NURSES SUMMARY: SEVEN DAY LOOK BACK
|
|
|
- Russell Evans
- 5 years ago
- Views:
Transcription
1 Select the appropriate responses, record vital signs and comments. VITAL SIGNS: T P R B/P WT HT HEARING, SPEECH AND VISION Section B COGNITIVE PATTERNS Section C Alert and oriented x 3 Disoriented: Person, Place, Time Comatose: Persistent, vegetative state/no discernible consciousness HEARING: Ability to hear (with hearing aid or hearing appliances if normally used) Adequate no difficulty in normal conversation, social interaction, listening to TV Minimal difficulty difficulty in some environments (e.g. when person speaks softly or setting is noisy) Moderate difficulty speaker has to increase volume and speak distinctly Highly impaired absence of useful hearing HEARING AID: Hearing aid or other hearing appliance used No Yes: Rt Lt Bilateral Present but not regularly used SPEECH CLARITY: Select best description of speech pattern Clear speech distinct intelligible words Unclear speech slurred or mumbled words No speech absence of spoken words MAKES SELF UNDERSTOOD: Ability to express ideas and wants, consider both verbal and non-verbal expression Understood Usually understood difficulty communicating some words or finishing thoughts but is able if prompted or given time Sometimes understood ability is limited to making concrete requests Rarely/never understood ABILITY TO UNDERSTAND OTHERS: Understanding verbal content, however able (with hearing aid or device if used) Understands clear comprehension Usually understands misses some part/intent of message but comprehends most conversation Sometimes understands responds adequately to simple, direct communication only Rarely/never understands VISION: Ability to see in adequate light (with glasses or other visual appliances) Adequate sees fine detail, including regular print in newspapers/books Impaired sees large print, but not regular print in newspapers/books Moderately impaired limited vision; not able to see newspaper headlines but can identify objects Highly impaired object identification in question, but eyes appear to follow objects Severely impaired no vision or sees only light, colors or shapes; eyes do not appear to follow objects CORRECTIVE LENSES: (Contacts, glasses, or magnifying glass used), specify: Eye prosthesis: Rt Lt Comments: SHORT TERM MEMORY: Seems or appears to recall after 5 minutes Memory problem LONG TERM MEMORY: Seems or appears to recall long past Memory problem MEMORY/RECALL ABILITY: Current season Location of own room Staff names and faces That he or she is in a nursing home None of the above were recalled COGNITIVE SKILLS FOR DAILY DECISION MAKING: Independent decisions consistent/reasonable Modified independence some difficulty in new situations only Modified impaired decisions poor, cues/supervision required Severely impaired never/rarely made decisions DELIRIUM: Inattention Did the resident have difficulty focusing attention (easily distracted, out of touch or difficulty following what was said)? Disorganized thinking Was the resident s thinking disorganized or incoherent (rambling or irrelevant conversation, unclear or illogical flow of ideas, or unpredictable switching from subject to subject)? Altered level of consciousness Did the resident have altered level of consciousness? (e.g., vigilant startled easily to any sound or touch; lethargic repeatedly dozed off when being asked questions, but responds to voice or touch; stuporous very difficult to arouse and keep aroused for the interview; comatose could not be aroused) Evidence of acute change in mental status from baseline? Comments: MOOD Section D No mood symptoms present Little interest or pleasure in doing things Feeling down, depressed, or hopeless Trouble falling or staying asleep, or sleeping too much Feeling tired or having little energy Poor appetite or overeating Feeling bad about yourself or that you are a failure or have let yourself or your family down Form 1950P Rev. 5/18 BRIGGS, Des Moines, IA (800) Unauthorized copying or use violates copyright law.
2 MOOD (Cont d.) Section D BEHAVIOR (Cont d.) Section E Trouble concentrating on things, such as reading the Behavior symptom(s) impact on others newspaper or watching television Puts others at significant risk for physical injury Moving or speaking so slowly that other people could have Significantly intrudes on the privacy or activity of others noticed. Or the opposite being so fidgety or restless that Significantly disrupts care or living environment you have been moving around a lot more than usual Change in behavior or other symptoms Thoughts that you would be better off dead, or of hurting Same Improved Worse yourself in some way NA no prior MDS assessment Short-tempered, easily annoyed Comments: Comments: BEHAVIOR Section E No behaviors exhibited Physical behavioral symptoms directed toward others (e.g., hitting, kicking, pushing, scratching, grabbing, abusing others sexually) Verbal behavioral symptoms directed toward others (e.g., threatening others, screaming at others, cursing at others) Other behavioral symptoms not directed toward others (e.g., physical symptoms such as hitting or scratching self, pacing, rummaging, public sexual acts, disrobing in public, throwing or smearing food or bodily wastes, or verbal/vocal symptoms like screaming, disruptive sounds) Rejection of care (e.g., bloodwork, taking medications, ADL assistance) that is necessary to achieve the resident s goals for health and well-being Wandering Wandering placed the resident at significant risk of getting to a potentially dangerous place (e.g., stairs, outside of the facility) Wandering significantly intrudes on the privacy or activities of others Hallucinations (perceptual experiences in the absence of real external sensory stimuli) Delusions (misconceptions or beliefs that are firmly held, contrary to reality) Behavior symptom(s) impact on resident Puts the resident at significant risk for physical illness or injury Significantly interferes with resident s care Significantly interferes with resident s participation in activities or social interactions FUNCTIONAL STATUS ADL ASSISTANCE CODE 1: SELF-PERFORMANCE Activity 3 or More Times 0. Independent 3. Extensive Assistance 1. Supervision 4. Total Dependence for 2. Limited Assistance Entire 7 Days Activity 2 or Less Times 7. Activity Occurred 1 or 2 Times 8. Activity Did Not Occur for Entire 7 Days Code 1 Section G Bed mobility Bed mobility Transfer Transfer Walk in room Walk in room Walk in corridor Walk in corridor Locomotion on unit Locomotion on unit Locomotion off unit Locomotion off unit Dressing Dressing Eating Eating Toilet use Toilet use Personal hygiene Personal hygiene Bathing Bathing FUNCTIONAL LIMITATION IN RANGE OF MOTION/ CONTRACTURES: Upper extremity (shoulder, elbow, wrist, hand) Lower extremity (hip, knee, ankle, foot) BALANCE DURING TRANSITIONS AND WALKING CODE: 0. Steady at all times 1. Not steady, but able to stabilize without staff assistance CODE 2: SUPPORT PROVIDED 0. No setup or physical help from staff 1. Setup help only 2. One person physical assist 3. Two+ persons physical assist 8. ADL activity itself did not occur during entire period; family and/or non-facility staff provided 100% of the time Code 2 2. Not steady, only able to stabilize with staff assistance 3. Activity did not occur Code Moving from seated to standing position Walking (with assistive device if used) Turning around and facing the opposite direction while walking Moving on and off toilet Surface-to-surface transfer (transfer between bed and chair or wheelchair MOBILITY DEVICES: (check all normally used) Cane/crutch Wheelchair (manual or electric) Walker Limb prosthesis None of the above used Comments:
3 BLADDER Section H BOWEL (Cont.d) Section H BLADDER APPLIANCES: Indwelling catheter (including suprapubic catheter and nephrostomy tube) Dx: Type: Date inserted: External (condom) catheter Ostomy (including urostomy, ileostomy, and colostomy) Intermittent catheterization None of the above URINARY TOILETING PROGRAM: Bladder retraining Scheduled toileting Prompted voiding Does not use toilet/commode/urinal Pads/briefs utilized None of the above URINARY CONTINENCE: Always continent Occasionally incontinent (less than 7 episodes of incontinence) Frequently incontinent (7 or more episodes of urinary incontinence, but at least one episode of continent voiding) Always incontinent (no episodes of continent voiding) Not rated, resident had a catheter (indwelling, condom), urinary ostomy, or no urine output for entire 7 days BLADDER SYMPTOMS: Burning Discharge Retention/distention Nocturia Frequency/urgency Pain with voiding Hematuria BOWEL Section H BOWEL SOUNDS: Present: Hyperactive Hypoactive Absent _ BOWEL CONTINENCE: Always continent Occasionally incontinent (one episode of bowel incontinence) Frequently incontinent (2 or more episodes of bowel incontinence, but at least one continent bowel movement) Always incontinent (no episodes of continent bowel movements) Not rated, resident had an ostomy or did not have a bowel movement for the entire 7 days BOWEL TOILETING PROGRAM: Is a toileting program currently being used to manage the resident s bowel continence? BOWEL PATTERNS: Constipation Hemorrhoids Diarrhea Fissures/fistulas _ HEART/CIRCULATION Regular rhythm/wnl? Radial pulse irregular? Apical pulse irregular? SaO 2 % % % Nebulizer Tx Suctioning Tracheostomy/care Ventilator/care BiPAP/CPAP Section I EDEMA: Dependent Pedal: Lt Pedal: Rt Abnormal peripheral pulses Vertigo/dizziness Pitting: +1 Pitting: +2 Pitting: +3 Pitting: +4 Weight increase, specify: RESPIRATORY: Normal, no problems Labored breathing Shallow respirations Rales/rhonchi Wheezing Cough Orthopnea O L/minute PRN Continuous Nasal cannula Mask _ PAIN INTENSITY NUMERIC RATING (00-10) (Enter 99 if unable to answer) VERBAL DESCRIPTOR SCALE Mild Moderate Severe Very severe, horrible Unable to answer PAIN MANAGEMENT No pain Pain within past 5 days Scheduled pain management regimen Received PRN medications Received non-medication pain interventions
4 PAIN MANAGEMENT (Cont d.) SWALLOWING/NUTRITIONAL STATUS Section K INDICATORS OF PAIN OR POSSIBLE PAIN: Non-verbal sounds (crying, whining, gasping, moaning, or groaning) Vocal complaints of pain (that hurts, ouch, stop) Facial expressions (grimaces, winces, wrinkled forehead, furrowed brow, clenched teeth or jaw) Protective body movements or postures (bracing, guarding, rubbing or massaging a body part/area, clutching or holding a body part during movement) FREQUENCY OF PAIN INDICATORS: Indicators of pain/possible pain observed 1 to 2 days Indicators of pain/possible pain observed 3 to 4 days Indicators of pain/possible pain observed daily OTHER HEALTH CONDITIONS None Shortness of breath or trouble breathing with exertion (e.g. walking, bathing, transferring) Shortness of breath or trouble breathing when sitting at rest Shortness of breath or trouble breathing when lying flat Current tobacco user Life expectancy of less than 6 months Fever Vomiting Dehydrated Internal bleeding FALL HISTORY No falls Fall any time in the last month prior to admit or reentry Fall any time in the last 2-6 months prior to admit or reentry Fracture related to fall in the 6 months prior to admit or reentry Fall since admit/reentry or prior assessment Coding: 0. None 1. One 2. Two or more No injury (no evidence of any injury noted or physical assessment by nurse or primary care clinician; no complaints of pain or injury by the resident; no change in resident behavior noted after the fall) Injury except major (skin tears, lacerations, superficial bruises, hematomas and sprains; any fall-related injury that causes resident to complain of pain) Major injury (bone fractures, joint dislocations, closed head injuries with altered consciousness, subdural hematoma) SWALLOWING DISORDER: No swallowing problems Loss of liquids/solids from mouth when eating or drinking Holding food in mouth/cheeks or residual food in mouth after meals Coughing or choking during meals or when swallowing medications WEIGHT LOSS/GAIN: Loss of 5% or more in last month or loss of 10% or more in last 6 months On physician-prescribed weight-loss regimen Not on physician-prescribed weight-loss regimen Gain of 5% or more in last month or gain of 10% or more in last 6 months On physician-prescribed weight-gain regimen Not on physician-prescribed weight-gain regimen Weight stable NUTRITIONAL APPROACHES: Parenteral/IV feeding While not a resident While a resident Feeding tube nasogastric or abdominal (PEG) While not a resident While a resident Mechanically altered diet (pureed foods, thickened liquids) While not a resident While a resident Therapeutic diet (low salt, diabetic, low cholesterol) No nutritional approaches needed PERCENT INTAKE BY ARTIFICIAL ROUTE: While not a resident (select one % and one fluid intake when applicable) 25% or less 26-50% 51% or more 500 cc/day or less fluid intake via IV or tube feeding 501 cc/day or more fluid intake via IV or tube feeding While a resident (select one % and one fluid intake when applicable) 25% or less 26-50% 51% or more 500 cc/day or less fluid intake via IV or tube feeding 501 cc/day or more fluid intake via IV or tube feeding During entire 7 days (select one % and one fluid intake when applicable) 25% or less 26-50% 51% or more 500 cc/day or less fluid intake via IV or tube feeding 501 cc/day or more fluid intake via IV or tube feeding No artificial routes of intake
5 SKIN CONDITIONS ORAL/DENTAL STATUS Section L SKIN CONDITIONS (Cont d.) Section M All natural teeth present, intact CURRENT NUMBER OF UNHEALED PRESSURE ULCERS/ Dentures INJURIES AT EACH STAGE (Cont d.): Partial Full upper Full lower Unstageable: non-removable dressing Broken or loosely fitting full or partial denture (chipped, Number of unstageable pressure ulcers/injuries due to cracked, uncleanable, or loose) non-removable dressing/device Abnormal mouth tissue (ulcers, masses, oral lesions, Number present on admission/entry or reentry including under denture or partial if one is worn) Unstageable: slough and/or eschar Obvious or likely cavity of natural teeth Number of unstageable pressure ulcers/injuries due to No natural teeth or tooth fragment(s) (edentulous) slough and/or eschar covering the wound bed Loose or broken natural teeth Number present on admission/entry or reentry Inflamed or bleeding gums Unstageable: deep tissue injury Normal mouth tissue (pink and moist) Number of unstageable pressure ulcers/injuries with deep Mouth or facial pain, discomfort or difficulty with chewing tissue injury in evolution Unable to examine Number present on admission/entry or reentry Venous and arterial ulcers Number of venous and arterial ulcers present _ Section M DETERMINATION OF PRESSURE ULCER/INJURY RISK: Stage 1 or greater, scar over bony prominence, or a nonremovable dressing/device Formal assessment instrument/tool (e.g., Braden, Norton or other) Date: Clinical assessment Date: No determination of risk assessed RISK OF PRESSURE ULCERS/INJURIES: At risk for developing pressure ulcers/injuries Not at risk for developing pressure ulcers/injuries UNHEALED PRESSURE INJURY STAGE 1 OR HIGHER: CURRENT NUMBER OF UNHEALED PRESSURE ULCER/ INJURY AT EACH STAGE: Number of unhealed Stage 1 pressure ulcers/injuries Number of unhealed Stage 2 pressure ulcers/injuries Number of Stage 2 ulcers/injuries present on admit/entry or reentry Date of oldest Stage 2 Number of unhealed Stage 3 pressure ulcers/injuries Number of Stage 3 ulcers/injuries present on admit/entry or reentry. Pressure ulcer/injury length of largest Stage 3 (head to toe). Pressure ulcer/injury width of largest Stage 3 (side to side perpendicular) same injury. Pressure ulcer/injury depth of largest Stage 3 (visible surface to deepest area) same injury Number of unhealed Stage 4 pressure ulcers/injuries Number of Stage 4 ulcers/injuries present on admit/entry or reentry. Pressure ulcer/injury length of largest Stage 4 (head to toe). Pressure ulcer/injury width of largest Stage 4 (side to side perpendicular) same injury. Pressure ulcer/injury depth of largest Stage 4 (visible surface to deepest area) same injury MOST SEVERE TISSUE TYPE FOR ANY PRESSURE ULCER/ INJURY: Epithelial tissue (new skin growing in superficial wound can be light pink and shiny even with darkly pigmented skin) Granulation tissue (pink or red tissue with shiny, moist granular appearance) Slough (yellow or white tissue that adheres to wound bed in strings or thick clumps or is mucinous) Eschar (black, brown or tan tissue that allows firmly to wound bed or injury edges, may be softer or harder than surrounding skin) Not applicable OTHER ULCERS, WOUNDS, SKIN PROBLEMS: No skin problems Infections of the foot (cellulitis, purulent drainage) Diabetic foot ulcers Other open lesion(s) on the foot Open lesion(s) other than ulcers, rashes, cuts Surgical wound(s) Burn(s) (second or third degree) Skin tear(s) Moisture Associated Skin Damage MASD (incontinence, perspiration, drainage) Rashes Abrasions SKIN AND WOUND TREATMENTS: No skin and/or wound treatments provided Pressure reducing device for chair Pressure reducing device for bed Turning/repositioning program Nutrition or hydration intervention (to manage skin problems) Pressure injury care Surgical wound care Application of nonsurgical dressings (with/without topical medications/other than to feet) Applications of ointments/medications other than to feet Application of dressings to feet (with/without topical medications)
6 SKIN CONDITIONS (Cont d.) Section M SURGICAL WOUND SITE: No surgical wound Dressing present Surgical site intact (staples, sutures) No signs of infection (redness, warmth, edema, drainage) FOOT CARE: Toenails trimmed Application of dressings/corn pads Seen by podiatrist Special shoes/inserts/orthotics used MEDICATIONS Section N INJECTIONS: No injections during the past 7 days Number of days received injection of any type Number of days received insulin injection Number of days insulin orders were changed MEDICATIONS RECEIVED IN PAST 7 DAYS: (record number of days) Antipsychotic Antidepressant Antianxiety Hypnotic Anticoagulant (warfarin, heparin, low-molecular weight heparin) Antibiotic Diuretic Opioid SPECIAL TREATMENTS, PROCEDURES Section O AND PROGRAMS Received no special treatments, procedures and/or programs Chemotherapy BiPAP/CPAP Radiation IV medications Oxygen therapy Transfusions Suctioning Dialysis Tracheostomy care Hospice care Ventilator or respirator Respite care Isolation or quarantine for active infectious disease PARTICIPATION IN SUMMARY Resident Family Staff members Dialysis staff Significant other/spouse Hospice staff OTHER COMMENTS SPECIAL TREATMENTS, PROCEDURES Section O AND PROGRAMS (Cont d.) RESTORATIVE NURSING PROGRAMS (record number of days restorative program performed for at least 15 minutes) Passive range of motion Active range of motion Splint or brace assistance Bed mobility Transfer Walking Dressing and/or grooming Eating and/or swallowing Amputation/prosthesis care Communication No restorative nursing programs RESTRAINTS AND ALARMS Section P Coding: 0. Not used 1. Used less than daily 2. Used daily RESTRAINTS USED IN BED: Bed rail Trunk restraint Limb restraint Other RESTRAINTS USED IN CHAIR OR OUT OF BED: Trunk restraint Limb restraint Chair prevents rising Other Bed alarm Chair alarm Floor mat alarm Motion sensor alarm Wander/elopement alarm Other alarm, specify: Guardian or legal representative Clergy Other, specify: Signature/Title: Date:
Identification Information.
 Section A. Identification Information. A1200. Marital Status. 1. Never married. 2. Married. 3. Widowed. 4. Separated. 5. Divorced. A1300. Optional Resident Items. A. Medical record number: B. Room number:
Section A. Identification Information. A1200. Marital Status. 1. Never married. 2. Married. 3. Widowed. 4. Separated. 5. Divorced. A1300. Optional Resident Items. A. Medical record number: B. Room number:
Identification Information
 Section A Medical Necessity and Level of Care Assessment - Version 3.0 Identification Information A0310. Type of Assessment A. Reason for Assessment 01. Initial assessment 03. Annual assessment 04. Significant
Section A Medical Necessity and Level of Care Assessment - Version 3.0 Identification Information A0310. Type of Assessment A. Reason for Assessment 01. Initial assessment 03. Annual assessment 04. Significant
MINIMUM DATA SET (MDS) - Version 3.0 RESIDENT ASSESSMENT AND CARE SCREENING Swing Bed Discharge (SD) Item Set
 MINIMUM DATA SET (MDS) - Version 3.0 RESIDENT ASSESSMENT AND CARE SCREENING Swing Bed Discharge (SD) Item Set Section A. Identification Information. A0100. Facility Provider Numbers. A. National Provider
MINIMUM DATA SET (MDS) - Version 3.0 RESIDENT ASSESSMENT AND CARE SCREENING Swing Bed Discharge (SD) Item Set Section A. Identification Information. A0100. Facility Provider Numbers. A. National Provider
MINIMUM DATA SET (MDS) - Version 3.0 RESIDENT ASSESSMENT AND CARE SCREENING ALL ITEM LISTING
 Resident Cynthia M. Identifier 55555 Date 2/27/ MINIMUM DATA SET (MDS) - Version 3. RESIDENT ASSESSMENT AND CARE SCREENING ALL ITEM LISTING Section A. Identification Information. A. Facility Provider Numbers.
Resident Cynthia M. Identifier 55555 Date 2/27/ MINIMUM DATA SET (MDS) - Version 3. RESIDENT ASSESSMENT AND CARE SCREENING ALL ITEM LISTING Section A. Identification Information. A. Facility Provider Numbers.
MDS 3.0: Recommended Form
 MDS 3.0: Recommended Form Recommended MDS 3.0 Recommended MDS 3.0 Nursing Home Assessment Record Identification Information A1. Facility Provider s a. National Provider Identifier (NPI) b. CMS Certification
MDS 3.0: Recommended Form Recommended MDS 3.0 Recommended MDS 3.0 Nursing Home Assessment Record Identification Information A1. Facility Provider s a. National Provider Identifier (NPI) b. CMS Certification
Assisted Living Resident Assessment (To be used when yes is indicated for skin issues under Section 5 of Assisted Living Resident Assessment)
 Skin Assessment Current open skin areas: Yes No Current pressure ulcer: Yes No A. Stage 1 Ulcers Report based on highest stage of existing ulcers at its worst; do not reverse stage. Number of existing
Skin Assessment Current open skin areas: Yes No Current pressure ulcer: Yes No A. Stage 1 Ulcers Report based on highest stage of existing ulcers at its worst; do not reverse stage. Number of existing
SN Visit Note. Vital Signs. Blood Sugar. Oxygen. Allergies. Pain Assessment. Visit Date: Episode Date: Patient Name: Patient ID:
 Patient Name: Patient ID: Visit Date: Episode Date: SN Visit Note Vital Signs Not ed Temperature: Pulse Apical: Reg Irreg Resp: / min Pulse Radial: Reg Irreg B/P (L) B/P (R) Sitting: / Sitting: / Standing:
Patient Name: Patient ID: Visit Date: Episode Date: SN Visit Note Vital Signs Not ed Temperature: Pulse Apical: Reg Irreg Resp: / min Pulse Radial: Reg Irreg B/P (L) B/P (R) Sitting: / Sitting: / Standing:
o Normal Balanced Diet for your Age o High in Carbohydrates o High in Fats o High in Protein o Other Diet
 HEALTH ASSESSMENT SCREENING FORM GO402 Welcome to G0438 First Annual G0439 Subsequent Other Code PATIENTS NAME: DATE OF BIRTH: DATE OF SERVICE: PLEASE LIST CURRENT MEDICATION, ALSO OVER THE COUNTER MEDICATIONS
HEALTH ASSESSMENT SCREENING FORM GO402 Welcome to G0438 First Annual G0439 Subsequent Other Code PATIENTS NAME: DATE OF BIRTH: DATE OF SERVICE: PLEASE LIST CURRENT MEDICATION, ALSO OVER THE COUNTER MEDICATIONS
SECTION H: BLADDER AND BOWEL. H0100: Appliances. Item Rationale Health-related Quality of Life. Planning for Care
 SECTION H: BLADDER AND BOWEL Intent: The intent of the items in this section is to gather information on the use of bowel and bladder appliances, the use of and response to urinary toileting programs,
SECTION H: BLADDER AND BOWEL Intent: The intent of the items in this section is to gather information on the use of bowel and bladder appliances, the use of and response to urinary toileting programs,
Southeastern Rehabilitation Medicine Initial (New) Outpatient Information Questionnaire
 Southeastern Rehabilitation Medicine Initial (New) Outpatient Information Questionnaire Name: MR#:_ Date: Date of Injury: Referred By: Age: Date of Birth: Handed: R L Ambidextrous Male Female **** Mark
Southeastern Rehabilitation Medicine Initial (New) Outpatient Information Questionnaire Name: MR#:_ Date: Date of Injury: Referred By: Age: Date of Birth: Handed: R L Ambidextrous Male Female **** Mark
CENTRAL CARE POLICY SYMPTOMS OF ILLNESS. Policy: Consumers will be observed for symptoms of physical problems, distress, pain, or unusual behaviors.
 Page 1 of 5 CENTRAL CARE POLICY SYMPTOMS OF ILLNESS SUBJECT: SYMPTOMS OF ILLNESS ANNUAL REVIEW MONTH: June RESPONSIBLE FOR REVIEW: Director of Central Care LAST REVISION DATE: June 2009 Policy: Consumers
Page 1 of 5 CENTRAL CARE POLICY SYMPTOMS OF ILLNESS SUBJECT: SYMPTOMS OF ILLNESS ANNUAL REVIEW MONTH: June RESPONSIBLE FOR REVIEW: Director of Central Care LAST REVISION DATE: June 2009 Policy: Consumers
Table to Demonstrate a method of working through Triggered CAPs.
 CAP Problem Goals Triggers Guidelines Physical Activities increase hours of exercises Reports less than 2 hours Personal choice Promotion and physical activity activity in last 3 days Instrumental Activities
CAP Problem Goals Triggers Guidelines Physical Activities increase hours of exercises Reports less than 2 hours Personal choice Promotion and physical activity activity in last 3 days Instrumental Activities
SECTION J: HEALTH CONDITIONS. J0100: Pain Management (5-Day Look Back) Item Rationale Health-related Quality of Life.
 SECTION J: HEALTH CONDITIONS Intent: The intent of the items in this section is to document a number of health conditions that impact the resident s functional status and quality of life. The items include
SECTION J: HEALTH CONDITIONS Intent: The intent of the items in this section is to document a number of health conditions that impact the resident s functional status and quality of life. The items include
TABLE OF CONTENTS. Page TAB 1. Overview of Resident Assessment Process 6. RAP REVIEW or Working the RAP Steps 10
 TABLE OF CONTENTS Page TAB 1 Overview of Resident Assessment Process 6 RAP REVIEW or Working the RAP Steps 10 Working the RAPS & Documentation Systems 2 TAB 2 RAP Key 31 RAP Training Guidelines and care
TABLE OF CONTENTS Page TAB 1 Overview of Resident Assessment Process 6 RAP REVIEW or Working the RAP Steps 10 Working the RAPS & Documentation Systems 2 TAB 2 RAP Key 31 RAP Training Guidelines and care
Please complete this form before your Doctor visit. We will review this together and make any changes needed.
 1 Medical History Please complete this form before your Doctor visit. We will review this together and make any changes needed. Name Date of Birth Date of visit What is your height? weight? Medical History,
1 Medical History Please complete this form before your Doctor visit. We will review this together and make any changes needed. Name Date of Birth Date of visit What is your height? weight? Medical History,
MDS 3.0. Acronyms. Terminology & Definitions 8/22/2016 CAA CAT ADL BMI BIMS PT/OT/ST QI QM MDS RAI OMRA (SOT) OBRA RUG CMS COT OMRA ARD
 MDS 3.0 Acronyms MDS RAI OMRA (SOT) OBRA RUG CMS COT OMRA ARD CAA CAT ADL BMI BIMS PT/OT/ST QI QM Terminology & Definitions Active Disease Diagnosis Acute Change in Mental Status Period Reference Date
MDS 3.0 Acronyms MDS RAI OMRA (SOT) OBRA RUG CMS COT OMRA ARD CAA CAT ADL BMI BIMS PT/OT/ST QI QM Terminology & Definitions Active Disease Diagnosis Acute Change in Mental Status Period Reference Date
Medicare Annual Wellness Visit HEALTH RISK ASSESSMENT
 Patient Name: Date of Birth: GENERAL HEALTH 1. How is your overall health? Excellent Good Fair Poor 2. How many different prescriptions are you taking? 0-3 4-6 7-10 10+ 3. Do you take all of your mediations
Patient Name: Date of Birth: GENERAL HEALTH 1. How is your overall health? Excellent Good Fair Poor 2. How many different prescriptions are you taking? 0-3 4-6 7-10 10+ 3. Do you take all of your mediations
If both a standardized, validated screening tool and an evaluation of clinical factors are utilized, select Response 2.
 (M1300) Pressure Ulcer Assessment: Was this patient assessed for Risk of Developing Pressure Ulcers? 0 - No assessment conducted [Go to M1306 ] 1 - Yes, based on an evaluation of clinical factors (for
(M1300) Pressure Ulcer Assessment: Was this patient assessed for Risk of Developing Pressure Ulcers? 0 - No assessment conducted [Go to M1306 ] 1 - Yes, based on an evaluation of clinical factors (for
Section H Bladder and Bowel
 Instructor Guide Section H Bladder and Bowel Objectives State the intent of Section H Bladder and Bowel. Describe how to conduct the assessment for urinary incontinence. Describe how to conduct the assessment
Instructor Guide Section H Bladder and Bowel Objectives State the intent of Section H Bladder and Bowel. Describe how to conduct the assessment for urinary incontinence. Describe how to conduct the assessment
OT Routine Visit Note Page 1
 OT Routine Visit Note Page 1 Vital Signs Temperature: Apical: Pulse Radial: Resp: Lung Sounds: (L) / min Sitting Standing Lying (L) B/P (R) Pain Pain Type: Aching Dull Aching Constant Nagging Burning Gnawing
OT Routine Visit Note Page 1 Vital Signs Temperature: Apical: Pulse Radial: Resp: Lung Sounds: (L) / min Sitting Standing Lying (L) B/P (R) Pain Pain Type: Aching Dull Aching Constant Nagging Burning Gnawing
Preparing for Approaching Death
 Preparing for Approaching Death Old Colony Hospice created this guide for our hospice family and caregivers by revising and adapting the following journal article: Hospice Techniques: Preparing for the
Preparing for Approaching Death Old Colony Hospice created this guide for our hospice family and caregivers by revising and adapting the following journal article: Hospice Techniques: Preparing for the
To: Our Medicare Patients. Subject: Your Welcome to Medicare Exam
 To: Our Medicare Patients Subject: Your Welcome to Medicare Exam Medicare covers a one-time Welcome to Medicare visit. The Welcome to Medicare visit must occur during your first twelve months as a Medicare
To: Our Medicare Patients Subject: Your Welcome to Medicare Exam Medicare covers a one-time Welcome to Medicare visit. The Welcome to Medicare visit must occur during your first twelve months as a Medicare
Medicare & Dual Options Annual Comprehensive Exam FAX COMPLETED FORM TO: Patient Personal Information
 FAX COMPLETED FM TO: 877-682-2216 All fields marked with an * are required to be completed in order to receive payment for the ACE Form, unless indicated otherwise. Please refer to the document titled
FAX COMPLETED FM TO: 877-682-2216 All fields marked with an * are required to be completed in order to receive payment for the ACE Form, unless indicated otherwise. Please refer to the document titled
NORTHWICK PARK DEPENDENCY SCORE
 NORTHWICK PARK DEPENDENCY SCORE PATIENT DETAILS: Surname:... Forename(s):... Hosp No:... Sex: Male/Female Date of birth:... Diagnosis:... NHS No:. OCCASION: Admission / Fortnightly review /Discharge Date
NORTHWICK PARK DEPENDENCY SCORE PATIENT DETAILS: Surname:... Forename(s):... Hosp No:... Sex: Male/Female Date of birth:... Diagnosis:... NHS No:. OCCASION: Admission / Fortnightly review /Discharge Date
QM Reports Technical Specifications: Version 1.0
 Exhibit 271 Introduction The measures contained on the Quality Measure (QM) Reports are calculated in two major steps. In the first step, two samples of assessments are selected: a long-stay sample and
Exhibit 271 Introduction The measures contained on the Quality Measure (QM) Reports are calculated in two major steps. In the first step, two samples of assessments are selected: a long-stay sample and
Why Do I need an Annual Wellness Visit?
 Why Do I need an Annual Wellness Visit? To Our Medicare Patients: Medicare covers once a year wellness exam. There is no deductible, copay or coinsurance with your wellness visit. Medicare is very specific
Why Do I need an Annual Wellness Visit? To Our Medicare Patients: Medicare covers once a year wellness exam. There is no deductible, copay or coinsurance with your wellness visit. Medicare is very specific
PT Routine Total Joint Program Visit Note Page 1
 PT Routine Total Joint Program Visit Note Page 1 Vital Signs Temperature: Apical: Pulse Radial: Resp: Lung Sounds: (L) / min Sitting Standing Lying (L) B/P (R) Pain Pain Type: Aching Dull Aching Constant
PT Routine Total Joint Program Visit Note Page 1 Vital Signs Temperature: Apical: Pulse Radial: Resp: Lung Sounds: (L) / min Sitting Standing Lying (L) B/P (R) Pain Pain Type: Aching Dull Aching Constant
Chapter 18. Assisting With Urinary Elimination. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 18 Assisting With Urinary Elimination The urinary system: The Urinary System Removes waste products from the blood Maintains the body s water balance 2 Normal Urination The healthy adult produces
Chapter 18 Assisting With Urinary Elimination The urinary system: The Urinary System Removes waste products from the blood Maintains the body s water balance 2 Normal Urination The healthy adult produces
Medical condition SELF Mother Father Sibling (list brother or sister) Anxiety Bipolar disorder Heart Disease Depression Diabetes High Cholesterol
 PRE-EVALUATION FORM Medical condition SELF Mother Father Sibling (list brother or sister) Anxiety Bipolar disorder Heart Disease Depression Diabetes High Cholesterol High Blood Pressure Obesity Heart Defect
PRE-EVALUATION FORM Medical condition SELF Mother Father Sibling (list brother or sister) Anxiety Bipolar disorder Heart Disease Depression Diabetes High Cholesterol High Blood Pressure Obesity Heart Defect
Experiential Session on the Aging Process: Understanding What is Normal/Expected. Kathleen Fletcher RN DNP GNP-BC FAAN Lyn vander Sommen, MD, CPP
 Experiential Session on the Aging Process: Understanding What is Normal/Expected Kathleen Fletcher RN DNP GNP-BC FAAN Lyn vander Sommen, MD, CPP Multidimensional Aspects of Aging How We Live Now http://columbia.news21.com/2010/
Experiential Session on the Aging Process: Understanding What is Normal/Expected Kathleen Fletcher RN DNP GNP-BC FAAN Lyn vander Sommen, MD, CPP Multidimensional Aspects of Aging How We Live Now http://columbia.news21.com/2010/
Section K Swallowing/ Nutritional Status
 Instructor Guide Section K Swallowing/ Nutritional Status Objectives State the intent of Section K Swallowing and Nutritional Status. Describe how to conduct an assessment of a resident s nutritional status.
Instructor Guide Section K Swallowing/ Nutritional Status Objectives State the intent of Section K Swallowing and Nutritional Status. Describe how to conduct an assessment of a resident s nutritional status.
PAIN POINT CHECKLIST THE ULTIMATE TO MAXIMISE COMPENSATION FROM YOUR CLAIM
 THE ULTIMATE PAIN POINT CHECKLIST TO MAXIMISE COMPENSATION FROM YOUR CLAIM A visual checklist for personal injury claimants that allows users to comprehensively list and discuss their injuries with their
THE ULTIMATE PAIN POINT CHECKLIST TO MAXIMISE COMPENSATION FROM YOUR CLAIM A visual checklist for personal injury claimants that allows users to comprehensively list and discuss their injuries with their
Medicare Wellness Visit
 of Birth: Today s : Medicare Wellness Visit Dear Patient, Your Medicare benefits include an Annual Wellness Visit to assist in preventing illness or detect illness at an early stage. Your Annual Wellness
of Birth: Today s : Medicare Wellness Visit Dear Patient, Your Medicare benefits include an Annual Wellness Visit to assist in preventing illness or detect illness at an early stage. Your Annual Wellness
Change in Condition: When to report to the MD/NP/PA
 Change in Condition: When to report to the MD/NP/PA Immediate Notification Any symptom, sign or apparent discomfort that is: Acute or Sudden in onset, and: A Marked Change (i.e. more severe) in relation
Change in Condition: When to report to the MD/NP/PA Immediate Notification Any symptom, sign or apparent discomfort that is: Acute or Sudden in onset, and: A Marked Change (i.e. more severe) in relation
Difficulty breathing Altered level of consciousness Amputated arm
 Difficulty breathing 22-year-old male, severe difficulty breathing, chest sinks in on inspiration, respirations over 30/min, radial pulse present, responds to instructions. Altered level of consciousness
Difficulty breathing 22-year-old male, severe difficulty breathing, chest sinks in on inspiration, respirations over 30/min, radial pulse present, responds to instructions. Altered level of consciousness
Preparing for the Death of a Loved One. Information for Patients & Visitors
 Preparing for the Death of a Loved One Information for Patients & Visitors This booklet is provided to help you know what to expect when your loved one is dying. It may help you to respond in ways that
Preparing for the Death of a Loved One Information for Patients & Visitors This booklet is provided to help you know what to expect when your loved one is dying. It may help you to respond in ways that
Resource: Pain Assessments
 Pain assessment is an integral part of patient care. The patient s pain should be assessed at each visit using consistent assessment tools based on the patient s ability to communicate. For all pain scales
Pain assessment is an integral part of patient care. The patient s pain should be assessed at each visit using consistent assessment tools based on the patient s ability to communicate. For all pain scales
QUALITY INDICATORS FOR RESIDENTIAL CARE FACILITIES Maine Bureau of Medical Services
 1.) Prevalence of Bladder Incontinence (High Degree of Incontinence) Previous QI103 2.) Prevalence of Bladder Incontinence (Low Degree of Incontinence) Previous QI104 3.) Prevalence of Bowel Incontinence
1.) Prevalence of Bladder Incontinence (High Degree of Incontinence) Previous QI103 2.) Prevalence of Bladder Incontinence (Low Degree of Incontinence) Previous QI104 3.) Prevalence of Bowel Incontinence
Objectives. Major Changes to Section M. MDS 3.0 Section M Pressure Ulcers. Risk assessment Introduction of NPUAP guidelines
 MDS 3.0 Section M Pressure Ulcers Moderator: Barbara Baylis Sr. VP of Clinical and Residential Services, Kindred Healthcare Presenter: Glenda Mack, Sr. Director of Clinical Operations, Peoplefirst Rehabilitation
MDS 3.0 Section M Pressure Ulcers Moderator: Barbara Baylis Sr. VP of Clinical and Residential Services, Kindred Healthcare Presenter: Glenda Mack, Sr. Director of Clinical Operations, Peoplefirst Rehabilitation
Roy Zagieboylo, MD Assistant Professor University of Connecticut Family Medicine Department
 Roy Zagieboylo, MD Assistant Professor University of Connecticut Family Medicine Department That weight gaining diet I put you on is really working! This won t hurt me a bit. You re in good shape for the
Roy Zagieboylo, MD Assistant Professor University of Connecticut Family Medicine Department That weight gaining diet I put you on is really working! This won t hurt me a bit. You re in good shape for the
Stroke. Objectives: After you take this class, you will be able to:
 Stroke Objectives: After you take this class, you will be able to: 1. Describe the signs of a stroke and how a stroke happens. 2. Discuss stroke risk factors. 3. Detail the care and rehabilitation of a
Stroke Objectives: After you take this class, you will be able to: 1. Describe the signs of a stroke and how a stroke happens. 2. Discuss stroke risk factors. 3. Detail the care and rehabilitation of a
Recognizing Pressure Injury
 Recognizing Pressure Injury Karen Zulkowski, DNS, RN Hawaii Recorded on March 8, 2017 1 A Little About Myself Executive editor of the Journal of the World Council of Enterostomal Therapists (JWCET) and
Recognizing Pressure Injury Karen Zulkowski, DNS, RN Hawaii Recorded on March 8, 2017 1 A Little About Myself Executive editor of the Journal of the World Council of Enterostomal Therapists (JWCET) and
QUALITY MEASURES NELIA ADACI RNC, BSN, CDONA, C-NE, RAC-CT VICE PRESIDENT, THE CHARTS GROUP
 HCANJ QUALITY MEASURES NELIA ADACI RNC, BSN, CDONA, C-NE, RAC-CT VICE PRESIDENT, THE CHARTS GROUP 1 OUTLINE What are Quality Measures? 4 Purposes of QM s Key Definitions Review the QM s Managing the QM
HCANJ QUALITY MEASURES NELIA ADACI RNC, BSN, CDONA, C-NE, RAC-CT VICE PRESIDENT, THE CHARTS GROUP 1 OUTLINE What are Quality Measures? 4 Purposes of QM s Key Definitions Review the QM s Managing the QM
All Videos will be available through the Evolve.Elsevier Student Resource: Clinical Skills Essentials Collection, 1 st Ed.
 1 NURS 0951 VOCATIONAL NURISNG PROGRAM FALL 2016 SKILLS LAB SCHEDULE The COS Nursing Lab Website can be found at www.cosnursinglab.weebly.com All Videos will be available through the Evolve.Elsevier Student
1 NURS 0951 VOCATIONAL NURISNG PROGRAM FALL 2016 SKILLS LAB SCHEDULE The COS Nursing Lab Website can be found at www.cosnursinglab.weebly.com All Videos will be available through the Evolve.Elsevier Student
ADULT QUESTIONNAIRE. Date of Birth: Briefly describe the history and development of this issue from onset to present.
 ADULT QUESTIONNAIRE Name: Address: Preferred phone number to reach you: Is it okay to leave a message? Yes No (Please check one) Date of Birth: Reason(s) for seeking treatment at this time? Briefly describe
ADULT QUESTIONNAIRE Name: Address: Preferred phone number to reach you: Is it okay to leave a message? Yes No (Please check one) Date of Birth: Reason(s) for seeking treatment at this time? Briefly describe
DANA COKER KINGDON, PA
 PERSONAL HEALTH HISTORY AGNES KINRA, MD, PA Board Certified in Internal Medicine DANA COKER KINGDON, PA 4104 West 15 th St # 101 Plano, TX 75093 Phone 972-596-0006 Fax 972-596-0904 Name (Last, First, M.I.):
PERSONAL HEALTH HISTORY AGNES KINRA, MD, PA Board Certified in Internal Medicine DANA COKER KINGDON, PA 4104 West 15 th St # 101 Plano, TX 75093 Phone 972-596-0006 Fax 972-596-0904 Name (Last, First, M.I.):
Geriatric Pain Assessment and Management. Robin Arends, DNP, CNP, FNP-BC
 + Geriatric Pain Assessment and Management Robin Arends, DNP, CNP, FNP-BC + Objectives List three reasons why elderly are less likely to report pain. List three barriers to pain management Describe two
+ Geriatric Pain Assessment and Management Robin Arends, DNP, CNP, FNP-BC + Objectives List three reasons why elderly are less likely to report pain. List three barriers to pain management Describe two
Pressure Ulcer Staging. Staging of Wounds are based on the deepest level of tissue damage
 Pressure Ulcer Staging Staging of Wounds are based on the deepest level of tissue damage Pressure Ulcer Staging New Pressure Ulcer Staging Stage I Stage II Stage III Stage IV Unstageable Suspected Deep
Pressure Ulcer Staging Staging of Wounds are based on the deepest level of tissue damage Pressure Ulcer Staging New Pressure Ulcer Staging Stage I Stage II Stage III Stage IV Unstageable Suspected Deep
Total Knee Replacement: Your Guide to Preparation and Recovery
 Total Knee Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 5 After Surgery.............................
Total Knee Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 5 After Surgery.............................
PRE-VISIT QUESTIONNAIRE FOR NEW PATIENTS
 UF Health Senior Care PO Box 100383 Gainesville, FL 32608 352-265-0615 Fax 352-294-5803 PRE-VISIT QUESTIONNAIRE FOR NEW PATIENTS Please complete this questionnaire at home and bring it with you to the
UF Health Senior Care PO Box 100383 Gainesville, FL 32608 352-265-0615 Fax 352-294-5803 PRE-VISIT QUESTIONNAIRE FOR NEW PATIENTS Please complete this questionnaire at home and bring it with you to the
NUTRITION CARE ALERTS
 APPENDIX 10 A NUTRITION CARE ALERTS and for Caregivers in Nursing Facilities or at Home Proper nutrition care is vital to the health and well-being of nursing facility residents and seniors living in their
APPENDIX 10 A NUTRITION CARE ALERTS and for Caregivers in Nursing Facilities or at Home Proper nutrition care is vital to the health and well-being of nursing facility residents and seniors living in their
Dexamethasone is used to treat cancer. This drug can be given in the vein (IV), by mouth, or as an eye drop.
 Dexamethasone Other Names: Decadron About This Drug Dexamethasone is used to treat cancer. This drug can be given in the vein (IV), by mouth, or as an eye drop. Possible Side Effects (More Common) Increased
Dexamethasone Other Names: Decadron About This Drug Dexamethasone is used to treat cancer. This drug can be given in the vein (IV), by mouth, or as an eye drop. Possible Side Effects (More Common) Increased
Annual Wellness Visit Form 2016
 Annual Wellness Visit Form 6 Initial G48/Subsequent G49 (circle one) Subjective: Past Medical History (mark X to confirm and note duration for chronic conditions only) Conditions Yrs Conditions Yrs Others:
Annual Wellness Visit Form 6 Initial G48/Subsequent G49 (circle one) Subjective: Past Medical History (mark X to confirm and note duration for chronic conditions only) Conditions Yrs Conditions Yrs Others:
Proof 2. CLINICAL PATHWAY PLAN CLINIQUE GENERAL SURGERY CHIRURGIE GÉNÉRAL Enhanced Recovery After Surgery (ERAS) Bowel Surgery /
 CLINICAL PATHWAY PLAN CLINIQUE GENERAL SURGERY CHIRURGIE GÉNÉRAL Enhanced Recovery After Surgery (ERAS) Bowel Surgery / Proof 2 Addressograph/Plaque Cancer Assessment Clinic (CAC) Date: yyaa mm dj Day
CLINICAL PATHWAY PLAN CLINIQUE GENERAL SURGERY CHIRURGIE GÉNÉRAL Enhanced Recovery After Surgery (ERAS) Bowel Surgery / Proof 2 Addressograph/Plaque Cancer Assessment Clinic (CAC) Date: yyaa mm dj Day
Capital Health Medical Center - Hopewell NEUROSURGICAL-ONCOLOGY Patient History
 Capital Health Medical Center - Hopewell NEUROSURGICAL-ONCOLOGY Patient History Please take a few minutes and complete the following questions before you see the doctors so that we may learn a bit more
Capital Health Medical Center - Hopewell NEUROSURGICAL-ONCOLOGY Patient History Please take a few minutes and complete the following questions before you see the doctors so that we may learn a bit more
History Form for Exceptional Home-Based Care
 Patient Name: ; Birth date: / / ; Date: / / Person filling out form: ; Relationship: Thank you for taking the time to fill out this valuable information. This allows us to provide the best care possible
Patient Name: ; Birth date: / / ; Date: / / Person filling out form: ; Relationship: Thank you for taking the time to fill out this valuable information. This allows us to provide the best care possible
Preventing delirium while in the hospital
 Preventing delirium while in the hospital What is delirium? When an older person becomes ill and goes into the hospital, there is an increased risk of developing delirium and other problems. Delirium is
Preventing delirium while in the hospital What is delirium? When an older person becomes ill and goes into the hospital, there is an increased risk of developing delirium and other problems. Delirium is
LUNCH WITH THE EXPERTS: Palliative Care for Advanced Dementia with Pain and Dementia
 LUNCH WITH THE EXPERTS: Palliative Care for Advanced Dementia with Pain and Dementia Carol Long, PhD, RN, FPCN Principal, Capstone Healthcare & Co-Director, Palliative Care for Advanced Dementia, Beatitudes
LUNCH WITH THE EXPERTS: Palliative Care for Advanced Dementia with Pain and Dementia Carol Long, PhD, RN, FPCN Principal, Capstone Healthcare & Co-Director, Palliative Care for Advanced Dementia, Beatitudes
Schodack Internal Medicine and Pediatrics. Annual Physical-Female
 Schodack Internal Medicine and Pediatrics Annual Physical-Female Please Fill out this form (or have your caregiver complete it) and discuss with your medical provider. Thank you! Please Mark the preferred
Schodack Internal Medicine and Pediatrics Annual Physical-Female Please Fill out this form (or have your caregiver complete it) and discuss with your medical provider. Thank you! Please Mark the preferred
Pressure Ulcer. Patient information leaflet. Category I. Category II. Category III. Category IV. Unstageable. Deep Tissue Injury
 Pressure Ulcers Patient information leaflet Pressure Ulcer Category I Category II Category III Category IV Unstageable Deep Tissue Injury Introduction This leaflet is about pressure ulcers and includes
Pressure Ulcers Patient information leaflet Pressure Ulcer Category I Category II Category III Category IV Unstageable Deep Tissue Injury Introduction This leaflet is about pressure ulcers and includes
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
Wound Care Program for Nursing Assistants-
 Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Determining Wound Diagnosis and Documentation Tips Job Aid
 Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
Determining Wound Diagnosis and Job Aid 1 Coding Is this a traumatic injury from an accident? 800 Codes - Injury Section of the Coding Manual Code by specific site of injury. Only use for accidents or
Patient Name: Date: Address: Primary Care Physician: Online Website On TV In print On the radio
 927 W. Myrtle St. Boise, ID 83702 (208) 947-0100 NEW PATIENT INTAKE Patient Name: Date: Email Address: Primary Care Physician: How did you hear about AVT? (Please mark all that apply) Online Website On
927 W. Myrtle St. Boise, ID 83702 (208) 947-0100 NEW PATIENT INTAKE Patient Name: Date: Email Address: Primary Care Physician: How did you hear about AVT? (Please mark all that apply) Online Website On
DEEP BRAIN STIMULATION SURGICAL CANDIDACY EVALUATION FORM
 Name: MR#: Date: DEEP BRAIN STIMULATION SURGICAL CANDIDACY EVALUATION FORM Referring Physician s Name: Primary Care Provider s Name: 1. What was/were your first movement disorder symptoms? What did you
Name: MR#: Date: DEEP BRAIN STIMULATION SURGICAL CANDIDACY EVALUATION FORM Referring Physician s Name: Primary Care Provider s Name: 1. What was/were your first movement disorder symptoms? What did you
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person
 Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Clinical Information for Wheeled Mobility Page 1 of 6
 Clinical Information for Wheeled Mobility Page 1 of 6 PART A: PATIENT / PROVIDER INFORMATION - Please Print Name: Sponsor Soc. Sec. No: Address: City: St: Zip: Phone: ( ) Age: Sex: Height: Weight: Date
Clinical Information for Wheeled Mobility Page 1 of 6 PART A: PATIENT / PROVIDER INFORMATION - Please Print Name: Sponsor Soc. Sec. No: Address: City: St: Zip: Phone: ( ) Age: Sex: Height: Weight: Date
HISTORY OF PRESENT ILLNESS A. TELL US ABOUT YOUR PAIN PROBLEM
 1 UT Health Austin Comprehensive Pain Management New Patient Questionnaire Thank you for scheduling a visit with the Comprehensive Pain Management Care Team. The responses you provide to these questions
1 UT Health Austin Comprehensive Pain Management New Patient Questionnaire Thank you for scheduling a visit with the Comprehensive Pain Management Care Team. The responses you provide to these questions
Health Intake Form. List your top five concerns or reasons for requesting your appointment with Dr. Weiss
 List your top five concerns or reasons for requesting your appointment with Dr. Weiss 1. 2. 3. 4. 5. Please give any information you think is important regarding these top concerns: Health Intake Form
List your top five concerns or reasons for requesting your appointment with Dr. Weiss 1. 2. 3. 4. 5. Please give any information you think is important regarding these top concerns: Health Intake Form
Physical/Emotional Symptoms and Appropriate Comfort Measures
 Physical/Emotional Symptoms and Appropriate Comfort Measures A. Diminishing Appetite Page 2 B. Decreased Socialization Page 2 C. Sleeping Page 2 E. Changes in Pain Level Page 3 D. Incontinence Page 3 F.
Physical/Emotional Symptoms and Appropriate Comfort Measures A. Diminishing Appetite Page 2 B. Decreased Socialization Page 2 C. Sleeping Page 2 E. Changes in Pain Level Page 3 D. Incontinence Page 3 F.
Enhanced Recovery Patient Diary
 Enhanced Recovery Patient Diary I found the diary was helpful. I was able to chart my progress and see a difference. I was eating more each day and able to shower myself. I found it to be encouraging.
Enhanced Recovery Patient Diary I found the diary was helpful. I was able to chart my progress and see a difference. I was eating more each day and able to shower myself. I found it to be encouraging.
Chapter 19. Nutrition and Fluids. All items and derived items 2015, 2011 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved.
 Chapter 19 Nutrition and Fluids Nutrition Nutrition--processes involved in the ingestion, digestion, absorption & use of foods & fluids by the body. The person s diet affects physical & mental wellbeing
Chapter 19 Nutrition and Fluids Nutrition Nutrition--processes involved in the ingestion, digestion, absorption & use of foods & fluids by the body. The person s diet affects physical & mental wellbeing
Symptom Review (page 1) Name Date
 v2.4, 2/13 JonathanTreasure.com Botanical Medicine & Cancer Herb Drug Interactions Herbalism 3.0 Symptom Review (page 1) Name Date INSTRUCTIONS Please read each section below carefully and, after each
v2.4, 2/13 JonathanTreasure.com Botanical Medicine & Cancer Herb Drug Interactions Herbalism 3.0 Symptom Review (page 1) Name Date INSTRUCTIONS Please read each section below carefully and, after each
To insure that your physical examination is of the highest quality and comfort, please observe the following:
 Dear Patient: To insure that your physical examination is of the highest quality and comfort, please observe the following: PHYSICAL EXAM NOTES Please bring the Physical Exam forms completely filled out
Dear Patient: To insure that your physical examination is of the highest quality and comfort, please observe the following: PHYSICAL EXAM NOTES Please bring the Physical Exam forms completely filled out
Patient & Family Guide. Bowel Surgery.
 Patient & Family Guide 2016 Bowel Surgery www.nshealth.ca Bowel Surgery This pamphlet will answer some of your questions about your stay in hospital and care at home. We hope this information will help
Patient & Family Guide 2016 Bowel Surgery www.nshealth.ca Bowel Surgery This pamphlet will answer some of your questions about your stay in hospital and care at home. We hope this information will help
Treatment Definitions. Behavior:
 Behavior: Treatment Definitions Behavior (Consult with skilled professional): Consulting with a professional for assistance in dealing with severe behavioral issues. A professional may be a physician,
Behavior: Treatment Definitions Behavior (Consult with skilled professional): Consulting with a professional for assistance in dealing with severe behavioral issues. A professional may be a physician,
Faces Pain Scale Hurts just. Hurts a little more. Hurts even Hurts a a little bit
 Faces Pain Scale 0 2 4 6 8 10 Hurts just Hurts even Hurts a a little bit more whole lot Very happy, no hurt Hurts a little more Hurts as much as you can imagine (don t have to be crying to feel this much
Faces Pain Scale 0 2 4 6 8 10 Hurts just Hurts even Hurts a a little bit more whole lot Very happy, no hurt Hurts a little more Hurts as much as you can imagine (don t have to be crying to feel this much
IRECA BLS Challenge 2015 Scenario 1
 Scenario 1 Team Name Team Number Captain Name Judge 1 # Judge 2 # JUDGE S SHEET Overview: This scenario challenges the competitors to use basic triage techniques and then to do the most good for the most
Scenario 1 Team Name Team Number Captain Name Judge 1 # Judge 2 # JUDGE S SHEET Overview: This scenario challenges the competitors to use basic triage techniques and then to do the most good for the most
WELCOME TO THE NORTHSHORE UNIVERSITY HEALTHSYSTEM SLEEP CENTERS
 WELCOME TO THE NORTHSHORE UNIVERSITY HEALTHSYSTEM SLEEP CENTERS Prior to your office visit, we request that you complete this questionnaire. It asks questions not only about your sleeping habits and behavior
WELCOME TO THE NORTHSHORE UNIVERSITY HEALTHSYSTEM SLEEP CENTERS Prior to your office visit, we request that you complete this questionnaire. It asks questions not only about your sleeping habits and behavior
Care Home Staffing Project
 Care Home Staffing Project A revised questionnaire suitable for use in care homes for older people has been designed based on the Indicator of Relative Need (IoRN). The revised questionnaire has taken
Care Home Staffing Project A revised questionnaire suitable for use in care homes for older people has been designed based on the Indicator of Relative Need (IoRN). The revised questionnaire has taken
Form 1: Modified Resident s Verbal Pain Inventory (M-RVBPI)
 Form 1: Modified Resident s Verbal Pain Inventory (M-RVBPI) te: This questionnaire is to be answered at interview Date: Time: Name: 1. Have you had any pain in the last 24 hours? Prompts: An ache; feeling
Form 1: Modified Resident s Verbal Pain Inventory (M-RVBPI) te: This questionnaire is to be answered at interview Date: Time: Name: 1. Have you had any pain in the last 24 hours? Prompts: An ache; feeling
Total Hip Replacement: Your Guide to Preparation and Recovery
 Total Hip Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 6 After Surgery.............................
Total Hip Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 6 After Surgery.............................
Patient Questionnaire
 Name: DOB: Date of Visit: Patient Questionnaire Social History Yes No Do you eat a healthy balanced diet with minimal salt and bad fats? For Example: Balanced Diet = Combination of fruits, vegetables,
Name: DOB: Date of Visit: Patient Questionnaire Social History Yes No Do you eat a healthy balanced diet with minimal salt and bad fats? For Example: Balanced Diet = Combination of fruits, vegetables,
Advanced Clinical Solutions. Pressure Ulcer. Carilex Medical Group 1
 Advanced Clinical Solutions Pressure Ulcer Carilex Medical Group 1 Advanced Clinical Solutions Contents About Pressure Ulcer! 2 Stages of Pressure Ulcer! 5 Reference! 7 Carilex Medical Group 1 About Pressure
Advanced Clinical Solutions Pressure Ulcer Carilex Medical Group 1 Advanced Clinical Solutions Contents About Pressure Ulcer! 2 Stages of Pressure Ulcer! 5 Reference! 7 Carilex Medical Group 1 About Pressure
Change in Condition: When to report to the MD/NP/PA
 Change in Condition: When to report to the MD/NP/PA Immediate Notification Any symptom, sign or apparent discomfort that is: Acute or Sudden in onset, and: A Marked Change (i.e. more severe) in relation
Change in Condition: When to report to the MD/NP/PA Immediate Notification Any symptom, sign or apparent discomfort that is: Acute or Sudden in onset, and: A Marked Change (i.e. more severe) in relation
STEP 1: Forms Please complete all the attached forms and bring them with you on the day of your visit.
 PATIENT HEALTH HISTORY FORM DIRECTIONS AND VISIT DAY INSTRUCTIONS Prior to your Appointment: STEP 1: Forms Please complete all the attached forms and bring them with you on the day of your visit. STEP
PATIENT HEALTH HISTORY FORM DIRECTIONS AND VISIT DAY INSTRUCTIONS Prior to your Appointment: STEP 1: Forms Please complete all the attached forms and bring them with you on the day of your visit. STEP
Esophagectomy Surgery
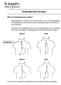 Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Type 2 Diabetes. Care for your body today for a healthier tomorrow
 Type 2 Diabetes Care for your body today for a healthier tomorrow Understanding diabetes You may already know that having diabetes means you have too much sugar in your blood. Why do you have high blood
Type 2 Diabetes Care for your body today for a healthier tomorrow Understanding diabetes You may already know that having diabetes means you have too much sugar in your blood. Why do you have high blood
HIP REPLACEMENT SURGERY
 HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
SLEEP HISTORY QUESTIONNAIRE
 Date of birth: Today s date: Dear Patient: SLEEP HISTORY QUESTIONNAIRE Thank you for taking the time to fill out a sleep history questionnaire. This will help our healthcare team to provide the best possible
Date of birth: Today s date: Dear Patient: SLEEP HISTORY QUESTIONNAIRE Thank you for taking the time to fill out a sleep history questionnaire. This will help our healthcare team to provide the best possible
The OK Health Check. For assessing and planning the Health Care Needs of People with Learning Disabilities. Client Assessment Sheets. Address
 The OK Health Check For assessing and planning the Health Care Needs of People with Learning Disabilities Client Assessment Sheets Name (1)... Address......... Date... fairfield PUBLICATIONS PC Based Record
The OK Health Check For assessing and planning the Health Care Needs of People with Learning Disabilities Client Assessment Sheets Name (1)... Address......... Date... fairfield PUBLICATIONS PC Based Record
Prevention and management of Pressure ulcers
 Prevention and management of Pressure ulcers A guide for patients, carers and relatives What is a pressure ulcer? Pressure ulcers are an injury to the skin and/or underlying tissues. They are also known
Prevention and management of Pressure ulcers A guide for patients, carers and relatives What is a pressure ulcer? Pressure ulcers are an injury to the skin and/or underlying tissues. They are also known
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions
 Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Test your Knowledge: Recognizing Delirium
 The Ottawa Hospital Name: Unit: Profession: RN RPN PT OT SW Other Note: Each question has only one correct answer. 1. If a patient is identified as being at high risk for developing delirium, his/her mental
The Ottawa Hospital Name: Unit: Profession: RN RPN PT OT SW Other Note: Each question has only one correct answer. 1. If a patient is identified as being at high risk for developing delirium, his/her mental
Everolimus (Afinitor )
 Everolimus (Afinitor ) ( e-ver-oh-li-mus ) How drug is given: By mouth Purpose: to slow the growth of cancer cells in kidney cancer and other cancers How to take the drug Take with or without food and
Everolimus (Afinitor ) ( e-ver-oh-li-mus ) How drug is given: By mouth Purpose: to slow the growth of cancer cells in kidney cancer and other cancers How to take the drug Take with or without food and
Chapter 21. Assisting With Assessment. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 21 Assisting With Assessment Vital Signs Vital signs reflect three body processes: Regulation of body temperature Breathing Heart function A person s vital signs: Vary within certain limits Are
Chapter 21 Assisting With Assessment Vital Signs Vital signs reflect three body processes: Regulation of body temperature Breathing Heart function A person s vital signs: Vary within certain limits Are
Women s and Men s Health Intake Form Comprehensive Physical Therapy Center
 Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Pressure Ulcers Patient Information Leaflet
 Pressure Ulcers Patient Information Leaflet Shining a light on the future Introduction This leaflet is about pressure ulcers and includes information about what they are what can cause them and how they
Pressure Ulcers Patient Information Leaflet Shining a light on the future Introduction This leaflet is about pressure ulcers and includes information about what they are what can cause them and how they
Pressure Ulcers Patient Information Leaflet
 Further information about the content, reference sources or production of this leaflet can be obtained from the Patient Information Centre. Pressure Ulcers Patient Information Leaflet This information
Further information about the content, reference sources or production of this leaflet can be obtained from the Patient Information Centre. Pressure Ulcers Patient Information Leaflet This information
CASE STUDY RESIDENT WITH SENILE DEMENTIA
 CASE STUDY RESIDENT WITH SENILE DEMENTIA INFORMATION COLLECTION Mr. Frank Miller, 72 years old Occupation: Has recently worked for the building authority Social situation: widowed, recently he lived with
CASE STUDY RESIDENT WITH SENILE DEMENTIA INFORMATION COLLECTION Mr. Frank Miller, 72 years old Occupation: Has recently worked for the building authority Social situation: widowed, recently he lived with
