that are not tolerated by an older person with Parkinson's. Instead of raw fruits and vegetables, nutritionists recommend dried fruits, hot prune juice, canned fruits and soft cooked vegetables. If you introduce bran or high fiber cereal into the diet, start slowly with small amounts and increase fluid intake. Fatigue Persons with Parkinson's have to pace their activities and take lots of rest breaks. It isn't lazy; it's smart. When your care recipient is having a really good day, feeling well and full of energy, there will be a tendency to do too much. Gently remind him or her that overdoing it will mean exhaustion and inactivity for the next couple of days. Better to ration that new-found energy. Irritability and Frustration Everyday tasks take longer with Parkinson's. They may take even longer on bad days. Allow time for this. Don't rush. Respond with tact and humor, not irritability and frustration. Place yourself in the mind and body of your care recipient and imagine how irritated and frustrated he or she must feel. If it's a bad day, set some activities aside for another day and do just what is possible and necessary. If you don't make these allowances, you create a stressful situation that aggravates the Parkinson's symptoms and may actually slow your care recipient even further. There's always tomorrow. Pets They are wonderful companions but be careful that they aren't surprise obstacles that cause tripping or falling. Drugs Some medications may cause nightmares and vivid dreams. Taking medications a few hours ahead of bedtime may help. Reactions to the dreams may make the sleeper noisy and violent. The person with Parkinson's will sleep on while the rest of the household thinks war has broken out. Hallucinations may be another side effect. Your care recipient may see small animals or children. Usually the patient knows it isn't real but if he or she insists It's real, maybe you should pay attention. One family got a bit of a surprise. Their family member with Parkinson's insisted that there was a mouse in their home. No one believed her until she presented them with a dead mouse in a trap. If your care recipient sees a number of physicians, make sure all physicians know the complete list of medications your care recipient is taking. This will help prevent unpleasant or dangerous drug interactions. It's a good idea to consult your pharmacist. Be careful about botanical or natural remedies. Ask your physician for advice. These remedies may interact with the medications your care recipient is already taking. Never change dosages without guidance from your physician. Exercise A well-designed exercise program can increase the benefits of Parkinson's medication, fight depression, and promote an overall sense of well being. Your care recipient will benefit from three types of exercise: Stretching and range-of-motion exercises to maintain joint and soft tissue flexibility. Strengthening exercises to improve and maintain strength of abdominal and back muscles. Aerobic exercises to aid cardio-respiratory fitness.
5 Prevent fatigue by pacing short exercise sessions throughout the day. Join in with your care recipient. It's good for you too. Don't stick to a rigid schedule. Instead, help your care recipient exercise when medications are working well and movement is easier. Urge your care recipient to be patient. The gains of regular exercise are not immediately obvious but the will come with time. Exercise should be fun. Look for organized programs at local community or commercial centers. If there is a Parkinson's support group in your community, they may offer programs specially designed for your care recipient. It may be possible to combine exercise with some social activities that are so important in fighting depression and maintaining a sense of independence. Walking It's great exercise for you and your care recipient. Here are some tips that make it easier and safer for someone with Parkinson's. Help your care recipient by encouraging him or her to stand up as straight as possible. Heads up- avoid looking at the ground. At home, remove unnecessary furniture and anything on the floor like loose rugs that could cause a fall. Avoid shoes with rubber or crepe souls. They can stick to the floor and cause a tumble. See a physiotherapist for tips on helping your care recipient if there are problems with starting, stopping, or maintaining momentum when walking. Offer your arm as support but try to avoid hanging on to your care recipient. It's easier for a person with Parkinson's to maintain balance if he or she isn't pinned to your side. To prevent falls, encourage your care recipient to consciously lift each foot. This strategy combats the foot drag that may come with Parkinson's. When turning, a person with Parkinson's should avoid pivoting on one foot to change direction. Balance problems make this a dangerous maneuver that leads to falls. It works better to take several steps in a U-turn. If your care recipient appears to freeze, feet glued to the floor or sidewalk, you can be sure that is exactly how it feels. Remain calm and quiet while he or she concentrates on getting going again. You can work together to find ways to overcome this temporary problem. Try rocking from side to side to get the feeling of moving again, or tell him or her to imagine stepping over a crack in the sidewalk or a small object immediately in front of one foot. You might try '1-2-3-go' or bending the arms and swinging them to set the rhythm for walking. Make it Easier in the Kitchen Here are some hints to encourage your care recipient to help out in the kitchen: 1. Be patient. People with Parkinson's move slowly and take longer to get things done. Allow extra time. 2. Use a microwave to shorten cooking times. This leaves more time for your care recipient to get food ready for cooking. It means less pressure to hurry. 3. Encourage your care recipient to sit rather than stand. It's less tiring and safer if balance is a concern. 4. Provide a cart with wheels- like a tea trolley- for moving things. It takes less energy and has the added advantage of providing support for maintaining balance. 5. Keep frequently used items like the kettle, teapot, and tea at countertop level. A lazy susan is ideal for making items accessible. Safety in the Bathroom The greatest danger is falling. The bathroom floor, bathtub, and shower are slick and slippery when wet. There isn't anything in the house more punishing in a fall than the unyielding sides of the bathtub. Install a grab bar by the tub or in the shower. Test it to be sure you feel confident it will hold your care recipient's weight. Don't use a wall-mounted soap dish or a towel rack as a substitute. If your care recipient is unsteady in the shower, get a shower bench. It's like a waterproof chair for the shower. If you don't have a hand-held shower head, install one on the existing shower head outlet. It makes a 'sitting-down shower' much easier. Non-skid strips or rubber mats in the tub or shower are a good idea but you have to be careful. If they accumulate soap residue, they are just as slippery as the yub or shower.
6 Use soap on a rope. It's always within reach and stays out from under your feet! Getting on and off the toilet can be a real challenge for someone with Parkinson's when the toilet is quite low relative to the floor. Use a raised toilet seat with armrests to help maintain balance and prevent falls. Consider getting your care recipient an electric toothbrush. It isn't a safety issue; it just does a better job cleaning teeth because it mimics the quick wrist movements that can be difficult for someone with Parkinson's. Comfort in the Bedroom Getting in and out of bed and turning in bed can be a real problem for your care recipient. These tips will make it easier: Adjust the height of the bed so it is neither too high nor too low. If you thought satin sheets were only for the rich and famous, you're in for a surprise. These slinky bed linens are great for Parkinson's because they make it much easier to turn and move in bed. There are different approaches to help your care recipient got into bed. You might suggest sitting on the edge of the bed, lowering sideways onto an elbow, and then bringing the legs up onto the bed. Try having your care recipient kneel on the bed and crawl further onto the bed and then lower his or her body sideways. Another choice is to have your care recipient sit on the edge of the bed and fall back onto a pillow. Then you can help raise his or her legs onto the bed. Turning in bed can be difficult if your care recipient has trouble initiating movement or is rigid. Suggest that he or she bend the knees and place the feet flat on the bed. Then he or she can turn the head in the direction of the turn. By reaching across the body toward the edge of the bed, the trunk and hip will follow- like rolling a log. It helps if they can grab the edge of the bed or a grab bar on an adjacent wall. This is where satin sheets make sliding and turning much easier. Getting out of bed is much like getting in. With your care recipient on his or her side, bend the knees toward the chest so the feet are near the edge of the bed. By supporting him or her with a forearm, the care recipient can push up using an elbow and hands and at the same time swing the feet over the edge of the bed onto the floor. An occupational therapist will have further suggestions that apply to your specific situation. Falls As Parkinson's progresses, gait (the kind of step used in walking) and balance problems are more pronounced. Hard as you try to prevent it, a fall may happen. Keep these points in mind, just in case: When a fall happens at home, encourage your care recipient to stay still and rest in a comfortable position for a few moments before getting up. Remain calm. If your care recipient becomes anxious, it will be more difficult to get up. If there appears to be injuries that would be aggravated by trying to get up, call for medical help. Don't attempt to lift the person from the floor unless you have been trained to do it in a way that won't cause you to injure yourself. If there are no apparent injuries, bring a chair to your care recipient and ask him or her to roll onto hands and knees. Have him or her bend one leg and put a foot firmly on the floor. With the opposite arm on the chair, your care recipient can use arms and legs to push up to a standing position. Provide support in case of dizziness or lightheadedness. Have a hug, a laugh, and a cup of tea.
Prevent Falls. with the Moore Balance Brace. Many falls can be prevented. By making minor changes, you can lower your chances of falling
 Prevent Falls with the Moore Balance Brace Many falls can be prevented. By making minor changes, you can lower your chances of falling Moore Balance Brace (MBB) Instructions for use Putting the MBB into
Prevent Falls with the Moore Balance Brace Many falls can be prevented. By making minor changes, you can lower your chances of falling Moore Balance Brace (MBB) Instructions for use Putting the MBB into
Hip Resurfacing with Precautions. Therapy Resources. xpe045 (4/2015) AHC
 Hip Resurfacing with Precautions Therapy Resources xpe045 (4/2015) AHC Hip Resurfacing Home Exercise Program - Phase I 1. Breathing Exercises Exercise can be done while sitting or lying down. Action: Place
Hip Resurfacing with Precautions Therapy Resources xpe045 (4/2015) AHC Hip Resurfacing Home Exercise Program - Phase I 1. Breathing Exercises Exercise can be done while sitting or lying down. Action: Place
Total Knee Arthroplasty
 Total Knee Arthroplasty Moving safely after surgery Walking Goal: Placing each foot in front of the other as naturally as possible. 1. Using either a walker or forearm crutches, step forward with the surgical
Total Knee Arthroplasty Moving safely after surgery Walking Goal: Placing each foot in front of the other as naturally as possible. 1. Using either a walker or forearm crutches, step forward with the surgical
Taking Care of Your Back
 Taking Care of Your Back Most people will feel back pain at some point in their lives, but not all back pain is the same for everyone. The good news is, most low back pain improves without any treatment
Taking Care of Your Back Most people will feel back pain at some point in their lives, but not all back pain is the same for everyone. The good news is, most low back pain improves without any treatment
Posterior Total Hip Replacement with Precautions. Therapy Resources
 Posterior Total Hip Replacement with Precautions Therapy Resources The information presented is intended for general information and educational purposes. It is not intended to replace the advice of your
Posterior Total Hip Replacement with Precautions Therapy Resources The information presented is intended for general information and educational purposes. It is not intended to replace the advice of your
GETTING READY FOR TOTAL HIP REPLACEMENT
 GETTING READY FOR TOTAL HIP REPLACEMENT Pre-Op Exercises for a Better Recovery Your Recovery Begins Now Even if your hip replacement surgery is weeks or months away, start getting ready now. People who
GETTING READY FOR TOTAL HIP REPLACEMENT Pre-Op Exercises for a Better Recovery Your Recovery Begins Now Even if your hip replacement surgery is weeks or months away, start getting ready now. People who
Posture. In this article
 Posture Posture is the way we hold our bodies against gravity and maintaining a good posture involves training yourself to become aware of how you hold yourself in all activities as your posture is constantly
Posture Posture is the way we hold our bodies against gravity and maintaining a good posture involves training yourself to become aware of how you hold yourself in all activities as your posture is constantly
Tips and Tricks. For Living Well with Parkinson s Disease
 Tips and Tricks For Living Well with Parkinson s Disease Amanda Avila MD Medical Director Hope Parkinson s Program Staff Neurologist Florida Neurology Group Motor Symptoms Bradykinesia Generalized slowness
Tips and Tricks For Living Well with Parkinson s Disease Amanda Avila MD Medical Director Hope Parkinson s Program Staff Neurologist Florida Neurology Group Motor Symptoms Bradykinesia Generalized slowness
A Patient s Guide to Artificial Hip Dislocation Precautions
 A Patient s Guide to Artificial Hip Dislocation Precautions Introduction Hip surgeries such as total joint replacement and hemiarthroplasty require the surgeon to open the hip joint capsule. This puts
A Patient s Guide to Artificial Hip Dislocation Precautions Introduction Hip surgeries such as total joint replacement and hemiarthroplasty require the surgeon to open the hip joint capsule. This puts
Your Guide to Independent Living
 Your Guide to Independent Living What you can do to reduce your risk for falls These are things you can do to stay strong and reduce your risk for falls. Begin a regular exercise program Do exercises that
Your Guide to Independent Living What you can do to reduce your risk for falls These are things you can do to stay strong and reduce your risk for falls. Begin a regular exercise program Do exercises that
Ups &Downs of Falling
 Falls Clinics within SHSCT If you have had a fall in the past or are concerned that you may in the future there is a Falls Clinic in your area that can provide assessment and treatment to reduce your risk
Falls Clinics within SHSCT If you have had a fall in the past or are concerned that you may in the future there is a Falls Clinic in your area that can provide assessment and treatment to reduce your risk
LOW BACK PAIN. what you can do
 LOW BACK PAIN what you can do Back pain Nearly 80 percent of adults will experience back pain at some point in their life. The good news is that back pain will normally go away within four to six weeks
LOW BACK PAIN what you can do Back pain Nearly 80 percent of adults will experience back pain at some point in their life. The good news is that back pain will normally go away within four to six weeks
Agenda and Objectives
 Agenda and Objectives Session 2 Handout: Activity Session One 1. Welcome & outline review today s agenda 2. Benefits of and barriers to regular exercise 3. Review of exercise homework and planning ahead
Agenda and Objectives Session 2 Handout: Activity Session One 1. Welcome & outline review today s agenda 2. Benefits of and barriers to regular exercise 3. Review of exercise homework and planning ahead
Workout to Go. A Sample Exercise Routine from the National Institute on Aging at NIH
 Workout to Go A Sample Exercise Routine from the National Institute on Aging at NIH i Workout to Go Are you just starting to exercise? Getting back into a routine after a break? Wanting to keep up your
Workout to Go A Sample Exercise Routine from the National Institute on Aging at NIH i Workout to Go Are you just starting to exercise? Getting back into a routine after a break? Wanting to keep up your
Post Lung Transplant Exercises
 Post Lung Transplant Exercises Post Lung Transplant Physical activity improves our strength and stamina, maintains optimal functioning of our major organs and increases our vitality, energy and overall
Post Lung Transplant Exercises Post Lung Transplant Physical activity improves our strength and stamina, maintains optimal functioning of our major organs and increases our vitality, energy and overall
DRAFT. Activities of Daily Living After Lung Surgery Self-care for safety and healing. Clamshell Precautions
 UW MEDICINE PATIENT EDUCATION Activities of Daily Living After Lung Surgery Self-care for safety and healing This handout gives important guidelines to follow to help your healing and keep you safe after
UW MEDICINE PATIENT EDUCATION Activities of Daily Living After Lung Surgery Self-care for safety and healing This handout gives important guidelines to follow to help your healing and keep you safe after
Body Mechanics When caring for a client
 Body Mechanics When caring for a client If assistance is needed, find out the client's strengths and weaknesses. Often one side of the body is stronger. The stronger side should be transferred first. When
Body Mechanics When caring for a client If assistance is needed, find out the client's strengths and weaknesses. Often one side of the body is stronger. The stronger side should be transferred first. When
The In Bed Workout or the Getting Up Routine
 The In Bed Workout or the Getting Up Routine This is a great way to wake up and make good use of time. Just think, instead of lying there wasting 10 minutes thinking about getting up, you can complete
The In Bed Workout or the Getting Up Routine This is a great way to wake up and make good use of time. Just think, instead of lying there wasting 10 minutes thinking about getting up, you can complete
Total Knee Replacement: Your Guide to Preparation and Recovery
 Total Knee Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 5 After Surgery.............................
Total Knee Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 5 After Surgery.............................
Strength and Balance Exercise Manual. Building Confidence and Reducing Falls in Older Adults. Lindy Clemson Megan Swann Jane Mahoney
 Building Confidence and Reducing Falls in Older Adults Strength and Balance Exercise Manual Lindy Clemson Megan Swann Jane Mahoney 3rd North American edition Exercises BALANCE AND STRENGTH EXERCISES TO
Building Confidence and Reducing Falls in Older Adults Strength and Balance Exercise Manual Lindy Clemson Megan Swann Jane Mahoney 3rd North American edition Exercises BALANCE AND STRENGTH EXERCISES TO
Your Guide to Independent Living
 Keeping you safe from falls and injuries Developed by Fraser Health Seniors Falls and Injury Prevention fallsprevention@fraserhealth.ca Print Shop # 264151 (November 2013) Table of Contents Are you at
Keeping you safe from falls and injuries Developed by Fraser Health Seniors Falls and Injury Prevention fallsprevention@fraserhealth.ca Print Shop # 264151 (November 2013) Table of Contents Are you at
Helpful Tips for the Unsteady Patient. Mairead Collins Senior Physiotherapist Bon Secours Hospital 20/09/14
 Helpful Tips for the Unsteady Patient Mairead Collins Senior Physiotherapist Bon Secours Hospital 20/09/14 AIMS Brief discussion of Causes & Implications of Unsteady Gait/Imbalance Falls & Falls Prevention
Helpful Tips for the Unsteady Patient Mairead Collins Senior Physiotherapist Bon Secours Hospital 20/09/14 AIMS Brief discussion of Causes & Implications of Unsteady Gait/Imbalance Falls & Falls Prevention
How to Save Your Energy
 How to Save Your Energy Sometimes people have trouble doing the things they want to do because they are too tired or have shortness of breath (SOB). Being over tired and/or having SOB can be caused by
How to Save Your Energy Sometimes people have trouble doing the things they want to do because they are too tired or have shortness of breath (SOB). Being over tired and/or having SOB can be caused by
Working together to prevent falls
 Quality Care - for you, with you Working together to prevent falls Introduction Falling is a common problem throughout our lifetime but as we get older the risk of injury from falls unfortunately gets
Quality Care - for you, with you Working together to prevent falls Introduction Falling is a common problem throughout our lifetime but as we get older the risk of injury from falls unfortunately gets
EXERCISES, TIPS AND STRATEGIES for Self-Improvement
 EXERCISES, TIPS AND STRATEGIES for Self-Improvement 03 :: INTRODUCTION 07 :: 1. MOVING AWAY FROM THE DIAGNOSIS OF I M CRAZY : THE STRENGTHS-BASED APPROACH 12 :: 2. CONNECTING TO OTHERS AND MANAGING YOUR
EXERCISES, TIPS AND STRATEGIES for Self-Improvement 03 :: INTRODUCTION 07 :: 1. MOVING AWAY FROM THE DIAGNOSIS OF I M CRAZY : THE STRENGTHS-BASED APPROACH 12 :: 2. CONNECTING TO OTHERS AND MANAGING YOUR
Occupational Therapy. Energy conservation and work simplification techniques
 Occupational Therapy Energy conservation and work simplification techniques Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified
Occupational Therapy Energy conservation and work simplification techniques Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified
Occupational Therapy: INTERVENTION AND INDEPENDENCE
 Occupational Therapy: INTERVENTION AND INDEPENDENCE What is Occupational Therapy? A therapy to help people find ways to do things that matter to them Dressing, bathing, toileting Housekeeping Leisure Community
Occupational Therapy: INTERVENTION AND INDEPENDENCE What is Occupational Therapy? A therapy to help people find ways to do things that matter to them Dressing, bathing, toileting Housekeeping Leisure Community
Falls Awareness & Prevention Guide
 Falls Awareness & Prevention Guide Prepare your home or assist a loved one today by following these fall-proofing recommendations, courtesy of the American Academy of Orthopaedic Surgeons. Falls Awareness
Falls Awareness & Prevention Guide Prepare your home or assist a loved one today by following these fall-proofing recommendations, courtesy of the American Academy of Orthopaedic Surgeons. Falls Awareness
Move More Wakefield District. Active at home programme
 Move More Wakefield District Active at home programme The active at home programme has been developed to increase your activity levels in the comfort of your own home, and in turn improving your balance
Move More Wakefield District Active at home programme The active at home programme has been developed to increase your activity levels in the comfort of your own home, and in turn improving your balance
Osteoporosis Exercise:
 Osteoporosis Exercise: Balance, Posture and Functional Exercises Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction You can help improve and maintain your balance, posture
Osteoporosis Exercise: Balance, Posture and Functional Exercises Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction You can help improve and maintain your balance, posture
Chapter 9: Exercise Instructions
 RESOURCES RESEARCHERS / MEDICAL HOW TO HELP SPONSORS GEHRIG CONNECTION MEDIA TELETHON MDA.ORG search our site Go MDA/ALS Newsmagazine Current Issue Home> Publications >Everyday Life With ALS: A Practical
RESOURCES RESEARCHERS / MEDICAL HOW TO HELP SPONSORS GEHRIG CONNECTION MEDIA TELETHON MDA.ORG search our site Go MDA/ALS Newsmagazine Current Issue Home> Publications >Everyday Life With ALS: A Practical
Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
OHIOHEALTH ORTHOPEDIC SURGEONS Dr. Nathaniel Long Sarah A. Domenicucci, PA-C POST OPERATIVE INSTRUCTIONS
 OHIOHEALTH ORTHOPEDIC SURGEONS Dr. Nathaniel Long 614-566-8691 Sarah A. Domenicucci, PA-C POST OPERATIVE INSTRUCTIONS Shoulder Arthroscopy with Labral Repair (SLAP/Bankart/Posterior) Latarjet Procedure
OHIOHEALTH ORTHOPEDIC SURGEONS Dr. Nathaniel Long 614-566-8691 Sarah A. Domenicucci, PA-C POST OPERATIVE INSTRUCTIONS Shoulder Arthroscopy with Labral Repair (SLAP/Bankart/Posterior) Latarjet Procedure
Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
postpartum fitness GETTING BACK IN SHAPE AFTER YOUR PREGNANCY
 postpartum fitness GETTING BACK IN SHAPE AFTER YOUR PREGNANCY While pregnancy and birth can be joyful, they also can be hard on your body. To regain the level of fitness you had before you became pregnant,
postpartum fitness GETTING BACK IN SHAPE AFTER YOUR PREGNANCY While pregnancy and birth can be joyful, they also can be hard on your body. To regain the level of fitness you had before you became pregnant,
Issues for Patient Discussion
 onmotor complications radykinesia Screening Tools asked PD micrographia eurodegeneration Designed for Use by Family Practitioners remor on-off opamine agonists tiffness depression ostural instability wearing
onmotor complications radykinesia Screening Tools asked PD micrographia eurodegeneration Designed for Use by Family Practitioners remor on-off opamine agonists tiffness depression ostural instability wearing
VON SMART. (Seniors Maintaining Active Role Together) In-Home Program. Exercise Instructions
 VON SMART (Seniors Maintaining Active Role Together) In-Home Program Exercise Instructions This VON SMART Exercise Instruction Packet is designed to guide you through the 15 VON SMART In- Home Exercises.
VON SMART (Seniors Maintaining Active Role Together) In-Home Program Exercise Instructions This VON SMART Exercise Instruction Packet is designed to guide you through the 15 VON SMART In- Home Exercises.
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
AgePage Preventing Falls and Fractures
 National Institute on Aging AgePage Preventing Falls and Fractures A simple fall can change your life. Just ask any of the thousands of older men and women who fall each year and break (sometimes called
National Institute on Aging AgePage Preventing Falls and Fractures A simple fall can change your life. Just ask any of the thousands of older men and women who fall each year and break (sometimes called
Practical Advice for Caring Safely: The ergonomics of providing care for a frail older adult
 Practical Advice for Caring Safely: The ergonomics of providing care for a frail older adult Emily King, MASc PhD Candidate at Toronto Rehab & U Toronto My background & interests Bachelor s: Mechanical
Practical Advice for Caring Safely: The ergonomics of providing care for a frail older adult Emily King, MASc PhD Candidate at Toronto Rehab & U Toronto My background & interests Bachelor s: Mechanical
8 Week Program: Intermediate
 8 Week Program: Intermediate Introduction The Program This program has been developed by an Exercise Physiologist to provide individuals at all fitness levels with a comprehensive exercise program that
8 Week Program: Intermediate Introduction The Program This program has been developed by an Exercise Physiologist to provide individuals at all fitness levels with a comprehensive exercise program that
QUAD NECK PUSH-UPS STRETCH STRETCH ROLLS HAMSTRING
 QUAD NECK STRETCH Start in a normal standing position. Bend one knee and raise the foot towards the buttock. Slightly flex the standing leg so the knees are together (but not touching). Hold the front
QUAD NECK STRETCH Start in a normal standing position. Bend one knee and raise the foot towards the buttock. Slightly flex the standing leg so the knees are together (but not touching). Hold the front
Total Hip Replacement: Your Guide to Preparation and Recovery
 Total Hip Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 6 After Surgery.............................
Total Hip Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 6 After Surgery.............................
Tobacco Cessation Toolkit
 You notice physical s, like moments of dizziness, sweating, hands trembling or a mild headache. When using tobacco, nicotine increases your heart rate (by about 10 20 beats per minute) and blood pressure.
You notice physical s, like moments of dizziness, sweating, hands trembling or a mild headache. When using tobacco, nicotine increases your heart rate (by about 10 20 beats per minute) and blood pressure.
Co-morbidities and Exercise with Parkinson s Disease (COPE) Exercise Manual
 Name: Date: Co-morbidities and Exercise with Parkinson s Disease (COPE) Exercise Manual This program is organized into 6 themed stations done like a circuit to address the specific difficulties that a
Name: Date: Co-morbidities and Exercise with Parkinson s Disease (COPE) Exercise Manual This program is organized into 6 themed stations done like a circuit to address the specific difficulties that a
Understanding Parkinson s Disease Important information for you and your loved ones
 Patient Education Understanding Parkinson s Disease Important information for you and your loved ones This handout explains the signs, symptoms, and possible treatments of Parkinson s disease. Parkinson
Patient Education Understanding Parkinson s Disease Important information for you and your loved ones This handout explains the signs, symptoms, and possible treatments of Parkinson s disease. Parkinson
Body Mechanics Training For Shelter Staff 2014
 Body Mechanics Training For Shelter Staff 2014 Valerie Risher, RN, BSN FDOH Region 5 Special Needs Consultant Terry B. Freeman, RN Disaster Health Services Advisor, Florida American Red Cross Robert Kosiba,
Body Mechanics Training For Shelter Staff 2014 Valerie Risher, RN, BSN FDOH Region 5 Special Needs Consultant Terry B. Freeman, RN Disaster Health Services Advisor, Florida American Red Cross Robert Kosiba,
The symptoms of the Parkinson s disease may vary from person to person. The symptoms might include the following:
 1 PARKINSON S DISEASE Parkinson's disease is a long term disease related to the central nervous system that mainly affects the motor system, resulting in the loss of dopamine, which helps in producing
1 PARKINSON S DISEASE Parkinson's disease is a long term disease related to the central nervous system that mainly affects the motor system, resulting in the loss of dopamine, which helps in producing
Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises. Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises
 Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction Weight-bearing and resistance exercises have
Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction Weight-bearing and resistance exercises have
Day 1 Day 2 Day 3 Day 4 Day 5 Day 6 Day 7 Workout 1 Workout 2 Workout 1 Workout 2 Rest Workout 1 Rest
 60 Day Workout Plan 1 Workout Schedule Day 1 Day 2 Day 3 Day 4 Day 5 Day 6 Day 7 Workout 1 Workout 2 Workout 1 Workout 2 Rest Workout 1 Rest Summary of workouts Workout 1 Workout 2 1. Cardiovascular-Walking/Jogging
60 Day Workout Plan 1 Workout Schedule Day 1 Day 2 Day 3 Day 4 Day 5 Day 6 Day 7 Workout 1 Workout 2 Workout 1 Workout 2 Rest Workout 1 Rest Summary of workouts Workout 1 Workout 2 1. Cardiovascular-Walking/Jogging
Terms and Conditions
 Terms and Conditions LEGAL NOTICE The Publisher has strived to be as accurate and complete as possible in the creation of this report, notwithstanding the fact that he does not warrant or represent at
Terms and Conditions LEGAL NOTICE The Publisher has strived to be as accurate and complete as possible in the creation of this report, notwithstanding the fact that he does not warrant or represent at
How to Create. a Safer Home. A room-by-room guide to eliminate
 How to Create a Safer Home A room-by-room guide to eliminate the most common causes of falls Clear away clutter Philips Lifeline Falls Prevention Tip Book It s not possible to prevent every fall. But a
How to Create a Safer Home A room-by-room guide to eliminate the most common causes of falls Clear away clutter Philips Lifeline Falls Prevention Tip Book It s not possible to prevent every fall. But a
Week Five Session 1. Improve balance in general Improve balance while performing daily activities
 Week Five Session 1 Session 5.1: Standing Balance Purpose Objectives Improve balance in general Improve balance while performing daily activities By the end of the session, elders will: Materials 1. Review
Week Five Session 1 Session 5.1: Standing Balance Purpose Objectives Improve balance in general Improve balance while performing daily activities By the end of the session, elders will: Materials 1. Review
Miami J Collar. General Guidelines. How to Put On Your. Miami J Collar. Safe Exercises to Do While in The Collar.
 Miami J Collar General Guidelines How to Put On Your Miami J Collar Safe Exercises to Do While in The Collar www.neurosurgery.med.miami.edu General Guidelines Wear the Miami J Collar at all times. Do not
Miami J Collar General Guidelines How to Put On Your Miami J Collar Safe Exercises to Do While in The Collar www.neurosurgery.med.miami.edu General Guidelines Wear the Miami J Collar at all times. Do not
Walking Program Sequence
 Walking Program Sequence 1. Warm up - Warming up is exercising at a lower intensity in order to get the blood circulating and let your body know that you are preparing for exercise. For many of your walks
Walking Program Sequence 1. Warm up - Warming up is exercising at a lower intensity in order to get the blood circulating and let your body know that you are preparing for exercise. For many of your walks
Commonwealth Health Corporation NEXT
 Commonwealth Health Corporation This computer-based learning (CBL) module details important aspects of musculoskeletal disorders, body mechanics and ergonomics in the workplace. It examines: what causes
Commonwealth Health Corporation This computer-based learning (CBL) module details important aspects of musculoskeletal disorders, body mechanics and ergonomics in the workplace. It examines: what causes
Back Safety Healthcare #09-066
 Back Safety Healthcare Version #09-066 I. Introduction A. Scope of training This training program applies to healthcare employees whose job requires them to lift patients or other heavy objects. Lifting
Back Safety Healthcare Version #09-066 I. Introduction A. Scope of training This training program applies to healthcare employees whose job requires them to lift patients or other heavy objects. Lifting
A word about incontinence
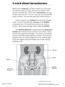 A word about incontinence When you re continent, you have control over your urine. You feel the need to urinate, and you can hold it until you get to a bathroom. When you re incontinent, you may urinate
A word about incontinence When you re continent, you have control over your urine. You feel the need to urinate, and you can hold it until you get to a bathroom. When you re incontinent, you may urinate
Session 16: Manage Your Stress
 Session 16: Manage Your Stress Stress is part of life. However, you can learn better ways to take care of yourself when faced with stress. Stress is not always bad. Some stress can make life interesting
Session 16: Manage Your Stress Stress is part of life. However, you can learn better ways to take care of yourself when faced with stress. Stress is not always bad. Some stress can make life interesting
Active Living with Arthritis Podcast #9 Being a Caregiver: Caring for Someone and Managing Your Arthritis
 Active Living with Arthritis Podcast #9 Being a Caregiver: Caring for Someone and Managing Your Arthritis Karen: Welcome to another Active Living with Arthritis podcast, presented by ENACT center at Boston
Active Living with Arthritis Podcast #9 Being a Caregiver: Caring for Someone and Managing Your Arthritis Karen: Welcome to another Active Living with Arthritis podcast, presented by ENACT center at Boston
BODY MECHANICS CMHA-CEI
 BODY MECHANICS CMHA-CEI Basics about backs Facts about Back Disorders Maintaining a Healthy Back Common activities Lifting Techniques Stretching Techniques Topics Your back Spine & Vertebrae Discs Nerves
BODY MECHANICS CMHA-CEI Basics about backs Facts about Back Disorders Maintaining a Healthy Back Common activities Lifting Techniques Stretching Techniques Topics Your back Spine & Vertebrae Discs Nerves
the back book Your Guide to a Healthy Back
 the back book Your Guide to a Healthy Back anatomy Your spine s job is to: Support your upper body and neck Increase flexibility of your spine Protect your spinal cord There are 6 primary components of
the back book Your Guide to a Healthy Back anatomy Your spine s job is to: Support your upper body and neck Increase flexibility of your spine Protect your spinal cord There are 6 primary components of
AFTER TOTAL HIP REPLACEMENT
 AFTER TOTAL HIP REPLACEMENT Living in Comfort with Your New Hip Getting Back in Step By having a total hip replacement, you re taking the first step toward returning to an active lifestyle. The next step
AFTER TOTAL HIP REPLACEMENT Living in Comfort with Your New Hip Getting Back in Step By having a total hip replacement, you re taking the first step toward returning to an active lifestyle. The next step
Strong and Stable: Exercises for Core, Strength and Balance
 Strong and Stable: Exercises for Core, Strength and Balance Exercise and physical activity before, during and after cancer treatment are important to recovery and general quality of life. Studies show
Strong and Stable: Exercises for Core, Strength and Balance Exercise and physical activity before, during and after cancer treatment are important to recovery and general quality of life. Studies show
I want to improve balance
 I want to improve balance Do these exercises several times throughout the day, increasing the time on each exercise as your balance and flexibility increase. If you are unsure about doing any of these
I want to improve balance Do these exercises several times throughout the day, increasing the time on each exercise as your balance and flexibility increase. If you are unsure about doing any of these
Osteoporosis Exercise:
 Osteoporosis Exercise: Posture, Body Mechanics, Alignment and Moving Safely Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction Using correct posture, proper body mechanics
Osteoporosis Exercise: Posture, Body Mechanics, Alignment and Moving Safely Osteoporosis Exercise: Weight-Bearing and Muscle Strengthening Exercises Introduction Using correct posture, proper body mechanics
return to sports after injury IMPROVING STRENGTH, POWER, AND AGILITY
 return to sports after injury IMPROVING STRENGTH, POWER, AND AGILITY This booklet is designed for people recovering from a knee or leg injury who participate in recreational or competitive sports such
return to sports after injury IMPROVING STRENGTH, POWER, AND AGILITY This booklet is designed for people recovering from a knee or leg injury who participate in recreational or competitive sports such
Exercise 1: Reverse Abdominals
 Exercise Guide Before starting this or any exercise program, please make sure to talk to your family Doctor. The information in this book works and has given thousands of people impressive results and
Exercise Guide Before starting this or any exercise program, please make sure to talk to your family Doctor. The information in this book works and has given thousands of people impressive results and
risk factors for falling
 Resource # 10 Page 1 of 8 1. Dizziness- What Can Cause Dizziness? Not eating regularly Change in body position (e.g. from sitting to standing) Low blood pressure High blood pressure Medication side effects
Resource # 10 Page 1 of 8 1. Dizziness- What Can Cause Dizziness? Not eating regularly Change in body position (e.g. from sitting to standing) Low blood pressure High blood pressure Medication side effects
SAVE YOUR BACK! How to Safely Use a Back Support Brace, Assisting with Body Positioning, Transfers, ADLs, Adapting the Home, Ambulation and Falling.
 SAVE YOUR BACK! How to Safely Use a Back Support Brace, Assisting with Body Positioning, Transfers, ADLs, Adapting the Home, Ambulation and Falling. 5/15/2017 Table of Contents How to Use a Back Support
SAVE YOUR BACK! How to Safely Use a Back Support Brace, Assisting with Body Positioning, Transfers, ADLs, Adapting the Home, Ambulation and Falling. 5/15/2017 Table of Contents How to Use a Back Support
Patient & Family Guide
 Patient & Family Guide 2017 Liver Transplant Physiotherapy Program Aussi disponible en français : Programme de physiothérapie avant une transplantation du foie (FF85-1839) www.nshealth.ca Contents Why
Patient & Family Guide 2017 Liver Transplant Physiotherapy Program Aussi disponible en français : Programme de physiothérapie avant une transplantation du foie (FF85-1839) www.nshealth.ca Contents Why
Modified Parkinson Activity Scale
 Modified Parkinson Activity Scale Chair transfers Analyses: Instruction: Chair with 40 cm seat height, or, when at the patient's home, the chair that causes the greatest problems to the patient and is
Modified Parkinson Activity Scale Chair transfers Analyses: Instruction: Chair with 40 cm seat height, or, when at the patient's home, the chair that causes the greatest problems to the patient and is
This Progressive Relaxation Procedure is yours to use and to distribute as you see fit.
 This Progressive Relaxation Procedure is yours to use and to distribute as you see fit. Jacobson s Progressive Relaxation Procedure Progressive Muscle Relaxation (PMR) Edmund Jacobson created the progressive
This Progressive Relaxation Procedure is yours to use and to distribute as you see fit. Jacobson s Progressive Relaxation Procedure Progressive Muscle Relaxation (PMR) Edmund Jacobson created the progressive
FOR THE SERVICE MEMBER: Rx3 REHABILITATION PROGRAM
 CREATED BY THE HUMAN PERFORMANCE RESOURCE CENTER / HPRC-ONLINE.ORG / FROM THE CONSORTIUM FOR HEALTH AND MILITARY PERFORMANCE HUMAN PERFORMANCE RESOURCE CENTER Injury/Condition: Injury/Condition: What is
CREATED BY THE HUMAN PERFORMANCE RESOURCE CENTER / HPRC-ONLINE.ORG / FROM THE CONSORTIUM FOR HEALTH AND MILITARY PERFORMANCE HUMAN PERFORMANCE RESOURCE CENTER Injury/Condition: Injury/Condition: What is
Advice: After the Removal of a Lower Leg Cast
 Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
Physical and Occupational Therapy after Spine Surgery. Preparation for your surgery
 Physical and Occupational Therapy after Spine Surgery Preparation for your surgery Agenda Pre-Operative Exercises What to Expect Post-Operative Plan Spinal Precautions Post-Discharge Plan S A I N T LU
Physical and Occupational Therapy after Spine Surgery Preparation for your surgery Agenda Pre-Operative Exercises What to Expect Post-Operative Plan Spinal Precautions Post-Discharge Plan S A I N T LU
Rehabilitation Program Following Shoulder Diagnostic Arthroscopy, Acromioplasty, Decompression, AC Resection, Debridement
 Rehabilitation Program Following Shoulder Diagnostic Arthroscopy, Acromioplasty, Decompression, AC Resection, Debridement Richard Holtby Assistant professor, Department of Surgery University of Toronto
Rehabilitation Program Following Shoulder Diagnostic Arthroscopy, Acromioplasty, Decompression, AC Resection, Debridement Richard Holtby Assistant professor, Department of Surgery University of Toronto
Sculpt Sexy GLUTES & ABS
 Sculpt Sexy GLUTES & ABS 10 Bodyweight Strength & Conditioning Moves for Your Stomach and Glutes by Bree Argetsinger aka The Betty Rocker www.thebettyrocker.com Page 1 Welcome Try this fun little glutes
Sculpt Sexy GLUTES & ABS 10 Bodyweight Strength & Conditioning Moves for Your Stomach and Glutes by Bree Argetsinger aka The Betty Rocker www.thebettyrocker.com Page 1 Welcome Try this fun little glutes
Keeping Home Safe WHAT CAN YOU DO?
 Keeping Home Safe or dementia may have trouble knowing what is dangerous or making safe decisions. By helping him or her feel more relaxed and less confused at home, you can help stop accidents. trip because
Keeping Home Safe or dementia may have trouble knowing what is dangerous or making safe decisions. By helping him or her feel more relaxed and less confused at home, you can help stop accidents. trip because
HEALTH FOCUS: MENTAL HEALTH
 HEALTH FOCUS: MENTAL HEALTH CONTENTS Introduction 1 Self-assessment quiz 2 Five steps to better mental 3 well-being Stress reduction exercises 4 Further support 5 INTRODUCTION There are two aspects to
HEALTH FOCUS: MENTAL HEALTH CONTENTS Introduction 1 Self-assessment quiz 2 Five steps to better mental 3 well-being Stress reduction exercises 4 Further support 5 INTRODUCTION There are two aspects to
Exercise, Physical Therapy and Fall Prevention
 Exercise, Physical Therapy and Fall Prevention University of Davis Medical Center Rosy Chow Neuro Clinical Specialist Physical Therapist Outline of Talk Role of Physical Therapy in care of people with
Exercise, Physical Therapy and Fall Prevention University of Davis Medical Center Rosy Chow Neuro Clinical Specialist Physical Therapist Outline of Talk Role of Physical Therapy in care of people with
Mindful yoga for stress movement practice
 Mindful yoga for stress movement practice The following sequence is more or less what we practised in the workshop. You can do it all if you have time, or if you just have a few minutes do one or two poses
Mindful yoga for stress movement practice The following sequence is more or less what we practised in the workshop. You can do it all if you have time, or if you just have a few minutes do one or two poses
A Guide to Fall Prevention
 A Guide to Fall Prevention Did you know? Falls can be a common problem for older people and are often result in people being admitted to hospital or move to a nursing home or hostel. As our bodies age
A Guide to Fall Prevention Did you know? Falls can be a common problem for older people and are often result in people being admitted to hospital or move to a nursing home or hostel. As our bodies age
Below Knee Amputation: Positioning and Exercise Program
 Below Knee Amputation: Positioning and Exercise Program The exercises and stretches in this handout will help to prepare you to wear a prosthesis properly. The positioning instructions and exercises in
Below Knee Amputation: Positioning and Exercise Program The exercises and stretches in this handout will help to prepare you to wear a prosthesis properly. The positioning instructions and exercises in
Regular physical activity is the best tool to improve health and wellbeing. The SAIL Home Activity Program has 3 levels: Reasons to Move Your Body
 Regular physical activity is the best tool to improve health and wellbeing. The SAIL Home Activity Program has 3 levels: level 1: Sitting level 2: Standing level 3: Moving Your health care provider has
Regular physical activity is the best tool to improve health and wellbeing. The SAIL Home Activity Program has 3 levels: level 1: Sitting level 2: Standing level 3: Moving Your health care provider has
20944_Exercise Diary:20944_Exercise Diary 7/10/09 09:46 Page 1 Exercise Diary
 Exercise Diary Name: Hospital number: Contact number for renal unit: Contents Page Introduction 4 Your clothing and trainers 5 Diet and fluid management 6 Starting your exercise programme 6 Tips for succeeding
Exercise Diary Name: Hospital number: Contact number for renal unit: Contents Page Introduction 4 Your clothing and trainers 5 Diet and fluid management 6 Starting your exercise programme 6 Tips for succeeding
AFTER KNEE REPLACEMENT
 AFTER KNEE REPLACEMENT Living in Comfort with Your New Knee Stepping into Recovery Before knee replacement surgery, your painful knee may have limited your activity. Replacing your knee joint was your
AFTER KNEE REPLACEMENT Living in Comfort with Your New Knee Stepping into Recovery Before knee replacement surgery, your painful knee may have limited your activity. Replacing your knee joint was your
Advice and exercises for managing knee and hip osteoarthritis October 2018 V1.2 April 2018 April 2021
 Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Advice and exercises for managing knee and hip osteoarthritis 0496 October 2018 V1.2 April 2018 April 2021 This advice and exercise booklet has been produced by senior physiotherapists working for DynamicHealth.
Yoga to Aid Sound Sleep.
 Yoga to Aid Sound Sleep. Relaxation in itself is not enough to counteract the effects of the stress and tension, which can lead to disturbed sleep. In order to sleep well, we need to eliminate stress and
Yoga to Aid Sound Sleep. Relaxation in itself is not enough to counteract the effects of the stress and tension, which can lead to disturbed sleep. In order to sleep well, we need to eliminate stress and
Lesson Sixteen Flexibility and Muscular Strength
 Lesson Sixteen Flexibility and Muscular Strength Objectives After participating in this lesson students will: Be familiar with why we stretch. Develop a stretching routine to do as a pre-activity before
Lesson Sixteen Flexibility and Muscular Strength Objectives After participating in this lesson students will: Be familiar with why we stretch. Develop a stretching routine to do as a pre-activity before
3. Poor Concentration - Children may appear less coordinated and have more accidents than their peers.
 Hypermobile Joints Information Sheet Children with hypermobility joints have too much movement in the joints. This can occur with just a couple of joints or all joints. A joint is the place on the body
Hypermobile Joints Information Sheet Children with hypermobility joints have too much movement in the joints. This can occur with just a couple of joints or all joints. A joint is the place on the body
This Manual is copyright under the Berne Convention. In terms of the Copyright Act 98 of 1978 no part of this leaflet may be reproduced or
 Basic Ball Exercise Manual Train your Core This Manual is copyright under the Berne Convention. In terms of the Copyright Act 98 of 1978 no part of this leaflet may be reproduced or transmitted in any
Basic Ball Exercise Manual Train your Core This Manual is copyright under the Berne Convention. In terms of the Copyright Act 98 of 1978 no part of this leaflet may be reproduced or transmitted in any
Session 3 or 6: Being Active: A Way of Life.
 Session 3 or 6: Being Active: A Way of Life. You can find the time to be active. Set aside one block of time every day to be active. When can you set aside 20 to 30 minutes to do an activity you like?
Session 3 or 6: Being Active: A Way of Life. You can find the time to be active. Set aside one block of time every day to be active. When can you set aside 20 to 30 minutes to do an activity you like?
FEEL GOOD GLOW Low intensity workout
 Welcome to the low intensity workout, Feel good glow. If this is your first time doing one of our workouts, we recommend you check out the introductory video at www.healthier.qld.gov.au to get more information
Welcome to the low intensity workout, Feel good glow. If this is your first time doing one of our workouts, we recommend you check out the introductory video at www.healthier.qld.gov.au to get more information
Back Protection. Training Guide
 Back Protection Training Guide Use a Back Support Belt to Prevent Back Injuries Because of the incidious progression of back problems, it is always difficult to determine how a back problem began. If you
Back Protection Training Guide Use a Back Support Belt to Prevent Back Injuries Because of the incidious progression of back problems, it is always difficult to determine how a back problem began. If you
Action TAKE. Prevent a fall. before it happens
 TAKE Action Prevent a fall before it happens 1 Who THIS BOOK IS FOR...adults of all ages. Slips, trips and falls happen to anyone. Many people think, it won t happen to me. They believe falls are not important
TAKE Action Prevent a fall before it happens 1 Who THIS BOOK IS FOR...adults of all ages. Slips, trips and falls happen to anyone. Many people think, it won t happen to me. They believe falls are not important
50 Things You Can Do To Save Your Back
 50 Things You Can Do To Save Your Back 1. Maintain your ideal weight. 2. Think before you lift. Plan your moves before you pick up the object. 3. Move your car seat as close to the steering wheel as is
50 Things You Can Do To Save Your Back 1. Maintain your ideal weight. 2. Think before you lift. Plan your moves before you pick up the object. 3. Move your car seat as close to the steering wheel as is
Stretch Packet. Stretch Packet
 Stretch Packet Stretch Packet Stretching is a form of physical exercise in which a specific muscle or tendon is deliberately flexed or stretched in order to improve the muscle's felt elasticity and achieve
Stretch Packet Stretch Packet Stretching is a form of physical exercise in which a specific muscle or tendon is deliberately flexed or stretched in order to improve the muscle's felt elasticity and achieve
