2: Symptoms and management
|
|
|
- Bertina Morgan
- 6 years ago
- Views:
Transcription
1 2: Symptoms and management This section will help you to find out about the likely symptoms of motor neurone disease (MND) and how these can be managed. The following information is an extracted section from our full guide Living with motor neurone disease. All of the extracted sections, and the full guide, can be found online at: The full guide can be ordered in hardcopy from our helpline, MND Connect: Telephone: Living with motor neurone disease Living with motor neurone disease
2 2: Symptoms and management This section will help you to find out about the likely symptoms of motor neurone disease (MND) and how these can be managed. What are the symptoms? Not everyone will experience all of the following symptoms, or in any particular order. You may even have symptoms that are not mentioned here, as the disease can affect everyone differently, or you could have another unrelated problem which also requires medical attention, so please speak to your GP about any concerns. At the moment the disease has only affected my left arm. See Further information at the end of this section for detailed publications linked to some of the symptoms listed here. Muscle weakness What is happening? When the messages from the motor neurones reduce, the muscle they connect to is used less and tends to decrease in mass (to waste). This causes weakness and can affect balance and posture, with the risk of falls. What can be done? Muscle wasting cannot be reversed by exercise, as the progression of the disease cannot be undone. What exercise can do is to assist flexibility and range of movement in your joints, help to maintain unaffected muscles, and support posture and balance. Ask your GP or health and social care team for a referral to a relevant physiotherapist, who can recommend an exercise programme appropriate to your needs. You can also ask for a referral to a dietitian to discuss ways of maintaining your weight, to prevent any further muscle breakdown through weight loss. See Swallowing problems later in this list of symptoms. Twitching (and fasciculations) What is happening? Twitching, and the rippling sensations under the skin called fasciculations, are often among the first and most annoying of symptoms. Some people feel the rippling effect in individual muscles, but this can be more widespread. What can be done? Talk to your GP, consultant or specialist nurse, as medication may help to relieve this symptom. In many cases, this symptom fades over time. Muscle tightness and/or cramping What is happening? Due to the breakdown of messages from the motor neurones, general muscle tightness or spasticity can impact on mobility, affect coordination of movement and may cause pain or increase the risk of falls. Sudden muscle cramps are also common and can be very painful. My limbs became unusually stiff in the middle of a climb I had made several times before. I dismissed the problem as paranoia for my approaching 40th birthday. 12
3 What can be done? Talk to your health and social care team as physiotherapy or medication may provide some relief and they can advise on managing falls. Appropriate positioning when seated or lying down can also help you feel more comfortable. Breathing problems What is happening? Problems with breathing may develop, usually in the later stages of the illness. The internal respiratory process is not affected, but the muscles involved in the voluntary control of breathing can become impaired. What can be done? If you have shortness of breath, fatigue, disturbed sleep, morning headaches or daytime sleepiness, you may be referred to a respiratory consultant for assessment. Depending on your needs and preferences, assistance can include breathing exercises, physiotherapy, advice on careful positioning, guidance on effective coughing, medication and specialist equipment for assistive ventilation. See heading Support for breathing problems later in this section. Swallowing problems What is happening? If the bulbar muscles weaken (those in the face, mouth and throat), swallowing can be affected. Disruption of the normal eating and swallowing process is referred to as dysphagia, which can result in inadequate food and fluid intake. Weight loss may occur, but this can also be due to muscle wasting. What can be done? Discuss any issues with your health and social care team and ask to be referred to a speech and language therapist (SLT) and a dietitian. They will assess your weight and ability to swallow, and advise on how to manage coughing and choking, should these occur. Calorie and protein content can be increased with supplements and changes to diet. Alternative feeding options, such as a gastrostomy (using a tube inserted into the abdomen) can supplement or replace meals. See Section 9: Eating and drinking for more details about nutrition and the types of gastrostomy available, such as PEG. Saliva and mucus problems What is happening? If swallowing is impaired, saliva can gather in the mouth and throat, and lead to drooling, which many find embarrassing. Saliva may be watery or thick and ropy. Decreased fluid intake can make mucus secretions thicker which may be more difficult to clear due to reduced coughing pressure. Dryness of the mouth can occur from medication, thrush, dehydration or breathing through the mouth. What can be done? Talk to your health care team as various options can be offered, depending on the circumstances. These can include advice on diet and fluid intake, the use of medication and occasionally suction machines for clearing out the mouth. Speech and communication difficulties What is happening? With weakening of the bulbar muscles (those in the lower face and throat), speech can be affected and poor respiratory support can also weaken the voice. Difficulty with speech is often referred to as dysarthria. What can be done? A speech and language therapist (SLT) can assess your needs, provide therapy techniques and advise on suitable communication aids. An occupational therapist (OT) can assess your requirements regarding how you physically access any equipment or aids. Speech and communication aids are often referred to as Augmentative and Alternative Communication (AAC) and can range from low tech (gestures, notepads, alphabet boards, etc) to high tech (computer based). See Section 8: Speech and communication. 13 Part 1: What is MND? / Symptoms and management
4 Fatigue What is happening? Loss of physical function means that everyday routines become more tiring. Fatigue can also occur from breathing problems and breathlessness, low calorie intake and dehydration. What can be done? Develop flexible routines to make the most of the times you feel alert and to allow for rest. Your occupational therapist (OT) can advise on fatigue management and aids to make daily tasks easier and your dietitian can advise you on increasing your calorie and fluid intake. See also Breathing difficulties and Swallowing problems as listed above. Pain What is happening? Pain may be experienced due to muscle cramps, stiff muscles and joints, muscle spasms, skin pressure or constipation. You may also experience discomfort from fluid retention or swelling, caused by limited mobility (known as oedema). However, in all cases it is important to have the pain assessed, as it may not be connected to MND. What can be done? Talk to your health and social care team for advice on careful positioning, support and pressure care, and suitable medication. If you have fluid retention or swelling, you may be referred to the lymphodema service. If pain is persistent, you can be referred to a palliative care or pain clinic. Emotional lability (also known as pseudo-bulbar effect) What is happening? You may experience inappropriate laughing and/or crying, which can be difficult to control and feels distressing. This does not affect everyone with MND and is an involuntary response. What can be done? Talk to your health and social care team who can support. Medication may help to relieve this symptom. This can also be alarming for those close to you or providing support, but if it is recognised as a part of MND, it can be easier to manage. 14 See Section 4: Emotional impact for more detail on emotional lability. Emotional reactions What is happening? You may feel you are on an emotional roller coaster, experiencing multiple emotions, such as anxiety, fear, anger, sadness, depression and disbelief. These reactions are normal. What can be done? Trying to understand what you are feeling can be the first step towards managing these emotions. If these feelings are persistent and extreme, you may find it helpful to talk to your health and social care team. In some instances medication can help and/or a referral to an appropriate counsellor or psychologist. See Section 4: Emotional impact. It s nice when I m treated as a whole person and not just an illness. Changes to thinking and behaviour What is happening? You may find it harder to think, concentrate, interact with others and plan things as easily as you used to. These changes to thinking and behaviour are known as cognitive change. Up to half of people with MND are thought to be affected, with mild effects in most cases. A few people experience more noticeable change and a very small percentage develop a type of dementia called Frontotemporal Dementia (FTD), which is more severe. What can be done? Additional support is likely to be needed, including mental health and psychological services. If you or your carer have any concerns, ask your neurologist about the possibility of screening. This assessment process can help detect changes to thinking and behaviour, so that appropriate support can be arranged. See Further information at the end of this section.
5 What is not affected by MND? The following are usually unaffected, although each individual has a different experience. Talk to your GP or health and social care team if you have any concerns, as there may be an underlying condition. Taste, sight, smell, touch and hearing Senses are generally unaffected, but some people experience changes to taste, skin hypersensitivity or problems with temperature regulation. Incontinence Bowel and bladder functions are not usually affected by MND, but mobility problems can make it more difficult to access and use toilet facilities. Constipation may occur due to changes in eating, dehydration, anxiety, medication and poor mobility. Diarrhoea can occur as a result of persistent constipation. Any changes to bladder and bowel function should be investigated and may not be due to MND. Sexual function and expression Sexual function is not usually affected, but a person s perception of their own sexuality may change. Physical changes can affect intimacy at all levels from cuddling to sexual expression. Open discussion with your partner, and possibly the help of your health and social care team, can help you to maintain intimacy if this is important to you. Eye muscles Most people with MND retain the ability to move their eyes. If neck muscles are affected, the use of appropriate head supports can help. It s very difficult to assess future needs as we all progress differently with MND and it is impossible to say how long it will take for conditions to change. Are there any specific treatments for MND? Much can be done to manage symptoms, to enable you to maintain independence for as long as possible and to help you deal with the emotional impact of MND. Through MND care centres and networks, and neurological centres, a wide range of health and social care professionals are likely to be involved with you and your family. This is often referred to as a multi-disciplinary team (MDT). MDT expert care, combined with treatments or therapies as featured below (when relevant to your needs), may help you to maintain the best possible quality of life, for as long as possible, when living with the condition. See Section 13: How health and social care professionals can help you. Depending on your symptoms and progression, discussions with your health and social care team are likely to include the following: Riluzole Currently, there is no treatment that will halt the progress of the disease, although one drug, riluzole, has shown a modest benefit for some people. Researchers continue to investigate other drugs in the laboratory and through clinical trials, with the help of people living with MND. Riluzole is licensed for the treatment of MND and has been approved for use on the NHS. It is not a cure, but it is the first medicine to show a modest impact on survival, of a few months. Riluzole is available in tablet or liquid form. See Further information at the end of this section. 15 Part 1: What is MND? / Symptoms and management
6 Support for breathing problems If you experience breathing difficulties, there are a number of treatments and therapies to help. Wearing my [NIV] ventilator 24 hours a day allows me to lead what I call a normal life and doesn t stop me from doing anything I want to do. Ask your health and social care team for a referral to a respiratory consultant for guidance. This will include discussion about supported breathing, which is your decision to make. This generally involves two options: Non-invasive ventilation (NIV), where a portable machine supports your own breathing by providing extra air through a mask. Invasive ventilation (tracheostomy), where a machine takes over your breathing through a tube inserted into the windpipe through the neck. Some people choose invasive ventilation to avoid the need for a mask. However, invasive ventilation can raise serious questions about quality of life when life is extended in this way, as other disabilities caused by MND will continue to progress. See Further information at the end of this section for information sheets on breathing and ventilation. Oxygen and MND: In most cases, ventilation uses normal air to help you breathe. Extra oxygen is not usually recommended with MND as it can upset the balance in your body between oxygen and carbon dioxide. However, it may be used with caution if your oxygen levels are low. you need emergency treatment and are unable to communicate for any reason, it lets hospital staff know you have MND and may be at risk with oxygen. They may not all be aware of this concern with MND. Tube feeding See Section 9: Eating and drinking for information about nutrition, swallowing difficulties and the possibility of tube feeding, if required. Physiotherapy See Section 6: Getting around for guidance on physiotherapy, exercise and assisted exercise. Complementary therapy Many people living with MND find that some use of complementary therapies can help to relieve some symptoms and reduce stress. However, it is important to recognise these therapies are not a treatment or cure for MND. Complementary therapy is not considered to be part of conventional medicine, but it is felt to complement conventional treatments if used in combination. A wide variety of complementary therapies exist, such as massage, acupuncture and reflexology. These therapies are increasingly available on the NHS and some general practices now provide access to them. Hospices usually offer a selection of complementary therapies as part of their service. A reflexologist kindly massages my feet, hands and arms, which helps with circulation and generally feels good. These appointments were facilitated by the local hospital. An alert wristband has been included in the folder with this guide. It is your choice whether to wear the wristband or not, but if 16
7 Key points Not all health and social care professionals are familiar with MND due to its rarity. They may not be aware of every symptom. Ask questions or request referrals if you notice signs of any symptoms that may require specialist help. Not everyone gets the same symptoms at the same time or in the same order. If planning ahead for equipment or aids, ask for an independent assessment of your needs by a relevant member of your health and social care team to avoid any unnecessary expense. Contact your GP before undertaking a complementary therapy, to check it will not conflict with any current treatment and ask to be referred to a registered practitioner. If you have any difficulties with the supply of riluzole, please contact MND Connect. See Further information for contact details. 9A to 9C: our range of sheets on thinking and emotions in MND 11C: Equipment and wheelchairs 13A: Sex and relationships for people living with MND 13B: Sex and relationships for partners of people living with MND Most of our publications can be downloaded from our website: or you can order them from MND Connect, our support and information helpline: Telephone: mndconnect@mndassociation.org MND Connect can also help you locate external services and providers, and introduce you to our services as available, including your local branch, group, Association visitor or regional care development adviser (RCDA). See Section 14: How we can help you. Part 1: What is MND? / Symptoms and management Further information: We have a range of numbered information sheets, including: 1A: NICE guideline on motor neurone disease 1B: Information about MND or Kennedy's disease in other languages or Braille 2A: Kennedy's disease 5A: Riluzole 6A: Physiotherapy 6B: Complementary therapies 7A: Swallowing difficulties 7B: Tube feeding 7C: Speech and communication support 8A: Support for breathing problems 8B: Ventilation for motor neurone disease 8D: Troubleshooting for non-invasive ventilation (NIV) 8E: Air travel and ventilation for motor neurone disease Online forum: hosted by the MND Association for you to share information and experiences with other people affected by MND. 17
8 Document dates: Last revised: 8/16 Next revision: 8/19 Version: 2 MND Association PO Box 246, Northampton NN1 2PR Tel: Fax: Website: For references and acknowledgements please refer to the full guide, Living with motor neurone disease. The full guide can be ordered in hardcopy from our helpline, MND Connect: Telephone: mndconnect@mndassociation.org Registered Charity No MND Association 2016 All rights reserved. No reproduction, copy or transmission of this publication without written permission. The MND Association would like to thank the Tesco Charity Trust, and the Evan Cornish Foundation for their support which has made the production of Living with motor neurone disease possible. The MND Association has been certified as a producer of reliable health and social care information.
This section will help you to identify and manage some of the more difficult emotional responses you may feel after diagnosis.
 4: Emotional impact This section will help you to identify and manage some of the more difficult emotional responses you may feel after diagnosis. The following information is an extracted section from
4: Emotional impact This section will help you to identify and manage some of the more difficult emotional responses you may feel after diagnosis. The following information is an extracted section from
5: Family, children and friends
 5: Family, children and friends This section will help you to manage difficult conversations as people close to you adjust to your diagnosis of MND. The following information is an extracted section from
5: Family, children and friends This section will help you to manage difficult conversations as people close to you adjust to your diagnosis of MND. The following information is an extracted section from
Kennedy s Disease. Information for people with or affected by Kennedy s Disease
 2B Kennedy s Disease Information for people with or affected by Kennedy s Disease If you have been diagnosed with Kennedy s disease, also known as spinal bulbar muscular atrophy or SBMA, you may be looking
2B Kennedy s Disease Information for people with or affected by Kennedy s Disease If you have been diagnosed with Kennedy s disease, also known as spinal bulbar muscular atrophy or SBMA, you may be looking
2: Emotional and psychological support
 2: Emotional and psychological support This section looks at the emotional and psychological impact of thinking about end of life decisions. The following information is an extracted section from our full
2: Emotional and psychological support This section looks at the emotional and psychological impact of thinking about end of life decisions. The following information is an extracted section from our full
Painless, progressive weakness Could this be Motor Neurone Disease?
 Painless, progressive weakness Could this be Motor Neurone Disease? The importance of early diagnosis removal of uncertainty for the person experiencing symptoms allowing for care and support to start
Painless, progressive weakness Could this be Motor Neurone Disease? The importance of early diagnosis removal of uncertainty for the person experiencing symptoms allowing for care and support to start
Palliative Care Asking the questions that matter to me
 Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Understanding late stage dementia Understanding dementia
 Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
SCOTTISH MUSCLE NETWORK DUCHENNE MUSCULAR DYSTROPHY TRANSITION SOME USEFUL THINGS TO KNOW ABOUT HEALTH AROUND ADOLESCENCE
 SCOTTISH MUSCLE NETWORK DUCHENNE MUSCULAR DYSTROPHY TRANSITION SOME USEFUL THINGS TO KNOW ABOUT HEALTH AROUND ADOLESCENCE 02 Changes in our lives can be stressful and leaving school and moving into the
SCOTTISH MUSCLE NETWORK DUCHENNE MUSCULAR DYSTROPHY TRANSITION SOME USEFUL THINGS TO KNOW ABOUT HEALTH AROUND ADOLESCENCE 02 Changes in our lives can be stressful and leaving school and moving into the
ROLE OF THE DIETITIAN. Aims of Dietetic Treatment NUTRITIONAL ISSUES WHY? MALNUTRITION NUTRITONAL MANAGEMENT OF MOTOR NEURONE DISEASE.
 NUTRITONAL MANAGEMENT OF MOTOR NEURONE DISEASE. ROLE OF THE DIETITIAN SALLY DARBY NEUROLOGY DIETITIAN Not just tube feeding Referral soon after diagnosis Advise on healthy eating for MND Monitor nutritional
NUTRITONAL MANAGEMENT OF MOTOR NEURONE DISEASE. ROLE OF THE DIETITIAN SALLY DARBY NEUROLOGY DIETITIAN Not just tube feeding Referral soon after diagnosis Advise on healthy eating for MND Monitor nutritional
20/11/2013. Dr. Sinead Maguire Neurology Registrar 22 nd November 2013
 Dr. Sinead Maguire Neurology Registrar 22 nd November 2013 The active total care of patients whose disease is not responsive to curative treatment. Control of pain, of other symptoms, and psychological,
Dr. Sinead Maguire Neurology Registrar 22 nd November 2013 The active total care of patients whose disease is not responsive to curative treatment. Control of pain, of other symptoms, and psychological,
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Motor neurone disease: the use of non-invasive ventilation in the management of motor neurone disease 1.1 Short title Motor
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Motor neurone disease: the use of non-invasive ventilation in the management of motor neurone disease 1.1 Short title Motor
9 End of life issues
 9 End of life issues In this part Key points: End of life issues 132 Palliative care 134 Grief and bereavement 136 130 131 Key points: End of life issues As a person with dementia approaches the end of
9 End of life issues In this part Key points: End of life issues 132 Palliative care 134 Grief and bereavement 136 130 131 Key points: End of life issues As a person with dementia approaches the end of
Call the National Dementia Helpline on
 128 Call the National Dementia Helpline on 1800 100 500 End of life issues 9 9 End of life issues In this part Key points: End of life issues 130 Palliative care 132 Grief and bereavement 134 For more
128 Call the National Dementia Helpline on 1800 100 500 End of life issues 9 9 End of life issues In this part Key points: End of life issues 130 Palliative care 132 Grief and bereavement 134 For more
Non-invasive ventilation (also called bi-level or BIPAP)
 Patient information service Bristol Royal Infirmary Non-invasive ventilation (also called bi-level or BIPAP) Respecting everyone Embracing change Recognising success Working together Our hospitals. 2 Why
Patient information service Bristol Royal Infirmary Non-invasive ventilation (also called bi-level or BIPAP) Respecting everyone Embracing change Recognising success Working together Our hospitals. 2 Why
Occupational therapy after stroke
 Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
The road to recovery. The support available to help you with your recovery after stroke
 The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Need to talk? Call our confidential Stroke Helpline on 0303 3033
The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Need to talk? Call our confidential Stroke Helpline on 0303 3033
9: Eating and drinking
 9: Eating and drinking This section will help you to find ways to adjust to any problems with eating and drinking. The following information is an extracted section from our full guide Living with motor
9: Eating and drinking This section will help you to find ways to adjust to any problems with eating and drinking. The following information is an extracted section from our full guide Living with motor
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers
 Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
Course Handouts & Disclosure
 ALS: DISEASE TRAJECTORY AND HOSPICE ELIGIBILITY Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Inc Hospice Education Network Inc Course Handouts & Disclosure To download presentation
ALS: DISEASE TRAJECTORY AND HOSPICE ELIGIBILITY Terri L. Maxwell PhD, APRN VP, Strategic Initiatives Weatherbee Resources Inc Hospice Education Network Inc Course Handouts & Disclosure To download presentation
What is frontotemporal dementia?
 What is frontotemporal dementia? Introduction Information in this introductory booklet is for anyone who wants to know more about frontotemporal dementia (FTD). This includes people living with FTD, their
What is frontotemporal dementia? Introduction Information in this introductory booklet is for anyone who wants to know more about frontotemporal dementia (FTD). This includes people living with FTD, their
Muscular Dystrophy UK s Adult North Star Network. Care recommendations for adults with Duchenne a consultation
 Muscular Dystrophy UK s Adult North Star Network Care recommendations for adults with Duchenne a consultation Background: The North Star Network was set up in 2003 to help drive improvements in services
Muscular Dystrophy UK s Adult North Star Network Care recommendations for adults with Duchenne a consultation Background: The North Star Network was set up in 2003 to help drive improvements in services
Managing emotions. Information for people with or affected by motor neurone disease
 9C Managing emotions Information for people with or affected by motor neurone disease Living with motor neurone disease (MND) can involve a range of emotional challenges and changes that may be difficult
9C Managing emotions Information for people with or affected by motor neurone disease Living with motor neurone disease (MND) can involve a range of emotional challenges and changes that may be difficult
Having a PEG tube inserted
 Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
If you have dementia, you may have some or all of the following symptoms.
 About Dementia Dementia may be caused by a number of illnesses that affect the brain. Dementia typically leads to memory loss, inability to do everyday things, difficulty in communication, confusion, frustration,
About Dementia Dementia may be caused by a number of illnesses that affect the brain. Dementia typically leads to memory loss, inability to do everyday things, difficulty in communication, confusion, frustration,
Dysphagia (swallowing problems)
 Dysphagia (swallowing problems) Speech and Language Therapy Department Patient Information Leaflet Introduction This leaflet is for people who have dysphagia. It gives information on what this condition
Dysphagia (swallowing problems) Speech and Language Therapy Department Patient Information Leaflet Introduction This leaflet is for people who have dysphagia. It gives information on what this condition
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 6 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 6 What can I do to help?... 7 Can friends and
Swallowing problems. Patient information. Name: Date: Speech and Language Therapist: Reviewed: May 2016 Next review: June 2017 Version 1
 Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
Occupational therapy after stroke
 Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
Tracheostomy. Information for patients and relatives
 Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Spinal cord compression: what it means and how it can be treated
 Spinal cord compression: what it means and how it can be treated Patient Information Oncology Department Author ID: Acute Oncology Nurse Specialist Leaflet Number: CC 036 Version: 2.1 Name of Leaflet:
Spinal cord compression: what it means and how it can be treated Patient Information Oncology Department Author ID: Acute Oncology Nurse Specialist Leaflet Number: CC 036 Version: 2.1 Name of Leaflet:
Botox for chronic migraine. Information for patients Neurology
 Botox for chronic migraine Information for patients Neurology This leaflet is not intended to replace the manufacturer's information page 2 of 8 What is Botox? Botox is the brand name for Botulinum Toxin
Botox for chronic migraine Information for patients Neurology This leaflet is not intended to replace the manufacturer's information page 2 of 8 What is Botox? Botox is the brand name for Botulinum Toxin
Having radiotherapy to the head and neck
 Sussex Cancer Care Having radiotherapy to the head and neck Brighton and Sussex University Hospitals NHS Trust Disclaimer The information in this leaflet is for guidance purposes only and is in no way
Sussex Cancer Care Having radiotherapy to the head and neck Brighton and Sussex University Hospitals NHS Trust Disclaimer The information in this leaflet is for guidance purposes only and is in no way
RESPIRATORY PROBLEMS IN MND RICHARD HARRISON MND RESPIRATORY ASSESSMENT SERVICE LUNG HEALTH UNIVERSITY HOSPITAL OF NORTH TEES
 RESPIRATORY PROBLEMS IN MND RICHARD HARRISON MND RESPIRATORY ASSESSMENT SERVICE LUNG HEALTH UNIVERSITY HOSPITAL OF NORTH TEES A TYPICAL HISTORY: NON BULBAR ONSET Difficulty walking Weak hands and arms
RESPIRATORY PROBLEMS IN MND RICHARD HARRISON MND RESPIRATORY ASSESSMENT SERVICE LUNG HEALTH UNIVERSITY HOSPITAL OF NORTH TEES A TYPICAL HISTORY: NON BULBAR ONSET Difficulty walking Weak hands and arms
MOTOR NEURONE DISEASE
 MOTOR NEURONE DISEASE Dr Arun Aggarwal Department of Rehabilitation Medicine, RPAH Department of Neurology, Concord Hospital. Motor Neurone Disease Umbrella term in UK and Australia (ALS in USA) Neurodegenerative
MOTOR NEURONE DISEASE Dr Arun Aggarwal Department of Rehabilitation Medicine, RPAH Department of Neurology, Concord Hospital. Motor Neurone Disease Umbrella term in UK and Australia (ALS in USA) Neurodegenerative
Tracheostomy. Hope Building Neurosurgery
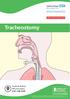 Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
Robotic-assisted lingual tonsillectomy for sleep apnoea
 Robotic-assisted lingual tonsillectomy for sleep apnoea You have been given this leaflet because you have been referred for a robotic-assisted lingual tonsillectomy for sleep apnoea. This leaflet offers
Robotic-assisted lingual tonsillectomy for sleep apnoea You have been given this leaflet because you have been referred for a robotic-assisted lingual tonsillectomy for sleep apnoea. This leaflet offers
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
Symptom Control and End of Life Care
 Symptom Control and End of Life Care MND Special Interest Groups Workshop Dr Cynthia Parr Staff Specialist in Palliative Medicine 12 September 2013 The best test of a physician s suitability for the specialized
Symptom Control and End of Life Care MND Special Interest Groups Workshop Dr Cynthia Parr Staff Specialist in Palliative Medicine 12 September 2013 The best test of a physician s suitability for the specialized
Non-epileptic attacks
 Non-epileptic attacks A short guide for patients and families Information for patients Neurology Psychotherapy Service What are non-epileptic attacks? Non-epileptic attacks are episodes in which people
Non-epileptic attacks A short guide for patients and families Information for patients Neurology Psychotherapy Service What are non-epileptic attacks? Non-epileptic attacks are episodes in which people
Background and Context
 Background and Context People affected by cancer need information that is timely and relevant to enable them to make decisions. It can be difficult for patients and others affected by cancer to identify
Background and Context People affected by cancer need information that is timely and relevant to enable them to make decisions. It can be difficult for patients and others affected by cancer to identify
High dose (radical) radiotherapy to the lung or bronchus
 The Clatterbridge Cancer Centre NHS Foundation Trust High dose (radical) radiotherapy to the lung or bronchus Radiotherapy A guide for patients and carers Contents When radiotherapy is given... 1 Chemotherapy
The Clatterbridge Cancer Centre NHS Foundation Trust High dose (radical) radiotherapy to the lung or bronchus Radiotherapy A guide for patients and carers Contents When radiotherapy is given... 1 Chemotherapy
Non-Motor Symptoms of Parkinson s Disease
 Non-Motor Symptoms of Parkinson s Disease Samantha Holden, MD University of Colorado Movement Disorders MOTOR SYMPTOMS Rigidity Bradykinesia Tremor Gait Imbalance NON-MOTOR SYMPTOMS Dementia Urinary frequency
Non-Motor Symptoms of Parkinson s Disease Samantha Holden, MD University of Colorado Movement Disorders MOTOR SYMPTOMS Rigidity Bradykinesia Tremor Gait Imbalance NON-MOTOR SYMPTOMS Dementia Urinary frequency
Spasticity triggers What to do if you have a worsening of your muscle stiffness and/or spasms
 Spasticity triggers What to do if you have a worsening of your muscle stiffness and/or spasms Jane Lough Paula Cowan We hope you find the information in this book helpful. If you would like to speak with
Spasticity triggers What to do if you have a worsening of your muscle stiffness and/or spasms Jane Lough Paula Cowan We hope you find the information in this book helpful. If you would like to speak with
Laryngeal Cancer. Understanding your diagnosis cancer.ca
 Laryngeal Cancer Understanding your diagnosis 1 888 939-3333 cancer.ca Laryngeal Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be
Laryngeal Cancer Understanding your diagnosis 1 888 939-3333 cancer.ca Laryngeal Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be
Eastman Dental Hospital. About Face Pain management programme. Facial Pain Team
 Eastman Dental Hospital About Face Pain management programme Facial Pain Team If you would like this document in another language or format or if you require the services of an interpreter contact us on
Eastman Dental Hospital About Face Pain management programme Facial Pain Team If you would like this document in another language or format or if you require the services of an interpreter contact us on
This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request.
 Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about acupuncture
Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about acupuncture
Palliative Care Victoria The Process of Dying Page 1. The Process of Dying. What to expect and how to help
 Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
OSA in children. About this information. What is obstructive sleep apnoea (OSA)?
 About this information This information explains all about sleep-related breathing problems in children, focusing on the condition obstructive sleep apnoea (OSA). It tells you what the risk factors are
About this information This information explains all about sleep-related breathing problems in children, focusing on the condition obstructive sleep apnoea (OSA). It tells you what the risk factors are
The Motor Neurone Disease Association
 The Motor Neurone Disease Association What s new in MND Care? Kerry Palmer Regional Care Development Adviser (Cornwall, Devon and Somerset) 23/03/17 Plan NICE Guideline Digital Communication Professional
The Motor Neurone Disease Association What s new in MND Care? Kerry Palmer Regional Care Development Adviser (Cornwall, Devon and Somerset) 23/03/17 Plan NICE Guideline Digital Communication Professional
University College Hospital
 University College Hospital Haematology Psychology and Counselling Service (for patients with blood cancer, red cell disorders and other non-cancer conditions) 1 If you would like this document in another
University College Hospital Haematology Psychology and Counselling Service (for patients with blood cancer, red cell disorders and other non-cancer conditions) 1 If you would like this document in another
MND Just in Case kit Information for GPs
 MND Just in Case kit Information for GPs What is the MND Just in Case kit? 2 Motor neurone disease (MND) is a progressive and terminal disease that results in degeneration of the motor neurones in the
MND Just in Case kit Information for GPs What is the MND Just in Case kit? 2 Motor neurone disease (MND) is a progressive and terminal disease that results in degeneration of the motor neurones in the
Hyperventilation Syndrome - what is it and how to manage it
 Hyperventilation Syndrome - what is it and how to manage it What is hyperventilation syndrome? Hyperventilation happens when you breathe more than your body naturally needs. Hyperventilation syndrome (HVS)
Hyperventilation Syndrome - what is it and how to manage it What is hyperventilation syndrome? Hyperventilation happens when you breathe more than your body naturally needs. Hyperventilation syndrome (HVS)
Delirium Information for relatives, carers and patients
 Delirium Information for relatives, carers and patients Contents Part A Introduction What is delirium? Quotes from relatives or carers showing what might happen to a patient suffering from delirium How
Delirium Information for relatives, carers and patients Contents Part A Introduction What is delirium? Quotes from relatives or carers showing what might happen to a patient suffering from delirium How
Radiotherapy to one side of the mouth and neck
 Clinical Oncology Radiotherapy to one side of the mouth and neck Consent information for patients Radiotherapy may be given on its own or with chemotherapy (separate information will be given about chemotherapy).
Clinical Oncology Radiotherapy to one side of the mouth and neck Consent information for patients Radiotherapy may be given on its own or with chemotherapy (separate information will be given about chemotherapy).
Ratified by: Care and Clinical Policies Date: 17 th February 2016
 Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
CANCER REHABILITATION PATHWAY - HAEMATOLOGY
 CANCER REHABILITATION PATHWAY - HAEMATOLOGY Statement: To be used in conjunction with Brain and CNS Rehabilitation Care Pathway as appropriate Diagnosis and Care Planning: The following symptom pathways
CANCER REHABILITATION PATHWAY - HAEMATOLOGY Statement: To be used in conjunction with Brain and CNS Rehabilitation Care Pathway as appropriate Diagnosis and Care Planning: The following symptom pathways
Getting Comfortable with Managing Pain and Pressure Care in individuals with Motor Neuron Disease Stephanie Williams Occupational Therapist
 Getting Comfortable with Managing Pain and Pressure Care in individuals with Motor Neuron Disease Stephanie Williams Occupational Therapist State-wide Progressive Neurological Diseases Service Calvary
Getting Comfortable with Managing Pain and Pressure Care in individuals with Motor Neuron Disease Stephanie Williams Occupational Therapist State-wide Progressive Neurological Diseases Service Calvary
Tamoxifen Tamoxifen. Your treatment Your doctor or nurse clinician has prescribed for you a treatment which includes the hormonal therapy tamoxifen.
 Tamoxifen Tamoxifen This leaflet is offered as a guide to you and your family. The possible benefits of treatment vary; for some people hormonal therapy may reduce the risk of cancer coming back, for others
Tamoxifen Tamoxifen This leaflet is offered as a guide to you and your family. The possible benefits of treatment vary; for some people hormonal therapy may reduce the risk of cancer coming back, for others
Huntington s disease. Eating and swallowing
 Huntington s disease Eating and swallowing People with Huntington s disease can experience difficulties with eating, drinking and swallowing. These can be among the most challenging aspects of this condition
Huntington s disease Eating and swallowing People with Huntington s disease can experience difficulties with eating, drinking and swallowing. These can be among the most challenging aspects of this condition
Botulinum toxin injections
 Botulinum toxin injections This leaflet explains more about using botulinum toxin injections in children and young people, including the benefits, risks and alternatives. It also provides information on
Botulinum toxin injections This leaflet explains more about using botulinum toxin injections in children and young people, including the benefits, risks and alternatives. It also provides information on
DIET, NUTRITION AND HEAD AND NECK CANCER TREATMENT
 DIET, NUTRITION AND HEAD AND NECK CANCER TREATMENT DIET, NUTRITION AND HEAD AND NECK CANCER TREATMENT HOW HEAD AND NECK CANCER MAY AFFECT NUTRITION Head and neck cancer may make it hard to eat and drink.
DIET, NUTRITION AND HEAD AND NECK CANCER TREATMENT DIET, NUTRITION AND HEAD AND NECK CANCER TREATMENT HOW HEAD AND NECK CANCER MAY AFFECT NUTRITION Head and neck cancer may make it hard to eat and drink.
Changes to your behaviour
 Life after stroke Changes to your behaviour Together we can conquer stroke Because there is so much to deal with after a stroke, it s normal for your behaviour to change in some way. In this booklet we
Life after stroke Changes to your behaviour Together we can conquer stroke Because there is so much to deal with after a stroke, it s normal for your behaviour to change in some way. In this booklet we
Clinical Oncology Radiotherapy to the larynx (4 week treatment) Consent information for patients
 Clinical Oncology Radiotherapy to the larynx (4 week treatment) Consent information for patients Radiotherapy treatment is used for early larynx cancer. We are aiming to cure the cancer and it is successful
Clinical Oncology Radiotherapy to the larynx (4 week treatment) Consent information for patients Radiotherapy treatment is used for early larynx cancer. We are aiming to cure the cancer and it is successful
Feeling low or anxious
 BRAIN INJURY SERIES Feeling low or anxious IN THIS BOOKLET What is depression? Anxiety explained Ways to overcome anxiety or depression Positive tips and advice Brain Injury Series This booklet was written
BRAIN INJURY SERIES Feeling low or anxious IN THIS BOOKLET What is depression? Anxiety explained Ways to overcome anxiety or depression Positive tips and advice Brain Injury Series This booklet was written
Swallowing difficulties
 7A Swallowing difficulties Information for people with or affected by motor neurone disease With MND, you may experience changes to the way you swallow. You may also experience problems with managing your
7A Swallowing difficulties Information for people with or affected by motor neurone disease With MND, you may experience changes to the way you swallow. You may also experience problems with managing your
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person
 Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Having inhalation sedation for your dental treatment
 Having inhalation sedation for your dental treatment This aim of this information sheet is to help answer some of the questions you may have about having inhalation sedation for your dental treatment.
Having inhalation sedation for your dental treatment This aim of this information sheet is to help answer some of the questions you may have about having inhalation sedation for your dental treatment.
National Cancer Action Team. Rehabilitation Care Pathway Brain CNS
 National Cancer Action Team Rehabilitation Care Pathway Brain CNS Rehabilitation Care Pathway Brain CNS Diagnosis & Care Planning Drop Down Pathways Dysphagia Mobility/ loss of function Intervention D1
National Cancer Action Team Rehabilitation Care Pathway Brain CNS Rehabilitation Care Pathway Brain CNS Diagnosis & Care Planning Drop Down Pathways Dysphagia Mobility/ loss of function Intervention D1
Bowel health and screening: carers guide. A booklet for carers of people who use easy read materials
 Bowel health and screening: carers guide A booklet for carers of people who use easy read materials Contents Page 3: About this booklet Page 4: What is the bowel? Page 5: Helping someone to have good bowel
Bowel health and screening: carers guide A booklet for carers of people who use easy read materials Contents Page 3: About this booklet Page 4: What is the bowel? Page 5: Helping someone to have good bowel
National Hospital for Neurology and Neurosurgery. Cerebral angiogram (Overnight stay) Neurovascular Team
 National Hospital for Neurology and Neurosurgery Cerebral angiogram (Overnight stay) Neurovascular Team If you would like this document in another language or format or if you require the services of an
National Hospital for Neurology and Neurosurgery Cerebral angiogram (Overnight stay) Neurovascular Team If you would like this document in another language or format or if you require the services of an
Mouth care for people with dementia. False beliefs and delusions in dementia. Caring for someone with dementia
 Mouth care for people with dementia False beliefs and delusions in dementia Caring for someone with dementia 2 Dementia UK False beliefs and delusions in dementia We understand the world through our senses.
Mouth care for people with dementia False beliefs and delusions in dementia Caring for someone with dementia 2 Dementia UK False beliefs and delusions in dementia We understand the world through our senses.
What is Dysphagia? An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION What is Dysphagia? An information guide What is Dysphagia? If someone has dysphagia, this means they have difficulty in swallowing. Dysphagia
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION What is Dysphagia? An information guide What is Dysphagia? If someone has dysphagia, this means they have difficulty in swallowing. Dysphagia
Speech and Language Therapy. Patient Information Leaflet Easy Read
 Speech and Language Therapy Patient Information Leaflet Easy Read This checklist can be downloaded from www.sunderlandactionforhealth.co.uk. It is free to use for personal use and with people you support.
Speech and Language Therapy Patient Information Leaflet Easy Read This checklist can be downloaded from www.sunderlandactionforhealth.co.uk. It is free to use for personal use and with people you support.
CT Colonography (Virtual Colonoscopy) Patient information
 CT Colonography (Virtual Colonoscopy) Patient information CT colonography is a way of looking inside your bowel and abdomen. This information explains how it is done, what to expect, and the risks involved.
CT Colonography (Virtual Colonoscopy) Patient information CT colonography is a way of looking inside your bowel and abdomen. This information explains how it is done, what to expect, and the risks involved.
Parkinson s for Care Staff
 Unit 28: Understand Parkinson s for Care Staff Unit reference number: A/616/7339 Level: 3 Unit type: Optional Credit value: 2 Guided learning hours: 14 Unit summary Parkinson s is a progressive neurological
Unit 28: Understand Parkinson s for Care Staff Unit reference number: A/616/7339 Level: 3 Unit type: Optional Credit value: 2 Guided learning hours: 14 Unit summary Parkinson s is a progressive neurological
FACTSHEET F37. COpIng with LOw MOOD/ DEpRESSIOn
 COpIng with LOw MOOD/ DEpRESSIOn If you are living with a chest, heart or stroke condition you may have periods when your mood is low: this is quite common. Feeling down for some of the time is a natural
COpIng with LOw MOOD/ DEpRESSIOn If you are living with a chest, heart or stroke condition you may have periods when your mood is low: this is quite common. Feeling down for some of the time is a natural
Mouth care for people with dementia. Eating and Drinking. Staying well with dementia
 Mouth care for people with dementia Eating and Drinking Staying well with dementia 2 Dementia UK Eating and Drinking 3 Eating and drinking for a person with dementia People with dementia may experience
Mouth care for people with dementia Eating and Drinking Staying well with dementia 2 Dementia UK Eating and Drinking 3 Eating and drinking for a person with dementia People with dementia may experience
SEXUALITY Information for Patients and Families
 SEXUALITY Information for Patients and Families Since my stroke I have difficulties with sexual performance. Is this normal? Yes. Studies estimate that 65-75% of people who have had a stroke do experience
SEXUALITY Information for Patients and Families Since my stroke I have difficulties with sexual performance. Is this normal? Yes. Studies estimate that 65-75% of people who have had a stroke do experience
Having a therapeutic gastroscopy with oesophageal dilatation
 Please telephone the Endoscopy Unit with regards information contained within this leaflet. A member of the nursing team will be glad to advise you. For all general enquiries please use the following contact
Please telephone the Endoscopy Unit with regards information contained within this leaflet. A member of the nursing team will be glad to advise you. For all general enquiries please use the following contact
The Liverpool Asperger Team
 The Liverpool Asperger Team This artwork was created by a service user of the Liverpool Asperger Team. It represents the diversity and union of shared experience that many people with Asperger Syndrome
The Liverpool Asperger Team This artwork was created by a service user of the Liverpool Asperger Team. It represents the diversity and union of shared experience that many people with Asperger Syndrome
a patient s guide Physiotherapy advice and exercises from four weeks after neck dissection surgery Contacts Consultant oncologist:...
 Physiotherapy advice and exercises from four weeks after neck dissection surgery Patient Information Series PI 47 East and North Hertfordshire NHS Trust 2 Contacts Members of Head & Neck Team: Consultant
Physiotherapy advice and exercises from four weeks after neck dissection surgery Patient Information Series PI 47 East and North Hertfordshire NHS Trust 2 Contacts Members of Head & Neck Team: Consultant
What to expect following spinal cord injury. Information for patients Therapy Services
 What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
Obinutuzumab (lymphoma) Obinutuzumab (lymphoma)
 Obinutuzumab (lymphoma) Obinutuzumab (lymphoma) This leaflet is offered as a guide to you and your family. The possible benefits of this treatment vary: for some people, this immune therapy may reduce
Obinutuzumab (lymphoma) Obinutuzumab (lymphoma) This leaflet is offered as a guide to you and your family. The possible benefits of this treatment vary: for some people, this immune therapy may reduce
Feeling depressed? Feeling anxious? What may help. What may help
 2. EMOTIONAL NEEDS A long and serious illness takes its toll as much on the mind as it does on the body. Distress or emotional upset can arise at any time and can last for days, weeks, or even months.
2. EMOTIONAL NEEDS A long and serious illness takes its toll as much on the mind as it does on the body. Distress or emotional upset can arise at any time and can last for days, weeks, or even months.
Huntington s disease General information about Huntington s and the Huntington's Disease Association
 Huntington s disease General information about Huntington s and the Huntington's Disease Association General information about Huntington s disease Huntington s disease (HD), is a hereditary disorder of
Huntington s disease General information about Huntington s and the Huntington's Disease Association General information about Huntington s disease Huntington s disease (HD), is a hereditary disorder of
Support for Kidney Cancer
 Page 1 Fact sheet Introduction Our series of kidney cancer fact sheets have been developed to help you understand more about kidney cancer. This fact sheet provides support information for people affected
Page 1 Fact sheet Introduction Our series of kidney cancer fact sheets have been developed to help you understand more about kidney cancer. This fact sheet provides support information for people affected
Subtotal and Total Gastrectomy
 DR ADEEB MAJID MBBS, MS, FRACS, ANZHPBA FELLOWSHIP GENERAL, HEPATOBILIARY AND PANCREATIC SURGEON CALVARY MATER HOSPITAL NEWCASTLE Information for patients and carers Subtotal and Total Gastrectomy Introduction
DR ADEEB MAJID MBBS, MS, FRACS, ANZHPBA FELLOWSHIP GENERAL, HEPATOBILIARY AND PANCREATIC SURGEON CALVARY MATER HOSPITAL NEWCASTLE Information for patients and carers Subtotal and Total Gastrectomy Introduction
4.2 Later in Life Issues Coping, Treatment and Decision Making at the End of Life
 4.2 Later in Life Issues Coping, Treatment and Decision Making at the End of Life This Help Sheet offers information that can help when someone with Progressive Supranuclear Palsy (PSP) is at the end of
4.2 Later in Life Issues Coping, Treatment and Decision Making at the End of Life This Help Sheet offers information that can help when someone with Progressive Supranuclear Palsy (PSP) is at the end of
Capecitabine (Xeloda )
 1 Capecitabine (Xeloda ) This fact sheet is for anyone diagnosed with pancreatic cancer who would like to find out more about capecitabine chemotherapy to treat pancreatic cancer. It provides information
1 Capecitabine (Xeloda ) This fact sheet is for anyone diagnosed with pancreatic cancer who would like to find out more about capecitabine chemotherapy to treat pancreatic cancer. It provides information
The Eating Disorders Service
 Contact us Clinical Team Leader Eating Disorders Service Steps Unit Southmead Hospital Bristol BS10 5NB 0117 3236113 www.awp.nhs.uk The Eating Disorders Service PALS To make a comment, raise a concern
Contact us Clinical Team Leader Eating Disorders Service Steps Unit Southmead Hospital Bristol BS10 5NB 0117 3236113 www.awp.nhs.uk The Eating Disorders Service PALS To make a comment, raise a concern
Oral care & swallowing
 Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Bowel health and screening: carers guide. A booklet for carers of people who use easy read materials
 Bowel health and screening: carers guide A booklet for carers of people who use easy read materials Contents About this booklet Page 3: Page 4: Page 5: Page 6: Page 6: Page 7: Page 8: Page 10: Page 10:
Bowel health and screening: carers guide A booklet for carers of people who use easy read materials Contents About this booklet Page 3: Page 4: Page 5: Page 6: Page 6: Page 7: Page 8: Page 10: Page 10:
Video swallow examination
 Radiology Department John Radcliffe Hospital and Churchill Hospital Video swallow examination Information for patients Video swallow examination The radiology department has received a request for you
Radiology Department John Radcliffe Hospital and Churchill Hospital Video swallow examination Information for patients Video swallow examination The radiology department has received a request for you
Therapy following a neck of femur fracture
 INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
1.0 Presenting complaint: Onset 1.1 When it started? 1.2 How did it start? Progress 1.3 Has the problem increased /decreased so far?
 Case history Sr. No. Name Sex M / F Age Marital Status B / S / M / W Occupation Date 1.0 Presenting complaint: Onset 1.1 When it started? 1.2 How did it start? Progress 1.3 Has the problem increased /decreased
Case history Sr. No. Name Sex M / F Age Marital Status B / S / M / W Occupation Date 1.0 Presenting complaint: Onset 1.1 When it started? 1.2 How did it start? Progress 1.3 Has the problem increased /decreased
Worcestershire Health and Care NHS Trust. Autism Assessment. The Umbrella Pathway
 Worcestershire Health and Care NHS Trust Autism Assessment The Umbrella Pathway www.hacw.nhs.uk Working together Autism for outstanding Assessment care 1 After a child s referral to the Umbrella Pathway
Worcestershire Health and Care NHS Trust Autism Assessment The Umbrella Pathway www.hacw.nhs.uk Working together Autism for outstanding Assessment care 1 After a child s referral to the Umbrella Pathway
Radiology Department CT Enteroclysis examination Information for patients
 Oxford University Hospitals NHS Trust Radiology Department CT Enteroclysis examination Information for patients This leaflet explains CT Enteroclysis, what is involved and the risks. Details of what you
Oxford University Hospitals NHS Trust Radiology Department CT Enteroclysis examination Information for patients This leaflet explains CT Enteroclysis, what is involved and the risks. Details of what you
CAMHS. Your guide to Child and Adolescent Mental Health Services
 CAMHS Your guide to Child and Adolescent Mental Health Services The support I received from CAHMS was invaluable and I do not know where I would be now without it. I now study Health and Social Care and
CAMHS Your guide to Child and Adolescent Mental Health Services The support I received from CAHMS was invaluable and I do not know where I would be now without it. I now study Health and Social Care and
What to expect in the last days and hours of life in the Intensive Care Unit (ICU)
 What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
Speech and language therapy exercises
 The Clatterbridge Cancer Centre NHS Foundation Trust Speech and language therapy exercises Rehabilitation and Support A guide for patients and carers Contents Why do I need these exercises?...1 How to
The Clatterbridge Cancer Centre NHS Foundation Trust Speech and language therapy exercises Rehabilitation and Support A guide for patients and carers Contents Why do I need these exercises?...1 How to
