Enhancing the Palliative and End of Life Care. One chance to get it right.
|
|
|
- Deirdre Williams
- 5 years ago
- Views:
Transcription
1 Enhancing the Palliative and End of Life Care Experience One chance to get it right.
2 The Palliative and End of Life Care Experience Why are we getting it wrong? Why is it important we get it right? What can I do to enhance the patient s / family experience? What strategies help? What resources are out there?
3 Finding your 1%
4 End of Life Care People are approaching the end of life when they are likely to die within the next 12 months. (GMC 2010) 1% of the population die each year
5
6 6
7 Helpful Tools SurpriseQuestion Would you be surprisedif the patient were to die in the next 6-12months?
8 General Indicators of Decline Look for 2 of the following; Poor performance status (needs help with personal care, in bed >50% or more of the day) 2 unplanned admissions Weight loss 5-10% or BMI <20 Persistent troublesome symptoms New event or diagnosis Nursing care resident or needs care at home
9 Specific Indicators of Decline
10 Cancer Single most important factor is functional ability >50% of time in lying down= approx 3 months or less 10
11 Benefits to Prediction Patient Patient s support Practice Secondary care CCGs
12 GSF Register Electronic Palliative Care Co-ordination System (EPaCCS) Optimal care Initiates ACP discussions Autonomy Increase QoL
13 Audit in Practice What % of dying patients are on your register? What % are non-cancer patients? What % die at home?
14 Let s Start the Conversation
15 EoLC Conversations - Why initiate? Ensures the patient feels heard and understood Achieves an understanding of the patient s concerns and needs Enables a trusting relationship Reduces uncertainty Prevents unrealistic expectations Maintains realistic hope Provides appropriate information and choices Maguire 2008
16 Effective EoLC Conversations Helps plan for the future Improves compliance Clarifies priorities Resolves ethical dilemmas Achieves informed consent Promotes effective MDT working Maguire 2008
17 Failure to start the conversation and find patient or family s perspective can lead to Failure to assess people s concerns Failure to identify and treat psychological morbidity Failure to tailor information and help psychological adjustment Lack of participation in decision-making Unnecessary distress and poor end of life care particularly over the last few days of life Increased risk of complaints and litigation
18 Why identify concerns? > 50% of cancer patients develop an affective disorder requiring intervention Burgess et al 2005, BMJ Patients were more involved when concerns taken seriously and acted upon de Silva D (2013)
19 Why Tailor information? Participants value the ability of an oncologist to recognize the gravity of the news of cancer recurrence for an individual patient and make a connection at the human -tohuman level Back, A L (2011) Patients who feel they are given inadequate information (too little or too much) at time of diagnosis are at greater risk of affective disorders (anxiety, depression) Fallowfield et al 1990, BMJ Patients who had all their questions answered reported cancer had less impact on their lives Schofield et al 2003, Annals of Oncology
20 Hence government recommend.. All health & social care professionals should demonstrate effective information giving, compassionate communication & general psychological support skills NICE (2004) Emphasis on early recognition/prognosis, advance care planning, holistic assessment and person centred decision making all of which requires sensitive, open and honest communication End of Life Strategy (2008)
21 However. Despite the high number of people with cancer who are distressed, many go undetected and untreated by clinicians, Butow,P et al 2007 Up to 60% of concerns remain undisclosed in hospice setting Heaven & Maguire 1996, Psychology Oncology Abstract 80% concerns remain undisclosed in in-patient hospital setting Farrell et al 2005, Pt Education and Counselling 24% cancer patients stated they need more support from their GPs, including information on who to contact with their concerns Royal College of Physicians (2012)
22 Psychological morbidity 70% of significant distress undetected by doctors in cancer centres Fallowfield et al 2001, British Journal of Cancer Psychological Distress Distress is often underdiagnosed during cancer care Despite the frequency, relevance to the provision of holistic treatment, morbidity, and amenability to management Ziegler L et al (2011)
23 Some good news though.. Cancer Patient Experience Survey 2011/12 (where 71,793 patients completed a survey with an overall national response rate of 68%) the most significant increases in positive scores are on information and communication issues. On the other hand
24 CQC NHS inpatient survey 2013 Key complaints 47% of patients do not feel fully involved with their discharge planning from hospital. 39% reported that they were completely told about medication side effects to watch out for when they went home. 43% were completely told about any danger signals they should watch out for at home
25 Chang, A et al 2014 A survey of prognosis discussions held by healthcare providers who request palliative care consultation found: Most HCPs interviewed stated they did not include psycho social issues 21% patients reported lack of information regarding prognosis
26
27 Let s Hear it from the patient.
28 Why is it so difficult sometimes?
29 What prevents people from sharing worries and needs? Why can we struggle to talk about dying?
30 Difficult because.. concerns about impact on patient Uncontrollably upset Angry and shout Go silent Start asking difficult questions That we may make things worse
31 Concerns for ourselves Taking up too much time Coping with our own emotions I won t know what to do about the problems raised I may not be able to manage the emotions /problems expressed Wanting to avoid problems that I can t change & focus on those I can help with I have no support for myself I have no-one to refer on to
32 But how can we be more effective?
33 Six attributes of an effective EoLC conversation: Playing it straight Staying the course Giving time Showing you care Making it clear Pacing information Kirk et al (2004, BMJ) interviewed 72 palliative care cancer patients and their families.
34 Key behaviours to help patients to talk Non-verbal: Being attentive Eye contact Nodding Appearing interested / concerned Leaving space for patient to talk Mirroring Responding to cues Verbal: Open questions (open directive) Questions about feelings / naming feelings Clarifying Summarising and reflecting back Use of silence Empathy Educated guesses Avoiding jargon Responding to cues
35 Recognise behaviours that block patients talking Leading questions Closed questions Multiple questions Focusing only on the physical Giving advice prematurely Offering premature or false reassurance Normalizing Using jargon Jollying along Changing the topic Blaming Being defensive
36 Pick up on Concerns and Cues: A Concern Concerns, contrary to cues, help the health provider to recognize emotional distress in patients. Concerns suggest greater accessibility of patients to their emotions Zimmermann, C (2011) A Cue.. something that a patient says or does that is a hint that there is something more to be explored
37 Importance of cues Facilitative questions linked to cues increase the probability of further cues and are key to a patient-centred consultation Open questions linked to a cue are 4.5 times more likely to lead to further significant disclosure than unlinked open questions Facilitating the first patient cue appears to be important (20% drop in cues during consultation if first cue is not facilitated) Zimmerman et al 2003, Epidemiology & Social Psychiatry Fletcher PhD thesis 2006
38 Cues Verbal Non-verbal Verbal hints to hidden concerns Words/phrases suggesting vague or undefined emotions Psychological symptoms Words / phrases describing physiological correlates of unpleasant emotional states Repeated or emphasised mention of an event or issue Clear expression of a negative or unpleasant emotion (e.g. crying, pacing room) Hints to hidden emotions (sighing, silence, frowning, negative body posture)
39 Apply our strategies for effective consultations: The Calgary-Cambridge model I.C.E SPIKES
40 SPIKES protocol for breaking bad news S- Setting P-Perception of condition/seriousness I-Invitation from the patient to give information K-Knowledge: giving (medical) facts E-Explore emotions and empathize S-Strategy and summary Baile, W et al. SPIKES- a six step protocol for delivering bad news. Oncologist 2000; 5:
41 Utilise the available Tools Advance Care Plan Documentation Preferred Priorities of Care Treatment Escalation Plans DNaCPR, ADRT Best Interest Decision Making EPCCS electronic register
42 What do we mean by Advance Care Planning? All people approaching the end of life need to have their needs assessed, their wishes and preferences discussed and an agreed set of actions reflecting the choices they make about their care recorded in a care plan The NHS End of Life Care Strategy (2010) 42
43 Preferred Priorities of Care Around 70% patients express a wish to die at home However about 50% die in hospital How can we in primary care help our patients to achieve their wishes? 43
44 A typical case Mrs Smith has been discharged from the acute hospital to a care home She is no longer able to cope at home She has multiple co-morbidities including COPD, heart failure and CKD She tells you she does not want to go back to hospital in any circumstances How can we ensure she gets her wishes? 44
45 45 Advance Care Planning Booklet
46 Advance Care Planning What I dowant Statement of wishes and care preferences Includes preferred place of care and next of kin details Not legally binding What I don t want Advance decision to refuse treatment (in specific circumstances) Related to capacity Is legally binding (if valid) 46
47 47
48 48
49 Additional features of booklet Putting your affairs in order Appointing someone to make decisions for you (lasting power of attorney) Making a Will Funeral Planning 49
50 Back to Mrs Smith Mrs Smith has now had an opportunity to discuss and document her wishes Now comes the difficult bit resuscitation How do you approach this? Do you ask would you like to be resuscitated? Is it her choice? 50
51 Treatment Escalation Plan and Resuscitation Decision Record Devon-wide form for use across all health care sectors, and into the home Enables continuity of decisions from secondary to primary care Avoids repeated resus discussion Original form travels with the patient 51
52 52
53 53
54 TEP form Key Messages Not legally binding common sense and professional judgment should be applied to who should have one and how it is used Wherever possible, discuss with patient and relative, and document this discussion It is only effective if everyone knows it exists update EPaCCS 54
55 How do we make sure everyone knows what Mrs Smith wants? Having had the conversation and completed the documents, it is now important to share this information with our colleagues. How do we achieve this? 55
56 Electronic Palliative Care Co-ordination System (EPaCCS) Held on Adastra system (with SPM) Accessible to SWAST, acute trusts, hospices, community nurses, as well as Devon Doctors Allows presence of TEP form, ACP document, anticipatory drugs to be flagged up Able to share other useful information about our patients with OOH clinicians 56
57 57
58
59 59
60 60
61
62 The Outcome Mrs Smith declines gradually and dies in her preferred place of care in the nursing home Her family are grateful that she achieved her wishes 62
63
64 Mental Capacity at End of Life But what if Mrs Smith had dementia? How would you assess her capacity to be involved in the decision making? How would you document this? Who else might you need to involve? 64
65 The Mental Capacity Act 2005 Always start by assuming the patient has capacity You are required to maximise the person s capacity All practicable steps must be taken to facilitate communication An eccentric or unwise decision does not imply lack of capacity 65
66 Assessing Capacity 1. Can they understand the information? 2. Can they retain the information? 3. Can they use or weigh up the information? 4. Can they communicate their decision? This can be recorded on a FACE document 66
67 Making a best interests decision Is there a valid ADRT and/or a Personal Welfare Power of Attorney? Is there anyone that could be consulted about the patient s best interests? If no to above: in an emergency act in the patient s best interests Otherwise involve an Independent Mental Capacity Advocate (IMCA)
68 Scenarios
69 References Back, A,L. Trinidad, S, B, Hopley, E K Arnold, R M Baile W F Edwards K A ( 2011). What Patients Value When Oncologists Give News of Cancer Recurrence The Oncologist 2011, 16: Burgess. C( 2005Depression and anxiety in women with early breast cancer: BMJ 2005;: D3 Butow P1 Cockburn J, Girgis A et al (2007) Increasing oncologists skills in eliciting and responding to emotional cues: evaluation of a communication skills training program Psycho- Oncology (2007)(in press)published online in Wiley InterScience ( DOI: /pon.1217
70 References Chang. A Datta-Barua, McLaughlin B, Daly, B (2014) A survey of prognosis discussions held by healthcare providers who request palliative care consultation Palliative Medicine, vol. 28, no. 4, p , (April 2014 CQC (2013) National Findings from 2013 Inpatients surveyhttp:// urvey_national_summary.pdf de Silva.D 2013 Health Foundation Evidence scan The Evidence Centre debra@evidencecentre.com
71 References Fallowfield,LJ. Hall,A. Maguire G,P. Bam M.(1990) Psychological outcomes of different treatment policies in women with early breast cancer outside a clinical trial. BMJ. Sep 22, 1990; 301(6752): PMCID: PMC Royal college of physicians (2012) Cancer patients in crisis, responding to urgent need
72 References Tuana Dowan (2014) and the website. Ref A Mehrabian (1939) Ziegler,L Hill,K Neilly,L Bennett M I,. Higginson,I J et al ( Ziegler,L Hill,K Neilly,L Bennett M I,. Higginson,I J et al ( 2011) Identifying Psychological Distress at Key Stages of the Cancer Illness Trajectory:A Systematic Review of ValidatedSelf-Report Measures Journal of Pain and Symptom Management 619 Vol. 41 No. 3 March 2011
73 References Zimmermann, C., Piccolo, L. del, Bensing, J., Bergvik, et al Coding patient emotional cues and concerns in medical consultations Patient Education and Counselling: 2011, 82(2),
Identify essential primary palliative care (PPC) communication skills that every provider needs AND clinical triggers for PPC conversations
 Identify essential primary palliative care (PPC) communication skills that every provider needs AND clinical triggers for PPC conversations Esmé Finlay, MD Division of Palliative Medicine University of
Identify essential primary palliative care (PPC) communication skills that every provider needs AND clinical triggers for PPC conversations Esmé Finlay, MD Division of Palliative Medicine University of
Difficult conversations. Dr Amy Waters MBBS, FRACP Staff Specialist in Palliative Medicine, St George Hospital Conjoint Lecturer, UNSW
 Difficult conversations Dr Amy Waters MBBS, FRACP Staff Specialist in Palliative Medicine, St George Hospital Conjoint Lecturer, UNSW What are difficult conversations? Why are they difficult? Difficult
Difficult conversations Dr Amy Waters MBBS, FRACP Staff Specialist in Palliative Medicine, St George Hospital Conjoint Lecturer, UNSW What are difficult conversations? Why are they difficult? Difficult
Let s get the Conversation Started. Helen Meehan - Lead Nurse Palliative and End of Life Care
 Let s get the Conversation Started Helen Meehan - Lead Nurse Palliative and End of Life Care Background Royal United Hospitals (RUH) catchment population of 500,000 with 565 acute beds Serves 4 CCGs End
Let s get the Conversation Started Helen Meehan - Lead Nurse Palliative and End of Life Care Background Royal United Hospitals (RUH) catchment population of 500,000 with 565 acute beds Serves 4 CCGs End
Patient-centred communication: involving the patients on their own terms
 Patient-centred communication: involving the patients on their own terms A workshop Jonathan Silverman and Pål Gulbrandsen Hindsgavl Castle, Denmark June 2016 Patient-centeredness doesn't come about by
Patient-centred communication: involving the patients on their own terms A workshop Jonathan Silverman and Pål Gulbrandsen Hindsgavl Castle, Denmark June 2016 Patient-centeredness doesn't come about by
Delivering Bad News. April 27, 2017
 Delivering Bad News April 27, 2017 Introduction Barbara Lewis, MBA Managing Editor DocCom Timothy E. Quill, MD, FACP, FAAHPM Distinguished Professor of Medicine Palliative Care Program University of Rochester
Delivering Bad News April 27, 2017 Introduction Barbara Lewis, MBA Managing Editor DocCom Timothy E. Quill, MD, FACP, FAAHPM Distinguished Professor of Medicine Palliative Care Program University of Rochester
We need to talk about Palliative Care. Pancreatic Cancer UK
 We need to talk about Palliative Care Pancreatic Cancer UK 1. Pancreatic Cancer UK welcomes the opportunity to respond to the Health and Sport Committee s inquiry on palliative care. About Pancreatic Cancer
We need to talk about Palliative Care Pancreatic Cancer UK 1. Pancreatic Cancer UK welcomes the opportunity to respond to the Health and Sport Committee s inquiry on palliative care. About Pancreatic Cancer
Unmet palliative care needs in heart failure heart failure. Dr Claire Hookey
 Unmet palliative care needs in heart failure heart failure Dr Claire Hookey Discomfort was not necessarily greatest in those dying from cancer; patients dying of heart failure, or renal failure, or both,
Unmet palliative care needs in heart failure heart failure Dr Claire Hookey Discomfort was not necessarily greatest in those dying from cancer; patients dying of heart failure, or renal failure, or both,
COMMUNICATION ISSUES IN PALLIATIVE CARE
 COMMUNICATION ISSUES IN PALLIATIVE CARE Palliative Care: Communication, Communication, Communication! Key Features of Communication in Appropriate setting Permission Palliative Care Be clear about topic
COMMUNICATION ISSUES IN PALLIATIVE CARE Palliative Care: Communication, Communication, Communication! Key Features of Communication in Appropriate setting Permission Palliative Care Be clear about topic
Challenging Medical Communications. Dr Thiru Thirukkumaran Palliative Care Services Northwest Tasmania
 Challenging Medical Communications Dr Thiru Thirukkumaran Palliative Care Services Northwest Tasmania What are the common Challenging situations? Common Challenging situations Handling difficult questions
Challenging Medical Communications Dr Thiru Thirukkumaran Palliative Care Services Northwest Tasmania What are the common Challenging situations? Common Challenging situations Handling difficult questions
AFSP SURVIVOR OUTREACH PROGRAM VOLUNTEER TRAINING HANDOUT
 AFSP SURVIVOR OUTREACH PROGRAM VOLUNTEER TRAINING HANDOUT Goals of the AFSP Survivor Outreach Program Suggested Answers To Frequently Asked Questions on Visits Roadblocks to Communication During Visits
AFSP SURVIVOR OUTREACH PROGRAM VOLUNTEER TRAINING HANDOUT Goals of the AFSP Survivor Outreach Program Suggested Answers To Frequently Asked Questions on Visits Roadblocks to Communication During Visits
You want us to do everything?! RETHINKING COMMUNICATION AROUND GOALS OF CARE
 You want us to do everything?! RETHINKING COMMUNICATION AROUND GOALS OF CARE Michael D. Barnett, MD, MS, FAAP, FAAHPM UAB Center for Palliative & Supportive Care OBJECTIVES 1. Gauge patient/family understanding
You want us to do everything?! RETHINKING COMMUNICATION AROUND GOALS OF CARE Michael D. Barnett, MD, MS, FAAP, FAAHPM UAB Center for Palliative & Supportive Care OBJECTIVES 1. Gauge patient/family understanding
Communication with relatives of critically ill patients. Dr WAN Wing Lun Specialist in Critical Care Medicine Yan Chai Hospital
 Communication with relatives of critically ill patients Dr WAN Wing Lun Specialist in Critical Care Medicine Yan Chai Hospital Why is communication with relatives important? Relatives of ICU patients suffer
Communication with relatives of critically ill patients Dr WAN Wing Lun Specialist in Critical Care Medicine Yan Chai Hospital Why is communication with relatives important? Relatives of ICU patients suffer
Goals of Care Conversations Training Goals of Care Conversations about Life-Sustaining Treatment Decisions
 Goals of Care Conversations Training Goals of Care Conversations about Life-Sustaining Treatment Decisions Shaida Talebreza, MD, FAAHPM, AGSF Associate Professor, University of Utah School of Medicine
Goals of Care Conversations Training Goals of Care Conversations about Life-Sustaining Treatment Decisions Shaida Talebreza, MD, FAAHPM, AGSF Associate Professor, University of Utah School of Medicine
Mental Health Strategy. Easy Read
 Mental Health Strategy Easy Read Mental Health Strategy Easy Read The Scottish Government, Edinburgh 2012 Crown copyright 2012 You may re-use this information (excluding logos and images) free of charge
Mental Health Strategy Easy Read Mental Health Strategy Easy Read The Scottish Government, Edinburgh 2012 Crown copyright 2012 You may re-use this information (excluding logos and images) free of charge
HERTS VALLEYS CCG PALLIATIVE AND END OF LIFE CARE STRATEGY FOR ADULTS AND CHILDREN
 HERTS VALLEYS CCG PALLIATIVE AND END OF LIFE CARE STRATEGY FOR ADULTS AND CHILDREN 2016-2021 1 1. Introduction Herts Valleys Palliative and End of Life Care Strategy is guided by the End of Life Care Strategic
HERTS VALLEYS CCG PALLIATIVE AND END OF LIFE CARE STRATEGY FOR ADULTS AND CHILDREN 2016-2021 1 1. Introduction Herts Valleys Palliative and End of Life Care Strategy is guided by the End of Life Care Strategic
Communication Skills Sharing Bad News
 Communication Skills Sharing Bad News Is communication a problem in healthcare? Globally Some studies indicate 70 to 80 percent of medical errors are related to interpersonal interaction issues. [1] Poor
Communication Skills Sharing Bad News Is communication a problem in healthcare? Globally Some studies indicate 70 to 80 percent of medical errors are related to interpersonal interaction issues. [1] Poor
What is dementia? Dementia is not a disease but is a group of signs and symptoms.
 Is it dementia? What is dementia? Dementia is not a disease but is a group of signs and symptoms. Dementia rates are increasing Around 850, 000 people in the UK have dementia. By 2025 this number is expected
Is it dementia? What is dementia? Dementia is not a disease but is a group of signs and symptoms. Dementia rates are increasing Around 850, 000 people in the UK have dementia. By 2025 this number is expected
If you would like to find out more about this service:
 Step by Step Information for parents and carers This guidance forms part of Samaritans Step by Step resources for communities working with and supporting young people. Step by Step is a Samaritans service
Step by Step Information for parents and carers This guidance forms part of Samaritans Step by Step resources for communities working with and supporting young people. Step by Step is a Samaritans service
MRCGP Clinical Skills Assessment CSA Candidate Feedback FOR EXAMS TAKEN FROM JANUARY 2012
 MRCGP Clinical Skills Assessment CSA Candidate Feedback FOR EXAMS TAKEN FROM JANUARY 2012 How to use the feedback After your Clinical Skills Assessment you will be informed of your performance overall
MRCGP Clinical Skills Assessment CSA Candidate Feedback FOR EXAMS TAKEN FROM JANUARY 2012 How to use the feedback After your Clinical Skills Assessment you will be informed of your performance overall
Delivering personalised care to end of life patients. Jane Naismith Nurse Consultant in Palliative care St Joseph s Hospice London
 Delivering personalised care to end of life patients Jane Naismith Nurse Consultant in Palliative care St Joseph s Hospice London Over View This session will cover Supporting patients with long term conditions
Delivering personalised care to end of life patients Jane Naismith Nurse Consultant in Palliative care St Joseph s Hospice London Over View This session will cover Supporting patients with long term conditions
Breaking bad news - communicating with the cancer patient
 Breaking bad news - communicating with the cancer patient Paweł Potocki, MD Jagiellonian University Medical College Kraków University Hospital Departament of Clinical Oncology pawel.potocki@uj.edu.pl Breaking
Breaking bad news - communicating with the cancer patient Paweł Potocki, MD Jagiellonian University Medical College Kraków University Hospital Departament of Clinical Oncology pawel.potocki@uj.edu.pl Breaking
Improving End of Life Care for People with Dementia. Lucy Sutton, End of Life Care Lead
 Improving End of Life Care for People with Dementia Lucy Sutton, End of Life Care Lead Why do we Need to? I stood outside her room and heard her scream with pain when they changed her. I asked for the
Improving End of Life Care for People with Dementia Lucy Sutton, End of Life Care Lead Why do we Need to? I stood outside her room and heard her scream with pain when they changed her. I asked for the
Deciding whether a person has the capacity to make a decision the Mental Capacity Act 2005
 Deciding whether a person has the capacity to make a decision the Mental Capacity Act 2005 April 2015 Deciding whether a person has the capacity to make a decision the Mental Capacity Act 2005 The RMBI,
Deciding whether a person has the capacity to make a decision the Mental Capacity Act 2005 April 2015 Deciding whether a person has the capacity to make a decision the Mental Capacity Act 2005 The RMBI,
!This booklet is for family and friends of anyone who.!these decisions may be related to treatment they re
 MENTAL CAPACITY ACT INFORMATION What is the Mental Capacity Act? The Mental Capacity Act 2005 (MCA) was implemented by parliament in 2007 and is a vitally important piece of legislation for England and
MENTAL CAPACITY ACT INFORMATION What is the Mental Capacity Act? The Mental Capacity Act 2005 (MCA) was implemented by parliament in 2007 and is a vitally important piece of legislation for England and
Communicating with Patients with Heart Failure and their Families
 Communicating with Patients with Heart Failure and their Families Nathan Goldstein, MD Associate Professor Hertzberg Palliative Care Institute Brookdale Department of Geriatrics and Palliative Medicine
Communicating with Patients with Heart Failure and their Families Nathan Goldstein, MD Associate Professor Hertzberg Palliative Care Institute Brookdale Department of Geriatrics and Palliative Medicine
We have other booklets with information for people living in either England and Wales or Northern Ireland, which we can send you.
 (SCOTLAND) About this booklet About this booklet This booklet is about some of the ways you can plan ahead and make choices about your future care if you live in Scotland. The booklet is for anyone who
(SCOTLAND) About this booklet About this booklet This booklet is about some of the ways you can plan ahead and make choices about your future care if you live in Scotland. The booklet is for anyone who
SEARCH AND RESCUE Supporting a colleague with a mental health problem
 SEARCH AND RESCUE Supporting a colleague with a mental health problem Blue Light Programme Supporting a colleague with a mental health problem This is a guide for search and rescue staff and volunteers
SEARCH AND RESCUE Supporting a colleague with a mental health problem Blue Light Programme Supporting a colleague with a mental health problem This is a guide for search and rescue staff and volunteers
Our plan for giving better care to people with dementia Oxleas Dementia
 Our plan for giving better care to people with dementia Oxleas Dementia 2013-2016 November 2013 1 Contents 1. What is our plan about? 2. Finding out if someone has dementia 3. Finding out the care and
Our plan for giving better care to people with dementia Oxleas Dementia 2013-2016 November 2013 1 Contents 1. What is our plan about? 2. Finding out if someone has dementia 3. Finding out the care and
Challenging conversations in the Emergency Department
 Challenging conversations in the Emergency Department ED Teaching Day, 27 th April 2017 Renton Perry Specialty Doctor in Emergency Medicine The Plan 1. SHORT INTRO Dying matters -Communications at the
Challenging conversations in the Emergency Department ED Teaching Day, 27 th April 2017 Renton Perry Specialty Doctor in Emergency Medicine The Plan 1. SHORT INTRO Dying matters -Communications at the
Living with Advanced Colorectal Cancer: A Balancing Act
 Living with Advanced Colorectal Cancer: A Balancing Act Simone Stenekes Clinical Nurse Specialist CancerCare Manitoba Symptom Management & Palliative Care Disease Site Group Presenter Disclosure Faculty:
Living with Advanced Colorectal Cancer: A Balancing Act Simone Stenekes Clinical Nurse Specialist CancerCare Manitoba Symptom Management & Palliative Care Disease Site Group Presenter Disclosure Faculty:
The Recovery Journey after a PICU admission
 The Recovery Journey after a PICU admission A guide for families Introduction This booklet has been written for parents and young people who have experienced a Paediatric Intensive Care Unit (PICU) admission.
The Recovery Journey after a PICU admission A guide for families Introduction This booklet has been written for parents and young people who have experienced a Paediatric Intensive Care Unit (PICU) admission.
Cancer and Advance Care Planning You ve been diagnosed with cancer. Now what?
 Cancer and Advance Care Planning You ve been diagnosed with cancer. Now what? ACP Cancer Booklet-- Patient_FINAL.indd 1 You have a lot to think about and it can be difficult to know where to start. One
Cancer and Advance Care Planning You ve been diagnosed with cancer. Now what? ACP Cancer Booklet-- Patient_FINAL.indd 1 You have a lot to think about and it can be difficult to know where to start. One
Preventing harmful treatment
 Preventing harmful treatment How can Palliative Care prevent patients receiving overzealous or futile treatment? Antwerp, November 2010 Prof Scott A Murray, St Columba s Hospice Chair of Primary Palliative
Preventing harmful treatment How can Palliative Care prevent patients receiving overzealous or futile treatment? Antwerp, November 2010 Prof Scott A Murray, St Columba s Hospice Chair of Primary Palliative
Beyond the Liverpool Care Pathway
 Beyond the Liverpool Care Pathway Bridget Withell EOLC Facilitator www.ellenorlions.org What was the LCP? What went wrong? The review What now? Liverpool Care Pathway Originally developed by Marie Curie
Beyond the Liverpool Care Pathway Bridget Withell EOLC Facilitator www.ellenorlions.org What was the LCP? What went wrong? The review What now? Liverpool Care Pathway Originally developed by Marie Curie
We need to talk about Palliative Care COSLA
 Introduction We need to talk about Palliative Care COSLA 1. Local government recognises the importance of high quality palliative and end of life care if we are to give people greater control over how
Introduction We need to talk about Palliative Care COSLA 1. Local government recognises the importance of high quality palliative and end of life care if we are to give people greater control over how
Module 3: Communicating bad news to cancer patients
 Module 3: Communicating bad news to cancer patients Luzia Travado, PhD Head of Psycho-oncology, Champalimaud Clinical Center, Lisbon, Portugal International Psycho-Oncology Society, Past-President Communicating
Module 3: Communicating bad news to cancer patients Luzia Travado, PhD Head of Psycho-oncology, Champalimaud Clinical Center, Lisbon, Portugal International Psycho-Oncology Society, Past-President Communicating
STOP, LOOK AND LISTEN: Supporting people with dementia and their families at the end of life
 STOP, LOOK AND LISTEN: Supporting people with dementia and their families at the end of life #DementiaEoLC Today 10.00 - Chair s welcome: Anita Hayes 10.10 - Setting the scene: Anita Hayes and Dr Jackie
STOP, LOOK AND LISTEN: Supporting people with dementia and their families at the end of life #DementiaEoLC Today 10.00 - Chair s welcome: Anita Hayes 10.10 - Setting the scene: Anita Hayes and Dr Jackie
A practical guide to living with and after cancer
 A practical guide to living with and after cancer About this booklet 1 About this booklet This booklet is about some of the ways you can plan ahead and make choices about your future care if you live in
A practical guide to living with and after cancer About this booklet 1 About this booklet This booklet is about some of the ways you can plan ahead and make choices about your future care if you live in
The Palliative Care Journey. By Sandra O Sullivan Clinical Nurse Manager 1 St Luke's home
 The Palliative Care Journey By Sandra O Sullivan Clinical Nurse Manager 1 St Luke's home Aims 1. To provide an overview of what palliative care involves. 2. Identify, at what stage should Dementia be acknowledged
The Palliative Care Journey By Sandra O Sullivan Clinical Nurse Manager 1 St Luke's home Aims 1. To provide an overview of what palliative care involves. 2. Identify, at what stage should Dementia be acknowledged
This information explains the advice about supporting people with dementia and their carers that is set out in NICE SCIE clinical guideline 42.
 Supporting people with dementia and their carers Information for the public Published: 1 November 2006 nice.org.uk About this information NICEclinicalguidelinesadvisetheNHSoncaringforpeoplewithspe cificconditionsordiseasesandthetreatmentstheyshouldreceive.
Supporting people with dementia and their carers Information for the public Published: 1 November 2006 nice.org.uk About this information NICEclinicalguidelinesadvisetheNHSoncaringforpeoplewithspe cificconditionsordiseasesandthetreatmentstheyshouldreceive.
What needs to happen in England
 What needs to happen in England We ve heard from over 9,000 people across the UK about what it is like to live with diabetes and their hopes and fears for the future. Over 6,000 of them live in England;
What needs to happen in England We ve heard from over 9,000 people across the UK about what it is like to live with diabetes and their hopes and fears for the future. Over 6,000 of them live in England;
PALLIATIVE CARE. A Brief Intervention. Euan Paterson Macmillan GP Facilitator (Glasgow)
 PALLIATIVE CARE A Brief Intervention Euan Paterson Macmillan GP Facilitator (Glasgow) euan.paterson@ntlworld.com 07792120108 or How to deal with ACP, epcs and the Palliative Care DES http://www.palliativecareggc.org.uk/
PALLIATIVE CARE A Brief Intervention Euan Paterson Macmillan GP Facilitator (Glasgow) euan.paterson@ntlworld.com 07792120108 or How to deal with ACP, epcs and the Palliative Care DES http://www.palliativecareggc.org.uk/
Supportive and Palliative care for patients with Pancreatic Cancer. Dr Holly Taylor September 2018
 Supportive and Palliative care for patients with Pancreatic Cancer Dr Holly Taylor September 2018 Aims of this session To discuss the principles of supportive and palliative care Identification of patients
Supportive and Palliative care for patients with Pancreatic Cancer Dr Holly Taylor September 2018 Aims of this session To discuss the principles of supportive and palliative care Identification of patients
Module 2 Mentalizing
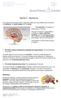 Module 2 Mentalizing It is thought that the human brain is essentially made up of three different brain structures: the brainstem, the limbic system and the cortex. 1. The brainstem: The reptilian or primitive
Module 2 Mentalizing It is thought that the human brain is essentially made up of three different brain structures: the brainstem, the limbic system and the cortex. 1. The brainstem: The reptilian or primitive
SERVICE SPECIFICATION 6 Conservative Management & End of Life Care
 SERVICE SPECIFICATION 6 Conservative Management & End of Life Care Table of Contents Page 1 Key Messages 2 2 Introduction & Background 2 3 Relevant Guidelines & Standards 2 4 Scope of Service 3 5 Interdependencies
SERVICE SPECIFICATION 6 Conservative Management & End of Life Care Table of Contents Page 1 Key Messages 2 2 Introduction & Background 2 3 Relevant Guidelines & Standards 2 4 Scope of Service 3 5 Interdependencies
Who, Me? Starting THE Conversation
 Who, Me? Starting THE Conversation Nancy Flowers, LCSW Social Work Manager Rainbow Hospice and Palliative Care nflowers@rainbowhospice.org 847-685-9900 Objectives Clarify the importance of advance directives
Who, Me? Starting THE Conversation Nancy Flowers, LCSW Social Work Manager Rainbow Hospice and Palliative Care nflowers@rainbowhospice.org 847-685-9900 Objectives Clarify the importance of advance directives
This section will help you to identify and manage some of the more difficult emotional responses you may feel after diagnosis.
 4: Emotional impact This section will help you to identify and manage some of the more difficult emotional responses you may feel after diagnosis. The following information is an extracted section from
4: Emotional impact This section will help you to identify and manage some of the more difficult emotional responses you may feel after diagnosis. The following information is an extracted section from
Setting up a Mental Health Support Group
 Setting up a Mental Health Support Group Colleague Toolkit Practical help from the Co-op Here at the Co-op we recognise that we all have a role to play in supporting each other s wellbeing. This toolkit
Setting up a Mental Health Support Group Colleague Toolkit Practical help from the Co-op Here at the Co-op we recognise that we all have a role to play in supporting each other s wellbeing. This toolkit
The NHS 10-year plan A chance for people with learning disabilities and autistic people s life and care to matter?
 The NHS 10-year plan A chance for people with learning disabilities and autistic people s life and care to matter? Key points We hope this NHS plan can lead to action and real change, so people know they
The NHS 10-year plan A chance for people with learning disabilities and autistic people s life and care to matter? Key points We hope this NHS plan can lead to action and real change, so people know they
Value of emotional intelligence in veterinary practice teams
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Value of emotional intelligence in veterinary practice teams Author : MAGGIE SHILCOCK Categories : Vets Date : February 17,
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Value of emotional intelligence in veterinary practice teams Author : MAGGIE SHILCOCK Categories : Vets Date : February 17,
PALLIATIVE CARE IN NEW YORK STATE
 Collaborative for Palliative Care In collaboration with its partners End of Life Choices New York Finger Lakes Geriatric Education Center at the University of Rochester COLLABORATIVE FOR PALLIATIVE CARE
Collaborative for Palliative Care In collaboration with its partners End of Life Choices New York Finger Lakes Geriatric Education Center at the University of Rochester COLLABORATIVE FOR PALLIATIVE CARE
End of end of life care in dementia opportunities for quality improvement
 End of end of life care in dementia opportunities for quality improvement Sube Banerjee Professor of Dementia, Brighton & Sussex Medical School Hon Consultant, Sussex Partnership NHS Foundation Trust National
End of end of life care in dementia opportunities for quality improvement Sube Banerjee Professor of Dementia, Brighton & Sussex Medical School Hon Consultant, Sussex Partnership NHS Foundation Trust National
Talking to Your Oncologist & Living with Cancer
 Talking to Your Oncologist & Living with Cancer Anthony Back, M.D. University of Washington Fred Hutchinson Cancer Research Center Seattle Cancer Care Alliance Highlights? The old way doctors talked What
Talking to Your Oncologist & Living with Cancer Anthony Back, M.D. University of Washington Fred Hutchinson Cancer Research Center Seattle Cancer Care Alliance Highlights? The old way doctors talked What
Caring for someone who has self-harmed or had suicidal thoughts. A family guide
 Caring for someone who has self-harmed or had suicidal thoughts A family guide This booklet is aimed at the families/carers of people who have self-harmed or had suicidal thoughts. It will be provided
Caring for someone who has self-harmed or had suicidal thoughts A family guide This booklet is aimed at the families/carers of people who have self-harmed or had suicidal thoughts. It will be provided
VNAA Blueprint for Excellence PATHWAY TO BEST PRACTICES
 VNAA Blueprint for Excellence PATHWAY TO BEST PRACTICES Patient and Caregiver Engagement: Artful Conversations VNAA Best Practice for Hospice and Palliative Care Case Study Mr. G is an 88 yo man with end-stage
VNAA Blueprint for Excellence PATHWAY TO BEST PRACTICES Patient and Caregiver Engagement: Artful Conversations VNAA Best Practice for Hospice and Palliative Care Case Study Mr. G is an 88 yo man with end-stage
Best Practice Model Communication/Relational Skills in Soliciting the Patient/Family Story Stuart Farber
 Best Practice Model Communication/Relational Skills in Soliciting the Patient/Family Story Stuart Farber Once you have set a safe context for the palliative care discussion soliciting the patient's and
Best Practice Model Communication/Relational Skills in Soliciting the Patient/Family Story Stuart Farber Once you have set a safe context for the palliative care discussion soliciting the patient's and
Utilizing Strength-Based Communication Strategies with Older Adults
 Utilizing Strength-Based Communication Strategies with Older Adults Linda J. Keilman, DNP, GNP-BC Objectives: 1. Identify interactive communication skills helpful to use with older adults to learn their
Utilizing Strength-Based Communication Strategies with Older Adults Linda J. Keilman, DNP, GNP-BC Objectives: 1. Identify interactive communication skills helpful to use with older adults to learn their
Child and Adolescent Mental Health Service (CAMHS)
 Oxford Health NHS Foundation Trust CAMHS Child and Adolescent Mental Health Service (CAMHS) CAMHS Introduction Welcome to Oxford Health NHS Foundation Trust. This leaflet aims to provide you with answers
Oxford Health NHS Foundation Trust CAMHS Child and Adolescent Mental Health Service (CAMHS) CAMHS Introduction Welcome to Oxford Health NHS Foundation Trust. This leaflet aims to provide you with answers
Symptoms Assess symptoms and needs across all domains. Screen using Edmonton Symptom Assessment System (ESAS) for: Pain Nausea Depression
 A Palliative Care Approach for Oncology Integrating a palliative care approach earlier in the disease trajectory improves the quality of living and dying, and relieves suffering for patients and families
A Palliative Care Approach for Oncology Integrating a palliative care approach earlier in the disease trajectory improves the quality of living and dying, and relieves suffering for patients and families
What happens if I cannot make decisions about my care and treatment?
 Information Line: 0800 999 2434 Website: compassionindying.org.uk What happens if I cannot make decisions about my care and treatment? This factsheet explains how decisions are made about your care or
Information Line: 0800 999 2434 Website: compassionindying.org.uk What happens if I cannot make decisions about my care and treatment? This factsheet explains how decisions are made about your care or
Managing conversations around mental health. Blue Light Programme mind.org.uk/bluelight
 Managing conversations around mental health Blue Light Programme 1 Managing conversations around mental health Managing conversations about mental wellbeing Find a quiet place with an informal atmosphere,
Managing conversations around mental health Blue Light Programme 1 Managing conversations around mental health Managing conversations about mental wellbeing Find a quiet place with an informal atmosphere,
Improving Safety through Key Components of Therapeutic Communication with Behaviorally-Challenged. Martin Reinsel, MA, LMHC, Navos Clinical
 Improving Safety through Key Components of Therapeutic Communication with Behaviorally-Challenged Individuals Martin Reinsel, MA, LMHC, Navos Clinical Educator & Therapist Best Practices for Communication
Improving Safety through Key Components of Therapeutic Communication with Behaviorally-Challenged Individuals Martin Reinsel, MA, LMHC, Navos Clinical Educator & Therapist Best Practices for Communication
MENTAL CAPACITY ACT POLICY (England & Wales)
 Stalbridge Surgery Reviewed June 2017 Next review date June 2018 INTRODUCTION MENTAL CAPACITY ACT POLICY (England & Wales) The Mental Capacity Act (MCA) 2005 became fully effective on 1 st October 2007
Stalbridge Surgery Reviewed June 2017 Next review date June 2018 INTRODUCTION MENTAL CAPACITY ACT POLICY (England & Wales) The Mental Capacity Act (MCA) 2005 became fully effective on 1 st October 2007
Palliative Care Asking the questions that matter to me
 Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
CAMHS. Your guide to Child and Adolescent Mental Health Services
 CAMHS Your guide to Child and Adolescent Mental Health Services The support I received from CAHMS was invaluable and I do not know where I would be now without it. I now study Health and Social Care and
CAMHS Your guide to Child and Adolescent Mental Health Services The support I received from CAHMS was invaluable and I do not know where I would be now without it. I now study Health and Social Care and
University Staff Counselling Service
 University Staff Counselling Service Anxiety and Panic What is anxiety? Anxiety is a normal emotional and physiological response to feeling threatened, ranging from mild uneasiness and worry to severe
University Staff Counselling Service Anxiety and Panic What is anxiety? Anxiety is a normal emotional and physiological response to feeling threatened, ranging from mild uneasiness and worry to severe
A guide to prostate cancer clinical trials
 1 A guide to prostate cancer clinical trials In this fact sheet: What is a clinical trial? Why are trials done? What are trials looking into at the moment? What happens in a clinical trial? Should I take
1 A guide to prostate cancer clinical trials In this fact sheet: What is a clinical trial? Why are trials done? What are trials looking into at the moment? What happens in a clinical trial? Should I take
DISCUSSING GOALS OF CARE:
 0 DISCUSSING GOALS OF CARE: Evidence based communication skills in action. Abstract Discussing goals of care and limitations of care and limitations of medical treatment with patients is a challenging
0 DISCUSSING GOALS OF CARE: Evidence based communication skills in action. Abstract Discussing goals of care and limitations of care and limitations of medical treatment with patients is a challenging
Look to see if they can focus on compassionate attention, compassionate thinking and compassionate behaviour. This is how the person brings their
 Compassionate Letter Writing Therapist Notes The idea behind compassionate mind letter writing is to help people engage with their problems with a focus on understanding and warmth. We want to try to bring
Compassionate Letter Writing Therapist Notes The idea behind compassionate mind letter writing is to help people engage with their problems with a focus on understanding and warmth. We want to try to bring
Mental Capacity Implementation Programme. Mental Capacity Act 2005
 Mental Capacity Implementation Programme Mental Capacity Act 2005 The Presentation Is an Overview and Will Cover: Part one - background and key policy Why we needed the act and who it affects The Mental
Mental Capacity Implementation Programme Mental Capacity Act 2005 The Presentation Is an Overview and Will Cover: Part one - background and key policy Why we needed the act and who it affects The Mental
Psychological wellbeing in heart failure
 Patient information Struggling to cope? Can trelax? Psychological wellbeing in heart failure Stressedout? Trouble sleeping? Feelinglow? i Living with heart failure can be challenging mentally as well as
Patient information Struggling to cope? Can trelax? Psychological wellbeing in heart failure Stressedout? Trouble sleeping? Feelinglow? i Living with heart failure can be challenging mentally as well as
4 Domains Public Health (NMC 2004)
 4 Domains Public Health (NMC 2004) 4. Facilitation of health enhancing activities 3.Influence on policies affecting health 2.Stimulation of awareness of health needs 1.Search for Health Need Work with
4 Domains Public Health (NMC 2004) 4. Facilitation of health enhancing activities 3.Influence on policies affecting health 2.Stimulation of awareness of health needs 1.Search for Health Need Work with
Guidelines for Working with People Affected by Trauma
 Guidelines for Working with People Affected by Trauma Guidelines For Working with People Affected by Trauma Strengths-Based Perspective Focusing on strengths instead of weaknesses is a basic tenant of
Guidelines for Working with People Affected by Trauma Guidelines For Working with People Affected by Trauma Strengths-Based Perspective Focusing on strengths instead of weaknesses is a basic tenant of
7th Annual Conference on Dementia & End of Life
 #dyingwithdementia #dementiachallenge 7th Annual Conference on Dementia & End of Life Rising to the Prime Minister s Dementia Challenge Tuesday 4 th December 15 Hatfields, London #dyingwithdementia #dementiachallenge
#dyingwithdementia #dementiachallenge 7th Annual Conference on Dementia & End of Life Rising to the Prime Minister s Dementia Challenge Tuesday 4 th December 15 Hatfields, London #dyingwithdementia #dementiachallenge
ADHD clinic for adults Feedback on services for attention deficit hyperactivity disorder
 ADHD clinic for adults Feedback on services for attention deficit hyperactivity disorder Healthwatch Islington Healthwatch Islington is an independent organisation led by volunteers from the local community.
ADHD clinic for adults Feedback on services for attention deficit hyperactivity disorder Healthwatch Islington Healthwatch Islington is an independent organisation led by volunteers from the local community.
(RGN, BN,FETC,MA,Independent Prescriber)
 Nicola West (RGN, BN,FETC,MA,Independent Prescriber) Consultant Nurse/ Lecturer Cardiff Breast Unit University Health Board Wales School of Healthcare Sciences Cardiff University Quality of Life-The patients
Nicola West (RGN, BN,FETC,MA,Independent Prescriber) Consultant Nurse/ Lecturer Cardiff Breast Unit University Health Board Wales School of Healthcare Sciences Cardiff University Quality of Life-The patients
WICKING DEMENTIA RESEARCH & EDUCATION CENTRE. Prof. Fran McInerney RN, BAppSci, MA, PhD Professor of Dementia Studies and Education
 WICKING DEMENTIA RESEARCH & EDUCATION CENTRE Prof. Fran McInerney RN, BAppSci, MA, PhD Professor of Dementia Studies and Education Wicking Dementia Research & Education Centre Engaging families in a palliative
WICKING DEMENTIA RESEARCH & EDUCATION CENTRE Prof. Fran McInerney RN, BAppSci, MA, PhD Professor of Dementia Studies and Education Wicking Dementia Research & Education Centre Engaging families in a palliative
Overcome your need for acceptance & approval of others
 Psoriasis... you won t stop me! Overcome your need for acceptance & approval of others Royal Free London NHS Foundation Trust Psoriasis You Won t Stop Me This booklet is part of the Psoriasis You Won t
Psoriasis... you won t stop me! Overcome your need for acceptance & approval of others Royal Free London NHS Foundation Trust Psoriasis You Won t Stop Me This booklet is part of the Psoriasis You Won t
The Wellbeing Course. Resource: Mental Skills. The Wellbeing Course was written by Professor Nick Titov and Dr Blake Dear
 The Wellbeing Course Resource: Mental Skills The Wellbeing Course was written by Professor Nick Titov and Dr Blake Dear About Mental Skills This resource introduces three mental skills which people find
The Wellbeing Course Resource: Mental Skills The Wellbeing Course was written by Professor Nick Titov and Dr Blake Dear About Mental Skills This resource introduces three mental skills which people find
Healthy Mind Healthy Weight
 Healthy Mind Healthy Weight Taking Control of your eating Part 2:Techniques and Strategies 1 Aims of Sessions The 3 main steps to controlling your eating pattern: - Starting well - Self monitoring - Regular
Healthy Mind Healthy Weight Taking Control of your eating Part 2:Techniques and Strategies 1 Aims of Sessions The 3 main steps to controlling your eating pattern: - Starting well - Self monitoring - Regular
Title Deactivation of Implantable Cardioverter Defibrillators (ICD) towards the end of life Guidelines
 Document Control Title Deactivation of Implantable Cardioverter Defibrillators (ICD) towards the end of life Guidelines Author Lead Nurse for Cardiac Support Services Northern Arrhythmia Care Coordinator
Document Control Title Deactivation of Implantable Cardioverter Defibrillators (ICD) towards the end of life Guidelines Author Lead Nurse for Cardiac Support Services Northern Arrhythmia Care Coordinator
How is primary breast cancer treated?
 How is primary breast cancer treated? The treatment team This information is for anyone who has primary breast cancer and wants to know more about how it is treated. It is written by Breast Cancer Care,
How is primary breast cancer treated? The treatment team This information is for anyone who has primary breast cancer and wants to know more about how it is treated. It is written by Breast Cancer Care,
Northamptonshire Hospice Charities Strategy
 Northamptonshire Hospice Charities Strategy Please note that sections in italics are comments related to the main statement above it. Introduction This document sets out how the hospice charities in Northamptonshire
Northamptonshire Hospice Charities Strategy Please note that sections in italics are comments related to the main statement above it. Introduction This document sets out how the hospice charities in Northamptonshire
Functional Analytic Group Therapy: In-Vivo Healing in Community Context (18)
 Functional Analytic Group Therapy: In-Vivo Healing in Community Context (18) Disclosure (no support): Luc Vandenberghe and Renee Hoekstra: We have not received and will not receive any commercial support
Functional Analytic Group Therapy: In-Vivo Healing in Community Context (18) Disclosure (no support): Luc Vandenberghe and Renee Hoekstra: We have not received and will not receive any commercial support
Background. Yet, as a nation, we find it hard to talk about and harder still to help people dealing with a bereavement.
 A better grief 2 A better grief Background We all experience bereavement and grief at some stage in our lives. Seventy-two per cent of us have been bereaved at least once in the last five years, according
A better grief 2 A better grief Background We all experience bereavement and grief at some stage in our lives. Seventy-two per cent of us have been bereaved at least once in the last five years, according
MOTIVATIONAL INTERVIEWING
 MOTIVATIONAL INTERVIEWING Facilitating Behaviour Change Dr Kate Hall MCCLP MAPS Senior Lecturer in Addiction and Mental Health School of Psychology, Faculty of Health, Deakin University. Lead, Treatment
MOTIVATIONAL INTERVIEWING Facilitating Behaviour Change Dr Kate Hall MCCLP MAPS Senior Lecturer in Addiction and Mental Health School of Psychology, Faculty of Health, Deakin University. Lead, Treatment
HULL AND EAST RIDING OF YORKSHIRE DEMENTIA, PALLIATIVE AND END OF LIFE CARE WORKING GROUP REPORT NOVEMBER 2011
 HULL AND EAST RIDING OF YORKSHIRE DEMENTIA, PALLIATIVE AND END OF LIFE CARE WORKING GROUP REPORT NOVEMBER 2011 Authors:- Laura Wigley, Macmillan Palliative & End of Life Care Programme Manager, Humber
HULL AND EAST RIDING OF YORKSHIRE DEMENTIA, PALLIATIVE AND END OF LIFE CARE WORKING GROUP REPORT NOVEMBER 2011 Authors:- Laura Wigley, Macmillan Palliative & End of Life Care Programme Manager, Humber
FINDING THE RIGHT WORDS IN ADVANCED AND METASTATIC BREAST CANCER (ABC/MBC)
 FINDING THE RIGHT WORDS IN ADVANCED AND METASTATIC BREAST CANCER (ABC/MBC) Real people. Real communication. Making a real difference. 000989_NOV19_Breast_Cancer_Language_Guide_HCPs_V4_CL.indd 1 What do
FINDING THE RIGHT WORDS IN ADVANCED AND METASTATIC BREAST CANCER (ABC/MBC) Real people. Real communication. Making a real difference. 000989_NOV19_Breast_Cancer_Language_Guide_HCPs_V4_CL.indd 1 What do
5: Family, children and friends
 5: Family, children and friends This section will help you to manage difficult conversations as people close to you adjust to your diagnosis of MND. The following information is an extracted section from
5: Family, children and friends This section will help you to manage difficult conversations as people close to you adjust to your diagnosis of MND. The following information is an extracted section from
Changes to your behaviour
 Life after stroke Changes to your behaviour Together we can conquer stroke Because there is so much to deal with after a stroke, it s normal for your behaviour to change in some way. In this booklet we
Life after stroke Changes to your behaviour Together we can conquer stroke Because there is so much to deal with after a stroke, it s normal for your behaviour to change in some way. In this booklet we
Depression and Low Mood. Easy read information
 Depression and Low Mood Easy read information A member of staff or a carer can support you to read this booklet. They will be able to answer any questions that you have. About this leaflet This leaflet
Depression and Low Mood Easy read information A member of staff or a carer can support you to read this booklet. They will be able to answer any questions that you have. About this leaflet This leaflet
Palliative & End of Life Care in Frailty & Dementia. Dr Ruth Ting Palliative Care Consultant Gateshead
 Palliative & End of Life Care in Frailty & Dementia Dr Ruth Ting Palliative Care Consultant Gateshead One Chance to get it right How people die remains in the memory of those who live on Dame Cicely Saunders
Palliative & End of Life Care in Frailty & Dementia Dr Ruth Ting Palliative Care Consultant Gateshead One Chance to get it right How people die remains in the memory of those who live on Dame Cicely Saunders
FRAILTY PATIENT FOCUS GROUP
 FRAILTY PATIENT FOCUS GROUP Community House, Bromley 28 November 2016-10am to 12noon In attendance: 7 Patient and Healthwatch representatives: 4 CCG representatives: Dr Ruchira Paranjape went through the
FRAILTY PATIENT FOCUS GROUP Community House, Bromley 28 November 2016-10am to 12noon In attendance: 7 Patient and Healthwatch representatives: 4 CCG representatives: Dr Ruchira Paranjape went through the
Invisible and in distress: prioritising the mental health of England's young carers
 Invisible and in distress: prioritising the mental health of England's young carers Foreword Becoming a carer can be daunting at any point in a person s life. Caring can take its toll on health and wellbeing.
Invisible and in distress: prioritising the mental health of England's young carers Foreword Becoming a carer can be daunting at any point in a person s life. Caring can take its toll on health and wellbeing.
QPR Suicide Prevention Training for Refugee Gatekeepers
 QPR Suicide Prevention Training for Refugee Gatekeepers 1 By the end of the training participants will be able to: Define suicide and describe how it is viewed within refugee communities. Identify risk
QPR Suicide Prevention Training for Refugee Gatekeepers 1 By the end of the training participants will be able to: Define suicide and describe how it is viewed within refugee communities. Identify risk
Deactivating the shock function of an implantable cardioverter defibrillator (ICD) towards the end of life
 Deactivating the shock function of an implantable cardioverter defibrillator (ICD) towards the end of life A guide for patients and carers This leaflet is for people who have an implantable cardiac defibrillator
Deactivating the shock function of an implantable cardioverter defibrillator (ICD) towards the end of life A guide for patients and carers This leaflet is for people who have an implantable cardiac defibrillator
Living Life with Persistent Pain. A guide to improving your quality of life, in spite of pain
 Living Life with Persistent Pain A guide to improving your quality of life, in spite of pain Contents What is Persistent Pain? 1 The Science Bit 2 Pain & Stress 3 Coping with Stress 4 The importance of
Living Life with Persistent Pain A guide to improving your quality of life, in spite of pain Contents What is Persistent Pain? 1 The Science Bit 2 Pain & Stress 3 Coping with Stress 4 The importance of
GP, Cognitive-behavioural. approach to heartsink patients. Dr Lee David. therapist
 A Cognitive-behavioural approach to heartsink patients Dr Lee David GP, Cognitive-behavioural therapist Aims of lecture Improve understanding of the nature of heartsink Overview of basic principles of
A Cognitive-behavioural approach to heartsink patients Dr Lee David GP, Cognitive-behavioural therapist Aims of lecture Improve understanding of the nature of heartsink Overview of basic principles of
We need to talk about Palliative Care. Parkinson s UK
 We need to talk about Palliative Care Parkinson s UK Introduction Parkinson s UK strongly welcomes the Committee s Inquiry, and hope that it will help to address inequalities in access to palliative and
We need to talk about Palliative Care Parkinson s UK Introduction Parkinson s UK strongly welcomes the Committee s Inquiry, and hope that it will help to address inequalities in access to palliative and
NHS SERVICES TO MEET YOUR NEEDS THE STANDARDS OF CARE YOU CAN EXPECT
 NHS SERVICES TO MEET YOUR NEEDS Meeting these unique needs requires special knowledge and skills, so NHS England has stated that there should be cancer services especially for teenagers and young adults
NHS SERVICES TO MEET YOUR NEEDS Meeting these unique needs requires special knowledge and skills, so NHS England has stated that there should be cancer services especially for teenagers and young adults
