White Paper. Primary Care and Sleep Apnea Testing: A Pilot Study for Home Testing with SleepView
|
|
|
- Ella Small
- 5 years ago
- Views:
Transcription
1 White Paper Primary Care and Sleep Apnea Testing: A Pilot Study for Home Testing with SleepView Thomas D. Schwieterman MD, Hani Kayyali, Kirk Scovill EXECUTIVE SUMMARY Obstructive sleep apnea (OSA) is a substantial health problem. Patients with OSA are at signifi cantly higher risk for developing hypertension, diabetes, heart disease, obesity and sudden death. Despite a high prevalence for OSA in all primary care practice populations, too few patients are screened for the disorder and fewer are tested. The gold standard and most common modality for achieving a diagnosis for OSA has traditonally been the in-lab polysomnogram (PSG). Yet, home sleep testing equipment and methodologies have been shown to be of comparable effi cacy, are lower cost and can be effectively administered by primary care physicians CleveMed Expanding the reach of your sleep services today and tomorrow 1
2 Background Every day, thousands of patients are seen in primary care offi ces for routine disease management visits for hypertension, diabetes, heart disease and obesity. To determine how the patient is doing, careful attention is given to the patient s laboratories and physical fi ndings. These indicators include the patient s systolic and diastolic blood pressure numbers, the current hemoglobin A1C levels, changes in cholesterol ratios or elevations in BMI. Optimizing these parameters continues to be the current standard of care for ensuring a favorable clinical outcome. But what about measuring the patient s RDI (respiratory disturbance index), a ratio used to assess severity of OSA? Like poorly controlled common metabolic indicators used for chronic disease management, an abnormally high RDI is strongly linked to adverse outcomes and progression to one or more of the major chronic diseases. It has been established that sufferers of sleep apnea have a 60% increased risk of developing heart failure, a 200% higher likelihood of developing a stroke, 300% increased chance of resistant hypertension and a dramatic 400% increased risk for developing atrial fi brillation. 2 Taken together, all-cause cardiovascular mortality is nearly twice as high for patients suffering from untreated moderate or severe sleep apnea. 2 OSA is a signifi cant health problem that too often goes unrecognized in primary care. Up to 90% of patients with signifi cant sleep apnea remain undiagnosed today. This is unfortunate since patients treated for OSA show lower rates of complications from the associated chronic diseases within the metabolic syndrome. Despite OSA being a largely undiagnosed problem, patients do admit to having problems with their sleep. A study done by James Mold from the University of Oklahoma Health Sciences Center showed that nearly 90% of all adult patients visiting a primary care clinic on any given day are actively experiencing sleep related symptoms. Yet, most fail to discuss their sleep-related symptoms with their physician and therefore are never evaluated for any sleep disorder. Nearly 1/3 of these unidentifi ed and untested patients are actually at high risk for sleep apnea. Studies suggest that a large percentage of high-risk patients will subsequently test positive for OSA in a diagnostic study. Today, patients of primary care physicians with clinically recognized symptoms of sleep apnea are most often sent to a sleep lab for evaluation. This method has proven to be an excellent work-up pathway for many years. Primary care clinicians know that while at the sleep lab, their patients will likely undergo a full diagnostic polysomnogram study (PSG). If the PSG is positive for OSA, their patients are often provided an immediate and appropriate treatment modality, such as continuous positive airway pressure therapy (CPAP). But, with the advent of home sleep testing (HST), is prescribing an in-lab PSG now necessary for the majority of primary care patients suspected of OSA? Could the primary care physician rather than Patients normally have an open airway during sleep, allowing respiration to occur freely. Onstructive sleep apnea occurs when the airway is repeatedly blocked by relaxed soft tissue in the throat and neck. the sleep specialist become the primary caregiver responsible for coordinating care including the diagnosis and treatment of routine sleep apnea? Primary care physicians are the primary caregivers for the other chronic disorders in the metabolic syndrome such as diabetes, hypertension and heart disease. It seems natural that OSA could be added to the list of conditions commonly managed by these front line providers. New technologies on the market for home sleep testing represent an attractive new option for diagnosing sleep apnea outside the sleep lab. Portable monitors designed for the home environment lower the complexity and costs for achieving a reliable diagnosis of OSA. The latest technologies are affordable and can now leverage the diagnostic support of sleep specialists using the Internet. This specialty-assisted model represents an attractive option that allows the primary care physician to take the role of the principal investigator and manager of OSA related conditions. In recent years, the technology utilized for assessing sleep apnea in the home has made remarkable advances. Some HST devices now fi t in the palm of one s hand. One of the most advanced devices on the market is the SleepView Monitor which is capable of simultaneously measuring seven independent sensor channels during sleep. When compared to the corresponding channels found in a full PSG study, the SleepView Monitor has been shown to exhibit a high diagnostic correlation for the key indicators of OSA. Developed by Cleveland Medical Devices Inc. (CleveMed), SleepView has been cleared by the FDA for home studies. SleepView was designed using the a b 2
3 guidelines provided by the American Academy of Sleep Medicine. Unlike many other devices, the SleepView system is integrated with an online service platform (portal) that adds valuable diagnostic functionality. Once the SleepView Monitor is connected to a portal-enabled computer, the clinician is supported with full test interpretation services. Within the secure HIPAA compliant webbased SleepView SM Portal, the ordering physician gains the advantage of remote test data validation and review by registered sleep technologists, a highly developed algorithm-assisted test scoring process, test interpretation services by board-certifi ed sleep physicians licensed in the state where the HST took place, online test setup and scheduling, and full study data management utilities. These services are aimed to support the primary care physician in the evaluation and management of patients with sleep disorders. HST as a preferred method for diagnosing OSA patients is growing. Improvements in accuracy and enhanced remote interpretive support methodologies have increased confi dence in HST as a viable alternative to in-lab PSG in many cases. Most of the major insurance carriers, including The Center for Medicare and Medicaid Services (CMS), have approved the use of HST within ambulatory care offi ces. Over time, many experts expect home sleep testing to become the most common method for evaluating sleep disordered breathing in low to moderate complexity patients. The advantages seen by payers include lower testing costs, improved patient convenience and improved patient access to reliable diagnostic studies. Enabling the primary care workforce to manage a broader spectrum of health conditions at lower costs to the system is also seen as a favorable outcome for HST. Insurers are also studying the effects widespread home sleep testing may have on reducing the number of patients suffering from major chronic diseases that can be triggered by untreated OSA. Patients with chronic diseases associated with chronic obstructive sleep apnea currently consume the majority of today s dollars. Testing the SleepView home sleep test in primary care offi ces To demonstrate effi cacy and effectiveness of the SleepView system for diagnosing OSA within a primary care setting, pilot programs were recently completed at four clinical sites. The test site physicians for the SleepView pilot included: Dr. Barrett Tilley of Medical Associates in Fremont, California Dr. Rodney Orr of Family Medical Group in Silverton, Oregon Dr. Stewart Segal of Lake Zurich Family Treatment Center near Chicago, Illinois Dr. Berto Zamora of Z&Z Medical Associates in Dallas, Texas The goal of establishing the reference accounts was to test three hypotheses regarding the integration of SleepView home sleep testing within primary care. The hypotheses were: 1. Patients are more willing to complete a home sleep study versus an in-lab polysomnogram. 2. The test is easy to administer for physicians and patients. Primary care physicians can effectively manage the entire testing process. Patients can effectively self-administer a home study with few test failures. 3. HST is effective as a standalone study for OSA disease management including, if necessary, direct CPAP titration without a follow-up PSG study. This paper examines the effectiveness of incorporating the SleepView HST monitor within primary care as an offi cebased diagnostic study for evaluating patients at-risk for OSA. Three hypotheses regarding integrating HST were tested in a SleepView pilot study conducted in
4 Methods The reference site physicians and their staff were not informed of these three hypotheses prior to the testing period. Rather, upon receiving a set of SleepView Monitors, each physician was simply asked to implement home sleep testing as part of their normal care delivery process. They were given training on the Epworth and STOP-BANG screening tests inventories that are commonly used to identify patients at-risk for OSA. Training was provided on using the SleepView Monitor, the secure SleepView SM Portal and method for providing patient instructions. Each account required just a few hours of training. A total of 60 studies were accomplished during the fi ve-month pilot study (see Table 1 below). Lake Zurich Silverton Fremont ZZ Medical Subjects (N) Gender (M,F) 14,4 8,12 11,1 9,1 Age (mean ± sd) 54.6 ± 14.2 yrs 49.2 ± 11 yrs 50.1 ± 11.1 yrs 51.5 ± 13.9 yrs BMI (mean ± sd) 30.1 ± ± ± ± 11.3 RDI (mean ± sd) 16.9 ± ± ± ± ESS (mean ± sd) 7 ± ± ± ± 6.5 Total rec. time (mean ± sd) 400 ± 120 min 410 ± 102 min 329 ± 107 min 353 ± 92.7 min Number of OSA positive Number of OSA negative Number of inconclusive HST Turnaround time for Specialist Report (avg.) 1.2 days 1.35 days 1.6 days 2.8 days Table 1: Summary of Reference Account HST Activity Results The results of the fi ve-month study demonstrated that the three hypotheses were confi rmed at all four test sites. We will discuss each hypothesis in more detail below. Hypothesis #1 Patients are more willing to participate in diagnostic study using HST as compared to in-lab PSG. Discussion Until recently, PSG was the only clinical test available to determine the presence, type, and severity of OSA. Yet, the practice of evaluating symptomatic patients via a sleep lab referral for a PSG study is problematic for many patients. It is anticipated that nearly 30% of patients scheduled for an in-lab polysomnogram fail to show up on the test night. Some refuse to go for cost reasons, others cite the inconvenience and still others may be in denial or choose not to go after the typical multi-week delay between test scheduling and PSG administration. Home sleep testing represents a new alternative for achieving a reliable diagnostic study that may mitigate some of these concerns. The fi rst hypothesis of the pilot project was to determine if primary care physicians could more effectively encourage their at-risk patient to have the home SleepView test over an in-lab PSG. Results for hypothesis #1 The four SleepView pilot sites demonstrated that a large majority of patients identifi ed as at-risk for OSA by their physicians were willing to complete a home study. For most of the physicians, this response differed from their past experiences of referring patients for in-lab PSG. Simply stated, arranging a home sleep study was an easier task than convincing patients to go to the sleep lab. The reasons cited by the physicians for increased patient willingness to conduct an HST over PSG can be summarized in three areas signifi cant cost savings for the patient, added convenience of testing at home, and immediate testing capability of HST (versus waiting several weeks for an in-lab PSG). 4
5 Dr. Orr and his colleagues commented that the cost savings found with HST over PSG was especially important in achieving a sleep diagnostic study on their patients. Dr. Orr s office completed 20 studies during their pilot. Several in the home study cohort had previously refused an in-lab PSG. According to Dr. Orr, The simple convenience of HST takes a backseat to the affordability of diagnostic testing. The physician s ability to order a home sleep study on the very night of the office visit proved to be a valuable asset. With the ability to achieve a diagnostic study immediately after identifying an at-risk individual, more patients agreed to be tested. As stated by Dr. Segal, The simple words, we can test you tonight at your own home as opposed to we can test you in two weeks at the sleep lab proved to be highly influential in getting the patients to agree to a test. He continued, When I said those words about having the test done immediately and at home, fewer patients objected. All the physicians found their existing and ongoing relationship was a useful asset for encouraging home testing. All the physicians felt that having the diagnostic study available within their office, as compared to the less familiar sleep lab, lowered the resistance to completing a study. Dr. Tilley noted, The biggest advantage with the SleepView program is that I have another way to gain important clinical information on my patients right from my office. My patients gain because they learn of their clinical situation regarding sleep apnea from the person they have a trusting relationship with their primary care physician. In general, the experience of our physicians verified that achieving a diagnostic study for OSA was improved by the incorporation of SleepView into their care delivery process. None of the physicians encountered much resistance by their patients when asked to directly participate with a self-administered monitor at home. While anecdotal, we believe the pilot supported the hypothesis that HST with SleepView markedly improved patients participation in OSA evaluation when compared to in-lab PSG. Hypothesis #2 (Part 1) The test is easy to administer for physicians and patients. Part 1- The physicians can effectively manage the testing process. Discussion Unlike existing medical devices used in their primary care settings, the SleepView had features and a workflow that were initially unfamiliar to the pilot physicians and office staff. Most medical devices in the market today (such as the ECG, spirometer, and Holter monitor) utilize an internal computer algorithm that produces an immediate diagnostic report after the sensor data is acquired. The SleepView device employs a new and more rigorous process for analyzing the sensor data. Rather than relying on an isolated algorithm resident in the device or on the attached computer, SleepView incorporates an online portal system that extends the diagnostics process to remotely situated sleep specialists. With SleepView, registered sleep technologist scoring and boardcertified physician interpretation is provided for every study. This virtualized support mechanism is unlike any other office-based study our physicians had previously encountered. When the patient completes a test, the monitor is returned to the physician s office where the data is uploaded to a secure SleepView SM Portal. A registered sleep technologist reviews the multiple sensor waveforms and validates the quality and length of every overnight study. If deemed scoreable a preliminary report is generated with the help of a sophisticated scoring algorithm. This report is forwarded to an in-state board-certified sleep physician for final review. The physician reviews the waveform data and records an official electronically signed diagnosis within the portal. This final report is then sent to the primary care physician for review with the patient. This Internet-enabled workflow for SleepView required new skills for the pilot physicians. As a result, it was necessary to test how well such a process could be integrated within the routine of a typical medical office. Would the process prove to be overly cumbersome? How difficult was it to transfer the monitor data to the portal system? Results for hypothesis #2 (Part 1) The results of the pilot demonstrated that all the sites became quickly adept at managing the new device data workflow requirements. Each of the four offices had little difficulty ordering tests online, setting up their monitors for each patient study and downloading completed reports from the SleepView SM Portal. Most physicians found the process to be easy to follow and quite effective. In fact, several physicians commented that the portal is one of the best features of the SleepView system. One physician commented It was like getting a sleep physician consult without having to send the patient. Another commented on the high confidence he experienced regarding the diagnostic credibility and reliability of the process. During the pilot, the four pilot sites completed a total of 60 studies (Table 1), all of which utilized the process described above. The studies were uploaded to the portal were scored and interpreted within the SleepView system. Results show that only 2 out of 60 studies (3.3%) were inconclusive and required an-lab PSG for confirmation (80% positive OSA, 16.7% negative OSA). The average turnaround from time of data upload to when the primary care physician received a final report was between 1.2 and 2.8 days for each office. The pilot confirmed that the physicians and their staff had little difficulty with the workflow requirements of SleepView and were pleased with the turnaround time and diagnostic expert support provided by the portal. 5
6 Hypothesis #2 (Part 2) The test is easy to administer for physicians and patients. Part 2- Patients can effectively self-administer their home study with few test failures. Discussion During an in-lab polysomogram, a staff of sleep technicians manage the sensor hook-up and monitor the nighttime study. The staff corrects any test-related issues that arise during the overnight recording period. With home sleep testing, these tasks are left for the patient to administer. While SleepView is certainly less complicated than a PSG, it was important to verify that patients were able to successfully complete a diagnostic SleepView study without direct supervision by medical staff. Results for hypothesis #2 (Part 2) A total of 67 studies were conducted; 60 scorable studies (89.6%) and 7 unscoreable studies (10.4%). Studies deemed scoreable were often due to sensor misplacement. However, it is clear that the number of test failures diminished greatly after the first four studies were completed. We attribute this significant improvement in performance of SleepView to better familiarity with the equipment and enhanced training techniques employed for patients. The failure rate for tests completed after the initial 4 studies was just 7.8% (Table 2). Pilot Site With over 92% of patients achieving successful studies at the end of the reference account study period, we determined that patient directed home sleep testing with SleepView is a valid and reliable diagnostic modality for OSA. For the two reference accounts where the most studies were performed (Lake Zurich and Silverton), the failure rate after the first 4 tests dropped to 3.1%. There were no failures during the last four studies of the pilot. Hypothesis #3 Total Test Failed tests first 4 patients Failed tests thereafter Lake Zurich 18 0 (0%) 1 (6.7%) ZZ Medical 12 1 (25%) 1 (12.5%) Fremont 15 1 (25%) 2 (18.2%) Silverton 21 1 (25%) 0 (0%) TOTAL 67 3 (18.8%) 4 (7.8%) Table 2: Test Failure Data HST is effective as a standalone study for OSA disease management including, if necessary, direct CPAP titration without a follow-up PSG study. Discussion An issue raised about home sleep studies in the past has been the concern that the clinical data generated from a patient selfadministered test would be insufficient to impact therapeutic decisions. If each patient found to have OSA on HST requires a subsequent PSG to confirm the diagnosis, its value as a cost saving and effective diagnostic tool would be marginalized. A goal of the pilot study was to determine if a patient diagnosed with OSA on HST could be effectively managed and treated without the frequent requirement of a follow-up in-lab PSG evaluation. Results for hypothesis #3 The results demonstrated that HST is an effective diagnostic modality for clinical decision-making, including the initiation of CPAP (Continuous Positive Airway Pressure) therapy. As mentioned before, the majority of tests (80%) performed at the pilot sites confirmed the presence of OSA, 16.7% negative and only 3.3% that required a repeat in-lab evaluation. The pilot clearly demonstrated that the vast majority of HST studies were of sufficient quality for full clinical decision making without the need for repeat in-lab testing. Therapy Number Percentage CPAP Titration % Lifestyle/Obesity Management % Oral Appliance Therapy 3 6.3% Referral to ENT Specialist 3 6.3% Referral to Sleep Lab 1 2.1% No Therapy 4 8.3% Unknown/Undisclosed % Table 4: Therapeutic Choice Summary * CPAP Titrations done at local sleep labs The physicians diagnosed a total of 48 patients with OSA during the pilot study. About half were subsequently prescribed CPAP therapy (see Table 4). All the patients receiving CPAP were referred to their local sleep lab for titration. This decision was an independent choice by each provider. No therapeutic guidance was provided by the study organizers. 12 percent were provided primary care directed weight loss and lifestyle modification counseling while 8 percent were referred to specialists for additional care. This included one referral for tonsillectomy. The capability of initiating CPAP therapy directly from HST without a subsequent in-lab PSG can lower the overall cost of care for patients. Exact reimbursement payments for this pilot are not available; however, if one uses CMS national average reimbursement rates, the pilot would demonstrate at 70.4% reduction in diagnostic testing costs to the patient and insurer. This amounted to $29,334 savings for the near 60 patients tested (see Table 5). The efficiency gains and cost savings of HST over PSG in this pilot study were key findings of the SleepView pilot. With recent studies indicating a similar outcome for patients treated with Automatic 6
7 PAP (APAP) machine versus conventional CPAP, the cost savings for therapy would be even greater had the patients in this study progressed directly to APAP therapy as opposed to in-lab CPAP titration. Venue - Traditional diagnosis Cost per Test (CMS national rate) Number of Studies Total Expenses Sleep Lab PSG $ $ Venue - HST Cost per Test (CMS national rate) Number of Studies Total Expense SleepView HST $ $ Inconclusive HST that require $ $1,388 in-lab PSG TOTAL 0 0 $12,314 Total Savings $29,334 Percentage Savings 70.4% Table 5: Cost Savings Analysis chose to counsel his patients on the signifi cance and meaning of the test results before he began discussing or initiating any type of therapy. He informed them of their many options, including weight loss, oral appliance therapy or CPAP. His more severe OSA patients, those who were unlikely to benefi t from conservative treatment, were immediately directed towards the sleep lab for initiation of CPAP therapy. Most of the study physicians were pleased to fi nd that their local sleep lab was willing to proceed to CPAP titration from the HST data without requiring the patient undergo second PSG study. With such success by our pilot physicians for managing the posttest therapy for OSA, it was determined that SleepView is a reliable and accurate monitor suitable for driving therapeutic choices within the PCP practice. The concern that many patients would require subsequent PSG evaluations before therapy was mitigated by the study outcomes. These primary care physicians also demonstrated that the diagnosis and management of OSA is a natural extension of their practice and is synergistic to the management of other diseases within the metabolic syndrome. In addition to CPAP therapy, the primary care physicians in the study found that sleep diagnostics using SleepView was a natural fi t within their comprehensive chronic disease management programs. While CPAP therapy was the therapy of choice for many of the patients diagnosed with OSA, on several occasions the physicians preferred less invasive therapies such as referral to ENT for oral surgery consideration, referral to a dentist for oral appliance fi tting or weight loss and exercise programs. The breadth of therapy options exercised by the PCP in our pilot confi rms the successful role of the PCP as a care coordinator for OSA management. The physicians in the pilot program found that their interventions for newly diagnosed OSA were synergistic with their treatments for other chronic diseases, such as diabetes and hypertension. Perhaps the most illustrative reference account for the successful incorporation of OSA management within primary care was found with Dr. Tilley. He found managing OSA within primary care to be a natural extension of his practice. Dr. Tilley, I know my patients lifestyle issues, their problems, and support systems and can therefore make a more signifi cant impact on initiating a best therapeutic approach one tailored for each patient. Many times, this involves a weight loss program, something I frequently use with my diabetic and hypertensive patients. With the family physician involved in home sleep testing, he argued that the patient benefi ts greatly by having a consistent and cost effective management plan for all their conditions. He continued, I see OSA as being analogous to those other disorders; that is why family docs need to be doing this. Once diagnosed with OSA using SleepView, Dr. Tilley found that his management of the patient was improved as compared to his previous experiences following referrals to the local sleep lab. Instead of immediately resorting to therapy with CPAP, Dr. Tilley Conclusion The proven association of OSA with the disorders of the metabolic syndrome, sudden cardiac death, and motor vehicle accidents makes this disorder a serious health concern. With up to 90% of OSA patients remaining undiagnosed today, improvements are urgently needed in identifying and formally diagnosing those at risk. After reviewing the results of this pilot study, we feel that home sleep testing with SleepView is a step in the right direction towards improving patient care related to sleep apnea. Our study has found that patients are easier to convince to undergo a sleep study and are thus are more likely to be tested. With 93% successful studies in hand, it was shown that patients can also effectively self-administer the at-home testing process. Physicians and their staff have also demonstrated profi ciency in implementing SleepView into their care delivery and were fully capable of managing the data and workfl ow found within the SleepView SM Portal. In addition, the remarkable success achieved we observed in our primary care physicians prescribing therapy directly from a home study provides solid evidence that SleepView is a reliable and accurate diagnostic solution. The pilot also demonstrated signifi cant cost advantages to the healthcare system with 70% lower diagnostic costs of care for patients found to have OSA. We also found that sleep apnea diagnostics and management is a natural extension of the existing primary care disease management programs, especially for those disorders found within the metabolic syndrome such as diabetes, hypertension, obesity and heart disease. Yet, as we conclude, it is important to note that sleep labs continue to 7
8 have an extremely important role in the overall management of OSA, even those that are diagnosed within a primary care setting. Many patients, diagnosed by their primary care physician with moderate to severe apnea on HST, require referral to sleep specialists for initiation of CPAP therapy. In many cases in this pilot study, the SleepView patients who required CPAP were sent to a local sleep lab for initiation of their therapy. Thus, the incorporation of home sleep testing in the primary care setting, while reliably diagnostic and cost effective, still requires tertiary sleep lab support in many ways. The incorporation of HST within primary care should be viewed not as a replacement for sleep lab but rather as an efficient and effective ancillary method for diagnosing and initiating care management for sleep disorders. Perhaps enabling our primary care physicians with the new capabilities afforded by SleepView, more patients will receive the care they need and reduce their risks for other chronic disease states. End Notes 1Redline S. et al. Obstructive Sleep Apnea Hypopnea and Incident Stroke: The Sleep Health Heart Study. Am Journal of Respiratory & Critical Care Medicine, 2010; 182(2): Epub 2010, Mar 25. 2Young T, et al. Sleep Disordered Breathing and Mortality: Eighteen-Year Follow-up of the Wisconsin Sleep Cohort. Sleep 2008; 31(): Demede, M. et al. Resistant Hypertension and Obstructive Sleep Apnea in the Primary Care Setting. International Journal of Hypertension, 2011; Article ID , Mar 28. 4Young T. et al. Estimation of the clinically diagnosed proportion of sleep apnea syndrome in middle-aged men and women. Sleep, 1997; 20: Buchner N.J. et al. Continuous Positive Airway Pressure Treatment of Mild to Moderate Sleep Apnea Reduces Cardiovascular Risk. American Journal of Respiratory and Critical Care Medicine, 2007; 176(12): Martin J.M. et al. Long-term cardiovascular outcomes in men with obstructive sleep apnea-hypopnea with or without treatment with CPAP: an observational study. Lancet 2005; 365(9484): Becker H.F. et al. Effect of Nasal CPAP Treatment on Blood Pressure Patients with Obstructive Sleep Apnea. Circulation, 2003; 107(1): Mold J.W. et al. Identification by Primary Care Clinicians of Patients with Obstructive Sleep Apnea: A practice-based research network study. Journal of the American Board of Family Medicine; 2011, Vol 24 No. 2, , March 9Foldvary-Schaefer N. et al. Accuracy of Automated Respiratory Scoring Algorithm Using Portable Monitoring; 2011, poster presentation. 10Hossain J.L. et al. The Prevalence, Cost Implications, and Management of Sleep Disorders: An Overview. Sleep and Breathing, 2002; Vol 6 No 2; Skomro R.P. et al. Outcomes of Home-Based Diagnosis and Treatment of Obstructive Sleep Apnea. Chest, August, 2010, Vol 138 no CLEVEMED Expanding the reach of your sleep services today and tomorrow 8
sleepview by midmark Home Sleep Test
 sleepview by midmark HST Home Sleep Test Introducing SleepView. Better for your patients, designed for your practice. Home sleep testing (HST) brings the diagnosis and management of OSA to the front lines
sleepview by midmark HST Home Sleep Test Introducing SleepView. Better for your patients, designed for your practice. Home sleep testing (HST) brings the diagnosis and management of OSA to the front lines
Web-Based Home Sleep Testing
 Editorial Web-Based Home Sleep Testing Authors: Matthew Tarler, Ph.D., Sarah Weimer, Craig Frederick, Michael Papsidero M.D., Hani Kayyali Abstract: Study Objective: To assess the feasibility and accuracy
Editorial Web-Based Home Sleep Testing Authors: Matthew Tarler, Ph.D., Sarah Weimer, Craig Frederick, Michael Papsidero M.D., Hani Kayyali Abstract: Study Objective: To assess the feasibility and accuracy
About VirtuOx. Was marketed exclusively by Phillips Healthcare division, Respironics for 3 years
 About VirtuOx VirtuOx, Inc. assists physicians and Durable Medical Equipment (DME)( companies diagnose respiratory diseases and qualify patients for home respiratory equipment under the guidelines of CMS
About VirtuOx VirtuOx, Inc. assists physicians and Durable Medical Equipment (DME)( companies diagnose respiratory diseases and qualify patients for home respiratory equipment under the guidelines of CMS
ASK US. A Study for Obstructive Sleep Apnea Patients Using a New At-Home Sleep Test ARE YOU ABOUT THE STUDY #
 #15420040.0 A Study for Obstructive Sleep Apnea Patients Using a New At-Home Sleep Test STUDY DENTIST Dr. Michael Simmons DMD, MSc ARE YOU Struggling with or given up on CPAP and don t know what to do?
#15420040.0 A Study for Obstructive Sleep Apnea Patients Using a New At-Home Sleep Test STUDY DENTIST Dr. Michael Simmons DMD, MSc ARE YOU Struggling with or given up on CPAP and don t know what to do?
Obstructive Sleep Apnea Syndrome. Common sleep disorder causes high blood pressure and heart attacks
 Obstructive Sleep Apnea Syndrome Common sleep disorder causes high blood pressure and heart attacks Message: Sleep apnea is very common. It is estimated that 158 million people worldwide suffer from sleep
Obstructive Sleep Apnea Syndrome Common sleep disorder causes high blood pressure and heart attacks Message: Sleep apnea is very common. It is estimated that 158 million people worldwide suffer from sleep
WHAT YOU NEED TO KNOW ABOUT SLEEP APNEA
 WHAT YOU NEED TO KNOW ABOUT SLEEP APNEA Wayne Driscoll Clinical Education Specialist 2 SLEEP APNEA IN THE NEWS Carrie Fisher died from sleep apnea, other factors, coroner says USA Today NJ Transit engineer
WHAT YOU NEED TO KNOW ABOUT SLEEP APNEA Wayne Driscoll Clinical Education Specialist 2 SLEEP APNEA IN THE NEWS Carrie Fisher died from sleep apnea, other factors, coroner says USA Today NJ Transit engineer
Hattie Perry, RN, RPSGT Intermountain Sleep Disorder Centers
 Hattie Perry, RN, RPSGT Intermountain Sleep Disorder Centers Not screened for OSA symptoms during PCP visits Not referred by PCP Patient unaware of symptoms or accepts symptoms as normal. Cost of testing
Hattie Perry, RN, RPSGT Intermountain Sleep Disorder Centers Not screened for OSA symptoms during PCP visits Not referred by PCP Patient unaware of symptoms or accepts symptoms as normal. Cost of testing
Sleep 101. Kathleen Feeney RPSGT, RST, CSE Business Development Specialist
 Sleep 101 Kathleen Feeney RPSGT, RST, CSE Business Development Specialist 2016 Why is Sleep Important More than one-third of the population has trouble sleeping (Gallup) Obstructive Sleep Apnea Untreated
Sleep 101 Kathleen Feeney RPSGT, RST, CSE Business Development Specialist 2016 Why is Sleep Important More than one-third of the population has trouble sleeping (Gallup) Obstructive Sleep Apnea Untreated
RESEARCH PACKET DENTAL SLEEP MEDICINE
 RESEARCH PACKET DENTAL SLEEP MEDICINE American Academy of Dental Sleep Medicine Dental Sleep Medicine Research Packet Page 1 Table of Contents Research: Oral Appliance Therapy vs. Continuous Positive Airway
RESEARCH PACKET DENTAL SLEEP MEDICINE American Academy of Dental Sleep Medicine Dental Sleep Medicine Research Packet Page 1 Table of Contents Research: Oral Appliance Therapy vs. Continuous Positive Airway
Introducing the WatchPAT 200 # 1 Home Sleep Study Device
 Introducing the WatchPAT 200 # 1 Home Sleep Study Device Top 10 Medical Innovation for 2010 Cleveland Clinic Fidelis Diagnostics & Itamar Medical Fidelis Diagnostics founded in 2004, is a privately-held
Introducing the WatchPAT 200 # 1 Home Sleep Study Device Top 10 Medical Innovation for 2010 Cleveland Clinic Fidelis Diagnostics & Itamar Medical Fidelis Diagnostics founded in 2004, is a privately-held
In-Patient Sleep Testing/Management Boaz Markewitz, MD
 In-Patient Sleep Testing/Management Boaz Markewitz, MD Objectives: Discuss inpatient sleep programs and if they provide a benefit to patients and sleep centers Identify things needed to be considered when
In-Patient Sleep Testing/Management Boaz Markewitz, MD Objectives: Discuss inpatient sleep programs and if they provide a benefit to patients and sleep centers Identify things needed to be considered when
Health Provider Partnerships for OSA Management in Transportation. Paul S. Valentine Chief Executive Officer Sleep HealthCenters LLC
 Health Provider Partnerships for OSA Management in Transportation Paul S. Valentine Chief Executive Officer Sleep HealthCenters LLC Sleep Apnea & Multi-Modal Transportation Conference November 2011 Programs
Health Provider Partnerships for OSA Management in Transportation Paul S. Valentine Chief Executive Officer Sleep HealthCenters LLC Sleep Apnea & Multi-Modal Transportation Conference November 2011 Programs
Total Sleep Solution. Growing Cardiac Sleep Health Management. Together. Health Being Made Simple
 Total Sleep Solution Growing Cardiac Sleep Health Management. Together. Health Being Made Simple Total Sleep Solution Sleep Apnea Management Improves Cardiac Health and Therapy Efficacy Sleep Apnea is
Total Sleep Solution Growing Cardiac Sleep Health Management. Together. Health Being Made Simple Total Sleep Solution Sleep Apnea Management Improves Cardiac Health and Therapy Efficacy Sleep Apnea is
Your Path Starts Here
 spring fall 2014 2014 Your Path Starts Here Our Wellness Portal is the perfect place to begin living healthier - Is sleep apnea hurting your health? - Call for 24/7 advice from a nurse - Optional dental
spring fall 2014 2014 Your Path Starts Here Our Wellness Portal is the perfect place to begin living healthier - Is sleep apnea hurting your health? - Call for 24/7 advice from a nurse - Optional dental
SleepView. SleepView. Monitor + SleepViewSM. Portal Clinical Validation Summary. CliniCal validation
 CliniCal validation Monitor + SM Portal Clinical Validation Summary 2007 AASM established guidelines for proper Portable Monitoring (PM) methodology to be used in home sleep apnea diagnosis Clinical Guidelines
CliniCal validation Monitor + SM Portal Clinical Validation Summary 2007 AASM established guidelines for proper Portable Monitoring (PM) methodology to be used in home sleep apnea diagnosis Clinical Guidelines
TOPIC: Continuing Coverage of CPAP Machines and Supplies for the Treatment of Obstructive Sleep Apnea
 These documents are not used to determine benefits or reimbursement. Please reference the appropriate certificate or contract for benefit information. BLUE CROSS BLUE SHIELD of MI MEDICAL POLICY Enterprise:
These documents are not used to determine benefits or reimbursement. Please reference the appropriate certificate or contract for benefit information. BLUE CROSS BLUE SHIELD of MI MEDICAL POLICY Enterprise:
Obstructive sleep apnoea How to identify?
 Obstructive sleep apnoea How to identify? Walter McNicholas MD Newman Professor in Medicine, St. Vincent s University Hospital, University College Dublin, Ireland. Potential conflict of interest None Obstructive
Obstructive sleep apnoea How to identify? Walter McNicholas MD Newman Professor in Medicine, St. Vincent s University Hospital, University College Dublin, Ireland. Potential conflict of interest None Obstructive
TESTIMONY OF JOHN RISCH NATIONAL LEGISLATIVE DIRECTOR SMART TRANSPORTATION DIVISION BEFORE THE FEDERAL MOTOR CARRIER SAFETY ADMINSTRATION
 TESTIMONY OF JOHN RISCH NATIONAL LEGISLATIVE DIRECTOR SMART TRANSPORTATION DIVISION BEFORE THE FEDERAL MOTOR CARRIER SAFETY ADMINSTRATION AND FEDERAL RAILROAD ADMINISTRATION Public Listening Sessions on
TESTIMONY OF JOHN RISCH NATIONAL LEGISLATIVE DIRECTOR SMART TRANSPORTATION DIVISION BEFORE THE FEDERAL MOTOR CARRIER SAFETY ADMINSTRATION AND FEDERAL RAILROAD ADMINISTRATION Public Listening Sessions on
DECLARATION OF CONFLICT OF INTEREST
 DECLARATION OF CONFLICT OF INTEREST Obstructive sleep apnoea How to identify? Walter McNicholas MD Newman Professor in Medicine, St. Vincent s University Hospital, University College Dublin, Ireland. Potential
DECLARATION OF CONFLICT OF INTEREST Obstructive sleep apnoea How to identify? Walter McNicholas MD Newman Professor in Medicine, St. Vincent s University Hospital, University College Dublin, Ireland. Potential
Clinical Trials in OSA
 24th ANNUAL ADVANCES IN SLEEP APNEA AND SNORING February 16-17, 2018 Grand Hyatt on Union Square San Francisco, California Clinical Trials in OSA Samuel T. Kuna, MD Department of Medicine Center for Sleep
24th ANNUAL ADVANCES IN SLEEP APNEA AND SNORING February 16-17, 2018 Grand Hyatt on Union Square San Francisco, California Clinical Trials in OSA Samuel T. Kuna, MD Department of Medicine Center for Sleep
A New, Clinically Proven Sleep Apnea Therapy for people unable to use CPAP.
 A New, Clinically Proven Sleep Apnea Therapy for people unable to use CPAP. Take Heart. If You Have OSA, You re Not Alone. Like you, more than 18 million Americans are estimated to have Obstructive Sleep
A New, Clinically Proven Sleep Apnea Therapy for people unable to use CPAP. Take Heart. If You Have OSA, You re Not Alone. Like you, more than 18 million Americans are estimated to have Obstructive Sleep
Oral Appliances for Obstructive Sleep Apnea Response to Comments
 Oral Appliances for Obstructive Sleep Apnea Response to Comments November 11, 2010 1. There are no randomized, controlled crossover trials that show efficacy of any prefabricated oral appliance. As the
Oral Appliances for Obstructive Sleep Apnea Response to Comments November 11, 2010 1. There are no randomized, controlled crossover trials that show efficacy of any prefabricated oral appliance. As the
3/13/2014. Home Sweet Home? New Trends in Testing for Obstructive Sleep Apnea. Disclosures. No relevant financial disclosures
 2014 Big Sky Pulmonary Conference Home Sweet Home? New Trends in Testing for Obstructive Sleep Apnea Eric Olson, MD Associate Professor of Medicine Co-Director, Center for Sleep Medicine Mayo Clinic olson.eric@mayo.edu
2014 Big Sky Pulmonary Conference Home Sweet Home? New Trends in Testing for Obstructive Sleep Apnea Eric Olson, MD Associate Professor of Medicine Co-Director, Center for Sleep Medicine Mayo Clinic olson.eric@mayo.edu
QUESTIONS FOR DELIBERATION
 New England Comparative Effectiveness Public Advisory Council Public Meeting Hartford, Connecticut Diagnosis and Treatment of Obstructive Sleep Apnea in Adults December 6, 2012 UPDATED: November 28, 2012
New England Comparative Effectiveness Public Advisory Council Public Meeting Hartford, Connecticut Diagnosis and Treatment of Obstructive Sleep Apnea in Adults December 6, 2012 UPDATED: November 28, 2012
Positive Airway Pressure (PAP) Devices Physician Frequently Asked Questions December 2008
 Positive Airway Pressure (PAP) Devices Physician Frequently Asked Questions December 2008 Based on questions received from the clinical community, the following Frequently Asked Questions will address
Positive Airway Pressure (PAP) Devices Physician Frequently Asked Questions December 2008 Based on questions received from the clinical community, the following Frequently Asked Questions will address
Selecting the Right Patients for Oral Appliance Therapy
 Selecting the Right Patients for Oral Appliance Therapy AN OVERVIEW OF THE IN-LAB MATRx TITRATION SYSTEM Oral Appliance Titration Made Simple Confidently Prescribe Oral Appliance Therapy The ONLY validated
Selecting the Right Patients for Oral Appliance Therapy AN OVERVIEW OF THE IN-LAB MATRx TITRATION SYSTEM Oral Appliance Titration Made Simple Confidently Prescribe Oral Appliance Therapy The ONLY validated
Rediscover the power of sleep
 Rediscover the power of sleep Patient Copy Apnea solutions for all ages Mobile Sleep Services Who We Are An experienced and well trained team of sleep care professionals consisting of Registered Sleep
Rediscover the power of sleep Patient Copy Apnea solutions for all ages Mobile Sleep Services Who We Are An experienced and well trained team of sleep care professionals consisting of Registered Sleep
Dental Sleep Medicine Basics
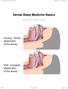 Dental Sleep Medicine Basics Written By: Patrick Tessier 2018 www.tap.wiki/ Page 1 of 8 INTRODUCTION Here are some basic aspect of Dental Sleep Medicine. This viewpoint is from an industry participant,
Dental Sleep Medicine Basics Written By: Patrick Tessier 2018 www.tap.wiki/ Page 1 of 8 INTRODUCTION Here are some basic aspect of Dental Sleep Medicine. This viewpoint is from an industry participant,
Simple diagnostic tools for the Screening of Sleep Apnea in subjects with high risk of cardiovascular disease
 Cardiovascular diseases remain the number one cause of death worldwide Simple diagnostic tools for the Screening of Sleep Apnea in subjects with high risk of cardiovascular disease Shaoguang Huang MD Department
Cardiovascular diseases remain the number one cause of death worldwide Simple diagnostic tools for the Screening of Sleep Apnea in subjects with high risk of cardiovascular disease Shaoguang Huang MD Department
ROBERT C. PRITCHARD DIRECTOR MICHAEL O. FOSTER ASSISTANT DIR. SLEEP APNEA
 ROBERT C. PRITCHARD DIRECTOR MICHAEL O. FOSTER ASSISTANT DIR. SLEEP APNEA A Person is physically qualified to drive a motor vehicle if that person; -(5) has no established medical history or clinical diagnosis
ROBERT C. PRITCHARD DIRECTOR MICHAEL O. FOSTER ASSISTANT DIR. SLEEP APNEA A Person is physically qualified to drive a motor vehicle if that person; -(5) has no established medical history or clinical diagnosis
Itamar Medical. December Investors Presentation.
 Itamar Medical December 2017. Investors Presentation. Disclaimer Itamar Medical Ltd. (the "Company") is furnishing this presentation and any information given during this presentation, solely for the consideration
Itamar Medical December 2017. Investors Presentation. Disclaimer Itamar Medical Ltd. (the "Company") is furnishing this presentation and any information given during this presentation, solely for the consideration
Inspire Therapy for Sleep Apnea
 Inspire Therapy for Sleep Apnea Take Heart. If you have OSA, you re not alone. More than 18 million Americans are estimated to have Obstructive Sleep Apnea (OSA). OSA occurs when the tongue and other soft
Inspire Therapy for Sleep Apnea Take Heart. If you have OSA, you re not alone. More than 18 million Americans are estimated to have Obstructive Sleep Apnea (OSA). OSA occurs when the tongue and other soft
Medicare CPAP/BIPAP Coverage Criteria
 Medicare CPAP/BIPAP Coverage Criteria For any item to be covered by Medicare, it must 1) be eligible for a defined Medicare benefit category, 2) be reasonable and necessary for the diagnosis or treatment
Medicare CPAP/BIPAP Coverage Criteria For any item to be covered by Medicare, it must 1) be eligible for a defined Medicare benefit category, 2) be reasonable and necessary for the diagnosis or treatment
CERT PAP Errors: The DME CERT Outreach and Education Task Force Responds
 CERT PAP Errors: The DME CERT Outreach and Education Task Force Responds DME CERT Outreach and Education Task Force National PAP Webinar, December 17, 2014 PAP CERT Errors Medical Records: Face-to-Face
CERT PAP Errors: The DME CERT Outreach and Education Task Force Responds DME CERT Outreach and Education Task Force National PAP Webinar, December 17, 2014 PAP CERT Errors Medical Records: Face-to-Face
CARDIOVIT CS-200 Excellence. Designed for high-volume workload, equipped with the latest technology to save time and boost productivity
 CARDIOVIT CS-200 Excellence Designed for high-volume workload, equipped with the latest technology to save time and boost productivity CARDIOVIT CS-200 EXCELLENCE Experience the CARDIOVIT CS-200 Excellence
CARDIOVIT CS-200 Excellence Designed for high-volume workload, equipped with the latest technology to save time and boost productivity CARDIOVIT CS-200 EXCELLENCE Experience the CARDIOVIT CS-200 Excellence
Learning Objectives. And it s getting worse. The Big Picture. Dr. Roger Roubal
 Learning Objectives How to screen for sleep apnea; questions to ask your patients Industry treatment guidelines; when to consider an oral appliance vs. a CPAP What goals/thresholds to set for successful
Learning Objectives How to screen for sleep apnea; questions to ask your patients Industry treatment guidelines; when to consider an oral appliance vs. a CPAP What goals/thresholds to set for successful
PORTABLE OR HOME SLEEP STUDIES FOR ADULT PATIENTS:
 Sleep Studies: Attended Polysomnography and Portable Polysomnography Tests, Multiple Sleep Latency Testing and Maintenance of Wakefulness Testing MP9132 Covered Service: Prior Authorization Required: Additional
Sleep Studies: Attended Polysomnography and Portable Polysomnography Tests, Multiple Sleep Latency Testing and Maintenance of Wakefulness Testing MP9132 Covered Service: Prior Authorization Required: Additional
Is the population appropriate? Population: Groups that will be covered: Are there any specific subgroups that have not been mentioned?
 Sleep Disordered Breathing scope: stakeholder subgroup discussions Date: Thursday 12 April 2018 Group: 2 Population: Groups that will be covered: Adults (18 and older) with obstructive sleep apnoea/hypopnoea
Sleep Disordered Breathing scope: stakeholder subgroup discussions Date: Thursday 12 April 2018 Group: 2 Population: Groups that will be covered: Adults (18 and older) with obstructive sleep apnoea/hypopnoea
Care for Patients Wherever They Are, Wherever You Are.
 Care for Patients Wherever They Are, Wherever You Are. Patients want the latest healthcare technology with the least impact on their daily lives. The AliveCor System helps you to partner with your patients
Care for Patients Wherever They Are, Wherever You Are. Patients want the latest healthcare technology with the least impact on their daily lives. The AliveCor System helps you to partner with your patients
WINDSOR DENTAL CARE 2224 WALKER ROAD SUITE 20 WINDSOR, ON N8W 5L7 PHONE FAX
 The quality of your sleep can impact you emotionally, physically and your overall general health. Poor sleep can cause chronic fatigue, daytime drowsiness, irritability and loss of focus. It affects your
The quality of your sleep can impact you emotionally, physically and your overall general health. Poor sleep can cause chronic fatigue, daytime drowsiness, irritability and loss of focus. It affects your
Works Cited 1. A Quantitative Assessment of Sleep Laboratory Activity in the United States. Tachibana N, Ayas NT, White DP. 2005, J Clin Sleep Med,
 Testimony Before the Medicare Evidence and Development and Coverage Advisory Committee (MedCAC) on its National Coverage Determination Continuous Positive Airway Pressure for Obstructive Sleep Apnea Wednesday,
Testimony Before the Medicare Evidence and Development and Coverage Advisory Committee (MedCAC) on its National Coverage Determination Continuous Positive Airway Pressure for Obstructive Sleep Apnea Wednesday,
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Process
 Quality ID #277: Sleep Apnea: Severity Assessment at Initial Diagnosis National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Management of Chronic Conditions 2019 COLLECTION
Quality ID #277: Sleep Apnea: Severity Assessment at Initial Diagnosis National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Management of Chronic Conditions 2019 COLLECTION
Sleep Quiz & Referral Form Inside
 Sleep Quiz & Referral Form Inside Rediscover the power of sleep Apnea solutions for all ages Mobile Sleep Services Who We Are An experienced and well trained team of sleep care professionals consisting
Sleep Quiz & Referral Form Inside Rediscover the power of sleep Apnea solutions for all ages Mobile Sleep Services Who We Are An experienced and well trained team of sleep care professionals consisting
Home Sleep Testing with Classic SleepCare
 Home Sleep Testing with Classic SleepCare Convenient Test performed in your own home Affordable A fraction of the price of an in-lab sleep study Accurate Measures breathing to evaluate for sleep apnea
Home Sleep Testing with Classic SleepCare Convenient Test performed in your own home Affordable A fraction of the price of an in-lab sleep study Accurate Measures breathing to evaluate for sleep apnea
Physician Dentist Collaboration
 Physician Dentist Collaboration Ronald S. Prehn, ThM, DDS Legal Perspective MD CAN LEGALLY MAKE PROPER DIAGNOSIS DDS CAN LEGALLY FABRICATE DENTAL SLEEP APPLIANCES Legal Perspective TWO PROFESSIONS WORK
Physician Dentist Collaboration Ronald S. Prehn, ThM, DDS Legal Perspective MD CAN LEGALLY MAKE PROPER DIAGNOSIS DDS CAN LEGALLY FABRICATE DENTAL SLEEP APPLIANCES Legal Perspective TWO PROFESSIONS WORK
Your Starting Point. Our Wellness Portal is the perfect place to begin your path to health
 Fall 2014 Your Starting Point Our Wellness Portal is the perfect place to begin your path to health - Time for a yearly check-up - Is sleep apnea hurting your health? - Cholesterol by the numbers ONE TO
Fall 2014 Your Starting Point Our Wellness Portal is the perfect place to begin your path to health - Time for a yearly check-up - Is sleep apnea hurting your health? - Cholesterol by the numbers ONE TO
The Clinician s Role in Educating Patients with Sleep Apnea
 The Clinician s Role in Educating Patients with Sleep Apnea Cindy Altman, RPSGT, R.EEG/EP T. Alegent Creighton Clinic/Omaha, NE Immediate Past President/BRPT The Early Years in Sleep 1929 1930 1950 s 1968
The Clinician s Role in Educating Patients with Sleep Apnea Cindy Altman, RPSGT, R.EEG/EP T. Alegent Creighton Clinic/Omaha, NE Immediate Past President/BRPT The Early Years in Sleep 1929 1930 1950 s 1968
SLEEP SOLUTION. AIM Insights
 SLEEP SOLUTION AIM Insights Protecting sleep health: The cost when Americans ignore sleep disorder treatment How AIM is leveraging data to identify gaps in clinical care and reduce health care spending
SLEEP SOLUTION AIM Insights Protecting sleep health: The cost when Americans ignore sleep disorder treatment How AIM is leveraging data to identify gaps in clinical care and reduce health care spending
Management of OSA in the Acute Care Environment. Robert S. Campbell, RRT FAARC HRC, Philips Healthcare May, 2018
 Management of OSA in the Acute Care Environment Robert S. Campbell, RRT FAARC HRC, Philips Healthcare May, 2018 1 Learning Objectives Upon completion, the participant should be able to: Understand pathology
Management of OSA in the Acute Care Environment Robert S. Campbell, RRT FAARC HRC, Philips Healthcare May, 2018 1 Learning Objectives Upon completion, the participant should be able to: Understand pathology
Snoring and Sleep Apnea
 The Patient s Guide To Snoring and Sleep Apnea The Complications May Be More Severe Than You Think Unit #245, 520 3rd Ave SW Calgary, AB T2P 0R3 Tel: (587) 353-5060 www.centennialsmiles.ca CONTENTS Introduction
The Patient s Guide To Snoring and Sleep Apnea The Complications May Be More Severe Than You Think Unit #245, 520 3rd Ave SW Calgary, AB T2P 0R3 Tel: (587) 353-5060 www.centennialsmiles.ca CONTENTS Introduction
Obstructive Sleep Apnea
 Obstructive Sleep Apnea Definition: Repetitive episodes of upper airway obstruction (complete or partial) that occur during sleep and are associated with arousals or desaturations +/or daytime sleepiness.
Obstructive Sleep Apnea Definition: Repetitive episodes of upper airway obstruction (complete or partial) that occur during sleep and are associated with arousals or desaturations +/or daytime sleepiness.
A Winning Combination
 The Physiologic Sleep Bite and the Micr0 2 Sleep Device A Winning Combination There is no doubt that using the best bite technique available will improve overall treatment success, but how important is
The Physiologic Sleep Bite and the Micr0 2 Sleep Device A Winning Combination There is no doubt that using the best bite technique available will improve overall treatment success, but how important is
Commissioning Policy Individual Funding Request
 Commissioning Policy Individual Funding Request Continuous Positive Airway Pressure (CPAP) Treatment of Obstructive Sleep Apnoea/Hypopnoea Syndrome (OSAHS) Criteria Based Access Policy Date Adopted: 13
Commissioning Policy Individual Funding Request Continuous Positive Airway Pressure (CPAP) Treatment of Obstructive Sleep Apnoea/Hypopnoea Syndrome (OSAHS) Criteria Based Access Policy Date Adopted: 13
Lowering epilepsy-related treatment costs in the era of patient choice and value-based care
 Lowering epilepsy-related treatment costs in the era of patient choice and value-based care In-home EEG offers cost-effective, reliable alternative to traditional diagnostic services 01 Introduction One
Lowering epilepsy-related treatment costs in the era of patient choice and value-based care In-home EEG offers cost-effective, reliable alternative to traditional diagnostic services 01 Introduction One
Melinda Trimble RPSGT, RST
 Melinda Trimble RPSGT, RST Conflict of Interest Disclosures for Speakers I have no Conflict of Interest on this topic I would like to disclose that I do work for Philips Respironics Objectives Review how
Melinda Trimble RPSGT, RST Conflict of Interest Disclosures for Speakers I have no Conflict of Interest on this topic I would like to disclose that I do work for Philips Respironics Objectives Review how
CPAP. The CPAP will be covered
 CPAP CPAP Did your patient have a face to face visit with the physician prior to having a sleep study that documented (1) Sleep History and symptoms and/or (2) Epworth Scale and/or (3) Physical Examination?
CPAP CPAP Did your patient have a face to face visit with the physician prior to having a sleep study that documented (1) Sleep History and symptoms and/or (2) Epworth Scale and/or (3) Physical Examination?
Sleep Market Panel. Results for June 2015
 Sleep Market Panel Results for June 2015 Notes: o This is a monthly trending report of panel member data along with additional analysis by: Sleep labs affiliated with Hospitals vs. Independent Labs o Hospital
Sleep Market Panel Results for June 2015 Notes: o This is a monthly trending report of panel member data along with additional analysis by: Sleep labs affiliated with Hospitals vs. Independent Labs o Hospital
Emerging Sleep Testing Methods
 Emerging Sleep Testing Methods Matt T. Bianchi MD PhD Director, Sleep Division MGH Neurology www.mghsleep.com May 2015 Funding and Disclosures Funding: MGH Neurology Department Harvard Clinical Investigator
Emerging Sleep Testing Methods Matt T. Bianchi MD PhD Director, Sleep Division MGH Neurology www.mghsleep.com May 2015 Funding and Disclosures Funding: MGH Neurology Department Harvard Clinical Investigator
National Sleep Disorders Research Plan
 Research Plan Home Foreword Preface Introduction Executive Summary Contents Contact Us National Sleep Disorders Research Plan Return to Table of Contents SECTION 5 - SLEEP DISORDERS SLEEP-DISORDERED BREATHING
Research Plan Home Foreword Preface Introduction Executive Summary Contents Contact Us National Sleep Disorders Research Plan Return to Table of Contents SECTION 5 - SLEEP DISORDERS SLEEP-DISORDERED BREATHING
Sleep Labs are Obsolete for Perioperative Assessment of Sleep-Disordered Breathing: Pro
 Sleep Labs are Obsolete for Perioperative Assessment of Sleep-Disordered Breathing: Pro Lawrence J. Epstein, MD Brigham and Women s Hospital Harvard Medical School Welltrinsic Sleep Network Conflicts of
Sleep Labs are Obsolete for Perioperative Assessment of Sleep-Disordered Breathing: Pro Lawrence J. Epstein, MD Brigham and Women s Hospital Harvard Medical School Welltrinsic Sleep Network Conflicts of
Coding for Sleep Disorders Jennifer Rose V. Molano, MD
 Practice Coding for Sleep Disorders Jennifer Rose V. Molano, MD Accurate coding is an important function of neurologic practice. This section of is part of an ongoing series that presents helpful coding
Practice Coding for Sleep Disorders Jennifer Rose V. Molano, MD Accurate coding is an important function of neurologic practice. This section of is part of an ongoing series that presents helpful coding
Today Is Not Tomorrow in Sleep Technology. Laura Linley, RPSGT, RST, CRT
 Today Is Not Tomorrow in Sleep Technology Laura Linley, RPSGT, RST, CRT Objectives Discuss changes in sleep testing standards. Describe the specific job responsibilities that sleep technologists will fulfill.
Today Is Not Tomorrow in Sleep Technology Laura Linley, RPSGT, RST, CRT Objectives Discuss changes in sleep testing standards. Describe the specific job responsibilities that sleep technologists will fulfill.
Fabrice Czarnecki, M.D., M.A., M.P.H., FACOEM I have no disclosures to make.
 Maryland College of Occupational and Environmental Medicine April 2014 Fabrice Czarnecki, M.D., M.A., M.P.H., FACOEM fczarnecki@gablesgroup.com I have no disclosures to make. Guidelines 2006: Joint Task
Maryland College of Occupational and Environmental Medicine April 2014 Fabrice Czarnecki, M.D., M.A., M.P.H., FACOEM fczarnecki@gablesgroup.com I have no disclosures to make. Guidelines 2006: Joint Task
THE SLEEP APNEA EPIDEMIC
 THE SLEEP APNEA EPIDEMIC DIAGNOSE AND TREAT WITH SLEEP TECH IN YOUR OFFICE Integrative Healthcare Symposium February 2018, New York City Jordan Stern, MD Founder & CEO, BlueSleep Founder and CEO of BlueSleep
THE SLEEP APNEA EPIDEMIC DIAGNOSE AND TREAT WITH SLEEP TECH IN YOUR OFFICE Integrative Healthcare Symposium February 2018, New York City Jordan Stern, MD Founder & CEO, BlueSleep Founder and CEO of BlueSleep
Sleep Studies: Attended Polysomnography and Portable Polysomnography Tests, Multiple Sleep Latency Testing and Maintenance of Wakefulness Testing
 Portable Polysomnography Tests, Multiple Sleep Latency Testing and Maintenance of Wakefulness Testing MP9132 Covered Service: Yes when meets criteria below Prior Authorization Required: Yes as indicated
Portable Polysomnography Tests, Multiple Sleep Latency Testing and Maintenance of Wakefulness Testing MP9132 Covered Service: Yes when meets criteria below Prior Authorization Required: Yes as indicated
OSA - Obstructive sleep apnoea What you need to know if you think you might have OSA
 OSA - Obstructive sleep apnoea What you need to know if you think you might have OSA Obstructive sleep apnoea, or OSA, is a breathing problem that happens when you sleep. It can affect anyone men, women
OSA - Obstructive sleep apnoea What you need to know if you think you might have OSA Obstructive sleep apnoea, or OSA, is a breathing problem that happens when you sleep. It can affect anyone men, women
PEDIATRIC SLEEP GUIDELINES Version 1.0; Effective
 MedSolutions, Inc. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Requests for patients with atypical symptoms or clinical presentations
MedSolutions, Inc. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Requests for patients with atypical symptoms or clinical presentations
What is SDB? Obstructive sleep apnea-hypopnea syndrome (OSAHS)
 Have a Good Sleep? Estimated 70 million Americans have clinically significant sleep problems Chronic insomnias report decreased quality of life, memory and attention problems, decreased physical health
Have a Good Sleep? Estimated 70 million Americans have clinically significant sleep problems Chronic insomnias report decreased quality of life, memory and attention problems, decreased physical health
Data Management of the Sleep Disordered Breathing Patient
 Data Management of the Sleep Disordered Breathing Patient 1 AARC or AAST CEU credit As Allies in Better Sleep and Breathing, we make it our #1 priority to work in harmony with caregivers and patients to
Data Management of the Sleep Disordered Breathing Patient 1 AARC or AAST CEU credit As Allies in Better Sleep and Breathing, we make it our #1 priority to work in harmony with caregivers and patients to
CHANGING SHAPE OF SLEEP STUDIES
 CHANGING SHAPE OF SLEEP STUDIES JAMES C. O BRIEN MD FCCP, FAASM MEDICAL DIRECTOR, PROHEALTH PHYSICIANS SLEEP CENTERS 10/19/2107 GOALS OF MY TALK-- Review the types of sleep studies Provide clinical information
CHANGING SHAPE OF SLEEP STUDIES JAMES C. O BRIEN MD FCCP, FAASM MEDICAL DIRECTOR, PROHEALTH PHYSICIANS SLEEP CENTERS 10/19/2107 GOALS OF MY TALK-- Review the types of sleep studies Provide clinical information
Welch Allyn Cardiology Solutions
 Welch Allyn Cardiology Solutions Clinical excellence. Connected solutions. Continuous innovation. Welch Allyn Cardiology is proud to be powered by Mortara. As part of a health system, you understand that
Welch Allyn Cardiology Solutions Clinical excellence. Connected solutions. Continuous innovation. Welch Allyn Cardiology is proud to be powered by Mortara. As part of a health system, you understand that
Complete Sleep Apnea Care and Diabetes A Study on Total Cost Savings
 A Study on Total Cost Savings Our Leadership In Sleep Apnea Care Nevada Sleep Diagnostics, Inc. has a fifteen year history of leadership in sleep apnea care. Nevada Sleep Diagnostics consistently raises
A Study on Total Cost Savings Our Leadership In Sleep Apnea Care Nevada Sleep Diagnostics, Inc. has a fifteen year history of leadership in sleep apnea care. Nevada Sleep Diagnostics consistently raises
Tired of being tired?
 Tired of being tired? Narval CC MRD ResMed.com/Narval Sleepiness and snoring are possible symptoms of sleep apnea. Did you know that one in every four adults has some form of sleep disordered-breathing
Tired of being tired? Narval CC MRD ResMed.com/Narval Sleepiness and snoring are possible symptoms of sleep apnea. Did you know that one in every four adults has some form of sleep disordered-breathing
Polysomnography (PSG) (Sleep Studies), Sleep Center
 Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Alaska Sleep Education Center
 Alaska Sleep Education Center The 3 Types of Sleep Apnea Explained: Obstructive, Central, & Mixed Posted by Kevin Phillips on Jan 28, 2015 6:53:00 PM Sleep apnea is a very common sleep disorder, affecting
Alaska Sleep Education Center The 3 Types of Sleep Apnea Explained: Obstructive, Central, & Mixed Posted by Kevin Phillips on Jan 28, 2015 6:53:00 PM Sleep apnea is a very common sleep disorder, affecting
AASP Sun Sand and Sleep. Laura Linley, RPSGT, RST, CRT. Today Is Not
 AASP Sun Sand and Sleep Laura Linley, RPSGT, RST, CRT Today Is Not Tomorrow in Sleep Technology Objectives Discuss how sleep education will progress in polysomnography. Describe the specific job responsibilities
AASP Sun Sand and Sleep Laura Linley, RPSGT, RST, CRT Today Is Not Tomorrow in Sleep Technology Objectives Discuss how sleep education will progress in polysomnography. Describe the specific job responsibilities
Medical Affairs Policy
 Medical Affairs Policy Service: Sleep Disorder Treatment: Positive Airway Pressure Devices and Oral Appliances (CPAP, BPAP, BiPAP, BiPAP ST, BiPAP with backup, BiPAP -Auto SV, VPAP, VPAP Adapt, VPAP adapt
Medical Affairs Policy Service: Sleep Disorder Treatment: Positive Airway Pressure Devices and Oral Appliances (CPAP, BPAP, BiPAP, BiPAP ST, BiPAP with backup, BiPAP -Auto SV, VPAP, VPAP Adapt, VPAP adapt
Inspire Therapy for Sleep Apnea
 Inspire Therapy for Sleep Apnea Patient Guide Giving You the FREEDOM TO SLEEP Like Everyone Else Take Comfort. Inspire therapy can help. Inspire therapy is a breakthrough implantable treatment option for
Inspire Therapy for Sleep Apnea Patient Guide Giving You the FREEDOM TO SLEEP Like Everyone Else Take Comfort. Inspire therapy can help. Inspire therapy is a breakthrough implantable treatment option for
Premier Health Plan considers Oral Appliances for Obstructive Sleep Apnea (OSA) medically necessary for the following indications:
 Premier Health Plan POLICY AND PROCEDURE MANUAL MP.063.PH - al Appliances for Obstructive Sleep Apnea This policy applies to the following lines of business: Premier Commercial Premier Employee Premier
Premier Health Plan POLICY AND PROCEDURE MANUAL MP.063.PH - al Appliances for Obstructive Sleep Apnea This policy applies to the following lines of business: Premier Commercial Premier Employee Premier
Future of Sleep Centers: Challenges and Opportunities
 Future of Sleep Centers: Challenges and Opportunities Challenges Diagnostic Panels Reimbursement Therapy Panels Any Willing Provider Challenges Reimbursement Changes (Medicare as basis) Sleep Benefits
Future of Sleep Centers: Challenges and Opportunities Challenges Diagnostic Panels Reimbursement Therapy Panels Any Willing Provider Challenges Reimbursement Changes (Medicare as basis) Sleep Benefits
Managed Care and Sleep Medicine
 Managed Care and Sleep Medicine Denice Logan, DO, FACOI Regional Medical Director Blue Cross Blue Shield of Michigan and Blue Care Network are nonprofit corporations and independent licensees of the Blue
Managed Care and Sleep Medicine Denice Logan, DO, FACOI Regional Medical Director Blue Cross Blue Shield of Michigan and Blue Care Network are nonprofit corporations and independent licensees of the Blue
in China Shanghai Office Beijing Office (+86) (+86)
 SLEEP Apnea in China Guide 2018-2019 Shanghai Office (+86) 21 2426 6400 Beijing Office (+86) 010 6464 0611 www.pacificprime.cn Follow us on WeChat t A comprehensive overview of sleep apnea Perhaps you
SLEEP Apnea in China Guide 2018-2019 Shanghai Office (+86) 21 2426 6400 Beijing Office (+86) 010 6464 0611 www.pacificprime.cn Follow us on WeChat t A comprehensive overview of sleep apnea Perhaps you
Best practices for a successful wellness screening program
 Health & Wellness Best practices for a successful wellness screening program Identify risk. Increase engagement. Incite change. Identifying health risks in your employee population People at risk for chronic
Health & Wellness Best practices for a successful wellness screening program Identify risk. Increase engagement. Incite change. Identifying health risks in your employee population People at risk for chronic
Advanced Skin Cancer Screenings. Research Collaboration
 Advanced Skin Cancer Screenings Research Collaboration Collaboration Opportunities April 2018 Advanced Skin Cancer Screenings Advanced Skin Cancer Screenings (ASCS) are the focus of a research collaboration
Advanced Skin Cancer Screenings Research Collaboration Collaboration Opportunities April 2018 Advanced Skin Cancer Screenings Advanced Skin Cancer Screenings (ASCS) are the focus of a research collaboration
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea
 Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO;
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO;
Drug Prior Authorization Form Alertec (modafinil)
 This document contains both information and form fields. To read information, use the Down Arrow from a form field. Drug Prior Authorization Form The purpose of this form is to obtain information required
This document contains both information and form fields. To read information, use the Down Arrow from a form field. Drug Prior Authorization Form The purpose of this form is to obtain information required
THN. Sleep Therapy Study. ImThera. Information for Participants. Caution: Investigational device. Limited by United States law to investigational use.
 THN Sleep Therapy Study Information for Participants Caution: Investigational device. Limited by United States law to investigational use. ImThera Obstructive sleep apnea (OSA) is a very serious condition.
THN Sleep Therapy Study Information for Participants Caution: Investigational device. Limited by United States law to investigational use. ImThera Obstructive sleep apnea (OSA) is a very serious condition.
An Engagement Solution You Won t Lose Sleep Over
 An Engagement Solution You Won t Lose Sleep Over Providing Results & A Positive ROI How two sleep centers utilize engagement technology to prepare patients, encourage attendance & increase use of CPAP
An Engagement Solution You Won t Lose Sleep Over Providing Results & A Positive ROI How two sleep centers utilize engagement technology to prepare patients, encourage attendance & increase use of CPAP
(HST) (95806, G0398, G0399)
 95800 Sleep study, unattended, simultaneous recording of, heart rate, oxygen saturation, respiratory analysis (e.g. by airflow or peripheral arterial tone), and sleep time 95801 Sleep study, unattended,
95800 Sleep study, unattended, simultaneous recording of, heart rate, oxygen saturation, respiratory analysis (e.g. by airflow or peripheral arterial tone), and sleep time 95801 Sleep study, unattended,
Split Night Protocols for Adult Patients - Updated July 2012
 Split Night Protocols for Adult Patients - Updated July 2012 SUMMARY: Sleep technologists are team members who work under the direction of a physician practicing sleep disorders medicine. Sleep technologists
Split Night Protocols for Adult Patients - Updated July 2012 SUMMARY: Sleep technologists are team members who work under the direction of a physician practicing sleep disorders medicine. Sleep technologists
10.2 Summary of the Votes and Considerations for Policy
 CEPAC Voting and Policy Implications Summary Supplemental Screening for Women with Dense Breast Tissue December 13, 2013 The last CEPAC meeting addressed the comparative clinical effectiveness and value
CEPAC Voting and Policy Implications Summary Supplemental Screening for Women with Dense Breast Tissue December 13, 2013 The last CEPAC meeting addressed the comparative clinical effectiveness and value
Healthy for Life Newsletter September/October 2010 Vol. 7 No. 5. Fibromyalgia a Sleep Disorder
 Healthy for Life Newsletter September/October 2010 Vol. 7 No. 5 Fibromyalgia a Sleep Disorder Introduction I have lived with fibromyalgia for over 30 years. No, I don t have fibromyalgia; however, my wife
Healthy for Life Newsletter September/October 2010 Vol. 7 No. 5 Fibromyalgia a Sleep Disorder Introduction I have lived with fibromyalgia for over 30 years. No, I don t have fibromyalgia; however, my wife
ASX Investor Presentation
 ASX Investor Presentation Sydney, Australia Dr Peter Neustadt Executive Chairman and CEO November 2014 Copyright and registered trademark notice ASX Investor Presentation Page 0 Who we are SomnoMed Limited
ASX Investor Presentation Sydney, Australia Dr Peter Neustadt Executive Chairman and CEO November 2014 Copyright and registered trademark notice ASX Investor Presentation Page 0 Who we are SomnoMed Limited
Critical Review Form Diagnostic Test
 Critical Review Form Diagnostic Test Diagnosis and Initial Management of Obstructive Sleep Apnea without Polysomnography A Randomized Validation Study Annals of Internal Medicine 2007; 146: 157-166 Objectives:
Critical Review Form Diagnostic Test Diagnosis and Initial Management of Obstructive Sleep Apnea without Polysomnography A Randomized Validation Study Annals of Internal Medicine 2007; 146: 157-166 Objectives:
SLEEP DISORDERED BREATHING The Clinical Conditions
 SLEEP DISORDERED BREATHING The Clinical Conditions Robert G. Hooper, M.D. In the previous portion of this paper, the definitions of the respiratory events that are the hallmarks of problems with breathing
SLEEP DISORDERED BREATHING The Clinical Conditions Robert G. Hooper, M.D. In the previous portion of this paper, the definitions of the respiratory events that are the hallmarks of problems with breathing
Commissioning for Better Outcomes in COPD
 Commissioning for Better Outcomes in COPD Dr Matt Kearney Primary Care & Public Health Advisor Respiratory Programme, Department of Health General Practitioner, Runcorn November 2011 What are the Commissioning
Commissioning for Better Outcomes in COPD Dr Matt Kearney Primary Care & Public Health Advisor Respiratory Programme, Department of Health General Practitioner, Runcorn November 2011 What are the Commissioning
FINAL ENDURING OUTCOMES REPORT
 FINAL ENDURING OUTCOMES REPORT OVERVIEW This report summarizes consolidated outcomes data from an enduring satellite symposium activity that was launched In March 2017 and ran for 12 months, cumulatively,
FINAL ENDURING OUTCOMES REPORT OVERVIEW This report summarizes consolidated outcomes data from an enduring satellite symposium activity that was launched In March 2017 and ran for 12 months, cumulatively,
Obstructive Sleep Apnea in Truck Drivers
 Rocky Mountain Academy of Occupational and Environmental Medicine Denver, Colorado February 6, 2010 Obstructive Sleep Apnea in Truck Drivers Philip D. Parks, MD, MPH, MOccH Medical Director, Lifespan Health
Rocky Mountain Academy of Occupational and Environmental Medicine Denver, Colorado February 6, 2010 Obstructive Sleep Apnea in Truck Drivers Philip D. Parks, MD, MPH, MOccH Medical Director, Lifespan Health
Precision Sleep Medicine
 Precision Sleep Medicine Picking Winners Improves Outcomes and Avoids Side-Effects North American Dental Sleep Medicine Conference February 17-18, 2017 Clearwater Beach, FL John E. Remmers, MD Conflict
Precision Sleep Medicine Picking Winners Improves Outcomes and Avoids Side-Effects North American Dental Sleep Medicine Conference February 17-18, 2017 Clearwater Beach, FL John E. Remmers, MD Conflict
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea
 Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO
