Chewing gum for the treatment of postoperative nausea and vomiting: a pilot randomized controlled trial
|
|
|
- Frederica Daniels
- 6 years ago
- Views:
Transcription
1 British Journal of Anaesthesia, 118 (1): 83 9 (2017) doi: /bja/aew375 Clinical Practice Chewing gum for the treatment of postoperative nausea and vomiting: a pilot randomized controlled trial J. N. Darvall 1,2,3, *, M. Handscombe 1 and K. Leslie 1,3,4,5 1 Department of Anaesthesia and Pain Management, Royal Melbourne Hospital, Melbourne, Victoria, Australia, 2 Royal Melbourne Hospital Clinical School, Faculty of Medicine, Dentistry and Health Sciences, University of Melbourne, Melbourne, Victoria, Australia, 3 Anaesthesia, Perioperative and Pain Medicine Unit, University of Melbourne, Melbourne, Victoria, Australia, 4 Department of Pharmacology and Therapeutics, University of Melbourne, Melbourne, Victoria, Australia and 5 Department of Epidemiology and Preventive Medicine, Monash University, Melbourne, Victoria, Australia *Corresponding author. jai.darvall@mh.org.au Abstract Background. A novel treatment, chewing gum, may be non-inferior to in inhibiting postoperative nausea and vomiting (PONV) in female patients after laparoscopic or breast surgery. In this pilot study, we tested the feasibility of a large randomized controlled trial. Methods. We randomized 94 female patients undergoing laparoscopic or breast surgery to 4 mg i.v. or chewing gum if PONV was experienced in the postanaesthesia care unit (PACU). The primary outcome was full resolution of PONV, with non-inferiority defined as a difference between groups of <15% in a per protocol analysis. Secondary outcomes were PACU stay duration, anti-emetic use, and acceptability of anti-emetic treatment. The feasibility of implementing the protocol in a larger trial was assessed. Results. Postoperative nausea and vomiting in the PACU occurred in 13 (28%) patients and 15 (31%) chewing gum patients (P¼0.75). Three chewing gum patients could not chew gum when they developed PONV. On a per protocol basis, full resolution of PONV occurred in five of 13 (39%) vs nine of 12 (75%) chewing gum patients [risk difference 37% (6.3 67%), P¼0.07]. There was no difference in secondary outcomes between groups. Recruitment was satisfactory, the protocol was acceptable to anaesthetists and nurses, and data collection was complete. Conclusions. In this pilot trial, chewing gum was not inferior to for treatment of PONV after general anaesthesia for laparoscopic or breast surgery in female patients. Our findings demonstrate the feasibility of a larger, multicentred randomized controlled trial to investigate this novel therapy. Clinical trial registration. Australian New Zealand Clinical Trials Registry: ACTRN Key words: chewing gum; ; postanaesthesia nursing; postoperative nausea and vomiting Postoperative nausea and vomiting (PONV) affects one-third of untreated patients after general anaesthesia. 1 2 It is a leading cause of admission after planned ambulatory surgery and may lead to dehydration, bleeding, surgical wound complications, and Editorial decision October 7, 2016; Accepted: October 7, 2016 VC The Author Published by Oxford University Press on behalf of the British Journal of Anaesthesia. All rights reserved. For Permissions, please journals.permissions@oup.com 83
2 84 Darvall et al. Editor s key points Chewing gum may be as effective as in inhibiting postoperative nausea and vomiting (PONV). Either 4 mg or chewing gum was randomly provided to female patients who had PONV after laparoscopic or breast surgery, to test the feasibility of a large randomized controlled trial. A large randomized controlled trial would be feasible, because recruitment was satisfactory, the protocol was acceptable to anaesthetists and nurses, and data collection was complete. aspiration of gastric contents. 3 4 Well-established guidelines for the pharmacological prophylaxis and treatment of PONV exist; however, medications such as the 5-hydroxytryptamine type 3 (5- HT) receptor antagonists are only partly effective and have sideeffects. 5 More recently, interest has emerged in nonpharmacological therapies, such as P6 stimulation with acupuncture modalities 6 and ginger, 7 which have advantages including low cost, favourable side-effect profile, and patient acceptability. Chewing gum has been prospectively evaluated as a therapy to reduce postoperative paralytic ileus after gastrointestinal surgery. Postulated mechanisms of its effect surround the principle of sham feeding, with chewing resulting in increased gastrointestinal activity via cephalic vagal stimulation. 8 Recent metaanalyses (the largest involving 272 patients across seven randomized controlled trials) have demonstrated a reduced time to first flatus and bowel motion, and a non-significant trend towards earlier hospital discharge To date, however, no study has examined the effect of gum chewing on PONV. We previously conducted a prospective cohort study to assess the safety and acceptability of chewing gum in the postanaesthesia care unit (PACU), enrolling 41 patients undergoing ambulatory gynaecological laparoscopy. 12 Thirty-one patients (76%) were awake enough to chew gum. Chewing gum was acceptable to patients and PACU nurses, with no identified safety concerns. Chewing gum has also been linked to lowered cortisol concentrations, improved stress and anxiety, and more positive mood in the research setting. We therefore conducted a pilot randomized controlled noninferiority trial to test the hypothesis that chewing gum in the PACU would prove to be non-inferior to for the treatment of PONV in female patients after laparoscopic or breast surgery and to test the feasibility of a large multicentre randomized controlled trial using this protocol. The primary outcome was full resolution of PONV after either or chewing gum. Secondary outcomes were the duration of PACU stay, anti-emetic use in the PACU, and patient acceptability of anti-emetic treatment. Feasibility outcomes were recruitment rate, protocol compliance, incidence of PONV, ability to chew gum, and the primary outcome. Methods This pilot randomized controlled non-inferiority trial was conducted in the Department of Anaesthesia and Pain Management, Royal Melbourne Hospital. Approval was gained from the hospital Human Research and Ethics Committee (21 December 2015, HREC number ), and the trial was registered with the Australian New Zealand Clinical Trials Registry (ACTRN ; 3 December 2015). Female patients aged 18 yr and of ASA physical status I III undergoing laparoscopic or breast surgery were enrolled between January and June 2016, after being advised that the principal purpose of the study was to assess the feasibility of a larger randomized controlled trial and after written informed consent had been obtained. Patients were excluded if they had inadequate English comprehension, significant cardiorespiratory impairment, impaired pharyngeal or oesophageal function, phenylketonuria (contraindication to the sweetener aspartame in chewing gum), a full upper or lower denture (not feasible to chew gum), or a contraindication to any of the protocolized anti-emetic drugs. Patients were randomized to either chewing gum or after written informed consent had been obtained and before surgery. The randomization schedule was created via a computerized random number generator, with sequentially numbered envelopes used for allocation concealment until PONV developed in the PACU. Patients, anaesthetists, PACU nurses, and observers therefore were blind to group allocation until PONV developed in the PACU. Procedure Induction of general anaesthesia was accomplished with either fentanyl or alfentanil, propofol, and a non-depolarizing neuromuscular blocker if indicated. Midazolam premedication was permitted at the discretion of the attending anaesthetist. Anaesthesia was maintained with sevoflurane without nitrous oxide. Patient monitoring was established in accordance with the standards published by the Australian and New Zealand College of Anaesthetists. At the conclusion of anaesthesia, antagonism of neuromuscular block was accomplished with neostigmine and glycopyrrolate, or if the train of four count was zero with sugammadex 200 mg. Non-opioid analgesics and additional fentanyl or morphine were given at the discretion of the attending anaesthetist. Anti-emetic prophylaxis Intraoperative anti-emetic prophylaxis was protocolized according to simplified Apfel risk factors, commensurate with the Consensus Guidelines for the Management of Postoperative Nausea and Vomiting published by the Society for Ambulatory Anesthesia. 5 Risk factors were female gender, non-smoking status, past history of PONV or motion sickness, or anticipated requirement for postoperative opioids (defined as estimated requirement of at least 20 mg oral oxycodone equivalent in the first 24 h after surgery, consistent with the initial validation trials of the Apfel scoring system). 15 Patients with one risk factor ( low risk ) received no prophylaxis; patients with two or three risk factors ( medium risk ) received dexamethasone 4 mg i.v.; and patients with four risk factors ( high risk ) received dexamethasone 4 mg i.v. and mg. Treatment of postoperative nausea and vomiting Patients randomized to chewing gum and experiencing PONV in the PACU, with an Observer s Assessment of Alertness/Sedation (OAA/S) rating scale of 5 16 ( responding readily to name spoken in normal tone ) and with the PACU nurse satisfied that the patient was not sleeping between observations, commenced gum chewing (Wrigley s Extra Sugarfree Gum VR, peppermint flavour), aiming for a period of 15 min. Patients randomized to, or those randomized to chewing gum who either refused it or were too drowsy, received 4 mg i.v. in the event of PONV. The feasibility of chewing gum was recorded (able; unable because of refusal; unable because of drowsiness). Rescue
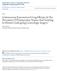
3 Chewing gum and PONV 85 anti-emetics if the first-line therapy was not fully successful consisted of the following: first line, 4 mg i.v. (if not already administered); second line, mg i.v.; third line, promethazine 6.25 mg i.v.; fourth line, dexamethasone 4 mg i.v.; fifth line, prochlorperazine 12.5 mg i.v.; and sixth line, propofol 20 mg i.v. bolus. Observers recorded the number of episodes of nausea, retching, and vomiting and the time when each one occurred. Relief of PONV was graded on a four-point verbal descriptive scale: worse, no change, partial resolution, or full resolution. At readiness for discharge from the PACU, patients graded their acceptability of both anti-emetic treatment and anaesthetic care using a five-point Likert scale ranging from completely unacceptable to completely acceptable. Antiemetic and analgesic requirements for the first 24 h after surgery were recorded. Sample size calculation The primary outcome was full resolution of PONV after the randomized treatment. The target sample size for a definitive non-inferiority randomized controlled trial was computed. A non-inferiority trial using a hypothesized difference for equivalence of 15% (i.e. effective treatment of PONV in 60 75% of chewing gum-treated patients considered equivalent to treatment) at a power of 80% and a¼0.05 would require 204 patients, 102 in each group. This clinically relevant margin for equivalence was chosen as, if achieved, it was considered likely to result in acceptance and potentially practice change by anaesthetists. In our previous cohort study, 12 85% of patients achieved an OAA/S score of 5 and were thus deemed sufficiently awake to chew gum, and 40% of patients experienced PONV despite appropriate prophylaxis. On the assumption that 40% of randomized patients would experience PONV, of whom 85% would be sufficiently awake to chew gum, a total of 600 patients would be required, 300 in each group. To guide a future large randomized controlled trial, we conducted an initial pilot trial on a targeted convenience sample of 100 patients. The feasibility objectives for this pilot trial were as follows: (i) to refine and test the trial protocol for a large multicentre study; (ii) to assess acceptability of the trial protocol to our patients and anaesthetic and nursing staff, because a high recruitment and participation rate will be required for a viable definitive study; (iii) to confirm the high rates of PONV despite prophylaxis seen in our previous study, to inform sample size estimates for a definitive trial; (iv) to assess the proportion of patients meeting criteria for chewing gum in the PACU, to guide the external validity of this trial; and (v) to assess the event rates using the protocol developed. Feasibility outcomes were recruitment rate, protocol compliance, incidence of PONV, ability to chew gum, and the primary outcome. Statistical analysis Continuous data were tested for normality. Normally distributed data were summarized using the mean (SD) and compared using Student s unpaired two-tailed t-tests. Skewed data were summarized using the median (interquartile range) and Enrolment Assessed for eligibility (n=155) Excluded (n=53) Patient declined (n=25) Anaesthetist declined (n=7) Direct to theatre from radiology (n=6) Other reasons (n=15) Consented (n=102) Excluded (n=8) Anaesthetist declined (n=5) Other reasons (n=3) Randomized (n=94) Allocated to chewing gum (n=48) Received allocated intervention (n=12) Did not receive allocated intervention (n=36) No PONV (n=33) Too sleepy to chew (n=2) Refused gum (n=1) Allocation Allocated to (n=46) Received allocated intervention (n=13) Did not receive allocated intervention (n=33) No PONV (n=33) Lost to follow-up (n=0) Discontinued intervention (n=0) Follow-up Lost to follow-up (n=0) Discontinued intervention (n=0) Analysed for primary outcome (n=12) Excluded from analysis (n=0) Analysis Analysed for primary outcome (n=13) Excluded from analysis (n=0) Fig 1 CONSORT diagram. PONV, postoperative nausea and vomiting.
4 86 Darvall et al. compared using ranksum tests. Categorical data were summarized using the number (%) and compared using the v 2 test or Fisher s exact test where applicable. Survival data were summarized using the median (interquartile range) and compared using log-rank tests. Statistical analyses were performed using Stata 14.1 (Stata Corporation, College Station, TX, USA). A value of P <0.05 was considered statistically significant. Table 1 Baseline characteristics of patients. Values are expressed as the mean (SD), median (interquartile range), or n (%). PONV, postoperative nausea and vomiting; postoperative opioid requirement is defined as at least 20 mg oral oxycodone equivalent requirement in first 24 h after surgery Variable Control group (n¼46) Chewing gum group (n¼48) Age (yr) 46 (14) 46 (16) BMI (kg m 2 ) 29 (24 36) 25 (22 30) ASA physical status I 15 (33) 19 (40) II 29 (63) 24 (50) III 2 (4) 5 (10) Non-smoker 41 (89) 41 (85) PONV/motion sickness 21 (46) 29 (60) Postoperative opioid 2 (4) 3 (6) Apfel score 1 2 (4) 2 (4) 2 25 (54) 19 (40) 3 18 (39) 27 (56) 4 1 (2) 0 (0) Type of surgery Laparoscopic 21 (46) 27 (56) Breast surgery 25 (54) 21 (44) Table 2 Intraoperative characteristics (intention to treat). Values are expressed as the mean (SD), median (interquartile range), or n (%) Variable Ondansetron group (n¼46) Chewing gum group (n¼48) P-value Midazolam 13 (28) 12 (25) 0.72 Dose (mg) 2.0 (0.6) 1.8 (0.2) 0.47 Morphine equivalents 13 (10 20) 13 (7 17) 0.83 (mg) Propofol (mg) 184 (40) 177 (40) 0.38 Neuromuscular block 23 (50) 28 (58) 0.42 Neostigmine 14 (30) 23 (48) 0.08 Sugammadex 9 (20) 5 (10) 0.21 Sevoflurane 2.0 ( ) 2.0 ( ) 0.50 (% end-tidal) I.V. fluid 45 (98) 47 (98) 0.98 Dose (litres) 0.6 ( ) 0.7 ( ) 0.43 Anti-emetic 44 (96) 47 (98) 0.53 Dexamethasone 44 (96) 47 (98) 0.53 Droperidol 1 (2) 0 (0) 0.49 Duration of anaesthesia (min) 57 (31 75) 62 (34 91) 0.39 We used a per protocol analysis for the primary outcome, because intention-to-treat analyses, with usually smaller differences in efficacy between treatments than per protocol analyses, make it easier to establish non-inferiority by rejecting the null hypothesis of no difference between treatments. 17 Risk differences with 90% confidence intervals (CIs) were calculated. 17 We also conducted intention-to-treat and per treatment analyses, because expert guidance suggests performing these analyses, with equivalence or non-inferiority established when both intention-to-treat and per protocol analyses agree. 17 Results A total of 155 patients were screened for inclusion in this pilot trial. After exclusions, 94 patients were enrolled and followed to the final analysis, 46 randomized to and 48 to chewing gum (Fig. 1) between 5 February 2016 and 23 June There were no protocol violations. The two groups were similar in terms of patient characteristics, PONV risk factors, and surgery and anaesthesia details (Tables 1 and 2). Table 3 Postoperative characteristics (intention to treat). Values are expressed as the mean (SD), median (interquartile range), or n (%). OAA/S, Observers Assessment of Alertness/Sedation Score; PACU, postanaesthesia care unit; PONV, postoperative nausea and vomiting Variable OndansetronChewing group gum group (n¼46) (n¼48) P-value Duration of PACU stay (min) 42 (30 63) 46.5 ( ) 0.22 PACU opioid 25 (54) 28 (58) 0.70 Morphine equivalents (mg) 6.7 ( ) 6.7 ( ) 0.94 PACU nausea First event 12 (26) 15 (31) 0.58 Second event 2 (4) 4 (8) 0.43 Third event 1 (2) 0 (0) 0.30 PACU vomiting First event 3 (7) 3 (6) 0.96 Second event 1 (2) 3 (6) 0.33 Third event 0 (0) 1 (2) 0.33 PACU PONV 13 (28) 15 (31) 0.75 PACU PONV initial treatment Ondansetron 13 (100) 3 (20) Chewing gum 0 (0) 12 (80) <0.001 Full resolution after initial 5 (38) 9 (60) 0.26 treatment Time to full resolution (min) 7 (4 7) 10 (7 15) 0.08 PACU PONV subsequent treatment 4 (9) 7 (15) 0.52 Acceptability (PONV treatment) Neither acceptable nor 1 (8) 0 (0) unacceptable Mildly acceptable 3 (23) 7 (47) Completely acceptable 9 (69) 8 (53) 0.32 Ward treatment of PONV patients Anti-emetic 8 (62) 7 (47) 0.43 Opioid 9 (69) 12 (80) 0.43 Morphine equivalents (mg) 10 ( ) 7.7 ( ) 0.62
5 Chewing gum and PONV 87 Postoperative nausea and vomiting in the PACU occurred in 13 (28%) of the group patients and 15 (31%) of the chewing gum group patients (P¼0.75; Table 3 and Fig. 2). Three patients randomized to chewing gum did not proceed with gum chewing (two patients were too drowsy; one refused) and received instead. Therefore, 13 group patients and 12 chewing gum group patients were included in the per protocol analysis (the primary analysis), 13 group patients and 15 chewing gum group patients were included in the intention-to-treat analysis, and 16 group patients and 12 chewing gum group patients were included in the per treatment analysis (Fig. 3). The median (interquartile range) time for which the gum was chewed was 31.5 (17 36) min. Full resolution of PONV was seen in five of 13 (39%) group patients and nine of 12 (75%) chewing gum group patients [per protocol risk difference (90% CI): 37% (6.3 67%), P¼0.07; confirming non-inferiority]. Both intention-to-treat risk difference (90% CI) of 22% ( 8.9 to 52.0%), P¼0.22 and per treatment risk difference (90% CI) of 44% ( %), P¼0.02 confirmed non-inferiority (Fig. 3). There was no difference in the time to full resolution of PONV between groups (Table 3). Recurrence of PONV in the PACU after full resolution was seen in one -treated patient (39 min after initial full resolution, requiring ) and two chewing gumtreated patients (one patient 24 min after initial full resolution, resolving completely with further chewing gum requested by the patient, and one patient 34 min after full resolution, requiring ). Rescue PONV treatment, duration of PACU stay, and requirement for ward anti-emetic treatment did not differ between groups (Table 3). All sticks of chewing gum were retrieved from patients, with no safety concerns identified. No differences in acceptability of PONV treatment were found, with all patients finding chewing gum either completely or mildly acceptable. Discussion In this randomized controlled pilot trial, we demonstrated the feasibility of conducting a large randomized controlled trial. We showed that chewing gum was not inferior to in the treatment of PONV in the PACU in female patients after laparoscopic or breast surgery. The incidence of PONV, acceptability of chewing gum, and effect size for full resolution recorded in this study will be valuable in planning the definitive study. This is the first randomized controlled trial assessing this novel treatment for PONV. Strengths of our study include a high recruitment rate, complete protocol adherence, and complete data collection, including follow-up of anti-emetic and opioid requirements for 24 h after surgery. Our study has several limitations. This study was planned as a pilot rather than a definitive randomized controlled trial, using a sample based on convenience rather than a sample size calculation. We did not measure nausea severity, merely recorded it as present or absent. We therefore cannot report whether the severity of nausea was similar in the two groups. Twenty per cent of the chewing gum group patients were unable to chew gum because of either Ondansetron group PONV = 13 Chewing gum group PONV = 15 1 (2 too drowsy, 1 refused gum) 12 received gum 5 fully 7 partially 1 no change 3 partially 9 fully 3 partially 1 recurrent event (fully after ) 1 received further promethazine 2 recurrent PONV episodes (1 fully after 2nd gum) (1 fully after ) 1 received further Fig 2 Flowchart of patients with postoperative nausea and vomiting (PONV) in the postanaesthesia care unit (PACU).
6 88 Darvall et al. Intention-to-treat 21.5% (90% CI: 9 52%); P=0.22 Ondansetron = 13; success = 5 (38.5%) Chewing gum = 15; success = 9 (60.0%) Per protocol 36.5% (90% CI: 6 67%); P=0.07 Ondansetron = 13; success = 5 (38.5%) Chewing gum = 12; success = 9 (75.0%) Per treatment 44% (90% CI: 16 72%); P=0.02 Ondansetron = 16; success = 5 (31.3%) Chewing gum = 12; success = 9 (75.0%) Risk difference (%) 75 Fig 3 Difference between percentage full resolution of postoperative nausea and vomiting (PONV) in chewing gum group vs group via intention-totreat, per protocol and as-treated analyses. CI, confidence interval. drowsiness or a preference to avoid it. The treatment is therefore not universally applicable to postoperative patients. Although chewing gum represented a potential PONV treatment for patients in this trial, whether it would be suitable for patients undergoing more major surgery, with higher opioid requirements and potentially longer emergence times, requires further research. We used a flavoured (peppermint) gum, which may have confounded the association between chewing and PONV treatment. Peppermint has been shown to have effects on gastric emptying, although literature is conflicting (evidence of both increasing and decreasing gastric motility) Some evidence also exists for aromatherapy as a treatment for PONV, with blends including ginger found to be efficacious. 20 A recent Cochrane review, however, suggests no benefit from peppermint aromatherapy for PONV. 21 Finally, PONV beyond the PACU was not measured in our study, although anti-emetic requirements were used as a surrogate marker for its incidence. This pilot study has potentially important implications for practice, if the results are confirmed in a definitive trial. Chewing gum is a readily accessible therapy, of negligible cost and without storage considerations. It is also familiar to patients and can be self-administered. In contrast, the requirement for equipment and training in some non-pharmacological techniques (e.g. acupressure or transcutaneous electrical nerve stimulation) limits applicability for the majority of anaesthetists. Chewing gum has been acceptable to patients and PACU staff in two studies by this group at different sites, which lends support to the external validity of our findings. Our protocol was simple to implement and acceptable to anaesthetists and nurses, and would be generalizable to a multicentred study. The non-inferiority margin remains appropriate, but the sample size calculation for the main study might need to be modified in light of the lower than expected incidence of PONV (30% instead of 40%). Inclusion of a flavourless gum group may also bear consideration. Measurement of the severity of PONV using a previously validated ordinal instrument will improve cross-study comparability, as will tracking rates of PONV and efficacy of treatment beyond the PACU. A future trial design may also benefit from randomization of patients when experiencing PONV, making analysis of end points simpler. Conclusion In summary, chewing gum was not inferior to for the treatment of PONV in this pilot, randomized controlled trial of female patients undergoing general anaesthesia for laparoscopic or breast surgery. Our findings demonstrate the feasibility of a larger, multicentred randomized controlled trial to investigate this novel therapy. Authors contributions Study conception: J.N.D. Study design, study coordination data analysis, manuscript preparation: J.N.D., K.L. Patient recruitment: M.H. Data collection: J.N.D., M.H. Data analysis: J.N.D., K.L. Manuscript review: M.H. Declaration of interest None declared. Funding Australian and New Zealand College of Anaesthetists (project grant 16/040). References 1. Apfel CC, Korttila K, Abdalla M, et al. A factorial trial of six interventions for the prevention of postoperative nausea and vomiting. N Engl J Med 2004; 350: Gan TJ. Postoperative nausea and vomiting can it be eliminated? JAMA 2002; 287:
7 Chewing gum and PONV Meeks GR, Waller GA, Meydrech EF, Flautt FH Jr. Unscheduled hospital admission following ambulatory gynecologic surgery. Obstet Gynecol 1992; 80: Apfel CC, Heidrich FM, Jukar-Rao S, et al. Evidence-based analysis of risk factors for postoperative nausea and vomiting. Br J Anaesth 2012; 109: Gan TJ, Diemunsch P, Habib AS, et al. Consensus guidelines for the management of postoperative nausea and vomiting. Anesth Analg 2014; 118: Frey UH, Scharmann P, Löhlein C, Peters J. P6 acustimulation effectively decreases postoperative nausea and vomiting in high-risk patients. Br J Anaesth 2009; 102: Chaiyakunapruk N, Kitikannakorn N, Nathisuwan S, Leeprakobboon K, Leelasettagool C. The efficacy of ginger for the prevention of postoperative nausea and vomiting: a meta-analysis. Am J Obstet Gynecol 2006; 194: Person B, Wexner SD. The management of postoperative ileus. Curr Prob Surg 2006; 43: Fitzgerald JE, Ahmed I. Systematic review and meta-analysis of chewing-gum therapy in the reduction of postoperative paralytic ileus following gastrointestinal surgery. World J Surg 2009; 33: Chan MK, Law WL. Use of chewing gum in reducing postoperative ileus after elective colorectal resection: a systematic review. Dis Colon Rectum 2007; 50: de Castro SM, van den Esschert JW, van Heek NT, et al. A systematic review of the efficacy of gum chewing for the amelioration of postoperative ileus. Dig Surg 2008; 25: Darvall JN, Simmons SW, Leslie K. Acceptability of chewing gum for postoperative nausea and vomiting prevention in high risk patients: a pilot study. Anaesth Intensive Care 2011; 39: Scholey A, Haskell C, Robertson B, Kennedy D, Milne A, Wetherell M. Chewing gum alleviates negative mood and reduces cortisol during acute laboratory psychological stress. Physiol Behav 2009; 97: Smith A. Effects of chewing gum on cognitive function, mood and physiology in stressed and non-stressed volunteers. Nutr Neurosci 2010; 13: Apfel CC, L a ar a E, Koivuranta M, Greim CA, Roewer N. A simplified risk score for predicting postoperative nausea and vomiting: conclusions from crossvalidations between two centers. Anesthesiology 1999; 91: Chernik D, Gillings D, Laine H, et al. Validity and reliability of the Observer s Assessment of Alertness/Sedation Scale: study with intravenous midazolam. J Clin Psychopharmacol 1990; 10: Walker E, Nowacki AS. Understanding equivalence and noninferiority testing. J Gen Intern Med 2011; 26: Inamori M, Akiyama T, Akimoto K, et al. Early effects of peppermint oil on gastric emptying: a crossover study using a continuous real-time 13 C breath test (BreathID system). J Gastroenterol 2007; 42: Hiki N, Kurosaka H, Tatsutomi Y, et al. Peppermint oil reduces gastric spasm during upper endoscopy: a randomized, double-blind, double-dummy controlled trial. Gastrointest Endosc 2003; 57: Hunt R, Dienemann J, Norton HJ, et al. Aromatherapy as treatment for postoperative nausea. A randomized trial. Anesth Analg 2013; 117: Hines S, Steels E, Chang A, Gibbons K. Aromatherapy for treatment of postoperative nausea and vomiting. Cochrane Database Syst Rev 2012; 4: CD Handling editor: T. Asai
Droperidol has comparable clinical efficacy against both nausea and vomiting
 British Journal of Anaesthesia 103 (3): 359 63 (2009) doi:10.1093/bja/aep177 Advance Access publication July 15, 2009 has comparable clinical efficacy against both nausea and vomiting C. C. Apfel 1 *,
British Journal of Anaesthesia 103 (3): 359 63 (2009) doi:10.1093/bja/aep177 Advance Access publication July 15, 2009 has comparable clinical efficacy against both nausea and vomiting C. C. Apfel 1 *,
SECTION 1: FEELING SICK
 Risks associated with your anaesthetic SECTION 1: This leaflet explains the causes of sickness following anaesthesia and surgery, what can text be done to prevent it occurring, and treatments available
Risks associated with your anaesthetic SECTION 1: This leaflet explains the causes of sickness following anaesthesia and surgery, what can text be done to prevent it occurring, and treatments available
DEXAMETHASONE WITH EITHER GRANISETRON OR ONDANSETRON FOR POSTOPERATIVE NAUSEA AND VOMITING IN LAPAROSCOPIC SURGERY
 DEXAMETHASONE WITH EITHER GRANISETRON OR ONDANSETRON FOR POSTOPERATIVE NAUSEA AND VOMITING IN LAPAROSCOPIC SURGERY Alia S. Dabbous *, Samar I. Jabbour-Khoury **, Viviane G Nasr ***, Adib A Moussa ***,
DEXAMETHASONE WITH EITHER GRANISETRON OR ONDANSETRON FOR POSTOPERATIVE NAUSEA AND VOMITING IN LAPAROSCOPIC SURGERY Alia S. Dabbous *, Samar I. Jabbour-Khoury **, Viviane G Nasr ***, Adib A Moussa ***,
4/18/2018. Disclosure. Learning Objectives. St. Vincent Healthcare. Supportive Literature. Background
 Implementation of a risk-score-dependent antiemetic protocol to reduce post-operative nausea and vomiting (PONV) in inpatient surgical patients Eugene P. Eldridge, PharmD, RPh PGY-1 Pharmacy Resident St.
Implementation of a risk-score-dependent antiemetic protocol to reduce post-operative nausea and vomiting (PONV) in inpatient surgical patients Eugene P. Eldridge, PharmD, RPh PGY-1 Pharmacy Resident St.
Measure Abbreviation: PONV 01 (MIPS 430)
 Measure Abbreviation: PONV 01 (MIPS 430) *PONV 01 is built to the specification outlined by the Merit Based Incentive Program (MIPS) 430: Prevention of Post-Operative Nausea and Vomiting (PONV) Combination
Measure Abbreviation: PONV 01 (MIPS 430) *PONV 01 is built to the specification outlined by the Merit Based Incentive Program (MIPS) 430: Prevention of Post-Operative Nausea and Vomiting (PONV) Combination
Efficacy of palonosetron for the prevention of postoperative nausea and vomiting: a randomized, double-blinded, placebo-controlled trial
 British Journal of Anaesthesia 112 (3): 485 90 (2014) Advance Access publication 22 October 2013. doi:10.1093/bja/aet340 CLINICAL PRACTICE Efficacy of palonosetron for the prevention of postoperative nausea
British Journal of Anaesthesia 112 (3): 485 90 (2014) Advance Access publication 22 October 2013. doi:10.1093/bja/aet340 CLINICAL PRACTICE Efficacy of palonosetron for the prevention of postoperative nausea
Measure Abbreviation: PONV 01 (MIPS 430)
 Measure Abbreviation: PONV 01 (MIPS 430) *PONV 01 is built to the specification outlined by the Merit Based Incentive Program (MIPS) 430: Prevention of Post-Operative Nausea and Vomiting (PONV) Combination
Measure Abbreviation: PONV 01 (MIPS 430) *PONV 01 is built to the specification outlined by the Merit Based Incentive Program (MIPS) 430: Prevention of Post-Operative Nausea and Vomiting (PONV) Combination
Satisfactory Analgesia Minimal Emesis in Day Surgeries. (SAME-Day study) A Randomized Control Trial Comparing Morphine and Hydromorphone
 Satisfactory Analgesia Minimal Emesis in Day Surgeries (SAME-Day study) A Randomized Control Trial Comparing Morphine and Hydromorphone HARSHA SHANTHANNA ASSISTANT PROFESSOR ANESTHESIOLOGY MCMASTER UNIVERSITY
Satisfactory Analgesia Minimal Emesis in Day Surgeries (SAME-Day study) A Randomized Control Trial Comparing Morphine and Hydromorphone HARSHA SHANTHANNA ASSISTANT PROFESSOR ANESTHESIOLOGY MCMASTER UNIVERSITY
Editor s key points. M. S. Green*, P. Green, S. N. Malayaman, M. Hepler, L. J. Neubert and J. C. Horrow
 British Journal of Anaesthesia 109 (5): 716 22 (2012) Advance Access publication 24 July 2012. doi:10.1093/bja/aes233 Randomized, double-blind comparison of oral aprepitant alone compared with aprepitant
British Journal of Anaesthesia 109 (5): 716 22 (2012) Advance Access publication 24 July 2012. doi:10.1093/bja/aes233 Randomized, double-blind comparison of oral aprepitant alone compared with aprepitant
Opioid-free total intravenous anaesthesia reduces postoperative nausea and vomiting in bariatric surgery beyond triple prophylaxis
 British Journal of Anaesthesia 112 (5): 906 11 (2014) Advance Access publication 18 February 2014. doi:10.1093/bja/aet551 Opioid-free total intravenous anaesthesia reduces postoperative nausea and vomiting
British Journal of Anaesthesia 112 (5): 906 11 (2014) Advance Access publication 18 February 2014. doi:10.1093/bja/aet551 Opioid-free total intravenous anaesthesia reduces postoperative nausea and vomiting
Dexamethasone combined with other antiemetics for prophylaxis after laparoscopic cholecystectomy
 Original Research Article Dexamethasone combined with other antiemetics for prophylaxis after laparoscopic cholecystectomy T. Uma Maheswara Rao * Associate Professor, Department of Surgery, Konaseema Institute
Original Research Article Dexamethasone combined with other antiemetics for prophylaxis after laparoscopic cholecystectomy T. Uma Maheswara Rao * Associate Professor, Department of Surgery, Konaseema Institute
Gastrointestinal and urinary complications in the postoperative period
 The 13 th Annual Perioperative Medicine Summit Fort Lauderdale, Florida Gastrointestinal and urinary complications in the postoperative period Dan Hunt, MD Professor of Medicine Director, Division of Hospital
The 13 th Annual Perioperative Medicine Summit Fort Lauderdale, Florida Gastrointestinal and urinary complications in the postoperative period Dan Hunt, MD Professor of Medicine Director, Division of Hospital
Efficacy of a single-dose ondansetron for preventing post-operative nausea and vomiting
 European Review for Medical and Pharmacological Sciences 2001; 5: 59-63 Efficacy of a single-dose ondansetron for preventing post-operative nausea and vomiting after laparoscopic cholecystectomy with sevoflurane
European Review for Medical and Pharmacological Sciences 2001; 5: 59-63 Efficacy of a single-dose ondansetron for preventing post-operative nausea and vomiting after laparoscopic cholecystectomy with sevoflurane
Management of post-strabismus nausea and vomiting in children using ondansetron: a value-based comparison of outcomes 1^
 British Journal of Anaesthesia 89 (3): 473-8 (2002) Management of post-strabismus nausea and vomiting in children using ondansetron: a value-based comparison of outcomes 1^ B. Sennaraj 1, D. Shende 1,
British Journal of Anaesthesia 89 (3): 473-8 (2002) Management of post-strabismus nausea and vomiting in children using ondansetron: a value-based comparison of outcomes 1^ B. Sennaraj 1, D. Shende 1,
Comparison of Drugs and Intravenous Crystalloid in Reduction of Postoperative Nausea and Vomiting after Laparoscopic Surgery
 Comparison of Drugs and World Intravenous Journal of Crystalloid Laparoscopic in Reduction Surgery, of January-April Postoperative 2008;1(1):29-34 Nausea and Vomiting after Lap Surgery Comparison of Drugs
Comparison of Drugs and World Intravenous Journal of Crystalloid Laparoscopic in Reduction Surgery, of January-April Postoperative 2008;1(1):29-34 Nausea and Vomiting after Lap Surgery Comparison of Drugs
Nausea and vomiting after surgery
 Sébastien Pierre MD Rachel Whelan Matrix reference 1A02 Key points 5-Hydroxytrytamine type 3 (5-HT 3 ) receptor antagonists, and specifically ondansetron, are the most commonly used antiemetics for both
Sébastien Pierre MD Rachel Whelan Matrix reference 1A02 Key points 5-Hydroxytrytamine type 3 (5-HT 3 ) receptor antagonists, and specifically ondansetron, are the most commonly used antiemetics for both
Pre-medication with controlled-release oxycodone in the management of postoperative pain after ambulatory laparoscopic gynaecological surgery
 Page 1 of 5 Anaesthetics & Critical Care Pre-medication with controlled-release oxycodone in the management of postoperative pain after ambulatory laparoscopic gynaecological surgery B Lim 1, SY Thong
Page 1 of 5 Anaesthetics & Critical Care Pre-medication with controlled-release oxycodone in the management of postoperative pain after ambulatory laparoscopic gynaecological surgery B Lim 1, SY Thong
Palonosetron vs Ondansetron for prevention of postoperative nausea and vomiting in...
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 2 Ver. XI (Feb. 2016), PP 45-49 www.iosrjournals.org Palonosetron vs Ondansetron for prevention
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 2 Ver. XI (Feb. 2016), PP 45-49 www.iosrjournals.org Palonosetron vs Ondansetron for prevention
X.-Y. Yang 1, J. Xiao 2, Y.-H. Chen 2, Z.-T. Wang 2, H.-L. Wang 1, D.-H. He 2 and J. Zhang 1,2, * Abstract
 British Journal of Anaesthesia, 115 (6): 883 9 (2015) doi: 10.1093/bja/aev352 Advance Access Publication Date: 27 October 2015 Clinical Practice Dexamethasone alone vs in combination with transcutaneous
British Journal of Anaesthesia, 115 (6): 883 9 (2015) doi: 10.1093/bja/aev352 Advance Access Publication Date: 27 October 2015 Clinical Practice Dexamethasone alone vs in combination with transcutaneous
Current evidence in acute pain management. Jeremy Cashman
 Current evidence in acute pain management Jeremy Cashman Optimal analgesia Best possible pain relief Lowest incidence of side effects Optimal analgesia Best possible pain relief Lowest incidence of side
Current evidence in acute pain management Jeremy Cashman Optimal analgesia Best possible pain relief Lowest incidence of side effects Optimal analgesia Best possible pain relief Lowest incidence of side
Low-dose Granisetron for the Prevention of Postoperative Nausea and Vomiting
 Low-dose Granisetron for the Prevention of Postoperative Nausea and Vomiting John D. Bridges, BS (Pharm)* Cindy B. Nettle, PharmD* Vijaya J. Dugirrala MD Katie J. Suda, PharmD Kevin W. Garey, PharmD *Baptist
Low-dose Granisetron for the Prevention of Postoperative Nausea and Vomiting John D. Bridges, BS (Pharm)* Cindy B. Nettle, PharmD* Vijaya J. Dugirrala MD Katie J. Suda, PharmD Kevin W. Garey, PharmD *Baptist
Dexamethasone Compared with Metoclopramide in Prevention of Postoperative Nausea and Vomiting in Orthognathic Surgery
 Article ID: WMC002013 2046-1690 Dexamethasone Compared with Metoclopramide in Prevention of Postoperative Nausea and Vomiting in Orthognathic Surgery Corresponding Author: Dr. Agreta Gashi, Anesthesiologist,
Article ID: WMC002013 2046-1690 Dexamethasone Compared with Metoclopramide in Prevention of Postoperative Nausea and Vomiting in Orthognathic Surgery Corresponding Author: Dr. Agreta Gashi, Anesthesiologist,
Alizaprideand ondansetronin the prevention of postoperative nausea and vomiting: a prospective, randomized, double-blind, placebocontrolled
 Alizaprideand ondansetronin the prevention of postoperative nausea and vomiting: a prospective, randomized, double-blind, placebocontrolled trial. M. Smets N. Van Langenhove G. Dewinter Vrijdagochtendkrans22
Alizaprideand ondansetronin the prevention of postoperative nausea and vomiting: a prospective, randomized, double-blind, placebocontrolled trial. M. Smets N. Van Langenhove G. Dewinter Vrijdagochtendkrans22
Management of Postoperative Nausea and Vomiting in Ambulatory Surgery The Big Little Problem
 Management of Postoperative Nausea and Vomiting in Ambulatory Surgery The Big Little Problem Mary Keyes, MD KEYWORDS Postoperative nausea and vomiting PONV prophylaxis PONV in ambulatory surgery KEY POINTS
Management of Postoperative Nausea and Vomiting in Ambulatory Surgery The Big Little Problem Mary Keyes, MD KEYWORDS Postoperative nausea and vomiting PONV prophylaxis PONV in ambulatory surgery KEY POINTS
Fentanyl-induced cough is a risk factor for postoperative nausea and vomiting
 British Journal of Anaesthesia, 2015, 444 8 doi: 10.1093/bja/aev157 Advance Access Publication Date: 1 June 2015 Clinical Practice Fentanyl-induced cough is a risk factor for postoperative nausea and vomiting
British Journal of Anaesthesia, 2015, 444 8 doi: 10.1093/bja/aev157 Advance Access Publication Date: 1 June 2015 Clinical Practice Fentanyl-induced cough is a risk factor for postoperative nausea and vomiting
post-operative, nausea, vomiting, antiemetics
 Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Guideline for the prevention and treatment of Postoperative
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) Directorate & Speciality Guideline for the prevention and treatment of Postoperative
KEYWORDS Obstetric Patient, Spinal Anesthesia, PONV (Post-Operative Nausea and Vomiting), Inj. Metoclopramide, Inj. Ondansetron.
 PREVENTION OF POSTOPERATIVE NAUSEA AND VOMITING IN ELECTIVE LSCS UNDER SPINAL ANAESTHESIA BY PRE-OPERATIVE ONDANSETRON VERSUS METOCLOPRAMIDE: A PROSPECTIVE SINGLE-BLINDED RANDOMISED CONTROL TRIAL Prasada
PREVENTION OF POSTOPERATIVE NAUSEA AND VOMITING IN ELECTIVE LSCS UNDER SPINAL ANAESTHESIA BY PRE-OPERATIVE ONDANSETRON VERSUS METOCLOPRAMIDE: A PROSPECTIVE SINGLE-BLINDED RANDOMISED CONTROL TRIAL Prasada
IJMDS January 2017; 6(1) Dr Robina Makker Associate professor 2 Dr Amit Bhardwaj
 Original Article Comparative efficacy of ondansetron versus granisetron to prevent perioperative nausea and vomiting in patients undergoing gynaecological surgery under spinal anaesthesia Makker R 1, Bhardwaj
Original Article Comparative efficacy of ondansetron versus granisetron to prevent perioperative nausea and vomiting in patients undergoing gynaecological surgery under spinal anaesthesia Makker R 1, Bhardwaj
Setting The setting was secondary care. The economic study was carried out in the USA.
 The effect of timing of ondansetron administration on its efficacy, cost-effectiveness, and cost-benefit as a prophylactic antiemetic in the ambulatory setting Tang J, Wang B G, White P F, Watcha M F,
The effect of timing of ondansetron administration on its efficacy, cost-effectiveness, and cost-benefit as a prophylactic antiemetic in the ambulatory setting Tang J, Wang B G, White P F, Watcha M F,
Page 1 of 6 PATIENT PRESENTATION PROPHYLAXIS. No risk factors from the categories
 Page 1 of 6 PATIENT PRESENTATION PROPHYLAXIS risk factors from the categories listed below more than one drug prophylaxis (see Appendix A for antiemetic choices) Patient scheduled for surgery Assess patient
Page 1 of 6 PATIENT PRESENTATION PROPHYLAXIS risk factors from the categories listed below more than one drug prophylaxis (see Appendix A for antiemetic choices) Patient scheduled for surgery Assess patient
JMSCR Vol 07 Issue 04 Page April 2019
 www.jmscr.igmpublication.org Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i4.76 A study to compare the antiemetic efficacy of ondansetron
www.jmscr.igmpublication.org Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i4.76 A study to compare the antiemetic efficacy of ondansetron
Automated reminders decrease postoperative nausea and vomiting incidence in a general surgical population
 British Journal of Anaesthesia 108 (6): 961 5 (2012) Advance Access publication 29 February 2012. doi:10.1093/bja/aes024 Automated reminders decrease postoperative nausea and vomiting incidence in a general
British Journal of Anaesthesia 108 (6): 961 5 (2012) Advance Access publication 29 February 2012. doi:10.1093/bja/aes024 Automated reminders decrease postoperative nausea and vomiting incidence in a general
Antiemetic Effect Of Propofol Administered At The End Of Surgery
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 11 Ver. III (November. 2016), PP 54-58 www.iosrjournals.org Antiemetic Effect Of Propofol Administered
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 11 Ver. III (November. 2016), PP 54-58 www.iosrjournals.org Antiemetic Effect Of Propofol Administered
Post-operative nausea and vomiting after gynecologic laparoscopic surgery: comparison between propofol and sevoflurane
 Clinical Research Article Korean J Anesthesiol 2011 January 60(1): 36-40 DOI: 10.4097/kjae.2011.60.1.36 Post-operative nausea and vomiting after gynecologic laparoscopic surgery: comparison between propofol
Clinical Research Article Korean J Anesthesiol 2011 January 60(1): 36-40 DOI: 10.4097/kjae.2011.60.1.36 Post-operative nausea and vomiting after gynecologic laparoscopic surgery: comparison between propofol
Fast Track Surgery and Surgical Carepath in Optimising Colorectal Surgery. R Sim Centre for Advanced Laparoscopic Surgery, TTSH
 Fast Track Surgery and Surgical Carepath in Optimising Colorectal Surgery R Sim Centre for Advanced Laparoscopic Surgery, TTSH Conventional Surgery Postop care Nasogastric tube Enteral feeds when ileus
Fast Track Surgery and Surgical Carepath in Optimising Colorectal Surgery R Sim Centre for Advanced Laparoscopic Surgery, TTSH Conventional Surgery Postop care Nasogastric tube Enteral feeds when ileus
Is Intravenous Ramosetron 0.3 mg Effective In The Prevention Of Postoperative Nausea And Vomiting In Women Undergoing Gynecologic Surgery?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2012 Is Intravenous Ramosetron 0.3 mg Effective
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2012 Is Intravenous Ramosetron 0.3 mg Effective
Postoperative nausea (PON) is a frequent complication
 Efficacy of Acupuncture in Prevention of Postoperative Nausea in Cardiac Surgery Patients Yuliya Korinenko, MD, Ann Vincent, MD, Susanne M. Cutshall, CNS, Zhuo Li, MS, and Thoralf M. Sundt III, MD Mayo
Efficacy of Acupuncture in Prevention of Postoperative Nausea in Cardiac Surgery Patients Yuliya Korinenko, MD, Ann Vincent, MD, Susanne M. Cutshall, CNS, Zhuo Li, MS, and Thoralf M. Sundt III, MD Mayo
Effects of high intraoperative inspired oxygen on postoperative nausea and vomiting in gynecologic laparoscopic surgery
 Thomas Jefferson University Jefferson Digital Commons Department of Anesthesiology Faculty Papers Department of Anesthesiology 11-2010 Effects of high intraoperative inspired oxygen on postoperative nausea
Thomas Jefferson University Jefferson Digital Commons Department of Anesthesiology Faculty Papers Department of Anesthesiology 11-2010 Effects of high intraoperative inspired oxygen on postoperative nausea
TAP blocks vs wound infiltration in laparoscopic colectomies Results of a Randomised Controlled Clinical Trial
 TAP blocks vs wound infiltration in laparoscopic colectomies Results of a Randomised Controlled Clinical Trial Kim Gorissen Frederic Ris Martijn Gosselink Ian Lindsey Dept of Colorectal Surgery Dept of
TAP blocks vs wound infiltration in laparoscopic colectomies Results of a Randomised Controlled Clinical Trial Kim Gorissen Frederic Ris Martijn Gosselink Ian Lindsey Dept of Colorectal Surgery Dept of
Clinical Research INTRODUCTION. Gwieun Yeo 1, Mi Kyoung Lee 1, Heezoo Kim 1, Myounghoon Kong 1, Hyo Jung Son 2, and Han Byeol Oh 2
 Anesth Pain Med 2018;13:256-263 https://doi.org/10.17085/apm.2018.13.3.256 pissn 1975-5171 ㆍ eissn 2383-7977 Clinical Research Received November 17, 2017 Revised 1st, January 29, 2018 2nd, March 15, 2018
Anesth Pain Med 2018;13:256-263 https://doi.org/10.17085/apm.2018.13.3.256 pissn 1975-5171 ㆍ eissn 2383-7977 Clinical Research Received November 17, 2017 Revised 1st, January 29, 2018 2nd, March 15, 2018
Simplified postoperative nausea and vomiting impact scale for audit and post-discharge review
 British Journal of Anaesthesia 108 (3): 423 9 (2012) Advance Access publication 25 January 2012. doi:10.1093/bja/aer505 Simplified postoperative nausea and vomiting impact scale for audit and post-discharge
British Journal of Anaesthesia 108 (3): 423 9 (2012) Advance Access publication 25 January 2012. doi:10.1093/bja/aer505 Simplified postoperative nausea and vomiting impact scale for audit and post-discharge
ISSN X (Print) India. *Corresponding author Dr. D. Shiva Prasad
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(9C):3311-3315 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(9C):3311-3315 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
A Comparative Clinical Study Of Prevention Of PostOperative Nausea And Vomiting Using Granisetron And
 ISPUB.COM The Internet Journal of Anesthesiology Volume 26 Number 1 A Comparative Clinical Study Of Prevention Of PostOperative Nausea And Vomiting Using Granisetron And Ondansetron In Laparoscopic Surgeries.
ISPUB.COM The Internet Journal of Anesthesiology Volume 26 Number 1 A Comparative Clinical Study Of Prevention Of PostOperative Nausea And Vomiting Using Granisetron And Ondansetron In Laparoscopic Surgeries.
Sedation in Children
 CHILDREN S SERVICES Sedation in Children See text for full explanation and drug doses Patient for Sedation Appropriate staffing Resuscitation equipment available Monitoring equipment Patient suitability
CHILDREN S SERVICES Sedation in Children See text for full explanation and drug doses Patient for Sedation Appropriate staffing Resuscitation equipment available Monitoring equipment Patient suitability
MEDICAL POLICY No R0
 TRANSCUTANEOUS ELECTRICAL ACUSTIMULATION (TEAS) FOR HYPEREMESIS GRAVIDARUM Effective Date: November 19, 2010 Review Dates: 10/10, 10/11, 10/12, 10/13, 11/14, 11/15, 11/16 Date Of Origin: October 13, 2010
TRANSCUTANEOUS ELECTRICAL ACUSTIMULATION (TEAS) FOR HYPEREMESIS GRAVIDARUM Effective Date: November 19, 2010 Review Dates: 10/10, 10/11, 10/12, 10/13, 11/14, 11/15, 11/16 Date Of Origin: October 13, 2010
JSLS. Analgesia Following Major Gynecological Laparoscopic Surgery - PCA versus Intermittent Intramuscular Injection
 Analgesia Following Major Gynecological Laparoscopic Surgery - PCA versus Intermittent Intramuscular Injection David M. B. Rosen, Alan M. Lam, Mark A. Carlton, Gregory M. Cario, Lindsay McBride 3 JSLS
Analgesia Following Major Gynecological Laparoscopic Surgery - PCA versus Intermittent Intramuscular Injection David M. B. Rosen, Alan M. Lam, Mark A. Carlton, Gregory M. Cario, Lindsay McBride 3 JSLS
A Cross Sectional Study on Postoperative Nausea and Vomiting Risk Prediction and Assessment in Patients Undergoing Elective Surgical Patients
 ORIGINAL RESEARCH www.ijcmr.com A Cross Sectional Study on Postoperative Nausea and Vomiting Risk Prediction and Assessment in Patients Undergoing Elective Surgical Patients Anu Karthiga Manoharan 1, Nazir
ORIGINAL RESEARCH www.ijcmr.com A Cross Sectional Study on Postoperative Nausea and Vomiting Risk Prediction and Assessment in Patients Undergoing Elective Surgical Patients Anu Karthiga Manoharan 1, Nazir
Comparison of midazolam sedation with or without fentanyl in cataract surgery
 (Acta Anaesth. Belg., 2008, 59, 27-32) Comparison of midazolam sedation with or without fentanyl in cataract surgery O. YALCIN COK (*), A. ERTAN (**) and M. BAHADIR (**) Abstract : We compared the effect
(Acta Anaesth. Belg., 2008, 59, 27-32) Comparison of midazolam sedation with or without fentanyl in cataract surgery O. YALCIN COK (*), A. ERTAN (**) and M. BAHADIR (**) Abstract : We compared the effect
A comparative study of the antiemetic efficacy of dexamethasone, ondansetron, and metoclopramide in patients undergoing gynecological surgery
 Med Sci Monit, 2010; 16(7): CR336-341 PMID: 20581776 WWW.MEDSCIMONIT.COM Clinical Research Received: 2008.04.25 Accepted: 2009.05.31 Published: 2010.07.01 A comparative study of the antiemetic efficacy
Med Sci Monit, 2010; 16(7): CR336-341 PMID: 20581776 WWW.MEDSCIMONIT.COM Clinical Research Received: 2008.04.25 Accepted: 2009.05.31 Published: 2010.07.01 A comparative study of the antiemetic efficacy
Ondansetron, a selective blocking agent of the. Timing of ondansetron administration to prevent postoperative nausea and vomiting
 Timing of ondansetron administration to prevent postoperative nausea and vomiting NORMA I. CRUZ, MD*; PETER PORTILLA, MD ; ROSENDO E. VELA, MD Background: The original guidelines for using ondansetron
Timing of ondansetron administration to prevent postoperative nausea and vomiting NORMA I. CRUZ, MD*; PETER PORTILLA, MD ; ROSENDO E. VELA, MD Background: The original guidelines for using ondansetron
Materials and Methods
 Anesthesiology 2002; 97:1075 81 2002 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Comparative Efficacy of Acustimulation (ReliefBand ) versus Ondansetron (Zofran ) in
Anesthesiology 2002; 97:1075 81 2002 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Comparative Efficacy of Acustimulation (ReliefBand ) versus Ondansetron (Zofran ) in
The Journal of International Medical Research 2011; 39:
 The Journal of International Medical Research 2011; 39: 399 407 A Randomized, Double-blind Trial of Palonosetron Compared with Ondansetron in Preventing Postoperative Nausea and Vomiting after Gynaecological
The Journal of International Medical Research 2011; 39: 399 407 A Randomized, Double-blind Trial of Palonosetron Compared with Ondansetron in Preventing Postoperative Nausea and Vomiting after Gynaecological
Postoperative Nausea and Vomiting: Update on Prevention, Rescue, and Novel Strategies
 Postoperative Nausea and Vomiting: Update on Prevention, Rescue, and Novel Strategies No conflicts of interest to disclose (sadly) 2 March 2016 Melissa Brooks Peterson, MD Department of Anesthesiology/Pediatric
Postoperative Nausea and Vomiting: Update on Prevention, Rescue, and Novel Strategies No conflicts of interest to disclose (sadly) 2 March 2016 Melissa Brooks Peterson, MD Department of Anesthesiology/Pediatric
Hypotension after induction, corrected with 20 mg ephedrine x cc LR EBL 250cc Urine output:
 Terry C. Wicks, CRNA, MHS Catawba Valley Medical Center Hickory, North Carolina 63 y.o., 5 2, 88 kg female for hand assisted laparoscopic tranversecolectomy Co-morbidities include: Hypertension controlled
Terry C. Wicks, CRNA, MHS Catawba Valley Medical Center Hickory, North Carolina 63 y.o., 5 2, 88 kg female for hand assisted laparoscopic tranversecolectomy Co-morbidities include: Hypertension controlled
Show Me the Evidence: Epidurals, PVBs, TAP Blocks Christopher L. Wu, MD Professor of Anesthesiology The Johns Hopkins Hospital
 Show Me the Evidence: Epidurals, PVBs, TAP Blocks Christopher L. Wu, MD Professor of Anesthesiology The Johns Hopkins Hospital Overview Review overall (ERAS and non-eras) data for EA, PVB, TAP Examine
Show Me the Evidence: Epidurals, PVBs, TAP Blocks Christopher L. Wu, MD Professor of Anesthesiology The Johns Hopkins Hospital Overview Review overall (ERAS and non-eras) data for EA, PVB, TAP Examine
Enhanced Recovery after Surgery - A Colorectal Perspective. R Sim Centre for Advanced Laparoscopic Surgery, TTSH
 Enhanced Recovery after Surgery - A Colorectal Perspective R Sim Centre for Advanced Laparoscopic Surgery, TTSH Conventional Surgery Postop care Nasogastric tube Enteral feeds when ileus resolves Opioid
Enhanced Recovery after Surgery - A Colorectal Perspective R Sim Centre for Advanced Laparoscopic Surgery, TTSH Conventional Surgery Postop care Nasogastric tube Enteral feeds when ileus resolves Opioid
NQS Domain: Patient Safety. Measure Type: Process
 Measure Abbreviation: PONV 02 (MIPS 463) *PONV 02 is built to the specification outlined by the Merit Based Incentive Program (MIPS) 463: Prevention of Post-Operative Vomiting (POV) Combination Therapy
Measure Abbreviation: PONV 02 (MIPS 463) *PONV 02 is built to the specification outlined by the Merit Based Incentive Program (MIPS) 463: Prevention of Post-Operative Vomiting (POV) Combination Therapy
Reexamining Metoclopramide s Role in the Prevention of Postoperative Nausea and Vomiting: A Secondary Analysis
 Reexamining Metoclopramide s Role in the Prevention of Postoperative Nausea and Vomiting: A Secondary Analysis Amy J. Masiongale, DNP, CRNA Jane T. Garvin, PhD, RN, FNP-BC Marguerite J. Murphy, DNP, RN
Reexamining Metoclopramide s Role in the Prevention of Postoperative Nausea and Vomiting: A Secondary Analysis Amy J. Masiongale, DNP, CRNA Jane T. Garvin, PhD, RN, FNP-BC Marguerite J. Murphy, DNP, RN
Received: 29/05/2017 Revised: 11/09/2017 Accepted: 26/07/2017 ABSTRACT
 International Journal of Medical Science and Education An official Publication of Association for Scientific and Medical Education (ASME) Original research Article PREOPERATIVE PALONOSETRON AND DEXAMETHASONE
International Journal of Medical Science and Education An official Publication of Association for Scientific and Medical Education (ASME) Original research Article PREOPERATIVE PALONOSETRON AND DEXAMETHASONE
Dexamethasone Compared with Metoclopramide in Prevention of Postoperative Nausea and Vomiting in Orthognathic Surgery
 Article ID: WMC002013 2046-1690 Dexamethasone Compared with Metoclopramide in Prevention of Postoperative Nausea and Vomiting in Orthognathic Surgery Corresponding Author: Dr. Agreta Gashi, Anesthesiologist,
Article ID: WMC002013 2046-1690 Dexamethasone Compared with Metoclopramide in Prevention of Postoperative Nausea and Vomiting in Orthognathic Surgery Corresponding Author: Dr. Agreta Gashi, Anesthesiologist,
If you reduce variability in volume administration, HOW. you can reduce post-surgical complications, LOS and associated costs 1-4
 A large body of clinical evidence* demonstrates If you reduce variability in volume administration, you can reduce post-surgical complications, LOS and associated costs 1-4 Complications Too Dry Too Wet
A large body of clinical evidence* demonstrates If you reduce variability in volume administration, you can reduce post-surgical complications, LOS and associated costs 1-4 Complications Too Dry Too Wet
Intravenous lidocaine infusions. Dr Ian McConachie FRCA FRCPC
 Intravenous lidocaine infusions Dr Ian McConachie FRCA FRCPC Thank the organisers for inviting me. No conflicts or disclosures Lidocaine 1 st amide local anesthetic Synthesized in 1943 by Lofgren in Sweden.
Intravenous lidocaine infusions Dr Ian McConachie FRCA FRCPC Thank the organisers for inviting me. No conflicts or disclosures Lidocaine 1 st amide local anesthetic Synthesized in 1943 by Lofgren in Sweden.
Type of intervention Anaesthesia. Economic study type Cost-effectiveness analysis.
 Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
To staple or to sew. Zeng Xuan Hu
 To staple or to sew Zeng Xuan Hu Fast Track Surgery Multimodal Rehabilitation Accelerated recovery Accelerated rehabilitation Enhanced recovery Optimize perioperative care by reducing the expected stress
To staple or to sew Zeng Xuan Hu Fast Track Surgery Multimodal Rehabilitation Accelerated recovery Accelerated rehabilitation Enhanced recovery Optimize perioperative care by reducing the expected stress
Setting The setting was tertiary care. The economic study appears to have been performed in Heidelberg, Germany.
 Comparative analysis of costs of total intravenous anaesthesia with propofol and remifentanil vs. balanced anaesthesia with isoflurane and fentanyl Epple J, Kubitz J, Schmidt H, Motsch J, Bottiger B W,
Comparative analysis of costs of total intravenous anaesthesia with propofol and remifentanil vs. balanced anaesthesia with isoflurane and fentanyl Epple J, Kubitz J, Schmidt H, Motsch J, Bottiger B W,
I ve Got You Under My Skin: A Comparison of IV and s/c PCA. Nick Williamson Clinical Nurse Specialist
 I ve Got You Under My Skin: A Comparison of IV and s/c PCA Nick Williamson Clinical Nurse Specialist How did PCA get under my skin? Started in 2009 when I started working at KCH Subcut PCA!!! PCA refers
I ve Got You Under My Skin: A Comparison of IV and s/c PCA Nick Williamson Clinical Nurse Specialist How did PCA get under my skin? Started in 2009 when I started working at KCH Subcut PCA!!! PCA refers
Postoperative nausea and vomiting prophylaxis: The efficacy of a novel antiemetic drug (palonosetron) combined with dexamethasone
 Egyptian Journal of Anaesthesia (2013) 29, 117 123 Egyptian Society of Anesthesiologists Egyptian Journal of Anaesthesia www.elsevier.com/locate/egja www.sciencedirect.com Research Article Postoperative
Egyptian Journal of Anaesthesia (2013) 29, 117 123 Egyptian Society of Anesthesiologists Egyptian Journal of Anaesthesia www.elsevier.com/locate/egja www.sciencedirect.com Research Article Postoperative
Dhawal R. Wadaskar*, Jyoti S. Magar, Bharati A. Tendolkar
 International Journal of Research in Medical Sciences Wadaskar DR et al. Int J Res Med Sci. 2016 Aug;4(8):3191-3197 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162214
International Journal of Research in Medical Sciences Wadaskar DR et al. Int J Res Med Sci. 2016 Aug;4(8):3191-3197 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162214
Intro Who should read this document 2 Key practice points 2 What is new in this version 3 Background 3 Guideline Subsection headings
 Enhanced Recovery for Major Urology and Gynaecological Classification: Clinical Guideline Lead Author: Dr Dominic O Connor Additional author(s): Jane Kingham Authors Division: Anaesthesia Unique ID: DDCAna3(12)
Enhanced Recovery for Major Urology and Gynaecological Classification: Clinical Guideline Lead Author: Dr Dominic O Connor Additional author(s): Jane Kingham Authors Division: Anaesthesia Unique ID: DDCAna3(12)
J Med Assoc Thai 2016; 99 (5): Full text. e-journal:
 A Randomized Placebo-Controlled Trial of Oral Ramosetron for Prevention of Post Operative Nausea and Vomiting after Intrathecal Morphine in Patients Undergoing Gynecological Surgery Suratsawadee Wangnamthip
A Randomized Placebo-Controlled Trial of Oral Ramosetron for Prevention of Post Operative Nausea and Vomiting after Intrathecal Morphine in Patients Undergoing Gynecological Surgery Suratsawadee Wangnamthip
Evaluation of postural stability after low-dose droperidol in outpatients undergoing gynaecological dilatation and curettage procedure
 British Journal of Anaesthesia 88 (6): 819±23 (2002) Evaluation of postural stability after low-dose droperidol in outpatients undergoing gynaecological dilatation and curettage procedure D. Song, F. Chung*,
British Journal of Anaesthesia 88 (6): 819±23 (2002) Evaluation of postural stability after low-dose droperidol in outpatients undergoing gynaecological dilatation and curettage procedure D. Song, F. Chung*,
A randomised, double-blind, parallel group, multicentre study to compare the tolerability, safety, and efficacy of oxycodone with morphine in
 A randomised, double-blind, parallel group, multicentre study to compare the tolerability, safety, and efficacy of oxycodone with morphine in patients using i.v. patient-controlled analgesia (PCA) for
A randomised, double-blind, parallel group, multicentre study to compare the tolerability, safety, and efficacy of oxycodone with morphine in patients using i.v. patient-controlled analgesia (PCA) for
Cost-effectiveness of ondansetron for postoperative nausea and vomiting
 Cost-effectiveness of ondansetron for postoperative nausea and vomiting M. R. Tramèr, 1 * C. Phillips, 2 D. J. M. Reynolds, 3 H. J. McQuay 1 and R. A. Moore 1 1 Pain Research, Nuffield Department of Anaesthetics,
Cost-effectiveness of ondansetron for postoperative nausea and vomiting M. R. Tramèr, 1 * C. Phillips, 2 D. J. M. Reynolds, 3 H. J. McQuay 1 and R. A. Moore 1 1 Pain Research, Nuffield Department of Anaesthetics,
Post-operative Analgesia for Caesarean Section
 Post-operative Analgesia for Caesarean Section Introduction Good quality analgesia after any surgery leads to earlier mobilisation, fewer pulmonary and cardiac complications, a reduced risk of DVT and
Post-operative Analgesia for Caesarean Section Introduction Good quality analgesia after any surgery leads to earlier mobilisation, fewer pulmonary and cardiac complications, a reduced risk of DVT and
ORIGINAL ARTICLE INTRODUCTION
 ORIGINAL ARTICLE The Efficacy of Propofol vs. Subcutaneous Sumatriptan for Treatment of Acute Migraine Headaches in the Emergency Department: A Double-Blinded Clinical Trial Hossein Moshtaghion, MD*; Najmeh
ORIGINAL ARTICLE The Efficacy of Propofol vs. Subcutaneous Sumatriptan for Treatment of Acute Migraine Headaches in the Emergency Department: A Double-Blinded Clinical Trial Hossein Moshtaghion, MD*; Najmeh
CONSORT 2010 checklist of information to include when reporting a randomised trial*
 Supplemental Figures for: Ramosetron Versus Ondansetron in Combination with Aprepitant and Dexamethasone for the Prevention of Highly Emetogenic Chemotherapy-induced Nausea and Vomiting: A Multicenter,
Supplemental Figures for: Ramosetron Versus Ondansetron in Combination with Aprepitant and Dexamethasone for the Prevention of Highly Emetogenic Chemotherapy-induced Nausea and Vomiting: A Multicenter,
Laparoscopic Cholecystectomy as a Day Surgery Procedure
 Anaesth Intens Care 1996; 24: 231-236 Laparoscopic Cholecystectomy as a Day Surgery Procedure R. J. SINGLETON*, G. E. RUDKIN, G. A. OSBORNE, D. S. WATKIN, J. A. R. WILLIAMS** Department of Anaesthesia
Anaesth Intens Care 1996; 24: 231-236 Laparoscopic Cholecystectomy as a Day Surgery Procedure R. J. SINGLETON*, G. E. RUDKIN, G. A. OSBORNE, D. S. WATKIN, J. A. R. WILLIAMS** Department of Anaesthesia
LOW DOSE INTRAVENOUS MIDAZOLAM FOR PREVENTION OF PONV, IN LOWER ABDOMINAL SURGERY
 LOW DOSE INTRAVENOUS MIDAZOLAM FOR PREVENTION OF PONV, IN LOWER ABDOMINAL SURGERY - Preoperative vs Intraoperative Administration - Mohammad Reza Safavi * and Azim Honarmand ** Abstract Background: The
LOW DOSE INTRAVENOUS MIDAZOLAM FOR PREVENTION OF PONV, IN LOWER ABDOMINAL SURGERY - Preoperative vs Intraoperative Administration - Mohammad Reza Safavi * and Azim Honarmand ** Abstract Background: The
Antiemetic and analgesic-sparing effects of diphenhydramine added to morphine intravenous patient-controlled analgesia
 British Journal of Anaesthesia 94 (6): 835 9 (2005) doi:10.1093/bja/aei137 Advance Access publication April 15, 2005 Antiemetic and analgesic-sparing effects of diphenhydramine added to morphine intravenous
British Journal of Anaesthesia 94 (6): 835 9 (2005) doi:10.1093/bja/aei137 Advance Access publication April 15, 2005 Antiemetic and analgesic-sparing effects of diphenhydramine added to morphine intravenous
General anesthetics. Dr. Shamil AL-Noaimy Lecturer of Pharmacology Dept. of Pharmacology College of Medicine
 General anesthetics Dr. Shamil AL-Noaimy Lecturer of Pharmacology Dept. of Pharmacology College of Medicine Rationale General anesthesia is essential to surgical practice, because it renders patients analgesic,
General anesthetics Dr. Shamil AL-Noaimy Lecturer of Pharmacology Dept. of Pharmacology College of Medicine Rationale General anesthesia is essential to surgical practice, because it renders patients analgesic,
Music medicine: A post-operative adjunct
 Music medicine: A post-operative adjunct Anesthesia Research Rounds January 8 th, 2013 Aaron Lau CC3 Marko Erak CC3 Outline Overview of current literature Identified research opportunity Proposed pilot
Music medicine: A post-operative adjunct Anesthesia Research Rounds January 8 th, 2013 Aaron Lau CC3 Marko Erak CC3 Outline Overview of current literature Identified research opportunity Proposed pilot
SINGLE BREATH INDUCTION OF ANAESTHESIA WITH ISOFLURANE
 Br. J. Anaesth. (987), 59, 24-28 SINGLE BREATH INDUCTION OF ANAESTHESIA WITH ISOFLURANE J. M. LAMBERTY AND I. H. WILSON Two studies have demonstrated that the induction of anaesthesia using a single breath
Br. J. Anaesth. (987), 59, 24-28 SINGLE BREATH INDUCTION OF ANAESTHESIA WITH ISOFLURANE J. M. LAMBERTY AND I. H. WILSON Two studies have demonstrated that the induction of anaesthesia using a single breath
Efficacy of Prophylactic Ondansetron in a Patient-controlled Analgesia Environment
 The Journal of International Medical Research 2004; 32: 160 165 Efficacy of Prophylactic Ondansetron in a Patient-controlled Analgesia Environment SH HAN, YJ LIM, YJ RO, SC LEE, YS PARK AND YC KIM Department
The Journal of International Medical Research 2004; 32: 160 165 Efficacy of Prophylactic Ondansetron in a Patient-controlled Analgesia Environment SH HAN, YJ LIM, YJ RO, SC LEE, YS PARK AND YC KIM Department
Comparison of surgical site and patient s history with a simplified risk score for the prediction of postoperative nausea and vomiting
 Comparison of surgical site and patient s history with a simplified risk score for the prediction of postoperative nausea and vomiting C. C. Apfel, 1,2 P. Kranke 2 and L. H. J. Eberhart 3 1 Department
Comparison of surgical site and patient s history with a simplified risk score for the prediction of postoperative nausea and vomiting C. C. Apfel, 1,2 P. Kranke 2 and L. H. J. Eberhart 3 1 Department
COBISS.SR-ID EFFECTIVNESS OF DEXAMETASONE VS. MAGNESIUM SULPHATE IN POSTOPERA- TIVE ANALGESIA (DEXAMETASONE VS. MAGNESIUM SULPHATE)
 COBISS.SR-ID 222299404 616-089.5-06:616.33-008.3 615.243.6 Original article EFFECTIVNESS OF DEXAMETASONE VS. MAGNESIUM SULPHATE IN POSTOPERA- TIVE ANALGESIA (DEXAMETASONE VS. MAGNESIUM SULPHATE) Brikena
COBISS.SR-ID 222299404 616-089.5-06:616.33-008.3 615.243.6 Original article EFFECTIVNESS OF DEXAMETASONE VS. MAGNESIUM SULPHATE IN POSTOPERA- TIVE ANALGESIA (DEXAMETASONE VS. MAGNESIUM SULPHATE) Brikena
Randomized Controlled Trial of Bisacodyl Suppository Versus Placebo for Postoperative Ileus After Elective Colectomy for Colon Cancer
 Original Article Randomized Controlled Trial of Bisacodyl Suppository Versus Placebo for Postoperative Ileus After Elective Colectomy for Colon Cancer Sukanya Wiriyakosol, Youwanuch Kongdan, Chakrapan
Original Article Randomized Controlled Trial of Bisacodyl Suppository Versus Placebo for Postoperative Ileus After Elective Colectomy for Colon Cancer Sukanya Wiriyakosol, Youwanuch Kongdan, Chakrapan
Fast-track surgery and anaesthesia
 Andrew J Kitching FRCA Sarah S O Neill FRCA Major surgery induces profound physiological responses; frequent sequelae include pain, nausea, ileus, increased cardiac demands, and impaired pulmonary function.
Andrew J Kitching FRCA Sarah S O Neill FRCA Major surgery induces profound physiological responses; frequent sequelae include pain, nausea, ileus, increased cardiac demands, and impaired pulmonary function.
Setting Department of Gynecology and Obstetrics, Cleveland Clinic Foundation (tertiary care academic centre), USA.
 Prospective randomized clinical trial of laparoscopically assisted vaginal hysterectomy versus total abdominal hysterectomy Falcone T, Paraiso M F, Mascha E Record Status This is a critical abstract of
Prospective randomized clinical trial of laparoscopically assisted vaginal hysterectomy versus total abdominal hysterectomy Falcone T, Paraiso M F, Mascha E Record Status This is a critical abstract of
Factors Contributing to a Prolonged Stay After Ambulatory Surgery
 Factors Contributing to a Prolonged Stay After Ambulatory Surgery Frances Chung, FRCPC, and Gabor Mezei, MD, PhD Department of Anesthesia, Toronto Western Hospital, University of Toronto, Toronto, Ontario,
Factors Contributing to a Prolonged Stay After Ambulatory Surgery Frances Chung, FRCPC, and Gabor Mezei, MD, PhD Department of Anesthesia, Toronto Western Hospital, University of Toronto, Toronto, Ontario,
COMPARISON OF INDUCTION WITH SEVOFLURANE-FENTANYL AND PROPOFOL-FENTANYL ON POSTOPERATIVE NAUSEA AND VOMITING AFTER LAPAROSCOPIC SURGERY
 RESEARCH ARTICLE COMPARISON OF INDUCTION WITH SEVOFLURANE-FENTANYL AND PROPOFOL-FENTANYL ON POSTOPERATIVE NAUSEA AND VOMITING AFTER LAPAROSCOPIC SURGERY ABSTRACT Ghanta.V. Nalini Kumari 1,*, Sushma Ladi
RESEARCH ARTICLE COMPARISON OF INDUCTION WITH SEVOFLURANE-FENTANYL AND PROPOFOL-FENTANYL ON POSTOPERATIVE NAUSEA AND VOMITING AFTER LAPAROSCOPIC SURGERY ABSTRACT Ghanta.V. Nalini Kumari 1,*, Sushma Ladi
The management of acute surgical pain has
 Intravenous Dexamethasone as an Analgesic: A Literature Review Sean G. Moore, MSN, CRNA The management of pain in surgical patients has shifted in recent years from a technique grounded in opioid administration,
Intravenous Dexamethasone as an Analgesic: A Literature Review Sean G. Moore, MSN, CRNA The management of pain in surgical patients has shifted in recent years from a technique grounded in opioid administration,
Effects of IV Ondansetron during spinal anaesthesia with Ropivacaine and Fentanyl
 Original article Effects of IV Ondansetron during spinal anaesthesia with Ropivacaine and Fentanyl 1Dr Bipul Deka, 2 Dr Bharat Talukdar, 3 Dr. Amal Kumar Laha, 4 Dr. Rupak Bhattacharjee 1Assistant Professor,
Original article Effects of IV Ondansetron during spinal anaesthesia with Ropivacaine and Fentanyl 1Dr Bipul Deka, 2 Dr Bharat Talukdar, 3 Dr. Amal Kumar Laha, 4 Dr. Rupak Bhattacharjee 1Assistant Professor,
Randomized controlled trial of the effect of depth of anaesthesia on postoperative pain
 British Journal of Anaesthesia Page 1 of 6 doi:10.1093/bja/aet419 BJA Advance Access published December 8, 13 Randomized controlled trial of the effect of depth of anaesthesia on postoperative pain C.
British Journal of Anaesthesia Page 1 of 6 doi:10.1093/bja/aet419 BJA Advance Access published December 8, 13 Randomized controlled trial of the effect of depth of anaesthesia on postoperative pain C.
ERAS: Enhanced Recovery After Surgery. Christopher L. Wu, M.D. Professor of Anesthesiology The Johns Hopkins University; Baltimore, Maryland
 ERAS: Enhanced Recovery After Surgery Christopher L. Wu, M.D. Professor of Anesthesiology The Johns Hopkins University; Baltimore, Maryland Overview History and basic principles of ERAS Review published
ERAS: Enhanced Recovery After Surgery Christopher L. Wu, M.D. Professor of Anesthesiology The Johns Hopkins University; Baltimore, Maryland Overview History and basic principles of ERAS Review published
Evaluation of Postoperative Complications Occurring in Patients after Desflurane or Sevoflurane in Outpatient Anaesthesia: A Comparative Study
 Original article Evaluation of Postoperative Complications Occurring in Patients after Desflurane or Sevoflurane in Outpatient Anaesthesia: A Comparative Study Shishir Ramachandra Sonkusale 1, RajulSubhash
Original article Evaluation of Postoperative Complications Occurring in Patients after Desflurane or Sevoflurane in Outpatient Anaesthesia: A Comparative Study Shishir Ramachandra Sonkusale 1, RajulSubhash
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Process-High Priority
 Quality ID #463: Prevention of Post-Operative Vomiting (POV) Combination Therapy (Pediatrics) National Quality Strategy Domain: Patient Safety Meaningful Measure Area: Preventive Care 2019 COLLECTION TYPE:
Quality ID #463: Prevention of Post-Operative Vomiting (POV) Combination Therapy (Pediatrics) National Quality Strategy Domain: Patient Safety Meaningful Measure Area: Preventive Care 2019 COLLECTION TYPE:
Does Anesthesia influence Cancer recurrence? Dr Ian McConachie FRCA FRCPC London, ON, Canada
 Does Anesthesia influence Cancer recurrence? Dr Ian McConachie FRCA FRCPC London, ON, Canada Why did my cancer come back? Inadequate resection Micro metastases Lymph spread Tumour biology Immune system
Does Anesthesia influence Cancer recurrence? Dr Ian McConachie FRCA FRCPC London, ON, Canada Why did my cancer come back? Inadequate resection Micro metastases Lymph spread Tumour biology Immune system
A SAFE AND EFFECTIVE WAY TO OPTIMIZE ANESTHESIA DURING SURGERY
 Clinical Evidence Guide A SAFE AD EFFECTIVE WAY TO OPTIMIZE AESTHESIA DURIG SURGERY Bispectral Index (BIS) Complete Monitoring System This guide will help you review the clinical evidence that supports
Clinical Evidence Guide A SAFE AD EFFECTIVE WAY TO OPTIMIZE AESTHESIA DURIG SURGERY Bispectral Index (BIS) Complete Monitoring System This guide will help you review the clinical evidence that supports
Update Update on Anaesthesia for c-section Dr Kerry Litchfield Consultant Anaesthetist Princess Royal Maternity Glasgow, Scotland
 Update Update on Anaesthesia for c-section Dr Kerry Litchfield Consultant Anaesthetist Princess Royal Maternity Glasgow, Scotland Caesarean section is the most common surgical procedure in the world 1
Update Update on Anaesthesia for c-section Dr Kerry Litchfield Consultant Anaesthetist Princess Royal Maternity Glasgow, Scotland Caesarean section is the most common surgical procedure in the world 1
