PUMANI bcpap GUIDELINES FOR CLINICIANS. An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use
|
|
|
- Bryan McGee
- 6 years ago
- Views:
Transcription
1 An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use
2 What is bcpap? bcpap stands for bubble Continuous Positive Airway Pressure. Sometimes called Continuous Distending Pressure, it is a constant pressure applied to the airway, generated by continuous, consistent flow of air during inspiration and expiration, with the aim of opening collapsed lung segments and maintaining patency in already opened air spaces. bcpap is now being introduced in Malawi as the next step in the management of severe respiratory distress in children after nasal prong oxygen. Why bcpap now? Respiratory problems are the most common cause of illness and death in children. Respiratory distress syndrome, meconium aspiration and pneumonia are examples of common causes of respiratory distress in neonates, while bronchiolitis and pneumonia predominate among older infants. In Malawian hospitals, there is no additional help available for children whose severe respiratory distress fails to respond to oxygen therapy. Studies have shown that introducing bcpap could improve survival in babies with severe respiratory disease by about 70%. Recently, a low cost bubble CPAP system has been designed and tested at Queen Elizabeth Central Hospital, with good results, which offers hope to neonatal and paediatric patients with respiratory distress who fail to improve on oxygen. A bcpap in use in the neonatal ward of QECH in March What happens when a child has a respiratory problem? In most respiratory diseases there is effectively a reduction in the amount of air exchanged in the alveoli. This might result from a reduction in the amount of air taken in from the outside; a reduction in the alveolar surface available for gas exchange or a reduction in the haemoglobin available to carry oxygen and carbon dioxide to and from the lungs. We will describe how these mechanisms come into play in some of the common causes of respiratory distress in children. These are some of the common respiratory diseases in neonates and young children: 1. Respiratory Distress Syndrome, RDS (also called Hyaline Membrane Disease, HMD) a. Lung is not mature and alveoli not well developed b. Thick sticky substance fills the alveoli c. Lung is solidified d. Insufficient levels of surfactant result in alveolar walls sticking in or collapsing in e. As a result, lungs cannot expand well f. The patient needs a lot of effort to initially open the stiff lungs and to keep the lungs open 2
3 2. Pneumonia/pneumonitis a. There is an inflammatory process going on in the lungs due to infection or other agents b. Lungs are swollen and firm c. Thick exudate fills the alveoli d. Some surfactant is destroyed during the inflammatory process e. As a result, areas of the lung will not expand well while others will collapse f. Additional effort or pressure is needed to open the lungs and to prevent them from collapsing back 3. Airway Obstruction a. Depends on cause and level of obstruction b. Mostly there is swelling of the lining of the airway, reducing the lumen c. The status in a and b will result in more effort needed to move air in and out through the airway, depending on the level of the obstruction d. Sometimes thick secretions in airway and/or the alveoli e. Might have segments of collapse, while others might be hyper-expanded f. Either the lung cannot expand, or cannot ventilate The major effect of these pathologies is to reduce the lung surface area available for gaseous exchange, resulting in hypoxia. Respiratory Distress Respiratory distress describes a response to the hypoxia. Initially the body fights to maintain oxygen levels delivered to the brain by increasing the work of the cardiovascular and respiratory systems. Clinically the patient will demonstrate the following: 1. Increased respiratory rate and heart rate 2. Chest in-drawings and use of accessory muscles 3. Grunting and nasal flaring 4. Poor feeding 5. Low oxygen saturations As the hypoxia progresses, the patient might become pale and cyanosed, and the level of consciousness may deteriorate. The aim of treatment in a patient with respiratory distress is to achieve better oxygenation and reverse the hypoxia and therefore improve some of the signs that are mentioned above. How does the bcpap help? On inspiration, bcpap drives air with additional pressure into collapsed alveoli and opens them. This is like what happens when you first blow into a collapsed balloon. This process is sometimes called recruitment. Because of the continuous airflow, this pressure is maintained even when the patient breathes out and therefore the alveoli do not collapse at the end of expiration. This makes the lungs expand more easily and increases the surface area available for gaseous exchange and therefore improves oxygenation. This in turn reduces the need for increased work of breathing. 3
4 When does my patient need bcpap? bcpap is usually used as the next step in respiratory therapy after oxygen in patients who present with respiratory distress. Therefore the majority of the patients who go on bcpap treatment will be those who remain with severe respiratory distress despite oxygen therapy. However, some patients might require bcpap right from the beginning judging from the degree of distress and the overall clinical picture. As a guide, patients with the following conditions can benefit from bcpap: 1. Respiratory distress syndrome 2. Meconium aspiration syndrome 3. Transient tachypnoea of the newborn (TTN) 4. All forms of pneumonia or pneumonitis 5. Bronchiolitis 6. Apnoea of prematurity 7. Lung collapse / atelectasis 8. Upper airway obstruction 9. Pneumocystis Pneumonia (PCP) All other indications should be discussed with senior clinicians in your hospital. In the situation where you have a child with severe respiratory distress and cannot be sure about the differential diagnosis, it will be safer to start the bcpap and then discuss with more senior people on how to proceed. Always remember that clinicians at the district or central hospitals in your service area should be at your disposal to give advice where you have questions about specific patients. Specific indications for bcpap Signs of severe respiratory distress as defined by the WHO: 1. Tachypnoea 2. Severe subcostal or intercostal recessions 3. Use of accessory muscles 4. Nasal flaring 5. Grunting; particularly in small babies, the presence of grunting represents a patient who may be struggling to maintain Positive End Expiratory Pressure (PEEP) and therefore may benefit from bcpap 6. Oxygen saturations below 90% despite 2 L/min of oxygen therapy 7. Cyanosis 8. Agitation / restlessness 9. Breathlessness / exhaustion 4
5 Patients who might not benefit from bcpap: 1. Patients who do not have severe respiratory distress 2. Patients whose respiratory distress improves on 2 L/min of oxygen or less 3. Upper airway abnormalities such as choanal atresia, tracheosophageal atresia/fistula, cleft palate 4. Severe cardiovascular instability and impending arrest 5. Absent respiratory drive/effort 6. Profound sepsis and shock 7. Congenital diaphragmatic hernia 8. Severe birth asphyxia The Pumani bcpap Machine All bcpap machines consist of four basic elements. The first is a high flow air pump run from a power source. Then there must be a conduit for air from the pump, through a flow valve with an air gauge to regulate airflow and then to a pressure regulator and patient interface. In the Pumani bcpap machine (pictured below), which is being rolled out in Malawi, two aquarium pumps powered by electrical mains and housed in a metal container provide the flow. The flow valves are attached on the outside front of the unit. A water bottle on the right side of the machine serves as a pressure regulator. The outlet to the patient interface is located on the front of the unit. Additionally, an inlet from an oxygen source is provided for attachment when a patient requires oxygen in addition to the bcpap flow and pressure. The oxygen flow is regulated either on the oxygen concentrator gauge or through the gauge on the bcpap unit itself. The oxygen and blended flows are set on the bcpap using the table below (also found in the Pumani User Manual). 5
6 Commencing a patient on bcpap Requirements: PUMANI bcpap GUIDELINES FOR CLINICIANS 1. Air flow and pressure source (Pumani bcpap machine) 2. Oxygen source (oxygen concentrator) 3. Power supply (Power cable should be attached from the back of the machine) 4. Bottle tubing, patient tubing 5. Hat, nasal prongs (sizes 1-4, depending on the size of the patient s nostrils), safety pins, elastics 6. Orogastric tubes 7. Suction machine and catheters 8. Saline drops 9. Pulse oximeter 10. Respiratory Rate timer Setting up a Patient on the Pumani bcpap Machine Location. The bcpap machine should be set up in the high care area / corner of your paediatric / neonatal ward to ensure above average monitoring. If possible, this location should be close to the nursing station so that the nursing staff can always easily keep an eye on the patient. It works better if all patients on bcpap are nursed close together instead of being scattered in different corners of the ward. Setting up the machine. If you have a patient with severe respiratory distress, first of all carry out the necessary ABC assessment. 1. Put the patient on nasal prong oxygen, starting with 1 L/min and assess response. Increase the oxygen flow to 2 L/min if there is no response. If at 2 L/min O2 administration there are still signs of severe distress or saturation below 90%, increase the oxygen flow to the maximum flow rate and, if possible, use face mask oxygen and then start setting up the bcpap. Face masks should be run with at least 5 liters of oxygen. Make sure you keep an eye on the patient while setting up the machine. 2. Check to ensure that the bcpap machine is in working order, the power is connected, and that the oxygen concentrator, tubings and attachments are all available 3. Fill the bottle with tap water, up to 6 cm 4. Connect the bottle tubing to the bottle connector (labeled with an picture of a bottle) and the patient tubing to the patient connector (labeled with a picture of a baby) 5. Start all patients on the following flow settings: Total Air flow at 6 L/min 6
7 Oxygen flow: o o Neonates: 3 L/min Patients over 1 month old: 4 L/min Preparing & inserting the prongs. Do not insert the prongs without the machine on. 1. Select appropriate sizes for the prongs and hat 2. Transfer the patient, while still on oxygen, to the CPAP bed or warming crib 3. Clean the nose with water; gently suction nostrils 4. Insert orogastric tube for feeds and for deflating the abdomen 5. Place hat on the baby 6. Ensure the nostrils are open, apply 2 drops of saline to each nostril to keep the nostrils open and moist 7. Attach the prongs to the hat with the pins and elastics 8. Remove the oxygen tubing immediately before inserting the nasal prongs 9. Put the nasal prongs far enough into the nose to completely fill the nostril, but maintain at least ¼ cm of space between the prongs and septum 10. Check for bubbling water in the bottle. If bubbling does not occur, check that the prongs fill the nostrils completely, that the tubings are well connected and are not kinking. Try increasing the total flow by 1 L at a time, up to 10 L/min. Monitoring patients on bcpap Patients on bcpap (as any other very sick patient) require more than average routine monitoring. However, this will depend on the nursing capacity on the ward. To ensure that the aim of providing bcpap to patients is achieved, the following standard of monitoring should be provided as a minimum: About an hour after putting a patient on bcpap, the patient should be reviewed and the following recorded in the notes: airway patency, current bcpap settings (water level, Total flow, Oxygen flow), RR, HR, grunting, nasal flaring, oxygen saturations, recessions, abdominal distention, and general clinical condition. This is useful in terms of reviewing response to bcpap and in helping to decide whether to change the bcpap settings or not. If there is no improvement in oxygen saturations: 1. Check the tubings; ensure all connections are correct and no kinking 2. Check the airway; apply saline drops to nose and suction thoroughly 3. Check for abdominal distension; aspirate stomach and leave OGT to openly drain 4. Increase oxygen flow by 0.5 L 7
8 5. Then increase the pressure by 1 cm water at a time, to a maximum of 8 cm (any further increase in pressure must be made by a registrar or consultant) 6. Call registrar or Medical Officer to review patient or help with management Then patients on bcpap should be reviewed at least every 6 hours; the above details recorded, and appropriate steps taken. Weaning a Patient off of bcpap Start weaning the patient on bcpap once the patient is clinically stable and the following criteria are achieved: 1. Patient has been on bcpap at least 24 hours 2. RR less than 60/minute for at least 6 hours (for neonates) 3. Oxygen saturation consistently > 90% for at least 6 hours 4. No significant grunting, recessions, nasal flaring, apnoea or bradycardia for at least 6 hours Procedure for weaning bcpap: 1. Decrease Water Level by 1 cm Every 6 hours until 5 cm level is reached Wait 6 hours to allow the patient to settle 2. Decrease Oxygen Flow by 0.5 L Every 6 hours until 1 L/min flow is reached Wait 6 hours to allow the patient to settle 3. Remove patient from CPAP and place on 2 L of O 2 1 Hour Later 6 Hours Later 12 Hours Later Assess patient Assess patient Assess patient Continue assessing every 12 hours 8
9 Flow chart for weaning: PUMANI bcpap GUIDELINES FOR CLINICIANS 9
10 Complications of bcpap PUMANI bcpap GUIDELINES FOR CLINICIANS Blocked nostrils Very common. Prevent and treat by regular saline drops and gentle suctioning. Nasoseptal irritation or necrosis Septal irritation common, necrosis less common. Prevented by careful selection of nasal prong sizes and not inserting the prongs too far into the nostrils. Further prevented by regular application of saline drops to the nostrils to prevent drying and crusting of the nasal mucosa. Distended abdomen This is common but prevented and treated by inserting an orogastric tube. You may need to aspirate stomach contents or leave the OGT on free drainage. Nose bleed Common in the dry season. Prevent and treat by applying regular nasal saline drops. Pneumothorax This is very uncommon. Usually due to excessive pressures applied to small, stiff lungs. Suspect if there is a sudden deterioration in respiration and oxygenation in a patient who was doing well on bcpap or a patient who seems to be worse after starting bcpap. Any patient not responding to CPAP of 8 cm water should be reviewed by a senior or trained clinician. Pulmonary haemorrhage This is very uncommon. Also due to very high pressures applied to small, immature lungs. Suspect if there is sudden deterioration in clinical condition, especially if there is associated pallor and significant bloody frothing from mouth or nose. Can be prevented by being cautious with the pressures applied to the baby s lungs. Any patient not responding to CPAP of 8 cm water should be reviewed by a senior or trained clinician. Restarting bcpap The criteria and procedure for restarting bcpap are the same as for the initial commencement as listed above. Restarting bcpap will also be subject to availability of a bcpap machine and at the reviewing clinician s discretion. Queries Further information about the Pumani bcpap machine, troubleshotting, patient set-up, etc. is available in the Pumani bcpap User Manual. 10
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION
 CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
Practical Application of CPAP
 CHAPTER 3 Practical Application of CPAP Dr. Srinivas Murki Neonatologist Fernadez Hospital, Hyderabad. A.P. Practical Application of CPAP Continuous positive airway pressure (CPAP) applied to premature
CHAPTER 3 Practical Application of CPAP Dr. Srinivas Murki Neonatologist Fernadez Hospital, Hyderabad. A.P. Practical Application of CPAP Continuous positive airway pressure (CPAP) applied to premature
Part I: How to Assemble the Pumani CPAP Part II: How to Prepare the Baby for CPAP Part III: How to Attach the Baby to the Pumani CPAP
 Pumani CPAP User Manual Table of Contents Part I: How to Assemble the Pumani CPAP 3 Pumani CPAP Components 4 Assembly Instructions 5-15 Part II: How to Prepare the Baby for CPAP 16-18 Part III: How to
Pumani CPAP User Manual Table of Contents Part I: How to Assemble the Pumani CPAP 3 Pumani CPAP Components 4 Assembly Instructions 5-15 Part II: How to Prepare the Baby for CPAP 16-18 Part III: How to
NON INVASIVE LIFE SAVERS. Non Invasive Ventilation (NIV)
 Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
User Manual & Repair Manual
 User Manual & Repair Manual 0120 Introduction Complications due to premature birth, including respiratory distress, are the leading cause of child mortality worldwide. Bubble continuous positive airway
User Manual & Repair Manual 0120 Introduction Complications due to premature birth, including respiratory distress, are the leading cause of child mortality worldwide. Bubble continuous positive airway
Review of Neonatal Respiratory Problems
 Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Scope This guideline is aimed at all healthcare professionals involved in the care of infants within the neonatal service.
 UHL Neonatal Guideline: CPAP Nursing Care University Hospitals of Leicester NHS NHS Trust Nov 2018 Nov 2021 Scope This guideline is aimed at all healthcare professionals involved in the care of infants
UHL Neonatal Guideline: CPAP Nursing Care University Hospitals of Leicester NHS NHS Trust Nov 2018 Nov 2021 Scope This guideline is aimed at all healthcare professionals involved in the care of infants
The Blue Baby. Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin
 The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) NICU POCKET GUIDE
 Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) TM NICU POCKET GUIDE Patient Selection Diagnoses Patient presents with one or more of the following symptoms: These
Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) TM NICU POCKET GUIDE Patient Selection Diagnoses Patient presents with one or more of the following symptoms: These
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers
 Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
Title Neonatal and Paediatric High-Flow Nasal Cannula Oxygen Therapy Guideline. Department Paediatrics / Neonates Date Issued
 Document Control Title Author Neonatal and Paediatric High-Flow Nasal Cannula Oxygen Therapy Guideline Author s job title Directorate Medical Version Department Paediatrics / Neonates Date Issued Status
Document Control Title Author Neonatal and Paediatric High-Flow Nasal Cannula Oxygen Therapy Guideline Author s job title Directorate Medical Version Department Paediatrics / Neonates Date Issued Status
PEPP Course: PEPP BLS Pretest
 PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
October Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE
 October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
Non-invasive Ventilation protocol For COPD
 NHS LANARKSHIRE MONKLANDS HOSPITAL Non-invasive Ventilation protocol For COPD April 2017 S Baird Review Date: Oct 2019 Approved by Medical Directorate Indications for Non-Invasive Ventilation (NIV) NIV
NHS LANARKSHIRE MONKLANDS HOSPITAL Non-invasive Ventilation protocol For COPD April 2017 S Baird Review Date: Oct 2019 Approved by Medical Directorate Indications for Non-Invasive Ventilation (NIV) NIV
Simulation 3: Post-term Baby in Labor and Delivery
 Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Hyaline membrane disease. By : Dr. Ch Sarishma Peadiatric Pg
 Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Advantages and disadvantages of different nasal CPAP systems in newborns
 Intensive Care Med (2004) 30:926 930 DOI 10.1007/s00134-004-2267-8 N E O N A T A L A N D P A E D I A T R I C I N T E N S I V E C A R E V. Buettiker M. I. Hug O. Baenziger C. Meyer B. Frey Advantages and
Intensive Care Med (2004) 30:926 930 DOI 10.1007/s00134-004-2267-8 N E O N A T A L A N D P A E D I A T R I C I N T E N S I V E C A R E V. Buettiker M. I. Hug O. Baenziger C. Meyer B. Frey Advantages and
5 Million neonatal deaths each year worldwide. 20% caused by neonatal asphyxia. Improvement of the outcome of 1 million newborns every year
 1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
Respiratory Management in Pediatrics
 Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY
 PS1006 SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY TITLE: NON-INVASIVE VENTILATION FOR THE Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE: Director, Respiratory Care Services 126.685 (neo) 3/26/15
PS1006 SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY TITLE: NON-INVASIVE VENTILATION FOR THE Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE: Director, Respiratory Care Services 126.685 (neo) 3/26/15
Neonatal Respiratory Physiotherapy. Nicky Hawkes Advanced Respiratory Physiotherapist Oct 2011
 Neonatal Respiratory Physiotherapy Nicky Hawkes Advanced Respiratory Physiotherapist Oct 2011 Respiratory Physiotherapy?..Not just percussion! Assessment of baby s respiratory status and deciding what
Neonatal Respiratory Physiotherapy Nicky Hawkes Advanced Respiratory Physiotherapist Oct 2011 Respiratory Physiotherapy?..Not just percussion! Assessment of baby s respiratory status and deciding what
Children & Young People s Directorate Paediatric-Neonatal Guidelines Checklist & Version Control Sheet
 Children & Young People s Directorate Paediatric-Neonatal Guidelines Checklist & Version Control Sheet 1. Name of Guideline / Policy/ Procedure 2. Purpose of Procedure/ Guidelines/ Protocol Guideline for
Children & Young People s Directorate Paediatric-Neonatal Guidelines Checklist & Version Control Sheet 1. Name of Guideline / Policy/ Procedure 2. Purpose of Procedure/ Guidelines/ Protocol Guideline for
Clinical Guideline: Management of a baby on CPAP
 Clinical Guideline: Management of a baby on CPAP Authors: EOE Neonatal Benchmarking Group For use in: EoE Neonatal Units Guidance specific to the care of neonatal patients. Used by: For use in neonatal
Clinical Guideline: Management of a baby on CPAP Authors: EOE Neonatal Benchmarking Group For use in: EoE Neonatal Units Guidance specific to the care of neonatal patients. Used by: For use in neonatal
Audu LI Otuneye AT Mairami AB Mukhtar MY ORIGINAL. Niger J Paed 2015; 42 (1): 12 16
 Niger J Paed 2015; 42 (1): 12 16 Audu LI Otuneye AT Mairami AB Mukhtar MY ORIGINAL Improvised bubble continuous positive airway pressure (BCPAP) device at the National Hospital Abuja gives immediate improvement
Niger J Paed 2015; 42 (1): 12 16 Audu LI Otuneye AT Mairami AB Mukhtar MY ORIGINAL Improvised bubble continuous positive airway pressure (BCPAP) device at the National Hospital Abuja gives immediate improvement
Acute Paediatric Respiratory Pathway
 Guideline for the use of high Flow Nasal Cannula Oxygen Therapy (Optiflow or Airvo) in Children with Bronchiolitis or an acute respiratory illness Introduction: High flow nasal cannula (HFNC) oxygen enables
Guideline for the use of high Flow Nasal Cannula Oxygen Therapy (Optiflow or Airvo) in Children with Bronchiolitis or an acute respiratory illness Introduction: High flow nasal cannula (HFNC) oxygen enables
Introducing Infant Flow Advance SIPAP. By Joanne Cookson March 2008
 Introducing Infant Flow Advance SIPAP By Joanne Cookson March 2008 Aim To introduce clinical practioners to the new SiPAP machine Objectives To define what is SiPAP To look at different modes able to be
Introducing Infant Flow Advance SIPAP By Joanne Cookson March 2008 Aim To introduce clinical practioners to the new SiPAP machine Objectives To define what is SiPAP To look at different modes able to be
Protocol for performing chest clearance techniques by nursing staff
 Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
10/17/2016 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT COURSE OBJECTIVES COMMON CAUSES OF RESPIRATORY FAILURE
 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube)
 This is an official Northern Trust policy and should not be edited in any way Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube) Reference Number: NHSCT/12/547
This is an official Northern Trust policy and should not be edited in any way Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube) Reference Number: NHSCT/12/547
Respiratory System Mechanics
 M56_MARI0000_00_SE_EX07.qxd 8/22/11 3:02 PM Page 389 7 E X E R C I S E Respiratory System Mechanics Advance Preparation/Comments 1. Demonstrate the mechanics of the lungs during respiration if a bell jar
M56_MARI0000_00_SE_EX07.qxd 8/22/11 3:02 PM Page 389 7 E X E R C I S E Respiratory System Mechanics Advance Preparation/Comments 1. Demonstrate the mechanics of the lungs during respiration if a bell jar
LRI Children s Hospital
 LRI Children s Hospital Humidified High Flow Nasal Cannula (HHFNC) Oxygen Therapy Staff relevant to: Medical and Nursing staff Team approval date: 5.01.18 Version: 1 Revision due: January 2020 Written
LRI Children s Hospital Humidified High Flow Nasal Cannula (HHFNC) Oxygen Therapy Staff relevant to: Medical and Nursing staff Team approval date: 5.01.18 Version: 1 Revision due: January 2020 Written
BRONCHIOLITIS. See also the PSNZ guideline - Wheeze & Chest Infections in infants under 1 year (www.paediatrics.org.nz)
 Definition What is Bronchiolitis? Assessment Management Flow Chart Admission Guidelines Investigations Management Use of Bronchodilators Other treatments Discharge Planning Bronchiolitis & Asthma References
Definition What is Bronchiolitis? Assessment Management Flow Chart Admission Guidelines Investigations Management Use of Bronchodilators Other treatments Discharge Planning Bronchiolitis & Asthma References
CHILDREN S SERVICES. Patient information Leaflet BRONCHIOLITIS
 CHILDREN S SERVICES Patient information Leaflet BRONCHIOLITIS Sept 2014 INTRODUCTION This leaflet aims to help you understand bronchiolitis, how to make your child comfortable and when to contact for emergency
CHILDREN S SERVICES Patient information Leaflet BRONCHIOLITIS Sept 2014 INTRODUCTION This leaflet aims to help you understand bronchiolitis, how to make your child comfortable and when to contact for emergency
Transfer guidelines for surgical infants
 Transfer guidelines for surgical infants Document Title and Reference : Transfer guidelines for surgical infants Main Author (s) Transport Team Clinical Guidelines group Ratified by: GMNICP Date Ratified:
Transfer guidelines for surgical infants Document Title and Reference : Transfer guidelines for surgical infants Main Author (s) Transport Team Clinical Guidelines group Ratified by: GMNICP Date Ratified:
Nottingham Children s Hospital
 High Flow Nasal Cannula Therapy Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Guide line for the use of HFNCT (High Flow Nasal Cannula Therapy) Contact Name
High Flow Nasal Cannula Therapy Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Guide line for the use of HFNCT (High Flow Nasal Cannula Therapy) Contact Name
1.1.2 CPAP therapy is used for patients who are suffering from an acute type 1 respiratory failure (Pa02 <8kPa with a normal or low Pac02).
 Guidelines for initiating and managing CPAP (Continuous Positive Airway Pressure) on a general ward. B25/2006 1.Introduction and Who Guideline applies to 1.1.1 This document provides guidance for Healthcare
Guidelines for initiating and managing CPAP (Continuous Positive Airway Pressure) on a general ward. B25/2006 1.Introduction and Who Guideline applies to 1.1.1 This document provides guidance for Healthcare
CHEST PHYSIOTHERAPY IN NICU PURPOSE POLICY STATEMENTS SITE APPLICABILITY PRACTICE LEVEL/COMPETENCIES. The role of chest physiotherapy in the NICU
 PURPOSE The role of chest physiotherapy in the NICU POLICY STATEMENTS In principle chest physiotherapy should be limited to those infants considered most likely to benefit with significant respiratory
PURPOSE The role of chest physiotherapy in the NICU POLICY STATEMENTS In principle chest physiotherapy should be limited to those infants considered most likely to benefit with significant respiratory
Dr. (Kate) Katherine Miller GUELPH ON 121 RESPIRATORY DISTRESS IN THE NEWBORN
 Society of Rural Physicians of Canada 26TH ANNUAL RURAL AND REMOTE MEDICINE COURSE ST. JOHN'S NEWFOUNDLAND AND LABRADOR APRIL 12-14, 2018 Dr. (Kate) Katherine Miller GUELPH ON 121 RESPIRATORY DISTRESS
Society of Rural Physicians of Canada 26TH ANNUAL RURAL AND REMOTE MEDICINE COURSE ST. JOHN'S NEWFOUNDLAND AND LABRADOR APRIL 12-14, 2018 Dr. (Kate) Katherine Miller GUELPH ON 121 RESPIRATORY DISTRESS
Surfactant Administration
 Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
Respiratory Failure in the Pediatric Patient
 Respiratory Failure in the Pediatric Patient Ndidi Musa M.D. Associate Professor of Pediatrics Medical College of Wisconsin Pediatric Cardiac Intensivist Children s Hospital of Wisconsin Objectives Recognize
Respiratory Failure in the Pediatric Patient Ndidi Musa M.D. Associate Professor of Pediatrics Medical College of Wisconsin Pediatric Cardiac Intensivist Children s Hospital of Wisconsin Objectives Recognize
Day-to-day management of Tracheostomies & Laryngectomies
 Humidification It is mandatory that a method of artificial humidification is utilised when a tracheostomy tube is in situ, for people requiring oxygen therapy dry oxygen should never be given to someone
Humidification It is mandatory that a method of artificial humidification is utilised when a tracheostomy tube is in situ, for people requiring oxygen therapy dry oxygen should never be given to someone
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Phases of Respiration. Chapter 18: The Respiratory System. Structures of the Respiratory System. Structures of the Respiratory System
 Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
-Tamara Wahbeh. -Razan Abu Rumman. Dr. Mohammed Al-Muhtaseb
 -2 -Tamara Wahbeh -Razan Abu Rumman Dr. Mohammed Al-Muhtaseb I tried to include everything the doctor mentioned in both the lecture and his slides in the simplest way possible, so hopefully there would
-2 -Tamara Wahbeh -Razan Abu Rumman Dr. Mohammed Al-Muhtaseb I tried to include everything the doctor mentioned in both the lecture and his slides in the simplest way possible, so hopefully there would
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Presented By : Kamlah Olaimat
 Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
Guidelines and Best Practices for High Flow Nasal Cannula (HFNC) Pediatric Pocket Guide
 Guidelines Best Practices for High Flow Nasal Cannula (HFNC) Pediatric Pocket Guide Patient Selection Diagnoses Patient presents with one or more of the following signs or symptoms of respiratory distress:
Guidelines Best Practices for High Flow Nasal Cannula (HFNC) Pediatric Pocket Guide Patient Selection Diagnoses Patient presents with one or more of the following signs or symptoms of respiratory distress:
Lung Wit and Wisdom. Understanding Oxygenation and Ventilation in the Neonate. Jennifer Habert, BHS-RT, RRT-NPS, C-NPT Willow Creek Women s Hospital
 Lung Wit and Wisdom Understanding Oxygenation and Ventilation in the Neonate Jennifer Habert, BHS-RT, RRT-NPS, C-NPT Willow Creek Women s Hospital Objectives To review acid base balance and ABG interpretation
Lung Wit and Wisdom Understanding Oxygenation and Ventilation in the Neonate Jennifer Habert, BHS-RT, RRT-NPS, C-NPT Willow Creek Women s Hospital Objectives To review acid base balance and ABG interpretation
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
LESSON ASSIGNMENT. Oral, Nasopharyngeal, and Nasotracheal Suctioning. After completing this lesson, you will be able to:
 LESSON ASSIGNMENT LESSON 4 Oral, Nasopharyngeal, and Nasotracheal Suctioning. LESSON ASSIGNMENT Paragraphs 4-1 through 4-4. LESSON OBJECTIVES After completing this lesson, you will be able to: 4-1. State/identify
LESSON ASSIGNMENT LESSON 4 Oral, Nasopharyngeal, and Nasotracheal Suctioning. LESSON ASSIGNMENT Paragraphs 4-1 through 4-4. LESSON OBJECTIVES After completing this lesson, you will be able to: 4-1. State/identify
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Airway and Breathing
 Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
CARDIOVASCULAR AND RESPIRATORY SYSTEMS
 CARDIOVASCULAR AND RESPIRATORY SYSTEMS KEY TERMS: Cardiovascular System, cardio, vascular, blood vessels, valves, arteries, capillaries, veins, systemic circulation, pulmonary circulation Your Cardiovascular
CARDIOVASCULAR AND RESPIRATORY SYSTEMS KEY TERMS: Cardiovascular System, cardio, vascular, blood vessels, valves, arteries, capillaries, veins, systemic circulation, pulmonary circulation Your Cardiovascular
Airway and Ventilation. Emergency Medical Response
 Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Vital Signs and Oxygen Administration
 Vital Signs and Oxygen Administration By Dr. Mohsen Dashti Patient Care and Management (202) May-9-2010 Vital Signs and Oxygen Administration What are the vital signs? Why do we need to know them? How
Vital Signs and Oxygen Administration By Dr. Mohsen Dashti Patient Care and Management (202) May-9-2010 Vital Signs and Oxygen Administration What are the vital signs? Why do we need to know them? How
Date Time PEWS Nurse Initials & NMBI Alert. Airway Behaviour and feeding. Accessory muscle use. Oxygen. Other
 Score Date / Time Minimum Observations 1 4 hourly 2 2-4 hourly Hospital Logo Paediatric Observation Chart 12+ Years Maximum Duration Nurse in Charge Escalation Guide Minimum Alert PEWS does not replace
Score Date / Time Minimum Observations 1 4 hourly 2 2-4 hourly Hospital Logo Paediatric Observation Chart 12+ Years Maximum Duration Nurse in Charge Escalation Guide Minimum Alert PEWS does not replace
Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube.
 Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube. Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube. Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Equipment: NRP algorithm, MRSOPA table, medication chart, SpO 2 table Warm
 NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2
 2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
Heated Humidified High Flow Nasal Cannula Treatment (HHHFNC)
 Heated Humidified High Flow Nasal Cannula Treatment (HHHFNC) 1. Introduction and Who Guideline applies to Heated humidified high flow nasal cannula treatment (HHHFNC), otherwise called as High flow oxygen
Heated Humidified High Flow Nasal Cannula Treatment (HHHFNC) 1. Introduction and Who Guideline applies to Heated humidified high flow nasal cannula treatment (HHHFNC), otherwise called as High flow oxygen
Respiratory Physiology
 Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Module 2: Facilitator instructions for Airway & Breathing Skills Station
 Module 2: Facilitator instructions for Airway & Breathing Skills Station 1. Preparation a. Assemble equipment beforehand. b. Make sure that you have what you need and that it is functioning properly. 2.
Module 2: Facilitator instructions for Airway & Breathing Skills Station 1. Preparation a. Assemble equipment beforehand. b. Make sure that you have what you need and that it is functioning properly. 2.
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Phases of Respiration
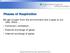 Phases of Respiration We get oxygen from the environment and it goes to our cells, there. Pulmonary ventilation External exchange of gases Internal exchange of gases Overview of respiration. In ventilation,
Phases of Respiration We get oxygen from the environment and it goes to our cells, there. Pulmonary ventilation External exchange of gases Internal exchange of gases Overview of respiration. In ventilation,
Nitric Resource Manual
 Nitric Resource Manual OBJECTIVES Describe the biologic basis for inhaled nitric oxide therapy Describe the indications for inhaled nitric oxide therapy Describe the potential hazards, side effects and
Nitric Resource Manual OBJECTIVES Describe the biologic basis for inhaled nitric oxide therapy Describe the indications for inhaled nitric oxide therapy Describe the potential hazards, side effects and
Chapter 11: Respiratory Emergencies
 29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Capnography Connections Guide
 Capnography Connections Guide Patient Monitoring Contents I Section 1: Capnography Introduction...1 I Section 2: Capnography & PCA...3 I Section 3: Capnography & Critical Care...7 I Section 4: Capnography
Capnography Connections Guide Patient Monitoring Contents I Section 1: Capnography Introduction...1 I Section 2: Capnography & PCA...3 I Section 3: Capnography & Critical Care...7 I Section 4: Capnography
Nasopharyngeal airways for craniofacial conditions
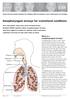 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Nasopharyngeal airways for craniofacial conditions This information sheet from Great Ormond Street Hospital (GOSH)
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Nasopharyngeal airways for craniofacial conditions This information sheet from Great Ormond Street Hospital (GOSH)
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
Chapter 10 The Respiratory System
 Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
TRAINING NEONATOLOGY SILVANA PARIS
 TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP)
 CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) Continuous Positive Airway Pressure (CPAP) may be used as an adjunctive therapy for the treatment of patients with suspected Acute Pulmonary Edema, Chronic Obstructive
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) Continuous Positive Airway Pressure (CPAP) may be used as an adjunctive therapy for the treatment of patients with suspected Acute Pulmonary Edema, Chronic Obstructive
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH
 Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor
 Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Positive Pressure Therapy
 Positive Pressure Therapy Positive Pressure Therapy...2 What is Sleep Apnea?....2 Positive Pressure Machines..................................................... 4 Types..................................................................................
Positive Pressure Therapy Positive Pressure Therapy...2 What is Sleep Apnea?....2 Positive Pressure Machines..................................................... 4 Types..................................................................................
NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP)
 Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Overview. The Respiratory System. Chapter 18. Respiratory Emergencies 9/11/2012
 Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Carole Wegner RN, MSN And Lori Leiser CRT
 Airway Clearance Carole Wegner RN, MSN And Lori Leiser CRT Topics Suctioning and suctioning equipment Medications to facilitate t airway clearance Bronchial hygiene modalities Preparing for suctioning
Airway Clearance Carole Wegner RN, MSN And Lori Leiser CRT Topics Suctioning and suctioning equipment Medications to facilitate t airway clearance Bronchial hygiene modalities Preparing for suctioning
OSA in children. About this information. What is obstructive sleep apnoea (OSA)?
 About this information This information explains all about sleep-related breathing problems in children, focusing on the condition obstructive sleep apnoea (OSA). It tells you what the risk factors are
About this information This information explains all about sleep-related breathing problems in children, focusing on the condition obstructive sleep apnoea (OSA). It tells you what the risk factors are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Respiratory Failure. Causes of Acute Respiratory Failure (ARF): a- Intrapulmonary:
 Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
WELCOME. Welcome to the Children s Hospital PICU (Pediatric Intensive Care Unit). We consider it a privilege to care for your child and your family.
 ECMO FAMILY GUIDE WELCOME Welcome to the Children s Hospital PICU (Pediatric Intensive Care Unit). We consider it a privilege to care for your child and your family. This book was created to give you the
ECMO FAMILY GUIDE WELCOME Welcome to the Children s Hospital PICU (Pediatric Intensive Care Unit). We consider it a privilege to care for your child and your family. This book was created to give you the
Handling Common Problems & Pitfalls During. Oxygen desaturation in patients receiving mechanical ventilation ACUTE SEVERE RESPIRATORY FAILURE
 Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease Document Control Information Author CATS/NTS Author Position CC Transport Services Document Owner E. Polke
UMC HEALTH SYSTEM Lubbock, Texas :
 Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
NRP Raising the Bar for Providers and Instructors
 NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
Section 2.1 Daily checks Humidification
 Bite- sized training from the GTC Section 2.1 Daily checks Humidification This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative. The GTC
Bite- sized training from the GTC Section 2.1 Daily checks Humidification This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative. The GTC
Chapter 10. The Respiratory System Exchange of Gases. Copyright 2009 Pearson Education, Inc.
 Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
NON-INVASIVE VENTILATION. Lijun Ding 23 Jan 2018
 NON-INVASIVE VENTILATION Lijun Ding 23 Jan 2018 Learning objectives What is NIV The difference between CPAP and BiPAP The indication of the use of NIV Complication of NIV application Patient monitoring
NON-INVASIVE VENTILATION Lijun Ding 23 Jan 2018 Learning objectives What is NIV The difference between CPAP and BiPAP The indication of the use of NIV Complication of NIV application Patient monitoring
The assessment helps decide if the patient is an emergency, priority or non-urgent case.
 Emergency Triage Assessment and Treatment The World Health Organisation (WHO) has produced some useful guidelines about how to improve the care of our patients and their survival in hospital. This is a
Emergency Triage Assessment and Treatment The World Health Organisation (WHO) has produced some useful guidelines about how to improve the care of our patients and their survival in hospital. This is a
Appendix E Choose the sign or symptom that best indicates severe respiratory distress.
 Appendix E-2 1. In Kansas EMT-B may monitor pulse oximetry: a. after they complete the EMT-B course b. when the service purchases the state approved pulse oximeters c. when the service director receives
Appendix E-2 1. In Kansas EMT-B may monitor pulse oximetry: a. after they complete the EMT-B course b. when the service purchases the state approved pulse oximeters c. when the service director receives
Post-Anesthesia Care In the ICU
 Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
NEWBORNS WITH RESPIRATORY DISTRESS: MANAGEMENT IN SPECIAL CARE NURSERIES (SCNS)
 NSW Pregnancy and newborn Services Network (PSN) NEWBORNS WITH RESPIRATORY DISTRESS: MANAGEMENT IN SPECIAL CARE NURSERIES (SCNS) PRACTICE GUIDELINE This document reflects what is currently regarded as
NSW Pregnancy and newborn Services Network (PSN) NEWBORNS WITH RESPIRATORY DISTRESS: MANAGEMENT IN SPECIAL CARE NURSERIES (SCNS) PRACTICE GUIDELINE This document reflects what is currently regarded as
Julie Zimmerman, MSN, RN, CCRN Clinical Nurse Specialist
 Julie Zimmerman, MSN, RN, CCRN Clinical Nurse Specialist Objectives Define capnography vs. end tidal CO2 (EtCO 2 ) Identify what normal vs. abnormal EtCO2 values mean and what to do Understand when to
Julie Zimmerman, MSN, RN, CCRN Clinical Nurse Specialist Objectives Define capnography vs. end tidal CO2 (EtCO 2 ) Identify what normal vs. abnormal EtCO2 values mean and what to do Understand when to
